Abstract
Background
There is growing evidence that memantine, a noncompetitive N-methyl-d-aspartate receptor antagonist, may be applied as an add-on in treating patients suffering from obsessive–compulsive disorders (OCD). The aim of the present study was therefore to assess the effect of adjuvant memantine in a double-blind, randomized, and placebo-controlled study of the treatment of patients suffering from OCD.
Method
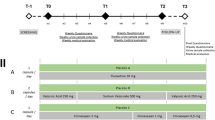
A total of 40 inpatients (32 females (80 %); mean age = 31.25 years) suffering from OCD were randomly assigned to a treatment (administration of memantine) or a control group (placebo). Treatment lasted for 12 consecutive weeks. All patients were treated with selective serotonin re-uptake inhibitors or clomipramine. Patients completed the Yale–Brown Obsessive Compulsive Scale four times. Experts’ ratings consisted in clinical global impression (clinical global impressions (CGI), illness severity and illness improvement; two to three times). Liver enzymes SGOT and SGPT were also assessed (twice).
Results
Of the 40 inpatients approached, 29 completed the 12 consecutive weeks of the study. Of the 11 dropouts, 6 were in the target group and five in the control group. Symptoms significantly decreased across the period of the study, but particularly in the treatment compared with the control group (significant time × group interaction). Illness severity (CGI severity) also significantly decreased over time but more so in the treatment than in the control group (significant time × group interaction). Illness improvements (CGI improvements) were not significant.
Conclusions
The pattern of results from the present double-blind, randomized, and placebo-controlled study for the treatment of patients suffering from OCD suggests that adjuvant memantine does significantly and favorably impact on OCD.


Similar content being viewed by others
Notes
The clinical trial number is: IRCT138712141743N1; www.irct.ir.
In the latter case, in strict accordance with the declaration of Helsinki, patients were free to withdraw from the study without any further justification or explanation. Moreover, they were assured that withdrawing from the study without any further justification was in no way associated with any disadvantages.
Once a week, patients received a list indicating possible side-effects due to adjuvant medication (answers; yes/no). The list was based on the Joint Formulary Committee (2004) and comprised the following side-effects: confusion, dizziness, drowsiness, headache, insomnia, agitation and/or hallucinations, vomiting, light-headedness, vertigo, and anxiety.
References
Ackerman DL, Greenland S (2002) Multivariate meta-analysis of controlled drug studies for obsessive–compulsive disorder. J Clin Psychopharmacol 22:309–317
Afshar H, Roohafza H, Mohammad-Beigi H, Haghighi M, Jahangard L, Shokouh P, Sadeghi M, Hafezian H (2012) N-acetylcysteine add-on treatment in refractory obsessive–compulsive disorder: a randomized, double-blind, placebo-controlled trial. J Clin Psychopharmacol 32:797–803
American Psychiatric Association (2000) Diagnostic and statistical manual of mental disorders, 4th edn. American Psychiatric Association, Washington, DC
Bhattacharyya S, Khanna S, Chakrabarty K, Mahadevan A, Christopher R, Shankar SK (2009) Anti-brain autoantibodies and altered excitatory neurotransmitters in obsessive–compulsive disorder. Neuropsychopharmacology 34:2489–2496
Carlsson ML (2001) On the role of prefrontal cortex glutamate for the antithetical phenomenology of obsessive compulsive disorder and attention deficit hyperactivity disorder. Prog Neuropsychopharmacol Biol Psychiatry 25:5–26
Chakrabarty K, Bhattacharyya S, Christopher R, Khanna S (2001) Glutamatergic dysfunction in OCD. Neuropsychopharmacology 30:1735–1740
Cohen J (1988) Statistical power analysis for the behavioural sciences, 2nd edn. Lawrence Erlbaum Associates, Hillsdale
Foa EB, Liebowitz MR, Kozak MJ, Davies S, Campeas R, Franklin ME, Huppert JD, Kjernisted K, Rowan V, Schmidt AB, Simpson HB, Tu X (2005) Randomized, placebo-controlled trial of exposure and ritual prevention, clomipramine, and their combination in the treatment of obsessive–compulsive disorder. Am J Psychiatry 162:151–161
Franklin ME, Foa EB (2011) Treatment of obsessive compulsive disorder. Annu Rev Clin Psychol 7:229–243
Ghaleiha A, Entezari N, Modabbernia A, Najand B, Askari N, Tabrizi M, Ashrafi M, Hajiaghaee R, Akhondzadeh S (2013) Memantine add-on in moderate to severe obsessive–compulsive disorder: randomized double-blind placebo-controlled study. J Psychiatr Res 47:175–180
Goodman WK, Price LH, Rasmussen SA, Mazure C, Delgado P, Heninger GR, Charney DS (1989) The Yale–Brown Obsessive Compulsive Scale. II. Validity. Arch Gen Psychiatry 46:1012–1016
Goodman WK, Kozak MJ, Liebowitz M, White KL (1996) Treatment of obsessive-compulsive disorder with fluvoxamine: a multicentre, double-blind, placebo-controlled trial. Int Clin Psychopharmacol 11:21–29
Guy W (1976) ECDEU assessment for psychopharmacology, revised edition. NIMH Publication, Rockville
Hanna GL, Himle JA, Curtis GC, Gillespie BW (2005) A family study of obsessive–compulsive disorder with pediatric probands. Am J Med Genet B Neuropsychiatr Genet 134:13–19
Hettema JM, Neale MC, Kendler KS (2001) A review and meta-analysis of the genetic epidemiology of anxiety disorders. Am J Psychiatry 158:1568–1578
Hezel DM, Beattie K, Stewart SE (2009) Memantine as an augmenting agent for severe pediatric OCD. Am J Psychiatry 166:237
Hollander E (1996) Obsessive-compulsive disorder-related disorders: the role of selective serotonergic reuptake inhibitors. Int Clin Psychopharmacol 11(suppl 5):75–87
Joint Formulary Committee (2004) British National Formulary (BNF), 47th edn. British Medical Association and the Royal Pharmaceutical Society of Great Britain, London
Karno M, Golding JM, Sorenson SB, Burnam MA (1988) The epidemiology of obsessive–compulsive disorder in five US communities. Arch Gen Psychiatry 45:1094–1099
Kessler RC, Berglund P, Demler O, Jin R, Merikangas KR, Walters EE (2005) Lifetime prevalence and age-of-onset distributions of DSM-IV disorders in the National Comorbidity Survey Replication. Arch Gen Psychiatry 62:593–602
Mataix-Cols D, Rauch SL, Baer L, Eisen JL, Shera DM, Goodman WK, Rasmussen SA, Jenike MA (2002) Symptom stability in adult obsessive–compulsive disorder: data from a naturalistic two-year follow-up study. Am J Psychiatry 159:263–268
McGrath MJ, Campbell KM, Parks CR, Burton FH (2000) Glutamatergic drugs exacerbate symptomatic behavior in a transgenic model of comorbid Tourette's syndrome and obsessive-compulsive disorder. Brain Res 877:23–30
Pallanti S, Quercioli L (2006) Treatment-refractory obsessive–compulsive disorder: methodological issues, operational definitions and therapeutic lines. Prog Neuropsychopharmacol Biol Psychiatry 30:400–412
Pasquini M, Biondi M (2006) Memantine augmentation for refractory obsessive–compulsive disorder. Prog Neuropsychopharmacol Biol Psychiatry 30:1173–1175
Pigott TA, Seay SM (1999) A review of the efficacy of selective serotonin reuptake inhibitors in obsessive–compulsive disorder. J Clin Psychiatry 60:101–106
Poyurovsky M, Weizman R, Weizman A, Koran L (2005) Memantine for treatment-resistant OCD. Am J Psychiatry 162:2191–2192
Rosenberg DR, Keshavan MS (1998) A.E. Bennett Research Award. Toward a neurodevelopmental model of obsessive–compulsive disorder. Biol Psychiatry 43:623–640
Rosenberg DR, MacMaster FP, Keshavan MS, Fitzgerald KD, Stewart CM, Moore GJ (2000) Decrease in caudate glutamatergic concentrations in pediatric obsessive–compulsive disorder patients taking paroxetine. J Am Acad Child Adolesc Psychiatry 39:1096–1103
Rosenberg DR, Mirza Y, Russell A, Tang J, Smith JM, Banerjee SP, Bhandari R, Rose M, Ivey J, Boyd C, Moore GJ (2004) Reduced anterior cingulate glutamatergic concentrations in childhood OCD and major depression versus healthy controls. J Am Acad Child Adolesc Psychiatry 43:1146–1153
Ruscio AM, Stein DJ, Chiu WT, Kessler RC (2010) The epidemiology of obsessive–compulsive disorder in the National Comorbidity Survey Replication. Mol Psychiatry 15:53–63
Saxena S, Rauch SL (2000) Functional neuroimaging and the neuroanatomy of obsessive–compulsive disorder. Psychiatr Clin North Am 23:563–586
Saxena S, Bota RG, Brody AL (2001) Brain-behavior relationships in obsessive–compulsive disorder. Semin Clin Neuropsychiatry 6:82–101
Starck G, Ljungberg M, Nilsson M, Jönsson L, Lundberg S, Ivarsson T, Ribbelin S, Ekholm S, Carlsson A, Forssell-Aronsson E, Carlsson ML (2008) A 1H magnetic resonance spectroscopy study in adults with obsessive compulsive disorder: relationship between metabolite concentrations and symptom severity. J Neural Transm 115:1051–1062
Stewart SE, Jenike EA, Hezel DM, Stack DE, Dodman NH, Shuster L, Jenike MA (2010) A single-blinded case–control study of memantine in severe obsessive–compulsive disorder. J Clin Psychopharmacol 30:34–39
Swedo SE, Snider LA (2004) The neurobiology and treatment of obsessive compulsive disorder. In: Nestler EJ, Charney DS (eds) Neurobiology of mental illness. Oxford University Press, New York, pp 628–638
Ting JT, Feng G (2011) Neurobiology of obsessive-compulsive disorder: insights into neural circuitry dysfunction through mouse genetics. Curr Opin Neurobiol 21:842–848
van Grootheest DS, Cath DC, Beekman AT, Boomsma DI (2005) Twin studies on obsessive–compulsive disorder: a review. Twin Res Hum Genet 8:450–458
Whiteside SP, Port JD, Deacon BJ, Abramowitz JS (2006) A magnetic resonance spectroscopy investigation of obsessive–compulsive disorder and anxiety. Psychiatry Res 146:137–147
Wu K, Hanna GL, Rosenberg DR, Arnold PD (2012) The role of glutamate signaling in the pathogenesis and treatment of obsessive–compulsive disorder. Pharmacol Biochem Behav 100:726–735
Yücel M, Wood SJ, Wellard RM, Harrison BJ, Fornito A, Pujol J, Velakoulis D, Pantelis C (2008) Anterior cingulate glutamate-glutamine levels predict symptom severity in women with obsessive–compulsive disorder. Aust N Z J Psychiatry 42:467–477
Conflict of interest
All authors declare no conflicts of interest; the entire study was performed without external funding
Author information
Authors and Affiliations
Corresponding author
Rights and permissions
About this article
Cite this article
Haghighi, M., Jahangard, L., Mohammad-Beigi, H. et al. In a double-blind, randomized and placebo-controlled trial, adjuvant memantine improved symptoms in inpatients suffering from refractory obsessive-compulsive disorders (OCD). Psychopharmacology 228, 633–640 (2013). https://doi.org/10.1007/s00213-013-3067-z
Received:
Accepted:
Published:
Issue Date:
DOI: https://doi.org/10.1007/s00213-013-3067-z