Abstract
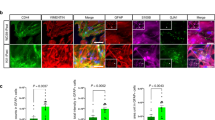
This study aimed to gain insights into the pathophysiology underlying PLA2G6-associated neurodegeneration that is implicated in three different neurological disorders, suggesting that other, unknown genetic or environmental factors might contribute to its wide phenotypic expression. To accomplish this, we downregulated the function of pla2g6 in the zebrafish nervous system, performed parkinsonism-related phenotypic characterization, and determined the effects of gene regulation upon the loss of pla2g6 function by using RNA sequencing and downstream analyses. Pla2g6 deficiency resulted in axonal degeneration, dopaminergic and motor neuron cell loss, and increased β-synuclein expression. We also observed that many of the identified, differentially expressed genes were implicated in other brain disorders, which might explain the variable phenotypic expression of pla2g6-associated disease, and found that top enriched canonical pathways included those already known or suggested to play a major role in the pathogenesis of Parkinson’s disease. Our data support that pla2g6 is relevant for cranial motor development with significant implications in the pathophysiology underlying Parkinson’s disease.








Similar content being viewed by others
References
Gallati S (2014) Disease-modifying genes and monogenic disorders: experience in cystic fibrosis. Appl Clin Genet 7:133–146. https://doi.org/10.2147/TACG.S18675
Gropman AL, Adams DR (2007) Atypical patterns of inheritance. Semin Pediatr Neurol 14(1):34–45. https://doi.org/10.1016/j.spen.2006.11.007
Krebs CE, Paisan-Ruiz C (2012) The use of next-generation sequencing in movement disorders. Front Genet 3:75
Khateeb S, Flusser H, Ofir R, Shelef I, Narkis G, Vardi G, Shorer Z, Levy R et al (2006) PLA2G6 mutation underlies infantile neuroaxonal dystrophy. Am J Hum Genet 79(5):942–948. https://doi.org/10.1086/508572
Morgan NV, Westaway SK, Morton JE, Gregory A, Gissen P, Sonek S, Cangul H, Coryell J et al (2006) PLA2G6, encoding a phospholipase A2, is mutated in neurodegenerative disorders with high brain iron. Nat Genet 38(7):752–754. https://doi.org/10.1038/ng1826
Paisan-Ruiz C, Bhatia KP, Li A, Hernandez D, Davis M, Wood NW, Hardy J, Houlden H et al (2009) Characterization of PLA2G6 as a locus for dystonia-parkinsonism. Ann Neurol 65(1):19–23. https://doi.org/10.1002/ana.21415
Dennis EA, Cao J, Hsu YH, Magrioti V, Kokotos G (2011) Phospholipase A2 enzymes: physical structure, biological function, disease implication, chemical inhibition, and therapeutic intervention. Chem Rev 111(10):6130–6185. https://doi.org/10.1021/cr200085w
Turk J, Ramanadham S (2004) The expression and function of a group VIA calcium-independent phospholipase A2 (iPLA2beta) in beta-cells. Can J Physiol Pharmacol 82(10):824–832. https://doi.org/10.1139/y04-064
Gregory A, Hayflick S (1993) Neurodegeneration with brain iron accumulation disorders overview. In: Pagon RA, Adam MP, Ardinger HH et al. (eds) GeneReviews(R). University of Washington, Seattle
Paisan-Ruiz C, Guevara R, Federoff M, Hanagasi H, Sina F, Elahi E, Schneider SA, Schwingenschuh P et al (2010) Early-onset L-dopa-responsive parkinsonism with pyramidal signs due to ATP13A2, PLA2G6, FBXO7 and spatacsin mutations. Mov Disord 25(12):1791–1800. https://doi.org/10.1002/mds.23221
Budick SA, O’Malley DM (2000) Locomotor repertoire of the larval zebrafish: swimming, turning and prey capture. J Exp Biol 203(Pt 17):2565–2579
Kastenhuber E, Kratochwil CF, Ryu S, Schweitzer J, Driever W (2010) Genetic dissection of dopaminergic and noradrenergic contributions to catecholaminergic tracts in early larval zebrafish. J Comp Neurol 518(4):439–458. https://doi.org/10.1002/cne.22214
Yamamoto K, Ruuskanen JO, Wullimann MF, Vernier P (2010) Two tyrosine hydroxylase genes in vertebrates. New dopaminergic territories revealed in the zebrafish brain. Mol Cell Neurosci 43(4):394–402. https://doi.org/10.1016/j.mcn.2010.01.006
Schweitzer J, Lohr H, Filippi A, Driever W (2012) Dopaminergic and noradrenergic circuit development in zebrafish. Dev Neurobiol 72(3):256–268. https://doi.org/10.1002/dneu.20911
Kaslin J, Panula P (2001) Comparative anatomy of the histaminergic and other aminergic systems in zebrafish (Danio rerio). J Comp Neurol 440(4):342–377. https://doi.org/10.1002/cne.1390
Bandmann O, Burton EA (2010) Genetic zebrafish models of neurodegenerative diseases. Neurobiol Dis 40(1):58–65. https://doi.org/10.1016/j.nbd.2010.05.017
Martin-Jimenez R, Campanella M, Russell C (2015) New zebrafish models of neurodegeneration. Curr Neurol Neurosci Rep 15(6):33
Xi Y, Noble S, Ekker M (2011) Modeling neurodegeneration in zebrafish. Curr Neurol Neurosci Rep 11(3):274–282. https://doi.org/10.1007/s11910-011-0182-2
Xi Y, Ryan J, Noble S, Yu M, Yilbas AE, Ekker M (2010) Impaired dopaminergic neuron development and locomotor function in zebrafish with loss of pink1 function. Eur J Neurosci 31(4):623–633. https://doi.org/10.1111/j.1460-9568.2010.07091.x
Flinn L, Mortiboys H, Volkmann K, Koster RW, Ingham PW, Bandmann O (2009) Complex I deficiency and dopaminergic neuronal cell loss in parkin-deficient zebrafish (Danio rerio). Brain 132(Pt 6):1613–1623. https://doi.org/10.1093/brain/awp108
Sheng D, Qu D, Kwok KH, Ng SS, Lim AY, Aw SS, Lee CW, Sung WK et al (2010) Deletion of the WD40 domain of LRRK2 in zebrafish causes parkinsonism-like loss of neurons and locomotive defect. PLoS Genet 6(4):e1000914. https://doi.org/10.1371/journal.pgen.1000914
Livak KJ, Schmittgen TD (2001) Analysis of relative gene expression data using real-time quantitative PCR and the 2(−Delta Delta C(T)) method. Methods 25(4):402–408. https://doi.org/10.1006/meth.2001.1262
Thisse C, Thisse B (2008) High-resolution in situ hybridization to whole-mount zebrafish embryos. Nat Protoc 3(1):59–69. https://doi.org/10.1038/nprot.2007.514
Turner KJ, Bracewell TG, Hawkins TA (2014) Anatomical dissection of zebrafish brain development. Methods Mol Biol 1082:197–214. https://doi.org/10.1007/978-1-62703-655-9_14
Trapnell C, Pachter L, Salzberg SL (2009) TopHat: discovering splice junctions with RNA-Seq. Bioinformatics 25(9):1105–1111. https://doi.org/10.1093/bioinformatics/btp120
Roberts A, Pimentel H, Trapnell C, Pachter L (2011) Identification of novel transcripts in annotated genomes using RNA-Seq. Bioinformatics 27(17):2325–2329. https://doi.org/10.1093/bioinformatics/btr355
Eden E, Navon R, Steinfeld I, Lipson D, Yakhini Z (2009) GOrilla: a tool for discovery and visualization of enriched GO terms in ranked gene lists. BMC Bioinformatics 10(1):48. https://doi.org/10.1186/1471-2105-10-48
Xie C, Mao X, Huang J, Ding Y, Wu J, Dong S, Kong L, Gao G et al (2011) KOBAS 2.0: a web server for annotation and identification of enriched pathways and diseases. Nucleic Acids Res 39(Web Server issue):W316–W322
Sina F, Shojaee S, Elahi E, Paisan-Ruiz C (2009) R632W mutation in PLA2G6 segregates with dystonia-parkinsonism in a consanguineous Iranian family. Eur J Neurol 16(1):101–104. https://doi.org/10.1111/j.1468-1331.2008.02356.x
Filippi A, Mahler J, Schweitzer J, Driever W (2010) Expression of the paralogous tyrosine hydroxylase encoding genes th1 and th2 reveals the full complement of dopaminergic and noradrenergic neurons in zebrafish larval and juvenile brain. J Comp Neurol 518(4):423–438. https://doi.org/10.1002/cne.22213
George JM (2002) The synucleins. Genome Biol 3(1):REVIEWS3002
Lee VM, Trojanowski JQ (2006) Mechanisms of Parkinson’s disease linked to pathological alpha-synuclein: new targets for drug discovery. Neuron 52(1):33–38. https://doi.org/10.1016/j.neuron.2006.09.026
Stefanis L (2012) Alpha-synuclein in Parkinson’s disease. Cold Spring Harb Perspect Med 2(2):a009399
Paisan-Ruiz C, Li A, Schneider SA, Holton JL, Johnson R, Kidd D, Chataway J, Bhatia KP et al (2010) Widespread Lewy body and tau accumulation in childhood and adult onset dystonia-parkinsonism cases with PLA2G6 mutations. Neurobiol Aging 33(4):814–823. https://doi.org/10.1016/j.neurobiolaging.2010.05.009
Scherzer CR, Jensen RV, Gullans SR, Feany MB (2003) Gene expression changes presage neurodegeneration in a Drosophila model of Parkinson’s disease. Hum Mol Genet 12(19):2457–2466. https://doi.org/10.1093/hmg/ddg265
Malik I, Turk J, Mancuso DJ, Montier L, Wohltmann M, Wozniak DF, Schmidt RE, Gross RW et al (2008) Disrupted membrane homeostasis and accumulation of ubiquitinated proteins in a mouse model of infantile neuroaxonal dystrophy caused by PLA2G6 mutations. Am J Pathol 172(2):406–416. https://doi.org/10.2353/ajpath.2008.070823
Sun Z, Gitler AD (2008) Discovery and characterization of three novel synuclein genes in zebrafish. Dev Dyn 237(9):2490–2495. https://doi.org/10.1002/dvdy.21569
Zannino DA, Appel B (2009) Olig2+ precursors produce abducens motor neurons and oligodendrocytes in the zebrafish hindbrain. J Neurosci 29(8):2322–2333. https://doi.org/10.1523/JNEUROSCI.3755-08.2009
Devine CA, Key B (2003) Identifying axon guidance defects in the embryonic zebrafish brain. Methods Cell Sci 25(1–2):33–37. https://doi.org/10.1023/B:MICS.0000006851.84998.e0
Uryu K, Richter-Landsberg C, Welch W, Sun E, Goldbaum O, Norris EH, Pham CT, Yazawa I et al (2006) Convergence of heat shock protein 90 with ubiquitin in filamentous alpha-synuclein inclusions of alpha-synucleinopathies. Am J Pathol 168(3):947–961. https://doi.org/10.2353/ajpath.2006.050770
Jeon GS, Park SW, Kim DW, Seo JH, Cho J, Lim SY, Kim SD, Cho SS (2004) Glial expression of the 90-kDa heat shock protein (HSP90) and the 94-kDa glucose-regulated protein (GRP94) following an excitotoxic lesion in the mouse hippocampus. Glia 48(3):250–258. https://doi.org/10.1002/glia.20075
Gegg ME, Cooper JM, Chau KY, Rojo M, Schapira AH, Taanman JW (2010) Mitofusin 1 and mitofusin 2 are ubiquitinated in a PINK1/parkin-dependent manner upon induction of mitophagy. Hum Mol Genet 19(24):4861–4870. https://doi.org/10.1093/hmg/ddq419
de Carvalho AP, Sweadner KJ, Penniston JT, Zaremba J, Liu L, Caton M, Linazasoro G, Borg M et al (2004) Mutations in the Na+/K+-ATPase alpha3 gene ATP1A3 are associated with rapid-onset dystonia parkinsonism. Neuron 43(2):169–175. https://doi.org/10.1016/j.neuron.2004.06.028
Carstea ED, Morris JA, Coleman KG, Loftus SK, Zhang D, Cummings C, Gu J, Rosenfeld MA et al (1997) Niemann-pick C1 disease gene: homology to mediators of cholesterol homeostasis. Science 277(5323):228–231. https://doi.org/10.1126/science.277.5323.228
Weber YG, Storch A, Wuttke TV, Brockmann K, Kempfle J, Maljevic S, Margari L, Kamm C et al (2008) GLUT1 mutations are a cause of paroxysmal exertion-induced dyskinesias and induce hemolytic anemia by a cation leak. J Clin Invest 118(6):2157–2168. https://doi.org/10.1172/JCI34438
Weber YG, Kamm C, Suls A, Kempfle J, Kotschet K, Schule R, Wuttke TV, Maljevic S et al (2011) Paroxysmal choreoathetosis/spasticity (DYT9) is caused by a GLUT1 defect. Neurology 77(10):959–964. https://doi.org/10.1212/WNL.0b013e31822e0479
Poirier K, Lebrun N, Broix L, Tian G, Saillour Y, Boscheron C, Parrini E, Valence S, Pierre BS, Oger M, Lacombe D, Genevieve D, Fontana E, Darra F, Cances C, Barth M, Bonneau D, Bernadina BD, N’Guyen S, Gitiaux C, Parent P, des Portes V, Pedespan JM, Legrez V, Castelnau-Ptakine L, Nitschke P, Hieu T, Masson C, Zelenika D, Andrieux A, Francis F, Guerrini R, Cowan NJ, Bahi-Buisson N, Chelly J (2013) Mutations in TUBG1, DYNC1H1, KIF5C and KIF2A cause malformations of cortical development and microcephaly. Nat Genet 45 (6):639–647, doi: https://doi.org/10.1038/ng.2613.
Rauch SM, Huen K, Miller MC, Chaudry H, Lau M, Sanes JR, Johanson CE, Stopa EG et al (2011) Changes in brain beta-amyloid deposition and aquaporin 4 levels in response to altered agrin expression in mice. J Neuropathol Exp Neurol 70(12):1124–1137. https://doi.org/10.1097/NEN.0b013e31823b0b12
Garthwaite J, Boulton CL (1995) Nitric oxide signaling in the central nervous system. Annu Rev Physiol 57(1):683–706. https://doi.org/10.1146/annurev.ph.57.030195.003343
Falls DL (2003) Neuregulins: Functions, forms, and signaling strategies. Exp Cell Res 284(1):14–30. https://doi.org/10.1016/S0014-4827(02)00102-7
Wu GY, Deisseroth K, Tsien RW (2001) Activity-dependent CREB phosphorylation: convergence of a fast, sensitive calmodulin kinase pathway and a slow, less sensitive mitogen-activated protein kinase pathway. Proc Natl Acad Sci U S A 98(5):2808–2813
Knapp RJ, Malatynska E, Yamamura HI (1990) From binding studies to the molecular biology of GABA receptors. Neurochem Res 15(2):105–112. https://doi.org/10.1007/BF00972199
Surmeier DJ, Obeso JA, Halliday GM (2017) Selective neuronal vulnerability in Parkinson disease. Nat Rev Neurosci 18(2):101–113. https://doi.org/10.1038/nrn.2016.178
Zhao T, Zondervan-van der Linde H, Severijnen LA, Oostra BA, Willemsen R, Bonifati V (2012) Dopaminergic neuronal loss and dopamine-dependent locomotor defects in Fbxo7-deficient zebrafish. PLoS One 7(11):e48911. https://doi.org/10.1371/journal.pone.0048911
Anichtchik O, Diekmann H, Fleming A, Roach A, Goldsmith P, Rubinsztein DC (2008) Loss of PINK1 function affects development and results in neurodegeneration in zebrafish. J Neurosci 28(33):8199–8207. https://doi.org/10.1523/JNEUROSCI.0979-08.2008
Sallinen V, Kolehmainen J, Priyadarshini M, Toleikyte G, Chen YC, Panula P (2010) Dopaminergic cell damage and vulnerability to MPTP in Pink1 knockdown zebrafish. Neurobiol Dis 40(1):93–101. https://doi.org/10.1016/j.nbd.2010.06.001
Wilson JM, Levey AI, Rajput A, Ang L, Guttman M, Shannak K, Niznik HB, Hornykiewicz O et al (1996) Differential changes in neurochemical markers of striatal dopamine nerve terminals in idiopathic Parkinson’s disease. Neurology 47(3):718–726. https://doi.org/10.1212/WNL.47.3.718
Schulz-Schaeffer WJ (2010) The synaptic pathology of alpha-synuclein aggregation in dementia with Lewy bodies, Parkinson’s disease and Parkinson’s disease dementia. Acta Neuropathol 120(2):131–143. https://doi.org/10.1007/s00401-010-0711-0
Abeliovich A, Gitler AD (2016) Defects in trafficking bridge Parkinson’s disease pathology and genetics. Nature 539(7628):207–216. https://doi.org/10.1038/nature20414
Day M, Wang Z, Ding J, An X, Ingham CA, Shering AF, Wokosin D, Ilijic E et al (2006) Selective elimination of glutamatergic synapses on striatopallidal neurons in Parkinson disease models. Nat Neurosci 9(2):251–259. https://doi.org/10.1038/nn1632
Sumi-Akamaru H, Beck G, Shinzawa K, Kato S, Riku Y, Yoshida M, Fujimura H, Tsujimoto Y et al (2016) High expression of alpha-synuclein in damaged mitochondria with PLA2G6 dysfunction. Acta Neuropathol Commun 4(1):27. https://doi.org/10.1186/s40478-016-0298-3
Hikosaka O, Sesack SR, Lecourtier L, Shepard PD (2008) Habenula: crossroad between the basal ganglia and the limbic system. J Neurosci 28(46):11825–11829. https://doi.org/10.1523/JNEUROSCI.3463-08.2008
Illingworth MA, Meyer E, Chong WK, Manzur AY, Carr LJ, Younis R, Hardy C, McDonald F et al (2014) PLA2G6-associated neurodegeneration (PLAN): further expansion of the clinical, radiological and mutation spectrum associated with infantile and atypical childhood-onset disease. Mol Genet Metab 112(2):183–189. https://doi.org/10.1016/j.ymgme.2014.03.008
Sumi-Akamaru H, Beck G, Kato S, Mochizuki H (2015) Neuroaxonal dystrophy in PLA2G6 knockout mice. Neuropathology 35(3):289–302. https://doi.org/10.1111/neup.12202
Labrador-Garrido A, Bertoncini CW, Roodveldt C (2011) The Hsp70 chaperone system in Parkinson’s disease, etiology and pathophysiology of Parkinson’s disease. In: PAQR (ed). InTech.
Daturpalli S, Waudby CA, Meehan S, Jackson SE (2013) Hsp90 inhibits alpha-synuclein aggregation by interacting with soluble oligomers. J Mol Biol 425(22):4614–4628. https://doi.org/10.1016/j.jmb.2013.08.006
Ebrahimi-Fakhari D, Saidi LJ, Wahlster L (2013) Molecular chaperones and protein folding as therapeutic targets in Parkinson’s disease and other synucleinopathies. Acta Neuropathol Commun 1(1):79. https://doi.org/10.1186/2051-5960-1-79
Minoia M, Grit C, Kampinga HH (2014) HSPA1A-independent suppression of PARK2 C289G protein aggregation by human small heat shock proteins. Mol Cell Biol 34(19):3570–3578. https://doi.org/10.1128/MCB.00698-14
Evgrafov OV, Mersiyanova I, Irobi J, Van Den Bosch L, Dierick I, Leung CL, Schagina O, Verpoorten N et al (2004) Mutant small heat-shock protein 27 causes axonal Charcot-Marie-Tooth disease and distal hereditary motor neuropathy. Nat Genet 36(6):602–606. https://doi.org/10.1038/ng1354
Abisambra JF, Jinwal UK, Jones JR, Blair LJ, Koren J 3rd, Dickey CA (2011) Exploiting the diversity of the heat-shock protein family for primary and secondary tauopathy therapeutics. Curr Neuropharmacol 9(4):623–631. https://doi.org/10.2174/157015911798376226
Zuchner S, Mersiyanova IV, Muglia M, Bissar-Tadmouri N, Rochelle J, Dadali EL, Zappia M, Nelis E et al (2004) Mutations in the mitochondrial GTPase mitofusin 2 cause Charcot-Marie-Tooth neuropathy type 2A. Nat Genet 36(5):449–451. https://doi.org/10.1038/ng1341
Fyfe JC, Al-Tamimi RA, Liu J, Schaffer AA, Agarwala R, Henthorn PS (2011) A novel mitofusin 2 mutation causes canine fetal-onset neuroaxonal dystrophy. Neurogenetics 12(3):223–232. https://doi.org/10.1007/s10048-011-0285-6
Santel A, Fuller MT (2001) Control of mitochondrial morphology by a human mitofusin. J Cell Sci 114(Pt 5):867–874
Chen Y, Dorn GW 2nd (2013) PINK1-phosphorylated mitofusin 2 is a Parkin receptor for culling damaged mitochondria. Science 340(6131):471–475. https://doi.org/10.1126/science.1231031
Poole AC, Thomas RE, Andrews LA, McBride HM, Whitworth AJ, Pallanck LJ (2008) The PINK1/Parkin pathway regulates mitochondrial morphology. Proc Natl Acad Sci U S A 105(5):1638–1643. https://doi.org/10.1073/pnas.0709336105
Clark IE, Dodson MW, Jiang C, Cao JH, Huh JR, Seol JH, Yoo SJ, Hay BA et al (2006) Drosophila pink1 is required for mitochondrial function and interacts genetically with parkin. Nature 441(7097):1162–1166. https://doi.org/10.1038/nature04779
Lee S, Sterky FH, Mourier A, Terzioglu M, Cullheim S, Olson L, Larsson NG (2012) Mitofusin 2 is necessary for striatal axonal projections of midbrain dopamine neurons. Hum Mol Genet 21(22):4827–4835. https://doi.org/10.1093/hmg/dds352
Kreitzer AC, Malenka RC (2008) Striatal plasticity and basal ganglia circuit function. Neuron 60(4):543–554. https://doi.org/10.1016/j.neuron.2008.11.005
Acknowledgements
We thank Joshua Barber at the Zebrafish core at the Columbia University Medical Center for his assistance with the MO and mRNA microinjections and the staff at the Microscopy Shared Resource Facility at the ISMMS for their training and assistance with the zebrafish imaging.
Funding
This work was supported by the National Institute of Neurological Disorders and Stroke of the National Institutes of Health (R01NS079388; CPR).
Author information
Authors and Affiliations
Corresponding author
Ethics declarations
Conflict of Interest
The authors declare that they have no competing interests.
Ethics Approval
All experiments involving animals were performed under the national (United States National Institutes of Health) and Institutional Animal Care and Use Committee at the Icahn School of Medicine at Mount Sinai (ISMMS) guidelines and approved by ISMMS IACUC (Protocol number: LA11-00313).
Electronic Supplementary Material
ESM 1
(XLS 282 kb)
Rights and permissions
About this article
Cite this article
Sánchez, E., Azcona, L.J. & Paisán-Ruiz, C. Pla2g6 Deficiency in Zebrafish Leads to Dopaminergic Cell Death, Axonal Degeneration, Increased β-Synuclein Expression, and Defects in Brain Functions and Pathways. Mol Neurobiol 55, 6734–6754 (2018). https://doi.org/10.1007/s12035-017-0846-2
Received:
Accepted:
Published:
Issue Date:
DOI: https://doi.org/10.1007/s12035-017-0846-2