Abstract
Objectives
Mandibular advancement devices (MADs) are the main therapeutic alternative to continuous positive airway pressure for obstructive sleep apnea. Our aim was to evaluate the long-term dentoskeletal side effects of MADs and to identify the predictive factors for these side effects.
Materials and methods
Patients from the Pays de la Loire cohort treated with a custom-made MAD for at least 1 year were included in this retrospective study. Digital cephalometric analyses were performed at baseline and at follow-up.
Results
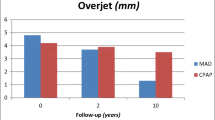
We included a total of 117 patients, treated with a MAD for a median [interquartile range] of 4.6 [2.6–6.6] years. The main significant side effects were a decrease in overbite (− 0.5 ± 1 mm), overjet (− 0.7 ± 1 mm) and maxillary incisor inclination (− 2.5 ± 2.8°) and an increase in mandibular incisor inclination (+ 2.2 ± 2.7°). Subjective side effects were not linked to the observed dentoskeletal changes. Current smokers were at higher risk of overjet modifications. A pre-existing anterior open-bite was associated with a greater decrease in overbite. Treatment duration was associated with a more pronounced mandibular incisor proclination. Propulsion was negatively associated with maxillary incisor retroclination.
Conclusions
Long-term dentoskeletal side effects were mainly moderate dental side effects. Some predictive factors were shown to be associated with more pronounced changes. Subjective side effects did not appear to be reliable tools to detect dentoskeletal side effects.
Clinical relevance
Regular follow-up with clinical examination and regular radiographs is mandatory. The predictive factors could be of interest for a better selection of patients and to individualize follow-up.



Similar content being viewed by others
References
Dempsey JA, Veasey SC, Morgan BJ, O’Donnell CP (2010) Pathophysiology of sleep apnea. Physiol Rev 90:47–112. https://doi.org/10.1152/physrev.00043.2008
George CF (2001) Reduction in motor vehicle collisions following treatment of sleep apnoea with nasal CPAP. Thorax 56:508–512. https://doi.org/10.1136/thorax.56.7.508
Marin JM, Carrizo SJ, Vicente E, Agusti AG (2005) Long-term cardiovascular outcomes in men with obstructive sleep apnoea-hypopnoea with or without treatment with continuous positive airway pressure: an observational study. Lancet 365:1046–1053. https://doi.org/10.1016/S0140-6736(05)71141-7
Gagnadoux F, Le Vaillant M, Goupil F, Pigeanne T, Chollet S, Masson P, Humeau MP, Bizieux-Thaminy A, Meslier N, group Isc (2011) Influence of marital status and employment status on long-term adherence with continuous positive airway pressure in sleep apnea patients. PLoS One 6:e22503. https://doi.org/10.1371/journal.pone.0022503
Sharples LD, Clutterbuck-James AL, Glover MJ, Bennett MS, Chadwick R, Pittman MA, Quinnell TG (2016) Meta-analysis of randomised controlled trials of oral mandibular advancement devices and continuous positive airway pressure for obstructive sleep apnoea-hypopnoea. Sleep Med Rev 27:108–124. https://doi.org/10.1016/j.smrv.2015.05.003
Chan AS, Sutherland K, Schwab RJ, Zeng B, Petocz P, Lee RW, Darendeliler MA, Cistulli PA (2010) The effect of mandibular advancement on upper airway structure in obstructive sleep apnoea. Thorax 65:726–732. https://doi.org/10.1136/thx.2009.131094
Minagi HO, Okuno K, Nohara K, Sakai T (2018) Predictors of side effects with long-term oral appliance therapy for obstructive sleep apnea. J Clin Sleep Med 14:119–125. https://doi.org/10.5664/jcsm.6896
Marklund M, Braem MJA, Verbraecken J (2019) Update on oral appliance therapy. Eur Respir Rev 28.https://doi.org/10.1183/16000617.0083-2019
Hamoda MM, Almeida FR, Pliska BT (2019) Long-term side effects of sleep apnea treatment with oral appliances: nature, magnitude and predictors of long-term changes. Sleep Med 56:184–191. https://doi.org/10.1016/j.sleep.2018.12.012
Vigie du Cayla G, Collet JM, Attali V, Kerbrat JB, Benslama L, Goudot P (2019) Long-term effectiveness and side effects of mandibular advancement devices on dental and skeletal parameters. J Stomatol Oral Maxillofac Surg 120:7–10. https://doi.org/10.1016/j.jormas.2018.09.005
Chen A, Burger MS, Rietdijk-Smulders M and Smeenk F (2020) Mandibular advancement device: Effectiveness and dental side effects. A real-life study. Cranio:1–10. https://doi.org/10.1080/08869634.2019.1708610
Fransson AMC, Benavente-Lundahl C, Isacsson G (2020) A prospective 10-year cephalometric follow-up study of patients with obstructive sleep apnea and snoring who used a mandibular protruding device. Am J Orthod Dentofacial Orthop 157:91–97. https://doi.org/10.1016/j.ajodo.2019.02.018
Uniken Venema JAM, Doff MHJ, Joffe-Sokolova DS, Wijkstra PJ, van der Hoeven JH, Stegenga B, Hoekema A (2020) Dental side effects of long-term obstructive sleep apnea therapy: a 10-year follow-up study. Clin Oral Investig 24:3069–3076. https://doi.org/10.1007/s00784-019-03175-6
Araie T, Okuno K, Ono Minagi H, Sakai T (2018) Dental and skeletal changes associated with long-term oral appliance use for obstructive sleep apnea: a systematic review and meta-analysis. Sleep Med Rev 41:161–172. https://doi.org/10.1016/j.smrv.2018.02.006
Justeau G, Gerves-Pinquie C, Le Vaillant M, Trzepizur W, Meslier N, Goupil F, Pigeanne T, Launois S, Leclair-Visonneau L, Masson P, Bizieux-Thaminy A, Humeau MP, Gosselin C, Blanchard M, Urban T, Gagnadoux F, Group ES (2020) Association between nocturnal hypoxemia and cancer incidence in patients investigated for OSA: data from a large multicenter French cohort. Chest 158:2610–2620. https://doi.org/10.1016/j.chest.2020.06.055
Gagnadoux F, Nguyen XL, Le Vaillant M, Priou P, Meslier N, Eberlein A, Kun-Darbois JD, Chaufton C, Villiers B, Levy M, Trzepizur W, Launois S (2017) Comparison of titrable thermoplastic versus custom-made mandibular advancement device for the treatment of obstructive sleep apnoea. Respir Med 131:35–42. https://doi.org/10.1016/j.rmed.2017.08.004
(1999) Sleep-related breathing disorders in adults: recommendations for syndrome definition and measurement techniques in clinical research. The Report of an American Academy of Sleep Medicine Task Force. Sleep 22:667–89
Mercier J (2000) Delaire’s craniofacial architectural analysis. A reminder of the changes introduced by its designer in 1994. Rev Stomatol Chir Maxillofac 101:12–16
Nimeskern N, Mercier JM (2002) The C0 line: from Delaire’s analysis of craniofacial structure to modeling it on a computer spreadsheet. Rev Stomatol Chir Maxillofac 103:327–334
Marion F, Mercier JM, Odri GA, Perrin JP, Longis J, Kun-Darbois JD, Corre P, Bertin H (2019) Associated relapse factors in Le Fort I osteotomy. A retrospective study of 54 cases. J Stomatol Oral Maxillofac Surg 120:419–427. https://doi.org/10.1016/j.jormas.2018.11.020
Delaire J (1978) Architectural and structural craniofacial analysis (lateral view). Theoretical principles. Some example of its use in maxillofacial surgery (author’s transl). Rev Stomatol Chir Maxillofac 79:1–33
Delaire J, Schendel SA, Tulasne JF (1981) An architectural and structural craniofacial analysis: a new lateral cephalometric analysis. Oral Surg Oral Med Oral Pathol 52:226–238. https://doi.org/10.1016/0030-4220(81)90252-8
Afrand M, Ling CP, Khosrotehrani S, Flores-Mir C, Lagravere-Vich MO (2014) Anterior cranial-base time-related changes: a systematic review. Am J Orthod Dentofacial Orthop 146:21-32.e6. https://doi.org/10.1016/j.ajodo.2014.03.019
Trzepizur W, Le Vaillant M, Meslier N, Pigeanne T, Masson P, Humeau MP, Bizieux-Thaminy A, Goupil F, Chollet S, Ducluzeau PH, Gagnadoux F, Institut de RechercheenSanteRespiratoire des Pays de la Loire Sleep Cohort G (2013) Independent association between nocturnal intermittent hypoxemia and metabolic dyslipidemia. Chest 143:1584–1589. https://doi.org/10.1378/chest.12-1652
Robertson CJ (2001) Dental and skeletal changes associated with long-term mandibular advancement. Sleep 24:531–537. https://doi.org/10.1093/sleep/24.5.531
Hammond RJ, Gotsopoulos H, Shen G, Petocz P, Cistulli PA, Darendeliler MA (2007) A follow-up study of dental and skeletal changes associated with mandibular advancement splint use in obstructive sleep apnea. Am J Orthod Dentofacial Orthop 132:806–814. https://doi.org/10.1016/j.ajodo.2005.08.047
Doff MH, Hoekema A, Pruim GJ, Huddleston Slater JJ, Stegenga B (2010) Long-term oral-appliance therapy in obstructive sleep apnea: a cephalometric study of craniofacial changes. J Dent 38:1010–1018. https://doi.org/10.1016/j.jdent.2010.08.018
Wang X, Gong X, Yu Z, Gao X, Zhao Y (2015) Follow-up study of dental and skeletal changes in patients with obstructive sleep apnea and hypopnea syndrome with long-term treatment with the Silensor appliance. Am J Orthod Dentofacial Orthop 147:559–565. https://doi.org/10.1016/j.ajodo.2015.01.013
Marklund M (2006) Predictors of long-term orthodontic side effects from mandibular advancement devices in patients with snoring and obstructive sleep apnea. Am J Orthod Dentofacial Orthop 129:214–221. https://doi.org/10.1016/j.ajodo.2005.10.004
Almeida FR, Lowe AA, Otsuka R, Fastlicht S, Farbood M, Tsuiki S (2006) Long-term sequellae of oral appliance therapy in obstructive sleep apnea patients: part 2. Study-model analysis. Am J Orthod Dentofacial Orthop 129:205–213. https://doi.org/10.1016/j.ajodo.2005.04.034
Pliska BT, Nam H, Chen H, Lowe AA, Almeida FR (2014) Obstructive sleep apnea and mandibular advancement splints: occlusal effects and progression of changes associated with a decade of treatment. J Clin Sleep Med 10:1285–1291. https://doi.org/10.5664/jcsm.4278
Alessandri-Bonetti G, D’Anto V, Stipa C, Rongo R, Incerti-Parenti S, Michelotti A (2017) Dentoskeletal effects of oral appliance wear in obstructive sleep apnoea and snoring patients. Eur J Orthod 39:482–488. https://doi.org/10.1093/ejo/cjw078
Almeida FR, Lowe AA, Sung JO, Tsuiki S, Otsuka R (2006) Long-term sequellae of oral appliance therapy in obstructive sleep apnea patients: part 1. Cephalometric analysis. Am J Orthod Dentofacial Orthop 129:195–204. https://doi.org/10.1016/j.ajodo.2005.10.001
Bondemark L (1999) Does 2 years’ nocturnal treatment with a mandibular advancement splint in adult patients with snoring and OSAS cause a change in the posture of the mandible? Am J Orthod Dentofacial Orthop 116:621–628. https://doi.org/10.1016/s0889-5406(99)70196-4
Garson S, Delay E, Sinna R, de Saint C, Cyr B, Taha F (2017) The third dimension of the face aging, improvement of its understanding. Ann Chir Plast Esthet 62:387–398. https://doi.org/10.1016/j.anplas.2017.09.001
Leite FRM, Nascimento GG, Scheutz F, Lopez R (2018) Effect of smoking on periodontitis: a systematic review and meta-regression. Am J Prev Med 54:831–841. https://doi.org/10.1016/j.amepre.2018.02.014
Giannasi LC, Almeida FR, Magini M, Costa MS, de Oliveira CS, de Oliveira JC, Kalil Bussadori S, de Oliveira LV (2009) Systematic assessment of the impact of oral appliance therapy on the temporomandibular joint during treatment of obstructive sleep apnea: long-term evaluation. Sleep Breath 13:375–381. https://doi.org/10.1007/s11325-009-0257-3
Martinez-Gomis J, Willaert E, Nogues L, Pascual M, Somoza M, Monasterio C (2010) Five years of sleep apnea treatment with a mandibular advancement device. Side effects and technical complications. Angle Orthod 80:30–36. https://doi.org/10.2319/030309-122.1
Doff MH, Veldhuis SK, Hoekema A, Slater JJ, Wijkstra PJ, de Bont LG, Stegenga B (2012) Long-term oral appliance therapy in obstructive sleep apnea syndrome: a controlled study on temporomandibular side effects. Clin Oral Investig 16:689–697. https://doi.org/10.1007/s00784-011-0555-6
Perez CV, de Leeuw R, Okeson JP, Carlson CR, Li HF, Bush HM, Falace DA (2013) The incidence and prevalence of temporomandibular disorders and posterior open bite in patients receiving mandibular advancement device therapy for obstructive sleep apnea. Sleep Breath 17:323–332. https://doi.org/10.1007/s11325-012-0695-1
Fransson AM, Tegelberg A, Johansson A, Wenneberg B (2004) Influence on the masticatory system in treatment of obstructive sleep apnea and snoring with a mandibular protruding device: a 2-year follow-up. Am J Orthod Dentofacial Orthop 126:687–693. https://doi.org/10.1016/j.ajodo.2003.10.040
Acknowledgements
The authors are greatly indebted to Carole Boudet, Mylène Gandubert, and Karine Robin for data collection. Our thanks also go to Jean-Marc Lebas for radiological acquisitions. We thank Jean-Louis Racineux from the Institut de Recherche en Santé Respiratoire des Pays de la Loire.
Funding
This study was supported by a grant from the Pays de la Loire Respiratory Health Research Institute (IRSRPL).
Author information
Authors and Affiliations
Contributions
NB: design of the study, project development; data collection and management; cephalometric analysis; data analysis and interpretation; manuscript writing/editing. FG, JD, CGP, NM, WT, FCG, and JDKD contributed substantially to the study design, data analysis and interpretation, manuscript writing, and critical revision of the article. NB, FG, JD, CGP and JDKD had full access to all of the data in the study and take responsibility for the integrity of the data and the accuracy of the data analysis.
Corresponding author
Ethics declarations
Conflict of interest
FG reports grants and personal fees from RESMED, personal fees and non-financial support from SEFAM, personal fees from CIDELEC, personal fees and non-financial support from NOVARTIS, personal fees from ACTELION, non-financial support from BOEHRINGER INGELHEIM, personal fees and non-financial support from AIR LIQUIDE SANTE, non-financial support from ASTEN, personal fees and non-financial support from NYXOAH, personal fees and non-financial support from JAZZ Pharmaceutical, outside the submitted work.
Additional information
Publisher's Note
Springer Nature remains neutral with regard to jurisdictional claims in published maps and institutional affiliations.
Supplementary Information
Below is the link to the electronic supplementary material.
Rights and permissions
About this article
Cite this article
Baldini, N., Gagnadoux, F., Trzepizur, W. et al. Long-term dentoskeletal side effects of mandibular advancement therapy in patients with obstructive sleep apnea: data from the Pays de la Loire sleep cohort. Clin Oral Invest 26, 863–874 (2022). https://doi.org/10.1007/s00784-021-04064-7
Received:
Accepted:
Published:
Issue Date:
DOI: https://doi.org/10.1007/s00784-021-04064-7