Abstract
The Rotterdam Study is a prospective cohort study ongoing since 1990 in the city of Rotterdam in The Netherlands. The study targets cardiovascular, endocrine, hepatic, neurological, ophthalmic, psychiatric, dermatological, oncological, and respiratory diseases. As of 2008, 14,926 subjects aged 45 years or over comprise the Rotterdam Study cohort. The findings of the Rotterdam Study have been presented in over a 1,000 research articles and reports (see www.erasmus-epidemiology.nl/rotterdamstudy). This article gives the rationale of the study and its design. It also presents a summary of the major findings and an update of the objectives and methods.
Similar content being viewed by others
Avoid common mistakes on your manuscript.
Introduction
The Rotterdam Study was designed in the mid-1980s as a response to the demographic changes that were leading to an increase of the proportion of elderly people in most populations [1]. It was clear that this would produce a strong rise in elderly people living with diseases, as most diseases cluster at the end of life, and that to discover the causes of diseases in the elderly one would have to study risk factors of those diseases [2]. A major approach to finding causes is the prospective follow-up study, which has proven quite effective in finding causes of heart disease and cancer.
The design of the Rotterdam Study
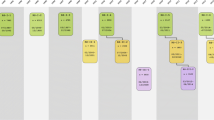
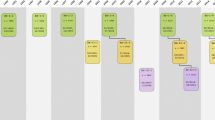
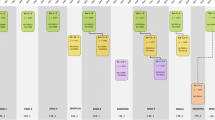
The design of the Rotterdam Study is that of a prospective cohort study among, initially, 7,983 persons living in the well-defined Ommoord district in the city of Rotterdam in The Netherlands (78% of 10,215 invitees). They were all 55 years of age or over and the oldest participant at the start was 106 years [3]. The study started with a pilot phase in the second half of 1989. From January 1990 onwards participants were recruited for the Rotterdam Study. Figure 1 gives a diagram of the various cycles in the study. In 2000, 3,011 participants (out of 4,472 invitees) who had become 55 years of age or moved into the study district since the start of the study were added to the cohort. In 2006, a further extension of the cohort was initiated in which 3,932 subjects were included, aged 45–54 years, out of 6,057 invited, living in the Ommoord district. By the end of 2008, the Rotterdam Study therefore comprised 14,926 subjects aged 45 years or over [4, 5]. The overall response figure for all three cycles at baseline was 72.0% (14,926 of 20,744).
Diagram of examination cycles of the Rotterdam Study (RS). RS-I-1 refers to the baseline examination of the original cohort (pilot phase 07/1989–12/1989; cohort recruitment 01/1990–09/1993). RS-I-2, RS-I-3, RS-I-4, and RS-I-5 refer to re-examination of the original cohort members. RS-II-1 refers to the extension of the cohort with persons in the study district that became 55 years since the start of the study or those of 55 years or over that migrated into the study district. RS-II-2 refers to re-examination of the extension cohort. RS-III-1 refers to the baseline examination of all persons aged 45 years and over living in the study district that had not been examined (i.e., mainly comprising those aged 45–60 years). RS-II-3 and RS-III-2 refer to ongoing and future re-examinations. Examination RS-I-4 and RS-II-2 were conducted as one project and feature an identical research program. Similarly, examinations RS-I-5, RS-II-3, and RS-III-2 will share the same program items
The participants were all examined in some detail at baseline. They were interviewed at home (2 h) and then had an extensive set of examinations (a total of 5 h) in a specially built research facility in the centre of their district. These examinations focussed on possible causes of invalidating diseases in the elderly in a clinically state-of-the-art manner, as far as the circumstances allowed. The emphasis was put on imaging (of heart, blood vessels, eyes, skeleton and later brain) and on collecting bodily fluids that enabled further in-depth molecular and genetic analyses. These examinations were repeated every 3–4 years in characteristics that could change over time. And so there were examination cycles from 1990 to 1993, from 1993 to 1995, from 1997 to 1999, from 2000 to 2001, from 2002 to 2004, from 2004 to 2005, from 2006 to 2008, and from 2009 to January 2011 (Fig. 1). In February 2011 the third examination cycle for the second cohort (RS-II-3) was started.
The participants in the Rotterdam Study are followed for a variety of diseases that are frequent in the elderly (and many are also in the not so elderly): coronary heart disease, heart failure and stroke, Parkinson disease, Alzheimer disease and other dementias, depression and anxiety disorders, macular degeneration and glaucoma, respiratory diseases, liver diseases, diabetes mellitus, osteoporosis, dermatological diseases and cancer. The Rotterdam Study has been approved by the institutional review board (Medical Ethics Committee) of the Erasmus Medical Center and by the review board of The Netherlands Ministry of Health, Welfare and Sports. The approval has been renewed every 5 years, as well as with the introduction of major new elements in the study (e.g., MRI investigations).
In the remainder of this article the objectives and major findings will be presented with an update of the research methods for cardiovascular diseases, dermatological diseases, endocrine diseases, liver diseases, neurological diseases, ophthalmic diseases, psychiatric diseases, respiratory diseases, as well as for genetic and biomarker studies and for pharmaco-epidemiologic studies. For relevant recent EJE references see [6–32].
Cardiovascular diseases
Objectives
Research on the epidemiology of cardiovascular disease focuses on the etiology and prediction of coronary heart disease and on cardiovascular conditions at older age, like heart failure and atrial fibrillation. Putative risk factors include three groups, endocrine factors, factors involved in hemostasis, inflammation and endothelial function, and genetic risk factors. A major focus is on non-invasive assessment of atherosclerosis to improve prediction of coronary heart disease, including measurement of coronary calcium with electron-beam and multi-detection CT and carotid plaque characterization by high-resolution MRI. Cerebrovascular diseases, including stroke, are also investigated in the Rotterdam Study. They are described under Neurological diseases.
Major findings
Recognized and unrecognized myocardial infarction
We found that a high proportion of incident myocardial infarctions remains clinically unrecognized. The incidence rate of recognized myocardial infarction in the Rotterdam Study was 5.0 per 1,000 person years. The incidence was higher in men (8.4) than in women (3.1). The incidence rate of unrecognized infarction was 3.8 per 1,000 person years. Men (4.2) and women (3.6) had approximately similar incidence. Hence, the proportion of unrecognized infarction is lower in men (33%) than in women (54%) [33].
Cardiovascular risk factors
Endocrine, inflammatory and hemostatic factors and risk of coronary heart disease were addressed in several studies. Subclinical hypothyroidism was an independent risk factor of atherosclerosis and myocardial infarction in older women [34]. Recently, we showed that amino-terminal pro-B-type natriuretic peptide (NT-ProBNP) improved cardiovascular and cerebrovascular risk prediction in an older population [35]. Plasma C-Reactive protein (CRP) and lipoprotein-associated phospholipase A2 (Lp-PLA2) activity were independent predictors of coronary heart disease [36, 37]. Early findings included the association of tissue plasminogen activator (TPA) with incident coronary heart disease [38].
Non-invasive measures of atherosclerosis
Multiple studies focused on the predictive value of non-invasive measures of atherosclerosis for risk of coronary heart disease. Strong associations with risk of coronary heart disease were found for carotid intima-media thickness [39], pulse wave velocity [40], and coronary calcification as assessed by electron-beam CT [41]. The relatively crude measures directly assessing plaques in the carotid artery and abdominal aorta predict coronary heart disease equally well as the more precisely measured carotid intima-media thickness [42]. In subjects at intermediate risk of cardiovascular disease, coronary calcium scoring proved to be a powerful method to reclassify persons into more appropriate risk categories [43].
Genetic studies
Genetic studies included candidate gene studies [44] and more recently genome-wide association studies of clinical disease and risk factor phenotypes. Genome-wide association studies are primarily conducted in the context of the Cohorts for Heart and Aging Research in Genomic Epidemiology (CHARGE) Consortium [45] of which major findings are reported here. We identified 3 genetic loci associated with uric acid concentration and gout [46]. We also identified a significant association between chronic kidney disease and the UMOD gene which encodes Tamm-Horsfall protein [47]. In the same consortium, we found four genes for systolic blood pressure, six for diastolic blood pressure and one for hypertension [48]. We found multiple loci that influenced erythrocyte phenotypes in the CHARGE Consortium [49]. Recently, we identified 18 loci for CRP levels in a meta-analysis in more than 80,000 individuals from 25 studies. The study highlighted immune response and metabolic regulatory pathways involved in the regulation of chronic inflammation [50]. Novel associations of multiple genetic loci with plasma levels of factor VII, factor VIII, and von Willebrand factor were also detected [51].
Heart failure and atrial fibrillation
The Rotterdam Study enabled accurate assessment of the incidence and lifetime risk of heart failure and atrial fibrillation in an elderly population [52, 53]. It was shown that inflammation is associated with risk of heart failure [54]. Subclinical atherosclerosis, cigarette smoking and high-normal thyroid function were identified as new risk factors of atrial fibrillation [55–57]. In a large collaborative study as part of the CHARGE consortium, we investigated the genetic variation responsible for 6 traits related to cardiac structure and function. We found two replicated loci for left ventricular dimension and 5 replicated loci for aortic root size [58]. Another topic of interest was the search for genetic determinants of several rhythm and conduction disturbances on the ECG, notably RR-interval, QRS, and QT(c) interval, as well as PR-interval and atrial fibrillation, and sudden cardiac death. For example, we identified several new loci for PR interval [59] and a new gene (ZFHX3) associated with atrial fibrillation [60] in a meta-analysis of studies of the CHARGE consortium.
Methods update
Cardiovascular risk factors
Three groups of putative risk factors for cardiovascular conditions are examined. The first are endocrine factors, including diabetes, sex hormones, thyroid gland and adrenal gland hormones and natriuretic peptides (e.g. [34, 35, 61]. The second group comprises factors involved in hemostasis, inflammation and endothelial function (e.g. [36–38]. The third group, and currently a major focus, covers genetic factors in these areas. In addition to the candidate gene approach, studies are more recently conducted through the genome-wide association approach (e.g. [46–51]. In genome-wide association studies, data from the Rotterdam Study are often combined with those from other studies in the context of the large collaborative CHARGE consortium [45].
Non-invasive measures of atherosclerosis
At baseline and follow-up examinations, ultrasonographic assessments of carotid intima-media thickness and carotid plaques were conducted in all subjects [39]. At these examinations, also measurements of the ankle-brachial index and aortic calcification (on X-rays of the lumbar spine) were performed [42]. Carotid-femoral pulse wave velocity, a measure of aortic stiffness, was measured in all subjects of RS-I-3 and RS-II-1 with an automatic device (CompliorArtech Medicla) [40]. Measurements of coronary calcification by electron-beam CT and more recently by multi-detector CT (MDCT) were conducted from 1997 onwards in RS-I and RS-II [41, 43]. From 2003 to 2006, MDCT was also used to quantify calcification in the aortic arch and carotid arteries in RS-I and RS-II. Measurement of carotid plaque components with high-resolution MRI started in October 2007 and will be continued until performance is completed in all subjects with carotid wall thickening from RS-I, RS-II and RS-III.
Electrocardiographic, echocardiographic and other ultrasound measurements
At every exam, 12-lead resting ECGs are made and processed by the Modular ECG Analysis System (MEANS) to obtain a series of ECG measurements [62]. Abdominal aortic diameters were measured by ultrasound at baseline. From 2002 onwards (RS-I-4), repeated ultrasonographic measurements are conducted of structural and functional parameters of the left ventricle and atrium [63]. From 2009 (RS-I-5), measurements of structure and function of the right side of the heart are also performed to diagnose subclinical pulmonary hypertension.
Clinical follow-up
Data on clinical cardiovascular outcomes are collected through an automated follow-up system. The follow-up system involves linkage of the study base to files from general practitioners in the study area and subsequent collection of information from letters of medical specialists and discharge reports in case of hospitalisation. With respect to the vital status of participants, information is also obtained regularly from the municipal health authorities in Rotterdam. After notification, cause and circumstances of death are established by questionnaire from the general practitioners. Clinical cardiovascular outcomes are coded by study physicians and medical experts in the field according to the International Classification of Diseases, 10th edition (ICD-10). Incident coronary heart disease is defined as the occurrence of a fatal or nonfatal myocardial infarction (I21), other forms of acute (I24) or chronic ischemic (I25) heart disease, sudden (cardiac) death (I46 and R96), death caused by ventricular fibrillation (I49), or death resulting from congestive heart failure (I50) during follow-up [37]. Other outcomes include heart failure [52] and atrial fibrillation [53]. For additional EJE references concerning cardiovascular disease see [64–111].
Dermatological diseases
Objectives
Dermatoepidemiologic research in the Rotterdam Study focuses on the frequency of the most common skin conditions as well as on genetic and environmental factors associated with these skin diseases. The emphasis of the skin component is on cutaneous malignancies such as basal and squamous cell carcinomas (BCC and SCC, respectively) and their precursor lesions, and inflammatory dermatoses such as eczema and psoriasis. In addition to skin diseases, we examine the contribution of genetics and environmental exposures to the skin fenotype (e.g., skin pigmentation, wrinkling and photodamage) of the cohort members.
Methods
In 2010, dermatology was introduced in the Rotterdam Study. To the home interview several items have been added questioning ultraviolet light exposure, history of (personal and familial) psoriasis, history of skin cancer, the diagnostic criteria of British association of dermatology for atopic eczema, adjusted diagnostic criteria for psoriatic arthritis.
A full body skin examination by physicians trained in dermatology with a focus on the most common skin diseases is the core contribution of dermatology. The clinical presence and extent of specific skin diseases (i.e., actinic keratosis, malignancies, psoriasis, xerosis, hand and flexural eczema, alopecia, and signs of chronic venous insufficiency based on the ‘C’ of the CEAP classification) at time of examination is assessed in a standardized fashion. Other dermatological diseases will just be noted.
The extent of facial photodamage and wrinkling are scored using a validated photonumeric scale and the Glogau scale, respectively. The Norwood-Hamilton classification and the Ludwig classification is used for male and female pattern hair loss, respectively. Fully standardized 3-dimensional photographs (Premier 3dMDface3-plus UHD, Atlanta, USA) of the face are taken to further assess skin characteristics. The pigmentation of the facial skin and at the inner side of the upper arm are measured using a spectrophotometer (Konica Minolta Sensing, spectrophotometer CM-700d, Singapore). In a subgroup of the cohort, skin topography measures will be taken at the inner side of the upper arm as well.
As for other cancers, pathology data of the cutaneous malignancies is obtained from a network of pathology laboratories in Rotterdam and its surroundings and the Dutch pathology database (PALGA). In a further attempt to identify cohort members with psoriasis, medical files and dispenses at pharmacies will be studied.
Major findings
The prevalence of single and multiple BCC was studied in the Rotterdam Study and showed that a total of 524 patients (4.8% of included population) had developed this type of keratinocytic cancer and that 31.1% had developed more than one tumor during observation [112]. A multi-failure survival model suggested that people with red hair and higher levels of education, and those who had their first BCC at younger age were significantly more likely to develop multiple malignancies. In a candidate gene approach, Vitamin D-binding protein (VDBP) genotype was not associated with (multiple) BCC development, except possibly in the youngest age-group (A/T variant of rs7041 was associated with; adjusted HR = 1.88, 95% CI 1.10–3.20), whereas homozygote Gc1s carriers had a significantly lower BCC risk; adjusted HR = 0.53, 95% CI 0.31–0.91) [113].
In a pharmaco-epdemiologic study, the hypothesis that (prior) exposure to drugs such as high-ceiling diuretics increase skin cancer risk due to enhanced photosensitivity of the skin was tested. In line with the hypothesis, use of potassium sparing and thiazide agents were not and use of high-ceiling diuretics was associated with an increased hazard of BCC (highest quartile compared to non users; HR 1.6, 95% CI 1.1–2.4).
Endocrine diseases
Objectives
The main objective of the programme of endocrine epidemiology research is to study frequency and etiology of major disorders of the endocrine glands (pituitary, reproductive, thyroid, parathyroid, adrenal, and neuro-endocrine pancreas) and the musculoskeletal system. These include endocrine and locomotor diseases, including diabetes mellitus, osteoporosis, osteoarthritis, growth-hormone deficiency, hypo- and hyper-thyroidism and parathyroidism. The evaluation of risk factors for the above mentioned conditions includes serum measurements (such as classical hormones and other endocrine molecules) and genetic determinants of endocrine factors and signalling pathways.
Major findings
We have provided epidemiological documentation on the hormone, growth factor and biomarker profiles in the general population and determined the association with several diseases. Within the topics of locomotor diseases and disability we have reported that heart failure, COPD, diabetes mellitus and chronic disorders leading to locomotor complaints, are risk factors which contribute considerably to locomotor disability [114, 115]. In relation to osteoporosis we have determined the incidence of vertebral [116] and non-vertebral fractures [117], and the relationship between bone mineral density (BMD), BMD change and the occurrence of fracture [117], as well as with heel ultrasound measurements [118] and bone resorption markers [119]. We have also studied the relation between endogenous sex hormones and their binding factors, with fractures [120], and showed that increased homocysteine levels are a strong and independent risk factor for osteoporotic fractures [121]. We studied the relations between osteoporosis and other chronic diseases like osteoarthritis [122], cancer [123], atherosclerosis [124] and diabetes [125, 126], and provided indications for the treatment and diagnosis of osteoporosis. Lastly, we were part of several large consortia studying epidemiological risk factors for osteoporosis [127–129]. For osteoarthritis (OA) we have shown how a new marker of disease (CTX-II), is associated with the prevalence and the progression of radiographic OA [130], independent of known clinical risk factors. In addition, we have studied different aspects of OA disease definition and classification [131], evaluation of disease progression [132] and determined the most prominent risk factors leading to OA [133, 134]. We have also studied inflammatory aspects of endocrine diseases like diabetes mellitus [135], and the relations of hypo/hyperthyroidism to cardiovascular and neurological disease [136]. We further examined the influence of genetic variation in endocrine genes influencing hormone levels [137, 138], interaction of genetic factors in relation to fracture risk [138, 139], to cardiovascular risk factors [140] and to neurological conditions [141]. Our team has played a leading role in bringing together the global GENOMOS consortium which has performed prospective meta-analyses across many epidemiological cohorts for the most prominent candidate genes for osteoporosis (see also “Genetic and biomarker studies”).
Methods update
For all participants DXA-based BMD measurements of the lumbar spine, dual hip and total body BMD, as well as determination of body composition parameters are assessed with a ProdigyTM total body fan-beam densitometer (GE Lunar Corp, Madison, WI, USA). Hip structural analysis [142] of DXA scans is available in a subset of participants, while hip strength indexes (software by GE Lunar) are determined for all scans. In the current follow-up cycle we have introduced since 2009 iDXA measurements (GE Lunar) which performs lumbar spine, dual hip and total body scans. Measurements include L1–L4 BMD, bilateral total hip and femoral neck BMD and total body BMD. From the total body scan, we measure lean mass and fat mass body composition, including total body, trunk, arm, legs, and android and gynoid regions of interest. X-ray examinations of vertebral bodies, hips, knees and hand/wrist are obtained by a digitalized Fuji FCR system (FUJIFILM Medical Systems) and assessed for the presence of fractures and/or degenerative changes of the joints. Vertebral fractures are assessed using the qualitative algorithm-based technique termed the ABQ method, an update to the quantitative McCloskey–Kanis method [143]. Incident clinical fractures are obtained from computerized records of the general practitioners and hospital registries which are regularly checked by research physicians who review and code the fracture information. Muscle strength is assessed in all participants with a hand grip dynamometer. The incidence and progression of OA is done using Kellgren scores obtained from X-rays of hip, knee, hands, en spine. The complete set of X-rays is also available in digitized form. Novel diagnostic assessments for OA are currently underway using Magnetic Resonance Imaging (MRI) on a large subset of the population. Several specific biomarker assessments in blood/serum/plasma and urine are done for the diagnosis and evaluation of risk factors of endocrine and metabolic diseases. Candidate gene and genome-wide association studies (GWAs) are actively pursued within the scope of our research for many of the above mentioned endocrine and locomotor traits and diseases. Finally, validated questionnaires evaluating nutrient intake (e.g., calcium and vitamins) and activities of daily living, allow to evaluate the role of environmental factors in endocrine conditions and locomotor diseases of the elderly. For recent references in EJE see [144–172].
Liver diseases
Objectives
Fibrogenesis of the liver is most probably not only the result of well known liver diseases, such as viral hepatitis, alcoholic liver disease or non-alcoholic fatty liver disease (NAFLD), but rather a complex interaction between a genetic predisposition and these liver disorders. Liver research in the Rotterdam Study will concern the association between these known causes of liver disease and the occurrence, magnitude, and progression of fibrosis in combination with genetic and environmental factors. Additional research focus will be on NAFLD. NAFLD is considered the hepatic manifestation of the metabolic syndrome and has become the most common chronic liver disease in Western countries in parallel with epidemics of obesity and type II diabetes mellitus. We aim to study the occurrence and risk factors of NAFLD in a general population and generate insight into the association with cardiovascular morbidity and mortality.
Methods
Abdominal ultrasound
From February 2009 trained technicians perform abdominal ultrasonography in Rotterdam Study participants. Liver, biliary tract, gall bladder, spleen, pancreas, and kidneys in combination with Doppler examination of hepatic veins, hepatic artery and portal vein will be evaluated. All images are stored digitally and will be reevaluated by an ultrasound trained physician.
Assessment of steatosis
The diagnosis and grading of liver steatosis will be based on ultrasonographic liver brightness, hepatorenal echo contrast, deep attenuation and vessel blurring [173].
Non alcoholic fatty liver is diagnosed by presence of steatosis on ultrasound and exclusion of excessive alcohol consumption, presence of viral hepatitis, use of fatty liver inducing pharmacological agents, recent bariatric surgery and a history of inflammatory bowel disease.
Assessment of fibrosis
Ultrasonographic evaluation of the liver parenchyma and liver surface will be performed in order to assess severe fibrosis and/or cirrhosis. Additionally, sonographic signs of portal hypertension will be studied (splenomegaly, venous collaterals, portal vein diameter and flow, hepatic venous flow, and the presence of ascites).
To assess and quantify the grade of fibrosis trained technicians will perform elastography in all participants. This test measures non-invasively and quantitatively the liver stiffness using a probe which includes an ultrasonic transducer transmitting a vibration wave through the liver. The velocity of the ultrasonic wave correlates directly with tissue stiffness [174, 175].
Determinants of interest
The association between factors known to influence liver function and the occurrence of steatosis and fibrosis will be studied. Additionally the association of these conditions with age, gender, nutritional intake, concurrent alcohol intake, risk factors for viral hepatitis, BMI, waist-to-hip ratio, serum glucose, insulin, and diabetes mellitus, serum cholesterol and triglycerides will be studied. All clinical information will be obtained by interview (updated with liver specific questions) and clinical examination. For recent EJE references see [176–183].
Neurological diseases
Objectives
Neuroepidemiologic research in the Rotterdam Study focuses on the frequency, etiology and early recognition of the most frequent neurologic diseases in the elderly, including dementia, in particular Alzheimer disease, Parkinson disease and stroke. In neurodegenerative and cerebrovascular disorders clinical symptoms typically become manifest late in the disease course, the occurrence of clinical disease does not reflect the underlying spectrum of disease-related pathology, and most of the clinical syndromes are etiologically heterogeneous. Therefore, an additional research focus is on the causes and consequences of pre-symptomatic brain pathology that can be assessed with non-invasive modalities, which include MR-imaging, neuropsychological testing and more recently gait assessment.
Major findings
Neurodegenerative and cerebrovascular diseases are highly frequent in the elderly. The prevalence increases from age 55 to 65 years to age 90 years and above from less than 1% to over 40% for dementia [184], from less than 0.5% to more than 4% for Parkinson disease [185], and from approximately 1% to nearly 10% for stroke [186]. The incidence figures follow this pattern of a strong increase with age over the entire age range, with the age-specific incidence of dementia being identical for men and women at least until the age of 85 [187] but with men having a higher age-specific incidence of both stroke and Parkinson disease than women throughout the age range [186, 188].
Vascular pathology and vascular risk factors are associated with worse cognitive performance [189], which also translates in people with vascular pathology or risk factors for vascular disease having an increased risk of dementia, including Alzheimer disease [190]. Moreover, several life style factors are associated with the risk of dementia and Alzheimer disease [191–193], suggesting that onset of dementia may at least partly be delayed or prevented. Commonly used drugs may have a role in this [194]. Similar risk factor profiles also underlie cognitive decline prior to the clinical diagnosis of dementia [195, 196].
The classical risk factors for stroke also predict risk of stroke in the Rotterdam Study [197]. Novel risk factors, including inflammatory markers, may be etiologically relevant but thus far add little to the identification of people at risk http://www.ncbi.nlm.nih.gov/pubmed/17015791 [198]. Possibly underlying this is that a large amount of stroke goes clinically undetected [199]. Nearly 20% of elderly people have at least one silent brain infarct, and thereby a nearly fourfold increased risk of clinical stroke, a more than doubled risk of dementia including Alzheimer disease, and an increased risk of depression [199].
With the advent of genome-wide association studies, the Rotterdam Study has contributed to large-scale collaborations and contributed to the identification of novel genes underlying the risk of Alzheimer disease and stroke [200, 201].
Neuroimaging reveals that brain pathology is widespread [202] and can go clinically undetected for a long time. In addition to the silent infarcts, many apparently healthy elderly have ischemic changes in their cerebral white matter, i.e. white matter lesions, that are associated with an increased risk of dementia, stroke and depression. Also brain atrophy, especially of the hippocampus, is already present years before onset of even the earliest sign of cognitive impairment or subjective complaints. This emphasizes the need to shift the attention in etiologic research of neurodegenerative and cerebrovascular disease to the causes of pre-symptomatic and underlying brain changes. Technological advances in image acquisition, optimized imaging sequences and automated post-processing of multispectral MR data are major drivers of the rapid developments in this field. With our current imaging protocol we can now not only investigate established markers of brain pathology, such as infarcts, white matter lesions, and atrophy, but also extend towards novel markers, such as cerebral microbleeds and diffusion tensor imaging (see further section on “Population imaging”).
Methods update
Assessment of dementia and Alzheimer disease
In the baseline and follow-up examinations participants undergo an initial screen for dementia with the Mini Mental State Examination (MMSE) and the Geriatric Mental Schedule (GMS), followed by an examination and informant interview with the Cambridge Examination for Mental Disorders of the Elderly (CAMDEX) in screenpositives (MMSE < 26 or GMS > 0), and subsequent neurological, neuropsychological and neuroimaging examinations [184, 187]. Of subjects who cannot be reexamined in person, information is obtained from the GPs and the regional institute for outpatient mental health care. A consensus panel makes the final diagnoses in accordance with standard criteria (DSM-III-R criteria; NINCDS-ADRDA; NINDS-AIREN).
Assessment of Parkinsonism and Parkinson disease
Participants are screened in the baseline and follow-up examinations for cardinal signs of Parkinsonism (resting tremor, rigidity, bradykinesia, or impaired postural reflexes). Persons with at least one sign present are examined with the Unified Parkinson’s Disease Rating Scale and a further neurologic exam. PD is diagnosed if two or more cardinal signs are present in a subject not taking antiparkinsonian drugs, or if at least one sign has improved through medication, and when all causes of secondary Parkinsonism (dementia, use of neuroleptics, cerebrovascular disease, multiple system atrophy, or progressive supranuclear palsy) can be excluded [185, 188].
Assessment of stroke and stroke subtypes
History of stroke at baseline was assessed through interview and verified in medical records. Putative incident strokes get identified through the linkage of the study database with files from general practitioners, the municipality, and nursing home physicians’ files, after which additional information (including brain imaging) is collected from hospital records. A panel discusses all potential strokes and subclassifies strokes into ischemic, hemorrhagic or unspecified [186, 198].
Assessment of cognitive function and motor function
Global cognitive function is measured through the Mini Mental State Examination (MMSE) in all surveys. From the third survey (RS-I-3) onwards we added a 30 min test battery that was designed to assess executive function and memory function, and which includes a Stroop test, a Letter Digit Substitution Task, a Word Fluency Test, and a 15 words Word List Learning test. This test battery was expanded from the fourth survey onwards (RS-I-4) to include motor function assessment using the Purdue Pegboard Test. Moreover, from 2009 onwards we expanded further by including the Design Orientation Test (DOT) and a modified version of the International Cooperative Ataxia Rating Scale (ICARS), which assess visuo-spatial orientation and ataxia respectively [203, 204]. Halfway through RS-III-1, we successfully implemented the assessment of gait in all participants using the GAITRite walkway (http://www.gaitrite.com/).
Rotterdam Scan Study: brain imaging within the Rotterdam Study
In 1991, a random sample of 111 participants underwent axial T2-weighted magnetic resonance (MR) imaging to assess presence and severity of white matter lesions [205]. In 1995, a random sample of 563 non-demented participants underwent brain MR imaging in the context of the Rotterdam Scan Study. From August 2005 onwards (RS-II-2 and further), a dedicated 1.5 Tesla scanner is operational in the research center of the Rotterdam Study, and brain imaging is performed in all study participants without contra-indications (see section on “Population imaging”). Currently, the follow-up of this latter sample extends to up to 5 years. Therefore, in the coming years we will be able to investigate how cerebral microbleeds and DTI-markers relate to incident neurological diseases. However, already cross-sectionally we have evidence that these novel MRI markers relate to cognitive function and motor speed [206]. For relevant recent EJE references see [207–214].
Ophthalmic diseases
The ophthalmic part of the Rotterdam Study focuses on frequency and risk factors of chronic ophthalmic diseases and on ophthalmological characteristics of systemic diseases. Our main research topics are age-related macular degeneration, open angle glaucoma, myopia, and retinal vessel diameters.
Major findings
Age-related macular degeneration (AMD)
During the last 5 years, international research strategies were directed towards revealing the genetic background of AMD. This has been very fruitful, and led to the identification of several genes which were consistently replicated. Many more genes had been launched by small studies and awaited validation. Our focus for AMD in 2010 was aimed at sorting out these relationships, as well as identification of gene-environment interactions. Working together with large consortia, we investigated the proposed genes C5, SERPING1, and TLR3. None of these genes appeared to show a consistent relation when studied in large populations [215–218] The genetic associations with the already known major genes, CFH and ARMS2, remained without a doubt considerable; risks were increased up to 10–15 times for individuals homozygous for both risk variants. These genes point to complement overactivation and oxidative stress as major pathways in AMD pathogenesis.
Earlier in RS, we found that a diet rich in antioxidants could lower the risk of early AMD. We now aimed to assess whether this diet could also lower risks in persons with a high genetic predisposition. This was indeed so, persons with high risk variants and a high dietary intake of beta-carotene, lutein and zeaxanthin, and omega-3 fatty acids, had significantly lower risks of early AMD than those who were genetically predisposed but had low intakes of these nutrients [219]. This biological interaction was statistically significant.
Research aims for 2012 and beyond are improving risk estimates for (combinations of) risk alleles using incident data from several population-based prospective studies; evaluation of gene effects on subclinical manifestations of disease, such as drusen on optical coherence tomography (OCT); and more in depth investigation of gene-environment interactions.
Open angle glaucoma (POAG)
In contrast to AMD, the genetic background of POAG was still largely unknown up to 2009. We aimed to elucidate associated genes for optic disc parameters using the GWAS platform in the RS I-III studies as well as the family-based ERF population. These cohorts revealed two genome-wide significant loci for optic disc area, one near the CDC7 gene and one near the ATOH7 gene; and two significant loci for vertical cup-disc ratio (VCDR), one in the CDKN2B gene and one near the SIX1 gene. Meta-analysis with Twins UK study confirmed associations and launched several other significant loci. Interestingly, ATOH7 was also associated with VCDR independent of optic disc area, suggesting a common pathway [220]. In collaboration with a large cohort from Singapore, these genes were validated and a novel locus near CARD10 was found for optic disc area [221].
Using the identified genes, we performed genetic risk modeling, and found that a polygenic model best explained VCDR and POAG, while an ologigenic model best fitted intra-ocular pressure (IOP) [222].
Non-genetic analyses were performed as well. We studied incidence of glaucomatous visual field loss during 10 years of follow up, and found that the overall incidence rate of field loss was 2.9 per 1,000 person-years, and that the 10-year risk of GVFL was 2.8% (95% CI 2.3–3.4). We determined whether lifestyle-related risk factors, such as socioeconomic status, smoking, alcohol consumption, and obesity, were associated with POAG, and found that obesity was associated with a higher intraocular pressure and a lower risk of developing POAG [223]. Future investigations will focus on further elucidation of the genetic background of POAG, risk modeling incorporating all known risk factors, and study of gene-environment interactions.
Myopia
Recently, we incorporated refractive error and myopia as a disease outcome in the Rotterdam Study. Using the Illumina platform, we performed a GWAS using the mean spherical equivalent of both eyes as an outcome, and found a significant locus on chrom. 15q14, near the genes GJD2 and ACTC1 [224]. More comprehensive analyses showed that variants in these genes could not explain the relationship, but that the associated region included regulatory elements which may influence these genes. A collaborative group in the UK found a locus on chromosome 15q25, which we were able to replicate [225]. The plans for the near future are a joint meta-analysis of virtually all studies with refractive error and GWAS data, and an in depth search for the causal variants at 15q14 by next generation sequencing.
Retinal vessel diameters
One of the current goals was to find genes which determine retinal vessel diameters. Within the CHARGE consortium, we found four novel loci associated with retinal venular caliber one within the RASIP1 locus, one adjacent to VTA1 and NMBR, one in the region of ATXN2, SH2B3 and PTPN11, and one adjacent to MEF2C [226].
Relationships with other disorders were investigated as well. Retinal venular widening appeared to be associated with an increased risk of vascular dementia [227]. We evaluated the relationship with stroke and found that larger retinal venular caliber was associated with an increased risk for stroke, in particular with an increased risk for intracerebral hemorrhage [228]. Lastly, we assessed whether smaller retinal arteriolar or larger venular calibers were associated with incident late-life depression, and found no evidence of an association. [229].
Methods update
At baseline and follow-up examinations participants undergo ophthalmic measurements including best-corrected ETDRS visual acuity, refractive error, Goldmann applanation tonometry, keratometry, slit lamp examination of the anterior segment and visual field testing. In pharmacological mydriasis we made 35° color photographs of the macular area, and 20° simultaneous stereoscopic imaging of the optic disc and macular area. Since the fifth follow-up, 35° stereoscopic color photographs of the optical disc and the macular area were made (RS-I-5). Analog fundus photography was replaced by stereoscopic digital imaging of the macular area and optic disc since the third follow-up examination. Optic nerve head analysis with a Heidelberg Retina Tomograph, macular pigment density, and melanin optical density measurements were added during the third follow-up (RS-I-3). At fifth follow-up examination, fourier domain optical coherence tomography of the macular area and optical disc, axial length and width measurements of cornea, anterior chamber, lens, posterior chamber and retina measured with Lensstar; and fundus autofluorescence, infra-red and red-free measurements were added (RS-I-5).
Classification of AMD, POAG, and retinal vessel diameters remained unchanged; refractive error was evaluated as spherical value + half cylindrical value, following clinical standards.
Psychiatric diseases
Objectives
The aim of the psychiatric research in the Rotterdam Study is to investigate the determinants, correlates and consequences of common psychiatric problems in the elderly. The focus has been on depressive disorders but anxiety disorders, sleep disturbances, addiction to smoking, and complicated grief are also being studied.
In the first years of the Rotterdam Study (RS-I-1) psychiatric data collection was very limited. However, in the second visit most participants were screened for depressive symptoms and from the third examination onwards, which began in 1997, depressive symptoms and disorders have been ascertained in all participants. An assessment of anxiety disorders, sleeping disturbances and complicated grief were added in the fourth examination and have been included in all follow-up visits of the Rotterdam Study I and II, and in the baseline of the Rotterdam Study III. Recent additions to the protocol include a screening for psychotic symptoms and, starting with the third examination of the Rotterdam Study II, ambulatory polysomnography.
Major determinants
Psychiatric research in the Rotterdam Study focuses on biological risk factors. The vascular depression hypothesis was tested with different measures of atherosclerosis, arterial stiffness and cerebral blood flow [230]. We also examined whether blood levels of vitamins and fatty acids, immune parameters, and markers of folate metabolism increased the likelihood of depression [231]. In one ongoing project, diurnal patterns of cortisol secretion are related to psychiatric and other disorders such as subclinical atherosclerosis [232]. Studies of genetic polymorphisms and brain morphology are underway [233]. Current data collection includes a dexamethasone suppression test to measure hypothalamic–pituitary–adrenal axis activity in all participants, which is unique in a population-based study. Also, psychiatric problems and psychological traits such as happiness, sleep duration and depression are increasingly studied as determinants of health and mortality [234, 235].
Major outcomes
Information on depression is obtained from (a) psychiatric examinations, (b) self-reported histories of depression, (c) medical records, and (d) registration of antidepressant use [236]. The psychiatric examination during follow-up visits consists of a screening with the Center for Epidemiologic Studies Depression Scale (CES-D), and in the screen-positive participants a semi-structured interview performed by a trained clinician (Schedules for Clinical Assessment in Neuropsychiatry, [237]). To continuously monitor incidence of depression throughout follow-up, trained research-assistants scrutinize the medical records of the general practitioners and copy the information about possible depressive episodes.
The following anxiety disorders are assessed with a slightly adapted Munich version of the Composite International Diagnostic Interview: generalized anxiety disorder, specific and social phobia, agoraphobia without panic disorder, and panic disorder [238, 239].
Sleep quality and disturbance is measured with the Pittsburgh Sleep Quality Index. In addition, sleep duration and fragmentation are assessed with actigraphy, a method that infers wakefulness and sleep from the presence or absence of limb movement [240]. In total, nearly 2,000 persons participated in this actigraphy study: they wore an actigraph and kept a sleep diary for, on average, six consecutive nights. In 2011 we have begun to follow these participants up with another 6 day assessment using actigraphy. In addition, 1,000 persons will receive one night of polysomnography in their home setting.
The Inventory of Complicated Grief is used to identify traumatic grief [241]. This is a condition distinct from normal grief and bereavement-related depression, characterized by symptoms like disbelief about the death and searching for the deceased.
Major findings
Depression
Recently we completed our study of the incidence and recurrence of depression [236]. During the follow-up period of 8 years on average, 566 depressive syndromes and 1,073 episodes of clinically relevant depressive symptoms occurred. For depressive syndromes, the incidence rate was 7.0 (95% CI: 6.0–8.3) per 1,000 person-years and the recurrence rate was 27.5 (95% CI: 23.7–32.1) per 1,000 person-years. The recurrence rate of depressive syndromes was equal for women and men.
In a series of initial studies we found some evidence for the vascular depression hypothesis. More severe coronary and extra-coronary atherosclerosis were associated with a higher prevalence of depression, as were cerebral haemodynamic changes [230, 231]. However, our data did not support a specific symptom profile of vascular depression as previously defined [242]. Most importantly, we found no longitudinal relation between peripheral atherosclerosis and incident depression [243]. This study refutes the vascular depression hypothesis that was largely based on cross-sectional data. Prospective studies to test the vascular hypothesis using cerebral imaging data are ongoing.
Sleep
We investigated the relationships of sleep duration with both cardiovascular risk factors and psychiatric disorders. We found a marked U-shaped association of actigraphically measured total sleep time with BMI and obesity [235]. Sleep fragmentation also increased the likelihood of a higher BMI and obesity, although, in the very old sleep fragmentation is a risk factor for low cholesterol levels [244]. We also investigated and aimed to explain sex differences in subjective and actigraphic sleep parameters [245]. If assessed by diary or interview, elderly women consistently reported shorter and poorer sleep than elderly men. In contrast, actigraphic sleep measures showed shorter and poorer sleep in men. These discrepancies were partly explained by sleep medication use and alcohol consumption.
Anxiety
We found that prevalent anxiety disorders fulfilling DSM-IV criteria may be much less co-morbid with depressive disorders than previously thought if the disorders are assessed with different diagnostic instruments. On the other hand, a history of depression is very common in persons with prevalent anxiety disorder (more than 50%; [246]).
Smoking
Typically, determinants of smoking cessation are studied by comparing former with current smokers [247]. We also used a prospective approach of studying smoking cessation in 1,200 smokers (mean years of smoking: 40 years, minimum: 10 years). Smoking status was repeatedly assessed during follow-up every 3- to 4-years. Thus, an individual could contribute any number of person-years to the analyses. In other words, people were classified as smokers or quitters on a day-by-day basis. This approach enabled us to detect genetic effect on the incidence of smoking cessation [248].
Complicated grief
In our population-based study of 5,741 elderly persons, current grief was reported by 1,089 participants, and of these 277 (25 or 4.8% of total) were diagnosed with complicated grief, the vast majority of which had no clinical symptoms of anxiety or depression. Persons with complicated grief were older, had a lower level of education, and more often had lost a child [249].
Genetics of common psychiatric disorders
In the past year, we have performed a series of genome-wide association studies of the above psychiatric and psychological phenotypes, mostly as part of the CHARGE consortium. Whereas several analyses have yielded no convincing genome wide significant results—possibly because initial studies were underpowered, psychiatric phenotypes do not present very homogenous entities, or are highly very multi-genetic—the genome wide analyses of intermediate phenotype such as cortisol or behavioural traits are more promising [250]. To study the genetics of cortisol, we have established a dedicated consortium of population-based studies: CORNET.
Finally, ongoing psychiatric research projects examine whether and how psychological well-being or psychiatric problems contribute to survival. Most importantly, we are interested in whether the effects are specific to certain behaviour or emotions, are independent of confounding by physical disease, or can be explained by lifestyle, immunological or hormonal regulation. For recent EJE references see [251–259].
Respiratory diseases
Objectives
The objectives are to study the incidence of chronic obstructive pulmonary disease (COPD), to investigate genetic and environmental risk factors for COPD, and to study the effect of COPD on mortality. COPD is defined as a disease state characterized by airflow limitation that is not fully reversible. The airflow limitation is usually both progressive and associated with an abnormal inflammatory response of the lungs to noxious particles or gases such as tobacco smoke [260]. COPD is a worldwide leading and still increasing cause of chronic morbidity and mortality that will change from the sixth to the third most common cause of death worldwide by 2020, whilst rising from fourth to third in terms of morbidity [261].
Major findings
In the first cohort of the Rotterdam Study (RS-I) of 7,983 participants, 648 cases were identified with incident COPD after a median follow-up time of 11 years. This resulted in an overall incidence rate of 9.2/1,000 person-years (PY) (95% CI, 8.5–10.0). The incidence rate of COPD was higher among men (14.4/1,000 PY; 95% CI, 13.0–16.0) than among women (6.2/1,000 PY; 95% CI, 5.5–7.0) and higher in smokers than in never-smokers (12.8/1,000 PY; 95% CI, 11.7–13.9 and 3.9/1,000 PY; 95% CI, 3.2–4.7, respectively). Remarkable was the high incidence in the youngest females in the age category of 55–59 years (7.4/1,000 PY; 95% CI, 4.1–12.6). For a 55 year-old man and woman, still free of COPD at cohort entry, the risk to develop COPD over the coming 40 years was 24 and 16%, respectively [260]. Since COPD is not only affecting the lungs, but is also characterised by extrathoracic manifestations, another line of research focuses on the role of systemic inflammation in the pathogenesis of COPD and its comorbidities. High levels of hsCRP (3 mg/l), a marker of systemic inflammation, were associated with a significantly increased risk of incident COPD (hazard ratio (HR), 1.7; 95% confidence interval (95% CI), 1.16–2.49) compared with persons with low CRP levels (<1 mg/l). The risk remained increased after adjustment for potential confounders and introduction of a potential latency period of 3 years. The risk was most pronounced for former smokers (HR, 2.2; 95% CI, 1.12–3.74). No CRP single nucleotide polymorphism or haplotype was associated with a significantly increased or decreased COPD risk [262].
Spirometric measures of lung function are heritable traits that reflect respiratory health and predict morbidity and mortality. We meta-analyzed genome-wide association studies for two clinically important lung-function measures: forced expiratory volume in the first second (FEV1) and its ratio to forced vital capacity (FEV1/FVC), an indicator of airflow obstruction. This meta-analysis included 20,890 participants of European ancestry from four CHARGE Consortium studies: Atherosclerosis Risk in Communities, Cardiovascular Health Study, Framingham Heart Study and Rotterdam Study. We identified eight loci associated with FEV1/FVC (HHIP, GPR126, ADAM19, AGER-PPT2, FAM13A, PTCH1, PID1 and HTR4) and one locus associated with FEV1 (INTS12-GSTCD-NPNT) at or near genome-wide significance [P < 5 × 10(−8)] in the CHARGE Consortium dataset [263]. The Hedgehog signalling pathway plays an important role in lung morphogenesis and cellular responses to lung injury. A genome-wide association study has demonstrated that two single nucleotide polymorphisms (SNPs) near the Hedgehog-interacting protein (Hip) gene, SNP identifiers rs1828591 and rs13118928, are associated with risk of chronic obstructive pulmonary disease (COPD). We investigated the association between genetic variation near the Hip gene and COPD, and whether risk estimates were modified by smoking behaviour in the Rotterdam Study. Both SNPs were significantly associated with risk of COPD (OR 0.80; 95% CI 0.72–0.91). Homozygosity for the minor G allele resulted in a decreased risk of COPD of approximately 40% (95% CI 0.47–0.78). There was a significant interaction with the number of pack-years of smoking (P = 0.004). The meta-analysis yielded an odds ratio for COPD of 0.80 per additional G allele [P = 3.4 × 10(−9)]. Genetic variation near the Hedgehog-interacting protein gene was significantly associated with risk of COPD, depending on the number of pack-years of smoking [264].
Methods update
Clinical assessment of COPD
For the validation of the COPD cases, we had access to hospital discharge letters, files from the general practitioners, spirometry reports and pharmacy dispensing data for patients participating in the Rotterdam Study. Spirometry was performed in the context of the first Rotterdam cohort study (RS-I) in 3,550 participants. In addition, throughout the entire study period, spirometries were also performed on clinical indication by respiratory specialists and internists with a subspeciality in respiratory medicine. In the absence of spirometry, all medical information of subjects who used respiratory medication for at least 6 months and all hospital discharge letters or mortality reports with a coded diagnosis of COPD were reviewed. Definite COPD was defined by a moderate-to-severe obstructive spirometry (FEV1/FVC < 0.7 and FEV1 < 80% predicted), and/or as COPD diagnosed by a specialist in internal medicine (mainly respiratory physicians or internists with a subspeciality in respiratory medicine) based upon the combination of clinical history, physical examination and spirometry. Probable COPD was defined by a mild obstructive spirometry (FEV1/FVC < 0.7 and FEV1 ≥ 80% predicted) and/or as COPD diagnosed by a physician in another medical speciality (e.g., a general practitioner). Clinical outcomes are collected during our continuous follow-up and include respiratory and non-respiratory death, hospitalisations due to exacerbations of COPD as well as moderate to severe COPD exacerbations treated with systemic corticosteroids and/or antibiotics. For pulmonary function testing in the 5th round of the first cohort of the Rotterdam Study (RS-I-5), the 3rd round of the second cohort (RS-II-3), and the 2nd round of the third cohort (RS-III-2), more detailed and sophisticated techniques are used to assess pulmonary function. Since COPD encompasses small airway disease (obstructive bronchiolitis) and parenchymal destruction of the lungs (emphysema), both components will be investigated by spirometry and measurement of pulmonary diffusion capacity, respectively.
Spirometry
Spirometry is performed by trained paramedical personnel using an electronic spirometer with pneumotachograph (Jaeger Masterscreen PFT, Cardinal Health, Hoechberg, Germany), according to the American Thoracic Society (ATS)/European Respiratory Society (ERS) guidelines. Forced expiratory volume in one second (FEV1), forced vital capacity (FVC) and FEV1/FVC ratio are measured; the spirogram (volume-time curve) and maximal expiratory flow-volume curve are also recorded. The interpretation of spirometries is performed independently by two research physicians; in case of discordance between both physicians, a senior respiratory physician decides. Measurement of pulmonary diffusion capacity Measurement of diffusion capacity by single-breath determination of carbon monoxide (CO) uptake in the lung (DL, CO) assesses the uptake of carbon monoxide (CO) from the lung over a breath-holding period [265]. The DL, CO is measured using the Jaeger Masterscreen PFT Pro Diffusion apparatus (Cardinal Health, Hoechberg, Germany) according to the guidelines of the ATS/ERS task force on standardisation of lung function testing [265]. The test gases used to calculate DL, CO include a tracer gas (methane), to measure alveolar volume (VA), as well as carbon monoxide (CO 0.3%). The remainder of the test gas mixture includes O2 and N2. For recent EJE references in this area see [266–279].
Genetic and biomarker studies
Objectives
The first objective of the laboratory team is to collect, store and manage the biological tissues mainly blood and urine sampled in the Rotterdam Study. The second objective of the group concerns genotyping and assessment of biomarkers.
Major findings
Among the biomarker analyses our study documenting the relationship between homocysteine and osteoporosis was novel [121] and has since been widely replicated. Across all research lines in the Rotterdam Study, several candidate gene studies have also yielded new insights coming from both exploratory studies as well as from collaborative replication efforts. A unique feature of the Rotterdam Study is exploited by studying the relationship between pleiotropic gene variants and multiple diseases and disease related endpoints. For example, the studies on the promoter region of the IGF-1 gene revealed a series of consistent associations ranging from birth weight to diabetes [280], while other consistent associations involve the estrogen receptor alpha (ESR1) gene in relation to osteoporosis [281], osteoarthritis, height, myocardial infarction [282], age-at-menopause, and depression. Rotterdam Study investigators are playing leading roles in the emerging large global consortia focussed on assessing the contribution of complex disease gene variants by prospective meta-analysis across many epidemiological cohorts [283], such as CHARGE, ENGAGE and the GENOMOS/GEFOS [284, 285]. Since 2005 the genome wide association study (GWAs) has changed the field of complex genetics, and identified an ever growing list of common variants contributing to disease risk and explaining genetic variance of traits. Initial findings in the Rotterdam Study from individual collaborations replicating early GWAs hits included CFH in age-related macula degeneration [286], NOS1AP in QT interval [287], and several SNPs involved in height, type 2 diabetes, and breast cancer (collaboration with WTCCC investigators). The Rotterdam Study has generated GWAs data for almost the complete dataset summing to over 11,000 DNA samples, and is involved as a major collaborative centre for meta-analysis studies of GWAs data, including national programs (RIDE, NGI-NCHA), EU-funded projects (GEFOS, TREATOA, ENGAGE), and voluntary collaborations (GIANT, MAGIC, CHARGE). Especially, from the CHARGE consortium (the Rotterdam Study together with the Framingham Study, AGES, CHS, and ARIC) many important publications have emerged on a wide variety of phenotypes and diseases from all major research lines in the Rotterdam Study [288–292].
Data collection, storage and management
At each examination, blood, serum, plasma (citrate, heparine, and EDTA based), sputum, and urine are collected. Fasting blood samples are collected along with challenged samples as part of a glucose tolerance test. Sputum is collected before and after a dexamethasone-suppression test. Sputum is frozen at −196°C before and after the challenge and stored at −80°C. To obtain serum and plasma, tubes are centrifuged according to a protocol standardising time and conditions from the drawing of blood to centrifugation. All samples are snap frozen at −196°C using liquid nitrogen and stored at −80°C. RNA is isolated from blood within 5 h after sampling and stored at −20°C. DNA is isolated from blood and extraction has been recently automated using a Hamilton STAR pipetting platform and AGOWA magnetic bead technology. DNA sample storage is in Matrix 2D-barcode tubes in 96 well format. Overnight urine samples are collected, frozen at −196°C and stored at −80°C. For data management, an in-house customized laboratory management system has been developed. Sample retrieval will be automated with an in-house customized laboratory track and trace system.
Blood assessments
For all participants, serum cholesterol, HDL, LDL, triglycerides, glucose and glucose levels are assessed. In urine, micro albumin and creatinine are determined in all participants. There have been a large number of specific blood/serum/plasma-based biomarker assessments, including steroids (e.g., estrogens, androgens, vitamin D, cortisol), interleukins, CRP, IGF1, insulin, iron-parameters (iron, ferritin and transferrin saturation), fibrinogen, homocysteine, folic acid, riboflavine, pyridoxine, SAM/SAH ratio, cobalamine, Lp-PLA2, Fas/Fas-L, vitamins, abeta42/40 and thyroid hormones (TSH).
Genotyping facilities
Affiliated laboratory facilities include a medium/high-throughput platform for candidate genes studies and GWAs analyses. The facilities use high-end automated machinery including a Caliper/Zymark ALH 3000 pipetting robot (including a TwisterII, and integrated plate sealer, plate reader (OD 260/280), a Tecan EVO 150 Freedom pipetting robot, a Deerac Equator NS808 nanoliter liquid dispenser, 15 electronic PCR machines (ABI 9700, 2 9 384), an ABI7900HT Taqman machine (running 1 ng gDNA in 2l reactions), a WAVE 3500HT dHPLC, Sequenom iPlex, and two ABI3100 sequencing machines. DNA sample handling is centred on 384-well plates. Candidate gene studies are done mostly using Taqman and Sequenom genotyping with throughputs at 30,000 genotypes per day. Continuous efforts are focussed on reducing the required amount of genomic DNA which is now down to 1 ng per genotype. GWAs genotyping studies are based on 500 K Affymetrix arrays (a pilot project of 450 women) and 550 and 610 K Illumina arrays for the complete Rotterdam Study cohort encompassing over 11,000 DNA samples. The in-house GWAs genotyping facility has been partly sponsored by NWO investment grants (911-03-012; 175.010.2005.011), is part of the Erasmus Medical Center Biomics core facility, and serves as knowledge center for polymorphism analysis attracting national and international interested parties, both academic and industrial.
Candidate gene studies
We have genotyped over 300 individual polymorphisms as part of candidate gene studies across the complete cohort and conducted a large number of candidate gene studies in the Rotterdam Study. These mostly concern individual potentially functional single nucleotide polymorphisms (SNPs) per gene, but sometimes also haplotype tagging (delete space) SNPs (e.g., ESR1, ESR2, HSD11B1, fibrinogen), and also high density SNP screening (e.g., the vitamin D receptor gene). The candidate genes studied include the apolipoprotein E gene (APOE), the angiotensin-converting enzyme (ACE), the gene encoding angiotensinogen (AGT), angiotensin II type 1 receptor (AT1R) gene, G protein beta3 (GNB3), adducine gene, Cholesteryl Ester Transfer Protein (CETP), Hepatic Lipase, Phosphodiesterase 4D (PDE4D), ALOX5AP encoding 5-lipoxygenase activating protein, a polymorphism in the regulatory region of the Insulin-like Growth Factor 1 (IGF-1) gene, the hemochromatosis (HFE) gene, Complement factor H gene (CFH), and several polymorphisms in genes from the estrogen-, thyroid-, cortisol-, vitamin D-, IGF-, and Wnt signalling pathways, the homocysteine pathway, and several matrix molecules.
Genome wide association studies (GWAs)
Genome Wide Association studies (GWAs) are based on genotyping epidemiological cohorts with ultra-high density SNP arrays with up to 1 million SNPs. The method has been shown to successfully identify common genetic factors for hundreds of traits and diseases (see www.genome.gov/ GWAstudies). Through a large grant from the Dutch research organisation NWO one of the world’s largest GWAs datasets has been facilitated involving over 11,000 DNA samples from the Rotterdam Study cohorts. This GWAs dataset is based on the Illumina 550 and 610 K arrays and will be useful for all research lines within the Rotterdam Study. In addition, it will also serve as a control GWAs dataset for other research centers in and outside The Netherlands for both SNP frequencies as well as copy number variations (CNVs). In addition our group has also been active in developing new software for GWAs analyses [292].
New developments
The new development in the basic sciences will be to move to transciptomic studies and proteomic studies. With this view, the data collection protocol has been adjusted, standardizing blood collection. For recent EJE references see [290–310].
Pharmaco-epidemiologic studies
Objectives
A major objective of the pharmaco-epidemiologic studies is to investigate the role of drugs as determinants of disease in the Rotterdam Study. This includes studying efficacy and effectiveness of drugs, as well as adverse reactions to drugs.
Major findings
Important findings have been published on pharmaco-epidemiological topics concerning the main outcomes in the Rotterdam Study. Studies about the association between dementia, and antihypertensive drugs [293] and NSAIDs [194] have strongly suggested a protective effect of both groups of drugs. However, beta-blockers were associated with an increased risk of depression [294]. Several studies have been performed on cardiovascular topics [62, 295, 296]. In one of these studies, NSAIDs were associated with an increased risk of heart failure. A recent study demonstrated that short-term use of NSAIDs is associated with transient impairment of echocardiographic parameters [297]. In line with the suspicion that QTc-prolonging drugs may cause sudden cardiac death, it was demonstrated in the Rotterdam Study that a prolonged QTc is indeed an important risk factor [62]. Non-cardiovascular drugs which inhibit hERG-encoded potassium channels were associated with an increased risk of sudden cardiac death [298]. Furthermore, in one study it was demonstrated that high-dose corticosteroids increase the risk of atrial fibrillation [296]. In how far this effect is modified by susceptibility markers on chromosome 4q25 [299] or on KCNN3, a gene of which variants were associated with lone atrial fibrillation in a meta-analysis in the Rotterdam Study and several cohorts from the USA [300], is currently being investigated. Other important susceptibility genes for PR-interval [59], resting heart rate [301] and QRS duration [302] may prove to be important effect modifiers for drug effects. In the important area of locomotor diseases, studies have demonstrated that thiazide diuretics protect against hip fracture [303] and that statins reduce the risk of vertebral fracture [304]. On the other hand, the risk that long-term use of certain NSAIDs may aggravate signs of osteoarthritis has been emphasized [305]. In the area of ophthalmic diseases, a protective effect of cholesterol-lowering agents on macular degeneration has been studied [306, 307]. In other areas, such as pharmacogenetics and other causes of interactions between drugs, several important findings have been published [287, 308–328]. In this regard, there proved to be important genetic variations in OCT1 and MATE1 transporters with consequences for metformin response in diabetics [329]. Genetic variation in the OCT1 transporter was also associated with response and survival time in users of drugs against Parkinsonism [330]. Interesting were the results of a GWA in users of the anticoagulant phenprocoumon which confirmed the important genetic variant for VKORC1, CYP2C9 and 4F2 [331]. An increasingly important topic is the association between long-term drug use and cancer. In the Rotterdam Study, high-ceiling diuretics were associated with an increased risk of basal cell carcinoma [332]. The importance of cytochrome P450 enzymes as effect modifiers was underlined by 2 studies, one of which showed increased survival in breast cancer patients on tamoxifen with a CYP2C19*2 polymorphism [333, 334].
Methods update
For several reasons, a drug is a highly attractive determinant in clinical epidemiologic research. First, drugs are probably the most important therapeutic intervention in health care. Despite rigorous clinical research before registration, many important effects of drugs are discovered after marketing. Second, all marketed drugs have proven biological activity, meaning that it concerns a determinant which really matters. Third, and as a consequence of the availability of complete medication histories in Dutch health care, the role of drug exposure can be assessed in a detailed way. In the Rotterdam Study, there is an almost complete coverage of the population as of January 1, 1991, thanks to the fact that all pharmacies which serve the Ommoord district are on one computer network. To date, more than three million prescriptions have been delivered to the population of the Rotterdam Study and of each prescription, details are available about the product name and contents, ATC-code, dosage and duration of drug therapy. This facilitates the use of detailed analyses with the drug as a time-varying determinant [335]. Drugs are a group of determinants which can be studied in association with a large variety of diseases. In the Rotterdam Study there is a strong interest in the association between drugs and the cardiovascular, neurological, endocrine, and ophthalmic diseases which have been the main topics since its start. However, there is also important information about the association with psychiatric diseases, cancer, and chronic obstructive pulmonary disease. Moreover, important information about secondary outcomes, such as drug blood levels, other laboratory information, and information about hospital discharge diagnoses, is gathered on a continuous basis to facilitate pharmaco-epidemiological studies. Further EJE references can be found in [336–342].
Imaging studies
Objectives
Biomedical imaging allows for non- or minimally-invasive assessment of structural and functional changes that may reflect specific pathology. Recent developments in image data acquisition and analysis enable to use these techniques on a large scale. The Population Imaging Unit within the Rotterdam Study aims to assess imaging biomarkers of disease in a pre-symptomatic phase at the population level. Advantages of imaging measures include that they mark early disease, can be assessed reliably and reproducibly, and are quantitative rather than qualitative which makes them more powerful than most conventional outcome measures such as clinical phenotypes. The main imaging modalities that are currently being applied in the Population Imaging Unit are multidetector computed tomography (MDCT) and magnetic resonance imaging (MRI).
Imaging infrastructure and storage
MDCT
CT imaging is currently performed with hospital-based 16-slice or 64-slice MDCT scanners (SOMATOM Sensation 16 or 64, Siemens, Forcheim, Germany), located at Erasmus University Medical Center. Scanners are operated by clinical technicians. CT images are acquired without contrast-enhancement and according to standardized protocols. Imaging data are transferred from the CT scanner to a securely backed-up research picture archiving system.
MRI
From August 2005 onwards, a dedicated 1.5 Tesla MRI scanner (GE Healthcare, Milwaukee, Wisconsin, USA) is operational in the Rotterdam Study research center. This scanner is operated by trained research technicians and all imaging data are collected according to standardized imaging protocols. Changes or updates in hardware or software configuration are avoided and regular quality checks are performed to secure validity of cross-subject and cross-scan comparisons. Imaging is performed without administration of contrast agents. All imaging data are directly transferred from the scanner facility to the Erasmus University Medical Center. Data are stored on a securely backed-up research picture archiving system, using programmed scripts to check for completeness of the data received.
Data management and processing
Assessment of incidental findings
All imaging data are visually evaluated within days after acquisition by trained physicians for the presence of clinically relevant incidental findings [202, 343]. Expert radiologists are consulted for all abnormal findings and the management of clinically relevant findings is based on protocols defined by expert panels. These protocols are updated on a regular basis incorporating the current best available knowledge regarding treatment and prognosis of the various abnormalities discovered.
Automated processing of MRI data
Though some measurements are still performed manually or scored visually, the majority of imaging data is now processed using semi- and fully-automated computer algorithms. The Population Imaging Unit collaborates with the Biomedical Imaging Group Rotterdam (BIGR) of Erasmus University Medical Center in the application and development of automated processing pipelines for high-throughput of large data quantities. These pipelines comprise on the one end image quality checks and procedures for non-uniformity correction, normalization and image registration and on the other end advanced algorithms to extract image features to use for analyses. Grid architectures and networked processing pipelines are used to process the large quantities or imaging data that are acquired in the Rotterdam Study.
Major findings
The Rotterdam Study research lines currently applying imaging within the Population Imaging Unit are those on neurological diseases and cardiovascular diseases.
Brain imaging (MRI)
Neurodegenerative and cerebrovascular disease are common disorders in the elderly that exert a large influence on brain functioning. Identifying underlying pathology in a preclinical state may help to recognize persons at risk, assess determinants of disease and develop preventive measures. Main objective for the Population Imaging Unit with respect to brain imaging is therefore to identify and quantify brain imaging biomarkers that mark the development of neurodegenerative and cerebrovascular disease.
From August 2005 onwards (RS-II-2 and onwards), brain imaging in the Population Imaging Unit is performed in all study participants without contra-indications in the context of the Rotterdam Scan Study. The current scanning protocol includes 4 high-resolution axial sequences (3D T1-weighted; 2D PD-weighted; 2D FLAIR; and 3D T2* GRE), 2D phase-contrast imaging, and diffusion tensor imaging (DTI). Total scanning time amounts to approximately 30 min. Currently, over 5,000 unique brain MRI scans and over 800 follow up scans after a time interval of three to 4 years have been acquired.
Fully automated methods are applied to quantify atrophy of brain tissues and structures and the severity of white matter lesions [343–345] Automated hippocampal segmentation has been successfully applied on multi-scanner acquired MR images (on scans acquired in the Rotterdam Scan Study in 1995 [346] and follow up examinations in 2006), showing that a decline in hippocampal volume over a 10-year follow up period predicted onset of clinical dementia [347].
Phase-contrast imaging allows for assessment of blood flow in the carotids and basilar artery. This yields measures of total brain perfusion [348], which when lower was found to be relate to worse cognition, an association that is mediated by brain atrophy [349].
The 3D T2* GRE sequence that we use was specifically developed to increase the conspicuity of cerebral microbleeds [350]. With this optimized sequence, we found that microbleed prevalence gradually increases with age, from 6.5% in persons aged 45–50 years to 35.7% in participants of 80 years and older; and that overall, 15.3% of all subjects over the age of 45 years has at least 1 microbleed; a much higher prevalence than was reported before [351, 352]. We found supportive evidence that deep or infratentorial microbleeds reflect arteriolosclerotic angiopathy, whereas strictly lobar microbleeds are caused by cerebral amyloid angiopathy [351, 352]. We furthermore recently demonstrated that incidence of microbleeds over a 3-year time interval is high and that risk factors for new microbleeds again differ according to microbleed location, in line with our findings regarding prevalent microbleeds [353]. These findings impact research into the causes of cerebral amyloid angiopathy, as well as fuel the ongoing discussion about the safety of antithrombotic therapy in persons with microbleeds [354, 355].
Diffusion tensor imaging (DTI) allows the assessment of the microstructural integrity of white matter. White matter microstructure loses its integrity with increasing age, but this can largely be explained by presence of white matter atrophy and white matter lesions [356]. Nevertheless, the microstructural integrity in the normal appearing white matter and in white matter lesions relates to cognitive function regardless of concurrent macrostructural changes, emphasizing the importance of the microstructural integrity of white matter [206]. Recent advances in image processing now allow us to quantify the degree of connectivity between brain regions [357], enabling the further exploration of structural integrity in relation to functional processes in aging.
Imaging of atherosclerotic calcifications (MDCT)
Main objectives with respect to imaging of vascular calcifications are to investigate distribution of and risk factors for atherosclerotic calcifications in the general elderly population and to study prognosis associated with calcifications in different vessel beds.
From September 2003 until February 2006, all participants from RS-I-4 and RS-II-2 who completed a center visit were invited to a MDCT scan of the coronary arteries and a second scan of the aortic arch and carotid arteries. A total of 2,521 participants (response rate 79%) were scanned. The cardiac scan reached from the apex of the heart to the tracheal bifurcation. The second scan reached from the aortic arch to the intracranial circulation. Images were analyzed by trained reviewers and calcification in the different vessel beds (coronaries, aortic arch, extracranial and intracranial carotids) were quantified using the Agatston score [358].
As expected, we found that calcification load was higher overall in men compared to women, though aortic arch calcification was more prevalent among women [359]. Age and current smoking were found to be the strongest independent risk factors for arterial calcification [360]. Furthermore, strong and graded associations of prevalent stroke were found with carotid artery, aortic arch and coronary artery calcification, independent of cardiovascular risk factors [361]. We are currently investigating the relation between arterial calcification in various vessel beds and ischemic brain disease on MRI.
Carotid plaque imaging (MRI)
Carotid wall thickening and atherosclerosis are highly prevalent at older age and are considered a major cause of cerebrovascular events [197]. Carotid atherosclerotic plaque constituents such as lipid core and hemorrhage, so-called “vulnerable” components, are considered important factors in development of clinical neurological events [362]. With MRI, it is possible to separately identify these plaque components [363]. Main objectives with respect to carotid imaging in the Rotterdam Study are to investigate distribution of and risk factors for carotid plaque components in the general elderly population and to study prognosis associated with specific carotid plaque composition.
From October 2007 onwards, all participants with carotid wall thickening of 2.5 mm or larger on ultrasound (approximately 25% of the Rotterdam Study population) are invited for carotid MRI. Imaging is performed with a bilateral phased-array surface coil (Machnet, Eelde, The Netherlands), stabilizing subjects in a custom-designed head holder to reduce motion. The imaging protocol consists of a series of high-resolution MRI sequences to image the carotid bifurcations on both sides: a PDw Fast Spin Echo (FSE) Black-blood (BB) sequence; a PDw-FSE-BB with an increased in-plane resolution; a PDw-Echo Planar Imaging (EPI) sequence and a T2w-EPI sequence; and 2 three-dimensional (3D) sequences: a 3D-T1w-Gradient Echo (GRE) sequence; and a 3D phased-contrast MR-Angiography. Total scanning time amounts to approximately 30 min. Plaques are reviewed by trained raters for the presence of three different plaque components (calcification, hemorrhage and lipid core). Furthermore, carotid plaque size is quantified by obtaining maximum carotid wall thickness and degree of luminal stenosis using the NASCET criteria [364] on the PDw-FSE images. Postprocessing techniques aimed at automated quantification of plaque volume and identification of different plaque components are currently being developed. So far, over 1,300 participants underwent a complete carotid MRI scan and data are currently being analyzed. There is a complete overlap between carotid and brain MRI participants, allowing for the investigation of carotid plaque constituents in relation to brain imaging markers.
New developments
New developments to be expected within the Population Imaging Unit are on the one hand implementation of new imaging methods and on the other hand to integrate imaging data with other available data such as genetic data. Also, focus will shift from purely structural imaging to also including functional imaging data, e.g. by incorporating functional MRI into the brain imaging protocol. Furthermore, besides ever-increasing advances in imaging hardware, software and sequence design, major advances are to be expected from (fully) automated image analysis. Computer processing of images will enable to make use of all information contained within the image, introducing new imaging biomarkers. Besides, the vast amount of imaging data that are acquired in population-based studies like the Rotterdam Study renders visual assessment or manual measurements virtually impossible, strengthening the need for (fully) automated methods of data extraction and analysis. For recent EJE references see [182, 365–369].
Management
The Rotterdam Study is directed by a Management Team comprising the scientific principal investigators Cornelia van Duijn (PI Genetic epidemiologic studies), Oscar Franco (PI Cardiovascular diseases), Albert Hofman (chairman, PI Rotterdam Study), Arfan Ikram (PI Neurological diseases), Harry Janssen (PI Hepatic diseases), Caroline Klaver (PI Ophthalmic diseases), Ernst Kuipers (PI Internal Medicine), Tamar Nijsten (Dermatological diseases), Bruno Stricker (PI Pharmaco-epidemiology), Henning Tiemeier (PI Psychiatric diseases), André Uitterlinden (PI Genomic studies), and Meike Vernooij (PI Population Imaging); and Jan Heeringa, MD, PhD, study coordinator, Eric Neeleman, head IT, and Frank van Rooij, DSc, head data-management. The study of respiratory diseases is conducted in close collaboration with Prof Guy Brusselle, Department of Respiratory Medicine, University of Gent, Belgium.
The following persons are Principal Investigator Emeritus of the Rotterdam Study: Frank van den Ouweland (PI Internal Medicine 1990–1992), Diederick Grobbee (PI Cardiovascular diseases 1990–1996), Albert Hofman (PI Neurological diseases 1990–1996), Paulus de Jong (PI Ophthalmic diseases 1990–2005), Huibert Pols (PI Internal Medicine 1993–2006), Monique Breteler (PI Neurological diseases 1997–2010), Gabriel Krestin (PI Population Imaging 1998–2010), Johannes Vingerling (PI Ophthalmic diseases 2005–2010), Jacqueline Witteman (PI Cardiovascular diseases 1997–2011).
References
Oeppen J, Vaupel JW. Demography. Broken limits to life expectancy. Science. 2002;296(5570):1029–31.
Peto R, Doll R. There is no such thing as aging. BMJ. 1997;315(7115):1030–2.
Hofman A, Grobbee DE, de Jong PT, van den Ouweland FA. Determinants of disease and disability in the elderly: the Rotterdam Elderly Study. Eur J Epidemiol. 1991;7(4):403–22.
Hofman A, Breteler MM, van Duijn CM, Krestin GP, Pols HA, Stricker BH, et al. The Rotterdam Study: objectives and design update. Eur J Epidemiol. 2007;22(11):819–29.
Hofman A, Breteler MM, van Duijn CM, Janssen HL, Krestin GP, Kuipers EJ, et al. The Rotterdam Study: 2010 objectives and design update. Eur J Epidemiol. 2009;24(9):553–72.
Hepworth SJ, Law GR, Lawlor DA, McKinney PA. Early life patterns of common infection: a latent class analysis. Eur J Epidemiol. 2010;25(12):875–83.
Gao X, Hofman A, Hu Y, Lin HD, Zhu CW, Jeekel J, et al. The Shanghai Changfeng Study: a community-based prospective cohort study of chronic diseases among middle-aged and elderly: objectives and design. Eur J Epidemiol. 2010;25(12):885–93.
Jaddoe VWV, van Duijn CM, van der Heijden AJ, Mackenbach JP, Moll HA, Steegers EAP, et al. The Generation R Study: design and cohort update 2010. Eur J Epidemiol. 2010;25(11):823–41.
Miettinen OS. Etiologic study vis-A-vis intervention study. Eur J Epidemiol. 2010;25(10):671–5.
Stang A. Critical evaluation of the Newcastle-Ottawa scale for the assessment of the quality of nonrandomized studies in meta-analyses. Eur J Epidemiol. 2010;25(9):603–5.
Harteloh P, de Bruin K, Kardaun J. The reliability of cause-of-death coding in The Netherlands. Eur J Epidemiol. 2010;25(8):531–8.
Pomp ER, Van Stralen KJ, Le Cessie S, Vandenbroucke JP, Rosendaal FR, Doggen CJM. Experience with multiple control groups in a large population-based case-control study on genetic and environmental risk factors. Eur J Epidemiol. 2010;25(7):459–66.
Schmidt-Pokrzywniak A, Stang A. Study of return rate and return time of undeliverable postal letters. Eur J Epidemiol. 2010;25(7):467–70.
Touvier M, Mejean C, Kesse-Guyot E, Pollet C, Malon A, Castetbon K, et al. Comparison between web-based and paper versions of a self-administered anthropometric questionnaire. Eur J Epidemiol. 2010;25(5):287–96.
Huybrechts KF, Mikkelsen EM, Christensen T, Riis AH, Hatch EE, Wise LA, et al. A successful implementation of e-epidemiology: the Danish pregnancy planning study ‘Snart-Gravid’. Eur J Epidemiol. 2010;25(5):297–304.
Jacobsen TN, Nohr EA, Frydenberg M. Selection by socioeconomic factors into the Danish National Birth Cohort. Eur J Epidemiol. 2010;25(5):349–55.
Wenemark M, Vernby A, Norberg AL. Can incentives undermine intrinsic motivation to participate in epidemiologic surveys? Eur J Epidemiol. 2010;25(4):231–5.
Kristensen P, Bjerkedal T. Dealing with emigration in cohort studies: follow-up of mortality and cancer incidence among Norwegians born between 1967 and 1976. Eur J Epidemiol. 2010;25(3):155–61.
Strandhagen E, Berg C, Lissner L, Nunez L, Rosengren A, Toren K, et al. Selection bias in a population survey with registry linkage: potential effect on socioeconomic gradient in cardiovascular risk. Eur J Epidemiol. 2010;25(3):163–72.
Tolonen H, Laatikainen T, Helakorpi S, Talala K, Martelin T, Prattala R. Marital status, educational level and household income explain part of the excess mortality of survey non-respondents. Eur J Epidemiol. 2010;25(2):69–76.
Walter S, Tiemeier H. Variable selection: current practice in epidemiological studies. Eur J Epidemiol. 2009;24(12):733–6.
Ludvigsson JF, Otterblad-Olausson P, Pettersson BU, Ekbom A. The Swedish personal identity number: possibilities and pitfalls in healthcare and medical research. Eur J Epidemiol. 2009;24(11):659–67.
Alperovitch A, Bertrand M, Jougla E, Vidal JS, Ducimetiere P, Helmer C, et al. Do we really know the cause of death of the very old? Comparison between official mortality statistics and cohort study classification. Eur J Epidemiol. 2009;24(11):669–75.
Stolk RP, Hutter I, Wittek RPM. Population ageing research: a family of disciplines. Eur J Epidemiol. 2009;24(11):715–8.
Nur U, Longford NT, Cade JE, Greenwood DC. The impact of handling missing data on alcohol consumption estimates in the UK women cohort study. Eur J Epidemiol. 2009;24(10):589–95.
Hofman A, Breteler MMB, van Duijn CM, Janssen HLA, Krestin GP, Kuipers EJ, et al. The Rotterdam Study: 2010 objectives and design update. Eur J Epidemiol. 2009;24(9):553–72.
Barakat-Haddad CP, Elliott S, Eyles J, Pengelly D. Predictors of locating children participants in epidemiological studies 20 years after last contact: internet resources and longitudinal research. Eur J Epidemiol. 2009;24(8):397–405.
Merry AHH, Boer JMA, Schouten LJ, Feskens EJM, Verschuren WMM, Gorgels APM, et al. Validity of coronary heart diseases and heart failure based on hospital discharge and mortality data in The Netherlands using the cardiovascular registry Maastricht cohort study. Eur J Epidemiol. 2009;24(5):237–47.
Bonneux LGA. Medical demography and epidemiology: dizygotic twins. Eur J Epidemiol. 2009;24(4):157–9.
Lagerros YT, Bellocco R, Adami HO, Nyren O. Measures of physical activity and their correlates: The Swedish National March Cohort. Eur J Epidemiol. 2009;24(4):161–9.
Jacobi D, Charles MA, Tafflet M, Lommez A, Borys JM, Oppert JM. Relationships of self-reported physical activity domains with accelerometry recordings in French adults. Eur J Epidemiol. 2009;24(4):171–9.
Lagerros Y. Physical activity-the more we measure, the more we know how to measure. Eur J Epidemiol. 2009;24(3):119–22.
de Torbal A, Boersma E, Kors JA, van Herpen G, Deckers JW, van der Kuip DA, et al. Incidence of recognized and unrecognized myocardial infarction in men and women aged 55 and older: the Rotterdam Study. Eur Heart J. 2006;27(6):729–36.
Hak AE, Pols HA, Visser TJ, Drexhage HA, Hofman A, Witteman JC. Subclinical hypothyroidism is an independent risk factor for atherosclerosis and myocardial infarction in elderly women: the Rotterdam Study. Ann Intern Med. 2000;132(4):270–8.
Rutten JH, Mattace-Raso FU, Steyerberg EW, Lindemans J, Hofman A, Wieberdink RG, et al. Amino-terminal pro-B-type natriuretic peptide improves cardiovascular and cerebrovascular risk prediction in the population: the Rotterdam Study. Hypertension. 2010;55(3):785–91.
Kardys I, de Maat MP, Uitterlinden AG, Hofman A, Witteman JC. C-reactive protein gene haplotypes and risk of coronary heart disease: the Rotterdam Study. Eur Heart J. 2006;27(11):1331–7.
Oei HH, van der Meer IM, Hofman A, Koudstaal PJ, Stijnen T, Breteler MM, et al. Lipoprotein-associated phospholipase A2 activity is associated with risk of coronary heart disease and ischemic stroke: the Rotterdam Study. Circulation. 2005;111(5):570–5.
van der Bom JG, de Knijff P, Haverkate F, Bots ML, Meijer P, de Jong PT, et al. Tissue plasminogen activator and risk of myocardial infarction: the Rotterdam Study. Circulation. 1997;95(12):2623–7.
Bots ML, Hoes AW, Koudstaal PJ, Hofman A, Grobbee DE. Common carotid intima-media thickness and risk of stroke and myocardial infarction: the Rotterdam Study. Circulation. 1997;96(5):1432–7.
Mattace-Raso FU, van der Cammen TJ, Hofman A, van Popele NM, Bos ML, Schalekamp MA, et al. Arterial stiffness and risk of coronary heart disease and stroke: the Rotterdam Study. Circulation. 2006;113(5):657–63.
Vliegenthart R, Oudkerk M, Hofman A, Oei HH, van Dijck W, van Rooij FJ, et al. Coronary calcification improves cardiovascular risk prediction in the elderly. Circulation. 2005;112(4):572–7.
van der Meer IM, Bots ML, Hofman A, del Sol AI, van der Kuip DA, Witteman JC. Predictive value of noninvasive measures of atherosclerosis for incident myocardial infarction: the Rotterdam Study. Circulation. 2004;109(9):1089–94.
Elias-Smale SE, Proenca RV, Koller MT, Kavousi M, van Rooij FJ, Hunink MG, et al. Coronary calcium score improves classification of coronary heart disease risk in the elderly: the Rotterdam Study. J Am Coll Cardiol. 2010;56(17):1407–14.
Kardys I, Klaver CC, Despriet DD, Bergen AA, Uitterlinden AG, Hofman A, et al. A common polymorphism in the complement factor H gene is associated with increased risk of myocardial infarction: the Rotterdam Study. J Am Coll Cardiol. 2006;47(8):1568–75.
Psaty BM, O’Donnell CJ, Gudnason V, Lunetta KL, Folsom AR, Rotter JI, et al. Cohorts for Heart and Aging Research in Genomic Epidemiology (CHARGE) Consortium: design of prospective meta-analyses of genome-wide association studies from 5 cohorts. Circ Cardiovasc Genet. 2009;2(1):73–80.
Dehghan A, Kottgen A, Yang Q, Hwang SJ, Kao WL, Rivadeneira F, et al. Association of three genetic loci with uric acid concentration and risk of gout: a genome-wide association study. Lancet. 2008;372(9654):1953–61.
Kottgen A, Glazer NL, Dehghan A, Hwang SJ, Katz R, Li M, et al. Multiple loci associated with indices of renal function and chronic kidney disease. Nat Genet. 2009;41(6):712–7.
Ganesh SK, Zakai NA, van Rooij FJ, Soranzo N, Smith AV, Nalls MA, et al. Multiple loci influence erythrocyte phenotypes in the CHARGE Consortium. Nat Genet. 2009;41(11):1191–8.
Levy D, Ehret GB, Rice K, Verwoert GC, Launer LJ, Dehghan A, et al. Genome-wide association study of blood pressure and hypertension. Nat Genet. 2009;41(6):677–87.
Dehghan A, Dupuis J, Barbalic M, Bis JC, Eiriksdottir G, Lu C, et al. Meta-analysis of genome-wide association studies in >80,000 subjects identifies multiple loci for C-reactive protein levels. Circulation. 2011;123(7):731–8.
Smith NL, Chen MH, Dehghan A, Strachan DP, Basu S, Soranzo N, et al. Novel associations of multiple genetic loci with plasma levels of factor VII, factor VIII, and von Willebrand factor: The CHARGE (Cohorts for Heart and Aging Research in Genome Epidemiology) Consortium. Circulation. 2010;121(12):1382–92.
Bleumink GS, Knetsch AM, Sturkenboom MC, Straus SM, Hofman A, Deckers JW, et al. Quantifying the heart failure epidemic: prevalence, incidence rate, lifetime risk and prognosis of heart failure: the Rotterdam Study. Eur Heart J. 2004;25(18):1614–9.
Heeringa J, van der Kuip DA, Hofman A, Kors JA, van Herpen G, Stricker BH, et al. Prevalence, incidence and lifetime risk of atrial fibrillation: the Rotterdam Study. Eur Heart J. 2006;27(8):949–53.
van Vark LC, Kardys I, Bleumink GS, Knetsch AM, Deckers JW, Hofman A, et al. Lipoprotein-associated phospholipase A2 activity and risk of heart failure: the Rotterdam Study. Eur Heart J. 2006;27(19):2346–52.
Heeringa J, Kors JA, Hofman A, van Rooij FJ, Witteman JC. Cigarette smoking and risk of atrial fibrillation: the Rotterdam Study. Am Heart J. 2008;156(6):1163–9.
Heeringa J, Hoogendoorn EH, van der Deure WM, Hofman A, Peeters RP, Hop WC, et al. High-normal thyroid function and risk of atrial fibrillation: the Rotterdam Study. Arch Intern Med. 2008;168(20):2219–24.
Heeringa J, van der Kuip DA, Hofman A, Kors JA, van Rooij FJ, Lip GY, et al. Subclinical atherosclerosis and risk of atrial fibrillation: the Rotterdam Study. Arch Intern Med. 2007;167(4):382–7.
Vasan RS, Glazer NL, Felix JF, Lieb W, Wild PS, Felix SB, et al. Genetic variants associated with cardiac structure and function: a meta-analysis and replication of genome-wide association data. JAMA. 2009;302(2):168–78.
Pfeufer A, van Noord C, Marciante KD, Arking DE, Larson MG, Smith AV, et al. Genome-wide association study of PR interval. Nat Genet. 2010;42(2):153–9.
Benjamin EJ, Rice KM, Arking DE, Pfeufer A, van Noord C, Smith AV, et al. Variants in ZFHX3 are associated with atrial fibrillation in individuals of European ancestry. Nat Genet. 2009;41(8):879–81.
Dehghan A, Kardys I, de Maat MP, Uitterlinden AG, Sijbrands EJ, Bootsma AH, et al. Genetic variation, C-reactive protein levels, and incidence of diabetes. Diabetes. 2007;56(3):872–8.
Straus SM, Kors JA, De Bruin ML, van der Hooft CS, Hofman A, Heeringa J, et al. Prolonged QTc interval and risk of sudden cardiac death in a population of older adults. J Am Coll Cardiol. 2006;47(2):362–7.
Kardys I, Deckers JW, Stricker BH, Vletter WB, Hofman A, Witteman J. Distribution of echocardiographic parameters and their associations with cardiovascular risk factors in the Rotterdam Study. Eur J Epidemiol. 2010;25(7):481–90.
Bellocco R, Jia CQ, Ye WM, Lagerros YT. Effects of physical activity, body mass index, waist-to-hip ratio and waist circumference on total mortality risk in the Swedish National March Cohort. Eur J Epidemiol. 2010;25(11):777–88.
Lindman AS, Veierod MB, Tverdal A, Pedersen JI, Selmer R. Nonfasting triglycerides and risk of cardiovascular death in men and women from the Norwegian Counties Study. Eur J Epidemiol. 2010;25(11):789–98.
Alberts VP, Bos MJ, Koudstaal PJ, Hofman A, Witteman JCM, Stricker BHC, et al. Heart failure and the risk of stroke: the Rotterdam Study. Eur J Epidemiol. 2010;25(11):807–12.
Geelhoed JJM, Jaddoe VWV. Early influences on cardiovascular and renal development. Eur J Epidemiol. 2010;25(10):677–92.
Daniel M, Paquet C, Auger N, Zang G, Kestens Y. Association of fast-food restaurant and fruit and vegetable store densities with cardiovascular mortality in a metropolitan population. Eur J Epidemiol. 2010;25(10):711–9.
Waller K, Kujala UM, Rantanen T, Kauppinen M, Silventoinen K, Koskenvuo M, et al. Physical activity, morbidity and mortality in twins: a 24-year prospective follow-up. Eur J Epidemiol. 2010;25(10):731–9.
Kallberg H, Alfredsson L, Feychting M, Ahlbom A. Do split your epidemiological data reply. Eur J Epidemiol. 2010;25(10):760.
Savela S, Koistinen P, Tilvis RS, Strandberg AY, Pitkala KH, Salomaa VV, et al. Leisure-time physical activity, cardiovascular risk factors and mortality during a 34-year follow-up in men. Eur J Epidemiol. 2010;25(9):619–25.
Carlsson AC, Theobald H, Wandell PE. Health factors and longevity in men and women: a 26-year follow-up study. Eur J Epidemiol. 2010;25(8):547–51.
Kettaneh A, Fardet L, Mario N, Retbi A, Taright N, Tiev K, et al. The 2003 heat wave in France: hydratation status changes in older inpatients. Eur J Epidemiol. 2010;25(7):517–24.
Leclerc A. Shift-work and cardiovascular disease. Eur J Epidemiol. 2010;25(5):285–6.
Thomas C, Power C. Shift work and risk factors for cardiovascular disease: a study at age 45 years in the 1958 British birth cohort. Eur J Epidemiol. 2010;25(5):305–14.
Hublin C, Partinen M, Koskenvuo K, Silventoinen K, Koskenvuo M, Kaprio J. Shift-work and cardiovascular disease: a population-based 22-year follow-up study. Eur J Epidemiol. 2010;25(5):315–23.
Alatupa S, Pulkki-Raback L, Hintsanen M, Ravaja N, Raitakari OT, Telama R, et al. School performance as a predictor of adulthood obesity: a 21-year follow-up study. Eur J Epidemiol. 2010;25(4):267–74.
Kvamme JM, Wilsgaard T, Florholmen J, Jacobsen BK. Body mass index and disease burden in elderly men and women: the Tromso Study. Eur J Epidemiol. 2010;25(3):183–93.
Schaeffner ES, van der Giet M, Gaedeke J, Tolle M, Ebert N, Kuhlmann MK, et al. The Berlin initiative study: the methodology of exploring kidney function in the elderly by combining a longitudinal and cross-sectional approach. Eur J Epidemiol. 2010;25(3):203–10.
Bonneux LG, Huisman CC, de Beer JA. Mortality in 272 European regions, 2002–2004. An update. Eur J Epidemiol. 2010;25(2):77–85.
Smith JG, Platonov PG, Hedblad B, Engstrom G, Melander O. Atrial fibrillation in the Malmo diet and cancer study: a study of occurrence, risk factors and diagnostic validity. Eur J Epidemiol. 2010;25(2):95–102.
van Noord C, Dorr M, Sturkenboom M, Straus S, Reffelmann T, Felix SB, et al. The association of serum testosterone levels and ventricular repolarization. Eur J Epidemiol. 2010;25(1):21–8.
Hofman A. Recent trends in cardiovascular epidemiology. Eur J Epidemiol. 2009;24(12):721–3.
Thelle DS. The dynamics of cardiovascular epidemiology. Eur J Epidemiol. 2009;24(12):725–6.
Gulsvik AK, Thelle DS, Mowe M, Wyller TB. Increased mortality in the slim elderly: a 42 years follow-up study in a general population. Eur J Epidemiol. 2009;24(11):683–90.
Wiesbauer F, Blessberger H, Goliasch G, Holy EW, Pfaffenberger S, Tentzeris I, et al. Elevated risk of myocardial infarction in very young immigrants from former Yugoslavia. Eur J Epidemiol. 2009;24(11):691–6.
Gasparrini A, Gorini G, Barchielli A. On the relationship between smoking bans and incidence of acute myocardial infarction. Eur J Epidemiol. 2009;24(10):597–602.
Setia MS, Quesnel-Vallee A, Abrahamowicz M, Tousignant P, Lynch J. Convergence of body mass index of immigrants to the Canadian-born population: evidence from the National Population Health Survey (1994–2006). Eur J Epidemiol. 2009;24(10):611–23.
Rey G, Fouillet A, Bessemoulin P, Frayssinet P, Dufour A, Jougla E, et al. Heat exposure and socio-economic vulnerability as synergistic factors in heat-wave-related mortality. Eur J Epidemiol. 2009;24(9):495–502.
Regidor E, Astasio P, Calle ME, Martinez D, Ortega P, Dominguez V. The association between birthplace in different regions of the world and cardiovascular mortality among residents of Spain. Eur J Epidemiol. 2009;24(9):503–12.
Hertel S, Le Tertre A, Jockel KH, Hoffmann B. Quantification of the heat wave effect on cause-specific mortality in Essen, Germany. Eur J Epidemiol. 2009;24(8):407–14.
Chimonas T, Fanouraki I, Liberopoulos EN, Chimonas E, Elisaf M. Diverging trends in cardiovascular morbidity and mortality in a low risk population. Eur J Epidemiol. 2009;24(8):415–23.
Oliveira A, Barros H, Azevedo A, Bastos J, Lopes C. Impact of risk factors for non-fatal acute myocardial infarction. Eur J Epidemiol. 2009;24(8):425–32.
Schlaefer K, Schlehofer B, Schuz J. Validity of self-reported occupational noise exposure. Eur J Epidemiol. 2009;24(8):469–75.
Mayer O, Simon J, Plaskova M, Cifkova R, Trefil L. N-terminal pro B-type natriuretic peptide as prognostic marker for mortality in coronary patients without clinically manifest heart failure. Eur J Epidemiol. 2009;24(7):363–8.
Pearce MS, Relton CL, Parker L, Unwin NC. Sex differences in the association between infant feeding and blood cholesterol in later life: the Newcastle thousand families cohort study at age 49–51 years. Eur J Epidemiol. 2009;24(7):375–80.
Dorr M, Wallaschofski H, Friedrich N. Association of low total testosterone levels and prevalent carotid plaques: result of the study of health in Pomerania. Eur J Epidemiol. 2009;24(7):389–91.
Corpeleijn E, Bakker SJL, Stolk RP. Obesity and impaired renal function: potential for lifestyle intervention? Eur J Epidemiol. 2009;24(6):275–80.
Vikan T, Johnsen SH, Schirmer H, Njolstad I, Svartberg J. Endogenous testosterone and the prospective association with carotid atherosclerosis in men: the Tromso study. Eur J Epidemiol. 2009;24(6):289–95.
Fallah N, Mohammad K, Nourijelyani K, Eshraghian MR, Seyyedsalehi SA, Raiessi M, et al. Nonlinear association between serum testosterone levels and coronary artery disease in Iranian men. Eur J Epidemiol. 2009;24(6):297–306.
Ruan LT, Chen W, Srinivasan S, Xu JH, Toprak A, Berenson G. Plasma homocysteine is adversely associated with glomerular filtration rate in asymptomatic black and white young adults: the Bogalusa heart study. Eur J Epidemiol. 2009;24(6):315–9.
Saleheen D, Zaidi M, Rasheed A, Ahmad U, Hakeem A, Murtaza M, et al. The Pakistan Risk of Myocardial Infarction Study: a resource for the study of genetic, lifestyle and other determinants of myocardial infarction in South Asia. Eur J Epidemiol. 2009;24(6):329–38.
Tasevska-Dinevska G, Kennedy LMA, Nilsson PM, Willenheimer R. Gender aspects on heart failure incidence and mortality in a middle-aged, urban, community-based population sample: the Malmo preventive project. Eur J Epidemiol. 2009;24(5):249–57.
Zheng H, Orsini N, Amin J, Wolk A, Nguyen VTT, Ehrlich F. Quantifying the dose-response of walking in reducing coronary heart disease risk: meta-analysis. Eur J Epidemiol. 2009;24(4):181–92.
Greiser KH, Kluttig A, Schumann B, Swenne CA, Kors JA, Kuss O, et al. Cardiovascular diseases, risk factors and short-term heart rate variability in an elderly general population: the CARLA study 2002–2006. Eur J Epidemiol. 2009;24(3):123–42.
Jaffe DH, Neumark YD, Eisenbach Z, Manor O. Parity-related mortality: shape of association among middle-aged and elderly men and women. Eur J Epidemiol. 2009;24(1):9–16.
Dragano N, Hoffmann B, Stang A, Moebus S, Verde PE, Weyers S, et al. Subclinical coronary atherosclerosis and neighbourhood deprivation in an urban region. Eur J Epidemiol. 2009;24(1):25–35.
Osler M, Lund R, Kriegbaum M, Andersen AMN. The influence of birth weight and body mass in early adulthood on early coronary heart disease risk among Danish men born in 1953. Eur J Epidemiol. 2009;24(1):57–61.
Klenk J, Nagel G, Ulmer H, Strasak A, Concin H, Diem G, et al. Body mass index and mortality: results of a cohort of 184,697 adults in Austria. Eur J Epidemiol. 2009;24(2):83–91.
Turin TC, Kita Y, Rumana N, Sugihara H, Morita Y, Tomioka N, et al. Incidence, admission and case-fatality of acute myocardial infarction: weekend versus weekday in a Japanese population: 16-year results from Takashima AMI Registry (1988–2003). Eur J Epidemiol. 2009;24(2):93–100.
Zhang HL, Yang Y, Wu JA. Can prevalence of apolipoprotein E epsilon 4 allele explain the geographical variation of coronary heart disease mortality rates in Western Europe? Eur J Epidemiol. 2010;25(12):897–8.
Kiiski V, de Vries E, Flohil SC, Bijl MJ, Hofman A, Stricker BH, et al. Risk factors for single and multiple basal cell carcinomas. Arch Dermatol. 2010;146(8):848–55.
Flohil SC, de Vries E, van Meurs JB, Fang Y, Stricker BH, Uitterlinden AG, et al. Vitamin D-binding protein polymorphisms are not associated with development of (multiple) basal cell carcinomas. Exp Dermatol. 2010;19(12):1103–5.
Odding E, Valkenburg HA, Stam HJ, Hofman A. Determinants of locomotor disability in people aged 55 years and over: the Rotterdam Study. Eur J Epidemiol. 2001;17(11):1033–41.
Tas U, Verhagen AP, Bierma-Zeinstra SM, Hofman A, Odding E, Pols HA, et al. Incidence and risk factors of disability in the elderly: the Rotterdam Study. Prev Med. 2007;44(3):272–8.
Van der Klift M, De Laet CE, McCloskey EV, Hofman A, Pols HA. The incidence of vertebral fractures in men and women: the Rotterdam Study. J Bone Miner Res. 2002;17(6):1051–6.
Schuit SC, van der Klift M, Weel AE, de Laet CE, Burger H, Seeman E, et al. Fracture incidence and association with bone mineral density in elderly men and women: the Rotterdam Study. Bone. 2004;34(1):195–202.
van Daele PL, Burger H, Algra D, Hofman A, Grobbee DE, Birkenhager JC, et al. Age-associated changes in ultrasound measurements of the calcaneus in men and women: the Rotterdam Study. J Bone Miner Res. 1994;9(11):1751–7.
van Daele PL, Seibel MJ, Burger H, Hofman A, Grobbee DE, van Leeuwen JP, et al. Case–control analysis of bone resorption markers, disability, and hip fracture risk: the Rotterdam Study. BMJ. 1996;312(7029):482–3.
Goderie-Plomp HW, van der Klift M, de Ronde W, Hofman A, de Jong FH, Pols HA. Endogenous sex hormones, sex hormone-binding globulin, and the risk of incident vertebral fractures in elderly men and women: the Rotterdam Study. J Clin Endocrinol Metab. 2004;89(7):3261–9.
van Meurs JB, Dhonukshe-Rutten RA, Pluijm SM, van der Klift M, de Jonge R, Lindemans J, et al. Homocysteine levels and the risk of osteoporotic fracture. N Engl J Med. 2004;350(20):2033–41.
Bergink AP, Uitterlinden AG, Van Leeuwen JP, Hofman A, Verhaar JA, Pols HA. Bone mineral density and vertebral fracture history are associated with incident and progressive radiographic knee osteoarthritis in elderly men and women: the Rotterdam Study. Bone. 2005;37(4):446–56.
van der Klift M, de Laet CE, Coebergh JW, Hofman A, Pols HA, Rotterdam S. Bone mineral density and the risk of breast cancer: the Rotterdam Study. Bone. 2003;32(3):211–6.
van der Klift M, Pols HA, Hak AE, Witteman JC, Hofman A, de Laet CE. Bone mineral density and the risk of peripheral arterial disease: the Rotterdam Study. Calcif Tissue Int. 2002;70(6):443–9.
van Daele PL, Stolk RP, Burger H, Algra D, Grobbee DE, Hofman A, et al. Bone density in non-insulin-dependent diabetes mellitus: the Rotterdam Study. Ann Intern Med. 1995;122(6):409–14.
de Liefde II, van der Klift M, de Laet CE, van Daele PL, Hofman A, Pols HA. Bone mineral density and fracture risk in type-2 diabetes mellitus: the Rotterdam Study. Osteoporos Int. 2005;16(12):1713–20.
van der Klift M, de Laet CD, Pols HA. Assessment of fracture risk: who should be treated for osteoporosis? Best Pract Res Clin Rheumatol. 2005;19(6):937–50.
de Laet CE, van der Klift M, Hofman A, Pols HA. Osteoporosis in men and women: a story about bone mineral density thresholds and hip fracture risk. J Bone Miner Res. 2002;17(12):2231–6.
De Laet C, Kanis JA, Oden A, Johanson H, Johnell O, Delmas P, et al. Body mass index as a predictor of fracture risk: a meta-analysis. Osteoporos Int. 2005;16(11):1330–8.
Reijman M, Hazes JM, Bierma-Zeinstra SM, Koes BW, Christgau S, Christiansen C, et al. A new marker for osteoarthritis: cross-sectional and longitudinal approach. Arthritis Rheum. 2004;50(8):2471–8.
Reijman M, Hazes JM, Pols HA, Bernsen RM, Koes BW, Bierma-Zeinstra SM. Validity and reliability of three definitions of hip osteoarthritis: cross sectional and longitudinal approach. Ann Rheum Dis. 2004;63(11):1427–33.
Reijman M, Hazes JM, Pols HA, Bernsen RM, Koes BW, Bierma-Zeinstra SM. Role of radiography in predicting progression of osteoarthritis of the hip: prospective cohort study. BMJ. 2005;330(7501):1183.
Brouwer GM, van Tol AW, Bergink AP, Belo JN, Bernsen RM, Reijman M, et al. Association between valgus and varus alignment and the development and progression of radiographic osteoarthritis of the knee. Arthritis Rheum. 2007;56(4):1204–11.
Dahaghin S, Bierma-Zeinstra SM, Reijman M, Pols HA, Hazes JM, Koes BW. Does hand osteoarthritis predict future hip or knee osteoarthritis? Arthritis Rheum. 2005;52(11):3520–7.
Hak AE, Pols HA, Stehouwer CD, Meijer J, Kiliaan AJ, Hofman A, et al. Markers of inflammation and cellular adhesion molecules in relation to insulin resistance in nondiabetic elderly: the Rotterdam Study. J Clin Endocrinol Metab. 2001;86(9):4398–405.
Kalmijn S, Mehta KM, Pols HA, Hofman A, Drexhage HA, Breteler MM. Subclinical hyperthyroidism and the risk of dementia: the Rotterdam Study. Clin Endocrinol (Oxf). 2000;53(6):733–7.
Smit P, van Schaik RH, van der Werf M, van den Beld AW, Koper JW, Lindemans J, et al. A common polymorphism in the CYP3A7 gene is associated with a nearly 50% reduction in serum dehydroepiandrosterone sulfate levels. J Clin Endocrinol Metab. 2005;90(9):5313–6.
Rivadeneira F, van Meurs JB, Kant J, Zillikens MC, Stolk L, Beck TJ, et al. Estrogen receptor beta (ESR2) polymorphisms in interaction with estrogen receptor alpha (ESR1) and insulin-like growth factor I (IGF1) variants influence the risk of fracture in postmenopausal women. J Bone Miner Res. 2006;21(9):1443–56.
Rivadeneira F, Houwing-Duistermaat JJ, Beck TJ, Janssen JA, Hofman A, Pols HA, et al. The influence of an insulin-like growth factor I gene promoter polymorphism on hip bone geometry and the risk of nonvertebral fracture in the elderly: the Rotterdam Study. J Bone Miner Res. 2004;19(8):1280–90.
van Rossum EF, Koper JW, Huizenga NA, Uitterlinden AG, Janssen JA, Brinkmann AO, et al. A polymorphism in the glucocorticoid receptor gene, which decreases sensitivity to glucocorticoids in vivo, is associated with low insulin and cholesterol levels. Diabetes. 2002;51(10):3128–34.
den Heijer T, Schuit SC, Pols HA, van Meurs JB, Hofman A, Koudstaal PJ, et al. Variations in estrogen receptor alpha gene and risk of dementia, and brain volumes on MRI. Mol Psychiatry. 2004;9(12):1129–35.
Beck TJ, Ruff CB, Warden KE, Scott WW Jr, Rao GU. Predicting femoral neck strength from bone mineral data. A structural approach. Invest Radiol. 1990;25(1):6–18.
McCloskey EV, Spector TD, Eyres KS, Fern ED, O’Rourke N, Vasikaran S, et al. The assessment of vertebral deformity: a method for use in population studies and clinical trials. Osteoporos Int. 1993;3(3):138–47.
Jansson KA, Blomqvist P, Svedmark P, Granath F, Buskens E, Larsson M, et al. Thoracolumbar vertebral fractures in Sweden: an analysis of 13,496 patients admitted to hospital. Eur J Epidemiol. 2010;25(6):431–7.
Schuur M, Henneman P, van Swieten JC, Zillikens MC, de Koning I, Janssens A, et al. Insulin-resistance and metabolic syndrome are related to executive function in women in a large family-based study. Eur J Epidemiol. 2010;25(8):561–8.
Forsen L, Berntsen GK, Meyer HE, Tell GS, Fonnebo V, Group NCR. Differences in precision in bone mineral density measured by SXA and DXA: the NOREPOS study. Eur J Epidemiol. 2008;23(9):615–24.
Yaegashi Y, Onoda T, Tanno K, Kuribayashi T, Sakata K, Orimo H. Association of hip fracture incidence and intake of calcium, magnesium, vitamin D, and vitamin K. Eur J Epidemiol. 2008;23(3):219–25.
Siggeirsdottir K, Aspelund T, Sigurdsson G, Mogensen B, Chang M, Jonsdottir B, et al. Inaccuracy in self-report of fractures may underestimate association with health outcomes when compared with medical record based fracture registry. Eur J Epidemiol. 2007;22(9):631–9.
Yang YJ, Wang YB, Lei SF, Long JR, Shen H, Zhao LJ, et al. AHSG gene polymorphisms are associated with bone mineral density in Caucasian nuclear families. Eur J Epidemiol. 2007;22(8):527–32.
Hong X, Niu T, Chen C, Wang B, Venners SA, Fang Z, et al. Familial aggregation of forearm bone mineral density in Chinese. Eur J Epidemiol. 2007;22(5):335–41.
Piirtola M, Vahlberg T, Lopponen M, Raiha I, Isoaho R, Kivela SL. Fractures as predictors of excess mortality in the aged-a population-based study with a 12-year follow-up. Eur J Epidemiol. 2008;23(11):747–55.
Wallensten A, Oliver I, Ricketts K, Kafatos G, Stuart JM, Joseph C. Windscreen wiper fluid without added screenwash in motor vehicles: a newly identified risk factor for Legionnaires’ disease. Eur J Epidemiol. 2010;25(9):661–5.
Hui WS, Liu Z, Ho SC. Metabolic syndrome and all-cause mortality: a meta-analysis of prospective cohort studies. Eur J Epidemiol. 2010;25(6):375–84.
Kowall B, Rathmann W, Strassburger K, Heier M, Holle R, Thorand B, et al. Association of passive and active smoking with incident type 2 diabetes mellitus in the elderly population: the KORA S4/F4 cohort study. Eur J Epidemiol. 2010;25(6):393–402.
Morseth B, Emaus N, Wilsgaard T, Jacobsen BK, Jorgensen L. Leisure time physical activity in adulthood is positively associated with bone mineral density 22 years later. The Tromso study. Eur J Epidemiol. 2010;25(5):325–31.
Kataja-Tuomola M, Sundell J, Mannisto S, Virtanen MJ, Kontto J, Albanes D, et al. Short-term weight change and fluctuation as risk factors for type 2 diabetes in Finnish male smokers. Eur J Epidemiol. 2010;25(5):333–9.
Nagaya T, Yoshida H, Takahashi H, Kawai M. Heart rate-corrected QT interval in resting ECG predicts the risk for development of type-2 diabetes mellitus. Eur J Epidemiol. 2010;25(3):195–202.
Laaksonen MA, Knekt P, Rissanen H, Harkanen T, Virtala E, Marniemi J, et al. The relative importance of modifiable potential risk factors of type 2 diabetes: a meta-analysis of two cohorts. Eur J Epidemiol. 2010;25(2):115–24.
Bot M, Spijkerman AMW, Twisk JWR, Verschuren WMM. Weight change over five-year periods and number of components of the metabolic syndrome in a Dutch cohort. Eur J Epidemiol. 2010;25(2):125–33.
Qin L, Knol MJ, Corpeleijn E, Stolk RP. Does physical activity modify the risk of obesity for type 2 diabetes: a review of epidemiological data. Eur J Epidemiol. 2010;25(1):5–12.
Manda SOM, Feltbower RG, Gilthorpe MS. Investigating spatio-temporal similarities in the epidemiology of childhood leukaemia and diabetes. Eur J Epidemiol. 2009;24(12):743–52.
Bruyere O, Varela AR, Adami S, Detilleux J, Rabenda V, Hiligsmann M, et al. Loss of hip bone mineral density over time is associated with spine and hip fracture incidence in osteoporotic postmenopausal women. Eur J Epidemiol. 2009;24(11):707–12.
Nguyen QM, Srinivasan SR, Xu JH, Chen W, Berenson GS. Influence of childhood parental history of type 2 diabetes on the pre-diabetic and diabetic status in adulthood: the Bogalusa Heart Study. Eur J Epidemiol. 2009;24(9):537–9.
Ahmed LA, Schirmer H, Bjornerem A, Emaus N, Jorgensen L, Stormer J, et al. The gender- and age-specific 10-year and lifetime absolute fracture risk in Tromso, Norway. Eur J Epidemiol. 2009;24(8):441–8.
Sylliaas H, Idland G, Sandvik L, Forsen L, Bergland A. Does mortality of the aged increase with the number of falls? Results from a nine-year follow-up study. Eur J Epidemiol. 2009;24(7):351–5.
Bloch F, Jegou D, Dhainaut JF, Rigaud AS, Coste J, Lundy JE, et al. Can metabolic abnormalities after a fall predict short term mortality in elderly patients? Eur J Epidemiol. 2009;24(7):357–62.
Sabanayagam C, Shankar A, Li JL, Pollard C, Ducatman A. Serum gamma-glutamyl transferase level and diabetes mellitus among US adults. Eur J Epidemiol. 2009;24(7):369–73.
Olafsdottir E, Aspelund T, Sigurdsson G, Thorsson B, Benediktsson R, Harris TB, et al. Unfavourable risk factors for type 2 diabetes mellitus are already apparent more than a decade before onset in a population-based study of older persons: from the Age, Gene/Environment Susceptibility-Reykjavik Study (AGES-Reykjavik). Eur J Epidemiol. 2009;24(6):307–14.
Emaus N, Omsland TK, Ahmed LA, Grimnes G, Sneve M, Berntsen GK. Bone mineral density at the hip in Norwegian women and men-prevalence of osteoporosis depends on chosen references: the Tromso Study. Eur J Epidemiol. 2009;24(6):321–8.
Moayyeri A, Kaptoge S, Luben RN, Wareham NJ, Bingham S, Reeve J, et al. Estimation of absolute fracture risk among middle-aged and older men and women: the EPIC-Norfolk population cohort study. Eur J Epidemiol. 2009;24(5):259–66.
Balk L, Hoekstra T, Twisk J. Relationship between long-term coffee consumption and components of the metabolic syndrome: the Amsterdam Growth and Health Longitudinal Study. Eur J Epidemiol. 2009;24(4):203–9.
de Sousa AGP, Pereira AC, Marquezine GF, do Nascimento-Neto RM, Freitas S, Nicolato RLD, et al. Derivation and external validation of a simple prediction model for the diagnosis of type 2 Diabetes Mellitus in the Brazilian urban population. Eur J Epidemiol. 2009;24(2):101–9.
Hamaguchi M, Kojima T, Itoh Y, Harano Y, Fujii K, Nakajima T, et al. The severity of ultrasonographic findings in nonalcoholic fatty liver disease reflects the metabolic syndrome and visceral fat accumulation. Am J Gastroenterol. 2007;102(12):2708–15.
Sandrin L, Fourquet B, Hasquenoph JM, Yon S, Fournier C, Mal F, et al. Transient elastography: a new noninvasive method for assessment of hepatic fibrosis. Ultrasound Med Biol. 2003;29(12):1705–13.
Talwalkar JA, Kurtz DM, Schoenleber SJ, West CP, Montori VM. Ultrasound-based transient elastography for the detection of hepatic fibrosis: systematic review and meta-analysis. Clin Gastroenterol Hepatol. 2007;5(10):1214–20.
Santibanez M, Vioque J, Alguacil J, de la Hera MG, Moreno-Osset E, Carrato A, et al. Occupational exposures and risk of pancreatic cancer. Eur J Epidemiol. 2010;25(10):721–30.
Aro P, Ronkainen J, Storskrubb T, Vieth M, Engstrand L, Johansson SE, et al. Use of tobacco products and gastrointestinal morbidity: an endoscopic population-based study (the Kalixanda study). Eur J Epidemiol. 2010;25(10):741–50.
Adamu MA, Weck MN, Gao L, Brenner H. Incidence of chronic atrophic gastritis: systematic review and meta-analysis of follow-up studies. Eur J Epidemiol. 2010;25(7):439–48.
Schmeisser N, Conway DI, McKinney PA, McMahon AD, Pohlabeln H, Marron M, et al. Life course social mobility and risk of upper aerodigestive tract cancer in men. Eur J Epidemiol. 2010;25(3):173–82.
Schmassmann A, Oldendorf MG, Gebbers JO. Changing incidence of gastric and oesophageal cancer subtypes in central Switzerland between 1982 and 2007. Eur J Epidemiol. 2009;24(10):603–9.
Asfeldt AM, Steigen SE, Lochen ML, Straume B, Johnsen R, Bernersen B, et al. The natural course of Helicobacter pylori infection on endoscopic findings in a population during 17 years of follow-up: the Sorreisa gastrointestinal disorder study. Eur J Epidemiol. 2009;24(10):649–58.
Erichsen R, Jepsen P, Vilstrup H, Ekbom A, Sorensen HT. Incidence and prognosis of cholangiocarcinoma in Danish patients with and without inflammatory bowel disease: a national cohort study, 1978–2003. Eur J Epidemiol. 2009;24(9):513–20.
Watanabe H, Kamijima Y, Sato T, Kaufman DW, Kubota K. Ex-drinking may be a surrogate for unmeasured risk factors for upper gastrointestinal bleeding: reappraisal and an additional survey of subjects from a case–control study in Japan. Eur J Epidemiol. 2009;24(3):143–7.
Ott A, Breteler MM, van Harskamp F, Claus JJ, van der Cammen TJ, Grobbee DE, et al. Prevalence of Alzheimer’s disease and vascular dementia: association with education: the Rotterdam Study. BMJ. 1995;310(6985):970–3.
de Rijk MC, Breteler MM, Graveland GA, Ott A, Grobbee DE, van der Meche FG, et al. Prevalence of Parkinson’s disease in the elderly: the Rotterdam Study. Neurology. 1995;45(12):2143–6.
Hollander M, Koudstaal PJ, Bots ML, Grobbee DE, Hofman A, Breteler MM. Incidence, risk, and case fatality of first ever stroke in the elderly population: the Rotterdam Study. J Neurol Neurosurg Psychiatry. 2003;74(3):317–21.
Ruitenberg A, Ott A, van Swieten JC, Hofman A, Breteler MM. Incidence of dementia: does gender make a difference? Neurobiol Aging. 2001;22(4):575–80.
de Lau LM, Giesbergen PC, de Rijk MC, Hofman A, Koudstaal PJ, Breteler MM. Incidence of Parkinsonism and Parkinson disease in a general population: the Rotterdam Study. Neurology. 2004;63(7):1240–4.
Breteler MM, Claus JJ, Grobbee DE, Hofman A. Cardiovascular disease and distribution of cognitive function in elderly people: the Rotterdam Study. BMJ. 1994;308(6944):1604–8.
Hofman A, Ott A, Breteler MM, Bots ML, Slooter AJ, van Harskamp F, et al. Atherosclerosis, apolipoprotein E, and prevalence of dementia and Alzheimer’s disease in the Rotterdam Study. Lancet. 1997;349(9046):151–4.
Ott A, Slooter AJ, Hofman A, van Harskamp F, Witteman JC, Van Broeckhoven C, et al. Smoking and risk of dementia and Alzheimer’s disease in a population-based cohort study: the Rotterdam Study. Lancet. 1998;351(9119):1840–3.
Engelhart MJ, Geerlings MI, Ruitenberg A, van Swieten JC, Hofman A, Witteman JC, et al. Dietary intake of antioxidants and risk of Alzheimer disease. JAMA. 2002;287(24):3223–9.
Ruitenberg A, van Swieten JC, Witteman JC, Mehta KM, van Duijn CM, Hofman A, et al. Alcohol consumption and risk of dementia: the Rotterdam Study. Lancet. 2002;359(9303):281–6.
int’ Veld BA, Ruitenberg A, Hofman A, Launer LJ, van Duijn CM, Stijnen T, et al. Nonsteroidal antiinflammatory drugs and the risk of Alzheimer’s disease. N Engl J Med. 2001;345(21):1515–21.
Euser SM, Sattar N, Witteman JC, Bollen EL, Sijbrands EJ, Hofman A, et al. A prospective analysis of elevated fasting glucose levels and cognitive function in older people: results from PROSPER and the Rotterdam Study. Diabetes. 2010;59(7):1601–7.
Euser SM, van Bemmel T, Schram MT, Gussekloo J, Hofman A, Westendorp RG, et al. The effect of age on the association between blood pressure and cognitive function later in life. J Am Geriatr Soc. 2009;57(7):1232–7.
Hollander M, Bots ML, Del Sol AI, Koudstaal PJ, Witteman JC, Grobbee DE, et al. Carotid plaques increase the risk of stroke and subtypes of cerebral infarction in asymptomatic elderly: the Rotterdam Study. Circulation. 2002;105(24):2872–7.
Bos MJ, Schipper CM, Koudstaal PJ, Witteman JC, Hofman A, Breteler MM. High serum C-reactive protein level is not an independent predictor for stroke: the Rotterdam Study. Circulation. 2006;114(15):1591–8.
Vermeer SE, Prins ND, den Heijer T, Hofman A, Koudstaal PJ, Breteler MM. Silent brain infarcts and the risk of dementia and cognitive decline. N Engl J Med. 2003;348(13):1215–22.
Seshadri S, Fitzpatrick AL, Ikram MA, DeStefano AL, Gudnason V, Boada M, et al. Genome-wide analysis of genetic loci associated with Alzheimer disease. JAMA. 2010;303(18):1832–40.
Ikram MA, Seshadri S, Bis JC, Fornage M, DeStefano AL, Aulchenko YS, et al. Genomewide association studies of stroke. N Engl J Med. 2009;360(17):1718–28.
Vernooij MW, Ikram MA, Tanghe HL, Vincent AJ, Hofman A, Krestin GP, et al. Incidental findings on brain MRI in the general population. N Engl J Med. 2007;357(18):1821–8.
Killgore WD, Glahn DC, Casasanto DJ. Development and validation of the design organization test (DOT): a rapid screening instrument for assessing visuospatial ability. J Clin Exp Neuropsychol. 2005;27(4):449–59.
Trouillas P, Takayanagi T, Hallett M, Currier RD, Subramony SH, Wessel K, et al. International Cooperative Ataxia Rating Scale for pharmacological assessment of the cerebellar syndrome. The Ataxia Neuropharmacology Committee of the World Federation of Neurology. J Neurol Sci. 1997;145(2):205–11.
Breteler MM, van Swieten JC, Bots ML, Grobbee DE, Claus JJ, van den Hout JH, et al. Cerebral white matter lesions, vascular risk factors, and cognitive function in a population-based study: the Rotterdam Study. Neurology. 1994;44(7):1246–52.
Vernooij MW, Ikram MA, Vrooman HA, Wielopolski PA, Krestin GP, Hofman A, et al. White matter microstructural integrity and cognitive function in a general elderly population. Arch Gen Psychiatry. 2009;66(5):545–53.
Sellier E, Surman G, Himmelmann K, Andersen G, Colver A, Krageloh-Mann I, et al. Trends in prevalence of cerebral palsy in children born with a birthweight of 2,500 g or over in Europe from 1980 to 1998. Eur J Epidemiol. 2010;25(9):635–42.
Heys M, Jiang CQ, Schooling CM, Zhang WS, Cheng KK, Lam TH, et al. Is childhood meat eating associated with better later adulthood cognition in a developing population? Eur J Epidemiol. 2010;25(7):507–16.
Risselada R, Lingsma HF, Bauer-Mehren A, Friedrich CM, Molyneux AJ, Kerr RSC, et al. Prediction of 60 day case-fatality after aneurysmal subarachnoid haemorrhage: results from the International Subarachnoid Aneurysm Trial (ISAT). Eur J Epidemiol. 2010;25(4):261–6.
Kerneis S, Boelle PY, Grais RF, Pavillon G, Jougla E, Flahault A, et al. Mortality trends in systemic sclerosis in France and USA, 1980–1998: an age-period-cohort analysis. Eur J Epidemiol. 2010;25(1):55–61.
Alonso A. Diagnostic validity of hospital discharge codes in the ascertainment of amyotrophic lateral sclerosis. Eur J Epidemiol. 2010;25(1):63.
Pisa FE, Verriello L, Deroma L, Drigo D, Bergonzi P, Gigli GL, et al. The accuracy of discharge diagnosis coding for Amyotrophic Lateral Sclerosis in a large teaching hospital. Eur J Epidemiol. 2009;24(10):635–40.
Ahlgren C, Toren K, Oden A, Andersen O. A population-based case–control study on viral infections and vaccinations and subsequent multiple sclerosis risk. Eur J Epidemiol. 2009;24(9):541–52.
Berg-Beckhoff G, Schuz J, Blettner M, Munster E, Schlaefer K, Wahrendorf J, et al. History of allergic disease and epilepsy and risk of glioma and meningioma (INTERPHONE study group, Germany). Eur J Epidemiol. 2009;24(8):433–40.
Baas DC, Ho L, Ennis S, Merriam JE, Tanck MW, Uitterlinden AG, et al. The complement component 5 gene and age-related macular degeneration. Ophthalmology. 2010;117(3):500–11.
Baas DC, Despriet DD, Gorgels TG, Bergeron-Sawitzke J, Uitterlinden AG, Hofman A, et al. The ERCC6 gene and age-related macular degeneration. PLoS One. 2010;5(11):e13786.
Allikmets R, Dean M, Hageman GS, Baird PN, Klaver CC, Bergen AA, et al. The SERPING1 gene and age-related macular degeneration. Lancet. 2009;374(9693):875–6 (author reply 6–7).
Allikmets R, Bergen AA, Dean M, Guymer RH, Hageman GS, Klaver CC, et al. Geographic atrophy in age-related macular degeneration and TLR3. N Engl J Med. 2009;360(21):2252–4 (author reply 5–6).
Ho L, van Leeuwen R, Witteman JC, van Duijn CM, Uitterlinden AG, Hofman A, et al. Reducing the genetic risk of age-related macular degeneration with dietary antioxidants, zinc, and {omega}-3 fatty acids: the Rotterdam Study. Arch Ophthalmol. 2011;129(6):758–66.
Ramdas WD, van Koolwijk LM, Ikram MK, Jansonius NM, de Jong PT, Bergen AA, et al. A genome-wide association study of optic disc parameters. PLoS Genet. 2010;6(6):e1000978.
Ramdas WD, van Koolwijk LM, Lemij HG, Pasutto F, Cree AJ, Thorleifsson G, et al. Common genetic variants associated with open-angle glaucoma. Hum Mol Genet. 2011;20(12):2464–71.
Ramdas WD, Amin N, van Koolwijk LM, Janssens AC, Demirkan A, de Jong PT, et al. Genetic architecture of open angle glaucoma and related determinants. J Med Genet. 2011;48(3):190–6.
Ramdas WD, Wolfs RC, Hofman A, de Jong PT, Vingerling JR, Jansonius NM. Lifestyle and risk of developing open-angle glaucoma: the Rotterdam Study. Arch Ophthalmol. 2011;129(6):767–72.
Solouki AM, Verhoeven VJ, van Duijn CM, Verkerk AJ, Ikram MK, Hysi PG, et al. A genome-wide association study identifies a susceptibility locus for refractive errors and myopia at 15q14. Nat Genet. 2010;42(10):897–901.
Hysi I, Wattez H, Benhamed L, Porte H. Primary pulmonary myoepithelial carcinoma. Interact Cardiovasc Thorac Surg. 2011.
Ikram MK, Sim X, Jensen RA, Cotch MF, Hewitt AW, Ikram MA, et al. Four novel Loci (19q13, 6q24, 12q24, and 5q14) influence the microcirculation in vivo. PLoS Genet. 2010;6(10):e1001184.
de Jong FJ, Schrijvers EM, Ikram MK, Koudstaal PJ, de Jong PT, Hofman A, et al. Retinal vascular caliber and risk of dementia: the Rotterdam Study. Neurology. 2011;76(9):816–21.
Wieberdink RG, Ikram MK, Koudstaal PJ, Hofman A, Vingerling JR, Breteler MM. Retinal vascular calibers and the risk of intracerebral hemorrhage and cerebral infarction: the Rotterdam Study. Stroke. 2010;41(12):2757–61.
Ikram MK, Luijendijk HJ, Hofman A, de Jong PT, Breteler MM, Vingerling JR, et al. Retinal vascular calibers and risk of late-life depression: the Rotterdam Study. Am J Geriatr Psychiatry. 2010;18(5):452–5.
Tiemeier H, van Dijck W, Hofman A, Witteman JC, Stijnen T, Breteler MM. Relationship between atherosclerosis and late-life depression: the Rotterdam Study. Arch Gen Psychiatry. 2004;61(4):369–76.
Tiemeier H, van Tuijl HR, Hofman A, Kiliaan AJ, Breteler MM. Plasma fatty acid composition and depression are associated in the elderly: the Rotterdam Study. Am J Clin Nutr. 2003;78(1):40–6.
Dekker MJ, Koper JW, van Aken MO, Pols HA, Hofman A, de Jong FH, et al. Salivary cortisol is related to atherosclerosis of carotid arteries. J Clin Endocrinol Metab. 2008;93(10):3741–7.
Ikram MA, Luijendijk HJ, Vernooij MW, Hofman A, Niessen WJ, van der Lugt A, et al. Vascular brain disease and depression in the elderly. Epidemiology. 2010;21(1):78–81.
Krijthe BP, Walter S, Newson RS, Hofman A, Hunink MG, Tiemeier H. Is positive affect associated with survival? A population-based study of elderly persons. Am J Epidemiol. 2011;173(11):1298–307.
van den Berg JF, Knvistingh Neven A, Tulen JH, Hofman A, Witteman JC, Miedema HM, et al. Actigraphic sleep duration and fragmentation are related to obesity in the elderly: the Rotterdam Study. Int J Obes (Lond). 2008;32(7):1083–90.
Luijendijk HJ, van den Berg JF, Dekker MJ, van Tuijl HR, Otte W, Smit F, et al. Incidence and recurrence of late-life depression. Arch Gen Psychiatry. 2008;65(12):1394–401.
Wing JK, Babor T, Brugha T, Burke J, Cooper JE, Giel R, et al. SCAN: schedules for clinical assessment in neuropsychiatry. Arch Gen Psychiatry. 1990;47(6):589–93.
Wittchen HU, Lachner G, Wunderlich U, Pfister H. Test–retest reliability of the computerized DSM-IV version of the Munich-Composite International Diagnostic Interview (M-CIDI). Soc Psychiatry Psychiatr Epidemiol. 1998;33(11):568–78.
van den Berg JF, Luijendijk HJ, Tulen JH, Hofman A, Neven AK, Tiemeier H. Sleep in depression and anxiety disorders: a population-based study of elderly persons. J Clin Psychiatry. 2009;70(8):1105–13.
Van Den Berg JF, Van Rooij FJ, Vos H, Tulen JH, Hofman A, Miedema HM, et al. Disagreement between subjective and actigraphic measures of sleep duration in a population-based study of elderly persons. J Sleep Res. 2008;17(3):295–302.
Prigerson HG, Maciejewski PK, Reynolds CF 3rd, Bierhals AJ, Newsom JT, Fasiczka A, et al. Inventory of complicated grief: a scale to measure maladaptive symptoms of loss. Psychiatry Res. 1995;59(1–2):65–79.
Naarding P, Tiemeier H, Breteler MM, Schoevers RA, Jonker C, Koudstaal PJ, et al. Clinically defined vascular depression in the general population. Psychol Med. 2007;37(3):383–92.
Newson RS, Hek K, Luijendijk HJ, Hofman A, Witteman JC, Tiemeier H. Atherosclerosis and incident depression in late life. Arch Gen Psychiatry. 2010;67(11):1144–51.
van den Berg JF, Miedema HM, Tulen JH, Neven AK, Hofman A, Witteman JC, et al. Long sleep duration is associated with serum cholesterol in the elderly: the Rotterdam Study. Psychosom Med. 2008;70(9):1005–11.
van den Berg JF, Miedema HM, Tulen JH, Hofman A, Neven AK, Tiemeier H. Sex differences in subjective and actigraphic sleep measures: a population-based study of elderly persons. Sleep. 2009;32(10):1367–75.
Hek K. Anxiety disorders and comorbid depression in community dwelling older adults. Int J Methods Psychiatr Res. (Accepted).
Tobacco, genetics C. Genome-wide meta-analyses identify multiple loci associated with smoking behavior. Nat Genet. 2010;42(5):441–7.
Omidvar M, Stolk L, Uitterlinden AG, Hofman A, Van Duijn CM, Tiemeier H. The effect of catechol-O-methyltransferase Met/Val functional polymorphism on smoking cessation: retrospective and prospective analyses in a cohort study. Pharmacogenet Genomics. 2009;19(1):45–51.
Newson RS, Boelen PA, Hek K, Hofman A, Tiemeier H. The prevalence and characteristics of complicated grief in older adults. J Affect Disord. 2011;132(1–2):231–8.
Velders FP, Kuningas M, Kumari M, Dekker MJ, Uitterlinden AG, Kirschbaum C, et al. Genetics of cortisol secretion and depressive symptoms: a candidate gene and genome wide association approach. Psychoneuroendocrinology. 2011.
Huisman M, Araya R, Lawlor DA, Ormel J, Verhulst FC, Oldehinkel AJ. Cognitive ability, parental socioeconomic position and internalising and externalising problems in adolescence: findings from two European cohort studies. Eur J Epidemiol. 2010;25(8):569–80.
Oksuzyan A, Crimmins E, Saito Y, O’Rand A, Vaupel JW, Christensen K. Cross-national comparison of sex differences in health and mortality in Denmark, Japan and the US. Eur J Epidemiol. 2010;25(7):471–80.
Lehto SM, Ruusunen A, Niskanen L, Tolmunen T, Voutilainen S, Viinamaki H, et al. Elevated depressive symptoms and compositional changes in LDL particles in middle-aged men. Eur J Epidemiol. 2010;25(6):403–9.
Horn O, Sloggett A, Ploubidis GB, Hull L, Hotopf M, Wessely S, et al. Upward trends in symptom reporting in the UK Armed Forces. Eur J Epidemiol. 2010;25(2):87–94.
Thomas S, Heinrich S, von Kries R, Radon K. Exposure to radio-frequency electromagnetic fields and behavioural problems in Bavarian children and adolescents. Eur J Epidemiol. 2010;25(2):135–41.
Rask CU, Olsen EM, Elberling H, Christensen MF, Ornbol E, Fink P, et al. Functional somatic symptoms and associated impairment in 5–7-year-old children: the Copenhagen Child Cohort 2000. Eur J Epidemiol. 2009;24(10):625–34.
Aarts S, van den Akker M, van Boxtel MPJ, Jolles J, Winkens B, Metsemakers JFM. Diabetes mellitus type II as a risk factor for depression: a lower than expected risk in a general practice setting. Eur J Epidemiol. 2009;24(10):641–8.
McFadden E, Luben R, Khaw KT. Different measures of social class in women and mortality. Eur J Epidemiol. 2009;24(5):231–6.
Turcinov D, Stanley C, Rutherford GW, Novotny TE, Begovac J. Adherence to the Mediterranean diet is associated with a lower risk of body-shape changes in Croatian patients treated with combination antiretroviral therapy. Eur J Epidemiol. 2009;24(5):267–74.
van Durme YM, Verhamme KM, Stijnen T, van Rooij FJ, Van Pottelberge GR, Hofman A, et al. Prevalence, incidence, and lifetime risk for the development of COPD in the elderly: the Rotterdam Study. Chest. 2009;135(2):368–77.
Lopez AD, Mathers CD, Ezzati M, Jamison DT, Murray CJ. Global and regional burden of disease and risk factors, 2001: systematic analysis of population health data. Lancet. 2006;367(9524):1747–57.
van Durme YM, Verhamme KM, Aarnoudse AJ, Van Pottelberge GR, Hofman A, Witteman JC, et al. C-reactive protein levels, haplotypes, and the risk of incident chronic obstructive pulmonary disease. Am J Respir Crit Care Med. 2009;179(5):375–82.
Hancock DB, Eijgelsheim M, Wilk JB, Gharib SA, Loehr LR, Marciante KD, et al. Meta-analyses of genome-wide association studies identify multiple loci associated with pulmonary function. Nat Genet. 2010;42(1):45–52.
Van Durme YM, Eijgelsheim M, Joos GF, Hofman A, Uitterlinden AG, Brusselle GG, et al. Hedgehog-interacting protein is a COPD susceptibility gene: the Rotterdam Study. Eur Respir J. 2010;36(1):89–95.
Macintyre N, Crapo RO, Viegi G, Johnson DC, van der Grinten CP, Brusasco V, et al. Standardisation of the single-breath determination of carbon monoxide uptake in the lung. Eur Respir J. 2005;26(4):720–35.
Lawlor DA, Cooper AR, Bain C, Davey Smith G, Irwin A, Riddoch C, et al. Associations of birth size and duration of breast feeding with cardiorespiratory fitness in childhood: findings from the Avon Longitudinal Study of Parents and Children (ALSPAC). Eur J Epidemiol. 2008;23(6):411–22.
Kompauer I, Demmelmair H, Koletzko B, Bolte G, Linseisen J, Heinrich J. Association of fatty acids in serum phospholipids with lung function and bronchial hyperresponsiveness in adults. Eur J Epidemiol. 2008;23(3):175–90.
de Luise C, Brimacombe M, Pedersen L, Sorensen HT. Chronic obstructive pulmonary disease and mortality following hip fracture: a population-based cohort study. Eur J Epidemiol. 2008;23(2):115–22.
Hugg T, Ruotsalainen R, Jaakkola MS, Pushkarev V, Jaakkola JJ. Comparison of allergic diseases, symptoms and respiratory infections between Finnish and Russian school children. Eur J Epidemiol. 2008;23(2):123–33.
Rzehak P, Schoefer Y, Wichmann HE, Heinrich J. A prospective study on the association between hay fever among children and incidence of asthma in East Germany. Eur J Epidemiol. 2008;23(1):17–22.
Svartberg J, Schirmer H, Medbo A, Melbye H, Aasebo U. Reduced pulmonary function is associated with lower levels of endogenous total and free testosterone. The Tromso study. Eur J Epidemiol. 2007;22(2):107–12.
Moreno T, Querol X, Alastuey A, Ballester F, Gibbons W. Airborne particulate matter and premature deaths in urban Europe: the new WHO guidelines and the challenge ahead as illustrated by Spain. Eur J Epidemiol. 2007;22(1):1–5.
Lacourt A, Rolland P, Gramond C, Astoul P, Chamming’s S, Ducamp S, et al. Attributable risk in men in two French case–control studies on mesothelioma and asbestos. Eur J Epidemiol. 2010;25(11):799–806.
Neovius K, Rasmussen F, Sundstrom J, Neovius M. Forecast of future premature mortality as a result of trends in obesity and smoking: nationwide cohort simulation study. Eur J Epidemiol. 2010;25(10):703–9.
Hertel S, Viehmann A, Moebus S, Mann K, Brocker-Preuss M, Mohlenkamp S, et al. Influence of short-term exposure to ultrafine and fine particles on systemic inflammation. Eur J Epidemiol. 2010;25(8):581–92.
Schneider C, Bothner U, Jick SS, Meier CR. Chronic obstructive pulmonary disease and the risk of cardiovascular diseases. Eur J Epidemiol. 2010;25(4):253–60.
McFadden E, Luben R, Wareham N, Bingham S, Khaw KT. How far can we explain the social class differential in respiratory function? A cross-sectional population study of 21,991 men and women from EPIC-Norfolk. Eur J Epidemiol. 2009;24(4):193–201.
Behrens T. Current trends in aetiological asthma research. Eur J Epidemiol. 2009;24(3):115–8.
Vaux S, Poujol I, Bonmarin I, Levy-Bruhl D, Desenclos JC. Surveillance of lower respiratory tract infections outbreaks in nursing homes in France. Eur J Epidemiol. 2009;24(3):149–55.
Vaessen N, Janssen JA, Heutink P, Hofman A, Lamberts SW, Oostra BA, et al. Association between genetic variation in the gene for insulin-like growth factor-I and low birthweight. Lancet. 2002;359(9311):1036–7.
van Meurs JB, Schuit SC, Weel AE, van der Klift M, Bergink AP, Arp PP, et al. Association of 5′ estrogen receptor alpha gene polymorphisms with bone mineral density, vertebral bone area and fracture risk. Hum Mol Genet. 2003;12(14):1745–54.
Schuit SC, Oei HH, Witteman JC, Geurts van Kessel CH, van Meurs JB, Nijhuis RL, et al. Estrogen receptor alpha gene polymorphisms and risk of myocardial infarction. JAMA. 2004;291(24):2969–77.
Ioannidis JP, Gwinn M, Little J, Higgins JP, Bernstein JL, Boffetta P, et al. A road map for efficient and reliable human genome epidemiology. Nat Genet. 2006;38(1):3–5.
Ioannidis JP, Ralston SH, Bennett ST, Brandi ML, Grinberg D, Karassa FB, et al. Differential genetic effects of ESR1 gene polymorphisms on osteoporosis outcomes. JAMA. 2004;292(17):2105–14.
Uitterlinden AG, Ralston SH, Brandi ML, Carey AH, Grinberg D, Langdahl BL, et al. The association between common vitamin D receptor gene variations and osteoporosis: a participant-level meta-analysis. Ann Intern Med. 2006;145(4):255–64.
Despriet DD, Klaver CC, Witteman JC, Bergen AA, Kardys I, de Maat MP, et al. Complement factor H polymorphism, complement activators, and risk of age-related macular degeneration. JAMA. 2006;296(3):301–9.
Aarnoudse AJ, Newton-Cheh C, de Bakker PI, Straus SM, Kors JA, Hofman A, et al. Common NOS1AP variants are associated with a prolonged QTc interval in the Rotterdam Study. Circulation. 2007;116(1):10–6.
Fang Y, van Meurs JB, d’Alesio A, Jhamai M, Zhao H, Rivadeneira F, et al. Promoter and 3′-untranslated-region haplotypes in the vitamin D receptor gene predispose to osteoporotic fracture: the Rotterdam Study. Am J Hum Genet. 2005;77(5):807–23.
Willer CJ, Speliotes EK, Loos RJ, Li S, Lindgren CM, Heid IM, et al. Six new loci associated with body mass index highlight a neuronal influence on body weight regulation. Nat Genet. 2009;41(1):25–34.
Prokopenko I, Langenberg C, Florez JC, Saxena R, Soranzo N, Thorleifsson G, et al. Variants in MTNR1B influence fasting glucose levels. Nat Genet. 2009;41(1):77–81.
Aulchenko YS, Ripatti S, Lindqvist I, Boomsma D, Heid IM, Pramstaller PP, et al. Loci influencing lipid levels and coronary heart disease risk in 16 European population cohorts. Nat Genet. 2009;41(1):47–55.
Aulchenko YS, Ripke S, Isaacs A, van Duijn CM. GenABEL: an R library for genome-wide association analysis. Bioinformatics. 2007;23(10):1294–6.
in’t Veld BA, Ruitenberg A, Hofman A, Stricker BH, Breteler MM. Antihypertensive drugs and incidence of dementia: the Rotterdam Study. Neurobiol Aging. 2001;22(3):407–12.
Luijendijk HJ, van den Berg JF, Hofman A, Tiemeier H, Stricker BH. Beta-blockers and the risk of incident depression in the elderly. J Clin Psychopharmacol. 2011;31(1):45–50.
Feenstra J, Heerdink ER, Grobbee DE, Stricker BH. Association of nonsteroidal anti-inflammatory drugs with first occurrence of heart failure and with relapsing heart failure: the Rotterdam Study. Arch Intern Med. 2002;162(3):265–70.
van der Hooft CS, Heeringa J, Brusselle GG, Hofman A, Witteman JC, Kingma JH, et al. Corticosteroids and the risk of atrial fibrillation. Arch Intern Med. 2006;166(9):1016–20.
van den Hondel KE, Eijgelsheim M, Ruiter R, Witteman JC, Hofman A, Stricker BH. Effect of short-term NSAID use on echocardiographic parameters in elderly people: a population-based cohort study. Heart. 2011;97(7):540–3.
van Noord C, Sturkenboom MC, Straus SM, Witteman JC, Stricker BH. Non-cardiovascular drugs that inhibit hERG-encoded potassium channels and risk of sudden cardiac death. Heart. 2011;97(3):215–20.
Lubitz SA, Sinner MF, Lunetta KL, Makino S, Pfeufer A, Rahman R, et al. Independent susceptibility markers for atrial fibrillation on chromosome 4q25. Circulation. 2010;122(10):976–84.
Ellinor PT, Lunetta KL, Glazer NL, Pfeufer A, Alonso A, Chung MK, et al. Common variants in KCNN3 are associated with lone atrial fibrillation. Nat Genet. 2010;42(3):240–4.
Eijgelsheim M, Newton-Cheh C, Sotoodehnia N, de Bakker PI, Muller M, Morrison AC, et al. Genome-wide association analysis identifies multiple loci related to resting heart rate. Hum Mol Genet. 2010;19(19):3885–94.
Sotoodehnia N, Isaacs A, de Bakker PI, Dorr M, Newton-Cheh C, Nolte IM, et al. Common variants in 22 loci are associated with QRS duration and cardiac ventricular conduction. Nat Genet. 2010;42(12):1068–76.
Schoofs MW, van der Klift M, Hofman A, de Laet CE, Herings RM, Stijnen T, et al. Thiazide diuretics and the risk for hip fracture. Ann Intern Med. 2003;139(6):476–82.
Schoofs MW, Sturkenboom MC, van der Klift M, Hofman A, Pols HA, Stricker BH. HMG-CoA reductase inhibitors and the risk of vertebral fracture. J Bone Miner Res. 2004;19(9):1525–30.
Reijman M, Bierma-Zeinstra SM, Pols HA, Koes BW, Stricker BH, Hazes JM. Is there an association between the use of different types of nonsteroidal antiinflammatory drugs and radiologic progression of osteoarthritis? The Rotterdam Study. Arthritis Rheum. 2005;52(10):3137–42.
van Leeuwen R, Vingerling JR, de Jong PT. Risk of macular degeneration with statin use should be interpreted with caution. BMJ. 2001;323(7324):1308.
van Leeuwen R, Vingerling JR, Hofman A, de Jong PT, Stricker BH. Cholesterol lowering drugs and risk of age related maculopathy: prospective cohort study with cumulative exposure measurement. BMJ. 2003;326(7383):255–6.
Visser LE, Penning-van Beest FJ, Kasbergen AA, De Smet PA, Vulto AG, Hofman A, et al. Overanticoagulation associated with combined use of antifungal agents and coumarin anticoagulants. Clin Pharmacol Ther. 2002;71(6):496–502.
Visser LE, Penning-van Bees FJ, Kasbergen AA, De Smet PA, Vulto AG, Hofman A, et al. Overanticoagulation associated with combined use of antibacterial drugs and acenocoumarol or phenprocoumon anticoagulants. Thromb Haemost. 2002;88(5):705–10.
Visser LE, van Vliet M, van Schaik RH, Kasbergen AA, De Smet PA, Vulto AG, et al. The risk of overanticoagulation in patients with cytochrome P450 CYP2C9*2 or CYP2C9*3 alleles on acenocoumarol or phenprocoumon. Pharmacogenetics. 2004;14(1):27–33.
Visser LE, Penning-van Beest FJ, Wilson JH, Vulto AG, Kasbergen AA, De Smet PA, et al. Overanticoagulation associated with combined use of lactulose and acenocoumarol or phenprocoumon. Br J Clin Pharmacol. 2004;57(4):522–4.
Visser LE, van Schaik RH, van Vliet M, Trienekens PH, De Smet PA, Vulto AG, et al. The risk of bleeding complications in patients with cytochrome P450 CYP2C9*2 or CYP2C9*3 alleles on acenocoumarol or phenprocoumon. Thromb Haemost. 2004;92(1):61–6.
Visser LE, Bleumink GS, Trienekens PH, Vulto AG, Hofman A, Stricker BH. The risk of overanticoagulation in patients with heart failure on coumarin anticoagulants. Br J Haematol. 2004;127(1):85–9.
Visser LE, van Schaik RH, van Vliet M, Trienekens PH, De Smet PA, Vulto AG, et al. Allelic variants of cytochrome P450 2C9 modify the interaction between nonsteroidal anti-inflammatory drugs and coumarin anticoagulants. Clin Pharmacol Ther. 2005;77(6):479–85.
Bleumink GS, Schut AF, Sturkenboom MC, van Duijn CM, Deckers JW, Hofman A, et al. Mortality in patients with hypertension on angiotensin-I converting enzyme (ACE)-inhibitor treatment is influenced by the ACE insertion/deletion polymorphism. Pharmacogenet Genomics. 2005;15(2):75–81.
Visser LE, Trienekens PH, De Smet PA, Vulto AG, Hofman A, van Duijn CM, et al. Patients with an ApoE epsilon4 allele require lower doses of coumarin anticoagulants. Pharmacogenet Genomics. 2005;15(2):69–74.
Schelleman H, Klungel OH, van Duijn CM, Witteman JC, Hofman A, de Boer A, et al. Drug-gene interaction between the insertion/deletion polymorphism of the angiotensin-converting enzyme gene and antihypertensive therapy. Ann Pharmacother. 2006;40(2):212–8.
Becker ML, Visser LE, Trienekens PH, Hofman A, van Schaik RH, Stricker BH. Cytochrome P450 2C9*2 and *3 polymorphisms and the dose and effect of sulfonylurea in type II diabetes mellitus. Clin Pharmacol Ther. 2008;83(2):288–92.
Visser LE, van Schaik RH, Jan Danser AH, Hofman A, Witteman JC, van Duijn CM, et al. The risk of myocardial infarction in patients with reduced activity of cytochrome P450 2C9. Pharmacogenet Genomics. 2007;17(7):473–9.
Schelleman H, Klungel OH, Witteman JC, Hofman A, van Duijn CM, de Boer A, et al. Pharmacogenetic interactions of three candidate gene polymorphisms with ACE-inhibitors or beta-blockers and the risk of atherosclerosis. Br J Clin Pharmacol. 2007;64(1):57–66.
Schelleman H, Klungel OH, Witteman JC, Breteler MM, Yazdanpanah M, Danser AH, et al. Angiotensinogen M235T polymorphism and the risk of myocardial infarction and stroke among hypertensive patients on ACE-inhibitors or beta-blockers. Eur J Hum Genet. 2007;15(4):478–84.
Schelleman H, Klungel OH, Witteman JC, Breteler MM, Hofman A, van Duijn CM, et al. Diuretic-gene interaction and the risk of myocardial infarction and stroke. Pharmacogenomics J. 2007;7(5):346–52.
Aarnoudse AJ, Dieleman JP, Visser LE, Arp PP, van der Heiden IP, van Schaik RH, et al. Common ATP-binding cassette B1 variants are associated with increased digoxin serum concentration. Pharmacogenet Genomics. 2008;18(4):299–305.
Teichert M, Visser LE, van Schaik RH, Hofman A, Uitterlinden AG, De Smet PA, et al. Vitamin K epoxide reductase complex subunit 1 (VKORC1) polymorphism and aortic calcification: the Rotterdam Study. Arterioscler Thromb Vasc Biol. 2008;28(4):771–6.
Bijl MJ, Visser LE, Hofman A, Vulto AG, van Gelder T, Stricker BH, et al. Influence of the CYP2D6*4 polymorphism on dose, switching and discontinuation of antidepressants. Br J Clin Pharmacol. 2008;65(4):558–64.
Becker ML, Visser LE, Newton-Cheh C, Witteman JC, Hofman A, Uitterlinden AG, et al. Genetic variation in the NOS1AP gene is associated with the incidence of diabetes mellitus in users of calcium channel blockers. Diabetologia. 2008;51(11):2138–40.
Becker ML, Aarnoudse AJ, Newton-Cheh C, Hofman A, Witteman JC, Uitterlinden AG, et al. Common variation in the NOS1AP gene is associated with reduced glucose-lowering effect and with increased mortality in users of sulfonylurea. Pharmacogenet Genomics. 2008;18(7):591–7.
Bijl MJ, Visser LE, van Schaik RH, Kors JA, Witteman JC, Hofman A, et al. Genetic variation in the CYP2D6 gene is associated with a lower heart rate and blood pressure in beta-blocker users. Clin Pharmacol Ther. 2009;85(1):45–50.
Becker ML, Visser LE, van Schaik RH, Hofman A, Uitterlinden AG, Stricker BH. Interaction between polymorphisms in the OCT1 and MATE1 transporter and metformin response. Pharmacogenet Genomics. 2010;20(1):38–44.
Becker ML, Visser LE, van Schaik RH, Hofman A, Uitterlinden AG, Stricker BH. OCT1 polymorphism is associated with response and survival time in anti-Parkinsonian drug users. Neurogenetics. 2011;12(1):79–82.
Teichert M, Eijgelsheim M, Uitterlinden AG, Buhre PN, Hofman A, De Smet PA, et al. Dependency of phenprocoumon dosage on polymorphisms in the VKORC1, CYP2C9, and CYP4F2 genes. Pharmacogenet Genomics. 2011;21(1):26–34.
Ruiter R, Visser LE, Eijgelsheim M, Rodenburg EM, Hofman A, Coebergh JW, et al. High-ceiling diuretics are associated with an increased risk of basal cell carcinoma in a population-based follow-up study. Eur J Cancer. 2010;46(13):2467–72.
Siemes C, Visser LE, de Jong FH, Coebergh JW, Uitterlinden AG, Hofman A, et al. Cytochrome P450 3A gene variation, steroid hormone serum levels and prostate cancer—the Rotterdam Study. Steroids. 2010;75(12):1024–32.
Ruiter R, Bijl MJ, van Schaik RH, Berns EM, Hofman A, Coebergh JW, et al. CYP2C19*2 polymorphism is associated with increased survival in breast cancer patients using tamoxifen. Pharmacogenomics. 2010;11(10):1367–75.
Stricker BH, Stijnen T. Analysis of individual drug use as a time-varying determinant of exposure in prospective population-based cohort studies. Eur J Epidemiol. 2010;25(4):245–51.
Davis S, Mirick DK. Medication use and the risk of breast cancer. Eur J Epidemiol. 2007;22(5):319–25.
de Luise C, Lanes SF, Jacobsen J, Pedersen L, Sorensen HT. Cardiovascular and respiratory hospitalizations and mortality among users of tiotropium in Denmark. Eur J Epidemiol. 2007;22(4):267–72.
Gouya G, Reichardt B, Ohrenberger G, Wolzt M. Survival of patients discharged after acute myocardial infarction and evidence-based drug therapy. Eur J Epidemiol. 2007;22(3):145–9.
Osterbrand M, Fahlen M, Oden A, Eliasson B. A method to predict the metabolic effects of changes in insulin treatment in subgroups of a large population based patient cohort. Eur J Epidemiol. 2007;22(3):151–7.
Bonovas S, Nikolopoulos G, Filioussi K, Peponi E, Bagos P, Sitaras NM. Can statin therapy reduce the risk of melanoma? A meta-analysis of randomized controlled trials. Eur J Epidemiol. 2010;25(1):29–35.
Ngo AD, Taylor R, Roberts CL. Paternal exposure to Agent Orange and spina bifida: a meta-analysis. Eur J Epidemiol. 2010;25(1):37–44.
Hsia YF, Maclennan K. Rise in psychotropic drug prescribing in children and adolescents during 1992–2001: a population-based study in the UK. Eur J Epidemiol. 2009;24(4):211–6.
Ikram MA, Vrooman HA, Vernooij MW, den Heijer T, Hofman A, Niessen WJ, et al. Brain tissue volumes in relation to cognitive function and risk of dementia. Neurobiol Aging. 2010;31(3):378–86.
Vrooman HA, Cocosco CA, van der Lijn F, Stokking R, Ikram MA, Vernooij MW, et al. Multi-spectral brain tissue segmentation using automatically trained k-nearest-neighbor classification. Neuroimage. 2007;37(1):71–81.
van der Lijn F, den Heijer T, Breteler MM, Niessen WJ. Hippocampus segmentation in MR images using atlas registration, voxel classification, and graph cuts. Neuroimage. 2008;43(4):708–20.
Ikram MA, Vrooman HA, Vernooij MW, van der Lijn F, Hofman A, van der Lugt A, et al. Brain tissue volumes in the general elderly population. The Rotterdam Scan Study. Neurobiol Aging. 2008;29(6):882–90.
den Heijer T, van der Lijn F, Koudstaal PJ, Hofman A, van der Lugt A, Krestin GP, et al. A 10-year follow-up of hippocampal volume on magnetic resonance imaging in early dementia and cognitive decline. Brain. 2010;133(Pt 4):1163–72.
Vernooij MW, van der Lugt A, Ikram MA, Wielopolski PA, Vrooman HA, Hofman A, et al. Total cerebral blood flow and total brain perfusion in the general population: the Rotterdam Scan Study. J Cereb Blood Flow Metab. 2008;28(2):412–9.
Poels MM, Ikram MA, Vernooij MW, Krestin GP, Hofman A, Niessen WJ, et al. Total cerebral blood flow in relation to cognitive function: the Rotterdam Scan Study. J Cereb Blood Flow Metab. 2008;28(10):1652–5.
Vernooij MW, Ikram MA, Wielopolski PA, Krestin GP, Breteler MM, van der Lugt A. Cerebral microbleeds: accelerated 3D T2*-weighted GRE MR imaging versus conventional 2D T2*-weighted GRE MR imaging for detection. Radiology. 2008;248(1):272–7.
Poels MM, Vernooij MW, Ikram MA, Hofman A, Krestin GP, van der Lugt A, et al. Prevalence and risk factors of cerebral microbleeds: an update of the Rotterdam Scan Study. Stroke. 2010;41(10 Suppl):S103–6.
Vernooij MW, van der Lugt A, Ikram MA, Wielopolski PA, Niessen WJ, Hofman A, et al. Prevalence and risk factors of cerebral microbleeds: the Rotterdam Scan Study. Neurology. 2008;70(14):1208–14.
Poels MM, Ikram MA, van der Lugt A, Hofman A, Krestin GP, Breteler MM, et al. Incidence of cerebral microbleeds in the general population: the Rotterdam Scan Study. Stroke. 2011;42(3):656–61.
Vernooij MW, Haag MD, van der Lugt A, Hofman A, Krestin GP, Stricker BH, et al. Use of antithrombotic drugs and the presence of cerebral microbleeds: the Rotterdam Scan Study. Arch Neurol. 2009;66(6):714–20.
Lovelock CE, Cordonnier C, Naka H, Al-Shahi Salman R, Sudlow CL, Edinburgh Stroke Study G, et al. Antithrombotic drug use, cerebral microbleeds, and intracerebral hemorrhage: a systematic review of published and unpublished studies. Stroke. 2010;41(6):1222–8.
Vernooij MW, de Groot M, van der Lugt A, Ikram MA, Krestin GP, Hofman A, et al. White matter atrophy and lesion formation explain the loss of structural integrity of white matter in aging. Neuroimage. 2008;43(3):470–7.
de Boer R, Schaap M, van der Lijn F, Vrooman HA, de Groot M, van der Lugt A, et al. Statistical analysis of minimum cost path based structural brain connectivity. Neuroimage. 2011;55(2):557–65.
Agatston AS, Janowitz WR, Hildner FJ, Zusmer NR, Viamonte M Jr, Detrano R. Quantification of coronary artery calcium using ultrafast computed tomography. J Am Coll Cardiol. 1990;15(4):827–32.
Odink AE, van der Lugt A, Hofman A, Hunink MG, Breteler MM, Krestin GP, et al. Association between calcification in the coronary arteries, aortic arch and carotid arteries: the Rotterdam Study. Atherosclerosis. 2007;193(2):408–13.
Odink AE, van der Lugt A, Hofman A, Hunink MG, Breteler MM, Krestin GP, et al. Risk factors for coronary, aortic arch and carotid calcification: the Rotterdam Study. J Hum Hypertens. 2010;24(2):86–92.
Elias-Smale SE, Odink AE, Wieberdink RG, Hofman A, Hunink MG, Krestin GP, et al. Carotid, aortic arch and coronary calcification are related to history of stroke: the Rotterdam Study. Atherosclerosis. 2010;212(2):656–60.
Takaya N, Yuan C, Chu B, Saam T, Underhill H, Cai J, et al. Association between carotid plaque characteristics and subsequent ischemic cerebrovascular events: a prospective assessment with MRI—initial results. Stroke. 2006;37(3):818–23.
Yuan C, Mitsumori LM, Ferguson MS, Polissar NL, Echelard D, Ortiz G, et al. In vivo accuracy of multispectral magnetic resonance imaging for identifying lipid-rich necrotic cores and intraplaque hemorrhage in advanced human carotid plaques. Circulation. 2001;104(17):2051–6.
North American Symptomatic Carotid Endarterectomy Trial. Methods, patient characteristics, and progress. Stroke. 1991;22(6):711–20.
Hofman A. New studies, technology, and the progress of epidemiology. Eur J Epidemiol. 2010;25(12):851–4.
Gondrie MJA, Mali W, Buckens CFM, Jacobs PCA, Grobbee DE, van der Graaf Y. The PROgnostic Value of unrequested Information in Diagnostic Imaging (PROVIDI) study: rationale and design. Eur J Epidemiol. 2010;25(10):751–8.
Kardys I, Deckers JW, Stricker BHC, Vletter WB, Hofman A, Witteman J. Distribution of echocardiographic parameters and their associations with cardiovascular risk factors in the Rotterdam Study. Eur J Epidemiol. 2010;25(7):481–90.
Delaney JAC, Scherzer R, Polak J, Biggs ML, Kronmal R, Chen HY, et al. Effect of inter-reader variability on outcomes in studies using carotid intima media thickness quantified by carotid ultrasonography. Eur J Epidemiol. 2010;25(6):385–92.
Holzhauer S, Zwijsen RML, Jaddoe VWV, Boehm G, Moll HA, Mulder PG, et al. Sonographic assessment of abdominal fat distribution in infancy. Eur J Epidemiol. 2009;24(9):521–9.
Acknowledgments
The Rotterdam Study is supported by the Erasmus Medical Center and Erasmus University Rotterdam, The Netherlands Organization for Scientific Research (NWO), The Netherlands Organization for Health Research and Development (ZonMw), the Research Institute for Diseases in the Elderly (RIDE), The Netherlands Genomics Initiative, the Ministry of Education, Culture and Science, the Ministry of Health, Welfare and Sports, the European Commission (DG XII), and the Municipality of Rotterdam. The contribution of inhabitants, general practitioners and pharmacists of the Ommoord district to the Rotterdam Study is gratefully acknowledged.
Open Access
This article is distributed under the terms of the Creative Commons Attribution Noncommercial License which permits any noncommercial use, distribution, and reproduction in any medium, provided the original author(s) and source are credited.
Author information
Authors and Affiliations
Corresponding author
Rights and permissions
Open Access This is an open access article distributed under the terms of the Creative Commons Attribution Noncommercial License (https://creativecommons.org/licenses/by-nc/2.0), which permits any noncommercial use, distribution, and reproduction in any medium, provided the original author(s) and source are credited.
About this article
Cite this article
Hofman, A., van Duijn, C.M., Franco, O.H. et al. The Rotterdam Study: 2012 objectives and design update. Eur J Epidemiol 26, 657–686 (2011). https://doi.org/10.1007/s10654-011-9610-5
Received:
Accepted:
Published:
Issue Date:
DOI: https://doi.org/10.1007/s10654-011-9610-5