Abstract
Previous meta-analyses have found higher self-compassion is associated with lower anxiety and depression. The aim of this study was to investigate the efficacy of self-compassion as an active ingredient in the treatment and prevention of anxiety and depression in youth. This was conducted through (i) a systematic review of the literature and (ii) qualitative consultation with young people and researchers in self-compassion. Fifty studies met our inclusion criteria. Eight studies evaluated self-compassion interventions among youth aged 14–24, and the remaining studies measured the association between self-compassion and anxiety, and/or depression among this age group. Qualitative interviews were conducted with four self-compassion researchers. Interviews were also conducted in two rounds of consultation with 20 young people (M age = 18.85 years, age range 14–24 years). Higher self-compassion was related to lower symptoms of anxiety, r = − 0.49, 95% CI (− 0.57, − 0.42), and depression, r = − 0.50, 95% CI (− 0.53, − 0.47). There was evidence for self-compassion interventions in decreasing anxiety and depression in young people. Consultation with young people indicated they were interested in self-compassion interventions; however, treatment should be available in a range of formats and tailored to address diversity. Self-compassion experts emphasised the importance of decreasing self-criticism as a reason why self-compassion interventions work. The importance of targeting self-criticism is supported by the preferences of young people who said they would be more likely to engage in a treatment reducing self-criticism than increasing self-kindness. Future research is required to add to the emerging evidence for self-compassion interventions decreasing symptoms of anxiety and depression in young people.
Similar content being viewed by others
Avoid common mistakes on your manuscript.
Introduction
There are two main approaches that underpin the study of self-compassion. Neff (2003a) proposes that self-compassion involves taking a balanced and self-supportive approach in times of difficulty and remembering one is not alone in one’s suffering. Gilbert (2017) states that compassion involves courage to engage in suffering, and wisdom on how best to act. Gilbert (2017) argues that self-criticism, defined as self-critical thoughts towards oneself (e.g., “I’m not good enough”), is a central process targeted by compassion interventions. The Self-Compassion Scale (SCS; Neff, 2003a) is the most commonly used measure of self-compassion consisting of six subscales, three representing positive factors; self-kindness, common humanity, and mindfulness and three negative factors; self-judgement, isolation, and over-identification. While many studies demonstrating a link between higher self-compassion and lower symptoms of anxiety/depression have used the SCS (Neff, 2003a), it has been argued that incorporating the negative subscales is problematic as items overlap with psychological symptoms, which over-inflates the relationship of the total self-compassion score with anxiety/depression (see Muris & Otgaar, 2020 and Neff, 2020 for a rebuttal). Further, some authors have argued self-compassion and self-kindness are distinct constructs (e.g., Gilbert et al., 2019).
Self-compassion is hypothesised to be an “active ingredient” in prevention and intervention for anxiety and depression in young people. Active ingredients refer to core aspects of psychological interventions that are effective in the prevention and treatment of anxiety and depression in young people (Wellcome Trust, 2021). Despite variation in the definition of self-compassion, it is proposed as an active ingredient for symptoms of anxiety and depression in young people on the basis of Marsh et al.’s (2018) findings in adolescents of a large effect size between higher self-compassion and lower psychological distress (including anxiety, depression and stress; r = − 0.55). Further, there is evidence for the efficacy of self-compassion interventions in reducing symptoms of anxiety and depression in youth. Some of these interventions are based on Gilbert’s Compassion Focused Therapy (CFT) and primarily focus on cognitive therapy techniques (e.g., Arimitsu, 2016; Foxx et al., 2020) while Mindful Self-Compassion (MSC) interventions are more closely aligned to Neff’s definition (e.g., Bluth et al., 2015, 2016). Previous meta-analyses have demonstrated the efficacy of self-compassion interventions (including CFT and MSC) for anxiety and depression, however none have specifically examined their efficacy among young people. Ferrari et al. (2019) conducted the most recent meta-analysis and found moderate effects of interventions on anxiety (g = 0.57) and depression (g = 0.66). However, they did not disaggregate by age, and they did not find any studies specifically with children and adolescents and therefore could not answer how self-compassion may be an active ingredient of interventions for anxiety and depression in young people. Further, Ferrari et al. (2019) only examined randomised controlled trials (RCTs) and did not report in detail on intervention content, which is critical for providing insight into for whom, and under which circumstances, self-compassion interventions work.
The aim was to synthesise the evidence and provide expert input from young people and researchers on self-compassion as an active ingredient of interventions for young people (aged 14–24) at risk of, or currently experiencing, symptoms of anxiety and depression. The overarching research question was: “drawing inferences from the current evidence: in which ways and in which contexts and for whom does your…active ingredient appear to work, and why; and in which ways and in which contexts and for whom does it appear not to work, and why?” (Wellcome Trust, 2020). While there have been meta-analyses examining self-compassion, anxiety and depression in adolescents (Marsh et al., 2018) and the efficacy of self-compassion interventions (Ferrari et al., 2019) there are no reviews integrating evidence for self-compassion in young people or that integrate the perspectives of young people. Young people aged 14–24 years were included given evidence for peak onset of psychological disorders during this period (Jones, 2018). Quantitative studies were examined in a systematic review, and where applicable, a meta-analysis, in addition to consultation with young people and researchers.
Methods
Search Strategy and Selection Criteria
The literature search using the search terms and in Table 1, was conducted on 15 June 2020 in Embase, PubMed/Medline, PsycINFO and Web of Science. Inclusion criteria were (a) in English; (b) used self-compassion or self-kindness for a significant part of an intervention, defined as at least 75% or more of the sessions containing a focus on self-compassion as judged by the senior authors who are experienced clinicians in self-compassion interventions (SE and CR), (c) measured self-compassion as well as symptoms of depression and/or anxiety (including related symptoms e.g., worry, trauma); (d) included participants aged range between 14 and 24 years (or if age range not available through the journal article and author contact, reported a mean age between 14 and 24); and (e) published between 1 January 1980 and 15 June 2020. The restriction of 1980 onwards was chosen due to limited self-compassion research prior to this year, as evidenced by only 18 search results prior to this year, with none of these studies measuring self-compassion. For intervention studies, there were no limits regarding timepoints for measurement, i.e., studies could include either post treatment or both pre-post treatment measurements. The exclusion criterion was single case designs. Grey literature and desk-drawer studies were also sought through emails sent to self-compassion researchers for in-preparation manuscripts. The inclusion criteria were applied to title and abstracts in the initial screening stage to remove duplicates and papers that were clearly out of range, for example not a study of self-compassion by MW). After this initial screening stage, full text screening was applied to all papers by MW.
Procedure
The PRISMA statement (Page et al., 2021) was followed and the protocol registered on PROSPERO in June 2020 (CRD42020188990). Article screening was conducted by MW, and a random 30% by DG, who had near perfect agreement (96%: Cohen’s Kappa = 0.90, p < 0.001). Discrepancies were resolved by SE and CR. The determination of whether an intervention was self-compassion was critical in the screening and selection of papers. All papers that were potentially relevant even if they did not explicitly label the intervention as self-compassion were carefully reviewed in terms of content by the senior authors who are experts in self-compassion. This involved reviewing journal article text and tables of session content for the intervention to determine through this clinical and research expertise in self-compassion that the intervention was indeed a self-compassion intervention. Where available through author contact, full treatment manuals for the interventions were also examined to determine the treatment content. The criteria of the intervention containing 75% content which was a self-compassion intervention was coded as “yes” or “no” to the 75% criteria. There was 100% agreement between the two senior authors (SE and CR) and no discrepancies, therefore inter-rater reliability in these ratings were not calculated.
A meta-analysis was conducted for associations between self-compassion and both anxiety and depression (i.e., question 2) in JASP (JASP Team, 2020). Hedges random effects model was used to pool the correlation coefficients across-studies (Hedges & Olkin, 1985). Study quality, as assessed by the National Institutes of Health (2014) Quality Assessment tools, measure of anxiety/depression and country were assessed as moderators in a meta-regression for both associations. Measure of anxiety/depression was chosen as a moderator because the method of measuring anxiety/depression differed across the studies (e.g., trait, state, social anxiety). Country was chosen as a moderator because culture and other location-based norms might impact the associations between self-compassion and both anxiety and depression (e.g., Neff et al., 2008). All moderators were dummy coded to contrast effect sizes across different groups of studies. Study quality was coded as follows, 1 = low (reference category), 2 = fair, and 3 = high. For measure of anxiety/depression and country a reference category had to be determined. We chose the reference category to be the category with the largest number of effect sizes. This was determined to be the STAI for anxiety and the BDI for depression. USA was entered as the referenced category for both meta-regressions for the country variable. We did not conduct a meta-analysis on intervention effects due to there being too few studies (less than 10; Watson et al., 2016).
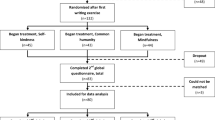
Interviews were conducted with four research experts in self-compassion (see Table 2)—Neff, Bluth, Ferrari and Gilbert. A Youth Advisory Group (YAG) of 20 young people aged 14–24 (see Table 3 for details) were consulted at two stages (see Table 4). The first consultation with youth was conducted in July 2020. In the second consultation (August 2020), feedback was sought on a summary of research findings (see Supplementary Material Table 1) which was emailed 5 days prior to the interview. Young people were given an AUD$95 Amazon voucher. The Youth Advisory Group was recruited in Australia via social media, word of mouth and email, and did not report having previously engaged in self-compassion interventions. Consent was received from people over 16 years, or from their parents if they were under 16. Interviews were conducted on Zoom either individually or in focus groups, depending on preference. The interviews were conducted by two research assistants, one of whom was an undergraduate psychology student, and the other a registered clinical psychologist with extensive experience in engagement of young people in clinical practice. The interviews were structured and included all questions in Table 4, which were asked in both the individual interviews and focus groups.
Interviews with the researchers and youth were transcribed and the results were analysed following guidelines for thematic analysis of Braun and Clarke (2006). The six steps of thematic analysis outlined by Braun and Clarke (2006) were followed. For example, the transcripts were examined by the author who conducted the qualitative analysis (JD) and the main ideas were described that emerged with key words, then ideas were grouped into overarching themes. To ensure quality and rigour of the process, initial themes were discussed with two senior authors (SE and CR) before being finalised. The researcher who conducted the thematic analysis (JD) selected quotations from transcripts that best represented the theme in question as per Braun and Clarke’s (2006) recommendations.
Results
Search Summary and Study Characteristics
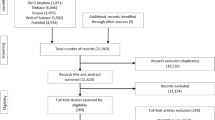
The search yielded 6506 results. After the removal of duplicates, 3922 studies were screened by title and abstract. Full-text screening was undertaken for 930 studies, as outlined in Fig. 1. A total of 49 studies (46 articles) met inclusion criteria. Just under half of the studies were from the USA (n = 23), thereafter a range of countries including China (n = 5), Japan (n = 5) and (n = 2) in Australia, Belgium, Canada, Portugal. There were single studies in 8 other countries (see Table 5). Pooled sample size was 21,792 (~ 60% female).
Quality Ratings
Quality ratings ranged from 28.57 to 90.91%, using the National Institutes of Health (2014) Quality Assessment tools, see Table 6. For the purposes of the meta-analysis for question 2, studies were coded based on quality as follows: (50% > poor, 51–74.99%- fair, and 75% < good).
Research Questions:
-
(1)
Do self-compassion interventions demonstrate efficacy for symptoms anxiety and depression in young people?
As seen in Table 5, eight studies (six RCTs, two open trials) examined self-compassion interventions in young people. Two studies were with adolescents (Bluth et al., 2015, 2016), and six with university students. Six of the eight studies (Armitsu, 2016; Bluth et al., 2015, 2016; Burke et al., 2020; Ko et al., 2018; Smeets et al., 2014) were group-based interventions, the remaining two interventions were individual lab-based studies where participants listened to the intervention on a computer (Arch et al., 2014; Polizzi et al., 2019). In terms of who provided the interventions, five of the eight studies were delivered by therapists who were trained in self-compassion (Armitsu, 2016; Bluth et al., 2015, 2016; Burke et al., 2020; Smeets et al., 2014), two were delivered by researchers in lab-based studies (Arch et al., 2014; Polizzi et al., 2019), and one study was delivered by a university lecturer (Ko et al., 2018). Of the eight studies, only two were targeted at either low-self-compassion (Arimutsu, 2016) or mild-moderate depressive symptoms (Burke et al., 2020), the remainder were not specifically reported as prevention or treatment studies. Of the eight intervention studies, three had relatively large sample sizes suggesting they were adequately powered (Arch et al., 2014; Burke et al., 2020; Polizzi et al., 2019), given the relatively small sample sizes of the remainder (see Table 5), it is likely that they were underpowered. See supplementary Tables 4, 5, 6, 7 for detailed examples of intervention content for five of the eight included studies (Arch et al., 2014; Arimitsu, 2016; Bluth et al., 2015, 2016; Burke et al., 2020), not all interventions are detailed due to consideration of length.
Bluth et al. (2015) examined a six-session self-compassion group intervention in community adolescents not selected for elevated anxiety/depression. This was an open trial but found significant reductions in stress and increases in self-compassion. A further waitlist-controlled crossover trial in adolescents conducted by Bluth et al. (2016) found the intervention group demonstrated medium effect size reductions in anxiety and depression.
Some studies examining university students included very brief interventions. Arch et al. (2014) examined the impact of a brief, two-session self-compassion intervention consisting of meditation practices in female university students, and found significantly decreased anxiety, as well as reduced sympathetic and cardiac parasympathetic responses to a social stress test, compared to attention placebo and control conditions. In contrast, Polizzi et al. (2019) found no impact of a two-session loving-kindness meditation intervention in university students on worry or depression and concluded the intervention was too brief (12 min per session). Smeets et al. (2014) examined a three-session self-compassion group intervention with female university students, and found compared to an active control, the intervention group demonstrated a medium effect size reduction in rumination, however there was no significant change in worry or negative affect. However, in an open trial evaluating a four-session group self-compassion intervention with university students with elevated depressive symptoms in the UK, Burke et al. (2020) found pre-post reductions in anxiety and depression.
Two RCTs with university students examined longer interventions. Arimitsu (2016) examined a seven-session self-compassion intervention (including loving-kindness meditation, mindfulness training and compassionate mind training) with Japanese university students who had low self-compassion on the total score of the SCS (Neff, 2003a). Significant decreases were observed in depressive and anxious symptoms compared to controls, maintained at three-month follow-up. However, with 28 participants, this study was underpowered. Ko et al. (2018) found an intervention in university students consisting of 30 seminars on self-compassion had no impact on anxiety or depression.
-
(2)
Is self-compassion associated with anxiety and depression in young people?
Forty articles reported on the associations between self-compassion and anxiety and/or depression (see Table 5). Articles were mostly cross-sectional (n = 32) with a small number of longitudinal studies (n = 5) and three controlled trials reporting relevant correlations at baseline. The majority of studies were with university students (n = 28). Seven studies comprised high school student samples and three were community samples. The remaining two samples were hospital outpatients (treated for migraine), and adolescents involved with child protection/welfare. Thirty-four articles with 39 samples provided sufficient data to calculate effect sizes for the associations between self-compassion (total score) and anxiety and/or self-compassion (total score) and depression. Twenty-one effect sizes were pooled for the anxiety association and 37 for depression association.
Across studies, significant negative correlations between self-compassion and anxiety were reported, ranging from r = − 0.19 to − 0.75, with a moderate-to-large, pooled effect size [Pooled r = − 0.49, 95% CI (− 0.57, − 0.42), p < 0.001]. However, heterogeneity was high [Q (20) = 273.37, p < 0.001, I2 = 93.42%], thus, we ran a meta-regression entering study quality, country, and measure of anxiety as moderators (Table 7). These three variables accounted for the heterogeneity across studies [Q (5) = 7.60, p = 0.18, I2 = 0.00%]. Specifically, high study quality accounted for a significant amount of variance in effect size and was associated with significantly smaller effect sizes than low study quality. Second, the DASS, BAI, and the SCL accounted for significant variance in effect sizes and were associated with significantly larger effects than the STAI. Lastly, studies taking place in Japan, Portugal, and Belgium accounted for a significant amount of variance in effect sizes and were associated with significantly larger effect sizes compared to studies taking place in the USA. However, these moderation effects should be considered with caution, due to the low number of studies for each category.
Table 7 Meta-regressions for the associations between self-compassion and anxiety (left), and self-compassion and depression (right) The results for depression were similar, with significant negative correlations between self-compassion and depression, (r = − 0.30 to − 0.63), with a moderate-large, pooled effect size [Pooled r = − 0.50, 95% CI (− 0.53, − 0.47), p < 0.001]. However, again, heterogeneity was high [Q (36) = 255.16, p < 0.001, I2 = 78.13%]. Country and measure of depression accounted for majority of the heterogeneity across studies [Q (14) = 23.99, p = 0.046, I2 = 10.32%: Table 7]. Specifically, the SMFQ and SCL accounted for a significant amount of variance in effect sizes. The SMFQ was associated with significantly larger effect sizes, whereas the SCL was associated with significantly smaller effect sizes, compared to the BDI. Second, studies taking place in Australia, Norway, and Japan accounted for significant variance in effect sizes. Studies taking place in Australia and Norway were associated with significantly larger effect sizes, whereas studies taking place in Japan were associated with significantly smaller effect sizes, compared to studies taking place in the USA. However, these moderation effects should be considered with caution, due to the low number of studies for each category.
-
(3)
How do young people experience self-compassion and how does this relate to their experience of anxiety and depression?
Feedback from Youth Advisory Group (stage 1):
Numerous themes emerged from the first advisory group (see Table 8 and Supplementary Table 2).
Theme 1. Self-compassion as the opposite of self-criticism
Nearly all the young people (95%) identified that self-criticism acted as a barrier to practicing self-compassion due to fears it would lead to decreased performance and mean having to sacrifice on their goals and achievements. One young person said self-compassion would “prevent her from trying to strive for excellence” (Female, 24 years old, Participant 8). Another said: “It feels counterintuitive to try to have compassion for yourself when there’s another part of you that’s like if you just bully yourself enough maybe you’ll get up and get on with the day”. (Non-binary, 19 years old, Participant 18).
Some young people (35%) associated self-compassion with being “weak” or “lazy”, others said other concepts like self-care and self-love had a “cringe” factor, for example: “I think definitely as a teenager it’s a little bit stigmatised as you’re weak or it’s a little bit cringy maybe to try and do these things for yourself”. (Female, 16 years old, Participant 12).
Young people said it was difficult to practice self-compassion in moments of high distress. Although they recognised its benefits, they identified that a significant mindset shift would be required to switch from an experience of anxiety and depression, characterised in large part by self-criticism, to being self-compassionate.
Young people talked about self-compassion as a method of coping with failure and reducing self-criticism, defining self-compassion as “being compassionate towards your own failure”. Young people also identified self-compassion as a helpful tool to disengage from negative thoughts and improve self-worth. Some said having more self-compassion would mean being “less likely to be anxious and depressed” and would “make it easier to control anxiety”. Many young people (75%) identified that self-compassion would reduce negative self-talk, for example: “If you want to judge yourself fairly then you have to be kind to yourself because you can't judge yourself fairly if you're always being harsh on yourself.” (Male, 17-year-old, Participant 6).
Theme 2. Young people’s understanding and awareness of self-compassion
The majority (85%) of young people had limited exposure to self-compassion, five assumed self-compassion to be synonymous with or similar to self-care. Young people stressed the importance of raising awareness of self-compassion:
“I think you need to get the concept out there, none of us really knew about what self-compassion was…” (Female, 16 years old, Participant 12).
From their understanding of self-compassion, young people largely felt it would help reduce and prevent symptoms of anxiety and depression.
“If you learn how to have self-compassion, and learn how to treat yourself better, it can probably help with symptoms of anxiety and depression.” (Male, 14 years old, Participant 2).
Young people identified that family background, culture and relationships played a large part in awareness of self-compassion, and ability to practice it:
“Asian people, we grow in families that often are more critical and so with a family background like that, understandably you develop a habit of criticising yourself, and it's harder for us to practice self-compassion.” (Female, 24 years old, Participant 8).
Theme 3. Preferences for self-compassion programmes
Most young people (90%) felt self-compassion programmes would be helpful to prevent and treat anxiety and depression, especially in decreasing self-critical thoughts. One 22-year-old male said a programme would help “as a framework to allow someone to reframe their thought process” (Participant 9). Preferences for intervention formats varied. Some chose an online programme or an app, while others preferred face-to-face interventions—either one-on-one or in a group. A common theme was that young people wanted to feel they could apply strategies to suit their own individual challenges. Rather than a “cookie-cutter” solution, they wanted to feel that the programme was targeted, for example:
"I think [researchers] should consider that, it would be quite different for different people, like they might struggle with different things depending on their experiences." (Female, 14 years old, Participant 5).
Young people suggested tailoring programmes to specific minority groups, including cultural minorities and LGBTQIA + individuals. Young people also warned researchers should be aware of how certain words and behaviours come across. The word “intervention”, for example, was associated with drug or alcohol interventions in movies and television. Participants also warned against programmes where adults try to sound “cool”, as the attempt at relatability usually falls short.
“…terms like self-compassion, self-love, mindfulness, they sort of, they feel like buzzwords to people, and in a way have negative connotations because of that.” (Female, 21 years old, Participant 13).
(4) How do experts in self-compassion research view self-compassion as an active ingredient in youth?
Research experts said self-compassion is the same regardless of age, however developmental differences might mean the concept needs to be explained differently depending on age. They believed self-compassion could help young people experiencing anxiety by providing a feeling of safety and preventing overidentification and rumination. In relation to depression, self-compassion could help improve self-acceptance.
“When you start being kind to yourself and realising that you’re imperfect…that everyone’s imperfect, that life is imperfect, and you stop being attached to things being a certain way and you accept yourself as you are, then you stop judging yourself so much, you start accepting yourself more, and that directly reduces depression.” Neff (2020).
Self-compassion was believed to work as an active ingredient by targeting mechanisms like self-criticism, central to anxiety and depression.
“…rumination and self-criticism are core maintaining factors for (depression)… I think self-compassion directly targets the mechanisms that maintain depression.” Ferrari (2020).
A key barrier was the misinterpretation of self-compassion as an act of laziness, or that self-criticism is necessary to push oneself, for example:
“[Young people] are raised with this idea that in order to be successful… they have to be hard on themselves, they have to beat themselves up. So the idea that they can actually be kind to themselves and achieve what they’re supposed to achieve in life—meaning getting into a good college, eventually getting a good job—it’s eye opening to them that they can do that”. Bluth (2020).
Gilbert raised the importance of distinguishing between self-compassion and self-kindness. Unlike self-kindness, which focuses primarily on the promotion of wellbeing, self-compassion requires courage and wisdom—courage to recognise and engage with your own pain and suffering rather than turning away from it, and wisdom to differentiate between helpful and harmful behaviours in moments of distress.
“We find that clinically, self-compassion enables people to develop the courage and strengths they need, along with the capacity to think empathically and gain insight into ‘what my pain is about’, learning to tolerate those feelings and make sense of them, and then working out wise ways of dealing with them. While obviously useful and important, kindness does not involve that courageous and wise engagement with suffering. So when you really dig into the issue of suffering, we have to descend and enter into it not away from it, that’s compassion”. Gilbert (2020).
Experts said group interventions work particularly well for young people, and highlighted the value of psychoeducation for young people in their late teens and early 20s.
(5) How do young people view the review, and what are their recommendations for interventions focused on self-compassion?
Three themes emerged in the second consultations (see Table 9 and supplementary Table 3).
Theme 1. Research and expert opinions were relevant to lived experience of anxiety and depression
Research findings about changes in depression and anxiety being related to changes in self-criticism, rather than self-kindness, were particularly relevant for young people. Six young people (30%) were interested in this finding specifically. They said the idea that reduced self-criticism is related to less anxiety and depression made sense. A point raised by Gilbert, which described self-compassion in terms of courage and wisdom, also strongly resonated with young people. Young people found this idea noteworthy and engaging, and felt framing a programme in this way—rather than with a focus on “self-kindness” and “self-compassion”—would be more appealing.
“I think that for me if someone would say, you should practice self-compassion, I would be like, ah, I don't know. But if someone would relate it to wisdom and you’d be a lot wiser and more courageous, I think that would appeal to me more.” (Female, 21 years old, Participant 10).
Theme 2. The relative novelty of self-compassion means it might take time for it to garner credibility among young people
Some of the young people (55%) stressed the importance of differentiating between terms like self-compassion, self-care, self-love, self-kindness and mindfulness. They said providing definitions of these key terms would help provide clarity on what self-compassion actually is, and consequently increase interest in self-compassion programmes. There was also confusion about what self-compassion programmes would look like in practical terms.
“I'm kind of struggling to see what the actual programme would entail. I kind of understand the basis of it but I can't really see like the final, like how it would look like in the end.” (Female, 21 years old, Participant 10).
Most young people (80%) said that now they knew more about it, they recognised the merits of self-compassion to reduce anxiety and depression. However, they said others who were not familiar might not respond this way. Young people said time and focus should be spent raising awareness of self-compassion and dispelling some of the misconceptions around it (e.g., associations with self-indulgence and laziness).
“Self-compassion is maybe a bit of a new concept and might take people some time to warm up to it…” (Female, 24 years old, Participant 11)
Seven young people (35%) mentioned being involved in the research process and learning more about self-compassion had raised their interest to the point where they would actively engage with a self-compassion programme.
Theme 3. Self-compassion programmes are appealing but initial engagement can be difficult
A large proportion of the young people (75%) said information about mental health concepts should be dynamic—using videos and/or animation—reasonably brief and tailored to individuals. Young people stressed the importance of tailoring programmes and methods of engagement to individuals or groups, with particular consideration for family environment, culture, sexual identity and specific challenges faced. They had a range of ideas for how to engage young people with self-compassion programmes—for example, while some said a video would be good, others said it would be too impersonal.
Young people said consideration should be given to the platforms used to promote mental health concepts and/or programmes. While social media may reach a wide audience, most said they were unlikely to engage with serious content on such platforms.
“I definitely think social media is a big one. But I think you run the risk of people just scrolling past it… A lot of serious topics on social media, people don't really want to look through…” (Female, 16 years old, Participant 12).
Young people responded positively to a suggestion for a short quiz, linked from social media, to help them determine how self-compassionate they are or how much they would benefit from a self-compassion programme.
“I think (a quiz) is an acknowledgement that it's not the same for everyone, obviously we've talked a lot about that, but it can't be the same programme…it will pay attention to you and what you need.” (Female, 21 years old, Participant 13).
Discussion
The purpose of this review was to synthesise the existing literature and expert opinion (young people and researchers), to determine evidence for self-compassion as an active ingredient of interventions for symptoms of anxiety and depression in youth. We believe that combining evidence from these sources provided a comprehensive and inclusive approach to answering the overarching research question about how the proposed active ingredient of self-compassion may or may not work, and why.
What Works?
There is some evidence that interventions to increase self-compassion reduce symptoms of anxiety and depression in young people aged 14–24, when the intervention is of a sufficient length (minimum 4 sessions) and when it is a specific self-compassion intervention, as opposed to brief (e.g., 2 sessions) mindfulness training. Evidence was found to support group and individual formats, in both high school and university settings. However, these conclusions should be considered cautiously due to a number of limitations. First, there have only been a small number of controlled trials conducted to date. Second, while we judged the content of the intervention as self-compassion based on treatment manuals where possible, some were on the basis of more limited information contained in the publication. Future research should judge interventions as being self-compassion based on treatment manuals for all studies. Third of the trials conducted, the majority had small samples sizes and are likely to have been underpowered. Fourth, most studies were not treatment studies targeting elevated symptoms of anxiety and depression and were not prevention trials. Consequently, this limits generalisations regarding the efficacy of self-compassion interventions in young people. Future research on self-compassion interventions should examine mediation to determine which are the effective elements of treatment in young people. Fifth, we did not include qualitative studies in the review due to the limited number of studies, and future reviews should seek to include these in order to generalise results more broadly to young people beyond those who were consulted in this study. There is a need for more qualitative studies, particularly given the importance of increasing youth involvement in the co-creation and development of interventions for anxiety and depression. Finally, a limitation is that higher study quality was associated with smaller effect sizes when examining associations between self-compassion and anxiety. This limitation of study quality, in combination with the limited number of controlled and repeated-measure designs, indicates that the pooled effect sizes may have been slightly inflated and should therefore be interpreted relative to these limitations.
What Does Not Work?
Brief mindfulness and loving-kindness training did not appear to work. Additionally, an important barrier to engagement identified through consultation was the belief that self-criticism helps achievement, and this should be addressed in future self-compassion interventions.
Young People’s Recommendations
Young people were unanimous that self-compassion was relevant to their experience of anxiety and depression. Importantly, young people identified self-compassion as being opposite to self-criticism. They explained the idea of being kind to yourself and recognising that everyone struggles is hard when your usual mindset is focused on goals and striving for excellence. Young people felt more programmes were needed to teach self-compassion, and these should be tailored to individual preferences in delivery (e.g., group, individual, online) and be inclusive of diversity in gender, culture, sexuality and individual experiences. Both young people and researchers recognised that adolescence is a ‘powerful moment’ to learn about self-compassion because young people face numerous developmental challenges and stressors. Indeed, young people highlighted family pressures, exam pressures and general stress making it harder to be self-compassionate.
There are several limitations of the youth consultation we engaged in. It is important to note that the Youth Advisory Group did not report previous engagement in self-compassion interventions. We did not specifically seek young people to engage in the consultation process who had completed a self-compassion intervention, and this is a limitation as it may have been difficult for young people to share their views on an intervention of which they did not have experience. Despite this limitation, young people’s lived experience of anxiety and depression provided important and meaningful insights regarding self-compassion, for example, with some commenting on the negative connotation of words like ‘self-compassion’, which is important for researchers to consider when engaging young people in interventions. Another limitation is that we did not ask young people for details of their race or ethnicity, and the Youth Advisory Group were all from Australia. Hence the findings should be considered in the context of the views of young people in a high-income country. Future research should seek to engage young people from a broader geographical area, including low- and middle-income countries. A final limitation is that some of the interview questions asked questions such as whether the young person thinks self-compassion relates to their own, or their friends, experiences of symptoms of anxiety or depression. It is possible that because the interviews were conducted by research assistants employed in the study that young people may potentially have thought the interviewers had a vested interest in this research question, so may have been more likely to say yes to these types of questions. Hence, this potential limitation of young people potentially agreeing with the questions should be considered, and future research should seek to consult young people from another perspective, for example, with young people with lived experience of anxiety and depression leading the consultation process rather than research assistants.
Future Research Directions and Policy Implications
Despite some debate over definition, a positive feature of the literature was self-compassion was measured consistently, with all but one study using the SCS (Neff, 2003a). This consistency in measurement strengthens conclusions regarding self-compassion, as averaging the findings across the same scale means that the studies were measuring self-compassion in the same way. As noted in previous meta-analyses (Marsh et al., 2018), higher self-compassion was related to lower symptoms of anxiety, r = − 0.49, 95% CI (− 0.57, − 0.42), and depression, r = − 0.50, 95% CI (− 0.53, − 0.47). Nevertheless, while we did not predetermine the particular definition of self-compassion that would be used in the review, the use of the SCS (Neff, 2003a) in almost all studies included may have resulted in the findings being more closely aligned with Neff’s (2003a) definition. Hence, future reviews may seek to include a broader range of measures of self-compassion which are in line with other definitions of compassion, such as Gilbert (2017).
There were few intervention studies specifically focused on building self-compassion with young people, and few controlled trials of specific self-compassion interventions (e.g., Arimistu, 2016; Bluth et al., 2016). Based on feedback from young people, future self-compassion programmes need to be available in multiple formats (online, individual, group) as there is no ‘one size fits all’ for preferred mode of delivery. Also, self-compassion programmes should be co-designed with young people and using language they find appropriate (e.g., not using the word ‘intervention’). Future research should compare self-compassion treatments with active treatments, such as Mindfulness Based Cognitive Therapy, or CBT for perfectionism which has efficacy for anxiety and depression in adolescents (e.g., Shu et al., 2019) and focuses on reducing self-criticism, and examine changes in self-compassion. Treatment trials with larger samples are needed as most were small. Trials that include young people with elevated anxiety and depression are required as well as longer follow-up periods, since only one study to date included young people with elevated depressive symptoms (Burke et al., 2020). Future research should also compare the efficacy of self-compassion interventions in adolescents compared to young adults, given studies of psychotherapy for depression have indicated greater effects in young adults than adolescents (Cuijpers et al., 2020).
Engagement with young people in the review process was critical as their views have highlighted the importance of targeting self-criticism in a manner which is seen as acceptable and does not detract from their ability to succeed and attain their goals. The findings highlight the importance of future research maximizing youth involvement in developing and tailoring interventions, with young people as co-researchers who design the interventions. Further, while the findings of our consultation with young people and researchers highlighted some important mechanisms by which they view self-compassion may influence symptoms of anxiety and depression, such as increasing self-acceptance and decreased rumination, on the basis of the results of the systematic review component, questions of how and for whom self-compassion interventions work need to be explored in future research. This is particularly important given the various definitions of self-compassion and intervention approaches in the literature, to improve understanding of reasons for the associations between self-compassion and anxiety/depression in young people.
Conclusions
There is clear evidence that higher self-compassion is associated with lower anxiety and depression in young people. Young people recognise the importance of self-compassion in relation to anxiety and depression and in particular, noted the need for tailored treatments which are inclusive and address diversity. Further controlled trials of self-compassion intervention programmes are required to add to the emerging evidence that increasing self-compassion in young people reduces anxiety and depression.
References
*Denotes articles included in the review
*Arch, J. J., Warren Brown, K., Dean, D. J., Landy, L. N., Brown, K., & Laudenslager, M. L. (2014). Self-compassion training modulates alpha-amylase, heart rate variability and subjective responses to social evaluative threat in women. Psychoneuroendocrinology, 42, 49–58. https://doi.org/10.1016/j.psyneuren.2013.12.018
*Arimitsu, K. (2016). The effects of a program to enhance self-compassion in Japanese individuals: A randomised controlled trial. The Journal of Positive Psychology, 11, 559–571. https://doi.org/10.1080/17439760.2016.1152593
*Arimitsu, K., & Hofmann, S. G. (2015). Cognitions as mediators in the relationship between self-compassion and affect. Personality and Individual Differences, 74, 41–48. https://doi.org/10.1016/j.paid.2014.10.008
*Asano, K., Kotera, Y., Tsuchiya, M., Ishimura, I., Lin, S. Z., Matsumoto, Y., Matos, M., Basran, J., & Gilbert, P. (2020). The development of the Japanese version of the compassionate engagement and action scales. PLoS ONE. https://doi.org/10.1371/journal.pone.0230875
*Bluth, K., Roberson, P. N. E., & Gaylord, S. A. (2015). A pilot study of a mindfulness intervention for adolescents and the potential role of self-compassion in reducing stress. Explore, 11, 292–295. https://doi.org/10.1016/j.explore.2015.04.005
*Bluth, K., Gaylord, S. A., Campo, R. A., Mullarkey, M. C., & Hobbs, L. (2016). Making friends with yourself: A mixed methods pilot study of a mindful self-compassion program for adolescents. Mindfulness, 7, 479–492. https://doi.org/10.1007/s12671-015-0476-6
*Bluth, K., Campo, R., Futch, W., & Gaylord, S. (2017). Age and gender differences in the associations of self-compassion and emotional wellbeing in a large adolescent sample. Journal of Youth and Adolescence, 46, 840–853.
Braun, V., & Clarke, V. (2006). Using thematic analysis in Psychology. Qualitative Research in Psychology, 3, 77–101. https://doi.org/10.1191/1478088706qp0630a
*Burke, A. S., Shapero, B. G., Pelletier-Baldelli, A., Deng, W. Y., Nyer, M. B., Leathem, L., Namey, L., Landa, C., Cather, C., & Holt, D. J. (2020). Rationale, methods, feasibility and preliminary outcomes of a transdiagnostic prevention program for at-risk college students. Frontiers in Psychiatry. https://doi.org/10.3389/fpsyt.2019.01030
*Castilho, P., Carvalho, S. A., Marques, S., & Pinto-Gouveia, J. (2017). Self-compassion and emotional intelligence in adolescence: A multigroup mediational study of the impact of shame memories on depressive symptoms. Journal of Child and Family Studies, 26, 759–768. https://doi.org/10.1007/s10826-016-0613-4
Cuijpers, P., Karyotaki, E., Eckshtain, D., Ng, M. Y., Corteselli, K. A., Noma, H., Quero, S., & Weisz, J. R. (2020). Psychotherapy for depression across different age groups: A systematic review and meta-analysis. JAMA Psychiatry, 77, 694–702. https://doi.org/10.1001/jamapsychiatry.2020.0164
*Cunha, M., Xavier, A., & Castilho, P. (2016). Understanding self-compassion in adolescents: Validation study of the self-compassion scale. Personality and Individual Differences, 93, 56–62. https://doi.org/10.1016/j.paid.2015.09.023
*Ferrari, M., Yap, K., Scott, N., Einstein, D. A., & Ciarrochi, J. (2018). Self-compassion moderates the perfectionism and depression link in both adolescence and adulthood. PLoS ONE. https://doi.org/10.1371/journal.pone.0192022
Ferrari, M., Hunt, C., Harrysunker, A., Abbott, M. J., Beath, A. P., & Einstein, D. A. (2019). Self-compassion interventions and psychosocial outcomes: A meta-analysis of RCTs. Mindfulness, 10, 1455–1473. https://doi.org/10.1007/s12671-019-01134-6
Foxx, J., Cattani, K., & Burlingame, G. M. (2020). Compassion focused therapy in a university counselling and psychological services center: A feasibility trial of a new standardized group manual. Psychotherapy Research. https://doi.org/10.1080/10503307.2020.1783708
*Galla, B. M. (2016). Within-person changes in mindfulness and self-compassion predict enhanced emotional well-being in healthy, but stressed adolescents. Journal of Adolescence, 49, 204–217. https://doi.org/10.1016/j.adolescence.2016.03.016
*Garcia-Campayo, J., Navarro-Gil, M., Andres, E., Montero-Marin, J., Lopez-Artal, L., & Demarzo, M. M. P. (2014). Validation of the Spanish versions of the long (26 items) and short (12 items) forms of the self-compassion scale (SCS). Health and Quality of Life Outcomes. https://doi.org/10.1186/1477-7525-12-4
*Ghorbani, N., Watson, P. J., Chen, Z., & Norballa, F. (2012). Self-compassion in Iranian muslims: Relationships with integrative self-knowledge, mental health, and religious orientation. International Journal for the Psychology of Religion, 22, 106–118. https://doi.org/10.1080/10508619.2011.638601
Gilbert, P. (2017). Compassion: Definitions and controversies. In P. Gilbert (Ed.), Compassion: Concepts, research and applications (pp. 3–15). Routledge.
Gilbert, P., Basran, J., MacArthur, M., & Kirby, J. N. (2019). Differences in the semantics of prosocial words: An exploration of compassion and kindness. Mindfulness, 10, 2259–2271. https://doi.org/10.1007/s12671-109-01191-x
*Gill, C., Watson, L., Williams, C., & Chan, S. W. Y. (2018). Social anxiety and self-compassion in adolescents. Journal of Adolescence, 69, 163–174. https://doi.org/10.1016/j.adolescence.2018.10.004
*Hall, C. W., Row, K. A., Wuensch, K. L., & Godley, K. R. (2013). The role of self-compassion in physical and psychological well-being. Journal of Psychology, 147, 311–323. https://doi.org/10.1080/00223980.2012.693138
Hedges, L. V., & Olkin, I. (1985). Statistical methods for meta-analysis. Academic Press.
*Hou, X. L., Bian, X. H., Zuo, Z. H., Xi, J. Z., Ma, W. J., & Owens, L. D. (2020). Childhood maltreatment on young adult depression: A moderated mediation model of negative automatic thoughts and self-compassion. Journal of Health Psychology. https://doi.org/10.1177/1359105320918351
JASP Team (2020). JASP (Version 0.14.1) [Computer software].
Jones, P. B. (2018). Adult mental health disorders and their age of onset. British Journal of Psychiatry, 202, 5–10. https://doi.org/10.1192/bjp.bp.112.119164
*Kemper, K. J., Heyer, G., Pakalnis, A., & Binkley, P. F. (2016). What factors contribute to headache-related disability in teens? Pediatric Neurology, 56, 48–54. https://doi.org/10.1016/j.pediatrneurol.2015.10.024
*Ko, C. M., Grace, F., Chavez, G. N., Grimley, S. J., Dalrymple, E. R., & Olson, L. E. (2018). Effect of seminar on compassion on student self-compassion, mindfulness and well-being: A randomized controlled trial. Journal of American College Health, 66, 537–545. https://doi.org/10.1080/07448481.2018.1431913
*Lathren, C., Bluth, K., & Park, J. (2019). Adolescent self-compassion moderates the relationship between perceived stress and internalizing symptoms. Personality and Individual Differences, 143, 36–41. https://doi.org/10.1016/j.paid.2019.02.008
*Luo, Y., Meng, R., Li, J., Liu, B., Cao, X., & Ge, W. (2019). Self-compassion may reduce anxiety and depression in nursing students: A pathway through perceived stress. Public Health, 174, 1–10. https://doi.org/10.1016/j.puhe.2019.05.015
Marsh, I. C., Chan, S. W. Y., & MacBeth, A. (2018). Self-compassion and psychological distress in adolescents: A meta-analysis. Mindfulness, 9, 1011–1027. https://doi.org/10.1007/s12671-017-0850-7
*Mingkwan, A., Ratta-Apha, W., Phattharayuttawat, S., Imaroonrak, S., Sumalrot, T., & Auampradit, N. (2018). The relationship between self-compassion and mental health in naresuan university students. Journal of the Medical Association of Thailand, 101(1 Supplement 1), S51-S56. Retrieved from http://www.jmatonline.com/index.php/jmat/article/viewfile/9339/8112
*Miron, L. R., Seligowski, A. V., Boykin, D. M., & Orcutt, H. K. (2016). The potential indirect effect of childhood abuse on posttrauma pathology through self-compassion and fear of self-compassion. Mindfulness, 7, 596–605. https://doi.org/10.1007/s12671-016-0493-0
Muris, P., & Otgaar, H. (2020). The process of science: A critical evaluation of more than 15 years of research on self-compassion with the self-compassion scale. Mindfulness, 11, 1469–1482. https://doi.org/10.1007/s12671-020-01363-0
National Institutes of Health. (2014). Quality Assessment Tool for Cross-Sectional and Observational Studies. Retrieved from 22 August 2020, https://www.nhlbi.nih.gov/health-topics/study-quality-assessment-tools.
Neff, K. D. (2003a). Self-compassion: An alternative conceptualization of a healthy attitude toward oneself. Self and Identity, 2, 85–101. https://doi.org/10.1080/15298860309032
*Neff, K. D. (2003b). Development and validation of a scale to measure self-compassion. Self and Identity, 2, 223–250. https://doi.org/10.1080/15298860309027
Neff, K. D. (2020). Commentary on Muris and Otgaar (2020): Let the empirical evidence speak on the self-compassion scale. Mindfulness. https://doi.org/10.1007/s12671-020-01411-9
*Neff, K. D., Pisitsungkagarn, K., & Hsieh, Y. P. (2008). Self-compassion and self-construal in the United States, Thailand, and Taiwan. Journal of Cross-Cultural Psychology, 39, 267–285. https://doi.org/10.1177/0022022108314544
Page, M. J., McKenzie, J. E., Bossuyt, P. M., Boutron, I., Hoffmann, T. C., Mulrow, C. D., Shamseer, L., Tetzlaff, J. M., Akl, E. A., Brennan, S. E., Chou, R., Glanville, J., Grimshaw, J. M., Hrobjartsson, A., Lalu, M. M., Li, F., Loder, E. W., Mayo-Wilson, E., McDonald, S., … Moher, D. (2021). The PRISMA 2020 statement: An updated guideline for reporting systematic reviews. BMJ, 372, n72. https://doi.org/10.1136/bmj.n71
*Podina, I., Jucan, A., & David, D. (2015). Self-compassion: A buffer in the pathway from maladaptive beliefs to depression: an explanatory study. Journal of Evidence-Based Psychotherapies, 15, 97–109. Retrieved from <Go to ISI>://WOS:000352465800008
*Polizzi, C. P., Baltman, J., & Lynn, S. J. (2019). Brief meditation interventions: Mindfulness, implementation instructions and loving kindness. Psychology of Consciousness: Theory, Research and Practice. https://doi.org/10.1037/cns0000194
*Rabon, J. K., Sirois, F. M., & Hirsch, J. K. (2018). Self-compassion and suicidal behavior in college students: Serial indirect effects via depression and wellness behaviors. Journal of American College Health, 66, 114–122. https://doi.org/10.1080/07448481.2017.1382498
*Raes, F. (2010). Rumination and worry as mediators of the relationship between self-compassion and depression and anxiety. Personality and Individual Differences, 48, 757–761. https://doi.org/10.1016/j.paid.2010.01.023
Shu, C., Watson, H. J., Anderson, R. A., Wade, T. D., Kane, R. T., & Egan, S. J. (2019). A randomized controlled trial of unguided internet cognitive behavior therapy for perfectionism: Impact on risk for eating disorders. Behaviour Research and Therapy, 120, 103429. https://doi.org/10.1016/j.brat.2019.103429
*Smeets, E., Neff, K., Alberts, H., & Peters, M. (2014). Meeting suffering with kindness: Effects of a brief self-compassion intervention for female college students. Journal of Clinical Psychology, 70, 794–807. https://doi.org/10.1002/jclp.22076
*Stefan, C. A., Capraru, C., & Szilagyi, M. (2018). Investigating effects and mechanisms of a mindfulness-based stress reduction intervention in a sample of college students at risk for social anxiety. Mindfulness, 9, 1509–1521. https://doi.org/10.1007/s12671-018-0899-y
*Stephenson, E., Watson, P. J., Chen, Z. J., & Morris, R. J. (2018). Self-compassion, self-esteem, and irrational beliefs. Current Psychology, 37, 809–815. https://doi.org/10.1007/s12144-017-9563-2
*Stutts, L. A., Leary, M. R., Zeveney, A. S., & Hufnagle, A. S. (2018). A longitudinal analysis of the relationship between self-compassion and the psychological effects of perceived stress. Self and Identity, 17, 609–626. https://doi.org/10.1080/15298868.2017.1422537
*Svendsen, J. L., Kvernenes, K. V., Wiker, A. S., & Dundas, I. (2017). Mechanisms of mindfulness: Rumination and self-compassion. Nordic Psychology, 69, 71–82. https://doi.org/10.1080/19012276.2016.1171730
*Tanaka, M., Wekerle, C., Schmuck, M. L., & Paglia-Boak, A. (2011). The linkages among childhood maltreatment, adolescent mental health, and self-compassion in child welfare adolescents. Child Abuse and Neglect, 35, 887–898. https://doi.org/10.1016/j.chiabu.2011.07.003
*Terry, M. L., Leary, M. R., & Mehta, S. (2013). Self-compassion as a buffer against homesickness, depression, and dissatisfaction in the transition to college. Self and Identity, 12, 278–290. https://doi.org/10.1080/15298868.2012.667913
*Van der Gucht, K., Takano, K., Raes, F., & Kuppens, P. (2018). Processes of change in a school-based mindfulness programme: Cognitive reactivity and self-coldness as mediators. Cognition & Emotion, 32, 658–665. https://doi.org/10.1080/02699931.2017.1310716
Wellcome Trust (2020). Active ingredients commission guidelines. Unpublished document.
Wellcome Trust (2021). Mental health: transforming research and treatments. Retrieved from 28 July 2021, https://wellcome.org.
Watson, H. J., Joyce, T., French, E., Willan, V., Kane, R. T., Tanner-Smith, E. E., McCormack, J., Dawkins, H., Hoiles, K. J., & Egan, S. J. (2016). Prevention of eating disorders: A systematic review of randomized, controlled trials. International Journal of Eating Disorders, 49, 833–862. https://doi.org/10.1002/eat.22577
*Wilson, J. M., Weiss, A., & Shook, N. J. (2020). Mindfulness, self-compassion, and savoring: Factors that explain the relation between perceived social support and well-being. Personality and Individual Differences. https://doi.org/10.1016/j.paid.2019.109568
*Woodruff, S. C., Glass, C. R., Arnkoff, D. B., Crowley, K. J., Hindman, R. K., & Hirschhorn, E. W. (2014). Comparing self-compassion, mindfulness, and psychological inflexibility as predictors of psychological health. Mindfulness, 5, 410–421. https://doi.org/10.1007/s12671-013-0195-9
*Yamaguchi, A., Kim, M. S., & Akutsu, S. (2014). The effects of self-construals, self-criticism, and self-compassion on depressive symptoms. Personality and Individual Differences, 68, 65–70. https://doi.org/10.1016/j.paid.2014.03.013
*Zeifman, R. J., Ip, J., Antony, M. M., & Kuo, J. R. (2019). On loving thyself: Exploring the association between self-compassion, self-reported suicidal behaviors, and implicit suicidality among college students. Journal of American College Health. https://doi.org/10.1080/07448481.2019.1679154
*Zhang, H. P., & Wang, Y. L. (2019). Bullying victimization and depression among young Chinese adults with physical disability: Roles of gratitude and self-compassion. Children and Youth Services Review, 103, 51–56. https://doi.org/10.1016/j.childyouth.2019.05.035
*Zhou, L., Liu, L., & Chen, J. (2017). Self-compassion and confucian coping as a predictor of depression and anxiety in impoverished Chinese undergraduates. Psychological Reports, 120, 627–638. https://doi.org/10.1177/003329411770085
*Zhou, L., Chen, J., Liu, X., Lu, D., & Su, L. (2013). Negative cognitive style as a mediator between self-compassion and hopelessness depression. Social Behavior and Personality: An International Journal, 41, 1511–1518. https://doi.org/10.2224/sbp.2013.41.9.1511
Funding
This work was funded by a Wellcome Trust Mental Health Priority Area ‘Active Ingredients’ commission awarded to principal investigator Sarah Egan at Curtin University. The funder of the study, Wellcome Trust, had no role in study design, data collection, data analysis, data interpretation, or writing of the report. The corresponding author had full access to all the data in the study and had final responsibility for the decision to submit for publication.
Author information
Authors and Affiliations
Contributions
SE wrote the first draft of the manuscript and all authors contributed to and have approved the final manuscript. SE, CR and AFJ designed the study. MW and DG conducted literature searches and study screening, DG conducted the meta-analysis. GF conducted quality rating of studies. JD and SB conducted qualitative interviews and transcribing of interviews, JD conducted qualitative analysis.
Corresponding author
Ethics declarations
Conflict of interest
All authors declare that they have no conflicts of interest.
Ethical Approval
The study was approved by the Curtin University Ethics Committee (HRE2020-0342).
Informed Consent
Young people and researchers provided written informed consent to participate. The study was performed in accordance with the ethical standards of the 1964 Helsinki declaration.
Additional information
Publisher's Note
Springer Nature remains neutral with regard to jurisdictional claims in published maps and institutional affiliations.
Supplementary Information
Below is the link to the electronic supplementary material.
Rights and permissions
Open Access This article is licensed under a Creative Commons Attribution 4.0 International License, which permits use, sharing, adaptation, distribution and reproduction in any medium or format, as long as you give appropriate credit to the original author(s) and the source, provide a link to the Creative Commons licence, and indicate if changes were made. The images or other third party material in this article are included in the article's Creative Commons licence, unless indicated otherwise in a credit line to the material. If material is not included in the article's Creative Commons licence and your intended use is not permitted by statutory regulation or exceeds the permitted use, you will need to obtain permission directly from the copyright holder. To view a copy of this licence, visit http://creativecommons.org/licenses/by/4.0/.
About this article
Cite this article
Egan, S.J., Rees, C.S., Delalande, J. et al. A Review of Self-Compassion as an Active Ingredient in the Prevention and Treatment of Anxiety and Depression in Young People. Adm Policy Ment Health 49, 385–403 (2022). https://doi.org/10.1007/s10488-021-01170-2
Accepted:
Published:
Issue Date:
DOI: https://doi.org/10.1007/s10488-021-01170-2