Abstract
Alzheimer’s disease (AD) and traumatic brain injury (TBI) are major public health issues worldwide, with over 38 million people living with AD and approximately 48 million people (27–69 million) experiencing TBI annually. Neurodegenerative conditions are characterised by the accumulation of neurotoxic amyloid beta (Aβ) and microtubule-associated protein Tau (Tau) with current treatments focused on managing symptoms rather than addressing the underlying cause. Heparan sulfate proteoglycans (HSPGs) are a diverse family of macromolecules that interact with various proteins and ligands and promote neurogenesis, a process where new neural cells are formed from stem cells. The syndecan (SDC) and glypican (GPC) HSPGs have been implicated in AD pathogenesis, acting as drivers of disease, as well as potential therapeutic targets. Human mesenchymal stem cells (hMSCs) provide an attractive therapeutic option for studying and potentially treating neurodegenerative diseases due to their relative ease of isolation and subsequent extensive in vitro expansive potential. Understanding how HSPGs regulate protein aggregation, a key feature of neurodegenerative disorders, is essential to unravelling the underlying disease processes of AD and TBI, as well as any link between these two neurological disorders. Further research may validate HSPG, specifically SDCs or GPCs, use as neurodegenerative disease targets, either via driving hMSC stem cell therapy or direct targeting.
Graphical Abstract
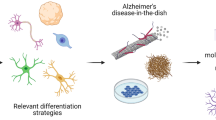
Graphical abstract: Heparan sulfate proteoglycans as regulators of human mesenchymal stem cell neurogenesis. Traumatic brain injury (TBI) and genetic factors increase Alzheimer’s disease (AD) risk (yellow). Potential AD treatment targets (green) include human mesenchymal stem cells (hMSCs). Manipulating pathway and growth factor interactions with heparan sulfate proteoglycans (HSPGs) could regulate hMSC neurogenesis, potentially offering functional neural stem cell transplants as AD treatments

Similar content being viewed by others
Avoid common mistakes on your manuscript.
Alzheimer’s Disease and Traumatic Brain Injury: Neurodegenerative Diseases with No Cure
In 2022, over 38 million people were estimated to be living with Alzheimer’s disease (AD) worldwide (World Health Organization 2023). In addition, between 27 and 69 million people experience a traumatic brain injury (TBI) annually, significantly increasing their risk of developing AD (Dewan et al. 2018). The accumulation of amyloid beta (Aβ) and microtubule-associated protein Tau (Tau) has been linked to both AD and TBI disease models (Golde et al. 2010; Ramos-Cejudo et al. 2018). Current treatment options unsuccessfully target the symptoms of these neurodegenerative diseases and without a treatment the healthcare burden continues to amplify in aging populations worldwide.
AD is characterised by progressive cognitive decline in language, visuospatial and executive function, as well as personality and behavioural changes (Naasan et al. 2021; Weller and Budson 2018). TBI is a heterogeneous condition characterised by similar symptoms, with disease presentation dependant on the injury and its location (McKee and Daneshvar 2015; Najem et al. 2018) The neural and structural damage seen in AD and TBI can affect people of all ages (Dams-O’Connor et al. 2016) with AD and TBI patients demonstrating significant cognitive decline secondary to neuronal death. The application of stem cell transplants to induce repair processes, such as neurogenesis, have the potential to provide improved treatment options for these neurodegenerative disorders (Jullienne et al. 2014; Reiss et al. 2018). Under specific culture conditions and with the use of appropriate growth factors, human mesenchymal stem cells (hMSCs) can be induced to undergo neural differentiation. A deeper understanding underlying the biological processes guiding hMSC differentiation are needed to progress stem cell therapy and their application to neurological repair.
Heparan Sulfate Proteoglycans
Heparan sulfate proteoglycans (HSPGs) are a diverse family of macromolecules, decorated with multiple glycosaminoglycan (GAG) chains (Okolicsanyi et al. 2014a). These heterogeneous side chains are characterised by specific sulfation patterns, which enable HSPGs to interact with various protein families and ligands, including growth factors, enzymes, lipases and extracellular matrix (ECM) components (Knelson et al. 2014). As most of the current understanding of HSPGS stems from murine models, further investigating neurogenesis from human stem cells and the involvement of HSPGs is essential to advance neural stem cell therapies (Oikari et al. 2014). Two major HSPG families include the four transmembrane syndecans (SDC1-4) and six via Glycosylphosphatidylinositol (GPI)-anchored glypicans (GPC1-6) (Leonova and Galzitskaya 2013; Oikari et al. 2020; Tkachenko et al. 2005). In addition, secreted ECM HSPGs include perlecan, agrin and type XVIII collagen (Sarrazin et al. 2011; Ughy et al. 2019). SDCs have been reported to mediate angiogenesis, tumourigenesis and embryonic growth, while GPCs mediate signalling activity (Okolicsanyi et al. 2015). In particular, syndecan-3 (SDC3) and glypican-1 (GPC1) have been linked to key features of neurodegenerative disorders—increased intracellular Aβ accumulation and to alteration of amyloid beta precursor protein (APP) gene function (Letoha et al. 2019; O’Callaghan et al. 2008; Snow et al. 1994). SDC1 controls hMSC lineage determination in an osteogenic model (Yu et al. 2020) and GPC1 and GPC4 core proteins have been linked to neural lineage commitment in human NSC experiments (Oikari et al. 2016; Yu et al. 2017). While the role of HSPGs in various cellular processes has been extensively investigated, their specific involvement in neural differentiation and neurogenesis of hMSCs remains poorly understood.
Heparan Sulfate Biosynthesis
Complex temporal biosynthesis within the Golgi apparatus determines the final nature of GAG chains, specifying them as heparan sulfate (HS), dermatan sulfate (DS), keratan sulfate (KS) or chondroitin sulfate (CS) (Christianson and Belting 2014; Couchman et al. 2015). HS consists of N-acetyl glucosamine (GlcNAc) and glucuronic acid (GlcA) repeats that are polymerised by the exostosin (EXT) enzymes EXT1 and EXT2 (Annaval et al. 2020; Okolicsanyi et al. 2018). C5-epimerase enzyme action improves HS flexibility and protein ligand recognition, enabling protein binding and polymer function (Debarnot et al. 2019; Qin et al. 2015). This process is followed by N-sulfation of HS by N-Deacetylase/N-Sulfotransferase (NDSTs), specifying the chains as HS GAGs (Okolicsanyi et al. 2014a). When the NDSTs are active, a HS chain is formed, however, as with all GAGs, the biosynthesis of HS starts with Exostosin-like 3 (EXTL3), which adds an N-acetylglucosamine residue (GlcNAc) to the glucuronic acid (GlcA) residue onto a tetrasaccharide linker (Okolicsanyi et al. 2014b; McMillan et al. 2023). N-sulfation introduced by NDSTs only occurs as part of HS chain formation and is absent in chondroitin sulfate (CS), dermatan sulfate (DS) and keratan sulfate (KS) chains (Aikawa and Esko 1999; Pikas et al. 2000). The final length and sulfation pattern of GAG chains elicit various functions, including regulation of cellular behaviour, migration and differentiation (Okolicsanyi et al. 2014b). HS side chains stimulate these cellular processes via binding to a wide variety of protein ligands, such as cytokines, enzymes, growth factors and protein structures within the ECM (Sugahara and Kitagawa 2002).
SDCs and GPCs as Targets for Neurodegenerative Disease Research
The SDCs and GPCs are crucial for mediating cellular functions, including neurogenesis; however, the exact functional mechanisms of these interactions have not yet been fully elucidated. The transmembrane SDCs carry either a HS or both HS and CS chains and consist of an ectodomain at their N-terminal, along with a transmembrane domain and a cytoplasmic domain at their C-terminal (Hudák et al. 2021; Lopes et al. 2006; Xian et al. 2010). Each SDC has distinct expression patterns and functions in their respective tissues. SDC1 expression is mainly found within epithelial and mesenchymal cells, SDC2 in mesenchymal, neuronal and epithelial cells, SDC3 in neuronal and musculoskeletal cells and SDC4 expressed in most tissues (Lambaerts et al. 2009; Tkachenko et al. 2005). SDCs can function as receptors and co-receptors for ECM components and interact with growth factors and other ligands to regulate downstream signalling pathways, regulating cellular behaviours (Xian et al. 2010). Specifically, SDCs have been shown to interact with a variety of growth factor signalling pathways, including the Wnt and fibroblast growth factor (FGF) pathways (Dong et al. 2021; Sakane et al. 2012; Sarrazin et al. 2011).
In contrast, GPCs are covalently linked to the cell surface via GPI anchors and are characterised by their 14 cysteine residues near their N-terminus or central domain of the core protein (Awad et al. 2015; De Cat and David 2001; Dong et al. 2021). The cysteine residues may form disulfide bonds intramolecularly, accounting for their globular tertiary structure (De Cat and David 2001; Fico et al. 2011). The GPCs are expressed in various tissue types primarily during development, functioning though interactions with Wnt and FGF signalling pathways (Sarrazin et al. 2011; Wang et al. 2019). GPC1 is expressed in the central nervous system (CNS) in differentiated neurons, while GPC2 is expressed in developing neuronal cells (Lugert et al. 2017; Shi et al. 2021). GPC3 has been found to be ubiquitous during development in cells other than the CNS and GPC4 localised to the kidneys, adrenal tissue and neural precursor cells (Sakane et al. 2012). Low levels of GPC5 expression have been identified in various tissues, including the brain, heart and lungs with GPC5 reported to mediate cell proliferation and migration (Li et al. 2018; Yuan et al. 2016). GPC5 has also been shown to interact with various growth factors and signalling molecules, including Wnt and fibroblast growth factor 2, to modulate their activity (Li et al. 2018; Tkachenko et al. 2005; Yuan et al. 2016). Increased expression of GPC5 has also been correlated with poor prognosis in some cancer types (Li et al. 2018; Yuan et al. 2016). GPC6 has been suggested to be important in neural development and plasticity and to interact with various signalling molecules to modulate their activity (Kamimura and Maeda 2021; Tkachenko et al. 2005). In particular, GPC6 has been shown to bind FGF2 to enhance its signalling, promote neurite outgrowth and neural stem cell differentiation (Filmus et al. 2008; Tkachenko et al. 2005). Investigating SDCs and GPCs in their diverse expression patterns and various tissue types, as well as their interactions with signalling pathways (Wnt, FGF) that regulate neurogenesis will further our understanding of normal and pathological processes. Specifically, the interactions between these pathways and relevant HSPGs, such as “neuronal” SDC3 and GPC1, expressed in differentiated neurons, holds potential for deeper insight into understanding the complex mechanisms regulating human neurogenesis.
Alzheimer’s Disease Aetiology
The aetiology of AD is complex and remains poorly understood; however, genetic, environmental and lifestyle factors have all been identified to influence AD risk (Breijyeh and Karaman 2020). AD pathogenesis is characterised by the extensive formation of Aβ plaques, neurofibrillary tangles (NFTs) resulting from Tau and hyperphosphorylated Tau (p-Tau) aggregates and vascular amyloid angiopathy (Ramos-Cejudo et al. 2018; Reiss et al. 2018; Solis et al. 2020). These pathogenetic features result in neural cell death and subsequent disease presentation, with stem cell therapy actively pursued as a potential treatment option including via stimulation of neurogenesis. Aβ plaques, p-Tau, total Tau protein and NFTs have long been considered hallmark pathological features of AD development (Horie et al. 2020; Rajmohan and Reddy 2017). In addition, AD disease phenotypes have been linked to neuropil threads, dystrophic neurites, astrogliosis, microglial activation as well as cerebral amyloid angiopathy (Lane et al. 2018). The pathogenesis of AD involves the complex interplay between protein aggregation, cell surface proteins and their receptors. HSPGs, namely SDC and GPC, the focus of this review, have been implicated in various processes driving neurodegeneration as detailed below. Unravelling the processes permissive of AD aetiology, along with the associated signalling pathways and potential HSPG involvement may allow for improved understanding of how these factors may be targeted to slow down or treat neurodegeneration.
APP Processing and Amyloid Beta Accumulation
While AD is widely considered to be polygenically influenced (Williamson et al. 2009), the impaired cleavage of amyloid precursor protein (APP) is currently thought to be the major pathogenic event in the development of the disease (Huse et al. 2002). APP is encoded by the similarly named APP gene (O’Brien and Wong 2011), that is ubiquitous in the central nervous system (CNS) and is proteolysed intracellularly (Muller and Zheng 2012; O’Brien and Wong 2011). Impaired cleavage by γ-secretase at the C-terminus of APP produces Aβ fragments, which are internalised and then can accumulate and become neurotoxic (Fig. 1) (Gu and Guo 2013; O’Brien and Wong 2011). Recent evidence suggests that SDCs may contribute to the internalisation of Aβ peptides, however, the mechanism and degree of impact remain unknown (Ozsan McMillan et al. 2023). SDC3 and SDC4 were shown to exhibit enhanced uptake of Aβ1–42 in SH-SY5Y cell models (Letoha et al. 2019).
Impaired amyloid precursor protein (APP) cleavage and the resulting formation of amyloid beta (Aβ) oligomers and senile plaques in Alzheimer’s disease (AD). The major pathogenic event in AD is the impaired cleavage of APP by γ-secretase, which leads to the aggregation of Aβ fragments. The impaired cleavage of APP by γ-secretase results in the formation of Aβ peptides, which are internalised and then aggregate to form senile Aβ plaques. The syndecan (SDC) heparan sulfate proteoglycans (HSPGs) are present on the cell membrane and extracellular matrix, and their full mediation of Aβ internalisation remains elusive. SDC3 and SDC4 increase the internalisation of Aβ via attachment to heparan sulfate (HS) chains, with potential contribution to AD pathogenesis. The presence of these neurotoxic aggregates results in the shrinkage of key brain regions, including the cerebral cortex, which is responsible for language, memory, decision making, and personality, and the hippocampus, which is responsible for learning and memory
As such, AD is characterised by the pathological intracellular accumulation of Aβ fragments (Abu Hamdeh et al. 2018). Additionally, extracellular Aβ aggregates can induce hyperphosphorylation of Tau, increasing NFT aggregation (Bettens et al. 2010). The primary constituents of these senile plaques include the insoluble aggregates of the 4-kDa Aβ peptides, Aβ40 and Aβ42, generated by sequential proteolytic processing of APP by β-site APP cleaving enzyme 1 (BACE1) and γ-secretase (O’Brien and Wong 2011; Picone et al. 2020). While Aβ40 is the most abundant Aβ peptide in the cerebrospinal fluid (CSF), the slightly longer and less abundant Aβ42 has been implicated as the key pathogenic species in AD brain (Baldeiras et al. 2018; Gu and Guo 2013). Aβ42 is a major component of amyloid plaques in the AD brain, however Aβ40 has only been detected in trivial amounts (Ferrari and Sorbi 2021). The Aβ42/Aβ40 ratio is considered to be indicative of AD severity and progression, with increased ratios representative of higher neurotoxicity and Tau pathology via induction of Aβ fibril formation (Kumar-Singh et al. 2006; Kuperstein et al. 2010). Several studies have also found that the two isoforms influence aggregation rates and toxicity of each other (Kuperstein et al. 2010; Pauwels et al. 2012; Snyder et al. 1994). Additionally, Aβ42 binding may be preferential in the ECM or cell membrane, leading to increased concentrations (Banerjee et al. 2020; Chen et al. 2017). A recent study found that the structural variability of Aβ42 and Aβ40 fibrils may also affect the phenotypical and clinical differences observed in AD (Banerjee et al. 2020; Chen et al. 2017; Qiang et al. 2017). These differences also may, however, be due to genetic and environmental differences as well as fibril structure (Qiang et al. 2017). Mouse models have demonstrated that HS GAG chains colocalise with Aβ in AD patient brains and interact with Aβ and amyloid fibrils; however, the mechanisms underlying this interaction remains elusive (van Horssen et al. 2003; Zhang et al. 2014). One hypothesis suggests that the HS GAG side chains may allow HSPGs to act as chaperones, protecting Aβ from proteolytic degradation, potentially hindering the clearance of Aβ (Gupta-Bansal et al. 1995; Snow et al. 1994). Furthermore, early studies have identified global expression of HSPGs in human tissue NFTs via immunostaining (Snow et al. 1988; Su et al. 1992), with SDC1-3 and GPC1 core proteins detected in amyloid plaques (van Horssen et al. 2002a, b; Verbeek et al. 1999). Additionally, elevated levels of SDC3, SDC4, GPC1 and GPC3 have also been observed in AD patient brain tissues (Liu et al. 2016). Identification of the intricate roles of SDCs and GPCs in amyloid accumulation and AD will aid in understanding specific disease targets to slow down neurodegeneration. For example, downregulation of key SDCs and GPCs driving amyloid fibrillisation may reduce the build-up of amyloid plaques, thus slowing down disease progression; however, further research is essential to validate this. Recent rodent studies revealed that reducing HS in these brain models improved Aβ clearance and reduced fibril formation (Jen et al. 2009; Poon et al. 2020); however, little has been uncovered regarding HSPG-Aβ interactions in the human brain. This suggests that elucidating the role of HSPGs in HSPG-Aβ interactions may improve our understanding of factors driving neurodegeneration via Aβ accumulation due to impaired clearance. This in turn would enhance the molecular profiles of AD and TBI and provide the foundation for more detailed exploration of HS and HSPGs as molecular targets for use in stem cell and other treatment options.
Tau and Neurofibrillary Tangles (NFTs)
In a healthy brain, Tau contributes to microtubular stability and regulation of intracellular trafficking (Congdon and Sigurdsson 2018). Tau pathology in AD begins in the entorhinal cortex and spreads to the hippocampus and other regions of the brain (Lane et al. 2018; Serrano-Pozo et al. 2011). Typically, Tau pathology spares the primary areas controlling sensory, motor and visual functions (DeTure and Dickson 2019; Lane et al. 2018). p-Tau then form the neuropathological feature of AD—aggregating NFTs (Fig. 2) (Metaxas and Kempf 2016).
The role of Tau protein in a healthy brain and its pathological accumulation in Alzheimer’s disease (AD). In a healthy brain, Tau protein serves a critical function in maintaining the stability of microtubules, which are abundant in neurons and present in both axons and dendrites. In an AD brain, hyperphosphorylated Tau protein accumulates and forms neurofibrillary tangles (NFTs). The exact mechanism of NFT formation is unknown, but NFTs cause disintegration in microtubules resulting in a diseased neuronal state
How NFTs are formed is yet to be determined; however, both intracellular and extracellular NFTs have been found to contain HSPGs (Siedlak et al. 1991). The accumulation of p-Tau is a hallmark of the AD hippocampal-sparing subtype, with this accumulation also observed in other subtypes of AD, including typical AD and limbic-predominant AD (Ferreira et al. 2020; Mohanty et al. 2022; Risacher et al. 2017). Improving our understanding of the Aβ and Tau proteins and their interaction with HSPGs in their accumulation into the plaques associated with AD and TBI could improve diagnostics and treatments for these patients.
SDCs and GPCs in Alzheimer’s Disease
SDCs and GPCs have been implicated in AD and TBI pathogenesis. As discussed above, the SDC1-3 and GPC1 core proteins detected in amyloid plaques characteristic of AD pathogenesis (van Horssen et al. 2002a, b; Verbeek et al. 1999). Additionally, SDC3, which is highly expressed in neuronal cells, has been shown to increase Aβ aggregation in double mutant transgenic mouse models with both an APP and MAPT mutation (APPSwe-Tau) (Hudák et al. 2022). Elevated SDC3 expression was also recently reported in neurons and glia of AD patients, suggesting that some HSPGs may be produced in response to Aβ accumulation (Lorente-Gea et al. 2020). The effects of SDC3 have also been studied in rodent models, with SDC3 deficiency resulting in memory and learning difficulties, symptoms known in both AD and TBI (Lambaerts et al. 2009). In the CNS and during axon guidance, SDC3 has been found to facilitate extracellular Aβ attachment and Aβ fibrillation in SH-SY5Y neuroblastoma cell models (Condomitti and de Wit 2018; Letoha et al. 2019). In addition, increased SDC3 and SDC4 expression has been found in post-mortem human AD brains (Grothe et al. 2018; Hudák et al. 2021) and SDC2 and GPC1 to act as Aβ receptors (Jarosz-Griffiths et al. 2016; Letoha et al. 2019; Reinhard et al. 2013). HS-Aβ interactions at these receptor sites contribute to various stages of pathogenesis in AD, including the production, clearance, accumulation, aggregation and toxicity of Aβ (Cui et al. 2013; Liu et al. 2016; Reinhard et al. 2013). Recently, it was suggested that SDC1 expression may provide an indication of the severity of TBI, with higher expression correlating with poorer outcomes in severely injured patients (Gonzalez Rodriguez et al. 2018; Xie et al. 2024). Impaired neurogenesis is one of the first pathological signs of AD, making the SDC HSPG core proteins important subjects of current AD research (Disouky and Lazarov 2021; Zhang et al. 2014).
The core protein and the HS chains decorating GPC1 have been found to be crucial for brain function, with reduced GPC1 gene expression resulting in decreased brain size by up to 30% along with increased Aβ accumulation in mouse models (Jen et al. 2009; Ohmi et al. 2011). Membrane-bound interactions between the GPC1 and Aβ proteins have also been documented in vivo, with Aβ bound by GPC1 potentially facilitated by HS GAGs (Cheng et al. 2013; Reinhard et al. 2013). Additionally, while no direct evidence demonstrates a specific role of GPCs in TBI, a cryoinjury mouse model of TBI has suggested increased GPC1 expression following TBI in the injured mouse brain tissue by in situ hybridisation (Hagino et al. 2003). Recently, the regulatory roles of GPC1 and GPC4 have been confirmed in human neural differentiation (Oikari et al. 2020). The expression of these HSPGs is necessary for neuronal differentiation in human neural stem cells (NSCs) and was found to have altered expression when cultures were augmented with brain-derived neurotrophic factor (BDNF) and platelet-derived growth factor (PDGF), suggesting that GPCs may be novel neuronal lineage markers (Oikari et al. 2020). Elucidating the specific roles of the SDC and GPC core proteins in AD pathogenesis will likely help identify how these ubiquitous proteins within the extracellular microenvironment may be targeted, for example, in conjunction with amyloid clearing therapies.
Other HSPGs and HS Related Genes in Alzheimer’s Disease
The focus of this review is primarily the SDCs and GPCs, however, to more broadly understand HSPG involvement in AD, it is essential to examine how secreted HSPGs may also contribute to AD pathogenesis. As an example, perlecan has been shown to accumulate in the fibrillar Aβ found in human AD patient brains (Perl 2010; van Horssen et al. 2003). The binding of perlecan to predominant isoforms of Aβ may accelerate Aβ fibril formation to stabilise the fibrils, contributing to AD pathogenesis (van Horssen et al. 2003; Lavorgna et al. 2023). In addition, earlier studies indicated that the secreted HSPG agrin may enable organisation of amyloid plaques as well as increase the immunoreactivity observed in AD (Berzin et al. 2000). Type XVIII collagen has also been associated with amyloid deposits and plaques characteristic of AD (Salza et al. 2015; van Horssen et al. 2002a, b). As such, secreted HSPGs likely pose an interesting avenue of research into neurodegenerative diseases such as AD.
HS biosynthesis enzymes have also been identified as contributors to AD pathogenesis. Recent mouse models have identified 3-O-sulfotransferase isoform 1 (3-OST-1), encoded by the Heparan Sulfate-Glucosamine 3-Sulfotransferase 1 (HS3ST1) gene, in Tau cellular uptake via generation of specific 3-O-sulfation sites on HS chains (Wang et al. 2023). Wang et al. (2023) suggest overexpression of the HS3ST1 gene, a member of the HS biosynthetic enzyme family, may enhance Tau pathology spread, presenting a novel therapeutic target for AD (Wang et al. 2023). More recently, several genes involved in HS biosynthesis, including EXT1 and Sulfatase 2 (SULF2), were found to be downregulated in AD mouse models. In contrast, in this same model, several late-stage HS biosynthesis genes, including HS3STs and Sulfatase 1 (SULF1) were shown to be upregulated (McMillan et al. 2023). The extracellular sulfatases SULF1 and SULF2, encoded by SULF1 and SULF2, respectively, were also investigated with findings suggesting the HS moieties binding to Aβ contained 6-O-sulfation, further highlighting the involvement of HSPGs and HS biosynthesis in AD (McMillan et al. 2023).
In 1989 it was proposed by Snow and Wight that HSPGs were central to the initiation of AD pathogenesis, with subsequent research further validating this initial hypothesis (Snow et al. 2021). In 2021, Snow et al. proposed a new HSPG-AD hypothesis, where increased HSPGs, GAGs and HS sulfation as well as HS degradation in neural cells occur due to a myriad of factors that all contribute to AD pathogenesis. Similarly, the hypothesis posits that increased HS levels accelerate neurodegeneration in AD via increased Aβ and Tau protein aggregation, as well as Aβ plaque formation and hinderance of Aβ fibril and Tau tangle clearance (Liu et al. 2016; Snow et al. 2021). Extensive research into this hypothesis continues, however, the specific interactions between HSPGs and key stages of AD pathogenesis are yet to be fully elucidated.
As such, with HSPGs and HS biosynthesis genes and proteins implicated in the pathogenesis of AD, it is likely that SDCs and GPCS are not the only contributors to AD, although they are the primary focus of this review. Understanding the interactions between HSPG-related genes, including the SDCs and GPCs, Aβ accumulation, Tau pathology and other features of neural lineage specification may facilitate the development of a molecular profile of AD and TBI to identify key signalling events of early diagnosis along with more targeted therapies.
Alzheimer’s Disease Risk Genes
AD is typically classified into two subtypes, familial AD (FAD) and sporadic AD (SAD), where FAD is most often early onset (< 65 years) and SAD is late onset (> 65 years) (Lista et al. 2015). Mutations in the APP, presenilin-1 (PSEN1) and presenilin-2 (PSEN2) genes have been identified to be causative in AD, particularly FAD, while apolipoprotein E (APOE) and microtubule-associated protein Tau (MAPT) genes are thought to increase the risk of late onset AD (Lanoiselee et al. 2017). These AD risk genes and their products each have specific connections to HS and HSPGs, as briefly discussed below.
The second most common AD-related gene, the APP gene, located on chromosome 21, encodes for APP, a member of a protein family including the amyloid precursor-like proteins (APLP1 and APLP2) (Lanoiselee et al. 2017; O’Brien and Wong 2011). APP overexpression improves cellular health and growth (O’Brien and Wong 2011) with alternate splicing of APP thought to escalate Aβ accumulation and increase the risk of AD development (O’Brien and Wong 2011; Xiao et al. 2021). Soluble APP (sAPP) interacts with cell surface HSPGs, namely SDC2 and GPC1, with overexpression of these HSPG core proteins shown to have a higher affinity for the sAPP receptor in rodent models (Reinhard et al. 2013). The specific interactions between APP and HSPGs need to be further studied to fully understand the extent of SDC and GPC involvement as well as the HS GAG chains affiliated with these proteins.
The APOE gene, located on chromosome 19, encodes for Apolipoprotein E (ApoE) and is currently classified as the biggest risk factor in SAD development (Lane et al. 2018; Liu et al. 2013). Within the CNS, ApoE has the vital function of lipid distribution (Frieden et al. 2017). The most studied APOE variants refer to the variation of amino acids at positions 112 and 158 (Frieden et al. 2017; Liu et al. 2013; Marais 2019) and include ApoE2 (protective), ApoE3 (common allele) and ApoE4 (risk). The ApoE2 variant has been found to be beneficial for neurological and cardiovascular health, while the ApoE4 variant is associated with higher risk of AD development (Liu et al. 2013; Marais 2019). Additionally, several studies have also shown a link between the presence of the ApoE4 allele and poorer outcomes for TBI patients (Diaz-Arrastia et al. 2003; McFadyen et al. 2021; Teasdale et al. 1997). Interactions between ApoE and HSPGs, specifically SDC3, have been linked to increased Aβ uptake and aggregation (Hudák et al. 2021). Additionally, overexpression of GPC4 was found in ApoE4 carrier patient post-mortem brain, with ApoE4 surface trafficking via GPC4 gateways suggested to increase Tauopathy (Saroja et al. 2022).
The MAPT gene, located on chromosome 17, encodes the Tau protein, which, when hyperphosphorylated, leads to fibrillation and aggregation of NFTs (Caillet-Boudin et al. 2015; Strang et al. 2019). Up to 50 mutations in the MAPT gene have to date been demonstrated to increase the risk of select Tauopathies, a term used to describe a group of neurodegenerative disorders characterised by Tau protein accumulation in the brain, which includes AD (Strang et al. 2019). Presence of 3-O- and 6-O-sulfation have also been implicated in HS-mediated Tau protein internalisation and phosphorylation (Rauch et al. 2018; Sepulveda-Diaz et al. 2015). While in vitro evidence suggests HS and its sulfation patterns contribute to Tau aggregation, the extent of HSPG interactions in vivo remains unclear (Mah et al. 2021).
Mutations in the PSEN1 gene, located on chromosome 14, encodes the presenilin-1 (PS1) protein, and have been found to be the main causative mutations in FAD with PSEN1 considered the most common AD-related gene in this disorder (Kelleher and Shen 2017; Lanoiselee et al. 2017). PSEN2, located on chromosome 1 (Kumar-Singh et al. 2006), encodes the presenilin-2 (PS2) protein (Kabir et al. 2020; Lanoiselee et al. 2017). Both PS1 and PS2 catalyse the cleavage of APP and production of Aβ (Lanoiselee et al. 2017; Xiao et al. 2021). Mutations in these genes also have the potential to initiate greater production of toxic Aβ42 fragments, contributing to AD pathogenesis (Kabir et al. 2020; Kelleher and Shen 2017). Interestingly, SDC3 is a known substrate for the PS/γ-secretase complex (Schulz et al. 2003), however, little is known about the interactions between the PSENs and HSPGs.
Similar to the PSENs, few interactions between HSPGs and A disintegrin and metalloprotease10 (ADAM10) encoded by the similarly named ADAM10 gene, have been identified. ADAM10 is a key enzyme in the non-amyloidogenic pathway of APP processing and may be another AD therapeutic target (Khezri et al. 2023). Elevated BACE1 activity and decreased ADAM10 expression in late onset AD, is thought to contribute to increased Aβ production and neurodegeneration (Suh et al. 2013). Understanding the interactions between these high-risk genes and any connections with HSPGs, identified as contributors to AD risk such as SDC3 and GPC4, will improve our knowledge of drivers in AD and other neurodegenerative diseases.
Traumatic Brain Injury Increases Risk of Alzheimer’s Disease
TBI is a complex injury caused by major head trauma, such as gunshot wound and motor vehicle accidents (Dams-O’Connor et al. 2016; Ramos-Cejudo et al. 2018). TBI is characterised by vascular dysfunction and hypoxia with consequent ischemia and individuals with brain trauma are likely to experience delayed cognitive decline years after injury (Ramos-Cejudo et al. 2018). The extent of cellular damage and repair processes following a TBI remain elusive due to the diverse array of type and location of TBIs. However, the injury is known to trigger Aβ-genesis and plaque accumulation, and subsequent neurodegeneration may exhibit similar characteristics to those of AD (Abu Hamdeh et al. 2018; O’Callaghan et al. 2008; Veitch et al. 2013).
Amyloid Beta and Tau
Diffuse axonal injury (DAI) accounts for approximately 70% of TBI cases (Ng and Lee 2019). Patients with DAI have elevated Aβ levels compared to non-DAI injuries (Marklund et al. 2009). Aβ plaques similar to those found in early-stage AD patient brains have been found in approximately 30% of patients of all ages who die suddenly due to TBI (Johnson et al. 2010b). Interestingly, these plaques have also been found in surviving TBI patients (DeKosky et al. 2007). Aβ deposits similar to those seen in AD may occur within hours of TBI with dense plaque formation reported in rare cases (Ikonomovic et al. 2004; Johnson et al. 2010a; Smith et al. 2013). Similar to Aβ plaque formation in TBI, Tau aggregation occurs within days or even hours after the injury is sustained (Edwards et al. 2020). A demonstrated link between Tau aggregates and TBI was found with one third of surviving moderate to severe TBI patients identified to have post-mortem NFT aggregates (Johnson et al. 2012). Mouse models have been used to demonstrate AD-like tauopathies in TBI-induced conditions, supporting a clear link between AD and TBI (Edwards et al. 2020). Mouse models continue to be used as a basis for human models of Aβ and Tau features in AD and TBI. However, utilising human stem cells has the potential to more accurately model the events leading to these neurodegenerative diseases.
Current Diagnosis and Treatment of AD and TBI
There are currently no effective early diagnostic or treatment options for AD, with diagnosis only occurring once symptoms are established (Tarawneh and Holtzman 2012; Teipel et al. 2022). Current definitive AD diagnosis requires post-mortem brain tissue biopsy and evaluation (Weller and Budson 2018). Diagnosis for living patients is slowly developing and improving in accuracy, via the combination of CSF and positron emission tomography (PET) biomarkers in conjunction with clinical criteria including cognitive function and memory decline (Teipel et al. 2022; Weller and Budson 2018). Currently, CSF can be tested for Aβ42, total Tau and p-Tau protein with up to 90% diagnostic accuracy (Tariciotti et al. 2018; Weller and Budson 2018).
Meanwhile, TBI is assessed and diagnosed with relative accuracy using neurological medical assessment tools, such as the Glasgow Coma Scale (GCS), as well as imaging tools such as computerised tomography (CT) and magnetic resonance imaging (MRI) (Galgano et al. 2017). The severity of injury is challenging to determine and the long-term implications even harder to predict with difficulty in simultaneously targeting multiple aspects of the disease with a single therapeutic approach (Herrmann et al. 2022; Lyu et al. 2022). The development of diagnostic techniques via cellular and genomic research to investigate early symptoms, risk factors or underlying pathology of both AD and TBI may provide opportunities for earlier and more targeted treatment options. Insight into the initiation events of neurodegeneration at the earliest stages, will provide avenues for direct intervention, potentially preventing or slowing down disease progression. This in turn may contribute to more positive patient outcomes.
Wnt Signalling in hMSCs
The SDC and GPC HSPGs regulate several cellular signalling pathways, which in turn regulate neural lineage specification (Okolicsanyi et al. 2014b; Ornitz and Itoh 2015). Specifically, the Wnt pathway has documented interactions with HSPGs and influences neural regeneration (Colombres et al. 2008; Oikari et al. 2016). The structure of the HS chain determines its ligand binding activity and other functions of these proteoglycans (Sarrazin et al. 2011). As identified earlier, heparin binding ligands include the Wnt and FGF growth factor families, as well as BDNF and PDGF (Ling et al. 2009).
Wnt signalling pathways are a group of conserved signalling pathways regulating cellular development and in adult stem cells, including proliferation, apoptosis, migration and polarity (Ai et al. 2003; Palomer et al. 2019; Sethi and Vidal-Puig 2010). The Wnt pathways are broadly classified into the canonical and non-canonical pathways (Ackers and Malgor 2018; Liu et al. 2022). Wnt signalling, activated through Wnt and FGF protein interactions with structurally diverse HSPGs, is crucial during neurogenesis and neural development (Ai et al. 2003; Pulsipher et al. 2015). Dysregulation of this signalling has been linked to cerebral synaptic decline in memory loss, dementias and other neurological disorders such as Parkinson’s disease (Berwick and Harvey 2012; Palomer et al. 2019).
The cysteine rich glycol-lipoprotein Wnt proteins function by binding to the Frizzled (FZD) family of receptors and low-density lipoprotein receptor-related protein 5 or 6 (LRP5/6) co-receptors (Boland et al. 2004; Ren et al. 2021). Stabilisation and accumulation of β-catenin occurs followed by its translocation to the nucleus to activate transcription of target genes (Hua et al. 2018; Ren et al. 2021). Canonical Wnt/β-catenin signalling has been suggested to regulate hMSC proliferation with Wnt expression levels influenced by cell density and lineage commitment of hMSCs (Alfaro et al. 2011). Wnt signalling has also been reported to regulate hMSC self-renewal and stem cell lineage differentiation potential (Ai et al. 2003; Ling et al. 2009; Xu et al. 2016). Specifically, Wnt signalling activation inhibits differentiation of hMSCs toward osteogenic and adipogenic lineages, while activation of the pathway has been linked to neuronal differentiation in hMSCs (Liu et al. 2009; Tsai et al. 2014). Interestingly, downregulation of Wnt signalling (Wnt ligands WNT2B, WNT6 and WNT7a and FZD receptors FZD2 and FZD3) has been observed in the aging brain (Folke et al. 2019). This may increase synapse vulnerability characteristic of AD pathogenesis, with potential indirect effects influencing Aβ aggregation (Liu et al. 2014; Palomer et al. 2019).
The non-canonical Wnt pathway is activated by Wnt ligands binding to FZD receptors and other co-receptors, such as Ror2 and Ryk (Ackers and Malgor 2018). This leads to the activation of several signalling pathways, including the planar cell polarity pathway, the Wnt/Ca2 + pathway and the Wnt/β-catenin-independent pathway (Komiya and Habas 2008). Non-canonical Wnt signalling mediates developmental processes, including cell migration, axon guidance and tissue patterning (Mehta et al. 2021). Recent work has shown that HS chains decorating HSPG core proteins, including GPC1, GPC3 and GPC5, bind to Wnt, negatively regulating the protein, resulting in inhibition and downregulation of canonical Wnt signalling (Annaval et al. 2020).
Key growth factors, such as BDNF and PDGF, have been identified to influence neurogenesis and interact with HSPGs to subsequently activate signalling pathways including the Wnt pathway (Houlton et al. 2019). BDNF is a member of the neurotrophin family and binds to tropomyosin-related kinase receptors, activating downstream signalling cascades, including the Wnt/β-catenin signalling pathway (Li et al. 2009). Through stimulation of neuronal growth, cellular differentiation and maturation, BDNF is commonly used in neuronal differentiation of human pluripotent stem cells, including induced pluripotent stem cells (iPSCs) (Colucci-D’Amato et al. 2020; Kanato et al. 2009; Tao and Zhang 2016) making BDNF an ideal growth factor for hMSC growth stimulation and differentiation. PDGF binds to members of the receptor tyrosine kinase (RTK) family (Chen et al. 2013; Moore et al. 2014) to regulate cell proliferation, neuronal development and stem cell marker expression (Funa and Sasahara 2014). The PDGF family of growth factors consists of several ligands (PDGF-A, -B, -C and -D) and receptor isoforms (PDGFRα and PDGFRβ), which can act as mitogens for cells of mesenchymal origin (Funa and Sasahara 2014). In NSC models, PDGF-A has been identified to induce differentiation to oligodendrocytes (Douvaras and Fossati 2015; Yan et al. 2013) and several studies report PDGF-B to have neurogenic stimulatory effects in the rodent model in vivo and in vitro, similar to effects established for BDNF (Mohapel et al. 2005; Yang et al. 2013; Yao et al. 2012). The reported binding of PDGF-B to HS, as well as its reported neurogenic effects in the rodent, suggest that PDGF-B could provide an additional means to control human neurogenesis. The effects of both BDNF PDGF on human neurogenesis and Wnt signalling activation, as well as their interaction with the SDCs and GPCs, have not yet been fully explored, requiring further investigations. Exploring intrinsic regulators of neurogenesis, including signalling pathways such as Wnt and growth factor interactions (BDNF, PDGF) in hMSCs will aid the development and understanding of the processes to differentiate these cells into functional neural cells.
hMSCs as Stem Cell Therapy Models
Stem cell therapy and neurogenesis may provide a potential method to replace injured or dead neural cells that are a feature of AD and TBI (Abdelnour et al. 2022; Neirinckx et al. 2013). The role of stem cell therapy would be to aid in the preservation of existing functional neural cells and to potentially restore and reintegrate new cells to areas of neurodegeneration for improved or repaired functionality. Various stem cell models, including hMSCs, the focus of this review, are being researched in context of neural regeneration and the use of stem cell models for their repair. hMSCs are adult-derived stem cells that have the ability to self-renew, proliferate and differentiate into various mesenchymal cell types, including osteoblasts, adipocytes and chondrocytes, but also cells of neural lineages (Ullah et al. 2015). They are commonly isolated from the bone marrow of the iliac crest, but can also be isolated from dental pulp, umbilical cord blood, adipose tissue, trabecular bone and the placenta (DiGirolamo et al. 1999; Ma 2010). hMSC multilineage capacity including differentiation into neurons, astrocytes and oligodendrocytes has been demonstrated during extended culture in vitro (Okolicsanyi et al. 2015; Yu et al. 2017). hMSCs express various markers of stemness, the molecular basis of a stem cell’s ability to self-renew and generate differentiated cells, along with specific neural lineage markers such as Nestin (NES), glial fibrillary acidic protein (GFAP) and βIII–tubulin (TUBB3), indicating hMSC potential in neural differentiation (Okolicsanyi et al. 2015, 2014a). In murine models, MSCs have been demonstrated to migrate to the brain and differentiate into glial-like cells after transplantation (Mathot et al. 2020). Recent literature reports minimal side effects and safety concerns in small scale human clinical trials applying both autologous and allogeneic hMSCs to treat neurological diseases such as TBI and stroke. However, clinical outcomes have only demonstrated marginal improvements (Andrzejewska et al. 2021; Tian et al. 2013). While hMSCs are a potential promising candidate for use in stem cell therapies for neurodegeneration, it is evident that significant research needs to be undertaken to elucidate the mechanisms driving neurogenesis and how these may be employed to treat areas of damage.
Improving hMSC Neurogenerative Potential: Opportunities and Challenges
Neuroregenerative therapy research is yet to reach its full potential, posing a myriad of challenges for both research and therapeutic applications. The challenges are primarily rooted in our limited understanding of the complex processes behind the neurological damage that occurs in both in AD and TBI (Feng and Gao 2012). Without comprehensive understanding of the factors driving disease, they cannot be used as targets to prevent, slow down or cure localised damage. Additionally, while stem cell therapies and neurogenesis show promising potential in the treatment of AD and TBI, a significant knowledge gap remains. One of the challenges posed is the availability of human cell stem cell models that are applicable for both ex vivo research, as well as clinical use due to complications such as stem cell rejection (Guy and Offen 2020). Further challenges exist surrounding the terminal differentiation of hMSCs into specific neural lineages and the comprehensive characterisation of their functional capabilities. Although hMSCs have been successfully induced to form neural-like progenitor cells known as hMSC-INs (Okolicsanyi et al. 2018), limited research has been conducted on the process of terminally differentiating these cells in sufficient quantities along with functionality tests on the differentiated cells. These gaps, however, provide an opportunity for the development of hMSC-based models to study healthy neural lineage specification in various populations from a diverse range of donors, as well as the development of relevant human cellular models of AD or TBI. Understanding the differentiation potential and functional properties of hMSCs as well as how HSPG, growth factor and signalling pathway interactions influence neural differentiation processes is crucial for evaluating their suitability as a regenerative therapy. Further investigation is required to explore the differentiation process, identify specific markers indicative of neural lineages, and assess the functional capabilities of terminally differentiated hMSCs.
There is also a need to further elucidate how SDCs and GPCs mediate neural lineage specification and their interactions with crucial signalling pathways. The precise mechanisms through which SDCs and GPCs regulate cellular signalling pathways of neural lineage specification, particularly their interactions with the Wnt and FGF pathways, requires further investigation. It is also an imperative to decipher the specific interactions between HS chains and various growth factors in these pathways in neural regeneration and lineage specification. These interactions influence neural regeneration and are critical to the therapeutic potential of hMSCs in more effective treatment strategies. Additionally, investigating the mechanisms by which HSPGs regulate protein aggregation may provide new and novel avenues of diagnosis as well as develop effective therapies for AD, TBI and other neurodegenerative disorders.
Summary
Stem cell therapy has the potential to revolutionise AD treatment via neurogenesis. HSPGs play a vital role in neurogenesis from healthy stem cells, making them essential targets for AD research (Ravikumar et al. 2020; Yu et al. 2017). Identifying the genetic contributors and associated expression changes of neurodegeneration in AD and TBI is integral to developing effective disease-specific treatments. hMSCs are ideal therapeutic candidates for the treatment of neurodegenerative diseases due to their relative ease of isolation and extensive in vitro expansive potential. HSPGs, a diverse family of macromolecules, are decorated with multiple GAG side chains that enable interactions with various protein families and ligands. HSPGs of interest include the cell membrane bound SDC and the GPI-anchored GPCs due to their known and postulated contributions to cellular regulation. SDCs mediate angiogenesis and embryonic growth, while GPCs mediate signalling activity as well as a myriad of other essential functions. Further elucidation of how these HSPGs control these events in neurogenesis will likely improve the efficacy of hMSC regenerative applications in treating AD and TBI.
Data Availability
Not applicable.
References
Abdelnour C, Agosta F, Bozzali M, Fougere B, Iwata A, Nilforooshan R, Takada LT, Vinuela F, Traber M (2022) Perspectives and challenges in patient stratification in Alzheimer’s disease. Alzheimers Res Ther 14(1):112. https://doi.org/10.1186/s13195-022-01055-y
Abu Hamdeh S, Waara ER, Möller C, Söderberg L, Basun H, Alafuzoff I, Hillered L, Lannfelt L, Ingelsson M, Marklund N (2018) Rapid amyloid-β oligomer and protofibril accumulation in traumatic brain injury. Brain Pathol 28(4):451–462. https://doi.org/10.1111/bpa.12532
Ackers I, Malgor R (2018) Interrelationship of canonical and non-canonical Wnt signalling pathways in chronic metabolic diseases. Diab Vasc Dis Res 15(1):3–13. https://doi.org/10.1177/1479164117738442
Ai X, Do AT, Lozynska O, Kusche-Gullberg M, Lindahl U, Emerson CP Jr (2003) QSulf1 remodels the 6-O sulfation states of cell surface heparan sulfate proteoglycans to promote Wnt signaling. J Cell Biol 162(2):341–351. https://doi.org/10.1083/jcb.200212083
Aikawa J, Esko JD (1999) Molecular cloning and expression of a third member of the heparan sulfate/heparin GlcNAc N-deacetylase/ N-sulfotransferase family. J Biol Chem 274(5):2690–2695. https://doi.org/10.1074/jbc.274.5.2690
Alfaro MP, Saraswati S, Young PP (2011) Molecular mediators of mesenchymal stem cell biology. Vitam Horm 87:39–59. https://doi.org/10.1016/B978-0-12-386015-6.00023-8
Andrzejewska A, Dabrowska S, Lukomska B, Janowski M (2021) Mesenchymal stem cells for neurological disorder. Adv Sci 8(7):2002944. https://doi.org/10.1002/advs.202002944
Annaval T, Wild R, Cretinon Y, Sadir R, Vives RR, Lortat-Jacob H (2020) Heparan sulfate proteoglycans biosynthesis and post synthesis mechanisms combine few enzymes and few core proteins to generate extensive structural and functional diversity. Molecules. https://doi.org/10.3390/molecules25184215
Awad W, Adamczyk B, Ornros J, Karlsson NG, Mani K, Logan DT (2015) Structural aspects of N-glycosylations and the C-terminal region in human glypican-1. J Biol Chem 290(38):22991–23008. https://doi.org/10.1074/jbc.M115.660878
Baldeiras I, Santana I, Leitão MJ, Gens H, Pascoal R, Tábuas-Pereira M, Beato-Coelho J, Duro D, Almeida MR, Oliveira CR (2018) Addition of the Aβ42/40 ratio to the cerebrospinal fluid biomarker profile increases the predictive value for underlying Alzheimer’s disease dementia in mild cognitive impairment. Alzheimer’s Res Ther 10(1):33. https://doi.org/10.1186/s13195-018-0362-2
Banerjee S, Hashemi M, Zagorski K, Lyubchenko YL (2020) Interaction of Aβ42 with membranes triggers the self-assembly into oligomers. Int J Mol Sci 21(3):1129. https://doi.org/10.3390/ijms21031129
Berwick DC, Harvey K (2012) The importance of Wnt signalling for neurodegeneration in Parkinson’s disease. Biochem Soc Trans 40(5):1123–1128. https://doi.org/10.1042/BST20120122
Berzin TM, Zipser BD, Rafii MS, Kuo-Leblanc V, Yancopoulos GD, Glass DJ, Fallon JR, Stopa EG (2000) Agrin and microvascular damage in Alzheimer’s disease. Neurobiol Aging 21(2):349–355. https://doi.org/10.1016/s0197-4580(00)00121-4
Bettens K, Sleegers K, Van Broeckhoven C (2010) Current status on Alzheimer disease molecular genetics: from past, to present, to future. Human Mol Genet 19(R1):R4–R11. https://doi.org/10.1093/hmg/ddq142
Boland GM, Perkins G, Hall DJ, Tuan RS (2004) Wnt 3a promotes proliferation and suppresses osteogenic differentiation of adult human mesenchymal stem cells. J Cell Biochem 93(6):1210–1230. https://doi.org/10.1002/jcb.20284
Breijyeh Z, Karaman R (2020) Comprehensive review on Alzheimer’s disease: causes and treatment. Molecules. https://doi.org/10.3390/molecules25245789
Caillet-Boudin ML, Buee L, Sergeant N, Lefebvre B (2015) Regulation of human MAPT gene expression. Mol Neurodegener 10:28. https://doi.org/10.1186/s13024-015-0025-8
Chen PH, Chen X, He X (2013) Platelet-derived growth factors and their receptors: structural and functional perspectives. Biochim Et Biophys Acta 1834(10):2176–2186. https://doi.org/10.1016/j.bbapap.2012.10.015
Chen GF, Xu TH, Yan Y, Zhou YR, Jiang Y, Melcher K, Xu HE (2017) Amyloid beta: structure, biology and structure-based therapeutic development. Acta Pharmacol Sin 38(9):1205–1235. https://doi.org/10.1038/aps.2017.28
Cheng F, Ruscher K, Fransson LA, Mani K (2013) Non-toxic amyloid beta formed in the presence of glypican-1 or its deaminatively generated heparan sulfate degradation products. Glycobiology 23(12):1510–1519. https://doi.org/10.1093/glycob/cwt079
Christianson H, Belting M (2014) Heparan sulfate proteoglycan as a cell-surface endocytosis receptor. Matrix Biol: J Int Soc Matrix Biol. https://doi.org/10.1016/j.matbio.2013.10.004
Colombres M, Henriquez JP, Reig GF, Scheu J, Calderon R, Alvarez A, Brandan E, Inestrosa NC (2008) Heparin activates Wnt signaling for neuronal morphogenesis. J Cell Physiol 216(3):805–815. https://doi.org/10.1002/jcp.21465
Colucci-D’Amato L, Speranza L, Volpicelli F (2020) Neurotrophic factor BDNF, physiological functions and therapeutic potential in depression, neurodegeneration and brain cancer. Int J Mol Sci 21(20):7777. https://doi.org/10.3390/ijms21207777
Condomitti G, de Wit J (2018) Heparan sulfate proteoglycans as emerging players in synaptic specificity. Front Molecular Neurosci 11:14. https://doi.org/10.3389/fnmol.2018.00014
Congdon EE, Sigurdsson EM (2018) Tau-targeting therapies for Alzheimer disease. Nat Rev Neurol 14(7):399–415. https://doi.org/10.1038/s41582-018-0013-z
Couchman JR, Gopal S, Lim HC, Norgaard S, Multhaupt HA (2015) Fell-muir lecture: syndecans: from peripheral coreceptors to mainstream regulators of cell behaviour. Int J Exp Pathol 96(1):1–10. https://doi.org/10.1111/iep.12112
Cui H, Freeman C, Jacobson GA, Small DH (2013) Proteoglycans in the central nervous system: role in development, neural repair, and Alzheimer’s disease. IUBMB Life 65(2):108–120. https://doi.org/10.1002/iub.1118
Dams-O’Connor K, Guetta G, Hahn-Ketter AE, Fedor A (2016) Traumatic brain injury as a risk factor for Alzheimer’s disease: current knowledge and future directions. Neurodegener Dis Manag 6(5):417–429. https://doi.org/10.2217/nmt-2016-0017
De Cat B, David G (2001) Developmental roles of the glypicans. Semin Cell Dev Biol 12(2):117–125. https://doi.org/10.1006/scdb.2000.0240
Debarnot C, Monneau YR, Roig-Zamboni V, Delauzun V, Le Narvor C, Richard E, Henault J, Goulet A, Fadel F, Vives RR, Priem B, Bonnaffe D, Lortat-Jacob H, Bourne Y (2019) Substrate binding mode and catalytic mechanism of human heparan sulfate d-glucuronyl C5 epimerase. Proc Natl Acad Sci U S A 116(14):6760–6765. https://doi.org/10.1073/pnas.1818333116
DeKosky ST, Abrahamson EE, Ciallella JR, Paljug WR, Wisniewski SR, Clark RS, Ikonomovic MD (2007) Association of increased cortical soluble abeta42 levels with diffuse plaques after severe brain injury in humans. Arch Neurol 64(4):541–544. https://doi.org/10.1001/archneur.64.4.541
DeTure MA, Dickson DW (2019) The neuropathological diagnosis of Alzheimer’s disease. Mol Neurodegener 14(1):32. https://doi.org/10.1186/s13024-019-0333-5
Dewan MC, Rattani A, Gupta S, Baticulon RE, Hung YC, Punchak M, Agrawal A, Adeleye AO, Shrime MG, Rubiano AM, Rosenfeld JV, Park KB (2018) Estimating the global incidence of traumatic brain injury. J Neurosurg 130(4):1080–1097. https://doi.org/10.3171/2017.10.JNS17352
Diaz-Arrastia R, Gong Y, Fair S, Scott KD, Garcia MC, Carlile MC, Agostini MA, Van Ness PC (2003) Increased risk of late posttraumatic seizures associated with inheritance of APOE epsilon4 allele. Arch Neurol 60(6):818–822. https://doi.org/10.1001/archneur.60.6.818
DiGirolamo CM, Stokes D, Colter D, Phinney DG, Class R, & Prockop DJ (1999) Propagation and senescence of human marrow stromal cells in culture: a simple colony-forming assay identifies samples with the greatest potential to propagate and differentiate. Br J Haematol 107(2):275–281. https://doi.org/10.1046/j.1365-2141.1999.01715.x
Disouky A, Lazarov O (2021) Adult hippocampal neurogenesis in Alzheimer’s disease. Prog Mol Biol Transl Sci 177:137–156. https://doi.org/10.1016/bs.pmbts.2020.09.002
Dong C, Choi YK, Lee J, Zhang XF, Honerkamp-Smith A, Widmalm G, Lowe-Krentz LJ, Im W (2021) Structure, dynamics, and interactions of gpi-anchored human glypican-1 with heparan sulfates in a membrane. Glycobiology 31(5):593–602. https://doi.org/10.1093/glycob/cwaa092
Douvaras P, Fossati V (2015) Generation and isolation of oligodendrocyte progenitor cells from human pluripotent stem cells. Nat Protoc 10(8):1143–1154. https://doi.org/10.1038/nprot.2015.075
Edwards G 3rd, Zhao J, Dash PK, Soto C, Moreno-Gonzalez I (2020) Traumatic brain injury induces Tau aggregation and spreading. J Neurotrauma 37(1):80–92. https://doi.org/10.1089/neu.2018.6348
Feng Z, Gao F (2012) Stem cell challenges in the treatment of neurodegenerative disease. CNS Neurosci Ther 18(2):142–148. https://doi.org/10.1111/j.1755-5949.2011.00239.x
Ferrari C, Sorbi S (2021) The complexity of Alzheimer’s disease: an evolving puzzle. Physiol Rev 101(3):1047–1081. https://doi.org/10.1152/physrev.00015.2020
Ferreira D, Nordberg A, Westman E (2020) Biological subtypes of Alzheimer disease: a systematic review and meta-analysis. Neurology 94(10):436–448. https://doi.org/10.1212/WNL.0000000000009058
Fico A, Maina F, Dono R (2011) Fine-tuning of cell signaling by glypicans. Cell Mol Life Sci 68(6):923–929. https://doi.org/10.1007/s00018-007-7471-6
Filmus J, Capurro M, Rast J (2008) Glypicans. Genome Biol 9(5):224. https://doi.org/10.1186/gb-2008-9-5-224
Folke J, Pakkenberg B, Brudek T (2019) Impaired Wnt signaling in the prefrontal cortex of Alzheimer’s disease. Mol Neurobiol 56(2):873–891. https://doi.org/10.1007/s12035-018-1103-z
Frieden C, Wang H, Ho CMW (2017) A mechanism for lipid binding to apoE and the role of intrinsically disordered regions coupled to domain-domain interactions. Proc Natl Acad Sci U S A 114(24):6292–6297. https://doi.org/10.1073/pnas.1705080114
Funa K, Sasahara M (2014) The roles of PDGF in development and during neurogenesis in the normal and diseased nervous system. J Neuroimmune Pharmacol 9(2):168–181. https://doi.org/10.1007/s11481-013-9479-z
Galgano M, Toshkezi G, Qiu X, Russell T, Chin L, Zhao LR (2017) Traumatic brain injury: current treatment strategies and future endeavors. Cell Transplant 26(7):1118–1130. https://doi.org/10.1177/0963689717714102
Golde TE, Petrucelli L, Lewis J (2010) Targeting Abeta and Tau in Alzheimer’s disease, an early interim report. Exp Neurol 223(2):252–266. https://doi.org/10.1016/j.expneurol.2009.07.035
Gonzalez Rodriguez E, Cardenas JC, Cox CS, Kitagawa RS, Stensballe J, Holcomb JB, Johansson PI, Wade CE (2018) Traumatic brain injury is associated with increased syndecan-1 shedding in severely injured patients. Scand J Trauma Resusc Emerg Med 26(1):102. https://doi.org/10.1186/s13049-018-0565-3
Grothe MJ, Sepulcre J, Gonzalez-Escamilla G, Jelistratova I, Scholl M, Hansson O, Teipel SJ, Alzheimer’s Disease Neuroimaging (2018) Molecular properties underlying regional vulnerability to Alzheimer’s disease pathology. Brain 141(9):2755–2771
Gu L, Guo Z (2013) Alzheimer’s Abeta42 and Abeta40 peptides form interlaced amyloid fibrils. J Neurochem 126(3):305–311. https://doi.org/10.1111/jnc.12202
Gupta-Bansal R, Frederickson RC, Brunden KR (1995) Proteoglycan-mediated inhibition of A beta proteolysis. A potential cause of senile plaque accumulation. J Biol Chem 270(31):18666–18671. https://doi.org/10.1074/jbc.270.31.18666
Guy R, Offen D (2020) Promising opportunities for treating neurodegenerative diseases with mesenchymal stem cell-derived exosomes. Biomolecules. https://doi.org/10.3390/biom10091320
Hagino S, Iseki K, Mori T, Zhang Y, Sakai N, Yokoya S, Hikake T, Kikuchi S, Wanaka A (2003) Expression pattern of glypican-1 mRNA after brain injury in mice. Neurosci Lett 349(1):29–32. https://doi.org/10.1016/s0304-3940(03)00690-6
Herrmann N, Wang HJ, Song BX, Bawa KK, Lanctot KL (2022) Risks and benefits of current and novel drugs to treat agitation in Alzheimer’s disease. Expert Opin Drug Saf 21(10):1289–1301. https://doi.org/10.1080/14740338.2022.2136162
Horie K, Barthelemy NR, Mallipeddi N, Li Y, Franklin EE, Perrin RJ, Bateman RJ, Sato C (2020) Regional correlation of biochemical measures of amyloid and Tau phosphorylation in the brain. Acta Neuropathol Commun 8(1):149. https://doi.org/10.1186/s40478-020-01019-z
Houlton J, Abumaria N, Hinkley S, Clarkson AN (2019) Therapeutic potential of neurotrophins for repair after brain injury: a helping hand from biomaterials. Front Neurosci 13:790. https://doi.org/10.3389/fnins.2019.00790
Hua Y, Yang Y, Li Q, He X, Zhu W, Wang J, Gan X (2018) Oligomerization of Frizzled and LRP5/6 protein initiates intracellular signaling for the canonical WNT/beta-catenin pathway. J Biol Chem 293(51):19710–19724. https://doi.org/10.1074/jbc.RA118.004434
Hudák A, Josvay K, Domonkos I, Letoha A, Szilak L, Letoha T (2021) The interplay of apoes with syndecans in influencing key cellular events of amyloid pathology. Int J Mol Sci. https://doi.org/10.3390/ijms22137070
Hudák A, Letoha A, Vizler C, Letoha T (2022) Syndecan-3 as a Novel Biomarker in Alzheimer's Disease. Int J Mol Sci 23(6):3407. https://doi.org/10.3390/ijms23063407
Huse JT, Liu K, Pijak DS, Carlin D, Lee VM, Doms RW (2002) Beta-secretase processing in the trans-Golgi network preferentially generates truncated amyloid species that accumulate in Alzheimer’s disease brain. J Biol Chem 277(18):16278–16284. https://doi.org/10.1074/jbc.M111141200
Ikonomovic MD, Uryu K, Abrahamson EE, Ciallella JR, Trojanowski JQ, Lee VM, Clark RS, Marion DW, Wisniewski SR, DeKosky ST (2004) Alzheimer’s pathology in human temporal cortex surgically excised after severe brain injury. Exp Neurol 190(1):192–203. https://doi.org/10.1016/j.expneurol.2004.06.011
Jarosz-Griffiths HH, Noble E, Rushworth JV, Hooper NM (2016) Amyloid-beta receptors: the good, the bad, and the prion protein. J Biol Chem 291(7):3174–3183. https://doi.org/10.1074/jbc.R115.702704
Jen Y, Musacchio M, Lander AD (2009) Glypican-1 controls brain size through regulation of fibroblast growth factor signaling in early neurogenesis. Neural Develop 4:33. https://doi.org/10.1186/1749-8104-4-33
Johnson VE, Stewart W, Smith DH (2010a) Traumatic brain injury and amyloid-beta pathology: a link to Alzheimer’s disease? Nat Rev Neurosci 11(5):361–370. https://doi.org/10.1038/nrn2808
Johnson VE, Stewart W, Smith DH (2010b) Traumatic brain injury and amyloid-β pathology: a link to Alzheimer’s disease? Nat Rev Neurosci 11(5):361–370. https://doi.org/10.1038/nrn2808
Johnson VE, Stewart W, Smith DH (2012) Widespread Tau and amyloid-beta pathology many years after a single traumatic brain injury in humans. Brain Pathol 22(2):142–149. https://doi.org/10.1111/j.1750-3639.2011.00513.x
Jullienne A, Roberts JM, Pop V, Paul Murphy M, Head E, Bix GJ, Badaut J (2014) Juvenile traumatic brain injury induces long-term perivascular matrix changes alongside amyloid-beta accumulation. J Cereb Blood Flow Metab 34(10):1637–1645. https://doi.org/10.1038/jcbfm.2014.124
Kabir MT, Uddin MS, Setu JR, Ashraf GM, Bin-Jumah MN, Abdel-Daim MM (2020) Exploring the role of psen mutations in the pathogenesis of Alzheimer’s disease. Neurotox Res 38(4):833–849. https://doi.org/10.1007/s12640-020-00232-x
Kamimura K, Maeda N (2021) Glypicans and heparan sulfate in synaptic development, neural plasticity, and neurological disorders. Front Neural Circuits 15:595596. https://doi.org/10.3389/fncir.2021.595596
Kanato Y, Ono S, Kitajima K, Sato C (2009) Complex formation of a brain-derived neurotrophic factor and glycosaminoglycans. Biosci Biotechnol Biochem 73(12):2735–2741. https://doi.org/10.1271/bbb.90637
Kelleher RJ 3rd, Shen J (2017) Presenilin-1 mutations and Alzheimer’s disease. Proc Natl Acad Sci U S A 114(4):629–631. https://doi.org/10.1073/pnas.1619574114
Khezri MR, Mohebalizadeh M, Ghasemnejad-Berenji M (2023) Therapeutic potential of ADAM10 modulation in Alzheimer’s disease: a review of the current evidence. Cell Commun Signal 21(1):60. https://doi.org/10.1186/s12964-023-01072-w
Knelson EH, Nee JC, Blobe GC (2014) Heparan sulfate signaling in cancer. Trends Biochem Sci 39(6):277–288. https://doi.org/10.1016/j.tibs.2014.03.001
Komiya Y, Habas R (2008) Wnt Signal Transduction Pathways. Organogenesis 4(2):68–75. https://doi.org/10.4161/org.4.2.5851
Kumar-Singh S, Theuns J, Van Broeck B, Pirici D, Vennekens K, Corsmit E, Cruts M, Dermaut B, Wang R, Van Broeckhoven C (2006) Mean age-of-onset of familial alzheimer disease caused by presenilin mutations correlates with both increased Abeta42 and decreased Abeta40. Human Mutat 27(7):686–695. https://doi.org/10.1002/humu.20336
Kuperstein I, Broersen K, Benilova I, Rozenski J, Jonckheere W, Debulpaep M, Vandersteen A, Segers-Nolten I, Van Der Werf K, Subramaniam V, Braeken D, Callewaert G, Bartic C, D’Hooge R, Martins IC, Rousseau F, Schymkowitz J, De Strooper B (2010) Neurotoxicity of Alzheimer’s disease Aβ peptides is induced by small changes in the Aβ42 to Aβ40 ratio. EMBO J 29(19):3408–3420. https://doi.org/10.1038/emboj.2010.211
Lambaerts K, Wilcox-Adelman SA, Zimmermann P (2009) The signaling mechanisms of syndecan heparan sulfate proteoglycans. Curr Opin Cell Biol 21(5):662–669. https://doi.org/10.1016/j.ceb.2009.05.002
Lane CA, Hardy J, Schott JM (2018) Alzheimer’s disease. Eur J Neurol 25(1):59–70. https://doi.org/10.1111/ene.13439
Lanoiselee HM, Nicolas G, Wallon D, Rovelet-Lecrux A, Lacour M, Rousseau S, Richard AC, Pasquier F, Rollin-Sillaire A, Martinaud O, Quillard-Muraine M, de la Sayette V, Boutoleau-Bretonniere C, Etcharry-Bouyx F, Chauvire V, Sarazin M, le Ber I, Epelbaum S, Jonveaux T, Rouaud O, Ceccaldi M, Felician O, Godefroy O, Formaglio M, Croisile B, Auriacombe S, Chamard L, Vincent JL, Sauvee M, Marelli-Tosi C, Gabelle A, Ozsancak C, Pariente J, Paquet C, Hannequin D, Campion D, Collaborators of the, C. N. R. M. A. J. p. (2017) APP, PSEN1, and PSEN2 mutations in early-onset Alzheimer disease: A genetic screening study of familial and sporadic cases. PLoS Med 14(3):e1002270. https://doi.org/10.1371/journal.pmed.1002270
Lavorgna TR, Gressett TE, Chastain WH, Bix GJ (2023) Perlecan: a review of its role in neurologic and musculoskeletal disease. Front Physiol 14:1189731. https://doi.org/10.3389/fphys.2023.1189731
Leonova EI, Galzitskaya OV (2013) Structure and functions of syndecans in vertebrates. Biochemistry (mosc) 78(10):1071–1085. https://doi.org/10.1134/S0006297913100015
Letoha T, Hudak A, Kusz E, Pettko-Szandtner A, Domonkos I, Josvay K, Hofmann-Apitius M, Szilak L (2019) Contribution of syndecans to cellular internalization and fibrillation of amyloid-beta(1–42). Sci Rep 9(1):1393. https://doi.org/10.1038/s41598-018-37476-9
Li T, Jiang L, Zhang X, Chen H (2009) In-vitro effects of brain-derived neurotrophic factor on neural progenitor/stem cells from rat hippocampus. NeuroReport 20(3):295–300. https://doi.org/10.1097/WNR.0b013e32832000c8
Li N, Gao W, Zhang YF, Ho M (2018) Glypicans as cancer therapeutic targets. Trends in Cancer 4(11):741–754
Ling L, Nurcombe V, Cool SM (2009) Wnt signaling controls the fate of mesenchymal stem cells. Gene 433(1–2):1–7. https://doi.org/10.1016/j.gene.2008.12.008
Lista S, O’Bryant SE, Blennow K, Dubois B, Hugon J, Zetterberg H, Hampel H (2015) Biomarkers in sporadic and familial Alzheimer’s disease. J Alzheimers Dis 47(2):291–317. https://doi.org/10.3233/JAD-143006
Liu G, Vijayakumar S, Grumolato L, Arroyave R, Qiao H, Akiri G, Aaronson SA (2009) Canonical Wnts function as potent regulators of osteogenesis by human mesenchymal stem cells. J Cell Biol 185(1):67–75. https://doi.org/10.1083/jcb.200810137
Liu CC, Liu CC, Kanekiyo T, Xu H, Bu G (2013) Apolipoprotein E and Alzheimer disease: risk, mechanisms and therapy. Nat Rev Neurol 9(2):106–118. https://doi.org/10.1038/nrneurol.2012.263
Liu CC, Tsai CW, Deak F, Rogers J, Penuliar M, Sung YM, Maher JN, Fu Y, Li X, Xu H, Estus S, Hoe HS, Fryer JD, Kanekiyo T, Bu G (2014) Deficiency in LRP6-mediated Wnt signaling contributes to synaptic abnormalities and amyloid pathology in Alzheimer’s disease. Neuron 84(1):63–77. https://doi.org/10.1016/j.neuron.2014.08.048
Liu CC, Zhao N, Yamaguchi Y, Cirrito JR, Kanekiyo T, Holtzman DM, Bu G (2016) Neuronal heparan sulfates promote amyloid pathology by modulating brain amyloid-beta clearance and aggregation in Alzheimer’s disease. Sci Transl Med 8(332):332ra344. https://doi.org/10.1126/scitranslmed.aad3650
Liu J, Xiao Q, Xiao J, Niu C, Li Y, Zhang X, Zhou Z, Shu G, Yin G (2022) Wnt/beta-catenin signalling: function, biological mechanisms, and therapeutic opportunities. Signal Transduct Target Ther 7(1):3. https://doi.org/10.1038/s41392-021-00762-6
Lopes CC, Dietrich CP, Nader HB (2006) Specific structural features of syndecans and heparan sulfate chains are needed for cell signaling. Braz J Med Biol Res 39(2):157–167. https://doi.org/10.1590/s0100-879x2006000200001
Lorente-Gea L, Garcia B, Martin C, Ordiales H, Garcia-Suarez O, Pina-Batista KM, Merayo-Lloves J, Quiros LM, Fernandez-Vega I (2020) Heparan sulfate proteoglycans undergo differential expression alterations in Alzheimer disease brains. J Neuropathol Exp Neurol 79(5):474–483. https://doi.org/10.1093/jnen/nlaa016
Lugert S, Kremer T, Jagasia R, Herrmann A, Aigner S, Giachino C, Mendez-David I, Gardier AM, Carralot JP, Meistermann H, Augustin A, Saxe MD, Lamerz J, Duran-Pacheco G, Ducret A, Taylor V, David DJ, Czech C (2017) Glypican-2 levels in cerebrospinal fluid predict the status of adult hippocampal neurogenesis. Sci Rep 7:46543. https://doi.org/10.1038/srep46543
Lyu D, Gong M, Zhang Y, Lyu X (2022) Effects of different kinds of anti-Alzheimer’s disease drugs on cognitive improvement: protocol for a systematic review and network meta-analysis of phase III clinical trials. Syst Rev 11(1):84. https://doi.org/10.1186/s13643-022-01964-x
Ma, T. (2010). Mesenchymal stem cells: From bench to bedside. World J Stem Cells 2(2):13–17. https://doi.org/10.4252/wjsc.v2.i2.13
Mah D, Zhao J, Liu X, Zhang F, Liu J, Wang L, Linhardt R, Wang C (2021) The sulfation code of tauopathies: heparan sulfate proteoglycans in the prion like spread of Tau pathology. Front Mol Biosci 8:671458. https://doi.org/10.3389/fmolb.2021.671458
Marais AD (2019) Apolipoprotein E in lipoprotein metabolism, health and cardiovascular disease. Pathology 51(2):165–176. https://doi.org/10.1016/j.pathol.2018.11.002
Marklund N, Blennow K, Zetterberg H, Ronne-Engstrom E, Enblad P, Hillered L (2009) Monitoring of brain interstitial total Tau and beta amyloid proteins by microdialysis in patients with traumatic brain injury. J Neurosurg 110(6):1227–1237. https://doi.org/10.3171/2008.9.JNS08584
Mathot F, Rbia N, Bishop AT, Hovius SER, Van Wijnen AJ, Shin AY (2020) Adhesion, distribution, and migration of differentiated and undifferentiated mesenchymal stem cells (MSCs) seeded on nerve allografts. J Plast Reconstr Aesthet Surg 73(1):81–89. https://doi.org/10.1016/j.bjps.2019.05.030
McFadyen CA, Zeiler FA, Newcombe V, Synnot A, Steyerberg E, Gruen RL, Rosand J, Palotie A, Maas AIR, Menon DK (2021) Apolipoprotein E4 polymorphism and outcomes from traumatic brain injury: a living systematic review and meta-analysis. J Neurotrauma 38(8):1124–1136. https://doi.org/10.1089/neu.2018.6052
McKee AC, Daneshvar DH (2015) The neuropathology of traumatic brain injury. Handb Clin Neurol 127:45–66. https://doi.org/10.1016/B978-0-444-52892-6.00004-0
McMillan OI, Li JP, Wang L (2023) Heparan sulfate proteoglycan in Alzheimer’s disease: aberrant expression and functions in molecular pathways related to amyloid-beta metabolism. Am J Physiol Cell Physiol 324(4):C893–C909. https://doi.org/10.1152/ajpcell.00247.2022
Mehta S, Hingole S, Chaudhary V (2021) The emerging mechanisms of Wnt secretion and signaling in development. Front Cell Dev Biol 9:714746. https://doi.org/10.3389/fcell.2021.714746
Metaxas A, Kempf SJ (2016) Neurofibrillary tangles in Alzheimer’s disease: elucidation of the molecular mechanism by immunohistochemistry and Tau protein phospho-proteomics. Neural Regen Res 11(10):1579–1581. https://doi.org/10.4103/1673-5374.193234
Mohanty R, Ferreira D, Frerich S, Muehlboeck JS, Grothe MJ, Westman E, For the Alzheimer's Disease Neuroimaging, I. (2022) Neuropathologic features of antemortem atrophy-based subtypes of Alzheimer disease. Neurology. https://doi.org/10.1212/WNL.0000000000200573
Mohapel P, Frielingsdorf H, Haggblad J, Zachrisson O, Brundin P (2005) Platelet-derived growth factor (PDGF-BB) and brain-derived neurotrophic factor (BDNF) induce striatal neurogenesis in adult rats with 6-hydroxydopamine lesions. Neuroscience 132(3):767–776. https://doi.org/10.1016/j.neuroscience.2004.11.056
Moore L, Bain JM, Loh JM, Levison SW (2014) PDGF-responsive progenitors persist in the subventricular zone across the lifespan. ASN Neuro. https://doi.org/10.1042/AN20120041
Muller UC, Zheng H (2012) Physiological functions of APP family proteins. Cold Spring Harb Perspect Med 2(2):a006288. https://doi.org/10.1101/cshperspect.a006288
Naasan G, Shdo SM, Rodriguez EM, Spina S, Grinberg L, Lopez L, Karydas A, Seeley WW, Miller BL, Rankin KP (2021) Psychosis in neurodegenerative disease: differential patterns of hallucination and delusion symptoms. Brain 144(3):999–1012. https://doi.org/10.1093/brain/awaa413
Najem D, Rennie K, Ribecco-Lutkiewicz M, Ly D, Haukenfrers J, Liu Q, Nzau M, Fraser DD, Bani-Yaghoub M (2018) Traumatic brain injury: classification, models, and markers. Biochem Cell Biol 96(4):391–406. https://doi.org/10.1139/bcb-2016-0160
Neirinckx V, Coste C, Rogister B, Wislet-Gendebien S (2013) Concise review: adult mesenchymal stem cells, adult neural crest stem cells, and therapy of neurological pathologies: a state of play. Stem Cells Transl Med 2(4):284–296. https://doi.org/10.5966/sctm.2012-0147
Ng SY, Lee AYW (2019) Traumatic brain injuries: pathophysiology and potential therapeutic targets. Front Cell Neurosci 13:528. https://doi.org/10.3389/fncel.2019.00528
O’Brien RJ, Wong PC (2011) Amyloid precursor protein processing and Alzheimer’s disease. Annu Rev Neurosci 34:185–204. https://doi.org/10.1146/annurev-neuro-061010-113613
O’Callaghan P, Sandwall E, Li JP, Yu H, Ravid R, Guan ZZ, van Kuppevelt TH, Nilsson LN, Ingelsson M, Hyman BT, Kalimo H, Lindahl U, Lannfelt L, Zhang X (2008) Heparan sulfate accumulation with Abeta deposits in Alzheimer’s disease and Tg2576 mice is contributed by glial cells. Brain Pathol 18(4):548–561. https://doi.org/10.1111/j.1750-3639.2008.00152.x
Ohmi K, Zhao HZ, Neufeld EF (2011) Defects in the medial entorhinal cortex and dentate gyrus in the mouse model of Sanfilippo syndrome type B. PLoS ONE 6(11):e27461. https://doi.org/10.1371/journal.pone.0027461
Oikari L, Griffiths L, Haupt L (2014) The current state of play in human neural stem cell models: what we have learnt from the rodent. OA Stem Cells 2(1):7
Oikari LE, Okolicsanyi RK, Qin A, Yu C, Griffiths LR, Haupt LM (2016) Cell surface heparan sulfate proteoglycans as novel markers of human neural stem cell fate determination. Stem Cell Res 16:92–104
Oikari LE, Yu C, Okolicsanyi RK, Avgan N, Peall IW, Griffiths LR, Haupt LM (2020) HSPGs glypican-1 and glypican-4 are human neuronal proteins characteristic of different neural phenotypes. J Neurosci Res 98(8):1619–1645. https://doi.org/10.1002/jnr.24666
Okolicsanyi RK, Griffiths LR, Haupt LM (2014a) Mesenchymal stem cells, neural lineage potential, heparan sulfate proteoglycans and the matrix. Dev Biol 388(1):1–10. https://doi.org/10.1016/j.ydbio.2014.01.024
Okolicsanyi RK, van Wijnen AJ, Cool SM, Stein GS, Griffiths LR, Haupt LM (2014b) Heparan sulfate proteoglycans and human breast cancer epithelial cell tumorigenicity. J Cell Biochem 115(5):967–976. https://doi.org/10.1002/jcb.24746
Okolicsanyi RK, Camilleri ET, Oikari LE, Yu C, Cool SM, van Wijnen AJ, Griffiths LR, Haupt LM (2015) Human mesenchymal stem cells retain multilineage differentiation capacity including neural marker expression after extended in vitro expansion. PLoS ONE 10(9):e0137255. https://doi.org/10.1371/journal.pone.0137255
Okolicsanyi RK, Oikari LE, Yu C, Griffiths LR, Haupt LM (2018) Heparan sulfate proteoglycans as drivers of neural progenitors derived from human mesenchymal stem cells. Front Mol Neurosci 11:134. https://doi.org/10.3389/fnmol.2018.00134
Ornitz DM, Itoh N (2015) The fibroblast growth factor signaling pathway. Develop Biol 4(3):215–266. https://doi.org/10.1002/wdev.176
Ozsan McMillan I, Li JP, Wang L (2023) Heparan sulfate proteoglycan in Alzheimer’s disease: aberrant expression and functions in molecular pathways related to amyloid-beta metabolism. Am J Physiol Cell Physiol 324(4):C893–C909. https://doi.org/10.1152/ajpcell.00247.2022
Palomer E, Buechler J, Salinas PC (2019) Wnt signaling deregulation in the aging and Alzheimer’s brain. Front Cell Neurosci 13:227. https://doi.org/10.3389/fncel.2019.00227
Pauwels K, Williams TL, Morris KL, Jonckheere W, Vandersteen A, Kelly G, Schymkowitz J, Rousseau F, Pastore A, Serpell LC, Broersen K (2012) Structural basis for increased toxicity of pathological abeta42:abeta40 ratios in Alzheimer disease. J Biol Chem 287(8):5650–5660. https://doi.org/10.1074/jbc.M111.264473
Perl DP (2010) Neuropathology of Alzheimer’s disease. Mt Sinai J Med 77(1):32–42. https://doi.org/10.1002/msj.20157
Picone P, Nuzzo D, Giacomazza D, Di Carlo M (2020) Beta-amyloid peptide: the cell compartment multi-faceted interaction in Alzheimer’s disease. Neurotox Res 37(2):250–263. https://doi.org/10.1007/s12640-019-00116-9
Pikas DS, Eriksson I, Kjellen L (2000) Overexpression of different isoforms of glucosaminyl N-deacetylase/N-sulfotransferase results in distinct heparan sulfate N-sulfation patterns. Biochemistry 39(15):4552–4558. https://doi.org/10.1021/bi992524l
Poon CH, Wang Y, Fung ML, Zhang C, Lim LW (2020) Rodent models of amyloid-beta feature of Alzheimer’s disease: development and potential treatment implications. Aging Dis 11(5):1235–1259. https://doi.org/10.14336/AD.2019.1026
Pulsipher A, Griffin ME, Stone SE, Hsieh-Wilson LC (2015) Long-lived engineering of glycans to direct stem cell fate. Angew Chem Int Ed Engl 54(5):1466–1470. https://doi.org/10.1002/anie.201409258
Qiang W, Yau WM, Lu JX, Collinge J, Tycko R (2017) Structural variation in amyloid-beta fibrils from Alzheimer’s disease clinical subtypes. Nature 541(7636):217–221. https://doi.org/10.1038/nature20814
Qin Y, Ke J, Gu X, Fang J, Wang W, Cong Q, Li J, Tan J, Brunzelle JS, Zhang C, Jiang Y, Melcher K, Li JP, Xu HE, Ding K (2015) Structural and functional study of D-glucuronyl C5-epimerase. J Biol Chem 290(8):4620–4630. https://doi.org/10.1074/jbc.M114.602201
Rajmohan R, Reddy PH (2017) Amyloid-beta and phosphorylated Tau accumulations cause abnormalities at synapses of Alzheimer’s disease neurons. J Alzheimer’s Dis 57(4):975–999. https://doi.org/10.3233/JAD-160612
Ramos-Cejudo J, Wisniewski T, Marmar C, Zetterberg H, Blennow K, de Leon MJ, Fossati S (2018) Traumatic brain injury and Alzheimer’s disease: the cerebrovascular link. EBioMedicine 28:21–30. https://doi.org/10.1016/j.ebiom.2018.01.021
Rauch JN, Chen JJ, Sorum AW, Miller GM, Sharf T, See SK, Hsieh-Wilson LC, Kampmann M, Kosik KS (2018) Tau Internalization is regulated by 6-O sulfation on heparan sulfate proteoglycans (HSPGs). Sci Rep 8(1):6382. https://doi.org/10.1038/s41598-018-24904-z
Ravikumar M, Smith RAA, Nurcombe V, Cool SM (2020) Heparan sulfate proteoglycans: key mediators of stem cell function. Front Cell Dev Biol 8:581213. https://doi.org/10.3389/fcell.2020.581213
Reinhard C, Borgers M, David G, De Strooper B (2013) Soluble amyloid-beta precursor protein binds its cell surface receptor in a cooperative fashion with glypican and syndecan proteoglycans. J Cell Sci 126(Pt 21):4856–4861. https://doi.org/10.1242/jcs.137919
Reiss AB, Arain HA, Stecker MM, Siegart NM, Kasselman LJ (2018) Amyloid toxicity in Alzheimer’s disease. Rev Neurosci 29(6):613–627. https://doi.org/10.1515/revneuro-2017-0063
Ren Q, Chen J, Liu Y (2021) LRP5 and LRP6 in Wnt signaling: similarity and divergence. Front Cell Dev Biol 9:670960. https://doi.org/10.3389/fcell.2021.670960
Risacher SL, Anderson WH, Charil A, Castelluccio PF, Shcherbinin S, Saykin AJ, Schwarz AJ, Alzheimer’s Disease Neuroimaging I (2017) Alzheimer disease brain atrophy subtypes are associated with cognition and rate of decline. Neurology 89(21):2176–2186. https://doi.org/10.1212/WNL.0000000000004670
Sakane H, Yamamoto H, Matsumoto S, Sato A, Kikuchi A (2012) Localization of glypican-4 in different membrane microdomains is involved in the regulation of Wnt signaling. J Cell Sci 125:449–460. https://doi.org/10.1242/jcs.091876
Salza R, Oudart JB, Ramont L, Maquart FX, Bakchine S, Thoannes H, Ricard-Blum S (2015) Endostatin level in cerebrospinal fluid of patients with Alzheimer’s disease. J Alzheimers Dis 44(4):1253–1261. https://doi.org/10.3233/JAD-142544
Saroja SR, Gorbachev K, Julia T, Goate AM, Pereira AC (2022) Astrocyte-secreted glypican-4 drives APOE4-dependent Tau hyperphosphorylation. Proc Natl Acad Sci U S A 119(34):e2108870119. https://doi.org/10.1073/pnas.2108870119
Sarrazin S, Lamanna WC, Esko JD (2011) Heparan sulfate proteoglycans. Cold Spring Harbor Perspect Biol 3(7):a004952. https://doi.org/10.1101/cshperspect.a004952
Schulz JG, Annaert W, Vandekerckhove J, Zimmermann P, De Strooper B, David G (2003) Syndecan 3 intramembrane proteolysis is presenilin/gamma-secretase-dependent and modulates cytosolic signaling. J Biol Chem 278(49):48651–48657. https://doi.org/10.1074/jbc.M308424200
Sepulveda-Diaz JE, Alavi Naini SM, Huynh MB, Ouidja MO, Yanicostas C, Chantepie S, Villares J, Lamari F, Jospin E, van Kuppevelt TH, Mensah-Nyagan AG, Raisman-Vozari R, Soussi-Yanicostas N, Papy-Garcia D (2015) HS3ST2 expression is critical for the abnormal phosphorylation of Tau in Alzheimer’s disease-related Tau pathology. Brain 138:1339–1354. https://doi.org/10.1093/brain/awv056
Serrano-Pozo A, Frosch MP, Masliah E, Hyman BT (2011) Neuropathological alterations in Alzheimer disease. Cold Spring Harb Perspect Med 1(1):a006189. https://doi.org/10.1101/cshperspect.a006189
Sethi JK, Vidal-Puig A (2010) Wnt signalling and the control of cellular metabolism. Biochem J 427(1):1–17. https://doi.org/10.1042/BJ20091866
Shi D, Sheng A, Chi L (2021) Glycosaminoglycan-protein interactions and their roles in human disease. Front Mol Biosci 8:639666. https://doi.org/10.3389/fmolb.2021.639666
Siedlak SL, Cras P, Kawai M, Richey P, Perry G (1991) Basic fibroblast growth factor binding is a marker for extracellular neurofibrillary tangles in Alzheimer disease. Journal Histochem Cytochem: off J Histochem Soc 39(7):899–904. https://doi.org/10.1177/39.7.1865106
Smith DH, Johnson VE, Stewart W (2013) Chronic neuropathologies of single and repetitive TBI: substrates of dementia? Nat Rev Neurol 9(4):211–221. https://doi.org/10.1038/nrneurol.2013.29
Snow AD, Sekiguchi RT, Nochlin D, Kalaria RN, Kimata K (1994) Heparan sulfate proteoglycan in diffuse plaques of hippocampus but not of cerebellum in Alzheimer’s disease brain. Am J Pathol 144(3):337–347
Snow AD, Cummings JA, Lake T (2021) The Unifying hypothesis of Alzheimer’s disease: heparan sulfate proteoglycans/glycosaminoglycans are key as first hypothesized over 30 years ago. Front Aging Neurosci 13:710683. https://doi.org/10.3389/fnagi.2021.710683
Snyder SW, Ladror US, Wade WS, Wang GT, Barrett LW, Matayoshi ED, Huffaker HJ, Krafft GA, Holzman TF (1994) Amyloid-beta aggregation: selective inhibition of aggregation in mixtures of amyloid with different chain lengths. Biophys J 67(3):1216–1228. https://doi.org/10.1016/S0006-3495(94)80591-0
Solis E, Hascup KN, Hascup ER (2020) Alzheimer’s disease: the link between amyloid-β and neurovascular dysfunction. J Alzheimer’s Dis 76(4):1179–1198. https://doi.org/10.3233/JAD-200473
Strang KH, Golde TE, Giasson BI (2019) MAPT mutations, tauopathy, and mechanisms of neurodegeneration. Lab Invest 99(7):912–928. https://doi.org/10.1038/s41374-019-0197-x
Su JH, Cummings BJ, Cotman CW (1992) Localization of heparan sulfate glycosaminoglycan and proteoglycan core protein in aged brain and Alzheimer’s disease. Neuroscience 51(4):801–813. https://doi.org/10.1016/0306-4522(92)90521-3
Sugahara K, Kitagawa H (2002) Heparin and heparan sulfate biosynthesis. IUBMB Life 54(4):163–175. https://doi.org/10.1080/15216540214928
Suh J, Choi SH, Romano DM, Gannon MA, Lesinski AN, Kim DY, Tanzi RE (2013) ADAM10 missense mutations potentiate beta-amyloid accumulation by impairing prodomain chaperone function. Neuron 80(2):385–401
Tao Y, Zhang SC (2016) Neural subtype specification from human pluripotent stem cells. Cell Stem Cell 19(5):573–586. https://doi.org/10.1016/j.stem.2016.10.015
Tarawneh R, Holtzman DM (2012) The clinical problem of symptomatic Alzheimer disease and mild cognitive impairment. Cold Spring Harb Perspect Med 2(5):a006148. https://doi.org/10.1101/cshperspect.a006148
Tariciotti L, Casadei M, Honig LS, Teich AF, McKhann Ii GM, Tosto G, Mayeux R (2018) Clinical experience with cerebrospinal fluid abeta42, total and phosphorylated Tau in the evaluation of 1,016 individuals for suspected dementia. J Alzheimers Dis 65(4):1417–1425. https://doi.org/10.3233/JAD-180548
Teasdale GM, Nicoll JA, Murray G, Fiddes M (1997) Association of apolipoprotein E polymorphism with outcome after head injury. Lancet 350(9084):1069–1071. https://doi.org/10.1016/S0140-6736(97)04318-3
Teipel S, Gustafson D, Ossenkoppele R, Hansson O, Babiloni C, Wagner M, Riedel-Heller SG, Kilimann I, Tang Y (2022) Alzheimer disease: standard of diagnosis, treatment, care, and prevention. J Nucl Med 63(7):981–985. https://doi.org/10.2967/jnumed.121.262239
Tian C, Wang X, Wang X, Wang L, Wang X, Wu S, Wan Z (2013) Autologous bone marrow mesenchymal stem cell therapy in the subacute stage of traumatic brain injury by lumbar puncture. Exp Clin Transplant: off J Middle East Soc Organ Transplant 11(2):176–181. https://doi.org/10.6002/ect.2012.0053
Tkachenko E, Rhodes JM, Simons M (2005) Syndecans: new kids on the signaling block. Circ Res 96(5):488–500. https://doi.org/10.1161/01.RES.0000159708.71142.c8
Tsai HL, Deng WP, Lai WF, Chiu WT, Yang CB, Tsai YH, Hwang SM, Renshaw PF (2014) Wnts enhance neurotrophin-induced neuronal differentiation in adult bone-marrow-derived mesenchymal stem cells via canonical and noncanonical signaling pathways. PLoS ONE 9(8):e104937. https://doi.org/10.1371/journal.pone.0104937
Ughy B, Schmidthoffer I, Szilak L (2019) Heparan sulfate proteoglycan (HSPG) can take part in cell division: inside and outside. Cell Mol Life Sci: CMLS 76(5):865–871. https://doi.org/10.1007/s00018-018-2964-z
Ullah I, Subbarao RB, Rho GJ (2015) Human mesenchymal stem cells - current trends and future prospective. Biosci Rep. https://doi.org/10.1042/BSR20150025
van Horssen J, Kleinnijenhuis J, Maass CN, Rensink AA, Otte-Holler I, David G, van den Heuvel LP, Wesseling P, de Waal RM, Verbeek MM (2002a) Accumulation of heparan sulfate proteoglycans in cerebellar senile plaques. Neurobiol Aging 23(4):537–545. https://doi.org/10.1016/s0197-4580(02)00010-6
van Horssen J, Wilhelmus MM, Heljasvaara R, Pihlajaniemi T, Wesseling P, de Waal RM, Verbeek MM (2002b) Collagen XVIII: a novel heparan sulfate proteoglycan associated with vascular amyloid depositions and senile plaques in Alzheimer’s disease brains. Brain Pathol 12(4):456–462. https://doi.org/10.1111/j.1750-3639.2002.tb00462.x
van Horssen J, Wesseling P, van den Heuvel LP, de Waal RM, Verbeek MM (2003) Heparan sulphate proteoglycans in Alzheimer’s disease and amyloid-related disorders. Lancet Neurol 2(8):482–492. https://doi.org/10.1016/s1474-4422(03)00484-8
Veitch DP, Friedl KE, Weiner MW (2013) Military risk factors for cognitive decline, dementia and Alzheimer’s disease. Curr Alzheimer Res 9:907–930. https://doi.org/10.2174/15672050113109990142
Verbeek MM, Otte-Höller I, van den Born J, van den Heuvel LP, David G, Wesseling P, de Waal RM (1999) Agrin is a major heparan sulfate proteoglycan accumulating in Alzheimer’s disease brain. Am J Pathol 155(6):2115–2125
Wang S, Qiu Y, Bai B (2019) The expression, regulation, and biomarker potential of glypican-1 in cancer. Front Oncol 9:614. https://doi.org/10.3389/fonc.2019.00614
Wang Z, Patel VN, Song X, Xu Y, Kaminski AM, Doan VU, Su G, Liao Y, Mah D, Zhang F, Pagadala V, Wang C, Pedersen LC, Wang L, Hoffman MP, Gearing M, Liu J (2023) Increased 3-O-sulfated heparan sulfate in Alzheimer’s disease brain is associated with genetic risk gene HS3ST1. Sci Adv 9(21):eadf6232. https://doi.org/10.1126/sciadv.adf6232
Weller J, Budson A (2018) Current understanding of Alzheimer’s disease diagnosis and treatment. F1000Research 7:1161. https://doi.org/10.12688/f1000research.14506.1
Williamson J, Goldman J, Marder KS (2009) Genetic aspects of Alzheimer disease. Neurologist 15(2):80–86. https://doi.org/10.1097/NRL.0b013e318187e76b
World Health Organization. (2023). Dementia. https://www.who.int/news-room/fact-sheets/detail/dementia
Xian X, Gopal S, Couchman JR (2010) Syndecans as receptors and organizers of the extracellular matrix. Cell Tissue Res 339(1):31–46. https://doi.org/10.1007/s00441-009-0829-3
Xiao X, Liu H, Liu X, Zhang W, Zhang S, Jiao B (2021) APP, PSEN1, and PSEN2 variants in Alzheimer’s disease: systematic re-evaluation according to ACMG guidelines. Front Aging Neurosci 13:695808. https://doi.org/10.3389/fnagi.2021.695808
Xie WW, Ding YJ, Bhandari S, Li H, Chen HS, Jin SW, Weng HX, Hao Y (2024) Clinical value of syndecan-1 levels in trauma brain injury: a meta-analysis. Shock 61(1):49–54. https://doi.org/10.1097/SHK.0000000000002255
Xu Z, Robitaille AM, Berndt JD, Davidson KC, Fischer KA, Mathieu J, Potter JC, Ruohola-Baker H, Moon RT (2016) Wnt/beta-catenin signaling promotes self-renewal and inhibits the primed state transition in naive human embryonic stem cells. Proc Natl Acad Sci U S A 113(42):E6382–E6390. https://doi.org/10.1073/pnas.1613849113
Yan Y, Shin S, Jha BS, Liu Q, Sheng J, Li F, Zhan M, Davis J, Bharti K, Zeng X, Rao M, Malik N, Vemuri MC (2013) Efficient and rapid derivation of primitive neural stem cells and generation of brain subtype neurons from human pluripotent stem cells. Stem Cells Transl Med 2(11):862–870. https://doi.org/10.5966/sctm.2013-0080
Yang L, Chao J, Kook YH, Gao Y, Yao H, Buch SJ (2013) Involvement of miR-9/MCPIP1 axis in PDGF-BB-mediated neurogenesis in neuronal progenitor cells. Cell Death Dis 4:e960. https://doi.org/10.1038/cddis.2013.486
Yao H, Duan M, Yang L, Buch S (2012) Platelet-derived growth factor-BB restores human immunodeficiency virus Tat-cocaine-mediated impairment of neurogenesis: role of TRPC1 channels. J Neurosci 32(29):9835–9847. https://doi.org/10.1523/JNEUROSCI.0638-12.2012
Yu C, Griffiths LR, Haupt LM (2017) Exploiting heparan sulfate proteoglycans in human neurogenesis-controlling lineage specification and fate. Front Integr Neurosci 11:28. https://doi.org/10.3389/fnint.2017.00028
Yu C, Peall IW, Pham SH, Okolicsanyi RK, Griffiths LR, Haupt LM (2020) Syndecan-1 facilitates the human mesenchymal stem cell osteo-adipogenic balance. Int J Mol Sci. https://doi.org/10.3390/ijms21113884
Yuan S, Yu Z, Liu Q, Zhang M, Xiang Y, Wu N, Wu L, Hu Z, Xu B, Cai T, Ma X, Zhang Y, Liao C, Wang L, Yang P, Bai L, Li Y (2016) GPC5, a novel epigenetically silenced tumor suppressor, inhibits tumor growth by suppressing Wnt/beta-catenin signaling in lung adenocarcinoma. Oncogene 35(47):6120–6131. https://doi.org/10.1038/onc.2016.149
Zhang GL, Zhang X, Wang XM, Li JP (2014) Towards understanding the roles of heparan sulfate proteoglycans in Alzheimer’s disease. Biomed Res Int 2014:516028. https://doi.org/10.1155/2014/516028
Funding
Open Access funding enabled and organized by CAUL and its Member Institutions. SIP is supported by an Australian Government Research Training Program (RTP) Stipend. RKO is supported by a National Health and Medical Research Council-Australian Research Council (NHRMC-ARC) Dementia Research Development Fellowship.
Author information
Authors and Affiliations
Contributions
The concept of this manuscript was developed and drafted by SIP, RKO and LMH. SIP wrote the manuscript with RKO, LRG and LMH providing supervision in the structure, design and revision of the manuscript. All authors approved the final version.
Corresponding author
Ethics declarations
Competing Interests
The authors have no relevant financial or non-financial interests to disclose.
Ethics Approval
Not applicable.
Consent to Participate
Not applicable.
Consent for Publication
Not applicable.
Additional information
Publisher's Note
Springer Nature remains neutral with regard to jurisdictional claims in published maps and institutional affiliations.
Rights and permissions
Open Access This article is licensed under a Creative Commons Attribution 4.0 International License, which permits use, sharing, adaptation, distribution and reproduction in any medium or format, as long as you give appropriate credit to the original author(s) and the source, provide a link to the Creative Commons licence, and indicate if changes were made. The images or other third party material in this article are included in the article's Creative Commons licence, unless indicated otherwise in a credit line to the material. If material is not included in the article's Creative Commons licence and your intended use is not permitted by statutory regulation or exceeds the permitted use, you will need to obtain permission directly from the copyright holder. To view a copy of this licence, visit http://creativecommons.org/licenses/by/4.0/.
About this article
Cite this article
Petersen, S.I., Okolicsanyi, R.K. & Haupt, L.M. Exploring Heparan Sulfate Proteoglycans as Mediators of Human Mesenchymal Stem Cell Neurogenesis. Cell Mol Neurobiol 44, 30 (2024). https://doi.org/10.1007/s10571-024-01463-8
Received:
Accepted:
Published:
DOI: https://doi.org/10.1007/s10571-024-01463-8