Abstract
Parkinson’s disease is a neurodegenerative disorder characterized by slow movement, tremors, and stiffness caused due to loss of dopaminergic neurons caused in the brain’s substantia nigra. The concentration of dopamine is decreased in the brain. Parkinson’s disease may be happened because of various genetic and environmental factors. Parkinson’s disease is related to the irregular expression of the monoamine oxidase (MAO) enzyme, precisely type B, which causes the oxidative deamination of biogenic amines such as dopamine. MAO-B inhibitors, available currently in the market, carry various adverse effects such as dizziness, nausea, vomiting, lightheadedness, fainting, etc. So, there is an urgent need to develop new MAO-B inhibitors with minimum side effects. In this review, we have included recently studied compounds (2018 onwards). Agrawal et al. reported MAO-B inhibitors with IC50 0.0051 µM and showed good binding affinity. Enriquez et al. reported a compound with IC50 144 nM and bind with some critical amino acid residue Tyr60, Ile198, and Ile199. This article also describes the structure–activity relationship of the compounds and clinical trial studies of related derivatives. These compounds may be used as lead compounds to develop potent compounds as MAO-B inhibitors.
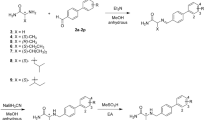
Graphic Abstract

Similar content being viewed by others
Avoid common mistakes on your manuscript.
Introduction
Parkinson’s disease (PD) is a progressive neurodegenerative disease clinically known as a movement disorder. It is a leading cause of motor problems and mental disabilities [1, 2]. Loss of dopaminergic neurons in substantia nigra which results in reduction in the concentration of dopamine (which is an inhibitory neurotransmitter) in the brain [3,4,5] is characteristic in PD. Due to inadequate dopamine concentration (Fig. 1), there is less inhibition of striatal neurons(control the balance of body movements), which is responsible for the difficulty in controlling movements in PD patients [6].
Age is a significant risk factor in Parkinson’s disease development, majorly older people are affected, but people below the age of 21 years(juvenile cases) are also affected [7, 8]. There are two types of symptoms of PD, motor symptoms such as tremors, stiffness, and slow movements, and a problem with balance and non-motor symptoms such as depression, insomnia, and cognitive dysfunction [9, 10]. Parkinsonism caused by Parkinson’s disease is called primary parkinsonism, and the parkinsonism caused by other neurodegenerative diseases is called secondary parkinsonism [11, 12]. Parkinson’s disease is a multifactorial condition that contains genetic and various environmental factors which give rise to the genesis of the disease [1]. This disease has diverse nature as its symptomology differs from one individual to another; this disease may be influenced by demographical factors, environmental factors, and exposure to some neurotoxins which target the substantia nigra neurons [13]. Risk factors that may cause PD are exposure to some pesticides or cleaning chemicals, old age, family history, and inhalation of heavy metals [14,15,16]. The most important mechanisms involved in the development of Parkinson’s disease include misfolded aggregates of proteins, oxidative stress, mitochondrial damage, failure of protein clearance pathway, neuroinflammation, and genetic mutation [17, 18]. According to the survey, the prevalence of Parkinson’s disease in elderly patients ranges from 20 to 70% [19]. A report by global trends 2019 suggested that the age-standardized incidence rate of Parkinson’s disease was 13.43/100,000 [20]. For society, Parkinson’s disease conveys a mounting socioeconomic burden [9]. Cases of Parkinson’s disease are higher in men than women, which may be due to estrogen, which may act as a neuroprotective agent. The risk of disease development is lower in females, but they have higher mortality and progression of the disease [21, 22]. Out of various reasons, the leading cause of PD is recognized as the irregular expression of mitochondrial monoamine oxidases (MAO) enzyme, which may be related to the unnecessary metabolism of monoamine neurotransmitters, responsible for various neurodegenerative disorders [23,24,25,26].
The therapy which is currently in use focuses on treating PD by improving motor problems by increasing the dopamine concentration in the brain or by stimulating the dopamine (DA) receptors [27, 28]. Approved drugs that are used to treat Parkinson’s disease (Fig. 2). Dopamine precursor Levodopa, Carbidopa/Benserazide [29, 30], which are peripheral decarboxylase inhibitors. Agonists of dopamine receptors such as pramipexole/Apomorphine [31]. MAO-B inhibitors [32] such as Selegiline/Rasagiline/Safinamide. COMT inhibitors [33] as Tolcapone/Opicapone/Entacapone comprises the approved drugs which are in use to treat Parkinson’s disease.rasagiline and Selegiline are irreversible MAO-B inhibitors, whereas Safinamide is a reversible MAO-B inhibitor recently approved by the food and Drug Administration (FDA) as an anti-parkinsonian agent [34, 35]. However, these drugs have limitations, such as safinamide causing retinopathy and several clinical problems in patients with liver impairment [36]. So, there is an urgent need to design and develop novel reversible MAO-B inhibitors to circumvent these problems. Other than MAO-B other targets which can be used to treat PD are α-Syn, Glutamate receptors, Molecular chaperones and autophagic pathways, and GPR109A [37]. PD belongs to synucleinopathy which develops with time. Degeneration of dopaminergic neurons and accumulation of alpha-syn protein intracellularly as Lewy bodies is the major reason for pathology of PD progression [38]. Glutamate receptors modulate neural transmission in basal ganglia and this ability of glutamate receptors is used as possible targets for the treatment of PD. The primary motor symptoms of PD are alleviated due to modulated activity of the receptors in the dopamine replacement therapy. The reduced progression of PD is delaying the neurodegenerative process due to the antagonism of these receptors [39]. Molecular chaperones regulate cellular proteostasis by balancing the folding and misfolding processes. Misfolded proteins are corrected by the chaperone system and contribute to proteostasis. In the PD brain, autophagic mechanisms are markedly dysregulated. The autophagic mechanisms that influence the illness phenotype include genes associated to PD [40, 41]. GPR109A is a G protein-coupled receptor which is also knowns as hydroxycarboxylic acid receptor 2. The GPR109A is found in macrophages and has a role in inflammation. In PD, GPR109A mediates inflammatory action in PD and can be targeted for treatment [42]. Various medications are used to treat PD, but MAO-B inhibitors play a significant role in treating PD. MAO-B inhibitors reduce the degradation of dopamine by penetrating the blood–brain barrier and inhibit central MAO activity [43]. MAO-B inhibitors showed very good safety and efficacy in early and advanced stages of PD. It is reported in some clinical studies that when the patient use the MAO-B inhibitors for a longer duration there is a decrease in the consumption of levodopa [44, 45].
Mechanism of anti-parkinsonian drugs
Tyrosine, which is transferred from the blood–brain barrier, is converted to levodopa with the help of Tyrosine hydroxylase (TH) (Fig. 3). Levodopa is then converted to Dopamine by aromatic amino acid decarboxylase (AADC) [46,47,48]. Dopamine formed is stored in vesicles until they are released into the synaptic cleft and binds and activates dopamine receptors in the striatum's neurons [49, 50]. The free dopamine is metabolized by the MAO-B enzyme into 3,4-dihydroxy phenylacetic acid (DOPAC) and further converted to Homovanillic acid (HMV) by COMT [51, 52]. Levodopa used in the treatment of PD, is a Dopamine precursor. Levodopa can cross the blood–brain barrier and be converted to Dopamine by the Dopa decarboxylase (DDC) enzyme in the presynaptic neuron of substantia nigra [53, 54]. The Dopamine formed is stored in vesicles until they are released into the synaptic cleft and binds and activates dopamine receptors on the neurons of the striatum, which control the motor activities of the body, smoothening movements and reducing muscle tone [55, 56]. After binding to the receptors and its activation, the DA quickly unbound from the receptor reuptake by the Dopamine transporter (DAT) [57, 58].
Mechanism of action of Drugs which are used in Parkinson’s disease. COMT catechol-O-methyl transferase, DA dopamine, DDC dopa-decarboxylase, DOPAC 3,4-dihydroxyphenylacetic acid, HVA homovanillic acid, L-DOPA levodopa, MAO-B monoamine oxidase B, 3-MT 3-methoxytyramine, 3-O-MD 3-O-methyldopa, DAT dopamine transporter
Levodopa in the periphery is susceptible to the metabolism by Catechol-O-methyl transferase (COMT), which can be inhibited by drugs such as Tolcapone or Entacapone and Dopa decarboxylase (DDC), which are inhibited by drugs such as Carbidopa or Benserazide [59, 60].
To prevent the metabolism of Dopamine in the brain, drugs such as MAO-B (Monoamine oxidase type B) inhibitors (Selegiline, Rasagiline, Safinamide) and COMT inhibitors (Tolcapone or Entacapone) are used [61, 62]. In addition, dopamine receptor agonists (Bromocriptine, Pramipexole, Ropinirole) activate the Dopamine receptors, which further control the mobility of the body [63, 64].
Problems in currently available mao inhibitors
The major metabolic enzymes for regulating biogenic amine levels in the brain and other tissues are monoamine oxidases (MAOs). They are present in the outer membrane of mitochondria [65].
There are two isoforms of this enzyme, MAO-A and MAO-B which are around 70% the same in amino acid sequence and have a similar structure of the active site [66]. All human tissues contain MAOs, but MAO-A predominates in the gastrointestinal system, placenta, and heart, whereas MAO-B predominates in platelets and glial cells in the brain [67]. MAOs are linked covalently to flavin adenine dinucleotide (FAD) [68]. The substrates for MAO-A are adrenaline and serotonin, whereas for MAO-B, the substrates are benzylamine and phenylethylamine [69, 70]. Inhibitors of the MAO-A enzyme have therapeutic value against depression and anxiety, and MAO-B inhibitors are used in the treatment of Parkinson’s disease and Alzheimer’s disease [71, 72]. Earlier non-selective MAOs inhibitors were used, which were irreversible, but because of their toxicity, their use was reduced because Tyramine enters the systemic circulation when MAO-A is irreversibly blocked, which causes the release of norepinephrine from peripheral adrenergic neurons resulting in a hypertensive crisis, sometimes known as the "cheese reaction” [73]. It is a highly effective and helpful strategy to create novel MAO inhibitors (MAOIs) for treating various neurological and psychiatric illnesses [74]. So reversible inhibitors of MAO-A, such as moclobemide and clorgyline are used in the treatment of depression [75, 76], but these drugs have some adverse effects, such as headache, insomnia, and liver damage [77]. MAO inhibitors used in the treatment of depressive disorder, may promote the impairment of cognition and result in the progression of dementia [78]. Drugs that are in use in the treatment of Parkinson's disease areSelegiline, Rasagiline, and safinamide, which are the selective inhibitors of MAO-B [79]. Selegiline and Rasagiline's lack of an apparent neuroprotective effect in clinical trials restricts their therapeutic applicability [80]. The main side effects of Selegiline, when used to treat Parkinson's disease, are hypotension, vertigo, and akinesia [81, 82]. It was also suggested that MAO inhibitors might have anticancer properties. Multiple cancer cells have been shown to overexpress MAO, and inhibiting the enzyme had an antiproliferative effect [83]. Rasagiline is an irreversible inhibitor of MAO-B, and it binds covalently with the active site resulting in side effects, but safinamide is a reversible inhibitor with lesser side effects [84, 85]. But safinamide cause retinopathy and several clinical problems in patients with liver impairment [36]. Due to all these limitations of the currently present MAO inhibitors, there is a demand to develop novel MAO-B inhibitors that could be used to treat Parkinson’s disease.
Recent advancements
In a study, Yeon et al. synthesized a novel series of 4-(Benzyloxy)phenyl and Biphenyl-4-yl derivatives for monoamine oxidase B (MAO-B) inhibition. In the synthesized series, compound 1 showed potential activity with an IC50 value of 0.009 µM against MAO-B. Additionally, structure–activity relationship (SAR) studies showed that compounds that carried no carbon between biaryl-linked units showed lower inhibitory activity. At the same time, amine and trifluoromethyl substitutions at the para position were responsible for the more significant activity of compounds rather than ortho or meta substituents. Furthermore, according to substrate-dependent kinetics, compound 1 was a competitive MAO-B inhibitor. In vivo study of compound 1 for Parkinson’s disease by MPTP assay showed improved motor impairment activity further correlated with MAO-B inhibitory activity in the brain. The most potent compound 1 (4-((4-(Trifluoromethyl)benzyl)oxy)phenyl)methanaminium chloride, showed better activity against PD, and it was found in the shielding of Dopaminergic neurons. Several behavioral abnormalities have been observed with the MPTP-induced mouse model used in the treatment of PD. (Fig. 4) showed the various substituents and linkers for generating potential compounds as MAO-B inhibitors [86].
Mellado et al. reported a new series of seven prenylated chalcone derivatives against MAOs. Out of those seven derivatives, compound 3 (E)-3-(4-(Dimethylamino)phenyl)-1-(4-hydroxy-3-(3-methylbut-2-en-1-yl)phenyl)prop-2-en-1-one showed the most potent MAO-B inhibitory activity with an IC50 value of 8.19 µM. Furthermore, structure–activity relationship (SAR) studies revealed that Phenyl and methoxy group substitution inactivates the compound due to steric impedance at the active site of the enzyme, ortho substitution is less active than para substitution, and introduction of dimethylamino group increased the MAOs inhibitory potency (Fig. 5). The Kinetics study indicated that compound 3 competitively inhibited the enzyme MAO-B. It was found that compounds 2 (E)-1-(4-Hydroxy-3-(3-methylbut-2-en-1-yl)phenyl)-3-(4-methoxyphenyl)prop-2-en-1-one and 3 showed potential MAOs inhibitory activity with better antioxidant activity as compared to standard compound BHT (Butylated hydroxytoluene). The molecular docking studies showed that the activities of MAO-B inhibitors are related to hydrogen bonds and hydrophobic bonds with Tyr398 and Tyr435 amino acid residues, respectively. So, these compounds can be suitable candidates for lead discovery for PD [87].
Agrawal et al. designed and synthesized a series of isoxazole carbohydrazides derivatives against MAOs enzyme. In vitro studies showed that compounds did not show significant activity against MAO-A, but some compounds showed MAO-B inhibitory activity at IC50 equal to 50 µM. Compound 4 (Z)-5-Phenyl-N'-(1-(m-tolyl)ethylidene)isoxazole-3-carbohydrazide, which carried a methyl group at the para position of the phenyl ring, appeared as the most potent MAO-B inhibitor with an IC50 value of 0.0051 μM, followed by compound 5 (Z)-N'-(1-(3,4-Dimethoxyphenyl)ethylidene)-5-phenylisoxazole-3-carbohydrazide with methoxy substituent at the meta and para positions of phenyl ring showed an IC50 value of 0.0059 μM. The SAR showed that the substitution of the phenyl ring with the electron-withdrawing group (EWG) decreased the activity, and substituting the electron-donating group (EDG) improves the activity (Fig. 6). The enzyme kinetic studies revealed that compounds 4 and 5 were reversible and competitive inhibitors. The docking studies further unlocked the potent inhibitors' binding site interactions, and compounds fit well in the active site of MAO-B near the FAD cofactor. The synthesized compounds were subjected to in silico ADME evaluation. All the compounds displayed favorable ADME profiles and were predicted to have good oral bioavailability. Thus, the active compounds 4 and 5 obtained in this series can be promising leads for developing isoxazole-based potent MAO-B inhibitors for treating PD [88].
In a recent study, Parambi et al. reported the synthesis of 26 oxygenated chalcone derivatives as the inhibitors of MAOs enzyme. All derivatives were potent against MAO-B, out of which compound 6 (E)-1-(Benzo[d][1,3]dioxol-5-yl)-3-(4-fluorophenyl)prop-2-en-1-one, was the most potent compound with an IC50 value of 0.0021 μM. On the other hand, most of the derivatives potently inhibited MAO-A, and Compound 7 (E)-1-(Benzo[d][1,3]dioxol-5-yl)-3-(4-ethylphenyl)prop-2-en-1-one, was the most potent MAO-A inhibitor showed an IC50 value of 0.029 μM. Additionally, dialysis experiments showed that compounds 6 and 7 were reversible inhibitions of the MAOs enzyme. The SAR studies disclosed that replacement of halogen atoms such as fluorine from para to any other position results in a decrease in the MAO-B inhibition, ethyl group at para position results in non-selective MAO-A inhibition and increasing the number of ‘n’ (number of alkyl groups between two oxygen atoms) results in an increase of inhibition potency (Fig. 7). The Kinetic studies showed that 6 and 7 competitively inhibited both the MAO isoforms, MAO-A and MAO-B (Ki values of 0.016 and 0.00050 μM respectively). Cytotoxicity studies revealed that potent compounds were non-toxic at 200 µg/ml with a tiny percentage of cell death [89].
Enriquez et al. reported twelve novel 3-thiophenylcoumarins as effective inhibitors of MAOs enzyme. Compound 8 3-(4-Bromothiophen-2-yl)-7-hydroxy-2H-chromen-2-one was found to be the most potent compound with an IC50 value of 144 nM. Additionally, structure–activity relationship studies (Fig. 8) showed that the presence of a hydroxy group at 8-position of coumarin enhances the MAO-A inhibitory activity, coumarin scaffold is essential for activity, selectivity for MAO-B increased when a single hydroxy group is present at 7-position of the coumarin ring. The Kinetics studies showed that compounds were reversible inhibitors. The derivatives showed neuroprotective agents in patients who were suffering from Parkinson’s Disease according to free radical scavenging assay. In this assay, compound 9 3-(4-Bromothiophen-2-yl)-7,8-dihydroxy-2H-chromen-2-one displayed an EC50 value of 5.82 µM near the EC50 value of vitamin C i.e., 5.02 µM. MTT (dimethyldiphenyltetrazolium bromide) method was used to check the neurotoxicity profile of the compounds, and it found that there is a significant decrease in cell viability. Compound 9 was evaluated against ROS (reactive oxygen species) in SH-SY5Y using DCFDA assay (conversion of dichlorofluorescindiacetate to fluorescence dye dichlorofluorescein) and found that the compounds showed a significant effect against ROS formation. In vivo studies on the most potent compound 8 revealed an increased locomotor activity, time percentage in movement, and movement velocity compared to reference compound selegiline. All the compounds showed a good pharmacokinetic profile and suitable physicochemical parameters in silico methods to be used as a candidate for lead optimization [90].
The same research group synthesized twelve novel Coumarin-pyridazine derivatives as MAO-B inhibitors. In vitro studies showed compound 3 was the most potent compound with an IC50 value of 60 nM against MAO-B. In vivo studies suggested compound 10 7-Bromo-3-(6-bromopyridazin-3-yl)-2H-chromen-2-one was a promising anti-parkinsonian agent. In structure–activity relationship studies, it was found that the presence of a bromine atom at C6 of pyridazine was good for the activity, and an additional increase in the inhibitory potency and selectivity was observed when bromine atom was present at the coumarin fragment, particularly at C7 (Fig. 9). In silico (by ADME-Tox prediction) study suggested that all the compounds exhibited drug-like properties [91]. The molecular docking studies disclosed some critical amino acid residues, such as Tyr60, Ile198, and Ile199, responsible for the activity of these coumarin-pyridazine derivatives [91].
Saglik et al. designed and synthesized a series of novel Benzylamine-sulphonamide derivatives for MAO-B. The structure was determined using spectroscopic methods such as 1H-NMR, 13C-NMR, and HRMS. In vitro studies revealed that all the compounds selectively inhibit the MAO-B enzyme and compounds 11 N-benzyl-2-((5-chlorobenzo[d]thiazol-2-yl)thio)-N-(4-sulfamoylphenyl)acetamide and compound 12 2-((5-chlorobenzo[d]thiazol-2-yl)thio)-N-(3-methylbenzyl)-N-(4-sulfamoylphenyl)acetamide were found to be most potent with IC50 values of 0.041 µM and 0.065 µM, respectively. In contrast, the reference compound selegiline had an IC50 value of 0.037 µM. Additionally, structure–activity relationship studies showed that the Presence of the sulfonamide group increased the inhibitory activity, the presence of the electron-withdrawing group (NO2) decreased the activity, and the Presence of the Benzothiazole enhanced the MAO-B inhibitory activity (Fig. 10). Kinetics studies revealed that compounds 11 and 12 showed a reversible and non-competitive inhibition in contrast to the conventional MAO inhibitors which were irreversible. Cytotoxicity assay was performed against the NIH3T3 cell line and found that compounds 11 and 12 showed an IC50 value of greater than 1000 which is significantly higher than the effective concentration, and it can be concluded that these compounds were non-cytotoxic at their effective concentration. Molecular docking studies were performed for compound 11, and found that it has a good binding affinity with the MAO-B enzyme [92].
In a study, Mathew et al. synthesized ten derivatives of methylthiosemicarbazones and evaluated them against MAOs and acetylcholinesterase. The most potent activity was shown by compounds 13 (E)-2-(1-(2,3-dihydrobenzo[b][1,4]dioxin-6-yl)ethylidene)-N-methylhydrazine-1-carbothioamide, compound 14 (E)-N-methyl-2-(1-(4-morpholinophenyl)ethylidene)hydrazine-1-carbothioamide, and compound 15 (E)-2-(1-(4-ethoxyphenyl)ethylidene)-N-methylhydrazine-1-carbothioamide with IC50 values 5.48, 7.06, and 8.03 µM, respectively. Additionally, SARs studies showed that the Presence of morpholine moiety is important for activity, compounds which contain five-membered attachments were less potent than the compounds which contain a six-membered attachment, and the introduction of methylenedioxy ring increases the activity (Fig. 11). Kinetics studies which were performed on compound 14, revealed that compound 14 is a competitive and reversible inhibitor of MAO-B with a mean Ki value of 2.39 µM. Cytotoxicity studies revealed that 14 is non-toxic to (African green monkey kidney cells) Vero cells (IC50 = 198.95 µg/mL). In silico studies revealed that compound 14 interacted with Tyr326 of MAO-B with pi-pi interactions and hydrophobic interactions, which played a vital role in holding the phenyl system in the entrance cavity of monoamine oxidase B enzyme [93, 94].
Lazewska et al. reported a novel series of 27 compounds based on 1-(3-(4-tert-butylphenoxy)propyl)piperidine ( compound 16b) as MAO-B inhibitors. Compound 16a 1-(3-(4-(tert-butyl)phenoxy)propyl)pyrrolidine was the most potent (IC50 = 2.7 nM), even higher than the reference compounds rasagiline and safinamide. The Structure–activity relationship studies showed that compounds that contain a cyclic amine moiety (such as pyrrolidine and piperidine) played a very significant role in hMAO-B inhibition. A decrease in activity was observed with an increase in the length of the linker carbon chain (Fig. 12). According to reversibility studies it was found that all the tested compounds are reversible inhibitors. The Kinetic studies suggested that the compounds have a mixed mode of inhibition. In vitro toxicity studies in the HER293 cell line revealed that 16b is safe at 50 µM concentration. In vivo studies showed that 16b possesses significant anti-parkinsonian as observed in the cross-leg position test, but a low positive effect was seen in the bar test [95].
In a recent study, Panova et al. synthesized a series of pyrazolo[1,5-a]qunoxalin-4-ones derivatives as MAOs inhibitors. Compound 17 2-(4-methoxyphenyl)-4-oxo-1l2,10l4-pyrazolo[2,3-a]quinoxaline-5(4H)-carbonitrile (IC50 = 0.763 µM) and compound 18 5-acetamido-4-oxo-2-phenyl-4,5-dihydro-1l2,10l4-pyrazolo[2,3-a]quinoxalin-7-yl acetate (IC50 = 0.181 µM) were specific inhibitors of MAO-A and MAO-B respectively. Compound 19 5-acetamido-2-(4-chlorophenyl)-4-oxo-4,5-dihydro-1l2,10l4-pyrazolo[2,3-a]quinoxalin-7-yl acetate (IC50 = 0.028 µM) was found to be the most potent inhibitor of MAO-A.
Additionally, SAR studies showed that the substituted chlorophenyl group at R1 is suitable for MAO-A inhibition, the Presence of the CN group at R2 improves the MAO-B specificity, and the acetyl group at R3 is essential for inhibitory activity (Fig. 13) [96].
Li et al. designed and synthesized pyridoxine-resveratrol derivatives as MAO-B inhibitors. In vitro studies revealed that compounds 20 (E)-3-(2-(2,2,8-trimethyl-4H-[1,3]dioxino[4,5-c]pyridin-5-yl)vinyl)phenol, compound 21 (E)-N-methyl-N-(prop-2-yn-1-yl)-4-(2-(2,2,8-trimethyl-4H-[1,3]dioxino[4,5-c]pyridin-5-yl)vinyl)aniline, and 22 (E)-2,2,8-trimethyl-5-(4-(4-methylpiperazin-1-yl)styryl)-4H-[1,3]dioxino[4,5-c]pyridine were the most potent inhibitors with IC50 values 0.01 µM, 0.01 µM, and 0.02 µM, respectively.
The Structure–activity relationship studies revealed that a decrease in the ability of electron-donating substituent would decrease the inhibitory activity, significant reduction of the activity observed when N-methyl-N-propargylamine is replaced with N, N-propargylamine. No change in activity when there is an extension of the carbon chain. The Presence of a cyclic amine group was found on the aromatic ring (Fig. 14). According to reversibility studies, it was found that compounds 20 and 22 were reversible inhibitors, but compound 21 was an irreversible inhibitor. Molecular docking of the most potent compound with the MAO enzyme revealed modes of interaction such as hydrogen bonds, hydrophobic interactions, and π–π interactions. The binding energy of compound 20 was found to be − 9.44 kcal/mol and − 11.65 kcal/mol for MAO-A and MAO-B, respectively. Synthesized compounds were checked for antioxidant activity, and results revealed that the compounds have good antioxidant activity and antioxidant capacity index between 1.98 and 2.89. All three derivatives showed a high blood–brain barrier permeability and the neuroprotective effect on H2O2-induced PC-12 cell injury. So they can become excellent MAO-B inhibitors [97].
In a study, Osmaniye et al. reported a new series of thiosemicarbazide derivatives and evaluated them against the MAO-B enzyme. Compounds 23 (E)-2-(benzofuran-2-ylmethylene)-N-(2-methoxyethyl)hydrazine-1-carbothioamide and compound 24 (E)-2-(benzo[b]thiophen-2-ylmethylene)-N-(2-methoxyethyl)hydrazine-1-carbothioamide were the most effective agent with an IC50 value of 0.042 µM and 0.056 µM, respectively. These compounds showed a similar inhibitory effect as Selegiline (reference compound). The SAR studies (Fig. 15) revealed that the methoxyethyl group increased the MAO-B inhibitory activity, and benzofuran was more active than benzothiophene. The Kinetic studies disclosed that compounds were reversible and non-competitive, and Ki values of compounds 23 and 24 were 0.035 µM and 0.046 µM, respectively. Cytotoxicity assay revealed that compounds 23 and 24 were non-cytotoxic at therapeutic concentration against MAO-B. According to molecular docking studies, compounds showed various interactions, such as π–π interaction and hydrogen bonds; hydrazine moiety was essentia for polar interactionsl. Compounds showed favorable van der Waals interactions with amino acid residues such as Leu171, Ile198, Cys172, Gln206, Phe343, Tyr326, Tyr398, Tyr435, and FAD molecule. Similarly, electrostatic interactions of these compounds were found with amino acid residues such as Gln65, Tyr188, Cys172, Ile198, Tyr326, Gln206, Tyr435, and FAD molecule [98].
Liu et al. designed and synthesized a series of novel 3,4-dihydrocoumarin derivatives and evaluated their inhibitory activity against the MAO-B enzyme. Compound 25 7-((4-(2-fluorobenzyl)benzyl)oxy)-2H-chromen-2-one was found the most potent with IC50 equal to 0.37 nM. This compound was even more potent than reference iproniazid. The kinetics study showed that compound 25 is a reversible and competitive inhibitor of MAO-B. Additionally, Structure–Activity relationship studies showed that benzyloxy substituent is critical for activity, fluorine at ortho position enhanced the activity, an electron-withdrawing group such NO2 decreased the activity, electron-donating CH3 increased the activity as shown in (Fig. 16). Molecular modeling studies were done to explain the selectivity toward human monoamine oxidase enzyme. Dihydro coumarin moiety interacted with Lle 198, Leu 171, Gln 206, and Cys 172 amino acid residues. Cytotoxic and neuroprotective studies in the PC12 cell line revealed that compounds showed little toxicity at 200 µM, but most were safe at 50 µM and 100 µM, and compound 25 showed a 48% increase in protection against 6-OHDA treated cells. According to ADMET prediction studies, new compounds showed a good pharmacokinetic profile which exhibits their biological importance [99].
In a recent study, Besada et al. synthesized a series of Pyridazinon-dithiocarbamate hybrids as MAO-B inhibitors. The in vitro studies revealed that all the compounds showed selectivity for the hMAO-B enzyme. The most potent compounds were 26 2-(1-Methyl-6-oxo-1,6-dihydropyridazin-3-yl)ethyl di(piperidin-1-yl)carbamodithioate, 27 (1,4-Dimethyl-6-oxo-1,6-dihydropyridazin-3-yl)methyl di(piperidin-1-yl)carbamodithioate, 28 (1-Methyl-6-oxo-1,6-dihydropyridazin-4-yl)methyl di(piperidin-1-yl)carbamodithioate, and 29 (1-Benzyl-6-oxo-1,6-dihydropyridazin-4-yl)methyl di(piperidin-1-yl)carbamodithioate with IC50 values 11.88 µM, 7.48 µM, 16.51 µM, and 6.71 µM respectively. It has been found that all the potent compounds showed reversible behavior. Additionally, the SAR studies (Fig. 17) revealed that the Presence of dithiocarbamate moiety at different positions of pyridazinone is essential for activity, and the substitution of dithiocarbamate at C4 slightly increased potency. The activity increased when the linker magnitude was increased from 1 to 2, and the Presence of a phenyl ring at the diazaheterocyclic core increased the the inhibition profile and selectivity of the compound. Methyl substitution on nitrogen was more potent than the bulky benzyl group. Furthermore, cell toxicity studies on human cell line SH-SY5V revealed that compounds exhibited no significant cellular toxicity at the effective concentration. The Molecular Docking studies showed two different binding modes for the compounds i.e., the alkyl chain linking both scaffolds and the binding of the dithiocarbamate group in the proximity of the basic residues Phe168, Leu171, and Cys172. Finally, the predicted ADME descriptors showed that the novel pyridazinone/dithiocarbamate derivatives showed good drug-like properties for oral absorption and BBB permeation [100].
Halaby et al. synthesized 21 new biphenyl piperazine derivatives and screened them against MAOs. In vitro tests were performed, and compound 30 2-(4-(4-(2-ethoxyphenyl)piperazin-1-yl)phenyl)-5-methyl-1H-benzo[d]imidazole was found to be the most potent compound with an IC50 value of 0.053 µM while the reference compound rasagiline and selegiline with IC50 value of 0.237 µM and 0.040 µM, respectively. The Structure–activity relationship studies (Fig. 18) revealed that 1,4-biphenylpiperazine moieties were significant for MAO inhibitory activity, the presence of benzimidazole scaffold increased the activity and substitutions with electron-donating groups such as methoxy showed more selectivity toward MAO-A enzyme.
Furthermore, the kinetics study revealed that compound 30 is a mixed inhibitor (Ki = 0.017 µM). The reversibility studies showed that compound 30 was a reversible inhibitor. According to cytotoxicity studies IC50 value was calculated to be 54.45 µM against the SH-SY5Y cell line, which showed that synthesized derivatives were non-toxic at active concentration. The compound 30 showed excellent drug-like properties as per ADME prediction studies. Molecular docking studies showed the binding interactions and essential amino acid residue in the binding cavity. Finally, this information is helpful in developing safe and potent new anti-parkinsonian drugs [101]. The Molecular docking studies revealed that the most potent compound 30 does not correctly fit in the active site of the MAO-A enzyme, so the compound may bind due to displacement of conserved water molecules and the reason for the significant affinity of the compound for the MAO-A enzyme. ADME parameters were predicted using the swissADME tool by calculations of various physicochemical parameters such as lipophilicity, molecular weight, solubility, polarity, and polar surface area, etc., and concluded that these compounds may have good brain penetration and oral bioavailability and can be potential MAO-B inhibitors.
Tok et al. designed and synthesized thirty novel 2,5-disubstituted-1,3,4-oxadiazole derivatives and evaluated their inhibitory activity against MAOs enzyme. In vitro studies showed that none of the compounds were active against MAO-A, but compound 31 1-(4-Chlorophenyl)-3-(5-(5-(4-chlorophenyl)-1,3,4-oxadiazol-2-yl)pyridin-2-yl)urea, compound 32 1-(4-Chlorophenyl)-3-(5-(5-(4-nitrophenyl)-1,3,4-oxadiazol-2-yl)pyridin-2-yl)urea, and compound 33 1-(4-Chlorophenyl)-3-(5-(5-(4-methoxyphenyl)-1,3,4-oxadiazol-2-yl)pyridin-2-yl)urea were the most potent compounds with IC50 values 0.039, 0.066, and 0.045 µM, respectively against the MAO-B isoform. Additionally, structure–activity relationship studies revealed that the presence of 1,3,4-oxadiazole ring was necessary for the activity, substitution of phenyl ring with chloro-group enhanced the activity and replacing with nitro group decreased the activity as compared to chloro-group (Fig. 19). Furthermore, the Docking studies were performed to determine the interaction between compound H8 and active site of the enzyme. A halogen bond was formed between the chlorine atom of the 4-chlorophenyl ring attached to the urea group of compound 31 with the carbonyl of Leu164 amino acid, and a hydrogen bond was established between the amino group and the carbonyl of Pro102. So, all this information provides us with lead i.e. Compound 31 which is a potent and selective MAO-B inhibitor that can be used for further development of the treatment for Parkinson’s Disease [102].
Ozdemir et al. designed and synthesized a series of pyridazinone derivatives as MAO-B inhibitors in a recent study. In vitro assay was carried out to check the MAO-inhibitory activity and selectivity of synthesized derivatives and found that compound 34 2-(3-(4-(4-Chlorophenyl)piperazin-1-yl)-6-oxopyridazin-1(6H)-yl)acetohydrazide was the most effective MAO-B inhibitor with Ki and selectivity index equal to 0.022 µM and 206.82, respectively. Furthermore, structure–activity relationship studies showed that piperazine-linked pyridazinone is necessary for the activity, the substituted phenyl at the piperazine ring enhanced the hMAO-B inhibitory activity, and halogen substitutions are significant for the activity. In contrast, the addition of a second halogen decreased the activity (Fig. 20). Additionally, the Docking studies revealed that pyridazinone and hydrazine group are essential for the interaction between the compound and active site of the enzyme. According to in silico ADME prediction studies, the compounds were drug-like for various physicochemical parameters [103].
Elkamhawy et al. synthesized 36 novel Safinamide derivatives and evaluated them against MAO-B. Compound 35 N-(3-chloro-4-((4-fluorobenzyl)oxy)phenyl)pyrazine-2-carboxamide, compound 36 N-(3-chloro-4-((3-chlorobenzyl)oxy)phenyl)pyrazine-2-carboxamide, and compound 37 N-(3-chloro-4-((3-(trifluoromethyl)benzyl)oxy)phenyl)pyrazine-2-carboxamide showed the most potent inhibitory activity with IC50 values of 9.7 nM, 5.1 nM, and 3.9 nM, respectively. Additionally, the SAR studies revealed that the presence of carboxamide moiety (2-pyrazinyl) enhanced the activity, and the presence of halogen at the 3,4-position enhanced the MAO-B inhibitory activity as shown in (Fig. 21). Furthermore, the Docking studies provided knowledge about the interaction between the inhibitor and enzyme. In vivo studies showed that the nigrostriatal dopaminergic neurons were significantly protected by oral administration of 37, so compound 37 can be considered a novel, potent, and selective hMAO-B inhibitor for treating Parkinson’s disease [104].
In a study, Rehuman et al. designed and synthesized two series of dimethoxy-halogenated chalcone derivatives and evaluated their MAO inhibitory activity. In vitro studies showed that compound 38 (E)-3-(4-Chlorophenyl)-1-(2,4-dimethoxyphenyl)prop-2-en-1-one was the most potent inhibitor of MAO-B with an IC50 value of 0.067 µM and followed by compound 39 (E)-1-(2,3-dimethoxyphenyl)-3-(4-fluorophenyl)prop-2-en-1-one with an IC50 value of 0.118 µM. Additionally, structure–activity relationship studies revealed that different orientation of halogen atoms at different locations of B ring changed the activity of the compounds, such as chloro at ortho position was more potent as compared to meta or para position (Fig. 22). According to kinetics study, compounds 38 and 39 show competitive and reversible inhibition with Ki value 0.032 and 0.045 µM, respectively. Cytotoxicity was checked using the MTT assay method on the Vero epithelial cell line, and it found that 38 was non-toxic below 100 µg/ml. Induced fit docking simulations were performed to determine the binding mode between the synthesized compounds and MAO-B enzyme and found the two compounds with similar binding pockets with ortho-chlorine and ortho-fluorine interact with Y326 and F168, and hydrogen bond stabilized the side chain of Y188 within the binding pocket. It was concluded that compounds 38 and 39 were good candidates for the development of the new class of MAO-B inhibitors [105].
Alagoz et al. reported the synthesis of 16 novel compounds and evaluated their MAO inhibitory activity against two isoforms of the enzyme, i.e., MAO-A and MAO-B. The most potent compound found to be 40 (E)-N'-(4-chlorobenzylidene)-2-(3-(4-(4-methoxyphenyl)piperazin-1-yl)-6-oxopyridazin-1(6H)-yl)acetohydrazide with an IC50 value of 0.17 µM followed by compound 41 (E)-N'-(4-chlorobenzylidene)-2-(3-morpholino-6-oxopyridazin-1(6H)-yl)acetohydrazide (IC50 = 0.27 µM). Additionally, structure–activity relationship studies revealed that para-chloro substitution increased the MAO-B inhibitory activity, and the substitution of R1 with -OCH3 showed higher activity than -CF3 substitution (Fig. 23). These compounds were reversible and competitive inhibitors with Ki value 0.230 and 0.146 µM, respectively. According to the PAMPA test, it is revealed that compounds 40 and 41 transverse the blood–brain barrier very quickly as it has good CNS permeability. The docking studies revealed that the reason for the potent inhibitory efficiency of compounds 40 and 41 might be due to interaction with some essential residue i.e., E84 and Y326 in MAO-B. Bioavailability prediction studies showed that compounds 40 and 41 have drug-like properties, so they can be considered a candidate for developing MAO-B inhibitors [106].
Drugs in clinical trial for Parkinson’s disease
The MAO-B inhibitors and therapy under clinical trial in past years are listed in Table 1. Rasagiline, an irreversible inhibitor of monoamine oxidase B, has completed a clinical trial in which change in the cognitive brain biomarker was compared over 2.5 years in 12 patients, assessed by MRI in Parkinson’s disease (NCT02278588). In another phase two trials Brain and Motor behavior changes were investigated in Parkinson’s disease in response to the drug (NCT02789020). In a different clinical trial study effect of rasagiline was determined on gait treatment (NCT01098396). Rasagiline’s effect was evaluated on cognition in the early stages of PD and entered in phase 4 clinical trial (NCT01382342). Completed the clinical trial for the effect of rasagiline on sleep disturbance in Parkinson’s disease and showed a positive effect on sleep disturbance by reducing nocturnal akinesia (NCT01442610). In another study under phase 4, rasagiline as an add-on dopamine agonist in the treatment of Parkinson’s disease was evaluated, and it found that it is not optimally controlled on dopamine as compared to placebo (NCT01049984).
Safinamide, a reversible MAO-B inhibitor, completed the clinical trial for the study of the overnight switch from Rasagiline to Safinamide, and safety and tolerability were checked when there was a sudden switch from one medication to another (NCT03843944). A different study showed that clinical outcome assessment of Parkinson’s disease with XADAGO (Safinamide) in Phase 4 of the clinical trial. In this study, the effect of XADAGO on motor and non-motor symptoms in Parkinson’s disease was evaluated (NCT03944785).
Zelapar (orally disintegrating Selegiline), an irreversible MAO-B inhibitor, completed the clinical trial titled efficacy of orally disintegrating selegiline in Parkinson’s patients experiencing adverse effects with dopamine agonists. This study was performed to evaluate the side effects of dopamine, such as swelling of lower limbs or feet or hallucinations during the addition of orally disintegrating selegiline which can reduce the adverse effect and maintain the symptoms of Parkinson’s disease (NCT00443872).
Treatment by Chinese herbal medicine as adjuvant therapy for the treatment of Parkinson’s disease is in Phase 2 for conventional medicine and Phase 3 for Chinese herbal medicine. This study explores the effect of Chinese herbal medicine on Parkinson’s disease parameters (NCT05001217).
Apomorphine, a non-selective dopamine agonist, is in a Phase 3 clinical trial to determine the safety and tolerability of continuous subcutaneous infusion (NCT02339064).
Data from patents documents
Some patents on MAO-B inhibitors that were published last few years are listed in Table 2. The Data of patent literature focuses structure of various compounds which may be used for Parkinson’s disease and other neurological disorders. Papers that were published were added to this review.
Conclusion
Parkinson's disease (PD) is the second most common age-related complex, idiopathic neurological disorder. Although there are several treatments available, none of them are very successful in preventing the loss of dopaminergic neurons and restoring DA levels in the striatum. Thus, the development of novel anti-parkinsonians is the requirement of the present era. In-depth information on the design and synthesis of various MAO-B inhibitors that are currently being developed (as of 2018) is presented in this review. We have also gone through SAR analyses for these derivatives, which showed the importance of various substituents on the basic moieties. The coumarin derivatives showed the presence of hydroxy in the seventh position enhances the activity, and halogen-substituted heterocyclics or substituted benzoxy group increases the activity. The chalcone moiety-containing compounds showed important for the activity in which the A ring may be substituted by the prenyl group of the methoxy group for good activity and ring B to be substituted by electron-withdrawing groups at ortho position for better MAO-B inhibitory activity. Piperazine-linked pyridazinone is necessary for the activity, phenyl substituted at piperazine enhances the MAO-B inhibitory activity, and the presence of halogen improves the activity. This knowledge can be used as a springboard for creating novel anti-parkinsonian drugs. A multitarget approach is more beneficial than compared to single target approach for the treatment of the neurodegenerative disorder. MDLTs show an effective outcome for the treatment of PD by targeting sigma receptors. The multi-target disease modification approach can be used in the modification of misfolded alpha-syn in the treatment of PD. The multi-target approach is very effective to predict the effectiveness of MAO-B inhibitors. For the treatment of PD, deep brain stimulation by the multi-target approach is very beneficial. Dual- acetylcholinesterase inhibitors and monoamine oxidase can be used as a multi-target approach for the treatment of PD. The monoaminergic and histaminergic systems both can also be targeted by the multi-target approach for PD. Therefore, a multi-target approach can be used for the potential treatment of PD. This review also highlights that drug in the early or late stages of clinical trials for Parkinson’s disease. This review provides useful information for developing new drugs with minimum side effects and better effectiveness for treatment of Parkinson’s disease.
Abbreviations
- MAO:
-
Monoamine oxidase
- PD:
-
Parkinson’s disease
- DA:
-
Dopamine
- FDA:
-
The food and Drug Administration
- TH:
-
Tyrosine hydroxylase
- AADC:
-
Aromatic amino acid decarboxylase
- DOPAC:
-
3,4-Dihydroxy phenylacetic acid
- HMV:
-
Homovanillic acid
- DDC:
-
Dopa decarboxylase
- DAT:
-
Dopamine transporter
- COMT:
-
Catechol-O-methyl transferase
- FAD:
-
Flavin adenine dinucleotide
- MAOIs:
-
MAO inhibitors
- SAR:
-
Structure–activity relationship
- BHT:
-
Butylated hydroxytoluene
- EWG:
-
Electron-withdrawing group
- EDG:
-
Electron donating group
- BBB:
-
Blood Brain Barrier
- CNS:
-
Central nervous system
References
Ball N, Teo W-P, Chandra S, Chapman J (2019) Parkinson’s disease and the environment. Front Neurol 10:218
Shimohama S, Sawada H, Kitamura Y, Taniguchi T (2003) Disease model: Parkinson’s disease. Trends Mol Med 9(8):360–365
Surmeier DJ (2018) Determinants of dopaminergic neuron loss in Parkinson’s disease. FEBS J 285(19):3657–3668
Latif S, Jahangeer M, Razia DM, Ashiq M, Ghaffar A, Akram M et al (2021) Dopamine in Parkinson’s disease. Clin Chim Acta 522:114–126
Levey AI, Hersch SM, Rye DB, Sunahara RK, Niznik HB, Kitt CA et al (1993) Localization of D1 and D2 dopamine receptors in brain with subtype-specific antibodies. Proc Natl Acad Sci 90(19):8861–8865
Alexander GE (2022) Biology of Parkinson’s disease: pathogenesis and pathophysiology of a multisystem neurodegenerative disorder. Dialogues Clin Neurosci 6:259–280
Collier TJ, Kanaan NM, Kordower JH (2011) Ageing as a primary risk factor for Parkinson’s disease: evidence from studies of non-human primates. Nat Rev Neurosci 12(6):359–366
Paviour DC, Surtees RA, Lees AJ (2004) Diagnostic considerations in juvenile parkinsonism. Mov Disord 19(2):123–135
Bloem BR, Okun MS, Klein C (2021) Parkinson’s disease. The Lancet 397(10291):2284–2303
Sveinbjornsdottir S (2016) The clinical symptoms of Parkinson’s disease. J Neurochem 139:318–324
Hayes MT (2019) Parkinson’s disease and parkinsonism. Am J Med 132(7):802–807
Skogar O, Nilsson M (2018) Distribution of non-motor symptoms in idiopathic Parkinson’s disease and secondary Parkinsonism. J Multidiscip Healthc 11:525
Di Monte DA (2003) The environment and Parkinson’s disease: is the nigrostriatal system preferentially targeted by neurotoxins? Lancet Neurol 2(9):531–538
Emamzadeh FN, Surguchov A (2018) Parkinson’s disease: biomarkers, treatment, and risk factors. Front Neurosci 12:612
Agnihotri A, Aruoma OI (2020) Alzheimer’s disease and Parkinson’s disease: a nutritional toxicology perspective of the impact of oxidative stress, mitochondrial dysfunction, nutrigenomics and environmental chemicals. J Am Coll Nutr 39(1):16–27
Quinteros E, Ribó A, Mejía R, López A, Belteton W, Comandari A et al (2017) Heavy metals and pesticide exposure from agricultural activities and former agrochemical factory in a Salvadoran rural community. Environ Sci Pollut Res 24(2):1662–1676
Bertram L, Tanzi RE (2005) The genetic epidemiology of neurodegenerative disease. J Clin Investig 115(6):1449–1457
Cannon JR, Greenamyre JT (2011) The role of environmental exposures in neurodegeneration and neurodegenerative diseases. Toxicol Sci 124(2):225–250
Nicoletti A, Luca A, Baschi R, Cicero CE, Mostile G, Davì M et al (2019) Incidence of mild cognitive impairment and dementia in Parkinson’s disease: the Parkinson’s disease cognitive impairment study. Front Aging Neurosci 11:21
Zejin O, Jing P, Shihao T, Danping D, Danfeng Y, Huiqi N et al (2021) Global trends in the incidence, prevalence, and years lived with disability of Parkinson’s disease in 204 countries/territories from 1990 to 2019. Front Public Health 9:2296–2565
Cerri S, Mus L, Blandini F (2019) Parkinson’s disease in women and men: what’s the difference? J Parkinsons Dis 9(3):501–515
Zarate S, Stevsner T, Gredilla R (2017) Role of estrogen and other sex hormones in brain aging Neuroprotection and DNA repair. Front Aging Neurosci 9:430
Thase ME (2012) The role of monoamine oxidase inhibitors in depression treatment guidelines. Prim Care Companion CNS Disord 14:27265
Naoi M, Maruyama W (2010) Monoamine oxidase inhibitors as neuroprotective agents in age-dependent neurodegenerative disorders. Curr Pharm Des 16(25):2799–2817
Zindo FT, Joubert J, Malan SF (2015) Propargylamine as functional moiety in the design of multifunctional drugs for neurodegenerative disorders: MAO inhibition and beyond. Future Med Chem 7(5):609–629
Saha M, Gupta S, Dhiman S, Asati V, Ali A, Ali A (2023) Field and atom-based 3D-QSAR models of chromone (1-benzopyran-4-one) derivatives as MAO inhibitors. J Biomol Struct Dyn 1–15
Antonini A, Moro E, Godeiro C, Reichmann H (2018) Medical and surgical management of advanced Parkinson’s disease. Mov Disord 33(6):900–908
Jenner P (2015) Treatment of the later stages of Parkinson’s disease–pharmacological approaches now and in the future. Transl Neurodegener 4(1):1–9
Müller T (2020) Pharmacokinetics and pharmacodynamics of levodopa/carbidopa cotherapies for Parkinson’s disease. Expert Opin Drug Metab Toxicol 16(5):403–414
Jiang D-Q, Zang Q-M, Jiang L-L, Wang Y, Li M-X, Qiao J-Y (2021) Comparison of pramipexole and levodopa/benserazide combination therapy versus levodopa/benserazide monotherapy in the treatment of Parkinson’s disease: a systematic review and meta-analysis. Naunyn Schmiedebergs Arch Pharmacol 394(9):1893–1905
Carbone F, Djamshidian A, Seppi K, Poewe W (2019) Apomorphine for Parkinson’s disease: efficacy and safety of current and new formulations. CNS Drugs 33(9):905–918
Dezsi L, Vecsei L (2017) Monoamine oxidase B inhibitors in Parkinson's disease. CNS Neurol Disord 16(4):425–439
Jenner P, Rocha J-F, Ferreira JJ, Rascol O, Soares-da-Silva P (2021) Redefining the strategy for the use of COMT inhibitors in Parkinson’s disease: the role of opicapone. Expert Rev Neurother 21(9):1019–1033
Parambi DG (2020) Treatment of Parkinson’s Disease by MAO-B inhibitors, new therapies and future challenges: a mini-review. Comb Chem High Throughput Screen 23(9):847–861
Mao Q, Qin W-Z, Zhang A, Ye N (2020) Recent advances in dopaminergic strategies for the treatment of Parkinson’s disease. Acta Pharmacol Sin 41(4):471–482
Krösser S, Marquet A, Gallemann D, Wolna P, Fauchoux N, Hermann R et al (2012) Effects of ketoconazole treatment on the pharmacokinetics of safinamide and its plasma metabolites in healthy adult subjects. Biopharm Drug Dispos 33(9):550–559
Rai SN, Singh P, Varshney R, Chaturvedi VK, Vamanu E, Singh M et al (2021) Promising drug targets and associated therapeutic interventions in Parkinson’s disease. Neural Regen Res 16(9):1730
Xu L, Pu J (2016) Alpha-synuclein in Parkinson’s disease: from pathogenetic dysfunction to potential clinical application. Parkinson’s Dis 2016:1–10
Crupi R, Impellizzeri D, Cuzzocrea S (2019) Role of metabotropic glutamate receptors in neurological disorders. Front Mol Neurosci 12:20
Fields CR, Bengoa-Vergniory N, Wade-Martins R (2019) Targeting alpha-synuclein as a therapy for Parkinson’s disease. Front Mol Neurosci 12:299
Zhang L, Dong Y, Xu X, Xu Z (2012) The role of autophagy in Parkinson’s disease. Neural Regen Res 7(2):141
Digby JE, Martinez F, Jefferson A, Ruparelia N, Chai J, Wamil M et al (2012) Anti-inflammatory effects of nicotinic acid in human monocytes are mediated by GPR109A dependent mechanisms. Arterioscler Thromb Vasc Biol 32(3):669–676
Gershanik OS (2015) Improving l-dopa therapy: the development of enzyme inhibitors. Mov Disord 30(1):103–113
Hauser RA, Li R, Pérez A, Ren X, Weintraub D, Elm J et al (2017) Longer duration of MAO-B inhibitor exposure is associated with less clinical decline in Parkinson’s disease: an analysis of NET-PD LS1. J Parkinsons Dis 7(1):117–127
Chang Y, Wang L-B, Li D, Lei K, Liu S-Y (2017) Efficacy of rasagiline for the treatment of Parkinson’s disease: an updated meta-analysis. Ann Med 49(5):421–434
Nutt JG, Curtze C, Hiller A, Anderson S, Larson PS, Van Laar AD et al (2020) Aromatic L-amino acid decarboxylase gene therapy enhances levodopa response in Parkinson’s disease. Mov Disord 35(5):851–858
Adams JD (2021) Possible causes of Parkinson’s disease. Front Biosci 26(8):387–394
Maini Rekdal V, Bess EN, Bisanz JE, Turnbaugh PJ, Balskus EP (2019) Discovery and inhibition of an interspecies gut bacterial pathway for Levodopa metabolism. Science 364(6445):eaau6323
Liu C, Kaeser PS (2019) Mechanisms and regulation of dopamine release. Curr Opin Neurobiol 57:46–53
Wiencke K, Horstmann A, Mathar D, Villringer A, Neumann J (2020) Dopamine release, diffusion and uptake: a computational model for synaptic and volume transmission. PLoS Comput Biol 16(11):e1008410
Xu H, Yang F (2022) The interplay of dopamine metabolism abnormalities and mitochondrial defects in the pathogenesis of schizophrenia. Transl Psychiatry 12(1):1–13
Chakraborty A, Diwan A (2019) Selection of cells for Parkinson’s disease cell-therapy. Int J Stem Cell Res Ther 6:063
Bogetofte H, Alamyar A, Blaabjerg M, Meyer M (2020) Levodopa therapy for Parkinson's disease: history, current status and perspectives. CNS Neurol Disord 19(8):572–583
Khan ST, Ahmed S, Gul S, Khan A, Al-Harrasi A (2021) Search for safer and potent natural inhibitors of Parkinson’s disease. Neurochem Int 149:105135
Grillner S, Robertson B, Kotaleski JH (2020) Basal ganglia: a motion perspective. Compr Physiol 10:1241–1275
Ribot B, Aupy J, Vidailhet M, Mazère J, Pisani A, Bezard E et al (2019) Dystonia and dopamine: from phenomenology to pathophysiology. Prog Neurobiol 182:101678
Jayaramayya K, Iyer M, Venkatesan D, Balasubramanian V, Narayanasamy A, Subramaniam MD et al (2020) Unraveling correlative roles of dopamine transporter (DAT) and Parkin in Parkinson’s disease (PD): a road to discovery? Brain Res Bull 157:169–179
Vidyadhara D, Somayaji M, Wade N, Yücel B, Zhao H, Shashaank N, et al (2022) Dopamine transporter and synaptic vesicle sorting defects initiate auxilin-linked Parkinson’s disease. bioRxiv
Müller T (2020) Entacapone/tolcapone/opicapone for treating Parkinson’s disease. NeuroPsychopharmacotherapy 1–18
Baba Y, Futamura A, Kinno R, Nomoto S, Takahashi S, Yasumoto T et al (2022) The relationship between the distinct ratios of benserazide and carbidopa to levodopa and motor complications in Parkinson’s disease: a retrospective cohort study. J Neurol Sci 437:120263
Youdim MB (2018) Monoamine oxidase inhibitors, and iron chelators in depressive illness and neurodegenerative diseases. J Neural Transm 125(11):1719–1733
Song Z, Zhang J, Xue T, Yang Y, Wu D, Chen Z et al (2021) Different catechol-O-methyl transferase inhibitors in Parkinson’s disease: a Bayesian network meta-analysis. Front Neurol 12:707723
Latt MD, Lewis S, Zekry O, Fung VS (2019) Factors to consider in the selection of dopamine agonists for older persons with Parkinson’s disease. Drugs Aging 36(3):189–202
Yeni Y, Wu X, Arman B, Anggia V. Pharmaceutical and Biomedical Sciences Journal.
Binda C, Newton-Vinson P, Hubálek F, Edmondson DE, Mattevi A (2002) Structure of human monoamine oxidase B, a drug target for the treatment of neurological disorders. Nat Struct Biol 9(1):22–26
Shih J, Chen K, Ridd M (1999) Monoamine oxidase: from genes to behavior. Annu Rev Neurosci 22:197
Ramsay R (2012) Monoamine oxidases: the biochemistry of the proteins as targets in medicinal chemistry and drug discovery. Curr Top Med Chem 12(20):2189–209
Westlund K, Denney R, Rose R, Abell C (1988) Localization of distinct monoamine oxidase A and monoamine oxidase B cell populations in human brainstem. Neuroscience 25(2):439–456
Hall D, Logan BW, Parsons G (1969) Further studies on the inhibition of monoamine oxidase by M & B 9302 (clorgyline)—I: Substrate specificity in various mammalian species. Biochem Pharmacol 18(6):1447–1454
Kaya B, Yurttaş L, Sağlik BN, Levent S, Özkay Y, Kaplancikli ZA (2017) Novel 1-(2-pyrimidin-2-yl) piperazine derivatives as selective monoamine oxidase (MAO)-A inhibitors. J Enzyme Inhib Med Chem 32(1):193–202
Youdim MB, Edmondson D, Tipton KF (2006) The therapeutic potential of monoamine oxidase inhibitors. Nat Rev Neurosci 7(4):295–309
Finberg JP (2014) Update on the pharmacology of selective inhibitors of MAO-A and MAO-B: focus on modulation of CNS monoamine neurotransmitter release. Pharmacol Ther 143(2):133–152
Lasbennes F, Sercombe R, Seylaz J (1983) Monoamine oxidase activity in brain microvessels determined using natural and artificial substrates: relevance to the blood—brain barrier. J Cereb Blood Flow Metab 3(4):521–528
Nagatsu T (2004) Progress in monoamine oxidase (MAO) research in relation to genetic engineering. Neurotoxicology 25(1–2):11–20
Teo DCL, Mok VWL (2020) 127 successful treatment of major depressive disorder with moclobemide after recurrent hyponatremia induced by multiple antidepressant classes. CNS Spectr 25(2):280–281
Wang K, Luo J, Yeh S, You B, Meng J, Chang P et al (2020) The MAO inhibitors phenelzine and clorgyline revert enzalutamide resistance in castration resistant prostate cancer. Nat Commun 11(1):1–14
Xie S-S, Liu J, Tang C, Pang C, Li Q, Qin Y et al (2020) Design, synthesis and biological evaluation of rasagiline-clorgyline hybrids as novel dual inhibitors of monoamine oxidase-B and amyloid-β aggregation against Alzheimer’s disease. Eur J Med Chem 202:112475
do Carmo Carreiras M, Ismaili L, Marco-Contelles J (2020) Propargylamine-derived multi-target directed ligands for Alzheimer’s disease therapy. Bioorg Med Chem Lett 30(3):126880
Finberg JP (2019) Inhibitors of MAO-B and COMT: their effects on brain dopamine levels and uses in Parkinson’s disease. J Neural Transm 126(4):433–448
Huleatt PB, Khoo ML, Chua YY, Tan TW, Liew RS, Balogh BZ, et al (2015) Novel arylalkenylpropargylamines as neuroprotective, potent, and selective monoamine oxidase B inhibitors for the treatment of Parkinson’s disease. J Med Chem 58(3):1400–1419
Peretz C, Segev H, Rozani V, Gurevich T, El-Ad B, Tsamir J et al (2016) Comparison of selegiline and rasagiline therapies in Parkinson disease: a real-life study. Clin Neuropharmacol 39(5):227
Jiang D-Q, Li M-X, Jiang L-L, Chen X-B, Zhou X-W (2020) Comparison of selegiline and levodopa combination therapy versus levodopa monotherapy in the treatment of Parkinson’s disease: a meta-analysis. Aging Clin Exp Res 32(5):769–779
Shih JC (2018) Monoamine oxidase isoenzymes: genes, functions and targets for behavior and cancer therapy. J Neural Transm 125(11):1553–1566
Borgohain R, Szasz J, Stanzione P, Meshram C, Bhatt M, Chirilineau D et al (2014) Randomized trial of safinamide add-on to levodopa in Parkinson’s disease with motor fluctuations. Mov Disord 29(2):229–237
Bianchini E, Sforza M, Rinaldi D, Alborghetti M, De Carolis L, Della Gatta F et al (2021) Switch from rasagiline to safinamide in fluctuating Parkinson’s disease patients: a retrospective, pilot study. Neurol Res 43(11):950–954
Yeon SK, Choi JW, Park J-H, Lee YR, Kim HJ, Shin SJ et al (2018) Synthesis and evaluation of biaryl derivatives for structural characterization of selective monoamine oxidase B inhibitors toward Parkinson’s disease therapy. Bioorg Med Chem 26(1):232–244
Mellado M, Salas CO, Uriarte E, Viña D, Jara-Gutiérrez C, Matos MJ et al (2019) Design, synthesis and docking calculations of prenylated chalcones as selective monoamine oxidase B inhibitors with antioxidant activity. ChemistrySelect 4(26):7698–7703
Agrawal N, Mishra P (2019) Novel isoxazole derivatives as potential antiparkinson agents: synthesis, evaluation of monoamine oxidase inhibitory activity and docking studies. Med Chem Res 28(9):1488–1501
Parambi D, Oh J, Baek S, Lee J, Tondo A, Nicolotti O et al (2019) Design, synthesis and biological evaluation of oxygenated chalcones as potent and selective MAO-B inhibitors. Bioorg Chem 93:103335
Rodríguez-Enríquez F, Viña D, Uriarte E, Fontenla JA, Matos MJ (2020) Discovery and optimization of 3-thiophenylcoumarins as novel agents against Parkinson’s disease: Synthesis, in vitro and in vivo studies. Bioorg Chem 101:103986
Rodríguez-Enríquez F, Costas-Lago MC, Besada P, Alonso-Pena M, Torres-Terán I, Viña D et al (2020) Novel coumarin-pyridazine hybrids as selective MAO-B inhibitors for the Parkinson’s disease therapy. Bioorg Chem 104:104203
Sağlık BN, Osmaniye D, AcarÇevik U, Levent S, Kaya Çavuşoğlu B, AtlıEklioğlu Ö et al (2020) Synthesis, in vitro enzyme activity and molecular docking studies of new benzylamine-sulfonamide derivatives as selective MAO-B inhibitors. J Enzyme Inhib Med Chem 35(1):1422–1432
Mathew GE, Oh JM, Mohan K, Tengli A, Mathew B, Kim H (2021) Development of methylthiosemicarbazones as new reversible monoamine oxidase-B inhibitors for the treatment of Parkinson’s disease. J Biomol Struct Dyn 39(13):4786–4794
Mathew B, Baek SC, Lee JP, Joy M, Rilda PA, Randev RV et al (2018) Selected aryl thiosemicarbazones as a new class of multi-targeted monoamine oxidase inhibitors. MedChemComm 9(11):1871–1881
Łażewska D, Olejarz-Maciej A, Reiner D, Kaleta M, Latacz G, Zygmunt M et al (2020) Dual target ligands with 4-tert-butylphenoxy scaffold as histamine H3 receptor antagonists and monoamine oxidase B inhibitors. Int J Mol Sci 21(10):3411
Panova VA, Filimonov SI, Chirkova ZV, Kabanova MV, Shetnev AA, Korsakov MK et al (2021) Investigation of pyrazolo [1, 5-a] quinoxalin-4-ones as novel monoamine oxidase inhibitors. Bioorg Chem 108:104563
Li W, Yang X, Song Q, Cao Z, Shi Y, Deng Y et al (2020) Pyridoxine-resveratrol hybrids as novel inhibitors of MAO-B with antioxidant and neuroprotective activities for the treatment of Parkinson’s disease. Bioorg Chem 97:103707
Osmaniye D, Kurban B, Sağlık BN, Levent S, Özkay Y, Kaplancıklı ZA (2021) Novel thiosemicarbazone derivatives: in vitro and in silico evaluation as potential MAO-B inhibitors. Molecules 26(21):6640
Liu L, Chen Y, Zeng R-F, Liu Y, Xie S-S, Lan J-S et al (2021) Design and synthesis of novel 3, 4-dihydrocoumarins as potent and selective monoamine oxidase-B inhibitors with the neuroprotection against Parkinson’s disease. Bioorg Chem 109:104685
Besada P, Viña D, Costas T, Costas-Lago MC, Vila N, Torres-Terán I et al (2021) Pyridazinones containing dithiocarbamoyl moieties as a new class of selective MAO-B inhibitors. Bioorg Chem 115:105203
El-Halaby LO, El-Husseiny WM, El-Messery SM, Goda FE (2021) Biphenylpiperazine based MAO inhibitors: synthesis, biological evaluation, reversibility and molecular modeling studies. Bioorg Chem 115:105216
Tok F, Uğraş Z, Sağlık BN, Özkay Y, Kaplancıklı ZA, Koçyiğit-Kaymakçıoğlu B (2021) Novel 2, 5-disubstituted-1, 3, 4-oxadiazole derivatives as MAO-B inhibitors: synthesis, biological evaluation and molecular modeling studies. Bioorg Chem 112:104917
Özdemir Z, Alagöz MA, Uslu H, Karakurt A, Erikci A, Ucar G et al (2020) Synthesis, molecular modelling and biological activity of some pyridazinone derivatives as selective human monoamine oxidase-B inhibitors. Pharmacol Rep 72(3):692–704
Elkamhawy A, Paik S, Park J-H, Kim HJ, Hassan AH, Lee K et al (2021) Discovery of novel and potent safinamide-based derivatives as highly selective hMAO-B inhibitors for treatment of Parkinson’s disease (PD): design, synthesis, in vitro, in vivo and in silico biological studies. Bioorg Chem 115:105233
Rehuman NA, Oh JM, Abdelgawad MA, Beshr EA, Abourehab MA, Gambacorta N et al (2022) Development of halogenated-chalcones bearing with dimethoxy phenyl head as monoamine oxidase-B inhibitors. Pharmaceuticals 15(9):1152
Alagöz MA, Oh JM, Zenni YN, Özdemir Z, Abdelgawad MA, Naguib IA et al (2022) Development of a novel class of pyridazinone derivatives as selective MAO-B inhibitors. Molecules 27(12):3801
Stocchi F, Vacca L, Grassini P, Tomino C, Caminiti G, Casali M et al (2021) Overnight switch from rasagiline to safinamide in Parkinson’s disease patients with motor fluctuations: a tolerability and safety study. Eur J Neurol 28(1):349–354
A Prospective, Observational Study to Evaluate Changes in Non-Motor Symptoms and Other Clinical Outcome Assessments of Parkinson's Disease Patients Treated With XADAGO (Safinamide)Tablets 2021
Isaacson S, Espay A, Pahwa R, Clinch T, LeWitt P (2020) Safety and Efficacy of continuous apomorphine infusion in patients with Parkinson’s disease: results from a phase 3, open-label study (1771). AAN Enterprises
Yuen SCS, Chua KK, Zhong LL, Chan KW, Chan CKH, Chan KL et al (2022) Chinese herbal medicine treatment based on subgroup differentiation as adjunct therapy for Parkinson’s disease: study protocol of a pilot add-on, randomised, controlled, pragmatic clinical trial. Chin Med 17(1):16
Guttuso T, Bergsland N, Hagemeier J, Lichter DG, Pasternak O, Zivadinov R (2018) Substantia nigra free water increases longitudinally in Parkinson disease. Am J Neuroradiol 39(3):479–484
Sharma V, Singh TG, Kaur A, Mannan A, Dhiman S (2022) Brain-derived neurotrophic factor: a novel dynamically regulated therapeutic modulator in neurological disorders. Neurochem Res 48: 317–339
Schrempf W, Fauser M, Wienecke M, Brown S, Maaß A, Ossig C et al (2018) Rasagiline improves polysomnographic sleep parameters in patients with Parkinson’s disease: a double-blind, baseline-controlled trial. Eur J Neurol 25(4):672–679
Dézsi L, Vécsei L (2014) Safinamide for the treatment of Parkinson’s disease. Expert Opin Investig Drugs 23(5):729–742
Goldman JG, Weintraub D (2015) Advances in the treatment of cognitive impairment in P arkinson’s disease. Mov Disord 30(11):1471–1489
Rasagiline for the Treatment of Gait Disturbances in Patients With Parkinson’s Disease (PD): an Open Label Study 2010
Karthivashan G, Ganesan P, Park S-Y, Lee H-W, Choi D-K (2020) Lipid-based nanodelivery approaches for dopamine-replacement therapies in Parkinson’s disease: from preclinical to translational studies. Biomaterials 232:119704
Crowley BM, Campbell BT, Chobanian HR, Fells JI, Guiadeen DG, Greshock TJ, Leavitt KJ, Rada VL, Bell IM (2022) Spiropiperidine allosteric modulators of nicotinic acetylcholine receptors. U.S. Patent 11,332,463
Crowley BM, Bell IM, Harvey AJ, Shipe WD, Leavitt KJ, Sanders JM, Guiadeen, DG, Suen LM, Greshock TJ, Rada VL (2020) Substituted bicyclic heteroaryl allosteric modulators of nicotinic acetylcholine receptors. U.S. Patent 10,870,630
Tzvetkov N (2017) Substituted benzamide derivatives as in vitro MAO-B inhibitors. U.S. Patent 9,738,640
Mazhari R, Mezaache D, Paterson BM, Vornov J, Garner RM, Nelson T (2022) Compounds, compositions and methods. U.S. Patent 11,479,542
Tzvetkov N (2017) Substituted indazole derivatives as in vitro MAO-B inhibitors. U.S. Patent 9,643,930
Terán MD, Besada PP, Costas CT, Costas LD, Vila MN, Viña CD (2019) Pyridazin-3(2H)-one derivatives as monoamine oxidase selective isoform B inhibitors. U.S. Patent 10,253,000
Chuanfei J, Kangzhi C, Yingjun Z (2022) Pyrrolidineamide derivatives and uses thereof. U.S. Patent 11,225,460
Tzvetkov N (2017) Substituted Indazole or Indole Derivatives as in Vitro Mao-B Inhibitors. E. Patent 2,964,219
Tzvetkov N (2017) Substituted benzamide derivatives as mao-B inhibitors. E. Patent 2,991,986
Park KD, Lee CJ, Kim DJ, Pae A, Nim Choo HA, Min SJ, Kang YK, Kim YK, Song H J, Choi JW, Nam M H, Heo JY, Yeon SK, Jang BK, Ju EJ, Jo SM, Park JH (2019) Alpha-aminoamide derivative compound and pharmaceutical composition containing the same. E. Patent 3,202,759
Acknowledgements
The authors thank the Chairman and Director of ISF College of Pharmacy, Moga, Punjab for supporting this work.
Author information
Authors and Affiliations
Contributions
Gurkaran singh wrote the main manuscript text and Shankar gupta prepared figures . All authors reviewed the manuscript.
Corresponding author
Ethics declarations
Conflict of interest
The authors declare no conflict of interest.
Additional information
Publisher's Note
Springer Nature remains neutral with regard to jurisdictional claims in published maps and institutional affiliations.
Rights and permissions
Springer Nature or its licensor (e.g. a society or other partner) holds exclusive rights to this article under a publishing agreement with the author(s) or other rightsholder(s); author self-archiving of the accepted manuscript version of this article is solely governed by the terms of such publishing agreement and applicable law.
About this article
Cite this article
Baweja, G.S., Gupta, S., Kumar, B. et al. Recent updates on structural insights of MAO-B inhibitors: a review on target-based approach. Mol Divers (2023). https://doi.org/10.1007/s11030-023-10634-6
Received:
Accepted:
Published:
DOI: https://doi.org/10.1007/s11030-023-10634-6