Abstract
Purpose
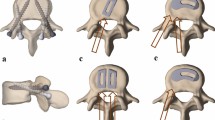
To investigate biomechanical properties of posterior transpedicular–transdiscal (TPTD) oblique lumbar screw fixation whereby the screw traverses the inferior pedicle across the posterior disc space into the super-adjacent body and lateral trapezoidal interbody spacer.
Methods
Eight fresh–frozen osteoligamentous human cadaveric spines (L1–S1) were tested in flexion–extension (FE), lateral bending (LB), and axial rotation (AR), with pure bending moment set at 7.5 Nm. Surgical constructs included (1) intact spine; (2) bilateral pedicle screw (BPS) fixation at L3–L4; (3) TPTD screw fixation at L3–L4; (4) lateral L3–L4 discectomy; (5) TPTD screw fixation with lateral interbody spacer (TPTD+S); and (6) BPS fixation with lateral interbody spacer (BPS+S). Peak range of motion (ROM) at L3–L4 was normalized to intact for statistical analysis.
Results
In FE and LB, all posterior fixation with or without interbody spacers significantly reduced motion compared with intact and discectomy. BPS and BPS+S provided increased fixation in all planes of motion; significantly reducing FE and LB motion relative to TPTD (p = 0.005, p = 0.002 and p = 0.020, p = 0.004, respectively). In AR, only BPS significantly reduced normalized ROM to intact (p = 0.034); BPS+S provided greater fixation compared with TPTD+S (p = 0.005).
Conclusions
Investigators found less stiffness with TPTD screw fixation than with BPS regardless of immediate stabilization with lateral discectomy and spacer. Clinical use should be decided by required biomechanical performance, difficulty of installation, and extent of paraspinal tissue disruption.






Similar content being viewed by others
References
Umeta RS, Avanzi O (2011) Techniques of lumbar-sacral spine fusion in spondylosis: systematic literature review and meta-analysis of randomized clinical trials. Spine J 11:668–676. doi:10.1016/j.spinee.2011.04.026
Suk SI, Kim JH, Kim SS, Lim DJ (2012) Pedicle screw instrumentation in adolescent idiopathic scoliosis (AIS). Eur Spine J 21:13–22. doi:10.1007/s00586-011-1986-0
Boos N, Webb JK (1997) Pedicle screw fixation in spinal disorders: a European view. Eur Spine J 6:2–18
Adogwa O, Parker SL, Davis BJ, Aaronson O, Devin C, Cheng JS, McGirt MJ (2011) Cost-effectiveness of transforaminal lumbar interbody fusion for Grade I degenerative spondylolisthesis. J Neurosurg Spine 15:138–143. doi:10.3171/2011.3.SPINE10562
Jutte PC, Castelein RM (2002) Complications of pedicle screws in lumbar and lumbosacral fusions in 105 consecutive primary operations. Eur Spine J 11:594–598. doi:10.1007/s00586-002-0469-8
Koutsoumbelis S, Hughes AP, Girardi FP, Cammisa FP Jr, Finerty EA, Nguyen JT, Gausden E, Sama AA (2011) Risk factors for postoperative infection following posterior lumbar instrumented arthrodesis. J Bone Joint Surg Am 93:1627–1633. doi:10.2106/JBJS.J.00039
Lonstein JE, Denis F, Perra JH, Pinto MR, Smith MD, Winter RB (1999) Complications associated with pedicle screws. J Bone Joint Surg Am 81:1519–1528
Dickman CA, Fessler RG, MacMillan M, Haid RW (1992) Transpedicular screw-rod fixation of the lumbar spine: operative technique and outcome in 104 cases. J Neurosurg 77:860–870. doi:10.3171/jns.1992.77.6.0860
Birkenmaier C (2012) Guided Oblique Lumbar Interbody Fusion (GO-LIF®). In: Vieweg U, Grochulla F (eds) Manual of spine surgery. Springer, Berlin, pp 391–401
Logroscino CA, Tamburrelli FC, Scaramuzzo L, Schiro GR, Sessa S, Proietti L (2012) Transdiscal L5-S1 screws for the treatment of adult spondylolisthesis. Eur Spine J 21(Suppl 1):S128–S133. doi:10.1007/s00586-012-2229-8
Palejwala A, Fridley J, Jea A (2016) Transsacral transdiscal L5-S1 screws for the management of high-grade spondylolisthesis in an adolescent. J Neurosurg Pediatr 17:645–650. doi:10.3171/2015.12.PEDS15535
Grob D, Humke T, Dvorak J (1996) Direct pediculo-body fixation in cases of spondylolisthesis with advanced intervertebral disc degeneration. Eur Spine J 5:281–285
Zagra A, Giudici F, Minoia L, Corriero AS, Zagra L (2009) Long-term results of pediculo-body fixation and posterolateral fusion for lumbar spondylolisthesis. Eur Spine J 18(Suppl 1):151–155. doi:10.1007/s00586-009-0997-6
St Clair S, Tan JS, Lieberman I (2012) Oblique lumbar interbody fixation: a biomechanical study in human spines. J Spinal Disord Tech 25:183–189. doi:10.1097/BSD.0b013e318211fc6b
Wu AM, Ni WF, Shao ZX, Kong XJ, Tian NF, Huang YX, Lin ZK, Xu HZ, Chi YL (2015) Percutaneous posterior transdiscal oblique screw fixation with lateral interbody fusion: a radiological and cadaveric study. Eur Spine J 24:852–858. doi:10.1007/s00586-014-3663-6
Wu AM, Tian NF, Wu LJ, He W, Ni WF, Wang XY, Xu HZ, Chi YL (2013) A radiological and cadaveric study of oblique lumbar interbody fixation in patients with normal spinal anatomy. Bone Joint J. 95:977–982. doi:10.1302/0301-620X.95B7.31393
Minamide A, Akamaru T, Yoon ST, Tamaki T, Rhee JM, Hutton WC (2003) Transdiscal L5-S1 screws for the fixation of isthmic spondylolisthesis: a biomechanical evaluation. J Spinal Disord Tech 16:144–149
Aghayev K, Gonzalez-Blohm SA, Doulgeris JJ, Lee WE 3rd, Waddell JK, Vrionis FD (2014) Feasibility and biomechanical performance of a novel transdiscal screw system for one level in non-spondylolisthetic lumbar fusion: an in vitro investigation. Spine J 14:705–713. doi:10.1016/j.spinee.2013.08.033
Birkenmaier C, Suess O, Pfeiffer M, Burger R, Schmieder K, Wegener B (2010) The European multicenter trial on the safety and efficacy of guided oblique lumbar interbody fusion (GO-LIF). BMC Musculoskelet Disord 11:199. doi:10.1186/1471-2474-11-199
Arlet V, Aebi M (2013) Junctional spinal disorders in operated adult spinal deformities: present understanding and future perspectives. Eur Spine J 22(Suppl 2):S276–S295. doi:10.1007/s00586-013-2676-x
Liu X, Wang Y, Qiu G, Weng X, Yu B (2014) A systematic review with meta-analysis of posterior interbody fusion versus posterolateral fusion in lumbar spondylolisthesis. Eur Spine J 23:43–56. doi:10.1007/s00586-013-2880-8
Tan JS, Kayanja MM, St Clair SF (2010) The difference in spine specimen dual-energy X-ray absorptiometry bone mineral density between in situ and in vitro scans. Spine J 10:784–788. doi:10.1016/j.spinee.2010.02.016
Frost HM (1994) Wolff’s Law and bone’s structural adaptations to mechanical usage: an overview for clinicians. Angle Orthod 64:175–188. doi:10.1043/0003-3219(1994)064<0175:WLABSA>2.0.CO;2
Wilke HJ, Krischak S, Claes L (1996) Biomechanical comparison of calf and human spines. J Orthop Res 14:500–503. doi:10.1002/jor.1100140321
Panjabi MM, Oxland TR, Yamamoto I, Crisco JJ (1994) Mechanical behavior of the human lumbar and lumbosacral spine as shown by three-dimensional load-displacement curves. J Bone Joint Surg Am 76:413–424
Maletsky LP, Sun J, Morton NA (2007) Accuracy of an optical active-marker system to track the relative motion of rigid bodies. J Biomech 40:682–685. doi:10.1016/j.jbiomech.2006.01.017
Schmidt J, Berg DR, Ploeg HL, Ploeg L (2009) Precision, repeatability and accuracy of Optotrak optical motion tracking systems. Int J Exp Comput Biomech. 1(1):114–127
Erdfelder E, Faul F, Buchner A (1996) GPOWER: a General Power Analysis Program. Behav Res Methods Instrum Comput 28:1–11. doi:10.3758/BF03203630
Klemencsics I, Lazary A, Szoverfi Z, Bozsodi A, Eltes P, Varga PP (2016) Risk factors for surgical site infection in elective routine degenerative lumbar surgeries. Spine J. doi:10.1016/j.spinee.2016.08.018
Olsen MA, Nepple JJ, Riew KD, Lenke LG, Bridwell KH, Mayfield J, Fraser VJ (2008) Risk factors for surgical site infection following orthopaedic spinal operations. J Bone Joint Surg Am 90:62–69. doi:10.2106/JBJS.F.01515
Davne SH, Myers DL (1992) Complications of lumbar spinal fusion with transpedicular instrumentation. Spine (Phila Pa 1976) 17:S184–S189
Galbusera F, Volkheimer D, Reitmaier S, Berger-Roscher N, Kienle A, Wilke HJ (2015) Pedicle screw loosening: a clinically relevant complication? Eur Spine J 24:1005–1016. doi:10.1007/s00586-015-3768-6
Abdu WA, Wilber RG, Emery SE (1994) Pedicular transvertebral screw fixation of the lumbosacral spine in spondylolisthesis. A new technique for stabilization. Spine (Phila Pa 1976). 19:710–715
West JL, Ogilvie JW, Bradford DS (1991) Complications of the variable screw plate pedicle screw fixation. Spine (Phila Pa 1976). 16:576–579
McAfee PC, Yuan HA, Fredrickson BE, Lubicky JP (1983) The value of computed tomography in thoracolumbar fractures. An analysis of one hundred consecutive cases and a new classification. J Bone Joint Surg Am 65:461–473
Bergmark A (1989) Stability of the lumbar spine. A study in mechanical engineering. Acta Orthop Scand Suppl 230:1–54
Zhou ZJ, Zhao FD, Fang XQ, Zhao X, Fan SW (2011) Meta-analysis of instrumented posterior interbody fusion versus instrumented posterolateral fusion in the lumbar spine. J Neurosurg Spine 15:295–310. doi:10.3171/2011.4.SPINE10330
Hart RA, Domes CM, Goodwin B, D’Amato CR, Yoo JU, Turker RJ, Halsey MF (2014) High-grade spondylolisthesis treated using a modified Bohlman technique: results among multiple surgeons. J Neurosurg Spine 20:523–530. doi:10.3171/2014.1.SPINE12904
Bohlman HH, Cook SS (1982) One-stage decompression and posterolateral and interbody fusion for lumbosacral spondyloptosis through a posterior approach. Report of two cases. J Bone Joint Surg Am 64:415–418
Pimenta L (2001) Lateral endoscopic transpsoas retroperitoneal approach for lumbar spine surgery. Paper presentation at the VIII Brazilian Spine Society Meeting, Belo Horizonte, Minas Gerais, Brazil, May
Ozgur BM, Aryan HE, Pimenta L, Taylor WR (2006) Extreme lateral interbody fusion (XLIF): a novel surgical technique for anterior lumbar interbody fusion. Spine J 6:435–443. doi:10.1016/j.spinee.2005.08.012
Kelly MR, Perez-Orribo L, Reyes P, Godzik J, Kalb E. Martinez del-Campo V, Singh A. Newcomb N. Crawford (2016) Biomechanical Evaluation of Interbody Fixation with Secondary Augmentation: Direct Lateral versus Posterior and Transforaminal Interbody Fusion. In: International Society for the Advancement of Spine Surgery. Las Vegas
Sembrano JN, Yson SC, Horazdovsky RD, Santos ER, Polly DW Jr (2015) Radiographic comparison of lateral lumbar interbody fusion versus traditional fusion approaches: analysis of sagittal contour change. Int J Spine Surg 9:16. doi:10.14444/2016
Rodgers WB, Gerber EJ, Patterson J (2011) Intraoperative and early postoperative complications in extreme lateral interbody fusion: an analysis of 600 cases. Spine (Phila Pa 1976). 36:26–32. doi:10.1097/BRS.0b013e3181e1040a
Youssef JA, McAfee PC, Patty CA, Raley E, DeBauche S, Shucosky E, Chotikul L (2010) Minimally invasive surgery: lateral approach interbody fusion: results and review. Spine (Phila Pa 1976). 35:S302–S311. doi:10.1097/BRS.0b013e3182023438
Shen FH, Samartzis D, Khanna AJ, Anderson DG (2007) Minimally invasive techniques for lumbar interbody fusions. Orthop Clin N Am 38:373–386. doi:10.1016/j.ocl.2007.04.002
Pimenta L, Turner AW, Dooley ZA, Parikh RD, Peterson MD (2012) Biomechanics of lateral interbody spacers: going wider for going stiffer. Sci World J 2012:381814. doi:10.1100/2012/381814
Haughton VM, Schmidt TA, Keele K, An HS, Lim TH (2000) Flexibility of lumbar spinal motion segments correlated to type of tears in the annulus fibrosus. J Neurosurg 92(1 Suppl):81–86
Li N, He D, Xing Y, Lv Y, Tian W (2015) The effect of lateral wall perforation on screw pull-out strength: a cadaveric study. J Orthop Surg Res 10:6. doi:10.1186/s13018-015-0157-0
Goda Y, Higashino K, Toki S, Suzuki D, Kobayashi T, Matsuura T, Fujimiya M, Hutton WC, Fukui Y, Sairyo K (2016) The pullout strength of pedicle screws following redirection after lateral wall breach or end-plate breach. Spine (Phila Pa 1976). 41:1218–1223. doi:10.1097/BRS.0000000000001600
Nottmeier EW, Pirris SM (2013) Placement of thoracic transvertebral pedicle screws using 3D image guidance. J Neurosurg Spine 18:479–483. doi:10.3171/2013.2.SPINE12819
Acknowledgements
The authors would like to thank Dolores Matthews, MEd, ELS, for contributions in editing the manuscript.
Funding
National Natural Sciences Foundation of China (No. 81501933) and Xinmiao Talent Plan of Zhejiang Province (No. 2014R413053).
Author information
Authors and Affiliations
Corresponding author
Ethics declarations
The authors performed this study in the biomechanical laboratory at Globus Medical, Inc. (GMI), using its six-degrees-of-freedom motion simulator. A-MW and Y-LC have no financial relationships with GMI. A-MW was supported by National Natural Sciences Foundation of China (No. 81501933) and Xinmiao Talent Plan of Zhejiang Province (No. 2014R413053). National Natural Sciences Foundation of China and Xinmiao Talent Plan of Zhejiang Province paid all travel fees but had no role in designing or conducting this study. Funders had no role in study design, data collection and analysis, decision to publish, or manuscript preparation. Cadaveric specimens and related materials were provided by GMI, at which JAH and BSB are employees. JCH and SMJ are visiting interns.
Conflict of interest
BSB and JAH are paid employees of Globus Medical, Inc., JCH and SMJ were temporary, hourly paid interns of Globus Medical, Inc., YLC and AMW have nothing to disclose.
Rights and permissions
About this article
Cite this article
Wu, AM., Harris, J.A., Hao, J.C. et al. Biomechanical properties of posterior transpedicular–transdiscal oblique lumbar screw fixation with novel trapezoidal lateral interbody spacer: an in vitro human cadaveric model. Eur Spine J 26, 2873–2882 (2017). https://doi.org/10.1007/s00586-017-5050-6
Received:
Revised:
Accepted:
Published:
Issue Date:
DOI: https://doi.org/10.1007/s00586-017-5050-6