Abstract
This review provides a concise overview of the cellular and clinical aspects of the role of zinc, an essential micronutrient, in human physiology and discusses zinc-related pathological states. Zinc cannot be stored in significant amounts, so regular dietary intake is essential. ZIP4 and/or ZnT5B transport dietary zinc ions from the duodenum into the enterocyte, ZnT1 transports zinc ions from the enterocyte into the circulation, and ZnT5B (bidirectional zinc transporter) facilitates endogenous zinc secretion into the intestinal lumen. Putative promoters of zinc absorption that increase its bioavailability include amino acids released from protein digestion and citrate, whereas dietary phytates, casein and calcium can reduce zinc bioavailability. In circulation, 70% of zinc is bound to albumin, and the majority in the body is found in skeletal muscle and bone. Zinc excretion is via faeces (predominantly), urine, sweat, menstrual flow and semen. Excessive zinc intake can inhibit the absorption of copper and iron, leading to copper deficiency and anaemia, respectively. Zinc toxicity can adversely affect the lipid profile and immune system, and its treatment depends on the mode of zinc acquisition. Acquired zinc deficiency usually presents later in life alongside risk factors like malabsorption syndromes, but medications like diuretics and angiotensin-receptor blockers can also cause zinc deficiency. Inherited zinc deficiency condition acrodermatitis enteropathica, which occurs due to mutation in the SLC39A4 gene (encoding ZIP4), presents from birth. Treatment involves zinc supplementation via zinc gluconate, zinc sulphate or zinc chloride. Notably, oral zinc supplementation may decrease the absorption of drugs like ciprofloxacin, doxycycline and risedronate.
Similar content being viewed by others
Avoid common mistakes on your manuscript.
Introduction
Significance of zinc in human health
Zinc cannot be synthesised within the human body, so external intake of zinc is essential to maintain adequate levels in the body [1]. It is the second most abundant trace element in the body, after iron [2]. One in ten proteins found in the body is a zinc protein [3], and more than 300 enzymes and 1000 transcription factors depend on zinc for their activities [4]. Thus, zinc is an essential micronutrient involved in many cellular processes such as protein synthesis, nucleic acid metabolism including DNA synthesis, gene transcription [1], cell proliferation and differentiation, and mitosis [5].
These zinc-requiring cellular processes extend the significance of zinc to physiological level. For example, zinc is a structural component of the bone tissue and plays a role in collagen matrix synthesis, mineralisation, and bone turnover [6]. Also, zinc regulates intracellular signalling pathways of innate and adaptive immune cells [7], influences immune responses including antibody production, inflammatory signalling and lymphocyte differentiation [8], and thereby plays an essential role in the functionality of the immune system.
Zinc also plays a role in the endocrine system. For example, zinc is required in the formation and structural stability of insulin [9]. Essentially, insulin dimers form hexameric units, coordinated by two zinc ions in the central axis of the hexamer [10]. No wonder the beta cells of the pancreas contain significantly higher concentrations of zinc than other cells of the body. Furthermore, zinc ions act on the insulin signalling pathway and stimulate lipogenesis and glucose uptake into the adipocytes [9]. Zinc transporter (ZnT)-8 mediates signalling between the pancreas and liver to allow optimal insulin release, while zinc/iron-regulated-transporter-like-protein-(ZIP)7 is thought to play a role in glycaemic control within skeletal muscle. [9].
Thyroid hormones are involved in many physiological functions, such as the anabolism of proteins and increasing the basal metabolic rate and bone growth in children [11]. Zinc plays an important role in the metabolism of thyroid hormones. It regulates the synthesis of thyroid-releasing hormone (TRH) and thyroid-stimulating hormone (TSH). Zinc modulates their structure and thereby regulates the transcription factors which are essential for thyroid hormone synthesis [12]. Thus, in humans with zinc deficiency, levels of TSH, serum triiodothyronine (T3) and thyroxine (T4) also decrease [13], with several studies suggesting zinc deficiency as a cause of subclinical hypothyroidism [14]. Unsurprisingly, zinc supplementation appears to enhance thyroid hormone levels, particularly T3 [15].
Zinc is essential for male fertility. A zinc-sensing receptor, known as GPR39, has been found in the sperm tail and acrosome. When extracellular Zinc(II) binds to this receptor, it triggers an intracellular signalling pathway that ultimately results in increased sperm motility and acrosomal exocytosis [16]. Thus, zinc could have a role in the prevention, diagnosis and treatment of male infertility [17].
Additionally, zinc is important for the normal development and functioning of the central nervous system (CNS). Zinc balance is vital for neural tube formation and stem cell proliferation during development. Various zinc-dependent enzymes contribute to the function of the CNS, and ‘free’ zinc appears to modulate a variety of post-synaptic receptors. For example, zinc inhibits GABA-A receptors, which reduces their inhibitory actions. Alterations in zinc levels thereby affect the CNS and play a role in conditions such as Alzheimer’s disease and depression [18].
The human retina contains zinc in high concentrations [19]. Studies have suggested a link between higher anti-oxidant intake, including zinc (likely because zinc is a cofactor of superoxide dismutase, an anti-oxidant enzyme and also because zinc is an inhibitor of NADPH oxidase [20], which catalyses the production of reactive oxygen species [21]) and a decreased risk of age-related macular degeneration (AMD) [22], a leading cause of vision loss [23]. Studies have proposed the benefits of anti-oxidant supplementation, including zinc, in slowing the progression of AMD through the prevention of cellular damage in the retina [24].
Importantly, randomised trials in children six months to twelve years of age showed a positive effect of zinc supplementation in reducing all-cause and infectious disease mortality. It also showed a minor positive impact on linear growth [25].
Collectively, these examples highlight the significance of zinc in human health.
Micro-deficiencies and prevalence of zinc deficiency
It is estimated that 372 million (56%) preschool-aged children and 1.2 billion (69%) non-pregnant women of reproductive age across the globe have a deficiency in at least one of the micronutrients, namely zinc, folate, vitamin A and iron. Geographically, 75% of micronutrient-deficient preschool-aged children live in South Asia, sub-Saharan Africa, or East Asia and the Pacific. 57% of micronutrient-deficient non-pregnant women of reproductive age live in East Asia and the Pacific or South Asia [26]. An estimated 17% of the world’s population is at risk of insufficient zinc intake [1, 27]. In Southeast Asia and sub-Saharan Africa, zinc deficiency is endemic, affecting up to 33% of the population. Zinc deficiency is also prevalent in Turkey, Egypt, and Iran due to high phytate intake in their diets, which decreases zinc absorption and, therefore, its bioavailability. Other countries have a markedly lower prevalence of zinc deficiency, notably China, where its incidence decreased from 17 to 8%, as recorded in 2005 [1].
Zinc uptake, absorption, and regulators of its bioavailability
Zinc: location, dietary sources, and intake recommendation
Table 1 provides an overview of the level and proportion of zinc at physiological and cellular levels in the human body.
Zinc cannot be stored in substantial amounts, and so, regular dietary intake is essential to ensure sufficient zinc availability [17]. Dietary sources of zinc include fish, oysters, meat, legumes, nuts, beans, whole grains, beef, eggs, and dairy. Oysters are the richest source of zinc, while fruits and vegetables are the poorest source. Although beans, nuts, and whole grains contain zinc, the bioavailability of zinc from these is lower than food from animal sources due to the presence of phytates [37].
There are differences in the dietary recommendations of zinc. Data around this include recommendations of 7.4 mg/day (approximately) [38]. In the US, recommendations include 15 mg/day [30], 11 mg/day [39] and 11 mg/day and 8 mg/day for adult men and women, respectively, who are age 19 and above [37]. In the UK, the recommendation is 9.5 mg/day for an adult man and 7 mg/day for an adult woman. The UK Department of Health recommends that zinc intake should not exceed 25 mg/day [40].
Zinc transporters: ZIPs and ZnTs
During digestion, zinc is released from food as free Zn2+ ions. These ions need to be transported from the intestinal lumen to the enterocyte, then from here into the circulation and from circulation to the cells that require zinc for their activities. Also, within cells, there is intracellular zinc movement and compartmentalisation. These zinc transport processes are facilitated by two important types of zinc transporters: Zinc/iron-regulated-transporter-like-proteins (ZIPs) and Zinc transporters (ZnTs). ZIPs increase intracellular/cytoplasmic zinc levels by transporting zinc from the extracellular space and/or intracellular organelles into the cytoplasm. In general, ZnTs (the exception is ZnT5B, which is a bidirectional transporter) reduce intracellular/cytoplasmic zinc by transporting zinc from the cytoplasm to extracellular space (promoting zinc efflux from cells) or into an organelle for its compartmentalisation [38]. ZnTs and ZIPs are located in several different tissues/cells, on different regions of the cell surface, and on the surface of intracellular organelles (Tables 2 and 3).
Process of zinc uptake, absorption, and circulation
Zinc absorption/uptake primarily occurs in the proximal part of the small intestine, in the distal duodenum and proximal jejunum [39]. Zn2+ ion entry into the enterocyte is mediated via ZIP4 and/or ZnT5B in the duodenum and jejunum (Fig. 1). Another transmembrane ion transporter potentially involved in zinc uptake into the enterocyte is Divalent Metal Transporter-1 (DMT-1) [29]. Regardless of the transporter used, once Zn+2 ions are in the enterocyte, ZnT1 transports zinc from the enterocyte into the portal blood [45]. From here, these ions travel through the hepatic portal vein, mostly likely bound to ligands such as amino acids and citrate [96]. A previous study in rats found that most zinc travels to the liver in portal blood bound to transferrin [97]. At the liver, the portal vein branches, and the blood drains through sinusoids [98]. Some zinc enters hepatocytes, most likely via ZIP14 [99]. After the blood passes through the sinusoids, it is directed to the central vein, then hepatic veins and eventually the systemic circulation [98]. From the systemic circulation, zinc ions are transported to various body tissues such as the in brain, muscle, and bone [100] (Fig. 1).
Zinc uptake under physiological conditions. Zinc ions are transported from the intestinal lumen into the enterocyte by ZIP4. Other zinc transporters on the apical membrane include ZIP8 [101], ZnT10 [67] and ZnT5B [56]. ZnT5B has a bidirectional transport function [56]. Transporters located on the basolateral membrane of the enterocyte include ZnT1 [44], ZIP14 [102] and ZIP5 [103]. ZnT1 transports zinc ions from the enterocyte into the portal vein. Zinc ions travel in the portal blood to the liver, most likely bound to citrate, amino acids [96] and transferrin [97]. At the liver, portal blood drains through sinusoids, from where some zinc is taken up by hepatocytes. The rest of the zinc joins the systemic circulation from where it can reach distant tissues such as the brain, muscle, and bone via their respective ZIP transporters. Figure created with BioRender.com
There is a wide consensus that, in the systemic circulation, the majority of zinc is bound to albumin, a lesser amount bound to α2-macroglobulin, and a fraction bound to amino acids. There is a debate over whether transferrin has a role to play as a zinc carrier in the systemic circulation. Some studies suggest it may play a role [28, 29], whilst others state that transferrin does not have a primary role in the distribution of zinc [104].
Variability in data regarding the proportion of zinc bound to albumin and α 2-macroglobulin in systemic circulation
There have been various propositions regarding the proportions of these zinc carriers, particularly albumin. While some stated 80–85% of zinc is bound to albumin [105], others stated that this figure is 60% (with the remaining 30% bound to α2-macroglobulin and 10% to transferrin) [29], or 70% [38], or 80% (with the remaining 20% bound to α2-macroglobulin) [28], and yet others believe that approximately 98% zinc in the systemic circulation is bound to albumin [106].
Regardless of the exact percentage, conditions affecting albumin concentration, such as liver cirrhosis, may affect serum zinc levels [38]. For example, patients with liver cirrhosis and hepatic encephalopathy show decreased serum zinc levels [107].
Binding of Zn+2 ions to the different ligands could be the reason for the concentration of “free” Zn+2 ions in the circulation to be low (~ 0.1–1.0 nM) [96].
Regulators of zinc bioavailability
Bioavailability is the fraction of intake that can be absorbed into the blood and can be used for physiological processes in the body. Studies suggest that the typical range of zinc absorption from the intestinal lumen into the circulation is 16–50% [29], with an average of around 33% [38].
An important factor affecting zinc bioavailability is the solubility of zinc in the intestinal lumen. Previously, it was proposed that amino acids released from protein digestion enhanced zinc absorption by increasing its solubility [108]. Recent reviews have suggested that protein levels in the diet positively correlate with zinc uptake, and the presence of animal-based protein enhances zinc absorption more than the presence of plant-based protein. However, it is still uncertain whether amino acids can enhance zinc bioavailability due to a lack of consensus among studies. Citrate is a low molecular weight ligand found in milk which is thought to have a positive effect on zinc bioavailability by forming zinc-citrate complexes, thereby enhancing zinc uptake. These complexes are found in higher concentrations in human milk than in cow’s milk. Therefore, zinc absorption from human milk is higher than cow’s milk [29]. Also, food fermentation and germination enhance zinc absorption by reducing the phytate content of food [108]. Essentially, fermentation and germination both promote endogenous phytase activity [109, 110]. Germination also facilitates de novo synthesis of phytases, enzymes which hydrolyse phytic acid [110].
On the other hand, several inhibitors decrease zinc solubility and, thereby, its bioavailability, for example, phytic acid/phytates found in food such as legumes, beans, and nuts. Phytates bind to zinc in the intestine, form insoluble complexes and thereby limit zinc absorption. Thus, zinc bioavailability from plant-based foods is lower than foods from animal sources [37]. Calcium and casein in cow’s milk may also reduce the bioavailability of zinc [25].
In addition, some medications may reduce serum zinc levels. For example, long-term use of distal-tube diuretics such as chlortalidone may result in significant zinc depletion due to increased urinary zinc excretion (hyperzincuria) [111]. Angiotensin-converting enzyme inhibitors (ACEis) or angiotensin-receptor blockers (ARBs), commonly used to treat heart failure, may cause zinc deficiency [112]. Also, when consuming or prescribing oral zinc supplements for zinc deficiency, interactions of medications must be carefully monitored. For example, orally consumed zinc may decrease the absorption of many orally taken drugs, such as alendronate and risedronate, which are used to prevent and treat osteoporosis. Similarly, zinc can inhibit the absorption of many antibiotics such as ciprofloxacin and doxycycline [113].
Zinc homeostasis at physiological level
At the physiological level, zinc homeostasis is primarily maintained by controlling zinc absorption and excretion. Of the zinc that is excreted from the body, ~ 50% is lost via faeces [38] (including zinc in sloughed epithelial cells) [28], and the rest is lost through urine, sweat, menstrual flow, semen, loss of hair and nails, and shedding of skin [29]. The zinc absorption mechanism adapts more slowly, while zinc excretion mechanisms can alter quickly [29, 38]. During zinc deficiency, absorption of zinc can be increased up to 90% [28] and faecal and urinal excretion of zinc is rapidly reduced [29]. Certain tissues, such as the bone marrow, liver, and testes, secrete zinc into the circulation as a response to zinc deficiency. Other organs such as skin, skeletal muscle, heart, and kidney conserve their zinc levels even in zinc-deficient states [114].
Endogenous zinc secretion
The process of endogenous zinc secretion into the intestinal lumen may play a role in maintaining zinc homeostasis [115]. There are many ways of mediating zinc secretion into the intestinal lumen, for example, via biliary, pancreatic and gastroduodenal secretions and sloughing of mucosal cells [56, 114, 116]. Zinc transport from the portal circulation into the enterocyte is mediated by ZIP5 and ZIP14 on the basolateral membrane of enterocytes. ZnT5B transporter on the apical membrane of enterocytes is a bidirectional transporter that can transport enterocyte zinc ions into the intestinal lumen and vice versa, thereby mediating both, enterocyte uptake and endogenous secretion of zinc [29, 117].
In the context of zinc secretion into intestinal lumen from the exocrine secretions of the pancreas, there are several zinc transporters that participate in this process. For example, zinc ions are transported into the pancreas from the plasma via ZIP5. These ions are then transported into zymogen granules via ZnT2 and excreted into the digestive tract as pancreatic secretions. Interestingly, zinc concentration in pancreatic tissues and secretions is influenced by dietary zinc intake. Excess dietary zinc leads to upregulation of ZnT2 in acinar cells, and restriction of dietary zinc leads to reduced zinc concentration in both pancreatic tissue and secretions. Thus, zinc homeostasis is regulated by adjusting zinc excretion through the entero-pancreatic axis.
Regardless of the pathway, some zinc in the lumen is reabsorbed into the circulation through uptake via enterocytes. Thus, the balance between the absorption of dietary zinc, and the excretion and reabsorption of endogenous zinc collectively maintain zinc levels in the body [29].
Zinc homeostasis at the cellular level
Zinc concentration at the physiological level is determined by zinc regulation at the cellular level, which is determined by zinc transporters (Tables 2 and 3). Zinc transporters are regulated through various mechanisms, including activation of transcription, stabilisation of mRNA, modification of protein, trafficking to specific organelles, and transporter degradation. Regulatory stimuli include zinc, cytokines, hormones, endoplasmic reticulum stress, oxidative stress, and hypoxia [28].
Effect of high and low zinc on ZnTs: how zinc regulates ZnT expression
ZnT transporters are differentially regulated by zinc levels but with some similarities in mechanisms. Table 2 presents a detailed view of ZnTs, their cellular and tissue distribution, and the stimuli and mechanisms involved in the upregulation or downregulation of the ZnTs. Essentially, high zinc levels increased ZnT1 and ZnT2 mRNA expressions [44] but decreased ZnT10 mRNA levels [68]. Interestingly, ZnT5 expression is unique and complex because high or low zinc levels have been shown to increase or decrease its expression [43]. This could be due to the B variant of ZnT5, which has a bidirectional functionality in zinc transport [29].
Effect of high and low zinc on ZIPs: how zinc regulates ZIP expression
Table 3 details the ZIPs, and their cellular and tissue distribution, along with the stimuli and mechanisms involved in their upregulation or downregulation.
Most ZIP transporters were confirmed to increase their expression in response to low zinc levels including ZIP2 [74], ZIP3 [70, 76], ZIP4 [44], ZIP10 [86], and ZIP14 [92], while only ZIP5 expression was found to decrease [71]. There is some uncertainty regarding ZIP transporter regulation in response to high zinc levels. For example, ZIP7 levels inversely correlated with cellular zinc levels in CLN6 neurons [81] implying that higher cellular zinc would lead to lower ZIP7 levels. However, a causal link is yet to be confirmed because this finding could be confounded by the presence of CLN6 disease. In another example, dietary zinc restriction led to decreased ZIP11 expression in the mouse stomach. However, upon dietary zinc repletion, ZIP11 expression levels were not restored. This suggests that ZIP11 may be unaffected by zinc excess and possibly downregulated by zinc deficiency [89]. This unresponsiveness to zinc (in the form of dietary zinc repletion) [89] is unexpected, given the presence of multiple metal-response elements (MREs) upstream of the first exon of the ZIP11 gene [44].
Other regulators of ZnTs and ZIPs
Zinc transporters respond to various stimuli other than zinc (Tables 2 and 3). For example, in the immune system, T-cell stimulation by phytohaemagglutinin decreases the mRNA expressions of ZnT1, ZnT4, ZnT6 and ZnT7 [47]. These observations reiterate the importance of zinc in modulating the immune response. Moreover, in dendritic cells, lipopolysaccharide stimulation during toll-like receptor signalling increased the mRNA transcripts of ZnT1, ZnT4 and ZnT6 but decreased those of ZIP6 and ZIP10 [46].
Cytokines (namely IL-6) are known to increase ZIP14 levels [59] but decrease ZnT10 levels [44]. Hormones such as glucocorticoid and prolactin can increase ZnT2 levels [44], while thyroid hormone can increase ZIP10 levels [88]. In addition, glucose was found to increase ZIP14 levels [94].
Metals other than zinc, such as manganese [67] and iron [91, 95], can also regulate zinc transporters, which reflects their role in assisting general metal homeostasis. Interestingly, high manganese intake upregulated liver ZIP14 expression in male and female mice but upregulated ZIP14 expression in the small intestine of only male mice. ZnT10 expression was upregulated in the same regions but only in male mice [67]. These observations indicate that there might be sex-based differences in the regulation of zinc transporters.
Metallothioneins (MTs): at the interface of physiological and cellular zinc regulation
MTs are a family of proteins, ubiquitously expressed (in most cells and tissues), which have a high affinity for d10 electron configuration metals, including zinc and copper [118]. MT1 and MT2 are the main isoforms expressed in most adult mammalian tissues. MT3 has been identified in the brain, kidney, breast, pancreas, intestine, and bladder. MT4 has been reported in stratified squamous epithelium around the body and plays an important role in cell differentiation [119].
MTs are thought to play a key role in the systemic regulation of trace elements, including that of zinc [35, 118]. To execute this function, MTs within the enterocyte exhibit their regulatory effect at the absorption stage. Here, MTs can bind to zinc ions within the enterocyte cytoplasm and thereby reduce the availability of free intracellular zinc. Also, when zinc is needed by the cell, MTs can unbind zinc ions and make zinc available. So, if enterocyte zinc concentration is high, then MTs can bind to intracellular zinc and reduce free zinc ions [120, 121]. Consequently, this would reduce the amount of zinc exported into the portal blood, which, in turn, would reduce the amount of zinc distributed around the body. MTs are also thought to mediate zinc trafficking within the cell and zinc transfer to zinc transporters. Thus, through their zinc buffering and muffling properties, MTs help in maintaining zinc homeostasis [29].
Acquired zinc deficiency: diagnosis and treatment
Acquired zinc deficiency could be due to insufficient intake (seen in anorexia nervosa), increased loss (seen in chronic diarrhoea or burns patients), increased requirement (seen in pregnant and breastfeeding individuals) or malabsorption (seen in Crohn’s disease [1] and coeliac disease [122]). It shows clinical features like diarrhoea, frequent infections, and skin lesions. However, these patients usually present the symptoms later in life alongside the aforementioned factors [123]. Due to overlap of symptoms, other differentials that should be considered whilst diagnosing zinc deficiency include: depression, hypothyroidism, vitamin (A, B12 and D) deficiencies, and iron deficiency [1].
Mild zinc deficiency can manifest clinically with serum values ranging from 40 to 60 µg/dL [124]. It has been suggested that acquired zinc deficiency can be diagnosed by a simple blood test showing fasting serum zinc < 70 µg /dL. Furthermore, since low albumin levels can cause low zinc levels, serum albumin levels should also be measured [125].
Some suggest that plasma zinc as a biomarker is non-specific, and it is difficult to develop a single biomarker of zinc status due to zinc’s diverse functions [25]. However, taking a fasting sample in the morning, separating plasma or serum from cells within 45 min and using zinc-free vacuum tubes can improve accuracy [1]. In general, urinary zinc levels are not a useful diagnostic parameter for zinc deficiency, whereas hair zinc levels are useful only in the context of chronic deficiency [1, 126]. In addition to laboratory investigations, the clinical aspects comprising patient risk factors, geographical prevalence, and age of presentation, alongside physical examination and an appropriate history-taking, can help to establish the diagnosis [1].
Oral zinc supplementation, such as zinc gluconate for either short-term or long-term depending on the underlying aetiology, is usually used to cure the acquired deficiency [1]. Interestingly, zinc supplements can be formulated as zinc oxide or as salts with acetate, gluconate and sulphate [2]. A clinical trial reported that zinc oxide administered without food is less well absorbed than other zinc formulations as it is more insoluble [127]. Zinc citrate has a relatively higher zinc content, yet this is countered by the finding that zinc absorption in the form of citrate does not differ from that of zinc gluconate. However, the affordability of zinc citrate may make this an attractive alternative to zinc gluconate [127]. A potential complication of zinc deficiency treatment is overcorrection with zinc supplementation since this can cause acute zinc toxicity [1]
Other clinical conditions that may show low zinc levels are tabulated in Table 4.
Inherited zinc deficiency acrodermatitis enteropathica: diagnosis and treatment
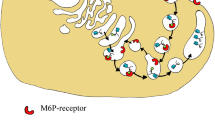
Many inherited defects of zinc deficiencies are known. Most cases are associated with mutations in the SLC39A4 gene on chromosome 8. This gene encodes the zinc transporter ZIP4 [134,135,136]. The pathological condition is referred to as acrodermatitis enteropathica, a rare autosomal recessive condition with the incidence of roughly 1 in 500,000 births [1, 137]. It affects males and females equally [137]. Because ZIP4 mediates the transport of zinc ions from the intestinal lumen into the enterocyte, a mutation in the gene encoding ZIP4 does not allow zinc ions to be transported into the enterocyte through this transporter. Consequently, insufficient zinc ions reach the systemic circulation or distant tissues (Fig. 2) [29]. Although a small amount of zinc may be taken up via the passive paracellular route [138], the result is zinc deficiency.
Mechanisms/events underlying zinc deficiency due to mutation in ZIP4 (Acrodermatitis enteropathica). In acrodermatitis enteropathica, there is a mutation in the SLC39A4 gene which encodes the ZIP4 protein. Dysfunctionality in ZIP4 transporter causes limited zinc uptake by the enterocyte, and therefore, insufficient zinc transported into the portal vein via ZnT1. Insufficient zinc ions enter the liver and the systemic circulation, leading to less zinc reaching other tissues. The result is zinc deficiency, which can be life-threatening, if not treated promptly. Figure created with BioRender.com
Notably, while ZIP4 has two zinc-binding sites and thereby can show increased efficiency in capturing and delivering zinc to the enterocytes, how ZnT5B (another zinc importer on the enterocyte) transports zinc ions into the enterocyte is not known [139]. It is conceivable that ZnT5B may have a lower affinity to zinc ions than ZIP4, and therefore, although it can allow the entry of zinc ions into the enterocyte, it cannot compensate for ZIP4 dysfunction. Left untreated, acrodermatitis enteropathica is fatal within the first few years of life [125]
Acrodermatitis enteropathica patients usually manifest symptoms early in life [1] in the phase of weaning from breastfeeding [140]. Symptoms include a triad of alopecia, diarrhoea, and dermatitis [141]. Patients may also show growth impairment, psoriasiform lesions (well-defined scaly plaques most often found on the elbows) and frequent infections [1]. Alongside the consideration of clinical symptoms, serum zinc level < 70 µg/dL in fasting and low serum alkaline phosphatase may be suggestive of acrodermatitis enteropathica [125]. Note that alkaline phosphatase is a zinc-dependent enzyme [142]. Molecular genetic testing can identify SLC39A4 mutation and confirm acrodermatitis enteropathica.
Treatment involves zinc supplementation, but the formulation of zinc depends on the route of administration. For example, zinc gluconate and sulphate [1] are commonly used orally, while zinc chloride is preferred parenterally [125]. Treatment is lifelong with patient compliance being crucial [40].
Another genetic cause of acrodermatitis enteropathica is due to a mutation in the SLC30A2 gene of the breastfeeding mother. This gene encodes for ZnT2, a zinc transporter expressed in the mammary glands [143]. In secreting mammary epithelial cells, ZnT2 imports zinc into vesicles, mediating zinc secretion into the breast milk. A mutation in this gene results in decreased zinc secretion into the breast milk. This can lead to severe zinc deficiency in exclusively breastfed infants [44]. This can be treated by supplementation of zinc at 5 mg per day whilst breastfeeding. After weaning, no further action is needed [143]. Most paediatric patients with acrodermatitis enteropathica do not present with the classic triad of periorificial and acral dermatitis, diarrhoea, and alopecia. Less than one-third of paediatric patients present in this way. Common presentations in children include recurrent infections, irritability, behavioural changes, neurological disturbances, and failure to thrive [140].
ZIP8 mutations result in cortical atrophy and, consequently, intellectual disability in the affected patient. A mutation in the SLC39A14 gene (encoding ZIP14) can lead to parkinsonism-dystonia in children [144], whilst a mutated ZIP13 protein is responsible for the spondylocheirodysplastic form of Ehlers-Danlos syndrome [145]. In mice, ZIP7 knockout was lethal, whilst a morpholino knockdown of ZIP7 caused neurodevelopmental issues in zebrafish [144].
Zinc toxicity: diagnosis and treatment
To our knowledge, there have been no reports on zinc overload/toxicity due to mutations in zinc transporters. The reported cases of zinc toxicity are due to acquired causes rather than inherited ones. Causes include pesticide exposure and exposure to compounds used to make paints, rubber and dyes [40].
The tolerable upper intake level of zinc, according to the US Institute of Medicine, is as follows: 4 mg in youngest infants, 12 mg in children 4–8 years old, 34 mg in adolescents (14–18 years), and 40 mg for persons aged 19 or older [146]. Acute and chronic zinc toxicities are defined as zinc intake of more than 200 mg/day and 50–150 mg/day, respectively [40]. Acute zinc toxicity is likely due to excessive zinc supplementation as opposed to excessive dietary zinc intake. Longer-term causes of zinc toxicity include occupational exposure to zinc [147] and iatrogenic causes such as overprescribing of zinc-containing medication, zinc present in dental fixtures (though modern preparations in the UK and US are now zinc-free) and overconsumption of over-the-counter zinc supplements [148].
At zinc doses higher than 50 mg/day, symptoms such as nausea, diarrhoea and abdominal discomfort may occur, whilst doses higher than 150 mg/day can adversely affect the body’s lipid profile and immune system. On the other hand, it has been suggested that symptoms of zinc toxicity may not manifest until intake exceeds 1–2 g [30]. The most common cause of zinc excess is taking too many zinc supplements [149]. Chronic zinc toxicity can lead to disturbances in copper metabolism causing low copper status, which affects iron distribution and causes anaemia, red blood cell microcytosis, neutropenia and reduced immune function [150, 151].
Zinc toxicity presents in different ways depending on the mode of zinc overload. For example, acute dietary ingestion presents as nausea, vomiting, diarrhoea, and muscle cramps. If toxicity is caused by inhalation of fumes, it presents with flu-like symptoms such as cough, fever, and chills. Chronic ingestion slowly leads to a syndrome of neuropathy, anaemia, fatigue, and spasticity. The 2017 Annual Report of the American Association of Poison Control Centres’ (AAPCC) National Poison Data System (NPDS) reported 1236 cases of exposure to zinc compounds, most of which were unintentional exposures in children less than five years of age. There were no deaths or major adverse health events as a consequence of this though [30].
An investigation to diagnose zinc poisoning includes several aspects like a thorough history to gain an understanding of the mode of overload, levels of serum zinc, copper and ceruloplasmin, liver function tests, platelet count, and chest X-ray. Treatment for acute ingestion involves anti-emetics, fluids and proton pump inhibitors [30]. Treatment for metal fume inhalation focuses on oral rehydration, anti-pyretics and supplemental oxygen with bronchodilators [152]. In chronic zinc toxicity, first the identification and then the removal of the source of zinc is essential. This can be followed by treatment with copper sulphate [30]. This treatment works because copper competes with zinc for absorption, so exogenous copper intake reduces zinc absorption [1]. Very severe cases may require zinc chelation with agents such as diethylenetriamine pentaacetate (DTPA) [30].
Zinc-induced copper deficiency (ZICD)
An important complication of chronic zinc toxicity is zinc-induced copper deficiency (ZICD). Excess zinc levels in the small intestine stimulate increased expression of MTs in the enterocytes. Since copper has a greater affinity for MTs compared to zinc, copper outcompetes zinc for MT binding sites, and consequently, the copper bound to MT is excreted via sloughing of enterocytes. This results in decreased absorption of copper and, therefore, copper deficiency [153]. The co-existence of hyperzincaemia (high zinc in serum) and hypocupraemia (low copper in serum) is suggestive of ZICD [154]. Measurements of urinary zinc can be useful in the diagnostics of ZICD because urinary zinc levels are usually high in this condition [155].
ZICD tends to develop slowly over many months or years, although this apparent slow onset may be due to delayed diagnosis [155]. Early manifestation includes neutropenia, leukopenia and anaemia [154]. This anaemia is likely due to the disruption of copper’s physiological role in the differentiation of haematopoietic stem cells as well as intestinal iron absorption [156].
Under physiological conditions, copper plays a vital role in the synthesis and stabilisation of myelin, and in several enzymatic pathways required for the functioning of the nervous system. Therefore, if ZICD is left undiagnosed, it can lead to severe and permanent neurological complications including gait disturbances, paraesthesia and myelopathy [156].
One study highlighted that the over-prescription of zinc was a significant cause of ZICD. This shows that zinc can have potentially serious side effects, and it is not a harmless agent that can be prescribed without a strong justification [155]. Removal of the source of excess zinc along with oral copper gluconate treatment is often sufficient to revert anaemia, neutropenia and leukopenia seen in ZICD. Neurological deficits may also improve with this treatment; however, many never fully recover and will be left with permanent neurological deficits [156].
Summary
Trace elements play an important role in human health and disease. For example, the role of iron in various diseases, including liver fibrosis, alcohol-related liver disease, and COVID-19, has been reviewed [157,158,159,160].
Zinc is an essential micronutrient which cannot be stored in significant amounts, so regular dietary intake is vital. There does not seem to be a clear consensus on the recommended zinc intake, where the recommendation ranges from 7.4 to 15 mg/day. Citrate and food processing such as fermentation and germination, can enhance zinc uptake. It is unclear whether amino acids enhance zinc uptake. Phytic acid, found in cereals, legumes, and nuts, is known to decrease zinc bioavailability.
Zinc absorption occurs primarily in the proximal small intestine, where ZIP4 mediates zinc entry into enterocytes. ZnT5B and DMT-1 are also thought to play a role in this process. ZnT1 transports zinc from the enterocyte into the portal vein, via which zinc travels to the liver. Here, some zinc may enter the hepatocytes via ZIP14, and the rest may eventually drain into the systemic circulation for distribution to various bodily tissues. In the circulation, most zinc is bound to albumin, and the majority in the body can be found in skeletal muscle and bone.
Zinc deficiency can be inherited or acquired. The acquired form is due to insufficient intake, malabsorption, increased requirement, or excessive loss of zinc. Inherited zinc deficiency is mostly associated with mutations in the SLC39A4 gene (which encodes for ZIP4), resulting in a triad of alopecia, diarrhoea and dermatitis in a condition known as acrodermatitis enteropathica. In both inherited and acquired deficiencies, oral zinc supplementation is the mainstay of treatment with an excellent prognosis.
Zinc toxicity is only known to be acquired, not inherited, and may be acute or chronic. Symptoms include nausea, diarrhoea and abdominal discomfort but may vary depending on the mode of overload. Treatment involves the chelation of excess zinc using drugs.
Recommendations for future work
This review helped us identify the knowledge gaps in the literature on zinc. For example, there is no clear consensus on the proportion of zinc that is bound to albumin in the systemic circulation. Albumin levels decrease in several conditions, including liver cirrhosis, and so, knowledge of the proportion of zinc bound to albumin may inform alternative or supplementary treatments for those with albumin-depletion-induced zinc deficiency. In such patients, only oral zinc supplementation may not be enough to resolve the deficiency because there is an insufficient level of the zinc carrier albumin to distribute zinc around the body. Should albumin be the predominant zinc carrier in the circulation, albumin supplementation may play an important role in treating zinc deficiency. There are some other uncertainties in the context of zinc carriers. For example, there are contrasting suggestions on whether transferrin has a role to play as a zinc carrier in the systemic circulation or not. Thus, the knowledge on zinc carriers will aid in our understanding of the pathogenesis of zinc-related conditions.
Another knowledge gap exists in the mechanisms by which the levels of certain zinc transporters increase or decrease in cells in response to a stimulus, as reflected in Tables 2 and 3. Dedicated studies are required to elucidate these mechanisms as this might help devise ways of altering zinc levels within cells in a tissue-specific manner and thereby help ameliorate a zinc-related diseased state. Also, while our knowledge so far indicates that zinc toxicity is not caused by mutations in zinc transporters, examining genetics as a predisposing factor in the development of zinc toxicity might be helpful, as it has been in the case of zinc deficiency. Given the multi-faceted physiological role of zinc, such studies would improve the diagnostics and therapeutics of a range of conditions, positively impacting the health of the general population as well as of those with zinc-related diseases.
References
Maxfield L, Shukla S, Crane JS. Zinc Deficiency. In: StatPearls [Internet]. Treasure Island (FL): StatPearls Publishing; 2022 [cited 2022 Jul 4]. Available from: http://www.ncbi.nlm.nih.gov/books/NBK493231/.
Saper RB, Rash R. Zinc: an essential micronutrient. Am Fam Physician. 2009;79:768.
Hernández-Camacho JD, Vicente-García C, Parsons DS, Navas-Enamorado I. Zinc at the crossroads of exercise and proteostasis. Redox Biol. 2020;35: 101529.
Prasad AS. Discovery of human zinc deficiency: its impact on human health and disease. Adv Nutr. 2013;4:176–90.
Beyersmann D, Haase H. Functions of zinc in signaling, proliferation and differentiation of mammalian cells. Biometals. 2001;14:331–41.
Molenda M, Kolmas J. The role of zinc in bone tissue health and regeneration—a review. Biol Trace Elem Res. 2023;201:5640–51.
Wessels I, Maywald M, Rink L. Zinc as a gatekeeper of immune function. Nutrients. 2017;9:1286.
Lin P-H, Sermersheim M, Li H, Lee PHU, Steinberg SM, Ma J. Zinc in wound healing modulation. Nutrients. 2017;10:16.
Fukunaka A, Fujitani Y. Role of zinc homeostasis in the pathogenesis of diabetes and obesity. Int J Mol Sci. 2018;19:476.
Weiss M, Steiner DF, Philipson LH, et al. Insulin biosynthesis, secretion, structure, and structure-activity relationships. In: Feingold KR, Anawalt B, Blackman MR, Boyce A, Chrousos G, Corpas E, et al., editors. Endotext [Internet]. South Dartmouth: MDText.com Inc; 2000.
Shahid MA, Ashraf MA, Sharma S. Physiology, thyroid hormone. In: StatPearls [Internet]. Treasure Island (FL): StatPearls Publishing; 2022 [cited 2023 Jan 17]. Available from: http://www.ncbi.nlm.nih.gov/books/NBK500006/.
Severo JS, Morais JBS, de Freitas TEC, Andrade ALP, Feitosa MM, Fontenelle LC, et al. The role of zinc in thyroid hormones metabolism. Int J Vitam Nutr Res. 2019;89:80–8.
Knezevic J, Starchl C, Tmava Berisha A, Amrein K. Thyroid-gut-axis: How does the microbiota influence thyroid function? Nutrients. 2020;12:1769.
Betsy A, Binitha M, Sarita S. Zinc deficiency associated with hypothyroidism: an overlooked cause of severe alopecia. Int J Trichol. 2013;5:40–2.
Maxwell C, Volpe SL. Effect of zinc supplementation on thyroid hormone function. ANM. 2007;51:188–94.
Allouche-Fitoussi D, Breitbart H. The role of zinc in male fertility. Int J Mol Sci. 2020;21:7796.
Fallah A, Mohammad-Hasani A, Colagar AH. Zinc is an essential element for male fertility: A review of Zn roles in men’s health, germination, sperm quality, and fertilization. J Reprod Infertil. 2018;19:69–81.
Gower-Winter SD, Levenson CW. Zinc in the central nervous system: from molecules to behavior. BioFactors. 2012;38:186–93.
Ugarte M, Osborne NN. Zinc in the retina. Prog Neurobiol. 2001;64:219–49.
De Nascimento Marreiro D, Cruz KJC, Morais JBS, Beserra JB, Severo JS, de Oliveira ARS. Zinc and oxidative stress: current mechanisms. Antioxidants (Basel). 2017;6:24.
Sedeek M, Nasrallah R, Touyz RM, Hébert RL. NADPH oxidases, reactive oxygen species, and the kidney: friend and foe. J Am Soc Nephrol. 2013;24:1512–8.
van Leeuwen R, Boekhoorn S, Vingerling JR, Witteman JCM, Klaver CCW, Hofman A, et al. Dietary intake of antioxidants and risk of age-related macular degeneration. JAMA. 2005;294:3101–7.
Fleckenstein M, Keenan TDL, Guymer RH, Chakravarthy U, Schmitz-Valckenberg S, Klaver CC, et al. Age-related macular degeneration. Nat Rev Dis Prim. 2021;7:31.
Evans JR, Lawrenson JG. Antioxidant vitamin and mineral supplements for slowing the progression of age-related macular degeneration. Cochrane Database Syst Rev. 2017;7:CD000254.
Bailey RL, West KP Jr, Black RE. The epidemiology of global micronutrient deficiencies. ANM. 2015;66:22–33.
Stevens GA, Beal T, Mbuya MNN, Luo H, Neufeld LM, Addo OY, et al. Micronutrient deficiencies among preschool-aged children and women of reproductive age worldwide: a pooled analysis of individual-level data from population-representative surveys. Lancet Glob Health. 2022;10:e1590–9.
Wessells KR, Brown KH. Estimating the global prevalence of zinc deficiency: results based on zinc availability in national food supplies and the prevalence of stunting. PLoS ONE. 2012;7: e50568.
Hara T, Takeda T, Takagishi T, Fukue K, Kambe T, Fukada T. Physiological roles of zinc transporters: molecular and genetic importance in zinc homeostasis. J Physiol Sci. 2017;67:283–301.
Maares M, Haase H. A guide to human zinc absorption: general overview and recent advances of in vitro intestinal models. Nutrients. 2020;12:762.
Agnew UM, Slesinger TL. Zinc toxicity. In: StatPearls [Internet]. Treasure Island (FL): StatPearls Publishing; 2022 [cited 2022 Jul 4]. Available from: http://www.ncbi.nlm.nih.gov/books/NBK554548/.
Andrew D, Gail R, Morag B, Kishor R. Recommended reference intervals for copper and zinc in serum using the US national health and nutrition examination surveys (NHANES) data. Clin Chim Acta. 2023;546: 117397.
Barman N, Salwa M, Ghosh D, Rahman MW, Uddin MN, Haque MA. Reference value for serum zinc level of adult population in Bangladesh. EJIFCC. 2020;31:117–24.
Maywald M, Rink L. Zinc in human health and infectious diseases. Biomolecules. 2022;12:1748.
Plum LM, Rink L, Haase H. The essential toxin: impact of zinc on human health. Int J Environ Res Public Health. 2010;7:1342–65.
Bafaro E, Liu Y, Xu Y, Dempski RE. The emerging role of zinc transporters in cellular homeostasis and cancer. Sig Transduct Target Ther. 2017;2:1–12.
Rabinovich D, Smadi Y. Zinc. In: StatPearls [Internet]. Treasure Island (FL): StatPearls Publishing; 2023 [cited 2023 Sep 23]. Available from: http://www.ncbi.nlm.nih.gov/books/NBK547698/.
Office of Dietary Supplements—Zinc [Internet]. [cited 2022 Dec 19]. Available from: https://ods.od.nih.gov/factsheets/Zinc-HealthProfessional/.
Roohani N, Hurrell R, Kelishadi R, Schulin R. Zinc and its importance for human health: an integrative review. J Res Med Sci. 2013;18:144–57.
Skrovanek S, DiGuilio K, Bailey R, Huntington W, Urbas R, Mayilvaganan B, et al. Zinc and gastrointestinal disease. World J Gastrointest Pathophysiol. 2014;5:496–513.
Zinc Deficiency, Excess and Supplementation. Zinc problems [Internet]. 2019 [cited 2023 Aug 20]. Available from: https://patient.info/doctor/zinc-deficiency-excess-and-supplementation-pro.
Mor M, Beharier O, Cook DI, Campbell CR, Gheber LA, Katz A, et al. ZnT1 induces a crosstalk between T-type and L-type calcium channels through interactions with Raf-1 kinase and the calcium channel β2 subunit. Metallomics. 2023;15:mfad031.
McMahon RJ, Cousins RJ. Regulation of the zinc transporter ZnT-1 by dietary zinc. Proc Natl Acad Sci USA. 1998;95:4841–6.
Lichten LA, Cousins RJ. Mammalian zinc transporters: nutritional and physiologic regulation. Annu Rev Nutr. 2009;29:153–76.
Kambe T, Tsuji T, Hashimoto A, Itsumura N. The physiological, biochemical, and molecular roles of zinc transporters in zinc homeostasis and metabolism. Physiol Rev. 2015;95:749–84.
Nishito Y, Kambe T. Zinc transporter 1 (ZNT1) expression on the cell surface is elaborately controlled by cellular zinc levels. J Biol Chem. 2019;294:15686–97.
Kitamura H, Morikawa H, Kamon H, Iguchi M, Hojyo S, Fukada T, et al. Toll-like receptor–mediated regulation of zinc homeostasis influences dendritic cell function. Nat Immunol. 2006;7:971–7.
Feske S, Skolnik EY, Prakriya M. Ion channels and transporters in lymphocyte function and immunity. Nat Rev Immunol. 2012;12:532–47.
Lopez V, Kelleher SL. Zinc transporter-2 (ZnT2) variants are localized to distinct subcellular compartments and functionally transport zinc. Biochem J. 2009;422:43–52.
Guo L, Lichten LA, Ryu M-S, Liuzzi JP, Wang F, Cousins RJ. STAT5-glucocorticoid receptor interaction and MTF-1 regulate the expression of ZnT2 (Slc30a2) in pancreatic acinar cells. Proc Natl Acad Sci U S A. 2010;107:2818–23.
Qian L, Lopez V, Seo YA, Kelleher SL. Prolactin regulates ZNT2 expression through the JAK2/STAT5 signaling pathway in mammary cells. Am J Physiol Cell Physiol. 2009;297:C369-377.
Seo YA, Lee S, Hennigar SR, Kelleher SL. Prolactin (PRL)-stimulated ubiquitination of ZnT2 mediates a transient increase in zinc secretion followed by ZnT2 degradation in mammary epithelial cells. J Biol Chem. 2014;289:23653–61.
Smidt K, Rungby J. ZnT3: a zinc transporter active in several organs. Biometals. 2012;25:1–8.
Niu L, Li L, Yang S, Wang W, Ye C, Li H. Disruption of zinc transporter ZnT3 transcriptional activity and synaptic vesicular zinc in the brain of Huntington’s disease transgenic mouse. Cell Biosci. 2020;10:106.
Patrushev N, Seidel-Rogol B, Salazar G. Angiotensin II requires zinc and downregulation of the zinc transporters ZnT3 and ZnT10 to induce senescence of vascular smooth muscle cells. PLoS ONE. 2012;7: e33211.
Liuzzi JP, Cousins RJ. Mammalian zinc transporters. Annu Rev Nutr. 2004;24:151–72.
Cousins RJ. Gastrointestinal factors influencing zinc absorption and homeostasis. Int J Vitam Nutr Res. 2010;80:243–8.
Jackson KA, Helston RM, McKay JA, O’Neill ED, Mathers JC, Ford D. Splice variants of the human zinc transporter ZnT5 (SLC30A5) are differentially localized and regulated by zinc through transcription and mRNA stability. J Biol Chem. 2007;282:10423–31.
Valentine RA, Jackson KA, Christie GR, Mathers JC, Taylor PM, Ford D. ZnT5 variant B is a bidirectional zinc transporter and mediates zinc uptake in human intestinal Caco-2 cells. J Biol Chem. 2007;282:14389–93.
Liuzzi JP, Lichten LA, Rivera S, Blanchard RK, Aydemir TB, Knutson MD, et al. Interleukin-6 regulates the zinc transporter Zip14 in liver and contributes to the hypozincemia of the acute-phase response. Proc Natl Acad Sci USA. 2005;102:6843–8.
Huang L, Kirschke CP, Gitschier J. Functional characterization of a novel mammalian zinc transporter, ZnT6. J Biol Chem. 2002;277:26389–95.
Kirschke CP, Huang L. ZnT7, a novel mammalian zinc transporter, accumulates zinc in the golgi apparatus. J Biol Chem. 2003;278:4096–102.
Kambe T, Hashimoto A, Fujimoto S. Current understanding of ZIP and ZnT zinc transporters in human health and diseases. Cell Mol Life Sci. 2014;71:3281–95.
Daniels MJ, Jagielnicki M, Yeager M. Structure/function analysis of human ZnT8 (SLC30A8): a diabetes risk factor and zinc transporter. Curr Res Struct Biol. 2020;2:144–55.
Merriman C, Fu D. Down-regulation of the islet-specific zinc transporter-8 (ZnT8) protects human insulinoma cells against inflammatory stress. J Biol Chem. 2019;294:16992–7006.
Liu C, Jursa T, Aschner M, Smith DR, Mukhopadhyay S. Up-regulation of the manganese transporter SLC30A10 by hypoxia-inducible factors defines a homeostatic response to manganese toxicity. Proc Natl Acad Sci USA. 2021;118: e2107673118.
Fujishiro H, Yoshida M, Nakano Y, Himeno S. Interleukin-6 enhances manganese accumulation in SH-SY5Y cells: implications of the up-regulation of ZIP14 and the down-regulation of ZnT10. Metallomics. 2014;6:944–9.
Felber DM, Wu Y, Zhao N. Regulation of the metal transporters ZIP14 and ZnT10 by manganese intake in mice. Nutrients. 2019;11:2099.
Bosomworth HJ, Ford D, Valentine RA. ZnT10 is expressed in adult human tissues. Proc Nutr Soc. 2011;70:E127.
Jeong J, Eide DJ. The SLC39 family of zinc transporters. Mol Asp Med. 2013;34:612–9.
Wang F, Dufner-Beattie J, Kim B-E, Petris MJ, Andrews G, Eide DJ. Zinc-stimulated endocytosis controls activity of the mouse ZIP1 and ZIP3 zinc uptake transporters. J Biol Chem. 2004;279:24631–9.
Weaver BP, Dufner-Beattie J, Kambe T, Andrews GK. Novel zinc-responsive post-transcriptional mechanisms reciprocally regulate expression of the mouse Slc39a4 and Slc39a5 zinc transporters (Zip4 and Zip5). Biol Chem. 2007;388:1301–12.
Huang L, Kirschke CP. A di-leucine sorting signal in ZIP1 (SLC39A1) mediates endocytosis of the protein. FEBS J. 2007;274:3986–97.
Tang Z, Sahu SN, Khadeer MA, Bai G, Franklin RB, Gupta A. Overexpression of the ZIP1 zinc transporter induces an osteogenic phenotype in mesenchymal stem cells. Bone. 2006;38:181–98.
Cousins RJ, Blanchard RK, Popp MP, Liu L, Cao J, Moore JB, et al. A global view of the selectivity of zinc deprivation and excess on genes expressed in human THP-1 mononuclear cells. Proc Natl Acad Sci USA. 2003;100:6952–7.
Gou Y, Yang D, Tian T, Zhu X, Zhang R, Ren J, et al. The transcription of ZIP9 is associated with the macrophage polarization and the pathogenesis of hepatocellular carcinoma. Front Immunol. 2022;13:725595. https://doi.org/10.3389/fimmu.2022.725595.
Zheng D, Feeney GP, Kille P, Hogstrand C. Regulation of ZIP and ZnT zinc transporters in zebrafish gill: zinc repression of ZIP10 transcription by an intronic MRE cluster. Physiol Genom. 2008;34:205–14.
Kelleher SL, Lönnerdal B. Zip3 plays a major role in zinc uptake into mammary epithelial cells and is regulated by prolactin. Am J Physiol Cell Physiol. 2005;288:C1042–7.
Yin S, Duan M, Fang B, Zhao G, Leng X, Zhang T. Zinc homeostasis and regulation: Zinc transmembrane transport through transporters. Crit Rev Food Sci Nutr. 2022;63(25):7627–37.
Takagishi T, Hara T, Fukada T. Recent advances in the role of SLC39A/ZIP zinc transporters in vivo. Int J Mol Sci. 2017;18:2708.
Weaver BP, Andrews GK. Regulation of zinc-responsive Slc39a5 (Zip5) translation is mediated by conserved elements in the 3’-untranslated region. Biometals. 2012;25:319–35.
Grubman A, Lidgerwood GE, Duncan C, Bica L, Tan J-L, Parker SJ, et al. Deregulation of subcellular biometal homeostasis through loss of the metal transporter, Zip7, in a childhood neurodegenerative disorder. Acta Neuropathol Commun. 2014;2:25.
Bowers K, Srai SKS. The trafficking of metal ion transporters of the Zrt- and Irt-like protein family. Traffic. 2018;19:813–22.
Aydemir TB, Liuzzi JP, McClellan S, Cousins RJ. Zinc transporter ZIP8 (SLC39A8) and zinc influence IFN-γ expression in activated human T cells. J Leukoc Biol. 2009;86:337–48.
Liu M-J, Bao S, Gálvez-Peralta M, Pyle CJ, Rudawsky AC, Pavlovicz RE, et al. The zinc transporter SLC39A8 is a negative feedback regulator of NF-κB through zinc-mediated inhibition of IKK. Cell Rep. 2013;3:386–400.
Wang C-Y, Jenkitkasemwong S, Duarte S, Sparkman BK, Shawki A, Mackenzie B, et al. ZIP8 is an iron and zinc transporter whose cell-surface expression is up-regulated by cellular iron loading. J Biol Chem. 2012;287:34032–43.
Lichten LA, Ryu M-S, Guo L, Embury J, Cousins RJ. MTF-1-mediated repression of the zinc transporter Zip10 is alleviated by zinc restriction. PLoS ONE. 2011;6: e21526.
Miyai T, Hojyo S, Ikawa T, Kawamura M, Irié T, Ogura H, et al. Zinc transporter SLC39A10/ZIP10 facilitates antiapoptotic signaling during early B-cell development. Proc Natl Acad Sci U S A. 2014;111:11780–5.
Pawan K, Neeraj S, Sandeep K, Kanta Ratho R, Rajendra P. Upregulation of Slc39a10 gene expression in response to thyroid hormones in intestine and kidney. Biochim Biophys Acta. 2007;1769:117–23.
Martin AB, Aydemir TB, Guthrie GJ, Samuelson DA, Chang S-M, Cousins RJ. Gastric and colonic zinc transporter ZIP11 (Slc39a11) in mice responds to dietary zinc and exhibits nuclear localization123. J Nutr. 2013;143:1882–8.
Zhao L, Oliver E, Maratou K, Atanur SS, Dubois OD, Cotroneo E, et al. The zinc transporter, ZIP12, regulates the pulmonary vascular response to chronic hypoxia. Nature. 2015;524:356–60.
Xu J, Wan Z, Zhou B. Drosophila ZIP13 is posttranslationally regulated by iron-mediated stabilization. Biochim Biophys Acta BBA Mol Cell Res. 2019;186:1487–97.
Homma K, Fujisawa T, Tsuburaya N, Yamaguchi N, Kadowaki H, Takeda K, et al. SOD1 as a molecular switch for initiating the homeostatic ER stress response under zinc deficiency. Mol Cell. 2013;52:75–86.
Lichten LA, Liuzzi JP, Cousins RJ. Interleukin-1β contributes via nitric oxide to the upregulation and functional activity of the zinc transporter Zip14 (Slc39a14) in murine hepatocytes. Am J Physiol Gastrointest Liver Physiol. 2009;296:G860–7.
Maxel T, Smidt K, Petersen CC, Honoré B, Christensen AK, Jeppesen PB, et al. The zinc transporter Zip14 (SLC39a14) affects beta-cell function: proteomics, gene expression, and insulin secretion studies in INS-1E cells. Sci Rep. 2019;9:8589.
Nam H, Wang C-Y, Zhang L, Zhang W, Hojyo S, Fukada T, et al. ZIP14 and DMT1 in the liver, pancreas, and heart are differentially regulated by iron deficiency and overload: implications for tissue iron uptake in iron-related disorders. Haematologica. 2013;98:1049–57.
Costello LC, Franklin RB. The status of zinc in the development of hepatocellular cancer. Cancer Biol Ther. 2014;15:353–60.
Evans GW, Winter TW. Zinc transport by transferrin in rat portal blood plasma. Biochem Biophys Res Commun. 1975;66:1218–24.
Carneiro C, Brito J, Bilreiro C, Barros M, Bahia C, Santiago I, et al. All about portal vein: a pictorial display to anatomy, variants and physiopathology. Insights Imaging. 2019;10:38.
Kim M-H, Aydemir TB, Kim J, Cousins RJ. Hepatic ZIP14-mediated zinc transport is required for adaptation to endoplasmic reticulum stress. Proc Natl Acad Sci. 2017;114:E5805–14.
Willekens J, Runnels LW. Impact of zinc transport mechanisms on embryonic and brain development. Nutrients. 2022;14:2526.
Wu Y. The function of intestinal ZIP8 in manganese metabolism. 2023 [cited 2023 Sep 26]; Available from: https://repository.arizona.edu/handle/10150/668217.
Guthrie GJ, Aydemir TB, Troche C, Martin AB, Chang S-M, Cousins RJ. Influence of ZIP14 (slc39A14) on intestinal zinc processing and barrier function. Am J Physiol Gastrointest Liver Physiol. 2015;308:171–8.
Geiser J, De Lisle RC, Andrews GK. The zinc transporter Zip5 (Slc39a5) regulates intestinal zinc excretion and protects the pancreas against zinc toxicity. PLoS ONE. 2013;8: e82149.
Herrera C, Pettiglio MA, Bartnikas TB. Investigating the role of transferrin in the distribution of iron, manganese, copper and zinc. J Biol Inorg Chem. 2014;19:869–77.
Cuajungco MP, Ramirez MS, Tolmasky ME. Zinc: multidimensional effects on living organisms. Biomedicines. 2021;9:208.
Blindauer CA, Harvey I, Bunyan KE, Stewart AJ, Sleep D, Harrison DJ, et al. Structure, properties, and engineering of the major zinc binding site on human albumin. J Biol Chem. 2009;284:23116–24.
Mohommad MK, Zhou Z, Cave M, Barve A, McClain CJ. Zinc and liver disease. Nutr Clin Pract. 2012;27:8–20.
Dietary LB, Absorption FIZ. Dietary factors influencing zinc absorption. J Nutr. 2000;130:1378S-1383S.
Samtiya M, Aluko RE, Puniya AK, Dhewa T. Enhancing micronutrients bioavailability through fermentation of plant-based foods: a concise review. Fermentation. 2021;7:63.
Gibson RS, Yeudall F, Drost N, Mtitimuni B, Cullinan T. Dietary interventions to prevent zinc deficiency123. Am J Clin Nutr. 1998;68:484S-487S.
Reyes AJ, Leary WP, Lockett CJ, Alcocer L. Diuretics and zinc. S Afr Med J. 1982;62:373–5.
Cohen N, Golik A. Zinc balance and medications commonly used in the management of heart failure. Heart Fail Rev. 2006;11:19–24.
Zinc sulfate|Drugs|BNF content published by NICE [Internet]. [cited 2022 Dec 5]. Available from: https://bnf.nice.org.uk/drugs/zinc-sulfate/.
Kondaiah P, Yaduvanshi PS, Sharp PA, Pullakhandam R. Iron and zinc homeostasis and interactions: Does enteric zinc excretion cross-talk with intestinal iron absorption? Nutrients. 2019;11:1885.
Gopalsamy GL, Alpers DH, Binder HJ, Tran CD, Ramakrishna BS, Brown I, et al. The relevance of the colon to zinc nutrition. Nutrients. 2015;7:572–83.
Krebs NF. Overview of zinc absorption and excretion in the human gastrointestinal tract. J Nutr. 2000;130:1374S-S1377.
Ohashi W, Hara T, Takagishi T, Hase K, Fukada T. Maintenance of intestinal epithelial homeostasis by zinc transporters. Dig Dis Sci. 2019;64:2404–15.
Isani G, Carpenè E. Metallothioneins, unconventional proteins from unconventional animals: a long journey from nematodes to mammals. Biomolecules. 2014;4:435–57.
Wei H, Desouki MM, Lin S, Xiao D, Franklin RB, Feng P. Differential expression of metallothioneins (MTs) 1, 2, and 3 in response to zinc treatment in human prostate normal and malignant cells and tissues. Mol Cancer. 2008;7:7.
Liu S, Wang N, Long Y, Wu Z, Zhou S. Zinc homeostasis: an emerging therapeutic target for neuroinflammation related diseases. Biomolecules. 2023;13:416.
Moltedo O, Verde C, Capasso A, Parisi E, Remondelli P, Bonatti S, et al. Zinc transport and metallothionein secretion in the intestinal human cell line Caco-2. J Biol Chem. 2000;275:31819–25.
Fathi F, Ektefa F, Tafazzoli M, Rostami K, Nejad MR, Fathi M, et al. The concentration of serum zinc in celiac patients compared to healthy subjects in Tehran. Gastroenterol Hepatol Bed Bench. 2013;6:92.
Human HM, Deficiency Z. Human zinc deficiency. J Nutr. 2000;130:1344S-1349S.
Maxfield L, Shukla S, Crane JS. Zinc deficiency. In: StatPearls [Internet]. Treasure Island (FL): StatPearls Publishing; 2023 [cited 2023 Aug 20]. Available from: http://www.ncbi.nlm.nih.gov/books/NBK493231/.
Jagadeesan S, Kaliyadan F. Acrodermatitis enteropathica. In: StatPearls [Internet]. Treasure Island (FL): StatPearls Publishing; 2022 [cited 2022 Sep 1]. Available from: http://www.ncbi.nlm.nih.gov/books/NBK441835/.
Kumar P, Lal NR, Mondal AK, Mondal A, Gharami RC, Maiti A. Zinc and skin: a brief summary. Dermatol Online J. 2012;18:1.
Wegmüller R, Tay F, Zeder C, Brnić M, Hurrell RF. Zinc absorption by young adults from supplemental zinc citrate is comparable with that from zinc gluconate and higher than from zinc oxide123. J Nutr. 2014;144:132–6.
Baum MK, Lai S, Sales S, Page JB, Campa A. Randomized, controlled clinical trial of zinc supplementation to prevent immunological failure in HIV-infected adults. Clin Infect Dis. 2010;50:1653–60.
Tokuyama A, Kanda E, Itano S, Kondo M, Wada Y, Kadoya H, et al. Effect of zinc deficiency on chronic kidney disease progression and effect modification by hypoalbuminemia. PLoS ONE. 2021;16: e0251554.
Squitti R, Pal A, Picozza M, Avan A, Ventriglia M, Rongioletti M, et al. Zinc therapy in early Alzheimer’s disease: safety and potential therapeutic efficacy. Biomolecules. 2020;10:1164.
McClain C, Vatsalya V, Cave M. Role of zinc in the development/progression of alcoholic liver disease. Curr Treat Options Gastroenterol. 2017;15:285–95.
Yesiladali M, Yazici MGK, Attar E, Kelestimur F. Differentiating polycystic ovary syndrome from adrenal disorders. Diagnostics (Basel). 2022;12:2045.
Office of Dietary Supplements—Copper [Internet]. [cited 2022 Aug 14]. Available from: https://ods.od.nih.gov/factsheets/Copper-HealthProfessional/
Ackland ML, Michalczyk A. Zinc deficiency and its inherited disorders: a review. Genes Nutr. 2006;1:41–9.
Andrews GK. Regulation and function of Zip4, the acrodermatitis enteropathica gene. Biochem Soc Trans. 2008;36:1242–6.
Wang K, Zhou B, Kuo Y-M, Zemansky J, Gitschier J. A novel member of a zinc transporter family is defective in acrodermatitis enteropathica. Am J Hum Genet. 2002;71:66–73.
Acrodermatitis Enteropathica [Internet]. NORD (National Organization for Rare Disorders). [cited 2022 Dec 14]. Available from: https://rarediseases.org/rare-diseases/acrodermatitis-enteropathica/.
Goff JP. Invited review: mineral absorption mechanisms, mineral interactions that affect acid–base and antioxidant status, and diet considerations to improve mineral status. J Dairy Sci. 2018;101:2763–813.
Hall AG, King JC. The molecular basis for zinc bioavailability. Int J Mol Sci. 2023;24:6561.
Pediatric Acrodermatitis Enteropathica: Background, Pathophysiology, Etiology. 2022 [cited 2023 Jan 18]; Available from: https://emedicine.medscape.com/article/912075-overview?reg=1#a4&icd=login_success_email_match_norm.
George AA, Mishra AK, Sahu KK, Sargent J. Acquired acrodermatitis enteropathica. Am J Med. 2021;134:e2-3.
Cho Y-E, Lomeda R-AR, Ryu S-H, Sohn H-Y, Shin H-I, Beattie JH, et al. Zinc deficiency negatively affects alkaline phosphatase and the concentration of Ca, Mg and P in rats. Nutr Res Pract. 2007;1:113–9.
Golan Y, Assaraf YG. Genetic and physiological factors affecting human milk production and composition. Nutrients. 2020;12:1500.
Woodruff G, Bouwkamp CG, De Vrij FM, Lovenberg T, Bonaventure P, Kushner SA, et al. The zinc transporter SLC39A7 (ZIP7) is essential for regulation of cytosolic zinc levels. Mol Pharmacol. 2018;94:1092–100.
Bin B-H, Hojyo S, Ryong Lee T, Fukada T. Spondylocheirodysplastic Ehlers–Danlos syndrome (SCD-EDS) and the mutant zinc transporter ZIP13. Rare Dis. 2014;2: e974982.
Sandstead HH. Chapter 61—Zinc. In: Nordberg GF, Fowler BA, Nordberg M, editors. Handbook on the toxicology of metals. 4th ed. San Diego: Academic Press; 2015. p. 1369–85.
Ryu M-S, Aydemir TB. Chapter 23—Zinc. In: Marriott BP, Birt DF, Stallings VA, Yates AA, editors. Present knowledge in nutrition. 11th ed. Cambridge: Academic Press; 2020. p. 393–408.
Prasad R, Hawthorne B, Durai D, McDowell I. Zinc in denture adhesive: a rare cause of copper deficiency in a patient on home parenteral nutrition. BMJ Case Rep. 2015;2015:bcr2015211390.
Zinc Deficiency, Excess, and Supplementation [Internet]. 2022 [cited 2023 Nov 25]. Available from: https://patient.info/healthy-living/zinc-deficiency-excess-and-supplementation-leaflet
Wazir SM, Ghobrial I. Copper deficiency, a new triad: anemia, leucopenia, and myeloneuropathy. J Community Hosp Intern Med Perspect. 2017;7:265–8.
Collins JF, Prohaska JR, Knutson MD. Metabolic crossroads of iron and copper. Nutr Rev. 2010;68:133–47.
Greenberg MI, Vearrier D. Metal fume fever and polymer fume fever. Clin Toxicol (Phila). 2015;53:195–203.
Munie S, Pintavorn P. Erythropoietin-resistant anemia secondary to zinc-induced hypocupremia in a hemodialysis patient. Case Rep Nephrol Dial. 2021;11:167–75.
Amisha F, Saluja P, Gautam N, Biyani S, Kakadia S. Acquired hyperzincaemia due to zinc-laden denture adhesives leading to hypocupraemia as a cause of neutropenia. Eur J Case Rep Intern Med. 2021;8: 002983.
Duncan A, Morrison I, Bryson S. Iatrogenic copper deficiency: risks and cautions with zinc prescribing. Br J Clin Pharmacol. 2023;89:2825–9.
Gupta N, Carmichael MF. Zinc-induced copper deficiency as a rare cause of neurological deficit and anemia. Cureus. 2023;15:e43856.
Mehta KJ, Farnaud SJ, Sharp PA. Iron and liver fibrosis: mechanistic and clinical aspects. World J Gastroenterol. 2019;25:521–38.
Ali N, Ferrao K, Mehta KJ. Liver iron loading in alcohol-associated liver disease. Am J Pathol. 2022;193(10):1427–39.
Suriawinata E, Mehta KJ. Iron and iron-related proteins in COVID-19. Clin Exp Med. 2022;23(4):969–91. https://doi.org/10.1007/s10238-022-00851-y.
Ferrao K, Ali N, Mehta KJ. Iron and iron-related proteins in alcohol consumers: cellular and clinical aspects. J Mol Med. 2022;100:1673–89.
Acknowledgements
This article is made open access with the financial support of King’s College London, UK. Thanks to Najma Ali (GKT School of Medical Education, Faculty of Life Sciences and Medicine, King’s College London, UK) for providing some data that acted as a reference for writing a couple of paragraphs.
Funding
No funding was accessed/obtained for writing this review.
Author information
Authors and Affiliations
Contributions
LIS contributed to primary investigation and writing-original draft; KF contributed to further literature search, analysis, and interpretation of data; and KJM contributed to conceptualisation, supervision, writing and editing.
Corresponding author
Ethics declarations
Conflict of interest
Authors declare that they have no competing or financial interests to disclose.
Additional information
Publisher's Note
Springer Nature remains neutral with regard to jurisdictional claims in published maps and institutional affiliations.
Rights and permissions
Open Access This article is licensed under a Creative Commons Attribution 4.0 International License, which permits use, sharing, adaptation, distribution and reproduction in any medium or format, as long as you give appropriate credit to the original author(s) and the source, provide a link to the Creative Commons licence, and indicate if changes were made. The images or other third party material in this article are included in the article's Creative Commons licence, unless indicated otherwise in a credit line to the material. If material is not included in the article's Creative Commons licence and your intended use is not permitted by statutory regulation or exceeds the permitted use, you will need to obtain permission directly from the copyright holder. To view a copy of this licence, visit http://creativecommons.org/licenses/by/4.0/.
About this article
Cite this article
Stiles, L.I., Ferrao, K. & Mehta, K.J. Role of zinc in health and disease. Clin Exp Med 24, 38 (2024). https://doi.org/10.1007/s10238-024-01302-6
Received:
Accepted:
Published:
DOI: https://doi.org/10.1007/s10238-024-01302-6