Abstract
Pharmaceuticals and environmental contaminants contribute to hypercholesterolemia. Several chemicals known to cause hypercholesterolemia, activate pregnane X receptor (PXR). PXR is a nuclear receptor, classically identified as a sensor of chemical environment and regulator of detoxification processes. Later, PXR activation has been shown to disrupt metabolic functions such as lipid metabolism and recent findings have shown PXR activation to promote hypercholesterolemia through multiple mechanisms. Hypercholesterolemia is a major causative risk factor for atherosclerosis and greatly promotes global health burden. Metabolic disruption by PXR activating chemicals leading to hypercholesterolemia represents a novel toxicity pathway of concern and requires further attention. Therefore, we constructed an adverse outcome pathway (AOP) by collecting the available knowledge considering the molecular mechanisms for PXR-mediated hypercholesterolemia. AOPs are tools of modern toxicology for systematizing mechanistic knowledge to assist health risk assessment of chemicals. AOPs are formalized and structured linear concepts describing a link between molecular initiating event (MIE) and adverse outcome (AO). MIE and AO are connected via key events (KE) through key event relationships (KER). We present a plausible route of how PXR activation (MIE) leads to hypercholesterolemia (AO) through direct regulation of cholesterol synthesis and via activation of sterol regulatory element binding protein 2-pathway.
Similar content being viewed by others
Avoid common mistakes on your manuscript.
Background
Hypercholesterolemia is a lipid metabolism disorder, defined by high level of low-density lipoprotein (LDL) cholesterol in the blood. Hypercholesterolemia is a major contributor to the development of atherosclerosis, the leading cause of mortality in developed countries (Ziegler et al. 2020). The risk factors for hypercholesterolemia include sedentary lifestyle, western diet, obesity as well as genetic predisposition (Garg and Simha 2007; Ziegler et al. 2020). In addition, pharmaceuticals and environmental chemicals elevate lipid levels and in fact more than hundred drugs increasing total cholesterol levels have been identified (Karpale et al. 2022). However, the mechanisms underlying chemical-induced hypercholesterolemia remain poorly understood. Interestingly, several drugs, which increase lipid levels, are known to activate pregnane X receptor (PXR, NR1I2) (Karpale et al. 2022).
PXR is a sensor of xenobiotics, detecting fluctuations in chemical environment (Blumberg et al. 1998; Kliewer et al. 1998). PXR recognizes various structurally diverse endogenous and exogenous substances as ligands in a species-specific manner (Kliewer et al. 1998). Known ligands for PXR include pharmaceuticals (e.g., rifampicin, phenobarbital, clotrimazole) (Lehmann et al. 1998), pesticides (e.g., metolachlor, propiconazole, permethrin pyrethroid) and environmental contaminants such as polychlorinated biphenyls (Lemaire et al. 2006). In addition to the originally identified function as a regulator of detoxification functions, PXR activation has been found to disturb cardiometabolic functions such as glucose tolerance, lipid metabolism and regulation of blood pressure (Hukkanen and Hakkola 2020).
Cholesterol homeostasis in mammalian cells is maintained by a feedback system depending on cholesterol level and modulating the transcription of genes responsible for cholesterol synthesis and uptake (Brown and Goldstein 1997). A family of transcription factors called sterol regulatory element binding proteins (SREBPs) are the master regulators of the feedback system. SREBP pathway activity is regulated by cellular sterol level. In the condition of high sterol level, SREBPs remain inactive, the expression of the target genes is low, and consequently cholesterol synthesis is repressed. Recently, PXR was shown to increase lipid levels by SREBP-mediated mechanism inducing genes participating in cholesterol synthesis and uptake (Karpale et al. 2021). Furthermore, PXR has been shown to directly regulate at least one of the cholesterol synthesis genes (Gwag et al. 2019).
We applied an adverse outcome pathway (AOP) framework to elucidate the mechanisms linking PXR activation to increased level of plasma LDL cholesterol. AOPs are formalized and structured linear concepts connecting a molecular initiating event (MIE) to an adverse outcome (AO) via key events (KE) and key event relationships (KER) (Ankley et al. 2010). AOP summarizes existing knowledge to support health risk assessment of chemicals. AOPs do not describe complex cellular or molecular mechanisms but rather are simplified versions of toxicity pathways focusing on essential events (Svingen et al. 2021). Based on AOP-wiki database (https://aopwiki.org/events/245 accessed 25 Nov 2022), PXR activation has been proposed as an MIE in two AOPs, but neither of them links PXR activation to hypercholesterolemia. Here, we describe strategy of AOP development, which aims to explain the observed AO in terms of a MIE and KEs (Villeneuve et al. 2014). The AOP was developed according to the “Users' Handbook supplement to the Guidance Document for developing and assessing Adverse Outcome Pathways”, issued by the Organisation for Economic Co-operation and Development the users’ handbook (OECD 2018).
Proposed mechanism for PXR-induced hypercholesterolemia
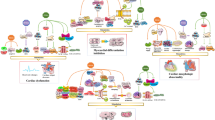
Binding of a suitable ligand activates PXR, being the MIE of the AOP (Fig. 1.). PXR activation leads to destabilized structure of insulin-induced gene 1 (INSIG1) protein, the first KE. Unstable structure of INSIG1 allows cholesterol-independent activation of sterol regulatory element binding protein 2 (SREBP2) which is the second KE in the pathway. This further increases the transcription of SREBP2 target genes, leading to increased synthesis and activation of proprotein convertase subtilisin kexin type 9 (PCSK9) (KE3) and enzymes participating in cholesterol synthesis (KE4). Moreover, PXR is able to directly activate squalene epoxidase (SQLE) (KE5), the rate-limiting enzyme of cholesterol synthesis. Increased level of PCSK9 in serum leads to decreased amount of LDL receptors (LDLR) in hepatocyte plasma membrane, causing diminished uptake of LDL from circulation by liver. Simultaneously, activation of cholesterol synthesis enzymes enhances cholesterol synthesis. Together these mechanisms lead to increased level of plasma LDL cholesterol, which is the adverse outcome (AO) of the pathway.
Graphic representation of the adverse outcome pathway from PXR activation to increased level of plasma LDL cholesterol. The molecular initiating event (MIE) is activation of pregnane X receptor (PXR), which leads to the first key event (KE), unstabilized structure of insulin-induced gene (INSIG1). Unstable structure of INSIG1 allows activation of sterol regulatory element binding protein 2 (SREBP2), the second KE in the pathway. Activation of SREBP2 increases the transcription of its target genes, leading to increased synthesis and activation of proprotein convertase subtilisin kexin type 9 (PCSK9) (KE3) and enzymes participating in cholesterol synthesis (KE4). PXR directly activates squalene epoxidase (SQLE) (KE5), rate-limiting enzyme of cholesterol synthesis. Increased serum level of PCSK9 leads to decreased amount of low-density lipoprotein (LDL) receptors, causing diminished uptake of LDL from circulation by liver. Simultaneously, activation of cholesterol synthesis enzymes enhances cholesterol synthesis. These mechanisms lead to increased level of plasma LDL cholesterol, the adverse outcome (AO) of the pathway. Arrows represent direct key event relationships (KERs) that link the KEs
MIE: PXR activation (KE:245)
Key event description
The MIE, activation of PXR (NR1I2), is already described in AOP-Wiki as a KE (KE:245, Activation PXR/SXR https://aopwiki.org/events/245 accessed 25 Nov 2022). PXR recognizes various structurally divergent endogenous and exogenous ligands (di Masi et al. 2009) due to its large, flexible, and hydrophobic ligand binding domain (Zhou et al. 2009b). Upon ligand binding, PXR forms a heterodimer with another nuclear receptor, retinoid X receptor. The heterodimer then binds to specific promoter sequences regulating transcription of various genes involved in cellular metabolism and clearance of xenobiotics and endotoxins in the liver and intestine such as genes encoding cytochrome P450 enzymes and transporter proteins (Kliewer et al. 1998; Zhou et al. 2009b; Hakkola et al. 2016). PXR also interacts with other transcription factors, which increases the complexity of regulatory networks (Hakkola et al. 2016).
Domain of applicability
PXR expression is well established in humans and rodents, and PXR gene has been characterized in several vertebrate species including zebrafish, frog, chicken, dog, pig, and rhesus monkey (Jones et al. 2000; Moore et al. 2002). PXR is expressed mainly in liver and intestine, and in low levels in lungs, stomach, peripheral blood monocytes, the blood–brain barrier, uterus, ovary, placenta, breast, osteoclasts, heart, adrenal gland, bone marrow, and certain regions of the brain (Kliewer et al. 1998; Lamba et al. 2004; Daujat-Chavanieu and Gerbal-Chaloin 2020). Expression of PXR increases through life stages starting with low expression level during fetal and neonatal stages and reaching the highest expression level in the adulthood (Daujat-Chavanieu and Gerbal-Chaloin 2020). Despite the low expression level during fetal development, the activity of PXR is induced by PXR ligands in fetal liver (Xiang et al. 2020; Dai et al. 2021).
The DNA-binding domain of PXR is highly conserved, but the ligand-binding domain differs between species (Jones et al. 2000). Consequently, the ligand preference of PXR differs significantly between species (Kliewer et al. 1998). Additionally, circadian variation and sex dimorphism of PXR have been observed in murine models (Wolbold et al. 2003; Lu et al. 2013; Xiang et al. 2020; Dai et al. 2021). Sex-specific activation of PXR has also been detected in human hepatic cell lines, whereas the findings of sex-dependent expression of PXR mRNA in human liver samples are inconsistent (Wolbold et al. 2003; Lamba et al. 2004; Xiang et al. 2020).
KER1 between PXR activation and stability of INSIG1
Key event relationship description
Recently, PXR activation was suggested to destabilize the structure of INSIG1 protein (Karpale et al. 2021). Previously, PXR activation has been shown to alter the expression of Insig1 in vivo and in vitro (Roth et al. 2008; Zhou et al. 2009a; Farmahin et al. 2019; Knebel et al. 2019). Insulin-induced genes (INSIG1 and INSIG2) code endoplasmic reticulum (ER) membrane proteins with similar functions (Yang et al. 2002; Yabe et al. 2002). INSIG1 maintains the intracellular lipid metabolism homeostasis in hepatocytes and adipocytes by regulating de novo synthesis and uptake of cholesterol and fatty acids (Ouyang et al. 2020). Therefore, deviation in expression or function of INSIG1 is linked with the pathogenesis of lipid disorders. Due to its crucial role in lipid metabolism, INSIG1 is highly expressed in hepatocytes and adipocytes (Diamond et al. 1993; Peng et al. 1997). In humans and rodents, INSIG1 is mostly expressed in the liver, but at low levels also in other tissues (Peng et al. 1997; Uhlén et al. 2015). The conservation of INSIG1 sequence varies among vertebrate species (mouse, hamster, zebrafish) between 70 and 92% compared to human (Yabe et al. 2002). The variation is mostly exerted in the hydrophilic NH2- and COOH-terminal sequences. INSIG1 is expressed already during development (Iritani et al. 1993; Lou et al. 2014).
Biological plausibility
Biological plausibility for PXR activation leading to altered function of INSIG1 is moderate. PXR is shown to bind to DR-4 site in the upstream promoter region of INSIG1 and induce INSIG1 mRNA expression (Roth et al. 2008). The mechanism causing destabilization of INSIG1 protein is currently unknown.
Empirical evidence
The ability of PXR to increase (Roth et al. 2008; Zhou et al. 2009a; Knebel et al. 2019) or decrease (Farmahin et al. 2019) Insig1 mRNA expression is described in few studies characterizing the effects of PXR on INSIG1 in rodents and hepatic cells in vitro. Recently, Karpale et al. (2021) reported increased Insig1 mRNA expression after PXR activation in livers of obese male C57BL/6 N mice treated with a rodent PXR ligand, pregnenolone 16α-carbonitrile (PCN); this induction was not seen in Pxr knockout mice (Karpale et al. 2021). On the contrary, PXR did not affect the protein level of INSIG1, despite cholesterol accumulation, which should enhance INSIG1 production and stabilize the protein structure. The authors concluded that PXR may alter the proteolytic machinery controlling INSIG1 stability (Karpale et al. 2021). Alternatively, the INSIG1 translation could be repressed.
Uncertainties and inconsistencies
Even though activation of PXR is observed to alter Insig1 expression on mRNA level, there is only one study determining the effects on protein level or further on INSIG1 stability (Table 1). In addition, the mechanism by which PXR would alter the stability of INSIG1 is unknown.
KER2 between INSIG1 stability and SREBP2 activation
Key event relationship description
INSIG1 controls cholesterol synthesis and uptake via regulating the activation of SREBP2 in a cholesterol-dependent fashion by binding to SREBP cleavage-activating protein (SCAP) (Brown and Goldstein 1999). Binding of INSIG1 to SCAP promotes the retention of SREBP2 in ER and inhibits transfer to Golgi and activation of SREBP2.
The SREBP family of membrane-bound transcription factors consists of three members, SREBP1a, SREBP1c, and SREBP2 (Brown and Goldstein 1997). Cholesterol metabolism is regulated especially by SREBP2. The three members of SREBPs are expressed ubiquitously in several mammalian species and are detected in all tissues (Horton et al. 2002; Eberlé et al. 2004). SREBP1a and SREBP2 are the predominant isoforms in majority of cell lines, whereas SREBP1c and SREBP2 are the most abundant isoforms in the liver of mice and human (Shimomura et al. 1997). SREBP1a and -1c are produced by SREBPF1 and SREBP2 by SREBPF2 genes, respectively (Hua et al. 1995; Miserez et al. 1997) and share 47% homology with each other (Eberlé et al. 2004). SREBP2 seems to have a crucial role already in the early stages of development, since deletion of Srebpf2 gene is observed to be lethal in animal models (Shimano et al. 1997).
Biological plausibility
Activation of SREBP2 is controlled by a cholesterol-dependent transport system between ER and Golgi (Fig. 2). SREBPs locate in the ER as heterodimers with another ER membrane protein, SCAP, which has as a sterol-sensing domain regulating the transport from ER to Golgi (Brown and Goldstein 1999). SCAP functions as an escort protein for SREBP and is essential for SREBP stability (Sever et al. 2003). In a case of sterol depletion, the SCAP/SREBP complex locates to the Golgi apparatus in the coat protein complex II (COP2) coated vesicles (Goldstein et al. 2006). In Golgi, SREBP goes through proteolytic processing by two cleavage enzymes: membrane-bound transcription factor site-1-protease (S1P) and site-2-protease (S2P) (Brown and Goldstein 1999). As a result, an active, soluble N-terminal-cleaved transcription factor of the basic helix-loop-helix leucine zipper family is created (Brown and Goldstein 1997; Goldstein et al. 2006). This structural change allows SREBPs to enter the nucleus as homodimers, bind to sterol regulating element (SRE) sequences and induce gene transcription. On the contrary, when sterol level is high, S1P reaction is blocked and the SCAP/SREBP complex remains in ER.
Graphical illustration of sterol regulatory element binding protein 2 (SREBP2) activation pathway. After the complex formed by SREBP2 and SREBP cleavage activating protein (SCAP) detaches from insulin-induced gene 1(INSIG1) the complex locates from endoplasmic reticulum (ER) to Golgi in the Coat Protein Complex II (COP2) coated vesicles. In Golgi, SREBP2 goes through a proteolytic processing by two cleavage enzymes known as membrane-bound transcription factor site-1-protease (S1P) and site-2-protease (S2P). Consequently, the active transcription factor (N-SREBP2) is released, and translocates to the nucleus where it binds to sterol regulating element (SRE) sequences and induces transcription of genes participating in cholesterol biosynthesis and uptake
Empirical evidence
The ability of INSIG1 to control SREBP2 activity is widely established (Brown and Goldstein 1997; Ouyang et al. 2020). Under normal conditions, increased cholesterol level and SREBP2 processing induce INSIG1 mRNA expression, which abolishes SREBP2 activity. PXR activation may alter INSIG1 stability as described in KER1. Karpale et al. (2021) observed that activation of SREBP2 was independent from cholesterol level, indicating a perturbation in the normal regulation of SREBP2 pathway possibly mediated by altered INSIG1 function. Similar results have been observed in the liver and intestine of Insig knockout mice, where nuclear SREBP and mRNA level of SREBP target genes remain elevated despite overaccumulation of sterols, which should downregulate SREBP activity (Engelking et al. 2005; McFarlane et al. 2014). When INSIG1 proteins are absent, SREBPs are resistant to cholesterol-dependent suppression (McFarlane et al. 2014). In vitro studies have revealed that SREBP transport to nucleus is inhibited by binding of SCAP to INSIG when ER cholesterol level reaches above 5% of total ER lipid level (Radhakrishnan et al. 2008). INSIG depletion allows cleaving of SREBPs despite high cholesterol levels by increasing the threshold that should initiate the negative feedback (McFarlane et al. 2014). Similarly, the excess of cholesterol fails to stabilize INSIG1 in SCAP-deficient cells (Gong et al. 2006). Furthermore, saturation of INSIG1 allows remaining unbound SCAP to transport SREBP2 to Golgi and is also, therefore, resistant to sterol-mediated inhibition of proteolytic processing of SREBP (Yang et al. 2002).
Known feedback loops influencing KER2
Transcription of INSIG1 is dependent on cholesterol level and activation of SREBPs (Goldstein et al. 2006). INSIG1 mRNA production is enhanced when cells are sterol depleted or if cleaved SREBP occurs in the nucleus and is prevented when cholesterol accumulates or if inactive SREBP is retained in ER. Quite the opposite, the INSIG1 protein is ubiquitinated and degraded rapidly when cells are sterol depleted. In sterol-accumulated cells, INSIG1 structure is stabilized by SCAP. Moreover, the expression of INSIG1 is reliant on SREBP1c, whose transcription is controlled by insulin (Chen et al. 2004; Goldstein et al. 2006). Low insulin level during fasting leads to repression of SREBP1c and suppression of Insig1 mRNA. When insulin level increases, SREBP1c processing and Insig1 mRNA increases concordantly.
Two classes of sterols, cholesterol, and oxysterols, regulate SREBP2 activity by inhibiting the proteolytic processing of SREBP2, which reduces the level of active transcription factor in the nucleus (Goldstein et al. 1979). To inhibit the translocation of SREBP2 to be processed in Golgi, cholesterol binds to SCAP and oxysterols bind to INSIGs, which triggers INSIG to bind to SCAP (Sun et al. 2007). These mechanisms result in conformational changes in SCAP preventing clustering of SREBP with COP2 vesicles that are responsible of the translocation of SREBP to Golgi.
High-fat diet seems to dysregulate SREBP2 activation. Upregulated expression of SREBP2 mRNA and protein has been observed in the livers of mice exposed to high-fat diet (Wu et al. 2013). In accordance with Karpale et al. (2021), increased Insig1 mRNA level was also observed. On the other hand, in the study by Karpale and colleagues (2021), high-fat diet alone did not induce the expression of SREBP2, but the activation was shown to be PXR dependent.
KER3 between SREBP2 activation and increased level of PCSK9
Key event relationship description
PCSK9 is a circulating hepatic protein and has a crucial role in regulating cholesterol level (Seidah et al. 2003; Poirier et al. 2008). The transcription of PCSK9 is controlled by SREBP2. PCSK9 is expressed mainly in liver, especially during development and it is also present in small intestine, kidney, and brain (Seidah et al. 2003).
Biological plausibility
SREBP2 acts as a main regulator of PCSK9 transcription (Horton et al. 2007) via functional sterol regulatory element (SRE) in proximal promoter of PCSK9 (Li et al. 2009). PCSK9 is secreted by the liver as a zymogen precursor and is autocatalytically cleaved in the ER, releasing the N-terminal prodomain of PCSK9, which further forms a noncovalent bond with the catalytic or C-terminal domain (Seidah 2013). N-terminal prodomain prevents PCSK9 function and to activate, catalytic domain of PCSK9 needs to be released from the prodomain.
Empirical evidence
The role of SREBP2 as the main transcriptional regulator of Pcsk9 expression is well established in transgenic and Srebp knockout mice as well as in vitro studies (Horton et al. 2003; Maxwell et al. 2003; Hyun et al. 2008). As mentioned above, SREBP2 level is highly correlated with plasma cholesterol level, which further reflects to PCSK9 transcription (Lagace 2014). PCSK9 expression is also increased after PXR activation both in mice and humans and in mouse this was shown to be associated with increased nuclear SREBP2 level (Karpale et al. 2021).
KER4 between SREBP2 activation and increased level of cholesterol synthesis enzymes
Key event relationship description
The genes induced by SREBP2 encode enzymes that are involved in different phases of the mevalonate pathway of cholesterol synthesis including 3-hydroxy-3-methylglutaryl-coenzyme (HMGCR) (Hua et al. 1993). HMGCR is the first rate-limiting enzyme in the mevalonate pathway emphasizing its role as a main target for regulation (DeBose-Boyd 2008). HMGCR is localized in ER of all mammalian species studied including human, mouse, rat, and hamster.
Biological plausibility
SREBP2 induces the expression of several genes involved in cholesterol synthesis and uptake by binding to SREs in the regulatory regions (Horton et al. 2002). Only few SREs in the promoters of these genes are characterized in humans and in some extent in other species (Sharpe and Brown 2013). However, SREs might not be conserved among species.
Empirical evidence
HMGCR is directly regulated by SREBP2 via gene transcription (Howe et al. 2017). This is supported by the finding that decreased amount of active SREBP2 leads to reduction of mRNA levels of Hmgcr both in vivo and in vitro (König et al. 2007). SREBP2-regulated inhibition of mevalonate pathway is a target for cancer therapy and several preclinical studies have shown that modulating SREBP2 activity reflects to the activity of the mevalonate pathway, as reviewed by Xue and coworkers (Xue et al. 2020). Moreover, PXR activation in obese mice yielded in increased expression level of nearly all genes participating in cholesterol synthesis and the effect is predicted to be SREBP2 mediated. (Karpale et al. 2021).
Known feedforward/feedback loops influencing KER4
In addition to rather slow SREBP2 mediated regulation, HMGCR is more rapidly regulated post-translationally by INSIG1 (Sharpe and Brown 2013). INSIG1 accelerates degradation of HMGCR in ER by combining to the sterol sensing domain of HMGCR (Ouyang et al. 2020). In cellular cholesterol depletion, INSIG1 protein is unstable and unable to bind HMGCR, but when the cholesterol level increases, the structure stabilizes and binds to HMGCR causing the degradation and preventing the further increase of cholesterol level. INSIG1 dysfunction, possibly caused by PXR, induces perturbations in the INSIG1-mediated regulation of HMGCR (Karpale et al. 2021). The effect was observed in obese mice, where HMGCR mRNA and protein levels were increased, despite cholesterol accumulation.
KER5 between PXR activation and increased activity of SQLE
Key event relationship description
SQLE, encoded by SQLE gene, is the second rate-limiting enzyme in the mevalonate pathway (Hidaka et al. 1990; Nagai et al. 1997; Gill et al. 2011). SQLE is a vital enzyme among eukaryotes (Chua et al. 2020), but it serves as a controller of cholesterol synthesis only in mammals. SQLE is expressed ubiquitously in mammals, yet is the most abundant in esophagus, testis, and liver, the latest serving as the main organ for cholesterol synthesis (Uhlén et al. 2015; Chua et al. 2020). Activation of PXR has been shown to directly activate SQLE (Gwag et al. 2019).
Biological plausibility
The ability of PXR to bind DR-2 site in Sqle gene promoter region was recently identified, indicating that Sqle is a direct transcriptional target of PXR (Gwag et al. 2019). Additionally, PXR activation has been observed to increase both mRNA and protein level of SQLE (Gwag et al. 2019; Karpale et al. 2021). On the other hand, Sqle is a target gene for SREBP2, which activity is also shown to be controlled by PXR, as described above.
Empirical evidence
Increased Sqle mRNA expression after PXR activation has been observed in few studies (Table 1.) (Gwag et al. 2019; Jiang et al. 2021; Karpale et al. 2021). In addition to mRNA level, Gwag et al. (2019) discovered increased protein level of SQLE both in vivo and in vitro. SQLE was also identified as a direct transcriptional target of PXR (Gwag et al. 2019).
Known feedforward/feedback loops influencing KER5
SQLE activity is controlled by cholesterol via direct feedback mechanism, abundance of cholesterol causing degradation of SQLE enzyme (Chua et al. 2020). The activation of SQLE transcription is controlled by SREBP2 and its cofactors, and transcriptional activity increases in sterol-depleted conditions. The regulation of SQLE activity is thought to be independent from the rest of the cholesterol synthesis pathway, since the SQLE enzyme adjusts the cholesterol synthesis within the pathway, making it suitable for fast and flexible adapting of cholesterol levels (Gill et al. 2011; Chua et al. 2020).
Uncertainties and inconsistencies
Long-term treatment with a PXR agonist PCN does not seem to induce Sqle mRNA level in male C57BL/6 mice (Zhang et al. 2022). However, the liver samples from PCN-treated mice were collected after 7 days of the last dose, which might cause reversal of PXR activation. Also, long-term treatment may cause alterations in the status of the receptor due to adaptation of liver to external stimuli (Zhang et al. 2022). In accordance with Zhang & co-workers, Ann Barretto et al. (2019) did not observe any changes in Sqle regulation in male C57BL/6 mice after 4-day administration of PCN regardless of PXR activation. Increase in cholesterol biosynthesis was not observed either, but previous studies had shown that mice on normal chow diet are resistant to changes in lipid profile, which might be the case in this study as well (Ann Barretto et al. 2019; Hassani-Nezhad-Gashti et al. 2019). On the other hand, effect of PXR activation on SQLE activation and lipid level has been observed in mice on a regular diet in other studies (Gwag et al. 2019; Jiang et al. 2021).
KER6 between increased level of PCSK9 and increased level of plasma LDL cholesterol
Key event relationship description
Liver is the main organ clearing LDL from plasma and excreting cholesterol from the body (Spady et al. 1985). Fluctuations in the regulation of the efflux pathway lead to unbalanced homeostasis of sterols. Sufficient hepatic uptake of LDL cholesterol by LDLRs is crucial for regulation of circulating LDL cholesterol level. Decreased LDL uptake by liver caused by downregulated number of LDLRs in plasma membrane of hepatocytes leads to inadequate hepatic clearance of cholesterol. This results in increased level of circulating LDL cholesterol. PCSK9 controls the amount of LDLRs in hepatocytes (Seidah et al. 2014).
Biological plausibility
In the bloodstream, activated PCSK9 binds to hepatic LDLRs enhancing the lysosomal degradation of the receptors (Seidah 2013). Two different pathways of PCSK9 mediated LDLR degradation have been identified (Lagace 2014). PCSK9 binds to LDLR intracellularly and escorts it from trans-Golgi to lysosomal degradation. Secondly, secreted PCSK9 may bind to the first epidermal-growth factor-like repeat of LDLR on the cell surface leading to internalization of the PCSK9-LDLR-complex in endocytic vesicles.
Empirical evidence
The role of PCSK9 as a regulator of LDLRs and in development of hypercholesterolemia is well described (Grefhorst et al. 2008; Lambert et al. 2008; Seidah 2013) and overexpression of PCSK9 accumulates LDL in the circulation (Benjannet et al. 2004; Lalanne et al. 2005; Lambert et al. 2006). Enhanced excretion of PCSK9 from liver causes degradation of LDLRs and is resulted in increased plasma LDL levels (Seidah 2013). Discovery of the mechanism has resulted in the development of pharmacological applications and nowadays PCSK9 inhibitors are a common treatment for hypercholesterolemia (Seidah et al. 2014).
Known feedback loops influencing KER6
In addition to post-transcriptional regulation of LDLRs by PCSK9, transcription of LDLRs is regulated by SREBP2 (Horton et al. 2002). SREBP2 activation increases the expression of LDLRs thereby increasing cholesterol uptake from plasma. Since SREBP2 regulates Pcsk9 at transcriptional level, it induces simultaneous opposite effects on LDLRs by regulating the amount of LDLRs at both transcriptional and post-transcriptional levels. (Rashid et al. 2005).
KER7 between increased level of cholesterol synthesis enzymes and increased level of plasma LDL cholesterol
Key event relationship description
In addition to LDL clearance, regulation of cholesterol synthesis is critical in maintaining cholesterol homeostasis (Spady et al. 1985). In mammals, almost all cells synthesize cholesterol (Brown and Sharpe 2016). However, level of plasma cholesterol is dictated by liver cholesterol synthesis. Cholesterol synthesis is a complex process, and it is highly regulated by negative feedback mechanism to avoid cholesterol depletion or excess. Therefore, in cases where the cholesterol synthesis pathway is dysregulated, the process of cholesterol synthesis may persist even in the presence of cholesterol accumulation. This is in contrast to the feedback mechanism, as the accumulation of cholesterol should typically impede the function of the enzymes responsible for maintaining cholesterol homeostasis (Engelking et al. 2005).
Biological plausibility
As described above, cholesterol regulates several proteins by enhancing or inhibiting their function depending on the needs of a cell. The first step in the mevalonate pathway of cholesterol synthesis (Fig. 3) is conversion of acetyl coenzyme A to acetoacetyl coenzyme A by thiolase 2 (Brown and Sharpe 2016). Methylglutaryl-coenzyme A synthase is the second enzyme condensing acetyl coenzyme A with acetoacetyl coenzyme A to form 3-hydroxy-3-methylglutaryl coenzyme A. Next, HMGCR reduces the synthetized 3-hydroxy-3-methylglutaryl coenzyme A to mevalonic acid. Mevalonic acid is phosphorylated to mevalonate-P by mevalonate kinase and mevalonate-P is further produced to mevalonate-PP by phosphomevalonate kinase. Next, diphosphomevalonate decarboxylase catalyzes the reaction of mevalonate-PP to isopentenyl-PP, followed by isomerization to dimethylallyl-PP by isopentenyl-diphosphate Δ-isomerase. These isoprenoid-pyrophosphates are then condensed to isoprenoid geranyl-PP by farnesyl diphosphate synthase or to farnesyl-PP by geranylgeranyl pyrophosphate synthase and finally, squalene synthase converts farnesyl-PP to squalene. Then squalene is converted to (S)-2,3-epoxysqualene by SQLE and (S)-2,3-epoxysqualene is further converted to lanosterol and finally to cholesterol via Bloch or Kandutch–Russel pathways. Furthermore, surplus cholesterol undergoes esterification through acyl coenzyme A, resulting in the formation of cholesteryl esters (Luo et al. 2019). These esters serve as a cholesterol reserve within cytosolic lipid droplets or are released as prominent constituents of plasma lipoproteins, such as chylomicrons, very low-density lipoproteins (VLDLs), LDLs, and high-density lipoproteins (HDLs). PXR may induce enzymes participating in hydrolysis of cholesterol esters in the intestine (Helsley et al. 2013).
Mevalonate pathway of cholesterol synthesis. First, acetyl-CoA is converted to acetoacetyl-CoA by thiolase 2. Secondly, methylglutaryl-coenzyme A synthase (HMGCS) condenses acetyl-CoA with acetoacetyl-CoA to form HMG-CoA (Brown and Sharpe 2016). Next, HMGCR reduces HMG-CoA to mevalonic acid. Mevalonic acid is phosphorylated to mevalonate-P by mevalonate kinase (MK) and mevalonate-P is further produced to mevalonate-PP by phosphomevalonate kinase (PMK). This is followed by catalyzation of mevalonate-PP to isopentenyl-PP by diphosphomevalonate decarboxylase. Next, dimethylallyl-PP is isomerized by isopentenyl-diphosphate Δ-isomerase (IDI1/IDI2). The isoprenoid-pyrophosphates are condensed to isoprenoid geranyl-PP by farnesyl diphosphate synthase (FPPS) or to farnesyl-PP by geranylgeranyl pyrophosphate synthase (GGPPS) and finally, squalene synthase (SQS) converts farnesyl-PP to squalene. Squalene is converted to (S)-2, 3-epoxysqualene by squalene epoxidase (SQLE) and (S)-2,3-epoxysqualene is further converted to lanosterol and finally to 7-dehydrodesmosterol or 7-dehydrocholesterol via Bloch or Kandutch-Russel (K-R) pathways, respectively
Due to the criticalness of the enzymes involved in the cholesterol synthesis pathway, their inhibition has yielded several pharmacological applications. For example, the mechanism of action of common LDL cholesterol-lowering drugs, statins, is based on inhibition of HMGCR, which prevents further processing of cholesterol precursors in the mevalonate pathway and therefore decreases plasma cholesterol levels (Sirtori 2014).
Empirical evidence
In Insig1 knockout mice, the degradation of the rate-limiting enzyme HMGCR, is prevented, allowing the prolonged continuation of cholesterol synthesis resistant to cholesterol-dependent regulation (Engelking et al. 2005; McFarlane et al. 2014). On the contrary, in Hmgcr knockout mice, hepatic cholesterol synthesis is decreased (Nagashima et al. 2012). In addition, increased expression of the second rate-limiting enzyme of cholesterol synthesis, SQLE, results in elevated plasma, total, LDL, and HDL cholesterol in C57BL/6 wild-type, liver-specific Pxr-flox allele-carrying, and PXR-humanized C57BL/6 mice (Gwag et al. 2019).
Known feedforward/feedback loops influencing KER7
Cholesterol synthesis pathway is highly regulated to avoid fluctuations in cholesterol level. The feedback inhibition pathways controlling SREBP2 and HMGCR activity (KER2 & KER4), lead to downregulation of most of the enzymes in cholesterol synthesis pathway and degradation of HMGCR, respectively (Goldstein et al. 1979; DeBose-Boyd 2008). As a result, cholesterol synthesis decreases.
Modulating factors
Generally, squalene, an intermediate of cholesterol synthesis, tends to accumulate in the liver in the presence of high cholesterol level due to downregulation of SQLE (Gill et al. 2011). However, decreased squalene level has been observed in mice with PXR-induced hypercholesterolemia (Karpale et al. 2021). The authors suggest that this indicates enhanced squalene metabolism caused by increased SQLE activity mediated by PXR.
Interestingly, Karpale et al. (2021) also showed that PXR activation induces the activation of Kandutsch–Russel pathway in both humans and mice, but the mechanism is unknown. Increased level of plasma and hepatic markers of the pathway and induction of the 24-dehydrocholesterol reductase enzyme was described, leading cholesterol synthesis towards Kandutsch–Russel pathway (Karpale et al. 2021).
AO: increased plasma LDL cholesterol
Key event description
The main function of LDL is to provide cholesterol to the cells and, therefore, it has a major role in cholesterol transfer and metabolism (Hevonoja et al. 2000). The LDL particle consists of a core formed of triglycerides and cholesteryl esters and of a surface comprised of phospholipids and a copy of a ApoB-100 lipoprotein. As a consequence of decreased hepatic clearance and overproduction of LDL, the concentration of circulating LDL increases. Next, LDL penetrates the vascular wall, especially on the parts with existing dysfunction or reduced blood flow and accumulates within the intima of arteries (Ziegler et al. 2020). Accumulated LDL particles are oxidized via reactive oxygen species, which triggers an inflammatory response and foam cell formation by macrophages further promoting the inflammatory state in the artery (Huff et al. 2016). Hypercholesterolemia is the most common atherogenic dyslipidemia, and ultimately leads to atherosclerosis characterized by formation of calcified and prone to rupture plaques in arteries, leading to complete obstruction of the artery.
Modulating factors
Development of hypercholesterolemia involves not only hepatic cholesterol synthesis but also the absorption of biliary and dietary cholesterol in the intestine (Jia et al. 2011). Niemann-Pick C1 Like 1 (NPC1L1) and ATP-binding cassette transporters G5 and G8 (ABCG5/G8) play crucial roles in regulating cholesterol uptake and efflux not only in the intestine but also in the liver and PXR and SREBP2 may contribute to their regulation (Alrefai et al. 2007; Tremblay et al. 2011; Sui et al. 2015; Meng et al. 2019). On the contrary, in obese mice PXR strongly induced hepatic cholesterol synthesis but had no effect on Npc1l1 expression but prompted Abcg5 expression (Karpale et al. 2021). Additionally, PXR activation led to elevated serum hepatic apolipoprotein B levels, reduced intestinal apolipoprotein B48 levels, and did not affect intestinal Apob expression in humans. These findings provide evidence for the repression of intestinal cholesterol absorption and propose that the PXR-induced increase in serum cholesterol occurs independently of intestinal cholesterol absorption and synthesis (Karpale et al. 2021). However, there is other evidence suggesting that also intestinal processes may play a role (Meng et al. 2019; Sui et al. 2021).
Overall assessment of AOP
Hypercholesterolemia is a major risk factor for vascular damage, cardiovascular diseases, and a critical contributor to global health burden. Several intrinsic and external factors such as environmental pollutants contribute to hypercholesterolemia. To elucidate the unclear mechanism behind chemical-induced hypercholesterolemia we applied an AOP framework for PXR activation leading to hypercholesterolemia. Essentiality of KEs, the biological plausibility and empirical evidence of KERs are described thoroughly in respective KER chapters and summarized in Table 2. Additionally, the quality of evidence rating is summarized in Table 1.
The first KER focuses on the effect of PXR activation on INSIG1 function. As INSIG1 controls cholesterol synthesis and uptake, an aberration in expression or function of INSIG1 is causal to lipid disorders (Ouyang et al. 2020). Even though PXR has been shown to bind the DR-4 site in the upstream promoter region of Insig1 (Roth et al. 2008) and the recent results suggest that PXR may regulate the translation or protein stability of INSIG1 (Karpale et al. 2021), further research is needed to determine the underlying mechanism.
Disturbed function of INSIG1 is a critical key point in the cholesterol synthesis pathway, since INSIG1 controls the activation of SREBP2. Activation of SREBP-pathway activates enzymes participating in cholesterol synthesis as well as the PCKS9 enzyme. In addition to PXR-mediated activation of SREBP-pathway, PXR affects directly on cholesterol synthesis pathway by regulating SQLE transcription. Together these mechanisms lead to increased cholesterol synthesis and decreased uptake of LDL by liver and finally to increased plasma LDL cholesterol (AO).
This AOP is a plausible description of the link between PXR activation and hypercholesterolemia and combines information from reviews and published data from in vivo and in vitro studies. Evidence regarding KERs 1 and 5 is scarce, and more studies are needed to better understand the relationships. On the other hand, the rest of the KERs are well established and supported by solid background of biological knowledge and empirical evidence. It must be noted that AOPs aim to simplify the toxicity pathways and focus merely on the essential events, as done in the current AOP. We acknowledge that all the KEs and KERs are also affected by other mechanism not described in the AOP.
Even though most of the described molecular interactions occur in various tissues and the KEs are applicable in both sexes through all life stages across taxa, we choose to limit the AOP to consider liver due to its criticalness in cholesterol metabolism and in chemical-induced hypercholesterolemia. This also reflects the predominant expression of PXR in the liver.
As a conclusion, the AOP illustrates how PXR potentially disturbs the regulation of cholesterol synthesis and LDL metabolism. The AOP was developed to offer an insight into the molecular mechanism of PXR mediated hypercholesterolemia, since the mechanisms of drug- and chemical-induced hypercholesterolemia are poorly understood. In the future, the AOP can be elaborated and possibly be included in the AOP-Wiki, which could promote safety assessment.
Availability of data and materials
Data sharing not applicable to this manuscript as no datasets were created or analyzed during the current study.
References
Alrefai WA, Annaba F, Sarwar Z et al (2007) Modulation of human Niemann-Pick C1-like 1 gene expression by sterol: Role of sterol regulatory element binding protein 2. Am J Physiol Gastrointest Liver Physiol 292:G369-376. https://doi.org/10.1152/ajpgi.00306.2006
Ankley GT, Bennett RS, Erickson RJ et al (2010) Adverse outcome pathways: a conceptual framework to support ecotoxicology research and risk assessment. Environ Toxicol Chem 29:730–741. https://doi.org/10.1002/etc.34
Ann Barretto S, Lasserre F, Fougerat A et al (2019) Gene expression profiling reveals that PXR activation inhibits hepatic PPARα activity and decreases FGF21 secretion in male C57Bl6/J mice. Int J Mol Sci 20:3767. https://doi.org/10.3390/IJMS20153767
Benjannet S, Rhainds D, Essalmani R et al (2004) NARC-1/PCSK9 and its natural mutants. J Biol Chem 279:48865–48875. https://doi.org/10.1074/jbc.m409699200
Blumberg B, Sabbagh W, Juguilon H et al (1998) SXR, a novel steroid and xenobiotic-sensing nuclear receptor. Genes Dev 12:3195–3205. https://doi.org/10.1101/gad.12.20.3195
Brown MS, Goldstein JL (1997) The SREBP pathway: regulation of cholesterol metabolism by proteolysis of a membrane-bound transcription factor. Cell 89:331–340. https://doi.org/10.1016/S0092-8674(00)80213-5
Brown AJ, Sharpe LJ (2016) Cholesterol Synthesis. Biochemistry of Lipids, Lipoproteins and Membranes: Sixth Edition 327–358. https://doi.org/10.1016/B978-0-444-63438-2.00011-0
Brown MS, Goldstein JL (1999) A proteolytic pathway that controls the cholesterol content of membranes, cells, and blood. PNAS 96:11041–11048. https://doi.org/10.1073/pnas.96.20.11041
Chen G, Liang G, Ou J et al (2004) Central role for liver X receptor in insulin-mediated activation of Srebp-1c transcription and stimulation of fatty acid synthesis in liver. PNAS 101:11245–11250. https://doi.org/10.1073/PNAS.0404297101
Chua NK, Coates HW, Brown AJ (2020) Squalene monooxygenase: a journey to the heart of cholesterol synthesis. Prog Lipid Res 79:101033. https://doi.org/10.1016/J.PLIPRES.2020.101033
Dai Y, Luo J, Xiang E et al (2021) Prenatal Exposure to retrorsine induces developmental toxicity and hepatotoxicity of fetal rats in a sex-dependent manner: the role of pregnane X receptor activation. J Agric Food Chem 69:3219–3231. https://doi.org/10.1021/acs.jafc.0c06748
Daujat-Chavanieu M, Gerbal-Chaloin S (2020) Regulation of CAR and PXR expression in health and disease. Cells 9(11):2395. https://doi.org/10.3390/cells9112395
DeBose-Boyd RA (2008) Feedback regulation of cholesterol synthesis: sterol-accelerated ubiquitination and degradation of HMG CoA reductase. Cell Res 18:609–621. https://doi.org/10.1038/cr.2008.61
di Masi A, de Marinis E, Ascenzi P, Marino M (2009) Nuclear receptors CAR and PXR: Molecular, functional, and biomedical aspects. Mol Aspects Med 30:297–343. https://doi.org/10.1016/j.mam.2009.04.002
Diamond RH, Du K, Lee VM et al (1993) Novel delayed-early and highly insulin-induced growth response genes. Identification of HRS, a potential regulator of alternative pre-mRNA splicing. J Biol Chem 268:15185–15192. https://doi.org/10.1016/S0021-9258(18)82454-1
Dong B, Wu M, Li H et al (2010) Strong induction of PCSK9 gene expression through HNF1α and SREBP2: Mechanism for the resistance to LDL-cholesterol lowering effect of statins in dyslipidemic hamsters. J Lipid Res 51:1486–1495. https://doi.org/10.1194/jlr.M003566
Eberlé D, Hegarty B, Bossard P et al (2004) SREBP transcription factors: master regulators of lipid homeostasis. Biochimie 86:839–848. https://doi.org/10.1016/J.BIOCHI.2004.09.018
Engelking LJ, Liang G, Hammer RE et al (2005) Schoenheimer effect explained – feedback regulation of cholesterol synthesis in mice mediated by Insig proteins. J Clin Invest 115:2489–2498. https://doi.org/10.1172/JCI25614
Farmahin R, Gannon AM, Gagné R et al (2019) Hepatic transcriptional dose-response analysis of male and female Fischer rats exposed to hexabromocyclododecane. Food Chem Toxicol 133:110262. https://doi.org/10.1016/j.fct.2018.12.032
Garg A, Simha V (2007) Update: Update on dyslipidemia. J Clin Endocrinol Metab 92:1581–1589. https://doi.org/10.1210/jc.2007-0275
Gill S, Stevenson J, Kristiana I, Brown AJ (2011) Cholesterol-dependent degradation of squalene monooxygenase, a control point in cholesterol synthesis beyond HMG-CoA reductase. Cell Metab 13:260–273. https://doi.org/10.1016/J.CMET.2011.01.015
Goldstein JL, Ho YK, Basu SK, Brown MS (1979) Binding site on macrophages that mediates uptake and degradation of acetylated low density lipoprotein, producing massive cholesterol deposition. PNAS 76:333–337. https://doi.org/10.1073/PNAS.76.1.333
Goldstein JL, DeBose-Boyd RA, Brown MS (2006) Protein sensors for membrane sterols. Cell 124:35–46. https://doi.org/10.1016/J.CELL.2005.12.022
Gong Y, Lee JN, Lee PCW et al (2006) Sterol-regulated ubiquitination and degradation of Insig-1 creates a convergent mechanism for feedback control of cholesterol synthesis and uptake. Cell Metab 3:15–24. https://doi.org/10.1016/J.CMET.2005.11.014
Grefhorst A, McNutt MC, Lagace TA, Horton JD (2008) Plasma PCSK9 preferentially reduces liver LDL receptors in mice. J Lipid Res 49:1303–1311. https://doi.org/10.1194/jlr.M800027-JLR200
Gwag T, Meng Z, Sui Y et al (2019) Non-nucleoside reverse transcriptase inhibitor efavirenz activates PXR to induce hypercholesterolemia and hepatic steatosis. J Hepatol 70:930–940. https://doi.org/10.1016/j.jhep.2018.12.038
Hakkola J, Rysä J, Hukkanen J (2016) Regulation of hepatic energy metabolism by the nuclear receptor PXR. Biochim Biophys Acta 1859:1072–1082. https://doi.org/10.1016/j.bbagrm.2016.03.012
Hassani-Nezhad-Gashti F, Kummu O, Karpale M et al (2019) Nutritional status modifies pregnane X receptor regulated transcriptome. Sci Rep 9:16728. https://doi.org/10.1038/s41598-019-53101-9
Helsley RN, Sui Y, Ai N et al (2013) Pregnane X receptor mediates dyslipidemia induced by the HIV protease inhibitor amprenavir in mice. Mol Pharmacol 83:1190–1199. https://doi.org/10.1124/mol.113.085753
Hevonoja T, Pentikäinen MO, Hyvönen MT et al (2000) Structure of low density lipoprotein (LDL) particles: Basis for understanding molecular changes in modified LDL. Biochim Biophys Acta 1488:189–210. https://doi.org/10.1016/S1388-1981(00)00123-2
Hidaka Y, Satoh T, Kamei T (1990) Regulation of squalene epoxidase in HepG2 cells. J Lipid Res 31:2087–2094. https://doi.org/10.1016/s0022-2275(20)42273-4
Horton JD, Goldstein JL, Brown MS (2002) SREBPs: activators of the complete program of cholesterol and fatty acid synthesis in the liver. J Clin Invest 109:1125–1131. https://doi.org/10.1172/JCI15593
Horton JD, Shah NA, Warrington JA et al (2003) Combined analysis of oligonucleotide microarray data from transgenic and knockout mice identifies direct SREBP target genes. PNAS 100:12027–12032. https://doi.org/10.1073/PNAS.1534923100
Horton JD, Cohen JC, Hobbs HH (2007) Molecular biology of PCSK9: its role in LDL metabolism. Trends Biochem Sci 32:71–77. https://doi.org/10.1016/J.TIBS.2006.12.008
Howe V, Sharpe LJ, Prabhu A, v., Brown AJ, (2017) New insights into cellular cholesterol acquisition: promoter analysis of human HMGCR and SQLE, two key control enzymes in cholesterol synthesis. Biochim Biophys Acta 1862:647–657. https://doi.org/10.1016/J.BBALIP.2017.03.009
Hua X, Yokoyama C, Wu J et al (1993) SREBP-2, a second basic-helix-loop-helix-leucine zipper protein that stimulates transcription by binding to a sterol regulatory element. PNAS 90:11603–11607. https://doi.org/10.1073/pnas.90.24.11603
Hua X, Wu J, Goldstein JL et al (1995) Structure of the human gene encoding sterol regulatory element binding protein-1 (SREBF1) and localization of SREBF1 and SREBF2 to chromosomes 17p11.2 and 22q13. Genomics 25:667–673. https://doi.org/10.1016/0888-7543(95)80009-B
Huff MW, Daugherty A, Lu H (2016) Atherosclerosis. Biochemistry of Lipids, Lipoproteins and Membranes: Sixth Edition 519–548. https://doi.org/10.1016/B978-0-444-63438-2.00018-3
Hukkanen J, Hakkola J (2020) PXR and 4β-Hydroxycholesterol Axis and the Components of Metabolic Syndrome. Cells 9:1–13. https://doi.org/10.3390/cells9112445
Hyun JJ, Lee HS, Kim KS et al (2008) Sterol-dependent regulation of proprotein convertase subtilisin/kexin type 9 expression by sterol-regulatory element binding protein-2. J Lipid Res 49:399–409. https://doi.org/10.1194/jlr.M700443-JLR200
Iritani N, Fukuda H, Matsumura Y (1993) Lipogenic enzyme gene expression in rat liver during development after birth. J Biochem 113:519–525. https://doi.org/10.1093/oxfordjournals.jbchem.a124076
Jia L, Betters JL, Yu L (2011) Niemann-pick C1-like 1 (NPC1L1) protein in intestinal and hepatic cholesterol transport. Annu Rev Physiol 73:239–259. https://doi.org/10.1146/annurev-physiol-012110-142233
Jiang Y, Yao X, Fan S et al (2021) Lipidomic profiling reveals triacylglycerol accumulation in the liver during pregnane X receptor activation-induced hepatomegaly. J Pharm Biomed Anal 195:113851. https://doi.org/10.1016/J.JPBA.2020.113851
Jones SA, Moore LB, Shenk JL et al (2000) The pregnane X receptor: a promiscuous xenobiotic receptor that has diverged during evolution. J Mol Endocrinol 14:27–39. https://doi.org/10.1210/MEND.14.1.0409
Karpale M, Käräjämäki AJ, Kummu O et al (2021) Activation of pregnane X receptor induces atherogenic lipids and PCSK9 by a SREBP2-mediated mechanism. Br J Pharmacol 178:2461–2481. https://doi.org/10.1111/bph.15433
Karpale M, Hukkanen J, Hakkola J (2022) Nuclear receptor PXR in drug-induced hypercholesterolemia. Cells 11:313. https://doi.org/10.3390/2Fcells11030313
Kliewer SA, Moore JT, Wade L et al (1998) An orphan nuclear receptor activated by pregnanes defines a novel steroid signaling pathway. Cell 92:73–82. https://doi.org/10.1016/S0092-8674(00)80900-9
Knebel C, Buhrke T, Süssmuth R et al (2019) Pregnane X receptor mediates steatotic effects of propiconazole and tebuconazole in human liver cell lines. Arch Toxicol 93:1311–1322. https://doi.org/10.1007/s00204-019-02445-2
König B, Koch A, Spielmann J et al (2007) Activation of PPARα lowers synthesis and concentration of cholesterol by reduction of nuclear SREBP-2. Biochem Pharmacol 73:574–585. https://doi.org/10.1016/J.BCP.2006.10.027
Lagace TA (2014) PCSK9 and LDLR degradation: regulatory mechanisms in circulation and in cells. Curr Opin Lipidol 25:387. https://doi.org/10.1097/MOL.0000000000000114
Lalanne F, Lambert G, Amar MJA et al (2005) Wild-type PCSK9 inhibits LDL clearance but does not affect apoB-containing lipoprotein production in mouse and cultured cells. J Lipid Res 46:1312–1319. https://doi.org/10.1194/jlr.M400396-JLR200
Lamba V, Yasuda K, Lamba JK et al (2004) PXR (NR1I2): splice variants in human tissues, including brain, and identification of neurosteroids and nicotine as PXR activators. Toxicol Appl Pharmacol 199:251–265. https://doi.org/10.1016/J.TAAP.2003.12.027
Lambert G, Jarnoux AL, Pineau T et al (2006) Fasting induces hyperlipidemia in mice overexpressing proprotein convertase subtilisin kexin type 9: lack of modulation of very-low-density lipoprotein hepatic output by the low-density lipoprotein receptor. Endocrinology 147:4985–4995. https://doi.org/10.1210/EN.2006-0098
Lambert G, Ancellin N, Charlton F et al (2008) Plasma PCSK9 concentrations correlate with LDL and total cholesterol in diabetic patients and are decreased by fenofibrate treatment. Clin Chem 54:1038–1045. https://doi.org/10.1373/CLINCHEM.2007.099747
Lehmann JM, McKee DD, Watson MA et al (1998) The human orphan nuclear receptor PXR is activated by compounds that regulate CYP3A4 gene expression and cause drug interactions. J Clin Invest 102:1016–1023. https://doi.org/10.1172/JCI3703
Lemaire G, Mnif W, Pascussi J et al (2006) Identification of new human Pregnane X receptor ligands among pesticides using a stable reporter cell system. Toxicol Sci 91:501–509. https://doi.org/10.1093/toxsci/kfj173
Li H, Dong B, Park SW et al (2009) Hepatocyte nuclear factor 1α plays a critical role in PCSK9 gene transcription and regulation by the natural hypocholesterolemic compound berberine. J Biol Chem 284:28885–28895. https://doi.org/10.1074/JBC.M109.052407
Lou H, Le F, Zheng Y et al (2014) Assisted reproductive technologies impair the expression and methylation of insulin-induced gene 1 and sterol regulatory element-binding factor 1 in the fetus and placenta. Fertil Steril 101:974–980. https://doi.org/10.1016/J.FERTNSTERT.2013.12.034
Lu YF, Jin T, Xu Y et al (2013) Sex differences in the circadian variation of cytochrome P450 genes and corresponding nuclear receptors in mouse liver. Chronobiol Int 30:1135. https://doi.org/10.3109/07420528.2013.805762
Luo J, Yang H, Song BL (2019) Mechanisms and regulation of cholesterol homeostasis. Nat Rev Mol Cell Biol 21:225–245. https://doi.org/10.1038/s41580-019-0190-7
Maxwell KN, Soccio RE, Duncan EM et al (2003) Novel putative SREBP and LXR target genes identified by microarray analysis in liver of cholesterol-fed mice. J Lipid Res 44:2109–2119. https://doi.org/10.1194/jlr.M300203-JLR200
McFarlane MR, Liang G, Engelking LJ (2014) Insig proteins mediate feedback inhibition of cholesterol synthesis in the intestine. J Biol Chem 289:2148–2156. https://doi.org/10.1074/JBC.M113.524041
Meng Z, Gwag T, Sui Y et al (2019) The atypical antipsychotic quetiapine induces hyperlipidemia by activating intestinal PXR signaling. JCI Insight 4:e125657. https://doi.org/10.1172/jci.insight.125657
Miserez AR, Cao G, Probst LC, Hobbs HH (1997) Structure of the human gene encoding sterol regulatory element binding protein 2 (SREBF2). Genomics 40:31–40. https://doi.org/10.1006/geno.1996.4525
Moore LB, Maglich JM, McKee DD et al (2002) Pregnane X receptor (PXR), constitutive androstane receptor (CAR), and benzoate X receptor (BXR) define three pharmacologically distinct classes of nuclear receptors. Mol Endocrinol 16:977–986. https://doi.org/10.1210/mend.16.5.0828
Nagai M, Sakakibara J, Wakui K et al (1997) Localization of the squalene epoxidase gene (SQLE) to human chromosome region 8q24.1. Genomics 44:141–143. https://doi.org/10.1006/GENO.1997.4825
Nagashima S, Yagyu H, Ohashi K et al (2012) Liver-specific deletion of 3-hydroxy-3-methylglutaryl coenzyme a reductase causes hepatic steatosis and death. Arterioscler Thromb Vasc Biol 32:1824–1831. https://doi.org/10.1161/ATVBAHA.111.240754
OECD (2018) Users’ handbook supplement to the guidance document for developing and assessing adverse outcome pathways. OECD Series on Adverse Outcome Pathways. No. 1 OECD Publishing, Paris. https://doi.org/10.1787/2415170X (Accessed 29 Nov 2022)
Ouyang S, Mo Z, Sun S et al (2020) Emerging role of Insig-1 in lipid metabolism and lipid disorders. Clin Chim Acta 508:206–212. https://doi.org/10.1016/J.CCA.2020.05.042
Peng Y, Schwarz EJ, Lazar MA et al (1997) Cloning, human chromosomal assignment, and adipose and hepatic expression of the CL-6/INSIG1 gene. Genomics 43:278–284. https://doi.org/10.1006/GENO.1997.4821
Poirier S, Mayer G, Benjannet S et al (2008) The proprotein convertase PCSK9 induces the degradation of low density lipoprotein receptor (LDLR) and its closest family members VLDLR and ApoER2. J Biol Chem 283:2363–2372. https://doi.org/10.1074/jbc.M708098200
Radhakrishnan A, Goldstein JL, McDonald JG, Brown MS (2008) Switch-like control of SREBP-2 transport triggered by small changes in ER cholesterol: a delicate balance. Cell Metab 8:512–521. https://doi.org/10.1016/J.CMET.2008.10.008
Rashid S, Curtis DE, Garuti R et al (2005) Decreased plasma cholesterol and hypersensitivity to statins in mice lacking Pcsk9. PNAS 102:5374–5379. https://doi.org/10.1073/pnas.0501652102
Roth A, Looser R, Kaufmann M et al (2008) Regulatory cross-talk between drug metabolism and lipid homeostasis: Constitutive androstane receptor and pregnane X receptor increase Insig-1 expression. Mol Pharmacol 73:1282–1289. https://doi.org/10.1124/mol.107.041012
Seidah NG (2013) Proprotein convertase subtilisin kexin 9 (PCSK9) inhibitors in the treatment of hypercholesterolemia and other pathologies. Curr Pharm Des 19:3161–3172. https://doi.org/10.2174/13816128113199990313
Seidah NG, Benjannet S, Wickham L et al (2003) The secretory proprotein convertase neural apoptosis-regulated convertase 1 (NARC-1): Liver regeneration and neuronal differentiation. PNAS 100:928–933. https://doi.org/10.1073/pnas.0335507100
Seidah NG, Awan Z, Chrétien M, Mbikay M (2014) PCSK9: A key modulator of cardiovascular health. Circ Res 114:1022–1036. https://doi.org/10.1161/CIRCRESAHA.114.301621
Sever N, Yang T, Brown MS et al (2003) Accelerated Degradation of HMG CoA Reductase Mediated by Binding of Insig-1 to Its Sterol-Sensing Domain. Mol Cell 11:25–33. https://doi.org/10.1016/s1097-2765(02)00822-5
Sharpe LJ, Brown AJ (2013) Controlling cholesterol synthesis beyond 3-hydroxy-3-methylglutaryl-CoA reductase (HMGCR). J Biol Chem 288:18707–18715. https://doi.org/10.1074/jbc.R113.479808
Shimano H, Sato R (2017) SREBP-regulated lipid metabolism: convergent physiology-divergent pathophysiology. Nat Rev Endocrinol 13:710–730. https://doi.org/10.1038/nrendo.2017.91
Shimano H, Shimomura I, Hammer RE et al (1997) Elevated levels of SREBP-2 and cholesterol synthesis in livers of mice homozygous for a targeted disruption of the SREBP-1 gene. J Clin Invest 100:2115–2124. https://doi.org/10.1172/JCI119746
Shimomura I, Shimano H, Horton JD et al (1997) Differential expression of exons 1a and 1c in mRNAs for sterol regulatory element binding protein-1 in human and mouse organs and cultured cells. J Clin Invest 99:838–845. https://doi.org/10.1172/JCI119247
Sirtori CR (2014) The pharmacology of statins. Pharmacol Res 88:3–11. https://doi.org/10.1016/J.PHRS.2014.03.002
Spady DK, Turley SD, Dietschy JM (1985) Rates of low density lipoprotein uptake and cholesterol synthesis are regulated independently in the liver. J Lipid Res 26:465–472. https://doi.org/10.1016/S0022-2275(20)34361-3
Sui Y, Helsley RN, Park SH et al (2015) Intestinal pregnane X receptor links xenobiotic exposure and hypercholesterolemia. Mol Endocrinol 29:765–776. https://doi.org/10.1210/me.2014-1355
Sui Y, Meng Z, Jianzhong Chen J et al (2021) Effects of dicyclohexyl phthalate exposure on PXR activation and lipid homeostasis in mice. Environ Health Perspect 129:127001. https://doi.org/10.1289/EHP9262Sun
Sun LP, Seemann J, Goldstein JL, Brown MS (2007) Sterol-regulated transport of SREBPs from endoplasmic reticulum to Golgi: Insig renders sorting signal in Scap inaccessible to COPII proteins. PNAS 104:6519–6526. https://doi.org/10.1073/pnas.0700907104
Svingen T, Villeneuve DL, Knapen D et al (2021) A pragmatic approach to adverse outcome pathway development and evaluation. Toxicol Sci 184:183–190. https://doi.org/10.1093/toxsci/kfab113
Tremblay AJ, Lamarche B, Lemelin V et al (2011) Atorvastatin increases intestinal expression of NPC1L1 in hyperlipidemic men. J Lipid Res 52:558–565. https://doi.org/10.1194/jlr.M011080
Uhlén M, Fagerberg L, Hallström BM et al (2015) Tissue-based map of the human proteome. Science. https://doi.org/10.1126/science.1260419
Villeneuve DL, Crump D, Garcia-Reyero N et al (2014) Adverse outcome pathway (AOP) development I: Strategies and principles. Toxicol Sci 142:312–320. https://doi.org/10.1093/toxsci/kfu199
Wolbold R, Klein K, Burk O et al (2003) Sex is a major determinant of CYP3A4 expression in human liver. Hepatology 38:978–988. https://doi.org/10.1002/HEP.1840380424
Wu N, Sarna LK, Hwang SY et al (2013) Activation of 3-hydroxy-3-methylglutaryl coenzyme A (HMG-CoA) reductase during high fat diet feeding. Biochim Biophys Acta 1832:1560–1568. https://doi.org/10.1016/J.BBADIS.2013.04.024
Xiang E, Guo Q, Yong- Guo D et al (2020) Female-specific activation of pregnane X receptor mediates sex difference in fetal hepatotoxicity by prenatal monocrotaline exposure. Toxicol Appl Pharmacol 406:115137. https://doi.org/10.1016/J.TAAP.2020.115137
Xue L, Qi H, Zhang H et al (2020) Targeting SREBP-2-Regulated Mevalonate Metabolism for Cancer Therapy. Front Oncol 10:1510. https://doi.org/10.3389/FONC.2020.01510
Yabe D, Brown MS, Goldstein JL (2002) Insig-2, a second endoplasmic reticulum protein that binds SCAP and blocks export of sterol regulatory element-binding proteins. PNAS 99:12753. https://doi.org/10.1073/PNAS.162488899
Yang T, Espenshade PJ, Wright ME et al (2002) Crucial step in cholesterol homeostasis: sterols promote binding of SCAP to INSIG-1, a membrane protein that facilitates retention of SREBPs in ER. Cell 110:489–500. https://doi.org/10.1016/S0092-8674(02)00872-3
Zhang Y, Gao Y, Yang J et al (2022) Long-term treatment with the mPXR agonist PCN promotes hepatomegaly and lipid accumulation without hepatocyte proliferation in mice. Acta Pharmacol Sin 44:169–177. https://doi.org/10.1038/s41401-022-00925-3
Zhou C, King N, Chen KY, Breslow JL (2009a) Activation of PXR induces hypercholesterolemia in wild-type and accelerates atherosclerosis in apoE deficient mice. J Lipid Res 50:2004–2013. https://doi.org/10.1194/jlr.M800608-JLR200
Zhou C, Verma S, Blumberg B (2009) The steroid and xenobiotic receptor (SXR), beyond xenobiotic metabolism. Nucl Recept Signal. https://doi.org/10.1621/nrs.07001
Ziegler T, Rahman FA, Jurisch V, Kupatt C (2020) Atherosclerosis and the capillary network; pathophysiology and potential therapeutic strategies. Cells 9:1–13. https://doi.org/10.3390/cells9010050
Funding
Open access funding provided by University of Eastern Finland (UEF) including Kuopio University Hospital. This project has received funding from the European Union’s Horizon 2020 research and innovation programme under grant agreement No 825762. The research work of Jukka Hakkola was also supported by a grant from the Academy of Finland (323706).
Author information
Authors and Affiliations
Contributions
Conceptualization: all authors; writing–original draft preparation: AI; visualization: AI; writing–review & editing: all authors.
Corresponding author
Ethics declarations
Conflict of interest
The authors declare that they have no conflict of interest.
Ethical approval
The manuscript does not contain experimental work, clinical studies, or patient data.
Additional information
Publisher's Note
Springer Nature remains neutral with regard to jurisdictional claims in published maps and institutional affiliations.
Rights and permissions
Open Access This article is licensed under a Creative Commons Attribution 4.0 International License, which permits use, sharing, adaptation, distribution and reproduction in any medium or format, as long as you give appropriate credit to the original author(s) and the source, provide a link to the Creative Commons licence, and indicate if changes were made. The images or other third party material in this article are included in the article's Creative Commons licence, unless indicated otherwise in a credit line to the material. If material is not included in the article's Creative Commons licence and your intended use is not permitted by statutory regulation or exceeds the permitted use, you will need to obtain permission directly from the copyright holder. To view a copy of this licence, visit http://creativecommons.org/licenses/by/4.0/.
About this article
Cite this article
Itkonen, A., Hakkola, J. & Rysä, J. Adverse outcome pathway for pregnane X receptor-induced hypercholesterolemia. Arch Toxicol 97, 2861–2877 (2023). https://doi.org/10.1007/s00204-023-03575-4
Received:
Accepted:
Published:
Issue Date:
DOI: https://doi.org/10.1007/s00204-023-03575-4