Abstract
Background
We validated the prevalence of albuminuria and its association with kidney function and hemodynamics in pre-school children who underwent surgery for congenital heart disease (CHD).
Methods
From 403 patients who had undergone surgery for CHD at least 6 months before pre-school and were admitted to our hospital between 2011 and 2015, 75 who underwent blood and urine tests and cardiac catheterization were included in this study. The urinary albumin-to-creatinine ratio (ACR) was quantified, and the relationship of ACR with physical and laboratory findings and hemodynamics assessed using cardiac catheterization was analyzed.
Results
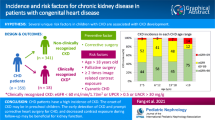
The study cohort was divided into three groups: Fontan group (n = 25), tetralogy of Fallot (TOF) group (n = 18), and control group (other biventricular CHDs; n = 32). The median age of patients was 5.9 years. ACR was higher in the Fontan group than in the TOF and control groups (median: 15.0 vs. 5.0 and 0.0 mg/g, p < 0.001). Moreover, albuminuria (ACR > 30 mg/g) was observed in 20.0% of Fontan patients, while ACR was associated with potential complicating factors of Fontan circulation: high central venous pressure, high mean pulmonary artery pressure, and worse than moderate atrioventricular regurgitation. ACR showed a moderate correlation with the cystatin C-based estimated glomerular filtration rate (r = − 0.725, p < 0.001).
Conclusions
Measurement of albuminuria in Fontan patients before they join elementary school is useful because it reflects kidney function and hemodynamic factors that can worsen their condition. Identification and management of patients with albuminuria may facilitate early therapeutic intervention for worsening Fontan factors, eventually delaying the deterioration of kidney function.
Graphical abstract

A higher resolution version of the Graphical abstract is available as Supplementary information






Similar content being viewed by others
Data availability
The data that support the findings of this study are available on request from the corresponding author, Kentaro Ueno. The data are not publicly available due to privacy restrictions.
References
Morgan C, Al-Aklabi M, Guerra GG (2015) Chronic kidney disease in congenital heart disease patients: a narrative review of evidence. Can J Kidney Health Dis 2:27. https://doi.org/10.1186/s40697-015-0063-8
Schwartz GJ, Work DF (2009) Measurement and estimation of GFR in children and adolescents. Clin J Am Soc Nephrol 4:1832–1843. https://doi.org/10.2215/CJN.01640309
Peralta CA, Shlipak MG, Judd S et al (2011) Detection of chronic kidney disease with creatinine, cystatin C, and urine albumin-to-creatinine ratio and association with progression to end-stage renal disease and mortality. JAMA 305:1545–1552. https://doi.org/10.1001/jama.2011.468
Rajpal S, Alshawabkeh L, Almaddah N et al (2018) Association of albuminuria with major adverse outcomes in adults with congenital heart disease: results from the Boston adult congenital heart biobank. JAMA Cardiol 3:308–316. https://doi.org/10.1001/jamacardio.2018.0125
Seliger SL, Salimi S, Pierre V et al (2016) Microvascular endothelial dysfunction is associated with albuminuria and CKD in older adults. BMC Nephrol 17:82. https://doi.org/10.1186/s12882-016-0303-x
Lee BJ (2019) The kidney in congenital cyanotic heart disease. Methodist Debakey Cardiovasc J 15:158–159. https://doi.org/10.14797/mdcj-15-2-158
Ross RD (2012) The Ross classification for heart failure in children after 25 years: a review and an age-stratified revision. Pediatr Cardiol 33:1295–1300. https://doi.org/10.1007/s00246-012-0306-8
Kellum JA, Lameire N, Aspelin P et al (2012) Kidney disease: improving global outcomes (KDIGO) acute kidney injury work group. KDIGO clinical practice guideline for acute kidney injury. Kidney Int Suppl 2:1–138. https://doi.org/10.1038/kisup.2012.1
Ueno K, Seki S, Shiokawa N et al (2019) Validation of acute kidney injury according to the modified KDIGO criteria in infants after cardiac surgery for congenital heart disease. Nephrology (Carlton) 24:294–300. https://doi.org/10.1111/nep.13240
Uemura O, Nagai T, Ishikura K et al (2014) Creatinine-based equation to estimate the glomerular filtration rate in Japanese children and adolescents with chronic kidney disease. Clin Exp Nephrol 18:626–633. https://doi.org/10.1007/s10157-013-0856-y
Gotoh Y, Uemura O, Ishikura K et al (2018) Validation of estimated glomerular filtration rate equations for Japanese children. Clin Exp Nephrol 22:931–937. https://doi.org/10.1007/s10157-018-1529-7
Uemura O, Nagai T, Ishikura K et al (2014) Cystatin C-based equation for estimating glomerular filtration rate in Japanese children and adolescents. Clin Exp Nephrol 18:718–725. https://doi.org/10.1007/s10157-013-0910-9
Anil AB, Anil M, Yildiz M et al (2014) The importance of albuminuria in predicting patient outcome in a PICU. Pediatr Crit Care Med 15:e220–e225. https://doi.org/10.1097/PCC.0000000000000113
Stevens PE, Levin A, Kidney Disease: Improving Global Outcomes Chronic Kidney Disease Guideline Development Work Group Members (2012) Evaluation and management of chronic kidney disease: synopsis of the kidney disease: improving global outcomes 2012 clinical practice guideline. Ann Intern Med 158:825–830. https://doi.org/10.7326/0003-4819-158-11-201306040-00007
Daymont C, Neal A, Prosnitz A et al (2013) Growth in children with congenital heart disease. Pediatrics 131:e236–e242. https://doi.org/10.1542/peds.2012-1157
Schwartz S, Olsen M, Woo JG et al (2017) Congenital heart disease and the prevalence of underweight and obesity from age 1 to 15 years: data on a nationwide sample of children. BMJ Pediatr Open 1:e000127. https://doi.org/10.1136/bmjpo-2017-000127
Tran D, D’Ambrosio P, Verrall C et al (2020) Body composition in young adults living with a Fontan circulation: the myopenic profile. J Am Heart Assoc 9:e015639. https://doi.org/10.1161/JAHA.119.015639
Coca SG, Yalavarthy R, Concato J et al (2008) Biomarkers for the diagnosis and risk stratification of acute kidney injury: a systematic review. Kidney Int 73:1008–1016. https://doi.org/10.1038/sj.ki.5002729
Bacchetta J, Cochat P, Rognant N et al (2011) Which creatinine and cystatin C equations can be reliably used in children? Clin J Am Soc Nephrol 6:552–560. https://doi.org/10.2215/CJN.04180510
Andersen TB, Eskild-Jensen A, Frokiaer J et al (2009) Measuring glomerular filtration rate in children; can cystatin C replace established methods? A review. Pediatr Nephrol 24:929–941. https://doi.org/10.1007/s00467-008-0991-y
Anne P, Du W, Mattoo TK et al (2009) Nephropathy in patients after Fontan palliation. Int J Cardiol 132:244–247. https://doi.org/10.1016/j.ijcard.2007.11.079
Opotowsky AR, Baraona FR, McCausland FR et al (2017) Estimated glomerular filtration rate and urine biomarkers in patients with single-ventricle Fontan circulation. Heart 103:434–442. https://doi.org/10.1136/heartjnl-2016-309729
Wilson TG, d’Udekem Y, Winlaw DS et al (2019) Creatinine-based estimation of glomerular filtration rate in patients with a Fontan circulation. Congenit Heart Dis 14:454–463. https://doi.org/10.1111/chd.12746
Fattah H, Layton A, Vallon V (2019) How do kidneys adapt to a deficit or loss in nephron number? Physiology (Bethesda) 34:189–197. https://doi.org/10.1152/physiol.00052.2018
Ritmeester E, Veger VA, van der Ven JPG et al (2022) Fontan circulation associated organ abnormalities beyond the heart, lungs, liver, and gut: a systematic review. Front Cardiovasc Med 9:826096. https://doi.org/10.3389/fcvm.2022.826096
Zafar F, Lubert AM, Katz DA et al (2020) Long-term kidney function after the Fontan operation: JACC review topic of the week. J Am Coll Cardiol 76:334–341. https://doi.org/10.1016/j.jacc.2020.05.042
Wilson T, d’Udekem Y, Winlaw D et al (2018) Hepatic and renal end-organ damage in the Fontan circulation: a report from the Australian and New Zealand Fontan Registry. Int J Cardiol 273:100–107. https://doi.org/10.1016/j.ijcard.2018.07.118
Madsen NL, Goldstein SL, Frøslev T et al (2017) Cardiac surgery in patients with congenital heart disease is associated with acute kidney injury and the risk of chronic kidney disease. Kidney Int 92:751–756. https://doi.org/10.1016/j.kint.2017.02.021
Greenberg JH, Zappitelli M, Devarajan P et al (2016) Kidney outcomes 5 years after pediatric cardiac surgery: the TRIBE-AKI study. JAMA Pediatr 170:1071–1078. https://doi.org/10.1001/jamapediatrics.2016.1532
Goldstein SL (2014) Renal recovery at different ages. Nephron Clin Pract 127:21–24. https://doi.org/10.1159/000363679
Brenner BM, Lawler EV, Mackenzie HS (1996) The hyperfiltration theory: a paradigm shift in nephrology. Kidney Int 49:1774–1777. https://doi.org/10.1038/ki.1996.265
Van den Eynde J, Salaets T, Louw JJ et al (2022) Persistent markers of kidney injury in children who developed acute kidney injury after pediatric cardiac surgery: a prospective cohort study. J Am Heart Assoc 11:e024266. https://doi.org/10.1161/JAHA.121.024266
Priyanka P, Zarbock A, Izawa J et al (2021) The impact of acute kidney injury by serum creatinine or urine output criteria on major adverse kidney events in cardiac surgery patients. J Thorac Cardiovasc Surg 162:143-151.e7. https://doi.org/10.1016/j.jtcvs.2019.11.137
Broda C, Sriraman H, Wadhwa D et al (2018) Renal dysfunction is associated with higher central venous pressures in patients with Fontan circulation. Congenit Heart Dis 13:602–607. https://doi.org/10.1111/chd.12617
Shimada S, Hirose T, Takahashi C et al (2018) Pathophysiological and molecular mechanisms involved in renal congestion in a novel rat model. Sci Rep 8:16808. https://doi.org/10.1038/s41598-018-35162-4
Owji SM, Nikeghbal E, Moosavi SM (2018) Comparison of ischaemia–reperfusion-induced acute kidney injury by clamping renal arteries, veins or pedicles in anaesthetized rats. Exp Physiol 103:1390–1402. https://doi.org/10.1113/EP087140
Rychik J (2016) The relentless effects of the Fontan paradox. Semin Thorac Cardiovasc Surg Pediatr Card Surg Annu 19:37–43. https://doi.org/10.1053/j.pcsu.2015.11.006
Husain-Syed F, Grone HJ, Assmus B et al (2021) Congestive nephropathy: a neglected entity? Proposal for diagnostic criteria and future perspectives. ESC Heart Fail 8:183–203. https://doi.org/10.1002/ehf2.13118
Acknowledgements
We thank the patients and their guardians for showing support for this project.
We thank Editage (www.editage.jp) for English proofreading.
Author information
Authors and Affiliations
Contributions
Conceptualization: Kentaro Ueno; methodology: Kentaro Ueno; formal analysis and investigation: Kentaro Ueno, Tsubasa Shimozono, Yoshihiro Takahashi, Koji Nakae, and Jumpei Kawamura; writing – original draft preparation: Kentaro Ueno; writing – review and editing: Yasuhiro Okamoto; supervision: Yasuhiro Okamoto. All authors read and approved the final manuscript.
Corresponding author
Ethics declarations
Ethical approval
All procedures performed in studies involving human participants were in accordance with the ethical standards of the institutional and/or national research committee (Kagoshima University Ethics Committee, 190055) and with the 1964 Helsinki Declaration and its later amendments or comparable ethical standards.
Informed consent
Due to the retrospective nature of this study, parental and patient informed consents were waived.
Competing interests
The authors declare no competing interests.
Additional information
Publisher's note
Springer Nature remains neutral with regard to jurisdictional claims in published maps and institutional affiliations.
Supplementary Information
Below is the link to the electronic supplementary material.
Rights and permissions
Springer Nature or its licensor (e.g. a society or other partner) holds exclusive rights to this article under a publishing agreement with the author(s) or other rightsholder(s); author self-archiving of the accepted manuscript version of this article is solely governed by the terms of such publishing agreement and applicable law.
About this article
Cite this article
Ueno, K., Shimozono, T., Takahashi, Y. et al. Association of albuminuria with kidney function and hemodynamic disturbance in pre-school children who undergo congenital heart disease surgery. Pediatr Nephrol 39, 493–503 (2024). https://doi.org/10.1007/s00467-023-06130-6
Received:
Revised:
Accepted:
Published:
Issue Date:
DOI: https://doi.org/10.1007/s00467-023-06130-6