Abstract
Introduction
The efficacy of nebulized sodium nitrite (AIR001) has been demonstrated in animal models of pulmonary arterial hypertension (PAH), but it was not known if inhaled nitrite would be well tolerated in human subjects at exposure levels associated with efficacy in these models.
Methods
Inhaled nebulized sodium nitrite was assessed in three independent studies in a total of 82 healthy male and female subjects. Study objectives included determination of the maximum tolerated dose (MTD) and dose-limiting toxicity (DLT) under normal and mildly hypoxic conditions, and following co-administration with steady-state sildenafil, assessment of nitrite pharmacokinetics, and evaluation of the fraction exhaled nitric oxide (FENO) and concentrations of iron-nitrosyl hemoglobin (Hb(Fe)-NO) and S-nitrosothiols (R-SNO) as biomarkers of local and systemic NO exposure, respectively.
Results
Nebulized sodium nitrite was well tolerated following 6 days of every 8 h administration up to 90 mg, producing significant increases in circulating Hb(Fe)-NO, R-SNO, and FENO. Pulmonary absorption of nitrite was rapid and complete, and plasma exposure dose was proportional through the MTD dosage level of 90 mg, without accumulation following repeated inhalation. At higher dosage levels, DLTs were orthostasis (observed at 120 mg) and hypotension with tachycardia (at 176 mg), but venous methemoglobin did not exceed 3.0 % at any time in any subject. Neither the tolerability nor pharmacokinetics of nitrite was impacted by conditions of mild hypoxia, or co-administration with sildenafil, supporting the safe use of inhaled nitrite in the clinical setting of PAH.
Conclusion
On the basis of these results, nebulized sodium nitrite (AIR001) has been advanced into randomized trials in PAH patients.
Similar content being viewed by others
Avoid common mistakes on your manuscript.
Nebulized sodium nitrite (AIR001) produced dose-proportional plasma exposure with no evidence of systemic or pulmonary accumulation following 6 days of inhalation in healthy male and female subjects |
Three times-daily inhalation of sodium nitrite for 6 days was well tolerated in healthy subjects at dosage levels producing increases in local and systemic markers of nitric oxide exposure associated with efficacy in animal models of pulmonary arterial hypertension |
Neither the tolerability nor the pharmacokinetics of nitrite in healthy subjects was impacted by mild hypoxia or co-administration with steady-state sildenafil, supporting the safe use of sodium nitrite in the clinical setting of pulmonary arterial hypertension |
1 Introduction
Pulmonary arterial hypertension (PAH) is a progressive disease of uncertain etiology characterized by increased vascular resistance in the distal pulmonary arterioles. Untreated PAH is associated with vascular proliferation and remodeling, hypertrophy, and eventual failure of the right ventricle and a median untreated life expectancy of less than 3 years. Approved therapeutic options for PAH are currently limited to endothelin receptor antagonists, phosphodiesterase type 5 inhibitors, and prostanoids, but these treatment options suffer from significant side effects, burdensome dosing regimens, and/or limited efficacy [1].
Although the vasodilatatory properties of nitric oxide (NO) have long been appreciated [2, 3] it has only more recently become apparent that the inorganic anion nitrite (NO2 −), which was previously considered an inactive NO metabolite, can be reduced to bioactive NO by numerous enzyme systems under either moderate to low oxygen tension or reduced pH [4]. An important nitrite reductase in blood is deoxyhemoglobin [5, 6], but many cellular enzymes can also catalyze this reduction under hypoxic conditions, such as myoglobin [7–9], xanthine oxidase [10–12], aldehyde oxidase [13, 14], cytochrome c oxidase [15], and endothelial NO synthase [16, 17], all of which are expressed in human lung tissue and/or vascular smooth muscle [18–21].
In addition to its direct activity on tissues, liberated NO can form complexes with hemoproteins, such as iron-nitrosyl hemoglobin (Hb(Fe)-NO) [22], or following oxidation can react with protein thiols to form S-nitrosothiol species (R-SNO) [6, 23]. Thus, the circulating concentrations of these species can be considered biomarkers of systemic NO exposure, and increases in concentrations of both Hb(Fe)-NO and R-SNO have been measured in the human circulation following nitrite infusion [6, 24–26].
The ability of nitrite to mediate local vasodilatation in a hypoxic- and pH-dependent manner suggests potential therapeutic utility in PAH. Indeed, in a mouse model of hypoxia-induced PAH, once-weekly nitrite inhalation was found to completely prevent increases in right ventricular pressure (RVP) and right ventricle mass (RVM) in hypoxic animals, while exposure to nebulized sodium nitrite three times per week in rats was able to significantly reduce monocrotaline-induced right ventricle hypertrophy and hyperplasia of the small pulmonary arteries [12]. In an ovine model of pulmonary hypertension induced by hypoxia, pulmonary artery pressure (PAP) was significantly reduced by inhalation of both NO gas and nebulized sodium nitrite, but the effects of NO gas disappeared immediately after cessation of exposure, while decreases in PAP following inhalation of nitrite were maintained throughout the experimental hypoxia period (out to 60 min post end of inhalation) [27]. Finally, a study in healthy human subjects reported that intravenous infusion of low doses of sodium nitrite significantly reduced the PAP measured by echocardiography under conditions of temporarily induced hypoxia [28].
Nitrite has been extensively studied in human subjects following parenteral administration, and a number of published studies have assessed the pharmacokinetics and pharmacodynamics of sodium nitrite in humans following intravenous [25, 28–30] or intra-arterial [6, 24, 26, 31, 32] administration. Parenteral administration routes, however, provide minimal opportunity for patient self-administration in the setting of this chronic and progressive disease. Here, we report the first assessment of the pharmacokinetics, pharmacodynamics, safety, and tolerability of nebulized sodium nitrite (AIR001) following inhalation in human subjects.
These phase I studies were designed with a number of objectives: (1) to determine the maximum tolerated dose (MTD) and dose-limiting toxicities (DLT) of nebulized sodium nitrite following a single dose, or 6 days of every 8 h administration in healthy male and female subjects; (2) to determine the pharmacokinetic profiles in plasma of nitrite and nitrate metabolite following single and repeated inhalation; (3) to assess the impact of either mild hypoxia (SaO2 of 75–80 %) or co-administration with steady-state sildenafil on the tolerability and pharmacokinetics of inhaled nitrite, and (4) to assess the response of fraction exhaled nitric oxide (FeNO) and circulating Hb(Fe)-NO and R-SNO (pharmacodynamic markers of local and systemic NO exposure, respectively), following nitrite inhalation. The results reported here have facilitated the design and conduct of ongoing randomized trials of nebulized sodium nitrite (AIR001) in PAH patients.
2 Methods
2.1 Study Design and Subjects
The pharmacokinetics, pharmacodynamics, and tolerability of nebulized sodium nitrite (AIR001) following single and repeated inhalation were assessed in three individual studies, in which a total of 82 healthy male and female subjects were treated.
AIR001-CS01 was an open-label, phase 1a, single ascending dose study in 33 healthy male and female subjects. Dosage levels were sequentially escalated in cohorts of three subjects each at roughly half-log intervals from 0.04 to 176 mg/subject. Pharmacodynamic endpoints included assessment of the FENO at various timepoints before and after nitrite inhalation.
AIR001-CS02 was an open-label, phase Ib, single ascending dose study in 12 healthy male and female subjects under conditions of mild hypoxia induced by exposure to a low oxygen atmosphere (FiO2 of 10.5–12.5 %, titrated to a SaO2 of 75–80 %) from 1 h prior to 2 h post sodium nitrite administration. As discussed above, results in humans, animals, and in vitro systems suggest that the fate and biological utilization of nitrite are altered under conditions of low oxygen tension and/or low pH. Study AIR001-CS02 was therefore designed to assess the tolerability and pharmacokinetics of inhaled sodium nitrite in human subjects under mild hypoxia, which may approximate conditions expected in patients with advanced PAH. Dosage levels were sequentially escalated in cohorts of four subjects each from 5 to 113 mg—with the high dose representing about 90 % of the normoxic MTD determined in study AIR001-CS01. The hypoxia protocols used in this study were optimized as part of a “hypoxia training study” (study AIR001-CS03), which assessed pulmonary hemodynamics in nine healthy volunteers during exposure to a range of hypoxic conditions, although no sodium nitrite was administered to any subject in this study. Results of study AIR001-CS03 are not presented here.
AIR001-CS04 was a blinded, placebo-controlled, multiple ascending dose study, and results from two study phases are presented here: Part A investigated the tolerability, pharmacokinetics, and pharmacodynamics of multiple ascending doses of three times-daily sodium nitrite (every 8 h) for 6 days in 28 healthy male and female subjects randomized eight per cohort (six treatment and two placebo) to dosage levels of 15, 45, and 90 mg, and four subjects (three treatment and one placebo) to a dose of 120 mg. In addition to sample collection for determination of nitrite, nitrate, Hb(Fe)-NO, and R-SNO species, Part A also included assessment of the FENO at various timepoints before and after nitrite inhalation. Part B investigated the tolerability and pharmacokinetics of four times-daily (every 6 h) multiple ascending doses of 22.5, 45, and 90 mg nebulized nitrite in nine subjects co-administered with steady-state oral sildenafil (4 days pre-treatment at 20 mg every 8 h prior to first nitrite dosing). In addition, plasma concentrations of sildenafil and its primary N-desmethyl metabolite were assessed daily at trough prior to and during sodium nitrite administration to assess any impact of nitrite on sildenafil exposure.
These studies are hereafter referred to as CS01, CS02, and CS04. Studies CS01 and CS02 were both conducted at a single center (DaVita Clinical Research; Minneapolis, MN, USA), and were completed in September and December of 2008, respectively, while study CS04 was conducted at PAREXEL International (Baltimore, MD, USA) and was completed in January of 2012. The three trials featured a number of common elements: (1) subjects were maintained at the clinical site on a low nitrate diet for at least 24 h prior to dosing and throughout data and sample collection; (2) sodium nitrite was administered to subjects via an electronic nebulizer (Solo-Idehaler combination device) over approximately 10 min; (3) all study subjects received nebulization device training with placebo solution, including regular collection of post-dose vital signs, at least 1 day prior to the first dose of sodium nitrite; (4) inhalation of sodium nitrite was followed by blood sampling for plasma nitrite and biomarkers, clinical pathology assessments including venous methemoglobin, percutaneous oxygen saturation, standard laboratory assessments including urinalysis and coagulation; (5) vital signs and 12-lead ECGs were assessed at multiple timepoints; typically pre-dose, immediately post-inhalation, and at 15, 30 min, and 1, 2, 4, 8, and 24 h post-inhalation, while pulmonary function via spirometry was typically assessed pre-dose, and at 30 min, 1, 4, 12, and 24 h post-inhalation.
Details of subject exclusion criteria and definitions of adverse events and DLTs are presented in Supplemental Methods (Online Resource 1).
2.2 Informed Consent
All clinical trials were conducted with the full informed consent of all participating subjects, under the authority of an institutional review board in compliance with regulations on the Protection of Human Subjects as outlined in US CFR 21, Part 50; International Conference on Harmonization Good Clinical Practices Guidelines (E6) [33] and the general principles that have their origin in the 1964 Declaration of Helsinki and its later amendments.
2.3 Materials
Sodium nitrite for all studies was manufactured by E. Merck KG (Darmstadt, Germany). Sildenafil citrate (Revatio®, 20 mg) was manufactured by Pfizer, Inc. (New York, NY, USA). AIR001 inhalation solution was prepared for dosing by admixture of prefilled vials of sodium nitrite solution with an appropriate volume of placebo/diluent solution to achieve the required concentration and osmolarity. Prefilled vials were manufactured by Bioserv Corporation (San Diego, CA, USA). In all cases, a final volume of 4 mL was loaded into the nebulizer medication chamber for administration to subjects.
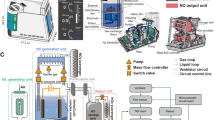
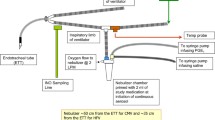
2.4 Solo-Idehaler Device
In all studies, AIR001 inhalation solution was administered via a high efficiency electronic nebulizer. The device was a combination of the Aeroneb® Solo nebulization head (Aerogen, Galway, Ireland) and the Idehaler™ aerosol-reservoir attachment (Diffusion Technique Francais, Saint Etienne, France), and is referred to as the Solo-Idehaler. The efficiency of the Solo-Idehaler, defined as the ratio of the emitted dose (delivered at the mouthpiece) to the dose of AIR001 inhalation solution loaded into the nebulizer medication chamber, was determined to be 76 % (Supplemental Methods—Online Resource 1).
2.5 Exhaled Nitric Oxide
FENO was assessed at various timepoints before and after dosing in studies CS01 and CS04, Part A using the NIOX MINO Model 09-1000 (Aerocrine, Inc. Morrisville, NC, USA) according to the manufacturer’s instructions.
2.6 Bioanalytical Methods
Concentrations of plasma nitrite in all studies were determined via a liquid chromatography-fluorometric assay (BASi, West Lafayette, IN, USA) based on derivatization of nitrite with 1,2-diaminonapthalene, reversed-phase chromatography, and flow-through fluorometric detection. Sildenafil and its N-desmethyl metabolite were measured in human plasma samples from Part B of study CS04 using an liquid chromatography-tandem mass spectrometry assay (PPD, Richmond, VA, USA). Both these assays were fully validated consistent with the US Food and Drug Administration Guidance for Industry [34]. In addition, the sildenafil and N-desmethyl sildenafil methods were both confirmed to be devoid of interference from the presence of either nitrite or nitrate. Concentrations of nitrate metabolite, R-SNO, and Hb(Fe)-NO were determined in selected samples in Part A of study CS04 using a reductive chemiluminescence assay as previously described [35, 36]. Bioanalytical method details, including sample processing, are presented in Supplemental Methods (Online Resource 1).
2.7 Pharmacokinetic Analysis
Pharmacokinetic parameters for plasma nitrite and metabolite nitrate were estimated using standard non-compartmental analysis of individual subject concentration vs. time data. Details of the pharmacokinetic data analysis are presented in Supplemental Methods (Online Resource 1).
3 Results
3.1 Subject Demographics and Baseline Assessments
A total of 82 healthy male and female subjects were treated with nebulized sodium nitrite (AIR001) or placebo in the three trials. Demographics and baseline assessments for all treated subjects across the trials are presented in Table 1.
3.2 Safety and Tolerability of Nebulized Sodium Nitrite
In study CS01, two subjects (one male and one female) out of 6 at the 176-mg dosage level experienced symptomatic hypotension (reduction in both systolic and diastolic blood pressure) and tachycardia. The most severely affected subject experienced a 33-mmHg decrease in mean arterial pressure (MAP) and a 40-bpm increase in heart rate immediately after inhalation; however, this subject recovered within 20 min following intravenous fluids and supine positioning. An additional two subjects at this dosage level also experienced hypotension per blood pressure measurements, although these subjects were asymptomatic. When averaged across the six subjects in this cohort, maximal decreases in MAP were 13 mmHg, which was associated with a mean heart rate increase of 12 bpm. The effects generally occurred immediately or shortly following nitrite inhalation, and had resolved by 2 or 4 h post-dose. Dose escalation was halted because of this DLT, and the maximum tolerated dose (MTD) was defined to be the next lower dosage level of 125 mg, for which average maximal decreases in MAP across six subjects were only 5.9 mmHg.
In study CS02, symptomatic hypotension was observed in one of four subjects in a low-dose cohort (15 mg sodium nitrite), which was presumed to have been the result of inadvertent overdosing based on pharmacokinetics, methemoglobin concentrations, and pulmonary hemodynamic responses (data not shown). When this same dosage level was repeated in four additional subjects, there were no adverse events, nor were adverse events observed in subsequent cohorts of 45 and 113 mg sodium nitrite. Results from the first “15-mg” cohort in study CS02 are not included here because the actual dose administered could not be established with certainty. The MTD was thus determined to be 113 mg, the highest dosage level tested in this study.
In study CS04, two subjects (one man and one woman) out of three treated at the high dosage level of 120 mg experienced transient but symptomatic orthostasis (without change in systolic blood pressure) that resolved without intervention following their first dose, thus lowering the MTD to the next lower dose of 90 mg. No serious adverse events were reported following repeated inhalation of 15, 45, or 90 mg AIR001 once every 8 h for 6 days (16 total administrations), or in subjects who received nitrite dosage levels up to 90 mg four times daily co-administered with steady-state oral sildenafil (20 mg every 8 h for 4 days prior to nitrite dosing). No clinically significant changes in ECG parameters or on pulmonary function via spirometry testing were recorded following administration of any dosage level of sodium nitrite in these studies.
Increases in methemoglobin (MetHb) were observed in all studies at dosage levels of 45 mg and above. MetHb was generally maximal at 30 min, and returned to baseline by 4 h post end of inhalation. Maximal MetHb concentrations did not exceed 3.0 % in any subject, nor were any changes in SaO2 observed in any subject in the three trials presented. No accumulation in MetHb concentrations were apparent following repeated inhalation of nitrite for 6 days in Part A of study CS04 (data not shown).
3.3 Plasma Pharmacokinetics of Nitrite
Noncompartmental pharmacokinetic parameters of plasma nitrite were calculated for all evaluable cohorts across all three studies (Table 2). Plasma nitrite concentrations in subjects receiving dosage levels below 5 mg were generally not different from pre-dose baseline, and pharmacokinetic evaluation was therefore not attempted for these cohorts.
The time of maximal nitrite concentrations (t max) in plasma was generally either immediately, or within 5 min, after the end of the 10-min inhalation period (i.e., 0.17–0.25 h after start of inhalation), and plasma nitrite concentrations decreased mono-exponentially (Fig. 1), with a terminal half-life (t 1/2) in plasma across all three studies of 0.59 (0.19) h; mean (standard deviation). Both maximum plasma concentration (C max) and area under the plasma concentration–time curve (AUC) of plasma nitrite increased with dose administered across studies, and increases were generally dose proportional through the repeat-dose MTD level of 90 mg (Fig. 2). The apparent clearance (CL/F) of nitrite in plasma was high in all studies (1–2 L/h/kg).
Concentration–time profiles of plasma nitrite relative to the start of a 10-min sodium nitrite inhalation in healthy male and female subjects following a single dose (left) or on day 6 (right) following a total of 16 (every 8 h) administrations in Part A of study CS04. Values represent mean (n = 3 or 6), and error bars represent standard deviation. Dosage levels represent the mass of sodium nitrite loaded into the nebulizer medication chamber. 120-mg dosage level discontinued after day 1 due to DLT in two of three subjects
Inter-study comparison of dose response for plasma nitrite C max and AUCinf (or AUC0–t for cohorts where AUCinf could not be calculated) following a single sodium nitrite inhalation in healthy male and female subjects. Nitrite concentrations in subjects from studies CS01 and CS02 were individually background subtracted prior to calculation of C max and AUC, while no correction was used for study CS04 because pre-dose nitrite was below the limit of detection in all subjects (cf Online Resource 1; Table 1). Values represent mean (n = 3–6), and error bars represent standard deviation. AUC inf area under the plasma concentration–time curve from time zero to infinity, AUC 0–t area under the plasma concentration-time curve from time zero to last quantifiable, C max maximum plasma concentration
In general, the pharmacokinetics of inhaled nitrite in normoxic subjects were not different from those in subjects exposed to mild hypoxia in study CS02, nor were nitrite pharmacokinetics impacted by co-administration with steady-state sildenafil (4 days of every 8 h sildenafil pretreatment) in Part B of study CS04 (Table 2). Conversely, plasma trough concentrations of sildenafil and its N-desmethyl metabolite were not impacted by repeated co-administration of sodium nitrite, even when the nitrite dosing frequency was increased to four times daily (every 6 h) (Table 3). These findings support the safe use of nebulized sodium nitrite in the clinical setting of PAH.
3.4 Plasma Pharmacokinetics of Nitrate Metabolite
Plasma concentrations of the nitrate metabolite were assessed in Part A of study CS04 as a secondary measure of total nitrite exposure, and to assess accumulation of this metabolite following repeated administration. Baseline corrected C max and AUC from time zero to 8 h (AUC0–8 h) of nitrate increased with dose only for dosage levels of 45 mg and higher on study day 1, but increases were dose proportional across all dosage levels by study day 6 (Fig. 3). At the MTD dosage level of 90 mg, there was an accumulation of approximately 50 % in the C max and AUC0–8 h of the nitrate metabolite on day 6 relative to those following a single dose (Fig. 3), in contrast to the situation for nitrite where no accumulation was observed following repeated inhalation. The t 1/2 of nitrate could not be directly determined in this study because of a limited sampling time of only 8 h (i.e., one dosing interval), but steady-state accumulation of 50 % following every 8 h dosing is consistent with an effective t 1/2 of approximately 5 h [37].
Dose response of C max and AUC0–8 h for nitrate metabolite in plasma following single (day 1) or repeated (day 6, after 16 total every 8 h doses) inhalation of sodium nitrite in healthy male and female subjects from Part A of study CS04. Nitrate concentrations in subjects were individually background subtracted prior to calculation of C max and AUC. Values represent mean (n = 3 or 6), and error bars represent standard deviation. AUC area under the plasma concentration–time curve, AUC 0–8 h area under the plasma concentration–time curve from time zero to 8 h, C max maximum plasma concentration
3.5 Pharmacodynamic Effects
The FENO was assessed in studies CS01 and CS04 (Part A) as a measure of local NO exposure. Increases in FENO were found to be maximal at the first post-inhalation measurement (immediately post or 5 min post end of inhalation, respectively), and were generally not different from baseline by 30 min post-inhalation in either study. There appeared to be a threshold dosage level of 17 mg in study CS01, below which post-dose increases in FENO were not observed, and above which FENO increases were observed at all dosage levels without a clear dose response. Similarly, in Part A of study CS04, post-dose FENO increased at all dosage levels, but again without dose response. Values averaged across all dose cohorts were 4- to 5-fold over pre-dose baseline on both days 1 and 6 (Fig. 4).
Fraction exhaled nitric oxide (FENO) in parts per billion (ppb), pre-dose and 5 min after the end of inhalation following single dose (left) or after 16 total every 8 h doses (right) in all sodium nitrite-treated subjects at well-tolerated dosage levels of 15, 45, and 90 mg from Part A of study CS04 (n = 18). p values from paired Student’s t tests of pre- vs. post-dose values on each study day. Mean FENO increased from 16.1 to 68.7 ppb on day 1 (4.3-fold increase) and from 14.8 to 84.3 ppb on day 6 (5.7-fold increase)
Concentrations of Hb(Fe)-NO and R-SNO were assessed in Part A of study CS04 as independent measures of systemic NO exposure. Blood concentrations of both markers were found to be maximal at the first collection time of 1-h post-dose, and levels in most subjects had returned to baseline by 4 h post-dose (Fig. 5). Concentrations of both markers increased with the inhaled nitrite dose, indicating systemic exposure to NO in these subjects. The profiles were not different between study days 1 and 6 (day 6, data not shown), indicating a lack of accumulation of these markers despite 6 days of every 8 h administration. The concentration–time profiles of R-SNO in plasma were similar to those in blood (plasma data not shown); however, the magnitude of the response in plasma was approximately 10-fold lower. For example, the maximal R-SNO concentrations at the MTD dosage level of 90 mg on study day 6 were 0.026 ± 0.005 µmol/L (mean ± standard deviation) in plasma vs. 0.274 ± 0.058 µmol/L in blood.
Concentration–time profiles (n = 3 or 6) of S-nitrosothiol (R-SNO) species (upper) and iron-nitrosyl-hemoglobin (lower) in whole blood following a single 10-min inhalation of sodium nitrite in healthy male and female subjects in Part A of study CS04. Values represent mean (n = 3–6), and error bars represent standard deviation. Dosage levels represent the mass of sodium nitrite loaded into the nebulizer medication chamber. FE NO fraction exhaled nitric oxide
3.6 Nitrite Stability in Human Blood
The stability of nitrite was assessed in heparinized human blood, and the in vitro t 1/2 was found to be 30 min at 4 °C; however, following centrifugation, nitrite in plasma was found to be relatively stable during incubation over packed red blood cells (Online Resource 2). The authors have considered the potential impact of nitrite instability in blood on results reported here by reviewing laboratory records on sample collection and processing times in a subset of 590 samples from study CS04. The median time to centrifugation was found to be 7 min on ice after blood collection. Assuming a t 1/2 in chilled whole blood of 30 min and negligible loss post-centrifugation, the typical loss of nitrite would not be expected to exceed 15 % prior to freezing for bioanalysis.
4 Discussion
Nebulized sodium nitrite administered every 8 h for 6 days was well tolerated in healthy subjects at dosage levels up to and including 90 mg, and tolerability was not impacted by mild hypoxia or coadministration with steady-state sildenafil. These results support the safe use of sodium nitrite in the clinical setting of PAH, where both transient hypoxia and sildenafil exposure are likely. At higher dosage levels, DLTs were symptomatic orthostasis (120 mg) or hypotension with tachycardia (176 mg), and these adverse events, which were reported in one male and one female subject each, generally resolved without intervention beyond a short period of supine recumbency. Thus, the safety profile of nebulized sodium nitrite (AIR001) is considered acceptable for use in out-patient studies.
Clinically significant decreases in MAP have also been reported following parenteral administration of sodium nitrite, with many of these studies reporting compensatory tachycardia in hypotensive subjects. A blood nitrite C max of 16 µmol/L was associated with a MAP decrease of 7 mmHg following intra-arterial infusion [6], while a 30 µmol/L blood C max was associated with a MAP decrease of 10 mmHg, also following intra-arterial infusion [24]. Finally, a plasma nitrite C max of 67 µmol/L was associated with a mean MAP decrease of 14 mmHg following intravenous administration of sodium nitrite [29]. Thus, the mean decrease in MAP of 5.9 mmHg at plasma C max of 11.9 µmol/L (at the MTD dosage level of 125 mg in study CS01) appears consistent with these reports following parenteral administration, and suggests that blood pressure effects following inhalation are primarily mediated by systemic exposure to nitrite. Note that in the hypoxia-induced mouse model of PAH [12], once-weekly, peak plasma nitrite concentrations of 1.5 µmol/L were associated with complete prevention of increases in RVP and RVM, while peak plasma nitrite exposure of 0.4 µmol/L (only a 2-fold increase over baseline) was associated with significant PAP reduction in healthy subjects under conditions of hypoxia [28]. The relatively low plasma nitrite concentrations required for efficacy in these models suggest an acceptable safety margin exists (i.e., 7- to 25-fold) relative to the steady-state nitrite plasma C max of 10 µmol/L at the repeat-dose MTD of 90 mg in study CS04, where neither hypotension nor orthostasis where observed.
Venous blood MetHb did not exceed 3.0 % in any subject following nitrite inhalation, and there was no accumulation of MetHb with repeated inhalation. MetHb levels below 15 % are generally asymptomatic in otherwise healthy individuals [38], thus methemoglobinemia does not appear to present a significant safety concern for the use of nebulized sodium nitrite.
The pre-dose baseline levels of plasma nitrite in subjects in studies CS01 and CS02 (0.6 and 0.8 µmol/L, respectively, Table 1) are 3- to 6-fold greater than values published elsewhere (0.13 µmol/L [24], 0.13 µmol/L [28], and 0.25 µmol/L [25]) or those measured pre-dose in study CS04 using the chemiluminescence assay (0.11 µmol/L, Table 1). This was unexpected given that all subjects in all three of our studies were maintained on a low nitrite diet throughout all study phases. Note that the same validated liquid chromatography-fluorometric assay was used for plasma nitrite in all three studies, and the authors could identify no changes in materials or procedures between studies that could explain this discrepancy.
Per protocol, subjects in all studies were permitted to drink up to two 8-oz glasses of municipal tap water per day. A typical maximum allowable nitrate level of 10 ppm in the water supplied could thus produce a theoretical dosage of 4.8 mg nitrates/subject/day. If significant differences in municipal water supplies existed between Minneapolis, MN (CS01/CS02 study site) and Baltimore, MD (CS04 study site) during the respective periods of study conduct, this could account for the discrepancy in background nitrite levels observed between these studies. Importantly, the plasma nitrite data for all subjects in studies CS01 and CS02 were background subtracted (see Online Resource 1) prior to the pharmacokinetic parameter calculation, so as to allow appropriate comparison to data from study CS04 and other published reports where background levels of nitrite were significantly lower.
The plasma t 1/2 of 0.6 h following nitrite inhalation did not change following 6 days of repeated administration, and this value is comparable to that reported following intra-arterial (0.7 h [24]) or intravenous (0.5 h [29] and 0.8 h [25]) administration of nitrite in healthy subjects. The relative comparability of the t 1/2 to that following parenteral administration, combined with the lack of prolongation following repeated administration, indicates that pulmonary absorption of nebulized nitrite is rapid and complete, without significant deposition in the lung.
Given the short systemic t 1/2 of nitrite, a three times-daily dosing regimen (every 8 h) was selected for Part A of repeat-dose study CS04 as it represented the maximum dosing frequency considered feasible for extended trials in PAH patients [although four times-daily (every 6 h) nitrite inhalation was assessed with sildenafil coadministration in Part B of study CS04 as a worst case scenario]. Note that in mice, even once-weekly nitrite inhalation both prevented and reversed hypoxia-induced vascular remodeling, while plasma nitrite concentrations in these animals were not different from baseline by the 120-min post-dose [12], and in rats, three times per week nitrite inhalation was able to significantly reduce monocrotaline-induced right ventricle hypertrophy and hyperplasia of the small pulmonary arteries [12]. Finally, in human subjects, decreases in hypoxia-induced pulmonary arterial pressure were found to persist 1 h after cessation of a low-dose nitrite infusion, a timepoint by which plasma nitrite concentrations had returned to pre-infusion baseline levels in these subjects [28]. These results suggest that efficacy in PAH may not require persistence of nitrite concentrations above endogenous levels, and thus patients may reasonably expect clinical benefit with every 8 h administration of nebulized sodium nitrite despite its short plasma t 1/2.
The CL/F of nitrite in plasma following inhalation in healthy subjects was high (1.8 L/h/kg at the MTD of 90 mg in Part A of study CS04). When expressed as blood clearance using the blood-to-plasma ratio (R b) of 1.5 reported for nitrite [39], the resulting CL/F value of 1.2 L/h/kg represents 25 % of total human cardiac output (4.8 L/h/kg [40]). Such high apparent CL could be simply due to low systemic bioavailability following inhalation; however, high values for plasma CL have also been reported following parenteral administration of sodium nitrite. A plasma CL of 0.8 L/h/kg was reported following a 5-min intra-arterial infusion of 40 mg sodium nitrite [24], while CL of 1.1 L/h/kg could be calculated based on plasma AUC values reported following a 30-min intravenous infusion of 210 mg of sodium nitrite [29]. Although no intravenous group was included in the present studies, comparison to these published results following parenteral administration suggest that systemic bioavailability following inhalation of nebulized sodium nitrite could be 50 % or more. The V ss/F of nitrite in plasma was large (1.3 L/kg at MTD of 90 mg). Assuming systemic bioavailability of 50 %, and R b of 1.5, the resulting V ss in blood would approach the volume of total body water (0.6 L/kg [40]), indicating extensive distribution of nitrite following inhalation.
The effective t 1/2 of 5 h estimated for the nitrate metabolite is in good agreement with that reported for nitrate following intra-arterial nitrite infusion (6 h [24]), intravenous nitrite infusion (8 h [29]), or following oral administration of nitrate itself (5 h [41]). As was the case with the t 1/2 of nitrite, the comparability of the t 1/2 of the nitrate metabolite following repeated inhalation to that following parenteral administration of nitrite further implies that absorption of sodium nitrite from the lung is rapid and complete, without significant pulmonary accumulation.
The FENO following administration of sodium nitrite has not been previously reported in humans, although studies in anesthetized newborn lambs have demonstrated that nitrite inhalation under conditions of temporary pulmonary hypertension induced by breathing a hypoxic atmosphere (FiO2 of 12 %) produced an immediate 3- to 5-fold increase over baseline in FENO, which was associated with significant decreases in PAP in this ovine model [27]. Thus, the 4- to 5-fold increases of FENO over baseline observed in healthy subjects in the present studies confirm local exposure to NO and are of a similar magnitude to those associated with therapeutic dilatation of the pulmonary vasculature in lambs.
Dose-dependent increases in Hb(Fe)-NO and R-SNO species were observed in healthy subjects following nitrite inhalation in study CS04, and the increases in these biomarkers independently confirm systemic exposure to NO following nitrite inhalation [22]. The levels of R-SNO measured in plasma were 10-fold lower than those in whole blood, suggesting that the major S-nitrosylated blood protein is erythrocytic hemoglobin, while our methods cannot differentiate the specific S-nitrosothiols represented by the smaller plasma fraction (e.g., S-nitrosylated albumin, nitrosoglutathione, and/or other low-molecular-weight R-SNO species).
5 Conclusion
We report the first investigation of the pharmacokinetics, pharmacodynamics, and safety of nebulized sodium nitrite in human subjects. The MTD of inhaled sodium nitrite was determined to be 90 mg when delivered every 8 h for 6 days, and the tolerability was not impacted by mild hypoxia or co-administration with sildenafil. DLTs of inhaled nitrite were symptomatic orthostasis and/or hypotension, which resolve rapidly without intervention. Nebulized sodium nitrite was found to produce dose-proportional plasma pharmacokinetics without accumulation following repeated administration, and was well tolerated at dosage levels producing significant increases in markers of both local and systemic NO exposure. On the basis of these results, inhaled nebulized sodium nitrite (AIR001) has been advanced into randomized trials in PAH patients.
References
Rubin LJ. Pulmonary arterial hypertension. Proc Am Thorac Soc. 2006;3(1):111–5.
Arnold WP, Mittal CK, Katsuki S, Murad F. Nitric oxide activates guanylate cyclase and increases guanosine 3′:5′-cyclic monophosphate levels in various tissue preparations. Proc Natl Acad Sci. 1977;74:3203–7.
Moncada S, Palmer RM, Higgs EA. The discovery of nitric oxide as the endogenous nitrovasodilator. Hypertension. 1988;12:365–72.
Gladwin MT, Shelhamer JH, Schechter AN, Pease-Fye ME, Waclawiw MA, Panza JA, et al. Role of circulating nitrite and S-nitrosohemoglobin in the regulation of regional blood flow in humans. Proc Natl Acad Sci. 2000;97:11482–7.
Doyle MP, Pickering RA, DeWeert TM, Hoekstra JW, Pater D. Kinetics and mechanism of the oxidation of human deoxyhemoglobin by nitrites. J Biol Chem. 1981;256:12393–8.
Cosby K, Partovi KS, Crawford JH, Patel RP, Reiter CD, Martyr S, et al. Nitrite reduction to nitric oxide by deoxyhemoglobin vasodilates the human circulation. Nat Med. 2003;9:1498–505.
Shiva S, Huang Z, Grubina R, Sun J, Ringwood LA, MacArthur PH, et al. Deoxymyoglobin is a nitrite reductase that generates nitric oxide and regulates mitochondrial respiration. Circ Res. 2007;100:654–61.
Rassaf T, Flögel U, Drexhage C, Hendgen-Cotta U, Kelm M, Schrader J. Nitrite reductase function of deoxymyoglobin: oxygen sensor and regulator of cardiac energetics and function. Circ Res. 2007;100:1749–54.
Hendgen-Cotta UB, Merx MW, Shiva S, Schmitz J, Becher S, Klare JP, et al. Nitrite reductase activity of myoglobin regulates respiration and cellular viability in myocardial ischemia-reperfusion injury. Proc Natl Acad Sci. 2008;105:10256–61.
Godber BL, Doel JJ, Sapkota GP, Blake DR, Stevens CR, Eisenthal R, et al. Reduction of nitrite to nitric oxide catalyzed by xanthine oxidoreductase. J Biol Chem. 2000;275:7757–63.
Li H, Samouilov A, Liu X, Zweier JL. Characterization of the magnitude and kinetics of xanthine oxidase-catalyzed nitrite reduction: evaluation of its role in nitric oxide generation in anoxic tissues. J Biol Chem. 2001;276:24482–9.
Zuckerbraun BS, Shiva S, Ifedigbo E, Mathier MA, Mollen KP, Rao J, et al. Nitrite potently inhibits hypoxic and inflammatory pulmonary arterial hypertension and smooth muscle proliferation via xanthine oxidoreductase-dependent nitric oxide generation. Circulation. 2010;121:98–109.
Li H, Kundu TK, Zweier JL. Characterization of the magnitude and mechanism of aldehyde oxidase-mediated nitric oxide production from nitrite. J Biol Chem. 2009;284:33850–8.
Pinder AG, Pittaway E, Morri K, James PE. Nitrite directly vasodilates hypoxic vasculature via nitric oxide-dependent and -independent pathways. Br J Pharmacol. 2009;157:1523–30.
Castello PR, David PS, McClure T, Crook Z, Poyton RO. Mitochondrial cytochrome oxidase produces nitric oxide under hypoxic conditions: implications for oxygen sensing and hypoxic signaling in eukaryotes. Cell Metab. 2006;3:277–87.
Gautier C, van Faassen E, Mikula I, Martasek P, Slama-Schwok A. Endothelial nitric oxide synthase reduces nitrite anions to NO under anoxia. Biochem Biophys Res Commun. 2006;341:816–21.
Vanin AF, Bevers LM, Slama-Schwok A, van Faassen EE. Nitric oxide synthase reduces nitrite to NO under anoxia. Cell Mol Life Sci. 2007;64:96–103.
Qiu Y, Sutton L, Riggs AF. Identification of myoglobin in human smooth muscle. J Biol Chem. 1998;273:23426–32.
Pryde DC, Dalvie D, Hu Q, Jones P, Obach RS, Tran TD. Aldehyde oxidase: an enzyme of emerging importance in drug discovery. J Med Chem. 2010;53:8441–60.
Bueno M, Wang J, Mora AL, Gladwin MT. Nitrite signaling in pulmonary hypertension: mechanisms of bioactivation, signaling, and therapeutics. Antioxid Redox Signal. 2013;18:1797–809.
Hendgen-Cotta UB, Kelm M, Rassaf T. Myoglobin’s novel role in nitrite-induced hypoxic vasodilation. Trends Cardiovasc Med. 2014;24:69–74.
Cannon RO 3rd, Schechter AN, Panza JA, Ognibene FP, Pease-Fye ME, Waclawiw MA, et al. Effects of inhaled nitric oxide on regional blood flow are consistent with intravascular nitric oxide delivery. J Clin Invest. 2001;108:279–87.
Curtis E, Hsu LL, Noguchi AC, Geary L, Shiva S. Oxygen regulates tissue nitrite metabolism. Antioxid Redox Signal. 2012;17:951–61.
Dejam A, Hunter CJ, Tremonti C, Pluta RM, Hon YY, Grimes G, et al. Nitrite infusion in humans and nonhuman primates: endocrine effects, pharmacokinetics, and tolerance formation. Circulation. 2007;116:1821–31.
Pluta RM, Oldfield EH, Bakhtian KD, Fathi AR, Smith RK, Devroom HL, et al. Safety and feasibility of long-term intravenous sodium nitrite infusion in healthy volunteers. PLoS One. 2011;6(1):e14504.
Maher AR, Arif S, Madhani M, Abozguia K, Ahmed I, Fernandez BO, et al. Impact of chronic congestive heart failure on pharmacokinetics and vasomotor effects of infused nitrite. Br J Pharmacol. 2013;169:659–70.
Hunter CJ, Dejam A, Blood AB, Shields H, Kim-Shapiro DB, Machado RF, et al. Inhaled nebulized nitrite is a hypoxia-sensitive NO-dependent selective pulmonary vasodilator. Nat Med. 2004;10:1122–7.
Ingram TE, Pinder AG, Bailey DM, Fraser AG, James PE. Low-dose sodium nitrite vasodilates hypoxic human pulmonary vasculature by a means that is not dependent on a simultaneous elevation in plasma nitrite. Am J Physiol Heart Circ Physiol. 2010;298:H331–9.
Hunault CC, van Velzen AG, Sips AJ, Schothorst RC, Meulenbelt J. Bioavailability of sodium nitrite from an aqueous solution in healthy adults. Toxicol Lett. 2009;190:48–53.
Oldfield EH, Loomba JJ, Monteith SJ, Crowley RW, Medel R, Gress DR, et al. Safety and pharmacokinetics of sodium nitrite in patients with subarachnoid hemorrhage: a phase IIa study. J Neurosurg. 2013;119:634–41.
Mack AK, McGowan Ii VR, Tremonti CK, Ackah D, Barnett C, Machado RF, et al. Sodium nitrite promotes regional blood flow in patients with sickle cell disease: a phase I/II study. Br J Haematol. 2008;142:971–8.
Maher AR, Milsom AB, Gunaruwan P, Abozguia K, Ahmed I, Weaver RA, et al. Hypoxic modulation of exogenous nitrite-induced vasodilation in humans. Circulation. 2008;117:670–7.
International Conference on Harmonisation (ICH) guideline for good clinical practice: E6(R1). 1996. http://www.ich.org/fileadmin/Public_Web_Site/ICH_Products/Guidelines/Efficacy/E6_R1/Step4/E6_R1__Guideline.pdf. Accessed 15 Dec 2011.
FDA/CDER/CVM Guidance for industry. Bioanalytical method validation. U.S. Department of Health and Human Services, Food and Drug Administration, Center for Drug Evaluation and Research (CDER), Center for Veterinary Medicine (CVM). 2001.
MacArthur PH, Shiva S, Gladwin MT. Measurement of circulating nitrite and S-nitrosothiols by reductive chemiluminescence. J Chromatogr B. 2007;851:93–105.
Yang BK, Vivas EX, Reiter CD, Gladwin MT. Methodologies for the sensitive and specific measurement of S-nitrosothiols, iron-nitrosyls, and nitrite in biological samples. Free Radic Res. 2003;37:1–10.
Boxenbaum H, Battle M. Effective half-life in clinical pharmacology. J Clin Pharmacol. 1995;35:763–6.
Wright RO, Lewander WJ, Woolf AD. Methemoglobinemia: etiology, pharmacology, and clinical management. Ann Emerg Med. 1999;34:646–56.
Dejam A, Hunter CJ, Pelletier MM, Hsu LL, Machado RF, Shiva S, et al. Erythrocytes are the major intravascular storage sites of nitrite in human blood. Blood. 2005;106:734–9.
Davies B, Morris T. Physiological parameters in laboratory animals and humans. Pharm Res. 1993;10:1093–5.
Wagner DA, Schultz DS, Deen WM, Young VR, Tannenbaum SR. Metabolic fate of an oral dose of 15N-labeled nitrate in humans: effect of diet supplementation with ascorbic acid. Cancer Res. 1983;43:1921–5.
Acknowledgments
Aires Pharmaceuticals, Inc. (San Diego, CA, USA) was the sole funding source for all studies, and no other company or institution claims financial support or ownership of the data presented. The authors gratefully acknowledge Madhu Cherukury, Ronald Christopher, and Ajay Madan for their careful review of the manuscript.
Disclosures
PJR and MTG are currently or have previously served as consultants for Aires Pharmaceuticals, Inc. MTG is named as a co-inventor on a US government patent for the use of nitrite salts in the treatment of cardiovascular indications. AV was employed by Seventh Wave Laboratories, Inc., NJA and AH are employed by PAREXEL International, AWB is employed by BAS, Inc., and HA is employed by DaVita Clinical Research, all of which are or were under contract with Aires Pharmaceuticals, Inc. GEB, SB, WLH, ELP, and HM are current or former employees and/or shareholders of Aires Pharmaceuticals, Inc.
Author contributions
SB, ELP, MTG, and HM conceived and designed the research; GEB, AWB, AH, HA, and SS performed the experiments; PJR, AV, NJA, GEB, AWB, HA, MTG, SS, and WLH analyzed the data, and PJR wrote the manuscript.
Author information
Authors and Affiliations
Corresponding author
Electronic supplementary material
Below is the link to the electronic supplementary material.
Rights and permissions
Open Access This article is distributed under the terms of the Creative Commons Attribution Noncommercial License which permits any noncommercial use, distribution, and reproduction in any medium, provided the original author(s) and the source are credited.
About this article
Cite this article
Rix, P.J., Vick, A., Attkins, N.J. et al. Pharmacokinetics, Pharmacodynamics, Safety, and Tolerability of Nebulized Sodium Nitrite (AIR001) Following Repeat-Dose Inhalation in Healthy Subjects. Clin Pharmacokinet 54, 261–272 (2015). https://doi.org/10.1007/s40262-014-0201-y
Published:
Issue Date:
DOI: https://doi.org/10.1007/s40262-014-0201-y