Abstract
Optimal fluid management is one of the main challenges in the care of the critically ill. However, the physiological parameters that are commonly monitored and used to guide fluid management are often inadequate and even misleading. From 1987 to 1989 we published four experimental studies which described a method for predicting the response of the cardiac output to fluid administration during mechanical ventilation. The method is based on the analysis of the variations in the arterial pressure in response to a mechanical breath, which serves as a repetitive hemodynamic challenge. Our studies showed that the systolic pressure variation and its components are able to reflect even small changes in the circulating blood volume. Moreover, these dynamic parameters provide information about the slope of the left ventricular function curve, and therefore predict the response to fluid administration better than static preload parameters.
Many new dynamic parameters have been introduced since then, including the pulse pressure (PPV) and stroke volume (SVV) variations, and various echocardiographic and other parameters. Though seemingly different, all these parameters are based on measuring the response to a predefined preload-modifying maneuver. The clinical usefulness of these ‘dynamic’ parameters is limited by many confounding factors, the recognition of which is absolutely necessary for their proper use.
With more than 20 years of hindsight we believe that our early studies helped pave the way for the recognition that fluid administration should ideally be preceded by the assessment of “fluid responsiveness”. The introduction of dynamic parameters into clinical practice can therefore be viewed as a significant step towards a more rational approach to fluid management.
Similar content being viewed by others
Our initial study(ies)
In 1987 we published an experimental study in which we quantified the respiratory-induced variations in the arterial pressure (AP) in ten mechanically ventilated dogs during graded hemorrhage followed by re-transfusion [1]. A continuously inflated vest was wrapped around the dogs’ chest to maintain the ratio of lung to chest wall compliance similar to that of humans. Another important feature was the gradual rate of blood withdrawal, allowing time for the development of ‘latent’ hypovolemia that was not reflected by the AP and the heart rate (HR). At each step of the protocol we recorded the following parameters for off-line analysis: the systolic pressure variation [SPV which is the difference between the maximal and minimal systolic blood pressure (SBP) values during one respiratory cycle], the delta down (dDown, ΔDown, the difference between the SBP during a short apnea and the minimal value of the SBP), and the delta up (dUp, ΔUp, the difference between the SBP during a short apnea and the maximal value of the SBP) (Fig. 1).
The systolic pressure variation (SPV) is the difference between the maximal and minimal systolic blood pressure (SBP) values during one mechanical breath. The horizontal reference line indicates the SBP during end-expiration and serves to separate the SPV into its ΔUp and ΔDown components. Reproduced from Ref. [1] with permission
The main finding of our study was that, in addition to the cardiac output (CO) itself, the SPV and the dDown were the parameters that best correlated with the degree of blood withdrawal, and did it better than the central venous pressure (CVP) and the pulmonary artery occlusion pressure (PAOP) (Fig. 2). In the discussion of this initial paper, we postulated that the SPV reflects ventilation-induced changes in the left ventricular (LV) stroke volume (SV), and that the observed increases in SPV and the dDown during the graded hemorrhage are caused by the more significant transient impact that the mechanical breath has on the venous return in the presence of hypovolemia. We also pointed out that the size of the tidal volume (TV), decreased chest wall compliance, and arrhythmias may seriously confound the clinical usefulness of these variables [1].
The effects of graded blood withdrawal in ventilated dogs (our original study). B baseline; 5, 10, 20, 30 = % of estimated blood volume withdrawal; R retransfusion, HR heart rate, BP blood pressure, CVP central venous pressure, PCWP pulmonary capillary wedge pressure, SPV systolic pressure variation, ΔDown delta down, ΔUp delta up, SVR systemic vascular resistance, r s mean Spearman’s rank coefficient correlation to amount of blood withdrawn. Reproduced from Ref. [1] with permission
In a subsequent study we induced hypotension (mean AP of 50 mmHg) in two groups of dogs by either nitroprusside administration or by hemorrhage [2]. The CO was lower and the SPV and dDown significantly greater in the hemorrhaged group, though the AP, HR, CVP, and PAOP were similar in both groups. In a later clinical study, done in anesthetized patients during spine surgery under controlled hypotension, we found that increases in the SPV and the dDown were frequently the only warning signs of excessive blood loss, and that the dDown was the only parameter that correlated with the CO [3].
In 1989 we published the results of an experimental study in which we examined the effects of pharmacologically induced acute LV failure on the SPV and its components [4]. The depression of LV contractility was associated with a significant decrease in the magnitude of the SPV, which decreased even further after additional fluid loading simulating a state of congestive heart failure (CHF). The observed decrease in the SPV was due to a near disappearance of the dDown, while the dUp became its major component, denoting a transient augmentation of the LV SV (see later). Externally applied chest compressions by an inflatable vest synchronized to the mechanical breaths were found to improve cardiac function and serve as an “LV assist device” during CHF. This study allowed us to conclude that a small SPV indicates a state of hypervolemia and/or CHF (preload independence), and that a prominent dUp component reflects the inspiratory augmentation of the LV SV [4].
In the last study of this initial series, also from 1989, we examined the effects of the size of the TV on the SPV [5]. The SPV was found again to be maximal during hypovolemia and minimal during hypervolemia, and was significantly increased by higher TVs at each volume state (Fig. 3). We concluded that before considering the presence of a large SPV as an indication for fluid administration, the presence of excessive TVs should be excluded [5].
The arterial pressure waveform at tidal volumes of 15 and 25 ml/kg during hypo-, normo-, and hypervolemia in ventilated dogs. a apnea, V T tidal volume. Reproduced from Ref. [5] with permission
We believe that this initial series of experimental studies, done more than 20 years ago, contributed significantly to the clinical use of functional hemodynamic parameters, and helped set the stage for the later introduction of the term “fluid responsiveness” [6], which has become such an integral part of the present care of critically ill patients.
Physiological context
Our work has been inspired by the seminal work of earlier scientists to whom we are greatly indebted. Morgan et al. [7] beautifully described, as early as 1966, the cyclic changes in blood flow in the aorta, vena cava, and pulmonary artery during mechanical ventilation. Massumi et al. [8] described the “reversed pulsus paradoxus”, i.e., the dUp, during CHF. Jardin et al. [9] described the effects of increased intrathoracic pressure on the afterload of the right ventricle (RV). Robotham et al. [10] contributed most significantly to our understanding of heart–lung interaction in their elaborate paper from 1983. Brower et al. [11] made us aware of the importance of the pulmonary blood volume as a reservoir of LV preload. Pinsky et al. [12] showed that the LV SV can be augmented by a mechanical breath. We were especially inspired by an abstract by Coyle et al. [13], published in Anesthesiology in 1983, wherein they described the “positive pressure paradox”, defined as the difference between the maximal and minimal SBP values during one mechanical breath, and further divided it into a “Δdown” and “Δup”. In 15 patients who were ventilated with TV of 12–18 cc/kg (it was 1983 after all!), the Δdown decreased significantly following fluid administration and was therefore marked as an indicator of hypovolemia. In spite of its obligatory limited length, this abstract described all the major hemodynamic effects of the mechanical breath and how they relate to the respiratory variations in the AP.
There are a few more studies that merit our recognition. These include the study by Rick and Burke [14] who linked the “respiratory paradox” to the volume status, the study by Fukamachi et al. [15] done in a model of calves with artificial hearts, and the elegant echocardiographic study by Vieillard-Baron et al. [16] in which the dUp was associated with the inspiratory increase in pulmonary venous blood flow. These studies constitute only a small fraction of the extensive work done by many others who contributed to our current understanding of heart–lung interaction during mechanical ventilation.
Basics of heart–lung interaction and arterial pressure waveform analysis
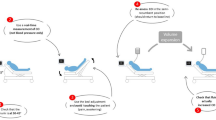
The simplistic physiological explanation for the variations in the AP waveform during mechanical ventilation is based on the fact that, normally, the main hemodynamic effect of the mechanical breath is a transient reduction in venous return. The resulting decreased filling of the right atrium causes a reduction in RV SV which, after a few beats, leads to a reduction in LV preload and a decrease in LV SV. The impact of the transient decrease in the LV preload is dependent on the prevailing slope of the LV function curve. When the slope is steep, as is normally the case during hypovolemia, the decrease in preload will cause more pronounced decreases in LV SV, while during hypervolemia or LV failure, the decrease in preload will have a much lesser effect on LV SV, if at all [4, 17]. The surprisingly dependable sensitivity of the SPV and the dDown to small changes in the circulating blood volume is what struck us most during our preliminary series of experiments. In a much more recent study that we have done in 118 patients undergoing autologous hemodilution, the SPV and dDown, like other dynamic parameters, have increased significantly after the removal of only 4 % of the estimated circulating blood volume [18]. Nearly a third of these patients tolerated a 20 % decrease of their circulating blood volume without hypotension, attesting to the usefulness of dynamic parameters to detect compensated (latent) hypovolemia [19]. Similarly, in fluid-responsive patients, dynamic parameters decrease significantly following fluid loading (Fig. 4), and may detect a fluid-induced increase in CO with excellent sensitivity and specificity [20].
Arterial blood pressure and airway pressure waveform before (left) and after (right) volume loading, which caused the systolic pressure variation (SPV) to decrease from 20 mmHg (left) to 10 mmHg (right). The horizontal reference line indicates a short period of apnea, which defines the SPV into its ΔDown and ΔUp components. Reproduced from Ref. [32] with permission
While the increased intrathoracic pressure transiently decreases venous return to the right heart, it normally increases the filling of the LV by squeezing the pulmonary blood volume which serves as a reservoir of LV preload. This normally occurring increase in LV preload causes a transient increase in the LV SV during early inspiration. This increase is more pronounced in the presence of LV failure, since the increase in pleural pressure facilitates LV ejection when contractility is impaired (afterload reduction). A more detailed description of the physiology of heart–lung interaction and how they are reflected in the respiratory variations of the AP can be found elsewhere [21–24].
Where our findings have been directly or indirectly confirmed
The penetration of the SPV concept into mainstream clinical practice was exceedingly slow at first [23], but has increased dramatically over the last 10 years. Listing all the confirmatory studies on the value of dynamic parameters in predicting fluid responsiveness is beyond the scope of this article, and interested readers are referred to the following reviews which attest to the growing interest in these parameters [25–31].
The first important clinical study was done in patients following abdominal aortic surgery by Coriat et al. [32], who showed that the initial SPV and dDown, unlike the PAOP, were the only hemodynamic variables that correlated significantly with the LV end-diastolic area (EDA). Another significant clinical study, done by Tavernier et al. [33] in patients with sepsis-induced hypotension, demonstrated that the dDown was a more accurate indicator of the SV response volume loading than the EDA and the PAOP, and introduced the terms “responders” and “non-responders”. In an accompanying invited editorial we described the usefulness of dynamic parameters in assessing fluid responsiveness, their normal values, and the factors that may render them inaccurate and misleading, including spontaneous ventilation, arrhythmias, reduced chest wall compliance, and air-trapping [6]. The next major step in the story of pressure waveform analysis was the introduction of the pulse pressure variation (PPV) by Michard and Teboul et al. in two seminal studies in 1999 and 2000 [34, 35]. The first of these studies showed a strong relationship between PPV and the effects of both PEEP and fluid loading on the CO [34]. This study validated our previous experimental study in which we showed that the PEEP-induced decrease in CO was reflected by the SPV, and that this effect was absent in the presence of acute LV failure [36].
The definitive PPV study by the group of Michard and Teboul [35] was done in septic patients with acute circulatory failure, in which the PPV and the SPV were found to be higher in “responders” than in “non-responders”. The 13 % reported cutoff value for the PPV has been validated, with a few variations, by others as well and has become a well-known parameter in hemodynamic monitoring. The PPV was also found to be somewhat more accurate than the SPV in predicting fluid responsiveness (Fig. 4), since the pulse pressure (PP) is directly proportional to LV SV (when aortic compliance is constant), while the SPV may have an element of transmitted pleural pressure [10, 24, 35]. This finding has been demonstrated by others as well, including our own study in patients following cardiac surgery (Fig. 5) [37].
ROC curves comparing the ability of ΔPP (pulse pressure variation, PPV), ΔPS (systolic pressure variation, SPV), RAP (right atrial pressure), and PAOP (pulmonary artery occlusion pressure) to discriminate responder (CI increase >15 %) and non-responder patients to volume expansion. Reproduced from Ref. [35] with permission
The introduction of automated calculation of dynamic parameters into many different modern monitors has contributed significantly to their growing popularity. In addition to an automated measurement of PPV, the pulse contour analysis method for the determination of continuous CO has enabled the continuous measurement of the stroke volume variation (SVV) as well. In 2001 we published the first study, done in neurosurgical patients, to show that the SVV is a better predictor of fluid responsiveness than the CVP and the AP [38]. Reuter et al. followed with a series of similar studies in cardiac surgical patients [39–42]. Of special note is their finding that even patients with decreased LV function (EF <35 %) can present with increased values of SVV and can respond favorably to fluid loading [42]. In a later study, we also found that the distribution of ‘responders’ and ‘non-responders’ was equal between cardiac surgical patients with normal and abnormal LV function [37].
Since the year 2000 many more studies exploring mainly the PPV and SVV were published by various groups using various devices. In addition, many other functional hemodynamic parameters were described, including the respiratory changes in the aortic blood velocity and velocity–time integral [43–45], in the diameter of the superior and inferior vena cava [46–49], in the pre-ejection period [50], and in the plethysmographic signal, described by our group as early as 1999 [51]. Although seemingly different from each other, all these parameters are based on the hemodynamic response to the mechanical breath, and therefore share the same general principles and confounding factors [52].
Contradictions and controversies
There were very few early studies in which the SPV was not found to be a useful indicator of changes in the volume status. These include the one by Dalibon et al. [53], who allowed for the BP to drop to very low levels during graded hemorrhage in pigs without using %SPV and %dDown values as previously recommended [6], and another small clinical study which found the PAOP to be a better predictor of the response to a fluid challenge than the SPV and dDown [54]. Another reservation regarding the concept and clinical significance of the SPV was raised by Pinsky, who suggested that the SPV does not reflect true changes in LV SV since it is caused by direct transmission of intrathoracic pressure to the aorta, similar to a Valsalva maneuver [24, 55, 56].
Indeed the respiratory variations in the SBP may be somewhat influenced by the transmission of airway pressure during the mechanical breath [23]. This may account for the SPV being somewhat less accurate than the PPV, as previously mentioned. However, the clinical significance of this potential source of inaccuracy needs to be put in perspective. According to a systematic review of the literature from 2009 [28], the pooled correlation coefficients between the baseline PPV, SVV and SPV and the change in CO following a fluid challenge were 0.78, 0.72, and 0.72, respectively, while the area under the ROC curves were 0.94, 0.84, and 0.86, respectively (as compared with 0.55 for the CVP, 0.56 for the global end-diastolic volume index, and 0.64 for the LV EDA). The small difference between the SPV, PPV, and SVV can also be seen in Figs. 5 [35] and 6 [37], both of which show how much better all these dynamic parameters perform in comparison to static parameters of preload.
Comparison of areas under the ROC curves for parameters used to predict fluid responsiveness. a Static preload parameters. EDAI left ventricular end-diastolic area, ITBVI intrathoracic blood volume index, MAP mean arterial pressure, CVP central venous pressure. b Dynamic parameters. RSVT respiratory systolic variation test, SPV systolic pressure variation, PPV pulse pressure variation, dDOWN delta Down, SVV stroke volume variation. Reproduced from Ref. [37] with permission
Another important factor that is rarely taken into account when comparing the SPV to the PPV is that the latter changes more when hypovolemia develops, owing to the changing relationship between the SV and the PP when the compliance of the aorta is greatly increased. This has been shown by us both experimentally [57] and clinically [18]. In this recent clinical study the SPV had the same sensitivity to blood withdrawal, less magnitude of change but more consistency than the PPV [18]. Our last argument for regarding the SPV as a parameter that still has great clinical value is that, unlike the PPV [58], the SPV can be “eyeballed” directly from the monitor screen [59]. This makes the SPV more clinically available than the PPV, which is displayed on selected monitors only.
Recognizing the limitations
There are many confounding factors that reduce the clinical usability of dynamic parameters [30]. These limitations preclude the use of these parameters in many patients, both in the operating room [60] and especially in the ICU [61]. These limitations should be well recognized so that dynamic parameters are used only when appropriate. The most significant of these limitations include the presence of any form of spontaneous breathing activity [62, 63] and the magnitude of the TV [5, 41]. Very large TVs may create inordinately high variations [7], while TV less than 8 ml/kg [64] or less than 7 ml/kg [65] may significantly reduce the sensitivity of these parameters. Traditionally, the TVs that were in use in the operating room were above or in [18] the range of 8 ml/kg, enabling the introduction of dynamic parameters into protocols of perioperative optimization [30]. However, the recent finding that lung-protective ventilation strategy may be associated with improved perioperative outcome [66] may reduce the usability of these parameters even in the operating room. The prevalent use of lung protective ventilation may also decrease the usefulness of dynamic parameters in patients with ARDS [67]. In addition, alveolar pressure is less transmitted to the pleural pressure in these patients, resulting in a lesser hemodynamic impact of the mechanical breath. Recent evidence also suggests that low compliance of the respiratory system reduces the accuracy of PPV [68]. And yet, significant hypovolemia may be reflected by dynamic parameters even in patients with ARDS [34].
We have previously suggested standardizing the respiratory ‘stimulus’ by using the respiratory systolic variation test (RSVT) [37, 69]. The RSVT calculates the slope of the minimal SBP values after each of three successive incremental (10, 20, and 30 cmH2O) pressure-controlled breaths. Although such a standardized maneuver may overcome some of the limitations of dynamic parameters, it necessitates a true linkage between the ventilator and the monitor which presents a real barrier to its clinical use.
A less appreciated source of inherent inaccuracy of all the parameters based on the difference between the maximal and minimal values of the SV is the early inspiratory augmentation of LV SV [4, 8, 10, 12, 16]. This augmentation is not related to fluid responsiveness and yet affects the calculation of parameters such as the SPV, PPV, and SVV. This potential source of inaccuracy may explain the “gray zone” phenomenon, namely, that PPV values of 9–13 % may be inconclusive in 25 % of anesthetized patients [70]. In theory, the dDown should be the best parameter to reflect fluid responsiveness as it measures only the decrease in SV following the mechanical breath. However, its measurement necessitates the introduction of a short apnea [1], which is clinically impractical.
Other significant limitations of dynamic parameters are arrhythmias and right heart failure. In the latter condition, large variations in the LV SV may erroneously be interpreted as a sign of fluid responsiveness [47]. However, a lack of response to a volume load in the presence of significantly high dynamic parameters should be seen as an indicator of RV dysfunction, and should trigger an echocardiographic evaluation to confirm the diagnosis [71].
Changing landscape of hemodynamic monitoring
The growing interest in dynamic parameters can be better understood when one considers recent development in hemodynamic monitoring. The declining use of the pulmonary artery catheter has left clinicians with the CVP as the only parameter that can presumably serve as an accurate guide for fluid management. This parameter, however, has been repeatedly shown to be a poor predictor of fluid responsiveness. The sobering realization that the concept of “preload” is both vague and inadequate, combined with the growing awareness of the inherent dangers of fluid overload, led to the recognition that the assessment of fluid responsiveness may be of great value. Fluid responsiveness may, of course, be assessed by a fluid challenge, the effects of which should ideally be monitored by a continuously measured CO. However, repeated fluid challenges may lead to detrimental fluid overload, especially in view of the fact that about 50 % of patients do not increase their CO in response to a fluid challenge [28]. Passive leg raising, which is another ‘dynamic’ maneuver, may be a better alternative to a fluid challenge if and when appropriate, but ideally should also be combined with a continuously monitored CO [68].
In conclusion, the use of dynamic parameters has become more widespread owing to their ability to help detect fluid needs and avoid unnecessary fluid loading. However, decisions regarding hemodynamic management should be based on the integration of parameters of various sources and not on any single parameter. Dynamic parameters may and should be used when making decisions about hemodynamic management, but only when appropriate and only after taking into consideration the entire clinical and physiological picture.
References
Perel A, Pizov R, Cotev S (1987) Systolic blood pressure variation is a sensitive indicator of hypovolemia in ventilated dogs subjected to graded hemorrhage. Anesthesiology 67:498–502
Pizov R, Ya’ari Y, Perel A (1988) Systolic pressure variation is greater during hemorrhage than during sodium nitroprusside-induced hypotension in ventilated dogs. Anesth Analg 67:170–174
Pizov R, Segal E, Kaplan L, Floman Y, Perel A (1990) The use of systolic pressure variation in hemodynamic monitoring during deliberate hypotension in spine surgery. J Clin Anesth 2:96–100
Pizov R, Ya’ari Y, Perel A (1989) The arterial pressure waveform during acute ventricular failure and synchronized external chest compression. Anesth Analg 68:150–156
Szold A, Pizov R, Segal E, Perel A (1989) The effect of tidal volume and intravascular volume state on systolic pressure variation in ventilated dogs. Intensive Care Med 15:368–371
Perel A (1998) Assessing fluid responsiveness by the systolic pressure variation in mechanically ventilated patients. Systolic pressure variation as a guide to fluid therapy in patients with sepsis-induced hypotension. Anesthesiology 89:1309–1310
Morgan BC, Martin WE, Hornbein TF, Crawford EW, Guntheroth WG (1966) Hemodynamic effects of intermittent positive pressure respiration. Anesthesiology 27:584–590
Massumi RA, Mason DT, Vera Z, Zelis R, Otero J, Amsterdam EA (1973) Reversed pulsus paradoxus. N Eng J Med 289:1272–1275
Jardin F, Farcot JC, Gueret P, Prost JF, Ozier Y, Bourdarias JP (1983) Cyclic changes in arterial pulse during respiratory support. Circulation 68:266–274
Robotham JL, Cherry D, Mitzner W, Rabson JL, Lixfeld W, Bromberger-Barnea B (1983) A re-evaluation of the hemodynamic consequences of intermittent positive pressure ventilation. Crit Care Med 11:783–793
Brower R, Wise RA, Hassapoyannes C, Bromberger-Barnea B, Permutt S (1985) Effect of lung inflation on lung blood volume and pulmonary venous flow. J Appl Physiol 58:954–963
Pinsky MR, Matuschak GM, Klain M (1985) Determinants of cardiac augmentation by elevations in intrathoracic pressure. J Appl Physiol 58:1189–1198
Coyle JP, Teplick RS, Long MC (1983) Respiratory variations in systemic arterial pressure as an indicator of volume status. Anesthesiology 59:A53
Rick JJ, Burke SS (1978) Respirator paradox. South Med J 71(1376–1378):1382
Fukamachi K, Irie H, Massiello A, Chen JF, Crouch R, Utoh J, Harasaki H, Golding LA, Kiraly RJ (1992) Effects of mechanical ventilation and spontaneous respiration on hemodynamics in calves with total artificial hearts. ASAIO J 38:M493–M496
Vieillard-Baron A, Chergui K, Augarde R, Prin S, Page B, Beauchet A, Jardin F (2003) Cyclic changes in arterial pulse during respiratory support revisited by Doppler echocardiography. Am J Respir Crit Care Med 168:671–676
Mesquida J, Kim HK, Pinsky MR (2011) Effect of tidal volume, intrathoracic pressure, and cardiac contractility on variations in pulse pressure, stroke volume, and intrathoracic blood volume. Intensive Care Med 37:1672–1679
Pizov R, Eden A, Bystritski D, Kalina E, Tamir A, Gelman S (2012) Hypotension during gradual blood loss: waveform variables response and absence of tachycardia. Br J Anaesth 109:911–918
Perner A, De Backer D (2014) Understanding hypovolaemia. Intensive Care Med 40(4):613–615
Le Manach Y, Hofer CK, Lehot JJ, Vallet B, Goarin JP, Tavernier B, Cannesson M (2012) Can changes in arterial pressure be used to detect changes in cardiac output during volume expansion in the perioperative period? Anesthesiology 117:1165–1174
Michard F, Teboul JL (2000) Using heart-lung interactions to assess fluid responsiveness during mechanical ventilation. Crit Care 4:282–289
Perel A (2005) The physiological basis of arterial pressure variation during positive-pressure ventilation. Reanimation 14:162–171
Michard F (2005) Changes in arterial pressure during mechanical ventilation. Anesthesiology 103:419–428
Pinsky MR (1997) The hemodynamic consequences of mechanical ventilation: an evolving story. Intensive Care Med 23:493–503
Michard F, Teboul JL (2002) Predicting fluid responsiveness in ICU patients: a critical analysis of the evidence. Chest 121:2000–2008
Bendjelid K, Romand JA (2003) Fluid responsiveness in mechanically ventilated patients: a review of indices used in intensive care. Intensive Care Med 29:352–360
Magder S (2004) Clinical usefulness of respiratory variations in arterial pressure. Am J Respir Crit Care Med 169:151–155
Marik PE, Cavallazzi R, Vasu T, Hirani A (2009) Dynamic changes in arterial waveform derived variables and fluid responsiveness in mechanically ventilated patients: a systematic review of the literature. Crit Care Med 37:2642–2647
Cannesson M, Aboy M, Hofer CK, Rehman M (2010) Pulse pressure variation: where are we today? J Clin Monit Comput 25:45–56
Perel A, Habicher M, Sander M (2013) Bench-to-bedside review: functional hemodynamics during surgery—should it be used for all high-risk cases? Crit Care 17:203
Marik PE, Lemson J (2014) Fluid responsiveness: an evolution of our understanding. Br J Anaesth 112:617–620
Coriat P, Vrillon M, Perel A, Baron JF, Le Bret F, Saada M, Viars P (1994) A comparison of systolic blood pressure variations and echocardiographic estimates of end-diastolic left ventricular size in patients after aortic surgery. Anesth Analg 78:46–53
Tavernier B, Makhotine O, Lebuffe G, Dupont J, Scherpereel P (1998) Systolic pressure variation as a guide to fluid therapy in patients with sepsis-induced hypotension. Anesthesiology 89:1313–1321
Michard F, Chemla D, Richard C, Wysocki M, Pinsky MR, Lecarpentier Y, Teboul JL (1999) Clinical use of respiratory changes in arterial pulse pressure to monitor the hemodynamic effects of PEEP. Am J Respir Crit Care Med 159:935–939
Michard F, Boussat S, Chemla D, Anguel N, Mercat A, Lecarpentier Y, Richard C, Pinsky MR, Teboul JL (2000) Relation between respiratory changes in arterial pulse pressure and fluid responsiveness in septic patients with acute circulatory failure. Am J Respir Crit Care Med 162:134–138
Pizov R, Cohen M, Weiss Y, Segal E, Cotev S, Perel A (1996) Positive end-expiratory pressure-induced hemodynamic changes are reflected in the arterial pressure waveform. Crit Care Med 24:1381–1387
Preisman S, Kogan S, Berkenstadt H, Perel A (2005) Predicting fluid responsiveness in patients undergoing cardiac surgery: functional haemodynamic parameters including the respiratory systolic variation test and static preload indicators. Br J Anaesth 95:746–755
Berkenstadt H, Margalit N, Hadani M, Friedman Z, Segal E, Villa Y, Perel A (2001) Stroke volume variation as a predictor of fluid responsiveness in patients undergoing brain surgery. Anesth Analg 92:984–989
Reuter DA, Felbinger TW, Kilger E, Schmidt C, Lamm P, Goetz AE (2002) Optimizing fluid therapy in mechanically ventilated patients after cardiac surgery by on-line monitoring of left ventricular stroke volume variations. Comparison with aortic systolic pressure variations. Br J Anaesth 88:124–126
Reuter DA, Felbinger TW, Schmidt C, Kilger E, Goedje O, Lamm P, Goetz AE (2002) Stroke volume variations for assessment of cardiac responsiveness to volume loading in mechanically ventilated patients after cardiac surgery. Intensive Care Med 28:392–398
Reuter DA, Bayerlein J, Goepfert MS, Weis FC, Kilger E, Lamm P, Goetz AE (2003) Influence of tidal volume on left ventricular stroke volume variation measured by pulse contour analysis in mechanically ventilated patients. Intensive Care Med 29:476–480
Reuter DA, Kirchner A, Felbinger TW, Weis FC, Kilger E, Lamm P, Goetz AE (2003) Usefulness of left ventricular stroke volume variation to assess fluid responsiveness in patients with reduced cardiac function. Crit Care Med 31:1399–1404
Feissel M, Michard F, Mangin I, Ruyer O, Faller JP, Teboul JL (2001) Respiratory changes in aortic blood velocity as an indicator of fluid responsiveness in ventilated patients with septic shock. Chest 119:867–873
Beaussier M, Coriat P, Perel A, Lebret F, Kalfon P, Chemla D, Lienhart A, Viars P (1995) Determinants of systolic pressure variation in patients ventilated after vascular surgery. J Cardiothorac Vasc Anesth 9:547–551
Slama M, Masson H, Teboul JL, Arnout ML, Susic D, Frohlich E, Andrejak M (2002) Respiratory variations of aortic VTI: a new index of hypovolemia and fluid responsiveness. Am J Physiol Heart Circ Physiol 283:H1729–H1733
Vieillard-Baron A, Augarde R, Prin S, Page B, Beauchet A, Jardin F (2001) Influence of superior vena caval zone condition on cyclic changes in right ventricular outflow during respiratory support. Anesthesiology 95:1083–1088
Vieillard-Baron A, Chergui K, Rabiller A, Peyrouset O, Page B, Beauchet A, Jardin F (2004) Superior vena caval collapsibility as a gauge of volume status in ventilated septic patients. Intensive Care Med 30:1734–1739
Feissel M, Michard F, Faller JP, Teboul JL (2004) The respiratory variation in inferior vena cava diameter as a guide to fluid therapy. Intensive Care Med 30:1834–1837
Barbier C, Loubieres Y, Schmit C, Hayon J, Ricome JL, Jardin F, Vieillard-Baron A (2004) Respiratory changes in inferior vena cava diameter are helpful in predicting fluid responsiveness in ventilated septic patients. Intensive Care Med 30:1740–1746
Bendjelid K, Suter PM, Romand J (2004) The respiratory change in preejection period: a new method to predict fluid responsiveness. J Appl Physiol 96:337–342
Shamir M, Eidelman LA, Floman Y, Kaplan L, Pizov R (1999) Pulse oximetry plethysmographic waveform during changes in blood volume. Brit J Anaesth 82:178–181
Perel A (2003) The value of functional hemodynamic parameters in hemodynamic monitoring of ventilated patients. Anaesthesist 52:1003–1004
Dalibon N, Schlumberger S, Saada M, Fischler M, Riou B (1999) Haemodynamic assessment of hypovolemia under general anaesthesia in pigs submitted to graded haemorrhage and retransfusion. Br J Anaesth 82:97–103
Bennett-Guerrero E, Kahn RA, Moskowitz DM, Falcucci O, Bodian CA (2002) Comparison of arterial systolic pressure variation with other clinical parameters to predict the response to fluid challenges during cardiac surgery. Mt Sinai J Med 69:96–100
Pinsky MR (2002) Functional hemodynamic monitoring. Intensive Care Med 28:386–388
Denault AY, Gasior TA, Gorcsan J, Mandarino WA, Deneault LG, Pinsky MR (1999) Determinants of aortic pressure variation during positive-pressure ventilation in man. Chest 116:176–186
Berkenstadt H, Friedman Z, Preisman S, Keidan I, Livingstone D, Perel A (2005) Pulse pressure and stroke volume variations during severe haemorrhage in ventilated dogs. Br J Anaesth 94:721–726
Rinehart J, Islam T, Boud R, Nguyen A, Alexander B, Canales C, Cannesson M (2012) Visual estimation of pulse pressure variation is not reliable: a randomized simulation study. J Clin Monit Comput 26:191–196
Thiele RH, Colquhoun DA, Blum FE, Durieux ME (2012) The ability of anesthesia providers to visually estimate systolic pressure variability using the “eyeball” technique. Anesth Analg 115:176–181
Maguire S, Rinehart J, Vakharia S, Cannesson M (2011) Technical communication: respiratory variation in pulse pressure and plethysmographic waveforms: intraoperative applicability in a North American academic center. Anesth Analg 112:94–96
Mahjoub Y, Lejeune V, Muller L, Perbet S, Zieleskiewicz L, Bart F, Veber B, Paugam-Burtz C, Jaber S, Ayham A, Zogheib E, Lasocki S, Vieillard-Baron A, Quintard H, Joannes-Boyau O, Plantefeve G, Montravers P, Duperret S, Lakhdari M, Ammenouche N, Lorne E, Slama M, Dupont H (2014) Evaluation of pulse pressure variation validity criteria in critically ill patients: a prospective observational multicentre point-prevalence study. Br J Anaesth 112:681–685
Rooke GA, Schwid HA, Shapira Y (1995) The effect of graded hemorrhage and intravascular volume replacement on systolic pressure variation in humans during mechanical and spontaneous ventilation. Anesth Analg 80:925–932
Heenen S, De Backer D, Vincent JL (2006) How can the response to volume expansion in patients with spontaneous respiratory movements be predicted? Crit Care 10:R102
De Backer D, Heenen S, Piagnerelli M, Koch M, Vincent JL (2005) Pulse pressure variations to predict fluid responsiveness: influence of tidal volume. Intensive Care Med 31:517–523
Lansdorp B, Lemson J, van Putten MJ, de Keijzer A, van der Hoeven JG, Pickkers P (2012) Dynamic indices do not predict volume responsiveness in routine clinical practice. Br J Anaesth 108:395–401
Futier E, Pereira B, Jaber S (2013) Intraoperative low-tidal-volume ventilation. N Eng J Med 369:1862–1863
Lakhal K, Ehrmann S, Benzekri-Lefevre D, Runge I, Legras A, Dequin PF, Mercier E, Wolff M, Regnier B, Boulain T (2011) Respiratory pulse pressure variation fails to predict fluid responsiveness in acute respiratory distress syndrome. Crit Care 15:R85
Monnet X, Bleibtreu A, Ferre A, Dres M, Gharbi R, Richard C, Teboul JL (2012) Passive leg-raising and end-expiratory occlusion tests perform better than pulse pressure variation in patients with low respiratory system compliance. Crit Care Med 40:152–157
Perel A, Minkovich L, Preisman S, Abiad M, Segal E, Coriat P (2005) Assessing fluid-responsiveness by a standardized ventilatory maneuver: the respiratory systolic variation test. Anesth Analg 100:942–945
Cannesson M, Le Manach Y, Hofer CK, Goarin JP, Lehot JJ, Vallet B, Tavernier B (2011) Assessing the diagnostic accuracy of pulse pressure variations for the prediction of fluid responsiveness: a “gray zone” approach. Anesthesiology 115:231–241
Michard F, Richards G, Biais M, Lopes M, Auler JO (2010) Using pulse pressure variation or stroke volume variation to diagnose right ventricular failure? Crit Care 14:451
Conflicts of interest
Azriel Perel is a member of the Medical Advisory Board of Pulsion Medical Systems, Munich, Germany, and is the holder of US Patent #5,769,082 on the Respiratory Systolic Variation Test, filing date 18 Jul 1995. RP and SC declare that they have no conflict of interest.
Ethical standard
All human and animal studies have been approved by the appropriate ethics committee and have therefore been performed in accordance with the ethical standards laid down in the 1964 Declaration of Helsinki and its later amendments.
Author information
Authors and Affiliations
Corresponding author
Rights and permissions
About this article
Cite this article
Perel, A., Pizov, R. & Cotev, S. Respiratory variations in the arterial pressure during mechanical ventilation reflect volume status and fluid responsiveness. Intensive Care Med 40, 798–807 (2014). https://doi.org/10.1007/s00134-014-3285-9
Received:
Accepted:
Published:
Issue Date:
DOI: https://doi.org/10.1007/s00134-014-3285-9