Abstract
Bone marrow-Multipotential stromal cells (BM-MSCs) are increasingly used to treat complicated fracture healing e.g., non-union. Though, the quality of these autologous cells is not well characterized. We aimed to evaluate bone healing-related capacities of non-union BM-MSCs. Iliac crest-BM was aspirated from long-bone fracture patients with normal healing (U) or non-united (NU). Uncultured (native) CD271highCD45low cells or passage-zero cultured BM-MSCs were analyzed for gene expression levels, and functional assays were conducted using culture-expanded BM-MSCs. Blood samples were analyzed for serum cytokine levels. Uncultured NU-CD271highCD45low cells significantly expressed fewer transcripts of growth factor receptors, EGFR, FGFR1, and FGRF2 than U cells. Significant fewer transcripts of alkaline phosphatase (ALPL), osteocalcin (BGLAP), osteonectin (SPARC) and osteopontin (SPP1) were detected in NU-CD271highCD45low cells. Additionally, immunoregulation-related markers were differentially expressed between NU- and U-CD271highCD45low cells. Interestingly, passage-zero NU BM-MSCs showed low expression of immunosuppressive mediators. However, culture-expanded NU and U BM-MSCs exhibited comparable proliferation, osteogenesis, and immunosuppression. Serum cytokine levels were found similar for NU and U groups. Collectively, native NU-BM-MSCs seemed to have low proliferative and osteogenic capacities; therefore, enhancing their quality should be considered for regenerative therapies. Further research on distorted immunoregulatory molecules expression in BM-MSCs could potentially benefit the prediction of complicated fracture healing.
Similar content being viewed by others
Introduction
Despite advances in trauma fixation techniques within the orthopaedic field, atrophic fracture non-union is still significant health and socioeconomic burden1,2,3,4,5. Multipotential stromal cells (BM-MSCs) have been acknowledged for enhancing bone healing particularly in complicated healing conditions such as atrophic fracture non-union6,7,8,9,10. However, autologous native BM-MSCs are usually applied as a part of bone marrow (BM) aspirates or concentrate without an assessment of the quality of these cells. Furthermore, inadequate research data on the quality of these potential therapeutic cells has led to a lack of consensus on whether complementary growth adjuvants are required to enhance their healing capacities.
MSCs can migrate from BM and other adjacent tissues within a few days of bone injury, and are highly involved in the three phases of the healing process; inflammatory, repair and remodelling11,12,13,14. During the inflammatory phase, a hematoma is formed involving several immune cells and mediators12,13,15,16,17,18. However, a balanced immune response is required for successful bone healing. A clinical removal of fracture hematoma in elderly or multi-diseased patients is perceived as a cause delayed or impaired healing19. Additionally, complicated healing was strongly inked to prolonged local inflammatory response20,21,22. The presence of MSCs within the fracture hematoma has been reported12 with an indication of their involvement in immunosuppression to end the inflammatory phase and to start bone repair23. Furthermore, applying MSCs has been linked to decrease the levels of inflammatory cytokines in association with enhancing the osteogenesis in experimental models of fractures and osteoporosis24,25,26. However, only MSCs primed by interferon gamma (IFN-γ), tumour necrosis factor-alpha (TNF-α), interleukin-1 (IL-1), and interleukin-17 (IL-17) can produce immunosuppressive factors such as Tumour Growth Factor-beta 1 (TGF-β1), Prostaglandin E2 (PGE2) and Indoleamine 2,3-Dioxygenase (IDO)23.
MSC differentiation into osteoblasts is also essential for bone repair and remodelling. The osteogenic capacity of MSCs typically starts with proliferation and expression of specific proteins, e.g., osteopontin (SPP1), followed by matrix maturation with alkaline phosphatase (ALP) expression. Finally, mineralisation is characterised by increased ALP and osteocalcin (BGLAP) expression27. Furthermore, MSCs support new bone vasculature via Vascular Endothelial Growth Factor (VEGF),28. Recently, Bone Marrow Stromal Cell Antigen-2 (BST2) was identified as a marker for some BM-MSC clones with immunoregulatory capacities29. Furthermore, BST2 knockdown in BM-MSCs has revealed its role in osteogenic differentiation through the regulation of the bone morphogenic protein 2 (BMP-2) signalling pathway30. Additionally, another protein related to mineralisation and highly expressed in osteoblasts, S100 calcium-binding protein A8 (S100A8) was linked to MSC-mediated immunoregulation31, but with no link to the MSC osteogenic capacity.
Several studies reported biological mechanisms underlying fracture atrophic non-union development with the involvement of the osteogenesis-related BMP and Wnt signalling pathways32,33,34,35,36. However, the research examining MSC biology in non-union fracture has been focused on their presence and quantities. These osteoprogenitors were detected within the tissues of non-union as expressing stem cell markers36,37,38. Noteworthy, lower numbers of BM-derived colony-forming cells were reported for atrophic non-union than healed fractures patients39; however, no difference was found in BM-MSC numbers expressing osteoprogenitor marker, CD271high in another study40. Other studies have reported a similar osteogenic function of MSCs resident within non-union tissues relative to donor-matched BM-MSCs but without comparison to union-MSCs36,37,41,42. Furthermore, the immunoregulatory potential of non-union BM-MSCs is mostly unknown despite being an important part of the bone healing process.
We aimed in this study to investigate bone healing-related functions of BM-MSCs in non-united fractures. Consequently, we compared proliferation, osteogenesis, and immunoregulation of BM-MSCs from patients who had established non-union fractures (NU) with those from patients with united fractures (U). These BM-MSCs were analysed either without culture as CD271high CD45low cells, the surrogates of BM-MSCs43,44,45,46, or with a minimal culture (passage-zero cells). Culture-expansion of these BM-MSCs as standardly characterised47 was conducted to generate sufficient cell numbers for the functional assays. To investigate the potential systemic/serum influence on NU BM-MSC functions, we assessed the serum levels of priming cytokines and their receptor expression in BM-MSCs. This knowledge could help to further understand the biological role of MSCs during the development of complicated bone healing and potentially aid to optimise the autologous BM-MSC based regenerative therapies.
Results
The isolation and characterisation of uncultured BM-cells
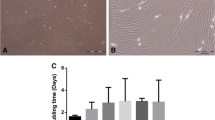
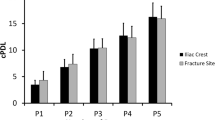
To test the functional markers of uncultured (native) BM-MSCs, the FACS isolation of BM-cells (both NU and U) was conducted. The live cells were marked as Calceinpositive Aquanegative cells, then CD271high CD45low (MSC surrogates) and CD271negative CD45positive cells hematopoietic lineage cells (HLCs) were isolated for gene expression assays (Fig. 1a). Distinct differences between CD271high CD45low cells and HLCs were evident as shown via the clustering of transcripts levels and comparative group analysis (Fig. 1b and Table 1). As expected, the transcript levels of NGFR (CD271) and osteogenic markers, BGLAP, ALPL, SPARC, LepR and SPP1 were higher for CD271high CD45low cells than HLCs (p < 0.0001). Uniquely, more transcripts of IL-1R1 (p = 0.003), Fibroblast growth factor receptors 1 (FGFR1), and epidermal growth factor receptor (EGFR) were also detected for CD271high CD45low cells (p < 0.001). However, PTPRC (CD45), TGF-ß, Prostaglandin E synthetase 2 (PGES2), IL-17RA, and TNFRS1A transcripts were significantly lower in CD271high CD45low cells than HLCs (p < 0.0001). Furthermore, IDO and IL-10 transcripts were not detected in CD271high CD45low cells. Collectively, uncultured sorted CD271high CD45low cells showed specific MSC gene profile compared to HLCs. Based on these findings, we consequently assessed the functional markers for sorted CD271high CD45low cells.
The isolation of uncultured BM CD271high CD45low cells. (a) The FACS plots show the gating strategy for isolation of live BM cells (as Aqua negative Calcein positive) then uncultured BM-MSCs as CD271high CD45low and HLCs (CD45positive CD271negative). (b) The clustering of donor-matched CD271high CD45low and HLCs (n = 6) for expression of growth, osteogenic, and immune-related markers. Green: low expression. Red: high expression. Grey: below detection.
A defective proliferation and osteogenic potential of uncultured and minimally-cultured BM-MSCs
Following the sorting of BM cells, the growth factor receptors and osteogenic markers were tested on isolated uncultured CD271high CD45low cells. Interestingly, fewer transcript levels of EGFR, FGFR1 and FGRF2 were detected in uncultured NU-CD271high CD45low than U-cells (p = 0.049, p = 0.021, and p < 0.001 respectively, Fig. 2a and Table 1) indicating potentially a low response to these growth factors. When measuring the growth factors related to angiogenesis, the VEGFA transcripts (but not VEGFC or ANGTP) were lower in NU-CD271high CD45low cells than U-cells (p = 0.032, Fig. 2a and Table 1). To test if serum has an impact (systemic) on the proliferation of BM-MSCs, BM cells were seeded in cultures with either NU- or U-serum then the levels of 18 s were assessed (without cell passage) as indicative of cell quantities. Noticeably, the donor-matched comparison showed that both NU- and U-passage-zero BM-MSCs had reduced 18 s levels when in NU serum cultures than those in U-serum cultures (p = 0.031 for both, Fig. 2b) indicating a negative effect of NU serum on MSC proliferation.
The proliferative potential and osteogenic markers of NU BM-MSCs. (a) The figure shows the median of relative gene expression of growth factors receptors and angiogenic factors. The unpaired t-test was used to compare uncultured isolated NU- CD271high CD45low cells (n = 8) and U-CD271high CD45low cells (n = 9). (b) The figure shows the relative gene expression of 18 s for passage-zero NU or U BM-MSCs in cultures supplemented with either U-serum or NU-serum. The Wilcoxon test was used to compare passage-zero either NU or U BM-MSCs (n = 3) between cultures supplemented with U-serum and NU-serum. (c) The figure shows the median of relative gene expression of osteogenic markers. The Mann Whitney test was used to compare uncultured isolated NU-CD271high CD45low cells (n = 8) and U-CD271high CD45low cells (n = 9). (d) The figure presents the median (with interquartile range) of relative gene expression of osteogenic markers for passage-zero BM-MSCs in either U-serum or NU-serum supplemented cultures. The Kruskal-Wallis test was used to compare the groups (n = 3).
The PCR data showed significantly lower levels of osteogenic markers, ALPL, BGLAP, SPARC and SPP1, but not LepR in uncultured NU-CD271high CD45low cells than U-cells (p = 0.040, p = 0.049, p = 0.043 & p = 0.047 respectively, Fig. 2c and Table 1) suggesting an impaired osteogenic potential for NU BM-MSCs. When cultured in NU-serum, passage-zero NU BM-MSCs had consistently less ALPL transcripts relative to U-serum cultures (p = 0.008) and U-MSCs in both serum cultures (both p = 0.029, Fig. 2d). However, BGLAP, SPP1 and SPARC transcripts were comparable in both U and NU serum-cultures (Fig. 2d). In summary, reduced the proliferative potential of NU BM-MSCs was noted, and apparently due to both cellular and serum-related causes. Also, osteogenic markers were less expressed on native BM-MSCs, but that was not as evident in serum-supplemented cultures.
An altered immunoregulatory phenotype of uncultured and minimally-cultured NU BM-MSCs
To assess the immunoregulatory potential of NU BM-MSCs, markers for immunosuppression and other new immunoregulation-related molecules were measured. Comparing uncultured NU- and U-CD271high CD45low cells, immunosuppressive TGF-β1 and PTGES2 transcripts were found similar (Fig. 3a). These data indicated no difference in the basal levels of these immunosuppressive mediators between U- and NU-MSCs. Notably, fewer transcripts of an immunoregulation-related marker, BST2 were detected for uncultured NU-CD271high CD45low cells compared to U cells (p = 0.019, Fig. 3a and Table 2). In contrast, higher transcript levels of another immunoregulation-related molecule S100A8 (p = 0.022, Fig. 3a and Table 2) were detected for NU-CD271high CD45low cells than U cells. Interestingly, the BST2 transcript levels were positively correlated with those of ALPL, BGLAP and SPARC, EGFR, FGFR1 & FGFR2 (p < 0.001, p = 0.003, p = 0.034, p = 0.012, p = 0.012, p = 0.021, respectively, Fig. 3b). However, S100A8 transcript levels did not correlate with these markers (Fig. 3c). These findings indicated altered immunoregulatory markers of NU-MSCs with verification of BST2 link to osteogenic and proliferation of BM-MSCs.
An altered immunoregulatory phenotype of NU BM-MSCs. (a) The figure shows the median of relative gene expression of immunoregulatory markers. The Mann-Whitney test was used to compare uncultured isolated NU-CD271high CD45low cells (n = 8) and U-CD271high CD45low cells (n = 9). (b) The plots show the correlation between the transcript levels of BST2 versus those of osteogenic and growth factor receptors in CD271high CD45low cells. Spearman r test was used for the correlation (n = 17). (c) The plots show the correlation between the transcript levels of S100A8 versus those of osteogenic and growth factor receptors in CD271high CD45low cells. Spearman r test was used for the correlation (n = 17). (d) The figure presents the mean of relative gene expression of IDO, PTGES2 and TGF-β1 when passage-zero BM-MSCs were treated with a mixture of IFN-γ, TNF-α, and IL-1 in U-serum or NU-serum supplemented cultures. The Kruskal-Wallis test was used to compare the groups (n = 3).
The expression of immunosuppressive markers was further evaluated following treating passage-zero NU BM-MSCs with a mixture of IFN-γ, TNF-α, IL-1 and IL-17 in serum-supplemented cultures. Noteworthy, cytokine-treated NU BM-MSCs had lower IDO, TGF-β1 and PGES2 expression than U BM-MSCs in their matched serum cultures (p = 0.001, p = 0.005, p = 0.001, respectively Fig. 3d). Furthermore, U BM-MSCs were found to express fewer transcripts of IDO, TGF-β1, and PGES2 in NU-serum cultures than U-serum cultures (p = 0.019, p = 0.019, p = 0.058, respectively Fig. 3d) suggesting an additional effect of NU-serum. Together, NU BM-MSCs demonstrated low expression levels of cytokine-induced immunosuppressive markers and particularly in NU-serum cultures suggesting both cellular and systemic-related causes.
U and NU BM-MSCs had similar functions when culture-expanded
The uncultured and minimally-cultured BM-MSCs showed reduced proliferative capacity, lower expression of osteogenic markers with altered expression immunoregulatory markers. To test if these detected changes have a functional impact on BM-MSCs, culture expansion of these progenitors was performed to get enough cells for the functional assays. The culture-expanded U- and NU BM-MSCs with/without cytokines had no significant differences in the XTT absorbance (Fig. 4a) indicating similar in vitro proliferative capacity. To further confirm these data, BM-MSCs were loaded on scaffolds, and the numbers of NU- and U-MSCs (counted as CD45− CD73+ CD90+ CD105+ cells using flow-cytometry,48) were similarly increased after 3-week cultures relative to 1-week cultures (p = 0.007 and p = 0.003 respectively, Fig. 4b) confirming similar proliferation for culture-expanded NU-MSCs and U-MSCs.
The comparison of culture-expanded NU-MSC and U-MSC functions. (a) The Whiskers plot shows the median of XTT absorbance (proliferation) for culture-expanded MSCs + /− treatment of inflammatory cytokines. The Mann-Whitney test was used to compare U-MSCs (n = 6) & NU-MSCs (n = 4). (b) The figure shows the mean (with the standard of the mean) of the MSC numbers released from scaffolds. The paired t-test was used for comparing 1-week and 3-week cultures and unpaired t-test for comparing U- and NU-MSCs (n = 3). (c) The Whiskers plot presents the median of calcium levels for culture-expanded MSCs following 3 weeks of culture in an osteogenic medium. The Mann-Whitney test was used to compare U-MSCs (n = 5) and NU-MSCs (n = 3). (d) The flow-cytometry plots show the gating of intracellular IDO expression by culture-expanded MSCs. (e) The mean (with the standard of the mean) of the percentages of positive-expressing IDO in culture-expanded MSCs. The paired t-test was used to compare donor-matched no-cytokine with cytokines groups. The unpaired t-test was used to compare U-MSCs and NU-MSCs (n = 4). (f) The median of the percentages of positive-expressing LAP in culture-expanded MSCs. The paired t-test was used to compare donor-matched no-cytokine with cytokines groups. The unpaired t-test was used to compare U-MSCs and NU-MSCs (n = 4).
For testing the osteogenic differentiation, culture-expanded BM-MSCs were cultured for 3 weeks in osteogenic medium with/without cytokine treatment then the calcium deposition levels were measured. While IL-1 and IL-17 (but not IFN-γ, and TNF-α) seemed to induce calcium levels in differentiating NU and U BM-MSCs (Fig. 4c), measured calcium levels were comparable for NU and U BM-MSCs either with or without cytokine treatments (Fig. 4c). These data demonstrated the similar osteogenic capacity of culture-expanded NU and U BM-MSCs.
For immunosuppression, cytokine-treated culture-expanded MSCs were assessed for the intracellular IDO levels using flow-cytometry (Fig. 4d). As expected, the IDO levels were similarly induced when MSCs were treated by IFN-γ alone or combined with TNF-α, IL-1 or IL-17 (all p < 0.001, Fig. 4e). Importantly, these induced IDO levels were similar for NU- and U-MSCs (Fig. 4e). Also, the percentage of culture-expanded NU- and U-MSCs expressing LAP (surface TGF-β1) were similarly increased after cytokine treatments (p = 0.040 p = 0.006, respectively, Fig. 4f). These results indicated comparable immunosuppressive functions of culture-expanded NU- and U-MSCs.
The expression of cytokine receptors on BM-MSCs and comparable serum cytokine levels during early fracture healing
As the minimal cultures data indicated that NU BM-MSCs were less immunosuppressive when cytokine-treated compared to U-MSCs, we next tested if the cytokine receptor levels could be a contributing factor. Interestingly, the uncultured NU-CD271high CD45low cells expressed fewer transcripts of IL-1R1 than U-CD271high CD45low cells (p = 0.005, Fig. 5a). However, no significant differences were detected for other cytokine receptor transcripts (Fig. 5a). Consistently, the surface protein expression of the cytokine receptors was similar for uncultured NU-and U-CD271high CD45low cells except for IL-1R1, which were less expressed on the surface of NU-CD271high CD45low cells (p = 0.049, Fig. 5b).
The measurements of cytokine receptor expression for BM-MSCs. (a) The scatter dot plots show the median of relative gene expression of cytokine receptors. The unpaired t-test was used to compare uncultured isolated NU-CD271high CD45low cells (n = 8) and U-CD271high CD45low cells (n = 9) for all cytokine receptors except for TNFR1, in which the Mann-Whitney test was used. (b) The scatter dot plots present the median of surface expression levels of cytokine receptors. The unpaired t-test was used to compare uncultured NU-CD271high CD45low cells and U-CD271high CD45low cells (n = 8 and 9 respectively) for all cytokine receptors except for CD217 (IL-17RA), in which the Mann-Whitney test was used. (c) The figure demonstrates the changes in cytokine receptor levels between donor-matched uncultured CD271high CD45low cells and culture-expanded MSCs. (d) The figure presents a comparison of cytokine receptor levels between culture-expanded NU-MSCs (n = 3) and U-MSCs (n = 6). The Mann-Whitney test was used for the comparison.
To explore why contrarily culture-expanded BM-MSCs have similar immunosuppressive functions, the surface cytokine receptor expressions were compared between donor-matched culture-expanded MSCs and uncultured CD271high CD45low cells. The data showed various changes in all receptors surface expression (mainly a decrease after culture-expansion) in both U-MSCs and NU-MSCs (Fig. 5c). Furthermore, comparable cytokine receptor levels were noted between culture-expanded NU- and U-MSCs (Fig. 5d) verifying changes of MSC surface phenotype during in vitro culture-expansion.
We further aimed to understand if serum cytokines levels are linked to the decreased proliferative potential and altered immunosuppressive phenotype of native BM-MSCs. Therefore, the levels of immunosuppression-related cytokines were measured in serum of fracture patients relative to control levels. The ELISA data showed that IFN-γ, TNF-α, and IL-1 levels were not different between U-sera, NU-sera and control sera (Fig. 6a–c). These findings indicated no systemic changes in these cytokine levels during fracture healing. Noteworthy, the measured IL-17 levels were alike for U and NU fractures during early healing. However, significant lower IL-17 levels were detected for late healing NU-serum than healed U-serum and control levels (p < 0.001 and p < 0.001, respectively, Fig. 6d). Collectively, apart from IL-17 measured in NU serum at late healing, comparable serum cytokine levels were noted for NU and U.
The measurements of serum cytokine levels. The figures show the median of serum levels of IFN-γ, TNF-α, IL-1 and IL-17 (a–d respectively) during a week of fracture (early healing), at or after 6 months of fracture (late healing) and healthy control levels (two-time points, 6-month apart). The Kruskal-Wallis test was used to compare levels of IFN-γ, TNF-α, IL-1 and IL-17 between U-serum (early healing: n = 9, 12, 9 and 13 respectively, late healing n = 9, 12, 9 and 11 respectively), NU-serum (early healing n = 5, late healing n = 9, 12, 9 and 6 respectively) and control serum (both time points: n = 8, 11, 7 and 5 respectively).
Discussion
The application of autologous BM to boost the healing of non-united fractures as a source of osteoprogenitors has gained lately a great popularity49,50,51,52. However, the quality of these BM-MSCs is poorly understood. In this study, we comprehensively compared various functional potentials of BM-MSCs from NU and U fracture patients utilising multiple assays and at different cell culture conditions. The functional potential of uncultured CD271high CD45low cells and minimal MSC cultures have shown significant differences between NU and U BM-MSCs, implying defective multifunction of NU BM-MSC. However, the functions of culture-expanded MSCs were similar. This masking of cell differences within the culture-expanded cells is most likely due to in vitro-related changes in cell phenotype such as those changes we detected for the expression of the surface cytokine receptors. Similarly, adipose-derived MSCs showed significant variations in cell cycle and functional transcripts during culture-expansion53. We think that foetal calf serum (FCS) could be a contributing factor to phenotype changes, particularly with previous research has shown that human serum, unlike FCS, can maintain the MSC genomic patterns54.
With regards to the proliferative capacity, we identified significant lower transcripts levels of EGF and FGF receptors for uncultured NU CD271high CD45low cells than U cells. These findings implied a weak response to EGF and FGF, which are known to be essential for the MSC proliferation and survival, particularly in fractures55,56,57,58. Also, a role for EGF in fracture healing has been suggested when its serum levels were found increased in patients with a brain injury combined with a limb fracture than those having brain injury only59. In agreement with our findings, a previous study has reported downregulation of FGF-R2 gene expression in human non-union osteoblast cultures35. In addition to the MSC response to growth factors, we noted an inadequate proliferation of passage-zero BM-MSCs in cultures supplemented with NU-serum compared to U-serum cultures inferring lower growth inducers in NU-serum. Our group previously showed that the proliferative capacity of BM-MSCs from fracture patients was positively correlated with serum growth factor levels, such as platelet-derived growth factors (PDGFs)55. In total, it seems that the proliferation of BM-MSCs in non-union patients could be defective due to both intrinsic cellular and extrinsic microenvironmental factors. Such complicated alterations of the NU BM-MSC proliferation could be potentially compensated for by applying adequate numbers of BM-MSCs as suggested for therapies of non-united fractures51.
We detected significantly lower osteogenic marker levels in uncultured NU BM- CD271high CD45low cells despite the osteogenic ability shown for culture-expanded cells in this study and previous work41. In NU-serum supplemented cultures, all osteogenic genes, except ALPL showed comparable levels versus U-cultures. These observations could be explained by the positive osteoinductive role of human serum effect on progenitor osteogenesis as reported before60. Together, unlike culture-expanded MSCs, our data uniquely suggested a lower osteogenic potential of native NU BM-MSCs compared to U BM-MSCs. This apparent osteogenic defect could be probably improved by co-application of autologous serum growth factors, e.g., concentrated platelet lysate products. Consistent with our findings of low osteogenic potential of BM-MSCs in NU patients, the serum levels of several osteogenic markers have been shown to decrease in NU fractures. Kurdy et al. and Emami et al. detected lower levels of ALP in patients with delayed healed tibial fractures than normal healers61,62. Additionally, other groups reported reduced levels or delayed induction of osteocalcin levels in NU than U fractures63,64,65. Furthermore, the concentrations of C-terminal cross-linking telopeptide of type I collagen measured in the serum of NU patients were significantly less than those in U group66.
Although early inflammatory response is critical for the healing of fractures and bone loss, unbalanced inflammation marked by high levels of cytokines, TNF-α, IFN- γ and IL-1 TNF-α in fracture hematoma or callus could hinder a successful bone regeneration and lead to complicated healing (or non-union)11,20,67,68,69. Schmidt-Bleek et al. also have reported that higher relative expression of the pro-inflammatory cytokines together with a higher percentage of cytotoxic T cells in the hematoma of delayed healing than those of normal healed fracture70. Several studies reported that MSCs could drive immunosuppressive response as a part of their role in bone healing e.g., decreasing cytokines levels in association with enhancing the osteogenesis in fractures or osteoporosis models24,25,26. Uniquely, we showed here that NU BM-MSCs had fewer transcripts of IDO, PTGES2 and TGF-β1 when cytokine-treated than those of U BM-MSCs. Furthermore, low expression of IL-1 receptors in NU BM-MSCs might also suggest less response to such a priming cytokine. Altogether, our findings showed that NU BM-MSCs could have less immunosuppressive potential that could negatively affect normal bone healing.
In addition to immunosuppressive markers, other markers related to BM-MSCs immunoregulatory potential have been recently described. An example is the detection of high levels of BST2 expression in specific clones of BM-MSCs that secrete an immunoregulatory cytokine, IL-629. We also have reported that S100A8 was highly expressed on hematopoietic cell-depleted cancellous bone populations that are capable of inhibition of T cell proliferation31. Our novel data here showed that NU BM-MSCs expressed lower BST2 transcripts, but higher S100A8 transcripts than U BM-MSCs. Furthermore, BTS2, but not S100A8 transcript levels were positively correlated with the osteogenic markers and growth receptor levels, confirming previous results of BST2 involvement in the MSC osteogenic differentiation30. The high S100A8 transcript levels in NU BM-MSCs could be linked to dysregulated bone remodelling as S100A8 has been shown as a contributor in the remodelling process71.
We detected significantly lower levels of IL-1 receptors consistently at protein and gene expression levels in NU BM-MSCs, also validating our PCR data. Growing evidence has indicated that IL-1 could have an individual or additive role to IFN-γ in enhancing MSC-mediated immunosuppression72,73. Additionally, IL-1 was shown to enhance osteogenesis, particularly for periodontal ligament stem cells74. Therefore, the functional impact of low expression of IL-1R on bone healing would be interesting for further investigations.
We measured the serum levels of cytokines that are known to prime BM-MSCs for immunosuppression. Our data showed no differences in serum levels of IFN-γ, TNF-α, IL-1, and IL-17 between patients or healthy non-fracture controls. Unlike serum, high levels of TNF-α were noted in fracture hematoma initially, then these levels were decreased with repair, but were highly expressed again during remodelling75,76,77. Also, IFN-γ expression levels were reported to be increased at hematoma78. Exceptionally, the IL-17 levels in NU-sera were significantly lower than U- and control serum in late healing. IL-17 was detected in soft callus during bone healing79 and shown to have a complicated role during remodelling being supportive of osteoblastic bone formation but also involved in the stimulation of osteoclasts formation80,81,82. Our data showing lower IL-17 levels in NU sera than controls might suggest a relation to the disturbance in the bone remodelling process. The expression levels of several serum cytokines, growth factors, and other inflammation-related molecules in NU fracture patients were thoroughly assessed in many previous studies. However, and up to our knowledge, we are the first to compare serum cytokines, IFN-γ, TNF-α, IL-1, and IL-17 between NU, U patients, and healthy controls and found comparable levels. Likewise, another study showed that serum levels of IL-8, which is linked to human MSC migration83 were not different between NU fractures and controls84. Furthermore, serum levels of other cytokines linked to BM-MSC migration, such as Macrophage colony-stimulating factor (M-CSF) and SDF-185, were found to be similar between patients with physiological fractures and those with impaired fracture healing84,86. In contrast, Mathieu et al. found higher serum levels of IL-6 and lower levels of soluble IL-6 receptors in NU patients compared to healthy individuals84. Interestingly, an in vitro work showed that high concentrations of IL-6 with low expression of soluble IL-6 receptors could inhibit MSC differentiation87.
In terms of growth factors, TGF-beta, PDGF, FGF, and IGF are critically important for differentiation and growth of MSCs58,88. In fractures, TGF-β1 serum levels were found peaked between 1 and 6 weeks after trauma in normal healers, but it lasted for a shorter time and lower levels in NU patients89,90. Additionally, reduced PDGF serum levels in NU fractures were noted compared to U fractures84,90,91. Similarly, lower serum levels of FGF-2 in paediatric NU patients than normal healers were reported92. Previous data also showed low and stable levels of serum insulin-like growth factor-1 (IGF-1) and its specific binding proteins in NU fractures84,90,93. While serum VEGF concentrations in NU patients were found comparable to those in patients with normal fracture healing in some studies84,94, others found that serum VEGF is increased when NU fracture is treated95. Compared to systemic changes in these growth factors, other growth factors seemed to have local changes. Serum BMP-2 and BMP-4 were below the detection level in both U and NU patients90. Another work demonstrated no significant difference in plasma levels of BMP-2, -4, -6, and -7 between patients with NU and those with normal fracture healing96. However, the expression levels of these BMPs were significantly lower when assessed within fibrous NU tissue relative to a standard healing callus33,97.
Additional serum factors that are related to skeletal tissue inflammation or BM-MSC immunomodulatory functions were also quantified by other groups. In one study, NU patients had significantly higher serum concentrations of metalloproteinase protein-1 (MMP-1) and MMP-8, which are linked to skeletal tissue inflammation98 compared with those with normal fracture healing99. S100A9 is also secreted by blood cells, and its high serum levels are linked to inflammation, particularly of musculoskeletal tissues100. Interestingly, serum S100A9 has been found elevated than normal in NU patients101, reflecting a local inflammation of NU tissues in which MSCs could be involved. Another work by Wang et al. demonstrated that Nitric oxide (NO), which is linked to MSC differentiation and bone remodelling102, had significantly lower levels in persistent NU patients relative to those having good healing progress95. Furthermore, proteomic analysis of serum showed that complement C6, C3 and C4, which their strongly activating phenotype is less favourable for MSC-related immunosuppression85, were up-regulated in the serum of NU patients compared to healthy controls101. Altogether, the systemic changes of various serum mediators could explain the lower proliferative and osteogenic potential as well as the altered immunomodulatory potential of the MSC pool in BM that we noted in our study and by others for NU fracture patients103.
Having NU BM-MSCs collected retrospectively was a limitation in our study. We could not prove that the altered immunoregulatory phenotype of these NU BM-MSCs (i.e. being less immunosuppressive, low BST-2 and IL-1R and high S100A8 expression) was consistently the same phenotype at the early phase of healing. Further research using a large panel of NU BM-MSCs prospectively collected within the early phase of fracture healing would be of great value to confirm our findings of the altered immunoregulatory phenotype. Such research could potentially help to introduce new predictive molecules for non-union fracture at the early phase and perhaps allowing earlier intervention with therapies to enhance bone repair.
In conclusion, our data of uncultured BM-MSCs indicated some interesting differences between union and non-union MSCs. These native NU BM-MSCs seemed to have a low proliferative capacity and osteogenic potential relative to U BM-MSCs. Additionally, our study is the first report of an altered immunoregulatory phenotype of NU BM-MSCs with these cells appeared to have reduced immunosuppressive potential and lower expression of BST2. Clinically, the quality of native uncultured autologous BM-MSCs used for enhancing bone regeneration should be considered. One may argue that the therapeutic value of autologous native BM-cells could be improved with growth adjuvants as well as placing adequate numbers of these BM-MSCs in situ to compensate for potentially low performance.
The functions of culture-expanded NU and U BM-MSCs were comparable most probably due to changes in cell phenotype. Therefore, to assess the MSC functions to a close picture as possible to in vivo cell performance, functional experiments would need to be optimised on minimally-cultured MSCs and in the presence of human serum. In such an experimental approach, future analysis of the functional impact of low IL-1 receptor levels in NU BM-MSCs could potentially help to improve cell-based bone regenerative therapies. Additionally, further work would be required to confirm a specific immunoregulatory phenotype of NU BM-MSCs at the early healing phase, which could potentially help to predict the risk of non-union fractures.
Methods
Ethics statement
Informed written consent was obtained from all the study participants before the samples were collected, and research was carried out in accordance with the Helsinki Declaration of ethics. The consents and sample collection (blood and bone marrow samples used to extract MSCs) for this study were under ethical approval with NREC number, 06/Q1206/127, National Research Ethics Committee Yorkshire and Humber–Leeds East. All study experiments were conducted according to the appropriate guidelines and regulations.
Participants and samples
Overall seventy-one participants were included in the study (Table 2). All patients had long bone fractures (femur, tibia, humerus). NU was defined by the absence of radiological features of fracture healing (lack of callus formation in at least 3 cortices) either on plane radiographs or computed tomography scans after 9 months from fracture fixation and with ongoing pain at the NU site during ambulation. Exclusion criteria were children, cancer, diabetes, bone metabolic diseases, inflammatory/immune disorders and intake of drugs with a negative impact on fracture healing (i.e. NSAIDs). BM samples (15 ml) were aspirated from the anterior iliac crest as previously described104; within one week following injury for U patients, and after diagnosis (>9 months) for NU patients. Peripheral venous blood samples (12 ml) were collected (from the patients) within one week from the date of fracture (early healing phase) or after fracture had united (4–6 months from injury) for U fractures and at the time of NU diagnosis. Serum from healthy individuals who did not have any bone fractures was used as control (twice, 6-month apart). Comparing the age of three groups showed no significant difference (Kruskal-Wallis test, p = 0.497).
Isolation of uncultured BM cells and real-time PCR
BM-cells were processed for erythrocyte lysis as reported before105 then labelled with CD45 and CD271 antibodies (Miltenyi) and live/dead cell markers; Calcein violet/Aqua (ThermoFisher) for cell sorting. Uncultured CD271high CD45low cells as surrogates of MSCs43,44,45,46 and control hematopoietic lineage cells (HLCs, CD271negative CD45positive cells) were isolated using Fluorescence-activated cell sorting (FACS, Becton-Dickinson).
The quantitative real-time PCR using TaqMan probes (ThermoFisher, Table 1) was conducted for measuring the relative gene expression levels of chosen markers. RNA extraction was performed as per manufacturer recommendation (Norgen Biotek). Extracted RNA samples were processed for reverse transcription and then pre-amplification using kits (Fluidigm) as recommended. Finally, the gene expression assays were performed using 48.48 chip/Integrated Fluid Circuit (IFC) and using the Biomark™ HD system (Fluidigm). The marker transcript levels were calculated relative to that of a housekeeping gene, Hypoxanthine Phosphoribosyl transferase 1 (HPRT1).
BM-MSC cultures
BM-cells were cultured till plastic-adherent MSCs become confluent then lysed and analysed without passage (passage-zero cells). These cultures were maintained in DMEM medium (Sigma) supplemented with 10% pooled U- or NU-serum (from five donors and collected within one week of fracture). Some cultures were treated with cytokines (20 ng/ml IFN-γ, 20 ng/ml TNF-α, 10 ng/ml IL-1 and 100 ng/ml IL-17) as per previous studies106,107,108. For the culture-expansion, BM-cells were maintained in the StemMACS MSC Expansion medium (Miltenyi Biotec) and plastic-adherent MSCs were passaged then analysed at passage 3–4.
Proliferation
The proliferation of culture-expanded BM-MSCs was assessed using the XTT colorimetric assay kit (Merck). For testing the growth of culture-expanded BM-MSCs on Orthoss collagen® scaffold (Geistlich), 10 × 104 cells were loaded on 60 mm2 pieces of the scaffolds for 3 hours before maintaining in cultures. The loaded scaffolds were digested after 1 and 3 weeks of culture using collagenase (Stem cell technologies). The released cells were then characterised and counted by flow-cytometry as shown previously105,109. For passage-zero BM-MSCs in serum-supplemented cultures, the housekeeping 18 S expression was evaluated, indicating cell quantities as reported before110.
Osteogenesis and immunosuppression assays
The culture-expanded BM-MSCs were assessed for the osteogenesis by measuring the calcium levels after 3 weeks in osteogenic cultures105. The calcium levels were measured using a colorimetric kit (Sentinel)105,99,78,78.
The immunosuppressive capacity of culture-expanded BM-MSCs was tested following treatment for 5 days with cytokines. The cells were then processed for measuring the intracellular IDO and surface TGF-β1 latency-associated peptide (LAP) levels using specific conjugated monoclonal antibodies (ThermoFisher) for flow-cytometer as demonstrated in previous studies111,112,113. For passage-zero cultured BM-MSCs that were cytokine-treated, the expression levels of IDO, PGE2 and TGF-ß transcripts was evaluated indicating the MSC immunosuppressive potential.
Surface cytokine receptor measurement
Flow-cytometry was used to measure the cytokine receptor levels on the surface of uncultured NU and U CD271high CD45low cells (and to validate PCR data) or on culture-expanded NU and U MSCs. The flow-cytometry conjugated monoclonal antibodies against IFN-γ receptor 1 (CD119), TNF-α receptor 1 (CD120a), (both from Miltenyi Biotec), IL-17 receptor A (CD217), (R&D systems) and IL-1β receptor 1 (BD Biosciences) were used for these assays.
Serum cytokine measurements
The blood samples were processed by centrifugation (2000g for 15 minutes) to extract the serum, as previously described114. The separated sera were analysed for the IFN-γ, TNF-α, IL-1 and IL-17 levels using the hypersensitive ELISA kits (R&D systems) as recommended by the manufacturer. The optical density values were acquired using MULTISCAN EX reader and analysed with Ascent software (Thermo electron corporation).
Statistical analysis
The statistical analysis and figures’ preparation were performed using GraphPad Prism 7 software. The Shapiro-Wilk normality test was applied to choose the comparative tests between groups. These comparative tests were also applied according to the group numbers and being paired or non-paired; all indicated in figure legends. Correlations were tested using the Spearman rho test. Any difference between the groups was considered as statistically significant when the p value < 0.05.
Data availability
The datasets supporting the conclusions of this study are included within the article and its additional supporting file.
References
Mills, L. A., Aitken, S. A. & Simpson, A. The risk of non-union per fracture: current myths and revised figures from a population of over 4 million adults. Acta orthopaedica 88, 434–439, https://doi.org/10.1080/17453674.2017.1321351 (2017).
Kanakaris, N. K. & Giannoudis, P. V. The health economics of the treatment of long-bone non-unions. Injury 38(Suppl 2), S77–84 (2007).
Zeckey, C. et al. The aseptic femoral and tibial shaft non-union in healthy patients - an analysis of the health-related quality of life and the socioeconomic outcome. Open Orthop J 5, 193–197, https://doi.org/10.2174/1874325001105010193 (2011).
Antonova, E., Le, T. K., Burge, R. & Mershon, J. Tibia shaft fractures: costly burden of nonunions. BMC Musculoskelet. Disord. 14, 42 (2013).
Panteli, M., Pountos, I., Jones, E. & Giannoudis, P. V. Biological and molecular profile of fracture non‐union tissue: current insights. Journal of cellular and molecular medicine 19, 685–713 (2015).
Sahu, R. L. Percutaneous autogenous bone marrow injection for delayed union or non-union of long bone fractures after internal fixation. Rev Bras Ortop 53, 668–673, https://doi.org/10.1016/j.rboe.2017.09.004 (2018).
Gross, J. B. et al. Percutaneous autologous bone marrow injection for treatment of delayed and non-union of long bone: a retrospective study of 45 cases. Biomed Mater Eng 25, 187–197, https://doi.org/10.3233/BME-141235 (2015).
Li, G. & Liu, Z. Treatment of long bone fracture nonunion in limbs by bone morphogenetic protein compounds combined with autologous red bone marrow graft. Zhongguo Gu Shang 26, 277–280 (2013).
Sir, M., Prochazka, V., Gumulec, J. & Pleva, L. Our first experiences with autologous transplantation of bone marrow stem cells to treat pseudarthrosis, delayed fracture healing and long bone defects fracture. Vnitr Lek 55, 187–189 (2009).
Giannoudis, P. V., Einhorn, T. A. & Marsh, D. Fracture healing: the diamond concept. Injury 38(Suppl 4), S3–6 (2007).
Schell, H. et al. The haematoma and its role in bone healing. J Exp Orthop 4, 5, https://doi.org/10.1186/s40634-017-0079-3 (2017).
Oe, K. et al. An in vitro study demonstrating that haematomas found at the site of human fractures contain progenitor cells with multilineage capacity. The Journal of bone and joint surgery. British volume 89, 133–138, https://doi.org/10.1302/0301-620X.89B1.18286 (2007).
Yellowley, C. CXCL12/CXCR4 signaling and other recruitment and homing pathways in fracture repair. Bonekey Rep 2, 300, https://doi.org/10.1038/bonekey.2013.34 (2013).
Oryan, A., Kamali, A., Moshiri, A. & Baghaban Eslaminejad, M. Role of Mesenchymal Stem Cells in Bone Regenerative Medicine: What Is the Evidence? Cells Tissues Organs 204, 59–83, https://doi.org/10.1159/000469704 (2017).
Kolar, P. et al. The early fracture hematoma and its potential role in fracture healing. Tissue Eng Part B Rev 16, 427–434, https://doi.org/10.1089/ten.TEB.2009.0687 (2010).
Schmidt-Bleek, K. et al. Inflammatory phase of bone healing initiates the regenerative healing cascade. Cell and tissue research 347, 567–573, https://doi.org/10.1007/s00441-011-1205-7 (2012).
Hoff, P. et al. Human immune cells’ behavior and survival under bioenergetically restricted conditions in an in vitro fracture hematoma model. Cellular & molecular immunology 10, 151–158, https://doi.org/10.1038/cmi.2012.56 (2013).
Konnecke, I. et al. T and B cells participate in bone repair by infiltrating the fracture callus in a two-wave fashion. Bone 64, 155–165, https://doi.org/10.1016/j.bone.2014.03.052 (2014).
Gibon, E., Lu, L. & Goodman, S. B. Aging, inflammation, stem cells, and bone healing. Stem Cell Res Ther 7, 44, https://doi.org/10.1186/s13287-016-0300-9 (2016).
Kovach, T. K., Dighe, A. S., Lobo, P. I. & Cui, Q. Interactions between MSCs and immune cells: implications for bone healing. J Immunol Res 2015, 752510, https://doi.org/10.1155/2015/752510 (2015).
Lienau, J. et al. Insight into the molecular pathophysiology of delayed bone healing in a sheep model. Tissue engineering. Part A 16, 191–199, https://doi.org/10.1089/ten.TEA.2009.0187 (2010).
Hoff, P. et al. Immunologically restricted patients exhibit a pronounced inflammation and inadequate response to hypoxia in fracture hematomas. Immunol Res 51, 116–122, https://doi.org/10.1007/s12026-011-8235-9 (2011).
El-Jawhari, J. J., Jones, E. & Giannoudis, P. V. The roles of immune cells in bone healing; what we know, do not know and future perspectives. Injury 47, 2399–2406, https://doi.org/10.1016/j.injury.2016.10.008 (2016).
Li, T. et al. Impact of bone marrow mesenchymal stem cell immunomodulation on the osteogenic effects of laponite. Stem Cell Res Ther 9, 100, https://doi.org/10.1186/s13287-018-0818-0 (2018).
Granero-Molto, F. et al. Regenerative effects of transplanted mesenchymal stem cells in fracture healing. Stem Cells 27, 1887–1898, https://doi.org/10.1002/stem.103 (2009).
Sui, B. D. et al. Gender-independent efficacy of mesenchymal stem cell therapy in sex hormone-deficient bone loss via immunosuppression and resident stem cell recovery. Experimental & molecular medicine 50, 166, https://doi.org/10.1038/s12276-018-0192-0 (2018).
Rutkovskiy, A., Stenslokken, K. O. & Vaage, I. J. Osteoblast Differentiation at a Glance. Med Sci Monit Basic Res 22, 95–106 (2016).
Katagiri, W. et al. Angiogenesis in newly regenerated bone by secretomes of human mesenchymal stem cells. Maxillofac Plast Reconstr Surg 39, 8, https://doi.org/10.1186/s40902-017-0106-4 (2017).
James, S. et al. Multiparameter Analysis of Human Bone Marrow Stromal Cells Identifies Distinct Immunomodulatory and Differentiation-Competent Subtypes. Stem Cell Reports 4, 1004–1015, https://doi.org/10.1016/j.stemcr.2015.05.005 (2015).
Yoo, S. H. et al. BST2 Mediates Osteoblast Differentiation via the BMP2 Signaling Pathway in Human Alveolar-Derived Bone Marrow Stromal Cells. PloS one 11, e0158481, https://doi.org/10.1371/journal.pone.0158481 (2016).
El-Sherbiny, Y. M., El-Jawhari, J. J., Moseley, T. A., McGonagle, D. & Jones, E. T cell immunomodulation by clinically used allogeneic human cancellous bone fragments: a potential novel immunotherapy tool. Sci Rep 8, 13535, https://doi.org/10.1038/s41598-018-31979-1 (2018).
Panteli, M., Pountos, I., Jones, E. & Giannoudis, P. V. Biological and molecular profile of fracture non-union tissue: current insights. Journal of cellular and molecular medicine 19, 685–713, https://doi.org/10.1111/jcmm.12532 (2015).
Fajardo, M., Liu, C. J. & Egol, K. Levels of expression for BMP-7 and several BMP antagonists may play an integral role in a fracture nonunion: a pilot study. Clinical orthopaedics and related research 467, 3071–3078, https://doi.org/10.1007/s11999-009-0981-9 (2009).
Kwong, F. N., Hoyland, J. A., Freemont, A. J. & Evans, C. H. Altered relative expression of BMPs and BMP inhibitors in cartilaginous areas of human fractures progressing towards nonunion. Journal of orthopaedic research: official publication of the Orthopaedic Research Society 27, 752–757, https://doi.org/10.1002/jor.20794 (2009).
Hofmann, A. et al. Cell viability, osteoblast differentiation, and gene expression are altered in human osteoblasts from hypertrophic fracture non-unions. Bone 42, 894–906, https://doi.org/10.1016/j.bone.2008.01.013 (2008).
Bajada, S., Marshall, M. J., Wright, K. T., Richardson, J. B. & Johnson, W. E. Decreased osteogenesis, increased cell senescence and elevated Dickkopf-1 secretion in human fracture non union stromal cells. Bone 45, 726–735, https://doi.org/10.1016/j.bone.2009.06.015 (2009).
Iwakura, T. et al. Human hypertrophic nonunion tissue contains mesenchymal progenitor cells with multilineage capacity in vitro. Journal of orthopaedic research: official publication of the Orthopaedic Research Society 27, 208–215, https://doi.org/10.1002/jor.20739 (2009).
Koga, T. et al. Effect of low-intensity pulsed ultrasound on bone morphogenetic protein 7-induced osteogenic differentiation of human nonunion tissue-derived cells in vitro. J Ultrasound Med 32, 915–922, https://doi.org/10.7863/ultra.32.6.915 (2013).
Seebach, C., Henrich, D., Tewksbury, R., Wilhelm, K. & Marzi, I. Number and proliferative capacity of human mesenchymal stem cells are modulated positively in multiple trauma patients and negatively in atrophic nonunions. Calcified tissue international 80, 294–300, https://doi.org/10.1007/s00223-007-9020-6 (2007).
Churchman, S. M. et al. Yield optimisation and molecular characterisation of uncultured CD271+ mesenchymal stem cells in the Reamer Irrigator Aspirator waste bag. European cells &. materials 26, 252–262 (2013).
Dilogo, I. H., Phedy Phedy, E. K., Djaja, Y. P., Kusnadi, Y. & Sandhow, L. Osteogenic potency of human bone marrow mesenchymal stem cells from femoral atrophic non-union fracture site. Journal of Clinical and Experimental Investigation 5, 159–163, https://doi.org/10.5799/ahinjs.01.2014.02.0382 (2014).
Qu, G. & von Schroeder, H. P. The osteogenic potential of pseudoarthrosis tissue and bone from human scaphoid non-unions. J Hand Surg Eur Vol 33, 449–456, https://doi.org/10.1177/1753193408090122 (2008).
El-Jawhari, J. J., Cuthbert, R., McGonagle, D., Jones, E. & Giannoudis, P. V. The CD45lowCD271high Cell Prevalence in Bone Marrow Samples May Provide a Useful Measurement of the Bone Marrow Quality for Cartilage and Bone Regenerative Therapy. The Journal of bone and joint surgery. American volume 99, 1305–1313, https://doi.org/10.2106/JBJS.16.01138 (2017).
Jones, E. et al. Large-scale extraction and characterization of CD271+ multipotential stromal cells from trabecular bone in health and osteoarthritis: implications for bone regeneration strategies based on uncultured or minimally cultured multipotential stromal cells. Arthritis Rheum 62, 1944–1954 (2010).
Cox, G. et al. High abundance of CD271(+) multipotential stromal cells (MSCs) in intramedullary cavities of long bones. Bone 50, 510–517, https://doi.org/10.1016/j.bone.2011.07.016 (2012).
Cuthbert, R. J. et al. Examining the feasibility of clinical grade CD271+ enrichment of mesenchymal stromal cells for bone regeneration. PloS one 10, e0117855, https://doi.org/10.1371/journal.pone.0117855 (2015).
Dominici, M. et al. Minimal criteria for defining multipotent mesenchymal stromal cells. The International Society for Cellular Therapy position statement. Cytotherapy 8, 315–317, https://doi.org/10.1080/14653240600855905 (2006).
El-Jawhari, J. J., Moisley, K., Jones, E. & Giannoudis, P. V. A crosslinked collagen membrane versus a non-crosslinked bilayer collagen membrane for supporting osteogenic functions of human bone marrow-multipotent stromal cells. European cells & materials 37, 292–309, https://doi.org/10.22203/eCM.v037a18 (2019).
Quarto, R. et al. Repair of large bone defects with the use of autologous bone marrow stromal cells. The New England journal of medicine 344, 385–386, https://doi.org/10.1056/NEJM200102013440516 (2001).
Ismail, H. D. et al. Mesenchymal stem cell implantation in atrophic nonunion of the long bones: A translational study. Bone Joint Res 5, 287–293, https://doi.org/10.1302/2046-3758.57.2000587 (2016).
Hernigou, P., Poignard, A., Beaujean, F. & Rouard, H. Percutaneous autologous bone-marrow grafting for nonunions. Influence of the number and concentration of progenitor cells. The Journal of bone and joint surgery. American volume 87, 1430–1437, https://doi.org/10.2106/JBJS.D.02215 (2005).
Hernigou, P. et al. Percutaneous injection of bone marrow mesenchymal stem cells for ankle non-unions decreases complications in patients with diabetes. International orthopaedics 39, 1639–1643, https://doi.org/10.1007/s00264-015-2738-2 (2015).
Boquest, A. C. et al. Isolation and transcription profiling of purified uncultured human stromal stem cells: alteration of gene expression after in vitro cell culture. Mol Biol Cell 16, 1131–1141, https://doi.org/10.1091/mbc.e04-10-0949 (2005).
Dahl, J. A. et al. Genetic and epigenetic instability of human bone marrow mesenchymal stem cells expanded in autologous serum or fetal bovine serum. Int J Dev Biol 52, 1033–1042, https://doi.org/10.1387/ijdb.082663jd (2008).
Tan, H. B., Giannoudis, P. V., Boxall, S. A., McGonagle, D. & Jones, E. The systemic influence of platelet-derived growth factors on bone marrow mesenchymal stem cells in fracture patients. BMC medicine 13, 6, https://doi.org/10.1186/s12916-014-0202-6 (2015).
Tamama, K., Fan, V. H., Griffith, L. G., Blair, H. C. & Wells, A. Epidermal growth factor as a candidate for ex vivo expansion of bone marrow-derived mesenchymal stem cells. Stem Cells 24, 686–695, https://doi.org/10.1634/stemcells.2005-0176 (2006).
Tsutsumi, S. et al. Retention of multilineage differentiation potential of mesenchymal cells during proliferation in response to FGF. Biochemical and biophysical research communications 288, 413–419, https://doi.org/10.1006/bbrc.2001.5777 (2001).
Ng, F. et al. PDGF, TGF-beta, and FGF signaling is important for differentiation and growth of mesenchymal stem cells (MSCs): transcriptional profiling can identify markers and signaling pathways important in differentiation of MSCs into adipogenic, chondrogenic, and osteogenic lineages. Blood 112, 295–307, https://doi.org/10.1182/blood-2007-07-103697 (2008).
Zhuang, Y. F. & Li, J. Serum EGF and NGF levels of patients with brain injury and limb fracture. Asian Pac J Trop Med 6, 383–386, https://doi.org/10.1016/S1995-7645(13)60043-7 (2013).
Bieback, K. et al. Human alternatives to fetal bovine serum for the expansion of mesenchymal stromal cells from bone marrow. Stem Cells 27, 2331–2341, https://doi.org/10.1002/stem.139 (2009).
Emami, A., Larsson, A., Petren-Mallmin, M. & Larsson, S. Serum bone markers after intramedullary fixed tibial fractures. Clinical orthopaedics and related research, 220–229 (1999).
Kurdy, N. M. Serology of abnormal fracture healing: the role of PIIINP, PICP, and BsALP. Journal of orthopaedic trauma 14, 48–53, https://doi.org/10.1097/00005131-200001000-00010 (2000).
Oni, O. O., Mahabir, J. P., Iqbal, S. J. & Gregg, P. J. Serum osteocalcin and total alkaline phosphatase levels as prognostic indicators in tibial shaft fractures. Injury 20, 37–38, https://doi.org/10.1016/0020-1383(89)90042-9 (1989).
Herrmann, M. et al. Different kinetics of bone markers in normal and delayed fracture healing of long bones. Clin Chem 48, 2263–2266 (2002).
Ohishi, T., Takahashi, M., Yamanashi, A., Suzuki, D. & Nagano, A. Sequential changes of bone metabolism in normal and delayed union of the spine. Clinical orthopaedics and related research 466, 402–410, https://doi.org/10.1007/s11999-007-0054-x (2008).
Moghaddam, A. et al. TRACP 5b and CTX as osteological markers of delayed fracture healing. Injury 42, 758–764, https://doi.org/10.1016/j.injury.2010.11.017 (2011).
Harty, M., Neff, A. W., King, M. W. & Mescher, A. L. Regeneration or scarring: an immunologic perspective. Dev Dyn 226, 268–279, https://doi.org/10.1002/dvdy.10239 (2003).
Toben, D. et al. Fracture healing is accelerated in the absence of the adaptive immune system. Journal of bone and mineral research: the official journal of the American Society for Bone and Mineral Research 26, 113–124, https://doi.org/10.1002/jbmr.185 (2011).
Hoff, P. et al. A Pronounced Inflammatory Activity Characterizes the Early Fracture Healing Phase in Immunologically Restricted Patients. International journal of molecular sciences, 18, https://doi.org/10.3390/ijms18030583 (2017).
Schmidt-Bleek, K. et al. Initial immune reaction and angiogenesis in bone healing. Journal of tissue engineering and regenerative medicine 8, 120–130, https://doi.org/10.1002/term.1505 (2014).
Zreiqat, H., Howlett, C. R., Gronthos, S., Hume, D. & Geczy, C. L. S100A8/S100A9 and their association with cartilage and bone. J Mol Histol 38, 381–391, https://doi.org/10.1007/s10735-007-9117-2 (2007).
Redondo-Castro, E. et al. Interleukin-1 primes human mesenchymal stem cells towards an anti-inflammatory and pro-trophic phenotype in vitro. Stem Cell Res Ther 8, 79, https://doi.org/10.1186/s13287-017-0531-4 (2017).
Ren, G. et al. Inflammatory cytokine-induced intercellular adhesion molecule-1 and vascular cell adhesion molecule-1 in mesenchymal stem cells are critical for immunosuppression. J Immunol 184, 2321–2328, https://doi.org/10.4049/jimmunol.0902023 (2010).
Mao, C. Y. et al. Double-edged-sword effect of IL-1beta on the osteogenesis of periodontal ligament stem cells via crosstalk between the NF-kappaB, MAPK and BMP/Smad signaling pathways. Cell death & disease 7, e2296, https://doi.org/10.1038/cddis.2016.204 (2016).
Gerstenfeld, L. C. et al. Impaired fracture healing in the absence of TNF-alpha signaling: the role of TNF-alpha in endochondral cartilage resorption. Journal of bone and mineral research: the official journal of the American Society for Bone and Mineral Research 18, 1584–1592, https://doi.org/10.1359/jbmr.2003.18.9.1584 (2003).
Gerstenfeld, L. C., Cullinane, D. M., Barnes, G. L., Graves, D. T. & Einhorn, T. A. Fracture healing as a post-natal developmental process: molecular, spatial, and temporal aspects of its regulation. Journal of cellular biochemistry 88, 873–884, https://doi.org/10.1002/jcb.10435 (2003).
Karnes, J. M., Daffner, S. D. & Watkins, C. M. Multiple roles of tumor necrosis factor-alpha in fracture healing. Bone 78, 87–93, https://doi.org/10.1016/j.bone.2015.05.001 (2015).
Haller, J. M., McFadden, M., Kubiak, E. N. & Higgins, T. F. Inflammatory cytokine response following acute tibial plateau fracture. The Journal of bone and joint surgery. American volume 97, 478–483, https://doi.org/10.2106/JBJS.N.00200 (2015).
Kokubu, T., Haudenschild, D. R., Moseley, T. A., Rose, L. & Reddi, A. H. Immunolocalization of IL-17A, IL-17B, and their receptors in chondrocytes during fracture healing. J Histochem Cytochem 56, 89–95, https://doi.org/10.1369/jhc.7A7223.2007 (2008).
Ono, T. et al. IL-17-producing gammadelta T cells enhance bone regeneration. Nature communications 7, 10928, https://doi.org/10.1038/ncomms10928 (2016).
Nam, D. et al. T-lymphocytes enable osteoblast maturation via IL-17F during the early phase of fracture repair. PloS one 7, e40044, https://doi.org/10.1371/journal.pone.0040044 (2012).
Takayanagi, H. Osteoimmunology: shared mechanisms and crosstalk between the immune and bone systems. Nat Rev Immunol 7, 292–304, https://doi.org/10.1038/nri2062 (2007).
Yang, A. et al. IL-8 Enhances Therapeutic Effects of BMSCs on Bone Regeneration via CXCR2-Mediated PI3k/Akt Signaling Pathway. Cell Physiol Biochem 48, 361–370, https://doi.org/10.1159/000491742 (2018).
Mathieu, M. et al. Decreased pool of mesenchymal stem cells is associated with altered chemokines serum levels in atrophic nonunion fractures. Bone 53, 391–398, https://doi.org/10.1016/j.bone.2013.01.005 (2013).
Moll, G. et al. Mesenchymal stromal cells engage complement and complement receptor bearing innate effector cells to modulate immune responses. PloS one 6, e21703, https://doi.org/10.1371/journal.pone.0021703 (2011).
Sarahrudi, K. et al. Elevated levels of macrophage colony-stimulating factor in human fracture healing. Journal of orthopaedic research: official publication of the Orthopaedic Research Society 28, 671–676, https://doi.org/10.1002/jor.21048 (2010).
Erices, A., Conget, P., Rojas, C. & Minguell, J. J. Gp130 activation by soluble interleukin-6 receptor/interleukin-6 enhances osteoblastic differentiation of human bone marrow-derived mesenchymal stem cells. Experimental cell research 280, 24–32, https://doi.org/10.1006/excr.2002.5627 (2002).
Pitaru, S., Kotev-Emeth, S., Noff, D., Kaffuler, S. & Savion, N. Effect of basic fibroblast growth factor on the growth and differentiation of adult stromal bone marrow cells: enhanced development of mineralized bone-like tissue in culture. Journal of bone and mineral research: the official journal of the American Society for Bone and Mineral Research 8, 919–929, https://doi.org/10.1002/jbmr.5650080804 (1993).
Zimmermann, G. et al. TGF-beta1 as a marker of delayed fracture healing. Bone 36, 779–785, https://doi.org/10.1016/j.bone.2005.02.011 (2005).
Westhauser, F. et al. Reaming in treatment of non-unions in long bones: cytokine expression course as a tool for evaluation of non-union therapy. Arch Orthop Trauma Surg 135, 1107–1116, https://doi.org/10.1007/s00402-015-2253-3 (2015).
Fischer, C. et al. Quantification of TGF-ss1, PDGF and IGF-1 cytokine expression after fracture treatment vs. non-union therapy via masquelet. Injury 47, 342–349, https://doi.org/10.1016/j.injury.2015.11.007 (2016).
Granchi, D. et al. Serum levels of fibroblast growth factor 2 in children with orthopedic diseases: potential role in predicting bone healing. Journal of orthopaedic research: official publication of the Orthopaedic Research Society 31, 249–256, https://doi.org/10.1002/jor.22219 (2013).
Weiss, S. et al. Systemic response of the GH/IGF-I axis in timely versus delayed fracture healing. Growth Horm IGF Res 18, 205–212, https://doi.org/10.1016/j.ghir.2007.09.002 (2008).
Sarahrudi, K. et al. VEGF serum concentrations in patients with long bone fractures: a comparison between impaired and normal fracture healing. Journal of orthopaedic research: official publication of the Orthopaedic Research Society 27, 1293–1297, https://doi.org/10.1002/jor.20906 (2009).
Wang, C. J. et al. The effects of shockwave on bone healing and systemic concentrations of nitric oxide (NO), TGF-beta1, VEGF and BMP-2 in long bone non-unions. Nitric Oxide 20, 298–303, https://doi.org/10.1016/j.niox.2009.02.006 (2009).
van Baardewijk, L. J. et al. Circulating bone morphogenetic protein levels and delayed fracture healing. International orthopaedics 37, 523–527, https://doi.org/10.1007/s00264-012-1750-z (2013).
Niikura, T., Hak, D. J. & Reddi, A. H. Global gene profiling reveals a downregulation of BMP gene expression in experimental atrophic nonunions compared to standard healing fractures. Journal of orthopaedic research: official publication of the Orthopaedic Research Society 24, 1463–1471, https://doi.org/10.1002/jor.20182 (2006).
Tchetverikov, I. et al. MMP profile in paired serum and synovial fluid samples of patients with rheumatoid arthritis. Annals of the rheumatic diseases 63, 881–883, https://doi.org/10.1136/ard.2003.013243 (2004).
Henle, P., Zimmermann, G. & Weiss, S. Matrix metalloproteinases and failed fracture healing. Bone 37, 791–798, https://doi.org/10.1016/j.bone.2005.06.015 (2005).
Wang, S. et al. S100A8/A9 in Inflammation. Frontiers in immunology 9, 1298, https://doi.org/10.3389/fimmu.2018.01298 (2018).
de Seny, D. et al. Biomarkers of inflammation and innate immunity in atrophic nonunion fracture. Journal of translational medicine 14, 258, https://doi.org/10.1186/s12967-016-1019-1 (2016).
van’t Hof, R. J. & Ralston, S. H. Nitric oxide and bone. Immunology 103, 255–261, https://doi.org/10.1046/j.1365-2567.2001.01261.x (2001).
Rupp, M. et al. Do Systemic Factors Influence the Fate of Nonunions to Become Atrophic? A Retrospective Analysis of 162 Cases. Biomed Res Int 2019, 6407098, https://doi.org/10.1155/2019/6407098 (2019).
Hernigou, P. et al. Benefits of small volume and small syringe for bone marrow aspirations of mesenchymal stem cells. International orthopaedics 37, 2279–2287, https://doi.org/10.1007/s00264-013-2017-z (2013).
Fragkakis, E. M. et al. Vertebral body versus iliac crest bone marrow as a source of multipotential stromal cells: Comparison of processing techniques, tri-lineage differentiation and application on a scaffold for spine fusion. PloS one 13, e0197969, https://doi.org/10.1371/journal.pone.0197969 (2018).
El-Zayadi, A. A. et al. Interleukin-22 drives the proliferation, migration and osteogenic differentiation of mesenchymal stem cells: a novel cytokine that could contribute to new bone formation in spondyloarthropathies. Rheumatology (Oxford) 56, 488–493, https://doi.org/10.1093/rheumatology/kew384 (2017).
Huang, H. et al. IL-17 stimulates the proliferation and differentiation of human mesenchymal stem cells: implications for bone remodeling. Cell Death Differ 16, 1332–1343, https://doi.org/10.1038/cdd.2009.74 (2009).
Pourgholaminejad, A., Aghdami, N., Baharvand, H. & Moazzeni, S. M. The effect of pro-inflammatory cytokines on immunophenotype, differentiation capacity and immunomodulatory functions of human mesenchymal stem cells. Cytokine 85, 51–60, https://doi.org/10.1016/j.cyto.2016.06.003 (2016).
El-Jawhari, J. J., Sanjurjo-Rodriguez, C., Jones, E. & Giannoudis, P. V. Collagen-containing scaffolds enhance attachment and proliferation of non-cultured bone marrow multipotential stromal cells. Journal of orthopaedic research: official publication of the Orthopaedic Research Society, https://doi.org/10.1002/jor.23070 (2015).
Bower, N. I., Moser, R. J., Hill, J. R. & Lehnert, S. A. Universal reference method for real-time PCR gene expression analysis of preimplantation embryos. Biotechniques 42, 199–206, https://doi.org/10.2144/000112314 (2007).
Lotfi, R. et al. ATP promotes immunosuppressive capacities of mesenchymal stromal cells by enhancing the expression of indoleamine dioxygenase. Immun Inflamm Dis 6, 448–455, https://doi.org/10.1002/iid3.236 (2018).
Guan, Q., Li, Y., Shpiruk, T., Bhagwat, S. & Wall, D. A. Inducible indoleamine 2,3-dioxygenase 1 and programmed death ligand 1 expression as the potency marker for mesenchymal stromal cells. Cytotherapy 20, 639–649, https://doi.org/10.1016/j.jcyt.2018.02.003 (2018).
Niu, J., Yue, W., Le-Le, Z., Bin, L. & Hu, X. Mesenchymal stem cells inhibit T cell activation by releasing TGF-beta1 from TGF-beta1/GARP complex. Oncotarget 8, 99784–99800, https://doi.org/10.18632/oncotarget.21549 (2017).
Tuck, M. K. et al. Standard operating procedures for serum and plasma collection: early detection research network consensus statement standard operating procedure integration working group. Journal of proteome research 8, 113–117, https://doi.org/10.1021/pr800545q (2009).
Acknowledgements
We would like to thank all the team of the Academic unit of Trauma and Orthopaedic Surgery, Leeds General Infirmary for their collaboration and help with the sample collection. This study was funded by the AO foundation Start-Up grant: S-16-132E.
Author information
Authors and Affiliations
Contributions
Conceptualization: J.J.E., E.J., R.W., P.V.G.; Formal analysis and investigation: J.J.E., Y.E.; Writing: J.J.E., G.K., Y.E., H.S., E.J., R.W. and P.V.G.; Samples/Resources: J.J.E., G.K., H.S. and P.V.G. All authors read and approved the final manuscript.
Corresponding author
Ethics declarations
Competing interests
The authors declare no competing interests.
Additional information
Publisher’s note Springer Nature remains neutral with regard to jurisdictional claims in published maps and institutional affiliations.
Supplementary information
Rights and permissions
Open Access This article is licensed under a Creative Commons Attribution 4.0 International License, which permits use, sharing, adaptation, distribution and reproduction in any medium or format, as long as you give appropriate credit to the original author(s) and the source, provide a link to the Creative Commons license, and indicate if changes were made. The images or other third party material in this article are included in the article’s Creative Commons license, unless indicated otherwise in a credit line to the material. If material is not included in the article’s Creative Commons license and your intended use is not permitted by statutory regulation or exceeds the permitted use, you will need to obtain permission directly from the copyright holder. To view a copy of this license, visit http://creativecommons.org/licenses/by/4.0/.
About this article
Cite this article
El-Jawhari, J.J., Kleftouris, G., El-Sherbiny, Y. et al. Defective Proliferation and Osteogenic Potential with Altered Immunoregulatory phenotype of Native Bone marrow-Multipotential Stromal Cells in Atrophic Fracture Non-Union. Sci Rep 9, 17340 (2019). https://doi.org/10.1038/s41598-019-53927-3
Received:
Accepted:
Published:
DOI: https://doi.org/10.1038/s41598-019-53927-3
- Springer Nature Limited
This article is cited by
-
Efficacy of adjuvant treatment for fracture nonunion/delayed union: a network meta-analysis of randomized controlled trials
BMC Musculoskeletal Disorders (2022)
-
Evaluation of the effect of preoperative hemoglobin level and proinflammatory factors on intertrochanteric fracture union
Wiener klinische Wochenschrift (2022)