Abstract
Background
Several studies have reported on the correlation between the experience level of an endoscopist and the outcomes of precut procedures. However, there are limited data on the early use of the precut fistulotomy in relation to the experience of an endoscopist.
Aim
To evaluate the efficacy and safety of precut fistulotomy in difficult biliary cannulation after ERCP training.
Methods
Two endoscopists, one at each tertiary referral center, performed the precut fistulotomy for difficult biliary cannulation between September 2008 and February 2010. The technical success, complications, and clinical outcomes in three groups were recorded prospectively over time.
Results
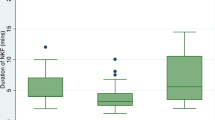
A total of 159 (23.1%) patients underwent precut fistulotomy. The mean procedure time was decreased as the number of procedures increased (p < 0.01). The success rates of selective biliary cannulation in the three groups were 86.8, 86.8, and 88.7% respectively, for the first attempt (p = 0.77) and 93.7% for the second attempt. Post-ERCP pancreatitis developed in nine (5.7%) patients, which was not statistically significant between the three groups. As the frequency of papillary contacts increased, post-ERCP pancreatitis tended to increase (p = 0.017). In the multivariate analysis, more than 15 attempts at cannulating the major papilla prior to fistulotomy was a risk factor for pancreatitis (odds ratio 4.8, 95% CI 1.178–19.580, p = 0.029).
Conclusions
After therapeutic ERCP training involving at least 100 ERCPs, including at least half that were therapeutic cases and more than ten that were precut papillotomies, a precut fistulotomy can be performed safely and effectively in low-risk patients.


Similar content being viewed by others
Abbreviations
- DBC:
-
Difficult biliary cannulation
- PF:
-
Precut fistulotomy
- CBD:
-
Common bile duct
- SOD:
-
Sphincter of Oddi dysfunction
References
Harewood GC, Baron TH. An assessment of the learning curve for precut biliary sphincterotomy. Am J Gastroenterol. 2002;97:1708–1712.
Mavrogiannis C, Liatsos C, Romanos A, Petoumenos C, Nakos A, Karvountzis G. Needle-knife fistulotomy versus needle-knife precut papillotomy for the treatment of common bile duct stones. Gastrointest Endosc. 1999;50:334–339.
Kasmin FE, Cohen D, Batra S, Cohen SA, Siegel JH. Needle-knife sphincterotomy in a tertiary referral center: efficacy and complications. Gastrointest Endosc. 1996;44:48–53.
Goff JS. Long-term experience with the transpancreatic sphincter pre-cut approach to biliary sphincterotomy. Gastrointest Endosc. 1999;50:642–645.
Foutch PG. A prospective assessment of results for needle-knife papillotomy and standard endoscopic sphincterotomy. Gastrointest Endosc. 1995;41:25–32.
de la Morena EJ, Domínguez M, Lumbreras M, Opio V, Moyano E, Garćia Alvarez J. Self-training in needle-knife sphincterotomy. Gastroenterol Hepatol. 2000;23:109–115.
Maydeo A, Borkar D. Techniques of selective cannulation and sphincterotomy. Endoscopy. 2003;35:19–23.
Rollhauser C, Johnson M, Al-Kawas FH. Needle-knife papillotomy: a helpful and safe adjunct to endoscopic retrograde cholangiopancreatography in a selected population. Endoscopy. 1998;30:691–696.
Masci E, Mariani A, Curioni S, Testoni PA. Risk factors for pancreatitis following endoscopic retrograde cholangiopancreatography: A meta-analysis. Endoscopy. 2003;35:830–834.
Cotton PB, Lehman G, Vennes J, et al. Endoscopic sphincterotomy complications and their management: An attempt at consensus. Gastrointest Endosc. 1991;37:383–393.
Freeman ML, Nelson DB, Sherman S, et al. Complications of endoscopic biliary sphincterotomy. N Engl J Med. 1996;335:909–918.
Cotton PB. Precut papillotomy—a risky technique for experts only. Gastrointest Endosc. 1989;35:578–579.
Freeman ML. Complications of endoscopic biliary sphincterotomy: A review. Endoscopy. 1997;29:288–297.
Akaraviputh T, Lohsiriwat V, Swangsri J, Methasate A, Leelakusolvong S, Lertakayamanee N. The learning curve for safety and success of precut sphincterotomy for therapeutic ERCP: A single endoscopist’s experience. Endoscopy. 2008;40:513–516.
Robison LS, Varadarajulu S, Wilcox CM. Safety and success of precut biliary sphincterotomy: Is it linked to experience or expertise? World J Gastroenterol. 2007;13:2183–2186.
Kaffes AJ, Sriram PV, Rao GV, Santosh D, Reddy DN. Early institution of pre-cutting for difficult biliary cannulation: A prospective study comparing conventional vs. a modified technique. Gastrointest Endosc. 2005;62:669–674.
Freeman ML, DiSario JA, Nelson DB, et al. Risk factors for post-ERCP pancreatitis: A prospective, multicenter study. Gastrointest Endosc. 2001;54:425–434.
Horiuchi A, Nakayama Y, Kajiyama M, Tanaka N. Effect of precut sphincterotomy on biliary cannulation based on the characteristics of the major duodenal papilla. Clin Gastroenterol Hepatol. 2007;5:1113–1118.
O’Connor HJ, Bhutta AS, Redmond PL, Carruthers DA. Suprapapillary fistulosphincterotomy at ERCP: A prospective study. Endoscopy. 1997;29:266–270.
Dowsett JF, Polydorou AA, Varia D. Needle knife papillotomy: How safe and how effective? Gut. 1990;31:905–908.
Leung JWC, Banez VP, Chung SCS. Precut (needle knife) papillotomy for impacted common bile duct stone at the ampulla. Am J Gastroenterol. 1990;85:991–998.
Rabenstein T, Ruppert T, Schneider HT, Hahn EG, Ell C. Benefits and risks of needle-knife papillotomy. Gastrointest Endosc. 1997;46:207–211.
Recchia S, Coppola F, Ferrari A, Righi D, Zanon E, Verme G. Fistulosphincterotomy in the endoscopic approach to biliary tract diseases. Am J Gastroenterol. 1992;87:1607–1609.
Bailey AA, Bourke MJ, Kaffes AJ, Byth K, Lee EY, Williams SJ. Needle-knife sphincterotomy: Factors predicting its use and the relationship with post-ERCP pancreatitis (with video). Gastrointest Endosc. 2010;71:266–271.
Huibregtse K, Kimmey MB. Endoscopic retrograde cholangiopancreatography, endoscopic sphincterotomy and endoscopic biliary and pancreatic drainage. In: Yamada T, ed. Textbook of Gastroenterology. Philadelphia: J. B. Lippincott; 1995:2590–2617.
Siegel JH. Precut papillotomy: A method to improve success of ERCP and papillotomy. Endoscopy. 1980;12:130–133.
Loperfido S, Angelini G, Benedetti G, et al. Major early complications from diagnostic and therapeutic ERCP: A prospective multicenter study. Gastrointest Endosc. 1998;48:1–10.
Masci E, Toti G, Mariani A, et al. Complications of diagnostic and therapeutic ERCP: A prospective multicenter study. Am J Gastroenterol. 2001;96:417–423.
Baillie J. Needle-knife papillotomy revisited. Gastrointest Endosc. 1997;46:282–284.
Cotton PB. Is your sphincterotomy really safe and necessary? Gastrointest Endosc. 1996;44:752–755.
Huibregtse K, Katon RM, Tytgat GN. Precut papillotomy via fine-needle knife papillotome: A safe and effective technique. Gastrointest Endosc. 1986;32:403–405.
Cennamo V, Fuccio L, Zagari RM, et al. Can early precut implementation reduce endoscopic retrograde cholangiopancreatography-related complication risk? Meta-analysis of randomized controlled trials. Endoscopy. 2010;42:381–388.
Figueiredo FA, Pelosi AD, Machado L, et al. Precut papillotomy: A risky technique not only for experts but also for average endoscopists skilled in ERCP. Dig Dis Sci. 2010;55:1485–1489.
Donnellan F, Zeb F, Courtney G, Aftab AR. Suprapapillary needleknife fistulotomy: A safe and effective method for accessing the biliary system. Surg Endosc. 2010;24:1937–1940.
Artifon EL, Sakai P, Cunha JE, Halwan B, Ishioka S, Kumar A. Guidewire cannulation reduces risk of post-ERCP pancreatitis and facilitates bile duct cannulation. Am J Gastroenterol. 2007;102:2147–2153.
Lella F, Bagnolo F, Colombo E, Bonassi U. A simple way of avoiding post-ERCP pancreatitis. Gastrointest Endosc. 2004;59:830–834.
Lee TH, Park do H, Park JY, et al. Can wire-guided cannulation prevent post-ERCP pancreatitis? A prospective randomized trial. Gastrointest Endosc. 2009;69:444–449.
Conflicts of interest
None to declare.
Author information
Authors and Affiliations
Corresponding author
Rights and permissions
About this article
Cite this article
Lee, T.H., Bang, B.W., Park, SH. et al. Precut Fistulotomy for Difficult Biliary Cannulation: Is It a Risky Preference in Relation to the Experience of an Endoscopist?. Dig Dis Sci 56, 1896–1903 (2011). https://doi.org/10.1007/s10620-010-1483-z
Received:
Accepted:
Published:
Issue Date:
DOI: https://doi.org/10.1007/s10620-010-1483-z