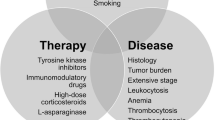
Opinion statement
Prophylaxis and treatment of thrombosis in leukemic patients still represent a major challenge with several clinical questions yet to be solved. Indeed, the paucity of evidence makes the management of venous thromboembolic events difficult and not uniform. Due to thrombocytopenia, patients with acute myeloid leukemia (AML) are underrepresented in trials investigating prophylaxis and treatment of thrombosis in cancer, and prospective data are lacking. Likewise, the therapeutic approach with anti-coagulants in leukemic patients is inferred from guidelines originally developed in the solid cancer setting and clear recommendations in the thrombocytopenic population are limited. Importantly, the discrimination of patients at high risk of bleeding from those with a predominant risk of thrombosis remains extremely difficult with no predictive score validated so far. Thus, the management of thrombosis often relies on clinician experience, and it is tailored to the individual patient, constantly balancing thrombotic and hemorrhagic risks. Who would benefit from primary prophylaxis and how a thrombotic event should be appropriately treated are some of the unanswered questions that the future guidelines and trials should address. Moreover, a greater effort should be made to identify robust predictive factors able to guide clinicians in the management of this potential serious complication for AML patients.

Similar content being viewed by others
References and Recommended Reading
Papers of particular interest, published recently, have been highlighted as: • Of importance •• Of major importance
Khorana AA. Venous thromboembolism and prognosis in cancer. Thromb Res. 2010;125(6):490–3.
Khorana AA, Francis CW, Culakova E, Kuderer NM, Lyman GH. Thromboembolism is a leading cause of death in cancer patients receiving outpatient chemotherapy. J Thromb Haemost. 2007;5:632–4.
Falanga A, Russo L, Verzeroli C. Mechanisms of thrombosis in cancer. Thromb Res. 2013;131(Suppl):S59-62.
Khorana AA, Francis CW, Culakova E, Kuderer NM, Lyman GH. Frequency, risk factors, and trends for venous thromboembolism among hospitalized cancer patients. Cancer. 2007;110(10):2339–46.
Kuderer NM, Francis CW, Culakova E, Khorana AA, Ortel T, Falanga A, et al. Venous thromboembolism and all-cause mortality in cancer patients receiving chemotherapy. J Clin Oncol [Internet]. 2008;26(15\_suppl):9521. Available from: https://doi.org/10.1200/jco.2008.26.15_suppl.9521.
Blom JW, Doggen CJM, Osanto S, Rosendaal FR. Malignancies, prothrombotic mutations, and the risk of venous thrombosis. JAMA. 2005;293(6):715–22.
Timp JF, Braekkan SK, Versteeg HH, Cannegieter SC. Epidemiology of cancer-associated venous thrombosis. Blood. 2013;122(10):1712–23. https://doi.org/10.1182/blood-2013-04-460121.
White RH, Chew HK, Zhou H, Parikh-Patel A, Harris D, Harvey D, et al. Incidence of venous thromboembolism in the year before the diagnosis of cancer in 528,693 adults. Arch Intern Med. 2005;165(15):1782–7.
Mulder FI, Horváth-Puhó E, van Es N, van Laarhoven HWM, Pedersen L, Moik F, et al. Venous thromboembolism in cancer patients: a population-based cohort study. Blood. 2021;137(14):1959–69.
Adelborg K, Corraini P, Darvalics B, Frederiksen H, Ording A, Horváth-Puhó E, et al. Risk of thromboembolic and bleeding outcomes following hematological cancers: a Danish population-based cohort study. J Thromb Haemost. 2019;17(8):1305–18.
Holstein SA, McCarthy PL. Immunomodulatory drugs in multiple myeloma: mechanisms of action and clinical experience. Drugs. 2017;77(5):505–20.
Leebeek FWG. Update of thrombosis in multiple myeloma. Thromb Res. 2016;140(Suppl):S76-80.
De Stefano V, Larocca A, Carpenedo M, Cavo M, Di Raimondo F, Falanga A, et al. Thrombosis in multiple myeloma: risk stratification, antithrombotic prophylaxis, and management of acute events. A consensus-based position paper from an ad hoc expert panel. Haematologica. 2022;107(11):2536–47.
Colombo R, Gallipoli P, Castelli R. Thrombosis and hemostatic abnormalities in hematological malignancies. Clin Lymphoma, Myeloma Leuk [Internet]. 2014;14(6):441–50. Available from: https://doi.org/10.1016/j.clml.2014.05.003.
Sorigue M, Orna E, Sancho J-M. Venous thromboembolism in patients with non-Hodgkin lymphoma or chronic lymphocytic leukemia treated with lenalidomide: a systematic review. Leuk Lymphoma. 2018;59(11):2602–11.
Reeves BN, Moliterno AR. Thrombosis in myeloproliferative neoplasms: update in pathophysiology. Curr Opin Hematol. 2021;28(5):285–91.
Sankar K, Stein BL, Rampal RK. Thrombosis in the Philadelphia chromosome-negative myeloproliferative neoplasms. Cancer Treat Res. 2019;179:159–78.
Falanga A, Rickles FR. Pathogenesis and management of the bleeding diathesis in acute promyelocytic leukaemia. Best Pract Res Clin Haematol. 2003;16(3):463–82.
David S, Mathews V. Mechanisms and management of coagulopathy in acute promyelocytic leukemia. Thromb Res. 2018;164(Suppl):S82–8.
Paterno G, Palmieri R, Forte V, Del Prete V, Gurnari C, Guarnera L, et al. Predictors of early thrombotic events in adult patients with acute myeloid leukemia: a real-world experience. Cancers (Basel). 2022;14(22).
Del Principe MI, Del Principe D, Venditti A. Thrombosis in adult patients with acute leukemia. Curr Opin Oncol. 2017;29(6):448–54.
López JA, Kearon C, Lee AY. Deep venous thrombosis. Hematology Am Soc Hematol Educ Program. 2004:439–56. https://doi.org/10.1182/asheducation-2004.1.439.
Falanga A, Marchetti M, Vignoli A. Coagulation and cancer: biological and clinical aspects. J Thromb Haemost. 2013;11(2):223–33.
Falanga A, Marchetti M. Venous thromboembolism in the hematologic malignancies. J Clin Oncol [Internet]. 2009 Oct 10;27(29):4848–57. Available from: https://doi.org/10.1200/JCO.2009.22.8197.
Rickles FR, Falanga A, Montesinos P, Sanz MA, Brenner B, Barbui T. Bleeding and thrombosis in acute leukemia: what does the future of therapy look like? Thromb Res. 2007;120(SUPPL. 2):99–106.
Kekre N, Connors JM. Venous thromboembolism incidence in hematologic malignancies. Blood Rev. 2019;33:24–32.
Falanga A, Marchetti M, Vignoli A, Balducci D, Russo L, Guerini V, et al. V617F JAK-2 mutation in patients with essential thrombocythemia: relation to platelet, granulocyte, and plasma hemostatic and inflammatory molecules. Exp Hematol. 2007;35(5):702–11.
Martella F, Cerrano M, Di Cuonzo D, Secreto C, Olivi M, Apolito V, et al. Frequency and risk factors for thrombosis in acute myeloid leukemia and high-risk myelodysplastic syndromes treated with intensive chemotherapy: a two centers observational study. Ann Hematol. 2022;101(4):855–67.
Lee Y-G, Kim I, Kwon J, Yoon S, Park S, Song L, et al. Implications of cytogenetics for venous thromboembolism in acute myeloid leukaemia. Thromb Haemost [Internet]. 2015 Jan 27;113(01):201–8. Available from: https://doi.org/10.1160/TH13-12-1020.
Perek S, Khatib A, Izhaki N, Khalaila AS, Brenner B, Horowitz NA. A prediction model for central venous catheter-related thrombosis in patients with newly-diagnosed acute myeloid leukemia: A derivation cohort analysis. Eur J Intern Med [Internet]. 2022;101(March):68–75. Available from: https://doi.org/10.1016/j.ejim.2022.04.025.
Kwaan HC. Complications of implanted nonbiologic devices: an overview. Semin Thromb Hemost. 2018;44(1):7–11.
Iba T, Levi M, Levy JH. Sepsis-induced coagulopathy and disseminated intravascular coagulation. Semin Thromb Hemost. 2020;46(1):89–95.
Khan F, Tritschler T, Kahn SR, Rodger MA. Venous thromboembolism. Lancet. 2021;398(10294):64–77.
Falanga A, Panova-Noeva M, Russo L. Procoagulant mechanisms in tumour cells. Best Pract Res Clin Haematol. 2009;22(1):49–60.
Dicke C, Amirkhosravi A, Spath B, Jiménez-Alcázar M, Fuchs T, Davila M, et al. Tissue factor-dependent and -independent pathways of systemic coagulation activation in acute myeloid leukemia: a single-center cohort study. Exp Hematol Oncol. 2015;4:22.
Tzoran I, Rebibo-Sabbah A, Brenner B, Aharon A. Disease dynamics in patients with acute myeloid leukemia: new biomarkers. Exp Hematol. 2015;43(11):936–43.
Key NS, Chantrathammachart P, Moody PW, Chang J-Y. Membrane microparticles in VTE and cancer. Thromb Res. 2010;125(Suppl):S80–3.
Horowitz NA, Brenner B. Thrombosis in hematological malignancies: mechanisms and implications. Thromb Res [Internet]. 2020;191(October 2019):S58–62. Available from: https://doi.org/10.1016/S0049-3848(20)30398-4.
Vallier L, Cointe S, Lacroix R, Bonifay A, Judicone C, Dignat-George F, et al. Microparticles and fibrinolysis. Semin Thromb Hemost. 2017;43(2):129–34.
Rickles FR, Falanga A. Molecular basis for the relationship between thrombosis and cancer. Thromb Res. 2001;102(6):V215–24.
Heit JA, O’Fallon WM, Petterson TM, Lohse CM, Silverstein MD, Mohr DN, et al. Relative impact of risk factors for deep vein thrombosis and pulmonary embolism: a population-based study. Arch Intern Med. 2002;162(11):1245–8.
Farge D, Frere C, Connors JM, Ay C, Khorana AA, Munoz A, et al. 2019 International Clinical Practice Guidelines for the treatment and prophylaxis of venous thromboembolism in patients with cancer. Lancet Oncol. 2019;20(10):e566–81.
Grilz E, Posch F, Nopp S, Königsbrügge O, Lang IM, Klimek P, et al. Relative risk of arterial and venous thromboembolism in persons with cancer vs. persons without cancer-a nationwide analysis. Eur Heart J. 2021;42(23):2299–307.
Cronin-Fenton DP, Søndergaard F, Pedersen LA, Fryzek JP, Cetin K, Acquavella J, et al. Hospitalisation for venous thromboembolism in cancer patients and the general population: a population-based cohort study in Denmark, 1997–2006. Br J Cancer. 2010;103(7):947–53.
Walker AJ, Card TR, West J, Crooks C, Grainge MJ. Incidence of venous thromboembolism in patients with cancer: a cohort study using linked United Kingdom databases. Eur J Cancer. 2013;49(6):1404–13.
Ziegler S, Sperr WR, Knöbl P, Lehr S, Weltermann A, Jäger U, et al. Symptomatic venous thromboembolism in acute leukemia. Incidence, risk factors, and impact on prognosis. Thromb Res. 2005;115(1–2):59–64.
Ku GH, White RH, Chew HK, Harvey DJ, Zhou H, Wun T. Venous thromboembolism in patients with acute leukemia: incidence, risk factors, and effect on survival. Blood. 2009;113(17):3911–7.
Vu K, Luong NV, Hubbard J, Zalpour A, Faderl S, Thomas DA, et al. A retrospective study of venous thromboembolism in acute leukemia patients treated at the University of Texas MD Anderson Cancer Center. Cancer Med. 2015;4(1):27–35.
Al-Ani F, Wang YP, Lazo-Langner A. Development of a clinical prediction rule for venous thromboembolism in patients with acute leukemia. Thromb Haemost. 2020;120(2):322–8.
De Stefano V, Sorà F, Rossi E, Chiusolo P, Laurenti L, Fianchi L, et al. The risk of thrombosis in patients with acute leukemia: occurrence of thrombosis at diagnosis and during treatment. J Thromb Haemost. 2005;3(9):1985–92.
Melillo L, Grandone E, Colaizzo D, Cappucci F, Valvano MR, Cascavilla N. Symptomatic venous thromboembolism and thrombophilic status in adult acute leukemia: a single-center experience of 114 patients at diagnosis. Acta Haematol. 2007;117(4):215–20.
Libourel EJ, Klerk CPW, van Norden Y, de Maat MPM, Kruip MJ, Sonneveld P, et al. Disseminated intravascular coagulation at diagnosis is a strong predictor for thrombosis in acute myeloid leukemia. Blood. 2016;128(14):1854–61.
Taylor FBJ, Toh CH, Hoots WK, Wada H, Levi M. Towards definition, clinical and laboratory criteria, and a scoring system for disseminated intravascular coagulation. Thromb Haemost. 2001;86(5):1327–30.
Hellou T, Cohen O, Avigdor A, Amitai I, Shimoni A, Misgav M, Canaani J. The occurrence of thrombosis during intensive chemotherapy treatment for acute myeloid leukemia patients does not impact on long-term survival. Ann Hematol. 2023;102(5):1037–43. https://doi.org/10.1007/s00277-023-05158-w.
Guzmán-Uribe P, Rosas-López A, Zepeda-León J, Crespo-Solís E. Incidence of thrombosis in adults with acute leukemia: a single center experience in Mexico. Rev Investig Clin organo del Hosp Enfermedades la Nutr. 2013;65(2):130–40.
Koprivnikar J, McCloskey J, Faderl S. Safety, efficacy, and clinical utility of asparaginase in the treatment of adult patients with acute lymphoblastic leukemia. Onco Targets Ther. 2017;10:1413–22.
Mohren M, Markmann I, Jentsch-Ullrich K, Koenigsmann M, Lutze G, Franke A. Increased risk of venous thromboembolism in patients with acute leukaemia. Br J Cancer. 2006;94(2):200–2.
Del Principe MI, Buccisano F, Maurillo L, Venditti D, Cefalo M, Sarlo C, et al. Infections increase the risk of central venous catheter-related thrombosis in adult acute myeloid leukemia. Thromb Res. 2013;132(5):511–4.
Gangaraju R, Gahagan A, Bhatia S, Kenzik K. Venous-thromboembolism in elderly patients with acute myeloid leukemia. Thromb Res. 2021;200:9–11.
Antoniak S, Phungphong S, Cheng Z, Jensen BC. Novel mechanisms of anthracycline-induced cardiovascular toxicity: a focus on thrombosis, cardiac atrophy, and programmed cell death. Front Cardiovasc Med. 2021;8: 817977.
Pantic N, Virijevic M, Pravdic Z, Sabljic N, Bukumiric Z, Cvetkovic M, Rajic J, Vidovic A, Todorovic-Balint M, Suvajdzic-Vukovic N, Antic D, Mitrovic M. PB1832: arterial thrombosis and acute myeloid leukemia – is there a connection? Hemasphere. 2022;6(Suppl):1712–13. https://doi.org/10.1097/01.HS9.0000850180.00913.18.
Kattih B, Shirvani A, Klement P, Garrido AM, Gabdoulline R, Liebich A, et al. IDH1/2 mutations in acute myeloid leukemia patients and risk of coronary artery disease and cardiac dysfunction-a retrospective propensity score analysis. Leukemia. 2021;35(5):1301–16.
Calvillo-Argüelles O, Schoffel A, Capo-Chichi J-M, Abdel-Qadir H, Schuh A, Carrillo-Estrada M, et al. Cardiovascular disease among patients with AML and CHIP-related mutations. JACC CardioOncol. 2022;4(1):38–49.
Khorana AA, Kuderer NM, Culakova E, Lyman GH, Francis CW. Development and validation of a predictive model for chemotherapy-associated thrombosis. Blood. 2008;111(10):4902–7.
Verso M, Agnelli G, Barni S, Gasparini G, LaBianca R. A modified Khorana risk assessment score for venous thromboembolism in cancer patients receiving chemotherapy: the Protecht score. Int Emerg Med. 2012;7:291–2.
Pelzer U, Sinn M, Stieler J, Riess H. Primary pharmacological prevention of thromboembolic events in ambulatory patients with advanced pancreatic cancer treated with chemotherapy? Dtsch Med Wochenschr. 2013;138(41):2084–8.
Ay C, Dunkler D, Marosi C, Chiriac A-L, Vormittag R, Simanek R, et al. Prediction of venous thromboembolism in cancer patients. Blood. 2010;116(24):5377–82.
Cella CA, Di Minno G, Carlomagno C, Arcopinto M, Cerbone AM, Matano E, et al. Preventing venous thromboembolism in ambulatory cancer patients: the ONKOTEV study. Oncologist. 2017;22(5):601–8.
Muñoz Martín AJ, Ortega I, Font C, Pachón V, Castellón V, Martínez-Marín V, et al. Multivariable clinical-genetic risk model for predicting venous thromboembolic events in patients with cancer. Br J Cancer. 2018;118(8):1056–61.
Gerotziafas GT, Taher A, Abdel-Razeq H, AboElnazar E, Spyropoulos AC, El Shemmari S, et al. A predictive score for thrombosis associated with breast, colorectal, lung, or ovarian cancer: the prospective COMPASS-Cancer-Associated Thrombosis Study. Oncologist. 2017;22(10):1222–31.
Pabinger I, van Es N, Heinze G, Posch F, Riedl J, Reitter E-M, et al. A clinical prediction model for cancer-associated venous thromboembolism: a development and validation study in two independent prospective cohorts. Lancet Haematol. 2018;5(7):e289–98.
Moik F, Englisch C, Pabinger I, Ay C. Risk assessment models of cancer-associated thrombosis - Potentials and perspectives. Thrombosis Update. 2021;5:100075. https://doi.org/10.1016/j.tru.2021.100075.
Mirza A-S, Yun S, Ali N Al, Shin H, O’Neil JL, Elharake M, et al. Validation of the Khorana score in acute myeloid leukemia patients: a single-institution experience. Thromb J. 2019;17:13.
Samuelson Bannow BT, Lee A, Khorana AA, Zwicker JI, Noble S, Ay C, Carrier M. Management of cancer-associated thrombosis in patients with thrombocytopenia: guidance from the SSC of the ISTH. J Thromb Haemost. 2018;16(6):1246–9. https://doi.org/10.1111/jth.14015.
Kopolovic I, Lee AYY, Wu C. Management and outcomes of cancer-associated venous thromboembolism in patients with concomitant thrombocytopenia: a retrospective cohort study. Ann Hematol. 2015;94(2):329–36.
Poh C, Brunson A, Keegan T, Wun T, Mahajan A. Incidence of upper extremity deep vein thrombosis in acute leukemia and effect on mortality. TH Open. 2020;04(04):e309–17.
• Falanga A, Ay C, Di Nisio M, Gerotziafas G, Jara-Palomares L, Langer F, Lecumberri R, Mandala M, Maraveyas A, Pabinger I, Sinn M, Syrigos K, Young A, Jordan K, ESMO Guidelines Committee, Electronic address: clinicalguidelines@esmo.org. Venous thromboembolism in cancer patients: ESMO clinical practice guideline. Ann Oncol. 2023:S0923-7534(22)04786-X. https://doi.org/10.1016/j.annonc.2022.12.014. Most recent Clinical Practice Guideline pubblicated by ESMO.
• Key NS, Khorana AA, Kuderer NM, Bohlke K, Lee AYY, Arcelus JI, et al. Venous thromboembolism prophylaxis and treatment in patients with cancer: ASCO clinical practice guideline update. J Clin Oncol . 2020;38(5):496–520. ASCO Clinical Practice Guideline based on randomized controlled trials (RCTs) and meta-analyses.
Streiff MB, Abutalib SA, Farge D, Murphy M, Connors JM, Piazza G. Update on guidelines for the management of cancer-associated thrombosis. Oncologist. 2021;26(1):e24–40. https://doi.org/10.1002/onco.13596.
• Streiff MB, Holmstrom B, Angelini D, Ashrani A, Elshoury A, Fanikos J, et al. Cancer-associated venous thromboembolic disease, Version 2.2021, NCCN Clinical Practice Guidelines in Oncology. J Natl Compr Canc Netw. 2021;19(10):1181–201. NCCN guidelines based on clinical data, meta-analyses and systematic reviews of clinical studies, and treatment guidelines developed by other organizations.
• Farge D, Frere C, Connors JM, Khorana AA, Kakkar A, Ay C, et al. 2022 international clinical practice guidelines for the treatment and prophylaxis of venous thromboembolism in patients with cancer, including patients with COVID-19. Lancet Oncol. 2022;23(7):e334–47. ITAC guidelines based on new evidence on the treatment and prophylaxis of cancer-associated thrombosis, including in patients with cancer and with COVID-19.
•• Falanga A, Leader A, Ambaglio C, Bagoly Z, Castaman G, Elalamy I, et al. EHA Guidelines on management of antithrombotic treatments in thrombocytopenic patients with cancer. HemaSphere. 2022;6(8):e750. Clinical practice guideline for management of patients with cancer and thrombocytopenia produced by EHA in collaboration with European Society of Cardiology.
Lee AYY, Kamphuisen PW, Meyer G, Bauersachs R, Janas MS, Jarner MF, et al. Tinzaparin vs Warfarin for treatment of acute venous thromboembolism in patients with active cancer: a randomized clinical trial. JAMA. 2015;314(7):677–86.
Lee AYY, Levine MN, Baker RI, Bowden C, Kakkar AK, Prins M, et al. Low-molecular-weight heparin versus a coumarin for the prevention of recurrent venous thromboembolism in patients with cancer. N Engl J Med. 2003;349(2):146–53.
Agnelli G, Becattini C, Meyer G, Muñoz A, Huisman MV, Connors JM, et al. Apixaban for the treatment of venous thromboembolism associated with cancer. N Engl J Med. 2020;382(17):1599–607.
Carrier M, Abou-Nassar K, Mallick R, Tagalakis V, Shivakumar S, Schattner A, et al. Apixaban to prevent venous thromboembolism in patients with cancer. N Engl J Med [Internet]. 2019;380(8):711–9. Available from: https://doi.org/10.1056/NEJMoa1814468.
Planquette B, Bertoletti L, Charles-Nelson A, Laporte S, Grange C, Mahé I, et al. Rivaroxaban vs dalteparin in cancer-associated thromboembolism: a randomized trial. Chest. 2022;161(3):781–90.
Young AM, Marshall A, Thirlwall J, Chapman O, Lokare A, Hill C, et al. Comparison of an oral factor Xa inhibitor with low molecular weight heparin in patients with cancer with venous thromboembolism: results of a randomized trial (SELECT-D). J Clin Oncol. 2018;36(20):2017–23.
McBane RD 2nd, Wysokinski WE, Le-Rademacher JG, Zemla T, Ashrani A, Tafur A, et al. Apixaban and dalteparin in active malignancy-associated venous thromboembolism: the ADAM VTE trial. J Thromb Haemost. 2020;18(2):411–21.
Raskob GE, van Es N, Verhamme P, Carrier M, Di Nisio M, Garcia D, et al. Edoxaban for the treatment of cancer-associated venous thromboembolism. N Engl J Med [Internet]. 2018;378(7):615–24. Available from: https://doi.org/10.1056/NEJMoa1711948.
Khorana AA, Soff GA, Kakkar AK, Vadhan-Raj S, Riess H, Wun T, et al. Rivaroxaban for thromboprophylaxis in high-risk ambulatory patients with cancer. N Engl J Med [Internet]. 2019;380(8):720–8. Available from: https://doi.org/10.1056/NEJMoa1814630.
Falanga A, Le GG, Carrier M, Abdel-Razeq H, Ay C, Martin AJM, et al. Management of cancer-associated thrombosis: unmet needs and future perspectives. TH Open Companion J Thromb Haemost. 2021;5(3):e376–86.
Crespo-Solís E. Thrombosis and acute leukemia. Hematology. 2012;17(Suppl 1):S169–73.
Kahale LA, Hakoum MB, Tsolakian IG, Matar CF, Terrenato I, Sperati F, et al. Anticoagulation for the long-term treatment of venous thromboembolism in people with cancer. Cochrane database Syst Rev. 2018;6(6):CD006650.
Houghton DE, Billett HH, Gaddh M, Onadeko O, George G, Wang T-F, et al. Risk of pulmonary emboli after removal of an upper extremity central catheter associated with a deep vein thrombosis. Blood Adv. 2021;5(14):2807–12.
Zwicker JI, Connolly G, Carrier M, Kamphuisen PW, Lee AYY. Catheter-associated deep vein thrombosis of the upper extremity in cancer patients: guidance from the SSC of the ISTH. J Thromb Haemost. 2014;12(5):796–800.
Wang T-F, Leader A, Sanfilippo KM. Thrombosis and bleeding in hematological malignancy. Best Pract Res Clin Haematol. 2022;35(1): 101353.
Author information
Authors and Affiliations
Corresponding author
Ethics declarations
Conflict of Interest
The authors report no relevant conflict of interest.
Human and Animal Rights and Informed Consent
All reported studies/experiments with human or animal subjects performed by the authors have been previously published and complied with all applicable ethical standards (including the Helsinki declaration and its amendments, institutional/national research committee standards, and international/national/institutional guidelines).
Additional information
Publisher's Note
Springer Nature remains neutral with regard to jurisdictional claims in published maps and institutional affiliations.
Rights and permissions
Springer Nature or its licensor (e.g. a society or other partner) holds exclusive rights to this article under a publishing agreement with the author(s) or other rightsholder(s); author self-archiving of the accepted manuscript version of this article is solely governed by the terms of such publishing agreement and applicable law.
About this article
Cite this article
Olivi, M., Di Biase, F., Lanzarone, G. et al. Thrombosis in Acute Myeloid Leukemia: Pathogenesis, Risk Factors and Therapeutic Challenges. Curr. Treat. Options in Oncol. 24, 693–710 (2023). https://doi.org/10.1007/s11864-023-01089-w
Accepted:
Published:
Issue Date:
DOI: https://doi.org/10.1007/s11864-023-01089-w