Abstract
Background
Since 2000, the United Nations’ Millennium Development Goals, which included a goal to improve maternal health by the end of 2015, has facilitated significant reductions in maternal morbidity and mortality worldwide. However, despite more focused efforts made especially by low- and middle-income countries, targets were largely unmet in sub-Saharan Africa, where women are plagued by many challenges in seeking obstetric care. The aim of this review was to synthesise literature on barriers to obstetric care at health institutions in sub-Saharan Africa.
Methods
This review was guided by the Preferred Reporting Items for Systematic Reviews and Meta-Analyses (PRISMA) checklist. PubMed, Cumulative Index to Nursing and Allied Health Literature (CINAHL), and Scopus databases were electronically searched to identify studies on barriers to health facility-based obstetric care in sub-Saharan Africa, in English, and dated between 2000 and 2015. Combinations of search terms ‘obstetric care’, ‘access’, ‘barriers’, ‘developing countries’ and ‘sub-Saharan Africa’ were used to locate articles. Quantitative, qualitative and mixed-methods studies were considered. A narrative synthesis approach was employed to synthesise the evidence and explore relationships between included studies.
Results
One hundred and sixty articles met the inclusion criteria. Currently, obstetric care access is hindered by several demand- and supply-side barriers. The principal demand-side barriers identified were limited household resources/income, non-availability of means of transportation, indirect transport costs, a lack of information on health care services/providers, issues related to stigma and women’s self-esteem/assertiveness, a lack of birth preparation, cultural beliefs/practices and ignorance about required obstetric health services. On the supply-side, the most significant barriers were cost of services, physical distance between health facilities and service users’ residence, long waiting times at health facilities, poor staff knowledge and skills, poor referral practices and poor staff interpersonal relationships.
Conclusion
Despite similarities in obstetric care barriers across sub-Saharan Africa, country-specific strategies are required to tackle the challenges mentioned. Governments need to develop strategies to improve healthcare systems and overall socioeconomic status of women, in order to tackle supply- and demand-side access barriers to obstetric care. It is also important that strategies adopted are supported by research evidence appropriate for local conditions. Finally, more research is needed, particularly, with regard to supply-side interventions that may improve the obstetric care experience of pregnant women.
Systematic review registration
PROSPERO 2014 CRD42014015549
Similar content being viewed by others

Explore related subjects
Find the latest articles, discoveries, and news in related topics.Background
The primary concern of a healthcare system is to efficiently provide evidence-based services that meet the clinical/medical needs of clients, as well as meeting their expectations for receiving good quality care. Ideally, healthcare services should be accessible, available, affordable and acceptable to clients at all times. This is particularly important for vulnerable populations with specific needs, such as pregnant women and their infants. Pregnancy is a particular case in point as it requires defined healthcare services, and at least 15% of all pregnancies (possibly more in sub-Saharan Africa) are complicated by potentially life-threatening conditions [1]. Maternal deaths remain lamentably high, and worldwide, 289,000 women are estimated to have lost their lives to maternal deaths in 2013 alone, approaching two thirds (62%) of these deaths occurred in sub-Saharan Africa. Although complications related to childbirth and pregnancy are not always predictable, most maternal deaths are from preventable or treatable causes [2]. Major contributors to maternal deaths are haemorrhage, hypertensive disorders, sepsis/infections, abortion-related deaths and obstructed labour [3].
Sub-Saharan Africa is currently the world region with the worst maternal health outcomes. In 2013, the maternal mortality ratio (MMR) for this region was 510 per 100,000 live births. By comparison, Eastern Asia, also a developing region, had an MMR of only 95 per 100,000 live births, making it a relatively rare event [2]. High MMRs are not uniformly distributed across sub-Saharan Africa, and it is also unlikely that barriers are evenly distributed. For instance, for every 100,000 live births in 2013, Sierra Leone had an MMR of 1100, Central African Republic had 880, South Sudan had 730, Nigeria had 560, and Ghana had 380 [2]. There is also evidence of substantial disparities in maternal health indicators, by place of residence (rural/urban), socioeconomic status and others, which are indicative of inequities in access to healthcare [2].
The key to averting pregnancy-related ill-health and associated adverse outcomes is ensuring regular and holistic care for women throughout pregnancy and, particularly, during child birth and 24 h after, the critical period with the highest incidence of adverse maternal health events [4]. In order to make such care possible, it is crucial to first identify and eliminate any factors that hinder healthcare access and utilisation. In the presence of adequate healthcare services, there is an opportunity to improve maternal health outcomes [5]. The concept of ‘access’ is better explained using three interrelated dimensions; availability, affordability and acceptability. Hence, efforts aimed at promoting equity of access need to be considered in the wider context of these dimensions. This is because the degree to which a population can gain access to services is not solely dependent on the availability of such services but also on such factors as poverty, organisational and sociocultural barriers [5, 6]. Given the contextual influences on barriers to access, it is best to examine healthcare access from the perspectives of different groups, which may have varying needs, interests and expectations. This notion is reflected in the fact that equity of access may be measured as the availability, utilisation or outcomes of services [5].
There is substantial research and literature on barriers to obstetric care services, as it is an important international public health issue. Similar reviews [7,8,9] have not specifically focused on demand- and supply-side factors or have more broadly examined facilitators and barriers in low- and middle-income countries [7, 9]. In a systematic review by Bohren and colleagues [9], a qualitative evidence synthesis of factors influencing the decision-making process for place of delivery in low- and middle-income countries was conducted. CA Moyer and A Mustafa [8], on the other hand, focused on only quantitative studies that assessed factors associated with facility-based delivery in sub-Saharan Africa. Other researchers adopted a much broader methodology by including reviews and primary studies, regardless of whether a qualitative or quantitative approach was used [7]. The scope of included studies was, however, global. Given that sub-Saharan Africa bears a disproportionately high burden of adverse obstetric outcomes, particularly maternal deaths [2], it is important to identify and consolidate information on trends contributing to the poor outcomes. This mixed-methods review adds to existing knowledge by examining barriers from a more comprehensive viewpoint of providers and service users. It also includes studies with varied methodological approaches. The aim of this review was to synthesise current evidence on barriers to obstetric care at health institutions in sub-Saharan Africa.
Methods
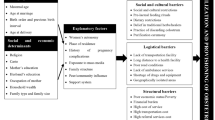
In this study, we systematically reviewed published quantitative research on barriers to obstetric care utilisation in sub-Saharan Africa and employed a narrative synthesis approach to summarising the findings. The study protocol was registered in PROSPERO, CRD42014015549 (http://www.crd.york.ac.uk/PROSPERO/display_record.asp?ID=CRD42014015549) and published in systematic reviews [10]. The analytical framework for barriers to healthcare access developed by Jacobs et al. [11] was employed in the data synthesis. The framework has two overarching categories; demand-side and supply-side barriers. Under each of these categories, there are four principal themes with sub-themes—geographic accessibility, availability, affordability and acceptability—which are based on the dimensions of access. Factors identified in the studies were grouped under the themes, and any factors that did not belong to the pre-defined themes (emergent themes) were listed under ‘other barriers’ and examined further. In order to obtain comprehensive data for the review, we considered studies focusing on the perspectives of health workers (supply-side factors) and health service users (demand-side factors). This approach enabled us to capture the multiple factors that may be at play in impeding efficient maternity care usage. Data from the review revealed similarities and differences across countries in the sub-Saharan African region and provided lessons for future policy planning, practice and research.
Search strategy
We searched the online databases PubMed, CINAHL, and Scopus. Search terms used to locate relevant articles included ‘obstetric care’ with ‘access’, ‘barriers’, ‘developing countries’, ‘pregnancy’, ‘morbidity’, ‘mortality’, ‘haemorrhage’, ‘eclampsia’, ‘sepsis/infection’, ‘obstructed labour’, ‘abortion-related complications’ and ‘sub-Saharan Africa’ (Additional file 1). Articles that met the inclusion criteria were primary research studies that examined barriers to obstetric care, targeted women/service users accessing such care as well as maternity care workers. Studies were also published in a peer reviewed scientific journal in English between 2000 and 2015 and conducted in sub-Saharan Africa. Studies which employed quantitative, qualitative or a mixed-methods design were included. Articles were excluded if the reports were based on secondary data analyses or if data regarding obstetric care barriers is not extractable from the text.
Study selection
The study selection stage, which involved screening of titles and abstracts and retrieval of full texts, was carried out by one author (MKN). Full-text articles were extracted and assessed against the inclusion and exclusion criteria. Selected full-text articles were re-evaluated for data extraction and assessed for quality.
Data extraction and evidence synthesis
The quality of included studies was assessed using the mixed methods appraisal tool (MMAT) by Pluye and colleagues [12]. The tool was suited for this review as it was specifically developed for quality appraisal in systematic reviews involving qualitative, quantitative and mixed-methods designs. MMAT is reported to have an inter-rater reliability score ranging from moderate to perfect [13] and has been applied by other researchers [14,15,16] in mixed-methods systematic reviews. There are five sections in the criteria which include qualitative, randomised controlled, non-randomised, descriptive and mixed-methods studies. Qualitative and quantitative sections have four criteria each, and studies are scored by dividing the number of criteria met by four to arrive at a value ranging from 25 to 100%. For studies with mixed-methods designs, the overall quality score is the lowest score of the study components [17]. All studies were included regardless of their quality ranking since the focus of the review was to examine the context in which barriers to obstetric care occurs (Additional file 2).
Given the range of the outcomes in the studies, identified barriers to obstetric care has been summarised using narrative synthesis. The Popay et al. guidance on the conduct of narrative synthesis in systematic reviews was employed in the synthesis [18]. The elements of the narrative synthesis process are developing a theory, developing a preliminary synthesis, exploring relationships within and between studies, and assessing the robustness of the synthesis. No new theory was developed as part of this review; instead, a pre-existing analytical framework [11] was adopted to facilitate organisation and interpretation of the data. The subsequent step involved the creation of a large table for the extraction of relevant data such as author, year of publication, country, study design, sample characteristics, study objectives, data analysis, major findings and quality assessment (Additional file 3). This important stage was iterative and involved studying the articles, taking notes and making initial comparisons so as to gain familiarisation with the data. Quality appraisal of studies was concomitantly carried out. From the table, the study findings were further examined and using thematic analysis, major themes were coded under pre-defined categories in the analytical framework by Jacobs et al. [11] (Table 1). Emergent themes were also aggregated under the label ‘other barriers’. The underlying methodology applied within the thematic analysis approach was the essentialist or realist method, which is based on the experiences, meanings and the reality of participants [19]. Subsequently, relevant information was drawn out and relationships between the studies were more comprehensively described under the discussion, to enhance interpretation of the review data. Greater attention was paid to differences and similarities between studies as regards the settings, populations, outcomes of interest, methodological approaches and how these might have been reflected in the results. Finally, a critical reflection on the narrative synthesis process was undertaken as regards the quality of the primary studies reviewed and strengths and limitations of this systematic review. In addition, the Preferred Reporting Items for Systematic Reviews and Meta-Analyses (PRISMA) checklist was followed to enhance the quality of reporting [20] (Additional file 4).
The current review was conducted as part of a PhD (by publication) study by MKN. While MKN conducted the data screening and extraction, quality assessment and data synthesis, she did so under the supervision of MCO and TVM, two experienced researchers. All authors had primary responsibility for the development of research questions and study design, and for the intellectual content of the paper. MCO and TVM provided direction and supervision for all aspects of the work and ensured that questions relating to the accuracy or integrity of the work were investigated and resolved. They critically reviewed the methods and made revisions, as required. They also reviewed and discussed the findings and reviewed and edited each draft of the final document.
Results
Overall, 2974 references were initially located through searching the databases, and an additional 63 located through other sources such as checking the reference lists of located papers. After exclusion of duplicates, 2766 remained, of which 385 were retrieved for full-text review. Of these, 225 studies were excluded for reasons such as using secondary data, country of study being outside sub-Saharan Africa and having primary outcomes that fell outside the scope of the present review. The number retained for further analysis was 160 as shown in the PRISMA 2009 flow diagram [20] (Additional file 5: Figure S1)).
Based on the MMAT scoring guide, 160 studies were assessed. Of the total number, 87 studies met all the quality criteria (100%) applicable to the study types, 60 studies fulfilled three criteria (75%), 11 fulfilled two (50%) and two met only one (25%) (Additional file 2).
Characteristics of included studies
Overall, about 51% (n = 82) of included studies employed a quantitative design, 28% (n = 45) were qualitative and 21% (n = 33) were mixed-methods studies. Most of the studies were population- or facility-based cross-sectional surveys, and a few were a combination of both. There were a minority of case-control and cohort studies (Additional file 3). Nearly two thirds (61%) of included studies were conducted in the Eastern African sub-region, about 32% were in Western Africa, 4% were in Southern Africa and 2% in Middle (central) Africa. The studies explored the use of antenatal care, delivery care, postnatal care or a combination of these categories. More than 70% of studies examined access barriers to obstetric care with outcomes relating to the health service users’ perspectives. Study populations identified as service users include females in their reproductive age, pregnant women, postnatal women and, in a few cases, their partners, household heads, mothers-in-law or community leaders. A minority of articles focused on either maternity care workers only or maternity care workers and service users. These studies with a main outcome measure relating to access barriers from maternal healthcare providers’ perspectives assessed the providers’ knowledge and competencies, quality of care, as well as gaps in training and supervision.
Demand- and supply-side barriers
Overall, the analytical framework by Jacobs and colleagues [11] was a valuable tool for organising the wide range of barriers often encountered by obstetric healthcare service providers and those they serve. The framework captured themes and sub-themes that are generally applicable to most healthcare systems/settings. With regards to the findings of this review, most challenges (sub-themes) that were not captured were those specific to the context of care (such as religious beliefs, requiring permission from family/spouse to seek care, rural residence) or to obstetric healthcare provision (unintended pregnancies, non-attendance/low attendance of antenatal clinic, parity, maternal age). Generally, the framework was suited to this review as it provided an effective means of summarising complex and varied data without losing vital aspects of the information gathered. The results are broadly organised under geographic accessibility, availability, affordability and acceptability of services. The main results are summarised in Table 1.
Demand-side barriers
Demand-side barriers include factors that influence health service users as individuals, households or at the community level [21] and include geographic accessibility, availability of health services, affordability and acceptability.
Geographic accessibility
Under geographic accessibility, two main sub-themes are identified; indirect transport costs and means of transport available. Challenges with geographic access at individual or household levels were reported by several studies as lack of transport/difficulty organising transportation or lack of money for the costs associated with transportation [22,23,24,25,26,27,28,29,30,31,32,33,34,35,36,37,38,39,40,41,42,43,44,45,46,47,48,49,50,51,52,53,54,55,56,57,58,59,60,61,62,63,64,65,66,67,68,69,70,71,72,73,74,75,76]. These difficulties may delay or prevent women from seeking appropriate obstetric care, when required.
Availability of services
Ideally, health service users should have the opportunity to utilise health care whenever the need arises; hence, the care available must be suited to the needs of clients, provided by qualified personnel, and equipped with relevant supplies [77]. As a demand-side element, availability encompasses information on health care services/providers and health education. Jacobs et al. [11] explain that services such as counselling and provision of consumer information on health services could help address barriers related to availability. Availability barriers were expressed in various forms, such as perceiving health facility-based care which was not different from other options/alternatives [78]; being unaware of care, type and nature of services [22, 28, 47, 78,79,80,81,82,83] and having limited media exposure [22, 79, 84].
Affordability of services
Affordability includes household resources and willingness to pay, opportunity costs (that is, other benefits lost as a result of seeking care) and cash flow within society. Studies which identified demand-side affordability as a barrier reported primarily on household resources and willingness to pay rather than cash flow within society [22, 23, 25, 26, 31, 32, 34, 36,37,38, 40, 41, 46,47,48, 50, 52, 61, 66,67,68,69,70,71, 73,74,75, 78, 79, 83, 85,86,87,88,89,90,91,92,93,94,95,96,97,98,99,100,101,102,103,104,105,106,107,108,109,110,111,112]. Some studies cited reports by pregnant women of being too busy or having no time as reasons for non-use of maternity care services [22, 26, 63, 86, 100, 113, 114], which represent opportunity costs.
Acceptability of services
From the service users’ perspectives, acceptability of health services encompasses a range of variables including the households’ expectations, women’s self-esteem and assertiveness, community and cultural preferences, stigma and a lack of health awareness. Household expectations included service users’ minimal expectations of cleanliness and non-interference during labour and delivery at health facilities, ability to meet cultural expectations [30] and a perception that health workers were too busy [91]. Social problems related to women’s low self-esteem and assertiveness were highly reported and manifested in various forms such as the husband’s denial of permission, the need for the husband’s/relative’s permission, women’s low decision-making power/autonomy [22, 23, 27,28,29, 33, 39, 46, 49, 51, 60, 62, 64, 66, 68, 69, 71, 73, 78,79,80, 94, 97, 104, 110, 111, 114,115,116,117,118,119,120,121,122] and delayed/ineffective decision-making within the family [47, 56, 65, 123, 124]. Shyness, fear or shame were also reported [28, 113], particularly among sub-groups like teenagers who were possibly afraid of being reprimanded. In an isolated instance, a study by Anyait et al. [38] indicates that women’s autonomy in decision-making promoted antenatal attendance but reduced the likelihood of delivery in health facilities. Also, Kabakyenga et al. [98] found that decisions made together with a husband increased the use of skilled birth attendants as opposed to women making the decision alone.
Community and cultural preferences [59, 121] covers a range of issues and include the following: home delivery being usual practice or feeling more comfortable at home [25, 27, 33, 46, 48, 54, 59, 80, 85, 113, 114]; cultural beliefs/customs [23, 36, 49,50,51, 59, 62, 64, 67,68,69, 71, 75, 78, 108,109,110,111, 125]; having relatives nearby to provide closer attention [22, 27, 80]; ethnicity [75, 90, 92, 126, 127]; unwillingness to see a male doctor [23, 57, 128] and not being afforded the freedom to assume preferred birthing positions [43, 51, 66, 104, 110, 129].
Additionally, a lack of health literacy among health service users was found to significantly impede access to obstetric services [53, 66,67,68, 70, 106, 111, 123, 129,130,131]. This barrier is often highlighted as a lack of perceived need [23, 45, 86, 121] and may be described in diverse ways, including women reporting an absence of illness or indicating that they are ‘doing fine’ [22, 27, 80, 86, 117, 132]; unexpected labour or being unprepared for birth [25, 27, 36, 39, 42, 45, 47, 55, 63, 64, 75, 80, 83, 85, 98, 100, 107, 117, 132, 133] and being unaware of the need to use available services [30, 33, 46, 86, 87, 95, 96, 100, 113, 134].
Stigma perception is another important sub-theme related to acceptability of health services to pregnant women and households. Link and Phelan [135] explain stigma as a phenomenon which involves labelling, stereotyping, separation, status loss and discrimination. Stigma is often associated with particular groups of people in society who may feel vulnerable or have negative attitudes/perceptions about specific social, medical or other problems. For instance, among adolescents, stigma may lead to fear of disclosing pregnancy [28] or non-use of services as a result of feeling shame [49]. Others include fear of HIV-related stigma in pregnancy [83, 94, 136, 137]. In Ethiopia, Fikre and Demissie [39] reported that the social stigma of being considered weak by family members was an important obstacle to utilising health care facilities for delivery.
Other demand-side barriers
Religious reasons for not using obstetric services were cited in some studies [60, 73, 79, 90, 97, 99, 111, 125, 128]. People belonging to Muslim religions [90, 99, 128] and African Traditional Religions (a general term for traditional African beliefs and practices) [79] tended to use services less often. This may be due to cultural restrictions on women within certain households or communities preventing them from leaving their homes or seeking care. Fear of medical procedures such as surgery, episiotomy and blood transfusion hindered access to maternity services in a number of studies [43, 66, 74, 81, 83, 89, 97, 122].
Generally, a low-level of formal education of a woman, husband, couple or household head was a significant barrier to using antenatal, delivery or postnatal services, whereas secondary school and above level of education was associated with better utilisation of maternity services [28, 34, 39, 58, 67, 70, 73, 75, 78,79,80,81,82, 84, 85, 88, 90, 92, 94, 95, 99,100,101, 103, 106, 108, 113, 117, 124, 127, 130, 132, 134, 138,139,140,141,142,143,144].
Several studies showed that obstetric services use decreased with increasing parity, that is, mothers with higher number of children used maternity services less often than nulliparous women and those with two or less children [22, 31, 38, 45, 57, 79, 81,82,83,84, 90, 92, 100, 101, 106, 113, 140, 141, 145,146,147,148]. Additionally, Nwameme et al. [89] reported that for referred obstetric clients, women with higher parity tended to be associated with greater delays between the time referred and compliance with referral.
Some studies reported that comparatively, older women tended to favour home births and utilised health facilities for birthing less often than younger women [32, 45, 58, 75, 80, 84, 106, 132, 146]. Only a few studies reported lower maternal age or teenage motherhood as a barrier [46, 82, 143]. A woman’s marital status, particularly, divorced, separated, single and widowed marital statuses were reported to be associated with lower or non-use of maternity services [57, 82, 101, 113, 117, 136, 145, 149], possibly due to stigma. Women with unplanned or unintended pregnancies made less use of obstetric care services [79, 84, 95, 99, 100, 148], as did women living in rural areas [39, 45, 58, 80, 98, 101, 118, 150]. Late initiation, fewer or non-attendance of antenatal clinics prior to birthing [46, 79, 80, 83, 94, 98, 100, 117, 130, 132, 142, 148] or not receiving counselling at antenatal clinic on facility birthing during pregnancy [118, 149] were important barriers. Women or their partners who were unemployed [82, 143] or employed in agricultural occupations or whose husbands/partners worked in agriculture were also reported to make less use of maternity care services [94, 134].
Supply-side barriers (health system factors)
Supply-side barriers are inhibiting factors that function at the service delivery level and are beyond the control of health service users, for instance, inadequate skilled personnel [21]. Similar to demand-side barriers, they include geographic accessibility, availability, affordability and acceptability of health services.
Geographic accessibility
Service location was widely reported to deter health facility utilisation, since women were often unwilling or unable to cover the distances required to access services [22, 23, 25, 27, 28, 31,32,33, 36, 45, 48, 51,52,53,54, 57, 58, 64,65,66, 68, 69, 71, 72, 76, 78, 82, 83, 85, 88, 89, 91, 92, 95, 96, 98, 104, 106, 107, 113, 114, 121, 123, 124, 130, 137, 139, 140, 142, 146, 151,152,153,154,155,156]. From the health system perspective, this constraint is related to poorly located obstetric health facilities and insufficient number of required facilities.
Availability of services
Women who used or intended to use maternity care services faced challenges such as inadequate facility opening hours [25, 157]; non-availability of services [111, 129, 158], poor (perceptions of) providers’ competence or clinical skills [64, 74, 76, 110, 111, 123, 151, 158,159,160] and knowledge [76, 158, 160,161,162]; inadequate staffing levels [48, 59, 67, 76, 82, 104, 106,107,108, 111, 153, 155, 157, 162,163,164,165] as well as previous experiences of unskilled birthing care from maternity care providers [29]. Generally, women expect to receive care promptly on reaching a health facility; therefore, long waiting times present a significant challenge to accessing health facility-based services [22, 29, 31, 53, 82, 87, 97, 107, 115, 123, 154, 155]. A shortage or absence of drugs and other essential supplies in health facilities were reported in other studies [31, 48, 56, 67, 76, 111, 115, 150, 155, 157, 163, 165,166,167,168], and poor referral practices/systems [104, 105, 159, 165] such as referred clients being transported unaccompanied by healthcare staff [89], lack of feedback mechanisms on referred patients [152], and late or no referral [29] hinder efficient patient care and may result in adverse outcomes.
Affordability of services
Costs of services were a deterrent to obstetric care utilisation for some service users [30, 33, 43, 55, 56, 65, 72, 74, 76, 83, 91, 100, 112, 114, 118, 121, 129, 134, 153], as was informal payments for services [110, 155]. Service costs is a particularly significant barrier for poorer rural populations which tend to be socioeconomically disadvantaged across sub-Saharan Africa.
Acceptability of services
Jacobs et al. [11] identify factors such as complexity of billing system, inability of patients to know prices beforehand and staff interpersonal skills as supply-side elements under acceptability. Poor staff interpersonal skills, either perceived or from previous experiences [53, 65, 68, 74, 75, 103, 111, 121, 128, 129, 133, 154], impacted negatively on service use. Significant issues included a lack of respect for service users [66, 108, 131, 158, 167, 169, 170], a lack of trust/confidence in health professionals or more trust in alternative care [50, 60,61,62, 106, 114, 122, 156, 167] and mistreatment by health workers [22, 27, 28, 30, 33, 41,42,43, 55, 56, 83, 87, 89, 91, 103, 104, 106, 153, 170, 171]. Other negative attitudes of staff, which discourage service users from using maternity services, include a lack of commitment/motivation to work [31, 119, 165, 167], or for instance, expressing a desire to work abroad [152].
Other supply-side barriers
Experiences and perceptions of poor quality of health services also presented challenges for women using obstetric care services [22, 25, 43, 45, 57, 63, 69, 71, 72, 97, 100, 110, 119, 129, 144, 150,151,152, 154, 156, 171, 172]. A lack of supportive care, neglect and poor assessment of labour was reported by Mselle et al. [29] as was a lack of supervision among healthcare workers [29, 44, 160, 167, 173]. Poor staff knowledge about emergency obstetric care (EmOC) and the contents of antenatal care counselling services [173,174,175,176], non-availability of guidelines and clinical protocols [160, 163], and inadequate pre-service and in-service training [160, 168] were additionally reported.
Poor/inadequate facilities and infrastructure [62, 67] such as poor laboratory and ambulance services [115], inadequate health facilities providing essential EmOC [29, 65, 134, 150, 152, 172, 176], lack of cleanliness in facilities [31, 155], overcrowding, [44] and an absence of a reliable power [152, 157, 163] and water supply [157, 163] were other challenges encountered.
Discussion
This review provides a cross-sectional description of published literature on barriers to obstetric care in sub-Saharan Africa between 2000 and 2015. The discussion follows the major themes in the analytical framework employed, which incorporates different dimensions of access and their determinants; geographic accessibility, availability, affordability and acceptability of services [11]. These themes are considered from service–user and service–provider perspectives. The major findings are discussed below and include financial difficulties, transportation-related barriers and sociocultural issues related to service acceptability and availability. Although these barriers are discussed separately, they are not mutually exclusive; hence, interventions have to be considered holistically.
Affordability of services
Health financing policies have received significant interest in recent years, especially in low- and middle-income countries, in a bid to promote equitable financial access to healthcare services, particularly, for the poor. For instance, different forms of user fee abolition have been implemented in Ghana, Kenya, South Africa and Uganda [177]. Reduction or elimination of user fees for maternity services has been reported to increase utilisation [79, 126]. Notwithstanding, this review indicates that limited household resources/income present a substantial barrier for service users across several sub-Saharan African countries, as is demonstrated in the broader literature [112, 178, 179]. Even in countries where maternity services are free, indirect costs, such as transport, may remain a significant barrier for the poor.
In South Asia, a number of countries including Nepal, India, Bangladesh and Pakistan have implemented cash transfer and voucher schemes, which are demand-side financial interventions, to improve maternity care access [180]. These interventions take the form of cash incentives, vouchers, reimbursement of transport cost or free delivery of services. Apart from India, the schemes were at least partly donor-funded. Generally, increased utilisation of maternity services was observed, despite the country-specific challenges encountered, such as corruption, unclear guidelines and inadequate plans for sustainability [180]. With available empirical evidence from other low- and middle-income countries, cash transfer and voucher schemes could be a feasible system for increasing maternity care utilisation in sub-Saharan Africa. The challenge remains to develop models/schemes which are founded on equity and transparency, and rely on state funds rather than donor funds to ensure sustainability.
Geographic accessibility
When obstetric complications are present, a delay in reaching and receiving EmOC can contribute to high MMR and perinatal mortality [181, 182]. Limited geographic access to care were linked to physical distance between health facilities and service users’ residence on the supply side and the availability of means of transportation and indirect costs incurred in order to reach the required facility on the demand side. This is similar to findings in related studies [7, 9]. It has been suggested that the minimum acceptable number of EmOC facilities is at least five facilities per 500,000 population (including at least one comprehensive facility); however, in dispersed settlements/populations, the minimum may need to be exceeded [1]. This review showed that while coverage of EmOC services was inadequate in several sub-Saharan African countries, especially in remote/rural areas, poverty remains a major constraint in accessing obstetric care, due to inability to afford transport costs. Some studies indicated that the poorest women travelled longer distances to reach health facilities. According to D Maine [183], the estimated average time between the onset of the most common major obstetric complication (postpartum haemorrhage) and death is 2 h and 12 h for antepartum haemorrhage, in the absence of medical interventions. It is, therefore, recommended that pregnant women should ideally live within 2 h of a basic EmOC facility and within 12 h of a comprehensive care facility [184].
Healthcare planners must bear in mind the nature of the terrain, means of transportation available to women and levels of health facilities when developing strategies to increase obstetric care coverage. There is a growing body of literature using geographic information system as a means to measure accessibility to health care and geographic coverage in sub-Saharan African countries [185,186,187]; however, most studies are small scale studies, suggesting the need to develop linked national data to support implementation decisions.
Availability of services
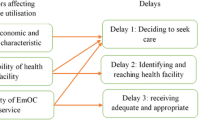
The principal demand-side concern related to health service availability was a lack of information on health care services/providers [22, 78, 79, 81, 84], which limits women’s choices. Knowledge about health services is important in decision-making regarding its utilisation. Hence, this deficit suggests the need for extra efforts to make services known to users, especially, through mass media like radio and television, which is associated with better use of health services in Ghana and Ethiopia [22, 79, 84]. On the supply-side, the most significant barriers were long waiting times at health facilities [22, 29, 31, 81, 87, 97, 115] and, to a lesser extent, poor referral practices [29, 89, 152]. Delays in seeking and receiving obstetric care have been studied extensively and cited frequently. Thaddeus and Maine’s 3-delay model [188] refer to delay in the decision to seek care, delay in arrival at a health facility and delay in the provision of adequate care. The third delay—delay in receiving care upon reaching a health facility—points to gaps in health service delivery [188], as reported by other authors [159, 182, 189]. A systematic review of the third delay reported problems such as under-resourced facilities, non-availability of essential drugs, equipment and blood, inadequate clinical guidelines, shortage of power and water, and referral-related issues such as inadequate emergency transport [181], contributing to adverse maternal outcomes [181, 182].
Acceptability of services
Acceptability encompasses the degree to which health service provision is responsive to the social and cultural expectations of service users [190]. Although the focus of the review literature varied with regard to this dimension of access, major concerns were a lack of health awareness, issues related to stigma and women’s self-esteem/assertiveness. These factors may be difficult to measure, or even anticipate, and may vary by context. Lack of health awareness was prominent in the review literature and may be summarised as showing ignorance about required obstetric health services, for instance, among some pregnant women, an absence of any physical illness meant no need to use maternity services [22, 86]. Stigma or fear of being shamed has been reported by Moyer and Mustapha [8] in a related study. Data from this review suggest that vulnerable populations, such as those with HIV/AIDS and teenagers/adolescents, require targeted approaches to eliminate stigma during their care. The Convention on Elimination of All Forms of Discrimination against Women adopted in 1979 by the United Nations General Assembly is an important document in the history of women’s rights and opportunities [191]. The convention upholds women’s reproductive health rights and, among other things, seeks to establish women’s equal access to good quality healthcare regardless of individual circumstances. Given that most United Nations member countries have ratified the convention, it is important that maternal health is given the attention it requires to reduce adverse outcomes.
Another key finding of this review was that women’s ability to make decisions regarding healthcare is generally weak, with a reliance on husbands/partners and other family members to make such decisions. Conversely, a study in Nepal shows that couple communication and shared decision-making strategies contribute to improvements in pregnancy health practices [192]. In sub-Saharan Africa, approaches to making obstetric care services more acceptable should involve partners and other influential family members like mothers-in-law and encourage joint decision-making. In addition, women should be made aware of their own health needs and taught assertive skills.
On the supply-side, poor interpersonal relationships by staff and associated lack of confidence/trust in services provided presented the most barrier. Poor staff attitudes, whether perceived or experienced, is known to hinder use of obstetric services [9, 193], as these directly influence perceptions of quality of care.
Transferability of findings
Central to the context of sub-Saharan African countries is the fact that healthcare systems mostly function within poor-resource settings, which contribute to several inequities in access to maternal healthcare. These inequities partly set the conditions for differing challenges identified as barriers. Given the similarities found, it appears that the results of this current review are transferable across the region, in a broad sense, since major barriers were common to most of the countries of publication. However, differences in cultural perspectives, values, and organisation of individual healthcare systems mean that detailed attention to the divergent ways and settings in which service provision and utilisation occur is essential to ensuring more meaningful outcomes.
Strengths and limitations
The aim of this review was to synthesise evidence on access barriers from obstetric care provider and service user perspectives. The methodological approach employed was a major strength of the review. By integrating articles with quantitative, qualitative and mixed-methods study designs, a broader cross section of findings was represented. In addition to other factors, quantitative studies were more likely to report socio-demographic-related barriers such as parity, birth order, educational level, place of residence, maternal age and marital status. Qualitative studies provided information on more contextual or descriptive factors such as cultural expectations and beliefs, perceptions, experiences with the health system and health decision-making processes within societies. Similar to the methodology adopted in this review, articles with a mixed-methods approach were more wide-ranging in the scope of obstetric care barriers captured. Generally, the barriers identified within the sub-themes of the analytical framework were from differing study designs rather than a homogeneous source.
Over 70% of studies identified focused on barriers from the perspectives of health service users only. Although the comparatively fewer number of studies on the providers’ perspective may result in less frequently reported health system-related barriers, some were captured through the reports of the service users.
Another limitation of the review should be noted. Data extraction and evidence synthesis in systematic reviews are ideally conducted by at least two reviewers in order to strengthen the reliability of the study outcomes. This is important in systematic reviews of effectiveness; it is critical in qualitative and mixed-method systematic reviews where data extraction and synthesis are even more prone to subjective interpretation. Single-person data extraction and evidence synthesis, as was the case in this study, therefore has implications for the study’s rigour, and the findings reported here must be considered in this context. A team-based process may have affected the reporting of findings in a number of ways, for example by retrieving additional findings, modifying specific findings or changing the relative emphasis on different findings. Nonetheless, efforts were made to ensure that the review process was systematic, with strict adherence to the inclusion and exclusion criteria, as well as the guidelines for quality appraisal for mixed methods [17]. MCO and TVM critically reviewed and discussed the study findings.
Also, the data sources used for this review were limited to primary research published in English and indexed in PubMed, CINAHL, and Scopus databases. Hence, we cannot exclude the possibility that some potentially relevant studies may have been missed as a consequence of being indexed elsewhere or being published in a language other than English. However, the search was comprehensive enough to provide insight into major barriers to obstetric care utilisation in sub-Saharan Africa.
Finally, it is note-worthy that even though an analytical framework provides an easy-to-use tool for analyses, it also has the potential for oversimplification or overfitting of information/data gathered. In order to maximise the technique’s usefulness, an additional generic label—‘other barriers’—was created under supply- and demand-side barriers, respectively, so as to accommodate variables that were not captured under the pre-existing themes.
Implications for research and practice
Previous reviews have helped consolidate knowledge on common barriers to obstetric care in African countries. Insights from the current review build on that knowledge by drawing attention to the significant number of studies reporting the barriers (and facilitators) to obstetric care utilisation and the possibility that the scope and focus of current research may be skewed. The felt needs of service users need to be prioritised and catered to by service providers and those of service providers addressed by policymakers and employers. However, given the relative dearth of research focusing on supply-side barriers, future research should focus on this issue. In particular, intervention studies may offer stronger evidence on workable implementation strategies and shed more light on supply-side issues that are often reported by service users (such as undignified or disrespectful care) but not by providers. This is because service provision characteristics that are frequently cited by service users as barriers may not be identified by providers and may remain largely unresolved. Providers need to address these issues in the same way they address more common barriers like a lack of equipment and supply or inadequate training. Additional research may help service providers understand or clarify why change is needed and to identify potential strategies for improving women’s experiences and expectations. Intervention studies may also assist the development of tools for the training and evaluation of service providers in this regard.
In this review, we highlight the need for greater attention to address barriers to obstetric services. It appears that a common thread between the deterrents to all the dimension of access is poverty/low socioeconomic status. Sub-Saharan African countries will have to more actively pursue interventions targeted at poorer populations, if MMR and other associated adverse outcomes are to be reduced. Although reduction/elimination of user fees for maternity care is gaining popularity in sub-Saharan Africa [177], more needs to be done to reduce indirect costs of care due to widespread poverty. Innovative approaches, such as cash incentives and voucher schemes discussed earlier, seem promising but may require research to test their feasibility and appropriateness for specific contexts. Development of country-level geospatial data on obstetric facilities and services is critical to improving geographic access, as is regular follow-up audits to reassess population changes and associated shifts in obstetric needs.
Additionally, greater focus on human resources for health as regards their knowledge, practical skills and interpersonal relationships is important, as these affect availability and acceptability of services. It appears that the unequal power dynamics between health service providers and service users negatively impacts interpersonal relationships with clients, which in turn influences clients’ willingness to utilise services or comply with health information. Disrespectful care (perceived or experienced), which was frequently reported across several countries, is an important deterrent for clients requiring obstetric care services. Hence, it is essential to sensitise service providers through more focused training and supervision. Finding appropriate avenues to reach potential service users with information about the nature and purpose of available services is also important, as is maternity care workers’ capacity to provide audience-appropriate information to pregnant women and their partners, mothers-in law, household heads and others who influence decisions related to obstetric care utilisation. Non-formal education may also provide a strategy to strengthen women’s decision-making abilities regarding their health care choices.
Healthcare systems may be made more responsive to the needs of target groups if more emphasis is placed on sociocultural sensitivity in midwifery education. The literature demonstrates that by overlooking women’s preferences and concerns such as freedom to choose birthing positions, having a birth partner or family present, and fear of various hospital procedures, vulnerable groups of women are excluded from accessing care. A more open and receptive approach by care providers may improve the acceptability of services and increase obstetric care utilisation.
Conclusion
Barriers to obstetric care access are complex and multi-faceted; hence, they require multi-dimensional approaches that take into consideration the needs of service providers and users. Although the barriers are similar across sub-Saharan African countries, variations exist with regards to the nature and extent of the problem. Country-specific strategies are thus needed to tackle the challenges raised.
Governments are best placed to create favourable conditions to raise the status of women and improve their overall socioeconomic well-being. Improved socio-economic status will have multiple effects and is generally associated with an increased ability to afford health services and associated indirect costs such as means of transport, better access to appropriate health information, higher assertiveness, a reduced likelihood to engage in negative sociocultural practices/beliefs and greater acceptability of maternity care.
Lastly, significant investments in healthcare systems, with a focus on improving healthcare infrastructure (obstetric care facilities, good roads, electricity, water supply, communication) and equipment, human resources for health and community level public health education may lead to improved access to obstetric healthcare services. Identifying and exploiting new opportunities for policies that include key perspectives of accessibility, availability, affordability and acceptability of obstetric care will ensure that important viewpoints or concerns are not overlooked.
Abbreviations
- CINAHL:
-
Cumulative Index to Nursing and Allied Health Literature
- EmOC:
-
Emergency obstetric care
- MMAT:
-
Mixed methods appraisal tool
- MMR:
-
Maternal mortality ratio
- PRISMA:
-
Preferred Reporting Items for Systematic Reviews and Meta-Analyses
References
WHO UNPF, UNICEF, Mailman School of Public Health Averting Maternal Death and Disability programme. Monitoring emergency obstetric care: a handbook. Geneva:WHO; 2009.
WHO, UNICEF, UNFPA, The World Bank and the United Nations Population Division. Trends in maternal mortality: 1990 to 2013: estimates by WHO, UNICEF, UNFPA, The World Bank and the United Nations Population Division. Geneva:WHO; 2014. p. 56.
Khan KS, Wojdyla D, Say L, Gülmezoglu AM, Van Look PF. WHO analysis of causes of maternal death: a systematic review. Lancet. 2006;367(9516):1066–74.
Ronsmans C, Graham WJ, group LMSSs. Maternal mortality: who, when, where, and why. Lancet. 2006;368(9542):1189–200.
Gulliford M, Figueroa-Munoz J, Morgan M, Hughes D, Gibson B, Beech R, Hudson M. What does ‘access to health care’ mean? J Health Serv Res Policy. 2002;7(3):186–8.
Thiede M, Akweongo P, McIntyre D, McIntyre D, Mooney G. Exploring the dimensions of access. Economics of Health Equity. 2007:103–23.
Gabrysch S, Campbell OM. Still too far to walk: literature review of the determinants of delivery service use. BMC Pregnancy Childbirth. 2009;9(1):34.
Moyer CA, Mustafa A. Drivers and deterrents of facility delivery in sub-Saharan Africa: a systematic review. Reprod Health. 2013;10(1):40.
Bohren MA, Hunter EC, Munthe-Kaas HM, Souza JP, Vogel JP, Gülmezoglu AM. Facilitators and barriers to facility-based delivery in low-and middle-income countries: a qualitative evidence synthesis. Reprod Health. 2014;11(1):71.
Kyei-Nimakoh M, Carolan-Olah M, McCann TV. Barriers to obstetric care at health facilities in sub-Saharan Africa—a systematic review protocol. Syst Rev. 2015;4(1):54.
Jacobs B, Ir P, Bigdeli M, Annear PL, Van Damme W. Addressing access barriers to health services: an analytical framework for selecting appropriate interventions in low-income Asian countries. Health Policy Plan. 2012;27(4):288–300.
Pluye P, Gagnon MP, Griffiths F, Johnson-Lafleur J. A scoring system for appraising mixed methods research, and concomitantly appraising qualitative, quantitative and mixed methods primary studies in Mixed Studies Reviews. Int J Nurs Stud. 2009;46(4):529–46.
Pace R, Pluye P, Bartlett G, Macaulay AC, Salsberg J, Jagosh J, Seller R. Testing the reliability and efficiency of the pilot Mixed Methods Appraisal Tool (MMAT) for systematic mixed studies review. Int J Nurs Stud. 2012;49(1):47–53.
McGinn CA, Grenier S, Duplantie J, Shaw N, Sicotte C, Mathieu L, Leduc Y, Légaré F, Gagnon M-P. Comparison of user groups’ perspectives of barriers and facilitators to implementing electronic health records: a systematic review. BMC Med. 2011;9(1):46.
Khanassov V, Vedel I, Pluye P. Case management for dementia in primary health care: a systematic mixed studies review based on the diffusion of innovation model. Clin Interv Aging. 2014;9:915–28.
Pieper MJC, van Dalen-Kok AH, Francke AL, van der Steen JT, Scherder EJA, Husebø BS, Achterberg WP. Interventions targeting pain or behaviour in dementia: a systematic review. Ageing Res Rev. 2013;12(4):1042–55.
Proposal: A mixed methods appraisal tool for systematic mixed studies reviews [http://mixedmethodsappraisaltoolpublic.pbworks.com]
Popay J, Roberts H, Sowden A, Petticrew M, Arai L, Rodgers M, Britten N, Roen K, Duffy S. Guidance on the conduct of narrative synthesis in systematic reviews. A Product from the ESRC Methods Programme Version. 2006;1:b92.
Braun V, Clarke V. Using thematic analysis in psychology. Qual Res Psychol. 2006;3(2):77–101.
Moher D, Liberati A, Tetzlaff J, Altman DG. Preferred reporting items for systematic reviews and meta-analyses: the PRISMA statement. PLoS Med. 2009;6(7):e1000097.
Ensor T, Cooper S. Overcoming barriers to health service access: influencing the demand side. Health Policy Plan. 2004;19(2):69–79.
Birmeta K, Dibaba Y, Woldeyohannes D. Determinants of maternal health care utilization in Holeta town, central Ethiopia. BMC Health Serv Res. 2013;13:256.
Doctor HV, Findley SE, Ager A, Cometto G, Afenyadu GY, Adamu F, Green C. Using community-based research to shape the design and delivery of maternal health services in Northern Nigeria. Reprod Health Matters. 2012;20(39):104–12.
Ekele BA, Tunau KA. Place of delivery among women who had antenatal care in a teaching hospital. Acta Obstet Gynecol Scand. 2007;86(5):627–30.
Exavery A, Kante AM, Njozi M, Tani K, Doctor HV, Hingora A, Phillips JF. Access to institutional delivery care and reasons for home delivery in three districts of Tanzania. Int J Equity Health. 2014;13(1):48.
Groen RS, Solomon J, Samai M, Kamara TB, Cassidy LD, Blok L, Kushner AL, Dhanaraj M, Stekelenburg J. Female health and family planning in Sierra Leone. Obstet Gynecol. 2013;122(3):525–31.
Hailu D, Berhe H. Determinants of institutional childbirth service utilisation among women of childbearing age in urban and rural areas of Tsegedie district, Ethiopia. Midwifery. 2014;30(11):1109–17.
Mbiza CR, Kazembe A, Simwaka A. Barriers to health-seeking practices during pregnancy among adolescents in rural Blantyre, Malawi. Afr J Midwifery Womens Health. 2014;8(2):59–65. 57p.
Mselle LT, Kohi TW, Mvungi A, Evjen-Olsen B, Moland KM. Waiting for attention and care: birthing accounts of women in rural Tanzania who developed obstetric fistula as an outcome of labour. BMC Pregnancy Childbirth. 2011;11(1):75.
Mugweni E, Ehlers VJ, Roos JH. Factors contributing to low institutional deliveries in the Marondera district of Zimbabwe. Curationis. 2008;31(2):5–13.
Mwaniki PK, Kabiru EW, Mbugua GG. Utilisation of antenatal and maternity services by mothers seeking child welfare services in Mbeere District, Eastern Province, Kenya. East Afr Med J. 2002;79(4):184–7.
Peltzer K, Mosala T, Shisana O, Nqeteko A. Utilization of delivery services in the context of prevention of HIV from mother-to-child (PMTCT) in a rural community, South Africa. Curationis. 2006;29(1):54–61.
Shiferaw S, Spigt M, Godefrooij M, Melkamu Y, Tekie M. Why do women prefer home births in Ethiopia? BMC Pregnancy Childbirth. 2013;13:5.
Tann CJ, Kizza M, Morison L, Mabey D, Muwanga M, Grosskurth H, Elliott AM. Use of antenatal services and delivery care in Entebbe, Uganda: a community survey. BMC Pregnancy Childbirth. 2007;7(1):23.
Tlebere P, Jackson D, Loveday M, Matizirofa L, Mbombo N, Doherty T, Wigton A, Treger L, Chopra M. Community-based situation analysis of maternal and neonatal care in South Africa to explore factors that impact utilization of maternal health services. J Midwifery Womens Health. 2007;52(4):342–50.
van den Boogaard J, Arntzen B, Chilwana J, Liyungu M, Mantingh A, Stekelenburg J. Skilled or traditional birth attendant? Choices of communities in Lukulu District, rural Zambia. World Health Popul. 2008;10(1):34–43.
Wilunda C, Putoto G, Manenti F, Castiglioni M, Azzimonti G, Edessa W, Atzori A, Merialdi M, Betran AP, Vogel J, et al. Measuring equity in utilization of emergency obstetric care at Wolisso Hospital in Oromiya, Ethiopia: a cross sectional study. Int J Equity Health. 2013;12:27.
Anyait A, Mukanga D, Oundo GB, Nuwaha F. Predictors for health facility delivery in Busia district of Uganda: a cross sectional study. BMC Pregnancy Childbirth. 2012;12:132.
Fikre AA, Demissie M. Prevalence of institutional delivery and associated factors in Dodota Woreda (district), Oromia regional state, Ethiopia. Reprod Health. 2012;9:33.
Ravit M, Philibert A, Tourigny C, Traore M, Coulibaly A, Dumont A, Fournier P. The hidden costs of a free caesarean section policy in West Africa (Kayes Region, Mali). Matern Child Health J. 2015;19(8):1734–43.
Silal SP, Penn-Kekana L, Barnighausen T, Schneider H. Local level inequalities in the use of hospital-based maternal delivery in rural South Africa. Glob Health. 2014;10:60.
Nakua EK, Sevugu JT, Dzomeku VM, Otupiri E, Lipkovich HR, Owusu-Dabo E. Home birth without skilled attendants despite millennium villages project intervention in Ghana: insight from a survey of women’s perceptions of skilled obstetric care. BMC Pregnancy Childbirth. 2015;15:243.
Liambila WN, Kuria SN. Birth attendance and magnitude of obstetric complications in Western Kenya: a retrospective case-control study. BMC Pregnancy Childbirth. 2014;14:311.
Austin A, Gulema H, Belizan M, Colaci DS, Kendall T, Tebeka M, Hailemariam M, Bekele D, Tadesse L, Berhane Y, et al. Barriers to providing quality emergency obstetric care in Addis Ababa, Ethiopia: healthcare providers’ perspectives on training, referrals and supervision, a mixed methods study. BMC Pregnancy Childbirth. 2015;15:74.
Wilunda C, Quaglio G, Putoto G, Takahashi R, Calia F, Abebe D, Manenti F, Dalla Riva D, Betrán AP, Atzori A. Determinants of utilisation of antenatal care and skilled birth attendant at delivery in South West Shoa Zone, Ethiopia: a cross sectional study. Reprod Health. 2015;12(1):74.
Lakew S, Tachbele E, Gelibo T. Predictors of skilled assistance seeking behavior to pregnancy complications among women at southwest Ethiopia: a cross-sectional community based study. Reprod Health. 2015;12(1):1.
Aarnio P, Chipeta E, Kulmala T. Men’s perceptions of delivery care in rural Malawi: exploring community level barriers to improving maternal health. Health Care Women Int. 2013;34(6):419–39.
Adewemimo AW, Msuya SE, Olaniyan CT, Adegoke AA. Utilisation of skilled birth attendance in Northern Nigeria: a cross-sectional survey. Midwifery. 2014;30(1):e7–e13.
Atuyambe L, Mirembe F, Annika J, Kirumira EK, Faxelid E. Seeking safety and empathy: adolescent health seeking behavior during pregnancy and early motherhood in central Uganda. J Adolesc. 2009;32(4):781–96.
Bazzano AN, Kirkwood B, Tawiah-Agyemang C, Owusu-Agyei S, Adongo P. Social costs of skilled attendance at birth in rural Ghana. Int J Gynaecol Obstet. 2008;102(1):91–4.
Bedford J, Gandhi M, Admassu M, Girma A. ‘A normal delivery takes place at home’: a qualitative study of the location of childbirth in rural Ethiopia. Matern Child Health J. 2013;17(2):230–9.
De Allegri M, Tiendrebeogo J, Muller O, Ye M, Jahn A, Ridde V. Understanding home delivery in a context of user fee reduction: a cross-sectional mixed methods study in rural Burkina Faso. BMC Pregnancy Childbirth. 2015;15:330.
Cham M, Sundby J, Vangen S. Maternal mortality in the rural Gambia, a qualitative study on access to emergency obstetric care. Reprod Health. 2005;2(1):1.
Cofie LE, Barrington C, Singh K, Sodzi-Tettey S, Akaligaung A. Birth location preferences of mothers and fathers in rural Ghana: implications for pregnancy, labor and birth outcomes. BMC Pregnancy Childbirth. 2015;15:165.
Crissman HP, Engmann CE, Adanu RM, Nimako D, Crespo K, Moyer CA. Shifting norms: pregnant women’s perspectives on skilled birth attendance and facility-based delivery in rural Ghana. Afr J Reprod Health. 2013;17(1):15–26.
Essendi H, Mills S, Fotso JC. Barriers to formal emergency obstetric care services’ utilization. J Urban Health. 2011;88 Suppl 2:S356–369.
Faye A, Niane M, Ba I. Home birth in women who have given birth at least once in a health facility: contributory factors in a developing country. Acta Obstet Gynecol Scand. 2011;90(11):1239–43.
Feyissa TR, Genemo GA. Determinants of institutional delivery among childbearing age women in Western Ethiopia, 2013: unmatched case control study. PLoS One. 2014;9(5):e97194.
Gebrehiwot T, San Sebastian M, Edin K, Goicolea I. Health workers’ perceptions of facilitators of and barriers to institutional delivery in Tigray, Northern Ethiopia. BMC Pregnancy Childbirth. 2014;14:137.
Gebrehiwot T, Goicolea I, Edin K, San Sebastian M. Making pragmatic choices: women’s experiences of delivery care in Northern Ethiopia. BMC Pregnancy Childbirth. 2012;12:113.
Kawuwa MB, Mairiga AG, Usman HA. Community perspective of maternal mortality: experience from Konduga Local Government Area, Borno State, Nigeria. Ann Afr Med. 2007;6(3):109–14.
Kwagala B. Birthing choices among the Sabiny of Uganda. Cult Health Sex. 2013;15(sup3):S401–14.
Lerberg PM, Sundby J, Jammeh A, Fretheim A. Barriers to skilled birth attendance: a survey among mothers in rural Gambia. Afr J Reprod Health. 2014;18(1):35–43.
Magoma M, Requejo J, Campbell OM, Cousens S, Filippi V. High ANC coverage and low skilled attendance in a rural Tanzanian district: a case for implementing a birth plan intervention. BMC Pregnancy Childbirth. 2010;10(1):1.
Mills S, Bertrand JT. Use of health professionals for obstetric care in northern Ghana. Stud Fam Plann. 2005;36(1):45–56.
Mwangome FK, Holding PA, Songola KM, Bomu GK. Barriers to hospital delivery in a rural setting in Coast Province, Kenya: community attitude and behaviours. Rural Remote Health. 2012;12:1852.
Oiyemhonlan B, Udofia E, Punguyire D. Identifying obstetrical emergencies at Kintampo Municipal Hospital: a perspective from pregnant women and nursing midwives. Afr J Reprod Health. 2013;17(2):129–40.
Seljeskog L, Sundby J, Chimango J. Factors influencing women's choice of place of delivery in rural Malawi-an explorative study. Afr J Reprod Health. 2006;10(3):66–75.
Sialubanje C, Massar K, Hamer DH, Ruiter RA. Reasons for home delivery and use of traditional birth attendants in rural Zambia: a qualitative study. BMC Pregnancy Childbirth. 2015;15(1):216.
Singh K, Osei-Akoto I, Otchere F, Sodzi-Tettey S, Barrington C, Huang C, Fordham C, Speizer I. Ghana’s National Health insurance scheme and maternal and child health: a mixed methods study. BMC Health Serv Res. 2015;15:108.
Somé DT, Sombie I, Meda N. What prevent women for a sustainable use of maternal care in two medical districts of Burkina Faso? A qualitative study. The Pan African Medical Journal. 2014;18:43. doi:10.11604/pamj.2014.18.43.2210.
Sorensen BL, Nielsen BB, Rasch V, Elsass P. User and provider perspectives on emergency obstetric care in a Tanzanian rural setting: a qualitative analysis of the three delays model in a field study. Afr J Reprod Health. 2011;15(2):117-130.
Moyer CA, Adongo PB, Aborigo RA, Hodgson A, Engmann CM, DeVries R. “It’s up to the woman’s people”: how social factors influence facility-based delivery in Rural Northern Ghana. Matern Child Health J. 2013;18(1):109–19.
Izugbara CO, Kabiru CW, Zulu EM. Urban poor Kenyan women and hospital-based delivery. Public Health Rep. 2009; 124(4):585–589.
Mrisho M, Schellenberg JA, Mushi AK, Obrist B, Mshinda H, Tanner M, Schellenberg D. Factors affecting home delivery in rural Tanzania. Trop Med Int Health. 2007;12(7):862–72.
Stekelenburg J, Kyanamina S, Mukelabai M, Wolffers I, Roosmalen J. Waiting too long: low use of maternal health services in Kalabo, Zambia. Trop Med Int Health. 2004;9(3):390–8.
Kyei-Nimakoh M, Carolan-Olah M, McCann TV. Millennium development Goal 5: progress and challenges in reducing maternal deaths in Ghana. BMC Pregnancy Childbirth. 2016;16(1):1.
Azuogu VC, Azuogu BN, Nwonwu EU. Factors affecting utilization of skilled-provider antenatal care in the rural communities of Ebonyi State, Nigeria. West African J Nursing. 2011;22(1):75–84.
Mills S, Williams JE, Adjuik M, Hodgson A. Use of health professionals for delivery following the availability of free obstetric care in northern Ghana. Matern Child Health J. 2008;12(4):509–18.
Teferra AS, Alemu FM, Woldeyohannes SM. Institutional delivery service utilization and associated factors among mothers who gave birth in the last 12 months in Sekela District, north west of Ethiopia: a community-based cross sectional study. BMC Pregnancy Childbirth. 2012;12:74.
Wanjira C, Mwangi M, Mathenge E, Mbugua G, Ng'ang'a Z. Delivery practices and associated factors among mothers seeking child welfare services in selected health facilities in Nyandarua South District, Kenya. BMC Public Health. 2011;11:360.
Tsawe M, Susuman AS. Determinants of access to and use of maternal health care services in the Eastern Cape, South Africa: a quantitative and qualitative investigation. BMC Res Notes. 2014;7:723.
Kinuthia J, Kohler P, Okanda J, Otieno G, Odhiambo F, John-Stewart G. A community-based assessment of correlates of facility delivery among HIV-infected women in western Kenya. BMC Pregnancy Childbirth. 2015;15(1):1.
Regassa N. Antenatal and postnatal care service utilization in southern Ethiopia: a population-based study. Afr Health Sci. 2011;11(3):390–7.
Amano A, Gebeyehu A, Birhanu Z. Institutional delivery service utilization in Munisa Woreda, South East Ethiopia: a community based cross-sectional study. BMC Pregnancy Childbirth. 2012;12:105.
Egbewale B, Bamidele J. Demographic profile of mothers and their utilisation of maternal health-care services in Osun State, Nigeria. Niger Postgrad Med J. 2009;16(2):132–8.
Fekede B. Antenatal care services utilization and factors associated in Jimma Town (south west Ethiopia). Ethiop Med J. 2007;45(2):123–33.
Hounton S, Chapman G, Menten J, De Brouwere V, Ensor T, Sombie I, Meda N, Ronsmans C. Accessibility and utilisation of delivery care within a Skilled Care Initiative in rural Burkina Faso. Trop Med Int Health. 2008;13 Suppl 1:44–52.
Nwameme A, Phillips J, Adongo P. Compliance with emergency obstetric care referrals among pregnant women in an urban informal settlement of Accra, Ghana. Matern Child Health J. 2014;18(6):1403–12.
Olusanya BO, Alakija OP, Inem VA. Non-uptake of facility-based maternity services in an inner-city community in Lagos, Nigeria: an observational study. J Biosoc Sci. 2010;42(3):341–58.
Silal SP, Penn-Kekana L, Harris B, Birch S, McIntyre D. Exploring inequalities in access to and use of maternal health services in South Africa. BMC Health Serv Res. 2012;12:120.
Spangler SA, Bloom SS. Use of biomedical obstetric care in rural Tanzania: the role of social and material inequalities. Soc Sci Med. 2010;71(4):760–8.
Trani JF, Browne J, Kett M, Bah O, Morlai T, Bailey N, Groce N. Access to health care, reproductive health and disability: a large scale survey in Sierra Leone. Soc Sci Med. 2011;73(10):1477–89.
Turan JM, Hatcher AH, Medema-Wijnveen J, Onono M, Miller S, Bukusi EA, Turan B, Cohen CR. The role of HIV-related stigma in utilization of skilled childbirth services in rural Kenya: a prospective mixed-methods study. PLoS Med. 2012;9(8):e1001295.
Wado YD, Afework MF, Hindin MJ. Unintended pregnancies and the use of maternal health services in Southwestern Ethiopia. BMC International Health and Human Rights. 2013;13:36.
Worku AG, Yalew AW, Afework MF. Maternal complications and women's behavior in seeking care from skilled providers in North Gondar, Ethiopia. PLoS One. 2013;8(3):e60171.
Ikeako LC, Onah HE, Iloabachie GC. Influence of formal maternal education on the use of maternity services in Enugu, Nigeria. J Obstet Gynaecol. 2006;26(1):30–4.
Kabakyenga JK, Ostergren PO, Turyakira E, Pettersson KO. Influence of birth preparedness, decision-making on location of birth and assistance by skilled birth attendants among women in south-western Uganda. PLoS One. 2012;7(4):e35747.
Onah HE, Ikeako LC, Iloabachie GC. Factors associated with the use of maternity services in Enugu, southeastern Nigeria. Soc Sci Med. 2006;63(7):1870–8.
Dutamo Z, Assefa N, Egata G. Maternal health care use among married women in Hossaina, Ethiopia. BMC Health Serv Res. 2015;15(1):1.
Mazalale J, Kambala C, Brenner S, Chinkhumba J, Lohmann J, Mathanga DP, Robberstad B, Muula AS, De Allegri M. Factors associated with delivery outside a health facility: cross‐sectional study in rural Malawi. Trop Med Int Health. 2015;20(5):617–26.
Semali IA, Leyna GH, Mmbaga EJ, Tengia-Kessy A. Social capital as a determinant of pregnant mother’s place of delivery: experience from Kongwa District in Central Tanzania. PLoS One. 2015;10(10):e0138887.
Feinstein L, Dimomfu BL, Mupenda B, Duvall S, Chalachala JL, Edmonds A, Behets F. Antenatal and delivery services in Kinshasa, Democratic Republic of Congo: care-seeking and experiences reported by women in a household-based survey. Trop Med Int Health. 2013;18(10):1211–21.
Anastasi E, Borchert M, Campbell OM, Sondorp E, Kaducu F, Hill O, Okeng D, Odong VN, Lange IL. Losing women along the path to safe motherhood: why is there such a gap between women’s use of antenatal care and skilled birth attendance? A mixed methods study in northern Uganda. BMC Pregnancy Childbirth. 2015;15:287.
Atuoye KN, Dixon J, Rishworth A, Galaa SZ, Boamah SA, Luginaah I. Can she make it? Transportation barriers to accessing maternal and child health care services in rural Ghana. BMC Health Serv Res. 2015;15:333.
Bayou NB, Gacho YHM. Utilization of clean and safe delivery service package of health services extension program and associated factors in rural kebeles of Kafa Zone, Southwest Ethiopia. Ethiopian J Health Sci. 2013;23(2):79–89.
Echoka E, Makokha A, Dubourg D, Kombe Y, Nyandieka L, Byskov J. Barriers to emergency obstetric care services: accounts of survivors of life threatening obstetric complications in Malindi District, Kenya. Pan Afr Med J. 2014;17 Suppl 1:4.
Kyomuhendo GB. Low use of rural maternity services in Uganda: impact of women’s status, traditional beliefs and limited resources. Reprod Health Matters. 2003;11(21):16–26.
Okafor I, Sekoni A, Ezeiru S, Ugboaja J, Inem V. Orthodox versus unorthodox care: a qualitative study on where rural women seek healthcare during pregnancy and childbirth in Southwest, Nigeria. Malawi Med J. 2014;26(2):45–9.
Odberg Pettersson K, Christensson K, da Gloria Gomes de Freitas E, Johansson E. Adaptation of health care seeking behavior during childbirth: focus group discussions with women living in the suburban areas of Luanda, Angola. Health Care Women Int. 2004;25(3):255–80.
Roro MA, Hassen EM, Lemma AM, Gebreyesus SH, Afework MF. Why do women not deliver in health facilities: a qualitative study of the community perspectives in south central Ethiopia? BMC Res Notes. 2014;7(1):1.
Storeng KT, Baggaley RF, Ganaba R, Ouattara F, Akoum MS, Filippi V. Paying the price: the cost and consequences of emergency obstetric care in Burkina Faso. Soc Sci Med. 2008;66(3):545–57.
Tsegay Y, Gebrehiwot T, Goicolea I, Edin K, Lemma H, Sebastian MS. Determinants of antenatal and delivery care utilization in Tigray region, Ethiopia: a cross-sectional study. Int J Equity Health. 2013;12:30.
King R, Jackson R, Dietsch E, Hailemariam A. Barriers and facilitators to accessing skilled birth attendants in Afar region, Ethiopia. Midwifery. 2015;31(5):540–6.
Lule GS, Tugumisirize J, Ndekha M. Quality of care and its effects on utilisation of maternity services at health centre level. East Afr Med J. 2000;77(5):250–5.
White D, Dynes M, Rubardt M, Sissoko K, Stephenson R. The influence of intrafamilial power on maternal health care in mali: perspectives of women, men and mothers-in-law. Int Perspect Sex Reprod Health. 2013;39(2):58–68.
Bayu H, Fisseha G, Mulat A, Yitayih G, Wolday M. Missed opportunities for institutional delivery and associated factors among urban resident pregnant women in South Tigray Zone, Ethiopia: a community-based follow-up study. Glob Health Action. 2015;8:28082.
Habte F, Demissie M. Magnitude and factors associated with institutional delivery service utilization among childbearing mothers in Cheha district, Gurage zone, SNNPR, Ethiopia: a community based cross sectional study. BMC Pregnancy Childbirth. 2015;15:299.
O’Donnell E, Utz B, Khonje D, Van Den Broek N. ‘At the right time, in the right way, with the right resources’: perceptions of the quality of care provided during childbirth in Malawi. BMC Pregnancy Childbirth. 2014;14(1):1.
Speizer IS, Story WT, Singh K. Factors associated with institutional delivery in Ghana: the role of decision-making autonomy and community norms. BMC Pregnancy Childbirth. 2014;14(1):1.
Ejembi C, Alti-Muazu M, Chirdan O, Ezeh H, Sheidu S, Dahiru T. Utilization of maternal health services by rural Hausa women in Zaria environs, northern Nigeria: has primary health care made a difference? J Community Med Primary Health Care. 2004;16(2):47–54.
Lori JR, Boyle JS. Cultural childbirth practices, beliefs, and traditions in postconflict Liberia. Health Care Women Int. 2011;32(6):454–73.
Kaye DK, Kakaire O, Nakimuli A, Osinde MO, Mbalinda SN, Kakande N. Lived experiences of women who developed uterine rupture following severe obstructed labor in Mulago hospital, Uganda. Reproductive Health. 2014;11:31.
Roka ZG, Akech M, Wanzala P, Omolo J, Gitta S, Waiswa P. Factors associated with obstetric fistulae occurrence among patients attending selected hospitals in Kenya, 2010: a case control study. BMC Pregnancy Childbirth. 2013;13(1):1.
Chapman RR. Endangering safe motherhood in Mozambique: prenatal care as pregnancy risk. Soc Sci Med. 2003;57(2):355–74.
De Allegri M, Ridde V, Louis VR, Sarker M, Tiendrebeogo J, Ye M, Muller O, Jahn A. Determinants of utilisation of maternal care services after the reduction of user fees: a case study from rural Burkina Faso. Health Policy (Amsterdam, Netherlands). 2011;99(3):210–8.
Sakeah E, Doctor HV, McCloskey L, Bernstein J, Yeboah-Antwi K, Mills S. Using the community-based health planning and services program to promote skilled delivery in rural Ghana: socio-demographic factors that influence women utilization of skilled attendants at birth in northern Ghana. BMC Public Health. 2014;14:344.
Ganle JK, Dery I. ‘What men don’t know can hurt women’s health’: a qualitative study of the barriers to and opportunities for men’s involvement in maternal healthcare in Ghana. Reproductive Health. 2015;12:93.
Osubor K, Fatusi AO, Chiwuzie J. Maternal health-seeking behavior and associated factors in a rural Nigerian community. Matern Child Health J. 2006;10(2):159–69.
Kawakatsu Y, Sugishita T, Oruenjo K, Wakhule S, Kibosia K, Were E, Honda S. Determinants of health facility utilization for childbirth in rural western Kenya: cross-sectional study. BMC Pregnancy Childbirth. 2014;14(1):1.
Keri L, Kaye D, Sibylle K. Referral practices and perceived barriers to timely obstetric care among Ugandan traditional birth attendants (TBA). Afr Health Sci. 2010;10(1):75–81.
Bayu H, Adefris M, Amano A, Abuhay M. Pregnant women’s preference and factors associated with institutional delivery service utilization in Debra Markos Town, North West Ethiopia: a community based follow up study. BMC Pregnancy Childbirth. 2015;15(1):1.
Kumbani L, Bjune G, Chirwa E, Malata A, Odland JO. Why some women fail to give birth at health facilities: a qualitative study of women’s perceptions of perinatal care from rural Southern Malawi. Reproductive Health. 2013;10:9.
Worku AG, Yalew AW, Afework MF. Factors affecting utilization of skilled maternal care in Northwest Ethiopia: a multilevel analysis. BMC International Health and Human Rights. 2013;13:20.
Link BG, Phelan JC. Conceptualizing stigma. Annu Rev Sociol. 2001:27(3);363–85.
Medema-Wijnveen JS, Onono M, Bukusi EA, Miller S, Cohen CR, Turan JM. How perceptions of HIV-related stigma affect decision-making regarding childbirth in rural Kenya. PLoS One. 2012;7(12):e51492.
Peltzer K, Skinner D, Mfecane S, Shisana O, Nqeketo A, Mosala T. Factors influencing the utilisation of prevention of mother-to-child-transmission (PMTCT) services by pregnant women in the Eastern Cape, South Africa. Health SA Gesondheid. 2005;10(1):26–40.
Vallieres F, Hansen A, McAuliffe E, Cassidy EL, Owora P, Kappler S, Gathuru E. Head of household education level as a factor influencing whether delivery takes place in the presence of a skilled birth attendant in Busia, Uganda: a cross-sectional household study. BMC Pregnancy Childbirth. 2013;13:48.
van den Broek NR, White SA, Ntonya C, Ngwale M, Cullinan TR, Molyneux ME, Neilson JP. Reproductive health in rural Malawi: a population-based survey. BJOG. 2003;110(10):902–8.
Joharifard S, Rulisa S, Niyonkuru F, Weinhold A, Sayinzoga F, Wilkinson J, Ostermann J, Thielman NM. Prevalence and predictors of giving birth in health facilities in Bugesera District, Rwanda. BMC Public Health. 2012;12:1049.
Asres A, Davey G. Factors associated with safe delivery service utilization among women in Sheka Zone, Southwest Ethiopia. Matern Child Health J. 2015;19(4):859–67.
Alemayehu M, Mekonnen W. The prevalence of skilled birth attendant utilization and its correlates in North West Ethiopia. Biomed Res Int. 2015;2015:436938.
Idris S, Gwarzo U, Shehu A. Determinants of place of delivery among women in a semi-urban settlement in Zaria, northern Nigeria. Ann Afr Med. 2006;5(2):68–72.
Oguntunde O, Aina O, Ibrahim MS, Umar HS, Passano P. Antenatal care and skilled birth attendance in three communities in Kaduna State, Nigeria. Afr J Reprod Health. 2010;14(3):89–96.
O’Meara WP, Platt A, Naanyu V, Cole D, Ndege S. Spatial autocorrelation in uptake of antenatal care and relationship to individual, household and village-level factors: results from a community-based survey of pregnant women in six districts in western Kenya. Int J Health Geogr. 2013;12(1):1.
Rockers PC, Wilson ML, Mbaruku G, Kruk ME. Source of antenatal care influences facility delivery in rural Tanzania: a population-based study. Matern Child Health J. 2009;13(6):879–85.
Kruk ME, Rockers PC, Mbaruku G, Paczkowski MM, Galea S. Community and health system factors associated with facility delivery in rural Tanzania: a multilevel analysis. Health Policy (Amsterdam, Netherlands). 2010;97(2-3):209–16.
Abel Ntambue ML, Francoise Malonga K, Dramaix-Wilmet M, Donnen P. Determinants of maternal health services utilization in urban settings of the Democratic Republic of Congo—a case study of Lubumbashi City. BMC Pregnancy Childbirth. 2012;12:66.
Ono M, Matsuyama A, Karama M, Honda S. Association between social support and place of delivery: a cross-sectional study in Kericho, Western Kenya. BMC Pregnancy Childbirth. 2013;13(1):1.
Wilunda C, Oyerinde K, Putoto G, Lochoro P, Dall’Oglio G, Manenti F, Segafredo G, Atzori A, Criel B, Panza A. Availability, utilisation and quality of maternal and neonatal health care services in Karamoja region, Uganda: a health facility-based survey. Reprod Health. 2015;12(1):30.
Hagos S, Shaweno D, Assegid M, Mekonnen A, Afework MF, Ahmed S. Utilization of institutional delivery service at Wukro and Butajera districts in the Northern and South Central Ethiopia. BMC Pregnancy Childbirth. 2014;14(1):178.
Nyango DD, Mutihir JT, Laabes EP, Kigbu JH, Buba M. Skilled attendance: the key challenges to progress in achieving MDG-5 in north central Nigeria. Afr J Reprod Health. 2010;14(2):129–38.
Dahlberg M, Södergård B, Thorson A, Alfvén T, Awiti-Ujiji O. Being perceived as ‘a real woman’ or following one’s own convictions: a qualitative study to understand individual, family, and community influences on the place of childbirth in Busia, Kenya. Cult Health Sex. 2015;17(3):326–42.
Ganle JK, Parker M, Fitzpatrick R, Otupiri E. A qualitative study of health system barriers to accessibility and utilization of maternal and newborn healthcare services in Ghana after user-fee abolition. BMC Pregnancy Childbirth. 2014;14:425.
Mahiti GR, Mkoka DA, Kiwara AD, Mbekenga CK, Hurtig A-K, Goicolea I. Women's perceptions of antenatal, delivery, and postpartum services in rural Tanzania. Glob Health Action. 2015;8. doi: 10.3402/gha.v8.28567.
Phiri SN, Kiserud T, Kvåle G, Byskov J, Evjen-Olsen B, Michelo C, Echoka E, Fylkesnes K. Factors associated with health facility childbirth in districts of Kenya, Tanzania and Zambia: a population based survey. BMC Pregnancy Childbirth. 2014;14(1):1.
Essendi H, Johnson FA, Madise N, Matthews Z, Falkingham J, Bahaj AS, James P, Blunden L. Infrastructural challenges to better health in maternity facilities in rural Kenya: community and healthworker perceptions. Reprod Health. 2015;12:103.
Conrad P, De Allegri M, Moses A, Larsson EC, Neuhann F, Müller O, Sarker M. Antenatal care services in rural Uganda missed opportunities for good-quality care. Qual Health Res. 2012;22(5):619–29.
Afari H, Hirschhorn LR, Michaelis A, Barker P, Sodzi-Tettey S. Quality improvement in emergency obstetric referrals: qualitative study of provider perspectives in Assin North district, Ghana. BMJ Open. 2014;4(5):e005052.
Kaye D. Quality of midwifery care in Soroti district, Uganda. East Afr Med J. 2000;77(10):558-61.
Bayley O, Colbourn T, Nambiar B, Costello A, Kachale F, Meguid T, Mwansambo C. Knowledge and perceptions of quality of obstetric and newborn care of local health providers: a cross-sectional study in three districts in Malawi. Malawi Med J. 2013;25(4):105–8.
Schack SM, Elyas A, Brew G, Pettersson KO. Experiencing challenges when implementing active management of third stage of labor (AMTSL): a qualitative study with midwives in Accra, Ghana. BMC Pregnancy Childbirth. 2014;14(1):1.
Oguntunde O, Charyeva Z, Cannon M, Sambisa W, Orobaton N, Kabo IA, Shoretire K, Danladi SE, Lawal N, Sadauki H. Factors influencing the use of magnesium sulphate in pre-eclampsia/eclampsia management in health facilities in Northern Nigeria: a mixed methods study. BMC Pregnancy Childbirth. 2015;15:130.
Doctor HV, Findley SE, Cometto G, Afenyadu GY. Awareness of critical danger signs of pregnancy and delivery, preparations for delivery, and utilization of skilled birth attendants in Nigeria. J Health Care Poor Underserved. 2013;24(1):152–70.
Chi PC, Bulage P, Urdal H, Sundby J. Barriers in the delivery of emergency obstetric and neonatal care in post-conflict Africa: qualitative case studies of Burundi and Northern Uganda. PLoS One. 2015;10(9):e0139120.
Mkoka DA, Goicolea I, Kiwara A, Mwangu M, Hurtig A-K. Availability of drugs and medical supplies for emergency obstetric care: experience of health facility managers in a rural District of Tanzania. BMC Pregnancy Childbirth. 2014;14(1):1.
Mselle LT, Moland KM, Mvungi A, Evjen-Olsen B, Kohi TW. Why give birth in health facility? Users’ and providers’ accounts of poor quality of birth care in Tanzania. BMC Health Serv Res. 2013;13(1):1.
Ridge AL, Bero LA, Hill SR. Identifying barriers to the availability and use of Magnesium Sulphate Injection in resource poor countries: a case study in Zambia. BMC Health Serv Res. 2010;10:340.
Kujawski S, Mbaruku G, Freedman LP, Ramsey K, Moyo W, Kruk ME. Association between disrespect and abuse during childbirth and women’s confidence in health facilities in Tanzania. Matern Child Health J. 2015;19(10):2243–50.
Moyer CA, Adongo PB, Aborigo RA, Hodgson A, Engmann CM. ‘They treat you like you are not a human being’: maltreatment during labour and delivery in rural northern Ghana. Midwifery. 2013;30(2):262–8.
Grossmann-Kendall F, Filippi V, De Koninck M, Kanhonou L. Giving birth in maternity hospitals in Benin: testimonies of women. Reprod Health Matters. 2001;9(18):90–8.
Harfouche M, Hosseinipour M, Kaliti S, Wilkinson J. Quality indicators and outcomes of emergency caesarean deliveries at a district-level maternity hospital. Afr J Reprod Health. 2015;19(3):61–7.
Kaye D. Quality of midwifery care in Soroti district, Uganda. East Afr Med J. 2000;77(10):558–61.
Ijadunola KT, Ijadunola MY, Esimai OA, Abiona TC. New paradigm old thinking: the case for emergency obstetric care in the prevention of maternal mortality in Nigeria. BMC Womens Health. 2010;10:6.
Tita AT, Selwyn BJ, Waller DK, Kapadia AS, Dongmo S. Evidence-based reproductive health care in Cameroon: population-based study of awareness, use and barriers. Bull World Health Organ. 2005;83(12):895–903.
Mirkuzie AH, Sisay MM, Reta AT, Bedane MM. Current evidence on basic emergency obstetric and newborn care services in Addis Ababa, Ethiopia; a cross sectional study. BMC Pregnancy Childbirth. 2014;14:354.
Morestin F, Ridde V. The abolition of user fees for health services in Africa Lessons from the literature. Montreal: University of Montreal; 2009.
Houweling TA, Ronsmans C, Campbell OM, Kunst AE. Huge poor-rich inequalities in maternity care: an international comparative study of maternity and child care in developing countries. Bull World Health Organ. 2007;85(10):745–54.
Essendi H, Mills S, Fotso J-C. Barriers to formal emergency obstetric care services’ utilization. J Urban Health. 2011;88(2):356–69.
Jehan K, Sidney K, Smith H, De Costa A. Improving access to maternity services: an overview of cash transfer and voucher schemes in South Asia. Reprod Health Matters. 2012;20(39):142–54.
Knight HE, Self A, Kennedy SH. Why are women dying when they reach hospital on time? A systematic review of the ‘third delay’. PLoS One. 2013;8(5):e63846.
Pacagnella RC, Cecatti JG, Parpinelli MA, Sousa MH, Haddad SM, Costa ML, Souza JP, Pattinson RC. Delays in receiving obstetric care and poor maternal outcomes: results from a national multicentre cross-sectional study. BMC Pregnancy Childbirth. 2014;14(1):1.
Maine D. Prevention of maternal deaths in developing countries: program options and practical considerations. In: international safe motherhood conference, Nairobi. 1987.
UNFPA. Program manager’s planning monitoring and evaluation toolkit, part II: indicators for reducing maternal mortality. 2004. http://dmeforpeace.org/sites/default/files/UNFPA_Programme%20Manager%27s%20Planning%20Monitoring%20%26%20Evaluation%20Toolkit.pdf. Accessed 28 May 2017.
Gething PW, Johnson FA, Frempong-Ainguah F, Nyarko P, Baschieri A, Aboagye P, Falkingham J, Matthews Z, Atkinson PM. Geographical access to care at birth in Ghana: a barrier to safe motherhood. BMC Public Health. 2012;12(1):1.
Munoz UH, Källestål C. Geographical accessibility and spatial coverage modeling of the primary health care network in the Western Province of Rwanda. Int J Health Geogr. 2012;11(1):1.
Gabrysch S, Cousens S, Cox J, Campbell OM. The influence of distance and level of care on delivery place in rural Zambia: a study of linked national data in a geographic information system. PLoS Med. 2011;8(1):e1000394.
Thaddeus S, Maine D. Too far to walk: maternal mortality in context. Soc Sci Med. 1994;38(8):1091–110.
Jammeh A, Sundby J, Vangen S. Barriers to emergency obstetric care services in perinatal deaths in rural gambia: a qualitative in-depth interview study. ISRN Obstetrics Gynecology. 2011. doi: 10.5402/2011/981096.
Peters DH, Garg A, Bloom G, Walker DG, Brieger WR, Hafizur Rahman M. Poverty and access to health care in developing countries. Ann N Y Acad Sci. 2008;1136(1):161–71.
United Nations Human Rights, office of the hugh commissioner, Committee on the Elimination of Discrimination Against Women [http://www.ohchr.org/en/hrbodies/cedaw/pages/cedawindex.aspx]
Mullany BC, Hindin MJ, Becker S. Can women’s autonomy impede male involvement in pregnancy health in Katmandu, Nepal? Soc Sci Med. 2005;61(9):1993–2006.
d'Ambruoso L, Abbey M, Hussein J. Please understand when I cry out in pain: women’s accounts of maternity services during labour and delivery in Ghana. BMC Public Health. 2005;5(1):1.
Acknowledgements
Not applicable.
Funding
MKN is supported by a doctoral scholarship—the Victoria University International Postgraduate Research Scholarship.
Availability of data and materials
Most data generated or analysed during this study are included in this published article and its supplementary information files. Additional information is available from the corresponding author on reasonable request.
Authors’ contributions
MKN, MCO and TVM conceived and designed the study. MKN conducted the literature search, extracted all the data and drafted the manuscript. All authors (MKN, MCO and TVM) contributed to the analysis and interpretation of the data as well as the critical revision of the study. All authors read and approved the final manuscript.
Authors’ information
None provided.
Competing interests
The authors declare that they have no competing interests.
Consent for publication
Not applicable.
Ethics approval and consent to participate
Not applicable.
Publisher’s Note
Springer Nature remains neutral with regard to jurisdictional claims in published maps and institutional affiliations.
Author information
Authors and Affiliations
Corresponding author
Additional files
Additional file 1:
PubMed search strategy. Sample search strategy (for PubMed database). (DOC 51 kb)
Additional file 2:
Quality assessment using the mixed methods appraisal tool (MMAT). Quality assessment of included studies. (DOC 160 kb)
Additional file 3: Table S1.
Characteristics of included studies. Description of eligible/retained studies. (DOC 378 kb)
Additional file 4:
PRISMA 2009 Checklist. PRISMA checklist for reporting of systematic review. (DOC 65 kb)
Additional file 5:
PRISMS 2009 Flow Diagram. Flow chart of data extraction process. (DOC 64 kb)
Rights and permissions
Open Access This article is distributed under the terms of the Creative Commons Attribution 4.0 International License (http://creativecommons.org/licenses/by/4.0/), which permits unrestricted use, distribution, and reproduction in any medium, provided you give appropriate credit to the original author(s) and the source, provide a link to the Creative Commons license, and indicate if changes were made. The Creative Commons Public Domain Dedication waiver (http://creativecommons.org/publicdomain/zero/1.0/) applies to the data made available in this article, unless otherwise stated.
About this article
Cite this article
Kyei-Nimakoh, M., Carolan-Olah, M. & McCann, T.V. Access barriers to obstetric care at health facilities in sub-Saharan Africa—a systematic review. Syst Rev 6, 110 (2017). https://doi.org/10.1186/s13643-017-0503-x
Received:
Accepted:
Published:
DOI: https://doi.org/10.1186/s13643-017-0503-x