Abstract
Aims
The objective of this study was to compare the safety and efficacy outcomes of stapled hemorrhoidectomy (PPH) with Milligan–Morgan hemorrhoidectomy (MMH) in the treatment of severe hemorrhoids.
Methods
A meta-analysis pooled the effects of the safety and efficacy outcomes on PPH, and MMH in ten randomized control trials was presented using a fixed effects model or a random effects model (via RevMan Version 4.2).
Results
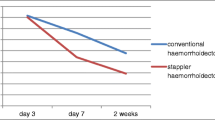
There was reasonably clear evidence in favor of PPH for operating time, length of hospital stay, pain, anal discharge, and patient satisfaction. However, skin tags and prolapse occurred at higher rates in the PPH group. PPH was not more superior than MMH as to postoperative bleeding, urinary retention, difficulty in defecating, anal fissure and stenosis, sphincter damage, resumption of normal activities, incontinence, pruritus, anal resting and squeeze pressures, and analgesia.
Conclusions
PPH may be at least as safe as MMH. However, the efficacy of PPH compared with MMH could not be determined absolutely. More rigorous studies with longer follow-up periods and larger sample sizes need to be conducted.
Similar content being viewed by others
References
Longo A (1998) Treatment of haemorrhoidal disease by reduction of mucosa and haemorrhoidal prolapse with a circular stapling device: a new procedure. In: Proceedings of the 6th World Congress of Endoscopic Surgery, Rome, Italy, pp 3–6
Milligan ETC, Morgan CN, Jones L et al (1937) Surgical anatomy of the anal canal and operative treatment of hemorrhoids. Lancet 2:1119–1124
Palimento D, Picchio M, Attanasio U et al (2003) Stapled and open hemorrhoidectomy: randomized controlled trial of early results. World J Surg 27:203–207
Smyth EF, Baker RP, Wilken BJ et al (2003) Stapled versus excision haemorrhoidectomy: long-term follow up of a randomized controlled trial. Lancet 361:1437–1438
Brown SR, Ballan K, Ho E et al (2001) Stapled mucosectomy for acute thrombosed circumferentially prolapsed piles: a prospective randomized comparison with conventional haemorrhoidectomy. Colorectal Dis 3:175–178
Ganio E, Altomare DF, Gabrielli F et al (2001) Prospective randomized multicentre trial comparing stapled with open haemorrhoidectomy. Br J Surg 88:669–674
Shalaby R, Desoky A (2001) Randomized clinical trial of stapled versus Milligan–Morgan haemorrhoidectomy. Br J Surg 88:1049–1053
Pavlidis T, Papaziogas B, Souparis A et al (2002) Modern stapled Longo procedure vs. conventional Milligan–Morgan hemorrhoidectomy: a randomized controlled trial. Int J Colorectal Dis 17:50–53
Mehigan BJ, Monson JRT, Hartley JE (2000) Stapling procedure for haemorrhoids vs. Milligan–Morgan haemorrhoidectomy: randomised controlled trial. Lancet 355:782–785
Wilson MS, Pope V, Doran HE et al (2002) Objective comparison of stapled anopexy and open hemorrhoidectomy: a randomized, controlled trial. Dis Colon Rectum 45:1437–1444
Racalbuto A, Aliotta I, Corsaro G et al (2001) Hemorrhoidal stapler prolapsectomy vs. Milligan–Morgan hemorrhoidectomy: a long-term randomized trial. Int J Colorectal Dis 19:239–244
Krska Z, Kvasnieka J, Faltyn J et al (2003) Surgical treatment of haemorrhoids according to Longo and Milligan–Morgan: an evaluation of postoperative tissue response. Colorectal Dis 5:573–576
Nisar PJ, Scholefield JH (2003) Clinical review: managing haemorrhoids. BMJ 327:845–851
Author information
Authors and Affiliations
Corresponding author
Rights and permissions
About this article
Cite this article
Lan, P., Wu, X., Zhou, X. et al. The safety and efficacy of stapled hemorrhoidectomy in the treatment of hemorrhoids: a systematic review and meta-analysis of ten randomized control trials. Int J Colorectal Dis 21, 172–178 (2006). https://doi.org/10.1007/s00384-005-0786-6
Accepted:
Published:
Issue Date:
DOI: https://doi.org/10.1007/s00384-005-0786-6