Abstract
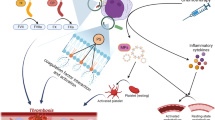
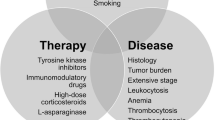
In patients with acute leukemia (AL), coagulation disorders, which include both thrombotic and hemorrhagic events, are part of the clinical spectrum both at diagnosis and during its evolution. The incidence of these events has been reported by several authors in the range of 1–36 %. This heterogeneity appears to be related to the type of patients included, the study design, and patient-related factors as well as the treatment used. The pathophysiology of thrombosis in AL is complex and multifactorial and includes a myriad of factors that contribute to cancer procoagulant state: synthesis of procoagulant factors by circulating blasts, cellular microparticles, use of endovascular devices (catheters), type of chemotherapy used (l-asparaginase) to name a few. Currently, treatment relies in the use of heparin, followed by vitamin K antagonists for 3 to 6 months. However, randomized controlled studies are required in patients with AL and thrombosis to confirm its safety, duration, and effectiveness.

Similar content being viewed by others
References
Papers of particular interest, published recently, have been highlighted as: • Of importance
Elice F, Rodeghiero F. Hematologic malignancies and thrombosis. Thromb Res. 2012;129:360–6.
Timp JF, Braejjan SK, Versteeg HH, et al. Epidemiology of cancer-associated venous thrombosis. Blood. 2013;122:1712–23.
Colombo R, Gallipoli P, Castelli R. Thrombosis and hemostatic abnormalities in hematological malignancies. Clin Lymphoma Myeloma Leuk. 2014; Article in press. A recent review of epidemiology, pathogenesis, prevention and treatment of thrombotic complications in several hematologic malignancies including acute leukemias.
Falanga A, Russo L, Verzeroli C. Mechanisms of thrombosis in cancer. Thromb Res. 2013;131:S59–62.
Falanga A, Russo L, Milesi V. The coagulopathy of cancer. Curr Opin Hematol. 2014;21:423–9.
Guzmán-Uribe P, Rosas-López A, Zepeda-León J, et al. Incidence of thrombosis in adults with acute leukemia: a single center experience in Mexico. Rev Investig Clin. 2013;65:130–40.
Falanga A, Marchetti M, Russo L. Venous thromboembolism in the hematologic malignancies. Curr Opin Oncol. 2012;24:702–10. This is an excellent review that focuses in venous thromboembolism in different hematological malignances, and highlights the need to create specific treatment guidelines and recommendations for this group of patients.
Crespo-Solis E. Thrombosis in acute leukemia. Hematology. 2012;17:S169–73.
Wun T, White RH. Venous thromboembolism in patients with acute leukemia, lymphoma, and multiple myeloma. Thromb Res. 2010;125:S96–102.
Ku GH, White RH, Chew HK, et al. Venous thromboembolism in patients with acute leukemia: incidence, risk factors and effect on survival. Blood. 2009;113:3911–7.
Grace RF, Dahlberg SE, Neuberg D, et al. The frequency and management of asparaginase-related thrombosis in paediatric and adult patients with acute lymphoblastic leukaemia treated on Dana-Farber Cancer Institute consortium protocols. Br J Haematol. 2011;152:452–9.
Truelove E, Fielding AK, Hunt BJ. The coagulopathy and thrombotic risk associated with L-asparaginase treatment in adults with acute lymphoblastic leukaemia. Leukemia. 2013;27:553–9.
De Stefano V, Za T, Ciminello A, et al. Haemostatic alterations induced by treatment with asparaginases and clinical consequences. Thromb Haemost 2015; 113. Published ahead of print. Great review about the role of L-asparaginase in the genesis of hemostatic alterations and thrombotic complications.
Ranta S, Tuckuviene R, Mäkipernaa A, et al. Cerebral sinus venous thromboses in children with acute lymphoblastic leukaemia—a multicentre study from the Nordic Society of Pediatric Haematology and Oncology. Br J Haematol. 2014; published ahead of print.
Breccia M, Lo CF. Thrombo-hemorrhagic deaths in acute promyelocytic leukemia. Thromb Res. 2014;133:S112–6.
Breccia M, Avvisati G, Latagliata R, et al. Occurrence of thrombotic events in acute promyelocytic leukemia correlates with consistent immunophenotypic and molecular features. Leukemia. 2007;21:79–83.
Falanga A, Tartari CJ, Marchetti M. Microparticles in tumor progression. Thromb Res. 2012;129:S132–6.
Van Aalderen MC, Trappenburg MC, Van Schilfgaarde M, et al. Procoagulant myeloblast-derived microparticles in AML patients: changes in numbers and thrombin generation potential during chemotherapy. J Thromb Haemost. 2011;9:223–6.
Guibo M, Fang L, Linlin LV, et al. Increased promyelocytic-derived microparticles: a novel potential factor for coagulopathy in acute promyelocytic leukemia. Ann Hematol. 2013;92:645–52.
Kwaan HC, Cull E. The coagulopathy in acute promyelocytic leukemia—what have we learned in the past twenty years. Best Pract Res Clin Hematol. 2014;27:11–8.
Falanga A, Marchetti M. Anticancer treatment and thrombosis. Thromb Res. 2012;129:353–9.
Johansson E, Hammarskjöld F, Lundberg D, et al. Advantages and disadvantages of peripherally inserted central venous catheters (PICC) compared to other central venous lines: a systematic review of the literature. Acta Oncol. 2013;52:886–92.
Chopra V, Anand S, Hickner A, et al. Risk of venous thromboembolism associated with peripherally inserted central catheters: a systematic review and meta-analysis. Lancet. 2013;382:311–25.
Boles JC, Williams JC, Hollinsgsworth RM, et al. Anthracycline treatment of the human monocytic leukemia cell line THP-1 increases phosphatidylserine exposure and tissue factor activity. Thromb Res. 2012;129:197–203.
Montesinos P, DIS J, Vellenga E, et al. Incidence and risk factors for thrombosis in patients with acute promyelocytic leukemia. Experience of the PETHEMA LPA 96 and LPA 99 protocols. Blood. 2011;108:1503.
Montesinos P, Sanz MA. The differentiation syndrome in patients with acute promyelocytic leukemia: experience of the PETHEMA group and review of the literature. Mediterr J Hematol Infect Dis. 2011;3:e2011059.
Mesri M, Altieri DC. Leukocyte microparticles stimulate endothelial cell cytokine release and tissue factor induction in a JNK1 signaling pathway. J Biol Chem. 1999;274(33):23111–8.
Morel O, Morel N, Jesel L, et al. Microparticles: a critical component in the nexus between inflammation, immunity and thrombosis. Semin Immunopathol. 2011;33:469–86.
Koch A, Meesters MI, Scheller B, et al. Systemic endotoxin activity correlates with clot formation: an observational study in patients with early systemic inflammation and sepsis. Crit Care. 2013;17:R198.
Kyriazi V, Theodoulou E. Assessing the risk and prognosis of thrombotic complications in cancer patients. Arch Pathol Lab Med. 2013;137:1286–95.
Khorana AA, Kuderer NM, Culakova E, et al. Development and validation of a predictive model for chemotherapy associated thrombosis. Blood. 2008;111:4902–7.
Couban S, Goodyear M, Burnell M, et al. Randomized placebo-controlled study of low-dose warfarin for the prevention of central venous catheter-associated thrombosis in patients with cancer. J Clin Oncol. 2005;23:4063–9.
Cortelezzi A, Moia M, Falanga A, et al. Incidence of thrombotic complications in patients with haematological malignancies with central venous catheters: a prospective multicentre study. Br J Haematol. 2005;129:811–7.
Lauw MN, Van der Holt B, Middeldorp S, et al. Venous thromboembolism in adults treated for acute lymphoblastic leukaemia: effect of fresh frozen plasma supplementation. Thromb Haemost. 2013;109:633–42.
Hunault-Berger M, Chevallier Delain M, Bulabois CE, et al. Changes in antithrombin and fibrinogen levels during induction chemotherapy with l-asparaginase in adult patients with acute lymphoblastic leukemia or lymphoblastic lymphoma. Use of supportive coagulation therapy and clinical outcome: the CAPELAL study. Haematologica. 2008;93:1488–94.
Farge D, Debourdeau P, Beckers M, et al. International clinical practice guidelines for the treatment and prophylaxis of venous thromboembolism in patients with cancer. J Thromb Haemost. 2013;11:56–70. These are the current guidelines to treat patients with cancer and thrombotic complications.
Lee AY, Levine MN, Baker RI, et al. Low-molecular weight heparin versus a coumarin for the prevention of recurrent venous thromboembolism in patients with cancer. N Engl J Med. 2003;349:146–53.
Rickles FR, Falanga A, Montesinos P, et al. Bleeding and thrombosis in acute leukemia: what does the future of therapy look like? Thromb Res. 2007;120 Suppl 2:S99–106.
Debordeau P, Farge D, Beckers M, et al. International clinical practice guidelines for the treatment and prophylaxis of thrombosis associated with central venous catheters in patients with cancer. J Thromb Haemost. 2013;11:71–80. These are the current guidelines for the treatment and prevention of thrombotic events in patients with cancer and central venous catheters.
Compliance with Ethics Guidelines
Conflict of Interest
Patricia Guzmán-Uribe and Ángel Gabriel Vargas-Ruíz declare that they have no conflict of interest.
Human and Animal Rights and Informed Consent
This article does not contain any studies with human or animal subjects performed by any of the authors.
Author information
Authors and Affiliations
Corresponding author
Additional information
This article is part of the Topical Collection on Leukemia
Rights and permissions
About this article
Cite this article
Guzmán-Uribe, P., Vargas-Ruíz, Á.G. Thrombosis in Leukemia: Incidence, Causes, and Practical Management. Curr Oncol Rep 17, 19 (2015). https://doi.org/10.1007/s11912-015-0444-2
Published:
DOI: https://doi.org/10.1007/s11912-015-0444-2