Abstract
Background
Frailty status among critically ill patients with acute kidney injury (AKI) is not well described despite its importance for prognostication and informed decision-making on life-sustaining therapies. In this study, we aim to describe the epidemiology of frailty in a cohort of older critically ill patients with severe AKI, the outcomes of patients with pre-existing frailty before AKI and the factors associated with a worsening frailty status among survivors.
Methods
This was a secondary analysis of a prospective multicentre observational study that enrolled older (age > 65 years) critically ill patients with AKI. The clinical frailty scale (CFS) score was captured at baseline, at 6 months and at 12 months among survivors. Frailty was defined as a CFS score of ≥ 5. Demographic, clinical and physiological variables associated with frailty as baseline were described. Multivariable Cox proportional hazard models were constructed to describe the association between frailty and 90-day mortality. Demographic and clinical factors associated with worsening frailty status at 6 months and 12 months were described using multivariable logistic regression analysis and multistate models.
Results
Among the 462 patients in our cohort, median (IQR) baseline CFS score was 4 (3–5), with 141 (31%) patients considered frail. Pre-existing frailty was associated with greater hazard of 90-day mortality (59% (n = 83) for frail vs. 31% (n = 100) for non-frail; adjusted hazards ratio [HR] 1.49; 95% CI 1.11–2.01, p = 0.008). At 6 months, 68 patients (28% of survivors) were frail. Of these, 57% (n = 39) were not classified as frail at baseline. Between 6 and 12 months of follow-up, 9 (4% of survivors) patients transitioned from a frail to a not frail status while 10 (4% of survivors) patients became frail and 11 (5% of survivors) patients died. In multivariable analysis, age was independently associated with worsening CFS score from baseline to 6 months (adjusted odds ratio [OR] 1.08; 95% CI 1.03–1.13, p = 0.003).
Conclusions
Pre-existing frailty is an independent risk factor for mortality among older critically ill patients with severe AKI. A substantial proportion of survivors experience declining function and worsened frailty status within one year.
Similar content being viewed by others
Background
Severe acute kidney injury (AKI) occurs in a significant proportion of critically ill patients. Its presence is a marker of the severity of critical illness, and therefore, severe AKI is often associated with organ dysfunction and with adverse outcomes [1]. Despite important advances in understanding the epidemiology of this condition, the long-term outcomes among survivors of severe AKI are more limited. There is a dearth of information on patient-centred concerns such as functional status, quality of life and socioeconomic status in this population.
A deterioration in health-related quality of life is known to occur in a significant proportion of patients after critical illness, whether they develop AKI or not [2, 3]. However, the presence of severe AKI might herald a higher risk of physical limitations and disability [2]. Frailty is a state of vulnerability characterized by a diminished resilience to external stressors [4] and has been shown to portend greater risk of adverse outcomes in critical illness [5,6,7]. Notably, a frail state before critical illness is associated with worse functional status and health-related quality of life among survivors during follow-up [8].
Recent data have suggested AKI may be associated with greater declines in functional status and frailty among survivors of critical illness at 12 months compared to those without AKI [9]. However, there has been no description of how frailty status may evolve among survivors whose course was complicated by severe AKI and whether there are identifiable factors associated with clinical deterioration. Accordingly, the primary aim of this study was to describe frailty status in a prospective cohort of older critically ill patients with severe AKI at 6 months and 12 months. As secondary objectives, we further aimed to describe the association of baseline frailty status and 90-day mortality and identify factors associated with deterioration in frailty status at follow-up.
Methods
Design, setting, and participants
We conducted a secondary analysis of the Optimal Selection for and Timing to Start Renal Replacement in Critically Ill Older Patients with Acute Kidney Injury (OPTIMAL-AKI), a multicentre prospective cohort study performed at 16 hospitals across Canada between September 23, 2013 and November 18, 2015 [10]. Approval for the study was received by the Research Ethics Board at the University of Alberta (File Pro00037850) and each participating centre. All participants or their legally authorized surrogate provided informed consent. This study follows the recommended reporting outlined in the strengthening the reporting of observational studies in epidemiology (STROBE) Statement [11].
OPTIMAL-AKI included patients ≥ 65 years old admitted to the intensive care unit (ICU) with severe AKI, defined as either: (1) a threefold increase in serum creatinine from a known premorbid baseline or during the current hospitalization, (2) a serum creatinine > 4.0 mg/dl (> 354 μmol/L) with evidence of a minimum increase of 0.3 mg/dl (27 μmol/L), (3) urine output < 7.2 ml/kg during the past 24 h, (4) complete anuria for the preceding 12 h or (5) twofold increase in serum creatinine from a known premorbid baseline or during the current hospitalization and total urine output < 6.0 ml/kg over the preceding 12 h (or < 2 ml/kg over 4 h). Patients who received renal replacement therapy (RRT) in the preceding 4 weeks or with drug intoxication representing an indication of urgent RRT initiation were excluded. For the purpose of this analysis, patients without frailty status data recorded at baseline were excluded.
Data collection
Trained research coordinators performed standardized data collection using a defined protocol, as originally described [10]. Pre-hospital frailty status was assessed using the 9-point clinical frailty scale (CFS) score [4]. However, it was pre-specified that patients could not be assigned a score of 9 (terminally ill). Trained coordinators captured the CFS using multiple data sources including the medical record and a baseline interview with the patient and/or family members. This assessment was previously demonstrated to be reliable in the ICU setting [12]. Patients and/or family members were contacted at 6-months and 12-months to ascertain vital status, disposition, and frailty status.
Definitions and outcomes
Our primary objective was to describe the trajectory of frailty from baseline through 12 months of follow-up. We defined frailty as a CFS score of ≥ 5 [4, 13]. Our secondary objective was to evaluate the association between baseline frailty status and 90-day all-cause mortality [10]. We also evaluated the incidence of new onset of frailty and deterioration of frailty status during follow-up at 6 months and 12 months [4, 13]. New onset frailty was defined as the transition from a baseline CFS score < 5 to a CFS score ≥ 5. Deterioration of frailty status was defined as a transition from a lower category of frailty status at baseline to a higher category. Frailty was categorically graded by stratifying CFS scores of 1–3 as fit; scores of 4 as vulnerable; scores of 5 as mildly frail; and 6–8 as moderate to severely frail. These categories have been used previously in the Canadian elderly population [4, 7].
Statistical analysis
We examined characteristics of subjects stratified by CFS (both binary and categorical classifications) at baseline. For continuous variables the association was tested using a t-test (or an Analysis of Variance F-test for categorical classification of CFS) and for categorical variables the association was tested using either Pearson’s Chi-square test or Fisher’s Exact test, as appropriate. Kaplan–Meier survival curves were created to display the natural history of all-cause mortality by CFS for up to 12 months of follow-up. Log-rank tests were used to test the difference in survival probability based on frailty status. The normality assumption for continuous variables was assessed through visual inspection of Normal Q-Q plots. In the presence of serious non-normality, the nonparametric Kruskal–Wallis rank sum test was used. The homogeneity of variance assumption was assessed through the Levene’s test for equality of variances.
To determine the association between frailty and 90-day mortality, we employed Cox proportional hazards regression for both unadjusted and adjusted analyses. In the Cox proportional hazards models, we evaluated the association between CFS and mortality, censored at date of last follow-up or at the end point of the time of interest. The covariates in the adjusted models included age, sex, Charlson Comorbidity Index (CCI) score, baseline eGFR, peak serum creatinine during current ICU admission and SOFA score and APACHE II score. These were a priori selected patient-level factors, physician-specific and site-specific factors or those deemed clinically important. The proportional hazards assumption was tested using visual inspection and statistical testing of the models Schoenfeld residuals. Model estimates and results from complete cases from the original dataset and using multiple imputed datasets were compared.
For variables used in multivariable models other than frailty and mortality, multiple imputations were used to impute the missing data. Different techniques were used according to variable type [14]. Predictive mean matching was used to impute continuous variables [15], logistic regression imputation was used for binary variables and polytomous regression imputation for unordered categorical data [14]. The set of variables that were used in the multiple imputation processes were the covariates in the adjusted models in the confirmatory analyses and other clinically important variables. The dataset used in the confirmatory analyses has roughly 10% missing data; thus, the imputation process was repeated 10 times which in turn produced 10 imputed datasets at random. The model estimates from the 10 datasets were then pooled to get final bias-adjusted estimates.
Multivariable prediction models were created using logistic regression with the same covariates. The performance of the model was assessed by evaluating the discrimination by the area under the receiver-operator curve (AUC) while calibration was assessed graphically. The Net Reclassification Improvement (NRI) index produced by the addition of the frailty information to a model containing the other baseline variables was computed.
To determine the predictors of a worsening CFS score from baseline to 6 months and subsequently to 12 months in survivors, we first performed univariable logistic regression to determine the association with clinically important variables including age, CCI score, APACHE II score, pre-hospital disposition, baseline CFS score, receipt of RRT, hospital and ICU length of stay. Patients who were already classified as moderately or severely frail at baseline, and thus could not get worse, were excluded from this analysis.
Additionally, we performed a multistate Markov model to determine the association between clinical variables and the transition between one of the following states to another: alive and not frail; alive and frail; and dead [16, 17].
All results are presented with a 95% confidence interval (CI) and a two-sided p-value of < 0.05 was considered significant. All statistical analyses were conducted in R (R Development team, 2010).
Results
Among the 499 patients enrolled in the OPTIMAL-AKI study, 462 (93%) had baseline CFS available (median score 4 [IQR 3–5]) and 141 (31%) patients were considered frail. Frailty data were available for 243 patients at 6 months (87% of surviving patients) and 216 patients at 12 months (81% of surviving patients) (Additional file 1: Figure S1). The complete distribution of CFS scores in the cohort is presented in Additional file 1: Table S1. During the 12-month follow-up period, 195 (42%) patients died and 51 (11%) were lost to follow-up. The evolution of frailty status from baseline to 12 months after enrolment is presented in Fig. 1.
Pre-existing frailty status
Patient characteristics stratified by baseline frailty status are presented in Table 1. Patients with frailty were older, more likely to be female and had more comorbid disease. Patients with frailty were also more likely to have baseline cognitive impairment, to require assistance at home or reside in an assisted living facility and to have been hospitalized in the preceding 6 months. Clinicians were less willing to offer RRT to patients with frailty compared to those not frail (63.1% vs 76.0%, OR 0.83; 95% CI 0.72–0.96, p = 0.0067, and frail patients were subsequently less likely to receive RRT (37.6% vs 51.4%, OR 0.73; 95% CI 0.58–0.93, p = 0.0064). Patient characteristics stratified by category of frailty score are presented in Additional file 1: Table S2.
Mortality at 90 days
At 90 days, 183 (40%) patients had died. Patients with frailty had greater risk of 90-day mortality compared to those not frail (59% [n = 83] vs. 31% [n = 100], HR 1.62; CI 1.24–2.13, p < 0.001; Fig. 2), and this difference was observed up to 12 months of follow-up (Additional file 1: Figure S2). After covariate adjustment, frailty was independently associated with 90-day mortality (adjusted HR 1.49; 95% CI 1.11–2.01, p = 0.008; Table 2). Complete case analysis yielded similar results (Table S3). However, the addition of frailty status to the model (AUC 0.672; CI 0.622–0.722) did not result in a substantial net reclassification improvement (NRI 0.068; 95% CI − 0.026; 0.162).
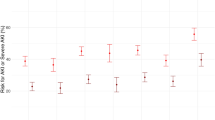
Kaplan–Meier survival curves stratified by baseline frailty status in the OPTIMAL-AKI cohort study. a Stratified by binary classification of frail (clinical frailty scale (CFS): 5–8) or not frail (CFS: 1–4). b Stratified by categorical classification of frailty status defined as fit (CFS: 1–3), vulnerable (CFS: 4), mild frailty (CFS: 5–6) and moderate-to-severe frailty (CFS: 7–8)
CFS score stratification showed that moderate-to-severe frailty was independently associated with 90-day mortality (adjusted OR 1.91; CI 1.08–3.40, p = 0.027) (Additional file 1: Table S4). The addition of the frailty status in this model also did not significantly improve risk prediction (NRI 0.076; CI − 0.016; 0.171]).
Frailty status at 6 months and 12 months
At 6 months of follow-up, 243 (53%) patients were alive and had CFS scores captured. Among these, 68 (28%) were frail including 39 (57%) patients who were not classified as frail at baseline (Fig. 1). When stratified by frailty severity category, 66 (27%) patients had a worse CFS score at 6 months, while 29 (12%) has an improved CFS score (Additional file 1: Table S5).
At 12 months of follow-up, 216 (47%) patients were alive and had CFS scores captured. Among these, 58 (27%) were considered frail. Between 6 and 12 months, 10 patients (6.0% of patients considered not frail at 6 months) became newly frail while 9 patients (13.2% of patients considered frail at 6 months) transitioned to not frail from previously being classified as frail. When stratified by frailty category, 27 (13%) patients declined to a worse state, while 23 (11%) patients improved (Additional file 1: Table S6).
Among patient characteristics at baseline, age was associated with a deterioration in CFS score at 6 months of follow-up after adjustment (OR 1.08; 95% CI 1.03–1.13, p = 0.003). Also, patients with a low CFS score at baseline had a greater likelihood of experiencing a deterioration of frailty status (OR 0.70; 95% CI 0.52–0.94, p = 0.019) (Table 3). No other variables were significantly associated with deterioration in frailty status after adjustments, including the receipt of RRT. The resulting model had acceptable discrimination power (AUC 0.70; 95% CI 0.62–0.78) and calibration. Exploratory analysis showed no association between baseline or peak serum creatinine (OR, 0.97; 95% CI 0.81; 1.17; p = 0.765 and OR, 1.02; 95% CI 0.97; 1.07; p = 0.478, respectively). No associations were found between the candidate variables and a deterioration of frailty status from baseline to 12 months (Additional file 1: Table S7).
Multistate analysis
A multistate model analysis was performed to determine the influence of individual risk factors on the probability of transitioning between two of the three following states between baseline and 6 months: 1) alive-and-not-frail, 2) alive-and-frail and 3) dead (Additional file 1: Table S8). No factors were associated with transition from alive-and-not frail to alive-and-frail or vice versa. Greater illness acuity was associated with a lower probability of transitioning from alive-and-frail to dead (HR 0.89 CI 0.79–0.997). No factors were associated with transition between states from baseline to 12 months (Additional file 1: Table S9).
Discussion
We describe the clinical correlates, outcomes and the evolution of frailty status in a large prospective cohort of critically ill older adults with severe AKI. Our data provide new knowledge on implications of frailty status among critically ill patients with severe AKI, a hallmark critical illness severity. Not only was frailty common, present in about 1/3 of patients at baseline, but we also found that frailty portends a higher risk for short and long-term mortality. We showed that clinicians may be less likely to offer RRT to patients perceived as frail. We also found that among survivors not classified as frail at baseline, a substantial proportion of survivors will develop de novo frailty or a worsened frailty status at 6 months and 12 months, while fewer show improvement. We propose that such a transition in functional status may represent a clinically important outcome for patients and/or their families.
Frailty status before critical illness may convey prognostic information and impact care decisions. Most notably, patients with known frailty before critical illness may be perceived differently by clinicians. In addition to clinical characteristics, decision-making at the time where an escalation in the intensity of care is contemplated is likely to be affected by information about previous daily life at home and functional status. We observed that clinicians were less likely to offer RRT for patients with pre-existing frailty and these frail patients were also less likely to receive RRT. However, it must be noted that while baseline frailty status was independently associated with 90-day mortality, the addition of this information to other clinical variables did not result in a meaningful improvement in the prediction of death.
Frailty after critically illness complicated by AKI may be challenging to predict given a “frail state” may be driven by heterogeneous social, cognitive and physical factors that are not readily apparent or measured at ICU admission. While frailty has increasingly been described in general ICU populations [5, 13, 18,19,20,21,22,23,24], it has seldom been the focus among critically ill patients with severe AKI. A single-centre analysis of 317 critically ill patients enrolled in a prospective cohort study reported that AKI was associated with a worsened frailty status at 3 and 12 months after hospital discharge compared to those without AKI [9]. Of note, the original study did not specifically focus on an older cohort and excluded patients with pre-existing cognitive deficits. The proportion of survivors with frailty at 12-month follow-up was greater (59%) than observed in our study while the mortality was lower (17%). Similar findings were reported in a recent multicentre observational study of unselected critically ill adults which reported a higher rate of transition to a newly frail state (40%) at 12 months of follow-up, albeit with a much lower mortality rate (25%)[24].
Severe AKI may identify patients more susceptible to prolonged ICU stay [25] and for which rehabilitation may be hampered by the use of RRT [26, 27]. However, neither the duration of ICU stay nor the receipt of RRT were associated with worsened frailty at follow-up in our cohort. Similarly, while it may be evident that a higher burden of baseline chronic disease or the higher acuity of illness should increase the risk of frailty [28], we did not observe this association. Our observations suggest that the risk of developing frailty, a complex multi-dimensional syndrome, cannot be simply extrapolated using simple baseline information. Interestingly, we also report that a substantial proportion of patients showed improvement in their CFS score and frailty status between 6 months and 12 months after critical illness, although the clinical characteristics associated with these transitions remain unclear. From a research perspective, these observations would imply that assessment of frailty status should be extended further than 6 months after critical illness to identify opportunities for intervening to improve outcomes and prevent further functional decline in these patients.
This work has several strengths. Its prospective design minimized recall bias in the assessment of frailty and permitted repeated standardized assessments using a validated scale. Furthermore, data were collected at multiple Canadian centres representative of a diverse critical care population thereby improving generalizability. Also, loss to follow-up (11%) was lower than previous studies [9, 24]. Additionally, this study was the first to study frailty in a population comprised exclusively of AKI patients and report data from an important number of patients with severe AKI. Furthermore, data collection was performed in a relatively short period of time (< 2 years) minimizing the potential impact of changing practice patterns. Finally, this study includes information about the willingness to deliver RRT in the setting of severe AKI which reflects the perceptions of bedside clinicians. The latter is likely to be impacted by information about pre-existing level of functioning prior to hospitalization, which is correlated to frailty.
We recognize some key limitations. Missing frailty assessments at follow-up, although not overly frequent, may have resulted in information bias. Furthermore, while the CFS is a validated tool, it is not the only method to assess frailty and CFS was not compared to other tools such as multi-domain assessments [29]. Most importantly, a single CFS assessment does not provide information about the functional trajectory in the months preceding critical illness which may carry important clinical implications [30, 31]. Inter-rater reliability assessment of CFS was not performed during the study but has previously been shown to be good in similar settings [12]. Second, potentially important socio-demographic and clinical variables that are known to impact frailty status were not collected [32]. Furthermore, most variables capturing illness acuity were recorded at study enrolment while factors occurring later during or after the index hospital stay might impacted frailty status. The lack of serial measures of these time-varying characteristics might explain the lack of associations with frailty status at follow-up. Lastly, the absence of an appropriate control group without severe AKI does not enable us to assess whether frailty develops more frequently in among critically ill survivors with severe AKI.
Conclusions
In this large multicentre prospective cohort study of older adults with severe AKI, we describe the evolution of frailty status from baseline to 12 months of follow-up and describe that transition to frail state occurs in a substantial proportion of survivors. Although the precise clinical risk factors for this deterioration remain elusive, this information may orient future investigations aimed at better understanding and improving functional outcomes in critically ill patients with severe AKI.
Availability of data and materials
The datasets used and/or analysed during the current study are available from the corresponding author on reasonable request.
Abbreviations
- AKI:
-
Acute kidney injury
- APACHE II:
-
Acute physiology and chronic health evaluation II
- AUC:
-
Area under the curve
- CCI:
-
Charlson comorbidity index
- CI:
-
Confidence interval
- CFS:
-
Clinical frailty scale
- eGFR:
-
Estimated glomerular filtration rate
- HR:
-
Hazard ratio
- ICU:
-
Intensive care unit
- NRI:
-
Net reclassification improvement
- OR:
-
Odds ratio
- SOFA:
-
Sequential organ failure assessment
- RRT:
-
Renal replacement therapy
References
Hoste EA, Bagshaw SM, Bellomo R, Cely CM, Colman R, Cruz DN, Edipidis K, Forni LG, Gomersall CD, Govil D, et al. Epidemiology of acute kidney injury in critically ill patients: the multinational AKI-EPI study. Intensive Care Med. 2015;41(8):1411–23.
Villeneuve PM, Clark EG, Sikora L, Sood MM, Bagshaw SM. Health-related quality-of-life among survivors of acute kidney injury in the intensive care unit: a systematic review. Intensive Care Med. 2016;42(2):137–46.
Oeyen S, De Corte W, Benoit D, Annemans L, Dhondt A, Vanholder R, Decruyenaere J, Hoste E. Long-term quality of life in critically ill patients with acute kidney injury treated with renal replacement therapy: a matched cohort study. Crit Care. 2015;19:289.
Rockwood K, Song X, MacKnight C, Bergman H, Hogan DB, McDowell I, Mitnitski A. A global clinical measure of fitness and frailty in elderly people. CMAJ. 2005;173(5):489–95.
Brummel NE, Bell SP, Girard TD, Pandharipande PP, Jackson JC, Morandi A, Thompson JL, Chandrasekhar R, Bernard GR, Dittus RS, et al. Frailty and subsequent disability and mortality among patients with critical illness. Am J Respir Crit Care Med. 2017;196(1):64–72.
Heyland DK, Stelfox HT, Garland A, Cook D, Dodek P, Kutsogiannis J, Jiang X, Turgeon AF, Day AG. Predicting performance status 1 year after critical illness in patients 80 years or older: development of a multivariable clinical prediction model. Crit Care Med. 2016;44(9):1718–26.
Bagshaw SM, Stelfox HT, McDermid RC, Rolfson DB, Tsuyuki RT, Baig N, Artiuch B, Ibrahim Q, Stollery DE, Rokosh E, et al. Association between frailty and short- and long-term outcomes among critically ill patients: a multicentre prospective cohort study. CMAJ. 2014;186(2):E95-102.
Bagshaw SM, Stelfox HT, Johnson JA, McDermid RC, Rolfson DB, Tsuyuki RT, Ibrahim Q, Majumdar SR. Long-term association between frailty and health-related quality of life among survivors of critical illness: a prospective multicenter cohort study. Crit Care Med. 2015;43(5):973–82.
Abdel-Kader K, Girard TD, Brummel NE, Saunders CT, Blume JD, Clark AJ, Vincz AJ, Ely EW, Jackson JC, Bell SP, et al. Acute kidney injury and subsequent frailty status in survivors of critical illness: a secondary analysis. Crit Care Med. 2018;46(5):e380–8.
Bagshaw SM, Adhikari N, Burns K, Friedrich J, Bouchard J, Lamontagne F, McIntrye L, Cailhier JF, Dodek P, Stelfox HT et al: Selection and receipt of kidney replacement in critically Ill Older Patients with AKI. Clin J Am Soc Nephrol 2019 (In Press), 14(April).
Von Elm E, Altman DG, Egger M, Pocock SJ, Gøtzsche PC, Vandenbroucke JP, Initiative S. The strengthening the reporting of observational studies in epidemiology (STROBE) statement: guidelines for reporting observational studies. Int J Surg. 2014;12(12):1495–9.
Shears M, Takaoka A, Rochwerg B, Bagshaw SM, Johnstone J, Holding A, Tharmalingam S, Millen T, Clarke F, Rockwood K, et al. Assessing frailty in the intensive care unit: a reliability and validity study. J Crit Care. 2018;45:197–203.
Bagshaw M, Majumdar SR, Rolfson DB, Ibrahim Q, McDermid RC, Stelfox HT. A prospective multicenter cohort study of frailty in younger critically ill patients. Crit Care. 2016;20(1):175.
Schafer JL. Multiple imputation: a primer. Stat Methods Med Res. 1999;8(1):3–15.
Morris TP, White IR, Royston P. Tuning multiple imputation by predictive mean matching and local residual draws. BMC Med Res Methodol. 2014;14:75.
Grimmett G, Grimmett GR, Stirzaker D. Probability and random processes. Oxford: Oxford University Press; 2001.
Ross SM. Introduction to probability models. Academic Press, Cambridge; 2014
Kizilarslanoglu MC, Civelek R, Kilic MK, Sumer F, Varan HD, Kara O, Arik G, Turkoglu M, Aygencel G, Ulger Z. Is frailty a prognostic factor for critically ill elderly patients? Aging Clin Exp Res. 2017;29(2):247–55.
Hamidi M, Zeeshan M, Leon-Risemberg V, Nikolich-Zugich J, Hanna K, Kulvatunyou N, Saljuqi AT, Fain M, Joseph B. Frailty as a prognostic factor for the critically ill older adult trauma patients. Am J Surg. 2019;218(3):484–9.
Fernando SM, McIsaac DI, Rochwerg B, Bagshaw SM, Muscedere J, Munshi L, Ferguson ND, Seely AJE, Cook DJ, Dave C, et al. Frailty and invasive mechanical ventilation: association with outcomes, extubation failure, and tracheostomy. Intensive Care Med. 2019;45(12):1742–52.
Hope AA, Law J, Nair R, Kim M, Verghese J, Gong MN: Frailty, acute organ dysfunction, and increased disability after hospitalization in older adults who survive critical illness: a prospective cohort study. J Intensive Care Med 2019:885066619881115.
Silva-Obregon JA, Quintana-Diaz M, Saboya-Sanchez S, Marian-Crespo C, Romera-Ortega MA, Chamorro-Jambrina C, Estrella-Alonso A, Andres-Esteban EM. Frailty as a predictor of short- and long-term mortality in critically ill older medical patients. J Crit Care. 2020;55:79–85.
Fernando SM, McIsaac DI, Rochwerg B, Cook DJ, Bagshaw SM, Muscedere J, Munshi L, Nolan JP, Perry JJ, Downar J et al: Frailty and associated outcomes and resource utilization following in-hospital cardiac arrest. Resuscitation 2019.
Brummel NE, Girard TD, Pandharipande PP, Thompson JL, Jarrett RT, Raman R, Hughes CG, Patel MB, Morandi A, Gill TM, et al. Prevalence and course of frailty in survivors of critical illness. Crit Care Med. 2020;48(10):1419–26.
Federspiel CK, Itenov TS, Mehta K, Hsu RK, Bestle MH, Liu KD. Duration of acute kidney injury in critically ill patients. Ann Intensive Care. 2018;8(1):30–30.
Dubb R, Nydahl P, Hermes C, Schwabbauer N, Toonstra A, Parker AM, Kaltwasser A, Needham DM. Barriers and strategies for early mobilization of patients in intensive care units. Ann Am Thorac Soc. 2016;13(5):724–30.
Wang YT, Haines TP, Ritchie P, Walker C, Ansell TA, Ryan DT, Lim PS, Vij S, Acs R, Fealy N, et al. Early mobilization on continuous renal replacement therapy is safe and may improve filter life. Crit Care. 2014;18(4):R161.
Vanmassenhove J, Van Biesen W, Lameire N. The interplay and interaction between frailty and acute kidney injury. Nephrol Dial Transplant. 2020;35(6):911–5.
Kim S-W, Han H-S, Jung H-W, Kim K-I, Hwang DW, Kang S-B, Kim C-H: Multidimensional frailty score for the prediction of postoperative mortality risk. JAMA Surg 2014, 149(7):633–640
Ferrante LE, Pisani MA, Murphy TE, Gahbauer EA, Leo-Summers LS, Gill TM. Functional trajectories among older persons before and after critical illness. JAMA Int Med. 2015;175(4):523–9.
Gross JL, Borkowski J, Brett SJ. Patient or family perceived deterioration in functional status and outcome after intensive care admission: a retrospective cohort analysis of routinely collected data. BMJ Open. 2020;10(10):e039416.
Gobbens RJ, van Assen MA, Luijkx KG, Wijnen-Sponselee MT, Schols JM. Determinants of frailty. J Am Med Dir Assoc. 2010;11(5):356–64.
Acknowledgements
Not applicable
Funding
This work was supported by Canadian Frailty Network Grant 2013-RFP2012-15–06. S.M.B. was supported by a Canada Research Chair in Critical Care Nephrology. W.B.S was supported by a Fonds de Recherche du Québec en Santé training award.
Author information
Authors and Affiliations
Contributions
WBS, SMB and RW designed the protocol for this study, AY and GL performed data analysis, WBS drafted the manuscript, all authors contributed to manuscript review and provided substantial contribution. All authors read and approved the final manuscript.
Corresponding author
Ethics declarations
Ethics approval and consent to participate
Approval for the study was received by the Research Ethics Board at the University of Alberta (File Pro00037850) and each participating centre.
Consent for publication
All participants or their legally authorized surrogate provided informed consent.
Competing interests
RW has received unrestricted research funding and speaker fees from Baxter.
Additional information
Publisher's Note
Springer Nature remains neutral with regard to jurisdictional claims in published maps and institutional affiliations.
Supplementary Information
Additional file 1
Supplementary materials
Rights and permissions
Open Access This article is licensed under a Creative Commons Attribution 4.0 International License, which permits use, sharing, adaptation, distribution and reproduction in any medium or format, as long as you give appropriate credit to the original author(s) and the source, provide a link to the Creative Commons licence, and indicate if changes were made. The images or other third party material in this article are included in the article's Creative Commons licence, unless indicated otherwise in a credit line to the material. If material is not included in the article's Creative Commons licence and your intended use is not permitted by statutory regulation or exceeds the permitted use, you will need to obtain permission directly from the copyright holder. To view a copy of this licence, visit http://creativecommons.org/licenses/by/4.0/. The Creative Commons Public Domain Dedication waiver (http://creativecommons.org/publicdomain/zero/1.0/) applies to the data made available in this article, unless otherwise stated in a credit line to the data.
About this article
Cite this article
Beaubien-Souligny, W., Yang, A., Lebovic, G. et al. Frailty status among older critically ill patients with severe acute kidney injury. Crit Care 25, 84 (2021). https://doi.org/10.1186/s13054-021-03510-y
Received:
Accepted:
Published:
DOI: https://doi.org/10.1186/s13054-021-03510-y