Abstract
Purpose
In clinical use of low-level laser therapy for bone regeneration (LLLT), application protocol (dose, duration, and repetitions) has not been established. This study aimed to depict a reliable dosage of LLLT by evaluating the efficacy of different dosing of LLLT (diode) on the healing of rabbit cranial defects.
Methods
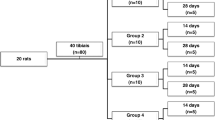
Critical size defects were prepared in calvarias of 26 New Zealand White Rabbits in such each animal containing both test and control groups. Test groups were irradiated with 4 Joule/cm2 (j/cm2), 6 j/cm2, and 8 j/cm2. The rabbits were subjected to six times of laser treatments in 10 days. At the end of the second week, 5 rabbits were sacrificed for histopathological and immunohistochemical analyses. At the 4th and 8th weeks, 20 rabbits (10 each) were sacrificed for micro-CT and histopathological analyses.
Results
Micro-CT evaluation revealed improved new bone formation in all test groups compared to the control group. 6 j/cm2 group demonstrated the highest bone formation. The highest bone morphogenic protein -2 levels were found in the 4 j/cm2 group. Osteocalcin expression was significantly higher in 4 j/cm2 group.
Conclusions
Our findings indicate that LLLT have a positive effect on new bone formation. The high efficacy of doses of 4 j/cm2 and 6 j/cm2 is promising to promote early bone healing.




Similar content being viewed by others
Availability of data and material
All data is available.
References
Eke P et al (2012) CDC Periodontal Disease Surveillance workgroup: James Beck, Gordon Douglass, Roy Page, 2012. Prevalence of periodontitis in adults in the United States: 2009 and 2010. J Dent Res 91: 914-920
Hansson S, Halldin A (2012) Alveolar ridge resorption after tooth extraction: a consequence of a fundamental principle of bone physiology. J Dent Biomech 3:1758736012456543
Seo B-M et al (2004) Investigation of multipotent postnatal stem cells from human periodontal ligament. The Lancet 364(9429):149–155
Pilipchuk SP et al (2015) Tissue engineering for bone regeneration and osseointegration in the oral cavity. Dent Mater 31(4):317–338
Sowmya S et al (2011) Biocompatible β-chitin hydrogel/nanobioactive glass ceramic nanocomposite scaffolds for periodontal bone regeneration. Artif Organs 25(1):1–11
Lindh T et al (1998) A meta-analysis of implants in partial edentulism. Clin Oral Implant Res 9(2):80–90
Giannobile WV et al (2019) Biological factors involved in alveolar bone regeneration: consensus report of Working Group 1 of the 15th European Workshop on Periodontology on Bone Regeneration. J Clin Periodontol 46:6–11
de Miranda, JR et al (2019) Histologic evaluation of early bone regeneration treated with simvastatin associated with low-level laser therapy. International Journal of Oral & Maxillofacial Implants 34(3):658–664
Fekrazad R et al (2015) The effects of combined low level laser therapy and mesenchymal stem cells on bone regeneration in rabbit calvarial defects. J Photochem Photobiol, B 151:180–185
Gabbai A et al (2018) Association of bioglass/collagen/magnesium composites and low level irradiation: effects on bone healing in a model of tibial defect in rats. Laser Ther 27(4):271–282
Hübler R et al (2010) Effects of low-level laser therapy on bone formed after distraction osteogenesis. Lasers Med Sci 25(2):213–219
Metin R, Tatli U, Evlice B (2018) Effects of low-level laser therapy on soft and hard tissue healing after endodontic surgery. Lasers Med Sci 33(8):1699–1706
Marques L et al (2015) New LLLT protocol to speed up the bone healing process—histometric and immunohistochemical analysis in rat calvarial bone defect. Lasers Med Sci 30(4):1225–1230
Medina-Huertas R et al (2014) The effects of low-level diode laser irradiation on differentiation, antigenic profile, and phagocytic capacity of osteoblast-like cells (MG-63). Lasers Med Sci 29(4):1479–1484
Kovacs I (1974) Stimulation of wound healing by laser rays as estimated by means of the rabbit ear chamber method. Acta Chir Acad Sci Hung 15(4):427–32
Cury V et al (2013) Low level laser therapy increases angiogenesis in a model of ischemic skin flap in rats mediated by VEGF, HIF-1α and MMP-2. J Photochem Photobiol, B 125:164–170
Khadra M, Kasem N, Haanaes HR, Ellingsen JE, Lyngstadaas SP (2004) Enhancement of bone formation in rat calvarial bone defects using low-level laser therapy. Oral Surg Oral Med Oral Pathol Oral Radiol Endod 97(6):693–700
Altan AB et al (2015) The effect of dosage on the efficiency of LLLT in new bone formation at the expanded suture in rats. Lasers Med Sci 30(1):255–262
Ng DY et al (2018) A pilot study of laser energy transmission through bone and gingiva. J Am Dent Assoc 149(8):704–711
Huang Y-Y, Chen A C-H, Carroll JD, Hamblin MR (2009) Biphasic dose response in low level light therapy. Dose Response 1;7(4):358–83
Kilkenny C et al (2010) Animal research: reporting in vivo experiments: the ARRIVE guidelines. Br J Pharmacol 160(7):1577
Mester E et al (1968) On the biologic effect of laser rays. Bulletin de la Societe internationale de chirurgie 27(1):68
Batista JD et al (2015) Low-level laser therapy on bone repair: is there any effect outside the irradiated field? Lasers Med Sci 30(5):1569–1574
Sohn JY, Park JC, Um YJ, Jung UW, Kim CS, Cho KS, Choi SH (2010) Spontaneous healing capacity of rabbit cranial defects of various sizes. J Periodontal Implant Sci 40(4):180–187
Zhang J et al (2016) Combination of simvastatin, calcium silicate/gypsum, and gelatin and bone regeneration in rabbit calvarial defects. Sci Rep 6(1):1–12
Fedchenko N, Reifenrath J (2014) Different approaches for interpretation and reporting of immunohistochemistry analysis results in the bone tissue–a review. Diagn Pathol 9(1):221
Kruse A et al (2011) Bone regeneration in the presence of a synthetic hydroxyapatite/silica oxide-based and a xenogenic hydroxyapatite-based bone substitute material. Clin Oral Implant Res 22(5):506–511
Bayat M et al (2005) Low-level laser therapy improves early healing of medial collateral ligament injuries in rats. Photomed Laser Surg 23(6):556–560
Lirani-Galvão AP, Jorgetti V, Da Silva OL (2006) Comparative study of how low-level laser therapy and low-intensity pulsed ultrasound affect bone repair in rats. Photomed Laser Ther 24(6):735–740
Miloro M, Miller JJ, Stoner JA (2007) Low-level laser effect on mandibular distraction osteogenesis. J Oral Maxillofac Surg 65(2):168–176
Wang YH, Wu JY, Kong SC, Chiang MH, Ho ML, Yeh ML, Chen CH (2018) Low power laser irradiation and human adipose-derived stem cell treatments promote bone regeneration in critical-sized calvarial defects in rats. PLoS One 5;13(4):e0195337
Pyo S-J et al (2013) Low-level laser therapy induces the expressions of BMP-2, osteocalcin, and TGF-β1 in hypoxic-cultured human osteoblasts. Lasers Med Sci 28(2):543–550
Silva Júnior AN et al (2002) Computerized morphometric assessment of the effect of low-level laser therapy on bone repair: an experimental animal study. J Clin Laser Med Surg 20(2):83–87
Gurler G, Gursoy B (2018) Investigation of effects of low level laser therapy in distraction osteogenesis. J Stomatol Oral Maxillofac Surg 119(6):469–476
Li Y, Chen SK, Li L, Qin L, Wang XL, Lai YX (2015) Bone defect animal models for testing efficacy of bone substitute biomaterials. J Orthop Translat 3(3):95–104
Atasoy KT, Korkmaz YT, Odaci E, Hanci H (2017) The efficacy of low-level 940 nm laser therapy with different energy intensities on bone healing. Braz Oral Res 31:e7. https://doi.org/10.1590/1807-3107BOR-2017.vol31.0007
Meyer KRM et al (2011) The effect of laser on the stimulation of bone-implant interaction: an experimental study in rabbits. Revista Odonto Ciência 26(3):242–246
Minamisako MC, Ribeiro GH, Lisboa ML, Mariela Rodríguez Cordeiro M, Grando LJ (2016) Medication-related osteonecrosis of jaws: a low-level laser therapy and antimicrobial photodynamic therapy case approach. Case Rep Dent 2016:6267406. https://doi.org/10.1155/2016/6267406
Petri AD et al (2010) Effects of low-level laser therapy on human osteoblastic cells grown on titanium. Braz Dent J 21(6):491–498
Shin S-H et al (2016) Effect of low-level laser therapy on bisphosphonate-treated osteoblasts. Maxillofac Plast Reconstr Surg 38(1):1–8
Garcia VG et al (2014) Effect of LLLT on autogenous bone grafts in the repair of critical size defects in the calvaria of immunosuppressed rats. J Craniomaxillofac Surg 42(7):1196–1202
Moreira GS, Machado Alves PH, Esper LA, Sbrana MC, da Silva Dalben G, Neppelenbroek KH, Fraga de Almeida, A (2018) Effect of low-level laser on the healing of bone defects filled with autogenous bone or bioactive glass: in vivo study. Int J Oral Maxillofac Implants 33(1):169–174
Acknowledgements
The authors express their gratitude to Hacettepe University Advanced Technologies Application and Research Center and also like to thank Ayhan Parmaksiz due to his significant contribution to statistical analyses of the study.
Funding
This project had been supported by Hacettepe University Scientific Research Projects Coordination Unit (Grant no: TSA-2017–14499).
Hacettepe Üniversitesi,Grant no: TSA-2017–14499,Birtan Tolga Yılmaz
Author information
Authors and Affiliations
Corresponding author
Ethics declarations
Conflict of interest
The authors declare no competing interests.
Ethics approval
The study protocol was approved by Hacettepe University Animal Experiments Local Ethics Committee (date/number:28.03.2017/52338575).
Additional information
Publisher's Note
Springer Nature remains neutral with regard to jurisdictional claims in published maps and institutional affiliations.
Rights and permissions
About this article
Cite this article
Yılmaz, B.T., Akman, A.C., Çetinkaya, A. et al. In vivo efficacy of low-level laser therapy on bone regeneration. Lasers Med Sci 37, 2209–2216 (2022). https://doi.org/10.1007/s10103-021-03487-8
Received:
Accepted:
Published:
Issue Date:
DOI: https://doi.org/10.1007/s10103-021-03487-8