Abstract
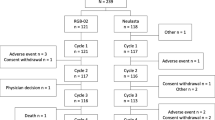
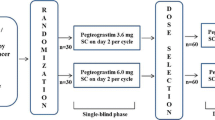
The recombinant human granulocyte colony-stimulating factor (G-CSF) known as filgrastim (Tevagrastim®, Ratiograstim®, Biograstim®) in Europe (approved in 2008) and tbo-filgrastim (Granix®) in the USA (approved in 2012; Teva Pharmaceutical Industries Ltd., Petach Tikva, Israel) is indicated to reduce the duration of severe neutropenia in patients with non-myeloid malignancies receiving myelosuppressive anti-cancer drugs associated with a clinically significant incidence of febrile neutropenia. This article presents pooled clinical data for tbo-filgrastim compared with Neupogen® (Amgen, Thousand Oaks, CA, USA) as well as tbo-filgrastim post-marketing safety data. The safety and efficacy of tbo-filgrastim were evaluated in three phase III studies in 677 patients receiving myelosuppressive chemotherapy and study drug (348 patients with breast cancer, 237 with lung cancer, 92 with non-Hodgkin lymphoma). In each study, the efficacy of tbo-filgrastim was similar to that of Neupogen. Overall, 633 (93.5 %) patients receiving the study drug experienced 6093 treatment-emergent adverse events (AEs), most of which were related to chemotherapy. Adverse events related to the study drug (tbo-filgrastim or Neupogen) were experienced by 185 (27.3 %) patients; 19 (2.8 %) had severe drug-related AEs, 5 (0.7 %) had drug-related serious AEs, and 6 (0.9 %) discontinued the study due to drug-related AEs. Overall, the most common drug-related AEs were bone pain (7.1 %), myalgia (4.0 %), and asthenia (4.4 %). The post-marketing safety profile of tbo-filgrastim was consistent with that observed during the clinical studies. The availability of tbo-filgrastim, a G-CSF with safety and efficacy comparable to those of Neupogen, provides physicians with an alternative treatment option for supportive care of patients with non-myeloid malignancies receiving myelosuppressive chemotherapy.

Similar content being viewed by others
References
Crawford J, Dale DC, Lyman GH (2004) Chemotherapy-induced neutropenia: risks, consequences, and new directions for its management. Cancer 100:228–237. doi:10.1002/cncr.11882
Bodey GP, Buckley M, Sathe YS, Freireich EJ (1966) Quantitative relationships between circulating leukocytes and infection in patients with acute leukemia. Ann Intern Med 64:328–340
Gabrilove JL, Jakubowski A, Scher H, et al. (1988) Effect of granulocyte colony-stimulating factor on neutropenia and associated morbidity due to chemotherapy for transitional-cell carcinoma of the urothelium. N Engl J Med 318:1414–1422. doi:10.1056/NEJM198806023182202
Morstyn G, Campbell L, Lieschke G, et al. (1989) Treatment of chemotherapy-induced neutropenia by subcutaneously administered granulocyte colony-stimulating factor with optimization of dose and duration of therapy. J Clin Oncol 7:1554–1562
Crawford J, Ozer H, Stoller R, et al. (1991) Reduction by granulocyte colony-stimulating factor of fever and neutropenia induced by chemotherapy in patients with small-cell lung cancer. N Engl J Med 325:164–170. doi:10.1056/NEJM199107183250305
Trillet-Lenoir V, Green J, Manegold C, et al. (1993) Recombinant granulocyte colony stimulating factor reduces the infectious complications of cytotoxic chemotherapy. Eur J Cancer 29A:319–324
Gatzemeier U, Ciuleanu T, Dediu M, Ganea-Motan E, Lubenau H, del Giglio A (2009) XM02, the first biosimilar G-CSF, is safe and effective in reducing the duration of severe neutropenia and incidence of febrile neutropenia in patients with small cell or non-small cell lung cancer receiving platinum-based chemotherapy. J Thorac Oncol 4:736–740. doi:10.1097/JTO.0b013e3181a52964
Engert A, Griskevicius L, Zyuzgin Y, Lubenau H, del Giglio A (2009) XM02, the first granulocyte colony-stimulating factor biosimilar, is safe and effective in reducing the duration of severe neutropenia and incidence of febrile neutropenia in patients with non-Hodgkin lymphoma receiving chemotherapy. Leuk Lymphoma 50:374–379. doi:10.1080/10428190902756081
del Giglio A, Eniu A, Ganea-Motan D, Topuzov E, Lubenau H (2008) XM02 is superior to placebo and equivalent to Neupogen in reducing the duration of severe neutropenia and the incidence of febrile neutropenia in cycle 1 in breast cancer patients receiving docetaxel/doxorubicin chemotherapy. BMC Cancer 8:332–338. doi:10.1186/1471-2407-8-332
Kuderer NM, Dale DC, Crawford J, Lyman GH (2007) Impact of primary prophylaxis with granulocyte colony-stimulating factor on febrile neutropenia and mortality in adult cancer patients receiving chemotherapy: a systematic review. J Clin Oncol 25:3158–3167. doi:10.1200/JCO.2006.08.8823
Smith TJ, Khatcheressian J, Lyman GH, et al. (2006) 2006 update of recommendations for the use of white blood cell growth factors: an evidence-based clinical practice guideline. J Clin Oncol 24:3187–3205. doi:10.1200/JCO.2006.06.4451
Crawford J, Althaus B, Armitage J, et al. (2007) Myeloid growth factors. Clinical practice guidelines in oncology. J Natl Compr Canc Netw 5:188–202
Aapro MS, Bohlius J, Cameron DA, et al. (2011) 2010 update of EORTC guidelines for the use of granulocyte-colony stimulating factor to reduce the incidence of chemotherapy-induced febrile neutropenia in adult patients with lymphoproliferative disorders and solid tumours. Eur J Cancer 47:8–32. doi:10.1016/j.ejca.2010.10.013
Crawford J, Caserta C, Roila F (2010) Hematopoietic growth factors: ESMO Clinical Practice Guidelines for the applications. Ann Oncol 21(suppl 5):v248–v251. doi:10.1093/annonc/mdq195
Kouroukis CT, Chia S, Verma S, et al. (2008) Canadian supportive care recommendations for the management of neutropenia in patients with cancer. Curr Oncol 15:9–23
Granix [package insert]. (2013) Teva Pharmaceuticals USA, Inc., North Wales, PA.
Abraham I, Tharmarajah S, MacDonald K (2013) Clinical safety of biosimilar recombinant human granulocyte colony-stimulating factors. Expert Opin Drug Saf 12:235–246. doi:10.1517/14740338.2013.770472
A study to evaluate 5 μg/kg tbo-filgrastim in infants, children and adolescents with solid tumors without bone marrow involvement. NCT02190721. ClinicalTrials.gov. https://clinicaltrials.gov/ct2/show/NCT02190721. Accessed 2 November 2015.
Nuamah NM, Goker H, Kilic YA, Dagmoura H, Cakmak A (2006) Spontaneous splenic rupture in a healthy allogeneic donor of peripheral-blood stem cell following the administration of granulocyte colony-stimulating factor (G-CSF). A case report and review of the literature. Haematologica 91:ECR08
Stroncek D, Shawker T, Follmann D, Leitman SF (2003) G-CSF-induced spleen size changes in peripheral blood progenitor cell donors. Transfusion 43:609–613
Masood N, Shaikh AJ, Memon WA, Idress R (2008) Splenic rupture, secondary to G-CSF use for chemotherapy induced neutropenia: a case report and review of literature. Cases J 1:418. doi:10.1186/1757-1626-1-418
Watring NJ, Wagner TW, Stark JJ (2007) Spontaneous splenic rupture secondary to pegfilgrastim to prevent neutropenia in a patient with non-small-cell lung carcinoma. Am J Emerg Med 25:247–248. doi:10.1016/j.ajem.2006.10.005
Tigue CC, McKoy JM, Evens AM, Trifilio SM, Tallman MS, Bennett CL (2007) Granulocyte-colony stimulating factor administration to healthy individuals and persons with chronic neutropenia or cancer: an overview of safety considerations from the Research on Adverse Drug Events and Reports project. Bone Marrow Transplant 40:185–192. doi:10.1038/sj.bmt.1705722
Neupogen [package insert]. (2013) Amgen Inc., Thousand Oaks, CA.
EMA-Guideline on good pharmacovigilance practice (GVP). Module VII—periodic safety update report (Rev1) (2015) European Medicines Agency Science Medicines Health. www.ema.europa.eu. Accessed 2 November 2015.
Martino M, Console G, Irrera G, et al. (2005) Harvesting peripheral blood progenitor cells from healthy donors: retrospective comparison of filgrastim and lenograstim. J Clin Apher 20:129–136. doi:10.1002/jca.20049
Beelen DW, Ottinger H, Kolbe K, et al. (2002) Filgrastim mobilization and collection of allogeneic blood progenitor cells from adult family donors: first interim report of a prospective German multicenter study. Ann Hematol 81:701–709. doi:10.1007/s00277-002-0553-5
Anderlini P, Donato M, Chan KW, et al. (1999) Allogeneic blood progenitor cell collection in normal donors after mobilization with filgrastim: the M.D. Anderson Cancer Center experience. Transfusion 39:555–560
Acknowledgments
This periodic safety update report was funded by Teva Branded Pharmaceutical Products R&D, Inc. The authors thank Anton Buchner and Reiner Elsaesser (both of Teva Ratiopharm/Teva Pharmaceuticals, Inc., Ulm, Germany) for their support in providing the clinical data for this article and Gabriella Letinic-Klier, MD, Pharmacovigilance Expert, for the preparation of the periodic safety update report.
Author information
Authors and Affiliations
Corresponding author
Ethics declarations
The studies were approved by all local institutional review boards and conducted in accordance with the principles of the Declaration of Helsinki and the ethical principles of Good Clinical Practice guidelines. Written informed consent was obtained from all patients before the start of any study-related procedures.
Conflict of interest
Ruth Pettengell has received speaker honoraria from Teva and Takeda. Peter Bias, Udo Mueller, and Nicole Lang are employees of Teva Ratiopharm/Teva Pharmaceuticals, Inc. Peter Bias and Udo Mueller own stocks in Teva Ratiopharm/Teva Pharmaceuticals, Inc. Medical writing assistance was provided by Lisa Feder, PhD, of Peloton Advantage LLC and was funded by Teva Branded Pharmaceutical Products R&D, Inc. Teva provided a full review of the article.
Rights and permissions
About this article
Cite this article
Pettengell, R., Bias, P., Mueller, U. et al. Clinical safety of tbo-filgrastim, a short-acting human granulocyte colony-stimulating factor. Support Care Cancer 24, 2677–2684 (2016). https://doi.org/10.1007/s00520-015-3057-2
Received:
Accepted:
Published:
Issue Date:
DOI: https://doi.org/10.1007/s00520-015-3057-2