Abstract
The present piece of research work is framed for improving the solubility of ketoprofen by forming co-crystal using fumaric acid as a coformer. Co-crystal of ketoprofen and fumaric acid was prepared by simple solvent-assisted grinding method, containing drug and coformer as independent variables and solubility and % drug release were assumed to be dependent variables. Differential scanning calorimetry, Fourier transform infrared spectroscopy, X-ray diffraction, nuclear magnetic resonance and scanning electron microscopy techniques were used to characterize the preparation of optimized batch of co-crystal and further, evaluated for in vitro and in vivo anti-inflammatory and analgesic activities. Based on results of solubility and dissolution rate studies the formulation showed magnified improvement in both the properties on co-crystallization. The values of Gibbs free energy are negative at all levels of carrier demonstrating spontaneity of the drug solubilization process. The IC50 value of optimized batch of co-crystal formulation and the pure drug was observed as 327.33 μg/ml and 556.11 μg/ml, respectively, demonstrating that co-crystal formulation possesses more percentage protection against protein denaturation than the drug ketoprofen. In vivo (anti-inflammatory and analgesic) activities revealed that optimized batch of co-crystal formulation delivered a rapid pharmacological response in Wistar rats and albino mice when compared with standard drug.
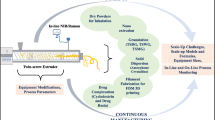
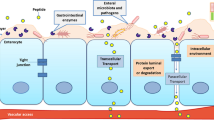
Graphical Abstract










Similar content being viewed by others
Data Availability
All the data are available in the manuscript.
References
Rasenack N, Müller BW. Micron-size drug particles: common and novel micronization techniques. Pharm Dev Technol. 2004;9(1):1–3. https://doi.org/10.1081/PDT-120027417.
Jain NK, Gupta U. Application of dendrimer–drug complexation in the enhancement of drug solubility and bioavailability. Expert Opin Drug Metab Toxicol. 2008;4(8):1035–52. https://doi.org/10.1517/17425255.4.8.1035.
Oprean C, Mioc M, Csányi E, Ambrus R, Bojin F, Tatu C, Cristea M, Ivan A, Danciu C, Dehelean C, Paunescu V. Improvement of ursolic and oleanolic acids’ antitumor activity by complexation with hydrophilic cyclodextrins. Biomed Pharmacother. 2016;83:1095–104. https://doi.org/10.1016/j.biopha.2016.08.030.
Medarević D, Kachrimanis K, Djurić Z, Ibrić S. Influence of hydrophilic polymers on the complexation of carbamazepine with hydroxypropyl-β-cyclodextrin. Eur J Pharm Sci. 2015;78:273–85. https://doi.org/10.1016/j.ejps.2015.08.001.
Bhatia M, Devi R. Enhanced Solubility and Drug Release of Ketoprofen Using Lyophilized Bovine Serum Albumin Solid Dispersion. Acta Pharm Sci. 2019;57(1):33. https://doi.org/10.23893/1307-2080.APS.05703.
Bhatia M, Devi S. Development Characterisation and Evaluation of PVP K-30/PEG Solid Dispersion Containing Ketoprofen. Acta Pharm Sci. 2020;58(1):83. https://doi.org/10.23893/1307-2080.APS.05806.
Strickley RG. Solubilizing excipients in oral and injectable formulations. Pharm Res. 2004;21(2):201–30. https://doi.org/10.1023/B:PHAM.0000016235.32639.23.
Witzigmann D, Kulkarni JA, Leung J, Chen S, Cullis PR, van der Meel R. Lipid nanoparticle technology for therapeutic gene regulation in the liver. Adv Drug Deliv Rev. 2020;159:344–63. https://doi.org/10.1016/j.addr.2020.06.026.
Wang Y, Zheng Z, Wang K, Tang C, Liu Y, Li J. Prebiotic carbohydrates: Effect on physicochemical stability and solubility of algal oil nanoparticles. Carbohydr Polym. 2020;228:115372. https://doi.org/10.1016/j.carbpol.2019.115372.
Dhiman P, Bhatia M. Microwave assisted quaternized cyclodextrin grafted chitosan (QCD-g-CH) nanoparticles entrapping ciprofloxacin. J Polym Res. 2021;28(5):1–14. https://doi.org/10.1007/s10965-021-02535-9.
Dhiman P, Bhatia M. Ketoconazole loaded quaternized chitosan nanoparticles-PVA film: preparation and evaluation. Polym Bull. 2021;79:1–19. https://doi.org/10.1007/s00289-020-03500-0.
Aloisio C, Bueno MS, Ponte MP, Paredes A, Palma SD, Longhi M. Development of solid self-emulsifying drug delivery systems (SEDDS) to improve the solubility of resveratrol. Ther Deliv. 2019;10(10):626–41. https://doi.org/10.4155/tde-2019-0054.
Czajkowska-Kośnik A, Szekalska M, Amelian A, Szymańska E, Winnicka K. Development and evaluation of liquid and solid self-emulsifying drug delivery systems for atorvastatin. Molecules. 2015;20(12):21010–22. https://doi.org/10.3390/molecules201219745.
Kadu PJ, Kushare SS, Thacker DD, Gattani SG. Enhancement of oral bioavailability of atorvastatin calcium by self-emulsifying drug delivery systems (SEDDS). Pharm Dev Technol. 2011;16(1):65–74. https://doi.org/10.3109/10837450903499333.
Gwak HS, Choi JS, Choi HK. Enhanced bioavailability of piroxicam via salt formation with ethanolamines. Int J Pharm. 2005;297(1–2):156–61. https://doi.org/10.1016/j.ijpharm.2005.03.016.
Coimbra M, Isacchi B, van Bloois L, Torano JS, Ket A, Wu X, Schiffelers RM. Improving solubility and chemical stability of natural compounds for medicinal use by incorporation into liposomes Int. J Pharm. 2011;416(2):433–42. https://doi.org/10.1016/j.ijpharm.2011.01.056.
Zhuang CY, Li N, Wang M, Zhang XN, Pan WS, Peng JJ, Tang X. Preparation and characterization of vinpocetine loaded nanostructured lipid carriers (NLC) for improved oral bioavailability. Int J Pharm. 2010;394(1–2):179–85. https://doi.org/10.1016/j.ijpharm.2010.05.005.
Sun M, Nie S, Pan X, Zhang R, Fan Z, Wang S. Quercetin-nanostructured lipid carriers: characteristics and anti-breast cancer activities in vitro. Colloids Surf B. 2014;113:15–24. https://doi.org/10.1016/j.colsurfb.2013.08.032.
Jornada DH, dos Santos Fernandes GF, Chiba DE, De Melo TRF, Dos Santos JL, Chung MC. The prodrug approach: a successful tool for improving drug solubility. Molecules. 2016;21(1):42. https://doi.org/10.3390/molecules21010042.
Bahr MN, Angamuthu M, Leonhardt S, Campbell G, Neau SH. Rapid screening approaches for solubility enhancement, precipitation inhibition and dissociation of a cocrystal drug substance using high throughput experimentation. J Drug Deliv Sci Technol. 2021;61:102196. https://doi.org/10.1016/j.jddst.2020.102196.
Bhatia M, Kumar A, Verma V, Devi S. Development of ketoprofen-p-aminobenzoic acid co-crystal: formulation, characterization, optimization, and evaluation. Med Chem Res. 2021;30(11):2090–102. https://doi.org/10.1007/s00044-021-02794-7.
Pantwalawalkar J, More H, Bhange D, Patil U, Jadhav N. Novel curcumin ascorbic acid cocrystal for improved solubility. J Drug Deliv Sci Technol. 2021;61:102233. https://doi.org/10.1016/j.jddst.2020.102233.
Cavanagh KL, Kuminek G, Rodríguez-Hornedo N. Cocrystal Solubility Advantage and Dose/Solubility Ratio Diagrams: A Mechanistic Approach To Selecting Additives and Controlling Dissolution–Supersaturation–Precipitation Behavior. Mol Pharm. 2020;17(11):4286–301. https://doi.org/10.1021/acs.molpharmaceut.0c00713.
Kimoto K, Yamamoto M, Karashima M, Hohokabe M, Takeda J, Yamamoto K, Ikeda Y. Pharmaceutical cocrystal development of TAK-020 with enhanced oral absorption. Curr Comput-Aided Drug Des. 2020;10(3):211. https://doi.org/10.3390/cryst10030211.
Guo C, Zhang Q, Zhu B, Zhang Z, Bao J, Ding Q, Mei X. Pharmaceutical Cocrystals of Nicorandil with Enhanced Chemical Stability and Sustained Release. Cryst Growth Des. 2020;20(10):6995–7005. https://doi.org/10.1021/acs.cgd.0c01043.
Sarraguça MC, Ribeiro PR, Dos Santos AO, Lopes JA. Batch statistical process monitoring approach to a cocrystallization process. J pharm sci. 2015;104(12):4099–108. https://doi.org/10.1002/jps.24623.
Soares FL, Carneiro RL. Green synthesis of ibuprofen–nicotinamide cocrystals and in-line evaluation by Raman spectroscopy. Cryst Growth Des. 2013;13(4):1510–7. https://doi.org/10.1021/cg3017112.
Maheshwari C, André V, Reddy S, Roy L, Duarte T, Rodríguez-Hornedo N. Tailoring aqueous solubility of a highly soluble compound via cocrystallization: effect of coformer ionization, pH max and solute–solvent interactions. Cryst Eng Comm. 2012;14(14):4801–11. https://doi.org/10.1039/C2CE06615G.
Sathisaran I, Dalvi SV. Engineering cocrystals of poorly water-soluble drugs to enhance dissolution in aqueous medium. Pharmaceutics. 2018;10(3):108. https://doi.org/10.3390/pharmaceutics10030108.
Amin MA, Osman SK, Aly UF. Preparation and characterization of ketoprofen nanosuspension for solubility and dissolution velocity enhancement. Int J Pharma Bio Sci. 2013;4:768–80.
Yadav PS, Kumar V, Singh UP, Bhat HR, Mazumder B. Physicochemical characterization and in vitro dissolution studies of solid dispersions of ketoprofen with PVP K30 and d-mannitol. SAUDI PHARM J. 2013;21(1):77–84. https://doi.org/10.1016/j.jsps.2011.12.007.
Nikumbh KV, Sevankar SG, Patil MP. Formulation development, in vitro and in vivo evaluation of microemulsion-based gel loaded with ketoprofen. Drug Deliv. 2015;22(4):509–15. https://doi.org/10.3109/10717544.2013.859186.
Ambala R, Vemula SK. Formulation and characterization of ketoprofen emulgels. J Applied Pharma Sci. 2015;5(7):112–7. https://doi.org/10.7324/JAPS.2015.50717.
Attia MF, Anton N, Khan IU, Serra CA, Messaddeq N, Jakhmola A, Vecchione R, Vandamme T. One-step synthesis of iron oxide polypyrrole nanoparticles encapsulating ketoprofen as model of hydrophobic drug. Int J Pharm. 2016;508(1–2):61–70. https://doi.org/10.1016/j.ijpharm.2016.04.073.
Shah PP, Desai PR, Singh M. Effect of oleic acid modified polymeric bilayered nanoparticles on percutaneous delivery of spantide II and ketoprofen. J control Release. 2012;158(2):336–45. https://doi.org/10.1016/j.jconrel.2011.11.016.
Gul R, Ahmed N, Ullah N, Khan MI, Elaissari A. Biodegradable ingredient-based emulgel loaded with ketoprofen nanoparticles. AAPS Pharm Sci Tech. 2018;19(4):1869–81. https://doi.org/10.1208/s12249-018-0997-0.
Kheradmandnia S, Vasheghani-Farahani E, Nosrati M, Atyabi F. Preparation and characterization of ketoprofen-loaded solid lipid nanoparticles made from beeswax and carnauba wax. NANOMED- NANOTECHNOL Bio Med. 2010;6(6):753–9. https://doi.org/10.1016/j.nano.2010.06.003.
Cirri M, Bragagni M, Mennini N, Mura P. Development of a new delivery system consisting in “drug–in cyclodextrin–in nanostructured lipid carriers” for ketoprofen topical delivery. Eur J Pharm Biopharm. 2012;80(1):46–53. https://doi.org/10.1016/j.ejpb.2011.07.015.
Xi MM, Wang XY, Fang KQ, Gu Y. Study on the characteristics of pectin–ketoprofen for colon targeting in rats. Int J Pharm. 2005;298(1):91–7. https://doi.org/10.1016/j.ijpharm.2005.04.012.
Kluge J, Fusaro F, Casas N, Mazzotti M, Muhrer G. Production of PLGA micro-and nanocomposites by supercritical fluid extraction of emulsions: I. Encapsulation of lysozyme J Supercrit fluids. 2009;50(3):327–35. https://doi.org/10.1016/j.supflu.2009.05.002.
Vittal GV, Deveswaran R, Bharath S, Basavaraj BV, Madhavan V. Formulation and characterization of ketoprofen liquisolid compacts by Box-Behnken design. Int J Pharm investig. 2012;2(3):150. https://doi.org/10.4103/2230-973X.104398.
Perpétuo GL, Chierice GO, Ferreira LT, Fraga-Silva TF, Venturini J, Arruda MS, Bannach G, Castro RA. A combined approach using differential scanning calorimetry with polarized light thermomicroscopy in the investigation of ketoprofen and nicotinamide cocrystal. Thermochim Acta. 2017;651:1. https://doi.org/10.1016/j.tca.2017.02.014.
Evora AO, Bernardes CE, Piedade MFM, Conceição AC, Minas da Piedade ME. Energetics of glycine cocrystal or salt formation with two regioisomers: fumaric acid and maleic acid. Cryst Growth Des. 2019;19(9):5054–64. https://doi.org/10.1021/acs.cgd.9b00379.
Fernandes RP, do Nascimento ALCS, Carvalho ACS, Teixeira JA, Ionashiro M, Caires FJ. Mechanochemical synthesis, characterization, and thermal behavior of meloxicam cocrystals with salicylic acid, fumaric acid, and malic acid. J Therm Anal Calorim. 2019;138(1):765–77. https://doi.org/10.1007/s10973-019-08118-7.
Gonnade RG, Iwama S, Mori Y, Takahashi H, Tsue H, Tamura R. Observation of efficient preferential enrichment phenomenon for a cocrystal of (DL)-phenylalanine and fumaric acid under nonequilibrium crystallization conditions. Cryst Growth Des. 2011;11(2):607–15. https://doi.org/10.1021/cg1015274.
Du Y, Fang HX, Zhang Q, Zhang HL, Hong Z. Spectroscopic investigation on cocrystal formation between adenine and fumaric acid based on infrared and Raman techniques. Spectrochim Acta Part A Mol Biomol Spectrosc. 2016;153:580–5. https://doi.org/10.1016/j.saa.2015.09.020.
Du Y, Cai Q, Xue J, Zhang Q, Qin D. Structural investigation of the cocrystal formed between 5-fluorocytosine and fumaric acid based on vibrational spectroscopic technique. Spectrochim Acta A: Mol Biomol Spectrosc. 2017;178:251–7. https://doi.org/10.1016/j.saa.2017.02.004.
Manoj K, Takahashi H, Iwama S, Gonnade RG, Tsue H, Tamura R. Crystal structure analysis of highly efficient chiral resolution of (RS)-arginine-fumaric acid cocrystal under preferential enrichment conditions. J Mol Struct. 2021;1245:131073. https://doi.org/10.1016/j.molstruc.2021.131073.
Yang D, Cao J, Jiao L, Yang S, Zhang L, Lu Y, Du G. Solubility and stability advantages of a new cocrystal of berberine chloride with fumaric acid. ACS Omega. 2020;5(14):8283–92. https://doi.org/10.1021/acsomega.0c00692.
Kacso I, Rus LM, Martin F, Miclaus M, Filip X, Dan M. Solid-state compatibility studies of Ketoconazole-Fumaric acid co-crystal with tablet excipients. J Therm Anal Calorim. 2021;143(5):3499–506. https://doi.org/10.1007/s10973-020-09340-4.
Bhogala BR, Basavoju S, Nangia A. Tape and layer structures in cocrystals of some di-and tricarboxylic acids with 4, 4’-bipyridines and isonicotinamide. From binary to ternary cocrystals. Cryst Eng Comm. 2005;7:551–62. https://doi.org/10.1039/B509162D.
Sarkar A, Rohani S. Cocrystals of acyclovir with promising physicochemical properties. J Pharm Sci. 2015;104(1):98–105. https://doi.org/10.1002/jps.24248.
Gautam MK, Besan M, Pandit D, Mandal S, Chadha R. Cocrystal of 5-fluorouracil: Characterization and evaluation of biopharmaceutical parameters. AAPS Pharm Sci Tech. 2019;20(4):1–7. https://doi.org/10.1208/s12249-019-1360-9.
Semalty A, Semalty M, Singh D, Rawat MSM. Preparation and characterization of phospholipid complexes of naringenin for effective drug delivery. J Incl phenom Macrocycl Chem. 2010;67(3–4):253–60. https://doi.org/10.1007/s10847-009-9705-8.
Luo Y, Chen S, Zhou J, Chen J, Tian L, Gao W, Zhang Y, Ma A, Li L, Zhou Z. Luteolin cocrystals: Characterization, evaluation of solubility, oral bioavailability and theoretical calculation. J Drug Deliv Sci Technol. 2019;50:248–54. https://doi.org/10.1016/j.jddst.2019.02.004.
Chavan RR, Hosamani KM. Microwave-assisted synthesis, computational studies and antibacterial/anti-inflammatory activities of compounds based on coumarin-pyrazole hybrid. R Soc Open Sci. 2018;5(5): 172435. https://doi.org/10.1098/rsos.172435.
Bhatia M, Rohilla S. Formulation and optimization of quinoa starch nanoparticles: Quality by design approach for solubility enhancement of piroxicam. Saudi Pharma J. 2020;28(8):927–35. https://doi.org/10.1016/j.jsps.2020.06.013.
Shandil A, Yadav M, Sharma N, Nagpal K, Jindal DK, Deep A, Kumar S. Targeting keratinocyte hyperproliferation, inflammation, oxidative species and microbial infection by biological macromolecule-based chitosan nanoparticle-mediated gallic acid–rutin combination for the treatment of psoriasis. Polym Bull. 2020;77(9):4713–38. https://doi.org/10.1007/s00289-019-02984-9.
Khullar R, Kumar D, Seth N, Saini S. Formulation and evaluation of mefenamic acid emulgel for topical delivery. SAUDI PHARMA J. 2012;20(1):63–7. https://doi.org/10.1016/j.jsps.2011.08.001.
Kulkarni SK. Heat and other physiological stress-induced analgesia: catecholamine mediated and naloxone reversible response. Life Sci. 1980;27(3):185–8. https://doi.org/10.1016/0024-3205(80)90136-8.
Olbert M, Gdula-Argasińska J, Nowak G, Librowski T. Beneficial effect of nanoparticles over standard form of zinc oxide in enhancing the anti-inflammatory activity of ketoprofen in rats. Pharmacol Rep. 2017;69(4):679–82.
Sun S, Zhang X, Cui J, Liang S. Identification of the Miller indices of a crystallographic plane: a tutorial and a comprehensive review on fundamental theory, universal methods based on different case studies and matters needing attention. Nanoscale. 2020;12(32):16657–77. https://doi.org/10.1039/D0NR03637D.
Yadav AV, Shete AS, Dabke AP, Kulkarni PV, Sakhare SS. Co-crystals: a novel approach to modify physicochemical properties of active pharmaceutical ingredients. Indian J Pharm Sci. 2009;71(4):359. https://doi.org/10.4103/0250-474X.57283.
Etter MC. Encoding and decoding hydrogen-bond patters of organic compounds. Acc Chem Res. 1990;23:120–6.
MOPAC2016, Version: 20.225W, James J. P. Stewart, Stewart Computational Chemistry, web: http://OpenMOPAC.net. Days left: 237
Alex A. Granovsky, Firefly version 8, www http://classic.chem.msu.su/gran/firefly/index.html
Lu T, Chen F. Quantitative analysis of molecular surface based on improved Marching Tetrahedra algorithm. J Mol Graph Model. 2012;38:314–23. https://doi.org/10.1016/j.jmgm.2012.07.004.
Tian Lu, Chen F. J Comput Chem. 2012;33:580–92.
Humphrey W, Dalke A, Schulten K. VMD - Visual Molecular Dynamics. J Molec Graphics. 1996;14(1):33–8.
Author information
Authors and Affiliations
Contributions
Sunita Devi contributed to conceptualization and writing—original draft preparation; Meenakshi Bhatia contributed to conceptualization and supervision; Ashwini Kumar contributed to review & editing and software; Vikas Verma contributed to writing—review & editing; Snehlata Yadav contributed to review & editing and data curation.
Corresponding authors
Ethics declarations
Ethical Approval and Consent to Participate
This investigation is approved by IAEC, Guru Jambheshwar University of Science and Technology, Hisar, India, under CPCSEA reg. no-IAEC/2021/10–19.
Consent for Publication
Not applicable.
Conflict of Interest
The authors declare that there is no conflict of interest.
Additional information
Publisher's Note
Springer Nature remains neutral with regard to jurisdictional claims in published maps and institutional affiliations.
Theme: Advancements in Modified-release Oral Drug Delivery - Delivery throughout the Gastro-intestinal Tract
Rights and permissions
About this article
Cite this article
Devi, S., Kumar, A., Kapoor, A. et al. Ketoprofen–FA Co-crystal: In Vitro and In Vivo Investigation for the Solubility Enhancement of Drug by Design of Expert. AAPS PharmSciTech 23, 101 (2022). https://doi.org/10.1208/s12249-022-02253-5
Received:
Accepted:
Published:
DOI: https://doi.org/10.1208/s12249-022-02253-5