Abstract
Purpose
Preoperative chemoradiotherapy (CRT) for rectal cancer is administered to improve local control, but can also induce severe anal dysfunction after surgery, while preoperative chemotherapy that significantly reduces the primary lesion in rectal cancer has recently been developed. The aim of the study was to examine differences in the effects of preoperative CRT and chemotherapy on tissue degeneration of patients with colorectal cancer.
Methods
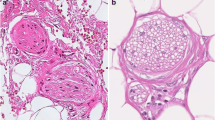
The subjects were 91 patients, including 68 with rectal cancer who underwent internal sphincteric resection with (n = 47, CRT group) or without (n = 21, control group) preoperative CRT, and 23 with colorectal cancer who received preoperative FOLFOX treatment. Peripheral nerve degeneration was evaluated histopathologically using H&E-stained sections, based on karyopyknosis, disparity of the nucleus, denucleation, vacuolar or acidophilic degeneration of the cytoplasm, and adventitial neuronal changes.
Results
The incidence of neural degeneration was significantly higher in the CRT group than in the control group and FOLFOX group. There were no differences in any items of neural degeneration between the FOLFOX and control groups.
Conclusion
CRT induced marked neural degeneration around the rectal tumor. FOLFOX treatment produced mild neural degeneration similar to that in the control group.


Similar content being viewed by others
References
Paty PB, Enker WE, Cohen AM, Lauwers GY (1994) Treatment of rectal cancer by low anterior resection with coloanal anastomosis. Ann Surg 219(4):365–373
Schiessel R, Karner-Hanusch J, Herbst F, Teleky B, Wunderlich M (1994) Intersphincteric resection for low rectal tumours. Br J Surg 81(9):1376–1378
Saito N, Sugito M, Ito M, Kobayashi A, Nishizawa Y, Yoneyama Y, Minagawa N (2009) Oncologic outcome of intersphincteric resection for very low rectal cancer. World J Surg. doi:10.1007/s00268-009-0079-2
Gamagami RA, Liagre A, Chiotasso P, Istvan G, Lazorthes F (1999) Coloanal anastomosis for distal third rectal cancer: prospective study of oncologic results. Dis Colon Rectum 42(10):1272–1275
Hohenberger W, Merkel S, Matzel K, Bittorf B, Papadopoulos T, Gohl J (2006) The influence of abdomino-peranal (intersphincteric) resection of lower third rectal carcinoma on the rates of sphincter preservation and locoregional recurrence. Colorectal Dis 8(1):23–33. doi:10.1111/j.1463-1318.2005.00839.x
Rullier E, Laurent C, Bretagnol F, Rullier A, Vendrely V, Zerbib F (2005) Sphincter-saving resection for all rectal carcinomas: the end of the 2-cm distal rule. Ann Surg 241(3):465–469
Bonadeo FA, Vaccaro CA, Benati ML, Quintana GM, Garione XE, Telenta MT (2001) Rectal cancer: local recurrence after surgery without radiotherapy. Dis Colon Rectum 44(3):374–379
Saito N, Ono M, Sugito M, Ito M, Morihiro M, Kosugi C, Sato K, Kotaka M, Nomura S, Arai M, Kobatake T (2004) Early results of intersphincteric resection for patients with very low rectal cancer: an active approach to avoid a permanent colostomy. Dis Colon Rectum 47(4):459–466. doi:10.1007/s10350-003-0088-4
Bretagnol F, Rullier E, Laurent C, Zerbib F, Gontier R, Saric J (2004) Comparison of functional results and quality of life between intersphincteric resection and conventional coloanal anastomosis for low rectal cancer. Dis Colon Rectum 47(6):832–838. doi:10.1007/s10350-004-0523-1
Tiret E, Poupardin B, McNamara D, Dehni N, Parc R (2003) Ultralow anterior resection with intersphincteric dissection—what is the limit of safe sphincter preservation? Colorectal Dis 5(5):454–457
Rullier E, Zerbib F, Laurent C, Bonnel C, Caudry M, Saric J, Parneix M (1999) Intersphincteric resection with excision of internal anal sphincter for conservative treatment of very low rectal cancer. Dis Colon Rectum 42(9):1168–1175
Kohler A, Athanasiadis S, Ommer A, Psarakis E (2000) Long-term results of low anterior resection with intersphincteric anastomosis in carcinoma of the lower one-third of the rectum: analysis of 31 patients. Dis Colon Rectum 43(6):843–850
Ito M, Saito N, Sugito M, Kobayashi A, Nishizawa Y, Tsunoda Y (2009) Analysis of clinical factors associated with anal function after intersphincteric resection for very low rectal cancer. Dis Colon Rectum 52(1):64–70. doi:10.1007/DCR.0b013e31819739a0
Chamlou R, Parc Y, Simon T, Bennis M, Dehni N, Parc R, Tiret E (2007) Long-term results of intersphincteric resection for low rectal cancer. Ann Surg 246(6):916–921, discussion 921-912. doi:10.1097/SLA.0b013e31815c29ff
Lim JF, Tang CL, Seow-Choen F, Heah SM (2005) Prospective, randomized trial comparing intraoperative colonic irrigation with manual decompression only for obstructed left-sided colorectal cancer. Dis Colon Rectum 48(2):205–209. doi:10.1007/s10350-004-0803-9
Chen FC, Mackay JR, Woods RJ, Collopy BT, Fink RJ, Guiney MJ (1995) Early experience with postoperative adjuvant chemoradiation for rectal carcinoma: focus on morbidity. Aust N Z J Surg 65(10):732–736
Kollmorgen CF, Meagher AP, Wolff BG, Pemberton JH, Martenson JA, Illstrup DM (1994) The long-term effect of adjuvant postoperative chemoradiotherapy for rectal carcinoma on bowel function. Ann Surg 220(5):676–682
Da Silva GM, Berho M, Wexner SD, Efron J, Weiss EG, Nogueras JJ, Vernava AM 3rd, Connor JT, Gervaz P (2003) Histologic analysis of the irradiated anal sphincter. Dis Colon Rectum 46(11):1492–1497. doi:10.1097/01.DCR.0000093642.89267.67
Nordlinger B, Sorbye H, Glimelius B, Poston GJ, Schlag PM, Rougier P, Bechstein WO, Primrose JN, Walpole ET, Finch-Jones M, Jaeck D, Mirza D, Parks RW, Collette L, Praet M, Bethe U, Van Cutsem E, Scheithauer W, Gruenberger T (2008) Perioperative chemotherapy with FOLFOX4 and surgery versus surgery alone for resectable liver metastases from colorectal cancer (EORTC intergroup trial 40983): a randomised controlled trial. Lancet 371(9617):1007–1016. doi:10.1016/S0140-6736(08)60455-9
Porschen R, Arkenau HT, Kubicka S, Greil R, Seufferlein T, Freier W, Kretzschmar A, Graeven U, Grothey A, Hinke A, Schmiegel W, Schmoll HJ (2007) Phase III study of capecitabine plus oxaliplatin compared with fluorouracil and leucovorin plus oxaliplatin in metastatic colorectal cancer: a final report of the AIO colorectal study group. J Clin Oncol 25(27):4217–4223. doi:10.1200/JCO.2006.09.2684
Diaz-Rubio E, Tabernero J, Gomez-Espana A, Massuti B, Sastre J, Chaves M, Abad A, Carrato A, Queralt B, Reina JJ, Maurel J, Gonzalez-Flores E, Aparicio J, Rivera F, Losa F, Aranda E (2007) Phase III study of capecitabine plus oxaliplatin compared with continuous-infusion fluorouracil plus oxaliplatin as first-line therapy in metastatic colorectal cancer: final report of the Spanish Cooperative Group for the treatment of digestive tumors trial. J Clin Oncol 25(27):4224–4230. doi:10.1200/JCO.2006.09.8467
Rothenberg ML, Cox JV, Butts C, Navarro M, Bang YJ, Goel R, Gollins S, Siu LL, Laguerre S, Cunningham D (2008) Capecitabine plus oxaliplatin (XELOX) versus 5-fluorouracil/folinic acid plus oxaliplatin (FOLFOX-4) as second-line therapy in metastatic colorectal cancer: a randomized phase III noninferiority study. Ann Oncol 19(10):1720–1726. doi:10.1093/annonc/mdn370
Chau I, Brown G, Cunningham D, Tait D, Wotherspoon A, Norman AR, Tebbutt N, Hill M, Ross PJ, Massey A, Oates J (2006) Neoadjuvant capecitabine and oxaliplatin followed by synchronous chemoradiation and total mesorectal excision in magnetic resonance imaging-defined poor-risk rectal cancer. J Clin Oncol 24(4):668–674. doi:10.1200/JCO.2005.04.4875
Sobin L, Wittekind CE, (UICC) IUAC (2002) TNM classification of malignant tumors, 6th edn. Wiley, New York
Saito N, Sarashina H, Nunomura M, Koda K, Takiguchi N, Nakajima N (1998) Clinical evaluation of nerve-sparing surgery combined with preoperative radiotherapy in advanced rectal cancer patients. Am J Surg 175(4):277–282
de Gramont A, Figer A, Seymour M, Homerin M, Hmissi A, Cassidy J, Boni C, Cortes-Funes H, Cervantes A, Freyer G, Papamichael D, Le Bail N, Louvet C, Hendler D, de Braud F, Wilson C, Morvan F, Bonetti A (2000) Leucovorin and fluorouracil with or without oxaliplatin as first-line treatment in advanced colorectal cancer. J Clin Oncol 18(16):2938–2947
Cavanna L, Artioli F, Codignola C, Lazzaro A, Rizzi A, Gamboni A, Rota L, Rodino C, Boni F, Iop A, Zaniboni A (2006) Oxaliplatin in combination with 5-fluorouracil (5-FU) and leucovorin (LV) in patients with metastatic gastric cancer (MGC). Am J Clin Oncol 29(4):371–375. doi:10.1097/01.coc.0000221358.57089.f2
Louvet C, Andre T, Tigaud JM, Gamelin E, Douillard JY, Brunet R, Francois E, Jacob JH, Levoir D, Taamma A, Rougier P, Cvitkovic E, de Gramont A (2002) Phase II study of oxaliplatin, fluorouracil, and folinic acid in locally advanced or metastatic gastric cancer patients. J Clin Oncol 20(23):4543–4548
Wilson RH, Lehky T, Thomas RR, Quinn MG, Floeter MK, Grem JL (2002) Acute oxaliplatin-induced peripheral nerve hyperexcitability. J Clin Oncol 20(7):1767–1774
Lehky TJ, Leonard GD, Wilson RH, Grem JL, Floeter MK (2004) Oxaliplatin-induced neurotoxicity: acute hyperexcitability and chronic neuropathy. Muscle Nerve 29(3):387–392. doi:10.1002/mus.10559
Gamelin L, Capitain O, Morel A, Dumont A, Traore S, le Anne B, Gilles S, Boisdron-Celle M, Gamelin E (2007) Predictive factors of oxaliplatin neurotoxicity: the involvement of the oxalate outcome pathway. Clin Cancer Res 13(21):6359–6368. doi:10.1158/1078-0432.CCR-07-0660
Park SB, Goldstein D, Lin CS, Krishnan AV, Friedlander ML, Kiernan MC (2009) Acute abnormalities of sensory nerve function associated with oxaliplatin-induced neurotoxicity. J Clin Oncol 27(8):1243–1249. doi:10.1200/JCO.2008.19.3425
Nishizawa Y, Fujii S, Saito N (2011) The association between anal function and neural degeneration after preoperative chemoradiotherapy followed by intersphincteric resection. Dis Colon Rectum 54. doi:10.1097/DCR.0b013e31822c94e6
Author information
Authors and Affiliations
Corresponding author
Rights and permissions
About this article
Cite this article
Nishizawa, Y., Fujii, S., Saito, N. et al. Differences in tissue degeneration between preoperative chemotherapy and preoperative chemoradiotherapy for colorectal cancer. Int J Colorectal Dis 27, 1047–1053 (2012). https://doi.org/10.1007/s00384-012-1434-6
Accepted:
Published:
Issue Date:
DOI: https://doi.org/10.1007/s00384-012-1434-6