Abstract
Hypoxia-inducible factors (HIFs) are transcription factors critical for the adaptive response to hypoxia. There is also an essential link between hypoxia and inflammation, and HIFs have been implicated in the dysregulated immune response to various insults. Despite the prevalence of hypoxia in tissue trauma, especially involving the lungs, there remains a dearth of studies investigating the role of HIFs in clinically relevant injury models. Here, we summarize the effects of HIF-1α on the vasculature, metabolism, inflammation, and apoptosis in the lungs and review the role of HIFs in direct lung injuries, including lung contusion, acid aspiration, pneumonia, and COVID-19. We present data that implicates HIF-1α in the context of arguments both in favor and against its role as adaptive or injurious in the propagation of the acute inflammatory response in lung injuries. Finally, we discuss the potential for pharmacological modulation of HIFs as a new class of therapeutics in the modern intensive care unit.
Similar content being viewed by others
Avoid common mistakes on your manuscript.
HYPOXIA-INDUCIBLE FACTORS
Hypoxia-inducible factors (HIFs) are a family of nuclear transcription factors that serve as the master regulator of the adaptive response to hypoxia. These transcription factors, including HIF-1, HIF-2, and HIF-3, control the transcription of numerous genes involved in metabolism, angiogenesis, erythropoiesis, and other adaptations to hypoxia. Hypoxia-inducible factor 1 (HIF-1) is composed of HIF-1 alpha and HIF-1 beta subunits. The basis of oxygen sensing for all three HIFs is the hydroxylation of proline residues in the oxygen-dependent degradation (ODD) domain by dioxygenase prolyl hydroxylase (PHD) [1–3] (Fig. 1). PHDs require an iron cofactor for their catalysis and, therefore, also function as sensors for intracellular iron [4]. Additionally, hydroxylation of the proline residues serves as an interaction scaffold for recognition of the Von Hippel–Lindau (VHL)-containing E3-ligase complex and the following degradation by the proteasome, but hydroxylation of the asparagine residue leads to the inhibition of Histone acetyltransferase p300 and cyclic adenosine monophosphate response element binding protein (p300/CBP) recruitment [5, 6].
Hypoxia-inducible factors (HIFs) signaling pathway in normoxic and hypoxic conditions: under normoxia conditions, HIF1/2 are hydroxylated by prolyl hydroxylase domain (PHD)-containing enzymes. Hydroxylated HIFs are degraded in the proteasomes by von Hippel-Lindau tumor suppressor protein (VHL) via polyubiquitination. On the other hand, during hypoxic conditions, PHDs and FIH are unable to hydroxylate HIF-α subunits, which are translocated into the nucleus, resulting in dimerization of HIF-1α and HIF1β, recruitment of p300 and CBP, and ultimately, binding to HREs at target genes to cause activation. This complex thereby activates specific genes, which will further trigger pathological activities.
In the setting of hypoxia, HIFs are stabilized and translocated to the nucleus, where they heterodimerize with the aryl hydrocarbon nuclear translocator (ARNT), also known as HIF-1β [7]. This heterodimer complex binds to the core DNA sequence 5′-TACGTG-3′ within the hypoxia response element (HRE) of target promoters in conjunction with the p300/CBP complex and other co-activators [8, 9]. HIF-1α is the most prominent isoform implicated in the pathogenesis of inflammatory lung injury [10]. It binds to the core DNA sequence within the HRE of target promoters and causes the activation of over 200 genes involved in various pathways, including inflammation and angiogenesis [11].
ROLE OF HIF IN SPECIFIC CELLULAR PROCESSES
Vascular Growth and Remodeling
HIFs upregulate genes involved in oxygen delivery. This effect manifests in the rapid angiogenesis and vascularization promoted in hypoxic tissues. The arterial vasculature is comprised of three layers. The tunica intima is the innermost layer and is composed of endothelial cells. Hypoxia stimulates hypertrophy and sub-endothelial edema in the tunica intima [12, 13]. Hypoxic stress has also been associated with increased endothelial cell barrier permeability, possibly due to alterations of actin fibers and increased secretions of various vasoconstrictive and pro-mitogenic factors. Vascular endothelium growth factor (VEGF), a prototypical pro-mitogenic factor, is a potent angiogenic agent excreted in response to hypoxia by endothelial and non-endothelial cells including alveolar epithelial cells (AEC) and alveolar macrophages (AM) [14–16]. HIF-1α in endothelial cells regulates the production of stromal-derived factor (SDF)-1, which recruits stem cells to areas of hypoxia and vascularization [17]. Recent evidence also suggests a role for HIFs in releasing the factors thrombospondin-1 and endothelin-1, which are involved in vasoconstriction and vascular remodeling [18, 19].
Furthermore, HIFs promote vascular remodeling and alveolarization in various models of lung injury and prolonged hypoxia [20–24]. These changes are also stimulated by inflammatory cytokines such as interleukin-6 (IL-6) and the recruitment of cells of monocytic lineage, both of which have been shown to act synergistically with hypoxia [25–27].
Cellular Metabolism
HIFs curtail functions associated with oxygen usage, shunting metabolism towards the glycolytic pathway. It was previously believed that the glycolytic pathway was employed under hypoxic conditions because oxygen is limiting. However, studies show that during hypoxia (1% O2), HIF-1α do not finish oxidative phosphorylation. These cells eventually undergo apoptosis due to excessive reactive oxygen species (ROS) [28, 29]. Notably, HIFs reduce ROS production formed as a byproduct of the electron transport chain (ETC). The aerobic glycolysis reaction favored by HIF signaling is called the Warburg effect.
Glycolysis is modulated under hypoxic conditions through HIF-controlled upregulation of the glycolytic enzymes aldolase A, phosphoglycerate kinase 1, enolase 1, phosphofructokinase 2, and pyruvate kinase, all of which have been found to contain HREs within their promoter regions [30–32]. HIF-1α also upregulates pyruvate dehydrogenase kinase and lactate dehydrogenase [33]. GLUT1, a vital glucose transporter, is upregulated by HIF-1α under hypoxic conditions to promote glycolysis further [34]. Inflammation has also been shown to trigger the switch to aerobic glycolysis through an AKT-mTOR-HIF-1α pathway mediated by the α-glucan receptor dectin-1 in response to immunogenic challenge [35]. In addition, Eckle et al. demonstrated, with models of ventilator-induced acute lung injury (ALI), that HIF-1α is stabilized even in normoxia, promoting glycolysis, the tricarboxylic acid (TCA) cycle, and preventing worsening of lung injury [36].
PHD activity is blocked by succinate and fumarate, stabilizing HIF-1α activity [37]. Succinate, specifically in macrophages, stabilizes HIF-1α, and is a predominant regulator of acute inflammation, mediated by IL1β [38]. Plasma level of succinate is reported to predict mortality in critically injured trauma patients [39]. Finally, HIFs downregulate the biosynthesis of mitochondria while simultaneously increasing mitophagy [40, 41].
Bidirectional Relationship of HIF-1α and Acute Inflammation
There is a well-known link between hypoxia and inflammation. Prominent among factors other than hypoxia that activate HIF-1α is nuclear factor kappa B (NF-κB). This transcription factor is controlled through the IkB (inhibitor of NF-κB) kinases, IKKα, and IKKβ. Once these kinases are phosphorylated, which occurs under hypoxic conditions, they phosphorylate IkBα-β, causing its degradation and the release of NF-κB [42, 43]. NF-κB, in turn, can upregulate the transcription of HIFs [43–45]. HIF-1α participates in a negative feedback loop by inducing the TAK-TAB complex and CDK6 to sequester NF-κB [46]. In addition to the IKK/NF-κB pathway, HIFs also modulate the PI3K/AKT pathway, of which NF-κB is a downstream effector [47]. HIF-1α, as a result, is directly involved in the regulation of a wide range of proinflammatory proteins, including interleukin-1β (IL-1β), IL-6, MIP-1, TNF-α, hydrogen peroxide, and prostaglandins in AM [38, 48–51]. A bidirectional relationship, therefore, exists between HIF-1α and NF-κB.
Our lab and others have characterized the role of the alveolar epithelium in hypoxic inflammation. Type II AECs are a significant source of chemotactic factors, such as CCL20 (chemokine ligand 20), CCL2, and CXCL1, which serve as recruitment signals for circulating leukocytes and adhesive factors for leukocyte extravasation, such as intercellular adhesion molecule 1 (ICAM-1) and vascular cell adhesion protein 1 (VCAM-1) [52–55]. Like AM, type II AECs produce many proinflammatory mediators, including MIP-2, GM-CSF, IL-6, and IL-1β [53, 55, 56]. Interestingly, recent work has revealed an anti-inflammatory mechanism involving HIFs in regulating extracellular adenosine, a metabolite involved in dampening the inflammatory response. HIF-1α regulation of heme oxygenase-1 (HO-1) has also been identified as an important anti-inflammatory pathway [57].
Apoptosis
The role of HIFs in apoptosis is complex. Multiple studies report that HIFs can stimulate or suppress apoptosis [58, 59]. Indeed, the function of HIFs in both the intrinsic and extrinsic apoptotic pathways seems to depend on the specific cell type, environmental factors, and particular pathology.
Broadly, apoptosis involves two separate regulatory pathways. In the intrinsic pathway, damage to DNA leads to the release of three interacting subgroups of Bcl-2 family proteins. The first group consists of proteins such as Bcl-2 and Bcl-xL, which have anti-apoptotic properties. The second group, including the proteins Bax and Bak, is crucial to apoptotic signaling and mediates mitochondrial outer membrane permeabilization and the release of cytochrome c into the cytosol [60, 61]. The third group includes proteins such as Bid and Bim, which regulate group 2 proteins and cause oligomerization of Bax and Bak [62]. Cytosolic cytochrome c binds to Apaf-1 and pro-Caspase 9 to form the apoptosome complex, ultimately activating caspase 3 and caspase 7 to execute apoptosis [63]. In the extrinsic pathway, a death ligand binds to a death receptor on the outer leaflet of the plasma membrane. Much of the research on the relationship between HIFs and apoptosis in the context of AEC, including from our group, suggests a generally pro-apoptotic relationship [64].
Several studies have also characterized the link between HIFs and p53 [65–67]. This subject has spawned significant interest because of the role of p53 as a master regulator of proliferative genes, tumor suppressor genes, and apoptotic signaling pathways [68, 69]. It has been proposed that direct protein–protein –HIFs ODD domain lead to the stabilization of p53 [65, 70, 71]. Other interactions between HIF-1α and the p53 ubiquitin ligase Mdm2 and between the VHL complex and p53 suggest different association mechanisms and induction between HIFs and p53 [66, 72].
Much of the body of evidence demonstrating the anti-apoptotic role of HIFs has been found in studies of cancer cell lines [73, 74]; the specific relevance to lung injury requires further investigation. In one such study, an inhibitor of a PHD was used to show that increased HIF-1α activity was associated with lower expression of Fas and caspase 3 [75]. Finally, in more clinically relevant studies, HIF-1α has been shown to downregulate the expression of Mcl-1 in hypoxic bronchial epithelial cells [76].
ROLE OF HIF-1α IN SPECIFIC ETIOLOGIES OF ACUTE RESPIRATORY DISTRESS SYNDROME
Acute respiratory distress syndrome (ARDS) is a clinical condition in which bilateral inflammation in the lung leads to the development of progressive respiratory failure. The clinical situation is characterized by the development of hypoxia, acute onset bilateral infiltrates, and reduced compliance of the lung. Despite advances in critical care that include low tidal volume ventilation [77], restrictive fluid strategies, and therapy directed at early identification and treatment of risk factors, ARDS-related mortality remains at 30–46% (increasing with ARDS severity) [78] with considerable morbidity [79, 80]. Prominent risk factors for ARDS development among direct insults to the lung include bacterial pneumonia, lung contusion, and aspiration-induced lung injury. Indirect lung insults include sepsis and pancreatitis. The broad impact of the response to hypoxia and HIF-mediated pathways on the progression of lung injuries is becoming better defined. The role of HIFs and the possible effects of HIF modulation is complex and primarily dependent on the clinical context [81, 82].
Lung Contusion
Lung contusion (LC) describes an injury caused most frequently by blunt force trauma to the chest, damaging the alveolar capillaries without ripping or tearing the lung tissue. Most injuries occur due to two underlying mechanisms: lighter alveolar tissue shearing from hilar tissue due to differential densities and rapid implosion and then expansion of air in alveolar spaces in the wake of a shock wave. These result in the accumulation of alveolar injury, accumulation of blood, and pulmonary edema. LC often presents with hypoxemia, reduced lung compliance, and tachycardia. There are currently no specific pharmacological treatments. Management is purely supportive, focusing on providing supplemental oxygen and mechanical ventilation. Importantly, LC is an independent risk factor for acute respiratory distress syndrome (ARDS), a condition characterized by fluid buildup in alveolar spaces and widespread inflammation associated with significant morbidity and mortality [83].
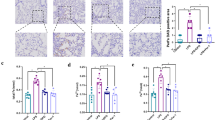
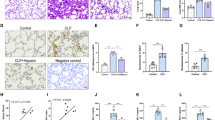
Using a standardized sterile unilateral model of LC, our lab has recently reported that hypoxic type II AEC is the primary driver of inflammation through the activation of HIF-1α. Using a chimeric HIF-1α with the ODD domain fused to luciferase, we demonstrated that LC results in profound global hypoxia with HIF-1α activation and subsequent upregulation of proinflammatory mediators, including IL-1β and IL-6. Following conditional knockout (cKO) of HIF-1α in type II AEC through a Cre-lox system, there were significant reductions in permeability injury, proinflammatory cytokines and chemokines, and AEC apoptosis. HIF-1α cKO mice were also found to have decreased activation of NF-κB, NLRP-3, caspase 1, and IL-1β. This data suggests that HIF-1α mediates inflammation by propagating NF-κB and the NLRP-3 inflammasome [53, 67]. HIF-1α cKO mice were also found to have diminished intra-alveolar hemorrhage, proteinaceous deposits, and infiltration of macrophages and neutrophils consistent with better preservation of lung tissue following LC [53]. Histologic evaluation confirmed that both inflammation and injury were mediated through HIF-1α. These results ultimately show that HIF-1α in AEC directly regulates the nature of the acute inflammatory response following LC. A summary of the findings is illustrated in Fig. 2. Importantly, these results indicate that blockade of HIF-1α activation with compounds represents a targeted therapy for blunt force trauma resulting in pulmonary contusion.
Alveolar epithelial cell (type II) regulation of HIF-1α promotes lung injury and inflammation. Mechanisms of activation include succinate dehydrogenase (SDH) accumulation due to mutation that further stabilizes HIF1. There is both direct and indirect (through NF-kB) mechanism of inflammasome activation leading to further injury and inflammation. HIF-1α is a nuclear transcription factor and regulates gene expression, and its role in lung injury and inflammation is transcription-dependent.
Aspiration-Induced Lung Injury
Aspiration is defined as the inhalation of foreign particles into the airways. The particles are highly variable depending on the situation and commonly consist of blood, bacteria, or ingested substances. Aspiration-induced injury can be challenging to diagnose as it is not uncommon for micro-aspiration events to occur sub-acutely in sedation, endotracheal intubation, and trauma. Aspiration injuries can be categorized as either aspiration pneumonitis (i.e., chemical pneumonitis) or aspiration pneumonia, characterized by infection secondary to the aspiration event. The severity of the aspiration-induced injury can vary from mild subclinical pneumonitis to progressive respiratory failure and ARDS [84, 85].
Our lab has recently published data on the crucial role of HIF-1α through type II AEC in hypoxia-mediated inflammation and injury following the aspiration of gastric acid (GA) and the combination of acid and small gastric particles (CASP) [55]. Using our previously mentioned murine models with luciferase-linked HIF-1α and type II AEC-specific HIF-1α cKO, we demonstrated hypopharyngeal injection of a suspension of gastric particles in hydrochloric acid produced significant hypoxia in the lungs and globally. There was diminished proinflammatory cytokine and chemokine production, including IL-1β and KC, in knockout mice and decreased histological injury with minor intra-alveolar hemorrhage, neutrophil infiltration, and edema. As with LC, reductions in aspiration-induced swelling and inflammation also appeared linked to attenuation in hypoxia-induced NF-kB activity [55].
Zhang et al. have also made significant contributions to our understanding of the role of HIFs in aspiration-induced injury. In their injury model, rats are anesthetized with sodium pentobarbital, and the prepared sea water is injected into the trachea. In this model, HIF-1α was shown to upregulate endothelial cell adhesion factor semaphorin 7A, resulting in a wide range of effects, including neutrophil infiltration, the release of proinflammatory cytokines, loosening of the barrier, and increased VEGF expression [86, 87].
Bacterial Pneumonia
Bacterial pneumonia is a significant cause of morbidity and mortality in the modern ICU and remains one of the most common nosocomial infections [88]. In a recent epidemiological study of ventilator-associated pneumonia (VAP), the most common bacterial pathogens identified were Staphylococcus aureus, Pseudomonas aeruginosa, Klebsiella pneumoniae, and Enterobacter species [89]. It is well-known that HIFs, particularly HIF-1α, are involved in responses to various human pathogens both in vitro and in vivo under hypoxic and normoxic conditions [90, 91]. HIF-1α has been reported to promote the innate immune response through myeloid cell lines, modulating the expression of primary proinflammatory mediators such as TNF-α [92]. In macrophages, HIF-1α improves phagocytosis and bactericidal capacity and is linked to the expression of immunologic surface markers, including TLR-4 and antigen-presenting structures [93–95].
P. aeruginosa (PA), the next most common pathogen implicated in VAP, also has varied interactions with HIFs. HIF-1α has been found to play a protective role in the immune response of airway epithelial cells to PA. Polke et al. demonstrated that the production of proinflammatory molecules, including IL-6, KC, and MIP-2, following exposure to PA and TLR ligands was reduced under hypoxia or in the presence of dimethyloxalylglycine (DMOG) in vitro with human bronchial epithelial cells (HBEC) and human lung cancer cell line (Calu-3) [96]. The administration of siRNA targeting HIF-1α resulted in the upregulation of proinflammatory molecules. Gil-Marques et al. illustrated another mechanism by which hypoxia and HIF-1α are potentially protective against infection with PA in vitro using A549 cells and RAW 264.7 murine macrophages and in vivo with a murine model of pneumonia. In vitro, HIF-1α expression in hypoxia was associated with improved bactericidal capacity, and a similar response was observed following DMOG administration under normoxic conditions. Bacterial burden in vivo in the lungs of mice was also reduced, although the levels of HIF-1α were found to be decreased compared to controls [97].
KP, Klebsiella pneumoniae, has been found to stimulate the epithelial–mesenchymal transition (EMT), the pathological process by which epithelial cells become undifferentiated and develop mesenchymal characteristics. In vitro, with A549 airway epithelial cells, Leone et al. have described that KP induces intracellular ROS production, thereby upregulating HIF-1α expression and leading to EMT. This process was found to be reversed by the administration of the antioxidant resveratrol, suggesting that this process is mediated upstream by ROS [98]. KP also employs siderophores, which function as iron chelators and improve virulence in a murine model of pneumonia with alveolar epithelial cell-specific HIF-1α cKO mice.
LPS-Induced Lung Injury
Lipopolysaccharide (LPS) is often used as a surrogate for bacterial pneumonia. It is used to illustrate the effects of LPS, a product constituent of the bacterial wall in gram-negative infections, in animal models to illustrate the effect of bacterial products without the impact of bacterial growth. Studies have linked HIF to NF-κB activity while observing marked reductions in proinflammatory cytokine production in response to an LPS challenge [99]. Xu et al. found that HIF-1α translation through the PI3K/AKT and MAPK pathways was blocked, and HIF-1α breakdown was increased with tanshinone IIA treatment following LPS exposure. Therefore, the improvement in inflammation following the administration of tanshinone IIA points to the upregulation of HIF-1α as a mechanism of LPS-mediated inflammation [100]. In myeloid cells, a synergistic effect with Toll-like receptor 4 (TLR-4), the LPS-sensitive pattern recognition receptor, was proposed in which HIF-1α directly upregulates proinflammatory cytokines and TLR-4 gene expression (101). Further experiments corroborated the detrimental effect of HIF-1α in myeloid cells, demonstrating worse edema, leukocyte infiltration, and cytokine release [102].
Interestingly, there exist conflicting reports regarding the role of HIF-1α in the setting of LPS-related lung injury. Tang et al. examined the alveolar–capillary interface in an LPS model of ALI [103]. They found that upregulation of the TNF-α/HIF-1α pathway reduced the expression of vasodilator-stimulated phosphoprotein, which is involved in maintaining cytoskeleton integrity. HIF-1α upregulation was associated with higher permeability of the alveolar–capillary barrier. There is also evidence for a protective metabolic effect of HIF-1α. In a recent report, Tojo et al. investigated the efficacy of the PHD inhibitor dimethyloxalylglycine (DMOG) in an LPS model of ARDS. They found both in vitro with MLE12 alveolar epithelial cells and in vivo with a murine model that cell viability was improved, likely through the HIF-1α mediated preference for glycolysis [104]. In another study, Hu et al. investigated the outcome of isoflurane treatment following an LPS model of ALI [105]. They found that the inhibitory microRNA miR-155 levels were decreased by isoflurane, thereby increasing the expression of HIF-1α and HO-1.
Role of HIF in SARS-CoV-2 (COVID-19)
Coronavirus disease 2019 (COVID-19), caused by severe acute respiratory syndrome coronavirus 2 (SARS-CoV-2), is a novel virus first identified in China and is responsible for the unprecedented 2019–2022 pandemic [106]. Andrey et al. reported that the first step of viral invasion is the interaction of SARS-CoV-2 with the angiotensin-converting enzyme 2 (ACE2) receptor on the cell surface [107]. ACE2 is the surface receptor for SARS-CoV-2, directly interacting with the spike glycoprotein (S protein) [108]. Previous studies demonstrated increased ACE2 expression in the setting of hypoxia [109, 110]. Several reports suggest that COVID-19 infection induces severe hypoxic conditions [107]. Hypoxia, in turn, activates HIF-1α with subsequent inflammatory cytokine production and glycolysis enhancement. Therefore, the COVID-19 hypoxic conditions and the following HIF-1α-dependent gene expression likely potentiate and exacerbate M1 polarization.
On the contrary, Endika Prieto-Fernández et al. reported that hypoxia decreases the attachment of the receptor-binding domain (RBD) and the S1 subunit (S1) of the spike protein to epithelial cells. However, hypoxia also inhibits the binding of the spike to human lung epithelial cells lacking ACE2 expression, indicating that hypoxia modulates the expression of additional binding partners of SARS-CoV-2 [111, 112]. Ultimately, hypoxia acts to prevent SARS-CoV-2 infection, suggesting that the hypoxia signaling pathway might offer therapeutic opportunities for treating COVID-19. In this context, elucidating the role of the HIF signaling pathway might unlock novel therapeutic targets that, when modulated, reduce the initial virus–host interaction and viral load [111].
Notably, the SARS-CoV-2 virus primarily attacks pulmonary tissues and impairs gas exchange, leading to acute respiratory distress syndrome (ARDS) and systemic hypoxia [113] Tian et al. reported that during SARS-CoV-2 infection, the viral ORF3a protein elevates the production of HIF-1α, which, in turn, promotes SARS-CoV-2 disease and inflammatory responses. Therefore, HIF-1α is a crucial activator for SARS-CoV-2 infection and inflammatory responses [114]. RNA sequencing shows that HIF-1α signaling, immune response, and metabolism pathways are dysregulated in COVID-19 patients [114]. Clinical analyses indicate that HIF-1α production, inflammatory responses, and high mortalities occur in elderly patients. HIF-1α and proinflammatory cytokines are elicited in patients and infected cells. HIF-1α plays an essential role in promoting SARS-CoV-2 infection and inducing proinflammatory responses to COVID-19 [114]. Zoya et al. speculated in their review article that the activation of the HIF-1α signaling pathway under mild hypoxic conditions would decrease ACE2 and TMPRSS2 and increase ADAM17 levels on the surface of alveolates and, therefore, decrease the invasiveness of SARS-CoV-2 [113]. On the contrary, the protein targets of HIF-1α are involved in the severe hypoxia-induced activation of proinflammatory cytokine expression and the subsequent inflammation process and cytokine storm phase of COVID-19 [113].
Finally, COVID-19 results in inflammatory solid response and ARDS in severe disease cases. Based on the available data, HIF-1α is a crucial factor that responds to the hypoxic microenvironment at the site of inflammation [19]. HIF-1α is an essential activator for SARS-CoV-2 infection and inflammatory response, serving as a potential therapeutic target for virus-induced inflammatory diseases and COVID-19. A summary of the current understanding of the role of HIF-1α in the pathogenesis of SARS-COV-2 is outlined in Fig. 3. HIF-1α inhibition through pharmacological strategies might provide a new approach to aid the treatment of patients affected with COVID-19.
Proposed pathological mechanisms of COVID-19 involve hypoxia and HIF-1α-dependent detrimental cell signaling pathways. SARS-CoV-2 attaches to the ACE2 receptor on the cell surface of type II alveolar epithelial cells. Moreover, HIF-1α induction in the hypoxic and inflammatory conditions increases the recruitment of inflammatory cells to the infection site and increases fluid accumulation leading to pneumonia and ARDS. Increasing the recruitment of inflammatory cells to the infection site and increased fluid accumulation leads to pneumonia and ARDS.
IS HIF IN LUNG INJURY ADAPTIVE OR MALADAPTIVE?
In models of LC and gastric aspiration (ACID and ACID + particulate), we have reported that hypoxia is seen as early as 30 min following insult. This coincides with increased nuclear activity of HIF-1α (confirmed by western blots and luciferase activity in ODD-Luc mice) [53]. Furthermore, direct abrogation of HIF-1α led to significant reductions in permeability injury and acute inflammatory responses. Post-mortem human samples of lungs from patients who died with LC show important HIF1-α protein localization in alveolar macrophages and airway epithelial cells. Notably, similar findings were discovered in acid aspiration [55]. Alveolar epithelial cells (AEC), including type II AEC, constitute the physical and functional barrier in the lung. Once considered innocent bystanders in ARDS, they are now understood as stem cells with a specific role in the reparative processes. Our lab and others have identified AEC to have a particular role in initiating and progressing certain forms of inflammatory lung injury (LC, ACID, and ACID + particulate aspiration) [53, 55]. Specifically, we have shown that the regulation of HIF-1α in type II AEC directly regulates the progression of the acute inflammatory response leading to hypoxia, diminished lung compliance, and robust inflammation [53, 55].
It is entirely possible that HIF-1α plays the role of an adaptive molecule by driving the metabolic pathway towards glycolysis in certain etiologies of lung injury. A body of evidence shows enhancement of glycolysis by inhibition of PHD and thereby activation of HIF-1α to protect alveolar epithelial cells [104]. Alveolar stretch is a phenomenon seen in ventilator-induced lung injury following the development of refractory hypoxia in lung injury. Eltzschig and colleagues have reported that, in a model of alveolar stretch-induced inflammation, HIF-1α plays a protective role [115]. Similarly, McClendon et al. concluded that HIF-1α is activated in ATII cells after lung injury and promotes proliferation and spreading during repair [116]. These results are contradictory to our experimental data. In our models of lung injury, HIF1-α increases lung injury and inflammation and is, therefore, maladaptive [53, 55].
It is highly likely that HIF-1α has disparate roles that depend on the cell type, nature of the inflammatory response, and timing of injury-acute versus chronic. For example, hypoxia is a direct consequence of LC and acid aspiration that prompts some patients to require mechanical ventilation.
THERAPEUTIC STRATEGIES FOR MODULATION OF HIF
Several recent reviews [74, 117–119] demonstrate mechanisms of pharmacological HIF modulation. In cases of sterile injury, HIF inhibitors acriflavine, 4-hydroxyphenyl acetic acid, and 3,5,4′-tri-O-acetyl resveratrol reduce inflammation with beneficial effects. By contrast, HIF inducers such as PHD inhibitors have been tested as therapeutic agents in non-sterile injury. Most PHD inhibitors are 2-oxoglutarate analogs, such as DMOG and mimosine, which induce HIFs [120]. PDH inhibitors represent a promising new drug class, and multiple recent reviews discuss their potential effectiveness [120–122]. Such compounds may constitute an original, desperately needed approach to lung injuries, especially as the increasing prevalence of antibiotic-resistant pathogens and conditions like ARDS continues to challenge the modern ICU (Table1).
DATA AVAILABILITY
All data collected and analyzed within this study are available from the corresponding author on request.
References
Jaakkola, P., D.R. Mole, Y.M. Tian, M.I. Wilson, J. Gielbert, S.J. Gaskell, A. von Kriegsheim, H.F. Hebestreit, M. Mukherji, C.J. Schofield, P.H. Maxwell, C.W. Pugh, and P.J. Ratcliffe. 2001. Targeting of HIF-alpha to the von Hippel-Lindau ubiquitylation complex by O2-regulated prolyl hydroxylation. Science 292: 468–472.
Masson, N., C. Willam, P.H. Maxwell, C.W. Pugh, and P.J. Ratcliffe. 2001. Independent function of two destruction domains in hypoxia-inducible factor-alpha chains activated by prolyl hydroxylation. EMBO Journal 20: 5197–5206.
Maynard, M.A., H. Qi, J. Chung, E.H. Lee, Y. Kondo, S. Hara, R.C. Conaway, J.W. Conaway, and M. Ohh. 2003. Multiple splice variants of the human HIF-3 alpha locus are targets of the von Hippel-Lindau E3 ubiquitin ligase complex. Journal of Biological Chemistry 278: 11032–11040.
Xu, M.M., J. Wang, and J.X. Xie. 2017. Regulation of iron metabolism by hypoxia-inducible factors. Sheng Li Xue Bao 69: 598–610.
Sang, N., J. Fang, V. Srinivas, I. Leshchinsky, and J. Caro. 2002. Carboxyl-terminal transactivation activity of hypoxia-inducible factor 1 alpha is governed by a von Hippel-Lindau protein-independent, hydroxylation-regulated association with p300/CBP. Molecular and Cellular Biology 22: 2984–2992.
Lando, D., D.J. Peet, D.A. Whelan, J.J. Gorman, and M.L. Whitelaw. 2002. Asparagine hydroxylation of the HIF transactivation domain a hypoxic switch. Science 295: 858–861.
Stolze, I., U. Berchner-Pfannschmidt, P. Freitag, C. Wotzlaw, J. Rossler, S. Frede, H. Acker, and J. Fandrey. 2002. Hypoxia-inducible erythropoietin gene expression in human neuroblastoma cells. Blood 100: 2623–2628.
Arany, Z., L.E. Huang, R. Eckner, S. Bhattacharya, C. Jiang, M.A. Goldberg, H.F. Bunn, and D.M. Livingston. 1996. An essential role for p300/CBP in the cellular response to hypoxia. Proceedings of the National Academy of Sciences of the USA 93: 12969–12973.
Bhattacharya, S., C.L. Michels, M.K. Leung, Z.P. Arany, A.L. Kung, and D.M. Livingston. 1999. Functional role of p35srj, a novel p300/CBP binding protein, during transactivation by HIF-1. Genes & Development 13: 64–75.
Shimoda, L.A., and G.L. Semenza. 2011. HIF and the lung: Role of hypoxia-inducible factors in pulmonary development and disease. American Journal of Respiratory and Critical Care Medicine 183: 152–156.
Semenza, G.L. 2014. Oxygen sensing, hypoxia-inducible factors, and disease pathophysiology. Annual Review of Pathology: Mechanisms of Disease 9: 47–71.
Meyrick, B., and L. Reid. 1980. Endothelial and subintimal changes in rat hilar pulmonary artery during recovery from hypoxia. A quantitative ultrastructural study. Laboratory Investigation 42: 603–615.
Stenmark, K.R., B. Meyrick, N. Galie, W.J. Mooi, and I.F. McMurtry. 2009. Animal models of pulmonary arterial hypertension: The hope for etiological discovery and pharmacological cure. American Journal of Physiology. Lung Cellular and Molecular Physiology 297: L1013-1032.
Forsythe, J.A., B.H. Jiang, N.V. Iyer, F. Agani, S.W. Leung, R.D. Koos, and G.L. Semenza. 1996. Activation of vascular endothelial growth factor gene transcription by hypoxia-inducible factor 1. Molecular and Cellular Biology 16: 4604–4613.
Kouvaras, E., Z. Christoni, I. Siasios, K. Malizos, G.K. Koukoulis, and M. Ioannou. 2019. Hypoxia-inducible factor 1-alpha and vascular endothelial growth factor in cartilage tumors. Biotechnic and Histochemistry 94: 283–289.
Li, J., S.X. Li, X.H. Gao, L.F. Zhao, J. Du, T.Y. Wang, L. Wang, J. Zhang, H.Y. Wang, R. Dong, and Z.Y. Guo. 2019. HIF1A and VEGF regulate each other by competing endogenous RNA mechanism and involve in the pathogenesis of peritoneal fibrosis. Pathology, Research and Practice 215: 644–652.
Ceradini, D.J., A.R. Kulkarni, M.J. Callaghan, O.M. Tepper, N. Bastidas, M.E. Kleinman, J.M. Capla, R.D. Galiano, J.P. Levine, and G.C. Gurtner. 2004. Progenitor cell trafficking is regulated by hypoxic gradients through HIF-1 induction of SDF-1. Nature Medicine 10: 858–864.
Labrousse-Arias, D., R. Castillo-Gonzalez, N.M. Rogers, M. Torres-Capelli, B. Barreira, J. Aragones, A. Cogolludo, J.S. Isenberg, and M.J. Calzada. 2016. HIF-2alpha-mediated induction of pulmonary thrombospondin-1 contributes to hypoxia-driven vascular remodelling and vasoconstriction. Cardiovascular Research 109: 115–130.
Gras, E., E. Belaidi, A. Briancon-Marjollet, J.L. Pepin, C. Arnaud, and D. Godin-Ribuot. 1985. (2016) Endothelin-1 mediates intermittent hypoxia-induced inflammatory vascular remodeling through HIF-1 activation. Journal of Applied Physiology 120: 437–443.
Choi, C.W., J. Lee, H.J. Lee, H.S. Park, Y.S. Chun, and B.I. Kim. 2015. Deferoxamine improves alveolar and pulmonary vascular development by upregulating hypoxia-inducible factor-1alpha in a rat model of bronchopulmonary dysplasia. Journal of Korean Medical Science 30: 1295–1301.
Vadivel, A., R.S. Alphonse, N. Etches, T. van Haaften, J.J. Collins, M. O’Reilly, F. Eaton, and B. Thebaud. 2014. Hypoxia-inducible factors promote alveolar development and regeneration. American Journal of Respiratory Cell and Molecular Biology 50: 96–105.
Tibboel, J., F.A. Groenman, J. Selvaratnam, J. Wang, I. Tseu, Z. Huang, I. Caniggia, D. Luo, M. van Tuyl, C. Ackerley, J.C. de Jongste, D. Tibboel, and M. Post. 2015. Hypoxia-inducible factor-1 stimulates postnatal lung development but does not prevent O2-induced alveolar injury. American Journal of Respiratory Cell and Molecular Biology 52: 448–458.
Yu, A.Y., L.A. Shimoda, N.V. Iyer, D.L. Huso, X. Sun, R. McWilliams, T. Beaty, J.S. Sham, C.M. Wiener, J.T. Sylvester, and G.L. Semenza. 1999. Impaired physiological responses to chronic hypoxia in mice partially deficient for hypoxia-inducible factor 1alpha. The Journal of Clinical Investigation 103: 691–696.
Brusselmans, K., V. Compernolle, M. Tjwa, M.S. Wiesener, P.H. Maxwell, D. Collen, and P. Carmeliet. 2003. Heterozygous deficiency of hypoxia-inducible factor-2alpha protects mice against pulmonary hypertension and right ventricular dysfunction during prolonged hypoxia. The Journal of Clinical Investigation 111: 1519–1527.
Steiner, M.K., O.L. Syrkina, N. Kolliputi, E.J. Mark, C.A. Hales, and A.B. Waxman. 2009. Interleukin-6 overexpression induces pulmonary hypertension. Circulation Research 104: 236–244, 228p following 244.
Frid, M.G., J.A. Brunetti, D.L. Burke, T.C. Carpenter, N.J. Davie, J.T. Reeves, M.T. Roedersheimer, N. van Rooijen, and K.R. Stenmark. 2006. Hypoxia-induced pulmonary vascular remodeling requires recruitment of circulating mesenchymal precursors of a monocyte/macrophage lineage. American Journal of Pathology 168: 659–669.
Epelman, S., K.J. Lavine, and G.J. Randolph. 2014. Origin and functions of tissue macrophages. Immunity 41: 21–35.
Samanta, D., and G.L. Semenza. 2017. Maintenance of redox homeostasis by hypoxia-inducible factors. Redox Biology 13: 331–335.
Li, Y., A. Jia, Y. Wang, L. Dong, Y. Wang, Y. He, S. Wang, Y. Cao, H. Yang, Y. Bi, and G. Liu. 2019. Immune effects of glycolysis or oxidative phosphorylation metabolic pathway in protecting against bacterial infection. Journal of Cellular Physiology 234: 20298–20309.
Semenza, G.L., P.H. Roth, H.M. Fang, and G.L. Wang. 1994. Transcriptional regulation of genes encoding glycolytic enzymes by hypoxia-inducible factor 1. Journal of Biological Chemistry 269: 23757–23763.
Semenza, G.L., B.H. Jiang, S.W. Leung, R. Passantino, J.P. Concordet, P. Maire, and A. Giallongo. 1996. Hypoxia response elements in the aldolase A, enolase 1, and lactate dehydrogenase A gene promoters contain essential binding sites for hypoxia-inducible factor 1. Journal of Biological Chemistry 271: 32529–32537.
Rodriguez-Prados, J.C., P.G. Traves, J. Cuenca, D. Rico, J. Aragones, P. Martin-Sanz, M. Cascante, and L. Bosca. 2010. Substrate fate in activated macrophages: A comparison between innate, classic, and alternative activation. The Journal of Immunology 185: 605–614.
Kim, J.W., I. Tchernyshyov, G.L. Semenza, and C.V. Dang. 2006. HIF-1-mediated expression of pyruvate dehydrogenase kinase: A metabolic switch required for cellular adaptation to hypoxia. Cell Metabolism 3: 177–185.
Iyer, N.V., L.E. Kotch, F. Agani, S.W. Leung, E. Laughner, R.H. Wenger, M. Gassmann, J.D. Gearhart, A.M. Lawler, A.Y. Yu, and G.L. Semenza. 1998. Cellular and developmental control of O2 homeostasis by hypoxia-inducible factor 1 alpha. Genes & Development 12: 149–162.
Cheng, S.C., J. Quintin, R.A. Cramer, K.M. Shepardson, S. Saeed, V. Kumar, E.J. Giamarellos-Bourboulis, J.H. Martens, N.A. Rao, A. Aghajanirefah, G.R. Manjeri, Y. Li, D.C. Ifrim, R.J. Arts, B.M. van der Veer, P.M. Deen, C. Logie, L.A. O’Neill, P. Willems, F.L. van de Veerdonk, J.W. van der Meer, A. Ng, L.A. Joosten, C. Wijmenga, H.G. Stunnenberg, R.J. Xavier, and M.G. Netea. 2014. mTOR- and HIF-1alpha-mediated aerobic glycolysis as metabolic basis for trained immunity. Science 345: 1250684.
Eckle, T., K. Brodsky, M. Bonney, T. Packard, J. Han, C.H. Borchers, T.J. Mariani, D.J. Kominsky, M. Mittelbronn, and H.K. Eltzschig. 2013. HIF1A reduces acute lung injury by optimizing carbohydrate metabolism in the alveolar epithelium. PLoS Biology 11: e1001665.
Selak, M.A., S.M. Armour, E.D. MacKenzie, H. Boulahbel, D.G. Watson, K.D. Mansfield, Y. Pan, M.C. Simon, C.B. Thompson, and E. Gottlieb. 2005. Succinate links TCA cycle dysfunction to oncogenesis by inhibiting HIF-alpha prolyl hydroxylase. Cancer Cell 7: 77–85.
Tannahill, G.M., A.M. Curtis, J. Adamik, E.M. Palsson-McDermott, A.F. McGettrick, G. Goel, C. Frezza, N.J. Bernard, B. Kelly, N.H. Foley, L. Zheng, A. Gardet, Z. Tong, S.S. Jany, S.C. Corr, M. Haneklaus, B.E. Caffrey, K. Pierce, S. Walmsley, F.C. Beasley, E. Cummins, V. Nizet, M. Whyte, C.T. Taylor, H. Lin, S.L. Masters, E. Gottlieb, V.P. Kelly, C. Clish, P.E. Auron, R.J. Xavier, and L.A. O’Neill. 2013. Succinate is an inflammatory signal that induces IL-1beta through HIF-1alpha. Nature 496: 238–242.
D’Alessandro, A., H.B. Moore, E.E. Moore, J.A. Reisz, M.J. Wither, A. Ghasasbyan, J. Chandler, C.C. Silliman, K.C. Hansen, and A. Banerjee. 2017. Plasma succinate is a predictor of mortality in critically injured patients. Journal of Trauma and Acute Care Surgery 83: 491–495.
Zhang, H., M. Bosch-Marce, L.A. Shimoda, Y.S. Tan, J.H. Baek, J.B. Wesley, F.J. Gonzalez, and G.L. Semenza. 2008. Mitochondrial autophagy is an HIF-1-dependent adaptive metabolic response to hypoxia. Journal of Biological Chemistry 283: 10892–10903.
Zhang, H., P. Gao, R. Fukuda, G. Kumar, B. Krishnamachary, K.I. Zeller, C.V. Dang, and G.L. Semenza. 2007. HIF-1 inhibits mitochondrial biogenesis and cellular respiration in VHL-deficient renal cell carcinoma by repression of C-MYC activity. Cancer Cell 11: 407–420.
Hacker, H., and M. Karin. 2006. Regulation and function of IKK and IKK-related kinases. Sciences STKE 2006: re13.
Rius, J., M. Guma, C. Schachtrup, K. Akassoglou, A.S. Zinkernagel, V. Nizet, R.S. Johnson, G.G. Haddad, and M. Karin. 2008. NF-kappaB links innate immunity to the hypoxic response through transcriptional regulation of HIF-1alpha. Nature 453: 807–811.
Jiang, H., Y.S. Zhu, H. Xu, Y. Sun, and Q.F. Li. 2010. Inflammatory stimulation and hypoxia cooperatively activate HIF-1{alpha} in bronchial epithelial cells: Involvement of PI3K and NF-{kappa}B. American Journal of Physiology. Lung Cellular and Molecular Physiology 298: L660-669.
van Uden, P., N.S. Kenneth, and S. Rocha. 2008. Regulation of hypoxia-inducible factor-1alpha by NF-kappaB. The Biochemical Journal 412: 477–484.
Bandarra, D., J. Biddlestone, S. Mudie, H.A. Muller, and S. Rocha. 2015. HIF-1alpha restricts NF-kappaB-dependent gene expression to control innate immunity signals. Disease Models & Mechanisms 8: 169–181.
Zhang, J., H. Guo, J.S. Zhu, Y.C. Yang, W.X. Chen, and N.W. Chen. 2014. Inhibition of phosphoinositide 3-kinase/Akt pathway decreases hypoxia inducible factor-1alpha expression and increases therapeutic efficacy of paclitaxel in human hypoxic gastric cancer cells. Oncology Letters 7: 1401–1408.
VanOtteren, G.M., T.J. Standiford, S.L. Kunkel, J.M. Danforth, and R.M. Strieter. 1995. Alterations of ambient oxygen tension modulate the expression of tumor necrosis factor and macrophage inflammatory protein-1 alpha from murine alveolar macrophages. American Journal of Respiratory Cell and Molecular Biology 13: 399–409.
Wilhelm, J., and Sojkov├í, J., and Herget, J. 1996. Production of hydrogen peroxide by alveolar macrophages from rats exposed to subacute and chronic hypoxia. Physiological Research 45: 185–191.
Compeau, C.G., J. Ma, K.N. DeCampos, T.K. Waddell, G.F. Brisseau, A.S. Slutsky, and O.D. Rotstein. 1994. In situ ischemia and hypoxia enhance alveolar macrophage tissue factor expression. American Journal of Respiratory Cell and Molecular Biology 11: 446–455.
Fernandez-Bustamante, A., J. Klawitter, P. Wilson, N.D. Elkins, A. Agazio, T. Shibata, K. Uchida, U. Christians, and J.E. Repine. 2013. Early increase in alveolar macrophage prostaglandin 15d-PGJ2 precedes neutrophil recruitment into lungs of cytokine-insufflated rats. Inflammation 36: 1030–1040.
Thorley, A.J., P. Goldstraw, A. Young, and T.D. Tetley. 2005. Primary human alveolar type II epithelial cell CCL20 (macrophage inflammatory protein-3alpha)-induced dendritic cell migration. American Journal of Respiratory Cell and Molecular Biology 32: 262–267.
Suresh, M.V., S.K. Ramakrishnan, B. Thomas, D. Machado-Aranda, Y. Bi, N. Talarico, E. Anderson, S.M. Yatrik, and K. Raghavendran. 2014. Activation of hypoxia-inducible factor-1alpha in type 2 alveolar epithelial cell is a major driver of acute inflammation following lung contusion. Critical Care Medicine 42: e642-653.
Beck-Schimmer, B., R.C. Schimmer, C. Madjdpour, J.M. Bonvini, T. Pasch, and P.A. Ward. 2001. Hypoxia mediates increased neutrophil and macrophage adhesiveness to alveolar epithelial cells. American Journal of Respiratory Cell and Molecular Biology 25: 780–787.
Suresh, M.V., S. Balijepalli, B. Zhang, V.V. Singh, S. Swamy, S. Panicker, V.A. Dolgachev, C. Subramanian, S.K. Ramakrishnan, B. Thomas, T.C. Rao, M.J. Delano, D. Machado-Aranda, Y.M. Shah, and K. Raghavendran. 2019. Hypoxia-inducible factor (HIF)-1alpha promotes inflammation and injury following aspiration-induced lung injury in mice. Shock 52: 612–621.
Sturrock, A., D. Woller, A. Freeman, K. Sanders, and R. Paine 3rd. 2018. Consequences of hypoxia for the pulmonary alveolar epithelial cell innate immune response. The Journal of Immunology 201: 3411–3420.
Hanze, J., B.G. Eul, R. Savai, S. Krick, P. Goyal, F. Grimminger, W. Seeger, and F. Rose. 2003. RNA interference for HIF-1alpha inhibits its downstream signalling and affects cellular proliferation. Biochemical and Biophysical Research Communications 312: 571–577.
Zhao, X., L. Liu, R. Li, X. Wei, W. Luan, P. Liu, and J. Zhao. 2018. Hypoxia-inducible factor 1-alpha (HIF-1alpha) induces apoptosis of human uterosacral ligament fibroblasts through the death receptor and mitochondrial pathways. Medical Science Monitor 24: 8722–8733.
Saint-Martin, A., J. Martinez-Rios, M.C. Castaneda-Patlan, M.A. Sarabia-Sanchez, N. Tejeda-Munoz, A. Chinney-Herrera, G. Soldevila, R. Benelli, P. Santoyo-Ramos, A. Poggi, and M. Robles-Flores. 2019. Functional interaction of hypoxia-inducible factor 2-alpha and autophagy mediates drug resistance in colon cancer cells. Cancers (Basel) 11: 755–794.
Chao, D.T., and S.J. Korsmeyer. 1998. BCL-2 family: Regulators of cell death. Annual Review of Immunology 16: 395–419.
Wei, M.C., W.X. Zong, E.H. Cheng, T. Lindsten, V. Panoutsakopoulou, A.J. Ross, K.A. Roth, G.R. MacGregor, C.B. Thompson, and S.J. Korsmeyer. 2001. Proapoptotic BAX and BAK: A requisite gateway to mitochondrial dysfunction and death. Science 292: 727–730.
Puthalakath, H., and A. Strasser. 2002. Keeping killers on a tight leash: Transcriptional and post-translational control of the pro-apoptotic activity of BH3-only proteins. Cell Death and Differentiation 9: 505–512.
Acehan, D., X. Jiang, D.G. Morgan, J.E. Heuser, X. Wang, and C.W. Akey. 2002. Three-dimensional structure of the apoptosome: Implications for assembly, procaspase-9 binding, and activation. Molecular Cell 9: 423–432.
Sherman, M.A., M.V. Suresh, V.A. Dolgachev, L.K. McCandless, X. Xue, L. Ziru, D. Machado-Aranda, Y.M. Shah, and K. Raghavendran. 2018. Molecular characterization of hypoxic alveolar epithelial cells after lung contusion indicates an important role for HIF-1alpha. Annals of Surgery 267: 382–391.
Sanchez-Puig, N., D.B. Veprintsev, and A.R. Fersht. 2005. Binding of natively unfolded HIF-1alpha ODD domain to p53. Molecular Cell 17: 11–21.
Chen, D., M. Li, J. Luo, and W. Gu. 2003. Direct interactions between HIF-1 alpha and Mdm2 modulate p53 function. Journal of Biological Chemistry 278: 13595–13598.
Schmid, T., J. Zhou, R. Kohl, and B. Brune. 2004. p300 relieves p53-evoked transcriptional repression of hypoxia-inducible factor-1 (HIF-1). The Biochemical Journal 380: 289–295.
Nakano, K., and K.H. Vousden. 2001. PUMA, a novel proapoptotic gene, is induced by p53. Molecular Cell 7: 683–694.
Oda, E., R. Ohki, H. Murasawa, J. Nemoto, T. Shibue, T. Yamashita, T. Tokino, T. Taniguchi, and N. Tanaka. 2000. Noxa, a BH3-only member of the Bcl-2 family and candidate mediator of p53-induced apoptosis. Science 288: 1053–1058.
An, W.G., M. Kanekal, M.C. Simon, E. Maltepe, M.V. Blagosklonny, and L.M. Neckers. 1998. Stabilization of wild-type p53 by hypoxia-inducible factor 1alpha. Nature 392: 405–408.
Ullah, K., A.H. Rosendahl, V. Izzi, U. Bergmann, T. Pihlajaniemi, J.M. Maki, and J. Myllyharju. 2017. Hypoxia-inducible factor prolyl-4-hydroxylase-1 is a convergent point in the reciprocal negative regulation of NF-kappaB and p53 signaling pathways. Science and Reports 7: 17220.
Roe, J.S., H. Kim, S.M. Lee, S.T. Kim, E.J. Cho, and H.D. Youn. 2006. p53 stabilization and transactivation by a von Hippel-Lindau protein. Molecular Cell 22: 395–405.
Shi, Y., M. Chang, F. Wang, X. Ouyang, Y. Jia, and H. Du. 2010. Role and mechanism of hypoxia-inducible factor-1 in cell growth and apoptosis of breast cancer cell line MDA-MB-231. Oncology Letters 1: 657–662.
Masoud, G.N., and W. Li. 2015. HIF-1alpha pathway: Role, regulation and intervention for cancer therapy. Acta Pharm Sin B 5: 378–389.
Nagamine, Y., K. Tojo, T. Yazawa, S. Takaki, Y. Baba, T. Goto, and K. Kurahashi. 2016. Inhibition of prolyl hydroxylase attenuates fas ligand-induced apoptosis and lung injury in mice. American Journal of Respiratory Cell and Molecular Biology 55: 878–888.
Liu, X.H., E.Z. Yu, Y.Y. Li, and E. Kagan. 2006. HIF-1alpha has an anti-apoptotic effect in human airway epithelium that is mediated via Mcl-1 gene expression. Journal of Cellular Biochemistry 97: 755–765.
Bernard, G.R. 2005. Acute respiratory distress syndrome: A historical perspective. American Journal of Respiratory and Critical Care Medicine 172: 798–806.
Bellani, G., J.G. Laffey, T. Pham, E. Fan, L. Brochard, A. Esteban, L. Gattinoni, F. van Haren, A. Larsson, D.F. McAuley, M. Ranieri, G. Rubenfeld, B.T. Thompson, H. Wrigge, A.S. Slutsky, and A. Pesenti. 2016. Epidemiology, patterns of care, and mortality for patients with acute respiratory distress syndrome in intensive care units in 50 countries. Journal of the American Medical Association 315: 788–800.
Davidson, T.A., E.S. Caldwell, J.R. Curtis, L.D. Hudson, and K.P. Steinberg. 1999. Reduced quality of life in survivors of acute respiratory distress syndrome compared with critically ill control patients. Journal of the American Medical Association 281: 354–360.
Mamary, A.J., S. Kondapaneni, G.B. Vance, J.P. Gaughan, U.J. Martin, and G.J. Criner. 2011. Survival in patients receiving prolonged ventilation: Factors that influence outcome. Clinical Medicine Insights: Circulatory, Respiratory and Pulmonary Medicine 5: 17–26.
Perl, M., J. Lomas-Neira, F. Venet, C.S. Chung, and A. Ayala. 2011. Pathogenesis of indirect (secondary) acute lung injury. Expert Review of Respiratory Medicine 5: 115–126.
Reiss, L.K., U. Uhlig, and S. Uhlig. 2012. Models and mechanisms of acute lung injury caused by direct insults. European Journal of Cell Biology 91: 590–601.
Ganie, F.A., H. Lone, G.N. Lone, M.L. Wani, S. Singh, A.M. Dar, N.U. Wani, S.N. Wani, and N.U. Nazeer. 2013. Lung contusion: A clinico-pathological entity with unpredictable clinical course. Bulletin Emergency Trauma 1: 7–16.
Raghavendran, K., J. Nemzek, L.M. Napolitano, and P.R. Knight. 2011. Aspiration-induced lung injury. Critical Care Medicine 39: 818–826.
Marik, P.E. 2001. Aspiration pneumonitis and aspiration pneumonia. New England Journal of Medicine 344: 665–671.
Zhang, M., L. Wang, M. Dong, Z. Li, and F. Jin. 2014. Endothelial Semaphorin 7A promotes inflammation in seawater aspiration-induced acute lung injury. International Journal of Molecular Sciences 15: 19650–19661.
Zhang, M., X. Yan, W. Liu, R. Sun, Y. Xie, and F. Jin. 2017. Endothelial semaphorin 7A promotes seawater aspiration-induced acute lung injury through plexin C1 and beta1 integrin. Molecular Medicine Reports 16: 4215–4221.
Spalding, M.C., M.W. Cripps, and C.T. Minshall. 2017. Ventilator-associated pneumonia: New definitions. Critical Care Clinics 33: 277–292.
Klompas, M., K. Kleinman, and M.V. Murphy. 2014. Descriptive epidemiology and attributable morbidity of ventilator-associated events. Infection Control and Hospital Epidemiology 35: 502–510.
Werth, N., C. Beerlage, C. Rosenberger, A.S. Yazdi, M. Edelmann, A. Amr, W. Bernhardt, C. von Eiff, K. Becker, A. Schafer, A. Peschel, and V.A. Kempf. 2010. Activation of hypoxia inducible factor 1 is a general phenomenon in infections with human pathogens. PLoS ONE 5: e11576.
Peyssonnaux, C., V. Datta, T. Cramer, A. Doedens, E.A. Theodorakis, R.L. Gallo, N. Hurtado-Ziola, V. Nizet, and R.S. Johnson. 2005. HIF-1alpha expression regulates the bactericidal capacity of phagocytes. The Journal of Clinical Investigation 115: 1806–1815.
Sharma, A.K., L.G. Fernandez, A.S. Awad, I.L. Kron, and V.E. Laubach. 2007. Proinflammatory response of alveolar epithelial cells is enhanced by alveolar macrophage-produced TNF-alpha during pulmonary ischemia-reperfusion injury. American Journal of Physiology. Lung Cellular and Molecular Physiology 293: L105-113.
Acosta-Iborra, B., A. Elorza, I.M. Olazabal, N.B. Martin-Cofreces, S. Martin-Puig, M. Miro, M.J. Calzada, J. Aragones, F. Sanchez-Madrid, and M.O. Landazuri. 2009. Macrophage oxygen sensing modulates antigen presentation and phagocytic functions involving IFN-gamma production through the HIF-1 alpha transcription factor. The Journal of Immunology 182: 3155–3164.
Ortiz-Masia, D., I. Diez, S. Calatayud, C. Hernandez, J. Cosin-Roger, J. Hinojosa, J.V. Esplugues, and M.D. Barrachina. 2012. Induction of CD36 and thrombospondin-1 in macrophages by hypoxia-inducible factor 1 and its relevance in the inflammatory process. PLoS ONE 7: e48535.
Kim, S.Y., Y.J. Choi, S.M. Joung, B.H. Lee, Y.S. Jung, and J.Y. Lee. 2010. Hypoxic stress up-regulates the expression of Toll-like receptor 4 in macrophages via hypoxia-inducible factor. Immunology 129: 516–524.
Polke, M., F. Seiler, P.M. Lepper, A. Kamyschnikow, F. Langer, D. Monz, C. Herr, R. Bals, and C. Beisswenger. 2017. Hypoxia and the hypoxia-regulated transcription factor HIF-1alpha suppress the host defence of airway epithelial cells. Innate Immunity 23: 373–380.
Gil-Marques, M.L., M.E. Pachon-Ibanez, J. Pachon, and Y. Smani. 2018. Effect of hypoxia on the pathogenesis of Acinetobacter baumannii and Pseudomonas aeruginosa in vitro and in murine experimental models of infection. Infection and Immunity 86.
Leone, L., F. Mazzetta, D. Martinelli, S. Valente, M. Alimandi, S. Raffa, and I. Santino. 2016. Klebsiella pneumoniae is able to trigger epithelial-mesenchymal transition process in cultured airway epithelial cells. PLoS ONE 11: e0146365.
Sun, H.L., M.L. Peng, S.S. Lee, C.J. Chen, W.Y. Chen, M.L. Yang, and Y.H. Kuan. 2016. Endotoxin-induced acute lung injury in mice is protected by 5,7-dihydroxy-8-methoxyflavone via inhibition of oxidative stress and HIF-1alpha. Environmental Toxicology 31: 1700–1709.
Xu, M., F. Cao, L. Liu, B. Zhang, Y. Wang, H. Dong, Y. Cui, M. Dong, D. Xu, Y. Liu, P. Zhao, W. Niu, and Z. Li. 2011. Tanshinone IIA-induced attenuation of lung injury in endotoxemic mice is associated with reduction of hypoxia-inducible factor 1alpha expression. American Journal of Respiratory Cell and Molecular Biology 45: 1028–1035.
Wu, G., G. Xu, D.W. Chen, W.X. Gao, J.Q. Xiong, H.Y. Shen, and Y.Q. Gao. 2018. Hypoxia exacerbates inflammatory acute lung injury via the Toll-like receptor 4 signaling pathway. Frontiers in Immunology 9: 1667.
Huang, Y., C. Zhao, J. Chen, and X. Su. 2018. Deficiency of HIF-1alpha in myeloid cells protects Escherichia coli or LPS-induced acute lung injury. QJM 111: 707–714.
Tang, M., Y. Tian, D. Li, J. Lv, Q. Li, C. Kuang, P. Hu, Y. Wang, J. Wang, K. Su, and L. Wei. 2014. TNF-alpha mediated increase of HIF-1alpha inhibits VASP expression, which reduces alveolar-capillary barrier function during acute lung injury (ALI). PLoS ONE 9: e102967.
Tojo, K., N. Tamada, Y. Nagamine, T. Yazawa, S. Ota, and T. Goto. 2018. Enhancement of glycolysis by inhibition of oxygen-sensing prolyl hydroxylases protects alveolar epithelial cells from acute lung injury. The FASEB Journal 32: 2258–2268.
Hu, R., Y. Zhang, X. Yang, J. Yan, Y. Sun, Z. Chen, and H. Jiang. 2015. Isoflurane attenuates LPS-induced acute lung injury by targeting miR-155-HIF1-alpha. Frontiers in Bioscience (Landmark Ed) 20: 139–156.
Chams, N., S. Chams, R. Badran, A. Shams, A. Araji, M. Raad, S. Mukhopadhyay, E. Stroberg, E.J. Duval, L.M. Barton, and I. Hajj Hussein. 2020. COVID-19: A multidisciplinary review. Frontiers in Public Health 8: 383.
Poloznikov, A.A., S.A. Nersisyan, D.M. Hushpulian, E.H. Kazakov, A.G. Tonevitsky, S.V. Kazakov, V.I. Vechorko, S.V. Nikulin, J.A. Makarova, and I.G. Gazaryan. 2020. HIF prolyl hydroxylase inhibitors for COVID-19 treatment: Pros and cons. Frontiers in Pharmacology 11: 621054.
Kuba, K., Y. Imai, S. Rao, H. Gao, F. Guo, B. Guan, Y. Huan, P. Yang, Y. Zhang, W. Deng, L. Bao, B. Zhang, G. Liu, Z. Wang, M. Chappell, Y. Liu, D. Zheng, A. Leibbrandt, T. Wada, A.S. Slutsky, D. Liu, C. Qin, C. Jiang, and J.M. Penninger. 2005. A crucial role of angiotensin converting enzyme 2 (ACE2) in SARS coronavirus-induced lung injury. Nature Medicine 11: 875–879.
Pinto, B.G.G., A.E.R. Oliveira, Y. Singh, L. Jimenez, A.N.A. Goncalves, R.L.T. Ogava, R. Creighton, J.P.S. Peron, and H.I. Nakaya. (2020) ACE2 expression is increased in the lungs of patients with comorbidities associated with severe COVID-19. medRxiv.
Goulter, A.B., M.J. Goddard, J.C. Allen, and K.L. Clark. 2004. ACE2 gene expression is up-regulated in the human failing heart. BMC Medicine 2: 19.
Prieto-Fernandez, E., L. Egia-Mendikute, L. Vila-Vecilla, A. Bosch, A. Barreira-Manrique, S.Y. Lee, A. Garcia-Del Rio, A. Antonana-Vildosola, B. Jimenez-Lasheras, L. Moreno-Cugnon, J. Jimenez-Barbero, E. Berra, J. Ereno-Orbea, and A. Palazon. 2021. Hypoxia reduces cell attachment of SARS-CoV-2 spike protein by modulating the expression of ACE2, neuropilin-1, syndecan-1 and cellular heparan sulfate. Emerging Microbes and Infection 10: 1065–1076.
Ferraro, E., M. Germano, R. Mollace, V. Mollace, and N. Malara. 2021. HIF-1, the Warburg effect, and macrophage/microglia polarization potential role in COVID-19 pathogenesis. Oxidative Medicine and Cellular Longevity 2021: 8841911.
Serebrovska, Z.O., E.Y. Chong, T.V. Serebrovska, L.V. Tumanovska, and L. Xi. 2020. Hypoxia, HIF-1alpha, and COVID-19: From pathogenic factors to potential therapeutic targets. Acta Pharmacologica Sinica 41: 1539–1546.
Tian, M., W. Liu, X. Li, P. Zhao, M.A. Shereen, C. Zhu, S. Huang, S. Liu, X. Yu, M. Yue, P. Pan, W. Wang, Y. Li, X. Chen, K. Wu, Z. Luo, Q. Zhang, and J. Wu. 2021. HIF-1alpha promotes SARS-CoV-2 infection and aggravates inflammatory responses to COVID-19. Signal Transduction and Targeted Therapy 6: 308.
Vohwinkel, C.U., E.J. Coit, N. Burns, H. Elajaili, D. Hernandez-Saavedra, X. Yuan, T. Eckle, E. Nozik, R.M. Tuder, and H.K. Eltzschig. 2021. Targeting alveolar-specific succinate dehydrogenase A attenuates pulmonary inflammation during acute lung injury. The FASEB Journal 35: e21468.
McClendon, J., N.L. Jansing, E.F. Redente, A. Gandjeva, Y. Ito, S.P. Colgan, A. Ahmad, D.W.H. Riches, H.A. Chapman, R.J. Mason, R.M. Tuder, and R.L. Zemans. 2017. Hypoxia-inducible factor 1alpha signaling promotes repair of the alveolar epithelium after acute lung injury. American Journal of Pathology 187: 1772–1786.
Eltzschig, H.K., D.L. Bratton, and S.P. Colgan. 2014. Targeting hypoxia signalling for the treatment of ischaemic and inflammatory diseases. Nature Reviews. Drug Discovery 13: 852–869.
Chan, M.C., J.P. Holt-Martyn, C.J. Schofield, and P.J. Ratcliffe. 2016. Pharmacological targeting of the HIF hydroxylases–a new field in medicine development. Molecular Aspects of Medicine 47–48: 54–75.
Gupta, N., and J.B. Wish. 2017. Hypoxia-inducible factor prolyl hydroxylase inhibitors: A potential new treatment for anemia in patients with CKD. American Journal of Kidney Diseases 69: 815–826.
Esfahani, M., F. Karimi, S. Afshar, S. Niknazar, S. Sohrabi, and R. Najafi. 2015. Prolyl hydroxylase inhibitors act as agents to enhance the efficiency of cell therapy. Expert Opinion on Biological Therapy 15: 1739–1755.
Kim, S.Y., and E.G. Yang. 2015. Recent advances in developing inhibitors for hypoxia-inducible factor prolyl hydroxylases and their therapeutic implications. Molecules 20: 20551–20568.
Maxwell, P.H., and K.U. Eckardt. 2016. HIF prolyl hydroxylase inhibitors for the treatment of renal anaemia and beyond. Nature Reviews. Nephrology 12: 157–168.
Funding
This work was supported by the National Institutes of Health Grant HL102013 to KR.
Ethics declarations
Ethics Approval and Consent to Participate
The review was written following the ethical standards and appropriate guidelines on consent to participate.
Consent for Publication
All authors consent for publication.
Competing Interests
The authors declare no competing interests.
Additional information
Publisher's Note
Springer Nature remains neutral with regard to jurisdictional claims in published maps and institutional affiliations.
Rights and permissions
Springer Nature or its licensor (e.g. a society or other partner) holds exclusive rights to this article under a publishing agreement with the author(s) or other rightsholder(s); author self-archiving of the accepted manuscript version of this article is solely governed by the terms of such publishing agreement and applicable law.
About this article
Cite this article
Suresh, M.V., Balijepalli, S., Solanki, S. et al. Hypoxia-Inducible Factor 1α and Its Role in Lung Injury: Adaptive or Maladaptive. Inflammation 46, 491–508 (2023). https://doi.org/10.1007/s10753-022-01769-z
Received:
Revised:
Accepted:
Published:
Issue Date:
DOI: https://doi.org/10.1007/s10753-022-01769-z