Abstract
Purpose
The objective of this study was to investigate the efficacy of an artificial intelligence-assisted 3D planning system (AIHIP) in total hip arthroplasty by direct anterior approach and assess the reliability of the AIHIP preoperative program in terms of both interobserver and intraobserver agreement.
Methods
A retrospective analysis was conducted on patients who underwent unilateral primary THA via direct anterior approach from June 2019 to March 2022. Participants were randomly assigned to receive either the AIHIP system (n = 220) or the 2D template (control group) (n = 220) for preoperative planning. The primary outcome aimed to evaluate the correspondence between the prosthesis selected intro-operation and the one planned preoperatively, as well as to calculate the intraclass correlation coefficient (ICC). Secondary outcomes included operation time, intraoperative blood loss, fluoroscopy times, Harris hip score (HHS), lower limb length difference (LLD), femoral offset (FO), and bilateral femoral offset difference.
Results
No significant differences were observed in gender, age, body mass index (BMI), aetiology, and American Society of Anesthesiologists (ASA) score between the two groups. Both planning methods exhibited good intraobserver agreement for component planning (ICC: 0.941–0.976). Interobserver agreement for component planning was comparable between the two methods (ICC: 0.882–0.929). In the AIHIP group, the accuracy of acetabular cup and femoral stem prosthetics planning significantly improved, with accuracies within the size range of ± 0 and ± 1 being 76.8% and 90.5% and 79.5% and 95.5%, respectively. All differences between two groups were statistically significant (p < 0.05). Patients receiving AIHIP preoperative planning experienced shorter operation times, reduced intraoperative blood loss, fewer fluoroscopy times, and lower leg length discrepancy (LLD) (p < 0.05). Moreover, they demonstrated a higher Harris hip score (HHS) at three days post-surgery (p < 0.05). However, no significant differences were found in femoral offset (FO), difference of bilateral femoral offsets, and HHS at 1 month after the operation.
Conclusion
Utilizing AIHIP for preoperative planning of direct anterior approach THA can significantly enhance the accuracy of prosthetic sizing with good reliability, decrease operation time, reduce intraoperative blood loss, and more effectively restore the length of both lower limbs. This approach has greater clinical application value.
Similar content being viewed by others
Avoid common mistakes on your manuscript.
Introduction
Total hip arthroplasty (THA) serves a crucial function in reestablishing the normal anatomical relationships and reconstructing the normal biomechanics of the hip joint [1]. Preoperative planning enables the testing of prosthesis models and simulates their placement in advance, which is vital for enhancing the efficiency, accuracy, and safety of the operation. At present, domestic preoperative planning primarily relies on two-dimensional templates [2], but their accuracy is relatively suboptimal in clinical practice due to limitations in shooting angles, magnification errors [3], and inadequate shooting postures [4]. These issues render traditional two-dimensional (2D) template-based preoperative planning less accurate [5]. The mismatch of intraoperative prostheses may result in prolonged operation time, increased intraoperative trauma, and consequently impact the surgical outcome, potentially even leading to surgical failure necessitating revision.
In recent years, artificial intelligence (AI) technology has advanced rapidly. AIHIP software (version 3.0, Longwood Valley Technology, China), which incorporates AI technology, can automatically recognize CT images, swiftly construct three-dimensional models of the hip joint, intelligently match prosthetic sizes, and aid medical staff in preoperative planning to increase the success rate of surgery [6]. AIHIP has been shown to improve the precision of preoperative templating and efficiency in total hip replacement using the posterolateral approach [6, 7]. However, the accuracy and reliability of AIHIP in different total hip replacement approaches still require further validation. This study represents the first investigation of AIHIP’s clinical applicability in direct anterior approach (DAA) total hip replacement.
The aim of this study was to compare the AIHIP software with 2D templates for preoperative prediction of total hip replacement prosthesis size and to evaluate the accuracy and clinical efficacy of the artificial intelligence 3D programming system in preoperative DAA planning prosthesis. The hypothesis is that the AIHIP system will provide more precise prosthetic size planning and better guidance for anatomical recovery.
Materials and methods
This study involved a retrospective analysis of patients who underwent THA treatment using the direct anterior approach at the Second Hospital of Fuzhou from June 2019 to March 2022. Inclusion criteria were as follows: ① Primary THA for unilateral hip disease; ② Pinnacle acetabular cup and Tri-Lock femur (DePuy Orthopaedics, USA) were utilized; ③ relevant clinical data were complete. Exclusion criteria included the following: ① patients who did not undergo surgery after preoperative planning; ② preoperative images that did not conform to preoperative planning criteria; ③ presence of active infected lesions in the hip joint or other parts of the body prior to surgery; ④ discontinuation or absence of follow-up data. Based on these criteria, 440 patients (193 men and 247 women) with a mean age of 57.16 years (range: 47 to 76 years) and a mean BMI of 23.61 kg/m2 (range: 15 to 31 kg/m2) were enrolled. The patient population included 177 cases of femoral head necrosis, 103 cases of femoral neck fracture, 80 cases of hip osteoarthritis, and 80 cases of developmental dysplasia of the hip.
The study was approved by the Medical Ethics Committee of Fuzhou No. 2 Hospital (No. 20220109), and informed consent was obtained from all participating patients.
Limb length discrepancy (LLD) was defined as the vertical distance from the tip of the lesser trochanter on both sides to the line of the inferior border of the teardrop on both sides. Femoral offset (FO) was defined as the vertical distance from the centre of rotation of the hip joint to the longitudinal axis of the femoral stem.
AIHIP preoperative planning
Collect hip CT image from 440 patients, including femoral head necrosis (ON), femoral neck fracture, dysplasia of the hip (DDH), hip osteoarthritis (OA), and other diseases of the hip. The CT scan ranged from the entire pelvis to 12 cm below the lesser trochanter of the femur with section thickness of 0.8 mm. Scan data is imported into AIHIP software in DICOM format.
Intelligent planning acetabular side
AIHIP system adopts the original CMG-NET neural network technology (Fig. 1), contributing to accurate clarification and segment of the acetabular anatomical structure by integrating Unet structure to perform first image recognition and segmentation of pelvis and femur, DenseBlock structure to smoothing fusion edge by the second segmentation, LSTM network to confirm the classification of acetabular side and femur side, and BoneDet network and PointRend technology to final confirm the defects on the acetabular side and femur side were identified by secondary image recognition. Then, based on key anatomical points, the acetabular structure is accurately reconstructed, the pelvis and both lower limbs are automatically corrected, and the anteroposterior diameter of the acetabulum is measured on the transverse position and the pelvis model, and the position of the acetabular prosthesis is intelligently placed to achieve the most suitable position and size of the acetabular component. Inclination, anteversion, and coverage of the acetabular component were planned as well (Fig. 2).
Intelligent planning of the femoral side
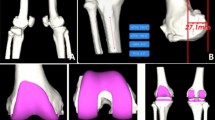
According to the calculated diameter of the femoral medullary cavity and the anteversion angle of the femur, the position of the femoral stem is planned by adopt segmentation module and prosthesis parameters of AHIP (Fig. 3), and the size of femoral head is matched on the basis of the difference between the lengths of lower limbs and the femoral offset as well as the level of femoral resection was determined by calculating the difference between contacting area according to coated line of the stem using Boolean operation. Moreover, AIPHIP software can enumerate the difference in the length of the lower limbs and the difference in the offset of the bilateral femurs after the placement of the femoral stem prosthesis according to the previous changes of the anatomical landmarks; also, it has good postoperative X-ray simulation ability to compare with preoperative X-ray (Fig. 4).
Preoperative planning
To assess intra- and interobserver reliability, digital template planning and software planning were performed by two independent investigators before surgery. The same data were template planned again by both investigators two weeks later to minimize recall bias. Both groups were conducted by two experienced joint surgeons who were not involved in the preoperative planning process, ensuring that the preoperative planning of the prosthesis did not influence the intraoperative prosthesis selection.
Observation group: Patients received preoperative pelvic CT plain scans, with the scanning range extending from the highest point of the iliac spine to 12 cm below the lesser trochanter of the femur, and a scanning layer thickness of 0.8 mm. The scanned data were imported into AIHIP software in DICOM format, and the software automatically constructed acetabular and femur structures, measured anatomical data, and matched appropriate prostheses.
Control group: Patients underwent preoperative imaging using the same radiographic machine with standard anterior–posterior pelvic radiographs. The patient was placed in a supine position, both lower extremities internally rotated, with the big toes touching each other and the patella facing forward. A uniform magnification of 1.15 was determined, and the prosthesis type was measured by the same operator using a film template.
Surgical methods
The patient was placed supine on a radiolucent operating table. The surgical incision began approximately 2–3 cm lateral and 2–3 cm distal to the anterior superior iliac spines and extended approximately 6 ~ 8 cm toward the fibular head. The surgeon separated the gap between the sartorius muscle and the tensor fascia lata muscle and entered the Heuter interval. The capsulotomy was performed to expose the femoral neck, and the femoral neck was resected according to the preoperative planning osteotomy height. After the femoral head was removed, the capsule around the acetabulum was released, and the acetabular labrum was resected. The acetabulum was concentrically reamed according to technique instruction. The appropriate type of acetabular cup and liner was inserted based on the plan and actual situation. Referring to the preoperative planning, capsule and co-joined tendon around proximal femur were entirely released in order to lift proximal femur. Then, femoral canal was broached, and the stem antevision was ascertained in order to implant the real femoral prosthesis. The hip stability was checked to require the maximum of range of motion. Finally, the capsule was sutured as well as possible.
Result indicators
The following indicators were compared between the two groups: prosthesis matching rate; operation time; intraoperative blood loss; fluoroscopy times; Harris hip score (HHS); bilateral lower limb length difference (LLD); femoral offset (FO); and the difference in femoral offset between the two sides.
Statistical methods
SPSS 23.0 statistical software was used for data analysis. Measurement data were expressed as mean ± standard deviation, and an independent sample t-test was used for comparison between groups. The χ2 test and rank sum test were used for comparing count data between groups. Due to non-normal distribution, fluoroscopy times were compared using the Mann–Whitney U test and expressed as median and interquartile range (IQR). Intraclass correlation coefficients (ICCs) were used to assess the reliability of intraobserver and interobserver repeated measures. ICC values less than 0.5 represented weak agreement, between 0.5 and 0.75 represented moderate agreement, between 0.75 and 0.9 represented strong agreement, and greater than 0.9 represented very strong agreement [8]. A p-value less than 0.05 was considered statistically significant.
Results
Patient characteristics
This study included a total of 440 patients. The observation group consisted of 220 patients with a mean age of 56.6 ± 14.5 years (range 47 to 76 years), comprising 92 males and 128 females, 91 cases of femoral head necrosis, 50 cases of femoral neck fracture, 44 cases of osteoarthritis, and 35 cases of hip dysplasia. The control group consisted of 220 patients with a mean age of 57.4 ± 15.2 years (range 50 to 75 years), including 101 males and 119 females, 86 cases of femoral head necrosis, 53 cases of femoral neck fracture, 36 cases of osteoarthritis, and 45 cases of hip dysplasia. No statistically significant differences were found between the two groups in terms of general characteristics or aetiology (Table 1).
Comparison of surgical results
Prosthesis matching degree: In the observation group, 169 cases demonstrated complete matching between the postoperative acetabular cup size and preoperative planning, 30 cases showed general matching (± 1 size), and 21 cases exhibited mismatch (± 2 size and above). The conformity rates within the size range of ± 0 and ± 1 were 76.8% and 90.5%, respectively. For the femoral stem type matching, 175 cases were complete matches, 35 cases were general matches (± 1 size), and 10 cases were mismatches (± 2 size and above). The coincidence rate within the size range of ± 0 and ± 1 was 79.5% and 95.5%, respectively. In the control group, 89 cases exhibited complete matching between postoperative acetabular cup size and preoperative planning, 82 cases showed general matching (± 1 size), and 49 cases demonstrated mismatch (± 2 size and above). The conformity rates within the size range of ± 0 and ± 1 were 40.5% and 77.7%, respectively. For the femoral stem type matching, 101 cases were complete matches, 77 cases were general matches (± 1 size), and 42 cases were mismatches (± 2 size and above). The coincidence rate within the size range of ± 0 and ± 1 was 45.9% and 80.9%, respectively. The difference between the groups was statistically significant (p < 0.05) (Figs. 5 and 6, Table 2). The interobserver ICC for the acetabular template in the AIHIP group was 0.887 (95% CI, 0.786–0.942), and the intraobserver ICC was 0.962 (95% CI, 0.927–0.981). For the femoral template, the interobserver ICC was 0.929 (95% CI). In the 2D group, the interobserver ICC was 0.914 (95% CI, 0.836–0.956), and the intraobserver ICC was 0.948 (95% CI). The interobserver ICC for the femoral template was 0.882 (95% CI, 0.778–0.939), and the intraobserver ICC was 0.941 (95% CI, 0.885–0.970) (Table 3).
General surgical outcomes: The observation group experienced significantly lower intraoperative blood loss (229.81 ± 97.69 ml) compared to the control group (267.17 ± 113.88 ml) (p < 0.05). The number of intraoperative fluoroscopies was 0 (0,0) in the observation group and 1 (1,2) in the control group, indicating that the observation group had fewer intraoperative fluoroscopies than the control group (p < 0.001). The operative time for the observation group (43.22 ± 12.65 min) was shorter than that of the control group (68.36 ± 14.45 min) (Table 4).
Imaging and hip function scores: The LLD in the observation group was 0.71 ± 0.54 mm, while the LLD in the control group was 1.14 ± 0.59 mm. The accuracy of restoring leg length in both lower limbs was higher in the observation group (p < 0.001). The FO for the observation group was 36.79 ± 7.94 mm, and the FO for the control group was 37.92 ± 6.77 mm, with no statistically significant difference between the two groups. The postoperative offset difference was 3.73 ± 0.65 mm in the observation group and 3.89 ± 0.68 mm in the control group, and the difference was not statistically significant. The HHS score was higher in the observation group (78.66 ± 3.32) than in the control group (74.01 ± 3.42) at three days postoperatively (p < 0.001). However, at one month postoperatively, there was no difference between the HHS score in the observation group (85.51 ± 3.69) and the control group (84.88 ± 2.68) (Table 4).
Discussion
This study compared the outcomes of AIHIP and 2D templates in patients undergoing unilateral DAA-THA, revealing several findings: (1) AIHIP was significantly more accurate in planning femoral and acetabular side prostheses compared to 2D templates. (2) Patients in the AIHIP group had shorter operative times, less intraoperative bleeding, and fewer intraoperative fluoroscopies, and AIHIP was more successful in reducing postoperative LLD compared to 2D templates. (3) Patients in the AIHIP group had higher HSS scores at three days postoperatively compared to 2D templates.
Previous studies have identified the difficulty of femoral exposure as a major challenge in the direct anterior approach to THA. The pursuit of adequate femoral exposure and excessive medullary reaming contributes to the occurrence of intraoperative fractures [9]. Some studies [10, 11] showed that most femoral complications were fractures of the calcar and the greater trochanter. Jewett et al. [12] described the prospect of using a fracture table to reduce the risk of femoral fracture in direct total approach hip replacement. The advantage of the DAA traction table, which can fix patients' lower limbs, reduces the incidence of complications of unequal lower limb lengths [13]. However, the current literature has raised much controversy about the time efficiency of intraoperative traction table [14, 15]. The difficulty in femoral exposure poses a threat to the undersized or malalignmental femoral stem implantation by the direct anterior approach (DAA), resulting in the risk of loosening and subsidence of the femoral stem [16]. The risk of femoral subsidence after THA has been reported to be 4–56.7% [17,18,19,20]. The AIHIP system can accurately segment and reconstruct the hip joint structure based on CT data through neural network technology and use intelligent algorithms to match the femoral stem prosthesis model, selecting the appropriate alignment and antevision. Chen et al. [21] reported that using AIHIP to predict the accuracy of the femoral stem is over 90%. It is believed that the AIHIP system can adjust the morphology of the femoral stalk in the medullary cavity and the degree of filling through various angles, which largely compensates for the shortcomings of the 2D template, which is limited in measuring the angle and cannot accurately measure the diameter of the medullary cavity, ultimately improving the prosthesis matching rate.
The direct anterior approach (DAA) accesses the hip socket through the muscle intervals, which preserves the integrity of soft tissue and muscles. However, it is challenging to adequately lift proximal femur and broach femoral canal and to avoid femur fracture stem malalignment compared to the posterior approach, leading to the risk of excessive anteversion of the acetabular cup when the surgeon employs DAA in the early stage [22]. The risk of dislocation after DAA has been reported to range from 0.5 to 3% [23,24,25,26]. Intraoperative fluoroscopy-guided acetabular component placement was deemed feasible [27, 28], as the use of fluoroscopy guidance offered favorable acetabular component positioning in an anterior approach THA, as described by Gosthe [29] et al. In this study, the number of intraoperative fluoroscopies was reduced in the AIHIP system group compared to the 2D template group, which could not accurately measure the anterior–posterior acetabular diameter [4]. The AIHIP system can adjust the anteversion and abduction angles of the cup based on the 3D model and calculate the acetabular cup coverage simultaneously, which has significant benefits in comparison with the 2D template in accurately predicting the size and anteversion of acetabular prosthesis, ultimately reducing the number of intraoperative fluoroscopic views.
This study demonstrated shorter operative time and less intraoperative bleeding in the AIHIP group compared to the 2D template group. The reduction in operative time may be attributed to decreased intraoperative fluoroscopy and faster prosthesis placement, while the decrease in operative time may contribute to reduce intraoperative bleeding. Intraoperative fluoroscopy can aid in positioning the prosthesis and evaluating its placement, but the C-arm machine takes time to position and fluoroscope, which can result in longer operative times [30]. AIHIP can accurately construct the anatomy of the hip joint and plan the size of prosthesis to assist the surgeon in planning the position and angle of the prosthesis preoperatively, thereby reducing the time for intraoperative prosthesis adjustment and the number of fluoroscopic views and ultimately shortening the operation time. Xia et al. [6] utilized AIHIP to assist in hip replacement in patients with Crowe type IV DDH and demonstrated that AIHIP was effective in assisting the surgeon in filing the acetabulum and selecting the type of prosthesis, which improved the efficiency of the procedure. These findings align with the results of this study. On the other hand, AIHIP improves surgical efficiency and reduces surgical time, which helps to reduce surgical trauma and promote early recovery and functional exercise, which may be the reason for the higher early HSS score of patients in AIHIP group.
Postoperative leg length difference (LLD) is a crucial indicator for evaluating the success of total hip arthroplasty (THA) surgery [31, 32]. Previous literature has reported that patients can perceive a leg length difference when it exceeds 5 mm [33]. LLD is considered the leading cause of postoperative pain, gait disturbance, and aseptic loosening [34,35,36], and in severe cases, it can even lead to prosthesis revision [37, 38]. It has been reported that there are differences in the morphology of the proximal femur across different regions and age groups, making it challenging for a common femoral prosthesis model to adapt to various hip joints [35]. Boese et al. [39] observed that only 25% of the implants were less than 2 mm away from the medial interface of the femur, and an excessive distance could result in a loosened prosthesis. Some studies have indicated that the morphological variation of the proximal femur [35] and the lack of surgical experience [40] are central factors contributing to postoperative LLD. The literature reported different rates of LLD after DAA, ranging from 8 to 40.4% [34, 41, 42]. The AIHIP system can calculate the bone marrow cavity diameter, leg length difference, and plan the osteotomy height through artificial intelligence (AI) based on high-precision reconstruction of the femoral structure, thereby reducing the postoperative leg length difference. The results of this study showed that the AIHIP group exhibited a reduction in postoperative leg length difference compared to the 2D template group, and the AIHIP system can restore the length balance of both lower extremities to a certain extent.
Femoral offset plays a vital role in the recovery of hip abductor strength after surgery [43,44,45]. Wu et al. [4] reported that the use of AIHIP positively influenced the postoperative recovery of offset; however, no significant difference was found in this study, which may be explained by different surgical approaches. Further research is urgently needed to confirm the recovery of femoral offset by AIHIP.
This study has some limitations. Firstly, the AIHIP system-assisted planning requires a CT scan, which increases the radiation dose to the patient. Secondly, this study only compared the AIHIP system with 2D templates for preoperative planning, lacking a comparison with 3D planning software. Thirdly, there is a lack of long-term follow-up data on hip joint activity and prosthesis revision.
Conclusion
The utilization of AIHIP-guided direct anterior approach THA demonstrates higher accuracy and reliability in predicting acetabular cup and femoral stem dimensions, as well as prosthesis implantation location, compared to the traditional 2D planning method. Additionally, it shortens operative time, reduces intraoperative bleeding, and better restores bilateral lower limb length, thus exhibiting greater clinical application value.
Data availability
The datasets used during the current study are available from the corresponding author on reasonable request.
References
Houcke JV, Khanduja V, Pattyn C, Audenaert E (2017) The history of biomechanics in total hip arthroplasty. Indian J Orthop 51:359–367. https://doi.org/10.4103/ortho.IJOrtho_280_17
Smith JBV, Bishi H, Wang C, Asopa V, Field RE, Sochart DH (2021) The accuracy and reliability of preoperative digital 2D templating in prosthesis size prediction in uncemented versus cemented total hip arthroplasty: a systematic review and meta-analysis. EFORT Open Rev 6:1020–1039. https://doi.org/10.1302/2058-5241.6.210048
Olmedo-Garcia NI, Martínez Vergara JL, ApariciMiralles TL, Sánchez Andrés JV, Mesado Vives A, Cruz Renovell E, Granell Beltran V (2018) Assessment of magnification of digital radiographs in total HIP arthroplasty. J Orthop 15:931–934. https://doi.org/10.1016/j.jor.2018.08.024
Wu D, Liu X, Zhang Y, Chen J, Tang P, Chai W (2020) Research and application of artificial intelligence based three-dimensional preoperative planning system for total hip arthroplasty. Zhongguo Xiu Fu Chong Jian Wai Ke Za Zhi 34:1077–1084. https://doi.org/10.7507/1002-1892.202005007
Miashiro EH, Fujiki EN, Yamaguchi EN, Chikude T, Rodrigues LH, Fontes GM, Rosa FB (2014) Preoperative planning of primary total hip arthroplasty using conventional radiographs. Rev Bras Ortop 49:140–148. https://doi.org/10.1016/j.rboe.2014.03.019
Xia T, Liu X, Liu J, Zhang C, Zhang Z, Fan Y, Zhang C, Zhang Y, Shen J (2021) Artificial intelligence assisted total hip arthroplasty for patients with Crowe type IV developmental dysplasia of the hip. Zhongguo Xiu Fu Chong Jian Wai Ke Za Zhi 35:1265–1272. https://doi.org/10.7507/1002-1892.202106103
Huo J, Huang G, Han D et al (2021) Value of 3D preoperative planning for primary total hip arthroplasty based on artificial intelligence technology. J Orthop Surg Res 16(1):156. https://doi.org/10.1186/s13018-021-02294-9
Koo TK, Li MY (2016) A guideline of selecting and reporting intraclass correlation coefficients for reliability research. J Chiropr Med 15(2):155–163. https://doi.org/10.1016/j.jcm.2016.02.012
Yang Z, Feng S, Guo KJ, Zha GC (2021) Patient-reported results of simultaneous direct anterior approach and posterolateral approach total hip arthroplasties performed in the same patients. J Orthop Traumatol 22(1):46. https://doi.org/10.1186/s10195-021-00611-w
Barnett SL, Peters DJ, Hamilton WG, Ziran NM, Gorab RS, Matta JM (2016) Is the anterior approach safe? Early complication rate associated with 5090 consecutive primary total hip arthroplasty procedures performed using the anterior approach. J Arthroplasty 31:2291–2294. https://doi.org/10.1016/j.arth.2015.07.008
Berend KR, Mirza AJ, Morris MJ, Lombardi AV Jr (2016) Risk of periprosthetic fractures with direct anterior primary total hip arthroplasty. J Arthroplasty 31:2295–2298. https://doi.org/10.1016/j.arth.2016.03.007
Jewett BA, Collis DK (2011) High complication rate with anterior total hip arthroplasties on a fracture table. Clin Orthop Relat Res 469:503–507. https://doi.org/10.1007/s11999-010-1568-1
Wernly D, Wegrzyn J, Lallemand G, Mahlouly J, Tissot C, Antoniadis A (2021) Total hip arthroplasty through the direct anterior approach with and without the use of a traction table: a matched-control, retrospective, single-surgeon study. J Orthop Surg Res 16:45. https://doi.org/10.1186/s13018-020-02184-6
Moslemi A, Kierszbaum E, Descamps J, Sigonney F, Biau D, Anract P, Hardy A (2021) Does using the direct anterior approach with a standard table for total hip arthroplasty reduce leg length discrepancies? Comparative study of traction table versus standard table. Orthop Traumatol Surg Res 107:102752. https://doi.org/10.1016/j.otsr.2020.102752
Sarraj M, Chen A, Ekhtiari S, Rubinger L (2020) Traction table versus standard table total hip arthroplasty through the direct anterior approach: a systematic review. Hip Int 30:662–672. https://doi.org/10.1177/1120700019900987
Angerame MR, Fehring TK, Masonis JL, Mason JB, Odum SM, Springer BD (2018) Early failure of primary total hip arthroplasty: is surgical approach a risk factor? J Arthroplasty 33:1780–1785. https://doi.org/10.1016/j.arth.2018.01.014
Suksathien Y, Chuvanichanon P, Tippimanchai T, Sueajui J (2022) Insufficient lateral stem contact is an influencing factor for significant subsidence in cementless short stem total hip arthroplasty. World J Orthop 13:444–453. https://doi.org/10.5312/wjo.v13.i5.444
Froimson MI, Garino J, Machenaud A, Vidalain JP (2007) Minimum 10-year results of a tapered, titanium, hydroxyapatite-coated hip stem: an independent review. J Arthroplasty 22:1–7. https://doi.org/10.1016/j.arth.2006.03.003
Kawai T, Goto K, Kuroda Y, Okuzu Y, Matsuda S (2022) High subsidence rate after primary total hip arthroplasty using a Zweymüller-type noncemented implant with a matte surface. J Am Acad Orthop Surg Glob Res Rev 6(6):e21.00126. https://doi.org/10.5435/JAAOSGlobal-D-21-00126
Ikemura S, Motomura G, Hamai S, Fujii M, Kawahara S, Sato T, Hara D, Shiomoto K, Nakashima Y (2022) Tapered wedge stems decrease early postoperative subsidence following cementless total hip arthroplasty in Dorr type C femurs compared to fit-and-fill stems. J Orthop Surg Res 17:223. https://doi.org/10.1186/s13018-022-03111-7
Chen X, Liu X, Wang Y, Ma R, Zhu S, Li S, Li S, Dong X, Li H, Wang G, Wu Y, Zhang Y, Qiu G, Qian W (2022) Development and validation of an artificial intelligence preoperative planning system for total hip arthroplasty. Front Med (Lausanne) 9:841202. https://doi.org/10.3389/fmed.2022.841202
Kobayashi H, Homma Y, Baba T, Ochi H, Matsumoto M, Yuasa T, Kaneko K (2016) Surgeons changing the approach for total hip arthroplasty from posterior to direct anterior with fluoroscopy should consider potential excessive cup anteversion and flexion implantation of the stem in their early experience. Int Orthop 40:1813–1819. https://doi.org/10.1007/s00264-015-3059-1
Tripuraneni KR, Munson NR, Archibeck MJ, Carothers JT (2016) Acetabular abduction and dislocations in direct anterior vs posterior total hip arthroplasty: a retrospective, matched cohort study. J Arthroplasty 31:2299–2302. https://doi.org/10.1016/j.arth.2016.03.008
Tay K, Tang A, Fary C, Patten S, Steele R, de Steiger R (2019) The effect of surgical approach on early complications of total hip arthroplasty. Arthroplasty 1:5. https://doi.org/10.1186/s42836-019-0008-2
Sheth D, Cafri G, Inacio MC, Paxton EW, Namba RS (2015) Anterior and anterolateral approaches for THA are associated with lower dislocation risk without higher revision risk. Clin Orthop Relat Res 473:3401–3408. https://doi.org/10.1007/s11999-015-4230-0
Wang Z, Hou JZ, Wu CH, Zhou YJ, Gu XM, Wang HH, Feng W, Cheng YX, Sheng X, Bao HW (2018) A systematic review and meta-analysis of direct anterior approach versus posterior approach in total hip arthroplasty. J Orthop Surg Res 13:229. https://doi.org/10.1186/s13018-018-0929-4
Beamer BS, Morgan JH, Barr C, Weaver MJ, Vrahas MS (2014) Does fluoroscopy improve acetabular component placement in total hip arthroplasty? Clin Orthop Relat Res 472:3953–3962. https://doi.org/10.1007/s11999-014-3944-8
Rathod PA, Bhalla S, Deshmukh AJ, Rodriguez JA (2014) Does fluoroscopy with anterior hip arthroplasty decrease acetabular cup variability compared with a nonguided posterior approach? Clin Orthop Relat Res 472:1877–1885. https://doi.org/10.1007/s11999-014-3512-2
Gosthe RG, Suarez JC, McNamara CA, Calvo C, Patel PD (2017) Fluoroscopically guided acetabular component positioning: does it reduce the risk of malpositioning in obese patients? J Arthroplasty 32:3052–3055. https://doi.org/10.1016/j.arth.2017.04.045
Rykov K, Reininga IHF, Sietsma MS, Knobben BAS, Ten Have BLEF (2017) Posterolateral vs direct anterior approach in total hip arthroplasty (POLADA trial): a randomized controlled trial to assess differences in serum markers. J Arthroplasty 32(12):3652-3658.e1. https://doi.org/10.1016/j.arth.2017.07.008
Wylde V, Whitehouse SL, Taylor AH, Pattison GT, Bannister GC, Blom AW (2009) Prevalence and functional impact of patient-perceived leg length discrepancy after hip replacement. Int Orthop 33:905–909. https://doi.org/10.1007/s00264-008-0563-6
Zhang Y, He W, Cheng T, Zhang X (2015) Total hip arthroplasty: leg length discrepancy affects functional outcomes and patient’s gait. Cell Biochem Biophys 72:215–219. https://doi.org/10.1007/s12013-014-0440-4
Sykes A, Hill J, Orr J, Humphreys P, Rooney A, Morrow E, Beverland D (2015) Patients’ perception of leg length discrepancy post total hip arthroplasty. Hip Int 25:452–456. https://doi.org/10.5301/hipint.5000276
Dunn H, Rohlfing G, Kollmorgen R (2020) A comparison of leg length discrepancy between direct anterior and anterolateral approaches in total hip arthroplasty. Arthroplasty 2:30. https://doi.org/10.1186/s42836-020-00051-7
Mavčič B, Antolič V (2021) Cementless femoral stem fixation and leg-length discrepancy after total hip arthroplasty in different proximal femoral morphological types. Int Orthop 45:891–896. https://doi.org/10.1007/s00264-020-04671-1
Khamis S, Carmeli E (2017) Relationship and significance of gait deviations associated with limb length discrepancy: a systematic review. Gait Posture 57:115–123. https://doi.org/10.1016/j.gaitpost.2017.05.028
Duethman NC, Statz JM, Trousdale RT, Taunton MJ (2020) Reasons for failure of primary total hip arthroplasty performed through a direct anterior approach. Orthopedics 43:239–244. https://doi.org/10.3928/01477447-20200521-01
Meneghini RM, Elston AS, Chen AF, Kheir MM, Fehring TK, Springer BD (2017) Direct anterior approach: risk factor for early femoral failure of cementless total hip arthroplasty: a multicenter study. J Bone Joint Surg Am 99:99–105. https://doi.org/10.2106/JBJS.16.00060
Boese CK, Dargel J, Jostmeier J, Eysel P, Frink M, Lechler P (2016) Agreement between proximal femoral geometry and component design in total hip arthroplasty: implications for implant choice. J Arthroplasty 31:1842–1848. https://doi.org/10.1016/j.arth.2016.02.015
Kishimoto Y, Suda H, Kishi T, Takahashi T (2020) A low-volume surgeon is an independent risk factor for leg length discrepancy after primary total hip arthroplasty: a case-control study. Int Orthop 44:445–451. https://doi.org/10.1007/s00264-019-04435-6
Lecoanet P, Vargas M, Pallaro J, Thelen T, Ribes C, Fabre T (2018) Leg length discrepancy after total hip arthroplasty: can leg length be satisfactorily controlled via anterior approach without a traction table? Evaluation in 56 patients with EOS 3D. Orthop Traumatol Surg Res 104:1143–1148. https://doi.org/10.1016/j.otsr.2018.06.020
Austin DC, Dempsey BE, Kunkel ST, Torchia MT, Jevsevar DS (2018) A comparison of radiographic leg-length and offset discrepancies between 2 intraoperative measurement techniques in anterior total hip arthroplasty. Arthroplast Today 5:181–186. https://doi.org/10.1016/j.artd.2018.09.005
Mahmood SS, Mukka SS, Crnalic S, Wretenberg P, Sayed-Noor AS (2016) Association between changes in global femoral offset after total hip arthroplasty and function, quality of life, and abductor muscle strength. A prospective cohort study of 222 patients. Acta Orthop 87:36–41. https://doi.org/10.3109/17453674.2015.1091955
Tezuka T, Inaba Y, Kobayashi N, Ike H, Kubota S, Kawamura M, Saito T (2015) Effects of hip joint center location and femoral offset on abductor muscle strength after total hip arthroplasty. Mod Rheumatol 25:630–636. https://doi.org/10.3109/14397595.2014.988863
Lopes BM, Spinelli LF, Galia CR, Schwartsmann CR, Silva MF (2022) Influence of femoral offset on functional capacity of patients with total hip arthroplasty. Acta Ortop Bras 30(3):e243763. https://doi.org/10.1590/1413-785220223003e243763
Acknowledgements
The authors express their gratitude to the Fujian Provincial Clinical Medical Research Center for First Aid and Rehabilitation in Orthopaedic Trauma for supporting this work. Appreciation is also extended to the colleagues in the radiology department for their assistance in this field.
Author information
Authors and Affiliations
Contributions
EF and YZ is responsible for the design. WY and TG wrote the paper. WY was responsible for statistical processing. FL provides technical support. YW and KS participated in the formation of viewpoints. BL, DL, and XL participated in the collection of clinical data.
Corresponding authors
Ethics declarations
Ethics approval
This study was performed in line with the principles of the Declaration of Helsinki. This study was approved by the Ethics Committee of Fuzhou Second Hospital Affiliated to Xiamen University (No. 20220109).
Consent to participate
Informed consent was obtained from all individual participants included in the study.
Consent for publication
The authors affirm that human research participants provided informed consent for publication of the images in Figs. 1, 2, 3, 4, 5, and 6.
Competing interests
The authors declare no competing interests.
Additional information
Publisher's Note
Springer Nature remains neutral with regard to jurisdictional claims in published maps and institutional affiliations.
Rights and permissions
Open Access This article is licensed under a Creative Commons Attribution 4.0 International License, which permits use, sharing, adaptation, distribution and reproduction in any medium or format, as long as you give appropriate credit to the original author(s) and the source, provide a link to the Creative Commons licence, and indicate if changes were made. The images or other third party material in this article are included in the article's Creative Commons licence, unless indicated otherwise in a credit line to the material. If material is not included in the article's Creative Commons licence and your intended use is not permitted by statutory regulation or exceeds the permitted use, you will need to obtain permission directly from the copyright holder. To view a copy of this licence, visit http://creativecommons.org/licenses/by/4.0/.
About this article
Cite this article
Yang, W., Gao, T., Liu, X. et al. Clinical application of artificial intelligence-assisted three-dimensional planning in direct anterior approach hip arthroplasty. International Orthopaedics (SICOT) 48, 773–783 (2024). https://doi.org/10.1007/s00264-023-06029-9
Received:
Accepted:
Published:
Issue Date:
DOI: https://doi.org/10.1007/s00264-023-06029-9