Abstract
Purpose
The aims of this study are to review the advantages and drawbacks of the ambulatory management of patients scheduled for haemorrhoidal surgery and to highlight the reasons for unplanned hospital admission and suggest preventive strategies.
Methods
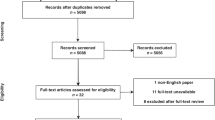
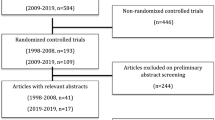
We conducted a systematic review of the literature from January 1999 to January 2013 using MEDLINE and EMBASE databases. Manuscripts were specifically analysed for failure and side effects of haemorrhoidal surgery in ambulatory settings.
Results
Fifty relevant studies (6082 patients) were retrieved from the literature review. The rate of ambulatory management failure ranged between 0 and 61 %. The main reasons for failure were urinary retention, postoperative haemorrhage and unsatisfactory pain control. Spinal anaesthesia was associated with the highest rates of urinary retention. Doppler-guided haemorrhoidal artery ligation has less frequent side effects susceptible to impair ambulatory management than haemorrhoidectomy and stapled haemorrhoidopexy. However, the fact that haemorrhoidopexy is less painful than haemorrhoidectomy may allow ambulatory management.
Conclusion
Day-case haemorrhoidal surgery can be performed whatever the surgical procedure. Postoperative pain deserves special prevention measures after haemorrhoidectomy, especially by using perineal block or infiltrations. Urinary retention is a common issue that can be responsible for failure; it requires a preventive strategy including short duration spinal anaesthesia. Doppler-guided haemorrhoidal artery ligation is easy to perform in outpatients but deserves more complete evaluation in this setting.

Similar content being viewed by others
References
The Standards Task Force (2003) The American Society of Colon and Rectal Surgeons. Practice parameters for ambulatory anorectal surgery. Dis Colon Rectum 46:573–576
Law WL, Tung HM, Chu KW, Lee FC (2003) Ambulatory stapled haemorrhoidectomy: a safe and feasible surgical technique. Hong Kong Med J 9:103–107
Guy RJ, Ng CE, Eu KW (2003) Stapled anoplasty for haemorrhoids: a comparison of ambulatory vs. in-patient procedures. Colorectal Dis 5:29–32
Lam TY, Lam SC, Kwok SP (2001) Feasibility case-controlled study of day-case haemorrhoidectomy. ANZ J Surg 71:652–654
Kosorok P, Mlakar B (2005) Haemorrhoidectomy as a one-day surgical procedure: modified Ferguson technique. Tech Coloproctol 9:57–59
Kushwaha R, Hutchings W, Davies C, Rao NG (2008) Randomized clinical trial comparing day-care open haemorrhoidectomy under local versus general anaesthesia. Br J Surg 95:555–563
Carapeti EA, Kamm MA, McDonald PJ, Chadwick SJ, Phillips RK (1999) Randomized trial of open versus closed day-case haemorrhoidectomy. Br J Surg 86:612–613
Ferrara A, Larach SW, Cebrian JP, Loprete P, Williamson PR, Arroyo M, Trevisani MF (1999) Outpatient haemorrhoidectomy in a colorectal surgical unit. Tech Coloproctol 3:75–78
Hunt L, Luck AJ, Rudkin G, Hewett PJ (1999) Day-case haemorrhoidectomy. Br J Surg 86:255–258
Labas P, Ohradka B, Cambal M, Olejnik J, Fillo J (2002) Haemorrhoidectomy in outpatient practice. Eur J Surg 168:619–620
Jayne DG, Botterill I, Ambrose NS, Brennan TG, Guillou PJ, O'Riordain DS (2002) Randomized clinical trial of Ligasure versus conventional diathermy for day-case haemorrhoidectomy. Br J Surg 89:428–432
Kairaluoma M, Nuorva K, Kellokumpu I (2003) Day-case stapled (circular) vs. diathermy hemorrhoidectomy: a randomized, controlled trial evaluating surgical and functional outcome. Dis Colon Rectum 46:93–99
Cheetham MJ, Cohen CR, Kamm MA, Phillips RK (2003) A randomized, controlled trial of diathermy hemorrhoidectomy vs. stapled hemorrhoidectomy in an intended day-care setting with longer-term follow-up. Dis Colon Rectum 46:491–497
Arroyo A, Pérez F, Miranda E, Serrano P, Candela F, Lacueva J, Hernández H, Calpena R (2004) Open versus closed day-case haemorrhoidectomy: is there any difference? Results of a prospective randomised study. Int J Colorectal Dis 19:370–373
Senagore AJ, Singer M, Abcarian H, Fleshman J, Corman M, Wexner S, Nivatvongs S, Procedure for Prolapse and Hemmorrhoids (PPH) Multicenter Study Group (2004) A prospective, randomized, controlled multicenter trial comparing stapled hemorrhoidopexy and Ferguson hemorrhoidectomy: perioperative and one-year results. Dis Colon Rectum 47:1824–1836
Miles AJ, Dunkley AJ (2007) Day case haemorrhoidectomy. Colorectal Dis 9:532–535
Haveran LA, Sturrock PR, Sun MY, McDade J, Singla S, Paterson CA, Counihan C (2007) Simple harmonic scalpel hemorrhoidectomy utilizing local anesthesia combined with intravenous sedation: a safe and rapid alternative to conventional hemorrhoidectomy. Int J Colorectal Dis 22:801–806
Muzi MG, Milito G, Nigro C, Cadeddu F, Andreoli F, Amabile D, Farinon AM (2007) Randomized clinical trial of LigaSure and conventional diathermy haemorrhoidectomy. Br J Surg 94:937–942
Stolfi VM, Sileri P, Micossi C, Carbonaro I, Venza M, Gentileschi P, Rossi P, Falchetti A, Gaspari A (2008) Treatment of in day surgery: stapled hemorrhoidopexy vs Milligan-Morgan hemorrhoidectomy. J Gastrointest Surg 12:795–801
Castellví J, Sueiras A, Espinosa J, Vallet J, Gil V, Pi F (2009) Ligasure versus diathermy hemorrhoidectomy under spinal anesthesia or pudendal block with ropivacaine: a randomized prospective clinical study with 1-year follow-up. Int J Colorectal Dis 24:1011–1018
Chan PY, Lee MP, Cheung HY, Chung CC, Li MK (2010) Unplanned admission after day-case haemorrhoidectomy: a retrospective study. Asian J Surg 33:203–207
Franceschilli L, Stolfi VM, D’Ugo S, Angelucci GP, Lazzaro S, Picone E, Gaspari A, Sileri P (2011) Radiofrequency versus conventional diathermy Milligan-Morgan hemorrhoidectomy: a prospective randomized study. Int J Colorectal Dis 26:1345–1350
Luo CH, Zang CB, Zhang GK, Liu HY (2010) Haemorrhoidectomy by vessel sealing system under local anaesthesia in an outpatient setting: preliminary experience. Colorectl Dis 12:236–240
Elmer SE, Nygren JO, Lenander CE (2013) A randomized trial of transanal hemorroidal dearterialization with anopexy compared with open hemorrhoidectomy in the treatment of hemorrhoids. Dis Colon Rectum 56:484–490
Gabrielli F, Chiarelli M, Cioffi U, Guttadauro A, De Simone M, Di Mauro P, Arriciati A (2001) Day surgery for mucosal-hemorrhoidal prolapse using a circular stapler and modified regional anesthesia. Dis Colon Rectum 44:842–844
Mlakar B, Kosorok P (2003) Complications and results after stapled haemorrhoidopexy as a day surgical procedure. Tech Coloproctol 7:164–167
Mariani P, Arrigoni G, Quartierini G, Dapri G, Leone S, Barabino M, Opocher E (2005) Local anesthesia for stapled prolapsectomy in day surgery: results of a prospective trial. Dis Colon Rectum 48:1447–1450
Ong CH, Chee Boon Foo E, Keng V (2005) Ambulatory circular stapled haemorrhoidectomy under local anaesthesia versus circular stapled haemorrhoidectomy under regional anaesthesia. ANZ J Surg 75:184–186
Gerjy R, Derwinger K, Nyström PO (2006) Perianal local block for stapled anopexy. Dis Colon Rectum 49:1914–1921
Beattie GC, McAdam TK, McIntosh SA, Loudon MA (2006) Day case stapled haemorrhoidopexy for prolapsing haemorrhoids. Colorectal Dis 8:56–61
Festen S, van Hoogstraten MJ, van Geloven AA, Gerhards MF (2009) Treatment of grade III and IV haemorrhoidal disease with PPH or THD. A randomized trial on postoperative complications and short-term results. Int J Colorectal Dis 24:1401–1405
Caviglia A, Del Grammastro A, Crocetta R, Straniero A, Giorgiano E (2009) Feasibility of stapled haemorrhoidopexy in day surgery. Eur Rev Med Pharmacol Sci 13:295–298
Cosenza UM, Conte S, Mari FS, Nigri G, Milillo A, Gasparrini M, Pancaldi A, Brescia A (2013) Stapled anopexy as a day surgery procedure: our experience over 400 cases. Surgeon 11(Suppl 1):S10–S13
Hidalgo Grau LA, Heredia Budó A, Llorca Cardeñosa S, Carbonell Roure J, Estrada Ferrer O, García Torralbo E, Suñol Sala X (2012) Day case stapled anopexy for the treatment of haemorrhoids and rectal mucosal prolapse. Colorectal Dis 14:765–768
Lim YK, Eu KW, Ho KS, Ooi BS, Tang CL (2006) PPH03 stapled hemorrhoidopexy: our experience. Tech Coloproctol 10:43–46
Perez-Vicente F, Arroyo A, Serrano P, Candela F, Sanchez A, Calpena R (2006) Prospective randomised clinical trial of single versus double purse-string stapled mucosectomy in the treatment of prolapsed haemorrhoids. Int J Colorectal Dis 21:38–43
Esser S, Khubchandani I, Rakhmanine M (2004) Stapled hemorrhoidectomy with local anesthesia can be performed safely and cost-efficiently. Dis Colon Rectum 47:1164–1169
Johnson DB, DiSiena MR, Fanelli RD (2003) Circumferential mucosectomy with stapled proctopexy is a safe, effective outpatient alternative for the treatment of symptomatic prolapsing hemorrhoids in the elderly. Surg Endosc 17:1990–1995
Brown SR, Shannugan P, Dobbs P (2006) Stapled haemorrhoidopexy for prolapsing haemorrhoids. Color Dis 8:525–530
Morinaga K, Hasuda K, Ikeda T (1995) A novel therapy for internal hemorrhoids: ligation of the hemorrhoidal artery with a newly devised instrument (Moricorn) in conjunction with a Doppler flowmeter. Am J Gastroenterol 90:610–613
Sohn N, Aronoff JS, Cohen FS, Weinstein MA (2001) Transanal hemorrhoidal dearterialization is an alternative to operative hemorrhoidectomy. Am J Surg 182:515–519
Bursics A, Morvay K, Kupcsulik P, Flautner L (2004) Comparison of early and 1-year follow-up results of conventional hemorrhoidectomy and hemorrhoid artery ligation: a randomized study. Int J Colorectal Dis 19:176–180
Felice G, Privitera A, Ellul E, Klaumann M (2005) Doppler-guided hemorrhoidal artery ligation: an alternative to hemorrhoidectomy. Dis Colon Rectum 48:2090–2093
Wallis de Vries BM, van der Beek ESJ, Wijkerslooth ME, van der Zwet WC, van der Hoeven JAB, Eeftinck Schattenkerk M, Eddes EH (2007) Treatment of grade 2 and 3 hemorrhoids with Doppler-guided hemorrhoidal artery ligation. Dig Surg 24:436–440
Faucheron JL, Gangner Y (2008) Doppler-guided hemorrhoidal artery ligation for the treatment of symptomatic hemorrhoids: early and three-year follow-up results in 100 consecutive patients. Dis Colon Rectum 51:945–949
Forrest NP, Mullerat J, Evans C, Middleton SB (2010) Doppler-guided haemorrhoidal artery ligation with recto anal repair: a new technique for the treatment of symptomatic haemorrhoids. Int J Colorectal Dis 25:1251–1256
Infantino A, Bellomo R, Dal Monte PP, Salafia C, Tagariello C, Tonizzo CA, Spazzafumo L, Romano G, Altomare DF (2010) Transanal haemorrhoidal artery echodoppler ligation and anopexy (THD) is effective for II and III degree haemorrhoids: a prospective multicentric study. Colorectal Dis 12:804–809
Faucheron JL, Poncet G, Voirin D, Badic B, Gangner Y (2011) Doppler-guided hemorrhoidal artery ligation and rectoanal repair (HAL-RAR) for the treatment of grade IV hemorrhoids: long-term results in 100 consecutive patients. Dis Colon Rectum 54:226–231
Tempel MB, Pearson EG, Page M, Pollock D, Gilmore-Lynch K, Peche W, Sklow B, Snyder M (2014) Survey of patient satisfaction after Doppler-guided transanal hemorrhoidal dearterialization performed in ambulatory settings. Tech Coloproctol 18:607–610. doi:10.1007/s10151-013-1104-x
Giamundo P, Cecchetti W, Esercizio L, Fantino G, Geraci M, Lombezzi R, Tibaldi L, Pittaluga M, Torre G, Valente M (2011) Doppler-guided hemorrhoidal laser procedure for the treatment of symptomatic hemorrhoids: experimental background and short-term clinical results of a new mini-invasive treatment. Surg Endosc 25:1369–1375
Laughlan K, Jayne DG, Jackson D, Rupprecht F, Ribaric G (2009) Stapled haemorrhoidopexy compared to Milligan-Morgan and Ferguson haemorrhoidectomy: a systematic review. Int J Colorectal Dis 24:335–344
Sajid MS, Parampalli U, Whitehouse P, Sains P, McFall MR, Baig MK (2012) A systematic review comparing transanal haemorrhoidal de-arterialisation to stapled haemorrhoidopexy in the management of haemorrhoidal disease. Tech Coloproctol 16:1–8
Burch J, Epstein D, Sari AB, Weatherly H, Jayne D, Fox D, Woolacott N (2009) Stapled haemorrhoidopexy for the treatment of haemorrhoids: a systematic review. Colorectal Dis 11:233–243
Imbelloni LE, Vieira EM, Gouveia MA, Netinho JG, Spirandelli LD, Cordeiro JA (2007) Pudendal block with bupivacaine for postoperative pain relief. Dis Colon Rectum 50:1656–1661
Vinson-Bonnet B, Coltat JC, Fingerhut A, Bonnet F (2002) Local infiltration with ropivacaine improves immediate postoperative pain control after hemorrhoidal surgery. Dis Colon Rectum 45:104–108
Joshi GP, Neugebauer EA, PROSPECT Collaboration (2010) Evidence-based management of pain after haemorrhoidectomy surgery. Br J Surg 97:1155–1168
Baldini G, Bagry H, Aprikian A, Carli F (2009) Postoperative urinary retention. Anesthesiology 110:1139–1157
Choi S, Mahon P, Awad IT (2012) Neuroaxial anesthesia and bladder dysfunction in the perioperative period: a systematic review. Can J Anaesth 59:681–703
Toyonaga T, Matsushima M, Sogawa N, Jiang SF, Matsumura N, Shimojima Y, Tanaka Y, Suzuki K, Masuda J, Tanaka M (2006) Postoperative urinary retention after surgery for benign anorectal disease: potential risk factors and strategy for prevention. In J Colorectal Dis 21:676–682
Kreutziger J, Frankenberger B, Luger TJ, Richard S, Zbinden S (2010) Urinary retention after spinal anaesthesia with hyperbaric prilocaine 2 % in an ambulatory setting. Br J Anaesth 104:582–586
Kim J, Lee DS, Jang SM, Shim MC, Jee DL (2005) The effect of pudendal block on voiding after hemorrhoidectomy. Dis Colon Rectum 48:518–523
Acknowledgments
We thank Dr. Alison Foote (Grenoble Clinical Research Centre) for the language editing.
Conflict of interest
The authors have no conflicts of interest to declare.
Source of funding
There was no specific funding for this review.
Contributions
BVB and TH conducted the literature search and analysed the retrieved articles. BVB wrote the manuscript which was reviewed and edited by all the other authors (BVB, TH, JLF, LS) who also participated in defining the methodology of the review.
Author information
Authors and Affiliations
Corresponding author
Rights and permissions
About this article
Cite this article
Vinson-Bonnet, B., Higuero, T., Faucheron, J.L. et al. Ambulatory haemorrhoidal surgery: systematic literature review and qualitative analysis. Int J Colorectal Dis 30, 437–445 (2015). https://doi.org/10.1007/s00384-014-2073-x
Accepted:
Published:
Issue Date:
DOI: https://doi.org/10.1007/s00384-014-2073-x