Abstract
The incorporation of osteoconductive hydroxyapatite (HA) into poly(Ɛ-polycaprolactone) (PCL) may enhance the material hydrophilicity, protein adsorption, roughness, and consequently, bone formation. In this work, PCL/HA composites with 5, 10, and 25 wt% of HA were prepared by melt compounding followed by hot compression, and their properties such as torque, molecular weight, mechanical resistance, and viscosity were compared to neat PCL to understand the influence of the filler on the polymer stability and printability. The addition of 5 and 10 wt% of HA leads to properties similar to the neat PCL; therefore, these compositions were chosen to produce scaffolds by 3D printing. The scaffolds presented excellent printability and homogenous dispersion of the HA. The compressive strength modulus of both compressed samples and scaffolds is around 30 MPa, similar to cancellous bone. The presence of increasing HA content combined with surface treatment using NaOH enhanced osteoblast proliferation.
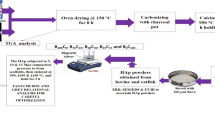
Graphical abstract








Similar content being viewed by others
References
R. Langer, J. Vacanti, Tissue engineering. Science 260, 920–926 (1993). https://doi.org/10.1126/science.8493529
M.A. Woodruff, D.W. Hutmacher, The return of a forgotten polymer—polycaprolactone in the 21st century. Prog. Polym. Sci. 35, 1217–1256 (2010). https://doi.org/10.1016/j.progpolymsci.2010.04.002
Y. Li, C. Liao, S.C. Tjong, Synthetic biodegradable aliphatic polyester nanocomposites reinforced with nanohydroxyapatite and/or graphene oxide for bone tissue engineering applications. Nanomaterials 9, 590 (2019). https://doi.org/10.3390/nano9040590
I. Armentano, M. Dottori, E. Fortunati, S. Mattioli, J.M. Kenny, Biodegradable polymer matrix nanocomposites for tissue engineering: a review. Polym. Degrad. Stab. 95, 2126–2146 (2010). https://doi.org/10.1016/j.polymdegradstab.2010.06.007
E.H. Backes, E.M. Fernandes, G.S. Diogo, C.F. Marques, T.H. Silva, L.C. Costa et al., Engineering 3D printed bioactive composite scaffolds based on the combination of aliphatic polyester and calcium phosphates for bone tissue regeneration. Mater. Sci. Eng. C (2021). https://doi.org/10.1016/j.msec.2021.111928
E.H. Backes, L.D.N. Pires, C.A.G. Beatrice, L.C. Costa, F.R. Passador, L.A. Pessan, Fabrication of biocompatible composites of poly(lactic acid)/hydroxyapatite envisioning medical applications. Polym. Eng. Sci. 60, pen.25322 (2020). https://doi.org/10.1002/pen.25322
S. Afewerki, N. Bassous, S.V. Harb, M.A.F. Corat, S. Maharjan, G.U. Ruiz-Esparza et al., Engineering multifunctional bactericidal nanofibers for abdominal hernia repair. Commun. Biol. 4, 233 (2021). https://doi.org/10.1038/s42003-021-01758-2
K. Rezwan, Q.Z. Chen, J.J. Blaker, A.R. Boccaccini, Biodegradable and bioactive porous polymer/inorganic composite scaffolds for bone tissue engineering. Biomaterials 27, 3413–3431 (2006). https://doi.org/10.1016/j.biomaterials.2006.01.039
L. Peponi, V. Sessini, M.P. Arrieta, I. Navarro-Baena, A. Sonseca, F. Dominici et al., Thermally-activated shape memory effect on biodegradable nanocomposites based on PLA/PCL blend reinforced with hydroxyapatite. Polym. Degrad. Stab. 151, 36–51 (2018). https://doi.org/10.1016/j.polymdegradstab.2018.02.019
L.D. Albrecht, S.W. Sawyer, P. Soman, Developing 3D scaffolds in the field of tissue engineering to treat complex bone defects. 3d Print. Addit. Manuf. 3, 106–112 (2016). https://doi.org/10.1089/3dp.2016.0006
C.A.G. Beatrice, K.M.B. Shimomura, E.H. Backes, S.V. Harb, L.C. Costa, F.R. Passador et al., Engineering printable composites of poly (ε-polycaprolactone)/β-tricalcium phosphate for biomedical applications. Polym. Compos. 42, 1198–1213 (2021). https://doi.org/10.1002/pc.25893
N.L. Leong, N. Kabir, A. Arshi, A. Nazemi, B. Wu, F.A. Petrigliano et al., Evaluation of polycaprolactone scaffold with basic fibroblast growth factor and fibroblasts in an athymic rat model for anterior cruciate ligament reconstruction. Tissue Eng. Part A 21, 1859–1868 (2015). https://doi.org/10.1089/ten.tea.2014.0366
G. Yang, H. Lin, B.B. Rothrauff, S. Yu, R.S. Tuan, Multilayered polycaprolactone/gelatin fiber-hydrogel composite for tendon tissue engineering. Acta Biomater. 35, 68–76 (2016). https://doi.org/10.1016/j.actbio.2016.03.004
F. Ghorbani, L. Moradi, M.B. Shadmehr, S. Bonakdar, A. Droodinia, F. Safshekan, In-vivo characterization of a 3D hybrid scaffold based on PCL/decellularized aorta for tracheal tissue engineering. Mater. Sci. Eng., C 81, 74–83 (2017). https://doi.org/10.1016/j.msec.2017.04.150
L. de Siqueira, F.R. Passador, A.O. Lobo, E.S. de Trichês, Morphological, thermal and bioactivity evaluation of electrospun PCL/β-TCP fibers for tissue regeneration. Polímeros (2019). https://doi.org/10.1590/0104-1428.02118
V. Raeisdasteh Hokmabad, S. Davaran, A. Ramazani, R. Salehi, Design and fabrication of porous biodegradable scaffolds: a strategy for tissue engineering. J. Biomater. Sci. Polym. Ed. 28, 1797–1825 (2017). https://doi.org/10.1080/09205063.2017.1354674
N. Xu, X. Ye, D. Wei, J. Zhong, Y. Chen, G. Xu et al., 3D artificial bones for bone repair prepared by computed tomography-guided fused deposition modeling for bone repair. ACS Appl. Mater. Interfaces 6, 14952–14963 (2014). https://doi.org/10.1021/am502716t
H. Seyednejad, T. Vermonden, N.E. Fedorovich, R. van Eijk, M.J. van Steenbergen, W.J.A. Dhert et al., Synthesis and characterization of hydroxyl-functionalized caprolactone copolymers and their effect on adhesion, proliferation, and differentiation of human mesenchymal stem cells. Biomacromol 10, 3048–3054 (2009). https://doi.org/10.1021/bm900693p
H. Tian, Z. Tang, X. Zhuang, X. Chen, X. Jing, Biodegradable synthetic polymers: preparation, functionalization and biomedical application. Prog. Polym. Sci. 37, 237–280 (2012). https://doi.org/10.1016/j.progpolymsci.2011.06.004
H.J. Jeon, M. Lee, S. Yun, D. Kang, K. Park, S. Choi et al., Fabrication and characterization of 3D-printed biocomposite scaffolds based on PCL and silanated silica particles for bone tissue regeneration. Chem. Eng. J. 360, 519–530 (2019). https://doi.org/10.1016/j.cej.2018.11.176
A. Bruyas, F. Lou, A.M. Stahl, M. Gardner, W. Maloney, S. Goodman et al., Systematic characterization of 3D-printed PCL/β-TCP scaffolds for biomedical devices and bone tissue engineering: Influence of composition and porosity. J. Mater. Res. 33, 1948–1959 (2018). https://doi.org/10.1557/jmr.2018.112
H. Zhang, X. Mao, Z. Du, W. Jiang, X. Han, D. Zhao et al., Three dimensional printed macroporous polylactic acid/hydroxyapatite composite scaffolds for promoting bone formation in a critical-size rat calvarial defect model. Sci. Technol. Adv. Mater. 17, 136–148 (2016). https://doi.org/10.1080/14686996.2016.1145532
C. Martin, H. Winet, J.Y. Bao, Acidity near eroding polylactide-polyglycolide in vitro and in vivo in rabbit tibial bone chambers. Biomaterials 17, 2373–2380 (1996). https://doi.org/10.1016/S0142-9612(96)00075-0
D. Lopes, C. Martins-Cruz, M.B. Oliveira, J.F. Mano, Bone physiology as inspiration for tissue regenerative therapies. Biomaterials 185, 240–275 (2018). https://doi.org/10.1016/j.biomaterials.2018.09.028
R. Khajavi, M. Abbasipour, A. Bahador, Electrospun biodegradable nanofibers scaffolds for bone tissue engineering. J. Appl. Polym. Sci. (2016). https://doi.org/10.1002/app.42883
J. Ren, Y. Wang, Y. Yao, Y. Wang, X. Fei, P. Qi et al., Biological material interfaces as inspiration for mechanical and optical material designs. Chem. Rev. 119, 12279–12336 (2019). https://doi.org/10.1021/acs.chemrev.9b00416
J. Kaur, M.L. Shofner, Surface area effects in hydroxyapatite/poly(ε-caprolactone) nanocomposites. Macromol. Chem. Phys. 210, 677–688 (2009). https://doi.org/10.1002/macp.200800508
J. Hao, M. Yuan, X. Deng, Biodegradable and biocompatible nanocomposites of poly(ϵ-caprolactone) with hydroxyapatite nanocrystals: thermal and mechanical properties. J. Appl. Polym. Sci. 86, 676–683 (2002). https://doi.org/10.1002/app.10955
K.T. Shalumon, J. Anjana, U. Mony, R. Jayakumar, J.P. Chen, Process study, development and degradation behavior of different size scale electrospun poly(caprolactone) and poly(lactic acid) fibers. J. Polym. Res. (2018). https://doi.org/10.1007/s10965-018-1475-9
K.V. Niaza, F.S. Senatov, S.D. Kaloshkin, A.V. Maksimkin, D.I. Chukov, 3D-printed scaffolds based on PLA/HA nanocomposites for trabecular bone reconstruction. J. Phys.: Conf. Ser. 741, 012068 (2016). https://doi.org/10.1088/1742-6596/741/1/012068
S.S.V. Dorozhkin, Bioceramics of calcium orthophosphates. Biomaterials 31, 1465–1485 (2010). https://doi.org/10.1016/j.biomaterials.2009.11.050
A.J. Salinas, M. Vallet-Regí, Evolution of ceramics with medical applications. Z. Anorg. Allg. Chem. 633, 1762–1773 (2007). https://doi.org/10.1002/zaac.200700278
M. Dziadek, E. Stodolak-zych, K. Cholewa-kowalska, Biodegradable ceramic-polymer composites for biomedical applications: a review. Mater. Sci. Eng. C 71, 1175–1191 (2017). https://doi.org/10.1016/j.msec.2016.10.014
S. Afewerki, N. Bassous, S. Harb, C. Palo-Nieto, G.U. Ruiz-Esparza, F.R. Marciano et al., Advances in Antimicrobial and Osteoinductive Biomaterials. Racing for the Surface (Springer, Cham, 2020), pp. 3–34. https://doi.org/10.1007/978-3-030-34471-9_1
G.L. Koons, M. Diba, A.G. Mikos, Materials design for bone-tissue engineering. Nat. Rev. Mater. (2020). https://doi.org/10.1038/s41578-020-0204-2
I.A.W.B. Siqueira, N.K. de Moura, J.P. de Barros Machado, E.H. Backes, F. Roberto Passador, T.E. de Sousa, Porous membranes of the polycaprolactone (PCL) containing calcium silicate fibers for guided bone regeneration. Mater. Lett. (2017). https://doi.org/10.1016/j.matlet.2017.07.011
M. Dziadek, J. Pawlik, E. Menaszek, E. Stodolak-Zych, K. Cholewa-Kowalska, Effect of the preparation methods on architecture, crystallinity, hydrolytic degradation, bioactivity, and biocompatibility of PCL/bioglass composite scaffolds. J. Biomed. Mater. Res. B Appl. Biomater. 103, 1580–1593 (2015). https://doi.org/10.1002/jbm.b.33350
J. Rogowska-Tylman, J. Locs, I. Salma, B. Woźniak, M. Pilmane, V. Zalite et al., In vivo and in vitro study of a novel nanohydroxyapatite sonocoated scaffolds for enhanced bone regeneration. Mater. Sci. Eng. C 99, 669–684 (2019). https://doi.org/10.1016/j.msec.2019.01.084
D. Liu, W. Nie, D. Li, W. Wang, L. Zheng, J. Zhang et al., 3D printed PCL/SrHA scaffold for enhanced bone regeneration. Chem. Eng. J. 362, 269–279 (2019). https://doi.org/10.1016/j.cej.2019.01.015
M.H. Kim, C. Yun, E.P. Chalisserry, Y.W. Lee, H.W. Kang, S.H. Park et al., Quantitative analysis of the role of nanohydroxyapatite (nHA) on 3D-printed PCL/nHA composite scaffolds. Mater. Lett. 220, 112–115 (2018). https://doi.org/10.1016/j.matlet.2018.03.025
S. Gerdes, A. Mostafavi, S. Ramesh, A. Memic, I.V. Rivero, P. Rao et al., Process–structure–quality relationships of three-dimensional printed poly(caprolactone)-hydroxyapatite scaffolds. Tissue Eng. Part A 26, 279–291 (2020). https://doi.org/10.1089/ten.tea.2019.0237
L. Tian, Z. Zhang, B. Tian, X. Zhang, N. Wang, Study on antibacterial properties and cytocompatibility of EPL coated 3D printed PCL/HA composite scaffolds. RSC Adv. 10, 4805–4816 (2020). https://doi.org/10.1039/c9ra10275b
R. Mangal, S. Srivastava, L.A. Archer, Phase stability and dynamics of entangled polymer–nanoparticle composites. Nat. Commun. 6, 7198 (2015). https://doi.org/10.1038/ncomms8198
E.H. Backes, L.N. de Pires, L.C. Costa, F.R. Passador, L.A. Pessan, Analysis of the degradation during melt processing of PLA/Biosilicate® composites. J. Compos. Sci. 3, 52 (2019). https://doi.org/10.3390/jcs3020052
Y. Fan, H. Nishida, S. Hoshihara, Y. Shirai, Y. Tokiwa, T. Endo, Pyrolysis kinetics of poly(l-lactide) with carboxyl and calcium salt end structures. Polym. Degrad. Stab. 79, 547–562 (2003). https://doi.org/10.1016/S0141-3910(02)00374-9
J.J. Blaker, A. Bismarck, A.R. Boccaccini, A.M. Young, S.N. Nazhat, Premature degradation of poly(α-hydroxyesters) during thermal processing of Bioglass®-containing composites. Acta Biomater. 6, 756–762 (2010). https://doi.org/10.1016/j.actbio.2009.08.020
E.H. Backes, L. de Nóbile Pires, H.S. Selistre-de-Araujo, L.C. Costa, F.R. Passador, L.A. Pessan, Development and characterization of printable PLA/β-TCP bioactive composites for bone tissue applications. J. Appl. Polym. Sci. (2020). https://doi.org/10.1002/app.49759
X. Guo, Z. Lin, Y. Wang, Z. He, M. Wang, G. Jin, In-Line Monitoring the Degradation of Polypropylene under Multiple Extrusions Based on Raman Spectroscopy. Polymers 11, 1698 (2019). https://doi.org/10.3390/polym11101698
L.C. Sanchez, C.A.G. Beatrice, C. Lotti, J. Marini, S.H.P. Bettini, L.C. Costa, Rheological approach for an additive manufacturing printer based on material extrusion. Int. J. Adv. Manuf. Technol. (2019). https://doi.org/10.1007/s00170-019-04376-9
R. Steller, Determination of the first normal stress difference from viscometric data for shear flows of polymer liquids. Rheol. Acta 55, 649–656 (2016). https://doi.org/10.1007/s00397-016-0938-3
P. Schümmer, Rheology principles, measurements, and applications. VCH Verlagsgesellschaft, Weinheim 1994. 550 Seiten, 306 Abb., 23 Tab., DM 165.00. CHRISTOPHER W. MACOSKO. Chem. Ing. Tec. 67, 1514–1514 (1995). https://doi.org/10.1002/cite.330671126
B. Huang, P.J. Bártolo, Rheological characterization of polymer/ceramic blends for 3D printing of bone scaffolds. Polym. Test. 68, 365–378 (2018). https://doi.org/10.1016/j.polymertesting.2018.04.033
C.A.G. Beatrice, M.C. Branciforti, R.M.V. Alves, R.E.S. Bretas, Rheological, mechanical, optical, and transport properties of blown films of polyamide 6/residual monomer/montmorillonite nanocomposites. J. Appl. Polym. Sci. 116, 3581–3592 (2010). https://doi.org/10.1002/app.31898
R. Schipani, D.R. Nolan, C. Lally, D.J. Kelly, Integrating finite element modelling and 3D printing to engineer biomimetic polymeric scaffolds for tissue engineering. Connect. Tissue Res. 61, 174–189 (2020). https://doi.org/10.1080/03008207.2019.1656720
S. Jeong, C. Baig, Molecular process of stress relaxation for sheared polymer melts. Polymer 202, 122683 (2020). https://doi.org/10.1016/j.polymer.2020.122683
A. Yeo, W.J. Wong, H.H. Khoo, S.H. Teoh, Surface modification of PCL-TCP scaffolds improve interfacial mechanical interlock and enhance early bone formation: An in vitro and in vivo characterization. J. Biomed. Mater. Res., Part A 92A, 311–321 (2010). https://doi.org/10.1002/jbm.a.32366
L.A. Bosworth, W. Hu, Y. Shi, S.H. Cartmell, Enhancing biocompatibility without compromising material properties: an optimised NaOH treatment for electrospun polycaprolactone fibres. J. Nanomater. 2019, 1–11 (2019). https://doi.org/10.1155/2019/4605092
S. Bagherifard, D.J. Hickey, A.C. de Luca, V.N. Malheiro, A.E. Markaki, M. Guagliano et al., The influence of nanostructured features on bacterial adhesion and bone cell functions on severely shot peened 316L stainless steel. Biomaterials 73, 185–197 (2015). https://doi.org/10.1016/j.biomaterials.2015.09.019
S.V. Harb, N.J. Bassous, T.A.C. de Souza, A. Trentin, S.H. Pulcinelli, C.V. Santilli et al., Hydroxyapatite and β-TCP modified PMMA-TiO2 and PMMA-ZrO2 coatings for bioactive corrosion protection of Ti6Al4V implants. Mater. Sci. Eng., C 116, 111149 (2020). https://doi.org/10.1016/j.msec.2020.111149
G. Hannink, J.J.C. Arts, Bioresorbability, porosity and mechanical strength of bone substitutes: what is optimal for bone regeneration? Injury 42, S22–S25 (2011). https://doi.org/10.1016/j.injury.2011.06.008
T. Almela, I.M. Brook, K. Khoshroo, M. Rasoulianboroujeni, F. Fahimipour, M. Tahriri et al., Simulation of cortico-cancellous bone structure by 3D printing of bilayer calcium phosphate-based scaffolds. Bioprinting 6, 1–7 (2017). https://doi.org/10.1016/j.bprint.2017.04.001
H. Zhou, J. Lee, Nanoscale hydroxyapatite particles for bone tissue engineering. Acta Biomater. 7, 2769–2781 (2011). https://doi.org/10.1016/j.actbio.2011.03.019
S. Afewerki, N. Bassous, S. Harb, C. Palo-Nieto, G.U. Ruiz-Esparza, F.R. Marciano et al., Advances in dual functional antimicrobial and osteoinductive biomaterials for orthopaedic applications. Nanomed.: Nanotechnol. Biol. Med. 24, 102143 (2020). https://doi.org/10.1016/j.nano.2019.102143
Acknowledgments
The authors are thankful to the LMA-IQ (UNESP, Araraquara, Brazil) for the scanning electron microscope facility, to Prof. Ph.D. Silvia H. P. Bettini and M.Sc. Livia G. Gonçalves for the GPC analysis (FAPESP; Grant Number 2011/21313-1), and to Gustavo Valio for donating the PCL. This study was financed in part by the Coordenação de Aperfeiçoamento de Pessoal de Nível Superior - Brasil (CAPES) - Finance Code 001. This work was also supported by CAPES PNPD20131474-33001014004P9 and Fundação de Amparo à Pesquisa do Estado de São Paulo (FAPESP), Grant Numbers 2017/09609-9, 2017/11366-7, 2018/14151-4 and 2018/26060-3.
Author information
Authors and Affiliations
Corresponding author
Ethics declarations
Conflict of interest
The authors whose names are listed immediately below certify that they have NO affiliations with or involvement in any organization or entity with any financial interest (such as honoraria; educational grants; participation in speakers’ bureaus; membership, employment, consultancies, stock ownership, or other equity interest; and expert testimony or patent-licensing arrangements), or non-financial interest (such as personal or professional relationships, affiliations, knowledge or beliefs) in the subject matter or materials discussed in this manuscript.
Supplementary Information
Below is the link to the electronic supplementary material.
Rights and permissions
About this article
Cite this article
Backes, E.H., Beatrice, C.A.G., Shimomura, K.M.B. et al. Development of poly(Ɛ-polycaprolactone)/hydroxyapatite composites for bone tissue regeneration. Journal of Materials Research 36, 3050–3062 (2021). https://doi.org/10.1557/s43578-021-00316-0
Received:
Accepted:
Published:
Issue Date:
DOI: https://doi.org/10.1557/s43578-021-00316-0