Abstract
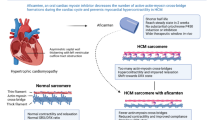
Cardiac transplantation is the best treatment available for patients with end-stage cardiomyopathy. Shortage of donor hearts is the main factor limiting the use of this treatment. Many donor hearts are rejected for transplantation because of left ventricular (LV) systolic dysfunction and/or wall motion abnormalities. While some donors have true cardiomyopathy, a significant proportion has reversible LV dysfunction due to neurogenic stunned myocardium. This condition is triggered by excess of catecholamines, which is typical for brain-dead donors. If given time to recover, LV function may improve, and the heart will be suitable for transplantation. Moreover, limiting of exogenous catecholamines may facilitate the recovery. In this review, we summarize the data on LV dysfunction/wall motion abnormalities in heart donors and propose the strategy to increase the utilization of donor hearts.


Similar content being viewed by others
References
Stehlik J, Edwards LB, Kucheryavaya AY, Benden C, Christie JD, Dipchand AI, Dobbels F, Kirk R, Rahmel AO, Hertz MI (2012) The registry of the international society for heart and lung transplantation: 29th official adult heart transplant report–2012. J Heart Lung Transplant Off Publ Int Soc Heart Transplant 31:1052–1064
Khush KK, Menza R, Nguyen J, Zaroff JG, Goldstein BA (2013) Donor predictors of allograft use and recipient outcomes after heart transplantation. Circ Heart Fail 6:300–309
Zaroff JG, Rosengard BR, Armstrong WF, Babcock WD, D’Alessandro A, Dec GW, Edwards NM, Higgins RS, Jeevanandum V, Kauffman M, Kirklin JK, Large SR, Marelli D, Peterson TS, Ring WS, Robbins RC, Russell SD, Taylor DO, Van Bakel A, Wallwork J, Young JB (2002) Consensus conference report: maximizing use of organs recovered from the cadaver donor: cardiac recommendations, March 28–29, 2001, crystal city, va. Circulation 106:836–841
Fukushima N, Ono M, Saito S, Saiki Y, Kubota S, Tanoue Y, Minami M, Konaka S, Ashikari J (2013) Japanese strategies to maximize heart and lung availabilities: experience from 100 consecutive brain-dead donors. Transpl Proc 45:2871–2874
Costanzo MR, Dipchand A, Starling R, Anderson A, Chan M, Desai S, Fedson S, Fisher P, Gonzales-Stawinski G, Martinelli L, McGiffin D, Smith J, Taylor D, Meiser B, Webber S, Baran D, Carboni M, Dengler T, Feldman D, Frigerio M, Kfoury A, Kim D, Kobashigawa J, Shullo M, Stehlik J, Teuteberg J, Uber P, Zuckermann A, Hunt S, Burch M, Bhat G, Canter C, Chinnock R, Crespo-Leiro M, Delgado R, Dobbels F, Grady K, Kao W, Lamour J, Parry G, Patel J, Pini D, Towbin J, Wolfel G, Delgado D, Eisen H, Goldberg L, Hosenpud J, Johnson M, Keogh A, Lewis C, O’Connell J, Rogers J, Ross H, Russell S, Vanhaecke J (2010) The international society of heart and lung transplantation guidelines for the care of heart transplant recipients. J Heart Lung Transplant Off Publ Int Soc Heart Transplant 29:914–956
Chamorro C, Romera MA, Silva JA, Valdivia M (2006) Ortega a [can heart donation exclusion factors be overcome?]. Rev Esp Cardiol 59:232–237
Venkateswaran RV, Bonser RS, Steeds RP (2005) The echocardiographic assessment of donor heart function prior to cardiac transplantation. Eur J Echocardiogr J Work Gr Echocardiogr Eur Soc Cardiol 6:260–263
Dujardin KS, McCully RB, Wijdicks EF, Tazelaar HD, Seward JB, McGregor CG, Olson LJ (2001) Myocardial dysfunction associated with brain death: clinical, echocardiographic, and pathologic features. J Heart Lung Transplant Off Publ Int Soc Heart Transplant 20:350–357
Zaroff JG, Babcock WD, Shiboski SC (2003) The impact of left ventricular dysfunction on cardiac donor transplant rates. J Heart Lung Transplant Off Publ Int Soc Heart Transplant 22:334–337
Novitzky D, Cooper DK, Rosendale JD, Kauffman HM (2006) Hormonal therapy of the brain-dead organ donor: experimental and clinical studies. Transplantation 82:1396–1401
Chiari P, Hadour G, Michel P, Piriou V, Rodriguez C, Budat C, Ovize M, Jegaden O, Lehot JJ, Ferrera R (2000) Biphasic response after brain death induction: prominent part of catecholamines release in this phenomenon. J Heart Lung Transplant Off Publ Int Soc Heart Transplant 19:675–682
Mertes PM, Carteaux JP, Jaboin Y, Pinelli G, el Abassi K, Dopff C, Atkinson J, Villemot JP, Burlet C, Boulange M (1994) Estimation of myocardial interstitial norepinephrine release after brain death using cardiac microdialysis. Transplantation 57:371–377
Shivalkar B, Van Loon J, Wieland W, Tjandra-Maga TB, Borgers M, Plets C, Flameng W (1993) Variable effects of explosive or gradual increase of intracranial pressure on myocardial structure and function. Circulation 87:230–239
Powner DJ, Hendrich A, Nyhuis A, Strate R (1992) Changes in serum catecholamine levels in patients who are brain dead. J Heart Lung Transplant Off Publ Int Soc Heart Transplant 11:1046–1053
Brouwers PJ, Westenberg HG, Van Gijn J (1995) Noradrenaline concentrations and electrocardiographic abnormalities after aneurysmal subarachnoid haemorrhage. J Neurol Neurosurg Psychiatr 58:614–617
Kawahara E, Ikeda S, Miyahara Y, Kohno S (2003) Role of autonomic nervous dysfunction in electrocardiographic abnormalities and cardiac injury in patients with acute subarachnoid hemorrhage. Circ J 67:753–756
Masuda T, Sato K, Yamamoto S, Matsuyama N, Shimohama T, Matsunaga A, Obuchi S, Shiba Y, Shimizu S, Izumi T (2002) Sympathetic nervous activity and myocardial damage immediately after subarachnoid hemorrhage in a unique animal model. Stroke J Cereb Circ 33:1671–1676
Guglin M, Novotorova I (2011) Neurogenic stunned myocardium and takotsubo cardiomyopathy are the same syndrome: a pooled analysis. Congest Heart Fail (Greenwich Conn) 17:127–132
Movahed A, Reeves WC, Mehta PM, Gilliland MG, Mozingo SL, Jolly SR (1994) Norepinephrine-induced left ventricular dysfunction in anesthetized and conscious, sedated dogs. Int J Cardiol 45:23–33
Allman FD, Herold W, Bosso FJ, Pilati CF (1998) Time-dependent changes in norepinephrine-induced left ventricular dysfunction and histopathologic condition. J Heart Lung Transplant Off Publ Int Soc Heart Transplant 17:991–997
Tung P, Kopelnik A, Banki N, Ong K, Ko N, Lawton MT, Gress D, Drew B, Foster E, Parmley W, Zaroff J (2004) Predictors of neurocardiogenic injury after subarachnoid hemorrhage. Stroke J Cerebr Circ 35:548–551
Offerhaus L, van Gool J (1969) Electrocardiographic changes and tissue catecholamines in experimental subarachnoid haemorrhage. Cardiovasc Res 3:433–440
Berman M, Ali A, Ashley E, Freed D, Clarke K, Tsui S, Parameshwar J, Large S (2010) Is stress cardiomyopathy the underlying cause of ventricular dysfunction associated with brain death? J Heart Lung Transplant Off Publ Int Soc Heart Transplant 29:957–965
Mori H, Ishikawa S, Kojima S, Hayashi J, Hoffman JI, Okino H (1993) Increased responsiveness of left ventricular apical myocardium to adrenergic stimuli. Cardiovasc Res 27:192–198
Abraham J, Mudd JO, Kapur NK, Klein K, Champion HC, Wittstein IS (2009) Stress cardiomyopathy after intravenous administration of catecholamines and beta-receptor agonists. J Am Coll Cardiol 53:1320–1325
Margey R, Diamond P, McCann H, Sugrue D (2009) Dobutamine stress echo-induced apical ballooning (takotsubo) syndrome. Eur J Echocardiogr J Work Gr Echocardiogr Eur Soc Cardiol 10:395–399
Mosley WJ, Manuchehry A, McEvoy C, Rigolin V (2010) Takotsubo cardiomyopathy induced by dobutamine infusion: A new phenomenon or an old disease with a new name. Echocardiogr Mt Kisco NY 27:E30–E33
Copetti R, Peric D, Amore G, Guglielmo N, Federici N, Cominotto F (2013) Transient takotsubo cardiomyopathy after cardiopulmonary resuscitation: a causal role of adrenaline? Resuscitation 84:e45–e46
Fulcher J, Wilcox I (2013) Basal stress cardiomyopathy induced by exogenous catecholamines in younger adults. Int J Cardiol 168:e158–e160
Quick S, Quick C, Schneider R, Sveric K, Katzke S, Strasser RH, Ibrahim K (2013) Guillain–Barre syndrome and catecholamine therapy. A potential risk for developing takotsubo cardiomyopathy? Int J Cardiol 165:e43–e44
Zaroff JG, Pawlikowska L, Miss JC, Yarlagadda S, Ha C, Achrol A, Kwok PY, McCulloch CE, Lawton MT, Ko N, Smith W, Young WL (2006) Adrenoceptor polymorphisms and the risk of cardiac injury and dysfunction after subarachnoid hemorrhage. Stroke J Cereb Circ 37:1680–1685
Nguyen H, Zaroff JG (2009) Neurogenic stunned myocardium. Curr Neurol Neurosci Rep 9:486–491
Banki N, Kopelnik A, Tung P, Lawton MT, Gress D, Drew B, Dae M, Foster E, Parmley W, Zaroff J (2006) Prospective analysis of prevalence, distribution, and rate of recovery of left ventricular systolic dysfunction in patients with subarachnoid hemorrhage. J Neurosurg 105:15–20
Ferrera R, Hadour G, Tamion F, Henry JP, Mulder P, Richard V, Thuillez C, Ovize M, Derumeaux G (2011) Brain death provokes very acute alteration in myocardial morphology detected by echocardiography: preventive effect of beta-blockers. Transplant Int Off J Eur Soc Organ Transplant 24:300–306
Khush KK, Menza R, Nguyen J, Goldstein BA, Zaroff JG, Drew BJ (2012) Electrocardiographic characteristics of potential organ donors and associations with cardiac allograft use. Circ Heart Fail 5:475–483
Wittstein IS, Thiemann DR, Lima JA, Baughman KL, Schulman SP, Gerstenblith G, Wu KC, Rade JJ, Bivalacqua TJ, Champion HC (2005) Neurohumoral features of myocardial stunning due to sudden emotional stress. New Engl J Med 352:539–548
Baroldi G, Silver MD, Lixfeld W, McGregor DC (1977) Irreversible myocardial damage resembling catecholamine necrosis secondary to acute coronary occlusion in dogs: its prevention by propranolol. J Mol Cell Cardiol 9:687–691
Frontera JA, Kalb T (2010) How i manage the adult potential organ donor: donation after neurological death (part 1). Neurocrit Care 12:103–110
Powner DJ, Hendrich A, Lagler RG, Ng RH, Madden RL (1990) Hormonal changes in brain dead patients. Crit Care Med 18:702–708
Gramm HJ, Meinhold H, Bickel U, Zimmermann J, von Hammerstein B, Keller F, Dennhardt R, Voigt K (1992) Acute endocrine failure after brain death? Transplantation 54:851–857
Masson F, Thicoipe M, Latapie MJ, Maurette P (1990) Thyroid function in brain-dead donors. Transplant Int Off J Eur Soc Organ Transplant 3:226–233
Novitzky D, Cooper DK, Reichart B (1987) Hemodynamic and metabolic responses to hormonal therapy in brain-dead potential organ donors. Transplantation 43:852–854
Roels L, Pirenne J, Delooz H, Lauwers P, Vandermeersch E (2000) Effect of triiodothyronine replacement therapy on maintenance characteristics and organ availability in hemodynamically unstable donors. Transpl Proc 32:1564–1566
Salim A, Vassiliu P, Velmahos GC, Sava J, Murray JA, Belzberg H, Asensio JA, Demetriades D (2001) The role of thyroid hormone administration in potential organ donors. Arch Surg (Chicago, Ill: 1960) 136:1377–1380
Jeevanandam V, Todd B, Regillo T, Hellman S, Eldridge C, McClurken J (1994) Reversal of donor myocardial dysfunction by triiodothyronine replacement therapy. J Heart Lung Transplant Off Publ Int Soc Heart Transplant 13:681–687 (discussion 685–687)
Jeevanandam V (1997) Triiodothyronine: spectrum of use in heart transplantation. Thyr Off J Am Thyr Assoc 7:139–145
Goarin JP, Cohen S, Riou B, Jacquens Y, Guesde R, Le Bret F, Aurengo A, Coriat P (1996) The effects of triiodothyronine on hemodynamic status and cardiac function in potential heart donors. Anesth Analg 83:41–47
Rosendale JD, Kauffman HM, McBride MA, Chabalewski FL, Zaroff JG, Garrity ER, Delmonico FL, Rosengard BR (2003) Aggressive pharmacologic donor management results in more transplanted organs. Transplantation 75:482–487
Rosendale JD, Kauffman HM, McBride MA, Chabalewski FL, Zaroff JG, Garrity ER, Delmonico FL, Rosengard BR (2003) Hormonal resuscitation yields more transplanted hearts, with improved early function. Transplantation 75:1336–1341
Macdonald PS, Aneman A, Bhonagiri D, Jones D, O’Callaghan G, Silvester W, Watson A, Dobb G (2012) A systematic review and meta-analysis of clinical trials of thyroid hormone administration to brain dead potential organ donors. Crit Care Med 40:1635–1644
Perez-Blanco A, Caturla-Such J, Canovas-Robles J, Sanchez-Paya J (2005) Efficiency of triiodothyronine treatment on organ donor hemodynamic management and adenine nucleotide concentration. Intensive Care Med 31:943–948
Randell TT, Hockerstedt KA (1992) Triiodothyronine treatment in brain-dead multiorgan donors—a controlled study. Transplantation 54:736–738
Venkateswaran RV, Steeds RP, Quinn DW, Nightingale P, Wilson IC, Mascaro JG, Thompson RD, Townend JN, Bonser RS (2009) The haemodynamic effects of adjunctive hormone therapy in potential heart donors: a prospective randomized double-blind factorially designed controlled trial. Eur Heart J 30:1771–1780
Pennefather SH, Bullock RE, Mantle D, Dark JH (1995) Use of low dose arginine vasopressin to support brain-dead organ donors. Transplantation 59:58–62
Yoshioka T, Sugimoto H, Uenishi M, Sakamoto T, Sadamitsu D, Sakano T, Sugimoto T (1986) Prolonged hemodynamic maintenance by the combined administration of vasopressin and epinephrine in brain death: a clinical study. Neurosurgery 18:565–567
Wood KE, Becker BN, McCartney JG, D’Alessandro AM, Coursin DB (2004) Care of the potential organ donor. N Engl J Med 351:2730–2739
Schnuelle P, Berger S, de Boer J, Persijn G, van der Woude FJ (2001) Donor employment of vasopressors and its impact on allograft survival after transplantation. Transpl Proc 33:1282–1283
Young JB, Naftel DC, Bourge RC, Kirklin JK, Clemson BS, Porter CB, Rodeheffer RJ, Kenzora JL (1994) Matching the heart donor and heart transplant recipient. clues for successful expansion of the donor pool: a multivariable, multiinstitutional report. the cardiac transplant research database group. J Heart Lung Transplant Off Publ Int Soc Heart Transplant 13:353–355 (discussion 364–355)
Nixon JL, Kfoury AG, Brunisholz K, Horne BD, Myrick C, Miller DV, Budge D, Bader F, Everitt M, Saidi A, Stehlik J, Schmidt TC, Alharethi R (2012) Impact of high-dose inotropic donor support on early myocardial necrosis and outcomes in cardiac transplantation. Clin Transplant 26:322–327
Paul JJ, Tani LY, Shaddy RE, Minich LL (2003) Spectrum of left ventricular dysfunction in potential pediatric heart transplant donors. J Heart Lung Transplant Off Publ Int Soc Heart Transplant 22:548–552
Zaroff JG, Rordorf GA, Ogilvy CS, Picard MH (2000) Regional patterns of left ventricular systolic dysfunction after subarachnoid hemorrhage: evidence for neurally mediated cardiac injury. J Am Soc Echocardiogr Off Publ Am Soc Echocardiogr 13:774–779
Grigoras I, Blaj M, Chelarescu O, Craus C, Florin G (2010) Functional improvement between brain death declaration and organ harvesting. Transpl Proc 42:147–149
Wheeldon DR, Potter CD, Oduro A, Wallwork J, Large SR (1995) Transforming the “unacceptable” donor: outcomes from the adoption of a standardized donor management technique. J Heart Lung Transplant Off Publ Int Soc Heart Transplant 14:734–742
Zaroff JG, Babcock WD, Shiboski SC, Solinger LL, Rosengard BR (2003) Temporal changes in left ventricular systolic function in heart donors: results of serial echocardiography. J Heart Lung Transplant Off Publ Int Soc Heart Transplant 22:383–388
Cantin B, Kwok BW, Chan MC, Valantine HA, Oyer PE, Robbins RC, Hunt SA (2003) The impact of brain death on survival after heart transplantation: time is of the essence. Transplantation 76:1275–1279
Mohamedali B, Bhat G, Zelinger A (2012) Frequency and pattern of left ventricular dysfunction in potential heart donors: implications regarding use of dysfunctional hearts for successful transplantation. J Am Coll Cardiol 60:235–236
Casartelli M, Bombardini T, Simion D, Gaspari MG, Procaccio F (2012) Wait, treat and see: echocardiographic monitoring of brain-dead potential donors with stunned heart. Cardiovasc Ultrasound 10:25
Bombardini T, Gherardi S, Leone O, Sicari R, Picano E (2013) Transplant of stunned donor hearts rescued by pharmacological stress echocardiography: a “proof of concept” report. Cardiovasc Ultrasound 11:27
Kono T, Nishina T, Morita H, Hirota Y, Kawamura K, Fujiwara A (1999) Usefulness of low-dose dobutamine stress echocardiography for evaluating reversibility of brain death-induced myocardial dysfunction. Am J Cardiol 84:578–582
Seiler C, Laske A, Gallino A, Turina M, Jenni R (1992) Echocardiographic evaluation of left ventricular wall motion before and after heart transplantation. J Heart Lung Transplant Off Publ Int Soc Heart Transplant 11:867–874
Novitzky D, Wicomb WN, Cooper DK, Rose AG, Reichart B (1986) Prevention of myocardial injury during brain death by total cardiac sympathectomy in the chacma baboon. Ann Thorac Surg 41:520–524
Cruickshank JM, Neil-Dwyer G, Degaute JP, Hayes Y, Kuurne T, Kytta J, Vincent JL, Carruthers ME, Patel S (1987) Reduction of stress/catecholamine-induced cardiac necrosis by beta 1-selective blockade. Lancet 2:585–589
Neil-Dwyer G, Cruickshank J, Stratton C (1986) Beta-blockers, plasma total creatine kinase and creatine kinase myocardial isoenzyme, and the prognosis of subarachnoid hemorrhage. Surg Neurol 25:163–168
Neil-Dwyer G, Walter P, Cruickshank JM, Doshi B, O’Gorman P (1978) Effect of propranolol and phentolamine on myocardial necrosis after subarachnoid haemorrhage. Br Med J 2:990–992
Mohamedali B, Bhat G, Tatooles A, Zelinger A (2014) Neurogenic stress cardiomyopathy in heart donors. J Card Fail 20:207–211
Conflict of interest
None of the co-authors have any conflicts of interest.
Author information
Authors and Affiliations
Corresponding author
Rights and permissions
About this article
Cite this article
Guglin, M. How to increase the utilization of donor hearts?. Heart Fail Rev 20, 95–105 (2015). https://doi.org/10.1007/s10741-014-9434-y
Published:
Issue Date:
DOI: https://doi.org/10.1007/s10741-014-9434-y