Abstract
Purpose
Stapled hemorrhoidopexy is designed to replace the hemorrhoids into the anal canal by excising the redundant rectal mucosa above the anorectal ring, thus resulting in an intrarectal suture. Few studies have evaluated rectal function after this procedure. This prospective study was designed to use the electronic barostat to assess whether rectal motor and sensory functions change after stapled hemorrhoidopexy.
Methods
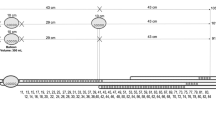
Ten patients (4 women, mean age, 46 ± 9 years) with third-degree and fourth-degree hemorrhoids who underwent stapled hemorrhoidopexy were studied. One week before and six months after surgery, they underwent three different rectal distensions (pressure-controlled stepwise, volume-controlled stepwise, and ramp) controlled by an electronic barostat.
Results
Rectal distensibility was significantly lower after surgery during pressure stepwise (P = 0.01), during volume stepwise (P = 0.006), and during ramp distension (P = 0.001). Volume thresholds for desire to defecate, urgency, and discomfort were significantly lower after surgery during all three distensions (P < 0.05). Volume threshold for first perception also was significantly lower after surgery during volume ramp distension (P = 0.01).
Conclusions
Rectal distensibility and volume thresholds for sensations decrease after stapled hemorrhoidopexy. These impairments persist for at least six months after surgery.




Similar content being viewed by others
References
Longo A. Treatment of hemorrhoidal disease by reduction of mucosa and hemorrhoidal prolapse with a circular stapling device: a new procedure. In: Proceedings of the 6th World Congress of Endoscopic Surgery. Rome: Monduzzi Editore, 1998:777–84.
Sutherland LM, Burchard AK, Matsuda K, et al. A systematic review of stapled hemorrhoidectomy. Arch Surg 2002;137:1395–406.
Nisar PJ, Acheson AG, Neal KR, Scholefield JH. Stapled hemorrhoidopexy compared with conventional hemorrhoidectomy. Systematic review of randomized, controlled trials. Dis Colon Rectum 2004;47:1837–45.
Lan P, Wu X, Zhou X, Wang J, Zhang L. The safety and efficacy of stapled hemorrhoidectomy in the treatment of hemorrhoids: a systematic review of ten randomized control trials. Int J Colorectal Dis 2006;21:172–8.
Jayaraman S, Colquhoun PH, Malthaner RA. Stapled versus conventional surgery for hemorrhoids. Cochrane Database Syst Rev 2006, Issue 4.
Tjandra JJ, Chan MK. Systematic review on the procedure for prolapse and hemorrhoids (stapled hemorrhoidopexy). Dis Colon Rectum 2007;50:878–92.
Longo A. Stapled anopexy and stapled hemorrhoidectomy: two concepts and procedures [letter]. Dis Colon Rectum 2002;45:571–2.
Pescatori M, Favetta U, Dedola S, Orsini S. Transanal stapled excision of rectal mucosal prolapse. Tech Coloproctol 1997;1:96–8.
Fantin AC, Hetzer FH, Christ AD, Fried M, Schwizer W. Influence of stapler hemorrhoidectomy on anorectal function and on patients’ acceptance. Swiss Med Wkly 2002;132:38–42.
Bharucha AE. Outcome measures for fecal incontinence: anorectal structure and function. Gastroenterology 2004;126:S90–98.
Mularczyk A, Contessini-Avesani E, Cesana B, Bianchi PA, Basilisco G. Local regulation of postprandial motor responses in ileal pouches. Gut 1999;45:575–80.
Corman ML, Gravié JF, Hager T, et al. Stapled haemorrhoidopexy: a consensus position paper by an international working party—indications, contra-indications and technique. Colorectal Dis 2003;5:304–10.
Orrom W, Hayashi A, Rusnak C, et al. Initial experience with stapled anoplasty in the operative management of prolapsing hemorrhoids and mucosal rectal prolapse. Am J Surg 2002;183:519–24.
Slawik S, Kenefick N, Greenslade GL, Dixon AR. A prospective evaluation of stapled haemorrhoidopexy/rectal mucosectomy in the management of 3rd and 4th degree haemorrhoids. Colorectal Dis 2007;9:352–6.
Kairaluoma M, Nuorva K, Kellokumpu I. Day-case stapled (circular) vs. diathermy hemorrhoidectomy: a randomized, controlled trial evaluating surgical and functional outcome. Dis Colon Rectum 2003;46:93–9.
Gravié JF, Lehur PA, Huten N, et al. Stapled hemorrhoidopexy versus Milligan-Morgan hemorrhoidectomy. A prospective, randomized, multicenter trial with 2-year postoperative follow up. Ann Surg 2005;242:29–35.
Zacharakis E, Kanellos D, Pramateftakis MG, et al. Long-term results after stapled haemorrhoidopexy for fourth-degree haemorrhoids: a prospective study with median follow-up of 6 years. Tech Coloproctol 2007;11:144–8.
Pessaux P, Tuech JJ, Laurent B, et al. Morbility after stapled haemorrhoidectomy: long-term results about 140 patients and review of the literature. Ann Chir 2004;129:571–7.
Pernice LM, Bartalucci B, Bencini L, Borri A, Catarzi S, Kröning K. Early and late (ten years) experience with circular stapler hemorrhoidectomy. Dis Colon Rectum 2001;44:836–41.
Correa-Rovelo JM, Tellez O, Obregon L, et al. Prospective study of factors affecting postoperative pain and symptom persistence after stapled rectal mucosectomy for hemorrhoids. A need for preservation of squamous epithelium. Dis Colon Rectum 2003;46:955–62.
Williams R, Kondylis L, Geisler D, Kondylis P. Stapled hemorrhoidopexy height as outcome indicator. Am J Surg 2007;193:336–40.
Longo A. Pain after stapled haemorrhoidectomy [letter]. Lancet 2000;356:2189–90.
Pescatori M. Pain after stapled haemorrhoidectomy [letter]. Lancet 2000;356:2188.
Ohana G, Myslovaty B, Ariche A, Dreznik Z, Koren R, Rath-Wolfson L. Mid-term results of stapled hemorrhoidopexy for third and fourth degree hemorrhoids. Correlation with the histological features of resected tissue. World J Surg 2007;31:1336–42.
George BD, Shetty D, Lindsey I, Mortensen NJ, Warren BF. Hystopathology of stapled hemorrhoidectomy specimens: a cautionary note. Colorectal Dis 2002;4:473–6.
Ortiz H, Marzo J, Armendariz P. Randomized clinical trial of stapler haemorrhopidopexy versus conventional diathermy haemorrhoidectomy. Br J Surg 2002;89:1376–81.
Cheetam MJ, Mortensen NJ, Nystrom PO, Kamm M, Phillips RK. Persistent pain and faecal urgency after stapled hemorrhoidectomy. Lancet 2000;356:730–3.
Altomare DF, Rinaldi M, Sallustio PL, Martino P, De Fazio M, Memeo V. Long-term effects of stapled haemorrhoidectomy on internal anal function and sensitivity. Br J Surg 2001;88:1487–91.
Ho YH, Cheong WK, Tsang C, et al. Stapled hemorrhoidectomy: cost and effectiveness. Randomized, controlled trial including incontinence scoring, anorectal manometry, and endoanal ultrasound assessments at up to three months. Dis Colon Rectum 2000;43:1666–75.
Kam MH, Mathur P, Peng XH, Seow-Choen F, Chew IW, Kumarasinghe MP. Correlation of hystology with anorectal function following stapled hemorrhoidectomy. Dis Colon Rectum 2005;48:1437–41.
Lane RH, Parks G. Function of the anal sphincters following colo-anal anastomosis. Br J Surg 1077;64:596–9.
Ganio E, Altomare DF, Milito G, Gabrielli F, Canuti S. Long-term outcome of a multicenter randomized clinical trial of stapled haemorrhoidopexy versus Milligan-Morgan haemorrhoidectomy. Br J Surg 2007;94:1033–7.
Van de Stadt J, D’Hoore A, Duinslaeger M, Chasse E, Penninckx F. Long-term results after excision haemorrhoidectomy versus stapled haemorrhoidopexy for prolapsing haemorrhoids; a Belgian prospective randomised trial. Acta Chir Belg 2005;105:44–52.
Boccasanta P, Venturi M, Salamina G, Cesana BM, Bernasconi F, Roviaro G. New trends in the surgical treatment of outlet obstruction: clinical and functional results of two novel transanal stapled techniques from a randomised controlled trial. Int J Colorectal Dis 2004;19:359–69.
Cooper ZR, Rose S. Fecal incontinence: a clinical approach. M Sinai J Med 2000;67:96–105.
Bharucha AE, Wald A, Enck P, Rao S. Functional anorectal disorders. Gastroenterology 2006;130:1510–8.
Author information
Authors and Affiliations
Corresponding author
About this article
Cite this article
De Nardi, P., Corsetti, M., Passaretti, S. et al. Evaluation of Rectal Sensory and Motor Function by Means of the Electronic Barostat After Stapled Hemorrhoidopexy. Dis Colon Rectum 51, 1255–1260 (2008). https://doi.org/10.1007/s10350-008-9349-6
Received:
Revised:
Accepted:
Published:
Issue Date:
DOI: https://doi.org/10.1007/s10350-008-9349-6