Abstract
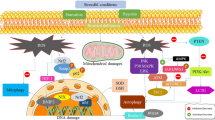
Systemic oxidative stress (SOS) has an important role in the mechanisms activation of neuronal death, involved in the neurodegenerative disease (ND) etiology. Brain is susceptible to oxidative stress injuries due to its high energy and metabolic request, therefore minimal imbalances of the redox state, as occurs in mitochondrial dysfunction, favour tissue injury and neuroinflammatory mechanisms activation. ND affect around the world about a billion people, without distinction of sex, educational level and economic status. Public measures generation that prevent ND from the SOS are possible promising therapeutic targets that could reduce the ND incidence. We discuss here the effects and mechanisms of SOS derived neurodegeneration, as well as the neuroinflammation repercussions for some cerebral structures.


Similar content being viewed by others
References
Torrell G. Enfermedades neurodegenerativas. Actualización en Medicina de Familia. 2015; 11(7): 374–383.
National Institute of Neurological Disorders and Stroke. Neurodegenerative diseases. 2017.
Noncommunicable Diseases Progress Monitor, 2017. Geneva: World Health Organization; 2017. Licence: CC BY-NC-SA 3.0 IGO. https://apps.who.int/iris/bitstream/handle/10665/258940/9789241513029-eng.pdf?sequence=1
Andersen J. (2004). Oxidative stress in neurodegeneration: cause or consequence? Nat Rev Neurosci. 10: S18–S25 https://doi.org/10.1038/nrn1434
Johri A, Beal MF. Mitochondrial dysfunction in neurodegenerative diseases. J Pharmacol Exp Ther. 2012; 342(3): 619–30 https://doi.org/10.1124/jpet.112.192138
Vitale G, Salvioli S, Franceschi C. Oxidative stress and the ageing endocrine system. Nat Rev Endocrinol. 2013; 9: 228–240 https://doi.org/10.1038/nrendo.2013.29
Hetz C, Saxena S. ER stress and the unfolded protein response in neurodegeneration. Nat Rev Neurol. 2017; 13: 477–491 https://doi.org/
Harman D. Aging: a theory based on free radical and radiation chemistry. Int J Gerontol. 1956; 11: 298–300.
Mechanick J, Hurley D, Garvey W. Adiposity-based chronic disease as a new diagnostic term: The American Association of Clinical Endocrinologists and American College of Endocrinology position statement. Endocrine Practice. 2017; 23(3): 372–378 https://doi.org/10.4158/EP161688.PS
Oliveira C, Villar-Delfino P, Dos Anjos P, Nogueira A. Cellular death, reactive oxygen species (ROS) and diabetic complications. Cell Death Dis. 2018; 9(119) https://doi.org/10.1038/s41419-017-0135-z.
Vaziri N, Rodríguez-Iturbide B. Mechanisms of Disease: oxidative stress and inflammation in the pathogenesis of hypertension. Nat Clin Prac Nephrol. 2006; 2: 582–593 https://doi.org/10.1038/ncpneph0283
Paschos A, Pandya R, Duivenvoorden WCM, Pinthus JH. Oxidative stress in prostate cancer: changing research concepts towards a novel paradigm for prevention and therapeutics. Prostate Cancer Prostatic Dis. 2013; 16: 217–225 https://doi.org/10.1038/pcan.2013.13
Roy-Sarkar S, Banerjee S. Gut microbiota in neurodegenerative disorders. J Neuroimmunol. 2019; 328(15): 98–104 https://doi.org/10.1016/jjneuroim.2019.01.004
Martine G, Diniz J. Economy, society and environment in the 21st century: three pillars or trilemma of sustainability?. Revista Brasileira de Estudos de População. 2015; 32(3): 433–459 https://doi.org/10.1590/S0102-3098201500000027
Monteiro C, Moubarac J, Cannon G, Ng S, Popkin B. Ultra-processed products are becoming dominant in the global food system. 2014; Obesity rev. 2: 21–28 https://doi.org/10.1111/obr.12107
Jovell AJ. The XXI century patient. Anales del Sistema Sanitario de Navarra. 2006; 29(3): 85–90.
Parimisetty A. Dorsemans AC, Awada R, Ravanan P, Diotel N, Lefebvre d’Hellencourt C. Secret talk between adipose tissueand central nervous system via secreted factors — an emerging frontier in the neurodegenerative research. J. Neuroinflammation. 2016; 13: 67 https://doi.org/10.1186/s12974-016-0530-x
Sies H. Oxidative stress: a concept in redox biology and medicine. Redox Biol. 2015; 4: 180–183 https://doi.org/10.1016/j.redox.2015.01.002
Orrenius S, Gogvadze V, Zhivotovsky B. Mitochondrial oxidative stress: implications for cell death. Annu Rev Pharmacol Toxicol. 2007; 47:143–183 https://doi.org/10.1146/annurev.pharmtox.47.120505.105122
Hernández A, Rull A, Rodríguez E, Riera M, Luciano F, Camps J, Menéndez J, Joven J. Mitochondrial Dysfunction: A Basic Mechanism in Inflammation-Related Non-Communicable Diseases and Therapeutic Opportunities. Mediators Inflamm. 2013; 1–13. https://doi.org/10.1155/2013/135698.
Schieber M, Chandel N. ROS Function in Redox Signaling and Oxidative Stress. Current Biol. 2014; 24(10): R453–R462 https://doi.org/10.1016/jxub.2014.03.034
Davis RE, Williams M. Mitochondrial function and dysfunction: an update. J Pharmacol Exp Ther. 2012; 342: 598–607 https://doi.org/10.1124/jpet.112.192104
Area-Gomez E, De Groof A, Bonilla E, Montesinos J, Tanji K, et al. A key role for MAM in mediating mitochondrial dysfunction in Alzheimer disease. Cell Death Dis. 2018; 9(335): 1–10 https://doi.org/10.1038/s41419-017-0215-0
Martínez-Leo E, Acevedo J, Segura M. Biopeptides with antioxidant and anti-inflammatory potential in the prevention and treatment of diabesity disease. Biomed Pharmacother. 2016; 83: 816–826 https://doi.org/10.1016/j.biopha.2016.07.051
Sies H, Berndt C, Jones D. Oxidative stress. Annu. Rev. Biochem. 2017; 86: 25.1–25.34 https://doi.org/10.1146/annurev-biochem-061516-045037
Pisoschi AM, Pop A. The role of antioxidants in the chemistry of oxidative stress: A review. Eur J Med Chem. 2015; 97(5): 55–74 https://doi.org/10.1016/j.ejmech.2015.04.040
Nissanka N, Moraes CT. Mitochondrial DNA damage and reactive oxygen species in neurodegenerative disease. FEBS Lett. 2018; 592(5): 728–742 https://doi.org/10.1002/1873-3468.12956.
Kim SY, Jeong JM, Kim S, Seo W, Kim MH, Choi WM, et al. Pro-inflammatory hepatic macrophages generate ROS through NADPH oxidase 2 via endocytosis of monomeric TLR4-MD2 complex. Nat Commun. 2017; 8 (2247) https://doi.org/10.1038/s41467-017-02325-2.
Kong MJ, Han SJ, Kim JI, Park JW, Park KM. Mitochondrial NADP+-dependent isocitrate dehydrogenase deficiency increases cisplatin-induced oxidative damage in the kidney tubule cells. Cell Death Dis. 2018; 9(488) https://doi.org/10.1038/s41419-018-0537-6.
Hu Q, Ren J, Li G, Wu J, Wu X, Wang G, Gu G, et al. The mitochondrially targeted antioxidant MitoQ protects the intestinal barrier by ameliorating mitochondrial DNA damage via the Nrf2/ARE signaling pathway. Cell Death Dis. 2018; 9(403) https://doi.org/10.1038/s41419-018-0436-x.
Mattson M, Magnus T. Ageing and neuronal vulnerability. Nat Rev Neurosci. 2006; 7: 278–294.
Guillemot-Legris O, Muccioli G. Obesity- induced neuroinflammation: Beyond the hypothalamus. Trends Neurosci. 2017; 40(4): 237–253.
Obermeier O, Daneman R, Ransohoff R. Development, maintenance and disruption of the blood-brain barrier. Nat Med. 2013; 19: 1584–1596.
Nzou G, Wicks RT, Wicks EE, Seale SA, Sane CH, Chen A, Murphy SV, et al. Human Cortex Spheroid with a Functional Blood Brain Barrier for High-Throughput Neurotoxicity Screening and Disease Modeling. Sci Rep. 2018; 8 (7413) https://doi.org/10.1038/s41598-018-25603-5
Forsberg SL, Ilieva M, Michel T. Epigenetics and cerebral organoids: promising directions in autism spectrum disorders. Transl Psychiatry. 2018; 8(14) https://doi.org/10.1038/s41398-017-0062-x
Baufeld C, Osterloh A, Prokop S, Miller K, Heppner F. High-fat diet-induced brain region specific phenotypic spectrum of CNS resident microglia. Acta Neuropathol. 2016; 132: 361–375 https://doi.org/10.1007/s00401-016-1595-4
Rhea E, Salameh T, Logsdon A, Hanson A, Erickson M, Banks W. Blood-Brain Barriers in Obesity. The AAPS Journal. 2017; 19(4): 921–930 https://doi.org/10.1208/s12248-017-0079-3
Lochhead J, McCaffrey G, Quigley C, Finch J, De Marco K. et al. Oxidative stress increases blood-brain barrier permeability and induces alterations in occluding during hypoxia-reoxygenation. J Cereb Blood Flow Metab. 2010; 30: 1625–1636 https://doi.org/10.1038/jcbfm.2010.29
McCaffrey G, Staatz WD, Quigley CA, Nametz N, Seelbach MJ, Campos CR, et al. Tight junctions contain oligomeric protein assembly critical for maintaining blood-brain barrier integrity in vivo. J Neurochem. 2007; 103(6): 2540–55 https://doi.org/10.1111/j.1471-4159.2007.04943.x
Walter JK, Rueckert C, Voss M, Mueller SL, Piontek J, Gast K, Blasig IE. The oligomerization of the coiled coil-domain of occludin is redox sensitive. Ann NY Acad Sci. 2009; 1165:19–27 https://doi.org/10.1111/j.1749-6632.2009.04058.x
Ouyang S, Hsuchou H, Kastin A, Wang Y, Yu C, Pan W. Diet-induced obesity suppresses expression of many proteins at the blood-brain barrier. J Cereb Blood Flow Metab. 2014; 34(1): 43–51.
Morel Y, Barouki R. Repression of gene expression by oxidative stress. Biochem J. 1999; 342: 481–496.
Tufekci K.U, Civi Bayin E, Genc S, Genc K. The Nrf2/ARE Pathway: A Promising Target to Counteract Mitochondrial Dysfunction in Parkinson’s Disease, Parkinsons Dis. 2011; 314082 https://doi.org/10.4061/2011/314082
Shrestha R, Millington O, Brewer J, Bushell T. Is Central Nervous System an Immune-Privileged site? Kathmandu University Med J. 2013; 41(1): 102–107.
Avena-Koenigsberger A, Misic B, Sporns O. Communication dynamics in complex brain networks. Nat Rev Neurosci. 2018; 19: 17–33 https://doi.org/10.1038/nrn.2017.149
Mizuno T. Neuron-microglia interactions in neuroinflammation. Clin Exp Neuroimmunol. 2015; 6: 225–231.
Moraes JC, Coope A, Morari J, Cintra DE, Roman EA, Pauli JR, et al. High-fat diet induces apoptosis of hypothalamic neurons. PLoS One. 2009; 4(4): e5045.
Chen W, Zhang X, Huang W. Role of neuroinflammation in neurodegenerative diseases. Mol Med Rep. 2016; 13: 3391–3396 https://doi.org/10.3892/mmr.2016.4948
Li T, Zhang S. Microgliosis in the Injured Brain: Infiltrating Cells and Reactive Microglia Both Play a Role. Neuroscientist. 2016; 22(2): 165–70 https://doi.org/10.1177/1073858415572079
Becher B, Spath S, Goverman J. Cytokine networks in neuroinflammation. Nat Rev Immunol. 2016; https://doi.org/10.1038/nri.2016.123
Zhang D, Hu X, Qian L, O’Callaghan J, Hong J. Astrogliosis in CNS pathologies: Is there a role for microglia?. Mol neurobiol. 2010; 41: 232–241 https://doi.org/10.1007/s12035-010-8098-4
Zhu W. Methylation of FOXO3 regulates neuronal cell death. Acta Pharmacol Sinica. 2012; 33: 577 https://doi.org/10.1038/aps.2012.48
Cai L, Wu X, Lv Y, Xu Y, Mi G, Li J. The neuroprotective and antioxidant activities of protein hydrolysates from grass carp (Ctenopharyngodon idella) skin. JFST. 2015; 52(6), 3750–3755 https://doi.org/10.1007/s13197-014-1438-z
Xie Q, Hao Y, Tao L, Peng S, Rao C, Chen H, You H, et al. Lysine methylation of FOXO3 regulates oxidative stress-induced neuronal cell death. EMBO Rep. 2012; 13: 371–377 https://doi.org/10.1038/embor.2012.25
Xin YJ, Yuan B, Yu B, Wang YQ, Wu JJ, Zhou WH, Qiu Z. Tet1-mediated DNA demethylation regulates neuronal cell death induced by oxidative stress. Sci Rep. 2015; 5 (7645): 1–9 https://doi.org/10.1038/srep07645
Mattson M. Apoptosis in neurodegenerative disorders. Nat Rev Mol Cell Biol. 2000; 1: 120–130 https://doi.org/10.1038/35040009
Zhang S, Tang M, Luo H, Shi C, Xu Y. Necroptosis in neurodegenerative diseases: a potential therapeutic target. Cell Death Dis. 2017; 8: e2905. https://doi.org/10.1038/cddis.2017.286.
Cusack C, Swahari V, Henley W, Ramsey M, Deshmukh M. Distinct pathways mediate axon degeneration during apoptosis and axon-specific pruning. Nat Commun. 2013; 4(1876): 1–11 https://doi.org/10.1038/ncomms2910
Sorrells S, Paredes M, Cebrian-Silla A, Sandoval K, Qi D, Kelley K. et al. Human hippocampal neurogenesis drops sharply in children to undetectable levels in adults. Letter. 2018; 1–5 https://doi.org/10.1038/nature25975.
Pelcastre D, Martínez-Leo E, Segura-Campos M. Functional and Biological Potential of Bioactive Compounds in Foods for the Dietary Treatment of Type 2 Diabetes Mellitus. In: Functional Food — Improve Health through Adequate Food, 1st edition. Ed. InTech; 2017.
Martínez-Leo E, Villavicencio T, Segura-Campos M. Functional Foods and Chemoprevention in Cancer. In: Grumezescu A, Holban AM, editors. Therapeutic Foods, 1st edition. Elsevier; 2017.
Martínez-Leo E, Rojas R, Segura-Campos M. Protective Effect of Omega 3 Fatty Acids EPA and DHA in the Neurodegenerative Disease. In Mérillon JM, Ramawat KG, editors. Bioactive Molecules in Food, 1st edition. Ed. Springer International. 2018.
Halliwell B. Free radicals and antioxidants — quo vadis?. Trends Pharmacol Sci. 2011; 32. 125–130 https://doi.org/10.1016/j.tips.2010.12.002
Potter A, Buck AC, Self WK, Callanan ME, Sunil S, Capadona JR. The effect of resveratrol on neurodegeneration and blood brain barrier stability surrounding intracortical microelectrodes. Biomaterials. 2013; 34:7001–7015 https://doi.org/10.1016/j.biomaterials.2013.05.035
Rodríguez C, Segura A, Del Mar M. Phenolic compounds as natural and multifunctional anti-obesity agents: A review. Crit Rev Food Sci Nutr. 2017; 20:1–18 https://doi.org/10.1080/10408398.2017.1399859
Dong W, Gao D, Lin H, Zhang X, Li N, Li F. New insights into mechanism for the effect of resveratrol preconditioning against cerebral ischemic stroke: possible role of matrix metalloprotease-9. Med Hypotheses. Medical Hypotheses. 2008; 70:52–55 https://doi.org/10.1016/j.mehy.2007.04.033
Shukitt-Hale B, Lau FC, Carey AN, Galli RL, Spangler EL, Ingram DK, Joseph JA. Blueberry polyphenols attenuate kainic acid-induced decrements in cognition and alter inflammatory gene expression in rat hippocampus. Nutr Neurosci. 2008; 11: 172–182 https://doi.org/10.1179/147683008X301487
Vauzour D. Dietary polyphenols as modulators of brain functions: biological actions and molecular mechanisms underpinning their beneficial effects. Oxid Med Cell Longev. 2012; 914273 https://doi.org/10.1155/2012/914273
Góngora JL. Caffeine as a preventive drug for Parkinson’s disease: epidemiologic evidence and experimental support. Rev Neurol. 2010; 50(4), 221–9.
Fehske CJ, Leuner K, Müller WE. Ginkgo biloba extract (EGb761®) influences monoaminergic neurotransmission via inhibition of NE uptake, but not MAO activity after chronic treatment. Pharmacol Res. 2009; 60: 68–77 https://doi.org/10.1016/j.phrs.2009.02.012
Grimm MO, Stahlmann CP, Mett J, Haupenthal VJ, Zimmer VC, et al. Vitamin E: Curse or benefit in Alzheimer’s disease? A systematic investigation of the impact of α-, γ- and δ-tocopherol on Aβ generation and degradation in neuroblastoma cells. J Nutr Health Aging. 2015; 19:646–654 https://doi.org/10.1007/s12603-015-0506-z.
Zbarsky V, Datla K, Parkar S, Rai D, Aruoma O, Dexter D. Neuroprotective properties of the natural phenolic antioxidants curcumin and naringenin but not quercetin and fisetin in a 6-OHDA model of Parkinson’s disease. Free Radical Res. 2005; 39: 1119–25 https://doi.org/10.1080/10715760500233113
Wu P, Zhang Z, Wang F, Che J. Natural compounds from traditional medicinal herbs in the treatment of cerebral ischemia/reperfusion injury. Acta Pharmacologica Sinica. 2010; 31: 1523–1531 https://doi.org/10.1038/aps.2010.186
Author information
Authors and Affiliations
Corresponding author
Ethics declarations
Conflict of Interest: The authors declare that they have no conflict of interest.
Rights and permissions
About this article
Cite this article
Martínez Leo, E.E., Segura Campos, M.R. Systemic Oxidative Stress: A Key Point in Neurodegeneration — A Review. J Nutr Health Aging 23, 694–699 (2019). https://doi.org/10.1007/s12603-019-1240-8
Received:
Accepted:
Published:
Issue Date:
DOI: https://doi.org/10.1007/s12603-019-1240-8