Abstract
Two connected histopathological hallmarks of Alzheimer’s disease (AD) are chronic neuroinflammation and synaptic dysfunction. The accumulation of the most prevalent posttranslationally modified form of Aβ1–42, pyroglutamylated amyloid-β (Aβ3(pE)-42) in astrocytes is directly linked to glial activation and the release of proinflammatory cytokines that in turn contribute to early synaptic dysfunction in AD. At present, the mechanisms of Aβ3(pE)-42 uptake to astrocytes are unknown and pharmacological interventions that interfere with this process are not available. Here we developed a simple screening assay to identify substances from a plant extract library that prevent astroglial Aβ3(pE)-42 uptake. We first show that this approach yields valid and reproducible results. Second, we show endocytosis of Aβ3(pE)-42 oligomers by astrocytes and that quercetin, a plant flavonol, is effective to specifically block astrocytic buildup of oligomeric Aβ3(pE)-42. Importantly, quercetin does not induce a general impairment of endocytosis. However, it efficiently protects against early synaptic dysfunction following exogenous Aβ3(pE)-42 application.
Similar content being viewed by others
Avoid common mistakes on your manuscript.
Introduction
Alzheimer’s disease (AD) is a devastating neurodegenerative condition with a poor prognosis. AD is the most common type of dementia and the histopathological hallmark of the disease is the accumulation of hyperphosphorylated tau tangles and extracellular plaques of amyloid-β (Aβ) [1, 2]. According to the most prominent hypothesis for causation of AD, the amyloid-hypothesis, the oligomerization and deposition of the Aβ peptide as fibrils in the brain is causative for disease progression [1,2,3,4,5]. Next to their direct neurotoxic properties, Aβ oligomers activate microglia and astrocytes, which in turn results in chronic sterile neuroinflammation and production of pro-inflammatory cytokines that are synaptotoxic [6,7,8]. Importantly, neuroinflammation is part of early disease pathology and is believed to contribute to late onset AD (LOAD) [1, 6]. Neuroinflammation in AD is orchestrated by microglia and astrocytes [6, 9]. Aβ can directly induce microglial immune response by binding to their receptors (e.g., Toll-like receptors or CD63) triggering the release of proinflammatory cytokines and microglia-driven synaptic pruning [6, 9]. Moreover, Aβ elicits astrocytic reactivity, leading to the release of synaptotoxic cytokines [6]. In addition, at early AD stages, astrocytes display disrupted homeostatic functions, especially calcium and glutamate dyshomeostasis, which contribute to synapse loss [10,11,12].
Multiple posttranslationally modified Aβ peptides were reported in AD patients and among those, the amino-terminally truncated, pyroglutamylated form of Aβ (Aβ3(pE)-42) is abundant in AD brains and seeds highly toxic co-oligomers with conventional Aβ1–42 [13,14,15]. So far, drug development was directed against various steps of these processes, e.g., against pyroglutamate formation [16, 17]. In previous work, we found that in contrast to Aβ1–42, Aβ3(pE)-42 is readily taken up by astrocytes, accumulates in the astrocytic endolysosomal system, leading to the lysosomal membrane permeabilization [18, 19]. The uptake of Aβ3(pE)-42 potently induces reactive astrogliosis and subsequent release of the proinflammatory cytokine TNFα, which results in synapse loss [18, 19]. Several lines of evidence support the notion that the synaptotoxic effects of N-terminally modified Aβ species are associated with glial activation [15, 19, 20]. It would therefore be beneficial to identify well-tolerated compounds that prevent the uptake of Aβ3(pE)-42 to astrocytes.
Plant-based natural products have a long history in medical applications although their full potential is still not appreciated [17]. In addition to their direct action, plant components can prevent disease or support treatment [21]. If they derive from food sources, they are well tolerated and allow rapid application, e.g., as nutraceutical with high patient acceptance and compliance and easy legal entrance to the market [22]. This includes plant natural products for the prevention or treatment of AD [23,24,25,26].
In the present study, we aimed to establish a screening assay that would allow to identify substances from plant libraries which can attenuate the reactive astrogliosis caused by Aβ3(pE)-42. In a second step, we then verified that one of the identified substances in this regard has indeed neuroprotective effects.
Materials and Methods
Aβ3(pE)-42 Oligomer Preparation
The Aβ3(pE)-42 peptide was ordered from AnaSpec (Cat. No. AS-29907). Aβ3(pE)-42 oligomers were prepared as described previously [19]. The quality of the production and procedure was controlled by SDS-PAGE (Fig. S1).
SDS-PAGE and Western Blot
For verification of Aβ3(pE)-42 oligomerization, standard SDS-PAGE protocol followed by Western blot was used. The samples were mixed with 4 × SDS—sample buffer (250 mM Tris–HCl, pH 6.8, 1% (w/v) SDS, 40% (v/v) glycerol 20% (v/v) β-mercaptoethanol, 0.004% Bromophenol Blue) and loaded onto 5–20% polyacrylamide gel. The gel was set under a constant electric field of 12 mA for 1.5 h followed by transfer to a nitrocellulose membrane (Merck, Cat. No. GE10600002). The membranes were probed with anti-pE3 antibody (1:1000, SySy, Cat. No. 218003, RRID:AB_2056424) detected with anti-rabbit secondary antibody conjugated with HRP (Dianova Cat. No. 111–035-144, RRID:AB_2337938).
Plant-Based Natural Products
Plant substances were selected from the Natural Product Library of the Leibniz-Institute of Plant Biochemistry, Dept. Bioorganic Chemistry, Halle (Saale). The substances were dissolved in dimethyl sulfoxide (DMSO, > 99%, Duchefa Biochemie) at a concentration of 10 mM. For treatment of astrocytes, the substances were further diluted in water with 0.5% DMSO to a concentration of 1 mM and subsequently applied to the culture medium resulting in a final concentration of 5 µM and 50 µM (max. DMSO content of 0.5%). The structures of the natural products are shown in Fig. S2.
Primary Astrocyte Cell Culture
All animal experiments were carried out in accordance with the European Communities Council Directive (2010/63/EU) and German animal welfare act. Astrocytes were isolated from new-born rat forebrain tissue (P0) and stored at − 80 °C in Dulbecco’s Modified Eagle’s Medium (DMEM) (Gibco, Cat. No. 41966–029) following previously described procedures [19]. The cells were thawed in a water bath on demand and added to pre-warmed DMEM supplemented with 10% FBS, 1% penicillin/streptomycin, and 0.8 mM L-glutamine. Astrocytes were plated in 24-well plates with poly-D-lysine (Sigma-Aldrich, Cat. No. P-1149)-coated coverslips and kept at 37 °C, 5% CO2, and 95% humidity in a Heraeus incubator. After 24 h, the medium was exchanged to serum-free DMEM containing 1% penicillin/streptomycin.
Screening Assay
Thirty-two hours following medium exchange, astrocytes were treated with the plant natural products for 16 h at a concentration of 5 µM or 50 µM and 500 nM Aβ3(pE)-42. Subsequently, cells were fixed in 4% PFA and 4% sucrose and permeabilized with 0.2% TX-100 in PBS for 10 min, blocked for 1 h in blocking solution (2% glycine, 0.2% gelatine, 2% BSA, and 50 mM NH4Cl (pH 7.4)), and incubated overnight at 4 °C with GFAP (1:500, SySy, Cat. No. 173–004, RRID:AB_10641162) and Aβ3(pE)-42 (1:500, SySy, Cat. No. 218003, RRID:AB_2056424) antibodies diluted in blocking buffer. Next, the samples were washed with PBS and incubated 2 h at RT with secondary antibodies: anti-guinea pig-AlexaFluor 488 (1:500, Thermo Fisher Scientific, Cat. No. A-11073, RRID:AB_2534117) and anti-rabbit-AlexaFluor 568 (1:500, Thermo Fisher Scientific, Cat. No. A-11036, RRID:AB_10563566) diluted in blocking buffer. Finally, the coverslips were mounted with Mowiol 4–88 (Merck Chemicals). Each condition was performed in duplicates. As controls, two coverslips were incubated with 500 nM Aβ3(pE)-42 only or vehicle control (0.5% DMSO, ITW Reagents, Cat. No. A3672).
Images were acquired from five randomly chosen field of views (FOV) per coverslip from two independent experiments, resulting in 20 FOVs per group, using a Zeiss Axio Imager A2 fluorescent microscope with 20 × objective (Zeiss, Plan-Apochromat, 20x/0,8 M27, Item No.: 420650–9901-000) equipped with the Cool Snap EZ Monochrome camera (Photometrics) and VisiView Imaging software (Visitron Systems) and analyzed with Image-J software [27]. For quantification of intracellular Aβ3(pE)-42 uptake, fixed threshold values were applied to both 16-bit channels (GFAP threshold at 135, Aβ3(pE)-42 at 1000). The following parameters were quantified: (1) area—the sum of areas from all detected Aβ3(pE)-42 deposits, (2) the number of deposits—the total number of Aβ3(pE)-42 deposits identified, (3) mean size—the average area from all Aβ3(pE)-42 deposits identified within one FOV. Aβ3(pE)-42 area and number of deposits were normalized to the respective GFAP area to account for the number of astrocytes within FOV and astrocytic size. Plotted values were normalized to the corresponding control. Since extracellular Aβ3(pE)-42 deposits were not observed, all signal from the Aβ3(pE)-42 channel was considered intracellular Aβ3(pE)-42. All experimental steps were performed blinded to the plant substances.
For endocytosis inhibition experiments, Aβ3(pE)-42 was co-applied with dynasore (Merck, Cat. No. 324410) at the final concentration of 5 µM for 16 h and analyzed in the same way as described above.
HEK-293T Cell Culture
HEK-293T (ATCC, Cat. No. CRL-3216) cells were cultured in DMEM (Gibco, Cat. No. 41966–029) supplemented with 10% FBS, 1% penicillin/streptomycin, and 0.8 mM L-glutamine in an incubator at 37 °C, 5% CO2, and 95% humidity. Cells were plated in 24-well plates with coverslips coated with poly-D-lysine; 500 nM Aβ3(pE)-42 oligomers and 5 µM or 50 µM quercetin were added simultaneously after 10 h. Each condition was performed in duplicates. Following 16 h of incubation, cells were fixed in 4% PFA and 4% sucrose and stained according to the protocol described above with vimentin (1:200, Sigma-Aldrich, Cat. No. V-6630, RRID:AB_477627) and Aβ3(pE)-42 (1:500, SySy, Cat. No. 218003, RRID:AB_2056424) antibodies with secondary antibodies anti-mouse-AlexaFluor 488 (1:500, Thermo Fisher Scientific, Cat. No. A-11001, RRID:AB_2534069) and anti-rabbit-AlexaFluor 568 (1:500, Thermo Fisher Scientific, Cat. No. A-11036, RRID:AB_10563566). Image acquisition and analysis were done like described above.
Mixed Primary Hippocampal Cultures
Rat hippocampi were dissected from E18-day-old Sprague Dawley rats and primary mixed astrocytic-neuronal cultures were prepared by technical assistants following a previously described protocol [19]. Cells were seeded in poly-D-lysine-coated 18-mm coverslips in 12-well plates at a density of 30,000 cells per coverslip. Neurons were kept in Neurobasal medium (Gibco, Cat. No. 21103049) supplemented with 0.8 mM glutamine (Gibco, Cat. No. 25030–024), 1% penicillin/streptomycin (Gibco, Cat. No. 15240–062), and 2% B27 (Gibco, Cat. No. 17504–044). Cultures were kept in the incubator at 37 °C, 5% CO2, and 95% humidity.
Nuclear pCREB and Synaptic Staining, Imaging, and Quantification
On DIV, 16–18 mixed hippocampal cultures were incubated with 50 µM quercetin or 50 µM aristolactam BII and/or 500 nM Aβ3(pE)-42 oligomers for 2 (synaptic density assay) or 3 days (CREB shutoff assay), fixed with 4% PFA and 4% sucrose, and stained according to the protocol described above with antibodies detecting pCREB (Ser133) (1:500, Cell Signaling, Cat. No. 9198, RRID:AB_2561044) and MAP2 (1:500, Sigma-Aldrich; Cat. No. M-4403, RRID:AB_477193), detected with secondary antibodies anti-mouse-AlexaFluor 488 (1:500, ThermoFisher Scientific, Cat. No. A-11001, RRID:AB_2534069) and anti-rabbit-AlexaFluor 568 (1:500, ThermoFisher Scientific, Cat. No. A-11036, RRID:AB_10563566). Next, the samples were washed and co-stained with DAPI. For synaptic staining, the samples were stained with anti-PSD95 minibody (1:500, NanoTag N3783), anti-synaptophysin 1 (1:500, SySy, Cat. No. 101011, RRID:AB_887824), and anti-MAP2 (1:500, Sysy, Cat. No. 188004, RRID:AB_2138181) detected with anti-guinea pig-AlexaFluor 568 (1:500, ThermoFisher Scientific, Cat. No. A-11075, RRID:AB_2534119), anti-rabbit-AlexaFluor 488 (1:500, ThermoFisher Scientific, Cat. No. A-11034, RRID:AB_2576217), and anti-mouse-AlexaFluor 647 (1:500, Thermo Fisher Scientific, Cat. No. A-32733, RRID:AB_2633282).
Images were acquired with an inverse Leica TCS STED-SP8 3 × microscope (Leica-Microsystems, Germany) equipped with pulsed White Light Laser (WLL) and diode 405 nm for excitation with 63 × (Leica) objective lens along the z-axis with 300-nm z-step in a 512 × 512-pixel formats at 8-bit image depth at 400-Hz laser frequency.
Images were analyzed with ImageJ [27]. Nuclear pCREB intensities were measured within region of interest defined by DAPI. Synapses (overlap or opposing pre- and post-synaptic signal) were counted along defined dendritic stretches.
Dextran Uptake Assay
To monitor endocytosis, 10-kDa fixable tetramethylrhodamine (TMR) dextran (5 mM, ThermoFisher Scientific, Cat. No. D1868) was applied to the cells together with 500 nM of Aβ3(pE)-42, 50 µM of quercetin, or Aβ3(pE)-42 with quercetin. Following 2-h pulse, the cells were kept 2 h in growth medium, and subsequently washed and fixed. The samples were next co-stained with antibodies detecting GFAP and Aβ3(pE)-42 as described above. The images were acquired with Olympus FV3000 confocal microscope (Evident, Germany) equipped with solid state laser lines 405 nm, 488 nm, and 561 nm for excitation with 60 × OlanApo Oil objective lens (NA: 1.4) along the z-axis with 300-nm z-step in a 512 × 512-pixel formats at 8-bit image depth. Averaged fluorescent intensity from four planes across optical axis was analyzed. Images were analyzed with ImageJ [27]. Dextran puncta were considered endocytosed if they appeared within GFAP region of the cell. The fluorescence maxima detection function was used to detect discrete dextran or Aβ3(pE)-42 puncta (circular region of interests (ROIs) with 3 pixels radius). For quantification of endocytosis rate, the total number of discrete puncta was normalized to GFAP area to account for size of astrocytic cell. The overlap between dextran and Aβ3(pE)-42 ROIs was considered as colocalization. Line profiles depict fluorescence intensity along the straight line normalized individually for each channel. For the representative images, the background subtraction and median filter were applied equally between groups.
Organotypic Slice Cultures
Rat, organotypic hippocampal slices were prepared as described previously (Gee et al., 2017). Experiments were performed with cultures at DIV8 or 16. 500 nM Aβ3(pE)-42 and 50 μM quercetin were applied for 24 h. Slices were stained according to the above-described protocol, with the modified permeabilization step—0.3% TX-100 for 1 h at RT. The astrocytes were labeled with GFAP (1:500, SySy, Cat. No. 173–004, RRID:AB_10641162) or vimentin antibody (1:500, Agilent, Cat. No. M0725, RRID:AB 10013485) detected with anti-guinea pig-AlexaFluor 488 (1:500, ThermoFisher Scientific, Cat. No. A-11073, RRID:AB_2534117) or anti-mouse AlexaFluor 488 (1:500, ThermoFisher Scientific, Cat. No. A-11001, RRID:AB 2534069) and subsequently counterstained with DAPI. The images of samples were acquired with a Zeiss LSM 900 (Plan-Apochromat 20 × /0.8). Ten images from z-optical plane were acquired with a step size of 0.5 μm for each region of interest. Excitation/emission filters were selected using the dye selection function of the Fluoview/Zen3.5 software (Alexa 405 (DAPI), Alexa 488 (GFAP or vimentin)). The maximum fluorescence intensity was quantified using ImageJ [27] excluding pyramidal layer region defined by DAPI. Images were not deconvolved or filtered for quantification. Representative images presented in the figures were linearly adjusted.
Acute Hippocampal Slice Preparation and Long-Term Potentiation (LTP) Recording
Acute hippocampal slices from 8- to 12-week-old male C57/B6J mice were prepared according to a previously described protocol [28]. Briefly, mouse brains were sliced by Vibratome (Leica VT1000ST) into 350-μm-thick slices. Hippocampal slices were incubated with 500 nM Aβ3(pE)-42 and 10 µM quercetin in carbogenated (CO2 5%, O2 95%) aCSF solution (110 mM NaCl, 2.5 mM KCl, 2.5 mM CaCl2, 1.5 mM MgSO4, 1.24 mM KH2PO4, 10 mM glucose, 27.4 mM NaHCO3, pH 7.3) at room temperature for 2 h. Field excitatory postsynaptic potentials (fEPSPs) were measured in stratum radiatum after stimulation of CA1 Schaffer-collateral fibers, amplified by Extracellular Amplifier (EXT-02B, npi, Germany), and digitated at a sample frequency of 5 kHz by Digidata 1201 plus AD/Da converter (CED, UK). To induce LTP tetanization with 3 × 1 s stimulus trains at 100 Hz with a 10-min inter-train interval and double-pulse width (0.2 ms) were used.
Statistical Analysis and Figure Preparation
GraphPad Prism was used to plot graphs and perform statistical analyses. For the screening assay, outliers were removed using ROUT method, with Q = 1% or Grubb’s outlier test α = 0.05 for synapse density, pCREB, and GFAP intensity quantification. The statistical test was chosen based on the normal distribution of the data sets determined by D’Agostino-Pearson test. For normally distributed data, two-way ANOVA with Tukey post hoc test for multiple comparisons was used. For not normally distributed data, Kruskal–Wallis followed by Dunn’s multiple comparisons test was used. For HEK293-T-cell experiments, one-way ANOVA was performed followed by Dunnett’s test for multiple comparisons. Results from statistical tests are indicated within each figure legend; statistical notations in the graphs are as follows: ns, nonsignificant; *p ≤ 0.05; **p ≤ 0.01; ***p ≤ 0.001; ****p ≤ 0.0001. All figures were prepared with Adobe Illustrator.
Results
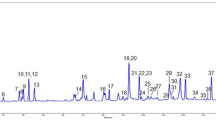
Aβ accumulation, oligomerization, and deposition are central to the pathogenesis of AD [1,2,3]. Here we took advantage of a Natural Product library from the Leibniz Institute of Plant Biochemistry to search for substances that directly target the uptake of Aβ3(pE)-42 oligomers in astroglia. We initially screened 61 substances that were pre-selected from the 30,000 entries library based on the following criteria: (1) availability/amounts accessible; (2) chemical stability; (3) small molecule, ideally obeying Lipinsky rules; (4) natural product (NP) or simple NP derivative, preferentially from plant or mushroom; (5) derived from a plant with reported anti-Alzheimer or similar neurological activity, including such data from our previous research; or: from a compound class reported beneficial to neuro-inflammation; or: compound with structural similarity to such with reported activity in mental health [16, 25, 26, 29,30,31,32]. The tested natural products comprised a wide range of compound classes, including flavonoids, alkaloids, lignans, anthraquinones, other diverse phenolics, and triterpenoids. The plant natural products were applied in two concentrations, namely 5 and 50 µM to the cell culture medium (Fig. 1a–h; Fig. S2; Fig. S3a–i).
Plant substances alter uptake and morphology of astrocytic, intracellular Aβ3(pE)-42 deposits. a, b Astrocytes take up Aβ3(pE)-42 oligomers in vitro, while no extracellular deposits are visible. Representative a fluorescence and b confocal images of astrocytes. Scale bar a 50 µm and b 25 µm. c Schematic workflow of the screening assay. d Segmentation of the GFAP and Aβ3(pE)-42 fluorescent signal used for analysis. Scale bar 50 µm. e–g Selected plant substances lead to altered e intracellular area, f number, and g size of intracellular Aβ3(pE)-42 deposits. Plant substances highlighted in green reduce intracellular Aβ3(pE)-42 area and number of deposits. Quercetin (50 μM), formononetin (50 µM), and aristolactam BII (50 µM) are marked in dark green. Twenty fields of view (FOVs) per condition from two independent experiments were analyzed. Data were normalized to the corresponding control and for e, f also to GFAP area per FOV. Control represents incubation with Aβ3(pE)-42 only; Aβ3(pE)-42 plus vehicle control for plant substances (DMSO) showed no effect (both in grey). h Number of Aβ3(pE)-42 deposits versus intracellular Aβ3(pE)-42 area was plotted for all tested plant substances. The same nine plant substances like in e–g are highlighted in green and dark green. e–g \(*\) p < 0.05; \(**\) p < 0.01; \(***\) p < 0.001; \(****\) p < 0.0001 by Kruskal–Wallis test followed by Dunn’s multiple comparisons test. Data are presented as mean \(\pm\) s.e.m
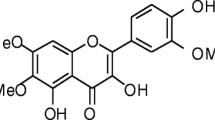
Primary astrocytes were kept in culture under standardized conditions and 500 nM of oligomeric Aβ3(pE)-42 (Fig. S1) was added to the medium. Uptake of Aβ3(pE)-42 was monitored following fixation and immunostaining with corresponding antibodies (Fig. 1a, b). Quantitation of Aβ3(pE)-42 immunofluorescence was done double-blind with the GFAP mask as ROI (Fig. 1d). Although GFAP, a cytoskeletal marker, does not outline the complete cell volume of an astrocyte, previous work has shown that this measurement yields reliable data on the intracellular accumulation of Aβ3(pE)-42, both for smaller and bigger inclusions [19]. We first analyzed the total area of Aβ3(pE)-42 deposits (Fig. 1e). Out of 61 screened substances, nine significantly reduced the uptake of oligomeric Aβ3(pE)-42 to astrocytes (quercetin—50 µM p = 0.0002; rutin—5 µM p = 0.015; epicatechin—50 µM p = 0.0008; apigenin—5 µM p = 0.025; spinosin C—50 µM p = 0.002; formononetin—50 µM p < 0.0001; aristolactam BII—50 µM p < 0.0001; resveratrol—50 µM p = 0.0002; isoasarone—50 µM p = 0.003), while the others showed no major effect on Aβ3(pE)-42 internalization (Fig. 1e, Fig. S2, Fig. S3a, d, g). Correspondingly, these nine substances also decreased the number of discrete intracellular Aβ3(pE)-42 deposits (Fig. 1f), while for other plant substances, a reduced number was compensated by larger intracellular deposits (Fig. 1g, Fig. S2, Fig. S3c, f, i), thus keeping Aβ3(pE)-42 uptake unaltered. While the majority of substances yielded stronger effect at the 50 µM, some proved more efficient at 5 µM concentration which can be accounted for by different dose–response curves or additional, detrimental activities at very high concentrations. The strongest effect was observed for three substances: the flavonoid quercetin (3′,4′,5,7-tetrahydroxyflavon-3-ol), the flavonoid formononetin (7-hydroxy-3-(4-methoxyphenyl)-4H-chromen-4-one), and the alkaloid aristolactam BII (1,2-dimethoxydibenzo[cd,f]indol-4(5H)-one) (Fig. 1e–h). We selected two substances representing different classes of natural products for more detailed studies, the alkaloid aristolactam BII and the flavonoid quercetin. While protective effects of both flavonoids were previously recognized in AD [33, 34], the literature search revealed that only for quercetin it was demonstrated that it mediates reduction of Aβ secretion in mammalian cells and protects age-associated neurodegeneration in vivo [35]. Therefore, we decided to verify whether our screen reveals also a novel, protective function of this substance. Of note, the glycosylated form of quercetin, rutin, to a smaller extent, also inhibited Aβ3(pE)-42 uptake [36] (Fig. 1e–h).
Aβ3(pE)-42 is not taken up by neurons and does not associate with neuronal membranes [19]. Its neurotoxic effects are a consequence of astrocytic uptake, subsequent astroglial activation, and release of synaptotoxic, proinflammatory TNFα [18, 19]. Therefore, we next used primary, mixed, astrocytic-neuronal cultures to further characterize quercetin and aristolactam BII. A hallmark of amyloid-pathology in AD is decreased phosphorylation of neuronal transcription factor cAMP response element-binding protein (CREB), leading to its transcriptional inactivation termed CREB shutoff [37]. Transcriptional inactivation of neuronal CREB leads to the abolishment of pro-survival gene expression and hence the activation of pro-apoptotic signaling [38]. We therefore assessed CREB shutoff in mixed hippocampal cultures with a pCREB-specific antibody detecting Ser133 phosphorylated CREB (Fig. 2a, b). As reported previously, the addition of 500 nM Aβ3(pE)-42 to these cultures resulted in robust neuronal CREB shutoff [19]. Interestingly, however, co-application of quercetin to the medium attenuated CREB shutoff (Fig. 2a, b). Thus, quercetin appears to be effective to reduce measures of early neuronal dysfunction in primary cell cultures. The second candidate effectively blocking Aβ3(pE)-42 accumulation in astrocyte, aristolactam BII, did not rescue Aβ3(pE)-42-induced CREB shutoff (Fig. S4a, b). Therefore, we focused on quercetin as the most promising candidate to efficiently block Aβ3(pE)-42 uptake (Fig. 1, Fig. S5). Interestingly, we found that the substance was effective in preventing uptake of Aβ3(pE)-42 to HEK293T cells (Fig. S6a–d), pointing to a general role in preventing cellular accumulation of this causative agent for AD pathology.
Quercetin rescues Aβ3(pE)-42-induced CREB shutoff and loss of synapse density in mixed hippocampal cultures. a, b Co-application of quercetin prevents Aβ3(pE)-42-induced loss in CREB Ser133 phosphorylation (CREB shutoff). a Representative confocal images of DIV18 mixed, neuronal-astrocytic cultures treated with 50 μM quercetin, 500 nM Aβ3(pE)-42 oligomers or 50 μM quercetin, and 500 nM Aβ3(pE)-42 oligomers for 72 h. Neurons were stained with MAP2 and pCREB antibodies and co-stained with DAPI. Scale bar is 10 μm. Lookup table indicates the pixel intensities from 0 to 255. b Mean pCREB fluorescence intensity within nuclear region (defined by DAPI) normalized to control. N = 46–53 nuclei from two independent cell cultures. c, d Co-application of quercetin prevents Aβ3(pE)-42-induced synapse loss. c Representative, confocal images of DIV18 mixed, neuronal-astrocytic cultures treated with 50 μM quercetin, 500 nM Aβ3(pE)-42 oligomers or 50 μM quercetin, and 500 nM Aβ3(pE)-42 oligomers for 48 h. Neurons were stained with Synaptophysin-1, PSD95, and MAP2 antibodies. Individual synapse was defined as overlapping or opposing Synaptophysin-1 and PSD95 immunosignal. Scale bar is 5 μm. d Mean number of synapses per 1 μm. N = 19–22 dendritic segments from at least two independent cultures. b, d **p < 0.01, ****p < 0.0001 by two-way ANOVA with post hoc Tukey test. Data are presented as mean \(\pm\) s.e.m
The dephosphorylation of CREB at a crucial serine at position 133 (Fig. 2a, b) is tightly linked to Aβ-induced early synaptic dysfunction and synapse loss [37]. Alterations in synaptic structure and number can be observed relatively early and were also reported in in vitro AD models using mixed hippocampal cell cultures [4, 19] and we have already demonstrated that Aβ3(pE)-42-induced, proinflammatory signaling is synaptotoxic [18, 19]. We followed up on this observation and quantified synapse density in hippocampal primary neurons at DIV16-18 (Fig. 2c, d). A single synapse was defined as overlapping or opposing immunosignals of Synaptophysin-1 and PSD95 (pre-and postsynaptic marker respectively; Fig. 2c, d). In accord to a previous study, we found clear synapse loss in response to Aβ3(pE)-42 application to the cell culture medium [19]. Like in previous work, this loss was visible after 72 h and we have shown that it is induced by astroglial release of TNFα [19]. In support of a role in blocking Aβ3(pE)-42 astroglial uptake, co-application of quercetin to mixed hippocampal cultures significantly reduced this synapse loss (Fig. 2c, d).
The earliest phase of AD, often called “cellular” phase, is characterized by gradual alterations in neuronal and glial cells [1, 4, 6, 7, 39]. To verify, whether Aβ3(pE)-42 is endocytosed by astrocytes, we treated astrocytes with dynasore, a potent endocytosis inhibitor [40]. The co-application with dynasore revealed significant decrease in Aβ3(pE)-42 area, number of deposits, and the mean size of Aβ3(pE)-42 deposits (Fig. S7a–d). Next, we used TMR-dextran, an endolysosomal fluorescent marker [41]. We incubated dextran or dextran with Aβ3(pE)-42 for 2 h, followed by 2 h chase (Fig. 3a–c, Fig. S7e). Our data revealed that the vast majority (75%) of Aβ3(pE)-42 puncta localized in the astrocytic endolysosomal compartment. Importantly, we observed that neither quercetin nor Aβ3(pE)-42 affect the overall endocytosis rate measured by number of dextran puncta normalized to the area of astrocytes (Fig. 3d, e). In accordance with previous results (Fig. 1, Fig. S5), we observed decreased amounts of intracellular Aβ3(pE)-42. All in all, the data indicate that quercetin selectively prevents Aβ3(pE)-42 endocytosis.
Quercetin prevents Aβ3(pE)-42 endocytosis. a–c Co-application of TMR-dextran and Aβ3(pE)-42 revealed prominent Aβ3(pE)-42 localization to the astrocytic endolysosomal system. a Representative, confocal images of primary astrocytes incubated with 5 mM TMR-dextran and 500 nM Aβ3(pE)-42. The dashed white line indicates the region along which the line profile was created. Scale bar is 10 µm. b The line profile of normalized mean grey values from the dextran and Aβ3(pE)-42 channel shows significant localization of Aβ3(pE)-42 to dextran-labeled endolysosomes. c Mean number of Aβ3(pE)-42 puncta (as % of total Aβ3(pE)-42 puncta within one cell) positive for TMR-dextran. N = 30 cells from two independent cultures. d, e Quercetin and Aβ3(pE)-42 do not influence general astrocytic endocytosis rate. d Representative, confocal images of primary astrocytes incubated with TMR-dextran with 50 µM quercetin, 500 nM Aβ3(pE)-42, or 500 nM Aβ3(pE)-42 + 50 µM quercetin. Scale bar is 30 µm. The image of the cell in a is a zoomed image of the Aβ3(pE)-42-treated group. e Box-whisker plot of the number of dextran puncta normalized to astrocytic area (defined by GFAP). Whiskers denote minimum and maximum value. Median is indicated within bar. N = 30–71 cells from two independent cell cultures. Ns for p > 0.05 by Kruskal–Wallis test followed by Dunn’s multiple comparisons test
Quercetin is a polyphenolic compound found in a variety of plants. It has many documented biological effects and a prominent anti-inflammatory action in a wide range of assays [33], including senolytic effects in senescent tissue [42, 43]. To test whether the protective effect of quercetin is associated with glia activation, we employed organotypic hippocampal slices, a three-dimensional culture system that preserves basic circuitry and cellular organization and that is therefore well suited to study glial proliferation as well as Aβ3(pE)-42 internalization. A common feature observed in AD is the transition of astrocytes to a state of reactive astrogliosis [6,7,8]. In previous work, it has been shown by us and others that oligomeric Aβ3(pE)-42 species induce a prominent glial inflammatory response that comes along with an increase in reactive GFAP-positive astroglia [6,7,8, 19]. Accordingly, we found that bath application of Aβ3(pE)-42 clearly increased GFAP-immunoreactivity in these slices (Fig. 4a, b), which is a measure of reactive astrogliosis [44]. When we co-administered quercetin at a concentration of 50 μM, the Aβ3(pE)-42-induced increase in GFAP-positive reactive astroglia was no longer visible (Fig. 4a, b). The same effect was observed for intermediate filament vimentin, another marker of reactive astrocytes [44] (Fig. 4c, d).
Quercetin prevents upregulation of GFAP and vimentin in astrocytes. a–d Co-application of quercetin prevents Aβ3(pE)-42-induced increased a, b GFAP or c, d vimentin immunoreactivity in organotypic hippocampal slices (OHSC). a Representative confocal images of DIV8 OHSC treated with 50 μM quercetin, 500 nM Aβ3(pE)-42 oligomers or 50 μM quercetin, and 500 nM Aβ3(pE)-42 oligomers for 24 h. OHSC were stained with antibody detecting GFAP and co-stained with DAPI (nuclear marker). Scale bar is 15 μm. Lookup table indicates the pixel intensities from 0 to 255. b Mean GFAP fluorescence intensity normalized to control. N = 14–16 ROIs from at least five slices per group from two independent cultures. c Representative confocal images of DIV8-15 OHSC treated with 50 μM quercetin, 500 nM Aβ3(pE)-42 oligomers or 50 μM quercetin, and 500 nM Aβ3(pE)-42 oligomers for 24 h. OHSC were stained with antibody detecting vimentin and co-stained with DAPI (nuclear marker). Scale bar is 15 μm. Lookup table indicates the pixel intensities from 0 to 255. d Mean vimentin fluorescence intensity normalized to control. N = 24–27 ROIs from at least three slices per group from two independent experiments. *p < 0.05, **p < 0.01, ***p < 0.001, ****p < 0.0001 by Kruskal–Wallis test followed by Dunn’s multiple comparisons test. Data are presented as mean \(\pm\) s.e.m
Aβ3(pE)-42-induced glia activation leads to an impairment in synaptic function [19]. Therefore, to see whether quercetin can rescue synaptic impairment, we next moved to acute hippocampal slices. Long-term potentiation (LTP) at hippocampal Schaffer collateral synapses is considered to be a cellular model of learning and memory [45] and this type of synaptic plasticity is very early on interrupted by oligomeric Aβ [19, 28, 46, 47]. Field recordings revealed a severe impairment of the late phase of LTP, following 2-h pre-treatment and administration of oligomeric Aβ3(pE)-42 to the perfusion medium at a concentration of 500 nM (Fig. 5a, b). The reduced field excitatory postsynaptic potential (fEPSP) following induction of LTP is a common readout of the efficacy of oligomer preparation and therefore indicates that our preparation indeed resulted in the formation of synaptotoxic Aβ3(pE)-42 species like reported previously [19]. In line with a role of quercetin in the inhibition of oligomeric Aβ3(pE)-42 endocytosis in astrocytes, we observed a stunning rescue of late-phase LTP in slices co-treated with quercetin (Fig. 5c–f). The substance as such had no effect on the fEPSP during the time of recording (Fig. 5d).
Quercetin rescues Aβ3(pE)-42-induced late LTP impairment. a–d LTP recordings revealed that a 2-h pre-treatment with Aβ3(pE)-42 oligomers causes impairment of late phase LTP, which is rescued by application of c quercetin, compared to control measurements. Accordingly, to the experimental group, the oligomers and quercetin were present in the bath during recordings. Insets show representative fEPSP analog traces at indicated time points: 1 = baseline, 2 = late LTP. b, d Basal synaptic transmission is not affected by bath application of b Aβ3(pE)-42 oligomers compared to a control and d by quercetin applied alone or with Aβ3(pE)-42 oligomers. e, f Dot plot representing e Aβ3(pE)-42-induced late phase LTP rescue by quercetin, while f early LTP and induction phase are not affected. N = 18 slices per group from at least six mice. e, f ***p < 0.001. ****p < 0.0001 by two-way ANOVA with Tukey’s multiple comparison test. Data are presented as mean \(\pm\) s.e.m
Discussion
Collectively, our data show that a simple screening approach can be used to identify bioactive substances extracted from plants that have neuroprotective effects based on the inhibition of oligomeric Aβ3(pE)-42 uptake to astrocytes. As proof of principle, we followed up on the neuroprotective effects of two hits from this first set of substances. While aristolactam BII did not prove efficient in preventing neuronal CREB shutoff, we identified a novel biological activity of quercetin—the prevention of Aβ3(pE)-42 astrocytic uptake, and, as a consequence, neuronal synaptic dysfunction and synapse loss.
Although it is well known that astrocytes endocytose neurodegeneration-associated proteins such as Aβ [7, 39, 48], the link between Aβ uptake, astrogliosis, and the disease onset and progression is unclear. The astrocytic phagocytic activity may result in neuroprotective reduction of Aβ concentration [49, 50]. On the other side, it was previously reported that the disruption of the astrocytic endolysosomal system is associated with AD progression [51, 52]. Among numerous posttranslationally modified Aβ species, Aβ3(pE)-42 is the most prominent one [53, 54]. Interestingly, unlike other Aβ forms, Aβ3(pE)-42 does not associate with neuronal membranes and is not taken up by neurons [19]. Instead, the oligomers are taken up by astrocytes, and accumulate in the endolysosomal system, which leads to its disruption and lysosomal membrane permeabilization [18, 19]. The intracellular leakage of lysosomal content induces upregulation of the proinflammatory signaling and release of TNFα, which drives Aβ3(pE)-42-induced synaptic stripping and LTP impairment [19]. This can be assigned to the unique biophysical properties of Aβ3(pE)-42, which displays higher propensity to aggregate and to form fibrillar species [55, 56]. Indeed, accumulation of fibrillar α-synuclein was reported to induce a lysosomal stress response characterized by loss of membrane integrity, disrupted catabolism and acidification, enlarged size, and increase in reactive oxygen species production [48, 57,58,59]. Thus, disruption of the endolysosomal system may result in a chronic inflammatory response that eventually leads to the release of proinflammatory cytokines and concomitant loss of physiological astrocytic functions, which in turn contribute to early synaptic dysfunction in AD [1, 60,61,62,63]. Very few approaches have centered on this process as a potential therapeutic target. We therefore aimed to identify plant-based substances with known biological activity that might interfere with Aβ3(pE)-42 uptake in astrocytes.
A long list of compounds deriving from herbal medicine have been in use or proposed for the treatment of neurological conditions, such as multiple forms of dementia, including AD [33, 64,65,66,67,68]. Plant-based substances are usually well tolerated and also well accepted as treatment options by the general public. This also applies to quercetin, which is a common component of food plants and even in clinical use for conditions of the heart and blood vessels and to prevent cancer [33, 69]. Its consumption is well tolerated and it has been safely used in doses up to 1 g daily for 12 weeks [69]. It has been previously reported that quercetin has antioxidant and anti-inflammatory effects [33, 70], which are probably its most prominent biological activities. Accordingly, quercetin has been shown to reduce neuronal cell death resulting from glutamate excitotoxicity [70, 71]. Recently, it has become the hallmark senolytic natural product for (synergistic) treatment of cancer and age-related diseases [33, 42, 43].
Furthermore, higher dietary intake of quercetin correlates with a slower rate of cognitive decline in healthy elderly individuals [72]. While the bioavailability of quercetin is low, and oral bioavailability and conversion of its glycones strongly depend on the gut microbiome [73, 74], the use of drug delivery systems, like nanosuspensions, can improve its oral adsorption [75]. Furthermore, its ability and rates to cross the blood–brain barrier require further investigation [33, 76, 77]. Likewise, the concentration-dependent effects on neuronal and glial cells warrant further studies. Some reports suggest that, depending on concentration and its metabolism, quercetin may exert the neuroprotective or neurotoxic function [77,78,79]. In this regard, the presence of glia in the in vitro system seems to be crucial, as glial metabolism of quercetin into glutathione conjugates leads to the reduction of neurotoxic effects of quercetin [80]. These findings also account for the fact that we did not observe any neurotoxic effects, in our mixed co-culture system containing both neurons and astrocytes or quercetin-dependent increase in neuronal CREB phosphorylation [78]. Along these lines, although quercetin acts as a phosphoinositide (PI) 3-kinase inhibitor which could potentially lead to the disruption in membrane trafficking [81,82,83], the dextran assay did not reveal any impairment in astrocytic endocytosis. Nevertheless, various neuroprotective effects have been reported for quercetin in various disease states including mouse models of AD [33, 72]. Interestingly, a recent study revealed that quercetin decreases the amount of secreted Aβ and rescued toxic effects of Aβ in vivo [35].
Here, using exogenously applied oligomers at defined concentration, we report a hitherto unknown biological activity that might become relevant in the context of amyloid-pathology in the brain. We found that quercetin efficiently blocked the endocytosis and accumulation of Aβ3(pE)-42 in astrocytes. At present, the mechanism by which quercetin exerts its effect on astrocytic Aβ3(pE)-42 accumulation is unclear. Since the dextran uptake assay revealed that quercetin has not significantly altered the overall endocytosis rate, a plausible explanation is that quercetin sequesters Aβ3(pE)-42 oligomers, thus preventing binding to astrocytic endocytic receptors [84]. It was shown that quercetin can bind to fibrillar α-synuclein and Aβ [85, 86]. Since pyroglutaminylation increases the hydrophobicity of soluble Aβ oligomers, this Aβ modification could facilitate binding to hydrophobic quercetin in a similar manner like to fibrillar species [87,88,89]. Another intriguing possibility concerns the regulation of ApoE expression and function. The APOEε4 gene is a genetic risk factor for LOAD, likely through its strong effect on the accumulation of Aβ [51, 90]. ApoE is mainly produced by astrocytes and astrocyte-derived ApoE is pivotal for clearance of oligomeric Aβ [51, 90, 91]. It was shown that quercetin increases ApoE levels most likely by inhibiting ApoE degradation [92]. While this might be an important aspect with respect to a long-term treatment, we here report an effect that is rather rapid and will occur before regulation of gene expression might kick in. Thus, the acute consequences of quercetin are likely a reduced uptake of Aβ3(pE)-42. Furthermore, other effects of long-term quercetin administration in vivo and in vitro on gene networks that were analyzed in silico and that might provide neuroprotection in the context of AD [33, 35, 93, 94] are unlikely to contribute to the acute effects of quercetin on the accumulation of Aβ3(pE)-42 in astrocytes.
Uptake of oligomeric Aβ has been shown for several different cell types [1, 8]. The mechanisms are to a large extent unclear and might in fact differ between neurons, microglia, and astrocytes [52]. Since quercetin also blocked uptake of Aβ3(pE)-42 in HEK293T cells, we speculate that the mechanism underlying its action is of general relevance. A direct interaction of quercetin with Aβ3(pE)-42 would explain the observed effects. Such a direct interaction was indeed recently reported for full-length Aβ [95]. Other studies have shown that OH groups and phenolic rings in flavonoids are essential for the noncovalent interactions with β-sheet structures, which are common to all amyloid proteins [96]. A consequence of quercetin binding to full length Aβ seems to be the prevention of fibril formation [95]. While it is unclear whether this also applies to Aβ3(pE)-42 quercetin binding, subsequent prevention of oligomerization cannot account for the effect of quercetin on Aβ3(pE)-42 accumulation in astrocytes since we have used preformed oligomers. However, if quercetin binds to oligomerized Aβ3(pE)-42, it is possible that this binding will hinder uptake.
Taken together, our study demonstrates that quercetin, by yet unknown mechanism, efficiently blocks astrocytic uptake of Aβ3(pE)-42 thus preventing Aβ3(pE)-42-induced synaptic impairment. In conjunction with other published work, these results point to a plausible scenario where this flavonoid is effective in preventing amyloid pathology by simultaneously influencing Aβ endocytosis, metabolism, and assembly of Aβ oligomeric species.
Data Availability
The original contributions presented in the study are included in the article/Supplementary Material. The datasets and material used in the study are available from corresponding authors on reasonable request.
References
Selkoe DJ, Hardy J (2016) The amyloid hypothesis of Alzheimer’s disease at 25 years. EMBO Mol Med 8(6):595–608. https://doi.org/10.15252/emmm.201606210
Mondragón JD, Maurits NM, De Deyn PP (2021) Functional connectivity differences in Alzheimer’s disease and amnestic mild cognitive impairment associated with AT(N) classification and anosognosia. Neurobiol Aging 101:22–39. https://doi.org/10.1016/j.neurobiolaging.2020.12.021
Haass C, Selkoe D (2022) If amyloid drives Alzheimer disease, why have anti-amyloid therapies not yet slowed cognitive decline? PLoS Biol 20(7):e3001694. https://doi.org/10.1371/journal.pbio.3001694
Selkoe DJ (2002) Alzheimer’s disease is a synaptic failure. Science 298(5594):789–791. https://doi.org/10.1126/science.1074069
Shankar GM, Bloodgood BL, Townsend M, Walsh DM, Selkoe DJ, Sabatini BL (2007) Natural oligomers of the Alzheimer amyloid-beta protein induce reversible synapse loss by modulating an NMDA-type glutamate receptor-dependent signaling pathway. J Neurosci 27(11):2866–2875. https://doi.org/10.1523/jneurosci.4970-06.2007
Heneka MT, Carson MJ, El Khoury J, Landreth GE, Brosseron F, Feinstein DL, Jacobs AH, Wyss-Coray T et al (2015) Neuroinflammation in Alzheimer’s disease. Lancet Neurol 14(4):388–405. https://doi.org/10.1016/s1474-4422(15)70016-5
Osborn LM, Kamphuis W, Wadman WJ, Hol EM (2016) Astrogliosis: an integral player in the pathogenesis of Alzheimer’s disease. Prog Neurobiol 144:121–141. https://doi.org/10.1016/j.pneurobio.2016.01.001
Sadick JS, Liddelow SA (2019) Don’t forget astrocytes when targeting Alzheimer’s disease. Br J Pharmacol 176(18):3585–3598. https://doi.org/10.1111/bph.14568
Hong S, Beja-Glasser VF, Nfonoyim BM, Frouin A, Li S, Ramakrishnan S, Merry KM, Shi Q et al (2016) Complement and microglia mediate early synapse loss in Alzheimer mouse models. Science 352(6286):712–716. https://doi.org/10.1126/science.aad8373
Hulshof LA, van Nuijs D, Hol EM, Middeldorp J (2022) The role of astrocytes in synapse loss in Alzheimer’s disease: a systematic review. Front Cell Neurosci 16:899251. https://doi.org/10.3389/fncel.2022.899251
Rodríguez-Arellano JJ, Parpura V, Zorec R, Verkhratsky A (2016) Astrocytes in physiological aging and Alzheimer’s disease. Neuroscience 323:170–182. https://doi.org/10.1016/j.neuroscience.2015.01.007
Brandebura AN, Paumier A, Onur TS, Allen NJ (2023) Astrocyte contribution to dysfunction, risk and progression in neurodegenerative disorders. Nat Rev Neurosci 24(1):23–39. https://doi.org/10.1038/s41583-022-00641-1
Kummer MP, Heneka MT (2014) Truncated and modified amyloid-beta species. Alzheimers Res Ther 6(3):28. https://doi.org/10.1186/alzrt258
Bayer TA, Wirths O (2014) Focusing the amyloid cascade hypothesis on N-truncated Abeta peptides as drug targets against Alzheimer’s disease. Acta Neuropathol 127(6):787–801. https://doi.org/10.1007/s00401-014-1287-x
Nussbaum JM, Schilling S, Cynis H, Silva A, Swanson E, Wangsanut T, Tayler K, Wiltgen B et al (2012) Prion-like behaviour and tau-dependent cytotoxicity of pyroglutamylated amyloid-β. Nature 485(7400):651–655. https://doi.org/10.1038/nature11060
Hielscher-Michael S, Griehl C, Buchholz M, Demuth HU, Arnold N, and Wessjohann LA (2016) Natural Products from microalgae with potential against Alzheimer’s disease: sulfolipids sre potent glutaminyl cyclase inhibitors. Mar Drugs 14(11) https://doi.org/10.3390/md14110203
Newman DJ, Cragg GM (2020) Natural products as sources of new drugs over the nearly four decades from 01/1981 to 09/2019. J Nat Prod 83(3):770–803. https://doi.org/10.1021/acs.jnatprod.9b01285
Wirth S, Schlößer A, Beiersdorfer A, Schweizer M, Woo MS, Friese MA, Lohr C, and Grochowska KM Astrocytic uptake of posttranslationally modified amyloid-β leads to endolysosomal system disruption and induction of pro-inflammatory signaling. Glia n/a(n/a) https://doi.org/10.1002/glia.24539
Grochowska KM, Yuanxiang P, Bär J, Raman R, Brugal G, Sahu G, Schweizer M, Bikbaev A et al (2017) Posttranslational modification impact on the mechanism by which amyloid-β induces synaptic dysfunction. EMBO Rep 18(6):962–981. https://doi.org/10.15252/embr.201643519
Alexandru A, Jagla W, Graubner S, Becker A, Bäuscher C, Kohlmann S, Sedlmeier R, Raber KA et al (2011) Selective hippocampal neurodegeneration in transgenic mice expressing small amounts of truncated Aβ is induced by pyroglutamate-Aβ formation. J Neurosci: off J Soc Neurosci 31(36):12790–12801. https://doi.org/10.1523/JNEUROSCI.1794-11.2011
Krajnović T, Kaluđerović GN, Wessjohann LA, Mijatović S, Maksimović-Ivanić D (2016) Versatile antitumor potential of isoxanthohumol: enhancement of paclitaxel activity in vivo. Pharmacol Res 105:62–73. https://doi.org/10.1016/j.phrs.2016.01.011
Williamson EM, Liu X, Izzo AA (2020) Trends in use, pharmacology, and clinical applications of emerging herbal nutraceuticals. Br J Pharmacol 177(6):1227–1240. https://doi.org/10.1111/bph.14943
Noori T, Dehpour AR, Sureda A, Sobarzo-Sanchez E, Shirooie S (2021) Role of natural products for the treatment of Alzheimer’s disease. Eur J Pharmacol 898:173974. https://doi.org/10.1016/j.ejphar.2021.173974
Deshpande P, Gogia N, Singh A (2019) Exploring the efficacy of natural products in alleviating Alzheimer’s disease. Neural Regen Res 14(8):1321–1329. https://doi.org/10.4103/1673-5374.253509
Mattioli R, Francioso A, d’Erme M, Trovato M, Mancini P, Piacentini L, Casale AM, Wessjohann L, et al (2019) Anti-inflammatory activity of a polyphenolic extract from Arabidopsis thaliana in in vitro and in vivo models of Alzheimer’s disease. Int J Mol Sci 20(3) https://doi.org/10.3390/ijms20030708
Michels B, Zwaka H, Bartels R, Lushchak O, Franke K, Endres T, Fendt M, Song I et al (2018) Memory enhancement by ferulic acid ester across species. Sci Adv 4(10):eaat6994. https://doi.org/10.1126/sciadv.aat6994
Schindelin J, Arganda-Carreras I, Frise E, Kaynig V, Longair M, Pietzsch T, Preibisch S, Rueden C et al (2012) Fiji: an open-source platform for biological-image analysis. Nat methods 9(7):676–682. https://doi.org/10.1038/nmeth.2019
Yuan Xiang P, Janc O, Grochowska KM, Kreutz MR, Reymann KG (2016) Dopamine agonists rescue Aβ-induced LTP impairment by Src-family tyrosine kinases. Neurobiol Aging 40:98–102. https://doi.org/10.1016/j.neurobiolaging.2016.01.008
Häke I, Schönenberger S, Neumann J, Franke K, Paulsen-Merker K, Reymann K, Ismail G, Bin Din L et al (2009) Neuroprotection and enhanced neurogenesis by extract from the tropical plant Knema laurina after inflammatory damage in living brain tissue. J Neuroimmunol 206(1–2):91–99. https://doi.org/10.1016/j.jneuroim.2008.10.007
Thuy TT, Porzel A, Franke K, Wessjohann L, Sung TV (2005) Isoquinolone and protoberberine alkaloids from Stephania rotunda. Pharmazie 60(9):701–704
Rizzo P, Altschmied L, Stark P, Rutten T, Gündel A, Scharfenberg S, Franke K, Bäumlein H et al (2019) Discovery of key regulators of dark gland development and hypericin biosynthesis in St. John’s Wort (Hypericum perforatum). Plant Biotechnol J 17(12):2299–2312. https://doi.org/10.1111/pbi.13141
Ware I, Franke K, Dube M, Ali El Enshasy H, Wessjohann LA (2023) Characterization and bioactive potential of secondary metabolites isolated from Piper sarmentosum Roxb. Int J Mol Sci 24(2):1328
Deepika and Maurya PK (2022) Health benefits of quercetin in age-related diseases. Molecules 27(8) https://doi.org/10.3390/molecules27082498
Geng L-M, Jiang J-G (2022) The neuroprotective effects of formononetin: signaling pathways and molecular targets. J Funct Foods 88:104911. https://doi.org/10.1016/j.jff.2021.104911
Schiavi A, Cirotti C, Gerber L-S, Di Lauro G, Maglioni S, Shibao PYT, Montresor S, Kirstein J et al (2023) Abl depletion via autophagy mediates the beneficial effects of quercetin against Alzheimer pathology across species. Cell Death Discovery 9(1):376. https://doi.org/10.1038/s41420-023-01592-x
Ulusoy HG, Sanlier N (2020) A minireview of quercetin: from its metabolism to possible mechanisms of its biological activities. Crit Rev Food Sci Nutr 60(19):3290–3303. https://doi.org/10.1080/10408398.2019.1683810
Grochowska KM, Gomes GM, Raman R, Kaushik R, Sosulina L, Kaneko H, Oelschlegel AM, Yuanxiang P, et al (2023) Jacob-induced transcriptional inactivation of CREB promotes Aβ-induced synapse loss in Alzheimer’s disease. The EMBO Journal n/a(n/a):e112453. https://doi.org/10.15252/embj.2022112453
Hardingham GE, Bading H (2010) Synaptic versus extrasynaptic NMDA receptor signalling: implications for neurodegenerative disorders. Nat Rev Neurosci 11(10):682–696. https://doi.org/10.1038/nrn2911
Brandebura AN, Paumier A, Onur TS, Allen NJ (2022) Astrocyte contribution to dysfunction, risk and progression in neurodegenerative disorders. Nat Rev Neurosci. https://doi.org/10.1038/s41583-022-00641-1
Macia E, Ehrlich M, Massol R, Boucrot E, Brunner C, Kirchhausen T (2006) Dynasore, a cell-permeable inhibitor of dynamin. Dev Cell 10(6):839–850. https://doi.org/10.1016/j.devcel.2006.04.002
Potokar M, Jorgačevski J, Zorec R (2021) Methods for monitoring endocytosis in astrocytes. Methods Mol Biol 2233:93–100. https://doi.org/10.1007/978-1-0716-1044-2_6
Alharbi KS, Afzal O, Altamimi ASA, Almalki WH, Kazmi I, Al-Abbasi FA, Alzarea SI, Makeen HA et al (2022) A study of the molecular mechanism of quercetin and dasatinib combination as senolytic in alleviating age-related and kidney diseases. J Food Biochem 46(12):e14471. https://doi.org/10.1111/jfbc.14471
Gonzales MM, Garbarino VR, Marques Zilli E, Petersen RC, Kirkland JL, Tchkonia T, Musi N, Seshadri S et al (2022) Senolytic therapy to modulate the progression of Alzheimer’s disease (SToMP-AD): a pilot clinical trial. J Prev Alzheimers Dis 9(1):22–29. https://doi.org/10.14283/jpad.2021.62
Escartin C, Galea E, Lakatos A, O’Callaghan JP, Petzold GC, Serrano-Pozo A, Steinhäuser C, Volterra A et al (2021) Reactive astrocyte nomenclature, definitions, and future directions. Nat Neurosci 24(3):312–325. https://doi.org/10.1038/s41593-020-00783-4
Lynch MA (2004) Long-term potentiation and memory. Physiol Rev 84(1):87–136. https://doi.org/10.1152/physrev.00014.2003
Rönicke R, Mikhaylova M, Rönicke S, Meinhardt J, Schröder UH, Fändrich M, Reiser G, Kreutz MR et al (2011) Early neuronal dysfunction by amyloid β oligomers depends on activation of NR2B-containing NMDA receptors. Neurobiol Aging 32(12):2219–2228. https://doi.org/10.1016/j.neurobiolaging.2010.01.011
Lambert MP, Barlow AK, Chromy BA, Edwards C, Freed R, Liosatos M, Morgan TE, Rozovsky I et al (1998) Diffusible, nonfibrillar ligands derived from Abeta1-42 are potent central nervous system neurotoxins. Proc Natl Acad Sci U S A 95(11):6448–6453. https://doi.org/10.1073/pnas.95.11.6448
Wong CO (2020) Endosomal-lysosomal processing of neurodegeneration-associated proteins in astrocytes. Int J Mol Sci 21(14) https://doi.org/10.3390/ijms21145149
Kim S, Chun H, Kim Y, Kim Y, Park U, Chu J, Bhalla M, Choi S-H et al (2024) Astrocytic autophagy plasticity modulates Aβ clearance and cognitive function in Alzheimer’s disease. Mol Neurodegener 19(1):55. https://doi.org/10.1186/s13024-024-00740-w
Jiwaji Z, Tiwari SS, Avilés-Reyes RX, Hooley M, Hampton D, Torvell M, Johnson DA, McQueen J et al (2022) Reactive astrocytes acquire neuroprotective as well as deleterious signatures in response to Tau and Aß pathology. Nat Commun 13(1):135. https://doi.org/10.1038/s41467-021-27702-w
Prasad H, Rao R (2018) Amyloid clearance defect in ApoE4 astrocytes is reversed by epigenetic correction of endosomal pH. Proc Natl Acad Sci 115(28):E6640–E6649. https://doi.org/10.1073/pnas.1801612115
Wegiel J, Wang KC, Tarnawski M, Lach B (2000) Microglial cells are the driving force in fibrillar plaque formation, whereas astrocytes are a leading factor in plaque degradation. Acta Neuropathol 100(4):356–364. https://doi.org/10.1007/s004010000199
Jawhar S, Wirths O, Bayer TA (2011) Pyroglutamate amyloid-β (Aβ): a hatchet man in Alzheimer disease*. J Biol Chem 286(45):38825–38832. https://doi.org/10.1074/jbc.R111.288308
Saido TC, Iwatsubo T, Mann DMA, Shimada H, Ihara Y, Kawashima S (1995) Dominant and differential deposition of distinct β-amyloid peptide species, AβN3(pE), in senile plaques. Neuron 14(2):457–466. https://doi.org/10.1016/0896-6273(95)90301-1
Schlenzig D, Rönicke R, Cynis H, Ludwig H-H, Scheel E, Reymann K, Saido T, Hause G et al (2012) N-Terminal pyroglutamate formation of Aβ38 and Aβ40 enforces oligomer formation and potency to disrupt hippocampal long-term potentiation. J Neurochem 121(5):774–784. https://doi.org/10.1111/j.1471-4159.2012.07707.x
Wulff M, Baumann M, Thümmler A, Yadav JK, Heinrich L, Knüpfer U, Schlenzig D, Schierhorn A et al (2016) Enhanced fibril fragmentation of N-terminally truncated and pyroglutamyl-modified Aβ peptides. Angew Chem Int Ed 55(16):5081–5084. https://doi.org/10.1002/anie.201511099
Bonam SR, Wang F, Muller S (2019) Lysosomes as a therapeutic target. Nat Rev Drug Discovery 18(12):923–948. https://doi.org/10.1038/s41573-019-0036-1
Lakpa KL, Khan N, Afghah Z, Chen X, Geiger JD (2021) Lysosomal stress response (LSR): physiological importance and pathological relevance. J Neuroimmune Pharmacol 16(2):219–237. https://doi.org/10.1007/s11481-021-09990-7
Bourdenx M, Bezard E, Dehay B (2014) Lysosomes and α-synuclein form a dangerous duet leading to neuronal cell death. Front Neuroanat 8:83. https://doi.org/10.3389/fnana.2014.00083
Yambire KF, Rostosky C, Watanabe T, Pacheu-Grau D, Torres-Odio S, Sanchez-Guerrero A, Senderovich O, Meyron-Holtz EG et al (2019) Impaired lysosomal acidification triggers iron deficiency and inflammation in vivo. eLife 8:e51031. https://doi.org/10.7554/eLife.51031
Barlan AU, Danthi P, Wiethoff CM (2011) Lysosomal localization and mechanism of membrane penetration influence nonenveloped virus activation of the NLRP3 inflammasome. Virology 412(2):306–314. https://doi.org/10.1016/j.virol.2011.01.019
Couturier J, Stancu IC, Schakman O, Pierrot N, Huaux F, Kienlen-Campard P, Dewachter I, Octave JN (2016) Activation of phagocytic activity in astrocytes by reduced expression of the inflammasome component ASC and its implication in a mouse model of Alzheimer disease. J Neuroinflammation 13:20. https://doi.org/10.1186/s12974-016-0477-y
Giovannoni F, Quintana FJ (2020) The role of astrocytes in CNS inflammation. Trends Immunol 41(9):805–819. https://doi.org/10.1016/j.it.2020.07.007
Barnes JE, Anderson LA, Phillipson JD (2002) Herbal medicine: a guide for health care professionals, 2nd edn. Pharmaceutical Press, UK
Kaushik R, Morkovin E, Schneeberg J, Confettura AD, Kreutz MR, Senkov O, Dityatev A (2018) Traditional Japanese herbal medicine Yokukansan targets distinct but overlapping mechanisms in aged mice and in the 5xFAD mouse model of Alzheimer’s disease. Front Aging Neurosci 10:411. https://doi.org/10.3389/fnagi.2018.00411
Dey A, Bhattacharya R, Mukherjee A, Pandey DK (2017) Natural products against Alzheimer’s disease: pharmaco-therapeutics and biotechnological interventions. Biotechnol Adv 35(2):178–216. https://doi.org/10.1016/j.biotechadv.2016.12.005
Cheung TS, Song TH, Ng TB, Wu FH, Lao LX, Tang SC, Ho JC, Zhang KY et al (2015) Therapeutic effects of herbal chemicals in traditional Chinese medicine on Alzheimer’s disease. Curr Med Chem 22(19):2392–2403. https://doi.org/10.2174/0929867322666150520095509
Michels B, Gerber B, Wessjohann L, Franke K, Sigrist S, Bhukel A, Lushchak O, Zwaka H, Bartels R, Dityatev A, Song I, Fendt M, Leßmann V, Endres T, and Kähne T (2019) Verbindung zur Anwendung bei der Steigerung von mentaler Leistungsfähigkeit
Andres S, Pevny S, Ziegenhagen R, Bakhiya N, Schäfer B, Hirsch-Ernst KI, Lampen A (2018) Safety aspects of the use of quercetin as a dietary supplement. Mol Nutr Food Res 62(1):1700447. https://doi.org/10.1002/mnfr.201700447
Islam MS, Quispe C, Hossain R, Islam MT, Al-Harrasi A, Al-Rawahi A, Martorell M, Mamurova A et al (2021) Neuropharmacological effects of quercetin: a literature-based review. Front Pharmacol 12:665031. https://doi.org/10.3389/fphar.2021.665031
Riche K and Lenard NR (2022) Quercetin’s effects on glutamate cytotoxicity. Molecules 27(21) https://doi.org/10.3390/molecules27217620
Holland TM, Agarwal P, Wang Y, Dhana K, Leurgans SE, Shea K, Booth SL, Rajan K, et al (2022) Association of dietary intake of flavonols with changes in global cognition and several cognitive abilities. Neurology:https://doi.org/10.1212/WNL.0000000000201541
Almeida AF, Borge GIA, Piskula M, Tudose A, Tudoreanu L, Valentová K, Williamson G, Santos CN (2018) Bioavailability of quercetin in humans with a focus on interindividual variation. Compr Rev Food Sci Food Saf 17(3):714–731. https://doi.org/10.1111/1541-4337.12342
Baky MH, Elshahed M, Wessjohann L, Farag MA (2022) Interactions between dietary flavonoids and the gut microbiome: a comprehensive review. Br J Nutr 128(4):577–591. https://doi.org/10.1017/s0007114521003627
Li H, Li M, Fu J, Ao H, Wang W, Wang X (2021) Enhancement of oral bioavailability of quercetin by metabolic inhibitory nanosuspensions compared to conventional nanosuspensions. Drug Delivery 28(1):1226–1236. https://doi.org/10.1080/10717544.2021.1927244
Jin Z, Ke J, Guo P, Wang Y, Wu H (2019) Quercetin improves blood-brain barrier dysfunction in rats with cerebral ischemia reperfusion via Wnt signaling pathway. Am J Transl Res 11(8):4683–4695
Ossola B, Kääriäinen TM, Männistö PT (2009) The multiple faces of quercetin in neuroprotection. Expert Opin Drug Saf 8(4):397–409. https://doi.org/10.1517/14740330903026944
Spencer JP, Rice-Evans C, Williams RJ (2003) Modulation of pro-survival Akt/protein kinase B and ERK1/2 signaling cascades by quercetin and its in vivo metabolites underlie their action on neuronal viability. J Biol Chem 278(37):34783–34793. https://doi.org/10.1074/jbc.M305063200
Baral S, Pariyar R, Kim J, Lee H-S, Seo J (2017) Quercetin-3-O-glucuronide promotes the proliferation and migration of neural stem cells. Neurobiol Aging 52:39–52. https://doi.org/10.1016/j.neurobiolaging.2016.12.024
Vafeiadou K, Vauzour D, Rodriguez-Mateos A, Whiteman M, Williams RJ, Spencer JPE (2008) Glial metabolism of quercetin reduces its neurotoxic potential. Arch Biochem Biophys 478(2):195–200. https://doi.org/10.1016/j.abb.2008.07.014
Williams RJ, Spencer JPE, Rice-Evans C (2004) Flavonoids: antioxidants or signalling molecules? Free Radical Biol Med 36(7):838–849. https://doi.org/10.1016/j.freeradbiomed.2004.01.001
Agullo G, Gamet-Payrastre L, Manenti S, Viala C, Rémésy C, Chap H, Payrastre B (1997) Relationship between flavonoid structure and inhibition of phosphatidylinositol 3-kinase: a comparison with tyrosine kinase and protein kinase C inhibition. Biochem Pharmacol 53(11):1649–1657. https://doi.org/10.1016/s0006-2952(97)82453-7
Bilanges B, Posor Y, Vanhaesebroeck B (2019) PI3K isoforms in cell signalling and vesicle trafficking. Nat Rev Mol Cell Biol 20(9):515–534. https://doi.org/10.1038/s41580-019-0129-z
Kanekiyo T, Bu G (2014) The low-density lipoprotein receptor-related protein 1 and amyloid-β clearance in Alzheimer’s disease. Front Aging Neurosci 6:93. https://doi.org/10.3389/fnagi.2014.00093
Zhu M, Han S, Fink AL (2013) Oxidized quercetin inhibits α-synuclein fibrillization. Biochim Biophys Acta 1830(4):2872–2881. https://doi.org/10.1016/j.bbagen.2012.12.027
Ono K, Yoshiike Y, Takashima A, Hasegawa K, Naiki H, Yamada M (2003) Potent anti-amyloidogenic and fibril-destabilizing effects of polyphenols in vitro: implications for the prevention and therapeutics of Alzheimer’s disease. J Neurochem 87(1):172–181. https://doi.org/10.1046/j.1471-4159.2003.01976.x
Schlenzig D, Manhart S, Cinar Y, Kleinschmidt M, Hause G, Willbold D, Funke SA, Schilling S et al (2009) Pyroglutamate formation influences solubility and amyloidogenicity of amyloid peptides. Biochemistry 48(29):7072–7078. https://doi.org/10.1021/bi900818a
Schilling S, Lauber T, Schaupp M, Manhart S, Scheel E, Böhm G, Demuth H-U (2006) On the seeding and oligomerization of pGlu-amyloid peptides (in vitro). Biochemistry 45(41):12393–12399. https://doi.org/10.1021/bi0612667
Tarahovsky YS, Muzafarov EN, Kim YA (2008) Rafts making and rafts braking: how plant flavonoids may control membrane heterogeneity. Mol Cell Biochem 314(1):65–71. https://doi.org/10.1007/s11010-008-9766-9
Liu C-C, Kanekiyo T, Xu H, Bu G (2013) Apolipoprotein E and Alzheimer disease: risk, mechanisms and therapy. Nat Rev Neurol 9(2):106–118. https://doi.org/10.1038/nrneurol.2012.263
Koistinaho M, Lin S, Wu X, Esterman M, Koger D, Hanson J, Higgs R, Liu F, Malkani S, Bales KR, Paul SM (2004) Apolipoprotein E promotes astrocyte colocalization and degradation of deposited amyloid-beta peptides. Nat Med 10(7):719–726. https://doi.org/10.1038/nm1058
Zhang X, Hu J, Zhong L, Wang N, Yang L, Liu CC, Li H, Wang X et al (2016) Quercetin stabilizes apolipoprotein E and reduces brain Aβ levels in amyloid model mice. Neuropharmacology 108:179–192. https://doi.org/10.1016/j.neuropharm.2016.04.032
Zu G, Sun K, Li L, Zu X, Han T, Huang H (2021) Mechanism of quercetin therapeutic targets for Alzheimer disease and type 2 diabetes mellitus. Sci Rep 11(1):22959. https://doi.org/10.1038/s41598-021-02248-5
Wei C, Li S, Zhu Y, Chen W, Li C, Xu R (2022) Network pharmacology identify intersection genes of quercetin and Alzheimer’s disease as potential therapeutic targets. Front Aging Neurosci 14:902092. https://doi.org/10.3389/fnagi.2022.902092
Alghamdi A, Birch DJS, Vyshemirsky V, Rolinski OJ (2022) Impact of the flavonoid quercetin on β-amyloid aggregation revealed by intrinsic fluorescence. J Phys Chem B 126(38):7229–7237. https://doi.org/10.1021/acs.jpcb.2c02763
Porat Y, Abramowitz A, Gazit E (2006) Inhibition of amyloid fibril formation by polyphenols: structural similarity and aromatic interactions as a common inhibition mechanism. Chem Biol Drug Des 67(1):27–37. https://doi.org/10.1111/j.1747-0285.2005.00318.x
Acknowledgements
The authors would like to thank I. Herbert and M. Brode for professional technical assistance. Prof. T. Oertner, I. Ohmert, and J. Schröder provided organotypic hippocampal slice cultures. Dr. A.V. Failla from the UKE Microscopy Imaging Facility (Deutsche Forschungsgemeinschaft Research Infrastructure; RI_00489 and INST152/933-1) CNI provided assistance in imaging experiments.
Funding
Open Access funding enabled and organized by Projekt DEAL. The study was supported by LSA (IB) “ProCognito – Pflanzliche Wirkstoffe zum Erhalt der kognitiven Leistungsfähigkeit im Alter” to LAW and KF in cooperation with MRK with support from the European Union program EFRE as part of the project Autonomy in Old Age (ZS/2018/11/95581), and additional grants from Alzheimer Forschung Initiative e.V to KMG (DE-20057p); RTG 2413 “SynAge” to HA, MB, and MRK.
Author information
Authors and Affiliations
Contributions
Michael R. Kreutz and Ludger A. Wessjohann initiated the project and designed the study. Helene Arndt established the astrocyte screening pipeline. Helene Arndt and Mark Bachurski conducted the screening experiments in astrocytes and HEK-293T cells and performed western blotting. Mark Bachurski and Katarzyna M. Grochowska analyzed pCREB immunofluorescence. Katarzyna M. Grochowska performed OHSC experiments, dextran assay, and synapse loss assay. PingAn Yuanxiang performed electrophysiological recordings. Michael R. Kreutz and Katarzyna M. Grochowska wrote the first draft of manuscript. Helene Arndt was responsible for data visualization. Katrin Franke and Ludger A. Wessjohann selected and provided substances, advised on the study, and commented on the manuscript. All authors read and approved the final manuscript.
Corresponding authors
Ethics declarations
Ethics Approval
All animal experiments were carried out in accordance with the European Communities Council Directive (2010/63/EU) and German Animal Welfare Act.
Consent to Participate
Not applicable.
Consent for Publication
Not applicable.
Competing Interests
The authors declare no competing interests.
Additional information
Publisher's Note
Springer Nature remains neutral with regard to jurisdictional claims in published maps and institutional affiliations.
Supplementary Information
Below is the link to the electronic supplementary material.
Rights and permissions
Open Access This article is licensed under a Creative Commons Attribution 4.0 International License, which permits use, sharing, adaptation, distribution and reproduction in any medium or format, as long as you give appropriate credit to the original author(s) and the source, provide a link to the Creative Commons licence, and indicate if changes were made. The images or other third party material in this article are included in the article's Creative Commons licence, unless indicated otherwise in a credit line to the material. If material is not included in the article's Creative Commons licence and your intended use is not permitted by statutory regulation or exceeds the permitted use, you will need to obtain permission directly from the copyright holder. To view a copy of this licence, visit http://creativecommons.org/licenses/by/4.0/.
About this article
Cite this article
Arndt, H., Bachurski, M., Yuanxiang, P. et al. A Screen of Plant-Based Natural Products Revealed That Quercetin Prevents Pyroglutamylated Amyloid-β (Aβ3(pE)-42) Uptake in Astrocytes As Well As Resulting Astrogliosis and Synaptic Dysfunction. Mol Neurobiol (2024). https://doi.org/10.1007/s12035-024-04509-6
Received:
Accepted:
Published:
DOI: https://doi.org/10.1007/s12035-024-04509-6