Abstract
Gentamicin is an aminoglycoside antibiotic with a small therapeutic window that is currently used primarily as part of short-term empirical combination therapy. Gentamicin dosing schemes still need refinement, especially for subpopulations where pharmacokinetics can differ from pharmacokinetics in the general adult population: obese patients, critically ill patients, paediatric patients, neonates, elderly patients and patients on dialysis. This review summarizes the clinical pharmacokinetics of gentamicin in these patient populations and the consequences for optimal dosing of gentamicin for infections caused by Gram-negative bacteria, highlighting new insights from the last 10 years. In this period, several new population pharmacokinetic studies have focused on these subpopulations, providing insights into the typical values of the most relevant pharmacokinetic parameters, the variability of these parameters and possible explanations for this variability, although unexplained variability often remains high. Both dosing schemes and pharmacokinetic/pharmacodynamic (PK/PD) targets varied widely between these studies. A gentamicin starting dose of 7 mg/kg based on total body weight (or on adjusted body weight in obese patients) appears to be the optimal strategy for increasing the probability of target attainment (PTA) after the first administration for the most commonly used PK/PD targets in adults and children older than 1 month, including critically ill patients. However, evidence that increasing the PTA results in higher efficacy is lacking; no studies were identified that show a correlation between estimated or predicted PK/PD target attainment and clinical success. Although it is unclear if performing therapeutic drug monitoring (TDM) for optimization of the PTA is of clinical value, it is recommended in patients with highly variable pharmacokinetics, including patients from all subpopulations that are critically ill (such as elderly, children and neonates) and patients on intermittent haemodialysis. In addition, TDM for optimization of the dosing interval, targeting a trough concentration of at least < 2 mg/L but preferably < 0.5–1 mg/L, has proven to reduce nephrotoxicity and is therefore recommended in all patients receiving more than one dose of gentamicin. The usefulness of the daily area under the plasma concentration–time curve for predicting nephrotoxicity should be further investigated. Additionally, more research is needed on the optimal PK/PD targets for efficacy in the clinical situations in which gentamicin is currently used, that is, as monotherapy for urinary tract infections or as part of short-term combination therapy.
Similar content being viewed by others
Avoid common mistakes on your manuscript.
A standard intravenous gentamicin starting dose of 7 mg/kg total body weight appears to optimize the chance of reaching the exposure target after the first administration in both non-obese adults and children older than 1 month, including critically ill patients. |
For obese patients, using a dosing nomogram specifically created for this population is recommended; alternatively, a gentamicin dose of 5–6 mg/kg adjusted body weight once daily can be used. |
To reduce the risk of nephrotoxicity, therapeutic drug monitoring is warranted in each patient receiving more than one dose of gentamicin. |
Studies are needed to establish the optimal exposure target for efficacy when gentamicin is given as part of short-term empirical combination therapy. |
1 Introduction
Gentamicin is an aminoglycoside antibiotic that has been in use for parenteral administration since 1971 [1]. Despite 50 years of clinical experience, optimal dosing schemes still need further refinement [2], especially for subpopulations where population pharmacokinetic (PPK) studies have been relatively sparse, including paediatric, elderly and critically ill patients [3]. Additionally, adjusting the dosage to individual needs remains a challenge due to the narrow therapeutic window and substantial interindividual variability (IIV) of gentamicin pharmacokinetics [3]. Moreover, the optimal pharmacokinetic/pharmacodynamic (PK/PD) target for clinical efficacy is still under debate [4].
Gentamicin pharmacokinetics in specific subpopulations like obese patients, critically ill patients, paediatric patients, neonates, elderly patients and patients on dialysis can differ from gentamicin pharmacokinetics in the general adult patient population. This manuscript aims to narratively review the clinical pharmacokinetics of gentamicin in these patient populations and the consequences for optimal dosing of gentamicin for infections caused by Gram-negative bacteria, focussing on new insights from the past 10 years.
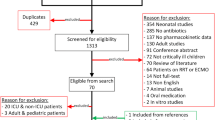
We searched PubMed for relevant articles from the past 10 years using the following search strategy: ((Pharmacokinetics [Mesh] OR Pharmacokinetics [Subheading] OR Monte Carlo Method [Mesh] OR Drug Monitoring [Mesh] OR Drug Dosage Calculations [Mesh] OR Pharmacokinetic*[tiab] OR Pharmacodynamic*[tiab] OR PK/PD[tiab] OR population Pk*[tiab] OR target attainment[tiab] OR target attainment[tiab] OR Drug monitoring[tiab] OR TDM[tiab] OR Dose calculation*[tiab] OR Drug dos*[tiab]) AND ("Gentamicins"[Mesh] OR gentamicin*[tiab])), limited to the last 10 years and to articles in English. Articles on aminoglycosides were included only if specific data on gentamicin were reported; data on other aminoglycosides (particularly tobramycin) were not extrapolated to gentamicin. Articles focusing exclusively on treatment for infections caused by Gram-positive bacteria (e.g. combination therapy for endocarditis) were not included. Articles were selected after reading titles and abstracts. In addition, references from selected articles were screened for relevance.
2 Pharmacokinetics in the General Adult Population
2.1 Pharmacokinetic Parameters
The median clearance (CL) of gentamicin in adult patients with normal renal function (creatinine clearance [CLCR] >60 mL/min) is 4.58 L/h/70 kg (range 4.31–5.12) [3]. Gentamicin distributes mainly into the extracellular fluid compartment, the volume of distribution (Vd) in non-critically ill adult patients with normal renal function is approximately 19.5 L/70 kg [5, 6]. The ranges of pharmacokinetic parameters in several subpopulations are reported in Table 1.
2.2 Variability and Causes
In five studies published between 1989 and 2006, included in a large review of PPK models of gentamicin that focused on patients from the general adult population (excluding patients on haemodialysis, cystic fibrosis, critically ill and elderly patients), IIV in CL ranged from 18.5 to 36% [3]. Two of these studies reported IIV in Vd or IIV in the volume of distribution in the central compartment (V1). In a one-compartment model, IIV in Vd was 11.9%. In a two-compartment model, IIV in V1 was 5.8% [3]. One study including 697 adult patients also reported 8% interoccasion variability (IOV) for CL and 19% IOV for volume of distribution in the peripheral compartment (V2) [5]. To the best of our knowledge, no new PPK studies focusing on the general adult population have been published in the last 10 years.
In the 14 studies on adults included in the aforementioned review, CLCR was the most common covariate found to have a significant impact on gentamicin CL (in 7/10 studies that tested it) [3]. Three studies that focused on the general population reported that addition of renal function as a covariate on CL decreased IIV in CL from 95 to 67%, from 55 to 27% and from 33.9 to 18.5%, respectively [5, 7, 8]. In several studies, the Chronic Kidney Disease Epidemiology Collaboration equation (CKD-EPI) performed better than the Cockcroft-Gault equation (CRGT) or the Modification of Diet in Renal Disease equation (MDRD) for their association with gentamicin CL, and adjustment for individual body surface area improved the performance of CKD-EPI, especially for obese or cachectic patients [9,10,11].
In the aforementioned review, total body weight (TBW) was the most common covariate on gentamicin Vd (in 9/14 studies that tested it) [3]. The pharmacokinetics of gentamicin in obese patients will be described in more detail separately.
2.3 Dosing and Pharmacokinetic/Pharmacodynamic (PK/PD) Targets
Although once-daily dosing (ODD) (or extended-interval dosing) of gentamicin has still not been universally implemented [12,13,14], there is consensus that this dosing scheme makes optimal use of the pharmacological characteristics of gentamicin, increasing the probability that the gentamicin concentration has dropped below the threshold for nephrotoxicity when the next dose is administered [2]. Pathophysiologically, ODD likely leads to less gentamicin accumulation in proximal renal tubular epithelial cells because of saturation of gentamicin uptake, which probably takes place through megalin-and cubilin-mediated endocytosis [2, 15, 16].
In recent decades, dosing of gentamicin has increased from 3 to 4.5 mg/kg/day and subsequently to 6 or 7 mg/kg/day to maximize the probability of target attainment (PTA) [17]. However, the optimal PK/PD target for clinical efficacy of aminoglycosides is still under debate [4]. Several clinical studies from the 1980s and 1990s found the ratio of peak concentration to minimal inhibitory concentration (Cmax/MIC) to be the PK/PD index that was primarily linked to clinical efficacy, with maximal efficacy at Cmax/MIC ≥ 8–10 (Fig. 1) [18,19,20]. A study analysing data from four earlier prospective studies including 236 patients with a Gram-negative bacterial infection receiving aminoglycosides, of which 103 received gentamicin, found increasing clinical response (a composite endpoint with clinical and/or microbiological parameters) with increasing Cmax/MIC [19]. All patients received combination therapy, but no concomitant antibiotics that had an antibiotic effect against the causative Gram-negative micro-organisms. A retrospective study including 78 patients treated with aminoglycosides for hospital-acquired pneumonia with a Gram-negative micro-organism (predominantly Pseudomonas aeruginosa), of which 38 received gentamicin, found that Cmax/MIC >10 in the first 48 hours of therapy was associated with a 90% probability of defervescence and normalisation of leucocyte count. Of the included patients, 94% received combination therapy with a β-lactam, of which 72% had a causative micro-organism that was also susceptible to the β-lactam antibiotic [18].
Illustration of the pharmacokinetic/pharmacodynamic parameters associated with efficacy and toxicity. AUC area under the concentration–time curve, Cmax peak concentration, Cmin trough concentration, MIC minimal inhibitory concentration, PAE post-antibiotic effect, persistent suppression of bacterial growth that occurs after the gentamicin concentration drops below the MIC [2]. A Cmax /MIC ratio ≥8–10 and a AUC/MIC ratio ≥70–100 are used as targets for efficacy when treating Gram-negative infections, Cmin <2 mg/L is associated with reduced risk of nephrotoxicity
Alternatively, the ratio of area under the concentration–time curve to minimal inhibitory concentration (AUC/MIC) has been proposed as the primary PK/PD index for aminoglycosides (Fig. 1), mostly based on animal studies [21]. Two small clinical studies found AUC0-24/MIC to be the superior PK/PD index for clinical efficacy of aminoglycosides, but these only included patients on tobramycin [22, 23]; a prospective study including 13 cystic fibrosis (CF) patients with an exacerbation caused by Pseudomonas aeruginosa, treated with the combination of tobramycin and ticarcillin (but most strains were resistant to ticarcillin, and no correlation was found between clinical effect and ticarcillin MIC or T>MIC) [22], and an analysis of data from two earlier prospective studies including 23 patients receiving tobramycin monotherapy for intra-abdominal infection (combined with clindamycin) or Gram-negative bacterial pneumonia [23]. Definitive AUC/MIC efficacy targets have not been established and could depend on the circumstances: an AUC/MIC of 30–50 may provide good outcomes in non-critically ill patients with lower and uncomplicated upper urinary tract infections or in patients receiving combination therapy, but an AUC/MIC of 80–100 may be needed in critically ill patients with non-urinary tract infections or in patients receiving gentamicin monotherapy [4]. For simulated patients with normal renal function treated with 7 mg/kg once daily, the probability of reaching an AUC/MIC of 30.7 was 99.8% for an MIC of 1 mg/L and 89.5% for an MIC of 2 mg/L [21]. However, the probability of reaching an AUC/MIC of 84.3 was 58.8% for an MIC of 1 mg/L and only 2.1% for an MIC of 2 mg/L [21]. Starting in January 2020, based on these considerations, the European Committee on Antimicrobial Susceptibility Testing (EUCAST) has restricted the clinical breakpoints for gentamicin to infections with Enterobacterales originating from the urinary tract treated with a daily dose of 6–7 mg/kg of ideal body weight (IBW), with the clinical breakpoint set at 2 mg/L [24]. Gentamicin is no longer considered an adequate treatment option for Pseudomonas aeruginosa, since wild-type MICs of P. aeruginosa are so high that the PTA is negligible. For lower and uncomplicated upper urinary tract infections with Enterobacterales, EUCAST notes that doses lower than 6–7 mg/kg may be adequate [25, 26] because gentamicin is concentrated in urine and renal tissues. Yet, they also note that the appropriate dosing regimen is not certain since most PK/PD data have been based on mouse thigh and lung models [27]. For other systemic infections, EUCAST states that aminoglycosides should only be used in combination with another active therapy because of low PTA in these infections [27]. Of note, treatment for pneumonia with systemic aminoglycosides is particularly difficult. Since only 12–30% of aminoglycoside serum levels are achieved in epithelial lining fluid [28, 29], the PTA when using a starting dose of 7 mg/kg will be negligible. In clinical practice, both Cmax/MIC and AUC/MIC may be used as target, since they are highly correlated when using ODD [30, 31]. Of note, if an AUC/MIC target is used instead of a Cmax target, patients with decreased CL would need a lower daily dose to reach the same AUC0-24. Theoretically, these patients might therefore have less risk of nephrotoxicity when dosing based on an AUC/MIC target compared with dosing on a Cmax/MIC target. However, the AUC threshold for nephrotoxicity remains to be established [4] and studies are needed to ascertain if AUC-guided dosing decreases the risk of nephrotoxicity, especially in patients with decreased CL, who are at increased risk of nephrotoxicity.
2.4 Predictors of Efficacy and Toxicity
Despite all mentioned considerations with regard to PK/PD targets, the question is whether these targets indeed predict efficacy in clinical situations. A large review from 2017 of PPK studies on aminoglycosides described nine studies that have associated PK/PD indices with efficacy, of which only one study included only patients on gentamicin [3]. The PK/PD indices evaluated in these studies were Cmax/MIC or Cmax in two studies, AUC/MIC or AUC in two studies and both Cmax /MIC and AUC/MIC in five studies. The most common PK/PD targets in these studies were Cmax /MIC ≥7–10 or AUC/MIC ≥70–100. However, no studies were identified that showed a correlation between estimated or predicted PK/PD target attainment and clinical success [3].
A meta-analysis from 2021 of the optimal target gentamicin trough concentration (Cmin) for reducing the risk of nephrotoxicity found no randomized controlled trials (RCTs) but included five observational studies (615 patients) evaluating a Cmin of 2 mg/L and one observational study (187 patients) evaluating a Cmin of 1 mg/L [32]. Patients with Cmin <2 mg/L had significantly less risk of nephrotoxicity (odds ratio [OR] 0.22, 95% confidence interval [CI] 0.12–0.40) compared with patients with Cmin ≥2 mg/L (Fig. 1). One of these studies used logistic regression to define the best Cmin cut-off point to predict acute kidney injury (AKI) and found a Cmin of 2.0 mg/L [33]. The only study using a Cmin <1 mg/L target also showed significantly less risk of nephrotoxicity compared with patients with Cmin ≥1.1 mg/L (OR 0.07, 95% CI 0.02–0.24) [34]. Of note, using a Cmin target to reduce the risk of nephrotoxicity has been under debate for several decades, since a Cmin above the threshold may be the result and not the cause of renal damage [35]. However, the largest and most recent study (from 2015) included in the aforementioned meta-analysis only used Cmin levels collected prior to the diagnosis of AKI, suggesting that high Cmin levels are indeed a risk factor for nephrotoxicity [33]. Daily AUC is also a predictor for aminoglycoside nephrotoxicity [36, 37], but the optimal daily AUC to reduce the risk of nephrotoxicity is currently unclear [4].
Gentamicin treatment is also associated with a risk of ototoxicity: cochleotoxicity (often permanent sensorineural hearing loss) and/or vestibulotoxicity (balance disorders). The number of doses, the duration of therapy and the cumulative dose are weak predictors of aminoglycoside ototoxicity [38]. ODD does not appear to significantly reduce the risk of ototoxicity compared with multiple day dosing (MDD) [2], possibly because clearance of aminoglycosides from the inner ear is very slow, resulting in a very long exposure time of the inner ear [39]. Of 35 PPK studies on gentamicin included in a large review from 2017, none have evaluated the association between PK/PD indices and ototoxicity [3]. In a PPK study to predict the risk of ototoxicity in CF patients treated with tobramycin using a two-compartment model, Cmax >2 mg/L in the peripheral compartment showed the highest correlation with hearing loss severity [38].
Interestingly, there appears to be a circadian variation of gentamicin toxicity [40]. A prospective study including 184 patients receiving 4 mg/kg gentamicin once daily reported increased risk of nephrotoxicity when gentamicin was administered during the night [41]. Although baseline renal function was not equally distributed between treatment groups, the results did not change when baseline clearance was added to the model in a multivariate analysis [41]. Increased risk of both ototoxicity and nephrotoxicity during the rest period was also found in animal studies [42, 43]. However, a more recent retrospective cohort study including 310 general ward patients and 411 ICU patients found no differences in pharmacokinetics or toxicity between patient groups that received aminoglycosides in the morning, afternoon or night and advised not to wait until the next morning but to start aminoglycosides as soon as possible [44].
2.5 Recommendations
For the general adult population, a starting dose of 7 mg/kg is recommended, followed by therapeutic drug monitoring (TDM) after the first administration for optimization of the dosing interval, in order to reduce the risk of nephrotoxicity. This dose is expected to reach both the Cmax /MIC and AUC/MIC targets, although we found no studies that showed a correlation between PK/PD target attainment and clinical success. A Cmax >16 mg/L target (Cmax /MIC >8 for a maximal MIC of 2 mg/L) can be achieved in a large majority of adult patients using 7 mg/kg (e.g. 85% of patients with sepsis at the emergency department [45]). Using a starting dose of 7 mg/kg also results in a simulated 89.5% PTA when aiming for an AUC/MIC target of 30.7 with a maximal MIC of 2 mg/L [21]. The starting dose recommendations for the general adult population and other subpopulations are reported in Table 2. We advise against the use of gentamicin monotherapy for infections caused by Pseudomonas aeruginosa and for pneumonia.
3 Pharmacokinetics in Obese Patients
3.1 Pharmacokinetic Parameters
In several studies from the 1980s and 1990s, gentamicin CL was reported to be increased in obese patients compared with non-obese patients [46]. For example, Bauer et al. reported a CL of 8.46 L/h in obese versus 5.76 L/h in non-obese patients [47]. After standardizing to a body surface area (BSA) of 1.73 m2 or a TBW of 70 kg, mean CL was comparable in these studies, with 4.3–4.6 L/h/1.73 m2 or L/h/70 kg in obese patients versus 4.0–5.5 L/h/1.73 m2 or L/h/70 kg in non-obese patients, leading to higher CL in patients with larger BSA or higher TBW [47,48,49]. However, CL in these studies is difficult to extrapolate to the current situation. The definition of obesity was different from today, with obese patients having an average TBW of 80–100 kg, which is significantly lower than the average TBW of obese patients in more recent studies. Moreover, dosing regimens were also different from today, with patients receiving MDD. A PPK study from 2019 including 20 richly sampled obese patients reported a CL of 5.4 L/h/70 kg, but excluded patients with glomerular filtration rate (GFR) <60 mL/min, so CL is expected to be lower than 5.4 L/h/70 kg in obese patients with renal impairment [46].
Gentamicin Vd is increased in obese patients compared with non-obese patients when not weight normalized, due to higher TBW and BSA, with mean Vd in seven studies ranging from 13.3 L to 26.8 L in obese patients versus 10.0 to 24.3 L in non-obese patients [46,47,48,49,50,51,52]. However, since the extracellular water (ECW) volume in adipose tissues is lower than in other tissues, Vd is decreased in obese patients when normalized to L/kg TBW, with mean Vd in five studies ranging from 0.15 to 0.29 L/kg in obese patients versus 0.19 to 0.35 L/kg in non-obese patients [11, 47, 49, 50, 52].
3.2 Variability and Causes
In a PPK model including 20 morbidly obese patients and eight non-obese patients, TBW was the best predictor for both CL and V1 [46]. Addition of TBW as a covariate for V1 and CL led to a large reduction in unexplained IIV, from 49.6 to 18.5% for V1 and from 32.2 to 17.4% for CL. Addition of lean body weight (LBW) or adjusted body weight (ABW) as a covariate to V1 was inferior to TBW [46].
Interestingly, a retrospective study including 335 patients, of whom 223 were overweight or obese, showed that skeletal muscle area and volume extracted from computed tomography (CT) images as measures of body composition explained more of IIV in CL than TBW, an observation to be confirmed in further studies [53].
3.3 Dosing and PK/PD Targets
Several weight-based dosing regimens have been proposed for obese patients. A large study including 2073 patients including underweight and obese patients advised the use of LBW for dosing, since LBW performed better in estimating gentamicin Vd across all weight strata than TBW and IBW [11]. However, most studies advise the use of ABW. ABW introduces a dosing weight correction factor (DWCF) for the excess body weight (TBW − IBW) to account for the limited gentamicin diffusion in adipose tissues [49]. The standard weight-based dose is then performed on ABW = IBW + (TBW − IBW) * DWCF instead of on TBW, with DWCF ranging from 0.3 to 0.55 in seven studies [47,48,49,50,51,52, 54], with 0.4 being currently most commonly used [54]. The aforementioned PPK study recommends using a dose nomogram for patients with GFR >60 mL/min, based on a TBW derived ‘dose weight’: 70 * (TBW/70)0.73 [46]. Based on simulations, dosing 5–6 mg/kg ABW (using a DWCF of 0.4) or 8 mg/kg LBW would lead to similar exposure in some obese patients and could be considered as alternatives [46]. However, calculated starting doses using ABW, ‘dose weight’ or the nomogram can differ substantially, particularly at the higher end of the weight range (see Table 3). Therefore, a conservative approach to dosing and prompt TDM are suggested to avoid toxicity. Several PK/PD targets have been used in studies on pharmacokinetics of obese patients. Several older studies used a Cmax of 5–8 mg/L as target [47, 49], studies from the last decade have used a Cmax of 16–20 mg/L [11], AUC0-24 of 68.7 mg·h/L [46] or a serum concentration of 0.5–2.0 mg/L 16 hours after infusion, based on a nomogram [54].
3.4 Predictors of Efficacy and Toxicity
We did not find any studies investigating the association between target attainment and clinical cure or toxicity specifically for obese patients.
3.5 Recommendations
Obese patients are at risk of overdosing when a starting dose of 7 mg/kg TBW is used. Instead, using the dosing nomogram based on a ‘dosing weight’ calculated as 70 * (TBW/70)0.73 or dosing 5–6 mg/kg ABW with a DWCF of 0.4 (ABW = IBW + 0.4 * [TBW – IBW]) is advised for obese patients with normal renal function, followed by TDM after the first administration for optimization of the dosing interval in order to reduce the risk of nephrotoxicity [46]. Lower doses and extension of the dosing interval is recommended in obese patients with reduced renal function [55].
4 Pharmacokinetics in Critically Ill Patients
4.1 Pharmacokinetic Parameters
In critically ill patients, many pathophysiological changes affecting both Vd and CL can occur that complicate gentamicin dosing [56]. Based on 11 studies summarized in a review from 2021 of aminoglycosides PPK studies in critically ill patients, the median CL of gentamicin in these patients is 3.0 L/h (range 1.15–5.7 L/h) and the median Vd 29 L (range 19–53 L) [57]. Two other studies also reported CL and Vd within these ranges [58, 59]. Several studies including only critically ill patients using renal replacement therapy (i.e. continuous venovenous haemodiafiltration [CVVHDF], continuous venovenous haemofiltration [CVVH], intermittent haemodialysis [IHD], and extended daily diafiltration [EDD-f]) showed a Vd ranging from 14.1 L to 46.9 L [60,61,62,63,64,65].
4.2 Variability and Causes
Even when using body weight standardized starting doses, large IIV in Vd (ranging from 10.9% to 64.4% [57, 59]) causes a wide range in Cmax, resulting in an increased risk of both supra- and subtherapeutic Cmax [58, 66, 67]. This variability in Vd can partially be explained by body weight (TBW [62, 67] or IBW [68]), disease severity [69], hypoalbuminaemia [68], the use of total parenteral nutrition [70] and several other variables that are associated with the capillary leak syndrome that can occur during septic shock [56].
Additionally, CL also shows large IIV, ranging from 29.3% to 83.7% [57]. GFR, often CLCR estimated using CRGT, is the most common retained covariate for CL in gentamicin PPK models in critically ill patients [57]. GFR is often decreased due to an interplay of sepsis-related AKI, pre-existing comorbidities and nephrotoxic drugs [71], leading to lower CL and an increased risk of Cmin >2 mg/L. While such reductions in GFR and increases in exposure have been associated with toxicity [32], data establishing a causal link between gentamicin exposure and AKI in humans do not yet exist; however, animal models support that increasing gentamicin exposure (AUC) increases the risk of AKI and that vulnerability to AKI may be greater in males [72]. Conversely, augmented renal clearance (ARC, defined as GFR >130 mL/min/1.73 m2) can also occur, most often in relatively young trauma patients without pre-existential comorbidities, for whom higher gentamicin doses may be indicated [73]. Other determinants reported to explain variability in CL include usage of CVVH [68] or IHD [63] and several measures of body weight [62, 68, 74].
Obesity in critically ill patients is associated with both increased CL and Vd compared with non-obese critically ill patients, which can lead to both sub- or supra-therapeutic gentamicin concentrations; strict TDM after the first dose is therefore recommended in this subpopulation [75].
4.3 Dosing and PK/PD Targets
The daily dosing regimens of gentamicin as reported in PPK studies in critically ill patients have ranged from 3 mg/kg to 8 mg/kg [57, 76,77,78]. The PK/PD target used varied between these studies; most have used a Cmax /MIC ≥8–10 as target [57], resulting in a Cmax target of ≥16–20 mg/L when targeting micro-organisms with a maximum MIC of 2 mg/L [24]. Studies dosing 8 mg/kg used a Cmax target of 30–40 mg/L, to also target microorganisms with an MIC of 4 mg/L [76,77,78]. Several recent studies have shown unsatisfactory Cmax target attainment in critically ill patients: 47% reached a target Cmax of ≥15 mg/L with 4 mg/kg [66], 59% reached a target Cmax of ≥16 mg/L with a median dose of 6.2 mg/kg [79] and only 0–6% achieved a target Cmax >30 mg/L when using 8 mg/kg [76,77,78]. Simulation studies showed that 11 mg/kg would be needed to achieve a Cmax >30 mg/L in more than half of the patients [80] and that even with the highest simulated dose of 12 mg/kg, <90% of patients in an ICU specializing in severe respiratory and infectious diseases would achieve Cmax >16 mg/L [59].
4.4 Predictors of Efficacy and Toxicity
In multiple studies evaluating aminoglycoside efficacy in critically ill patients, no significant correlation was found between PK/PD target attainment and clinical outcome [79, 81, 82]. The largest of these studies was a prospective observational cohort study in 59 intensive care units that included 931 patients on aminoglycosides, of which 303 received gentamicin. Of 90 patients with a measured gentamicin Cmax after the first dose, 59% attained the targeted Cmax of >20 mg/L. In multivariate analysis, there was no significant association between target attainment of aminoglycosides and clinical success (odds ratio 1.24, 95% confidence interval 0.79–1.94; p = 0.35).
To the best of our knowledge, there are no studies focusing specifically on the critically ill population that show an association between gentamicin Cmin and the risk of toxicity.
4.5 Recommendations
Especially in critically ill patients with increased Vd, a starting dose of 7 mg/kg is necessary to increase the PTA. Although using a starting dose of 8–10 mg/kg in this population would further increase the PTA, these higher doses can also result in an increased risk of nephrotoxicity as the Cmin will also increase, resulting in Cmin >2 mg/L in a proportion of patients if dosing intervals are not adjusted. In these patients, the risk of nephrotoxicity is already relatively high, since AKI can also develop because of the septic shock in itself, because of comorbidities like diabetes mellitus, pre-existent reduced renal function and dehydration and because of treatment with nephrotoxic co-medication like vancomycin, diuretics and contrast media [71]. In a propensity-based study including critically ill patients that had no AKI before day 3, no increased risk of nephrotoxicity was found in 39 patients receiving a short course of gentamicin 7 mg/kg for a mean of 2.6 days, compared with patients who did not receive gentamicin [83]. However, even a small decrease in renal function may negatively impact the clinical outcome in critically ill patients [84, 85]. Since targeting an adequate Cmax /MIC in all critically ill patients inevitably increases the risk of nephrotoxicity on a population level [86], one should carefully weigh the risks and benefits of gentamicin therapy in this patient population.
Although there is no evidence that attainment of the PK/PD target (with or without the use of TDM) is associated with clinical success, TDM is advised to optimize the PTA in critically ill patients.
5 Pharmacokinetics in Paediatric Patients
In the paediatric population, pharmacokinetics can vary between several subpopulations, each requiring a different dosing regimen. The pharmacokinetics in paediatric patients in general (infants aged >28 days to 12 months, children aged >12 months to 11 years and adolescents aged 12–18 years) will be reviewed separately from the pharmacokinetics in neonates (0–28 days).
5.1 Pharmacokinetics Parameters
The Vd of gentamicin is greater for paediatric patients than for adult patients. This is the result of body compositional changes with increasing age: at birth, ECW comprises 45% of TBW but rapidly declines to 27% of TBW at the age of 1 year, after which the ECW only slightly decreases to reach adult values of circa 20% [87, 88]. Although studies addressing the effect of age on pharmacokinetic parameters of gentamicin remain scarce, several studies have been published in the last 10 years that make it possible to define the actual pharmacokinetic differences more clearly [89]. In infants, Vd of gentamicin is estimated to be 0.35 L/kg [89], higher than reported in adults and lower compared with neonates [90]. Studies on pharmacokinetics of gentamicin in febrile neutropenic children aged 0–17 years showed a Vd ranging from 0.25 L/kg to 0.32 L/kg [91, 92].
Gentamicin CL is determined by the developmental stage of the renal function. The renal function is fully matured at the age of 1–2 years [88, 93]. CL is therefore expected to be lower during the first weeks of life, but higher in 2- to 5-year-old children, where the weight-corrected GFR is almost 70% higher compared with adults [94, 95]. Mean CL for infants is estimated to be 0.12 ± 0.01 L/h/kg [90]. In febrile neutropenic paediatric patients, CL was estimated to be 0.08–0.13 L/h/kg [91, 92].
5.2 Variability and Causes
A large variability of pharmacokinetic parameters can be observed in the paediatric population, which is to be expected considering the relatively rapidly changing body composition. Age and weight (birth and/or current weight) are the most important covariates influencing gentamicin Vd and CL [3], with significantly higher Vd and CL values for febrile neutropenic children aged ≤10 years compared with children aged >10 years [91]. In contrast with the adult population, CLCR was often not found to influence CL, possibly because the linear equations often used for estimating GFR (such as CRGT) do not accurately predict GFR in young children [96, 97], since renal function develops non-linearly with increasing age [98]. The IIV ranges from 21.6% to 49% for Vd and from 16% to 39% for CL [3].
Critically ill paediatric patients are subject to even larger pharmacokinetic variability due to pathophysiological changes affecting Vd and CL, as described in a systematic review from 2020 [95]. In a review of the pharmacokinetic alterations of gentamicin in critically ill paediatric patients treated with extracorporeal membrane oxygenation (ECMO), Vd was found to be enlarged by 28.8% to 58.8% and CL to be decreased by 26.3% to 31.7% [99]. Conversely, CL can also be increased due to ARC, which occurs in up to 67% of critically ill paediatric patients [95, 100]. These findings underscore the importance of TDM.
Obese children are subject to additional body compositional changes. Adipose tissue has a smaller ECW volume than other tissues, decreasing Vd (if measured in L/kg TBW) of gentamicin in obesity [101,102,103]. A retrospective study compared Vd of gentamicin in 25 obese children (defined as a body mass index [BMI] ≥95th percentile for age and gender) with that of 25 healthy weight children (defined as a BMI ≥5th percentile and ≤85th percentile) and found a significantly lower Vd in obese children (0.20 ± 0.05 vs 0.28 ± 0.07 L/kg TBW, p < 0.01) [101]. No changes in CL of gentamicin were observed in obese children compared with non-obese children [101, 103].
5.3 Dosing and PK/PD Targets
Gentamicin dosing recommendations for the paediatric population are inconsistent [3, 104]. In general, based on PK/PD targets from the general adult population, a starting dose of 7 mg/kg/24 h is recommended for children aged 1 month to 18 years, followed by TDM performed before administration of the second dose [89, 90, 105]. Higher doses of 8 mg/kg/24h have been suggested for oncology patients based on a PPK study targeting Cmax /MIC >10 [106]. Several studies have proposed to use separate dosing regimens for several age categories, where infants and children aged 1 month to 8–12 years should receive at least 7 mg/kg/day and older children should receive 5–7 mg/kg/day [89,90,91, 107, 108]. The exact cut-off age is unclear, as different age categories have been proposed. It is currently unknown whether a weight index other than TBW should be used for obese paediatric patients and, if so, what index should be used. Studies have suggested the use of fat-free mass (amongst others) instead of TBW, but evidence is limited [89, 106, 109].
In three studies on gentamicin in a review from 2020 of pharmacokinetics and target attainment of antibiotics in critically ill children, dosing recommendations ranged from 6 mg/kg to 9 mg/kg per day [95]. Currently, the same dosing regimens used for the general paediatric population are applied to the critically ill paediatric patients, but TDM is of even more importance due to the additional IIV. Special attention should be given to patients with renal failure and ARC to avoid toxic or subtherapeutic gentamicin exposure.
Despite the increasing evidence favouring ODD over MDD [110], both dosing regimens are still being used [104]. Altogether, ODD is considered the preferred dosing regimen in paediatric patients, based on the similar effectivity and toxicity rates, the reduced costs and increased convenience of ODD [110].
5.4 Predictors of Efficacy and Toxicity
We did not find studies investigating the association between target attainment and clinical cure in the paediatric population. It is therefore currently unknown which PK/PD target predicts efficacy best. The same holds true for toxicity: Cmin ranging from 0.5 mg/L to 2 mg/L are referred to in the literature [107]. However, nephrotoxicity and ototoxicity also occur in paediatric patients when adequate trough concentrations are maintained and ODD is used [105]. To our knowledge, no recent studies specifically reported toxicity of gentamicin in the critically ill paediatric patient.
5.5 Recommendations
For children older than 1 month, a starting dose of 7 mg/kg is advised, followed by TDM after the first administration for optimization of the dosing interval in order to reduce the risk of nephrotoxicity [89]. Simulations show that higher starting doses may be needed for optimal treatment of infections caused by micro-organisms with an MIC of 2 mg/L [107] and that younger children may need higher starting doses than older children (e.g. 10.8 mg/kg for children ≤10 years vs 6.4 mg/kg for children >10 years [91] or 9.5 mg/kg for children <2 years, 8.5 mg/kg for children 2–7 years and 7 mg/kg for children ≥8 years [108]). Clinical studies are needed to confirm these findings. In critically ill paediatric patients, TDM is also advised to optimize the PTA.
6 Pharmacokinetics in Neonates
6.1 Pharmacokinetic Parameters
The Vd of gentamicin in neonates ranges from 0.38 L/kg to 0.91 L/kg for both preterm and term neonates [89, 111,112,113,114,115,116, 117]. CL is largely linked to size and age and is estimated to range from 0.007 L/kg/h to 0.09 L/kg/h [89, 112, 114,115,116, 117]. Since nephrogenesis is not completed until 36 weeks of gestation, CL is lower for preterm neonates than for term neonates [112].
6.2 Variability and Causes
Neonates are subject to considerable pharmacokinetic variability, due to body compositional changes that are most pronounced in the first weeks of life and the functional maturation of organs [112]. Two reviews from 2017 and 2019 have extensively described PPK models of neonates [3, 89]. Weight (birthweight, current weight) is the most important covariate influencing Vd and age (predominantly gestational age [GA] or GA and postnatal age combined) and weight (birthweight, current weight) are the most important covariates influencing CL [3]. The IIV ranges from 10.3% to 35% for Vd and from 16.1% to 58.6% for CL. In neonates undergoing controlled hypothermia, there is no significant change in Vd but CL is 25–50% lower [117, 118].
6.3 Dosing and PK/PD Targets
Several dosing regimens have been suggested for neonates depending on GA and weight [89]. ODD is preferred over MDD, as CL of gentamicin is decreased and gentamicin half-life is therefore prolonged [119]. Altogether, most studies recommend dosages of 4–5 mg/kg bodyweight and prolonged (36–48 h) dosing intervals for preterm patients (GA <37 weeks) and for patients with very low birthweight [89, 111,112,113,114, 117, 120,121,122]. Most studies in neonates use this dose of 4–5 mg/kg bodyweight, resulting in a mean Cmax value of 5.4–11.2 mg/L; a few studies aimed for a Cmax of 15–20 mg/L [89].
6.4 Predictors of Efficacy and Toxicity
For neonates, peak concentrations of 5–12 mg/L and trough concentration of < 0.5–2 mg/L have been proposed based on adult data [19]. Yet, studies addressing target attainment and its association with clinical cure are lacking. With regard to toxicity, a retrospective study showed that patients weighing >1500 mg who had Cmax >10 mg/L had an increased risk of developing ototoxicity [111]. However, a review on aminoglycoside toxicity in neonates found no clear association between gentamicin use and ototoxicity and nephrotoxicity [123].
6.5 Recommendations
For neonates, most studies advise a starting dose of 4–5 mg/kg, with prolonged dosing intervals of 36–48 hours for preterm and very low birthweight neonates. TDM is advised after the first administration for optimization of the dosing interval in order to reduce the risk of nephrotoxicity. In critically ill neonates, TDM is also recommended to optimize the PTA.
7 Pharmacokinetics in Elderly Patients
7.1 Pharmacokinetics Parameters
Mean gentamicin CL is lower in elderly patients due to the decrease of mean GFR with advancing age, but age as an independent factor does not appear to be of influence [124]. Of note, a recent study in non-elderly adult CF patients (age range 19–50 years) did find age to be an independent modifier of aminoglycoside clearance [125]. Gentamicin Vd in the elderly is similar to Vd in the general patient population: in a review comparing pharmacokinetic parameters from several studies across a range of ages, patients with mean ages of 39, 61 and 80 years all had a mean Vd of approximately 25 L/70 kg [124].
7.2 Variability and Causes
A PPK study including 38 patients aged >65 years with a mean age of 80 years estimated IIV in CL to be 20.5% (after adding CLCR as a covariate) and IIV in Vd to be 10.5% (after adding LBW as a covariate) [126]. This study also found that gentamicin CL was reduced by 12% in frail elderly patients (scored using the Reported Edmonton Frailty Scale) compared with non-frail patients, even after adjustment for LBW and renal function [126].
7.3 Dosing and PK/PD Targets
To the best of our knowledge, the only recent study focusing on target attainment in the elderly was a large, multicentre, retrospective observational study including 128 patients >75 years receiving gentamicin with a mean dose of 3.5 ± 1.2 mg/kg/day [127]. Cmax was measured in 27 patients (21%), with a mean Cmax of 9.4 mg/L and adequate Cmax /MIC >10 in only 6/22 (27%) patients for whom an MIC was available. Cmin was measured in 57 patients (44%), with adequate Cmin <0.5 mg/L in only 16 patients (28%) [127].
7.4 Predictors of Efficacy and Toxicity
We did not find any studies investigating the association between PK/PD target attainment and clinical cure or toxicity specifically for elderly patients.
Elderly patients are at increased risk of nephrotoxicity, and probably of ototoxicity [124]. Based on eight studies, a meta-analysis from 2021 found the overall absolute risks of AKI following aminoglycoside exposure (with 68.6%–100% of patients receiving gentamicin) to be 15.1% among patients aged >65 years, significantly higher than the average 10.5% risk of AKI among patients >18 years (p < 0.00001) [128]. In the aforementioned retrospective study including patients >75 years, nephrotoxicity was associated with treatment length ≥3 days and concomitant use of nephrotoxic drugs [127].
7.5 Recommendations
Because of increased risk of toxicity in elderly patients, an individualized risk–benefit assessment should be performed in elderly patients for whom aminoglycoside therapy is indicated. If treatment with gentamicin is started, it is recommended to use a starting dose of 7 mg/kg, to limit treatment duration to <3 days, to perform TDM after the first administration for optimization of the dosing interval in order to reduce the risk of nephrotoxicity and to reduce use of other nephrotoxic drugs whenever possible [127]. In critically ill elderly, TDM is also recommended to optimize the PTA.
8 Pharmacokinetics in Patients on Intermittent Haemodialysis
8.1 Pharmacokinetic Parameters
During IHD sessions, mean gentamicin CL ranged from 4.68 L/h to 6.96 L/h, approximating normal renal function (but total daily CL is much lower in patients on IHD because of low CL between sessions) [63, 129,130,131,132]. Mean Vd ranges from 12.4 to 23.1 L or L/70 kg [63, 64, 129,130,131,132], which is also comparable to patients from the general population.
8.2 Variability and Causes
A wide range of CL of 1.1–22.2 L/h is reported in patients during IHD [64, 129, 130, 132]. IHD effectively clears aminoglycosides, but CL is highly variable because of differences in dialyzer types, length and frequency of dialysis sessions, blood flow rates, small solute clearance and patient characteristics such as residual renal function [130, 131, 133,134,135,136]. In a PPK study including six anuric patients, the addition of TBW as a covariate decreased IIV from 55.7% to 0.3% for non-IHD CL and from 90.7% to 50.7% for V1 [137]. In another PPK study including 46 patients with end-stage renal disease, CLCR explained 35% and 53% of IIV in non-IHD CL and Vd, respectively. Of note, here CLCR is likely to be a marker of LBW and non-renal CLCR [63].
8.3 Dosing and PK/PD Targets
For patients on IHD, data are limited and optimal dosing remains controversial [138]. Traditionally, gentamicin is administered at the end of an IHD session using a loading dose of 2–3 mg/kg, followed by a maintenance dose of 1.5 mg/kg [138, 139]. Using a range of simulated dosing schemes, several studies have evaluated the possible effects of higher doses of gentamicin preceding IHD, resulting in a higher Cmax, an acceptable AUC and a lower Cmin, maximizing efficacy while reducing the risk of toxicity, using Cmax /MIC >8–10 or Cmax >8 mg/L as PK/PD targets [64, 130, 137, 140]. One prospective observational study first performed simulations and subsequently treated ten critically ill patients using IHD with 6 mg/kg gentamicin just before dialysis, resulting in a mean Cmax of 31.8 mg/L, a mean Cmin (after 24 h) of 4.1 mg/L and a mean AUC of 190 mg·h/L [64]. This dosing schedule was subsequently validated in another prospective observational study [65]. A prospective PPK study including 23 patients on IHD concluded that pre-dialysis doses of 2 mg/kg (for an MIC of 1 mg/L), 4 mg/kg (for an MIC of 2 mg/L) or 8 mg/kg (for an MIC of 4 mg/L) were associated with the best efficacy/toxicity ratio [140].
8.4 Predictors of Efficacy and Toxicity
Nephrotoxicity concerns do not play a significant role in deciding on the optimal dose and time of aminoglycoside administration for patients with end-stage renal disease. For critically ill patients on IHD, a strategy with dosing of gentamicin preceding IHD may result in more potential for efficacy and less potential for toxicity [64]. However, we found no studies on the association between PK/PD target attainment and efficacy or toxicity in patients on IHD.
8.5 Recommendations
When gentamicin is administered after the IHD session, a loading dose of 2–3 mg/kg is currently recommended, followed by a maintenance dose of 1.5 mg/kg after each following session [139] and TDM for optimization of both the dosing interval (in order to reduce the risk of nephrotoxicity) and the probability of PK/PD target attainment. When gentamicin is administered before the IHD session, allowing a high Cmax and low Cmin, a first dose of 4–6 mg/kg is recommended, followed by TDM [64, 139]. A first dose of 6 mg/kg before the IHD session may be the optimal approach for critically ill patients [64, 65].
9 Pharmacokinetics in Patients on Peritoneal Dialysis
9.1 Pharmacokinetic Parameters
Gentamicin can be administered intraperitoneally (IP) to achieve higher local concentrations for treatment of peritoneal dialysis (PD)-related peritonitis. The pharmacokinetic parameters of gentamicin IP are not well described, particularly during inflammation and infection. The largest prospective pharmacokinetics study to date, including 24 patients with peritonitis treated with gentamicin IP, reported systemic CL of 0.25 L/h and Vd of 21.0 L/70 kg [141]. Median bioavailability of IP gentamicin was reported to be 76% (interquartile range 69–82%) [141].
9.2 Variability and Causes
Apart from residual renal function, peritonitis is an important determinant for gentamicin CL in PD patients. After IP gentamicin is absorbed into the circulation, CL takes place by glomerular filtration and through PD in anuric patients. Mean systemic half-life was 28.7 hours in peritonitis patients compared with 36 hours in volunteer PD patients without peritonitis [142, 143], which can be explained by increased membrane permeability in peritonitis patients, resulting in increased clearance from the plasma into the peritoneal cavity during the 18 hours that no IP gentamicin is administered [141].
9.3 Dosing and PK/PD Targets
The currently used gentamicin IP dose is 40 mg or 0.6 mg/kg TBW once daily with 6 hours dwell time [141, 144,145,146]. Using 0.6 mg/kg and a PK/PD target of Cmax /MIC >8 in peritoneal dialysate, median intraperitoneal Cmax and Cmin were 23.8 mg/L and 1.5 mg/L and median Cmax and Cmin in plasma were 3.1 mg/L and 1.9 mg/L, respectively [141]. In a prospective cohort study using a plasma Cmin of 0.5–2.0 mg/L at day 2 as PK/PD target, mean Cmin in plasma was 1.8 mg/L but 43% had Cmin >2 mg/L [146]. However, even in patients with a Cmin in plasma <2 mg/L, the high systemic absorption of 76% in patients with peritonitis and the prolonged plasma elimination half-life of 28.7 hours may lead to drug accumulation in the systemic circulation, increasing the risk of toxicity [141]. A lower dose would decrease plasma Cmin but also intraperitoneal Cmax, which may negatively impact efficacy. A shorter dwell time would decrease systemic absorption and result in lower plasma Cmin, while the intraperitoneal Cmax would not change. A recent PPK study including 24 patients evaluated the PTA for treatment success (defined as IP Cmax /MIC >10) and toxicity (defined as plasma AUC <120 mg*h/L) for a 2-week course using several dosing schemes with dwell times ranging from 2 to 6 hours using Monte Carlo simulations. They reported that a dose of 0.6 mg/kg with a dwell time of 5 hours or a dose of 0.7 mg/kg with a dwell time of 3 hours is sufficient (PTA >80% and >90%, respectively) to treat organisms with an MIC of ≤2 mg/L without the risk of significant systemic exposure (PTA >90%) [147]. However, to the best of our knowledge, there are no clinical studies that evaluate the efficacy and toxicity of dosing regimens with a shorter dwell time.
9.4 Predictors of Efficacy and Toxicity
There are no data on the association between drug levels, PK/PD target attainment and peritonitis outcomes or toxicity. In a prospective cohort study including 51 patients, gentamicin serum levels at day 2 did not predict gentamicin-related efficacy or toxicity during short-course gentamicin therapy for Gram-negative PD-related peritonitis, except in cases of polymicrobial peritonitis, where higher day 2 serum levels were associated with cure (2.06 ± 0.41 in cured patients vs 1.29 ± 0.71 in patients with treatment failure; p = 0.01) [146].
9.5 Recommendations
For patients on continuous ambulatory peritoneal dialysis (CAPD), the current recommended gentamicin IP dose is 40 mg or 0.6 mg/kg once daily with 6 hours’ dwell time [141, 146], although regimens with shorter dwell time should be evaluated in future clinical studies.
10 Discussion
We aimed to review the clinical pharmacokinetics and consequences for optimal dosing of gentamicin for infections caused by Gram-negative bacteria in various patient populations, focusing on new insights from the past decade. Several new PPK studies have focused on specific subpopulations including obese patients [46], critically ill patients [66, 68, 148], paediatric patients [90, 92, 106, 149], neonates [112, 115,116,117,118, 122], elderly patients [126] and patients on IHD [64, 137], providing insights into the typical values of CL and Vd in these patient groups, the variability of these parameters and possible explanations for this variability. But despite inclusion of covariates in many of these PPK models, unexplained IIV in CL and Vd often remained high, especially in critically ill patients, resulting in wide ranges of Cmax, Cmin and AUC. Because of this high variability, it is difficult to give unambiguous advice on optimal dosing, which is also illustrated by the wide range of dosing schemes used in the literature. Moreover, dosing advice from the literature is often based on simulations using PPK models that have not been externally validated and may therefore not be generalizable [3, 57, 89]. In addition, very limited new PPK data have been published in the last 10 years from healthy volunteers or the general adult patient population, which is quite remarkable since the general adult population may be the largest population in which gentamicin is used.
As described earlier, the PK/PD targets used in the literature vary widely and definitive clinical evidence on the optimal PK/PD target for gentamicin is still lacking, despite 50 years of clinical use. Both Cmax /MIC and AUC/MIC targets are advocated, and in clinical practice both may be used, since they show high collinearity when using ODD [30, 31]. The starting dose recommendations presented in Table 2 are expected to result in a high PTA after the first administration for both the Cmax /MIC and AUC/MIC targets associated with clinical efficacy.
However, a higher PTA does not automatically result in higher efficacy. Strikingly, a large review from 2017 of PPK studies on aminoglycosides identified no studies that showed a correlation between estimated or predicted PK/PD target attainment and clinical success [3]. Two more recent studies specifically focusing on ICU patients also failed to find this correlation; both studies also included patients treated with amikacin or tobramycin and used aminoglycosides as part of combination therapy [79, 82]. The failure to identify an association between target attainment and clinical efficacy may be due to the fact that gentamicin is often used as part of short courses of empirical combination therapy and rarely as targeted monotherapy. This complicates clinical evaluation of optimal dosing since co-administered antibiotics may be responsible for clinical success. Furthermore, the location of the infection could be a determinant of the optimal PK/PD target. Moreover, other factors such as severity of illness and comorbid conditions are probably stronger predictors of clinical outcome than PK/PD target attainment, especially in critically ill patients [81]. Consequently, before optimal dosing regimens can be defined, more research is needed on the targets for efficacy in the clinical situations in which gentamicin is currently used, that is, monotherapy for urinary tract infections or as part of combination therapy, with a focus on the validity of the AUC/MIC and Cmax /MIC targets.
Likewise, using a Cmin target to reduce the risk of nephrotoxicity has been under debate for several decades, but the best available evidence suggests that high Cmin levels are indeed a risk factor for nephrotoxicity [33]. Additionally, the usefulness of daily AUC for predicting nephrotoxicity should be further investigated [3, 4].
Several studies have evaluated if patients receiving short empirical courses of gentamicin (mostly 1–2 days, sometimes 3–5 days) are at increased risk of nephrotoxicity, with conflicting results. Two studies found an increased risk of nephrotoxicity: one study in critically ill patients reported an adjusted odds ratio of 1.39 for renal failure in patients receiving empirical gentamicin add-on therapy for a median duration of 2 days compared with patients who did not receive gentamicin [150] and one study in cardiac surgery patients reported an adjusted odds ratio of 1.38 for AKI in patients receiving a single prophylactic dose of gentamicin compared with patients who received non-aminoglycoside prophylaxis [151]. In contrast, three studies in patients with bacteraemia [152,153,154], one in septic patients at the emergency department [155] and one in critically ill patients [83] did not find an increased risk of nephrotoxicity after short empirical courses of gentamicin.
Performing TDM to optimize dosing intervals has been proven effective in reducing nephrotoxicity in non-critically ill patients, whether using only Cmin monitoring, both Cmin and Cmax monitoring or more complex Bayesian models [71]. An RCT has shown that TDM, using Cmax and a random concentration or Cmin measurement after the first administration of gentamicin in a Bayesian model, reduced nephrotoxicity and duration of hospital stay in non-critically ill patients who were treated for >48 hours [156]. In critically ill patients, where increasing the dosing interval is often necessary to reach a Cmin ≤0.5–1 mg/L, the interval recommended by the Hartford nomogram was correct in only 62% of all cases when compared with Bayesian TDM based on a Cmax measurement and a measurement after 6 hours [58]. Although, to the best of our knowledge, there is no evidence that TDM reduces the risk of gentamicin nephrotoxicity in critically ill patients, we consider it prudent to perform TDM for optimization of the dosing interval in both critically and non-critically ill patients who receive more than one administration of gentamicin.
TDM using Cmax monitoring, with or without the use of Bayesian models, can also be used to increase the PTA in patients who show large variability in Cmax and AUC, particularly in critically ill patients (regardless of whether they are adult, child or neonate) and patients on IHD, as some of these patients are still at risk for underexposure despite a starting dose of 7 mg/kg. However, several studies evaluating TDM have shown an improvement of the PTA but no increase in clinical success [71]. As mentioned earlier, studies evaluating efficacy in critically ill patients have found no significant correlation between PK/PD target attainment and clinical outcome. Moreover, there is often high variability in Vd within the same patient over time, at least in the critically ill population, limiting the predictive value of one Cmax or AUC estimation for the next [66]. It is therefore unclear if performing TDM for optimization of Cmax and/or AUC is of clinical value in critically ill patients. But despite a lack of evidence, we think that performing TDM for optimization of the PK/PD target would be sensible in populations with large variability in Vd and CL.
Meanwhile, there is ongoing debate on the value of gentamicin as part of empirical combination therapy, usually combined with a broad-spectrum β-lactam antibiotic, especially for critically ill patients. Some observational studies found added clinical benefit of gentamicin for specific subpopulations [157,158,159] while others did not [150, 160, 161], and meta-analyses have shown conflicting conclusions [162, 163]. An RCT is needed to evaluate the clinical value of gentamicin in empirical combination therapy [164], which is currently being performed [165]. If used, gentamicin should be dosed once daily and empirical treatment duration should be restricted to 2–5 days [31, 166, 167].
11 Conclusion
A standard gentamicin starting dose of 7 mg/kg based on TBW (or on ABW in obese patients) appears to be the optimal strategy for increasing the PTA after the first administration in both adults and children older than 1 month, including critically ill patients, although we found no studies that showed a correlation between PK/PD target attainment and clinical success. Higher starting doses may further increase the PTA but evidence for improved clinical efficacy is lacking while the risk of nephrotoxicity is likely to increase. To reduce the risk of nephrotoxicity, the optimal dosing interval for each patient should be established using TDM, targeting a Cmin of at least <2 mg/L but preferably <0.5–1 mg/L. TDM to optimize the probability of PK/PD target attainment is advised for patients with highly variable pharmacokinetics, including patients from all subpopulations that are critically ill (such as elderly, children and neonates) and patients on IHD. Despite numerous recent PPK studies in specific subpopulations, the optimal PK/PD target for efficacy is still unclear for the clinical setting in which gentamicin is currently mostly used, that is, as part of short-term empirical combination therapy.
References
Chen C, Chen Y, Wu P, Chen B. Update on new medicinal applications of gentamicin: evidence-based review. J Formos Med Assoc. 2014;113(2):72–82. https://doi.org/10.1016/j.jfma.2013.10.002.
Pagkalis S, Mantadakis E, Mavros MN, Ammari C, Falagas ME. Pharmacological considerations for the proper clinical use of aminoglycosides. Drugs. 2011;71(17):2277–94. https://doi.org/10.2165/11597020-000000000-00000.
Llanos-Paez CC, Hennig S, Staatz CE. Population pharmacokinetic modelling, Monte Carlo simulation and semi-mechanistic pharmacodynamic modelling as tools to personalize gentamicin therapy. J Antimicrob Chemother. 2017;72(3):639–67. https://doi.org/10.1093/jac/dkw461.
Bland CM, Pai MP, Lodise TP. Reappraisal of contemporary pharmacokinetic and pharmacodynamic principles for informing aminoglycoside dosing. Pharmacotherapy. 2018;38(12):1229–38. https://doi.org/10.1002/phar.2193.
Matthews I, Kirkpatrick C, Holford N. Quantitative justification for target concentration intervention–parameter variability and predictive performance using population pharmacokinetic models for aminoglycosides. Br J Clin Pharmacol. 2004;58(1):8–19. https://doi.org/10.1111/j.1365-2125.2004.02114.x.
Xuan D, Nicolau DP, Nightingale CH. Population pharmacokinetics of gentamicin in hospitalized patients receiving once-daily dosing. Int J Antimicrob Agents. 2004;23(3):291–5. https://doi.org/10.1016/j.ijantimicag.2003.07.010.
Staatz CE, Byrne C, Thomson AH. Population pharmacokinetic modelling of gentamicin and vancomycin in patients with unstable renal function following cardiothoracic surgery. Br J Clin Pharmacol. 2006;61(2):164–76. https://doi.org/10.1111/j.1365-2125.2005.02547.x.
Rosario MC, Thomson AH, Jodrell DI, Sharp CA, Elliott HL. Population pharmacokinetics of gentamicin in patients with cancer. Br J Clin Pharmacol. 1998;46(3):229–36. https://doi.org/10.1046/j.1365-2125.1998.00779.x.
Chin PK, Florkowski CM, Begg EJ. The performances of the Cockcroft-Gault, modification of diet in renal disease study and chronic kidney disease epidemiology collaboration equations in predicting gentamicin clearance. Ann Clin Biochem. 2013;50(Pt 6):546–57. https://doi.org/10.1177/0004563213492320.
Lim AK, Mathanasenarajah G, Larmour I. Assessment of aminoglycoside dosing and estimated glomerular filtration rate in determining gentamicin and tobramycin area under the curve and clearance. Intern Med J. 2015;45(3):319–29. https://doi.org/10.1111/imj.12684.
Pai MP, Nafziger AN, Bertino JS Jr. Simplified estimation of aminoglycoside pharmacokinetics in underweight and obese adult patients. Antimicrob Agents Chemother. 2011;55(9):4006–11. https://doi.org/10.1128/aac.00174-11.
Prescott WA Jr. A survey of extended-interval aminoglycoside dosing practices in United States adult cystic fibrosis programs. Respir Care. 2014;59(9):1353–9. https://doi.org/10.4187/respcare.02980.
Smyth AR, Campbell EL. Prescribing practices for intravenous aminoglycosides in UK cystic fibrosis clinics: a questionnaire survey. J Cyst Fibros. 2014;13(4):424–7. https://doi.org/10.1016/j.jcf.2013.11.007.
Tabah A, De Waele J, Lipman J, Zahar JR, Cotta MO, Barton G, et al. The ADMIN-ICU survey: a survey on antimicrobial dosing and monitoring in ICUs. J Antimicrob Chemother. 2015;70(9):2671–7. https://doi.org/10.1093/jac/dkv165.
Verpooten GA, Giuliano RA, Verbist L, Eestermans G, De Broe ME. Once-daily dosing decreases renal accumulation of gentamicin and netilmicin. Clin Pharmacol Ther. 1989;45(1):22–7. https://doi.org/10.1038/clpt.1989.4.
Nagai J, Takano M. Entry of aminoglycosides into renal tubular epithelial cells via endocytosis-dependent and endocytosis-independent pathways. Biochem Pharmacol. 2014;90(4):331–7. https://doi.org/10.1016/j.bcp.2014.05.018.
The European Committee on Antimicrobial Susceptibility Testing. Rationale Document Gentamicin v2.0 2020 [updated 30/4/2020. Available from: https://www.eucast.org/fileadmin/src/media/PDFs/EUCAST_files/Rationale_documents/Gentamicin_rationale_1.2_0906.pdf.
Kashuba AD, Nafziger AN, Drusano GL, Bertino JS Jr. Optimizing aminoglycoside therapy for nosocomial pneumonia caused by gram-negative bacteria. Antimicrob Agents Chemother. 1999;43(3):623–9. https://doi.org/10.1128/aac.43.3.623.
Moore RD, Lietman PS, Smith CR. Clinical response to aminoglycoside therapy: importance of the ratio of peak concentration to minimal inhibitory concentration. J Infect Dis. 1987;155(1):93–9. https://doi.org/10.1093/infdis/155.1.93.
Moore RD, Smith CR, Lietman PS. Association of aminoglycoside plasma levels with therapeutic outcome in gram-negative pneumonia. Am J Med. 1984;77(4):657–62. https://doi.org/10.1016/0002-9343(84)90358-9.
United States Committee on Antimicrobial Susceptibility Testing. USCAST report Aminoglycoside In Vitro Susceptibility Test Interpretation Criteria Evaluations v1.3 2019 [updated 24/2/2019. Available from: https://app.box.com/s/1hxc8inf8u3rranwmk3efx48upvwt0ww.
Mouton JW, Jacobs N, Tiddens H, Horrevorts AM. Pharmacodynamics of tobramycin in patients with cystic fibrosis. Diagn Microbiol Infect Dis. 2005;52(2):123–7. https://doi.org/10.1016/j.diagmicrobio.2005.02.011.
Smith PF, Ballow CH, Booker BM, Forrest A, Schentag JJ. Pharmacokinetics and pharmacodynamics of aztreonam and tobramycin in hospitalized patients. Clin Ther. 2001;23(8):1231–44. https://doi.org/10.1016/s0149-2918(01)80103-x.
The European Committee on Antimicrobial Susceptibility Testing. Breakpoint tables for interpretation of MICs and zone diameters. Version 11.0 2021 [updated 01/01/2021. Available from: http://www.eucast.org.
Wie SH, Kim HW, Chang UI. Use of gentamicin for women with community-acquired uncomplicated acute pyelonephritis caused by gentamicin-susceptible or -resistant Escherichia coli: 10-year experience. Microb Drug Resist. 2013;19(4):316–22. https://doi.org/10.1089/mdr.2012.0140.
Wie SH, Kim HW, Chang UI. Effects of gentamicin monotherapy for the initial treatment of community-onset complicated non-obstructive acute pyelonephritis due to Enterobacteriaceae in elderly and non-elderly women. Clin Microbiol Infect. 2014;20(11):1211–8. https://doi.org/10.1111/1469-0691.12711.
The European Committee on Antimicrobial Susceptibility Testing. Guidance Document on Implementation and Use of the Revised Aminoglycoside Breakpoints 2020 [updated 2020/01/21. Available from: https://www.eucast.org/fileadmin/src/media/PDFs/EUCAST_files/Guidance_documents/Aminoglycoside_guidance_document_20200121.pdf.
Boselli E, Breilh D, Djabarouti S, Guillaume C, Rimmelé T, Gordien JB, et al. Reliability of mini-bronchoalveolar lavage for the measurement of epithelial lining fluid concentrations of tobramycin in critically ill patients. Intensive Care Med. 2007;33(9):1519–23. https://doi.org/10.1007/s00134-007-0688-x.
Carcas AJ, García-Satué JL, Zapater P, Frías-Iniesta J. Tobramycin penetration into epithelial lining fluid of patients with pneumonia. Clin Pharmacol Ther. 1999;65(3):245–50. https://doi.org/10.1016/s0009-9236(99)70103-7.
Turnidge J. Pharmacodynamics and dosing of aminoglycosides. Infect Dis Clin North Am. 2003;17(3):503–28. https://doi.org/10.1016/s0891-5520(03)00057-6.
Drusano GL, Ambrose PG, Bhavnani SM, Bertino JS, Nafziger AN, Louie A. Back to the future: using aminoglycosides again and how to dose them optimally. Clin Infect Dis. 2007;45(6):753–60. https://doi.org/10.1086/520991.
Yamada T, Fujii S, Shigemi A, Takesue Y. A meta-analysis of the target trough concentration of gentamicin and amikacin for reducing the risk of nephrotoxicity. J Infect Chemother. 2021;27(2):256–61. https://doi.org/10.1016/j.jiac.2020.09.033.
Paquette F, Bernier-Jean A, Brunette V, Ammann H, Lavergne V, Pichette V, et al. Acute kidney injury and renal recovery with the use of aminoglycosides: a large retrospective study. Nephron. 2015;131(3):153–60. https://doi.org/10.1159/000440867.
Raveh D, Kopyt M, Hite Y, Rudensky B, Sonnenblick M, Yinnon AM. Risk factors for nephrotoxicity in elderly patients receiving once-daily aminoglycosides. QJM. 2002;95(5):291–7. https://doi.org/10.1093/qjmed/95.5.291.
McCormack JP, Jewesson PJ. A critical reevaluation of the “therapeutic range” of aminoglycosides. Clin Infect Dis. 1992;14(1):320–39. https://doi.org/10.1093/clinids/14.1.320.
Murry KR, McKinnon PS, Mitrzyk B, Rybak MJ. Pharmacodynamic characterization of nephrotoxicity associated with once-daily aminoglycoside. Pharmacotherapy. 1999;19(11):1252–60. https://doi.org/10.1592/phco.19.16.1252.30876.
Rybak MJ, Abate BJ, Kang SL, Ruffing MJ, Lerner SA, Drusano GL. Prospective evaluation of the effect of an aminoglycoside dosing regimen on rates of observed nephrotoxicity and ototoxicity. Antimicrob Agents Chemother. 1999;43(7):1549–55. https://doi.org/10.1128/aac.43.7.1549.
Dong M, Rodriguez AV, Blankenship CA, McPhail G, Vinks AA, Hunter LL. Pharmacokinetic modelling to predict risk of ototoxicity with intravenous tobramycin treatment in cystic fibrosis. J Antimicrob Chemother. 2021;76(11):2923–31. https://doi.org/10.1093/jac/dkab288.
Prins JM, Büller HR, Kuijper EJ, Tange RA, Speelman P. Once versus thrice daily gentamicin in patients with serious infections. Lancet. 1993;341(8841):335–9. https://doi.org/10.1016/0140-6736(93)90137-6.
Beauchamp D, Labrecque G. Chronobiology and chronotoxicology of antibiotics and aminoglycosides. Adv Drug Deliv Rev. 2007;59(9–10):896–903. https://doi.org/10.1016/j.addr.2006.07.028.
Prins JM, Weverling GJ, van Ketel RJ, Speelman P. Circadian variations in serum levels and the renal toxicity of aminoglycosides in patients. Clin Pharmacol Ther. 1997;62(1):106–11. https://doi.org/10.1016/s0009-9236(97)90156-9.
Blunston MA, Yonovitz A, Woodahl EL, Smolensky MH. Gentamicin-induced ototoxicity and nephrotoxicity vary with circadian time of treatment and entail separate mechanisms. Chronobiol Int. 2015;32(9):1223–32. https://doi.org/10.3109/07420528.2015.1082483.
McKinney W, Yonovitz A, Smolensky MH. Circadian variation of gentamicin toxicity in rats. Laryngoscope. 2015;125(7):E252–6. https://doi.org/10.1002/lary.25116.
van Maarseveen E, Man WH, Proost J, Neef C, Touw D. Chronopharmacokinetics of once daily dosed aminoglycosides in hospitalized infectious patients. Int J Clin Pharm. 2015;37(2):342–7. https://doi.org/10.1007/s11096-015-0066-7.
Cobussen M, Stassen PM, Posthouwer D, van Tiel FH, Savelkoul PHM, Havenith T, et al. Improving peak concentrations of a single dose regime of gentamicin in patients with sepsis in the emergency department. PLoS ONE. 2019;14(1): e0210012. https://doi.org/10.1371/journal.pone.0210012.
Smit C, Wasmann RE, Goulooze SC, Hazebroek EJ, Van Dongen EPA, Burgers DMT, et al. A prospective clinical study characterizing the influence of morbid obesity on the pharmacokinetics of gentamicin: towards individualized dosing in obese patients. Clin Pharmacokinet. 2019;58(10):1333–43. https://doi.org/10.1007/s40262-019-00762-4.
Bauer LA, Edwards WA, Dellinger EP, Simonowitz DA. Influence of weight on aminoglycoside pharmacokinetics in normal weight and morbidly obese patients. Eur J Clin Pharmacol. 1983;24(5):643–7. https://doi.org/10.1007/bf00542215.
Leader WG, Tsubaki T, Chandler MH. Creatinine-clearance estimates for predicting gentamicin pharmacokinetic values in obese patients. Am J Hosp Pharm. 1994;51(17):2125–30.
Traynor AM, Nafziger AN, Bertino JS Jr. Aminoglycoside dosing weight correction factors for patients of various body sizes. Antimicrob Agents Chemother. 1995;39(2):545–8. https://doi.org/10.1128/aac.39.2.545.
Schwartz SN, Pazin GJ, Lyon JA, Ho M, Pasculle AW. A controlled investigation of the pharmacokinetics of gentamicin and tobramycin in obese subjects. J Infect Dis. 1978;138(4):499–505. https://doi.org/10.1093/infdis/138.4.499.
Korsager S. Administration o gentamicin to obese patients. Int J Clin Pharmacol Ther Toxicol. 1980;18(12):549–53.
Sketris I, Lesar T, Zaske DE, Cipolle RJ. Effect of obesity on gentamicin pharmacokinetics. J Clin Pharmacol. 1981;21(7):288–93. https://doi.org/10.1002/j.1552-4604.1981.tb01769.x.
Crass RL, Ross BE, Derstine BA, Lichty M, Sullivan JA, Su GL, et al. Measurement of skeletal muscle area improves estimation of aminoglycoside clearance across body size. Antimicrob Agents Chemother. 2018;62:6. https://doi.org/10.1128/aac.00441-18.
Ross AL, Tharp JL, Hobbs GR, McKnight R, Cumpston A. Evaluation of extended interval dosing aminoglycosides in the morbidly obese population. Adv Pharmacol Sci. 2013;2013: 194389. https://doi.org/10.1155/2013/194389.
Smit C, van Schip AM, van Dongen EPA, Brüggemann RJM, Becker ML, Knibbe CAJ. Dose recommendations for gentamicin in the real-world obese population with varying body weight and renal (dys)function. J Antimicrob Chemother. 2020;75(11):3286–92. https://doi.org/10.1093/jac/dkaa312.
Roberts JA, Lipman J. Pharmacokinetic issues for antibiotics in the critically ill patient. Crit Care Med. 2009;37(3):840–51. https://doi.org/10.1097/CCM.0b013e3181961bff.
Duong A, Simard C, Wang YL, Williamson D, Marsot A. Aminoglycosides in the intensive care unit: what is new in population PK modeling? Antibiotics (Basel). 2021;10:5. https://doi.org/10.3390/antibiotics10050507.
Buijk SE, Mouton JW, Gyssens IC, Verbrugh HA, Bruining HA. Experience with a once-daily dosing program of aminoglycosides in critically ill patients. Intensive Care Med. 2002;28(7):936–42. https://doi.org/10.1007/s00134-002-1313-7.
Marsot A, Hraiech S, Cassir N, Daviet F, Parzy G, Blin O, et al. Aminoglycosides in critically ill patients: which dosing regimens for which pathogens? Int J Antimicrob Agents. 2020;56(4): 106124. https://doi.org/10.1016/j.ijantimicag.2020.106124.
D’Arcy DM, Corrigan OI, Deasy E, Gowing CM, Donnelly MB. Gentamicin pharmacokinetics in critically ill patients during treatment with continuous venovenous haemodiafiltration (CVVHDF). Eur J Clin Pharmacol. 2015;71(3):377–8. https://doi.org/10.1007/s00228-014-1765-z.
Petejova N, Zahalkova J, Duricova J, Kacirova I, Brozmanova H, Urbanek K, et al. Gentamicin pharmacokinetics during continuous venovenous hemofiltration in critically ill septic patients. J Chemother. 2012;24(2):107–12. https://doi.org/10.1179/1120009x12z.0000000006.
Roberts JA, Field J, Visser A, Whitbread R, Tallot M, Lipman J, et al. Using population pharmacokinetics to determine gentamicin dosing during extended daily diafiltration in critically ill patients with acute kidney injury. Antimicrob Agents Chemother. 2010;54(9):3635–40. https://doi.org/10.1128/aac.00222-10.
Teigen MM, Duffull S, Dang L, Johnson DW. Dosing of gentamicin in patients with end-stage renal disease receiving hemodialysis. J Clin Pharmacol. 2006;46(11):1259–67. https://doi.org/10.1177/0091270006292987.
Veinstein A, Venisse N, Badin J, Pinsard M, Robert R, Dupuis A. Gentamicin in hemodialyzed critical care patients: early dialysis after administration of a high dose should be considered. Antimicrob Agents Chemother. 2013;57(2):977–82. https://doi.org/10.1128/aac.01762-12.
Venisse N, Dupuis A, Badin J, Robert R, Pinsard M, Veinstein A. Efficacy and safety of high-dose gentamicin re-dosing in ICU patients receiving haemodialysis. J Antimicrob Chemother. 2015;70(1):308–10. https://doi.org/10.1093/jac/dku369.
Hodiamont CJ, Janssen JM, de Jong MD, Mathôt RA, Juffermans NP, van Hest RM. Therapeutic drug monitoring of gentamicin peak concentrations in critically ill patients. Ther Drug Monit. 2017;39(5):522–30. https://doi.org/10.1097/ftd.0000000000000432.
Rea RS, Capitano B, Bies R, Bigos KL, Smith R, Lee H. Suboptimal aminoglycoside dosing in critically ill patients. Ther Drug Monit. 2008;30(6):674–81. https://doi.org/10.1097/FTD.0b013e31818b6b2f.
Hodiamont CJ, Juffermans NP, Bouman CS, de Jong MD, Mathôt RA, van Hest RM. Determinants of gentamicin concentrations in critically ill patients: a population pharmacokinetic analysis. Int J Antimicrob Agents. 2017;49(2):204–11. https://doi.org/10.1016/j.ijantimicag.2016.10.022.
Tang GJ, Tang JJ, Lin BS, Kong CW, Lee TY. Factors affecting gentamicin pharmacokinetics in septic patients. Acta Anaesthesiol Scand. 1999;43(7):726–30. https://doi.org/10.1034/j.1399-6576.1999.430707.x.
Ronchera-Oms CL, Tormo C, Ordovás JP, Abad J, Jiménez NV. Expanded gentamicin volume of distribution in critically ill adult patients receiving total parenteral nutrition. J Clin Pharm Ther. 1995;20(5):253–8. https://doi.org/10.1111/j.1365-2710.1995.tb00659.x.
Boyer A, Gruson D, Bouchet S, Clouzeau B, Hoang-Nam B, Vargas F, et al. Aminoglycosides in septic shock: an overview, with specific consideration given to their nephrotoxic risk. Drug Saf. 2013;36(4):217–30. https://doi.org/10.1007/s40264-013-0031-0.
Pai MP, Chen WZ, Garba A, Cui H, Zaffo B, El-Fawal HA, et al. Effects of obesity and sex on antimicrobial pharmacokinetics and acute kidney injury: validation of a preclinical model. Antimicrob Agents Chemother. 2013;57(2):716–22. https://doi.org/10.1128/aac.01194-12.
Udy AA, Roberts JA, Boots RJ, Paterson DL, Lipman J. Augmented renal clearance: implications for antibacterial dosing in the critically ill. Clin Pharmacokinet. 2010;49(1):1–16. https://doi.org/10.2165/11318140-000000000-00000.
Gomes A, van der Wijk L, Proost JH, Sinha B, Touw DJ. Pharmacokinetic modeling of gentamicin in treatment of infective endocarditis: model development and validation of existing models. PLoS ONE. 2017;12(5): e0177324. https://doi.org/10.1371/journal.pone.0177324.
Velissaris D, Karamouzos V, Marangos M, Pierrakos C, Karanikolas M. Pharmacokinetic changes and dosing modification of aminoglycosides in critically ill obese patients: a literature review. J Clin Med Res. 2014;6(4):227–33. https://doi.org/10.14740/jocmr1858w.
Allou N, Allyn J, Levy Y, Bouteau A, Caujolle M, Delmas B, et al. Assessment of the National French recommendations regarding the dosing regimen of 8mg/kg of gentamicin in patients hospitalised in intensive care units. Anaesth Crit Care Pain Med. 2016;35(5):331–5. https://doi.org/10.1016/j.accpm.2015.12.012.
Coste A, Deslandes G, Jalin L, Corvec S, Caillon J, Boutoille D, et al. PK/PD targets of amikacin and gentamicin in ICU patients. Med Mal Infect. 2020;50(8):709–14. https://doi.org/10.1016/j.medmal.2019.12.003.
Roger C, Nucci B, Louart B, Friggeri A, Knani H, Evrard A, et al. Impact of 30 mg/kg amikacin and 8 mg/kg gentamicin on serum concentrations in critically ill patients with severe sepsis. J Antimicrob Chemother. 2016;71(1):208–12. https://doi.org/10.1093/jac/dkv291.
Roger C, Louart B, Elotmani L, Barton G, Escobar L, Koulenti D, et al. An international survey on aminoglycoside practices in critically ill patients: the AMINO III study. Ann Intensive Care. 2021;11(1):49. https://doi.org/10.1186/s13613-021-00834-4.
Allou N, Charifou Y, Augustin P, Galas T, Valance D, Corradi L, et al. A study to evaluate the first dose of gentamicin needed to achieve a peak plasma concentration of 30 mg/l in patients hospitalized for severe sepsis. Eur J Clin Microbiol Infect Dis. 2016;35(7):1187–93. https://doi.org/10.1007/s10096-016-2652-6.
Fish DN, Kiser TH. Correlation of pharmacokinetic/pharmacodynamic-derived predictions of antibiotic efficacy with clinical outcomes in severely ill patients with Pseudomonas aeruginosa pneumonia. Pharmacotherapy. 2013;33(10):1022–34. https://doi.org/10.1002/phar.1310.
Grucz TM, Kruer RM, Bernice F, Lipsett PA, Dorman T, Sugrue D, et al. Aminoglycoside Dosing and Volume of Distribution in Critically Ill Surgery Patients. Surg Infect (Larchmt). 2020;21(10):859–64. https://doi.org/10.1089/sur.2020.012.
Picard W, Bazin F, Clouzeau B, Bui HN, Soulat M, Guilhon E, et al. Propensity-based study of aminoglycoside nephrotoxicity in patients with severe sepsis or septic shock. Antimicrob Agents Chemother. 2014;58(12):7468–74. https://doi.org/10.1128/aac.03750-14.
Cartin-Ceba R, Haugen EN, Iscimen R, Trillo-Alvarez C, Juncos L, Gajic O. Evaluation of “Loss” and “End stage renal disease” after acute kidney injury defined by the Risk, Injury, Failure, Loss and ESRD classification in critically ill patients. Intensive Care Med. 2009;35(12):2087–95. https://doi.org/10.1007/s00134-009-1635-9.
Cuhaci B. More data on epidemiology and outcome of acute kidney injury with AKIN criteria: benefits of standardized definitions, AKIN and RIFLE classifications. Crit Care Med. 2009;37(9):2659–61. https://doi.org/10.1097/CCM.0b013e3181ad76c2.
Drusano GL, Louie A. Optimization of aminoglycoside therapy. Antimicrob Agents Chemother. 2011;55(6):2528–31. https://doi.org/10.1128/aac.01314-10.
Friis-Hansen B. Body water compartments in children: changes during growth and related changes in body composition. Pediatrics. 1961;28:169–81.
Kearns GL, Abdel-Rahman SM, Alander SW, Blowey DL, Leeder JS, Kauffman RE. Developmental pharmacology–drug disposition, action, and therapy in infants and children. N Engl J Med. 2003;349(12):1157–67. https://doi.org/10.1056/NEJMra035092.
Crcek M, Zdovc J, Kerec KM. A review of population pharmacokinetic models of gentamicin in paediatric patients. J Clin Pharm Ther. 2019;44(5):659–74. https://doi.org/10.1111/jcpt.12850.
Medellín-Garibay SE, Rueda-Naharro A, Peña-Cabia S, García B, Romano-Moreno S, Barcia E. Population pharmacokinetics of gentamicin and dosing optimization for infants. Antimicrob Agents Chemother. 2015;59(1):482–9. https://doi.org/10.1128/aac.03464-14.
Bialkowski S, Staatz CE, Clark J, Lawson R, Hennig S. Gentamicin pharmacokinetics and monitoring in pediatric patients with febrile neutropenia. Ther Drug Monit. 2016;38(6):693–8. https://doi.org/10.1097/ftd.0000000000000341.
Llanos-Paez CC, Staatz CE, Lawson R, Hennig S. Differences in the pharmacokinetics of gentamicin between oncology and nononcology pediatric patients. Antimicrob Agents Chemother. 2020;64:2. https://doi.org/10.1128/aac.01730-19.
Zhang Y, Mehta N, Muhari-Stark E, Burckart GJ, van den Anker J, Wang J. Pediatric renal ontogeny and applications in drug development. J Clin Pharmacol. 2019;59(Suppl 1):S9-s20. https://doi.org/10.1002/jcph.1490.
Chen N, Aleksa K, Woodland C, Rieder M, Koren G. Ontogeny of drug elimination by the human kidney. Pediatr Nephrol. 2006;21(2):160–8. https://doi.org/10.1007/s00467-005-2105-4.
Hartman SJF, Brüggemann RJ, Orriëns L, Dia N, Schreuder MF, de Wildt SN. Pharmacokinetics and target attainment of antibiotics in critically ill children: a systematic review of current literature. Clin Pharmacokinet. 2020;59(2):173–205. https://doi.org/10.1007/s40262-019-00813-w.
Filler G, Foster J, Acker A, Lepage N, Akbari A, Ehrich JH. The Cockcroft-Gault formula should not be used in children. Kidney Int. 2005;67(6):2321–4. https://doi.org/10.1111/j.1523-1755.2005.00336.x.
Pierrat A, Gravier E, Saunders C, Caira MV, Aït-Djafer Z, Legras B, et al. Predicting GFR in children and adults: a comparison of the Cockcroft-Gault, Schwartz, and modification of diet in renal disease formulas. Kidney Int. 2003;64(4):1425–36. https://doi.org/10.1046/j.1523-1755.2003.00208.x.
Hayton WL. Maturation and growth of renal function: dosing renally cleared drugs in children. AAPS PharmSci. 2000;2(1):E3. https://doi.org/10.1208/ps020103.
Sutiman N, Koh JC, Watt K, Hornik C, Murphy B, Chan YH, et al. Pharmacokinetics alterations in critically ill pediatric patients on extracorporeal membrane oxygenation: a systematic review. Front Pediatr. 2020;8:260. https://doi.org/10.3389/fped.2020.00260.
Avedissian SN, Rohani R, Bradley J, Le J, Rhodes NJ. Optimizing aminoglycoside dosing regimens for critically ill pediatric patients with augmented renal clearance: a convergence of parametric and nonparametric population approaches. Antimicrob Agents Chemother. 2021;65:4. https://doi.org/10.1128/aac.02629-20.
Choi JJ, Moffett BS, McDade EJ, Palazzi DL. Altered gentamicin serum concentrations in obese pediatric patients. Pediatr Infect Dis J. 2011;30(4):347–9. https://doi.org/10.1097/INF.0b013e3181ff023e.
Natale S, Bradley J, Nguyen WH, Tran T, Ny P, La K, et al. Pediatric obesity: pharmacokinetic alterations and effects on antimicrobial dosing. Pharmacotherapy. 2017;37(3):361–78. https://doi.org/10.1002/phar.1899.
Sampson M, Cohen-Wolkowiez M, Benjamin D Jr, Capparelli E, Watt K. Pharmacokinetics of antimicrobials in obese children. GaBI J. 2013;2(2):76–81. https://doi.org/10.5639/gabij.2013.0202.025.
Saddi V, Preddy J, Dalton S, Connors J, Patterson S. Variation in gentamicin dosing and monitoring in pediatric units across new south wales. Pediatr Qual Saf. 2017;2(2): e015. https://doi.org/10.1097/pq9.0000000000000015.
Best EJ, Gazarian M, Cohn R, Wilkinson M, Palasanthiran P. Once-daily gentamicin in infants and children: a prospective cohort study evaluating safety and the role of therapeutic drug monitoring in minimizing toxicity. Pediatr Infect Dis J. 2011;30(10):827–32. https://doi.org/10.1097/INF.0b013e31821e405d.
Llanos-Paez CC, Staatz CE, Lawson R, Hennig S. A Population Pharmacokinetic Model of Gentamicin in Pediatric Oncology Patients To Facilitate Personalized Dosing. Antimicrob Agents Chemother. 2017;61(8) DOI: https://doi.org/10.1128/aac.00205-17.
Alsultan A, Abouelkheir M, Elsharawy Y, Alkoraishi A, Osman R, Neely MN, et al. Optimizing gentamicin dosing in pediatrics using monte carlo simulations. Pediatr Infect Dis J. 2019;38(4):390–5. https://doi.org/10.1097/inf.0000000000002120.
McDade EJ, Wagner JL, Moffett BS, Palazzi DL. Once-daily gentamicin dosing in pediatric patients without cystic fibrosis. Pharmacotherapy. 2010;30(3):248–53. https://doi.org/10.1592/phco.30.3.248.
Moffett BS, Kam C, Galati M, Schmees L, Stitt GA, Revell PA, et al. The “Ideal” body weight for pediatric gentamicin dosing in the era of obesity: a population pharmacokinetic analysis. Ther Drug Monit. 2018;40(3):322–9. https://doi.org/10.1097/ftd.0000000000000505.
Contopoulos-Ioannidis DG, Giotis ND, Baliatsa DV, Ioannidis JP. Extended-interval aminoglycoside administration for children: a meta-analysis. Pediatrics. 2004;114(1):e111–8. https://doi.org/10.1542/peds.114.1.e111.
Cooper AC, Commers AR, Finkelstein M, Lipnik PG, Tollefson LM, Wilcox RA, et al. Otoacoustic emission screen results in critically ill neonates who received gentamicin in the first week of life. Pharmacotherapy. 2011;31(7):649–57. https://doi.org/10.1592/phco.31.7.649.
Fuchs A, Guidi M, Giannoni E, Werner D, Buclin T, Widmer N, et al. Population pharmacokinetic study of gentamicin in a large cohort of premature and term neonates. Br J Clin Pharmacol. 2014;78(5):1090–101. https://doi.org/10.1111/bcp.12444.
Low YS, Tan SL, Wan AS. Extended-interval gentamicin dosing in achieving therapeutic concentrations in malaysian neonates. J Pediatr Pharmacol Ther. 2015;20(2):119–27. https://doi.org/10.5863/1551-6776-20.2.119.
Lulic-Botica M, Sheer T, Edwards D, Thomas RL, Natarajan G. Impact of small-for-gestational age (SGA) status on gentamicin pharmacokinetics in neonates. J Clin Pharmacol. 2014;54(1):39–45. https://doi.org/10.1002/jcph.190.
Germovsek E, Kent A, Metsvaht T, Lutsar I, Klein N, Turner MA, et al. Development and evaluation of a gentamicin pharmacokinetic model that facilitates opportunistic gentamicin therapeutic drug monitoring in neonates and infants. Antimicrob Agents Chemother. 2016;60(8):4869–77. https://doi.org/10.1128/aac.00577-16.
Bijleveld YA, van den Heuvel ME, Hodiamont CJ, Mathôt RA, de Haan TR. Population pharmacokinetics and dosing considerations for gentamicin in newborns with suspected or proven sepsis caused by gram-negative bacteria. Antimicrob Agents Chemother. 2017;61:1. https://doi.org/10.1128/aac.01304-16.
Bijleveld YA, de Haan TR, van der Lee HJ, Groenendaal F, Dijk PH, van Heijst A, et al. Altered gentamicin pharmacokinetics in term neonates undergoing controlled hypothermia. Br J Clin Pharmacol. 2016;81(6):1067–77. https://doi.org/10.1111/bcp.12883.
Frymoyer A, Meng L, Bonifacio SL, Verotta D, Guglielmo BJ. Gentamicin pharmacokinetics and dosing in neonates with hypoxic ischemic encephalopathy receiving hypothermia. Pharmacotherapy. 2013;33(7):718–26. https://doi.org/10.1002/phar.1263.
Rao SC, Srinivasjois R, Moon K. One dose per day compared to multiple doses per day of gentamicin for treatment of suspected or proven sepsis in neonates. Cochrane Database Syst Rev. 2016;12(12):5091. https://doi.org/10.1002/14651858.CD005091.pub4.
Alshaikh B, Dersch-Mills D, Taylor R, Akierman AR, Yusuf K. Extended interval dosing of gentamicin in premature neonates ≤ 28-week gestation. Acta Paediatr. 2012;101(11):1134–9. https://doi.org/10.1111/j.1651-2227.2012.02820.x.
Sundaram A, Alshaikh B, Dersch-Mills D, Dobry J, Akierman AR, Yusuf K. Extended-interval dosing of gentamicin in premature neonates born at <32 weeks’ gestation and >7 days of age. Clin Ther. 2017;39(6):1233–41. https://doi.org/10.1016/j.clinthera.2017.05.343.
Valitalo PA, van den Anker JN, Allegaert K, de Cock RF, de Hoog M, Simons SH, et al. Novel model-based dosing guidelines for gentamicin and tobramycin in preterm and term neonates. J Antimicrob Chemother. 2015;70(7):2074–7. https://doi.org/10.1093/jac/dkv052.
Kent A, Turner MA, Sharland M, Heath PT. Aminoglycoside toxicity in neonates: something to worry about? Expert Rev Anti Infect Ther. 2014;12(3):319–31. https://doi.org/10.1586/14787210.2014.878648.
Triggs E, Charles B. Pharmacokinetics and therapeutic drug monitoring of gentamicin in the elderly. Clin Pharmacokinet. 1999;37(4):331–41. https://doi.org/10.2165/00003088-199937040-00004.
Rohani R, Hoff B, Jain M, Philbrick A, Salama S, Cullina JF, et al. Defining the importance of age-related changes in drug clearance to optimizing aminoglycoside dosing regimens for adult patients with cystic fibrosis. Eur J Drug Metab Pharmacokinet. 2022;47(2):199–209. https://doi.org/10.1007/s13318-021-00734-9.
Johnston C, Hilmer SN, McLachlan AJ, Matthews ST, Carroll PR, Kirkpatrick CM. The impact of frailty on pharmacokinetics in older people: using gentamicin population pharmacokinetic modeling to investigate changes in renal drug clearance by glomerular filtration. Eur J Clin Pharmacol. 2014;70(5):549–55. https://doi.org/10.1007/s00228-014-1652-7.
Fraisse T, Gras Aygon C, Paccalin M, Vitrat V, De Wazieres B, Baudoux V, et al. Aminoglycosides use in patients over 75 years old. Age Ageing. 2014;43(5):676–81. https://doi.org/10.1093/ageing/afu023.
Chinzowu T, Roy S, Nishtala PS. Risk of antimicrobial-associated organ injury among the older adults: a systematic review and meta-analysis. BMC Geriatr. 2021;21(1):617. https://doi.org/10.1186/s12877-021-02512-3.
Dager WE, King JH. Aminoglycosides in intermittent hemodialysis: pharmacokinetics with individual dosing. Ann Pharmacother. 2006;40(1):9–14. https://doi.org/10.1345/aph.1G064.
Sowinski KM, Magner SJ, Lucksiri A, Scott MK, Hamburger RJ, Mueller BA. Influence of hemodialysis on gentamicin pharmacokinetics, removal during hemodialysis, and recommended dosing. Clin J Am Soc Nephrol. 2008;3(2):355–61. https://doi.org/10.2215/cjn.02920707.
Vercaigne LM, Ariano RE, Zacharias JM. Bayesian pharmacokinetics of gentamicin in a haemodialysis population. Clin Pharmacokinet. 2004;43(3):205–10. https://doi.org/10.2165/00003088-200443030-00004.
Amin NB, Padhi ID, Touchette MA, Patel RV, Dunfee TP, Anandan JV. Characterization of gentamicin pharmacokinetics in patients hemodialyzed with high-flux polysulfone membranes. Am J Kidney Dis. 1999;34(2):222–7. https://doi.org/10.1016/s0272-6386(99)70347-1.
Dager WE. Aminoglycoside elimination in extended duration hemodialysis. Ann Pharmacother. 2006;40(4):783–4. https://doi.org/10.1345/aph.1G420.
Agarwal R, Cronin RE. Heterogeneity in gentamicin clearance between high-efficiency hemodialyzers. Am J Kidney Dis. 1994;23(1):47–51. https://doi.org/10.1016/s0272-6386(12)80811-0.
Halpren BA, Axline SG, Coplon NS, Brown DM. Clearance of gentamicin during hemodialysis: comparison of four artificial kidneys. J Infect Dis. 1976;133(6):627–36. https://doi.org/10.1093/infdis/133.6.627.
Manley HJ, Bailie GR, McClaran ML, Bender WL. Gentamicin pharmacokinetics during slow daily home hemodialysis. Kidney Int. 2003;63(3):1072–8. https://doi.org/10.1046/j.1523-1755.2003.00819.x.
Decker BS, Mohamed AN, Chambers M, Kraus MA, Moe SM, Sowinski KM. Gentamicin pharmacokinetics and pharmacodynamics during short-daily hemodialysis. Am J Nephrol. 2012;36(2):144–50. https://doi.org/10.1159/000339937.
Zhuang L, He Y, Xia H, Liu Y, Sy SK, Derendorf H. Gentamicin dosing strategy in patients with end-stage renal disease receiving haemodialysis: evaluation using a semi-mechanistic pharmacokinetic/pharmacodynamic model. J Antimicrob Chemother. 2016;71(4):1012–21. https://doi.org/10.1093/jac/dkv428.
Cimino C, Burnett Y, Vyas N, Norris AH. Post-Dialysis Parenteral Antimicrobial Therapy in Patients Receiving Intermittent High-Flux Hemodialysis. Drugs. 2021;81(5):555–74. https://doi.org/10.1007/s40265-021-01469-2.
Franck B, Monchaud C, Saint-Marcoux F, Rérolle JP, Allard J, Allot V, et al. Population pharmacokinetics of gentamicin in haemodialysis patients: modelling, simulations and recommendations. Eur J Clin Pharmacol. 2020;76(7):947–55. https://doi.org/10.1007/s00228-020-02867-3.
Varghese JM, Roberts JA, Wallis SC, Boots RJ, Healy H, Fassett RG, et al. Pharmacokinetics of intraperitoneal gentamicin in peritoneal dialysis patients with peritonitis (GIPD study). Clin J Am Soc Nephrol. 2012;7(8):1249–56. https://doi.org/10.2215/cjn.12211211.
Pancorbo S, Comty C. Pharmacokinetics of gentamicin in patients undergoing continuous ambulatory peritoneal dialysis. Antimicrob Agents Chemother. 1981;19(4):605–7. https://doi.org/10.1128/aac.19.4.605.
Low CL, Bailie GR, Evans A, Eisele G, Venezia RA. Pharmacokinetics of once-daily IP gentamicin in CAPD patients. Perit Dial Int. 1996;16(4):379–84.
Keane WF, Everett ED, Golper TA, Gokal R, Halstenson C, Kawaguchi Y, et al. Peritoneal dialysis-related peritonitis treatment recommendations. 1993 update. The Ad Hoc Advisory Committee on Peritonitis Management. International Society for Peritoneal Dialysis. Perit Dial Int. 1993;13(1):14-28.
Lye WC, van der Straaten JC, Leong SO, Sivaraman P, Tan SH, Tan CC, et al. Once-daily intraperitoneal gentamicin is effective therapy for gram-negative CAPD peritonitis. Perit Dial Int. 1999;19(4):357–60.
Tang W, Cho Y, Hawley CM, Badve SV, Johnson DW. The role of monitoring gentamicin levels in patients with gram-negative peritoneal dialysis-associated peritonitis. Perit Dial Int. 2014;34(2):219–26. https://doi.org/10.3747/pdi.2012.00318.
Farkas A, Oikonomou K, Ghanbar M, Villasurda P, Varghese J, Lipman J, et al. Population pharmacokinetics of intraperitoneal gentamicin and the impact of varying dwell times on pharmacodynamic target attainment in patients with acute peritonitis undergoing peritoneal dialysis. Antimicrob Agents Chemother. 2022;66(2): e0167921. https://doi.org/10.1128/aac.01679-21.
Bukkems LH, Roger C, Hodiamont CJ, Lefrant JY, Juffermans NP, Roberts JA, et al. Predictive performance of a gentamicin population pharmacokinetic model in two western populations of critically ill patients. Int J Antimicrob Agents. 2018;52(2):218–25. https://doi.org/10.1016/j.ijantimicag.2018.04.016.
Moffett BS, Morris J, Galati M, Munoz FM, Arikan AA. Population pharmacokinetic analysis of gentamicin in pediatric extracorporeal membrane oxygenation. Ther Drug Monit. 2018;40(5):581–8. https://doi.org/10.1097/ftd.0000000000000547.
Ong DSY, Frencken JF, Klein Klouwenberg PMC, Juffermans N, van der Poll T, Bonten MJM, et al. Short-course adjunctive gentamicin as empirical therapy in patients with severe sepsis and septic shock: A prospective observational cohort study. Clin Infect Dis. 2017;64(12):1731–6. https://doi.org/10.1093/cid/cix186.
Nielsen DV, Fedosova M, Hjortdal V, Jakobsen CJ. Is single-dose prophylactic gentamicin associated with acute kidney injury in patients undergoing cardiac surgery? A matched-pair analysis. J Thorac Cardiovasc Surg. 2014;148(4):1634–9. https://doi.org/10.1016/j.jtcvs.2014.05.090.
Carlsen S, Boel J, Jarløv JO, Gjørup I, Søborg C, Arpi M. The effect of short-course gentamicin therapy on kidney function in patients with bacteraemia-a retrospective cohort study. Eur J Clin Microbiol Infect Dis. 2018;37(12):2307–12. https://doi.org/10.1007/s10096-018-3376-6.
Freundlich M, Thomsen RW, Pedersen L, West H, Schønheyder HC. Aminoglycoside treatment and mortality after bacteraemia in patients given appropriate empirical therapy: a Danish hospital-based cohort study. J Antimicrob Chemother. 2007;60(5):1115–23. https://doi.org/10.1093/jac/dkm354.
Spanggaard MH, Hønge BL, Schønheyder HC, Nielsen H. Short-term gentamicin therapy and risk of renal toxicity in patients with bacteraemia. Scand J Infect Dis. 2011;43(11–12):953–6. https://doi.org/10.3109/00365548.2011.601755.
Cobussen M, de Kort JM, Dennert RM, Lowe SH, Stassen PM. No increased risk of acute kidney injury after a single dose of gentamicin in patients with sepsis. Infect Dis (Lond). 2016;48(4):274–80. https://doi.org/10.3109/23744235.2015.1109136.
van Lent-Evers NA, Mathôt RA, Geus WP, van Hout BA, Vinks AA. Impact of goal-oriented and model-based clinical pharmacokinetic dosing of aminoglycosides on clinical outcome: a cost-effectiveness analysis. Ther Drug Monit. 1999;21(1):63–73. https://doi.org/10.1097/00007691-199902000-00010.
Kumar A, Zarychanski R, Light B, Parrillo J, Maki D, Simon D, et al. Early combination antibiotic therapy yields improved survival compared with monotherapy in septic shock: a propensity-matched analysis. Crit Care Med. 2010;38(9):1773–85. https://doi.org/10.1097/CCM.0b013e3181eb3ccd.
Martínez JA, Cobos-Trigueros N, Soriano A, Almela M, Ortega M, Marco F, et al. Influence of empiric therapy with a beta-lactam alone or combined with an aminoglycoside on prognosis of bacteremia due to gram-negative microorganisms. Antimicrob Agents Chemother. 2010;54(9):3590–6. https://doi.org/10.1128/aac.00115-10.
Liljedahl Prytz K, Prag M, Fredlund H, Magnuson A, Sundqvist M, Källman J. Antibiotic treatment with one single dose of gentamicin at admittance in addition to a β-lactam antibiotic in the treatment of community-acquired bloodstream infection with sepsis. PLoS ONE. 2020;15(7): e0236864. https://doi.org/10.1371/journal.pone.0236864.
Benetazzo L, Delannoy PY, Houard M, Wallet F, Lambiotte F, Vachée A, et al. Combination therapy with aminoglycoside in bacteremiasdue to ESBL-producing enterobacteriaceae in ICU. Antibiotics (Basel). 2020;9:11. https://doi.org/10.3390/antibiotics9110777.
Llitjos JF, Meslin S, Bredin S, Jamme M, Pène F. Aminoglycosides for the treatment of septic shock: a propensity-based study. Crit Care. 2020;24(1):567. https://doi.org/10.1186/s13054-020-03284-9.
Kumar A, Safdar N, Kethireddy S, Chateau D. A survival benefit of combination antibiotic therapy for serious infections associated with sepsis and septic shock is contingent only on the risk of death: a meta-analytic/meta-regression study. Crit Care Med. 2010;38(8):1651–64. https://doi.org/10.1097/CCM.0b013e3181e96b91.
Paul M, Lador A, Grozinsky-Glasberg S, Leibovici L. Beta lactam antibiotic monotherapy versus beta lactam-aminoglycoside antibiotic combination therapy for sepsis. Cochrane Database Syst Rev. 2014;2014(1):344. https://doi.org/10.1002/14651858.CD003344.pub3.
Ong DSY, van Werkhoven CH, Cremer OL, Thwaites GE, Bonten MJM. Is a randomized trial of a short course of aminoglycoside added to β-lactam antibiotics for empirical treatment in critically ill patients with sepsis justified? Clin Microbiol Infect. 2018;24(2):95–6. https://doi.org/10.1016/j.cmi.2017.09.020.
Netherlands trial register. Trial NL9429: short-course aminoglycosides as adjunctive treatment in adults with sepsis 2021 [Available from: https://www.trialregister.nl/trial/9429.
Avent ML, Rogers BA, Cheng AC, Paterson DL. Current use of aminoglycosides: indications, pharmacokinetics and monitoring for toxicity. Intern Med J. 2011;41(6):441–9. https://doi.org/10.1111/j.1445-5994.2011.02452.x.
Craig WA. Optimizing aminoglycoside use. Crit Care Clin. 2011;27(1):107–21. https://doi.org/10.1016/j.ccc.2010.11.006.
Author information
Authors and Affiliations
Corresponding author
Ethics declarations
Funding
No funding was received for this study.
Conflict of interest
CH, AvdB, SdV, JP, RM and RvH declare that they have no conflict of interest.
Ethics approval
Not applicable.
Consent to participate
Not applicable.
Consent for publication
Not applicable.
Code availability
Not applicable.
Availability of data and material
Available from the corresponding author upon reasonable request.
Author contributions
Literature search, data analysis and first drafts of subsections were performed by CH (general adult population, critically ill patients), AvdB (paediatric population, neonates) and SdV (obese patients, elderly patients, patients on intermittent haemodialysis or peritoneal dialysis) under supervision of RvH. CH drafted the first version of the manuscript. RvH, JP and RM critically revised the work. All authors approved the final submitted version of the manuscript.
Rights and permissions
Open Access This article is licensed under a Creative Commons Attribution-NonCommercial 4.0 International License, which permits any non-commercial use, sharing, adaptation, distribution and reproduction in any medium or format, as long as you give appropriate credit to the original author(s) and the source, provide a link to the Creative Commons licence, and indicate if changes were made. The images or other third party material in this article are included in the article's Creative Commons licence, unless indicated otherwise in a credit line to the material. If material is not included in the article's Creative Commons licence and your intended use is not permitted by statutory regulation or exceeds the permitted use, you will need to obtain permission directly from the copyright holder. To view a copy of this licence, visit http://creativecommons.org/licenses/by-nc/4.0/.
About this article
Cite this article
Hodiamont, C.J., van den Broek, A.K., de Vroom, S.L. et al. Clinical Pharmacokinetics of Gentamicin in Various Patient Populations and Consequences for Optimal Dosing for Gram-Negative Infections: An Updated Review. Clin Pharmacokinet 61, 1075–1094 (2022). https://doi.org/10.1007/s40262-022-01143-0
Accepted:
Published:
Issue Date:
DOI: https://doi.org/10.1007/s40262-022-01143-0