Abstract
Purpose
Recombinant granulocyte colony-stimulating factors (rG-CSFs), such as filgrastim, are administered to prevent complications in patients receiving chemotherapy. In Europe, a biosimilar to filgrastim, tevagrastim/ratiograstim/biograstim, was approved in 2008. In the USA, the same product was approved as tbo-filgrastim under a 351(a) biologic license application in 2012 with the brand name Granix®. Postmarket surveillance remains a priority for monitoring the safety of biologics and biosimilars to identify rare and immunogenicity-related events. We report the global and US pharmacovigilance data for tevagrastim/ratiograstim/biograstim and tbo-filgrastim, respectively.
Methods
Cumulative exposure and adverse event data from initial approval in Europe to December 31, 2016, were collected globally from spontaneous reports submitted by healthcare professionals and consumers, scientific literature, competent authorities, and solicited case reports from non-interventional studies. A separate search was conducted on the global data set to identify reports originating from the USA and Puerto Rico to describe the US experience.
Results
Overall, the global safety profile of tevagrastim/ratiograstim/biograstim in the postmarket, real-world setting was comparable to clinical trial experience. Postmarket safety experience of tbo-filgrastim in the USA was consistent with global data. The most common SAEs were febrile neutropenia and decreased white blood cell count. The most common non-serious event was bone pain. There was no evidence of immunogenicity.
Conclusions
This pharmacovigilance analysis indicates that postmarket experience of tevagrastim/ratiograstim/biograstim and tbo-filgrastim is consistent with clinical trials. Adverse reactions associated with the originator rG-CSF (capillary leak syndrome and glomerulonephritis) have not been observed with tevagrastim/ratiograstim/biograstim or tbo-filgrastim during the postmarket period.
Similar content being viewed by others
Introduction
Myelosuppressive chemotherapy provides substantial clinical benefit in patients with cancer, but chemotherapy-induced febrile neutropenia and the potentially increased risk of life-threatening infection may limit optimal dosing or treatment schedule, and compromise treatment outcomes [1]. Recombinant granulocyte colony-stimulating factors (rG-CSFs), such as filgrastim, are the standard of care for preventing febrile neutropenia in patients receiving myelosuppressive chemotherapy. Filgrastim (Neupogen®) is a short-acting rG-CSF approved by the US Food and Drug Administration (FDA) in 1991 as a prophylaxis for chemotherapy-induced neutropenia [2, 3].
A biosimilar for filgrastim, known as Tevagrastim®, Ratiograstim®, or Biograstim®, was approved in Europe by the European Medicines Agency in 2008 [4]. In the USA, the same product was approved as tbo-filgrastim (Granix®) in 2012 under an original biologic license application for reducing the duration of severe neutropenia in patients with nonmyeloid malignancies receiving myelosuppressive anticancer drugs associated with a clinically significant incidence of febrile neutropenia [2, 4,5,6]. Tbo-filgrastim is a hematopoietic growth factor that binds to G-CSF receptors and stimulates proliferation of neutrophils. The structure, mechanism of action, and toxicity profile of tbo-filgrastim are similar to the originator G-CSF product [3, 5].
Overall, the safety experiences among the different commercially available rG-CSFs are comparable [3, 5, 7]. In several pivotal phase 3 studies, tbo-filgrastim demonstrated a similar safety profile to the reference product filgrastim in patients with lung cancer, breast cancer, and non-Hodgkin lymphoma receiving chemotherapy [8,9,10]. Typical adverse effects reported for rG-CSFs in patients with cancer include bone pain, myalgia, asthenia, nausea, and fever [4, 11, 12]. However, due to the small size, controlled study environment, and short study duration of clinical trials, it can be potentially challenging to detect rare safety events. For this reason, postmarket pharmacovigilance remains a priority for biologic products [11]. Marketed therapeutic products are subject to periodic safety update reports (PSURs), which provide comprehensive worldwide safety assessments [13].
Here, we present the real-world, cumulative postmarket safety experience from the PSUR for tbo-filgrastim/Tevagrastim/Ratiograstim/Biograstim (referred hereafter as tbo-filgrastim) collected through December 31, 2016, from 53 countries. Data from the US pharmacovigilance experience are also summarized, with an emphasis on pharmacovigilance data that resulted in safety updates in the product label since initial FDA approval of tbo-filgrastim in 2012.
Methods
Cumulative estimated exposure and pharmacovigilance reports were collected globally from Teva and acquired companies from initial marketing approval in Europe in 2008 until December 31, 2016. A separate search was conducted to identify postmarket reports from the global data set that originated from the USA and Puerto Rico.
Adverse event (AE) data were received from spontaneous reports submitted by healthcare professionals and consumers, from 19 competent authorities out of 53 countries where products registered by Teva Group are marketed, and the scientific literature,Footnote 1 solicited case reports were received from organized data collection systems, excluding cases received from clinical trials.
Adverse events were tabulated from a) spontaneous source defined as events received from Health Care Professionals, consumers, competent authorities and literature, and b) solicited source defined as cases received from organized data collection systems as non-interventional studies, and patient support programs.
Duplicate checks were performed according to procedures given in the CHMP Guideline on detection and management of duplicate individual cases and Individual Case Safety Reports (ICSRs) [14]. AEs were categorized according to the Medical Dictionary for Regulatory Activities (MedDRA) terms by system organ class, source, and seriousness for pharmacovigilance reporting. A serious adverse event (SAE) was defined as any adverse drug experience occurring at any dose that results in any of the following outcomes: death, a life-threatening adverse drug experience, inpatient hospitalization or prolongation of existing hospitalization, a persistent or significant disability/incapacity, or a congenital anomaly/birth defect. Important medical events that may not result in death, be life-threatening, or require hospitalization may be considered a serious adverse drug experience when, based on appropriate medical judgment, they may jeopardize the patient or subject and may require medical or surgical intervention to prevent one of the outcomes listed in this definition [15].
As with all therapeutic proteins, there is a potential for immunogenicity [11]. A product-specific process for immunogenicity testing of filgrastim in the post-marketing period was established according to the risk management plan (RMP) as a part of routine pharmacovigilance activities. On request by clinicians or by Teva for suspected cases, assessment of binding antibodies to tbo-filgrastim has been conducted on patient’s serum samples collected from postmarketing setting using validated assays.
Results
Exposure
As of December 31, 2016, the estimated global cumulative exposure to tbo-filgrastim in the postmarket setting was 11,589,592 patient-days as calculated from sales data. Cumulative postmarket exposure in the USA and Puerto Rico was estimated to be 1,820,381 patient-days.
Cumulative global and US postmarket experience
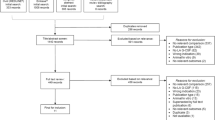
The global safety database processed 720 case reports from 2008 to 2016. Postmarket data sources cumulatively reported 1432 AEs, of those 1164 were spontaneous event reports while the remaining were serious and nonserious events from solicited sources. From spontaneous sources, 582 events were received from healthcare professionals and consumers, 448 cases were received from Health Authorities and 124 cases were received from literature source. Five hundred sixty-seven events out of the cumulative spontaneous cases were serious, from solicited source, 77 events were serious. A summary of clinically relevant AEs and frequently occurring AEs identified from cumulative global spontaneous and solicited reports is provided in Table 1. The most common AEs reported from global experience were pyrexia, bone pain, and back pain, most of which were not serious. The most common SAE reported were hematologic; there were 21 cases of febrile neutropenia (21 of 567, 3.7%), 17 of neutropenia (17 of 567, 2.9%), 12 of increased white blood cell count (12 of 567, 2.1%), and 10 of increased neutrophils (10 of 567, 1.7%).
In the USA, a total of 168 spontaneous events were received in the postmarket setting including 39 SAEs. Only 1 serious case reporting death was received from solicited source. Clinically relevant events are summarized in Table 2. Postmarket experience in the USA is generally similar to the global profile, with nonserious bone pain being the most common nonhematologic event reported. The most common clinically relevant events reported in the USA that were considered serious were decreased white blood cell count and acute febrile neutrophilic dermatosis (2 of 39 events each, 5.13%).
Reports of fatalities
Globally, 65 fatal outcomes were reported including 15 fatalities in the USA. In the USA, spontaneously reported cases of death are automatically considered “related” for reporting purposes. However, signal detection, analysis, and assessment according to Teva standard procedures revealed that the majority of fatalities are likely attributed to progression of underlying cancer or intercurrent disease and no new signal emerged based on available data. One caveat to this analysis is that it can be challenging to establish a causal relationship between tbo-filgrastim and fatal events in the USA because tbo-filgrastim is indicated for treatment of possible life-threatening complications of chemotherapy in a vulnerable patient population (Table 3).
Reports of immunogenicity
During the reporting period, 8 patients were tested for anti-drug-antibodies. Majority of patients were cancer patients undergoing chemotherapy treatment and reporting allergic symptoms after G-CSF administration. Anti-drug-antibody testing was performed by Teva, and all results were negative, i.e., no binding or neutralizing antibodies were detected.
Labeling updates to the US prescribing information
Global pharmacovigilance data for tbo-filgrastim have led to label updates related to safety since initial approval. There have been two updates to the US prescribing information (PI) for tbo-filgrastim from 2012 to 2016. An update was included per the originator drug in December 2014 for the occurrence of capillary leak syndrome (CLS) [16]. CLS was reported with a frequency of 4 of 2460 (0.16%) subjects in clinical trials and may be related to extreme leukocytosis and release of cytokines, such as interleukin-6. One SAE (1 of 567, 0.18%) of CLS was observed with tbo-filgrastim during the postmarket period.
A recent update to the PI in February 2017 included a contraindication for patients with a history of serious allergic reactions to filgrastim or pegfilgrastim products. This update also has additional information at the request of the FDA for the management of glomerulonephritis to align with updates to the PI of the originator drug. No case of glomerulonephritis has been observed to date with tbo-filgrastim treatment during the postmarket period. The FDA also requested the addition of other adverse reactions identified from postmarket experience including “Sweet’s syndrome,” also known as acute febrile neutrophilic dermatosis (4 of 567, 0.71%), diarrhea (4 of 567, 0.71%), asthenia (1 of 567, 0.18%), and fatigue (1 of 567, 0.18%).
Discussion
Postmarket pharmacovigilance remains a priority for biologic products to evaluate worldwide safety assessments and benefit-risk analyses, especially in light of the limitations of clinical trials (small size, controlled study environment, and short study duration), which may be insufficient to detect rare safety events when evaluating biologics.
Overall, the safety profile of tbo-filgrastim/tevagrastim/ratiograstim/biograstim observed in the global postmarket setting is comparable to clinical trial experience. The available data suggest that the postmarket experience in the USA is consistent with the global experience. In both global and US datasets, bone pain was a common, nonserious AE that is generally associated with rG-CSF use. Hematologic events, including febrile neutropenia and decreased white blood cell count, were the most common serious adverse reactions reported in the postmarket setting. These events are likely attributable to chemotherapy treatment or to underlying disease. No new signal emerged.
In the USA, additional safety updates were made to the tbo-filgrastim PI for consistency with the originator product (CLS and glomerulonephritis) or were requested by the regulatory agency (Sweet’s syndrome, asthenia, diarrhea, and fatigue). To date, there are few reported cases of these events in the global data set. Anaphylactic reaction that occurred during therapy was extremely rare. No events were reported for glomerulonephritis, splenic rupture, or pulmonary fibrosis with tbo-filgrastim treatment during the postmarket period. These labeling updates emphasize the need and value of ongoing safety surveillance after drug approval to assess emerging risks and improve patient care.
Limitations of this analysis include voluntary reporting in the spontaneous setting that may result in incomplete or missing medical information. Other confounding factors were (not reported) concomitant medications and comorbidities in this patient population that either limited signal detection or potentially introduced false positives in the data set.
Regarding the immunogenicity, no new cases were detected and no specific areas of concern have arisen from the post-marketing experience of filgrastim antibody testing.
For comparison, in three clinical trials of the previous clinical development program conducted in cancer patients receiving chemotherapy, the overall incidence of immunogenicity of tbo-filgrastim was 1.6% (7/436). Three patients in a study with breast cancer patients, 3 patients in a study with lung cancer patients, and 1 patient in a study with non-Hodgkin lymphoma patients were identified to have antidrug antibody response after tbo-filgrastim treatment, representing immunogenicity incidences of 1.4% (3/213), 1.9% (3/160), and 1.6% (1/63), respectively. None of these 7 patients had cross-reactive antibodies to native G-CSF, evidence of hypersensitive or anaphylactic reactions, or loss of efficacy. All antibody responses were transient and of low titers. Neutralizing antibodies were not detected [17].
Comparisons of immunogenicity between tbo-filgrastim/tevagrastim/ratiograstim/biograstim and other products may be misleading because of differences in the sensitivity and specificity of a particular assay. Antibody positivity may be influenced by several factors, including assay methodology, sample handling, timing of sample collection, concomitant medications, and underlying disease. These challenges underscore the need for standardized immunogenicity assays.
Conclusions
This pharmacovigilance analysis of tbo-filgrastim/tevagrastim/ratiograstim/biograstim indicates that the global postmarket safety experience is consistent with those of clinical trials and that the US experience with tbo-filgrastim does not significantly deviate from the known profile. Some adverse reactions associated with the originator rG-CSF, such as glomerulonephritis, have not been observed with tbo-filgrastim during the postmarket period. Long-term safety data from large and heterogeneous populations in real-world practice permit continuous monitoring for emerging risks to cancer patients treated with filgrastim and present an opportunity to improve patient care.
Notes
Searches were made for PSUR preparation and weekly using Embase, Biosis, and Medline/PubMed. The following search terms were used: “BIOGRASTIM” or “filgrastim” or “tbo-filgrastim” or “XM02” or “XM-02” or“GRANIX” or “RATIOGRASTIM” or “TEVAGRASTIM” or “NEUTROVAL” or“NEUPOGEN” or “ZARZIO” or “ZARXIO” or “NIVESTIM” or “EP2006”
References
Kamioner D, Fruehauf S, Maloisel F, Cals L, Lepretre S, Berthou C (2013) Study design: two long-term observational studies of the biosimilar filgrastim Nivestim (Hospira filgrastim) in the treatment and prevention of chemotherapy-induced neutropenia. BMC Cancer 13:547. https://doi.org/10.1186/1471-2407-13-547
National Comprehensive Cancer Network (2016) Clinical practice guidelines in oncology. Myeloid growth factors. Version 2.2016
Neupogen® (filgrastim) [prescribing information] (2016) Amgen, Inc., Thousand Oaks, CA
Pettengell R, Bias P, Mueller U, Lang N (2016) Clinical safety of tbo-filgrastim, a short-acting human granulocyte colony-stimulating factor. Support Care Cancer 24(6):2677–2684. https://doi.org/10.1007/s00520-015-3057-2
Granix® (tbo-filgrastim) [prescribing information] (2017) Teva Pharmaceuticals USA, Inc., North Wales, PA
Tevagrastim® (filgrastim [rbe]) [summary of product characteristics] (2013) European Medicines Agency
Zarxio® (filgrastim-sndz) [prescribing information] (2017) Sandoz. Inc., Princeton, NJ
del Giglio A, Eniu A, Ganea-Motan D, Topuzov E, Lubenau H (2008) XM02 is superior to placebo and equivalent to Neupogen in reducing the duration of severe neutropenia and the incidence of febrile neutropenia in cycle 1 in breast cancer patients receiving docetaxel/doxorubicin chemotherapy. BMC Cancer 8:332. https://doi.org/10.1186/1471-2407-8-332
Engert A, Griskevicius L, Zyuzgin Y, Lubenau H, del Giglio A (2009) XM02, the first granulocyte colony-stimulating factor biosimilar, is safe and effective in reducing the duration of severe neutropenia and incidence of febrile neutropenia in patients with non-Hodgkin lymphoma receiving chemotherapy. Leuk Lymphoma 50(3):374–379. https://doi.org/10.1080/10428190902756081
Gatzemeier U, Ciuleanu T, Dediu M, Ganea-Motan E, Lubenau H, Del Giglio A (2009) XM02, the first biosimilar G-CSF, is safe and effective in reducing the duration of severe neutropenia and incidence of febrile neutropenia in patients with small cell or non-small cell lung cancer receiving platinum-based chemotherapy. J Thoracic Oncol 4(6):736–740. https://doi.org/10.1097/JTO.0b013e3181a52964
Abraham I, Tharmarajah S, MacDonald K (2013) Clinical safety of biosimilar recombinant human granulocyte colony-stimulating factors. Expert Opin Drug Saf 12(2):235–246. https://doi.org/10.1517/14740338.2013.770472
Baldo BA (2014) Side effects of cytokines approved for therapy. Drug Saf 37(11):921–943. https://doi.org/10.1007/s40264-014-0226-z
ICH Expert Working Group (2012) Periodic benefit-risk evaluation report (PBRER) E2C(R2). International Council on Harmonisation (ICH), Geneva, Switzerland
(2012) CHMP Guideline on detection and management of duplicate individual cases and Individual Case Safety Reports (ICSRs)
US Code of Federal Regulations (2016) Postmarketing reporting of adverse drug experiences. Fed Regist 21 CFR §314.80
Granix® (tbo-filgrastim) [prescribing information] (2014) Teva Pharmaceuticals USA, Inc., North Wales, PA
Zou L, Buchner A, Field J, Barash S, Liu P (2017) Immunogenicity assessment of Tbo-filgrastim in cancer patients receiving chemotherapy. Blood 130:2274
Funding
This study as well as the development of this publication was sponsored by Teva Branded Pharmaceutical Products R&D, Inc. Medical writing assistance was provided by Powered 4 Significance LLC, Annandale, NJ, USA, and was funded by Teva Branded Pharmaceutical Products R&D, Inc., Frazer, PA, USA. The data in this manuscript were presented in part at the 58th American Society of Hematology (ASH) Annual Meeting and Exposition; December 3-6, 2016; San Diego, CA, USA.
Author information
Authors and Affiliations
Corresponding author
Ethics declarations
Camille Abboud reports research funding from Merck, Teva, Novartis, Pfizer, and Seattle Genetics (clinical trial support); and consulting for Gerson and Lehman Group, Agios, Jazz Pharma, Pfizer, and Cardinal Health. Anton Buchner reports employment of Teva ratiopharm, and reports equity ownership in Teva Branded Pharmaceutical Products R&D, Inc. Andreas Lammerich reports employment and equity ownership in Teva ratiopharm/Teva Pharmaceuticals, Inc. Nicole Lang reports employment with Teva ratiopharm/Teva Pharmaceuticals, Inc. Hartmut Link reports research funding from Amgen and Hexal and honoraria from Teva. Patrick Liu reports employment with Teva Pharmaceuticals, Inc. Udo W. Mueller reports employment and equity ownership with Teva Pharmaceuticals, Inc. Ashutosh Pathak reports employment with Teva Pharmaceuticals, Inc. Henry Fung reports receiving honoraria from Amgen and Teva. Ruth Pettengell reports honoraria from CTI, Servier, Teva, Roche, Takeda and Pfizer.
Appendix
Appendix
Rights and permissions
About this article
Cite this article
Abboud, C.N., Lang, N., Fung, H. et al. Real-world safety experience of tevagrastim/ratiograstim/biograstim and tbo-filgrastim, short-acting recombinant human granulocyte colony-stimulating factors. Support Care Cancer 27, 2569–2577 (2019). https://doi.org/10.1007/s00520-018-4522-5
Received:
Accepted:
Published:
Issue Date:
DOI: https://doi.org/10.1007/s00520-018-4522-5