Abstract
Background and aims
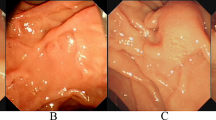
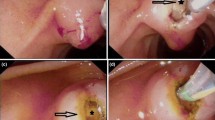
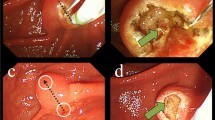
Needle-knife papillotomy and fistulotomy (NKPF) is a new, modified technique designed for difficult biliary cannulation. The safety and efficacy of performing NKPF based on characteristics of main duodenal papilla (MDP) was evaluated.
Methods
We performed a retrospective review of consecutive patients with intact papilla who were established as candidates for therapeutic ERCP at tertiary referral center. A total of 532 patients were included in conventional endoscopic retrograde cholangiopancreatography (ERCP) group in which repeated cannulation was tried in patients with difficult bile duct cannulation; and 598 patients enrolled in early NKPF group according to predefined parameters. Based on the characteristics of MDP, different types of NKPF were performed. The endoscopic data (mean procedure time, anatomy of the main papilla), rate of cannulation success, and post-ERCP complications were collected.
Results
A total of 82 patients underwent NKPF. The mean procedure time of the small papilla group was longer than bulging papilla group (P < 0.05). The success rate of biliary cannulation in the small papilla group (69.3 %) was lower than in the bulging papilla group (100 %, P < 0.01). The overall successful biliary cannulation of patients in the NKPF group was significantly higher than in the conventional group (98.8 vs 90.8 %, P > 0.05). The total complication rate was 6.6 % among conventional group patients and 5.7 % among NKPF group, respectively. The overall complication rate and rates of specific complications (pancreatitis, bleeding, cholangitis, and perforation) in the two groups were similar (P > 0.05).
Conclusion
Early NKPF based on characteristics of MDP raised the success rate of biliary cannulation when conventional cannulation failed and did not increase the complication rate post-ERCP. Clinic Trials. gov number, Hongwei-1102-12.

Similar content being viewed by others
References
Bailey AA, Bourke MJ, Williams SJ, Walsh PR, Murray MA, Lee EY, Kwan V, Lynch PM (2008) A prospective randomized trial of cannulation technique in ERCP: effects on technical success and post-ERCP pancreatitis. Endoscopy 40(4):296–301. doi:10.1055/s-2007-995566
Cennamo V, Fuccio L, Zagari RM, Eusebi LH, Ceroni L, Laterza L, Fabbri C, Bazzoli F (2010) Can early precut implementation reduce endoscopic retrograde cholangiopancreatography-related complication risk? Meta-analysis of randomized controlled trials. Endoscopy 42(5):381–388. doi:10.1055/s-0029-1243992
Figueiredo FA, Pelosi AD, Machado L, Francioni E, Freitas G, Hatum PB, de Mello Perez R (2010) Precut papillotomy: a risky technique not only for experts but also for average endoscopists skilled in ERCP. Dig Dis Sci 55(5):1485–1489. doi:10.1007/s10620-009-0860-y
Donnellan F, Zeb F, Courtney G, Aftab AR (2010) Suprapapillary needleknife fistulotomy: a safe and effective method for accessing the biliary system. Surg Endosc 24(8):1937–1940. doi:10.1007/s00464-010-0881-9
Bailey AA, Bourke MJ, Kaffes AJ (2010) Needle-knife sphincterotomy: factors predicting its use and the relationship with postERCP pancreatitis. Gastrointest Endosc 71(2):266–271. doi:10.1016/j.gie.2009.09.024
Gong B, Hao L, Bie L, Sun B, Wang M (2010) Does precut technique improve selective bile duct cannulation or increase post-ERCP pancreatitis rate? A meta-analysis of randomized controlled trials. Surg Endosc 24(11):2670–2680. doi:10.1007/s00464-010-1033-y
Swan MP, Alexander S, Moss A, Williams SJ, Ruppin D, Hope R, Bourke MJ (2013) Needle knife sphincterotomy does not increase the risk of pancreatitis in patients with difficult biliary cannulation. Clin Gastroenterol Hepatol 11(4):430–436. doi:10.1016/j.cgh.2012.12.017
Lim JU, Joo KR, Cha JM, Shin HP, Lee JI, Park JJ, Jeon JW, Kim BS, Joo S (2012) Early use of needle-knife fistulotomy is safe in situations where difficult biliary cannulation is expected. Dig Dis Sci 57(5):1384–1390. doi:10.1007/s10620-012-2030-x
Kaffes AJ, Sriram PV, Rao GV, Santosh D, Reddy DN (2005) Early institution of pre-cutting for difficult biliary cannulation: a prospective study comparing conventional vs. a modified technique. Gastrointest Endosc 62(5):669–674
Zhang QS, Han B, Xu JH, Bao WM, Tao JL, Zhang Y (2013) Needle knife precut papillotomy and fistulotomy for difficult biliary cannulation during endoscopic retrograde cholangiopancreatography. Digestion 88(2):95–100. doi:10.1159/000352027
Lee TH, Bang BW, Park SH, Jeong S, Lee DH, Kim SJ (2011) Precut fistulotomy for difficult biliary cannulation: is it a risky preference in relation to the experience of an endoscopist? Dig Dis Sci 56(6):1896–1903. doi:10.1007/s10620-010-1483-z
Avisse C, Flament JB, Delattre JF (2000) Ampulla of Vater. Anatomic, embryologic, and surgical aspects. Surg Clin North Am 80(1):201–212
Cotton PB, Lehman G, Vennes J, Geenen JE, Russell RC, Meyers WC, Liguory C, Nickl N (1991) Endoscopic sphincterotomy complications and their management: an attempt at consensus. Gastrointest Endosc 37(3):383–393
Freeman ML, Guda NM (2005) ERCP cannulation: a review of reported techniques. Gastrointest Endosc 61(1):112–125
Löhr J-M, Aabaken L, Arnelo U, Grönroos J, Halttunen J, Hauge T, Jonas E, Kleveland PM, Nordblad Schmidt P, Swahn F, Saarela A, Toth E, Meisner S (2012) How to cannulate? A survey of the scandinavian association for digestive endoscopy (SADE) in 141 endoscopists. Scand J Gastroenterol 47(7):861–869. doi:10.3109/00365521.2012.672588
Fukatsu H, Kawamoto H, Harada R, Tsutsumi K, Fujii M, Kato H, Hirao K, Nakanishi T, Mizuno O, Ogawa T, Ishida E, Okada H, Sakaguchi K (2009) Quantitative assessment of technical proficiency in performing needle-knife precut papillotomy. Surg Endosc 23(9):2066–2072. doi:10.1007/s00464-008-9969-x
Lopes L, Dinis-Ribeiro M, Rolanda C (2014) Safety and efficacy of precut needle-knife fistulotomy. Scand J Gastroenterol 49(6):759–765. doi:10.3109/00365521
Rabenstein T, Ruppert T, Schneider HT, Hahn EG, Ell C (1997) Benefits and risks of needle-knife papillotomy. Gastrointest Endosc 46(3):207–211
Horiuchi A, Nakayama Y, Kajiyama M, Tanaka N (2007) Effect of precut sphincterotomy on biliary cannulation based on the characteristics of the major duodenal papilla. Clin Gastroenterol Hepatol 5(9):1113–1118
Masci E, Mariani A, Curioni S, Testoni PA (2003) Risk factors for pancreatitis following endoscopic retrograde cholangiopancreatography: a meta-analysis. Endoscopy 35(10):830–834
Navaneethan U, Konjeti R, Venkatesh PG, Sanaka MR, Parsi MA (2014) Early precut sphincterotomy and the risk of endoscopic retrograde cholangiopancreatography related complications: an updated meta-analysis. World J Gastrointest Endosc 6(5):200–208. doi:10.4253/wjge.v6.i5.200
Masci E, Toti G, Mariani A, Curioni S, Lomazzi A, Dinelli M, Minoli G, Crosta C, Comin U, Fertitta A, Prada A, Passoni GR, Testoni PA (2001) Complications of diagnostic and therapeutic ERCP: a prospective multicenter study. Am J Gastroenterol 96(2):417–423
Freeman ML, Nelson DB, Sherman S, Haber GB, Herman ME, Dorsher PJ, Moore JP, Fennerty MB, Ryan ME, Shaw MJ, Lande JD, Pheley AM (1996) Complications of endoscopic biliary sphincterotomy. N Engl J Med 335(13):909–918
Andriulli A, Loperfido S, Napolitano G, Niro G, Valvano MR, Spirito F, Pilotto A, Forlano R (2007) Incidence rates of post-ERCP complications: a systematic survey of prospective studies. Am J Gastroenterol 102(8):1781–1788
Williams EJ, Taylor S, Fairclough P, Hamlyn A, Logan RF, Martin D, Riley SA, Veitch P, Wilkinson ML, Williamson PR, Lombard M (2007) Risk factors for complication following ERCP; results of a large-scale, prospective multicenter study. Endoscopy 39(9):793–801
Colton JB, Curran CC (2009) Quality indicators, including complications, of ERCP in a community setting: a prospective study. Gastrointest Endosc 70(3):457–467. doi:10.1016/j.gie.2008.11.022
Author information
Authors and Affiliations
Corresponding author
Ethics declarations
Disclosures
All authors disclosed no financial relationships relevant to this article.
Rights and permissions
About this article
Cite this article
Zhang, QS., Han, B., Xu, JH. et al. Needle-knife papillotomy and fistulotomy improved the treatment outcome of patients with difficult biliary cannulation. Surg Endosc 30, 5506–5512 (2016). https://doi.org/10.1007/s00464-016-4914-x
Received:
Accepted:
Published:
Issue Date:
DOI: https://doi.org/10.1007/s00464-016-4914-x