Abstract
Purpose
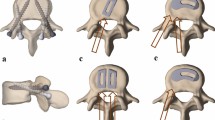
Discectomy and endplate preparation are important steps in interbody fusion for ensuring sufficient arthrodesis. While modern less-invasive approaches for lumbar interbody fusion have gained in popularity, concerns exist regarding their ability to allow for adequate disc space and endplate preparation. Thus, the purpose of this study was to quantitatively and qualitatively evaluate and compare disc space and endplate preparation achieved with four less-invasive approaches for lumbar interbody fusion in cadaveric spines.
Methods
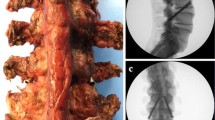
A total of 24 disc spaces (48 endplates) from L2 to L5 were prepared in eight cadaveric torsos using mini-open anterior lumbar interbody fusion (mini-ALIF), minimally invasive posterior lumbar interbody fusion (MAS PLIF), minimally invasive transforaminal lumbar interbody fusion (MAS TLIF) or minimally invasive lateral, transpsoas interbody fusion (XLIF) on two specimens each, for a total of six levels and 12 endplates prepared per procedure type. Following complete discectomy and endplate preparation, spines were excised and split axially at the interbody disc spaces. Endplates were digitally photographed and evaluated using image analysis software. Area of endplate preparation was measured and qualitative evaluation was also performed to grade the quality of preparation.
Results
The XLIF approach resulted in the greatest relative area of endplate preparation (58.3 %) while mini-ALIF resulted in the lowest at 35.0 %. Overall, there were no differences in percentage of preparation between cranial and caudal endplates, though this was significantly different in the XLIF group (65 vs 52 %, respectively). ALL damage was observed in 3 MAS TLIF levels. Percentage of endplate that was deemed to have complete disc removal was highest in XLIF group with 90 % compared to 65 % in MAS TLIF group, 43 % in MAS PLIF, and 40 % in mini-ALIF group. Endplate damage area was highest in the MAS TLIF group at 48 % and lowest in XLIF group at 4 %.
Conclusions
These results demonstrate that adequate endplate preparation for interbody fusion can be achieved utilizing various minimally invasive approach techniques (mini-ALIF, MAS TLIF, MAS PLIF, XLIF), however, XLIF appears to provide a greater area of and more complete endplate preparation.






Similar content being viewed by others
References
Madan S, Boeree NR (2002) Outcome of posterior lumbar interbody fusion versus posterolateral fusion for spondylolytic spondylolisthesis. Spine 27:1536–1542
Burkus JK (2002) Intervertebral fixation: clinical results with anterior cages. Orthop Clin North Am 33:349–357
Lowe TG, Hashim S, Wilson LA et al (2004) A biomechanical study of regional endplate strength and cage morphology as it relates to structural interbody support. Spine 29:2389–2394
Rihn JA, Gandhi SD, Sheehan P et al (2014) Disc space preparation in transforaminal lumbar interbody fusion: a comparison of minimally invasive and open approaches. Clin Orthop Relat Res 472:1800–1805
Brau SA (2002) Mini-open approach to the spine for anterior lumbar interbody fusion: description of the procedure, results and complications. Spine J 2:216–223
Ozgur BM, Yoo K, Rodriguez G, Taylor WR (2005) Minimally-invasive technique for transforaminal lumbar interbody fusion (TLIF). Eur Spine J 14:887–894
Berjano P, Lamartina C (2013) Far lateral approaches (XLIF) in adult scoliosis. Eur Spine J 22(Suppl 2):S242–S253
Ozgur BM, Aryan HE, Pimenta L, Taylor WR (2006) Extreme lateral interbody fusion (XLIF): a novel surgical technique for anterior lumbar interbody fusion. Spine J 6:435–443
Lane JD Jr, Moore ES Jr (1948) Transperitoneal approach to the intervertebral disc in the lumbar area. Ann Surg 127:537–551
Baker JK, Reardon PR, Reardon MJ, Heggeness MH (1993) Vascular injury in anterior lumbar surgery. Spine 18:2227–2230
Rajaraman V, Vingan R, Roth P, Heary RF, Conklin L, Jacobs GB (1999) Visceral and vascular complications resulting from anterior lumbar interbody fusion. J Neurosurg 91:60–64
Okuda S, Miyauchi A, Oda T, Haku T, Yamamoto T, Iwasaki M (2006) Surgical complications of posterior lumbar interbody fusion with total facetectomy in 251 patients. J Neurosurg Spine 4:304–309
Moskowitz A (2002) Transforaminal lumbar interbody fusion. Orthop Clin North Am 33:359–366
Javernick MA, Kuklo TR, Polly DW Jr (2003) Transforaminal lumbar interbody fusion: unilateral versus bilateral disk removal—an in vivo study. Am J Orthop (Belle Mead NJ) 32:344–348
Closkey RF, Parsons JR, Lee CK, Blacksin MF, Zimmerman MC (1993) Mechanics of interbody spinal fusion. Analysis of critical bone graft area. Spine 18:1011–1015
McAfee PC (1999) Interbody fusion cages in reconstructive operations on the spine. J Bone Joint Surg Am 81:859–880
Grant JP, Oxland TR, Dvorak MF (2001) Mapping the structural properties of the lumbosacral vertebral endplates. Spine 26:889–896
Conflict of interest
Dr Tatsumi is a consultant for NuVasive, Inc., Dr. Lee has no conflicts to report, Dr. Khajavi receives honoraria from and is a consultant for NuVasive, Inc., Dr. Taylor receives royalties from and is a consultant for NuVasive, Inc., Dr. Chen has no conflicts to report, and Dr. Bae is a consultant for and receives royalties from NuVasive, Inc.
Author information
Authors and Affiliations
Corresponding author
Rights and permissions
About this article
Cite this article
Tatsumi, R., Lee, YP., Khajavi, K. et al. In vitro comparison of endplate preparation between four mini-open interbody fusion approaches. Eur Spine J 24 (Suppl 3), 372–377 (2015). https://doi.org/10.1007/s00586-014-3708-x
Received:
Revised:
Accepted:
Published:
Issue Date:
DOI: https://doi.org/10.1007/s00586-014-3708-x