Abstract
The management of patients with isolated congenital complete atrioventricular block (CCAVB) has changed during the last decades. The current policy is to pace the majority of patients based on a variety of criteria, among which is limited exercise capacity. Data regarding exercise capacity in this population stems from previous publications reporting small case series of unpaced patients. Therefore, we have investigated the exercise capacity of a group of contemporary children with CCAVB. Sixteen children (mean age 11.5 ± 4; seven boys, nine girls) with CCAVB were tested. In 13 patients, a median number of three pacemakers were implanted, whereas in three patients no pacemaker was given. All patients had an echocardiogram and completed a cardiopulmonary cycle exercise test. Exercise parameters were determined and compared with reference values obtained from healthy Dutch peers. The peak oxygen uptake/body mass was reduced to 34.4 ± 9.5 ml kg−1 min−1 (79 ± 24% of predicted) and the ventilatory threshold was reduced to 52 ± 17% of peak oxygen uptake (78 ± 21% of predicted), whereas the peak work load/body mass was 2.8 ± 0.6 W/kg (91 ± 24% of predicted), which was similar to controls. Importantly, 25% of the paced patients showed upper rate restriction by the pacemaker. In conclusion, children with CCAVB show a reduced peak oxygen uptake and ventilatory threshold, whereas they show normal peak work rates. This indicates that they generate more energy during exercise from anaerobic energy sources. Paced children with CCAVB do not perform better than unpaced children.
Similar content being viewed by others
Avoid common mistakes on your manuscript.
Introduction
Isolated congenital complete atrioventricular block (CCAVB) is a rare cardiac disorder with an estimated incidence of 1/15,000–20,000 live births [27]. In most cases it occurs after damage of a normally structured fetal heart by maternal autoantibodies against ribonucleoproteins (anti-Ro/SSA, anti-La/SSB) [24]. Along with the congenital antibody-associated AV block, a variety of congenital forms of AV block occur secondary to other congenital cardiac defects [25].
Management of patients with CCAVB has changed during the last decennia. In the past, a minority of patients received a pacemaker whereas the current policy is to pace the majority of patients based on a variety of criteria, among which is limited exercise capacity [10].
Exercise capacity provides relevant information about the health status and the ability to perform age-appropriate activities. Furthermore, it is a known predictor of mortality in both healthy and diseased individuals, including patients with congenital heart disease [8, 9, 14, 15].
Data regarding exercise capacity in CCAVB stems from decades-old publications reporting small case series of unpaced patients [31, 32]. Although the current policy is to pace patients, it is unknown whether exercise capacity benefits from this approach.
Therefore, the aim of this cross-sectional study was to investigate the cardiopulmonary exercise capacity of a group of contemporary children with CCAVB with and without pacemaker.
Methods
Study Population
The databases of the two participating departments of pediatric cardiology (Utrecht and Nijmegen) were screened to identify all patients >5 years old with isolated CCAVB, which was classified as congenital if (1) CAVB was diagnosed in utero, at birth, or within the neonatal period (0 to 27 days after birth) as proposed by Brucato et al. [6] or (2) CAVB was diagnosed in early childhood without signs and findings of a specific etiology (as described by Yater et al. [46]). The diagnosis “isolated CCAVB” required the absence of major structural heart defects. Eighteen patients were identified, and 16 of them consented to participate in the study. The medical records of those participating patients were reviewed. Data collected included patient age at diagnosis, maternal antibody status, patient age at first pacemaker implantation, all pacemaker-related interventions, and patient status at follow-up.
Fitness Questionnaire
To obtain information on self-perceived fitness and health, physical activity in daily life, including sports, participation at school, and leisure, a questionnaire [4, 11] from the Department of Integrative Physiology, St. Radboud University Nijmegen Medical Centre, Nijmegen, The Netherlands, was used. The results were compared with those from healthy control subjects [11].
Anthropometry
Before the cardiopulmonary exercise test (CPET), anthropometric measurements were completed in all patients, including body mass (BM [kg]) and body height (m) using an electronic scale (Seca, Hamburg, Germany) and a stadiometer (Ulmer Stadiometer, Ulm, Germany), respectively. Body mass index (BMI [kg m−2]) was calculated as BM in kg divided by the square of the body height in meters. SD scores were calculated for BM for age, body height for age and BMI for age using reference values from the 1997 Dutch Growth Study [12, 13]. To estimate body surface area (BSA [m2]), the equation of Haycock et al. was used [19], which has been validated in infants, children, and adults.
Echocardiography
Before CPET all patients underwent transthoracic echocardiography, which was performed by the same pediatric cardiologist (A. C. B.) with the patient at rest in supine position using a Vivid 7 machine (GE Vingmed Ultrasound AS, Horten, Norway). Images were obtained using a 3.5- or 5.0-MHz transducer in the suprasternal, parasternal, and apical views. Cine-loops, including three cardiac cycles, were stored digitally and analyzed off-line using EchoPac version 7.0.0 software (GE Healthcare, Horten, Norway). After a brief assessment of the cardiac anatomy, the following measurements were performed: M-mode; pulsed-wave (PW) Doppler of the aortic, pulmonic, mitral, and tricuspid valves and descending aorta; PW tissue Doppler imaging (TDI) of the interventricular septum and left free wall; and color-coded TDI of the left ventricle.
Assessment of Left-Ventricular Size and Function
Parasternal M-mode images were used to measure left-ventricular (LV) end-diastolic (LVEDD) and end-systolic diameters (LVESD). The LVEDD was compared with the normal values of body weight-matched children [26] and expressed as percentage of normal. LV dilatation was defined as LVEDD ≥120% of normal.
Color-coded TDI of the left ventricle in the apical four-chamber view was used to measure the peak systolic and diastolic tissue velocity of the septal and lateral mitral valve (MV) annulus. The velocities were compared with values obtained in a group of healthy young individuals [17]. Abnormal LV function was defined as measured systolic and/ or diastolic velocities <1 SD of the mean velocities of healthy young individuals [17].
Assessment of Dyssynchrony
Two types of dyssynchrony were assessed: interventricular dyssynchrony and intraventricular dyssynchrony of the left ventricle. Interventricular dyssynchrony was examined by calculating the interventricular mechanical delay (IVMD) using PW Doppler measurements in the left-ventricular (LVOT) and right-ventricular outflow tracts (RVOT) according to the following formula: (time from the onset of QRS to the onset of PW curve in the LVOT)—(time from the onset of QRS to the onset of PW curve in the RVOT). Interventricular dyssynchrony was defined as being present if IVMD >40 ms. Intraventricular dyssynchrony of the left ventricle was assessed by analyzing color-coded TDI of the left ventricle in the apical four-chamber view according to the recommendations of the American Society of Echocardiography Dyssynchrony Writing Group [18]. Intraventricular dyssynchrony was defined as being present if the septal-to-lateral wall delay of the left ventricle was >65 ms.
CPET
Subjects performed a CPET using an electronically braked cycle ergometer (Ergoline 9000; Ergoline GmbH, Bitz, Germany) as recently described [5]. In short, patients performed a CPET according to the Godfrey protocol [16]. The end of the CPET was marked by symptom limitation. A 12-lead electrocardiogram (ECG) and pulse oximetry (Nellcor 200E; Nellcor, Breda, The Netherlands) were recorded continuously throughout the entire test. Blood pressure was measured every 2 min (SunTech Tango+; SunTech Medical, Morrisville, NC, USA) [36]. The CPET featured a breath-by-breath gas-exchange analysis using a calibrated expiratory gas analysis system (Oxycon Pro; Cardinal, Houten, The Netherlands). Peak values were defined as the highest mean value of any 30 s time interval during exercise. Predicted values were obtained from established values from age- and sex-matched Dutch controls [38].
Ventilatory Threshold (VT)
The VT was determined using the criteria of an increase in both the ventilatory equivalent of oxygen (VE/VO2) and end-tidal pressure of oxygen (PETO2) with no increase in the ventilatory equivalent of carbon dioxide (VE/VCO2) [7, 44]. PETO2 and PETCO2 were taken into account to differentiate lactate buffering from hyperventilation. This method has been validated in pediatric patients [30]. VT was expressed as a percentage of predicted VO2peak [35]. Predicted values were obtained from established values from age- and sex-matched Dutch controls [38].
VE/VCO2-Slope and Oxygen Uptake Efficiency Slope (OUES)
The VE/VCO2-slope was calculated by linear least-squares regression of the relation between VE and VCO2, respectively, during the entire CPET [38]. The OUES was calculated by a linear least-squares regression of the VO2 on the common logarithm of the VE, by using the following equation: VO2 = a logVE + b [1]. In this equation, the constant “a” stands for the regression coefficient (called the OUES), and “b” represents the intercept. Predicted VE/VCO2-slope and OUES values were obtained from established values of age- and sex- matched Dutch controls [38].
Analysis of CPET ECG
During CPET, an electrocardiogram (ECG) was recorded at a speed of 25 mm/s, a gain of 10 mm/mV, and muscle filter +50 Hz. Each minute, a 12-lead trace of several consecutive heartbeats was printed on paper. The traces were analyzed by the same pediatric cardiologist (A. C. B.), who measured the following parameters: rhythm, QRS morphology, QRS duration, and corrected QT interval (QTc) (in normal QRS duration) or corrected JT interval (JTc) (if QRS duration >+2SD). In addition, the presence of arrhythmic events, including pacemaker upper rate behavior (2:1 block or pseudo-Wenckebach), was assessed during exercise.
Statistical Analysis
Continuous variables are presented as mean ± SD with minimum and maximum. Nominal data are summarized as frequencies and percentages. Differences between patients and reference values were tested using one-sample Student t test. Differences between the paced and unpaced group were analyzed using independent-samples Student t test, and p < 0.05 was considered statistically significant. Statistical analysis was performed with IBM SPSS Statistics 18 for Mac (IBM SPSS, Chicago, IL, USA).
Results
Patient Characteristics
The characteristics of the 16 studied patients are listed in Table 1. Patients were diagnosed with CCAVB at a mean age of 0.2 ± 0.6 years. Maternal antibodies were detected at diagnosis in 12 patients (75%). Thirteen patients (81%) had a pacemaker implanted with a median number of three implanted pacemakers. Their first pacemaker was implanted at a mean age of 2.2 ± 4.1 years. Five patients (31%) had minor associated congenital heart defects, such as patent arterial duct (PDA = 2 patients [13%]), PDA and atrial septal defect (PDA + ASD = 1 patient [6%]), ventricular septal defect (VSD = 1 patient [6%]), or ASD and VSD (one patient [6%]). Two patients (13%) were on cardiac medication: one patient used an angiotensin-converting enzyme (ACE) inhibitor, and one patient used a combination of an ACE-inhibitor and a beta-blocker.
Self-Rated Fitness, Health, and Physical Activity
The results of the questionnaire, as listed in Table 2, identified no significant difference in the self-rated fitness and health of paced and unpaced patients. The majority of CCAVB patients were always able to perform physical activities without or with minor difficulties. Most of the CCAVB patients judged their physical condition to be equal to the average of their peers.
Analysis of LV Size, Function, and Dyssynchrony
The echocardiographic results are listed in Table 3. LVEDD of the studied patients was 110 ± 10% of normal. Three patients (19% [two paced and one unpaced]) had LV dilatation. Two patients (13% [both paced]) showed systolic and diastolic LV dysfunction. MV E velocity (0.99 ± 0.15 vs. 1.39 ± 0.08 m/s, p = 0.001), aortic valve (AoV) velocity (1.17 ± 0.13 vs. 1.60 ± 0.03 m/s, p < 0.0005), and color-coded TDI lateral MV E’ velocity (−7.8 ± 1.2 vs. −10.7 ± 0.7 cm/s, p = 0.002) were significantly higher in unpaced patients. Eight patients (50% [all paced]) showed interventricular dyssynchrony and one patient (6% [paced]) showed intraventricular dyssynchrony.
CPET ECG
Table 3 lists the ECG results. QRS duration during the rest phase of CPET (145 ± 13 vs. 97 ± 6 ms, p < 0.0005) was significantly shorter in unpaced patients. Eleven of the (RV) paced patients showed an LBBB-like QRS morphology. Two of the (cardiac resynchronization therapy [CRT]) paced patients had an indifferent QRS morphology. The JTc in paced patients was 311 ± 24 ms (normal value < 350 ms). The QTc in unpaced patients was 420 ± 18 ms (normal value < 440 ms). Despite of an average programmed pacemaker upper rate of 182 ± 11 bpm, four patients (25% [three DDDR (dual [atrial/ventricular] paced, dual [atrial/ventricular] sensed, dual [inhibited/triggered], rate responsive) paced and one CRT paced]) showed upper rate behavior of their pacemaker (one pseudo-Wenckebach and three 2:1 block). No patient displayed premature ventricular beats.
CPET
Table 4 lists the CPET data. Peak HR (135 ± 37 bpm), VO2peak (1.31 ± 0.50 l min−1 [79 ± 24% of predicted]), VO2peak kg−1 (34.4 ± 9.5 ml kg−1 min−1 [79 ± 24% of predicted]), peak minute ventilation (50.2 ± 22.9 l min−1 [76 ± 26% of predicted]), and VT (52 ± 17% of VO2peak [78 ± 21% of predicted]) were all significantly lower than those of healthy peers.
Peak work load corrected for body mass (2.8 ± 0.6 W kg−1 [91 ± 24% of predicted]), peak oxygen pulse (10.4 ± 5.1 ml beat−1 [111 ± 56% of predicted]), peak systolic blood pressure (131 ± 24 mmHg [99 ± 12% of predicted]), VE/VCO2-slope (33.3 ± 6.6 [108 ± 17% of predicted]), OUES (1424 ± 510 [92 ± 39% of predicted]), percentage of predicted FEV1 (92 ± 11%), percentage of predicted forced expiratory vital capacity (FVC) (87 ± 15%), and peak SpO2% (96 ± 2%) differed nonsignificantly from healthy peers.
Paced CCAVB patients showed a significantly higher HR at rest (77 ± 10 vs. 53 ± 2 bpm), lower VE/VCO2-slope (31.8 ± 6.3 vs. 40.0 ± 1.8) and higher OUES (1513 ± 528 vs. 1034 ± 57) compared with unpaced patients. There were no significant differences in all other CPET variables between paced and unpaced patients. There were no significant differences in VO2peak kg−1 between paced and unpaced patients (Fig. 1) and between the various pacemaker types (Fig. 2). Peak HR of the paced patients differed between the various pacemaker types. DDD (dual [atrial/ventricular] paced, dual [atrial ventricular] sensed, dual [inhibited/triggered])-paced patients had the highest peak HR (171 ± 8 bpm), followed by CRT (161 ± 8 bpm), VVIR (ventricular paced, ventricular sensed, inhibited, rate responsive) (114 ± 25 bpm), and DDDR-paced (98 ± 6 bpm) patients.
Percentage of predicted peak oxygen uptake/body mass (VO2peak kg−1) of unpaced and paced CCAVB patients. Box-and-whisker diagram: horizontal line in the box depicts median value; the box includes 50% of the values; the upper whisker represents the top 25% of the values; and the lower whisker represents the bottom 25% of the values
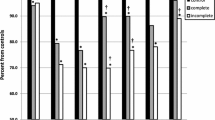
Percentage of predicted peak oxygen uptake/body mass (VO2peak kg−1) of unpaced and paced CCAVB patients. The paced patients are subdivided according to their pacemaker type. Box-and-whisker diagram: horizontal line in the box depicts median value; the box includes 50% of the values; the upper whisker represents the top 25% of the values; and the lower whisker represents the bottom 25% of the values
Discussion
The aim of this cross-sectional study was to investigate the cardiopulmonary exercise capacity of contemporary children with CCAVB with and without pacemaker. Our study showed that VO2peak kg−1 is significantly decreased in children with CCAVB. The VO2peak kg−1 values (34.4 ± 9.5 ml kg−1 min−1) are comparable with those observed approximately 30 years ago in unpaced children with CCAVB [29, 40, 43]. These studies reported an average VO2peak kg−1 of 36 ± 2, 37, and 31 ml kg−1 min−1, respectively.
Furthermore, the VO2 at VT was significantly decreased compared with healthy peers. The observed VO2 at VT (22.9 ± 6.2 ml kg−1 min−1) was comparable with the VT observed in unpaced children with CCAVB as reported >20 years ago by Reybrouck et al. (22.8 ± 5.5 ml kg−1 min−1) [32].
It is of interest to note that the peak workload corrected for body mass was not significantly decreased in children with CCAVB. This implies that children with CCAVB are generating more energy from anaerobic sources during exercise, compared with healthy peers, as a compensatory mechanism for their decreased cardiac output. Furthermore, this explains why children with CCAVB do not frequently report exercise intolerance [2]. Based on these figures, the question arises whether pacemaker therapy globally improves exercise capacity in children with CCAVB. Unexpectedly, our current results suggest that the VO2peak and VT values of our paced patients do not differ from those obtained in unpaced patients from 20 to 30 years ago. Moreover, VO2peak values between the paced and unpaced patients of our study population were not significantly different.
Our hypothesis is that by employing the current indications for pacing in CCAVB, as reviewed by Villain [41], only the “best” patients in terms of exercise capacity stay unpaced. Apparently, the exercise capacity of these “best” unpaced patients can compete with the paced patients. Thus, perhaps there are factors that prevent normalization of exercise capacity after insertion of a pacemaker.
VO2peak is regarded as the single best parameter to describe exercise capacity [34]. According to the Fick equation, VO2peak is the product of three parameters: peak heart rate (HRpeak), peak stroke volume (SVpeak), and peak arterial-venous oxygen difference (CaO2 − CvO2); (VO2peak = HRpeak × SVpeak × (CaO2 − CvO2)). Dynamic changes in one of these parameters related to exercise, therefore, might influence the oxygen transport during exercise.
Peak Heart Rate
Unpaced children with CCAVB mostly have an AV junctional escape rhythm with a lower frequency than healthy individuals at rest (average 46 [32] to 59 [37] bpm [in this study 53 bpm]). In these patients, this frequency approximately doubles (range 1.6 [37] to 2.3 [40]) during (peak) exercise to an average frequency of 94 [37] to 117 [in this study]). A pacemaker will restore the frequencies at rest as well as during exercise. The extent of frequency restoration depends on the pacemaker mode (e.g., single chamber [VVI] vs. dual chamber (DDD), use of rate response) and the pacemaker programming. Our study showed that the average peak HR of paced CCAVB patients is still lower than in healthy individuals. There are two reasons for that finding. First, approximately half of the paced patients had a rate-responsive pacemaker (i.e., VVIR or DDDR). They showed a lower average peak HR compared with DDD- or CRT-paced patients. This means that the sensor sensitivity was not appropriate for the type of exercise (cycling). All rate-responsive pacemakers in our study used an accelerometer as activity sensor. Theoretically, an accelerometer should be sensitive to bicycling because it detects horizontal movement [42]. However, it is designed for use in adult patients with the pacemaker implanted in the pectoral region [3]. The majority of patients with a rate-responsive pacemaker in our study had their device implanted in the abdominal region, which blunted the response of their accelerometer during bicycling. Our results underscore the necessity to use the treadmill instead of the bicycle for the exercise testing of pediatric patients with a rate-responsive pacemaker.
Second, despite an average programmed pacemaker upper rate (maximum tracking rate [MTR]) 182 ± 11 bpm minute, 25% of the paced patients showed upper rate behavior of the pacemaker during the CPET, which limited their exercise capacity significantly. These results show that pediatric CCAVB patients would benefit from MTRs > 180 bpm. Unfortunately, not all pacemaker models and manufacturers support MTRs in that range. Finally, another factor that might influence peak HR is the occurrence of premature ventricular beats (PVBs). Earlier studies showed a high incidence (27% [22] to 70% [45]) of PVBs in unpaced CCAVB patients. However, no patient in our study displayed PVBs.
Peak Stroke Volume
The stroke volume is influenced by cardiac preload, myocardial contractility, and cardiac afterload. There is a difference in these parameters between unpaced and paced CCAVB patients. In unpaced patients, according to Scarpelli and Rudolph [33], the long diastolic filling in bradycardia causes an increased end-diastolic volume with stretching of the myocardial fibres, augmenting myocardial contractility. Indeed, Kertesz et al. [23] demonstrated that moderate LV dilatation is common in these patients and is associated with a normal LV geometry, normal wall stress, and enhanced systolic function during the first two decades of life. The data of this study support the findings of Scarpelli and Rudolph and Kertesz et al. The LV end diastolic diameter was greater (although not significantly) in unpaced patients, and one patient had LV dilatation. The MV Doppler inflow velocity was significantly greater in unpaced patients, suggesting an unfavorable relaxation of the stretched left ventricle. All unpaced CCAVB patients had normal LV function.
Paced CCAVB patients had a lower LVEDD and MV Doppler inflow velocity, suggesting less stretching and better relaxation of the left ventricle. However, two of 13 paced patients (15%) showed LV dysfunction (with LV dilatation in one patient). This might be a result of chronic pacing. Earlier studies have shown that chronic (right) ventricular pacing causes an abnormal electrical activation that may lead to mechanical dyssynchrony (seen in 62% of the paced patients in this study), LV remodeling, LV dilatation, LV dysfunction, and low exercise capacity [28, 39].
The majority of our patients (87%) had normal LV function at rest. Yet, stroke volume can increase as well as decrease during exercise in the presence of normal LV function at rest [20, 21, 37]. Therefore, future studies should include exercise echocardiography with (noninvasive) measurement of stroke volume.
Arterial–Venous Oxygen Difference
Although our study does not include (invasive) measurement of the oxygen content of the arterial and venous blood, earlier studies showed a normal (13.8 [43] to 14.5 [29] ml/100 ml) or increased [21] average arterial–venous oxygen difference during (peak) exercise in patients with CCAVB. It is therefore unclear whether children with CCAVB have an increased arterial–venous oxygen difference during exercise as a compensatory mechanism for their decreased cardiac output.
Study Limitations
A limitation of this study was that our data were obtained cross-sectionally from a rather small group of patients in two University Children’s Hospitals. In contrast, all patients were tested by the same experienced staff using the same equipment to avoid interobserver or technical variability. Future additional studies should be performed in a larger patient population and should preferably include more unpaced CCAVB patients (although lack of availability is a limitation in itself). In addition, longitudinal exercise data are desirable for investigating the effects of pacemaker therapy on exercise capacity in this population.
In conclusion, children with CCAVB show a decreased peak oxygen uptake and VT, whereas they show normal peak work rates. This indicates that they generate more energy from anaerobic energy sources during exercise. Paced children with CCAVB do not perform better than unpaced children. Possible explanations for that finding might be: (1) a selection bias imposed by the current pacemaker criteria (only the clinically “best” CCAVB patients stay unpaced), (2) chronic RV pacing–induced LV dysfunction in some CCAVB patients, and (3) suboptimal pacemaker programming.
Future exercise studies, including a greater number of patients and longitudinal follow-up, are warranted to investigate the influence of myocardial properties (LV dysfunction), pacing mode, and optimal pacemaker programming on exercise capacity.
References
Baba R, Nagashima M, Goto M, Nagano Y, Yokota M, Tauchi N et al (1996) Oxygen uptake efficiency slope: a new index of cardiorespiratory functional reserve derived from the relation between oxygen uptake and minute ventilation during incremental exercise. J Am Coll Cardiol 28(6):1567–1572
Beaufort-Krol GCM, Schasfoort-van Leeuwen MJM, Stienstra Y, Bink-Boelkens MTE (2007) Longitudinal echocardiographic follow-up in children with congenital complete atrioventricular block. Pacing Clin Electrophysiol 30(11):1339–1343
Berul CI, Barrett KS (2001) Unique aspects of pacemaker implantation in pediatric patients. In: Walsh EP, Saul JP, Triedman JK (eds) Cardiac arrhythmias in children and young adults with congenital heart disease. Lippincott Williams & Wilkins, Philadelphia, pp 301–317
Binkhorst M, van de Belt T, de Hoog M, van Dijk A, Schokking M, Hopman M (2008) Exercise capacity and participation of children with a ventricular septal defect. Am J Cardiol 102(8):1079–1084
Bongers B, Hulzebos H, Blank A, Van Brussel M, Takken T (2011) The oxygen uptake efficiency slope in children with congenital heart disease: construct and group validity. Eur J Cardiovasc Prev Rehabil 18(3):384–92
Brucato A, Jonzon A, Friedman D, Allan LD, Vignati G, Gasparini M et al (2003) Proposal for a new definition of congenital complete atrioventricular block. Lupus 12(6):427–435
Caiozzo VJ, Davis JA, Ellis JF, Azus JL, Vandagriff R, Prietto CA et al (1982) A comparison of gas exchange indices used to detect the anaerobic threshold. J Appl Physiol 53(5):1184–1189
Diller G-P, Dimopoulos K, Okonko D, Li W, Babu-Narayan SV, Broberg CS et al (2005) Exercise intolerance in adult congenital heart disease: comparative severity, correlates, and prognostic implication. Circulation 112(6):828–835
Diller G-P, Giardini A, Dimopoulos K, Gargiulo G, Müller J, Derrick G et al. (2010) Predictors of morbidity and mortality in contemporary Fontan patients: results from a multicenter study including cardiopulmonary exercise testing in 321 patients. Eur Heart J 31(24):3073–83
Dolara A, Favilli S (2010) Controversies in the therapy of isolated congenital complete heart block. J Cardiovasc Med (Hagerstown) 11(6):426–430
Ev Beek, Binkhorst M, Hoog Md, Groot PD, Dijk Av, Schokking M et al (2010) Exercise performance and activity level in children with transposition of the great arteries treated by the arterial switch operation. Am J Cardiol 105(3):398–403
Fredriks AM, van Buuren S, Burgmeijer RJ, Meulmeester JF, Beuker RJ, Brugman E, Roede MJ, Verloove-Vanhorick SP, Wit JM (2000) Continuing positive secular growth change in The Netherlands 1955–1997. Pediatr Res 47:316–332
Fredriks AM, van Buuren S, van Heel WJM, Dijkman-Neerincx RHM, Verloove-Vanhorick SP, Wit JM (2005) Nationwide age references for sitting height, leg length, and sitting height/height ratio, and their diagnostic value for disproportionate growth disorders. Arch Dis Child 90(8):807–812
Giardini A, Specchia S, Tacy TA, Coutsoumbas G, Gargiulo G, Donti A et al (2007) Usefulness of cardiopulmonary exercise to predict long-term prognosis in adults with repaired tetralogy of Fallot. Am J Cardiol 99(10):1462–1467
Giardini A, Hager A, Lammers AE, Derrick G, Müller J, Diller G-P et al (2009) Ventilatory efficiency and aerobic capacity predict event-free survival in adults with atrial repair for complete transposition of the great arteries. J Am Coll Cardiol 53(17):1548–1555
Godfrey S (1974) Exercise testing in children. Saunders, Philadelphia
Goebel B, Arnold R, Koletzki E, Ulmer HE, Eichhorn J, Borggrefe M et al (2007) Exercise tissue Doppler echocardiography with strain rate imaging in healthy young individuals: feasibility, normal values and reproducibility. Int J Cardiovasc Imaging 23(2):149–155
Gorcsan J, Abraham T, Agler DA, Bax JJ, Derumeaux G, Grimm RA et al (2008) Echocardiography for cardiac resynchronization therapy: recommendations for performance and reporting—a report from the American Society of Echocardiography Dyssynchrony writing group endorsed by the heart rhythm society. J Am Soc Echocardiogr 21(3):191–213
Haycock GB, Schwartz GJ, Wisotsky DH (1978) Geometric method for measuring body surface area: a height-weight formula validated in infants, children, and adults. J Pediatr 93(1):62–66
Holmgren A, Karlberg P, Pernow B (1959) Circulatory adaptation at rest and during muscular work in patients with complete heart block. Acta Med Scand 164(2):119–130
Ikkos D, Hanson JS (1960) Response to exercise in congenital complete atrioventricular block. Circulation 22:583–590
Karpawich PP, Gillette PC, Garson A, Hesslein PS, Porter CB, McNamara DG (1981) Congenital complete atrioventricular block: clinical and electrophysiological predictors of need for pacemaker insertion. Am J Cardiol 48(6):1098–1102
Kertesz NJ, Friedman RA, Colan SD, Walsh EP, Gajarski RJ, Gray PS et al (1997) Left ventricular mechanics and geometry in patients with congenital complete atrioventricular block. Circulation 96(10):3430–3435
Lazzerini PE, Capecchi PL, Guideri F, Acampa M, Selvi E, Bisogno S et al (2008) Autoantibody-mediated cardiac arrhythmias: mechanisms and clinical implications. Basic Res Cardiol 103(1):1–11
Lev M (1964) Anatomic basis for atrioventricular block. Am J Med 37:742–748
Marek J (2006) Echokardiografie. Dětská kardiologie, Czech Republic
Michaelsson M (1995) Congential complete atrioventricular block. Prog Ped Card 4(1):1–10
Moak JP, Hasbani K, Ramwell C, Freedenberg V, Berger JT, DiRusso G et al (2006) Dilated cardiomyopathy following right ventricular pacing for AV block in young patients: resolution after upgrading to biventricular pacing systems. J Cardiovasc Electrophysiol 17(10):1068–1071
Mocellin R, Bastanier C (1977) Functional studies in children and adolescents with congenital complete heart block (author’s translation). Z Kardiol 66(6):298–302
Ohuchi H, Nakajima T, Kawade M, Matsuda M, Kamiya T (1996) Measurement and validity of the ventilatory threshold in patients with congenital heart disease. Pediatr Cardiol 17(1):7–14
Paul MH, Rudolph AM, Nadas AS (1958) Congenital complete atrioventricular block: problems of clinical assessment. Circulation 18(2):183–190
Reybrouck T, Vanden Eynde B, Dumoulin M, Van der Hauwaert LG (1989) Cardiorespiratory response to exercise in congenital complete atrioventricular block. Am J Cardiol 64(14):896–899
Scarpelli EM, Rudolph AM (1964) The hemodynamics of congenital heart block. Progr Cardiovasc Dis 6:327–342
Shephard RJ, Allen C, Benade AJ, Davies CT, Di Prampero PE, Hedman R et al. (1968) The maximum oxygen intake. An international reference standard of cardiorespiratory fitness. Bull World Health Org 38(5):757–764
Takken T, van der Net J, Engelbert RHH, Pater S, Helders PJM (2008) Responsiveness of exercise parameters in children with inflammatory myositis. Arthritis Rheum 59(1):59–64
Takken T, Blank AC, Hulzebos EH, van Brussel M, Groen WG, Helders PJ (2009) Cardiopulmonary exercise testing in congenital heart disease: equipment and test protocols. Neth Heart J 17(9):339–344
Taylor MR, Godfrey S (1972) Exercise studies in congenital heart block. Br Heart J 34(9):930–935
Ten Harkel ADJ, Takken T, Van Osch-Gevers M, Helbing WA (2010) Normal values for cardiopulmonary exercise testing in children. Eur J Cardiovasc Prev Rehabil 18(1):48–54s
Thambo J-B, Bordachar P, Garrigue S, Lafitte S, Sanders P, Reuter S et al (2004) Detrimental ventricular remodeling in patients with congenital complete heart block and chronic right ventricular apical pacing. Circulation 110(25):3766–3772
Thorén C, Herin P, Vávra J (1974) Studies of submaximal and maximal exercise in congenital complete heart block. Acta Paediatr Belg 28(Suppl):132–143
Villain E (2008) Indications for pacing in patients with congenital heart disease. Pacing Clin Electrophysiol 31(Suppl 1):S17–S20
Wang JW, Al-Ahmad A, Hsia HH, Zei PC (2008) Modes of pacemaker function. In: Kusumoto FM, Goldschlager NF (eds) Cardiac pacing for the clinician, 2nd ed. Springer, New York, pp 647–694
Watson G, Freed D, Strieder J (1977) Cardiac output during exercise in children with idiopathic complete heart block. Front Act Child Health 297(14):743–47
Whipp BJ, Davis JA, Torres F, Wasserman K (1981) A test to determine parameters of aerobic function during exercise. J Appl Physiol 50(1):217–221
Winkler RB, Freed MD, Nadas AS (1980) Exercise-induced ventricular ectopy in children and young adults with complete heart block. Am Heart J 99(1):87–92
Yater W, Lyon J, McNabb P (1933) Congenital heart block—review and report of the second case of complete heart block studied by serial sections through the conduction system. JAMA 100:183–1837
Acknowledgement
The authors thank A. P. van Dijk and H. B. C. Cornet for their assistance during this study, B. Bongers for calculating the CPET slopes, and M. L. Zonderland and D. A. de Wolf for careful reading and discussion of the manuscript. This study was supported by the Netherlands Heart Foundation (NHS-JUMP [Grant Number 2008T039]).
Open Access
This article is distributed under the terms of the Creative Commons Attribution License which permits any use, distribution, and reproduction in any medium, provided the original author(s) and the source are credited.
Author information
Authors and Affiliations
Corresponding author
Rights and permissions
Open Access This article is distributed under the terms of the Creative Commons Attribution 2.0 International License (https://creativecommons.org/licenses/by/2.0), which permits unrestricted use, distribution, and reproduction in any medium, provided the original work is properly cited.
About this article
Cite this article
Blank, A.C., Hakim, S., Strengers, J.L. et al. Exercise Capacity in Children With Isolated Congenital Complete Atrioventricular Block: Does Pacing Make a Difference?. Pediatr Cardiol 33, 576–585 (2012). https://doi.org/10.1007/s00246-012-0176-0
Received:
Accepted:
Published:
Issue Date:
DOI: https://doi.org/10.1007/s00246-012-0176-0