Abstract
The current outbreak of COVID-19 cases worldwide has been responsible for a significant number of deaths, especially in hospitalized patients suffering from comorbidities, such as obesity, diabetes, hypertension. The disease not only has prompted an interest in the pathophysiology, but also it has propelled a massive race to find new anti-SARS-CoV-2 drugs. In this scenario, known drugs commonly used to treat other diseases have been suggested as alternative or complementary therapeutics. Herein we propose the use of sitagliptin, an inhibitor of dipeptidyl peptidase-4 (DPP4) used to treat type-II diabetes, as an agent to block and inhibit the activity of two proteases, 3CLpro and PLpro, related to the processing of SARS-CoV-2 structural proteins. Inhibition of these proteases may possibly reduce the viral load and infection on the host by hampering the synthesis of new viruses, thus promoting a better outcome. In silico assays consisting in the modeling of the ligand sitagliptin and evaluation of its capacity to interact with 3CLpro and PLpro through the prediction of the ligand bioactivity, molecular docking, overlapping of crystal structures, and molecular dynamic simulations were conducted. The experiments indicate that sitagliptin can interact and bind to both targets. However, this interaction seems to be stronger and more stable to 3CLpro (ΔG = −7.8 kcal mol−1), when compared to PLpro (ΔG = −7.5 kcal mol−1). This study suggests that sitagliptin may be suitable to treat COVID-19 patients, beyond its common use as an anti-diabetic medication. In vivo studies may further support this hypothesis.
Similar content being viewed by others
Avoid common mistakes on your manuscript.
Introduction
The 2019 coronavirus disease (COVID-19) was first reported in Wuhan, China, and it is caused by a novel β-Coronavirus, a zoonotic emerging pathogen identified in 2019. Systemic complications associated with COVID-19 disease, usually involve gastrointestinal infections, renal injury, heart failure (Amaral et al. 2022), leading to a relatively high mortality rate. Since the clinical manifestations of this disease resemble those caused by the classic SARS-CoV virus, the new pathogen was named SARS-CoV-2. COVID-19 has been reported as the most devastating outbreak known to humans to date being responsible (Singh et al. 2021, 2022), only in Brazil, for a total of 683,965 deaths (https://covid.saude.gov.br/), until August 2022.
All CoVs are featured by a positive single-stranded RNA (Freire et al. 2020), and the increased lethality of this group is partly related to the presence of a high mutation rate due to their propensity to errors during the replication. In addition, it has been shown that during the infection, a mixture of different CoVs viral strains commonly causes an RNA homologous recombination of around 20% (Denison et al. 2011), which is assumed to explain the high tropism and pathogenicity the virus presents to the host (Cui et al. 2019).
Most CoVs, including SARS-CoV-2, use the C-terminal domain (CTD) of S1 subunit of the glycoprotein spike to bind to the angiotensin-converting enzyme 2 (ACE2). The high affinity of the CTD to ACE2 induces the virus-cell fusion (Huang et al. 2020) that later may result in serious organic disorders or death. SARS-CoV-2 is also capable to bind and interact with the transmembrane protease DPP4/CD26 (dipeptidyl peptidase 4), and this has been proposed as an alternative pathway the virus may use to enter the host cell (Li et al. 2020). DPP4 functions as a chemical modulator for several other molecules, such as cytokines, chemokines and growth factors, and some studies have reported that a high incidence of mortality and complications in diabetic patients suffering from MERS-CoV (a virus similar to SARS-CoV-2) infection may be related to dysregulated immune responses mediated by the DPP4 (Li et al. 2017; Fan et al. 2018).
Gliptins are a class of oral antihyperglycemic agents with demonstrated efficacy in the treatment of type-II diabetes (Scheen 2013) acting as DPP4 inhibitors (iDPP4). Sitagliptin is a member of the gliptin family that beyond its anti-diabetic effects presents low cardiovascular risks (Green et al. 2015; Yoshikawa et al. 2020). Considering that DPP4 is an additional receptor which SARS-CoV-2 may recognize to enter the host cells, we propose that an iDPP4, as sitagliptin, may act as an antiviral drug. In fact, a recent paper has shown that sitagliptin significantly reduced SARS-CoV-2 titer in cell culture supernatants from infected cells (Narayanan et al. 2022).
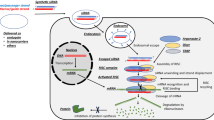
Once inside the cell SARS-CoV-2 uses two key proteases, a chymotrypsin-like protease (3CLpro), and a papain-like protease (PLpro), to process the precursors of its 16 non-structural proteins (NSPs) (Yilmaz et al. 2020; Ravi et al. 2022; Yavarian et al. 2022), by a cascade of cleavage process as schematized in Fig. 1. Thus, the roles of 3CLpro and PLpro are of critical importance to the successful of the viral infection, making these proteases important targets to antiviral drugs addressing to SARS-CoV-2.
Synthesis of non-structural proteins (NSPs) and post-translational modification mechanisms of SARS-CoV-2 virus. Stage 1: after recognition of the ACE2 and/or DPP4 cell receptors, the viral nucleocapsid is released into the cytoplasm by endocytosis, or fusion of the viral envelope, with the cell membrane. Stage 2: the translation of the pp1a and pp1b genes results in the synthesis of pp1a or pp1ab polyproteins, the latter being generated by a −1 frameshift of ribosomes. These polyproteins are then cleaved by viral 3CLpro and PLpro proteases generating 16 virus NSPs, including the RNA-dependent RNA polymerase (RdRp or NSP12)
The discovery and development of drugs against any disease or a target is a cumbersome and time-demanding task. On the other hand, as observed in several cases around the world, many clinical professionals have reported the use of the repositioning approach (off label treatment) to treat COVID-19 patients (Abd-Elsalam et al. 2021; Kashour et al. 2021; Amaral et al. 2022); therefore, the aim of this work was to carried out a detailed in silico analysis to evaluate the potential of the molecule sitagliptin as bifunctional candidate to be used as a new anti-SARS-CoV-2 drug targeting not only the human DPP4, but also the 3CLpro and PLpro SARS-CoV-2 proteases.
Methods
Domain analysis and linker prediction of the target receptors
The structures and amino acid sequences of the papain-like protease PLpro from SARS-CoV (Ratia et al. 2006) and chymotrypsin-like protease - 3CLpro (Su et al. 2020) from SARS-CoV-2 (Accession PDB IDs: 2FE8 and 6M2N, respectively) were downloaded in.pdb and.fasta formats from the Protein Data Bank (Burley et al. 2021). In order to identify possible boundary domains as well as to predict linker sequences, the amino acids sequences of PLpro and 3CLpro were submitted to the following servers: Database of Protein Domains, Families and Functional Sites - Prosite (Sigrist et al. 2012), Conserved Domains Database and Resources - CDD (Lu et al. 2020), and Classification of Protein Families - InterPro (Blum et al. 2021). The algorithms employed by FTSite (Ngan et al. 2012), FTMap (Kozakov et al. 2015), and CASTp (Tian et al. 2018) servers were used to identify the interaction regions (hotspots).
Ligand design, bioactivity prediction, and molecular docking studies
The structure of the ligand (sitagliptin) was designed with the software MarvinSketch 6.2.2 (ChemAxon - http://www.Chemaxon.com/products/marvin/marvinsketch/). The output file was submitted to Molinspiration Virtual Screening (www.molinspiration.com) and ChEMBL (Mendez et al. 2019) servers to calculate the molecular properties and bioactivity score of sitagliptin.
Docking simulations were conducted with the AutoDock Vina software v. 1.1.2 (Trott and Olson 2010). Initially, in order to validate our molecular docking, site-directed redocking simulations were carried out under conditions where all the torsion connections of the ligand and amino acids present in the catalytic site of the receptor were free to rotate. All hydrogen polar atoms were previously added to the receptor and then parameterized with Gasteiger charges. The ligand was prepared by addition of Kollman charges. The simulation has been performed in the following conditions: number of conformations = 50, exhaustiveness = 33, and seed = 1000. The dimensions of the boxes in all cases were: X = 58 Å, Y = 80 Å, and Z = 62 Å. The crystal structure (PDB ID: 6M2N) of 3CLpro co-crystallized with the ligand baicalein was used for this challenge. Afterward, simulations employing the same strategy were performed using the ligand and the crystal structures of both the PLpro and 3CLpro as targets. Predictions made by CASTp, FTMap, and FTSite servers were also used to determine the selected sites in PLpro and 3CLpro proteases for the molecular docking simulations.
All torsional bonds of the ligand (sitagliptin) were free to rotate, whereas the PLpro protease was held rigid except for the amino acids Trp107, Asp109, Cys112, Tyr113, Cys163, Gly164, Tyr265, Tyr269, Gln270, Cys271, His273, Tyr274, and Asp287. Similarly, the amino acids from 3CLpro protease (Thr25, Thr26, Leu27, Arg40, His41, Val42, Ser46, Met49, Asn142, Gly143, Ser144, Cys145, His163, His164, Glu166, and Gln189) were kept free to rotate. The following coordinates: X = −20.941, Y = 50.041, and Z = −2.974 to the PLpro, and X = 115. 371, Y = −17.804, and Z = 62.399 to the 3CLpro were used based on the predicted hotspots.
Molecular dynamics simulation and schematic representations
Sitagliptin-PLpro and sitagliptin-3CLpro complexes presenting the lowest binding energy according to docking simulations were submitted to stability tests by MD analysis using the GROMACS package, version 2019.5 (Abraham et al. 2015). The electroneutrality of both complexes was maintained by adding Na+ ions in the required amounts. System solvation was conducted using SPC/E (extended simple point charge model) water molecules in a periodic box (90 × 90 × 90 nm3 volume) containing buffer to enable substantial fluctuations of the conformation during MD simulations. MD simulations were performed using the GROMOS 54a7 force field, a force field recently developed from three previous force fields (GROMOS 45A3, 53A6, and 54A7), and validated to simulate the folding equilibrium of β-peptides (as in the case of sitagliptin). The energy minimization (2000 steps steepest descent followed by 200-ps-long MD simulation) was performed before initiating MD simulations to remove initial steric clashes. MD simulations were performed under constant pressure using anisotropic diagonal position scaling with a time step of 0.002 ps. The electrostatic interactions were assessed based on the principle of PME (Particle Mesh Ewald) previously defined with short-range cutoffs of 1.2 nm (Essmann et al. 1995). The temperature of the system was parameterized to gradually increase from 100 up to 310 K at 1 bar pressure in 1000 ps. The Berendsen weak-coupling algorithm (Berendsen et al. 1984) with a constant time of 0.2 ps was used. The LINCS algorithm (Hess 2008) was used to constrain the equilibrium distances between all bonds allowing only internal motions of bending and torsion during MD simulations. Finally, the 25-ns MD simulations were performed under the same conditions as the equilibration procedure.
Two-dimensional representations of the best ligand–protein complexes based on the theoretical binding energy value were generated using the ProteinsPlus server (Schöning-Stierand et al. 2020). The software PyMol Molecular Graphics System, version 1.7.4 (Schrodinger, LLC), and the Protein–Ligand Interaction Profiler server (Adasme et al. 2021) were used to build the three-dimensional structures.
Results
Domain analysis and linker prediction of the target receptors
CDD-based annotation data showed that PLpro belongs to the conserved protein domain family CoV- NSP3, also called β-Coronavirus non-structural protein 3, whereas 3CLpro is a member of the conserved protein domain family CoV-NSP5-Mpro, also called β-Coronavirus non-structural protein 5, or Main protease (Mpro). The analyses of the CDD-based annotation to PLpro and 3CLpro showed predictions with confidence indices in accordance with data previously presented: E-value (208−177, and 000), Bit-Score (492.10, and 565.11), and interval (4 to 306, and 4 to 300 amino acids residues), respectively. All data reported above are in agreement with the predictions obtained by Prosite and InterPro servers. Mapping based of binding hotspots data showed that PLpro presents only one organic probe cluster (site1), whereas for the 3CLpro the results suggest the existence of four organic probe clusters (site1, site2, site3, and site4). The position of the interaction sites on both receptors identified here (PLpro and 3CLpro) did not differ from those previously reported (Abdizadeh et al. 2022; Zhao et al. 2022).
Ligand bioactivity prediction
In silico predictions of sitagliptin bioactivity using Molinspiration Virtual Screening provided a score of 0.56, suggesting that this ligand can inhibit a broad range of proteases. In addition, the analysis returned a score of 0.25 which suggests that sitagliptin can bind to the G protein-coupled receptors (GPCR), while presented a reduced inhibitory activity against kinases, score of 0.01. The bioactivity of the whole ligand is predicted as the sum of the bioactivity scores of all individual fragments (a number typically ranging from -3 to 3). The results obtained from the ChEMBL server, indicated a significative pharmacological activity against the human DPP4, as indicated by confidence score values of 70%, 80%, and 90%, with a threshold value of 6. Furthermore, the analyses also suggested a probable interaction between sitagliptin and the viral proteins: Human Immunodeficiency virus - 1 integrase, and the RNA-dependent RNA polymerase from Hepatitis C virus NS5B, as showed by a confidence score value of 90%, also determined by a threshold value of 6 (Table 1).
Molecular docking studies and Molecular Dynamics
Molecular docking and molecular dynamics study: PLpro and 3CLpro proteases and the ligand sitagliptin
A total of 20 simulations (molecular docking) were performed for both systems: PLpro-sitagliptin and 3CLpro-sitagliptin. Molecular docking experiments for PLpro-sitagliptin and 3CLpro-sitagliptin returned best performance ΔG = −7.5 and ΔG = −7.8 kcal mol−1, respectively. It is important to note that ΔG values represent the combined result of the van der Waals dispersive and electrostatic interaction energy which indicates the approximate binding energy between ligand and receptor.
Molecular dynamics (MD) analysis demonstrated that some amino acids of the active site of PLpro and 3CLpro were capable to interact with sitagliptin, keeping a maximum distance of ligation of around 4.0 Å. After MD has been finalized, around 53.8% of PLpro amino acid residues that were kept flexible during docking simulations (Trp107, Cys112, Tyr113, Gly164, Gln270, His273, and Asp287) interacted with sitagliptin. From all the residues that were allowed to be flexible in 3CLpro (Thr26, His41, Gly143, Cys145, His163, Glu166, and Gln189), 43% showed some interaction with the ligand (Figs. 2a, b, 3a, b). The MD results show that both PLpro-sitagliptin and 3CLpro-sitagliptin complexes encompass a network characterized by the presence of charge and aromatic ring centers, hydrophobic interactions, hydrogen bonds, and π-cation (Figs. 2c, d, 3c, d, and Supplementary materials 1 and 2).
Three putative hotspots were detected in the PLpro receptor (PDB ID: 2FE8) using the CASTp 3.0, FTSite, and FTMap servers. a One cavity, which is the biggest, was called S1 (green color). b The predicted binding pocket of PLpro. c and d The 3D and 2D visualizations of the complex stablished by the interaction between PLpro amino acids and the sitagliptin ligand
Three putative hotspots were detected in the 3CLpro receptor (PDB id: 6M2Q) using the CASTp 3.0, FTSite, and FTMap servers. a One cavity, which is the biggest, was called S1 (magenta color), while the other three smaller cavities were called S2 (green color), S3 (salmon color), and S4 (slate color). b The predicted binding pocket of 3CLpro. c and d The 3D and 2D visualization and interaction within the amino acids of 3CLpro and ligand (sitagliptin) complex
Figure 4 compares the root-mean-square deviation (RMSD) and the radius of gyration (Rg) of PLpro and 3CLpro uncompleted or complexed with the ligand. A steady RMSD of around 0.2 nm during all the simulation time (25 ns) was observed for 3CLpro (Fig. 4c), while a slight variation on the stability of the PLpro-sitagliptin complex has been observed, especially in the range of 15–25 ns (Fig. 4a). This result suggests that, as a target, PLpro appears to have less affinity to sitagliptin than 3CLpro, despite both proteins had shown similar ligation energies with ΔG values of −7.8 and −7.5 kcal mol−1, for 3CLpro and PLpro, respectively. The variation on the Rg as a function of time of simulation was also a little different in both systems with the PLpro-sitagliptin complex displaying a profile that likely indicates a more compact and rigid folding of the target protein (Fig. 4b). In contrast, the 3Lpro-sitagliptin complex showed a more relaxed and favorable conformation which is observed by the tendency of increase in the Rg values when compared to the non-complexed (uncompleted) target, mainly at the final nanoseconds of the simulation (Fig. 4d). All together these results suggest that 3CLpro seemingly behaves as a better target for sitagliptin than PLpro which clearly displayed a less stable interaction.
Root-mean-square deviations (RMSD) of the backbone and radius of gyration (Rg) of the proteins from 25 ns long MD trajectory. a and c visualization of RMSD of PLpro and 3CLpro uncompleted (blue) and complexed (red). b and d visualization of Rg of PLpro and 3CLpro uncompleted (blue) and complexed (red)
Discussion
Pockets and cavities in receptors usually coincide with the active sites responsible for the biological processes; therefore, it is fundamental to pay close attention to them. The precise mapping of binding hotspots for macromolecules was determined for the catalytic pockets of SARS-CoV-2 PLpro and 3CLpro proteases, after the analysis of different positions with small organic molecules as probes. Canonically, hotspots are regions on the surface of a protein with the major contributions to the ligand binding free energy. The combination of the results obtained in our work revealed the presence of three “hotspots” in PLpro (Fig. 2a) and one “hotspot” in 3CLPro (Fig. 3a) as regions that can contribute to the ligand binding free energy (Gibbs free energy).
On the other hand, in silico prediction of sitagliptin ligand, using the Molinspiration Virtual Screening, indicated a bioactivity score of 0.56, suggesting that interactions between this ligand can occur with multiple proteases. As previously reported, sitagliptin appears to be a potent inhibitor of this group of enzymes (Chittepu et al. 2019; Abbas and Hegazy 2020; Solerte et al. 2020). Furthermore, the analysis with Molinspiration also suggested that sitagliptin has the ability (0.25) to bind to G protein-coupled receptors (GPCR) and poor capacity to inhibit protein kinases (0.01). Analysis using the ChEMBL server (Mendez et al. 2019) suggested a possible activity of sitagliptin against proteases belonging to two human viruses (Table 1). A previous study reported that the use of gliptins in the treatment of type-II diabetes attenuated the risk of several kind of infections including human viral infections (Yang et al. 2016). Based on the analysis presented by the ChEMBL server the sitagliptin was predicted to be able to bind and inhibit two viral proteins: an integrase from Immunodeficiency virus 1, and an RNA-dependent RNA polymerase from Hepatitis C virus NS5B, with a confidence score value of 90%, according to a confidence level greater than 30%. Other reports have demonstrated a correlation among sitagliptin, diabetes, and HIV infection (Best et al. 2015). Taking together these results are in agreement with our findings. In addition, the server showed that sitagliptin is also capable to bind and inhibit the human DPP4, as expected, as demonstrated by a confidence level greater than 30%.
Here, we show that the catalytic site of PLpro contains an active site formed by the classic catalytic triad (Cys112, His273, and Asp287) which are well conserved in terms of positioning and functionality at the interface of the thumb and palm sub-domains (Supplementary material 1). When the catalytic site of PLpro is not occupied by a ligand, the Cys112 is positioned at the N-terminal region of an α-helix α4 in the thumb domain with the side chain sulfur atom being stabilized at a 3.7 Å distance from the pros(π)-nitrogen atom of the His273. This histidine is located at the foot of the palm domain, near to the flexible loop BL2, also known as Gly267–Gly272 loop (Ratia et al. 2006) or β-turn (Báez-Santos et al. 2014). In contrast, one of the oxygen atoms of the side chain of Asp287 is located at a 2.7 Å distance from the tele(τ)-nitrogen of the His273 residue at the foot of the palm domain, while the side chain of Trp107 is buried inside the oxyanion hole. In addition, the indole-ring nitrogen of Trp107 seems to be pivotal for the stabilization of negatively charged tetrahedral intermediates produced throughout the reaction. Remarkably, in vitro experiments using PLpro protease inhibitors showed that those inhibitors were prone to interact and bind in a cavity next to the catalytic triad (Báez-Santos et al. 2014).
Our results suggest that SARS-CoV-2 protease PLpro can be a potential receptor for the sitagliptin ligand, as verified by the binding free energy of the interaction (ΔG = −7.5 kcal mol−1). The results point to a molecular mechanism of interaction by which sitagliptin forms a covalent adduct with PLpro protease through direct interaction with the Cys112 residue with high statistic confidence. The stable binding between the nitrile group of Cys112 and sitagliptin molecule would result in an inhibition of the PLpro activity (Supplementary material 2), thereby potentially inhibiting the natural pathway of SARS-CoV-2 replication. A number of compounds have been identified, using in silico approaches, as potential inhibitors of the PLpro catalytic site (Table 2), with Gibbs free energy ranging from −10.9 to − 6.5 kcal mol−1. Therefore, the Gibbs free energy obtained in our analysis is in agreement with previous analysis which used the PLpro protease as a ligand receptor. Different scientific approaches have demonstrated that negative functional implications of the innate immune response during SARS-CoV-2 infection can occur due to the presence of the PLpro. In so many cases, PLpro have been implicated in functions such as deubiquitinating (DUB) and deISGylating (deISG) during cellular infection by SARS-CoV-2, removing the ubiquitin (Ub) using a chemical mechanism similar to the ubiquitin-like protein ISG15–interferon-stimulated gene 15 (Clasman et al. 2020). Therefore, increasing pools of ISG15 are capable of modulation by downregulating USP18 (ubiquitin-specific protease 18) levels, resulting, in turn, in the upregulation of IFN-α/β exacerbated signaling in COVID-19 patients (Mielech et al. 2014; Speer et al. 2016; Moustaqil et al. 2021).
In addition, inhibition of the synthesis of cytokines involved in the activation of the host’s innate immune response against the SARS-CoV-2, and chemokines such as CCL5 and CXCL10, seems to be associated with the presence of PLpro (Báez-Santos et al. 2015). On the other hand, the increase in C-reactive protein (CRP) and inflammatory factors in the plasma, like the interleukins IL2, IL4, IL6, IL7, IL10, IL12, IL13, IL17, TNF-α, GCSF, MCSF, IP10, MCP1, MIP1α, and HGF can trigger a cytokine storm in the body of critical patients affected by SARS-CoV-2 (Guo et al. 2020; Prompetchara et al. 2020; Singhal, 2020; Zu et al. 2020). Therefore, the discovery of new therapeutics and/or drug repositioning approaches intended to inhibit the PLpro protease (SARS-CoV-2) are of great interest to prevent the emergence of new cases of COVID-19, since the number of cases grows up all over the world.
In addition to PLpro, SARS-CoV-2 3CLpro protease may also trigger some negative effects to the organism of infected patients such as the antagonization of IFN-stimulated response elements - ISRE (Wu et al. 2020; McGill et al. 2021; Moustaqil et al. 2021), cleavage of both the NF-kappa β essential modulator (NEMO), and the signal transducer and activator of transcription 2 - STAT2 (Fehr et al. 2016; Chen et al. 2019) resulting in the downregulation of IGSs, and the interaction with E3 ligase of tripartite motif-containing protein 25 - TRIM25 (Wu et al. 2020), and the interferon regulatory factor 3 - IRF3 (Moustaqil et al. 2021). Intriguingly, 3CLpro was also able to induce changes in the metabolism of the phosphorylation of IFN-mediated STAT1, resulting in metabolic damage due to a localized increase in the levels of autophagosomal membrane proteins - LC3B (Xia et al. 2020).
Furthermore, it was previously documented that 3CLpro is capable of inducing the cleavage of NLR family pyrin domain containing 12 (NLRP12) and TGF-β activated kinase 1 (MAP3K7) binding protein 1 (TAB1), as well as to induce an intense synthesis of cytokines and accentuated inflammatory response in SARS-CoV-2-infected patients (Moustaqil et al. 2021).
Analysis of the 3CLpro catalytic site showed a general topology quasi-ellipsoid due to the presence of three distinct domains (named domain I, domain II, and domain III), which are connected with flexible loops, being domains I and II related to the catalytic activity, and domain III to dimerization (Shi et al. 2004; Wang et al. 2020). The catalytic dyad His-Cys (His41 and Cys145) of 3CLpro, as previously reported in the literature (Yang et al. 2003; Das et al. 2020; Tahir ul Qamar et al. 2020), is located in a relatively shallow cavity between domains I and II defining the catalytic site (Supplementary material 3), to an optimum distance (at 3.6 Å) for hydrogen bonding interactions.
When the catalytic site of 3CLpro is not occupied by a ligand, the side chain sulfur atom of the Cys145 residue (Domain II) is located at a 3.6 Å distance from the tele(τ)-nitrogen atom of the His41 residue of the α-helix 2 (α2) of the sheet A (Domain I). Alternatively, the Glu166 residue also located in the Domain II is positioned at a distance in which the presence of two water molecules is necessary for the interaction with potential inhibitors of the 3CLpro (Table 3) catalytic site.
The binding free energy we encountered in our study suggests that SARS-CoV-2 3CLpro protease can be a potential receptor for sitagliptin (Supplementary material 4), with a ΔG = −7.8 kcal.mol−1. This result was nearly identical to what we found for PLpro protease (ΔG = −7.5 kcal mol−1). A list of compounds (Tables 2 and 3) has been identified, using in silico approaches, as potential good inhibitors for 3CLpro with Gibbs free energy values ranging from −10.9 to −6.5 (kcal mol−1). The results obtained here agree with these observations suggesting that, as observed for PLpro, sitagliptin may potentially be repositioned to be used as a drug directed to inhibit SARS-CoV-2 3CLpro and consequently suppress the spread and evolution of SARS-CoV-2 infection.
Structural analyses of the dipeptidyl peptidase 4 (DPP4) showed that this molecule is a cell membrane-bound receptor, expressed at high levels. DPP4 is formed by two subunits, each of one is composed by an 8-bladed β-propeller domain (N-terminal region) and an α/β hydrolase domain (C-terminal region). All known gliptins bind to a large pocket in the cavity located at the interface of the α/β-hydrolase domain and the 8-bladed β-propeller domain. The biological functions of DPP4 are associated with a variety of substrates, including incretin hormones, cytokines, chemokines, neuropeptides, and growth factors (Nar et al. 2021). In the context of the infections caused by Coronavirus, new evidences have shown that the human DPP4 is a functional receptor to SARS-CoV-2, due to the ability of the homotrimer structure of the spike protein (S1 domain) to interact and bind to these receptors (Vankadari and Wilce 2020).
Some recent studies have proposed that DPP4 inhibitors (iDDP4) with antiviral action might be useful for controlling the infection caused by SARS-CoV-2, especially for patients with diabetes (Drucker 2020; Eleftheriou et al. 2020; Iacobellis 2020), a group that deserves special attention due to its elevated risk to developing the severe acute respiratory syndrome, a very serious complication of COVID-19 disease. In the context of iDDP4, a series of indirect findings suggests that these drugs could be useful therapeutic off-target effects (Valencia et al. 2020), although there are several ongoing clinical discussions. About the gliptins (iDPP4 canonical class), it is important to emphasize that the use of these drugs is preferred in the treatment of individuals with diabetes, associated with chronic kidney disease or cardiovascular disease (Hanssen and Jandeleit-Dahm 2019). Therapeutic applications of sitagliptin in type 2 diabetic patients reduced the levels of C-reactive protein, interleukin-6 in mononuclear cells (Hussain et al. 2019; Katsiki and Ferrannini 2020), circulating TNF-α, interleukin-1β, and intracellular adhesion molecules (Tremblay et al. 2014), while it induced an increase in flow-mediated vasodilation in diabetic adults (Barchetta et al. 2019), and cardioprotection in diabetic patients with chronic kidney disease reducing the angiotensin II/angiotensin-(1–7) ratio (Tremblay et al. 2014; Beraldo et al. 2019; Barchetta et al. 2019).
Conclusion
By a series of in silico assays we demonstrated here that sitagliptin, a drug commonly used for treatment of type-II diabetes, exhibited potential dual-target inhibitory activity compatible with the active sites of two main SARS-CoV-2 proteases, 3CLpro, and PLpro. These findings justify the implementation of additional in vitro and in vivo studies aiming to validate the use of this drug as a repositioning medication in the fight against COVID-19 disease.
References
Aanouz I, Belhassan A, El-Khatabi K et al (2021) Moroccan medicinal plants as inhibitors against SARS-CoV-2 main protease: computational investigations. J Biomol Struct Dyn 39:2971–2979. https://doi.org/10.1080/07391102.2020.1758790
Abbas HA, Hegazy WAH (2020) Repurposing anti-diabetic drug “Sitagliptin” as a novel virulence attenuating agent in Serratia marcescens. PLoS ONE 15:e0231625. https://doi.org/10.1371/journal.pone.0231625
Abd-Elsalam S, Noor RA, Badawi R et al (2021) Clinical study evaluating the efficacy of ivermectin in COvid-19 treatment: a randomized controlled study. J Med Virol 93:5833–5838. https://doi.org/10.1002/jmv.27122
Abdizadeh R, Hadizadeh F, Abdizadeh T (2022) In silico analysis and identification of antiviral coumarin derivatives against 3-chymotrypsin-like main protease of the novel coronavirus SARS-CoV-2. Mol Divers 26:1053–1076. https://doi.org/10.1007/s11030-021-10230-6
Abraham MJ, Murtola T, Schulz R et al (2015) GROMACS: High performance molecular simulations through multi-level parallelism from laptops to supercomputers. SoftwareX 1–2:19–25. https://doi.org/10.1016/j.softx.2015.06.001
Adasme MF, Linnemann KL, Bolz SN et al (2021) PLIP 2021: expanding the scope of the protein–ligand interaction profiler to DNA and RNA. Nucleic Acids Res 49:W530–W534. https://doi.org/10.1093/nar/gkab294
Adegbola PI, Semire B, Fadahunsi OS, Adegoke AE (2021) Molecular docking and ADMET studies of Allium cepa, Azadirachta indica and Xylopia aethiopica isolates as potential anti-viral drugs for Covid-19. Virus Dis 32:85–97. https://doi.org/10.1007/s13337-021-00682-7
Amaral CML, Magalhaes ICL, Bezerra AS et al (2022) Insight into possible adjuvant role of phytol to fight SARS-CoV-2. Curr Sci 122:1241–1242
Báez-Santos YM, Barraza SJ, Wilson MW et al (2014) X-ray structural and biological evaluation of a series of potent and highly selective inhibitors of human coronavirus papain-like proteases. J Med Chem 57:2393–2412. https://doi.org/10.1021/jm401712t
Báez-Santos YM, St. John SE, Mesecar AD (2015) The SARS-coronavirus papain-like protease: structure, function and inhibition by designed antiviral compounds. Antiviral Res 115:21–38. https://doi.org/10.1016/j.antiviral.2014.12.015
Barchetta I, Ciccarelli G, Barone E et al (2019) Greater circulating DPP4 activity is associated with impaired flow-mediated dilatation in adults with type 2 diabetes mellitus. Nutr Metab Cardiovasc Dis 29:1087–1094. https://doi.org/10.1016/j.numecd.2019.07.010
Beraldo JI, Benetti A, Borges-Júnior FA et al (2019) Cardioprotection conferred by sitagliptin is associated with reduced cardiac angiotensin II/angiotensin-(1–7) balance in experimental chronic kidney disease. Int J Mol Sci 20:1940. https://doi.org/10.3390/ijms20081940
Berendsen HJC, Postma JPM, Van Gunsteren WF et al (1984) Molecular dynamics with coupling to an external bath. J Chem Phys 81:3684–3690. https://doi.org/10.1063/1.448118
Best C, Struthers H, Laciny E et al (2015) Sitagliptin reduces inflammation and chronic immune cell activation in HIV+ adults with impaired glucose tolerance. J Clin Endocrinol Metab 100:2621–2629. https://doi.org/10.1210/jc.2015-1531
Bhardwaj VK, Singh R, Sharma J et al (2021) Identification of bioactive molecules from tea plant as SARS-CoV-2 main protease inhibitors. J Biomol Struct Dyn 39:3449–3458. https://doi.org/10.1080/07391102.2020.1766572
Blum M, Chang H-Y, Chuguransky S et al (2021) The InterPro protein families and domains database: 20 years on. Nucleic Acids Res 49:D344–D354. https://doi.org/10.1093/nar/gkaa977
Burley SK, Bhikadiya C, Bi C et al (2021) RCSB Protein Data Bank: powerful new tools for exploring 3D structures of biological macromolecules for basic and applied research and education in fundamental biology, biomedicine, biotechnology, bioengineering and energy sciences. Nucleic Acids Res 49:D437–D451. https://doi.org/10.1093/nar/gkaa1038
Chen S, Tian J, Li Z et al (2019) Feline infectious peritonitis virus NSP5 inhibits type I interferon production by cleaving NEMO at multiple sites. Viruses 12:43. https://doi.org/10.3390/v12010043
Chittepu VCSR, Kalhotra P, Osorio-Gallardo T et al (2019) New molecular insights into the inhibition of dipeptidyl peptidase-4 by natural cyclic peptide oxytocin. Molecules 24:3887. https://doi.org/10.3390/molecules24213887
Clasman JR, Everett RK, Srinivasan K, Mesecar AD (2020) Decoupling deISGylating and deubiquitinating activities of the MERS virus papain-like protease. Antiviral Res 174:104661. https://doi.org/10.1016/j.antiviral.2019.104661
Cui J, Li F, Shi Z-L (2019) Origin and evolution of pathogenic coronaviruses. Nat Rev Microbiol 17:181–192. https://doi.org/10.1038/s41579-018-0118-9
Das S, Sarmah S, Lyndem S, Singha Roy A (2020) An investigation into the identification of potential inhibitors of SARS-CoV-2 main protease using molecular docking study. J Biomol Struct Dyn. https://doi.org/10.1080/07391102.2020.1763201
Denison MR, Graham RL, Donaldson EF et al (2011) Coronaviruses—an RNA proofreading machine regulates replication fidelity and diversity. RNA Biol 8:270–279. https://doi.org/10.4161/rna.8.2.15013
Drucker DJ (2020) Coronavirus infections and type 2 diabetes—shared pathways with therapeutic implications. Endocr Rev 41:457–470. https://doi.org/10.1210/endrev/bnaa011
Eleftheriou P, Amanatidou D, Petrou A, Geronikaki A (2020) In silico evaluation of the effectivity of approved protease inhibitors against the main protease of the novel SARS-CoV-2 virus. Molecules 25:2529. https://doi.org/10.3390/molecules25112529
Elekofehinti OO, Iwaloye O, Josiah SS et al (2021) Molecular docking studies, molecular dynamics and ADME/tox reveal therapeutic potentials of STOCK1N-69160 against papain-like protease of SARS-CoV-2. Mol Divers 25:1761–1773. https://doi.org/10.1007/s11030-020-10151-w
Essmann U, Perera L, Berkowitz ML et al (1995) A smooth particle mesh Ewald method. J Chem Phys 103:8577–8593. https://doi.org/10.1063/1.470117
Fan C, Wu X, Liu Q et al (2018) A human DPP4-knockin mouse’s susceptibility to infection by authentic and pseudotyped MERS-CoV. Viruses 10:448. https://doi.org/10.3390/v10090448
Fehr AR, Channappanavar R, Jankevicius G et al (2016) The conserved Coronavirus macrodomain promotes virulence and suppresses the innate immune response during severe acute respiratory syndrome Coronavirus infection. Mbio 7:1–12. https://doi.org/10.1128/mBio.01721-16
Freire CMAS, Fonseca FMP, Evangelista AJJ et al (2020) SARS-CoV2: a brief analysis of the history of an asymptomatic patient. Sylwan 164:486–505
Green JB, Bethel MA, Armstrong PW et al (2015) Effect of sitagliptin on cardiovascular outcomes in type 2 diabetes. N Engl J Med 373:232–242. https://doi.org/10.1056/NEJMoa1501352
Guo Y, Cao Q, Hong Z et al (2020) The origin, transmission and clinical therapies on coronavirus disease 2019 (COVID-19) outbreak—an update on the status. Mil Med Res 7:11. https://doi.org/10.1186/s40779-020-00240-0
Gyebi GA, Ogunro OB, Adegunloye AP et al (2020) Potential inhibitors of coronavirus 3-chymotrypsin-like protease (3CL pro ): an in silico screening of alkaloids and terpenoids from African medicinal plants. J Biomol Struct Dyn. https://doi.org/10.1080/07391102.2020.1764868
Hanssen NM, Jandeleit-Dahm KA (2019) Dipeptidyl peptidase-4 inhibitors and cardiovascular and renal disease in type 2 diabetes: what have we learned from the CARMELINA trial? Diabetes Vasc Dis Res 16:303–309. https://doi.org/10.1177/1479164119842339
Hess B (2008) P-LINCS: a parallel linear constraint solver for molecular simulation. J Chem Theory Comput 4:116–122. https://doi.org/10.1021/ct700200b
Huang Y, Yang C, Xu X et al (2020) Structural and functional properties of SARS-CoV-2 spike protein: potential antivirus drug development for COVID-19. Acta Pharmacol Sin 41:1141–1149. https://doi.org/10.1038/s41401-020-0485-4
Hussain M, Rafique MA, Iqbal J, Akhtar L (2019) Effect of sitagliptin and glimepiride on C-reactive protein (CRP) in overweight Type-2 diabetic patients. Pakistan J Med Sci 35:1–5. https://doi.org/10.12669/pjms.35.2.645
Iacobellis G (2020) COVID-19 and diabetes: can DPP4 inhibition play a role? Diabetes Res Clin Pract 162:108125. https://doi.org/10.1016/j.diabres.2020.108125
Islam R, Parves MR, Paul AS et al (2020) A molecular modeling approach to identify effective antiviral phytochemicals against the main protease of SARS-CoV-2. J Biomol Struct Dyn 2020:1–12. https://doi.org/10.1080/07391102.2020.1761883
Joshi RS, Jagdale SS, Bansode SB et al (2020) Discovery of potential multi-target-directed ligands by targeting host-specific SARS-CoV-2 structurally conserved main protease. J Biomol Struct Dyn. https://doi.org/10.1080/07391102.2020.1760137
Kashour Z, Riaz M, Garbati MA et al (2021) Efficacy of chloroquine or hydroxychloroquine in COVID-19 patients: a systematic review and meta-analysis. J Antimicrob Chemother 76:30–42. https://doi.org/10.1093/jac/dkaa403
Katsiki N, Ferrannini E (2020) Anti-inflammatory properties of antidiabetic drugs: a “promised land” in the COVID-19 era? J Diabetes Complications 34:107723. https://doi.org/10.1016/j.jdiacomp.2020.107723
Kozakov D, Grove LE, Hall DR et al (2015) The FTMap family of web servers for determining and characterizing ligand-binding hot spots of proteins. Nat Protoc 10:733–755. https://doi.org/10.1038/nprot.2015.043
Li K, Wohlford-Lenane CL, Channappanavar R et al (2017) Mouse-adapted MERS coronavirus causes lethal lung disease in human DPP4 knockin mice. Proc Natl Acad Sci 114:E3119–E3128. https://doi.org/10.1073/pnas.1619109114
Li Y, Zhang Z, Yang L et al (2020) The MERS-CoV receptor DPP4 as a candidate binding target of the SARS-CoV-2 spike. iScience 23:101160. https://doi.org/10.1016/j.isci.2020.101160
Li D, Luan J, Zhang L (2021) Molecular docking of potential SARS-CoV-2 papain-like protease inhibitors. Biochem Biophys Res Commun 538:72–79. https://doi.org/10.1016/j.bbrc.2020.11.083
Lu S, Wang J, Chitsaz F et al (2020) CDD/SPARCLE: the conserved domain database in 2020. Nucleic Acids Res 48:D265–D268. https://doi.org/10.1093/nar/gkz991
McGill AR, Kahlil R, Dutta R et al (2021) SARS–CoV-2 Immuno-pathogenesis and potential for diverse vaccines and therapies: opportunities and challenges. Infect Dis Rep 13:102–125. https://doi.org/10.3390/idr13010013
Mendez D, Gaulton A, Bento AP et al (2019) ChEMBL: towards direct deposition of bioassay data. Nucleic Acids Res 47:D930–D940. https://doi.org/10.1093/nar/gky1075
Mielech AM, Chen Y, Mesecar AD, Baker SC (2014) Nidovirus papain-like proteases: multifunctional enzymes with protease, deubiquitinating and deISGylating activities. Virus Res 194:184–190. https://doi.org/10.1016/j.virusres.2014.01.025
Moustaqil M, Ollivier E, Chiu H-P et al (2021) SARS-CoV-2 proteases PLpro and 3CLpro cleave IRF3 and critical modulators of inflammatory pathways (NLRP12 and TAB1): implications for disease presentation across species. Emerg Microbes Infect 10:178–195. https://doi.org/10.1080/22221751.2020.1870414
Nar H, Schnapp G, Hucke O et al (2021) Action of dipeptidyl peptidase-4 inhibitors on SARS-CoV-2 main protease. ChemMedChem 16:1425–1426. https://doi.org/10.1002/cmdc.202000921
Narayanan A, Narwal M, Majowicz SA et al (2022) Identification of SARS-CoV-2 inhibitors targeting Mpro and PLpro using in-cell-protease assay. Commun Biol 5:169. https://doi.org/10.1038/s42003-022-03090-9
Ngan C, Hall DR, Zerbe B et al (2012) FTSite: high accuracy detection of ligand binding sites on unbound protein structures. Bioinformatics 28:286–287. https://doi.org/10.1093/bioinformatics/btr651
Pitsillou E, Liang J, Ververis K et al (2020) Identification of small molecule inhibitors of the deubiquitinating activity of the SARS-CoV-2 papain-like protease: in silico molecular docking studies and in vitro enzymatic activity assay. Front Chem 8:1–15. https://doi.org/10.3389/fchem.2020.623971
Prompetchara E, Ketloy C, Palaga T (2020) Immune responses in COVID-19 and potential vaccines: lessons learned from SARS and MERS epidemic. Asian Pacific J Allergy Immunol 38:1–9. https://doi.org/10.12932/AP-200220-0772
Ratia K, Saikatendu KS, Santarsiero BD et al (2006) Severe acute respiratory syndrome coronavirus papain-like protease: structure of a viral deubiquitinating enzyme. Proc Natl Acad Sci 103:5717–5722. https://doi.org/10.1073/pnas.0510851103
Ravi V, Saxena S, Panda PS (2022) Basic virology of SARS-CoV 2. Indian J Med Microbiol 40:182–186. https://doi.org/10.1016/j.ijmmb.2022.02.005
Reiner Ž, Hatamipour M, Banach M et al (2020) Statins and the COVID-19 main protease: in silico evidence on direct interaction. Arch Med Sci 16:490–496. https://doi.org/10.5114/aoms.2020.94655
Scheen AJ (2013) Cardiovascular effects of gliptins. Nat Rev Cardiol 10:73–84. https://doi.org/10.1038/nrcardio.2012.183
Schöning-Stierand K, Diedrich K, Fährrolfes R et al (2020) ProteinsPlus: interactive analysis of protein–ligand binding interfaces. Nucleic Acids Res 48:W48–W53. https://doi.org/10.1093/nar/gkaa235
Shi J, Wei Z, Song J (2004) Dissection study on the severe acute respiratory syndrome 3C-like protease reveals the critical role of the extra domain in dimerization of the enzyme. J Biol Chem 279:24765–24773. https://doi.org/10.1074/jbc.M311744200
Sigrist CJA, de Castro E, Cerutti L et al (2012) New and continuing developments at PROSITE. Nucleic Acids Res 41:D344–D347. https://doi.org/10.1093/nar/gks1067
Singh R, Bhardwaj VK, Sharma J et al (2021) Identification of potential plant bioactive as SARS-CoV-2 Spike protein and human ACE2 fusion inhibitors. Comput Biol Med 136:104631. https://doi.org/10.1016/j.compbiomed.2021.104631
Singh R, Bhardwaj VK, Das P et al (2022) Benchmarking the ability of novel compounds to inhibit SARS-CoV-2 main protease using steered molecular dynamics simulations. Comput Biol Med 146:105572. https://doi.org/10.1016/j.compbiomed.2022.105572
Singhal T (2020) A review of Coronavirus disease-2019 (COVID-19). Indian J Pediatr 87:281–286. https://doi.org/10.1007/s12098-020-03263-6
Solerte SB, Di Sabatino A, Galli M, Fiorina P (2020) Dipeptidyl peptidase-4 (DPP4) inhibition in COVID-19. Acta Diabetol 57:779–783. https://doi.org/10.1007/s00592-020-01539-z
Speer SD, Li Z, Buta S et al (2016) ISG15 deficiency and increased viral resistance in humans but not mice. Nat Commun 7:11496. https://doi.org/10.1038/ncomms11496
Su H, Yao S, Zhao W et al (2020) Anti-SARS-CoV-2 activities in vitro of Shuanghuanglian preparations and bioactive ingredients. Acta Pharmacol Sin 41:1167–1177. https://doi.org/10.1038/s41401-020-0483-6
Tahir ul Qamar M, Alqahtani SM, Alamri MA, Chen L (2020) Structural basis of SARS-CoV-2 3CLpro and anti-COVID-19 drug discovery from medicinal plants. J Pharm Anal 10:313–319. https://doi.org/10.1016/j.jpha.2020.03.009
Tian W, Chen C, Lei X et al (2018) CASTp 3.0: computed atlas of surface topography of proteins. Nucleic Acids Res 46:W363–W367. https://doi.org/10.1093/nar/gky473
Tremblay AJ, Lamarche B, Deacon CF et al (2014) Effects of sitagliptin therapy on markers of low-grade inflammation and cell adhesion molecules in patients with type 2 diabetes. Metabolism 63:1141–1148. https://doi.org/10.1016/j.metabol.2014.06.004
Trott L, Olson AJ (2010) AutoDock Vina: improving the speed and accuracy of docking with a new scoring function, efficient optimization and multithreading. J Comput Chem 31:455–461. https://doi.org/10.1002/jcc.21334.AutoDock
Umesh KD, Selvaraj C et al (2020) Identification of new anti-nCoV drug chemical compounds from Indian spices exploiting SARS-CoV-2 main protease as target. J Biomol Struct Dyn. https://doi.org/10.1080/07391102.2020.1763202
Valencia I, Peiró C, Lorenzo Ó et al (2020) DPP4 and ACE2 in diabetes and COVID-19: therapeutic targets for cardiovascular complications? Front Pharmacol 11:1–14. https://doi.org/10.3389/fphar.2020.01161
Vankadari N, Wilce JA (2020) Emerging COVID-19 coronavirus: glycan shield and structure prediction of spike glycoprotein and its interaction with human CD26. Emerg Microbes Infect 9:601–604. https://doi.org/10.1080/22221751.2020.1739565
Wang H, He S, Deng W et al (2020) Comprehensive insights into the catalytic mechanism of middle east respiratory syndrome 3C-like protease and severe acute respiratory syndrome 3C-like protease. ACS Catal 10:5871–5890. https://doi.org/10.1021/acscatal.0c00110
Wu Y, Ma L, Zhuang Z et al (2020) Main protease of SARS-CoV-2 serves as a bifunctional molecule in restricting type I interferon antiviral signaling. Signal Transduct Target Ther 5:221. https://doi.org/10.1038/s41392-020-00332-2
Xia H, Cao Z, Xie X et al (2020) Evasion of type I interferon by SARS-CoV-2. Cell Rep 33:108234. https://doi.org/10.1016/j.celrep.2020.108234
Yang H, Yang M, Ding Y et al (2003) The crystal structures of severe acute respiratory syndrome virus main protease and its complex with an inhibitor. Proc Natl Acad Sci 100:13190–13195. https://doi.org/10.1073/pnas.1835675100
Yang W, Cai X, Han X, Ji L (2016) DPP-4 inhibitors and risk of infections: a meta-analysis of randomized controlled trials. Diabetes Metab Res Rev 32:391–404. https://doi.org/10.1002/dmrr.2723
Yavarian J, Nejati A, Salimi V et al (2022) Whole genome sequencing of SARS-CoV2 strains circulating in Iran during five waves of pandemic. PLoS ONE 17:e0267847. https://doi.org/10.1371/journal.pone.0267847
Yilmaz E, Akyön Y, Serdar M (2020) The molecular footprints of COVID-19. Turkish J Biochem 45:241–248. https://doi.org/10.1515/tjb-2020-0255
Yoshikawa K, Tsuchiya A, Kido T et al (2020) Long-term safety and efficacy of sitagliptin for type 2 diabetes mellitus in Japan: results of a multicentre, open-label, observational post-marketing surveillance study. Adv Ther 37:2442–2459. https://doi.org/10.1007/s12325-020-01293-2
Zhao Y, Tian Y, Pan C et al (2022) Target-based in silico screening for phytoactive compounds targeting SARS-CoV-2. Interdiscip Sci Comput Life Sci 14:64–79. https://doi.org/10.1007/s12539-021-00461-4
Zu ZY, Di JM, Xu PP et al (2020) Coronavirus disease 2019 (COVID-19): a perspective from China. Radiology 296:E15–E25. https://doi.org/10.1148/radiol.2020200490
Author information
Authors and Affiliations
Contributions
JEdCF, JEMJ, DPP, GEdCPL, CLdA, VRV, MPM, EBLF, RGO helped in conceptualization, methodology, data curation, writing—original draft preparation, validation, writing—reviewing and editing. VOF, APDRM, RCM performed visualization, investigation. RMMJ supervised the study.
Corresponding author
Ethics declarations
Conflict of interest
Authors declare that they have no conflict of interest.
Ethical approval
This article does not contain any studies with human participants or animals.
Supplementary Information
Below is the link to the electronic supplementary material.
Rights and permissions
Springer Nature or its licensor (e.g. a society or other partner) holds exclusive rights to this article under a publishing agreement with the author(s) or other rightsholder(s); author self-archiving of the accepted manuscript version of this article is solely governed by the terms of such publishing agreement and applicable law.
About this article
Cite this article
da Cruz Freire, J.E., Júnior, J.E.M., Pinheiro, D.P. et al. Evaluation of the anti-diabetic drug sitagliptin as a novel attenuate to SARS-CoV-2 evidence-based in silico: molecular docking and molecular dynamics. 3 Biotech 12, 344 (2022). https://doi.org/10.1007/s13205-022-03406-w
Received:
Accepted:
Published:
DOI: https://doi.org/10.1007/s13205-022-03406-w