Abstract
Summary
Key statements of the Russian clinical guidelines on the diagnosis and treatment of osteoporosis are summarized. They were developed by a task force representing the key Russian professional associations involved in the management of osteoporosis and approved by the Russian Ministry of Health.
Purpose
To summarize key statements of the Russian clinical practice guidelines for the diagnosis and treatment of osteoporosis.
Methods
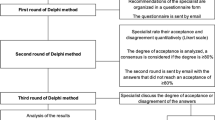
The Russian clinical guidelines on the diagnosis and treatment of osteoporosis were developed by a task force representing the key Russian professional associations involved in the management of osteoporosis: These comprised the Russian Association of Endocrinologists, the Russian Association for Osteoporosis, the Association of Rheumatologists of Russia, the Association of Orthopedic surgeons and Traumatologists of Russia, the Russian Association of Gynecologists-Endocrinologists, and the Russian Association of Gerontologists and Geriatrics. The guidelines are based on a systematic literature review and principles of evidence-based medicine and were compiled in accordance with the requirements for clinical recommendations developed by the Ministry of Health of the Russian Federation.
Results
Key statements included in the Russian guidelines of osteoporosis approved by the Russian Ministry of Health in 2021 are summarized. The statements are graded based on levels of evidence and supported by short comments. The guidelines are focused on the current approach to screening, diagnosis, differential diagnosis, and treatment of osteoporosis.
Conclusion
These guidelines are a practical tool for general practitioners, as well as medical specialists, primarily endocrinologists, rheumatologists, orthopedic surgeons, and other physicians who are involved in the management of patients with osteoporosis.

Similar content being viewed by others
References
Kanis JA, on behalf of the World Health Organization Scientific Group (2008) Assessment of osteoporosis at the primary healthcare level. Technical report. WHO Collaborating Centre, University of Sheffield, UK. Available at http://www.shef.ac.uk/FRAX/index.htm
Assessment of fracture risk and its application to screening for postmenopausal osteoporosis. Report of a WHO Study Group (1994) World Health Organ Tech Rep Ser 843:1–129
Mikhailov EE, Benevolenskaya LI (2003) Epidemiology of osteoporosis and fractures. In: Primary on Osteoporosis. BINOM. laboratoriya znanii, Moscow, рр 10–55 (in Russian)
Lesnyak OM (2011) AUDIT SOSTOYaNIYa PROBLEMY OSTEOPOROZA V STRANAKh VOSTOChNOY EVROPY I TsENTRAL'NOY AZII 2010. Osteo Bone Dis 14(2):3–6. (In Russ.) https://doi.org/10.14341/osteo201123-6
Ershova OB, Sinitsyna OS, Belova KY, Degtyarev AA, Ganert OA, Romanova MA, Nazarova AV (2013) Results of the analysis of risk factors and absolute risk of fracture (FRAX) in men with fractures of the proximal femur. Osteo Bone Dis 16(1):3–6. (In Russ.) https://doi.org/10.14341/osteo201313-6
Gladkova EN, Khodyrev VN, Lesnyak OM, Gladkova EN, Chodyrev VN, Lesnyak OM (2011) Analysis of epidemiology of osteoporotic fracturesusing data from primary care physicians. Osteo Bone Dis 14(1):14–18. (In Russ.) https://doi.org/10.14341/osteo2011114-18
Lesnyak OM, Baranova IA, Belova KY et al (2018) Osteoporosis in russian federation: epidemiology, socio-medical and economical aspects (review) // Traumatol Ortho Russ 24(1):155–168. https://doi.org/10.21823/2311-2905-2018-24-1-155-168, https://doi.org/10.21823/2311-2905-2018-24-1-155-168
Dedov II, Mel'nichenko GA, Belaia ZE, Rozhinskaia LI (2011) Osteoporosis: from a rare symptom of endocrine diseases to the tacit epidemic of XX-XXI centuries. Prob Endocrinol 57(1):35–45. https://doi.org/10.14341/probl201157135-45
Остеопороз. Диагностика, профилактика и лечение / Л. П. Евстигнеева, А. Г. Солодовников, О. Б. Ершова [и др.]. – Второе издание, переработанное и дополненное.. – Москва : Общество с ограниченной ответственностью Издательская группа "ГЭОТАР-Медиа", 2010. – 272 с. – (Клинические рекомендации). – ISBN 978-5-9704-1453-8. – EDN TIAYPN.
Mel’nichenko GA, Belaya ZE, Rozhinskaya LY, Toroptsova NV, Alekseeva LI, Biryukova EV, Grebennikova TA, Dzeranova LK, Dreval’ AV, Zagorodniy NV, Ilyin AV, Kryukova IV, Lesnyak OM, Mamedova EO, Nikitinskaya OA, Pigarova EA, Rodionova SS, Skripnikova IA, Tarbaeva NV, LYa Farba, Tsoriev TT, Chernova TO, Yureneva SV, Yakushevskaya OV, Dedov II (2017) Russian Federal clinical guidelines on diagnostics, treatment and prophylaxis of osteoporosis. Probl Endokrinol (Mosk) 63(6):392–426. https://doi.org/10.14341/probl2017636392-426
Belaya ZhE, Belova KYu, Biryukova EV, Dedov II, Dzeranova LK, Drapkina OM, Dreval AV, Dubovitskaya TA, Dudinskaya EN, Ershova OB, Zagorodniy NV, Ilyukhina OB, Kanis JA, Kryukova IV, Lesnyak OM, Mamedova EO, Marchenkova LA, Melnichenko GA, Nikankina LV, Nikitinskaya OA, Petryaikin AV, Pigarova EA, Rodionova SS, Lya R, Skripnikova IA, Tarbaeva NV, Tkacheva ON, Toroptsova NV, Farba LYA, Tsoriev TT, Chernova TO, Yureneva SV, Yakushevskaya OV (2021) Federal clinical guidelines for diagnosis, treatment and prevention of osteoporosis. Osteopor Bone Dis 24(2):4–47. https://doi.org/10.14341/osteo12930
Kanis JA, Cooper C, Rizzoli R, Reginster J-Y, Scientific Advisory Board of the European Society for Clinical and Economic Aspects of Osteoporosis (ESCEO) and the Committees of Scientific Advisors and National Societies of the International Osteoporosis Foundation (IOF) (2019) European guidance for the diagnosis and management of osteoporosis in postmenopausal women. Osteoporos Int 30(1):3–44. https://doi.org/10.1007/s00198-018-4704-5
Lesnyak O, Ershova O, Belova K, Gladkova E, Sinitsina O, Ganert O, Romanova M, Khodirev V, Johansson H, McCloskey E, Kanis JA (2012) Epidemiology of fracture in the Russian Federation and the development of a FRAX model. Arch Osteoporos 7(1–2):67–73. https://doi.org/10.1007/s11657-012-0082-3
Shepstone L, Lenaghan E, Cooper C, Clarke S, Fong-Soe-Khioe R, Fordham R, Gittoes N, Harvey I, Harvey N, Heawood A, Holland R, Howe A, Kanis J, Marshall T, O’Neill T, Peters T, Redmond N, Torgerson D, Turner D, McCloskey E (2018) Screening in the community to reduce fractures in older women (SCOOP): a randomised controlled trial. The Lancet 391(10122):741–777. https://doi.org/10.1016/S0140-6736(17)32640-5
Marques A, Ferreira RJO, Santos E, Loza E, Carmona L, da Silva JAP (2015) The accuracy of osteoporotic fracture risk prediction tools: a systematic review and meta-analysis. Ann Rheum Dis 74(11):1958–1967. https://doi.org/10.1136/annrheumdis-2015-207907
Turner DA, Khioe RFS, Shepstone L, Lenaghan E, Cooper C, Gittoes N, Harvey NC, Holland R, Howe A, McCloskey E, O’Neill TW, Torgerson D, Fordham R (2018) The cost-effectiveness of screening in the community to reduce osteoporotic fractures in older women in the UK: economic evaluation of the SCOOP study: cost-effectiveness of community screening for fracture risk. J Bone Miner Res 33(5):845–851. https://doi.org/10.1002/jbmr.3381
Hippisley-Cox J, Coupland C (2009) Predicting risk of osteoporotic fracture in men and women in England and Wales: prospective derivation and validation of QFractureScores. BMJ 339:4229–4229. https://doi.org/10.1136/bmj.b4229
Hoff M, Meyer HE, Skurtveit S, Langhammer A, Søgaard AJ, Syversen U, Dhainaut A, Skovlund E, Abrahamsen B, Schei B (2017) Validation of FRAX and the impact of self-reported falls among elderly in a general population: the HUNT study. Norway Osteoporos Int 28(10):2935–2944. https://doi.org/10.1007/s00198-017-4134-9
Fraser LA, Langsetmo L, Berger C, Ioannidis G, Goltzman D, Adachi JD, Papaioannou A, Josse R, Kovacs CS, Olszynski WP, Towheed T, Hanley DA, Kaiser SM, Prior J, Jamal S, Kreiger N, Brown JP, Johansson H, Oden A, McCloskey E, Kanis JA, Leslie WD (2011) Fracture prediction and calibration of a Canadian FRAX® tool: a population-based report from CaMos. Osteoporos Int 22(3):829–837. https://doi.org/10.1007/s00198-010-1465-1
Leslie WD, Lix LM, Johansson H, Oden A, McCloskey E, Kanis JA (2010) Independent clinical validation of a Canadian FRAX tool: fracture prediction and model calibration: validation of Canadian FRAX tool. J Bone Miner Res 25(11):2350–2358. https://doi.org/10.1002/jbmr.123
Jiang X, Gruner M, Trémollieres F, Pluskiewicz W, Sornay-Rendu E, Adamczyk P, Schnatz PF (2017) Diagnostic accuracy of FRAX in predicting the 10-year risk of osteoporotic fractures using the USA treatment thresholds: a systematic review and meta-analysis. Bone 99:20–25. https://doi.org/10.1016/j.bone.2017.02.008
Kanis JA, Johnell O, Oden A, Johansson H, McCloskey E (2008) FRAX™ and the assessment of fracture probability in men and women from the UK. Osteoporos Int 19(4):385–397. https://doi.org/10.1007/s00198-007-0543-5
Ferrari SL, Abrahamsen B, Napoli N, Akesson K, Chandran M, Eastell R, El-Hajj Fuleihan G, Josse R, Kendler DL, Kraenzlin M, Suzuki A, Pierroz DD, Schwartz AV, Leslie WD, Bone and Diabetes Working Group of IOF (2018) Diagnosis and management of bone fragility in diabetes: an emerging challenge. Osteoporos Int 29(12):2585–2596. https://doi.org/10.1007/s00198-018-4650-2
Leslie WD, Johansson H, McCloskey EV, Harvey NC, Kanis JA, Hans D (2018) Comparison of methods for improving fracture risk assessment in diabetes: the Manitoba BMD registry. J Bone Miner Res 33(11):1923–1930. https://doi.org/10.1002/jbmr.3538
Baleanu F, Bergmann P, Hambye AS, Dekelver C, Iconaru L, Cappelle SI, Moreau M, Paesmans M, Karmali R (2019) Body J (2019) Assessment of bone quality with trabecular bone score in type 2 diabetes mellitus: a study from the FRISBEE cohort. Int J Clin Pract 73(5):e13347. https://doi.org/10.1111/ijcp.13347
Kanis JA, Johansson H, Oden A, McCloskey EV (2011) Guidance for the adjustment of FRAX according to the dose of glucocorticoids. Osteoporos Int 22(3):809–816. https://doi.org/10.1007/s00198-010-1524-7
Kanis JA, Johansson H, Oden A, Johnell O, de Laet C, Melton LJ III, Tenenhouse A, Reeve J, Silman AJ, Pols HA, Eisman JA, McCloskey EV, Mellstrom D (2004) A meta-analysis of prior corticosteroid use and fracture risk. J Bone Miner Res 19(6):893–899. https://doi.org/10.1359/JBMR.040134
van Staa TP, Leufkens HGM, Cooper C (2002) The epidemiology of corticosteroid-induced osteoporosis: a meta-analysis. Osteoporos Int 13(10):777–787. https://doi.org/10.1007/s001980200108
Ross PD (1991) Pre-existing fractures and bone mass predict vertebral fracture incidence in women. Ann Intern Med 114(11):919. https://doi.org/10.7326/0003-4819-114-11-919
Camacho PM, Petak SM, Binkley N, Clarke BL, Harris ST, Hurley DL, Kleerekoper M, Lewiecki EM, Miller PD, Narula HS, Pessah-Pollack R, Tangpricha V, Wimalawansa SJ, Watts NB (2016) American association of clinical endocrinologists and American college of endocrinology clinical practice guidelines for the diagnosis and treatment of postmenopausal osteoporosis – 2016. Endocr Pract 22(9):1111–1118. https://doi.org/10.4158/EP161435.ESGL
Lindsay R, Silverman SL, Cooper C, Hanley DA, Barton I, Broy SB, Licata A, Benhamou L, Geusens P, Flowers K, Stracke H, Seeman E (2001) Risk of new vertebral fracture in the year following a fracture. JAMA 285(3):320–323. https://doi.org/10.1001/jama.285.3.320
Gehlbach S, Saag KG, Adachi JD, Hooven FH, Flahive J, Boonen S, Chapurlat RD, Compston JE, Cooper C, Díez-Perez A, Greenspan SL, LaCroix AZ, Netelenbos JC, Pfeilschifter J, Rossini M, Roux C, Sambrook PN, Silverman S, Siris ES, Watts NB, Lindsay R (2012) Previous fractures at multiple sites increase the risk for subsequent fractures: the Global Longitudinal Study of Osteoporosis in Women. J Bone Miner Res 27(3):645–653. https://doi.org/10.1002/jbmr.1476
Edwards BJ, Bunta AD, Simonelli C, Bolander M, Fitzpatrick LA (2007) Prior fractures are common in patients with subsequent hip fractures. Clin Orthop Relat Res 461:226–230. https://doi.org/10.1097/BLO.0b013e3180534269
Gallagher JC, Genant HK, Crans GG, Vargas SJ, Krege JH (2005) Teriparatide reduces the fracture risk associated with increasing number and severity of osteoporotic fractures. J of Clin Endocrinol Metab 90(3):1583–1587. https://doi.org/10.1210/jc.2004-0826
Marcus R, Wang O, Satterwhite J, Mitlak B (2003) The skeletal response to teriparatide is largely independent of age, initial bone mineral density, and prevalent vertebral fractures in postmenopausal women with osteoporosis. J Bone Miner Res 18(1):18–23. https://doi.org/10.1359/jbmr.2003.18.1.18
Kanis JA, Barton IP, Johnell O (2005) Risedronate decreases fracture risk in patients selected solely on the basis of prior vertebral fracture. Osteoporos Int 16(5):475–482. https://doi.org/10.1007/s00198-004-1698-y
Johnell O, Kanis JA, Black DM, Balogh A, Poor G, Sarkar S, Zhou C, Pavo I (2004) Associations between baseline risk factors and vertebral fracture risk in the Multiple Outcomes of Raloxifene Evaluation (MORE) study. J Bone Miner Res 19(5):764–772. https://doi.org/10.1359/JBMR.040211
Kanis JA, Johansson H, Oden A, McCloskey EV (2011) A meta-analysis of the effect of strontium ranelate on the risk of vertebral and non-vertebral fracture in postmenopausal osteoporosis and the interaction with FRAX(®). Osteoporos Int 22(8):2347–2355. https://doi.org/10.1007/s00198-010-1474-0
Kanis JA, Johnell O, De Laet C, Johansson H, Oden A, Delmas P, Eisman J, Fujiwara S, Garnero P, Kroger H, McCloskey EV, Mellstrom D, Melton LJ, Pols H, Reeve J, Silman A, Tenenhouse A (2004) A meta-analysis of previous fracture and subsequent fracture risk. Bone 35(2):375–382. https://doi.org/10.1016/j.bone.2004.03.024
Klotzbuecher CM, Ross PD, Landsman PB, Abbott TA, Berger M (2000) Patients with prior fractures have an increased risk of future fractures: a summary of the literature and statistical synthesis. J Bone Miner Res 15(4):721–739. https://doi.org/10.1359/jbmr.2000.15.4.721
Schousboe JT, Ensrud KE, Nyman JA, Kane RL, Melton LJ (2005) Potential cost-effective use of spine radiographs to detect vertebral deformity and select osteopenic post-menopausal women for amino-bisphosphonate therapy. Osteoporos Int 16(12):1883–1893. https://doi.org/10.1007/s00198-005-1956-7
Kanis JA, Oden A, Johnell O, Jonsson B, de Laet C, Dawson A (2001) The burden of osteoporotic fractures: a method for setting intervention thresholds. Osteoporos Int 12(5):417–427. https://doi.org/10.1007/s001980170112
Nevitt MC (1998) The association of radiographically detected vertebral fractures with back pain and function: a prospective study. Ann Intern Med 128(10):793. https://doi.org/10.7326/0003-4819-128-10-199805150-00001
Yamamoto M, Yamaguchi T, Yamauchi M, Kaji H, Sugimoto T (2009) Diabetic patients have an increased risk of vertebral fractures independent of BMD or diabetic complications. J Bone Miner Res 24(4):702–709. https://doi.org/10.1359/jbmr.081207
Siminoski K, Jiang G, Adachi JD, Hanley DA, Cline G, Ioannidis G, Hodsman A, Josse RG, Kendler D, Olszynski WP, Ste Marie LG, Eastell R (2005) Accuracy of height loss during prospective monitoring for detection of incident vertebral fractures. Osteoporos Int 16(4):403–410. https://doi.org/10.1007/s00198-004-1709-z
van Staa TP, Leufkens HGM, Abenhaim L, Zhang B, Cooper C (2000) Oral corticosteroids and fracture risk: relationship to daily and cumulative doses. Rheumatology 39(12):1383–1389. https://doi.org/10.1093/rheumatology/39.12.1383
Genant HK, Wu CY, van Kuijk C, Nevitt MC (2009) Vertebral fracture assessment using a semiquantitative technique. J Bone Miner Res 8(9):1137–1148. https://doi.org/10.1002/jbmr.5650080915
Bauer DC, Garnero P, Hochberg MC, Santora A, Delmas P, Ewing SK, Black DM (2005) Pretreatment levels of bone turnover and the antifracture efficacy of alendronate: the fracture intervention trial. J Bone Miner Res 21(2):292–299. https://doi.org/10.1359/JBMR.051018
Seibel MJ, Naganathan V, Barton I, Grauer A (2003) Relationship between pretreatment bone resorption and vertebral fracture incidence in postmenopausal osteoporotic women treated with risedronate. J Bone Miner Res 19(2):323–329. https://doi.org/10.1359/JBMR.0301231
Cosman F, de Beur SJ, LeBoff MS, Lewiecki EM, Tanner B, Randall S, Lindsay R (2014) Clinician’s guide to prevention and treatment of osteoporosis. Osteoporos Int 25(10):2359–2381. https://doi.org/10.1007/s00198-014-2794-2
Kanis JA, McCloskey EV, Johansson H, Strom O, Borgstrom F, Oden A (2008) National Osteoporosis Guideline Group Case finding for the management of osteoporosis with FRAX®—assessment and intervention thresholds for the UK. Osteoporos Int 19(10):1395–1408. https://doi.org/10.1007/s00198-008-0712-1
Kanis JA, Harvey NC, Cooper C, Johansson H, Odén A, McCloskey EV (2016) A systematic review of intervention thresholds based on FRAX: A report prepared for the National Osteoporosis Guideline Group and the International Osteoporosis Foundation. Arch Osteoporos 11(1):25. https://doi.org/10.1007/s11657-016-0278-z
Merlijn T, Swart KMA, van der Horst HE, Netelenbos JC, Elders PJM (2020) Fracture prevention by screening for high fracture risk: a systematic review and meta-analysis. Osteoporos Int 31(2):251–257. https://doi.org/10.1007/s00198-019-05226-w
Rubin KH, Rothmann MJ, Holmberg T, Høiberg M, Möller S, Barkmann R, Glüer CC, Hermann AP, Bech M, Gram J, Brixen K (2018) Effectiveness of a two-step population-based osteoporosis screening program using FRAX: the randomized Risk-stratified Osteoporosis Strategy Evaluation (ROSE) study. Osteoporos Int 29(3):567–578. https://doi.org/10.1007/s00198-017-4326-3
Kanis JA, Johnell O, De Laet C, Jonsson B, Oden A, Ogelsby AK (2002) International variations in hip fracture probabilities: implications for risk assessment. J Bone Miner Res 17(7):1237–1244. https://doi.org/10.1359/jbmr.2002.17.7.1237
De Laet CEDH, Van Hout BA, Burger H, Weel AEAM, Hofman A, Pols HAP (2009) Hip fracture prediction in elderly men and women: validation in the Rotterdam study. J Bone Miner Res 13(10):1587–1593. https://doi.org/10.1359/jbmr.1998.13.10.1587
Kanis JA, Delmas P, Burckhardt P, Cooper C, Torgerson D (1997) Guidelines for diagnosis and management of osteoporosis. Osteoporosis Int 7(4):390–406. https://doi.org/10.1007/BF01623782
Lekamwasam S, Adachi JD, Agnusdei D, Bilezikian J, Boonen S, Borgström F, Cooper C, Diez Perez A, Eastell R, Hofbauer LC, Kanis JA, Langdahl BL, Lesnyak O, Lorenc R, McCloskey E, Messina OD, Napoli N, Obermayer-Pietsch B, Ralston SH, Sambrook PN, Silverman S, Sosa M, Stepan J, Suppan G, Wahl DA, Compston JE (2012) A framework for the development of guidelines for the management of glucocorticoid-induced osteoporosis. Osteoporos Int 23(9):2257–2276. https://doi.org/10.1007/s00198-012-1958-1
Johansson H, Oden A, Johnell O, Jonsson B, de Laet C, Oglesby A, McCloskey EV, Kayan K, Jalava T, Kanis JA (2004) Optimization of BMD measurements to identify high risk groups for treatment–a test analysis. J Bone Miner Res 19(6):906–913. https://doi.org/10.1359/jbmr.2004.19.6.906
Leslie WD, Majumdar SR, Lix LM, Johansson H, Oden A, McCloskey E, Kanis JA (2012) Manitoba Bone Density Program High fracture probability with FRAX usually indicates densitometric osteoporosis: implications for clinical practice. Osteoporos Int 23(1):391–397. https://doi.org/10.1007/s00198-011-1592-3
Tosteson ANA, Melton LJ, Dawson-Hughes B, Baim S, Favus MJ, Khosla S, Lindsay RL (2008) Cost-effective osteoporosis treatment thresholds: the United States perspective. Osteoporos Int 19(4):437–447. https://doi.org/10.1007/s00198-007-0550-6
Leslie WD, Morin S, Lix LM, Johansson H, Oden A, McCloskey E, Kanis JA (2012) Fracture risk assessment without bone density measurement in routine clinical practice. Osteoporos Int 23(1):75–85. https://doi.org/10.1007/s00198-011-1747-2
Kanis JA, Oden A, Johnell O, Johansson H, De Laet C, Brown J, Burckhardt P, Cooper C, Christiansen C, Cummings S, Eisman JA, Fujiwara S, Glüer C, Goltzman D, Hans D, Krieg MA, La Croix A, McCloskey E, Mellstrom D, Melton LJ 3rd, Pols H, Reeve J, Sanders K, Schott AM, Silman A, Torgerson D, van Staa T, Watts NB, Yoshimura N (2007) The use of clinical risk factors enhances the performance of BMD in the prediction of hip and osteoporotic fractures in men and women. Osteoporos Int 18(8):1033–1046. https://doi.org/10.1007/s00198-007-0343-y
Kyriakos G, Vidal-Casariego A, Fernández-Martínez MN, Blanco-Suárez MD, Ballesteros-Pomar MD, Cano-Rodríguez I (2015) Impact of the NOGG and NOF guidelines on the indication of bone mineral density in routine clinical practice. J Clin Densitom 18(4):533–538. https://doi.org/10.1016/j.jocd.2015.08.001
National Osteoporosis Foundation (NOF) and International Society for Clinical Densitometry (ISCD) (2013) Recommendations to DXA manufacturers for FRAX® implementation. Available http://www.nof.org/files/nof/public/content/resource/862/files/392.pdf. Accessed 28 Jan 2013
Leib ES, Lewiecki EM, Binkley N, Hamdy RC (2004) International Society for Clinical Densitometry Official positions of the International Society for Clinical Densitometry. J Clin Densitom 7(1):1–6. https://doi.org/10.1385/jcd:7:1:1
The Writing Group for the International Society for Clinical Densitometry (ISCD) Position Development Conference (2004) Position statement: executive summary. J Clin Densitom 7(1):7–12. https://doi.org/10.1385/jcd:7:1:7
Shepherd JA, Blake GM (2007) T-scores and Z-scores. J Clin Densitom 10(4):349–350. https://doi.org/10.1016/j.jocd.2007.08.006
Watts NB, Leslie WD, Foldes AJ, Miller PD (2013) International Society for Clinical Densitometry Position Development Conference: task force on normative databases. J Clin Densitom 16(4):472–481. https://doi.org/10.1016/j.jocd.2013.08.001
Kelly TL (1990) Bone mineral density reference databases for American men and women. J Bone Miner Res 5(2):249
Hanson J (1997) Standardization of femur BMD. J Bone Miner Res 12(8):1316–1317. https://doi.org/10.1359/jbmr.1997.12.8.1316
Kanis JA, McCloskey EV, Johansson H, Oden A, Melton LJ, Khaltaev N (2008) A reference standard for the description of osteoporosis. Bone 42(3):467–475. https://doi.org/10.1016/j.bone.2007.11.001
Nelson HD, Haney EM, Dana T, Bougatsos C, Chou R (2010) Screening for osteoporosis: an update for the U.S. Preventive Services Task Force. Ann Intern Med 153(2):99–111. https://doi.org/10.7326/0003-4819-153-2-201007200-00262
McCloskey EV, Odén A, Harvey NC, Leslie WD, Hans D, Johansson H, Barkmann R, Boutroy S, Brown J, Chapurlat R, Elders PJM, Fujita Y, Glüer CC, Goltzman D, Iki M, Karlsson M, Kindmark A, Kotowicz M, Kurumatani N, Kwok T, Lamy O, Leung J, Lippuner K, Ljunggren Ö, Lorentzon M, Mellström D, Merlijn T, Oei L, Ohlsson C, Pasco JA, Rivadeneira F, Rosengren B, Sornay-Rendu E, Szulc P, Tamaki J, Kanis JA (2016) A meta-analysis of trabecular bone score in fracture risk prediction and its relationship to FRAX: TBS in fracture risk prediction and relationship to FRAX. J Bone Miner Res 31(5):940–948. https://doi.org/10.1002/jbmr.2734
Tannenbaum C, Clark J, Schwartzman K, Wallenstein S, Lapinski R, Meier D, Luckey M (2002) Yield of laboratory testing to identify secondary contributors to osteoporosis in otherwise healthy women. J Clin Endocrinol Metab 87(10):4431–4437. https://doi.org/10.1210/jc.2002-020275
Cerdá GD, Peris P, Monegal A, Albaladejo C, Martínez MA, Muxí A, Martínez de Osaba MJ, Surís X, Guañabens N (2010) Search for hidden secondary causes in postmenopausal women with osteoporosis. Menopause 17(1):135–139. https://doi.org/10.1097/gme.0b013e3181ade8e5
Priemel M, von Domarus C, Klatte TO, Kessler S, Schlie J, Meier S, Proksch N, Pastor F, Netter C, Streichert T, Püschel K, Amling M (2010) Bone mineralization defects and vitamin D deficiency: histomorphometric analysis of iliac crest bone biopsies and circulating 25-hydroxyvitamin D in 675 patients. J Bone Miner Res 25(2):305–312. https://doi.org/10.1359/jbmr.090728
Gallagher JC, Sai AJ (2010) Bone: Is screening for secondary causes of osteoporosis worthwhile? Nat Rev Endocrinol 6(7):360–362. https://doi.org/10.1038/nrendo.2010.86
Barzel US (2003) Recommended testing in patients with low bone density. J Clin Endocrinol Metab 88(3):1404–1405. https://doi.org/10.1210/jc.2002-021951
Deutschmann HA, Weger M, Weger W, Kotanko P, Deutschmann MJ, Skrabal F (2002) Search for occult secondary osteoporosis: impact of identified possible risk factors on bone mineral density. J Intern Med 252(5):389–397. https://doi.org/10.1046/j.1365-2796.2002.01040.x
Black DM, Cummings SR, Karpf DB, Cauley JA, Thompson DE, Nevitt MC, Bauer DC, Genant HK, Haskell WL, Marcus R, Ott SM, Torner JC, Quandt SA, Reiss TF, Ensrud KE (1996) Randomised trial of effect of alendronate on risk of fracture in women with existing vertebral fractures. Lancet 348(9041):1535–1541. https://doi.org/10.1016/s0140-6736(96)07088-2
Cummings SR (1998) Effect of alendronate on risk of fracture in women with low bone density but without vertebral fractures: results from the Fracture Intervention Trial. JAMA 280(24):2077. https://doi.org/10.1001/jama.280.24.2077
Orwoll E, Ettinger M, Weiss S, Miller P, Kendler D, Graham J, Adami S, Weber K, Lorenc R, Pietschmann P, Vandormael K, Lombardi A (2000) Alendronate for the treatment of osteoporosis in men. N Engl J Med 343(9):604–610. https://doi.org/10.1056/NEJM200008313430902
Saag KG, Emkey R, Schnitzer TJ, Brown JP, Hawkins F, Goemaere S, Thamsborg G, Liberman UA, Delmas PD, Malice MP, Czachur M, Daifotis AG (1998) Alendronate for the prevention and treatment of glucocorticoid-induced osteoporosis. N Engl J Med 339(5):292–299. https://doi.org/10.1056/NEJM199807303390502
Chesnut CH, Skag A, Christiansen C, Recker R, Stakkestad JA, Hoiseth A, Felsenberg D, Huss H, Gilbride J, Schimmer RC, Delmas PD (2004) Effects of oral ibandronate administered daily or intermittently on fracture risk in postmenopausal osteoporosis. J Bone Miner Res 19(8):1241–1249. https://doi.org/10.1359/JBMR.040325
Black DM, Delmas PD, Eastell R, Reid IR, Boonen S, Cauley JA, Cosman F, Lakatos P, Leung PC, Man Z, Mautalen C, Mesenbrink P, Hu H, Caminis J, Tong K, Rosario-Jansen T, Krasnow J, Hue TF, Sellmeyer D, Eriksen EF, Cummings SR (2007) Once-yearly zoledronic acid for treatment of postmenopausal osteoporosis. N Engl J Med 356(18):1809–1822. https://doi.org/10.1056/NEJMoa067312
Boonen S, Reginster JY, Kaufman JM, Lippuner K, Zanchetta J, Langdahl B, Rizzoli R, Lipschitz S, Dimai HP, Witvrouw R, Eriksen E, Brixen K, Russo L, Claessens F, Papanastasiou P, Antunez O, Su G, Bucci-Rechtweg C, Hruska J, Incera E, Vanderschueren D, Orwoll E (2012) Fracture risk and zoledronic acid therapy in men with osteoporosis. N Engl J Med 367(18):1714–1723. https://doi.org/10.1056/NEJMoa1204061
Reid DM, Devogelaer JP, Saag K, Roux C, Lau CS, Reginster JY, Papanastasiou P, Ferreira A, Hartl F, Fashola T, Mesenbrink P, Sambrook PN (2009) Zoledronic acid and risedronate in the prevention and treatment of glucocorticoid-induced osteoporosis (HORIZON): a multicentre, double-blind, double-dummy, randomised controlled trial. Lancet 373(9671):1253–1263. https://doi.org/10.1016/S0140-6736(09)60250-6
McClung MR, Geusens P, Miller PD, Zippel H, Bensen WG, Roux C, Adami S, Fogelman I, Diamond T, Eastell R, Meunier PJ, Reginster JY, Hip Intervention Program Study Group (2001) Effect of risedronate on the risk of hip fracture in elderly women. N Engl J Med 344(5):333–340. https://doi.org/10.1056/NEJM200102013440503
Boonen S, Orwoll ES, Wenderoth D, Stoner KJ, Eusebio R, Delmas PD (2009) Once-weekly risedronate in men with osteoporosis: results of a 2-year, placebo-controlled, double-blind, multicenter study. J Bone Miner Res 24(4):719–725. https://doi.org/10.1359/jbmr.081214
Eastell R, Devogelaer J-P, Peel NFA, Chines AA, Bax DE, Sacco-Gibson N, Nagant de Deuxchaisnes C, Russell RGG (2000) Prevention of bone loss with risedronate in glucocorticoid-treated rheumatoid arthritis patients. Osteoporos Int 11(4):331–337. https://doi.org/10.1007/s001980070122
Miller PD, McClung MR, Macovei L, Stakkestad JA, Luckey M, Bonvoisin B, Reginster JY, Recker RR, Hughes C, Lewiecki EM, Felsenberg D, Delmas PD, Kendler DL, Bolognese MA, Mairon N, Cooper C (2005) Monthly oral ibandronate therapy in postmenopausal osteoporosis: 1-year results from the MOBILE study. J Bone Miner Res 20(8):1315–1322. https://doi.org/10.1359/JBMR.050313
Recker RR, Ste-Marie L-G, Langdahl B, Czerwinski E, Bonvoisin B, Masanauskaite D, Rowell L, Felsenberg D (2010) Effects of intermittent intravenous ibandronate injections on bone quality and micro-architecture in women with postmenopausal osteoporosis: The DIVA study. Bone 46(3):660–665. https://doi.org/10.1016/j.bone.2009.11.004
Harris ST, Blumentals WA, Miller PD (2008) Ibandronate and the risk of non-vertebral and clinical fractures in women with postmenopausal osteoporosis: results of a meta-analysis of phase III studies. Curr Med Res Opin 24(1):237–245. https://doi.org/10.1185/030079908X253717
Hakala M, Kröger H, Valleala H, Hienonen-Kempas T, Lehtonen-Veromaa M, Heikkinen J, Tuomiranta T, Hannonen P, Paimela L (2012) Once-monthly oral ibandronate provides significant improvement in bone mineral density in postmenopausal women treated with glucocorticoids for inflammatory rheumatic diseases: a 12-month, randomized, double-blind, placebo-controlled trial. Scand J Rheumatol 41(4):260–266. https://doi.org/10.3109/03009742.2012.664647
Ringe JD, Dorst A, Faber H, Ibach K, Sorenson F (2003) Intermittent intravenous ibandronate injections reduce vertebral fracture risk in corticosteroid-induced osteoporosis: results from a long-term comparative study. Osteoporos Int 14(10):801–807. https://doi.org/10.1007/s00198-003-1425-0
Orwoll ES, Binkley NC, Lewiecki EM, Gruntmanis U, Fries MA, Dasic G (2010) Efficacy and safety of monthly ibandronate in men with low bone density. Bone 46(4):970–976. https://doi.org/10.1016/j.bone.2009.12.034
Lyles KW, Colón-Emeric CS, Magaziner JS, Adachi JD, Pieper CF, Mautalen C, Hyldstrup L, Recknor C, Nordsletten L, Moore KA, Lavecchia C, Zhang J, Mesenbrink P, Hodgson PK, Abrams K, Orloff JJ, Horowitz Z, Eriksen EF, Boonen S (2007) Zoledronic acid and clinical fractures and mortality after hip fracture. N Engl J Med 357(18):1799–1809. https://doi.org/10.1056/NEJMoa074941
Eriksen EF, Lyles KW, Colón-Emeric CS, Pieper CF, Magaziner JS, Adachi JD, Hyldstrup L, Recknor C, Nordsletten L, Lavecchia C, Hu H, Boonen S, Mesenbrink P (2009) Antifracture efficacy and reduction of mortality in relation to timing of the first dose of zoledronic acid after hip fracture. J Bone Miner Res 24(7):1308–1313. https://doi.org/10.1359/jbmr.090209
Avdeeva VA, Suplotova LA, Pigarova EA, Rozhinskaya LY, Troshina EA (2021) Vitamin D deficiency in Russia: the first results of a registered, non-interventional study of the frequency of vitamin D deficiency and insufficiency in various geographic regions of the country. Probl Endokrinol (Mosk) 67(2):84–92. https://doi.org/10.14341/probl12736
Dedov II, Mel’nichenko GA, Mokrysheva NG, Pigarova EA, Povaliaeva AA, Rozhinskaya LYa, Belaya ZhE, Dzeranova LK, Karonova TL, Suplotova LA, Troshina EA (2022) Draft federal clinical practice guidelines for the diagnosis, treatment, and prevention of vitamin D deficiency. Osteopor Bone Dis 24(4):4–26
Pludowski P, Takacs I, Boyanov M, Belaya Z, Diaconu CC, Mokhort T, Zherdova N, Rasa I, Payer J, Pilz S (2022) Clinical Practice in the Prevention, Diagnosis and Treatment of Vitamin D Deficiency: A Central and Eastern European Expert Consensus Statement. Nutrients 14(7):1483. https://doi.org/10.3390/nu14071483
McClung M, Miller P, Recknor C, Mesenbrink P, Bucci-Rechtweg C, Benhamou C-L (2009) Zoledronic acid for the prevention of bone loss in postmenopausal women with low bone mass: a randomized controlled trial. Obstet Gynecol 114(5):999–1007. https://doi.org/10.1097/AOG.0b013e3181bdce0a
Reid IR, Horne AM, Mihov B, Stewart A, Garratt E, Wong S, Wiessing KR, Bolland MJ, Bastin S (2018) Gamble GD (2018) Fracture prevention with zoledronate in older women with osteopenia. N Engl J Med 379(25):2407–2416. https://doi.org/10.1056/NEJMoa1808082
Cummings SR, San Martin J, McClung MR, Siris ES, Eastell R, Reid IR, Delmas P, Zoog HB, Austin M, Wang A, Kutilek S, Adami S, Zanchetta J, Libanati C, Siddhanti S, Christiansen C (2009) Denosumab for prevention of fractures in postmenopausal women with osteoporosis. N Engl J Med 361(8):756–765. https://doi.org/10.1056/NEJMoa0809493
Langdahl BL, Teglbjærg CS, Ho PR, Chapurlat R, Czerwinski E, Kendler DL, Reginster JY, Kivitz A, Lewiecki EM, Miller PD, Bolognese MA, McClung MR, Bone HG, Ljunggren Ö, Abrahamsen B, Gruntmanis U, Yang YC, Wagman RB, Mirza F, Siddhanti S, Orwoll E (2015) A 24-month study evaluating the efficacy and safety of denosumab for the treatment of men with low bone mineral density: results from the ADAMO trial. J Clin Endocrinol Metab 100(4):1335–1342. https://doi.org/10.1210/jc.2014-4079
Orwoll E, Teglbjærg CS, Langdahl BL, Chapurlat R, Czerwinski E, Kendler DL, Reginster JY, Kivitz A, Lewiecki EM, Miller PD, Bolognese MA, McClung MR, Bone HG, Ljunggren Ö, Abrahamsen B, Gruntmanis U, Yang YC, Wagman RB, Siddhanti S, Grauer A, Hall JW, Boonen S (2012) A randomized, placebo-controlled study of the effects of denosumab for the treatment of men with low bone mineral density. J Clin Endocrinol Metab 97(9):3161–3169. https://doi.org/10.1210/jc.2012-1569
Saag KG, Pannacciulli N, Geusens P, Adachi JD, Messina OD, Morales-Torres J, Emkey R, Butler PW, Yin X, Lems WF (2019) Denosumab versus risedronate in glucocorticoid-induced osteoporosis: final results of a twenty-four–month randomized, double-blind, double-dummy trial. Arthritis Rheumatol 71(7):1174–1184. https://doi.org/10.1002/art.40874
Gnant M, Pfeiler G, Dubsky PC, Hubalek M, Greil R, Jakesz R, Wette V, Balic M, Haslbauer F, Melbinger E, Bjelic-Radisic V, Artner-Matuschek S, Fitzal F, Marth C, Sevelda P, Mlineritsch B, Steger GG, Manfreda D, Exner R, Egle D, Bergh J, Kainberger F, Talbot S, Warner D, Fesl C, Singer CF (2015) Adjuvant denosumab in breast cancer (ABCSG-18): a multicentre, randomised, double-blind, placebo-controlled trial. Lancet 386(9992):433–443. https://doi.org/10.1016/S0140-6736(15)60995-3
Smith MR, Egerdie B, Hernández Toriz N, Feldman R, Tammela TL, Saad F, Heracek J, Szwedowski M, Ke C, Kupic A, Leder BZ, Goessl C (2009) Denosumab in men receiving androgen-deprivation therapy for prostate cancer. N Engl J Med 361(8):745–755. https://doi.org/10.1056/NEJMoa0809003
Amiche MA, Albaum JM, Tadrous M, Pechlivanoglou P, Lévesque LE, Adachi JD, Cadarette SM (2016) Efficacy of osteoporosis pharmacotherapies in preventing fracture among oral glucocorticoid users: a network meta-analysis. Osteoporos Int 27(6):1989–1998. https://doi.org/10.1007/s00198-015-3476-4
Coskun Benlidayi I (2018) Denosumab in the treatment of glucocorticoid-induced osteoporosis. Rheumatol Int 38(11):1975–1984. https://doi.org/10.1007/s00296-018-4106-1
Yanbeiy ZA, Hansen KE (2019) Denosumab in the treatment of glucocorticoid-induced osteoporosis: a systematic review and meta-analysis. DDDT 13:2843–2852. https://doi.org/10.2147/DDDT.S148654
Yamaguchi Y, Morita T, Kumanogoh A (2020) The therapeutic efficacy of denosumab for the loss of bone mineral density in glucocorticoid-induced osteoporosis: a meta-analysis. Rheumatol Adv Pract 4(1):rkaa008. https://doi.org/10.1093/rap/rkaa008
Brown JP, Prince RL, Deal C, Recker RR, Kiel DP, de Gregorio LH, Hadji P, Hofbauer LC, Alvaro-Gracia JM, Wang H, Austin M, Wagman RB, Newmark R, Libanati C, San Martin J, Bone HG (2009) Comparison of the effect of denosumab and alendronate on BMD and biochemical markers of bone turnover in postmenopausal women with low bone mass: a randomized, blinded, phase 3 trial. J Bone Miner Res 24(1):153–161. https://doi.org/10.1359/jbmr.0809010
Choi N-K, Solomon DH, Tsacogianis TN, Landon JE, Song HJ, Kim SC (2017) Comparative safety and effectiveness of denosumab versus zoledronic acid in patients with osteoporosis: a cohort study: safety and effectiveness of denosumab versus zoledronic acid. J Bone Miner Res 32(3):611–617. https://doi.org/10.1002/jbmr.3019
Tsai JN, Uihlein AV, Burnett-Bowie S-AM, Neer RM, Zhu Y, Derrico N, Lee H, Bouxsein ML, Leder BZ (2015) Comparative effects of teriparatide, denosumab, and combination therapy on peripheral compartmental bone density, microarchitecture, and estimated strength: the DATA-HRpQCT study: effects of combined teriparatide/denosumab on bone quality. J Bone Miner Res 30(1):39–45. https://doi.org/10.1002/jbmr.2315
Broadwell A, Chines A, Ebeling PR, Franek E, Huang S, Smith S, Kendler D, Messina O, Miller PD (2021) Denosumab safety and efficacy among participants in the FREEDOM extension study with mild to moderate chronic kidney disease. J Clin Endocrinol Metab 106(2):397–409. https://doi.org/10.1210/clinem/dgaa851
Kendler DL, Roux C, Benhamou CL, Brown JP, Lillestol M, Siddhanti S, Man H-S, Martin JS, Bone HG (2010) Effects of denosumab on bone mineral density and bone turnover in postmenopausal women transitioning from alendronate therapy. J Bone Miner Res 25(1):72–81. https://doi.org/10.1359/jbmr.090716
Meier C, Uebelhart B, Aubry-Rozier B, Birkhäuser M, Bischoff-Ferrari HA, Frey D, Kressig RW, Lamy O, Lippuner K, Stute P, Suhm N, Ferrari S (2017) Osteoporosis drug treatment: duration and management after discontinuation. A position statement from the SVGO/ASCO. Swiss Med Wkly 16(147):w14484. https://doi.org/10.4414/smw.2017.14484
Miller PD, Pannacciulli N, Brown JP, Czerwinski E, Nedergaard BS, Bolognese MA, Malouf J, Bone HG, Reginster JY, Singer A, Wang C, Wagman RB, Cummings SR (2016) Denosumab or zoledronic acid in postmenopausal women with osteoporosis previously treated with oral bisphosphonates. J Clin Endocrinol Metab 101(8):3163–3170. https://doi.org/10.1210/jc.2016-1801
Miller PD, Bolognese MA, Lewiecki EM, McClung MR, Ding B, Austin M, Liu Y, San Martin J (2008) Effect of denosumab on bone density and turnover in postmenopausal women with low bone mass after long-term continued, discontinued, and restarting of therapy: a randomized blinded phase 2 clinical trial. Bone 43(2):222–229. https://doi.org/10.1016/j.bone.2008.04.007
Baron R, Ferrari S, Russell RGG (2011) Denosumab and bisphosphonates: different mechanisms of action and effects. Bone 48(4):677–692. https://doi.org/10.1016/j.bone.2010.11.020
Masarachia P, Weinreb M, Balena R, Rodan GA (1996) Comparison of the distribution of 3H-alendronate and 3H-Etidronate in rat and mouse bones. Bone 19(3):281–290. https://doi.org/10.1016/8756-3282(96)00182-2
Mandema JW, Zheng J, Libanati C, Perez Ruixo JJ (2014) Time course of bone mineral density changes with denosumab compared with other drugs in postmenopausal osteoporosis: a dose-response–based meta-analysis. J Clin Endocrinol Metab 99(10):3746–3755. https://doi.org/10.1210/jc.2013-3795
Jalleh R, Basu G, Le Leu R, Jesudason S (2018) Denosumab-induced severe hypocalcaemia in chronic kidney disease. Case Rep Nephrol 2018:1–7. https://doi.org/10.1155/2018/7384763
Orwoll E, Scheele W, Paul S, Adami S, Syversen U, Diez-Perez A, Kaufman J-M, Clancy A, Gaich G (2003) The effect of teriparatide [human parathyroid hormone (1–34)] therapy on bone density in men with osteoporosis. J Bone Miner Res 18(1):9–17. https://doi.org/10.1359/jbmr.2003.18.1.9
Saag KG, Shane E, Boonen S, Marín F, Donley DW, Taylor KA, Dalsky GP, Marcus R (2007) Teriparatide or alendronate in glucocorticoid-induced osteoporosis. N Engl J Med 357(20):2028–2039. https://doi.org/10.1056/NEJMoa071408
Saag KG, Zanchetta JR, Devogelaer J-P, Adler RA, Eastell R, See K, Krege JH, Krohn K, Warner MR (2009) Effects of teriparatide versus alendronate for treating glucocorticoid-induced osteoporosis: thirty-six-month results of a randomized, double-blind, controlled trial. Arthritis Rheum 60(11):3346–3355. https://doi.org/10.1002/art.24879
Neer RM, Arnaud CD, Zanchetta JR, Prince R, Gaich GA, Reginster JY, Hodsman AB, Eriksen EF, Ish-Shalom S, Genant HK, Wang O, Mitlak BH (2001) Effect of parathyroid hormone (1–34) on fractures and bone mineral density in postmenopausal women with osteoporosis. N Engl J Med 344(19):1434–1441. https://doi.org/10.1056/NEJM200105103441904
Kendler DL, Marin F, Zerbini CAF, Russo LA, Greenspan SL, Zikan V, Bagur A, Malouf-Sierra J, Lakatos P, Fahrleitner-Pammer A, Lespessailles E, Minisola S, Body JJ, Geusens P, Möricke R, López-Romero P (2018) Effects of teriparatide and risedronate on new fractures in post-menopausal women with severe osteoporosis (VERO): a multicentre, double-blind, double-dummy, randomised controlled trial. Lancet 391(10117):230–240. https://doi.org/10.1016/S0140-6736(17)32137-2
Body JJ, Gaich GA, Scheele WH, Kulkarni PM, Miller PD, Peretz A, Dore RK, Correa-Rotter R, Papaioannou A, Cumming DC, Hodsman AB (2002) A randomized double-blind trial to compare the efficacy of teriparatide [recombinant human parathyroid hormone (1–34)] with alendronate in postmenopausal women with osteoporosis. J Clin Endocrinol Metab 87(10):4528–4535. https://doi.org/10.1210/jc.2002-020334
Liu C-L, Lee H-C, Chen C-C, Cho D-Y (2017) Head-to-head comparisons of bisphosphonates and teriparatide in osteoporosis: a meta-analysis. CIM 40(3):146–157. https://doi.org/10.25011/cim.v40i3.28394
Wang Y-K, Qin S-Q, Ma T, Song W, Jiang R-Q, Guo J-B, Li K, Zhang Y-M (2017) Effects of teriparatide versus alendronate for treatment of postmenopausal osteoporosis: a meta-analysis of randomized controlled trials. Medicine 96(21):e6970. https://doi.org/10.1097/MD.0000000000006970
Hadji P, Zanchetta JR, Russo L, Recknor CP, Saag KG, McKiernan FE, Silverman SL, Alam J, Burge RT, Krege JH, Lakshmanan MC, Masica DN, Mitlak BH, Stock JL (2011) Effect of teriparatide compared with risedronate on back pain and incident vertebral fractures in postmenopausal women with osteoporotic vertebral fractures. Bone 48:S82-83. https://doi.org/10.1016/j.bone.2011.03.108
Miller PD, Shergy WJ, Body J-J, Chen P, Rohe ME, Krege JH (2005) Long-term reduction of back pain risk in women with osteoporosis treated with teriparatide compared with alendronate. J Rheumatol 32(8):1556–1562
Bone HG, Hosking D, Devogelaer JP, Tucci JR, Emkey RD, Tonino RP, Rodriguez-Portales JA, Downs RW, Gupta J, Santora AC, Liberman UA (2004) Ten years’ experience with alendronate for osteoporosis in postmenopausal women. N Engl J Med 350(12):1189–1199. https://doi.org/10.1056/NEJMoa030897
Vasikaran S, Eastell R, Bruyère O, Foldes AJ, Garnero P, Griesmacher A, McClung M, Morris HA, Silverman S, Trenti T, Wahl DA, Cooper C, Kanis JA (2011) Markers of bone turnover for the prediction of fracture risk and monitoring of osteoporosis treatment: a need for international reference standards. Osteoporos Int 22(2):391–420. https://doi.org/10.1007/s00198-010-1501-1
Johansson H, Odén A, Kanis JA, McCloskey EV, Morris HA, Cooper C (2014) Vasikaran S (2014) A meta-analysis of reference markers of bone turnover for prediction of fracture. Calcif Tissue Int 94(5):560–567. https://doi.org/10.1007/s00223-014-9842-y
Eastell R, Barton I, Hannon RA, Chines A, Garnero P, Delmas PD (2003) Relationship of early changes in bone resorption to the reduction in fracture risk with risedronate. J Bone Miner Res 18(6):1051–1056. https://doi.org/10.1359/jbmr.2003.18.6.1051
Hochberg MC, Greenspan S, Wasnich RD, Miller P, Thompson DE, Ross PD (2002) Changes in bone density and turnover explain the reductions in incidence of nonvertebral fractures that occur during treatment with antiresorptive agents. J Clin Endocrinol Metab 87(4):1586–1592. https://doi.org/10.1210/jcem.87.4.8415
Black DM, Schwartz AV, Ensrud KE, Cauley JA, Levis S, Quandt SA, Satterfield S, Wallace RB, Bauer DC, Palermo L, Wehren LE, Lombardi A, Santora AC, Cummings SR (2006) Effects of continuing or stopping alendronate after 5 years of treatment: the Fracture Intervention Trial Long-term Extension (FLEX): a randomized trial. JAMA 296(24):2927. https://doi.org/10.1001/jama.296.24.2927
Delmas PD, Eastell R, Garnero P, Seibel MJ, Stepan J (2000) The use of biochemical markers of bone turnover in osteoporosis Committee of Scientific Advisors of the International Osteoporosis Foundation. Osteoporos Int 11(Suppl 6):2–17. https://doi.org/10.1007/s001980070002
Bauer DC, Black DM, Bouxsein ML, Lui LY, Cauley JA, de Papp AE, Grauer A, Khosla S, McCulloch CE, Eastell R (2018) Treatment-related changes in bone turnover and fracture risk reduction in clinical trials of anti-resorptive drugs: a meta-regression: bone turnover & fracture risk in clinical trials of antiresorptive drugs. J Bone Miner Res 33(4):634–642. https://doi.org/10.1002/jbmr.3355
Imaz I, Zegarra P, González-Enríquez J, Rubio B, Alcazar R, Amate JM (2010) Poor bisphosphonate adherence for treatment of osteoporosis increases fracture risk: systematic review and meta-analysis. Osteoporos Int 21(11):1943–1951. https://doi.org/10.1007/s00198-009-1134-4
Bergmann P, Body J-J, Boonen S, Boutsen Y, Devogelaer J-P, Goemaere S, Kaufman J-M, Reginster J-Y, Gangji V (2009) Evidence-based guidelines for the use of biochemical markers of bone turnover in the selection and monitoring of bisphosphonate treatment in osteoporosis: a consensus document of the Belgian Bone Club. Int J Clin Pract 63(1):19–26. https://doi.org/10.1111/j.1742-1241.2008.01911.x
Hwang JS, Lee S, Gong HS (2022) The impact of acute fracture on interpretation of bone turnover marker measurements for patients starting anti-resorptive therapies. Bone 154:116199. https://doi.org/10.1016/j.bone.2021.116199
Yamamoto T, Tsujimoto M, Hamaya E, Sowa H (2013) Assessing the effect of baseline status of serum bone turnover markers and vitamin D levels on efficacy of teriparatide 20 μg/day administered subcutaneously in Japanese patients with osteoporosis. J Bone Miner Metab 31(2):199–205. https://doi.org/10.1007/s00774-012-0403-z
Cummings SR, Karpf DB, Harris F, Genant HK, Ensrud K, LaCroix AZ, Black DM (2002) Improvement in spine bone density and reduction in risk of vertebral fractures during treatment with antiresorptive drugs. Am J Med 112(4):281–289. https://doi.org/10.1016/s0002-9343(01)01124-x
Chen P, Miller PD, Delmas PD, Misurski DA, Krege JH (2006) Change in lumbar spine BMD and vertebral fracture risk reduction in teriparatide-treated postmenopausal women with osteoporosis. J Bone Miner Res 21(11):1785–1790. https://doi.org/10.1359/jbmr.060802
Adler RA, El-Hajj Fuleihan G, Bauer DC, Camacho PM, Clarke BL, Clines GA, Compston JE, Drake MT, Edwards BJ, Favus MJ, Greenspan SL, McKinney R Jr, Pignolo RJ, Sellmeyer DE (2016) Managing osteoporosis in patients on long-term bisphosphonate treatment: report of a task force of the American Society for bone and mineral research: managing osteoporosis patients on long term BPs. J Bone Miner Res 31(1):16–35. https://doi.org/10.1002/jbmr.2708
Black DM, Reid IR, Boonen S, Bucci-Rechtweg C, Cauley JA, Cosman F, Cummings SR, Hue TF, Lippuner K, Lakatos P, Leung PC, Man Z, Martinez RL, Tan M, Ruzycky ME, Su G, Eastell R (2012) The effect of 3 versus 6 years of zoledronic acid treatment of osteoporosis: a randomized extension to the HORIZON-Pivotal Fracture Trial (PFT). J Bone Miner Res 27(2):243–254. https://doi.org/10.1002/jbmr.1494
Black DM, Reid IR, Cauley JA, Cosman F, Leung PC, Lakatos P, Lippuner K, Cummings SR, Hue TF, Mukhopadhyay A, Tan M, Aftring RP, Eastell R (2015) The effect of 6 versus 9 years of zoledronic acid treatment in osteoporosis: a randomized second extension to the HORIZON-Pivotal Fracture Trial (PFT). J Bone Miner Res 30(5):934–944. https://doi.org/10.1002/jbmr.2442
Dennison EM, Cooper C, Kanis JA, Bruyère O, Silverman S, McCloskey E, Abrahamsen B, Prieto-Alhambra D, Ferrari S, IOF Epidemiology/Quality of Life Working Group (2019) Fracture risk following intermission of osteoporosis therapy. Osteoporos Int 30(9):1733–1743. https://doi.org/10.1007/s00198-019-05002-w
Bone HG, Wagman RB, Brandi ML, Brown JP, Chapurlat R, Cummings SR, Czerwiński E, Fahrleitner-Pammer A, Kendler DL, Lippuner K, Reginster JY, Roux C, Malouf J, Bradley MN, Daizadeh NS, Wang A, Dakin P, Pannacciulli N, Dempster DW, Papapoulos S (2017) 10 years of denosumab treatment in postmenopausal women with osteoporosis: results from the phase 3 randomised FREEDOM trial and open-label extension. Lancet Diabetes Endocrinol 5(7):513–523. https://doi.org/10.1016/S2213-8587(17)30138-9
Bone HG, Bolognese MA, Yuen CK, Kendler DL, Miller PD, Yang Y-C, Grazette L, San Martin J, Gallagher JC (2011) Effects of denosumab treatment and discontinuation on bone mineral density and bone turnover markers in postmenopausal women with low bone mass. J Clin Endocrinol Metab 96(4):972–980. https://doi.org/10.1210/jc.2010-1502
Bone HG, Chapurlat R, Brandi ML, Brown JP, Czerwinski E, Krieg MA, Mellström D, Radominski SC, Reginster JY, Resch H, Ivorra JA, Roux C, Vittinghoff E, Daizadeh NS, Wang A, Bradley MN, Franchimont N, Geller ML, Wagman RB, Cummings SR, Papapoulos S (2013) The effect of three or six years of denosumab exposure in women with postmenopausal osteoporosis: results from the FREEDOM extension. J Clin Endocrinol Metab 98(11):4483–4492. https://doi.org/10.1210/jc.2013-1597
Anagnostis P, Paschou SA, Mintziori G, Ceausu I, Depypere H, Lambrinoudaki I, Mueck A, Pérez-López FR, Rees M, Senturk LM, Simoncini T, Stevenson JC, Stute P, Trémollieres FA, Goulis DG (2017) Drug holidays from bisphosphonates and denosumab in postmenopausal osteoporosis: EMAS position statement. Maturitas 101:23–30. https://doi.org/10.1016/j.maturitas.2017.04.008
Belaya ZE, Bilezikian JP, Ershova OB, Lesnyak OM, Marchenkova LA, Rodionova SS, Rozhinskaya LY, Toroptsova NV, Yureneva SV (2018) Long-term treatment options for postmenopausal osteoporosis: results of recent clinical studies of denosumab. Osteopor Bone Dis 21(1):17–22. https://doi.org/10.14341/osteo9760
Brown JP, Roux C, Törring O, Ho PR, Beck Jensen JE, Gilchrist N, Recknor C, Austin M, Wang A, Grauer A, Wagman RB (2013) Discontinuation of denosumab and associated fracture incidence: analysis from the Fracture Reduction Evaluation of Denosumab in Osteoporosis Every 6 Months (FREEDOM) trial. J Bone Miner Res 28(4):746–752. https://doi.org/10.1002/jbmr.1808
Tsourdi E, Zillikens MC, Meier C, Body JJ, Gonzalez Rodriguez E, Anastasilakis AD, Abrahamsen B, McCloskey E, Hofbauer LC, Guañabens N, Obermayer-Pietsch B, Ralston SH, Eastell R, Pepe J, Palermo A, Langdahl B (2021) Fracture risk and management of discontinuation of denosumab therapy: a systematic review and position statement by ECTS. J Clin Endocrinol Metab 106(1):264–281. https://doi.org/10.1210/clinem/dgaa756
McClung MR (2006) Inhibition of RANKL as a treatment for osteoporosis: Preclinical and early clinical studies. Curr Osteoporos Rep 4(1):28–33. https://doi.org/10.1007/s11914-006-0012-7
Popp AW, Zysset PK, Lippuner K (2016) Rebound-associated vertebral fractures after discontinuation of denosumab – from clinic and biomechanics. Osteoporos Int 27(5):1917–1921. https://doi.org/10.1007/s00198-015-3458-6
Tsourdi E, Langdahl B, Cohen-Solal M, Aubry-Rozier B, Eriksen EF, Guañabens N, Obermayer-Pietsch B, Ralston SH, Eastell R, Zillikens MC (2017) Discontinuation of Denosumab therapy for osteoporosis: a systematic review and position statement by ECTS. Bone 105:11–17. https://doi.org/10.1016/j.bone.2017.08.003
Anastasilakis AD, Polyzos SA, Makras P, Aubry-Rozier B, Kaouri S, Lamy O (2017) Clinical Features of 24 patients with rebound-associated vertebral fractures after denosumab discontinuation: systematic review and additional cases: denosumab discountinuation and vertebral fractures. J Bone Miner Res 32(6):1291–1296. https://doi.org/10.1002/jbmr.3110
Kendler D, Chines A, Clark P, Ebeling PR, McClung M, Rhee Y, Huang S, Stad RK (2020) Bone mineral density after transitioning from denosumab to alendronate. J Clin Endocrinol Metab 105(3):255–264. https://doi.org/10.1210/clinem/dgz095
Palacios S, Agodoa I, Bonnick S, Van den Bergh JP, Ferreira I, Ho P-R, Brown JP (2015) Treatment satisfaction in postmenopausal women suboptimally adherent to bisphosphonates who transitioned to denosumab compared with risedronate or ibandronate. J Clin Endocrinol Metab 100(3):487–492. https://doi.org/10.1210/jc.2014-3594
Freemantle N, Satram-Hoang S, Tang E-T, Kaur P, Macarios D, Siddhanti S, Borenstein J, Kendler DL (2012) Final results of the DAPS (Denosumab Adherence Preference Satisfaction) study: a 24-month, randomized, crossover comparison with alendronate in postmenopausal women. Osteoporos Int 23(1):317–326. https://doi.org/10.1007/s00198-011-1780-1
Kadaru T, Shibli-Rahhal A (2021) Zoledronic acid after treatment with denosumab is associated with bone loss within 1 year. J Bone Metab 28(1):51–58. https://doi.org/10.11005/jbm.2021.28.1.51
Sølling AS, Harsløf T, Langdahl B (2021) Treatment with zoledronate subsequent to denosumab in osteoporosis: a 2-year randomized study. J Bone Miner Res 36(7):1245–1254. https://doi.org/10.1002/jbmr.4305
Cummings SR, Cosman F, Lewiecki EM, Schousboe JT, Bauer DC, Black DM, Brown TD, Cheung AM, Cody K, Cooper C, Diez-Perez A, Eastell R, Hadji P, Hosoi T, Jan De Beur S, Kagan R, Kiel DP, Reid IR, Solomon DH, Randall S (2017) Goal-directed treatment for osteoporosis: a progress report from the ASBMR-NOF Working Group on goal-directed treatment for osteoporosis. J Bone Miner Res 32(1):3–10. https://doi.org/10.1002/jbmr.3039
Everts-Graber J, Reichenbach S, Ziswiler HR, Studer U, Lehmann T (2020) A single infusion of zoledronate in postmenopausal women following denosumab discontinuation results in partial conservation of bone mass gains. J Bone Miner Res 35(7):1207–1215. https://doi.org/10.1002/jbmr.3962
Ramchand SK, David NL, Lee H, Eastell R, Tsai JN, Leder BZ (2021) Efficacy of zoledronic acid in maintaining areal and volumetric bone density after combined denosumab and teriparatide administration: DATA-HD study extension. J Bone Miner Res 36(5):921–930. https://doi.org/10.1002/jbmr.4259
Horne AM, Mihov B, Reid IR (2018) Bone loss after romosozumab/denosumab: effects of bisphosphonates. Calcif Tissue Int 103(1):55–61. https://doi.org/10.1007/s00223-018-0404-6
Leder BZ, Tsai JN, Uihlein AV, Wallace PM, Lee H, Neer RM, Burnett-Bowie S-AM (2015) Denosumab and teriparatide transitions in postmenopausal osteoporosis (the DATA-Switch study): extension of a randomised controlled trial. Lancet 386(9999):1147–1155. https://doi.org/10.1016/S0140-6736(15)61120-5
Ebina K, Hashimoto J, Kashii M, Hirao M, Kaneshiro S, Noguchi T, Tsukamoto Y, Yoshikawa H (2017) The effects of switching daily teriparatide to oral bisphosphonates or denosumab in patients with primary osteoporosis. J Bone Miner Metab 35(1):91–98. https://doi.org/10.1007/s00774-015-0731-x
Rittmaster RS, Bolognese M, Ettinger MP, Hanley DA, Hodsman AB, Kendler DL, Rosen CJ (2000) Enhancement of bone mass in osteoporotic women with parathyroid hormone followed by alendronate. J Clin Endocrinol Metab 85(6):2129–2134. https://doi.org/10.1210/jcem.85.6.6614
Burkard D, Beckett T, Kourtjian E, Messingschlager C, Sipahi R, Padley M, Stubbart J (2018) Effects of bone remodeling agents following teriparatide treatment. Osteoporos Int 29(6):1351–1357. https://doi.org/10.1007/s00198-018-4434-8
Diez-Perez A, Adachi JD, Agnusdei D, Bilezikian JP, Compston JE, Cummings SR, Eastell R, Eriksen EF, Gonzalez-Macias J, Liberman UA, Wahl DA, Seeman E, Kanis JA, Cooper C (2012) Treatment failure in osteoporosis. Osteoporos Int 23(12):2769–2774. https://doi.org/10.1007/s00198-012-2093-8
Baber RJ, Panay N, Fenton A (2016) 2016 IMS Recommendations on women’s midlife health and menopause hormone therapy. Climacteric 19(2):109–150. https://doi.org/10.3109/13697137.2015.1129166
Rossouw JE, Anderson GL, Prentice RL, LaCroix AZ, Kooperberg C, Stefanick ML, Jackson RD, Beresford SA, Howard BV, Johnson KC, Kotchen JM, Ockene J (2002) Risks and benefits of estrogen plus progestin in healthy postmenopausal women: principal results From the Women’s Health Initiative randomized controlled trial. JAMA 288(3):321–333. https://doi.org/10.1001/jama.288.3.321
Ettinger B, Ensrud KE, Wallace R, Johnson KC, Cummings SR, Yankov V, Vittinghoff E, Grady D (2004) Effects of ultralow-dose transdermal estradiol on bone mineral density: a randomized clinical trial. Obstet Gynecol 104(3):443–451. https://doi.org/10.1097/01.AOG.0000137833.43248.79
de Villiers TJ, Hall JE, Pinkerton JV, Pérez SC, Rees M, Yang C, Pierroz DD (2016) Revised global consensus statement on menopausal hormone therapy. Maturitas 91:153–155. https://doi.org/10.1016/j.maturitas.2016.06.001
McLellan AR, Reid DM, Forbes K, Reid R, Campbell C, Gregori A, Raby N, Simpson A (2004) Effectiveness of strategies for the secondary prevention of osteoporotic fractures in Scotland, an audit funded by NHS Quality Improvement Scotland (Project CEPS 99/03). Available at http://www.healthcareimprovementscotland.org/previous_resources/audit_report/osteoporotic_fractures_audit.aspx
Åkesson K, Marsh D, Mitchell PJ, McLellan AR, Stenmark J, Pierroz DD, Kyer C, Cooper C (2013) Capture the fracture: a best practice framework and global campaign to break the fragility fracture cycle. Osteoporos Int 24(8):2135–2152. https://doi.org/10.1007/s00198-013-2348-z
Hagino H, Sawaguchi T, Endo N, Ito Y, Nakano T, Watanabe Y (2012) The risk of a second hip fracture in patients after their first hip fracture. Calcif Tissue Int 90(1):14–21. https://doi.org/10.1007/s00223-011-9545-6
Dell R (2011) Fracture prevention in Kaiser Permanente Southern California. Osteoporos Int 22(S3):457–460. https://doi.org/10.1007/s00198-011-1712-0
Nakayama A, Major G, Holliday E, Attia J, Bogduk N (2016) Evidence of effectiveness of a fracture liaison service to reduce the re-fracture rate. Osteoporos Int 27(3):873–879. https://doi.org/10.1007/s00198-015-3443-0
Marsh D, Akesson K, Beaton DE, Bogoch ER, Boonen S, Brandi ML, McLellan AR, Mitchell PJ, Sale JE, Wahl DA (2011) Coordinator-based systems for secondary prevention in fragility fracture patients. Osteoporos Int 22(7):2051–2065. https://doi.org/10.1007/s00198-011-1642-x
Ganda K, Mitchell PJ, Seibel MJ (2019) Models of secondary fracture prevention: systematic review and metaanalysis of outcomes. Academic Press, London. https://doi.org/10.1016/B978-0-12-813136-7.01001-2
Ganda K, Puech M, Chen JS, Speerin R, Bleasel J, Center JR, Eisman JA, March L, Seibel MJ (2013) Models of care for the secondary prevention of osteoporotic fractures: a systematic review and meta-analysis. Osteoporos Int 24(2):393–406. https://doi.org/10.1007/s00198-012-2090-y
Huntjens KMB, van Geel TACM, van den Bergh JPW, van Helden S, Willems P, Winkens B, Eisman JA, Geusens PP, Brink PRG (2014) Fracture Liaison Service: impact on subsequent nonvertebral fracture incidence and mortality. J Bone Joint Surg Am 96(4):e29. https://doi.org/10.2106/JBJS.L.00223
Hawley S, Javaid MK, Prieto-Alhambra D, Lippett J, Sheard S, Arden NK, Cooper C, Judge A (2016) Clinical effectiveness of orthogeriatric and fracture liaison service models of care for hip fracture patients: population-based longitudinal study. Age Ageing 45(2):236–242. https://doi.org/10.1093/ageing/afv204
Majumdar SR, Lier DA, Rowe BH, Russell AS, McAlister FA, Maksymowych WP, Hanley DA, Morrish DW, Johnson JA (2011) Cost-effectiveness of a multifaceted intervention to improve quality of osteoporosis care after wrist fracture. Osteoporos Int 22(6):1799–1808. https://doi.org/10.1007/s00198-010-1412-1
McLellan AR, Wolowacz SE, Zimovetz EA, Beard SM, Lock S, McCrink L, Adekunle F, Roberts D (2011) Fracture liaison services for the evaluation and management of patients with osteoporotic fracture: a cost-effectiveness evaluation based on data collected over 8 years of service provision. Osteoporos Int 22(7):2083–2098. https://doi.org/10.1007/s00198-011-1534-0
Gregson CL, Armstrong DJ, Bowden J, Cooper C, Edwards J, Gittoes NJL, Harvey NC, Kanis J, Leyland S, Low R, McCloskey E, Moss K, Parker J, Paskins Z, Poole KES, Reid DM, Stone M, Tomson J, Compston VN, J, (2022) UK clinical guideline for the prevention and treatment of osteoporosis. Arch Osteoporos 17:58. https://doi.org/10.1007/s11657-022-01061-5
Funding
Zhanna Belaya, Liudmila Rozhinskaya, Ivan Dedov, Elizaveta Mamedova, and Galina Melnichenko received state research funding AAAA-A20-120011690202–4 which compensated their work on a regular salary basis.
Author information
Authors and Affiliations
Corresponding author
Ethics declarations
Conflicts of interest
None.
Additional information
Publisher's note
Springer Nature remains neutral with regard to jurisdictional claims in published maps and institutional affiliations.
Rights and permissions
Springer Nature or its licensor (e.g. a society or other partner) holds exclusive rights to this article under a publishing agreement with the author(s) or other rightsholder(s); author self-archiving of the accepted manuscript version of this article is solely governed by the terms of such publishing agreement and applicable law.
About this article
Cite this article
Belaya, Z., Rozhinskaya, L., Dedov, I. et al. A summary of the Russian clinical guidelines on the diagnosis and treatment of osteoporosis. Osteoporos Int 34, 429–447 (2023). https://doi.org/10.1007/s00198-022-06667-6
Received:
Accepted:
Published:
Issue Date:
DOI: https://doi.org/10.1007/s00198-022-06667-6