Abstract
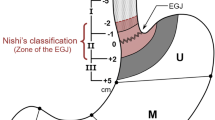
Classification of extramural invasion of esophagogastric junction carcinoma (EGJC) is not yet established. The anatomy surrounding the EGJ alters between the mediastinum and the abdominal cavity. This review proposed a T3 classification of EGJC based on anatomical continuity. Analysis of endoscopic ultrasound images, review of intraoperative images, and detailed observation of surgical specimens were followed by a review of the literature. In the EGJ, the muscularis propria of the esophagus is enclosed in mediastinal adipose tissue called the adventitia, which is surrounded by the diaphragmatic crus and contains the paraesophageal lymph nodes (LNs). After passing through the esophageal hiatus along with the vagus nerves and blood vessels, the adventitia joins the adipose tissue containing the paracardial LNs, which is covered by the peritoneum, and then further divides into the lesser and greater omentum. The connective tissue outside the muscularis propria of the stomach, including the adipose tissue of the omentum, is called the subserosa. According to the TNM classification, T3 esophageal and gastric cancer is defined as invasion of the adventitia and subserosa, respectively. Given that the adventitia is anatomically continuous with the subserosa, T3 tumors of the EGJ can be described as those that extend through the muscularis propria but do not invade the peritoneum or diaphragmatic crus. We propose classifying T3 EGJC as “tumor extends through muscularis propria” rather than using the separate terms “adventitia” and “submucosa”. T4 could be “tumor perforates serosa or invades adjacent structures”, as per the current gastric cancer classification.





Similar content being viewed by others
References
Yamashita H, Seto Y, Sano T, Makuuchi H, Ando N, Sasako M. Results of a nation-wide retrospective study of lymphadenectomy for esophagogastric junction carcinoma. Gastric Cancer. 2017;20:69–83.
Devesa SS, Blot WJ, Fraumeni JF. Changing patterns in the incidence of esophageal and gastric carcinoma in the United States. Cancer. 1998;83:2049–53.
Bollschweiler E, Wolfgarten E, Gutschow C, Hölscher AH. Demographic variations in the rising incidence of esophageal adenocarcinoma in white males. Cancer. 2001;92:549–55.
Buas MF, Vaughan TL. Epidemiology and risk factors for gastroesophageal junction tumors: understanding the rising incidence of this disease. Semin Radiat Oncol. 2013;23:3–9.
Brierley JD, Gospodarowicz MK, Wittekind C, editors. TNM classification of malignant tumours. 8th ed. Chichester: Wiley; 2017.
Kurokawa Y, Takeuchi H, Doki Y, Mine S, Terashima M, Yasuda T, et al. Mapping of lymph node metastasis from esophagogastric junction tumors: a prospective nationwide multicenter study. Ann Surg. 2021;274:120–7.
The Japan Esophageal Society, editor. Japanese Classification of Esophageal Cancer. 12th ed. Tokyo: Kanehara; 2022. (in Japanese).
Kumamoto T, Kurahashi Y, Niwa H, Nakanishi Y, Okumura K, Ozawa R, et al. True esophagogastric junction adenocarcinoma: background of its definition and current surgical trends. Surg Today. 2020;50:809–14.
Spechler SJ, Souza RF. Barrett’s esophagus. N Engl J Med. 2014;371:836–45.
Takubo K, Sasajima K, Yamashita K, Tanaka Y, Fujita K. Double muscularis mucosae in Barrett’s esophagus. Hum Pathol. 1991;22:1158–61.
Misumi A, Murakami A, Harada K, Baba K, Akagi M. Definition of carcinoma of the gastric cardia. Langenbecks Arch Chir. 1989;374:221–6.
Siewert JR, Stein HJ. Carcinoma of the gastroesophageal junction—classification, pathology and extent of resection. Dis Esophagus. 1996;9:173–82.
Siewert JR, Stein HJ. Classification of adenocarcinoma of the oesophagogastric junction. Br J Surg. 1998;85:1457–9.
Fujishima F, Nakamura Y, Kasajima A, Ozawa Y, Ito K, Taniuchi S, et al. Adenocarcinoma in the squamous-lined esophagus without Barrett’s mucosa, probably arising from esophageal gland duct. Esophagus. 2015;12:327–31.
Posner MC, Forastiere AAMB. Cancer of esophagus. In: Devita VT, Hellman SRS, editors. Cancer Princ. Pract. Oncol. Philadelphia: Lippincott Williams & Wilkins; 2005. p. 861–909.
Nishi M, Noumura H, Kajisa T, Aiko T, Kaneko YKT. Surgical problem of carcinoma in the esophagogastric junction. Stomach Intest. 1978;13:1497–507 (in Japanese with English abstract).
Bonavina L, Evander A, DeMeester TR, Walther B, Cheng SC, Palazzo L, et al. Length of the distal esophageal sphincter and competency of the cardia. Am J Surg. 1986;151:25–34.
Byrne PJ, Stuart RC, Lawlor P, Walsh TN, Hennessy TPJ. A new technique for measuring lower oesophageal sphincter competence in patients. Ir J Med Sci. 1993;162:351–4.
Sato T, Kato Y, Matsuura M, Gagner M. Significance of palisading longitudinal esophagus vessels: identification of the true esophagogastric junction has histopathological and oncological considerations. Dig Dis Sci. 2010;55:3095–101.
Maselli R, Inoue H, Ikeda H, Onimaru M, Yoshida A, Santi EG, et al. Microvasculature of the esophagus and gastroesophageal junction: Lesson learned from submucosal endoscopy. World J Gastrointest Endosc. 2016;8:690.
Stecco C, Sfriso MM, Porzionato A, Rambaldo A, Albertin G, Macchi V, et al. Microscopic anatomy of the visceral fasciae. J Anat. 2017;231:121–8.
Takubo K. Pathology of the esophagus. 3rd ed. Tokyo: Wiley; 2017. p. 41.
Shinohara H, Kurahashi Y, Ishida Y. Gastric equivalent of the ‘Holy Plane’ to standardize the surgical concept of stomach cancer to mesogastric excision: updating Jamieson and Dobson’s historic schema. Gastric Cancer. 2021;24:273–82.
Shinohara H, Kurahashi Y, Haruta S, Ishida Y, Sasako M. Universalization of the operative strategy by systematic mesogastric excision for stomach cancer with that for total mesorectal excision and complete mesocolic excision colorectal counterparts. Ann Gastroenterol Surg. 2018;2:28–36.
Shinohara H. Anatomy of the stomach and surrounding structures. In: Springer, editor. Illus. Abdom. Surg. based Embryol. Anat. Dig. Syst. Singapore; 2020. p. 1–19.
Sadler TWLJ. Langman’s medical embryology. 14th ed. Philadelphia: Lippincott Williams & Wilkins; 2019.
Moore KL, Persaud TVNTM. The developing human: clinically oriented embryology. 8th ed. Philadelphia: Saunders/Elsevier; 2008.
Mills SE, editor. Histology for pathologists. 5th ed. Wolters Kluwer: Osaka; 2020.
Jackson RG. Anatomy of the vagus nerves in the region of the lower esophagus and the stomach. Anat Rec. 1949;103:1–18.
Shapiro AL, Robillard GL. The esophageal arteries their configurational anatomy and variations in relation to surgery. Ann Surg. 1950;131:171–85.
Yan Y, Chen C, Chen Y, Wu Y, Shi Z. Arterial patterns in the thoracic and abdominal segments of the esophagus: anatomy and clinical significance. Surg Radiol Anat. 1998;20:399–402.
Piao DX, Ohtsuka A, Murakami T. Typology of abdominal arteries, with special reference to inferior phrenic arteries and their esophageal branches. Acta Med Okayama. 1998;52:189–96.
Byrnes KG, Walsh D, Lewton-Brain P, McDermott K, Coffey JC. Anatomy of the mesentery: historical development and recent advances. Semin Cell Dev Biol. 2019;92:4–11.
Nakamura T, Shinohara H, Okada T, Hisamori S, Tsunoda S, Obama K, et al. Revisiting the infracardiac bursa using multimodal methods: topographic anatomy for surgery of the esophagogastric junction. J Anat. 2019;235:88–95.
Broman I. Die Entwickelungsgeschichte der Bursa omentalis und ähnlicher Rezessbildungen bei den Wirbeltieren. In: Bergmann JF, editor. Wiesbaden; 1904.
Broman I. Warum wird die Entwicklung der Bursa Omentalis in Lehrbuchern fortwahrend unrichtig beschrieben? Anat Anz. 1938;86:195–202.
Japanese Gastric Cancer Association, editor. Japanese classification of gastric carcinoma. 15th ed. Tokyo: Kanehara; 2017. (in Japanese).
Acknowledgements
This work was supported in part by Japan Society for the Promotion of Science KAKENHI Grant Numbers 22H03153 (HS) and 21K08809 (YK).
Author information
Authors and Affiliations
Corresponding author
Ethics declarations
Ethical Statement
All procedures followed were in accordance with the ethical standards of the responsible committee on human experimentation (institutional and national) and with the Helsinki Declaration of 1964 and later versions. Informed consent or substitute for it was obtained from all patients for being included in the study.
Conflict of Interest
The authors declare no conflict of interest.
Additional information
Publisher's Note
Springer Nature remains neutral with regard to jurisdictional claims in published maps and institutional affiliations.
Rights and permissions
Springer Nature or its licensor (e.g. a society or other partner) holds exclusive rights to this article under a publishing agreement with the author(s) or other rightsholder(s); author self-archiving of the accepted manuscript version of this article is solely governed by the terms of such publishing agreement and applicable law.
About this article
Cite this article
Kurahashi, Y., Tomita, T., Nakamura, T. et al. Proposal for T3 classification of esophagogastric junction carcinoma based on the interconnection of extramural anatomical structures. Esophagus 20, 587–594 (2023). https://doi.org/10.1007/s10388-023-01023-x
Received:
Accepted:
Published:
Issue Date:
DOI: https://doi.org/10.1007/s10388-023-01023-x