Abstract
The numerous advantages that nanotechnology can bring to the design of pharmaceutical delivery systems are perhaps nowhere better illustrated than in the area of cancer treatment. These nanostructures not only can improve the anti-proliferative properties of the drugs but also ameliorate the side effects by providing site-specific drug delivery. Furthermore, food-based proteins, due to their biocompatibility and biodegradability, provide a ready-made ingredient as a carrier for various chemotherapeutic agents. The most popular proteins in this field are milk proteins including β-lactoglobulin (β-LG), lactoferrin (LF), and the caseins (CN), all of which have desirable properties to make them ideal for this purpose. Grafting these two approaches, different milk protein-based nanodrugs have been synthesized that show promising potential in providing more targeted delivery of drugs thereby reducing the cytotoxic effects of chemotherapy. In some cases, being encapsulated in these proteins (in nanoscale), the chemotherapeutic agents can be consumed orally while enhancing site-specific delivery. This article reviews various nanodrug delivery systems containing milk proteins, which are designed for cancer treatment. Moreover, their physical and their anti-proliferative characteristics are briefly described.
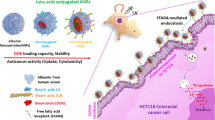
Graphic abstract



Similar content being viewed by others
References
Livney, Y.D.: Milk proteins as vehicles for bioactives. Cur. Opin. Coll. Interface. Sci. 15(1), 73–83 (2010). https://doi.org/10.1016/j.cocis.2009.11.002
Zimecki, M., Kruzel, M.L.: Milk-derived proteins and peptides of potential therapeutic and nutritive value. J. Exp. Ther. Oncol. 6(2), 89–106 (2007)
Jenness, R.: Biosynthesis and composition of milk. J. Invest. Dermatol. 63(1), 109–118 (1974). https://doi.org/10.1111/1523-1747.ep12678111
Dalgleish, D.G., Corredig, M.: The structure of the casein micelle of milk and its changes during processing. Ann. Rev. Food. Sci. Technol. 3, 449–467 (2012). https://doi.org/10.1146/annurev-food-022811-101214
Dickinson, E.: Surface and emulsifying properties of caseins. Res. J. Dairy Sci. 56(3), 471–477 (1989). https://doi.org/10.1017/S0022029900028958
Miller, M.J., Witherly, S.A., Clark, D.A.: Casein: a milk protein with diverse biologic consequences. Proc. Soc. Exp. Biol. Med. 195(2), 143–159 (1990). https://doi.org/10.3181/00379727-195-43129
Glantz, M., Devold, T.G., Vegarud, G.E., Lindmark Månsson, H., Stålhammar, H., Paulsson, M.: Importance of casein micelle size and milk composition for milk gelation. Int. J. Dairy Sci. 93(4), 1444–1451 (2010). https://doi.org/10.3168/jds.2009-2856
Vasbinder, A.J., Rollema, H.S., Bot, A., de Kruif, C.G.: Gelation mechanism of milk as influenced by temperature and pH; studied by the use of transglutaminase cross-linked casein micelles. Int. J. Dairy Sci. 86(5), 1556–1563 (2003). https://doi.org/10.3168/jds.S0022-0302(03)73741-2
Hoffman, J.R., Falvo, M.J.: Protein—which is best? J. Sports Sci. Med. 3(3), 118–130 (2004)
Madureira, A.R., Pereira, C.I., Gomes, A.M.P., Pintado, M.E., Xavier Malcata, F.: Bovine whey proteins—overview on their main biological properties. Food. Res. Int. 40(10), 1197–1211 (2007). https://doi.org/10.1016/j.foodres.2007.07.005
Smithers, G.W.: Whey and whey proteins—from ‘gutter-to-gold.’ Int. Dairy J. 18(7), 695–704 (2008). https://doi.org/10.1016/j.idairyj.2008.03.008
Davoodi, S.H., Shahbazi, R., Esmaeili, S., Sohrabvandi, S., Mortazavian, A., Jazayeri, S., Taslimi, A.: Health-related aspects of milk proteins. Iran. J. Pharm. Res. 15(3), 573–591 (2016)
Wu, L.C., Schulman, B.A., Peng, Z.Y., Kim, P.S.: Disulfide determinants of calcium-induced packing in alpha-lactalbumin. Biochemistry 35(3), 859–863 (1996). https://doi.org/10.1021/bi951408p
Layman, D.K., Lonnerdal, B., Fernstrom, J.D.: Applications for alpha-lactalbumin in human nutrition. Nutr. Rev. 76(6), 444–460 (2018). https://doi.org/10.1093/nutrit/nuy004
Kamau, S.M., Cheison, S.C., Chen, W., Liu, X.-M., Lu, R.-R.: Alpha-lactalbumin: its production technologies and bioactive peptides. Compr. Rev. Food Sci. Food Saf. 9(2), 197–212 (2010). https://doi.org/10.1111/j.1541-4337.2009.00100.x
Shafaei, Z., Ghalandari, B., Vaseghi, A., Divsalar, A., Haertle, T., Saboury, A.A., Sawyer, L.: beta-Lactoglobulin: an efficient nanocarrier for advanced delivery systems. Nanomedicine 13(5), 1685–1692 (2017). https://doi.org/10.1016/j.nano.2017.03.007
Wu, S.Y., Perez, M.D., Puyol, P., Sawyer, L.: beta-Lactoglobulin binds palmitate within its central cavity. J. Biol. Chem. 274(1), 170–174 (1999). https://doi.org/10.1074/jbc.274.1.170
Zimet, P., Livney, Y.: Beta-lactoglobulin and its nanocomplexes with pectin as vehicles for ω-3 polyunsaturated fatty acids. Food. Hydrocoll. 23, 1120–1126 (2009). https://doi.org/10.1016/j.foodhyd.2008.10.008
Dodin, G., Andrieux, M., Kabbani, H.A.: Binding of ellipticine to β-lactoglobulin. Eur. J. Biochem. 193(3), 697–700 (1990). https://doi.org/10.1111/j.1432-1033.1990.tb19389.x
Humphrey, W., Dalke, A., Schulten, K.: VMD: visual molecular dynamics. J. Mol. Graph. 14(1), 33–38 (1996). https://doi.org/10.1016/0263-7855(96)00018-5
Loch, J., Polit, A., Gorecki, A., Bonarek, P., Kurpiewska, K., Dziedzicka-Wasylewska, M., Lewinski, K.: Two modes of fatty acid binding to bovine beta-lactoglobulin-crystallographic and spectroscopic studies. J. Mol. Recognit. 24(2), 341–349 (2011). https://doi.org/10.1002/jmr.1084
Valenti, P., Berlutti, F., Conte, M.P., Longhi, C., Seganti, L.: Lactoferrin functions: current status and perspectives. J. Clin. Gastroenterol. 38(6 Suppl), S127-129 (2004). https://doi.org/10.1097/01.mcg.0000128941.46881.33
Chierici, R.: Antimicrobial actions of lactoferrin. Adv. Food. Nutr. Res. 10, 247–269 (2001). https://doi.org/10.1007/978-1-4615-0661-4_12
Zhang, Y., Lima, C.F., Rodrigues, L.R.: Anticancer effects of lactoferrin: underlying mechanisms and future trends in cancer therapy. Nutr. Rev. 72(12), 763–773 (2014). https://doi.org/10.1111/nure.12155
Brock, J.H.: The physiology of lactoferrin. Nanomed. NBM 80(1), 1–6 (2002). https://doi.org/10.1139/o01-212
Lim, L.Y., Koh, P.Y., Somani, S., Al Robaian, M., Karim, R., Yean, Y.L., Mitchell, J., Tate, R.J., Edrada-Ebel, R., Blatchford, D.R., Mullin, M., Dufès, C.: Tumor regression following intravenous administration of lactoferrin- and lactoferricin-bearing dendriplexes. Nanomed. NBM 11(6), 1445–1454 (2015). https://doi.org/10.1016/j.nano.2015.04.006
Golla, K., Bhaskar, C., Ahmed, F., Kondapi, A.: A target-specific oral formulation of doxorubicin–protein nanoparticles: efficacy and safety in hepatocellular cancer. J. Cancer. 4, 644–652 (2013). https://doi.org/10.7150/jca.7093
Moore, S.A., Anderson, B.F., Groom, C.R., Haridas, M., Baker, E.N.: Three-dimensional structure of diferric bovine lactoferrin at 2.8 A resolution. J. Mol. Biol. 274(2), 222–236 (1997). https://doi.org/10.1006/jmbi.1997.1386
Organization, W.H.: Cancer. (2019). https://www.who.int/cancer/resources/keyfacts/en/. Accessed 1 Dec 2019
Arruebo, M., Vilaboa, N., Sáez-Gutierrez, B., Lambea, J., Tres, A., Valladares, M., González-Fernández, A.: Assessment of the evolution of cancer treatment therapies. Cancers 3(3), 3279–3330 (2011). https://doi.org/10.3390/cancers3033279
Nurgali, K., Jagoe, R.T., Abalo, R.: Editorial: adverse effects of cancer chemotherapy: anything new to improve tolerance and reduce sequelae? Front. Pharmacol. 9, 245–245 (2018). https://doi.org/10.3389/fphar.2018.00245
Chakraborty, S., Rahman, T.: The difficulties in cancer treatment. Ecancermedicalscience 6, ed16 (2012). https://doi.org/10.3332/ecancer.2012.ed16
Housman, G., Byler, S., Heerboth, S., Lapinska, K., Longacre, M., Snyder, N., Sarkar, S.: Drug resistance in cancer: an overview. Cancers 6(3), 1769–1792 (2014). https://doi.org/10.3390/cancers6031769
Elshimali, Y.I., Wu, Y., Khaddour, H., Wu, Y., Gradinaru, D., Sukhija, H., Chung, S.S., Vadgama, J.V.: Optimization of cancer treatment through overcoming drug resistance. J. Cancer. Res. Clin. Oncol. 1(2), 107 (2018). https://doi.org/10.31021/jcro.20181107
Schirrmacher, V.: From chemotherapy to biological therapy: a review of novel concepts to reduce the side effects of systemic cancer treatment (review). Int. J. Oncol. 54(2), 407–419 (2019). https://doi.org/10.3892/ijo.2018.4661
Zhang, Q.-Y., Wang, F.-X., Jia, K.-K., Kong, L.-D.: Natural product interventions for chemotherapy and radiotherapy-induced side effects. Front. Pharmacol. 9, 1253–1253 (2018). https://doi.org/10.3389/fphar.2018.01253
Jansman, F.G., Sleijfer, D.T., de Graaf, J.C., Coenen, J.L., Brouwers, J.R.: Management of chemotherapy-induced adverse effects in the treatment of colorectal cancer. Drug. Saf. 24(5), 353–367 (2001). https://doi.org/10.2165/00002018-200124050-00002
Wang, X., Zhang, H., Chen, X.: Drug resistance and combating drug resistance in cancer. Cancer. Drug. Res. (2019). https://doi.org/10.20517/cdr.2019.10
Tran, S., DeGiovanni, P.-J., Piel, B., Rai, P.: Cancer nanomedicine: a review of recent success in drug delivery. CTM 6(1), 44–44 (2017). https://doi.org/10.1186/s40169-017-0175-0
Kumar, A., Kaur, H.: Sprayed in-situ synthesis of polyvinyl alcohol/chitosan loaded silver nanocomposite hydrogel for improved antibacterial effects. Int. J. Biol. Macromol. 145, 950–964 (2020). https://doi.org/10.1016/j.ijbiomac.2019.09.186
Kumar, A., Behl, T., Chadha, S.: A rationalized and innovative perspective of nanotechnology and nanobiotechnology in chronic wound management. J. Drug. Del. Sci. Technol. 60, 101930 (2020). https://doi.org/10.1016/j.jddst.2020.101930
Kumar, A., Sanjay, D., Jaiswal, M.: Enhanced intestinal permeability of Tinospora cordifolia extract through nanoemulsion formulation: in-vitro and ex-vivo studies. J. Nanopharm. Drug. Deliv. 2, 1–10 (2014)
Chadha, S., Kumar, A., Srivastava, S.A., Behl, T., Ranjan, R.: Inulin as a delivery vehicle for targeting colon-specific cancer. Curr. Drug Deliv. 17(8), 651–674 (2020). https://doi.org/10.2174/1567201817666200527133719
Arun, K., Tapan, B., Toshi, U., Swati, C.: Synthesis of nanostructured lipid carriers loaded chitosan/carbopol hybrid nanocomposite gel for oral delivery of artemether and curcumin. Pharm. Nanotechnol. 8(5), 418–432 (2020). https://doi.org/10.2174/2211738508666200907110444
Calzoni, E., Cesaretti, A., Polchi, A., Di Michele, A., Tancini, B., Emiliani, C.: Biocompatible polymer nanoparticles for drug delivery applications in cancer and neurodegenerative disorder therapies. J. Funct. Biomater. 10(1), 4 (2019). https://doi.org/10.3390/jfb10010004
Jadia, R., Scandore, C., Rai, P.: Nanoparticles for effective combination therapy of cancer. Int. J. Nanotechnol. Nanomed. (2016). https://doi.org/10.33140/IJNN/01/01/00003
Elzoghby, A.O., Samy, W.M., Elgindy, N.A.: Protein-based nanocarriers as promising drug and gene delivery systems. J. Control. Release 161(1), 38–49 (2012). https://doi.org/10.1016/j.jconrel.2012.04.036
Chen, L., Remondetto, G.E., Subirade, M.: Food protein-based materials as nutraceutical delivery systems. Trends. Food. Sci. Technol. 17(5), 272–283 (2006). https://doi.org/10.1016/j.tifs.2005.12.011
Shapira, A., Assaraf, Y.G., Livney, Y.D.: Beta-casein nanovehicles for oral delivery of chemotherapeutic drugs. Nanomedicine 6(1), 119–126 (2010). https://doi.org/10.1016/j.nano.2009.06.006
Bijari, N., Ghobadi, S., Derakhshandeh, K.: β-Lactoglobulin-irinotecan inclusion complex as a new targeted nanocarrier for colorectal cancer cells. Res. Pharm. Sci. 14(3), 216–227 (2019). https://doi.org/10.4103/1735-5362.258488
Farokhzad, O.C., Langer, R.: Impact of nanotechnology on drug delivery. ACS Nano 3(1), 16–20 (2009). https://doi.org/10.1021/nn900002m
Burgess, P., Hutt, P.B., Farokhzad, O.C., Langer, R., Minick, S., Zale, S.: On firm ground: IP protection of therapeutic nanoparticles. Biotechnol. Tech. 28(12), 1267–1270 (2010). https://doi.org/10.1038/nbt.1725
Choe, T.B., Park, I.C., Hong, S.I.: Enhancement of cationic liposome-mediated transfection by lactoferrin. Biotechnol. Tech. 12(7), 577–581 (1998). https://doi.org/10.1023/A:1008836110996
Salatin, S., Barar, J., Barzegar-Jalali, M., Adibkia, K., Kiafar, F., Jelvehgari, M.: Development of a nanoprecipitation method for the entrapment of a very water soluble drug into Eudragit RL nanoparticles. Res. Pharm. Sci. 12(1), 1–14 (2017). https://doi.org/10.4103/1735-5362.199041
Yadav, K.S., Sawant, K.K.: Modified nanoprecipitation method for preparation of cytarabine-loaded PLGA nanoparticles. AAPS Pharm. Sci. Tech. 11(3), 1456–1465 (2010). https://doi.org/10.1208/s12249-010-9519-4
Abdelmoneem, M.A., Mahmoud, M., Zaky, A., Helmy, M.W., Sallam, M., Fang, J.Y., Elkhodairy, K.A., Elzoghby, A.O.: Decorating protein nanospheres with lactoferrin enhances oral COX-2 inhibitor/herbal therapy of hepatocellular carcinoma. Nanomedicine 13(19), 2377–2395 (2018). https://doi.org/10.2217/nnm-2018-0134
Kanwar, J., Samarasinghe, R., Shegal, R., Kanwar, R.: Nano-lactoferrin in diagnostic, imaging and targeted delivery for cancer and infectious diseases. J. Cancer. Sci. Ther. 4, 31–42 (2012). https://doi.org/10.4172/1948-5956.1000107
Pang, Z., Feng, L., Hua, R., Chen, J., Gao, H., Pan, S., Jiang, X., Zhang, P.: Lactoferrin-conjugated biodegradable polymersome holding doxorubicin and tetrandrine for chemotherapy of glioma rats. Mol. Pharm. 7(6), 1995–2005 (2010). https://doi.org/10.1021/mp100277h
Chen, H., Tang, L., Qin, Y., Yin, Y., Tang, J., Tang, W., Sun, X., Zhang, Z., Liu, J., He, Q.: Lactoferrin-modified procationic liposomes as a novel drug carrier for brain delivery. Eur. J. Pharm. Sci. 40(2), 94–102 (2010). https://doi.org/10.1016/j.ejps.2010.03.007
Chen, H., Qin, Y., Zhang, Q., Jiang, W., Tang, L., Liu, J., He, Q.: Lactoferrin modified doxorubicin-loaded procationic liposomes for the treatment of gliomas. Eur. J. Pharm. Sci. 44(1–2), 164–173 (2011). https://doi.org/10.1016/j.ejps.2011.07.007
Kanwar, J.R., Mahidhara, G., Kanwar, R.K.: Novel alginate-enclosed chitosan-calcium phosphate-loaded iron-saturated bovine lactoferrin nanocarriers for oral delivery in colon cancer therapy. Nanomedicine 7(10), 1521–1550 (2012). https://doi.org/10.2217/nnm.12.29
Mahidhara, G., Kanwar, R.K., Roy, K., Kanwar, J.R.: Oral administration of iron-saturated bovine lactoferrin-loaded ceramic nanocapsules for breast cancer therapy and influence on iron and calcium metabolism. Int. J. Nanomed. 10, 4081–4098 (2015). https://doi.org/10.2147/IJN.S75877
Kanwar, J.R., Mahidhara, G., Roy, K., Sasidharan, S., Krishnakumar, S., Prasad, N., Sehgal, R., Kanwar, R.K.: Fe-bLf nanoformulation targets survivin to kill colon cancer stem cells and maintains absorption of iron, calcium and zinc. Nanomedicine 10(1), 35–55 (2015). https://doi.org/10.2217/nnm.14.132
Abdelmoneem, M.A., Elnaggar, M.A., Hammady, R.S., Kamel, S.M., Helmy, M.W., Abdulkader, M.A., Zaky, A., Fang, J.Y., Elkhodairy, K.A., Elzoghby, A.O.: Dual-targeted lactoferrin shell-oily core nanocapsules for synergistic targeted/herbal therapy of hepatocellular carcinoma. ACS Appl. Mat. Interfaces 11(30), 26731–26744 (2019). https://doi.org/10.1021/acsami.9b10164
Sabra, S.A., Elzoghby, A.O., Sheweita, S.A., Haroun, M., Helmy, M.W., Eldemellawy, M.A., Xia, Y., Goodale, D., Allan, A.L., Rohani, S.: Self-assembled amphiphilic zein-lactoferrin micelles for tumor targeted co-delivery of rapamycin and wogonin to breast cancer. Eur J Pharm Biopharm. 128, 156–169 (2018). https://doi.org/10.1016/j.ejpb.2018.04.023
Ko, S., Gunasekaran, S.: Preparation of sub-100-nm beta-lactoglobulin (BLG) nanoparticles. J. Microencapsul. 23(8), 887–898 (2006). https://doi.org/10.1080/02652040601035143
Sahoo, B.K., Ghosh, K.S., Dasgupta, S.: Investigating the binding of curcumin derivatives to bovine serum albumin. Biophys. Chem. 132(2), 81–88 (2008). https://doi.org/10.1016/j.bpc.2007.10.007
Barik, A., Mishra, B., Kunwar, A., Indira Priyadarsini, K.: Interaction of curcumin with human serum albumin: thermodynamic properties, fluorescence energy transfer and denaturation effects. Chem. Phys. Lett. 436(1), 239–243 (2007). https://doi.org/10.1016/j.cplett.2007.01.006
Mohammadi, F., Bordbar, A.K., Divsalar, A., Mohammadi, K., Saboury, A.A.: Interaction of curcumin and diacetylcurcumin with the lipocalin member beta-lactoglobulin. Protein J. 28(3–4), 117–123 (2009). https://doi.org/10.1007/s10930-009-9171-6
Divsalar, A., Zhila, I., Saboury, A.A., Nabiuni, M., Razmi, M., Mansuri-Torshizi, H.: Cytotoxic and spectroscopic studies on binding of a new synthesized bipyridine ethyl dithiocarbamate Pt(II) nitrate complex to the milk carrier protein of BLG. J. Iran. Chem. Soc. 10(5), 951–959 (2013). https://doi.org/10.1007/s13738-013-0232-6
Sneharani, A.H., Karakkat, J.V., Singh, S.A., Rao, A.G.: Interaction of curcumin with beta-lactoglobulin-stability, spectroscopic analysis, and molecular modeling of the complex. J. Agric. Food Chem. 58(20), 11130–11139 (2010). https://doi.org/10.1021/jf102826q
Teng, Z., Li, Y., Wang, Q.: Insight into curcumin-loaded β-lactoglobulin nanoparticles: incorporation, particle disintegration, and releasing profiles. J. Agric. Food Chem. 62(35), 8837–8847 (2014). https://doi.org/10.1021/jf503199g
Li, M., Cui, J., Ngadi, M.O., Ma, Y.: Absorption mechanism of whey-protein-delivered curcumin using Caco-2 cell monolayers. Food Chem. 180, 48–54 (2015). https://doi.org/10.1016/j.foodchem.2015.01.132
Aditya, N.P., Yang, H., Kim, S., Ko, S.: Fabrication of amorphous curcumin nanosuspensions using β-lactoglobulin to enhance solubility, stability, and bioavailability. Coll. Surf. B Biointerfaces 127, 114–121 (2015). https://doi.org/10.1016/j.colsurfb.2015.01.027
Divsalar, A., Saboury, A., Mansouri-Torshizi, H., Moosavi-Movahedi, A.: Binding properties of a new anti-tumor component (2,2′-bipyridin octylglycinato Pd(II) nitrate) with bovine β-lactoglobulin-A and -B. J. Biomol. Struct. Dyn. 25, 173–182 (2007). https://doi.org/10.1080/07391102.2007.10507166
Abazari, O., Divsalar, A., Ghobadi, R.: Inhibitory effects of oxali-platin as a chemotherapeutic drug on the function and structure of bovine liver catalase. J. Biomol. Struct. Dyn. 38(2), 609–615 (2020). https://doi.org/10.1080/07391102.2019.1581088
Mohammadgholi, A., Leilabadi-Asl, A., Divsalar, A., Eslami-Moghadam, M.: Multi-spectroscopic studies of the interaction of new synthesized platin complex with human carrier protein of serum albumin. J. Biomol. Struct. Dyn. 39, 1–6 (2020). https://doi.org/10.1080/07391102.2020.1745690
Divsalar, A., Saboury, A.A., Mansouri-Torshizi, H., Moghaddam, M.I., Ahmad, F., Hakimelahi, G.H.: Comparative studies on the interaction between bovine beta-lacto-globulin type A and B and a new designed Pd(II) complex with anti-tumor activity at different temperatures. J. Biomol. Struct. Dyn. 26(5), 587–597 (2009)
Divsalar, A., Saboury, A.A., Yousefi, R., Moosavi-Movahedi, A.A., Mansoori-Torshizi, H.: Spectroscopic and cytotoxic studies of the novel designed palladium(II) complexes: β-lactoglobulin and K562 as the targets. Int. J. Biol. Macromol. 40(4), 381–386 (2007). https://doi.org/10.1016/j.ijbiomac.2006.09.015
Divsalar, A., Saboury, A.A., Mansoori-Torshizi, H., Moosavi-Movahedi, A.A.: Binding properties of a new anti-tumor component (2,2’-bipyridin octylglycinato Pd(II) nitrate) with bovine beta-lactoglobulin-A and -B. J. Biomol. Struct. Dyn. 25(2), 173–182 (2007). https://doi.org/10.1080/07391102.2007.10507166
Divsalar, A., Saboury, A.A., Mansoori-Torshizi, H., Moghaddam, M.I., Ahmad, F., Hakimelahi, G.H.: Comparative studies on the interaction between bovine β-lacto-globulin type A and B and a new designed Pd(II) complex with anti-tumor activity at different temperatures. J. Biomol. Struct. Dyn. 26(5), 587–597 (2009). https://doi.org/10.1080/07391102.2009.10507274
Leilabadi-Asl, A., Divsalar, A., Saboury, A.A., Parivar, K.: Probing the interaction of two chemotherapeutic drugs of oxali-palladium and 5-fluorouracil simultaneously with milk carrier protein of β-lactoglobulin. J. Biomol. Struct. Dyn. 112, 422–432 (2018). https://doi.org/10.1016/j.ijbiomac.2018.01.067
Ghalandari, B., Divsalar, A., Saboury, A.A., Haertlé, T., Parivar, K., Bazl, R., Eslami-Moghadam, M., Amanlou, M.: Spectroscopic and theoretical investigation of oxali–palladium interactions with β-lactoglobulin. Spectrochim. Acta. A Mol. Biomol. Spectrosc. 118, 1038–1046 (2014). https://doi.org/10.1016/j.saa.2013.09.126
Ghalandari, B., Divsalar, A., Saboury, A.A., Parivar, K.: The new insight into oral drug delivery system based on metal drugs in colon cancer therapy through beta-lactoglobulin/oxali-palladium nanocapsules. J. Photochem. Photobiol. B. 140, 255–265 (2014). https://doi.org/10.1016/j.jphotobiol.2014.08.003
Divsalar, A., Saboury, A.A., Mansoori-Torshizi, H., Ahmad, F.: Design, synthesis, and biological evaluation of a new palladium(II) complex: β-lactoglobulin and K562 as targets. J. Phys. Chem. B. 114(10), 3639–3647 (2010). https://doi.org/10.1021/jp909143b
Divsalar, A., Barzegar, L., Behbehani, G.R.: Thermal study of a newly synthesized Cu(II) complex binding to bovine. J. Chem. 2013, 453056 (2013). https://doi.org/10.1155/2013/453056
Zheng, G., Liu, H., Zhu, Z., Zheng, J., Liu, A.: Selenium modification of beta-lactoglobulin (beta-Lg) and its biological activity. Food. Chem. 204, 246–251 (2016). https://doi.org/10.1016/j.foodchem.2016.01.016
Zhao, Y., Liu, Y., Wang, W., Wu, D., Shi, J., Liu, A.: Apoptosis and autophagy induction of seleno-β-lactoglobulin (Se-β-Lg) on hepatocellular carcinoma cells lines. J. Funct. Foods. 49, 412–423 (2018). https://doi.org/10.1016/j.jff.2018.09.011
Sun, S.-J., Feng, Y.-Y., Zhang, Y., Ji, H.-Y., Yu, J., Liu, A.-J.: Antitumor and immunoregulatory activities of seleno-β-lactoglobulin on S180 tumor-bearing mice. Molecules 23, 46 (2017). https://doi.org/10.3390/molecules23010046
Zheng, G.-Q., Ji, H.-Y., Zhang, S.-J., Yu, J., Liu, A.-J.: Selenious-β-lactoglobulin induces the apoptosis of human lung cancer A549 cells via an intrinsic mitochondrial pathway. Cytotechnology 70, 1551–1563 (2018). https://doi.org/10.1007/s10616-018-0248-y
Yu, J., Dong, X., Wang, L., Ji, H., Liu, A.: Antitumor effects of seleno-beta-lactoglobulin (Se-beta-Lg) against human gastric cancer MGC-803 cells. Eur. J. Pharmacol. 833, 109–115 (2018). https://doi.org/10.1016/j.ejphar.2018.05.042
Zhang, J., Teng, Z., Yuan, Y., Zeng, Q.Z., Lou, Z., Lee, S.H., Wang, Q.: Development, physicochemical characterization and cytotoxicity of selenium nanoparticles stabilized by beta-lactoglobulin. Int. J. Biol. Macromol. 107(Pt B), 1406–1413 (2018). https://doi.org/10.1016/j.ijbiomac.2017.09.117
Brauckmann, C., Wehe, C.A., Kieshauer, M., Lanvers-Kaminsky, C., Sperling, M., Karst, U.: The interaction of platinum-based drugs with native biologically relevant proteins. Anal. Bioanal. Chem. 405(6), 1855–1864 (2013). https://doi.org/10.1007/s00216-012-6410-z
Ghalandari, B., Divsalar, A., Eslami-Moghadam, M., Saboury, A.A., Haertle, T., Amanlou, M., Parivar, K.: Probing of the interaction between beta-lactoglobulin and the anticancer drug oxaliplatin. Appl. Biochem. Biotechnol. 175(2), 974–987 (2015). https://doi.org/10.1007/s12010-014-1341-0
Brauckmann, C., Faber, H., Lanvers-Kaminsky, C., Sperling, M., Karst, U.: Influence of cimetidine and its metabolites on cisplatin—investigation of adduct formation by means of electrochemistry/liquid chromatography/electrospray mass spectrometry. J. Chromatogr. A 1279, 49–57 (2013). https://doi.org/10.1016/j.chroma.2012.12.069
Izadi, Z., Divsalar, A., Saboury, A.A., Sawyer, L.: beta-Lactoglobulin-pectin nanoparticle-based oral drug delivery system for potential treatment of colon cancer. Chem Biol Drug Des. 88(2), 209–216 (2016). https://doi.org/10.1111/cbdd.12748
Jones, O., Decker, E.A., McClements, D.J.: Thermal analysis of β-lactoglobulin complexes with pectins or carrageenan for production of stable biopolymer particles. Food Hydrocoll. 24(2/3), 239–248 (2010). https://doi.org/10.1016/j.foodhyd.2009.10.001
Bijari, N., Ghobadi, S., Derakhshandeh, K.: Irinotecan binds to the internal cavity of beta-lactoglobulin: a multi-spectroscopic and computational investigation. Pharm. Res. 139, 109–115 (2017). https://doi.org/10.1016/j.jpba.2017.02.050
Langer, K., Balthasar, S., Vogel, V., Dinauer, N., von Briesen, H., Schubert, D.: Optimization of the preparation process for human serum albumin (HSA) nanoparticles. Int. J. Pharm. 257(1–2), 169–180 (2003). https://doi.org/10.1016/s0378-5173(03)00134-0
Jahanban-Esfahlan, A., Dastmalchi, S., Davaran, S.: A simple improved desolvation method for the rapid preparation of albumin nanoparticles. Int. J. Biol. Macromol. 91, 703–709 (2016). https://doi.org/10.1016/j.ijbiomac.2016.05.032
Rahimi Yazdi, S., Corredig, M.: Heating of milk alters the binding of curcumin to casein micelles. A fluorescence spectroscopy study. Food. Chem. 132(3), 1143–1149 (2012). https://doi.org/10.1016/j.foodchem.2011.11.019
Ghayour, N., Hosseini, S.M.H., Eskandari, M.H., Esteghlal, S., Nekoei, A.-R., Hashemi Gahruie, H., Tatar, M., Naghibalhossaini, F.: Nanoencapsulation of quercetin and curcumin in casein-based delivery systems. Food. Hydrocol. 87, 394–403 (2019). https://doi.org/10.1016/j.foodhyd.2018.08.031
Esmaili, M., Ghaffari, S.M., Moosavi-Movahedi, Z., Atri, M.S., Sharifizadeh, A., Farhadi, M., Yousefi, R., Chobert, J.-M., Haertlé, T., Moosavi-Movahedi, A.A.: Beta casein-micelle as a nano vehicle for solubility enhancement of curcumin; food industry application. LWT-Food Sci. Technol. 44(10), 2166–2172 (2011). https://doi.org/10.1016/j.lwt.2011.05.023
Priya, P., Mohan Raj, R., Vasanthakumar, V., Raj, V.: Curcumin-loaded layer-by-layer folic acid and casein coated carboxymethyl cellulose/casein nanogels for treatment of skin cancer. Arab. J. Chem. 13(1), 694–708 (2020). https://doi.org/10.1016/j.arabjc.2017.07.010
Bachar, M., Mandelbaum, A., Portnaya, I., Perlstein, H., Even-Chen, S., Barenholz, Y., Danino, D.: Development and characterization of a novel drug nanocarrier for oral delivery, based on self-assembled beta-casein micelles. J. Control. Release. 160(2), 164–171 (2012). https://doi.org/10.1016/j.jconrel.2012.01.004
Knepp, W.A., Jayakrishnan, A., Quigg, J.M., Sitren, H.S., Bagnall, J.J., Goldberg, E.P.: Synthesis, properties, and intratumoral evaluation of mitoxantrone-loaded casein microspheres in Lewis lung carcinoma. J. Pharm. Pharmacol. 45(10), 887–891 (1993). https://doi.org/10.1111/j.2042-7158.1993.tb05614.x
Latha, M.S., Latha, P.G., Subramoniam, A., Jayakrishnan, A.: Anti-tumor effect of mitoxantrone-loaded bovine casein microspheres on Ehrlich ascites carcinoma in mice. Drug. Deliv. 3(2), 75–79 (1996). https://doi.org/10.3109/10717549609031176
Shapira, A., Markman, G., Assaraf, Y.G., Livney, Y.D.: Beta-casein-based nanovehicles for oral delivery of chemotherapeutic drugs: drug-protein interactions and mitoxantrone loading capacity. Nanomedicine 6(4), 547–555 (2010). https://doi.org/10.1016/j.nano.2010.01.003
Shapira, A., Assaraf, Y.G., Epstein, D., Livney, Y.D.: Beta-casein nanoparticles as an oral delivery system for chemotherapeutic drugs: impact of drug structure and properties on co-assembly. Pharm. Res. 27(10), 2175–2186 (2010). https://doi.org/10.1007/s11095-010-0222-7
Shapira, A., Davidson, I., Avni, N., Assaraf, Y.G., Livney, Y.D.: beta-Casein nanoparticle-based oral drug delivery system for potential treatment of gastric carcinoma: stability, target-activated release and cytotoxicity. Eur. J. Pharm. Biopharm. 80(2), 298–305 (2012). https://doi.org/10.1016/j.ejpb.2011.10.022
Narayanan, S., Mony, U., Vijaykumar, D.K., Koyakutty, M., Paul-Prasanth, B., Menon, D.: Sequential release of epigallocatechin gallate and paclitaxel from PLGA-casein core/shell nanoparticles sensitizes drug-resistant breast cancer cells. Nanomed. NBM 11(6), 1399–1406 (2015). https://doi.org/10.1016/j.nano.2015.03.015
Elzoghby, A.O., Helmy, M.W., Samy, W.M., Elgindy, N.A.: Micellar delivery of flutamide via milk protein nanovehicles enhances its anti-tumor efficacy in androgen-dependent prostate cancer rat model. Pharm. Res. 30(10), 2654–2663 (2013). https://doi.org/10.1007/s11095-013-1091-7
Elzoghby, A.O., Saad, N.I., Helmy, M.W., Samy, W.M., Elgindy, N.A.: Ionically-crosslinked milk protein nanoparticles as flutamide carriers for effective anticancer activity in prostate cancer-bearing rats. Eur. J. Pharm. Biopharm. 85(3 Pt A), 444–451 (2013). https://doi.org/10.1016/j.ejpb.2013.07.003
Elzoghby, A.O., Helmy, M.W., Samy, W.M., Elgindy, N.A.: Novel ionically crosslinked casein nanoparticles for flutamide delivery: formulation, characterization, and in vivo pharmacokinetics. Int. J. Nanomed. 8, 1721–1732 (2013). https://doi.org/10.2147/ijn.S40674
Elgindy, N.A., Samy, W.A., Elzoghby, A.O.: Casein-based micelles: a novel vector for delivery of the poorly soluble anticancer drug, flutamide? Ther. Deliv. 5(1), 7–9 (2014). https://doi.org/10.4155/tde.13.122
Elzoghby, A.O., Helmy, M.W., Samy, W.M., Elgindy, N.A.: Spray-dried casein-based micelles as a vehicle for solubilization and controlled delivery of flutamide: formulation, characterization, and in vivo pharmacokinetics. Eur. J. Pharm. Biopharm. 84(3), 487–496 (2013). https://doi.org/10.1016/j.ejpb.2013.01.005
Gandhi, S., Roy, I.: Doxorubicin-loaded casein nanoparticles for drug delivery: preparation, characterization and in vitro evaluation. Int. J. Biol. Macromol. 121, 6–12 (2019). https://doi.org/10.1016/j.ijbiomac.2018.10.005
Huang, J., Shu, Q., Wang, L., Wu, H., Wang, A.Y., Mao, H.: Layer-by-layer assembled milk protein coated magnetic nanoparticle enabled oral drug delivery with high stability in stomach and enzyme-responsive release in small intestine. Biomaterials 39, 105–113 (2015). https://doi.org/10.1016/j.biomaterials.2014.10.059
Wang, D., Ma, B., Wang, Z., Zhao, Y., Sun, Y., Luan, Y., Wang, J.: Preparation and characterization of β-casein stabilized lipopeptide lyotropic liquid crystal nanoparticles for delivery of doxorubicin. Soft Matter 15(44), 9011–9017 (2019). https://doi.org/10.1039/C9SM01931F
Zhen, X., Wang, X., Xie, C., Wu, W., Jiang, X.: Cellular uptake, antitumor response and tumor penetration of cisplatin-loaded milk protein nanoparticles. Biomaterials 34(4), 1372–1382 (2013). https://doi.org/10.1016/j.biomaterials.2012.10.061
Huang, J., Qian, W., Wang, L., Wu, H., Zhou, H., Wang, A.Y., Chen, H., Yang, L., Mao, H.: Functionalized milk-protein-coated magnetic nanoparticles for MRI-monitored targeted therapy of pancreatic cancer. Int. J. Nanomed. 11, 3087–3099 (2016). https://doi.org/10.2147/ijn.S92722
Divsalar, A., Razmi, M., Saboury, A.A., Mansouri-Torshizi, H., Ahmad, F.: Biological evaluation of a new synthesized Pt(II) complex by cytotoxic and spectroscopic studies. Cell Biochem. Biophys. 71(3), 1415–1424 (2015). https://doi.org/10.1007/s12013-014-0364-z
Razmi, M., Divsalar, A.: The effect of Β-casein nanoparticles on bioavailability and cellular uptake of platinum complex as a cancer drug. Armaghane-danesh 18(9), 711–722 (2013)
Razmi, M., Divsalar, A., Saboury, A.A., Izadi, Z., Haertlé, T., Mansuri-Torshizi, H.: Beta-casein and its complexes with chitosan as nanovehicles for delivery of a platinum anticancer drug. Coll. Surf. B Biointerfaces 112, 362–367 (2013). https://doi.org/10.1016/j.colsurfb.2013.08.022
Divsalar, A., Razmi, M., Saboury, A.A., Seyedarabi, A.: The design and characterization of a novel beta-casein nano-vehicle loaded with platinum anticancer drug for drug delivery. Anticancer Agents Med. Chem. 14(6), 892–900 (2014). https://doi.org/10.2174/1871520614666140207123147
Liang, J., Gao, C., Zhu, Y., Ling, C., Wang, Q., Huang, Y., Qin, J., Wang, J., Lu, W., Wang, J.: Natural brain penetration enhancer-modified albumin nanoparticles for glioma targeting delivery. ACS Appl. Mater. Interfaces 10(36), 30201–30213 (2018). https://doi.org/10.1021/acsami.8b11782
Gao, C., Liang, J., Zhu, Y., Ling, C., Cheng, Z., Li, R., Qin, J., Lu, W., Wang, J.: Menthol-modified casein nanoparticles loading 10-hydroxycamptothecin for glioma targeting therapy. Acta. Pharm. Sin. B 9(4), 843–857 (2019). https://doi.org/10.1016/j.apsb.2019.01.006
Acknowledgements
The authors would like to thank the respectful Research Council of Kharazmi University for their financial support.
Author information
Authors and Affiliations
Corresponding author
Ethics declarations
Conflict of interest
The authors state that the content of this paper has strictly no conflict of interest.
Additional information
Publisher's Note
Springer Nature remains neutral with regard to jurisdictional claims in published maps and institutional affiliations.
Rights and permissions
About this article
Cite this article
Tavakoli, N., Divsalar, A., Haertlé, T. et al. Milk protein-based nanodelivery systems for the cancer treatment. J Nanostruct Chem 11, 483–500 (2021). https://doi.org/10.1007/s40097-021-00399-5
Received:
Accepted:
Published:
Issue Date:
DOI: https://doi.org/10.1007/s40097-021-00399-5