Abstract
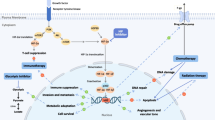
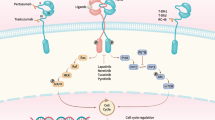
Human epidermal growth factor receptor 2-positive (HER2+) breast cancer is correlated with poor prognosis, the current treatment of which is still based on surgery and adjuvant targeted therapy with monoclonal antibody. Problems of drug resistance hinder the use of monoclonal antibodies. Subsequently, tyrosine kinase inhibitors (TKIs) have been noticed, TKIs have the advantages of multi-targets and reduced drug resistance. However, TKIs that target HER family proteins often cause adverse effects such as liver damage and diarrhea. Thus, TKIs with high selectivity are being developed. TH-4000, a prodrug that generated an active form TH-4000Effector (TH-4000E) under hypoxic condition, was evaluated in this research. We found that TH-4000E ([(E)-4-[[4-(3-bromo-4-chloroanilino)pyrido[3,4-d]pyrimidin-6-yl]amino]-4-oxobut-2-enyl]-dimethyl-[(3-methyl-5-nitroimidazol-4-yl)methyl]azanium) (1–1000 nM) had potent and highly selective toxic effects on HER2+ breast cancer cells and inhibited the phosphorylation of HER family kinases at lower doses than that of Lapatinib and Tucatinib. TH-4000E activated Caspase-3 and induced apoptosis through a reactive oxygen species (ROS)-dependent pathway. The prodrug TH-4000 ([(E)-4-[[4-(3-bromo-4-chloroanilino)pyrido[3,4-d]pyrimidin-6-yl]amino]-4-oxobut-2-enyl]-dimethyl-[(3-methyl-5-nitroimidazol-4-yl)methyl]azanium;bromide) (50 mg/kg) effectively suppressed the tumor growth with less liver damage in mouse tumor models. This hypoxia-targeted strategy has possessed advantage in avoiding drug-induced liver damage, TH-4000 could be a promising drug candidate for the treatment of HER2+ breast cancer.









Similar content being viewed by others
Data availability
The data is available upon request from the the lead contact, Dawei Yang (David_young1994@outlook.com).
Abbreviations
- EGFR:
-
Human epidermal growth factor receptor
- HER2:
-
Human epidermal growth factor receptor 2
- HER3:
-
Human epidermal growth factor receptor 3
- HER4:
-
Human epidermal growth factor receptor 4
- ERK:
-
Extracellular regulated protein kinase
- AKT:
-
Protein kinase b
- OS:
-
Overall survival
- PFS:
-
Progression-free survival
- ATP:
-
Adenosine triphosphate
- FDA:
-
Food and drug administration
- TKI:
-
Tyrosine kinase inhibitor
- TH-4000E:
-
TH-4000Effector
- DMSO:
-
Dimethyl sulfoxide
- CCK-8:
-
Cell counting kit-8
- IC50:
-
Half inhibitory concentration
- FBS:
-
Fetal bovine serum
- PBS:
-
Phosphate buffered saline
- DMEM:
-
Dulbecco’s modified eagle’s medium
- ROS:
-
Reactive oxygen species
- NAC:
-
N-Acetyl-l-cysteine
- Z-VAD:
-
Z-VAD(OMe)-FMK
- PARP:
-
Poly adp-ribose polymerase
- MMP:
-
Mitochondrial membrane potential
- CD36:
-
Platelet glycoprotein 4
- CPT1A:
-
Carnitine palmitoyltransferase 1A
- CPT1B:
-
Carnitine palmitoyltransferase 1B
- FAO:
-
Fatty acid oxidation
- mRNA:
-
Messenger RNA
- RT-PCR:
-
Reverse transcription-polymerase chain reaction
- qPCR:
-
Real-time quantitative PCR
- PI:
-
Propidium iodide
- IHC:
-
Immunohistochemistry
- HE:
-
Hematoxylin–eosin
- ALT:
-
Alanine aminotransferase
- AST:
-
Aspartate aminotransferase
- CREA:
-
Creatinine
- MRM:
-
Multiple reaction monitoring
- NSCLC:
-
Non-small cell lung cancer
- DLT:
-
Dose limiting toxicity
- MTD:
-
Maximum tolerated dose
References
Anido J, Scaltriti M, Bech Serra JJ et al (2006) Biosynthesis of tumorigenic HER2 C-terminal fragments by alternative initiation of translation. EMBO J 25(13):3234–3244. https://doi.org/10.1038/sj.emboj.7601191
Blair HA (2018) Pyrotinib: first global approval. Drugs 78(16):1751–1755. https://doi.org/10.1007/s40265-018-0997-0
Cesca MG, Vian L, Cristóvão-Ferreira S, Pondé N, de Azambuja E (2020) HER2-positive advanced breast cancer treatment in 2020. Cancer Treat Rev 88:102033. https://doi.org/10.1016/j.ctrv.2020.102033
Cocco E, Javier Carmona F, Razavi P et al (2018) Neratinib is effective in breast tumors bearing both amplification and mutation of ERBB2 (HER2). Sci Signal 11(551):eaat9773. https://doi.org/10.1126/scisignal.aat9773
Cronin KA, Harlan LC, Dodd KW, Abrams JS, Ballard-Barbash R (2010) Population-based estimate of the prevalence of HER-2 positive breast cancer tumors for early stage patients in the US. Cancer Investig 28(9):963–968. https://doi.org/10.3109/07357907.2010.496759
Cura Y, Pérez Ramírez C, Sánchez Martín A et al (2021) Genetic polymorphisms on the effectiveness or safety of breast cancer treatment: clinical relevance and future perspectives. Mutat Res Rev Mutat Res 788:108391. https://doi.org/10.1016/j.mrrev.2021.108391
Estrada-Bernal A, Le AT, Doak AE et al (2021) Tarloxotinib is a hypoxia-activated pan-HER kinase inhibitor active against a broad range of HER-family oncogenes. Clin Cancer Res 27(5):1463–1475. https://doi.org/10.1158/1078-0432.Ccr-20-3555
Fox DB, Garcia NMG, McKinney BJ et al (2020) NRF2 activation promotes the recurrence of dormant tumour cells through regulation of redox and nucleotide metabolism. Nat Metab 2(4):318–334. https://doi.org/10.1038/s42255-020-0191-z
Geyer CE, Forster J, Lindquist D et al (2006) Lapatinib plus capecitabine for HER2-positive advanced breast cancer. N Engl J Med 355(26):2733–2743. https://doi.org/10.1056/NEJMoa064320
Hou Y, Nitta H, Wei L et al (2017) HER2 intratumoral heterogeneity is independently associated with incomplete response to anti-HER2 neoadjuvant chemotherapy in HER2-positive breast carcinoma. Breast Cancer Res Treat 166(2):447–457. https://doi.org/10.1007/s10549-017-4453-8
Kataoka Y, Mukohara T, Shimada H, Saijo N, Hirai M, Minami H (2010) Association between gain-of-function mutations in PIK3CA and resistance to HER2-targeted agents in HER2-amplified breast cancer cell lines. Ann Oncol 21(2):255–262. https://doi.org/10.1093/annonc/mdp304
Kreutzfeldt J, Rozeboom B, Dey N, De P (2020) The trastuzumab era: current and upcoming targeted HER2+ breast cancer therapies. Am J Cancer Res 10(4):1045–1067
Kulukian A, Lee P, Taylor J et al (2020) Preclinical activity of HER2-selective tyrosine kinase inhibitor tucatinib as a single agent or in combination with trastuzumab or docetaxel in solid tumor models. Mol Cancer Ther 19(4):976–987. https://doi.org/10.1158/1535-7163.Mct-19-0873
Lee A (2020) Tucatinib: first approval. Drugs 80(10):1033–1038. https://doi.org/10.1007/s40265-020-01340-w
Maddox AL, Brehove MS, Eliato KR et al (2022) Molecular assessment of HER2 to identify signatures associated with therapy response in HER2-positive breast cancer. Cancers (basel) 14(11):2795. https://doi.org/10.3390/cancers14112795
McLean LS, Morris TA, Gramza A et al (2022) A phase II study of tarloxotinib (a hypoxia activated prodrug of a pan-erb tyrosine kinase inhibitor) in patients with recurrent or metastatic squamous cell carcinoma of the head and neck or skin. Investig New Drugs 40(4):782–788. https://doi.org/10.1007/s10637-022-01230-w
Medina PJ, Goodin S (2008) Lapatinib: a dual inhibitor of human epidermal growth factor receptor tyrosine kinases. Clin Ther 30(8):1426–1447. https://doi.org/10.1016/j.clinthera.2008.08.008
Murthy R, Borges VF, Conlin A et al (2018) Tucatinib with capecitabine and trastuzumab in advanced HER2-positive metastatic breast cancer with and without brain metastases: a non-randomised, open-label, phase 1b study. Lancet Oncol 19(7):880–888. https://doi.org/10.1016/s1470-2045(18)30256-0
Murthy RK, Loi S, Okines A et al (2020) Tucatinib, trastuzumab, and capecitabine for HER2-positive metastatic breast cancer. N Engl J Med 382(7):597–609. https://doi.org/10.1056/NEJMoa1914609
Nahta R, Yuan LX, Du Y, Esteva FJ (2007) Lapatinib induces apoptosis in trastuzumab-resistant breast cancer cells: effects on insulin-like growth factor I signaling. Mol Cancer Ther 6(2):667–674. https://doi.org/10.1158/1535-7163.Mct-06-0423
Owens MA, Horten BC, Da Silva MM (2004) HER2 amplification ratios by fluorescence in situ hybridization and correlation with immunohistochemistry in a cohort of 6556 breast cancer tissues. Clin Breast Cancer 5(1):63–69. https://doi.org/10.3816/cbc.2004.n.011
Paranjpe R, Basatneh D, Tao G et al (2019) Neratinib in HER2-positive breast cancer patients. Ann Pharmacother 53(6):612–620. https://doi.org/10.1177/1060028018824088
Patterson AV, Silva S, Guise C et al (2015) Abstract 5358: the hypoxia-activated EGFR-TKI TH-4000 overcomes erlotinib-resistance in preclinical NSCLC models at plasma levels achieved in a Phase 1 clinical trial. Can Res 75(15 Suppl):5358–5358. https://doi.org/10.1158/1538-7445.Am2015-5358
Phillips RM (2016) Targeting the hypoxic fraction of tumours using hypoxia-activated prodrugs. Cancer Chemother Pharmacol 77(3):441–457. https://doi.org/10.1007/s00280-015-2920-7
Pohlmann PR, Mayer IA, Mernaugh R (2009) Resistance to trastuzumab in breast cancer. Clin Cancer Res 15(24):7479–7491. https://doi.org/10.1158/1078-0432.Ccr-09-0636
Rimawi MF, Schiff R, Osborne CK (2015) Targeting HER2 for the treatment of breast cancer. Annu Rev Med 66:111–128. https://doi.org/10.1146/annurev-med-042513-015127
Slamon DJ, Leyland-Jones B, Shak S et al (2001) Use of chemotherapy plus a monoclonal antibody against HER2 for metastatic breast cancer that overexpresses HER2. N Engl J Med 344(11):783–792. https://doi.org/10.1056/nejm200103153441101
Swain SM, Shastry M, Hamilton E (2023) Targeting HER2-positive breast cancer: advances and future directions. Nat Rev Drug Discov 22(2):101–126. https://doi.org/10.1038/s41573-022-00579-0
Tai W, Mahato R, Cheng K (2010) The role of HER2 in cancer therapy and targeted drug delivery. J Control Release 146(3):264–275. https://doi.org/10.1016/j.jconrel.2010.04.009
Zhang YX, Knyazev PG, Cheburkin YV et al (2008) AXL is a potential target for therapeutic intervention in breast cancer progression. Cancer Res 68(6):1905–1915. https://doi.org/10.1158/0008-5472.Can-07-2661
Acknowledgements
This research was supported by the Natural Science Foundation of Jiangsu province (No. BK20230157), the Medical Engineering Cooperation Project of Nanjing Municipal Science and Technology Bureau (No. 202110032), the Talent Support Program by the Second Hospital of Nanjing (No. RCMS23004), the High-level Talents Program from the Second Hospital of Nanjing (No. 202302), Nanjing Pukou Program for Society and Science Development (No. S2022-1), Nanjing Healthcare and Science Development Program (No. YKK22231), Guangdong Basic and Applied Basic Research Foundation (2019A1515110993) and the Postgraduate Research and Practice Innovation Program of Jiangsu Province (No. KYCX22_1927).
We thank the Center for Analysis and Testing of China Pharmaceutical University for the use of HPLC‐QQQ‐MS/MS, and would like to thank Zi-Yuan Wang (China Pharmaceutical University).
Author information
Authors and Affiliations
Corresponding authors
Ethics declarations
Conflict of interest
The authors declare no conflict of interest. Each author agrees to the contents of the manuscript.
Declaration of generative AI in scientific writing
Generative AI was not used in this manuscript.
Additional information
Publisher's Note
Springer Nature remains neutral with regard to jurisdictional claims in published maps and institutional affiliations.
Supplementary Information
Below is the link to the electronic supplementary material.
Rights and permissions
Springer Nature or its licensor (e.g. a society or other partner) holds exclusive rights to this article under a publishing agreement with the author(s) or other rightsholder(s); author self-archiving of the accepted manuscript version of this article is solely governed by the terms of such publishing agreement and applicable law.
About this article
Cite this article
Shao, X., Yang, D., Shan, L. et al. TH-4000, a hypoxia-activated pan-HER inhibitor, shows excellent preclinical efficacy for the treatment of HER2+ breast cancer. Arch Toxicol 98, 865–881 (2024). https://doi.org/10.1007/s00204-023-03670-6
Received:
Accepted:
Published:
Issue Date:
DOI: https://doi.org/10.1007/s00204-023-03670-6