Abstract
Although liver transplantation is a potential effective cure for patients with end-stage liver diseases, this strategy has several drawbacks including high cost, long waiting list, and limited availability of liver organs. Therefore, stem cell-based therapy is presented as an alternative option, which showed promising results in animal models of acute and chronic liver injuries. ABCB5+ cells isolated from skin dermis represent an easy accessible and expandable source of homogenous stem cell populations. In addition, ABCB5+ cells showed already promising results in the treatment of corneal and skin injury. To date, the effect of these cells on liver injury is still unknown. In the current study, sixteen weeks old Mdr2KO mice were i.v. injected with 500,000 ABCB5+ cells using different experimental setups. The effects of cellular therapy on inflammation, fibrosis, apoptosis, and proliferation were analyzed in the collected liver tissues. Toxicity of ABCB5+ cells was additionally investigated in mice with partial liver resection. In vitro, the fibrosis- and inflammatory-modulating effects of supernatant from ABCB5+ cells were examined in the human hepatic stellate cell line (LX-2). Cell injections into fibrotic Mdr2KO mice as well as into mice upon partial liver resection have no signs of toxicity with regard to cell transformation, cellular damage, fibrosis or inflammation as compared to controls. We next investigated the effects of ABCB5+ cells on established biliary liver fibrosis in the Mdr2KO mice. ABCB5+ cells to some extent influenced the shape of the liver inflammatory response and significantly reduced the amount of collagen deposition, as estimated from quantification of sirius red staining. Furthermore, reduced apoptosis and enhanced death compensatory proliferation resulted from ABCB5+ cell transformation. The stem cells secreted several trophic factors that activated TGF-β family signaling in cultured LX-2 hepatic stellate cells (HSCs), therewith shaping cell fate to an αSMAhigh, Vimentinlow phenotype. Taken together, ABCB5+ cells can represent a safe and feasible strategy to support liver regeneration and to reduce liver fibrosis in chronic liver diseases.





Similar content being viewed by others
Change history
29 October 2019
We wish to submit a corrigendum to the above-mentioned article. Thank you very much for consideration and publication.
Abbreviations
- ABCB5:
-
ATP-binding cassette sub-family B, member 5 (ABCB5) P-glycoprotein
- ACLF:
-
Acute-on-chronic liver failure
- ALT:
-
Alanine aminotransferase
- AP:
-
Alkaline phosphatase
- AST:
-
Aspartate aminotransferase
- BDL:
-
Bile duct ligation
- CCl4 :
-
Carbon tetrachloride
- EVs:
-
Extracellular vesicles
- GLDH:
-
Glutamate dehydrogenase
- HCC:
-
Hepatocellular carcinoma
- HCV:
-
Hepatitis C virus
- HSCs:
-
Hepatic stellate cells
- IL-1RA:
-
Interleukin-1 receptor antagonist
- INF:
-
Interferon
- LPS:
-
Lipopolysaccharide
- LSC:
-
Limbal stem cells
- MACS:
-
Magnetic activated cell sorting
- Mdr2:
-
Multidrug resistance gene 2
- MHC:
-
Major histocompatibility complex
- MSCs:
-
Mesenchymal stromal cells
- PD-1:
-
Programmed death1
- PHH:
-
Primary hepatocytes
- PMA:
-
Phorbol 12-myristate 13-acetate
- PSC:
-
Primary sclerosing cholangitis
- RDEB:
-
Recessive dystrophic epidermolysis bullosa
- TG:
-
Triglycerides
- TIMP1:
-
Tissue inhibitor of metalloproteinases 1
- TGF:
-
Tumor growth factor
- VEGF:
-
Vascular endothelial growth factor
References
Abe T, Arai T, Ogawa A et al (2004) Kupffer cell-derived interleukin 10 is responsible for impaired bacterial clearance in bile duct-ligated mice. Hepatology 40:414–423. https://doi.org/10.1002/hep.20301
Abshagen K, König M, Hoppe A et al (2015) Pathobiochemical signatures of cholestatic liver disease in bile duct ligated mice. BMC Syst Biol 9:83. https://doi.org/10.1186/s12918-015-0229-0
Alhomrani M, Correia J, Zavou M et al (2017) The human amnion epithelial cell secretome decreases hepatic fibrosis in mice with chronic liver fibrosis. Front Pharmacol 8:748. https://doi.org/10.3389/fphar.2017.00748
Alwahsh SM, Rashidi H, Hay DC (2018) Liver cell therapy: is this the end of the beginning? Cell Mol Life Sci 75:1307–1324. https://doi.org/10.1007/s00018-017-2713-8
Baccarani U, Adani GL, Sainz M et al (2005) Human hepatocyte transplantation for acute liver failure: state of the art and analysis of cell sources. Transplant Proc 37:2702–2704. https://doi.org/10.1016/j.transproceed.2005.06.027
Boigk G, Stroedter L, Herbst H et al (1997) Silymarin retards collagen accumulation in early and advanced biliary fibrosis secondary to complete bile duct obliteration in rats. Hepatology 26:643–649. https://doi.org/10.1002/hep.510260316
Chen B, Ni Y, Liu J et al (2018) Bone marrow-derived mesenchymal stem cells exert diverse effects on different macrophage subsets. Stem Cells Int 2018:8348121. https://doi.org/10.1155/2018/8348121
Dhawan A, Puppi J, Hughes RD, Mitry RR (2010) Human hepatocyte transplantation: current experience and future challenges. Nat Rev Gastroenterol Hepatol 7:288–298. https://doi.org/10.1038/nrgastro.2010.44
Duffield JS, Forbes SJ, Constandinou CM et al (2005) Selective depletion of macrophages reveals distinct, opposing roles during liver injury and repair. J Clin Invest 115:56–65. https://doi.org/10.1172/JCI22675
El-Emshaty HM, Nasif WA, Mohamed IE (2015) Serum cytokine of IL-10 and IL-12 in chronic liver disease: the immune and inflammatory response. Dis Markers 2015:707254. https://doi.org/10.1155/2015/707254
Eom YW, Shim KY, Baik SK (2015) Mesenchymal stem cell therapy for liver fibrosis. Korean J Intern Med 30:580–589. https://doi.org/10.3904/kjim.2015.30.5.580
European Association for the Study of the Liver. Electronic address: easloffice@easloffice.eu (2016) EASL Clinical Practice Guidelines: liver transplantation. J Hepatol 64:433–485. https://doi.org/10.1016/j.jhep.2015.10.006
Fabriek BO, Dijkstra CD, van den Berg TK (2005) The macrophage scavenger receptor CD163. Immunobiology 210:153–160. https://doi.org/10.1016/j.imbio.2005.05.010
Frank NY, Pendse SS, Lapchak PH et al (2003) Regulation of progenitor cell fusion by ABCB5 P-glycoprotein, a novel human ATP-binding cassette transporter. J Biol Chem 278:47156–47165. https://doi.org/10.1074/jbc.M308700200
Gieling RG, Wallace K, Han Y-P (2009) Interleukin-1 participates in the progression from liver injury to fibrosis. Am J Physiol Gastrointest Liver Physiol 296:G1324–G1331. https://doi.org/10.1152/ajpgi.90564.2008
Gonzalez G, Sasamoto Y, Ksander BR et al (2018) Limbal stem cells: identity, developmental origin, and therapeutic potential. Wiley Interdiscip Rev Dev Biol 7:e303. https://doi.org/10.1002/wdev.303
Guicciardi ME, Trussoni CE, Krishnan A et al (2018) Macrophages contribute to the pathogenesis of sclerosing cholangitis in mice. J Hepatol 69:676–686. https://doi.org/10.1016/j.jhep.2018.05.018
Haga H, Yan IK, Takahashi K et al (2017) Extracellular vesicles from bone marrow-derived mesenchymal stem cells improve survival from lethal hepatic failure in mice. Stem Cells Transl Med 6:1262–1272. https://doi.org/10.1002/sctm.16-0226
Hammad S, Cavalcanti E, Werle J et al (2018) Galunisertib modifies the liver fibrotic composition in the Abcb4Ko mouse model. Arch Toxicol 92:2297–2309. https://doi.org/10.1007/s00204-018-2231-y
Hirasaki S, Koide N, Ujike K et al (2001) Expression of Nov, CYR61 and CTGF genes in human hepatocellular carcinoma. Hepatol Res 19:294–305
Hodge A, Lourensz D, Vaghjiani V et al (2014) Soluble factors derived from human amniotic epithelial cells suppress collagen production in human hepatic stellate cells. Cytotherapy 16:1132–1144. https://doi.org/10.1016/j.jcyt.2014.01.005
Ikenaga N, Liu SB, Sverdlov DY et al (2015) A new Mdr2(-/-) mouse model of sclerosing cholangitis with rapid fibrosis progression, early-onset portal hypertension, and liver cancer. Am J Pathol 185:325–334. https://doi.org/10.1016/j.ajpath.2014.10.013
Imaeda AB, Watanabe A, Sohail MA et al (2009) Acetaminophen-induced hepatotoxicity in mice is dependent on Tlr9 and the Nalp3 inflammasome. J Clin Invest 119:305–314. https://doi.org/10.1172/JCI35958
Jamall IS, Finelli VN, Hee SQ (1981) A simple method to determine nanogram levels of 4-hydroxyproline in biological tissues. Anal Biochem 112:70–75
Jiang D, Muschhammer J, Qi Y et al (2016) Suppression of neutrophil-mediated tissue damage—a novel skill of mesenchymal stem cells. Stem Cells 34:2393–2406. https://doi.org/10.1002/stem.2417
Junqueira LC, Bignolas G, Brentani RR (1979) Picrosirius staining plus polarization microscopy, a specific method for collagen detection in tissue sections. Histochem J 11:447–455
Katzenellenbogen M, Pappo O, Barash H et al (2006) Multiple adaptive mechanisms to chronic liver disease revealed at early stages of liver carcinogenesis in the Mdr2-knockout mice. Cancer Res 66:4001–4010. https://doi.org/10.1158/0008-5472.CAN-05-2937
Kleffel S, Lee N, Lezcano C et al (2016) ABCB5-targeted chemoresistance reversal inhibits merkel cell carcinoma growth. J Invest Dermatol 136:838–846. https://doi.org/10.1016/j.jid.2015.12.038
Krenkel O, Tacke F (2017) Liver macrophages in tissue homeostasis and disease. Nat Rev Immunol 17:306–321. https://doi.org/10.1038/nri.2017.11
Ksander BR, Kolovou PE, Wilson BJ et al (2014) ABCB5 is a limbal stem cell gene required for corneal development and repair. Nature 511:353–357. https://doi.org/10.1038/nature13426
Lammert F, Wang DQ-H, Hillebrandt S et al (2004) Spontaneous cholecysto- and hepatolithiasis in Mdr2-/- mice: a model for low phospholipid-associated cholelithiasis. Hepatology 39:117–128. https://doi.org/10.1002/hep.20022
Lee C-W, Chen Y-F, Wu H-H, Lee OK (2018) Historical perspectives and advances in mesenchymal stem cell research for the treatment of liver diseases. Gastroenterology 154:46–56. https://doi.org/10.1053/j.gastro.2017.09.049
Liedtke C, Luedde T, Sauerbruch T et al (2013) Experimental liver fibrosis research: update on animal models, legal issues and translational aspects. Fibrogenes Tissue Repair 6:19. https://doi.org/10.1186/1755-1536-6-19
Lin B-L, Chen J-F, Qiu W-H et al (2017) Allogeneic bone marrow-derived mesenchymal stromal cells for hepatitis B virus-related acute-on-chronic liver failure: a randomized controlled trial. Hepatology 66:209–219. https://doi.org/10.1002/hep.29189
Livak KJ, Schmittgen TD (2001) Analysis of relative gene expression data using real-time quantitative PCR and the 2(−ΔΔC(T)) Method. Methods 25:402–408. https://doi.org/10.1006/meth.2001.1262
Ma Y, Yang M, He Z et al (2017) The biological function of kupffer cells in liver disease. Biol Myelomonocytic Cells. https://doi.org/10.5772/67673
Mahmood T, Yang P-C (2012) Western blot: technique, theory, and trouble shooting. N Am J Med Sci 4:429–434. https://doi.org/10.4103/1947-2714.100998
Margini C, Vukotic R, Brodosi L et al (2014) Bone marrow derived stem cells for the treatment of end-stage liver disease. World J Gastroenterol 20:9098–9105. https://doi.org/10.3748/wjg.v20.i27.9098
Mauad TH, van Nieuwkerk CM, Dingemans KP et al (1994) Mice with homozygous disruption of the mdr2 P-glycoprotein gene. A novel animal model for studies of nonsuppurative inflammatory cholangitis and hepatocarcinogenesis. Am J Pathol 145:1237–1245
Meier RPH, Müller YD, Morel P et al (2013) Transplantation of mesenchymal stem cells for the treatment of liver diseases, is there enough evidence? Stem Cell Res 11:1348–1364. https://doi.org/10.1016/j.scr.2013.08.011
Meier RPH, Mahou R, Morel P et al (2015) Microencapsulated human mesenchymal stem cells decrease liver fibrosis in mice. J Hepatol 62:634–641. https://doi.org/10.1016/j.jhep.2014.10.030
Meyburg J, Das AM, Hoerster F et al (2009) One liver for four children: first clinical series of liver cell transplantation for severe neonatal urea cycle defects. Transplantation 87:636–641. https://doi.org/10.1097/TP.0b013e318199936a
Miura K, Kodama Y, Inokuchi S et al (2010) Toll-like receptor 9 promotes steatohepatitis by induction of interleukin-1beta in mice. Gastroenterology 139:323–334.e7. https://doi.org/10.1053/j.gastro.2010.03.052
Murphy AG, Selaru FM (2018) Extracellular vesicles as novel therapeutics in hepatic failure. Hepatology 67:1158–1160. https://doi.org/10.1002/hep.29576
Norozi F, Ahmadzadeh A, Shahrabi S et al (2016) Mesenchymal stem cells as a double-edged sword in suppression or progression of solid tumor cells. Tumour Biol 37:11679–11689. https://doi.org/10.1007/s13277-016-5187-7
Pellicoro A, Ramachandran P, Iredale JP, Fallowfield JA (2014) Liver fibrosis and repair: immune regulation of wound healing in a solid organ. Nat Rev Immunol 14:181–194. https://doi.org/10.1038/nri3623
Petrasek J, Bala S, Csak T et al (2012) IL-1 receptor antagonist ameliorates inflammasome-dependent alcoholic steatohepatitis in mice. J Clin Invest 122:3476–3489. https://doi.org/10.1172/JCI60777
Pikarsky E, Porat RM, Stein I et al (2004) NF-kappaB functions as a tumour promoter in inflammation-associated cancer. Nature 431:461–466. https://doi.org/10.1038/nature02924
Popov Y, Patsenker E, Fickert P et al (2005) Mdr2 (Abcb4)-/- mice spontaneously develop severe biliary fibrosis via massive dysregulation of pro- and antifibrogenic genes. J Hepatol 43:1045–1054. https://doi.org/10.1016/j.jhep.2005.06.025
Puchtler H, Waldrop FS, Valentine LS (1973) Polarization microscopic studies of connective tissue stained with picro-sirius red FBA. Beitr Pathol 150:174–187
Rachfal AW, Brigstock DR (2003) Connective tissue growth factor (CTGF/CCN2) in hepatic fibrosis. Hepatol Res 26:1–9
Reiter FP, Wimmer R, Wottke L et al (2016) Role of interleukin-1 and its antagonism of hepatic stellate cell proliferation and liver fibrosis in the Abcb4-/- mouse model. World J Hepatol 8:401–410. https://doi.org/10.4254/wjh.v8.i8.401
Ridge SM, Sullivan FJ, Glynn SA (2017) Mesenchymal stem cells: key players in cancer progression. Mol Cancer 16:31. https://doi.org/10.1186/s12943-017-0597-8
Roth KJ, Copple BL (2015) Role of hypoxia-inducible factors in the development of liver fibrosis. Cell Mol Gastroenterol Hepatol 1:589–597. https://doi.org/10.1016/j.jcmgh.2015.09.005
Russo FP, Alison MR, Bigger BW et al (2006) The bone marrow functionally contributes to liver fibrosis. Gastroenterology 130:1807–1821. https://doi.org/10.1053/j.gastro.2006.01.036
Schatton T, Yang J, Kleffel S et al (2015) ABCB5 identifies immunoregulatory dermal cells. Cell Rep 12:1564–1574. https://doi.org/10.1016/j.celrep.2015.08.010
Schuppan D, Afdhal NH (2008) Liver cirrhosis. Lancet 371:838–851. https://doi.org/10.1016/S0140-6736(08)60383-9
Sedlaczek N, Jia JD, Bauer M et al (2001) Proliferating bile duct epithelial cells are a major source of connective tissue growth factor in rat biliary fibrosis. Am J Pathol 158:1239–1244. https://doi.org/10.1016/S0002-9440(10)64074-6
Shen Z, Liu Y, Dewidar B et al (2016) Delta-like ligand 4 modulates liver damage by down-regulating chemokine expression. Am J Pathol 186:1874–1889. https://doi.org/10.1016/j.ajpath.2016.03.010
Song ATW, Avelino-Silva VI, Pecora RAA et al (2014) Liver transplantation: fifty years of experience. World J Gastroenterol 20:5363–5374. https://doi.org/10.3748/wjg.v20.i18.5363
Stock P, Brückner S, Ebensing S et al (2010) The generation of hepatocytes from mesenchymal stem cells and engraftment into murine liver. Nat Protoc 5:617–627. https://doi.org/10.1038/nprot.2010.7
Suk KT, Yoon J-H, Kim MY et al (2016) Transplantation with autologous bone marrow-derived mesenchymal stem cells for alcoholic cirrhosis: phase 2 trial. Hepatology 64:2185–2197. https://doi.org/10.1002/hep.28693
Tappenbeck N, Schröder HM, Niebergall-Roth E et al (2019) In vivo safety profile and biodistribution of GMP-manufactured human skin-derived ABCB5-positive mesenchymal stromal cells for use in clinical trials. Cytotherapy. https://doi.org/10.1016/j.jcyt.2018.12.005
Tietze L, Winkler S, Hempel M et al (2018) Assessment of the hepatocytic differentiation ability of human skin-derived ABCB5+ stem cells. Exp Cell Res 369:335–347. https://doi.org/10.1016/j.yexcr.2018.05.040
Tsutsui H, Cai X, Hayashi S (2015) Interleukin-1 family cytokines in liver diseases. Mediat Inflamm 2015:630265. https://doi.org/10.1155/2015/630265
Ujike K, Shinji T, Hirasaki S et al (2000) Kinetics of expression of connective tissue growth factor gene during liver regeneration after partial hepatectomy and D-galactosamine-induced liver injury in rats. Biochem Biophys Res Commun 277:448–454. https://doi.org/10.1006/bbrc.2000.3693
Vaahtomeri K, Ventelä E, Laajanen K et al (2008) Lkb1 is required for TGFbeta-mediated myofibroblast differentiation. J Cell Sci 121:3531–3540. https://doi.org/10.1242/jcs.032706
Volpicelli ER, Lezcano C, Zhan Q et al (2014) The multidrug-resistance transporter ABCB5 is expressed in human placenta. Int J Gynecol Pathol 33:45–51. https://doi.org/10.1097/PGP.0b013e31829c677f
Wang Y-H, Wu D-B, Chen B et al (2018) Progress in mesenchymal stem cell–based therapy for acute liver failure. Stem Cell Res Ther 9:227. https://doi.org/10.1186/s13287-018-0972-4
Webber BR, O’Connor KT, McElmurry RT et al (2017) Rapid generation of Col7a1-/- mouse model of recessive dystrophic epidermolysis bullosa and partial rescue via immunosuppressive dermal mesenchymal stem cells. Lab Invest 97:1218–1224. https://doi.org/10.1038/labinvest.2017.85
Wijesundera KK, Izawa T, Murakami H et al (2014) M1- and M2-macrophage polarization in thioacetamide (TAA)-induced rat liver lesions; a possible analysis for hepato-pathology. Histol Histopathol 29:497–511. https://doi.org/10.14670/HH-29.10.497
Wong VW, Levi B, Rajadas J et al (2012) Stem cell niches for skin regeneration. In: International journal of biomaterials. https://www.hindawi.com/journals/ijbm/2012/926059/. Accessed 19 Feb 2019
Zhang L-J, Wang X-Z (2006) Interleukin-10 and chronic liver disease. World J Gastroenterol 12:1681–1685. https://doi.org/10.3748/wjg.v12.i11.1681
Acknowledgements
Financial support for this study was provided by RHEACELL GmbH and Co. KG.
Author information
Authors and Affiliations
Contributions
Conception and design: SD, RV, AK. ABCB5+ cell isolation and preservation: TICEBA GmbH. Collecting animal model data performing experiments and analysis and interpretation of data: VH, BD, TL, AD, NT, LT, BC, SD. Collecting in vitro data, performing experiments and analyses and interpretation of data: VH, TL, BD, SD. Drafting the article: VH, BD, SD. Manuscript editing: VH, BD, NT, SD, BC. All authors read and approved the final manuscript.
Corresponding author
Ethics declarations
Conflict of interest
Vanessa Hartwig, Steven Dooley, Lysann Tietze, and Bruno Christ participate in corporate-sponsored research collaborations with RHEACELL GmbH and Co. KG. The remaining authors have no conflicting interests. Data and data presentation is uninfluenced by RHEACELL.
Ethics approval
TICEBA is holder of a manufacturing license according § 13 AMG (allogeneic mesenchymal ABCB5-positive cells, obtained from human skin) since 22.06.2017. Written informed consent was obtained from all donors before collecting skin samples. Animal experimental protocols were approved by the local council of animal care of Baden-Wuerttemberg, Germany (Permit number G254-15).
Additional information
Publisher's Note
Springer Nature remains neutral with regard to jurisdictional claims in published maps and institutional affiliations.
Electronic supplementary material
Below is the link to the electronic supplementary material.
Assessment of adverse effects of ABCB5+ cell transplantation in the PHx mouse model. Collagen fibers were visualized with the Sirius red stain (a) 2 days and 7 weeks after transplantation of ABCB5+ cells into livers of Pfp/Rag2KO mice. HRG was used as carrier control. Pictures show representative images of slices from 2 animals in each group. Scale bar – 100 µm. Using semiquantitative RT-PCR (b), the relative expression of mRNAs of TIMP1 and VEGF was determined 2 days (white columns) and 7 weeks (grey columns) after transplantation of ABCB5+ cells. (c, d) Relative expression of inflammation (c) and apoptosis (d) markers in livers of Pfp/Rag2KO mice 2 days (white columns) and 7 weeks (grey columns) after transplantation of ABCB5+cells. Values shown are means ± SD of n=4 animals in each group (* p < 0.05). Housekeeping genes β2-microglobulin and TATA-box binding protein were used for normalization of expression levels.
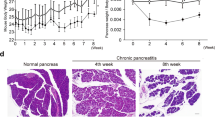
Comparison of male and female Mdr2KO mice. Quantification of Sirius red staining (a) in control mice at different ages, as indicated, and (b) after ABCB5+ cells treatment for the indicated time points; positive staining is presented as scatter plots, discriminating periportal, pericentral and mid-zonal areas, as indicated for n=4-8 for 4 weeks, n=4 for 6 days and 2 weeks time points. Black color represents saline-treated Mdr2KO mice, red color indicates ABCB5+ cell-treated Mdr2KO mice. Triangles represent nis and squares represent ABCB5+ mice with double cell treatment. Pink color represents female mice; ut, untreated; t, treated with ABCB5+ cells.
Effects of ABCB5+cells treatment on biliary fibrosis in Mdr2KO mice. Quantification of (a) αSMA and (b) SMA22α positive staining is presented as scatter plots, discriminating periportal, pericentral and mid-zonal areas, as indicated for n=4-8 for 4 weeks, n=4 for 6 days and 2 weeks time points. Representative IHC staining for SMA22α is shown in 10 and 40 fold magnification. (c) Real-time RT-PCR data for selected fibrogenesis-related gene expression, as indicated, and biochemical determination of hydroxyproline levels (HYP). Black color represents saline-treated Mdr2KO mice, red color indicates ABCB5+ cell-treated Mdr2KO mice. Triangles represent nis and squares represent ABCB5+ mice with double cell treatment.
Effects of ABCB5+cell treatment on liver inflammation in Mdr2KO mice. IHC staining of CD45 (a) is presented in 10 and 40 fold magnification. Quantification of CD45 (a) and CD163 (b) positive staining is presented as scatter plots, discriminating periportal, pericentral and mid-zonal areas, as indicated for n=4 for 6 days and 2 weeks time points. (c) Real-time RT-PCR data for selected inflammation related gene expression, as indicated. Black color represents saline-treated Mdr2KO mice, red color indicates ABCB5+ cells-treated Mdr2KO mice. Triangles represent nis and squares represent ABCB5+ mice with double cell treatment.
Effects of ABCB5+cells treatment on apoptosis and proliferation in Mdr2KO mice. (a) Representative documentation of apoptotic cells based on TUNEL assays and immunofluorescent staining (n=4) 2 and 6 days after cell treatment. (b) Quantification of Ki-67 immunostaining is presented as scatter plots, discriminating periportal, pericentral and mid-zonal areas, as indicated of n=8 for 4 weeks and n=4 for 6 days and 2 weeks time points. Black color represents saline-treated Mdr2KO mice, red color indicates ABCB5+ cell-treated Mdr2KO mice. Triangles represent nis and squares represent ABCB5+ mice with double cell treatment.
Rights and permissions
About this article
Cite this article
Hartwig, V., Dewidar, B., Lin, T. et al. Human skin-derived ABCB5+ stem cell injection improves liver disease parameters in Mdr2KO mice. Arch Toxicol 93, 2645–2660 (2019). https://doi.org/10.1007/s00204-019-02533-3
Received:
Accepted:
Published:
Issue Date:
DOI: https://doi.org/10.1007/s00204-019-02533-3