Abstract
Objectives
As mindfulness practices become mainstream, it is increasingly common for participants in mindfulness-based interventions (MBI) to have previous meditation experience. The primary aim of this study was to assess whether the impacts of a mindfulness-based stress reduction (MBSR) program on a variety of self-report measures differed for novice meditators (NM) and regular meditators (RM).
Methods
A total of 158 Japanese participants in 10 cohorts completed questionnaires before and after an 8-week community-based MBSR program. The questionnaire consisted of Five Facet Mindfulness Questionnaire (FFMQ), Self-Compassion Scale (SCS), Total Mood Disturbance (TMD) from Profile of Mood States 2, Mental Component Summary (MCS) and Physical Component Summary (PCS) of the 12-Item Short Form Health Survey (2nd version), and Perceived Stress Scale (PSS). Baseline scores and pre-post change scores were compared for RM (participants who had reported meditating ≥ 45 min/week prior to MBSR) and NM (< 45 min/week).
Results
At baseline, RM (38.0% of the sample) had significantly higher scores than NM on FFMQ, SCS, and MCS, and lower scores on TMD and PSS (i.e., less mood disturbance and less stress). Post-program, both groups showed significant improvements in all measures except PCS, with NM’s post-MBSR scores comparable to RM’s baseline scores. A significant Group (NM vs. RM) × Time (pre- vs. post-) interaction was observed only for FFMQ.
Conclusions
Regular meditators, who show greater self-compassion and better mental health than novice meditators at baseline, can benefit from MBSR to a similar extent in measures of self-compassion and other aspects of well-being.
Similar content being viewed by others
Avoid common mistakes on your manuscript.
Mindfulness-based stress reduction (MBSR) is an 8-week well-defined and systematic patient-centered educational approach which uses relatively intensive training in mindfulness meditation as the core of a program to teach people how to take better care of themselves and live healthier and more adaptive lives (Kabat-Zinn 1996). The program consists of 8 weekly 2.5-h classes of 15–40 participants, one full-day retreat, and approximately 45 min per day of formal and informal practice (Santorelli 2014). MBSR is different from conventional meditation training and/or medical therapy in that it has (1) an educational rather than a therapeutic orientation, which makes use of relatively large “classes” of participants in a time-limited course structure to provide a community of learning and practice, and a “critical mass” to help in cultivating ongoing motivation, support, and feelings of acceptance and belonging; and (2) a medically heterogeneous environment, in which people with a broad range of health status and medical conditions participate in classes together without segregation by diagnosis or conditions and specializations of intervention (Griffith et al. 2019; Kabat-Zinn 1996). Numerous studies have shown benefits of the program in clinical and non-clinical populations on a variety of self-reported measures, including those of mindfulness, self-compassion, mood states, and perceived stress (Janssen et al. 2018; Khoury et al. 2015). In a review of the literature on impacts of MBSR, de Vibe et al. (2017) reported mental health, somatic health, and health-related quality of life as among the key outcomes improved by MBSR, with effect sizes ranging from Hedges g = 0.39–0.54. MBSR also has been shown to potentially affect brain function and anatomy (Tang et al. 2015; Young et al. 2018), as well as multiple biological processes from immunity (e.g., Davidson et al. 2003) to aging (e.g., Conklin et al. 2019).
With expanding applications of mindfulness to such fields as education, workplace, and justice (e.g., “Mindfulness All-Party Parliamentary Group” 2015), the general population is increasingly practicing mindfulness; in one study, 13% of US workers reported engaging in mindfulness-enhancing practices (Olano et al. 2015). Thus, a substantial proportion of participants in mindfulness-based interventions (MBI) such as MBSR may have practiced a variety of forms of meditation prior to participation. It is not known whether those regular meditators benefit from MBSR, since their baseline well-being, self-compassion, and other outcomes may have reached a ceiling level. On the other hand, unique features of MBSR, including systematic informal mindfulness practice, class dialogue/inquiry, didactic teaching, and emphasis on attitudinal qualities (Kabat-Zinn 1996; Santorelli 2014), which are missing or more implicit in most meditation practices in non-secular settings, may confer benefits to regular meditators beyond the level they have reached with regular meditation practice.
The literature is scant on the impacts of MBSR on regular meditators. A meta-analysis of 29 MBSR studies on healthy individuals (Khoury et al. 2015) reported on twelve studies using a standard MBSR protocol; of these, two studies (Cordon et al. 2009; Greeson et al. 2011) had a sample size of > 100, the minimum sample size that the authors considered to be sufficient to compare sub-groups of participants. Neither study described the participants’ prior meditation experience. In a more recent meta-analysis of 101 randomized controlled studies of MBSR (de Vibe et al. 2017), 39 studies used a standard MBSR protocol, and of these, only one study (de Vibe and Moum 2006) had > 100 MBSR participants. We also identified two other university/community-based MBSR studies using a standard MBSR protocol with the number of participants exceeding 100 (Carmody and Baer 2008; Carmody et al. 2009). None of these studies considered participants’ prior meditation experience.
However, other types of studies have compared novice with longer-term meditators. For example, fMRI studies have found that, compared to novice meditators, long-term meditators show reduced activation of prefrontal regions and greater activation of somatosensory cortical regions in response to arising sensory events (Zeidan et al. 2019) and less amygdala reactivity to emotionally positive pictures (Kral et al. 2018). However, to our knowledge, potential impacts of MBSR on regular meditators have not been studied.
The primary aim of this study was to assess the impacts of a mindfulness-based stress reduction (MBSR) program on a variety of self-report measures for novice meditators (NM) and regular meditators (RM). It was hypothesized that (1) RM would show higher baseline levels than NM on outcome measures; (2) both RM and NM would show improvements on outcome measures from baseline to post-program; and (3) there would be a significant interaction between Time and Group, with NM showing greater improvements than RM from baseline to post-program.
Method
Participants
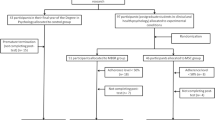
Participants were recruited via the internet for a self-paid 8-week MBSR course conducted in Japanese at the Kansai Medical University in Osaka and in a facility in Tokyo. The course was co-taught by two of the authors, Y.I. and K.Y., who were trained at the Center for Mindfulness, University of Massachusetts Medical Center, and who also had more than 15 years of experience of Rinzai Zen practice and Yoga practice, respectively. The MBSR program was conducted according to the standard protocol consisting of weekly classes (eight approximately 2.5-h classes and a 7-h “all day” class after the 6th class), 45 min per day of formal home practice 6 or more times per week, and informal home practice (Santorelli 2014). Participants were from 10 cohorts of classes, each with an average of 16 students. In this community self-paid program, those who initially applied were invited to attend an online orientation/information session, at which the exclusion criteria, as described in the MBSR standards of practice (Santorelli 2014), were explained. Exclusion criteria included clinical depression or other major psychiatric diagnosis currently uncontrolled by treatment. Of the individuals who subsequently registered for the program, the few who had indicated on their application form that they were in treatment for mental health issues were asked to get consent to participate from their treatment provider. All those who registered and who (if relevant) provided a consent form from their mental health provider were enrolled in the program.
A total of 178 Japanese individuals in 10 cohorts (12–31 individuals per cohort) participated in the 8-week MBSR program from October 2017 to October 2019. Analyses were conducted on data from 158 respondents (88.8% of the program participants) after excluding 20 whose data were not available for reasons including having participated previously, switching to a future program, and failing to complete the pre- and post-program questionnaires. The mean age (± SD) was 47.4 ± 9.9, and 69% were women (Table 1). About one-half (51%) had jobs in healthcare or education, while the remaining 49% had other jobs or were not in the workforce. NM (62% of the sample) and RM (38%) did not differ in mean age, sex ratio, or type of job (healthcare/education vs. other). Compared to NM, RM reported significantly more time spent in home meditation practice at baseline, as expected from how the groups were defined (136.9 ± 103.8 min/week vs. 3.3 ± 8.7, p < 0.001).
Procedure
Participants completed questionnaires prior to, or at, the first session. They included demographic information, experience with meditation practice, and Japanese versions of five survey instruments that measured (1) mindfulness, (2) self-compassion, (3) mood, (4) health-related quality of life (psychological and physical), and (5) perceived stress. They completed the same scales again at the end of the last session or up to 2 weeks after the last session. With respect to meditation practice prior to participation in MBSR, only the session time (minutes) and frequency per week were asked. Although most of the participants were not asked how long they had been meditating or the type of meditation they practiced (e.g., Vipassana/mindfulness, Zen), 14 RM participants in the last two cohorts were asked how long (in months) they had been meditating. Responses ranged from 1 month to 20 years; the median was 2.0 years. At the end of the program, participants were asked to report their home practice time (minutes per each practice and times per week). A written informed consent was obtained for possible publication of the results.
Measures
Mindfulness was assessed using the Five Facets of Mindfulness Questionnaire (FFMQ) (Baer et al. 2006). This instrument measures a trait-like general tendency to be mindful in daily life. It assesses five facets of mindfulness: (a) observing, defined as noticing or attending to internal and external experiences; (b) describing, defined as labeling internal experiences with words; (c) acting with awareness, defined as attending to the present moment (i.e., the opposite of acting on “automatic pilot”); (d) nonjudging of inner experience, defined as taking a nonevaluative stance toward thoughts and feelings; and (e) nonreactivity to inner experience, defined as allowing thoughts and feelings to come and go, without getting caught up in or carried away by them (Bohlmeijer et al. 2011). Items are rated on a Likert scale ranging from 1 (never or very rarely true) to 5 (very often or always true). We used a 24-item short form (Bohlmeijer et al. 2011) created by extracting essential items from the validated Japanese version (Sugiura et al. 2012). The total score was the sum of the 6 subscales, with a range of possible scores from 24 to 120. McDonald’s omega for each of the subscales in the total sample (n = 158) showed adequate values, ranging from 0.70 to 0.87.
Self-compassion was assessed using the 26-item Self-compassion Scale (SCS) (Neff 2003; Neff and Germer 2013), which assesses the positive and negative aspects of the three main components of self-compassion: (1) self-kindness (vs. self-judgment); (2) common humanity (vs. isolation); and (3) mindfulness (vs. overidentification). For each item, participants rated the frequency with which they agreed with a given statement on a 5-point scale ranging from 1 (almost never) to 5 (almost always). The statements reflected the three components of self-compassion. For example, the statements “I try to be understanding and patient toward aspects of my personality I don’t like” and “I’m disapproving and judgmental about my own flaws and inadequacies” measure self-kindness versus self-judgment; “I try to see my failings as part of the human condition” and “When I think about my inadequacies it tends to make me feel more separate and cut off from the rest of the world” measure common humanity versus isolation; and “When something painful happens I try to take a balanced view of the situation” and “When I’m feeling down I tend to obsess and fixate on everything that’s wrong” measure mindfulness versus over-identification. The total score was the sum of the means for the 6 subscales (after reversing the scores of negative items) with a range of possible scores from 6 to 30. We used a validated Japanese version (Arimitsu 2014). McDonald’s omega for each of the subscales in the total sample showed adequate values, ranging from 0.73 to 0.91.
Mood states were assessed using a 35-item short form of POMS Second Edition (POMS-2) (Henderson et al. 2012). The instruments are a collection of self-rating tools that allow for the assessment of transient, fluctuating feelings, and enduring affect states. It has six sub-scales: Anger-Hostility, Confusion-Bewilderment, Depression-Dejection, Fatigue-Inertia, Tension-Anxiety, and Vigor-Activity. The Total Mood Disturbance (TMD) score is the sum of the five negative mood scores minus the Vigor-Activity score. POMS-2 provides a series of adjectives describing mood states (e.g., tense, angry, and worn out), and respondents indicate their mood state by rating the extent to which each corresponds to how they feel on a 5-point scale ranging from 0 (Not at all) to 4 (Extremely). The Japanese version uses norm-based scoring algorithms [T-score transformation, mean = 50 ± 10 (SD)], enabling the characterization of participants in comparison to the national mean (Heuchert and McNair 2015). McDonald’s omega for each of the subscales in the total sample showed adequate values, ranging from 0.84 to 0.94.
Health-related QOL was assessed using the SF-12v2 (SF-12) (Fukuhara & Suzukamo 2011, 2019; McDowell 2006). The SF-12 yields a profile of scores consisting of eight sub-scales: physical functioning, role physical, bodily pain, general health, vitality, social functioning, role emotional, and mental health. Higher scores indicate higher quality of life (i.e., better physical functioning, fewer role limitations due to physical health problems, less bodily pain, higher general health, vitality/energy, and social functioning, fewer role limitations due to emotional problems, and better mental health/greater well-being). We used a Physical Component Summary score (PCS) and a Mental Component Summary score (MCS), which are composite scores based on scores in the physical and mental sub-scales, respectively. The Japanese version uses Japanese norm-based scoring algorithms, enabling the characterization of participants in comparison to the national mean. Spearman-Brown’s coefficients for each of the subscales with two items (i.e., physical functioning, role physical, role emotional and mental health) showed values ranging from 0.62 (physical functioning) to 0.90 (role emotional).
Perceived stress was assessed using PSS-14 (Mimura and Griffiths 2008). The scale was designed to measure “the degree to which individuals appraise situations in their lives as stressful” and “how unpredictable, uncontrollable, and overloaded respondents find their lives” (Cohen 1988). It is a 14-item instrument that assesses perceived stressful experiences or stress responses over the previous month using a 5-point Likert-type scale. Total possible scores range from 0 to 56, with higher scores representing higher stress levels. McDonald’s omega for the total sample was 0.81. The national norm for the Japanese population has not been established.
The recall period for all of the outcome scales was set to 4 weeks. Therefore, baseline responses reflected the 4-week period before the first session and post-program responses reflected the 4-week period starting from weeks 5 to 7 of the program, depending on when the post-program scales were completed.
Data Analyses
Participants who reported meditating < 45 min per week before the program were defined as novice meditators (NM) and those who reported meditating ≥ 45 min per week were defined as regular meditators (RM). The threshold of 45 min was chosen because previous research found that slightly less than 45 min per week appeared to be required to benefit from MBSR (Davidson et al. 2003). To test for group differences in background factors (age, and self-reported baseline meditation time per week) and group differences in baseline scores on the five survey instruments, independent sample t-tests were performed. Chi-square tests were used to compare sex and job type for the two groups. Independent sample t-tests were used to compare baseline scores on the instruments with national norms. To explore the effects of time (from baseline to post-program) and group membership (NM vs. RM) on outcome scores, mixed two-way ANOVAs were conducted. Effect sizes (Cohen’s d) of pre- to post-program changes for each group were calculated by dividing the mean change with the standard deviation. Correlations were measured using linear regression analysis. Reliability for each scale (or sub-scale, where relevant) was assessed using McDonald’s omega (Hayes and Coutts 2020), except for the four two-item subscales (PCS and MCS) within SF-12, for which Spearman-Brown’s coefficients were used (Eisinga et al. 2013). All the analyses were conducted with SPSS V.27 (IBM).
Results
Baseline Outcomes
Of the measures participants completed, three have established national norms with which to compare those of our sample: TMD from the POMS-2 scale of mood states and PCS and MCS from SF-12. As a whole, the sample was comparable to the norm of 50 ± 10 for the Japanese population on the TMD (49.4 ± 10.4; 95% CI = 47.8–51.1) and the MCS (50.4 ± 8.9; 95% CI = 49.0–51.8), while it was higher than the norm on the PCS (55.1 ± 9.9; 95% CI = 53.6–56.7). Comparing each group with the national norm showed that NM’s mean score on TMD and MCS was comparable to the national mean of 50 [51.0 ± 10.7 (48.9–53.2) and 49.0 ± 9.2 (47.2–50.8), respectively], whereas RM’s mean score was significantly lower than the national mean on TMD [46.9 ± 9.5 (44.4–49.3)] (indicating lower levels of mood disturbance), and higher than the national mean on MCS [52.6 ± 7.9 (50.6–54.7)].
Between-group comparisons revealed that mean baseline scores were significantly higher for RM than for NM on FFMQ (64.3 ± 10.1 vs. 57.9 ± 9.1, p < 0.001), SCS (20.9 ± 4.5 vs. 18.1 ± 4.2, p < 0.001), and MCS (52.6 ± 7.9 vs. 49.0 ± 9.2, p < 0.05), and significantly lower for RM than for NM on TMD (46.9 ± 9.5 vs. 51.0 ± 10.7, p < 0.05) and PSS (24.1 ± 7.4 vs. 26.7 ± 6.9, p < 0.001), indicating that at baseline regular meditators had higher levels than novice meditators of mindfulness, self-compassion, and mental health, and lower levels of mood disturbance and perceived stress.
Changes in Scores from Baseline to Post-Program
As shown in Fig. 1, both NM and RM showed significant pre- to post-MBSR changes in scores on all of the instruments except PCS. The effect sizes were generally larger for NM (d = 0.53–0.80) than for RM (d = 0.38–0.53). However, as shown in Table 2, the interaction between Group (NM vs. RM) and Time (pre vs. post) was significant only for FFMQ, with NM’s scores improving more from baseline to post-program than those for RM [F(1, 156) = 3.9, p = 0.049; partial η2 = 0.0025]. No significant Group × Time interaction was found for the other outcome measures, with partial η2 values for these measures ranging from 0.002 (p = 0.593) to 0.013 (p = 0.147). The absence of a Group × Time interaction for most of the measures suggests that improvements from the baseline were overall similar for NM and RM. NM and RM did not differ in class attendance (7.4 ± 0.8 vs. 7.4 ± 0.7 classes out of 8) or self-reported home practice time during the program (219.7 ± 120.4 vs. 277.9 ± 183.7 min per week). As self-reported practice time for RM increased significantly from before to after the program (from 136.9 ± 103.8 min to 277.9 ± 183.7, p < 0.001), linear regression analyses were conducted for RM to assess any associations between changes in practice time and changes in instrument scores from pre- to post-MBSR. No significant correlations were found between changes in practice time and any of the changes in instrument scores from pre- to post-program.
Pre to post changes in outcome measure scores for NM and RM. Error bars are 95% confidence intervals. FFMQ, Five facet Mindfulness Questionnaire; SCS, Self-Compassion Scale; TMD, Total Mood Disturbance in Profile of Mood States 2 (POMS 2); PCS, Physical Component Summary in SF-12v2; MCS, Mental Component Summary in SF-12v2; PSS, Perceived Stress Scale 14-item version. FFMQ, SCS, and PSS are raw scores whose potential ranges are 24–120, 6–30, and 0–56, respectively. TMD, MCS, and PSC are national norm-based scores [T-score transformation, mean = 50 ± 10 (SD)]. d, Cohen’s d **p < 0.01, ***p < 0.001 compared to pre-program values within each group
Discussion
The primary aim of this study was to compare the impacts of MBSR on mindfulness and various measures of well-being for novice meditators and regular meditators. The results showed that at baseline, RM scored higher on mindfulness and self-compassion scales than NM and had lower mood disturbance, lower perceived stress levels, and higher mental quality of life. After the program, both NM and RM showed significant improvements in these scales from baseline to post-program. NM’s post-MBSR scores were in fact comparable to RM’s baseline scores. The lack of a significant interaction between time (pre- to post-program) and group (NM vs. RM) on most of the outcome measures suggests that the improvements were generally comparable for the two groups.
The fact that a substantial proportion (38%) of the participants of the current MBSR program had already experienced meditation practice prior to joining MBSR may not be surprising, as secular meditation—particularly mindfulness—is increasingly practiced by the general population worldwide, and its application to a variety of areas in society is growing (e.g., Olano et al. 2015). We did not collect information on the type of meditation practiced by RM, so inferences about this are necessarily speculative. Nevertheless, the higher baseline FFMQ score for RM compared to NM may suggest that their primary practice was mindfulness (or Vipassana) meditation, which is gaining popularity in Japan primarily from Western influence and places emphasis on mindfulness skills such as observing as well as describing and acting with awareness, facets captured in FFMQ. It seems less likely that participants had been practicing Traditional Zen meditation (either the Soto or Rinzai tradition) as it places less emphasis on these skills. Other types of meditation, including Transcendental Meditation, are rarely practiced in Japan.
The overall effect sizes for NM on the scales (e.g., for FFMQ, d = 0.80; for PSS d = − 0.74) were roughly within the range reported in previous MBSR studies. For example, for a large community program, effect sizes were d = 0.67 (FFMQ) and d = − 0.50 (PSS) (Juul et al. 2018); for university-based programs cited in a review, effect sizes were d = 0.47–0.90 (FFMQ subscales) and d = − 1.02 (PSS) (Carmody and Baer 2008). Previous meditation experience was not reported for these studies, so it is not known if any of the participants were already regular meditators. It is notable that even a relatively brief intervention period of 8 weeks in MBSR improved scores on these measures for NM to levels comparable to those at baseline for RM, who had practiced meditation on a regular basis presumably much longer than 8 weeks (as a small sub-group of RM in our sample had practiced for a median of 2 years).
RM also showed significant improvements in the outcome measures. Although the effect sizes were generally numerically smaller in RM than NM, a significant interaction between Group (NM vs. RM) × Time (pre vs. post) was observed only for the FFMQ score (partial η2 = 0.0025), suggesting that scores on SCS, TMD, MCS, and PSS improved for the two groups to similar degrees (with partial η2 values for these measures ranging from 0.002 to 0.013). This is notable, as previous research has suggested that the impacts of MBSR appear to be greater for individuals with higher levels of distress at baseline (de Vibe and Moum 2006; Juul et al. 2018). The only outcome measure for which there was not an effect of Time for either group was PCS (the physical component summary of the Health-related Quality of Life Scale) [F(1, 156) = 0.3, p = 0.577, η2 = 0.002]. Previous research has similarly found no change in PCS from pre- to post-MBSR for populations whose baseline PCS score is at or above the national mean (e.g., Greeson et al. 2011).
The fact that RM significantly improved on these measures beyond the level achieved by their previous regular meditation practice is likely due to many factors. It is unlikely that these improvements can be attributed simply to an increase in meditation time, as amount of practice time during the program among RM did not correlate with degree of improvement in any of the variables. Two alternative possibilities are discussed here.
One factor that might contribute to RM’s improvement in well-being beyond their already relatively high baseline levels is that MBSR has unique features compared to meditation alone. These MBSR features include a variety of formal practices such as body scan, mindful yoga and walking meditation, systematic informal practices, didactic teaching (including the relationships among thoughts, emotions, and bodily sensations), and the use of “classes” of participants in a time-limited course structure (Kabat-Zinn 1996; Santorelli 2014).
Another unique feature of MBSR involves the “great deal of guidance” with which the formal practices in MBSR were introduced (Kabat-Zinn 2011), compared to meditation learned and practiced with less guidance. For example, a guiding instruction commonly used in MBSR, such as, “There is no need in this practice to judge yourself negatively because becoming distracted is just part of training your attention,” has been shown to decrease mind-wandering (Rahl et al. 2017), and also potentially could foster non-judging and non-reactive attitudes as well. Both are components of FFMQ and non-judging is a component of SCS. Reduced mind-wandering, along with non-judgment and non-reactiveness, in turn might contribute to improvements of TMD (Evans et al. 2018) and PSS (Bränström et al. 2010).
An additional unique aspect of MBSR is that participants are given out-of-class assignments including one that invites them to notice and document pleasant and unpleasant events during the week along with their reactions to the events. This assignment provides participants with opportunities to expose themselves to potential sources of stress reactions through the lens of observation, which may also contribute to nonreactivity as captured in the FFMQ (Holzel et al. 2011), and in turn, to improvements of TMD (Evans et al. 2018) and PSS (Bränström et al. 2010). Also, the class group activities were designed to help maintain participants’ motivation, provide support, and foster feelings of acceptance and belonging (Kabat-Zinn 1996). These factors could contribute to the observed improvements in components of self-compassion (SCS), such as common humanity/isolation.
Dismantling studies (i.e., comparing a standard MBSR program with a program consisting solely of formal meditation practices) would help elucidate differential contributions of different program components on specific outcomes, providing further insights on the mechanisms of MBSR. In addition to such an approach, future studies could include gathering qualitative data pre- and post-MBSR by asking questions about which features were more or less valuable at the conclusion of the 8 weeks. This information may tease out what elements of the class are supportive to RM and NM, and also could be beneficial for teachers to understand what elements might be more or less important for both groups.
A second factor that might have contributed to RM’s improvement from baseline to post-MBSR involves this group’s motivations for signing up to take the course when they already had an independent meditation practice. Future research could examine participants’ motivations and how they might be associated with impacts from MBSR.
A body of evidence amassed in the past decade or so shows that MBSR can be beneficial for those with compromised well-being in clinical populations, such as those with chronic insomnia (Gross et al. 2011), with chronic pain (la Cour and Petersen 2015), and with chronic back pain (Morone et al. 2008), and in chronic caregivers (Whitebird et al. 2013), as well as those in non-clinical populations, such as academic healthcare employees (Geary and Rosenthal 2011) and healthcare providers (Goodman & Schorling, 2012). The current study provides evidence that people with higher-than-average well-being—even those with previous meditation practice—can benefit from MBSR as well. Thus, MBSR might be beneficial for individuals along the entire spectrum of well-being. This is consistent with a claim that mindfulness interventions may be beneficial not only for those with compromised well-being but for those who are already “resilient or flourishing” (Kuyken et al. 2017).
The finding that NM reached well-being levels post-MBSR comparable to those of RM at baseline does not necessarily mean that this 8-week program has the same impact as does longer-term meditation practice. Research comparing short-term with long-term meditators on a neuronal level using fMRI has shown that some changes in brain activity can occur in a relatively short period of time, while other changes require much more practice. For example, Kral et al. (2018) showed emotionally positive and negative pictures to long-term meditators, short-term meditators (i.e., individuals who had undergone MBSR), and a control group of non-meditators. The authors measured reactivity in the amygdala, which is related to emotion regulation. Compared to non-meditators, both long-term and short-term meditators showed significantly less amygdala reactivity to emotionally positive pictures. It is notable that the short-term meditators’ amygdala reactivity in response to emotionally positive pictures post-MBSR decreased to levels comparable to those observed at baseline in the long-term meditators. In response to emotionally negative pictures, there were no group differences in amygdala reactivity between the non-meditators and either the short-term or the long-term meditators. However, among the long-term meditators, more retreat experience was related to reduced activation to negative pictures. In a similar study, Desbordes et al. (2012) measured right amygdala activation in response to positive and negative pictures both before and after an 8-week mindful attention training intervention. Post-intervention, participants showed decreased right amygdala activation in response to positive pictures as well as to the pictures overall (i.e., positive and negative combined), but there was no significant decrease in reactivity to the negative pictures. Reduced emotional reactivity to both positive and negative stimuli is understood to be associated with well-being, as the brain does not become “hijacked” by wanting/grasping and aversion. Thus, de-activation to positive stimuli appears to happen relatively quickly, and only after more time practicing does the reactivity to negative stimuli decrease. This points to a complex process of change occurring as a result of meditation that continues over months and years.
A study by Brand et al. (2012) also provides evidence that some benefits of meditation can begin to occur quickly (i.e., over an 8-week MBSR program), and then continue to improve if meditation is continued long-term. The authors measured cortisol levels (as well as self-report measures) in a small group of long-term meditators (LTM; n = 9) and novice meditators (NM) who completed MBSR (n = 11). Cortisol awakening response (CAR) was reduced from pre- to post-MBSR for NM to levels comparable to those observed in LTM, and for LTM, duration of meditation experience was negatively associated with CAR.
It is not known how long well-being related to decreased emotional reactivity and other underlying neurological and biochemical changes induced by MBSR remains if participants do not continue practicing after the program; it is possible that these later-occurring changes are necessary for more consistent, longer-term well-being. Addressing this important question will require longitudinal studies looking at post-MBSR changes over time in participants who do, versus do not, maintain meditation practice.
Limitations and Future Research
This study has both strengths and limitations. One source of strength was the use of instruments whose national normative data are established, which allowed us to compare NM and RM with the Japanese norm, with NM showing similar mood states and mental QOL, and RM showing lower mood disturbance and higher mental QOL compared to the Japanese norm. This comparison point enabled us to postulate potential implications of MBSR to a larger general population. An additional strength is the high response rate, ensuring minimal attrition bias; 87.5% of participants provided consent and pre- and post-assessment data. Similar studies typically have response rates between 50 and 75% (e.g., Carmody et al. 2009; Greeson et al. 2011; Juul et al. 2018). It is not entirely clear why our response rate was so much higher than that of similar studies, but contributing factors could include (1) differing norms and expectations within Japanese culture versus other cultures, (2) our efforts to stress to participants the importance of data collection at the orientation, (3) the high program completion rate among our initial participants who had provided consent (164 of 169, or 97.0%) as defined by attending 6 or more of the 8 weekly classes, and (4) our setting up time during the last session of the program to fill out the questionnaire.
One potential limitation of this study is the pre-post analysis design lacking a control group, which always raises the possibility that the observed improvements may have been temporary changes over time unrelated to the intervention. This seems unlikely, however, since the effects of MBSR observed in this study are in line with those reported in a systematic review and meta-analysis of randomized controlled studies (de Vibe et al. 2017) as well as a meta-analysis of studies for healthy individuals (Khoury et al. 2015). Furthermore, one could argue that observed improvements could be attributed to non-specific effects of treatment, such as attention or treatment contact, human interaction variables, and/or outcome expectations (Mohr et al. 2009). This is also unlikely, as many studies have shown that MBSR induces specific brain changes compared to active control conditions that included these non-specific effects of treatment (Gotink et al. 2016). Also, we did not collect detailed information on participants’ meditation practice prior to MBSR. In particular, we collected data on how long RM have been practicing meditation for only a small subset of participants. Furthermore, as there are variety of meditative practices and we did not collect data on the types of meditation practiced by participants, the conclusions of this study may not be generalizable to regular practitioners of all types of meditation. Future studies on the impacts of MBSR on participants with previous meditation experience should collect more detailed data, including type and duration of meditation practiced, retreat experience, etc.
Another potential limitation is the possibility of a common method bias (Podsakoff et al. 2012), as all of the outcome measures in this study consist of self-report Likert-type scales. Although procedural strategies to minimize the common method bias were used, such as explaining the purpose of the research to participants at the orientation to increase response accuracy and using scales containing both positive and negative (i.e., reverse coded) items (Jordan and Troth 2020), the potential impact of common method bias on the conclusion cannot be excluded.
A further limitation of this study, which is inherent in research comparing novices with non-novices, experts, or regular practitioners of any activity, is that the threshold we used to distinguish novices from regular meditators was somewhat arbitrary, at 45 min per week. While this threshold was chosen because of previous research showing that approximately this amount of time appeared to be required to benefit from MBSR (Davidson, et al. 2003), there is little research on the amount of regular meditation per week time required to derive benefits in the absence of formal programs that include weekly sessions with additional features beyond meditation alone. It is also likely that the amount of practice time per week is only one of many factors that contribute to the extent to which self-reported meditation is beneficial, including frequency and lifetime spent on practice (Soler et al. 2014), self-report accuracy, aspects of the particular meditation practiced, having the correct “attitude” while meditating (non-judgmental awareness, curiosity, gently bringing attention back when one becomes aware of being lost in thought, etc.), and interactions with person-level factors. Future research on the factors that contribute to beneficial impacts of meditation, including amount of time practiced, would help inform how studies should distinguish between different levels of meditation expertise. Future research should also address how long improvements from MBSR persist. Information from such research can inform potential changes to MBIs, such as encouraging ongoing practice after the program and developing “booster” MBIs for people who have previously participated in MBSR.
Data Availability
The data that support the findings of this study are available from the corresponding author upon reasonable request.
References
Arimitsu, K. (2014). Development and validation of the Japanese version of the Self-Compassion Scale. The Japanese Journal of Psychology, 85(1), 50–59. https://doi.org/10.4992/jjpsy.85.50
Baer, R. A., Smith, G. T., Hopkins, J., Krietemeyer, J., & Toney, L. (2006). Using self-report assessment methods to explore facets of mindfulness. Assessment, 13. https://doi.org/10.1177/2F1073191105283504
Bohlmeijer, E., Ten Klooster, P. M., Fledderus, M., Veehof, M., & Baer, R. (2011). Psychometric properties of the five facet mindfulness questionnaire in depressed adults and development of a short form. Assessment, 18(3), 308–320. https://doi.org/10.1177/1073191111408231
Brand, S., Holsboer-Trachsler, E., Naranjo, J. R., & Schmidt, S. (2012). Influence of mindfulness practice on cortisol and sleep in long-term and short-term meditators. Neuropsychobiology, 65(3), 109–118.
Bränström, R., Kvillemo, P., Brandberg, Y., & Moskowitz, J. T. (2010). Self-report mindfulness as a mediator of psychological well-being in a stress reduction intervention for cancer patients—a randomized study. Annals of Behavioral Medicine, 39(2), 151–161. https://doi.org/10.1007/s12160-010-9168-6
Carmody, J., & Baer, R. A. (2008). Relationships between mindfulness practice and levels of mindfulness, medical and psychological symptoms and well-being in a mindfulness-based stress reduction program. Journal of Behavioral Medicine, 31(1), 23–33. https://doi.org/10.1007/s10865-007-9130-7
Carmody, J., Baer, R. A., Lykins, E. B., & Olendzki, N. (2009). An empirical study of the mechanisms of mindfulness in a mindfulness-based stress reduction program. Journal of Clinical Psychology, 65(6), 613–626. https://doi.org/10.1002/jclp.20579
Cohen, J. (1988). Statistical power analysis for the behavioral sciences. Lawrence Erlbaum Associates.
Conklin, Q. A., Crosswell, A. D., Saron, C. D., & Epel, E. S. (2019). Meditation, stress processes, and telomere biology. Current Opinion in Psychology, 28, 92–101. https://doi.org/10.1016/j.copsyc.2018.11.009
Cordon, S. L., Brown, K. W., & Gibson, P. R. (2009). The role of mindfulness-based stress reduction on perceived stress: Preliminary evidence for the moderating role of attachment style. Journal of Cognitive Psychotherapy, 23(3), 258–269. https://doi.org/10.1891/0889-8391.23.3.258
Davidson, R. J., Kabat-Zinn, J., Schumacher, J., Rosenkranz, M., Muller, D., Santorelli, S. F., Urbanowski, F., Harrington, A., Bonus, K., & Sheridan, J. F. (2003). Alterations in brain and immune function produced by mindfulness meditation. Psychosomatic Medicine, 65(4), 564. https://doi.org/10.1097/01.PSY.0000077505.67574.E3
de Vibe, M., & Moum, T. (2006). Oppmerksomhetstrening for pasienter med stress og kroniske sykdommer [Training in mindfulness for patients with stress and chronic illness]. Tidsskrift for Den Norske Laegeforening: Tidsskrift for Praktisk Medicin, Ny Raekke, 126(15), 1898–1902.
de Vibe, M. F., Bjørndal, A., Fattah, S., Dyrdal, G. M., Halland, E., & Tanner-Smith, E. E. (2017). Mindfulness-based stress reduction (MBSR) for improving health, quality of life and social functioning in adults: A systematic review and meta-analysis. Campbell Systematic Reviews, 13(1), 1–264. https://doi.org/10.4073/csr.2017.11
Desbordes, G., Negi, L. T., Pace, T. W., Wallace, B. A., Raison, C. L., & Schwartz, E. L. (2012). Effects of mindful-attention and compassion meditation training on amygdala response to emotional stimuli in an ordinary, non-meditative state. Frontiers in Human Neuroscience, 6, 292. https://doi.org/10.3389/fnhum.2012.00292
Eisinga, R., Grotenhuis, M. T., & Pelzer, B. (2013). The reliability of a two-item scale: Pearson, Cronbach, or Spearman-Brown? International Journal of Public Health, 58(4), 637–642. https://doi.org/10.1007/s00038-012-0416-3
Evans, S., Wyka, K., Blaha, K. T., & Allen, E. S. (2018). Self-Compassion mediates improvement in well-being in a mindfulness-based stress reduction program in a community-based sample. Mindfulness, 9(4), 1280–1287. https://doi.org/10.1007/s12671-017-0872-1
Fukuhara, S., & Suzukamo, Y. (2011, 2019). Manual of SF-36v2. Japanese version. Institute for Health Outcome and Process Evaluation Research, Kyoto.
Geary, C., & Rosenthal, S. L. (2011). Sustained impact of MBSR on stress, well-being, and daily spiritual experiences for 1 year in academic health care employees. Journal of Alternative and Complementary Medicine, 17(10), 939–944. https://doi.org/10.1089/acm.2010.0335
Goodman, M. J., & Schorling, J. B. (2012). A mindfulness course decreases burnout and improves well-being among healthcare providers. International Journal of Psychiatry in Medicine, 43(2), 119–128. https://doi.org/10.2190/PM.43.2.b
Gotink, R. A., Meijboom, R., Vernooij, M. W., Smits, M., & Hunink, M. G. (2016). 8-week Mindfulness Based Stress Reduction induces brain changes similar to traditional long-term meditation practice - a systematic review. Brain and Cognition, 108, 32–41. https://doi.org/10.1016/j.bandc.2016.07.001
Greeson, J. M., Webber, D. M., Smoski, M. J., Brantley, J. G., Ekblad, A. G., Suarez, E. C., & Wolever, R. Q. (2011). Changes in spirituality partly explain health-related quality of life outcomes after Mindfulness-Based Stress Reduction. Journal of Behavioral Medicine, 34(6), 508–518. https://doi.org/10.1007/s10865-011-9332-x
Griffith, G. M., Bartley, T., & Crane, R. S. (2019). The inside out group model: Teaching groups in mindfulness-based programs. Mindfulness, 10(7), 1315–1327. https://doi.org/10.1007/s12671-019-1093-6
Gross, C. R., Kreitzer, M. J., Reilly-Spong, M., Wall, M., Winbush, N. Y., Patterson, R., Mahowald, M., & Cramer-Bornemann, M. (2011). Mindfulness-based stress reduction versus pharmacotherapy for chronic primary insomnia: A randomized controlled clinical trial. EXPLORE, 7(2), 76–87. https://doi.org/10.1016/j.explore.2010.12.00
Hayes, A. F., & Coutts, J. J. (2020). Use omega rather than Cronbach’s alpha for estimating reliability. But…. Communication Methods and Measures, 14(1), 1–24. https://doi.org/10.1080/19312458.2020.1718629
Henderson, V. P., Clemow, L., Massion, A. O., Hurley, T. G., Druker, S., & Hébert, J. R. (2012). The effects of mindfulness-based stress reduction on psychosocial outcomes and quality of life in early-stage breast cancer patients: A randomized trial. Breast Cancer Research and Treatment, 131(1), 99–109. https://doi.org/10.1007/s10549-011-1738-1
Heuchert, J., & McNair, D. (2015). Japanese translation of Profile of Mood States 2nd Edition (POMS 2) (Yokoyama, K. & Watanabe, K., Trans.). Tokyo: Kaneko Shobo.
Holzel, B. K., Lazar, S. W., Gard, T., Schuman-Olivier, Z., Vago, D. R., & Ott, U. (2011). How does mindfulness meditation work? Proposing mechanisms of action from a conceptual and neural perspective. Perspectives on Psychological Science, 6(6), 537–559. https://doi.org/10.1177/1745691611419671
Janssen, M., Heerkens, Y., Kuijer, W., van der Heijden, B., & Engels, J. (2018). Effects of mindfulness-based stress reduction on employees’ mental health: A systematic review. PLoS One, 13(1), e0191332. https://doi.org/10.1371/journal.pone.0191332
Jordan, P. J., & Troth, A. C. (2020). Common method bias in applied settings: The dilemma of researching in organizations. Australian Journal of Management, 45(1), 3–14. https://doi.org/10.1177/0312896219871976
Juul, L., Pallesen, K. J., Piet, J., Parsons, C., & Fjorback, L. O. (2018). Effectiveness of mindfulness-based stress reduction in a self-selecting and self-paying community setting. Mindfulness, 9(4), 1288–1298. https://doi.org/10.1007/s12671-017-0873-0
Kabat-Zinn, J. (1996). Mindfulness meditation: What it is, what it isn’t, and its role in health care and medicine. In Y. Haruki, Y. Ishii, & M. Suzuki (Eds.), Comparative and psychological study on meditation (pp. 161–170). Eburon.
Kabat-Zinn, J. (2011). Some reflections on the origins of MBSR, skillful means, and the trouble with maps. Contemporary Buddhism, 12(1), 281–306.
Khoury, B., Sharma, M., Rush, S. E., & Fournier, C. (2015). Mindfulness-based stress reduction for healthy individuals: A meta-analysis. Journal of Psychosomatic Research, 78(6), 519–528. https://doi.org/10.1016/j.jpsychores.2015.03.009
Kral, T. R. A., Schuyler, B. S., Mumford, J. A., Rosenkranz, M. A., Lutz, A., & Davidson, R. J. (2018). Impact of short- and long-term mindfulness meditation training on amygdala reactivity to emotional stimuli. NeuroImage, 181, 301–313. https://doi.org/10.1016/j.neuroimage.2018.07.013
Kuyken, W., Nuthall, E., Byford, S., Crane, C., Dalgleish, T., Ford, T., Greenberg, M. T., Ukoumunne, O. C., Viner, R. M., Williams, J., MYRIAD team. (2017). The effectiveness and cost-effectiveness of a mindfulness training programme in schools compared with normal school provision (MYRIAD): Study protocol for a randomised controlled trial. Trials, 18(1), 194. https://doi.org/10.1186/s13063-017-1917-4
la Cour, P., & Petersen, M. (2015). Effects of mindfulness meditation on chronic pain: A randomized controlled trial. Pain Medicine, 16(4), 641–652. https://doi.org/10.1111/pme.12605
McDowell, I. (2006). Measuring health: A guide to rating scales and questionnaires (3rd ed.). Oxford University Press. https://doi.org/10.1093/acprof:oso/9780195165678.001.0001
Mimura, C., & Griffiths, P. (2008). A Japanese version of the Perceived Stress Scale: Cross-cultural translation and equivalence assessment. BMC Psychiatry, 8(85). https://doi.org/10.1186/1471-244X-8-85
Mindfulness All-Party Parliamentary Group. (2015). MINDFUL NATION UK. https://www.themindfulnessinitiative.org/Handlers/Download.ashx?IDMF=1af56392-4cf1-4550-bdd1-72e809fa627a
Mohr, D. C., Spring, B., Freedland, K. E., Beckner, V., Arean, P., Hollon, S. D., Ockene, J., & Kaplan, R. (2009). The selection and design of control conditions for randomized controlled trials of psychological interventions. Psychotherapy and Psychosomatics, 78(5), 275–284. https://doi.org/10.1159/000228248
Morone, N. E., Greco, C. M., & Weiner, D. K. (2008). Mindfulness meditation for the treatment of chronic low back pain in older adults: A randomized controlled pilot study. Pain, 134(3), 310–319. https://doi.org/10.1016/j.pain.2007.04.038
Neff, K. (2003). Self-compassion: An alternative conceptualization of a healthy attitude toward oneself. Self and Identity, 2(2), 85–101. https://doi.org/10.1080/15298860309032
Neff, K. D., & Germer, C. K. (2013). A pilot study and randomized controlled trial of the mindful self-compassion program. Journal of Clinical Psychology, 69(1), 28–44. https://doi.org/10.1002/jclp.21923
Olano, H. A., Kachan, D., Tannenbaum, S. L., Mehta, A., Annane, D., & Lee, D. J. (2015). Engagement in mindfulness practices by US adults: Sociodemographic barriers. The Journal of Alternative and Complementary Medicine, 21(2), 100–102.
Podsakoff, P. M., MacKenzie, S. B., & Podsakoff, N. P. (2012). Sources of method bias in social science research and recommendations on how to control it. Annual Review of Psychology, 63(1), 539–569.
Rahl, H. A., Lindsay, E. K., Pacilio, L. E., Brown, K. W., & Creswell, J. D. (2017). Brief mindfulness meditation training reduces mind wandering: The critical role of acceptance. Emotion, 17(2), 224. https://doi.org/10.1037/emo0000250
Santorelli, S. (2014). Mindfulness-based stress reduction (MBSR): Standards of practice. Center for Mindfulness in Medicine, University of Massachusetts Medical School.
Soler, J., Cebolla, A., Feliu-Soler, A., Demarzo, M. M. P., Pascual, J. C., Baños, R., & García-Campayo, J. (2014). Relationship between meditative practice and self-reported mindfulness: The MINDSENS Composite Index. PLoS One, 9(1), e86622. https://doi.org/10.1371/journal.pone.0086622
Sugiura, Y., Sato, A., Ito, Y., & Murakami, H. (2012). Development and validation of the Japanese version of the Five Facet Mindfulness Questionnaire. Mindfulness, 3(2), 85–94. https://doi.org/10.1007/s12671-011-0082-1
Tang, Y. Y., Hölzel, B. K., & Posner, M. I. (2015). The neuroscience of mindfulness meditation. Nature Reviews Neuroscience, 16(4), 213–225. https://doi.org/10.1038/nrn3916
Whitebird, R. R., Kreitzer, M., Crain, A. L., Lewis, B. A., Hanson, L. R., & Enstad, C. J. (2013). Mindfulness-based stress reduction for family caregivers: A randomized controlled trial. The Gerontologist, 53(4), 676–686. https://doi.org/10.1093/geront/gns126
Young, K. S., van der Velden, A. M., Craske, M. G., Pallesen, J. K., Fjorback, L., Roepstorff, A., & Parsons, C. E. (2018). The impact of mindfulness-based interventions on brain activity: A systematic review of functional magnetic resonance imaging studies. Neuroscience and Biobehavioral Reviews, 84, 424–433. https://doi.org/10.1016/j.neubiorev.2017.08.003
Zeidan, F., Baumgartner, J. N., & Coghill, R. C. (2019). The neural mechanisms of mindfulness-based pain relief: A functional magnetic resonance imaging-based review and primer. Pain Reports, 4(4), e759. https://doi.org/10.1097/PR9.0000000000000759
Acknowledgements
The authors deeply appreciate Professor Mikihiko Fukunaga and Professor Yoshihide Nakai for their continued encouragement and support. We also appreciate Professor Kenji Kanbara for his insight and advice.
Author information
Authors and Affiliations
Contributions
YI: conducted the program and data collection, analyzed the data, conceptualized the study, and co-wrote the paper. CB: co-wrote the paper. KY: conducted the program and data collection, and reviewed the paper.
Corresponding author
Ethics declarations
Ethical Standards
Studies have been approved by the ethics committee (#2020230, Kansai Medical University IRB), and procedures conform to the 1964 Declaration of Helsinki and subsequent amendments. All subjects gave their informed consent prior to study inclusion.
All procedures performed in studies involving human participants were in accordance with the ethical standards of the institutional and/or national research committee and with the 1964 Helsinki declaration and its later amendments or comparable ethical standards. All procedures were approved by the University of Illinois Institutional Review Board and informed consent was obtained from all participants prior to study participation.
Conflict of Interest
The authors declare no competing interests.
Additional information
Publisher's Note
Springer Nature remains neutral with regard to jurisdictional claims in published maps and institutional affiliations.
Rights and permissions
Open Access This article is licensed under a Creative Commons Attribution 4.0 International License, which permits use, sharing, adaptation, distribution and reproduction in any medium or format, as long as you give appropriate credit to the original author(s) and the source, provide a link to the Creative Commons licence, and indicate if changes were made. The images or other third party material in this article are included in the article's Creative Commons licence, unless indicated otherwise in a credit line to the material. If material is not included in the article's Creative Commons licence and your intended use is not permitted by statutory regulation or exceeds the permitted use, you will need to obtain permission directly from the copyright holder. To view a copy of this licence, visithttp://creativecommons.org/licenses/by/4.0/.
About this article
Cite this article
Ito, Y., Browne, C.A. & Yamamoto, K. The Impacts of Mindfulness-Based Stress Reduction (MBSR) on Mindfulness and Well-being for Regular and Novice Meditators. Mindfulness 13, 1458–1468 (2022). https://doi.org/10.1007/s12671-022-01888-6
Accepted:
Published:
Issue Date:
DOI: https://doi.org/10.1007/s12671-022-01888-6