Abstract
Propose
High salt intake, correlated with high salt taste threshold, may accelerate renal injury in chronic kidney disease (CKD) patients. However, few studies have focused on factors that influence salt taste threshold. Therefore, we aimed to identify factors that influence the salt taste threshold of CKD patients, to provide more precise salt restriction recommendations in dietary therapy.
Methods
Between April 2016 and March 2019, we measured the salt taste threshold of 1019 CKD patients, aged 22–78 years, from 52 hospitals across southwestern China, and then we performed a cross-sectional study.
Results
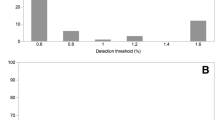
The mean salt taste threshold was 0.37 ± 0.16% NaCl. There were 115 (11.3%), 670 (65.7%), and 234 (23.0%), respectively, patients who had low (≤ 0.1% NaCl), medium (0.1–0.4% NaCl), and high (> 0.4% NaCl) salt taste thresholds. One-way ANOVA and regression results revealed that sex (male), age, decreased estimated glomerular filtration rate, and absence of salt restriction were factors that influenced CKD groups with high salt taste threshold.
Conclusion
We found an independent correlation between contributory factors including sex, age, eGFR, and salt restriction behavior of subjects with the salt taste threshold of CKD patients. Our findings also offer insights on salt taste thresholds that could be useful for clinicians advising salt restriction to impair the salt taste sensitivity of the corresponding populations.

Similar content being viewed by others
References
Kusaba T, Mori Y, Masami O et al (2009) Sodium restriction improves the gustatory threshold for salty taste in patients with chronic kidney disease. Kidney Int 76(6):638–643
Manley KJ (2015) Taste genetics and gastrointestinal symptoms experienced in chronic kidney disease. Eur J Clin Nutr 69(7):781–785
Lava SAG, Bianchetti MG, Simonetti GD (2015) Salt intake in children and its consequences on blood pressure. Pediatr Nephrol 30(9):1389–1396
Jeon JW, Kim SB (2017) Salt taste thresholds and salt preference in patients with chronic kidney disease according to the stage: A cross-sectional study. Nephrol Dial Transpl 32:MP348.
Kim TH, Kim YH, Bae NY et al (2018) Salty taste thresholds and preference in patients with chronic kidney disease according to disease stage: A cross-sectional study. Nutr Diet 75(1):59–64
McMahon EJ, Campbell KL, Bauer JD (2014) Taste perception in kidney disease and relationship to dietary sodium intake. Appetite 83:236–241
Gorstein J, van der Haar F, Codling K et al (2016) Performance of rapid test kits to assess household coverage of iodized salt. Public Health Nutr 19(15):2712–2724
Pingel J, Ostwald J, Pau HW et al (2010) Normative data for a solution-based taste test. Eur Arch Opto-Rhino-L 267(12):1911–1917
Wright JA, Cavanaugh KL (2010) Dietary sodium in chronic kidney disease: A comprehensive approach. Semin Dialysis 23(4):415–421
McMahon EJ, Bauer JD, Hawley CM et al (2012) The effect of lowering salt intake on ambulatory blood pressure to reduce cardiovascular risk in chronic kidney disease (Low salt CKD study): Protocol of a randomized trial. BMC Nephrol 13:137
van der Eijk I, Allman Farinelli MA (1997) Taste testing in renal patients. J Ren Nutr 7(1):3–9
Manley KJ, Haryono RY, Keast RSJ (2012) Taste changes and saliva composition in chronic kidney disease. Ren Soc Australas J 8(2):56–60
Yang WG, Chen CB, Wang ZX et al (2011) A case-control study on the relationship between salt intake and salty taste and risk of gastric cancer. World J Gastroentero 17(15):2049–2053
Pinhati RR, Ferreira RE, Carminatti M et al (2021) The prevalence and associated factors of nonadherence to antihypertensive medication in secondary healthcare. Int Urol Nephrol 53(8):1639–1648
World Health Organization (2006) BMI classification, global database on body mass index.
Lee JY, Cho DS, Kim HJ (2012) The effect of salt usage behavior on sodium intake and excretion among Korean women. Nutr Res Pract 6(3):232–237
Kim HJ, Paik HY, Lee SY et al (2007) Salt usage behaviors are related to urinary sodium excretion in normotensive Korean adults. Asia Pac J Clin Nutr 16(1):122–128
Kim MK, Lee KG (2014) Consumer awareness and interest toward sodium reduction trends in Korea. J Food Sci 79(7):S1416–S1423
Tanaka T, Okamura T, Miura K et al (2002) A simple method to estimate populational 24-h urinary sodium and potassium excretion using a casual urine specimen. J Hum Hypertens 16(2):97–103
Gravina SA, Yep GL, Khan M (2013) Human biology of taste. Ann Saudi Med 33(3):217–222
Shier D, Butler J, Lewis R (2015) Hole’s human anatomy and physiology. McGraw-Hill Education.
Manley KJ (2014) Saliva composition and upper gastrointestinal symptoms in chronic kidney disease. J Renal Care 40(3):172–179
Landis BN, Welge-Luessen A, Bramerson A et al (2009) “Taste Strips” - A rapid, lateralized, gustatory bedside identification test based on impregnated filter papers. J Neurol 256(2):242–248
Yoshinaka M, Ikebe K, Uota M et al (2016) Age and sex differences in the taste sensitivity of young adult, young-old and old-old Japanese. Geriatr Gerontol Int 16(12):1281–1288
Running CA, Mattes RD, Tucker RM (2013) Fat taste in humans: Sources of within- and between-subject variability. Prog Lipid Res 52(4):438–445
Doets EL, Kremer S (2016) The silver sensory experience: A review of senior consumers’ food perception, liking and intake. Food Qual Prefer 48:316–332
Manley KJ (2017) Will mouth wash solutions of water, salt, sodium bicarbonate or citric acid improve upper gastrointestinal symptoms in chronic kidney disease. Nephrology 22(3):213–219
Anuradha BR, Katta S, Kode VS et al (2015) Oral and salivary changes in patients with chronic kidney disease: A clinical and biochemical study. J Indian Soc Periodontol 19(3):297–301
Burge JC, Park HS, Whitlock CP et al (1979) Taste acuity in patients undergoing long-term hemodialysis. Kidney Int 15(1):49–53
Astbäck J, Fernström A, Hylander B et al (1999) Taste buds and neuronal markers in patients with chronic renal failure. Periton Dialysis Int 19(1):S315–S323
Acknowledgements
The authors thank Dr. J.X. Guo from Chengdu University for his support to discuss the data statistics. The authors thank AiMi Academic Services (www.aimieditor.com) for English language editing and review services. This work was financially supported by the Sichuan Provincial People's Hospital (no specific grant number).
Author information
Authors and Affiliations
Contributions
YW, MF and RT designed the experiments and wrote the manuscript. LL, FL and YY collected the data of salt restriction behaviors and spot tests for urine sodium. MF and FL collected the data from electronic medical records. YW, MF and RT performed and analyzed the AVONA results and regression relations. YW wrote and revised the manuscript. WY and MF supervised the cross-sectional study. All authors contributed to the scientific discussion and edited the manuscript.
Corresponding authors
Ethics declarations
Conflict of interest
The authors declare no conflict of interest.
Additional information
Publisher's Note
Springer Nature remains neutral with regard to jurisdictional claims in published maps and institutional affiliations.
Rights and permissions
Springer Nature or its licensor (e.g. a society or other partner) holds exclusive rights to this article under a publishing agreement with the author(s) or other rightsholder(s); author self-archiving of the accepted manuscript version of this article is solely governed by the terms of such publishing agreement and applicable law.
About this article
Cite this article
Wu, Y., Liao, F., Liao, L. et al. Salt taste threshold and contributory factors of chronic kidney disease patients: a cross-sectional study. Int Urol Nephrol 55, 1211–1218 (2023). https://doi.org/10.1007/s11255-022-03403-1
Received:
Accepted:
Published:
Issue Date:
DOI: https://doi.org/10.1007/s11255-022-03403-1