Abstract
Introduction and hypothesis
This manuscript from Chapter 3 of the International Urogynecology Consultation (IUC) on Pelvic Organ Prolapse (POP) describes the current evidence and suggests future directions for research on the effect of pelvic floor muscle training (PFMT) in prevention and treatment of POP.
Methods
An international group of four physical therapists, four urogynecologists and one midwife/basic science researcher performed a search of the literature using pre-specified search terms on randomized controlled trials (RCTs) in Ovid Medline, EMBASE, CINAHL, Cochrane, PEDro and Scopus databases for publications between 1996 and 2021. Full publications or expanded abstracts in English or in other languages with abstracts in English were included. The PEDro rating scale (0–10) was used to evaluate study quality. Included RCTs were reviewed to summarize the evidence in six key sections: (1) evidence for PFMT in prevention of POP in the general female population; (2) evidence for early intervention of PFMT in the peripartum period for prevention and treatment of POP; (3) evidence for PFMT in treatment of POP in the general female population; (4) evidence for perioperative PFMT; (5) evidence for PFMT on associated conditions in women with POP; (6) evidence for the long-term effect of PFMT on POP. Full publications in English or in other languages with abstracts in English and expanded abstracts presented at international condition specific societies were included. Internal validity was examined by the PEDro rating scale (0–10).
Results
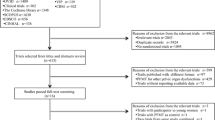
After exclusion of duplicates and irrelevant trials, we classified and included 2 preventive trials, 4 trials in the post-partum period, 11 treatment trials of PFMT for POP in the general female population in comparison with no treatment or lifestyle interventions, 10 on PFMT as an adjunct treatment to POP surgery and 9 long-term treatment trials. Only three treatment studies compared PFMT with the use of a pessary. The RCTs scored between 4 and 8 on the PEDro scale. No primary prevention studies were found, and there is sparse and inconsistent evidence for early intervention in the postpartum period. There is good evidence/recommendations from 11 RCTs that PFMT is effective in reducing POP symptoms and/or improving POP stage (by one stage) in women with POP-Q stage I, II and III in the general female population, but no evidence from 9/10 RCTs that adding PFMT pre- and post -surgery for POP is effective. There are few long-term follow-up studies, and results are inconsistent. There are no serious adverse effects or complications reported related to PFMT.
Conclusions
There are few studies on prevention and in the postpartum period, and the effect is inconclusive. There is high-level evidence from 11 RCTs to recommend PFMT as first-line treatment for POP in the general female population. PFMT pre- and post-POP surgery does not seem to have any additional effect on POP. PFMT is effective and safe but needs thorough instruction and supervision to be effective.
Similar content being viewed by others
Avoid common mistakes on your manuscript.
Introduction
This report is part of a series of articles that are the product of the International Urogynecology Consultation (IUC) sponsored by the International Urogynecological Association (IUGA). This is a 4-year, 4-chapter project with 16 reports dedicated to reviewing and summarizing the world’s literature on pelvic organ prolapse (POP). This report is from the third year and chapter of the project, which is dedicated to reviewing the literature on non-surgical management of POP. Years 1 and 2 were dedicated to defining the epidemiology of POP and the evaluation of patients with POP. The fourth or final chapter will evaluate the surgical treatment of POP. This report focuses on reviewing the literature on conservative treatment of patient with POP employing pelvic floor muscle training.
POP is a common condition in women. The reported prevalence varies widely (1–65%) based on whether its presence is ascertained by symptoms (1–31%), pelvic examination (10–50%) or both (20–65%) [1]. POP may negatively affect quality of life, participation in physical activities, body image and sexual function [2]. Multiple factors contribute to the development of primary and recurrent POP. These factors include childbirth, constipation, strenuous work and heavy lifting, congenital connective tissue weakness, obesity, menopause, chronic increased intra-abdominal pressure (IAP) and iatrogenic causes [1, 3]. Available treatments are watchful waiting, lifestyle interventions such as avoiding constipation and straining, pelvic floor muscle training (PFMT), pessaries or surgery.
POP is caused by a combination of impairment of the pelvic floor muscles (PFM) and the connective tissue [4]. The association between a decrease in levator plate angle, increase in levator hiatus area and presence of POP has been confirmed in several studies [5,6,7,8,9,10,11,12,13]. Women with POP have shown to have PFM impairment [4, 6, 8,9,10,11,12,13,14,15,16], and damage to the PFMs is three times more likely to be found in women with POP than in those without [4]. A recent systematic review by Siahkal et al. (2021) [10] summarized 21 studies in a meta-analysis and concluded that the dimensions of the levator hiatus are greater both at rest and during Valsalva maneuver in women with POP compared to women without POP. An increased levator hiatus area, measured by ultrasound, is associated with a low vaginal resting pressure, measured with manometry [17], and major tears of the PFM after vaginal birth result in a 50% reduction in muscle strength [18]. Women with Pelvic Organ Prolapse Quantification system (POP-Q) stage II or more have 40–62% reduced PFM strength [14, 19], 53% reduced PFM endurance and lower vaginal resting pressure compared to matched controls with normal supports, defined as POP-Q stage 0 and I [19]. When measuring PFM strength with manometry one longitudinal cohort study found that for every 5-cmH2O increase in pressure during maximal voluntary contraction, the odds for prolapse was reduced by 13% (OR 0.87, 95% CI 0.81, 0.94) [15].
Kegel (1952) [20] postulated that “With adequate PFMT the woman learns to maintain the perineum, bladder and uterus in a higher position, the slack in the supportive muscles will be taken up, and the vagina will become longer and tighter.” Today there is evidence for two mechanisms of how PFMT may be effective in prevention and treatment of SUI [21, 22], and the same mechanisms apply for the effect of PFMT to prevent and treat POP. The two mechanisms are:
(1) Women learn to consciously contract the PFM before and during increases in intra-abdominal pressure (IAP) (also termed ‘bracing’ or ‘performing the Knack’) and continue to perform such voluntary contractions as a behavior modification to prevent descent of the pelvic floor during these episodes.
(2) Women are taught to perform regular strength training to improve ‘firmness’ and structural support of the pelvic floor over time. These two hypotheses co-exist as they both build on an anatomical and biomechanical understanding of the function of the PFM, i.e., a voluntary contraction of the PFM constricts the levator hiatus, elevates and stabilizes the pelvic floor into a higher position. This results in an immediate effect during the PFM contraction of lifting the bladder neck and stabilizing the pelvic floor [23, 24]. This may also have an effect over time. Strength training has been shown to promote hypertrophy of targeted muscles, increasing constriction of the levator hiatus, shortening the PFM and lifting of the pelvic floor and reversing some of the changes associated with POP [25].
This narrative review summarizes the current evidence for PFMT in the treatment and prevention of POP with the following research questions:
-
1.
What is the evidence for PFMT in prevention of POP in the general female population?
-
2.
What is the evidence for early intervention of PFMT in the peripartum period for treatment of POP?
-
3.
What is the evidence for PFMT in treatment of POP in the general female population?
-
4.
What is the evidence for PFMT pre- and post POP surgery?
-
5.
What is the evidence for PFMT on associated conditions in women with POP?
-
6.
What is the evidence for long-term effect of PFMT in treatment of POP?
Methods
To complete an exhaustive literature search on this topic, the authors brainstormed search terms they felt most relevant to POP and selected the items listed below. This list of terms was presented at the IUGA annual scientific meeting in 2020 for input from the general membership. No additional terms were suggested as a result of that meeting. The search strategy included the following: Ovid Medline, EMBASE, CINAHL, Cochrane, PEDro and Scopus databases were searched for period January 1, 1996, to December 31, 2021, to identify studies. The keywords were combinations of “pelvic organ prolapse” or “urogenital prolapse” and “bulge” or “heaviness,” “exercise therapy,” “hypopressive exercise,” “kegel,” “long term,” “pelvic floor muscle training,” “pelvic floor exercise,” “peripartum,” “postpartum,” “pregnancy,” “prevention,” “symptomatic prolapse” and “treatment outcome”. Limitation was set on fully published randomized controlled trials (RCTs) or full publications with at least an English language abstract. The search also included the extended abstracts from International Continence Society (ICS) meetings. Finally, the authors hand-searched publications from International Consultation on Incontinence (ICI) [26], NICE (2019) [27] and the book chapter on PFMT for POP from Bø and Frawley (2015) [28]. Reference lists from studies initially selected were also searched to identify any additional relevant studies not identified by the electronic searches. RCTs using other exercise programs than PFMT and comparison between PFMT and other exercise programs for POP are excluded from this review and will be published in a separate manuscript.
The PEDro rating scale, widely used in physical therapy and rehabilitation science [29, 30], was applied to assess the risk of bias (internal validity) for the RCTs. Table 1 shows the ten criteria used in this rating scale. Criteria E (eligibility) concerns external validity (generalizability). A total PEDro score less than four is considered poor, four to five fair, six to eight good and nine to ten excellent [31]. The PEDro scale (Table 1) has been found to be a reliable and valid tool to evaluate methodological quality in clinical trials [30, 32, 33].
Methods, definitions, and units conform to the standards jointly recommended by the International Urogynecological Association and the ICS except where specifically noted [34,35,36].
Results
Outcome measures
A plethora of different outcome measures have been used in published studies on PFMT to treat POP. Table 2 gives an overview of the different measures found in the included studies. Most of the studies reported on training adherence, using appointment attendance and self-reported daily diary entries as outcome measures. Less than half reported on adverse events/complications related to PFMT. For primary outcome measures most of the studies used validated, condition-specific, self-reported questionnaires for symptoms, and the Pelvic Organ Prolapse Quantification (POP-Q) exam results for anatomic description. Few studies assessed muscle morphology using ultrasonography. A minority of the studies focused on cost analyses or need for further POP treatment.
Evidence for pelvic floor muscle training in prevention of POP
We found no primary prevention studies (interventions to stop prolapse from developing in asymptomatic women) of PFMT on POP. However, two studies focused on secondary prevention, as they included women who had not sought health care for assessment or treatment of the condition [37, 38] and a third published [39] 2-year follow-up of one of these [38] (Table 3).
In the unblinded RCT of Wiegersma et al. (2014) [38] PFMT was conducted individually over 3 months with a specialized physical therapist according to each participant’s PFM function assessed by vaginal palpation. Participants completed median 7 (range 5-9) visits with the physical therapist and were asked to do home exercises 3-5 times per week 2-3 times per day. They also received lifestyle advice to lose weight and improve toilet habits. In the assessor-blinded RCT by Hagen et al. (2017) [37] women were randomized to receive either printed lifestyle advice or 5 appointments with a physical therapist over 16 weeks and two blocks of once/week Pilates classes for 6 weeks. The Pilates class included specific PFMT in addition to the regular Pilates exercises
Both studies found statistically significant positive short-term effects on symptoms of POP, but not on POP-Q stage. Significant differences were maintained in some of the measures of symptoms at the 2-year longitudinal follow-up [39].
Evidence for PFMT to treat POP in the peripartum period
Wu et al. (2018) [53] reported results from a systematic review of PFMT in the peripartum period for pelvic floor disorders and found 15 RCTs. Some of these studies reported on UI, AI and sexual dysfunction only and some also included electrical stimulation. Three RCTs [54,55,56] reported on PFMT for POP symptoms (dichotomous outcome; presence/absence of bothersome vaginal bulging) and were included in a meta-analysis. The authors concluded that there is very low-quality evidence that structured PFMT reduces POP symptoms at 6 to 12 months postpartum. Furthermore, they reported that there is moderate-quality evidence that structured PFMT did not change POP stage up to 12 months postpartum. The authors pointed out that evidence remains scarce on the long-term effects of structured postpartum PFMT on pelvic floor outcomes. A 12-year follow-up of an RCT comparing PFMT with control found no effect of PFMT on symptoms or prevalence of POP [57]. However, POP was not reported as an outcome in the original study [58].
In the secondary analysis of an assessor-blinded RCT with PFMT alone compared with only teaching and assessment of PFM strength for UI, 175 primiparous women with and without POP 6 weeks postpartum were included [54]. No effect was found in symptoms of bulging, bladder neck position or POP-Q stage after 4 months of group PFMT + everyday PFMT home training, starting at 6 weeks postpartum. The women diagnosed with POP had POP-Q stage I and II.
Evidence for PFMT in treatment of POP in the general population
Table 3 shows RCTs assessing PFMT to treat anatomical POP or POP symptoms in the general female population. Eleven RCTs including women from 12 different countries were analyzed. Studies included POP of POP-Q stages I-III and results were generally reported for all stages together and not separately for each stage. Four studies compared PFMT with no treatment [40, 41, 44, 48]. The others compared PFMT with lifestyle intervention against lifestyle advice alone. Lifestyle advice included use of precontraction of the PFM before and during an increase in IAP (“the Knack”) and advice to avoid straining during defecation [25, 43] or general lifestyle advice only [42, 45, 47, 49]. Brækken et al. (2010a) [25] was the only study reporting on morphology and did not find any effect of advice to use “the Knack” on PFM strength or morphology. Adherence to the use of the Knack was not reported.
Quality of the interventions, dose response issues
There is some variation in the content of the PFMT interventions for POP in these trials. All the PFMT programs for POP included strength training of the PFM. In the study of Wiegersma et al. (2014) [38], the participants did strength training, but also many other exercise modalities and the chosen exercise program was up to the physical therapist with no standardization of the training protocol. All research groups included vaginal palpation to determine correctness of PFM contractions and some studies used additional biofeedback with the PFMT (Tables 3 and 4).
The training period varied between 4 weeks and 2 years, and number of visits with the physical therapist varied between 4 and 18. PFMT was taught individually in all but one trial [49], who did group training. Supervised PFMT was always combined with a home training program. Drop-outs were low and adherence high in most studies. The highest number of visits with the physical therapist was in the study of Brækken et al. (2010a, 2010b) [25, 43], which included 18 visits over 6 months. No studies compared different training dosages. Overall, more intensive and supervised programs showing better results, both for symptoms and POP-Q stage of POP.
For short-term effect of PFMT, the RCTs showed PFMT to be effective in treating POP, demonstrating statistically significant improvement in POP symptoms [41,42,43,44,45,46, 48, 49] and/or anatomical POP, assessed by POP-Q stage [40, 42,43,44, 46, 48] compared to the comparison group. The results typically show that PFMT can improve POP-Q exams by one stage (from I to 0, II to I and III to II). Frawley et al., (2012) [45], Due et al. (2016) [49] and Ahadi et al. (2017) [51] did not find a significant change in POP stage, but significant improvements were found in some of the individual POP-Q measurements (POP-Q points Ap and Bp) in the study by Frawley et al. (2012) [45]. Methodological scores on PEDro ranged from 4 to 8, with five of the studies scoring 7–8 (Table 3).
Table 4 reports RCTs that compared PFMT with a pessary. Three RCTs were found, but the studies used different pessaries and different PFMT protocols. One study did not find any differences in outcome between PFMT and PFMT + pessary [59] while two studies found significant differences in favor of pessary use. Both Panman et al. (2016) [61] and Cheung et al. (2016) [60] found that pessary fitting fails in a considerable number of women; 40% reported at 12 months [60]. De novo stress urinary incontinence was higher in the pessary group than in the PFMT group, 48% vs 22%, respectively [60].
Evidence for PFMT pre- and post-POP surgery
Table 5 shows the published RCTs on PFMT in connection with POP surgery. Eleven full publications or meeting abstracts which were published from 2005 until 2021 [62,63,64,65,66,67,68,69,70,71,72] were included. We excluded one study because of inclusion of SUI and POP surgery as well as lack of reports of symptoms or stage of POP [66]. PFMT started preoperatively in all studies with between one to four sessions and continued with individual visits post-surgery.
Only one of the RCTs showed any benefit of adding PFMT to surgery for POP [69]. The latter was a pilot feasibility study with 67 participants randomized to either PFMT or usual care in connection with surgery and showed that the training group had fewer prolapse symptoms at 12 months.
Evidence for PFMT in women with POP on sexual dysfunction, bladder and anorectal symptoms
The results of PFMT on sexual dysfunction, bladder and anorectal symptoms for women with POP are presented in Tables 3, 4 and 5. None of the studies had sexual function or bladder and anorectal symptoms as the primary outcome. The size of the studies varied from 57 [71] to 374 participants [72]. One study included women with POP-Q stage I, II and III, regardless of POP symptoms [74], while the others included women with symptoms.
Sexual dysfunction
Tables 3, 4 and 5 include studies reporting the effect of PFMT on sexual function in women with POP. Two studies found some effect of PFMT on sexual function [74, 75]. The short-term improvement of Pelvic Organ Prolapse Incontinence Sexual Questionnaire-12 (PISQ-12) and Female sexual function index (FSFI) scores described by Pauls et al. (2013) [75] was lost after 24 weeks [71]. Braekken et al. (2015) [74] using a validated questionnaire from Mouritsen et al. (2003) [73] found no significant change in the number of sexually active women and no significant differences between groups regarding change in satisfaction with frequency of intercourse. However, interview data showed that 19 (39%) of women in the PFMT group reported improved sexual function compared to only two participants (5%) in the control group (P < 0.01). Some participants reported increased control, strength and awareness of the pelvic floor, improved self-confidence, sensation of a "tighter" vagina, improved libido and orgasms, resolution of pain with intercourse and heightened sexual gratification for partners. Additionally, the study found that participants who described improved sexual function obtained the greatest increases in pelvic floor muscle (PFM) strength (mean 16 ± 10 cmH2O) and endurance (mean 150 ± 140 cmH2O s) (P < 0.01).
Bladder and bowel symptoms
The results related to PFMT on bladder and bowel symptoms in women with POP are shown in Tables 3, 4 and 5. Eight studies found that PFMT improved bladder symptoms [38, 39, 43, 44, 47, 60, 61, 74] and five studies found improvement of anorectal symptoms [39, 43, 44, 47, 61, 74]. Braekken et al. (2010b) [43] and Braekken et al. (2015) [74] report from the same RCT using different outcome measures.
Long-term effect of PFMT in treatment of POP
We defined “long term” as follow-up of at least 6 months after cessation of the intervention conducted in the original RCTs. There are a limited number of studies on the long-term effects of PFMT for POP (Tables 3, 4 and 5). The follow-up period varied between 6 months and 8 to 10 years, and there were no reminders or follow-up of PFMT during the follow-up period. Long-term effect was found in the findings of Panman et al. 2017 [39] and McClurg et al. 2019 [52], but not of Barber et al. 2015 [62], Jelovsek et al. 2018 [67] and Due et al. 2016b [50]. The studies with no long-term effect did not show any short-term effect.
Adverse effects of PFMT in women with POP are almost non-existent, and, if present, mostly not related to the PFMT.
Discussion
This narrative review found no primary prevention RCTs on PFMT for POP and sparse evidence on early interventions in the general female population and the peripartum period. PFMT has been shown to significantly improve POP symptoms and associated pelvic floor complaints. Anatomic POP has been shown to improve by one POP-Q stage. It is unclear how clinically relevant this is because there are insufficient data describing the elevation of the leading edge of prolapse from beyond to above the hymen with PFMT. Studies included women with POP-Q stage I to III POP, and the effect was generally reported for all stages together, and not separated between stages, possibly because of low sample sizes. One pilot feasibility RCT showed significant benefits of PFMT as an adjunct to surgery but this was not proven in the nine other studies. Long-term data are sparse, and results are inconsistent.
Prevention and early peripartum intervention
Given the anatomical and biomechanical rationale and evidence for PFMT to change pelvic floor morphology [25], it is theoretical to assume that PFMT would be effective in prevention of POP. Regular PFMT and early intervention to stop development and worsening of POP (primary prevention) would probably be the best health care investment to reduce suffering and cost of this prevalent female condition. If PFMT is provided as group training, it could be more cost-effective than individual training [22]. However, evidence from robust RCTs in prevention of POP is lacking. Furthermore, RCTs on PFMT in prevention of POP should optimally proceed over 20–30 years and include one PFMT training and one non-training group. It would be costly, time-consuming and probably not possible to keep women adhering to an exercise training program for such long time, nor would asking women not to do PFMT be ethically acceptable. The two included studies on secondary prevention in our review [37, 38] could have been classified as treatment as some of the included women had symptoms of POP, but as the participants had not sought help for POP, we chose to classify them as preventive studies. The results of these RCTs showed some benefit, but the effects were not that convincing [37, 38]. Lack of large effect sizes can be attributed to low training dosage (mode of exercise, frequency, intensity, duration and adherence to training) [76]. The idea of including correct PFMT into general exercise classes for women would probably be the only option to enable women adhere to regular PFMT for the purpose of preventive exercise [22]. However, that would only apply for women who are regularly physically active, and many of them would exercise independently and not in exercise classes.
Somewhat surprisingly, studies have found that POP is also prevalent in nullipara women [77]. As vaginal birth is a main risk factor for the condition, PFMT should be offered at an early stage either during pregnancy or after childbirth [78]. However, since there is insufficient evidence to suggest this based on results from RCTs, this would be based on expert opinion only. Some of the studies in the systematic review of Wu et al. (2018) [53] on postpartum PFMT for PFD were not registered in PubMed [55, 56, 79, 80], and only three RCTs were included in the meta-analysis of PFMT for POP. Three of the RCTs included electrical stimulation in addition to PFMT [79, 81]. The inclusion of these confounders means that we cannot conclude the effect of PFMT alone in these postpartum studies. The conclusion of Wu et al. (2018) [53] is that there is very low-quality evidence that structured PFMT reduces POP symptoms at 6 or 12 months postpartum, which is based on the two RCTs not found in PubMed [55, 56]. Additionally, the evidence for a positive effect in the postpartum period is not supported by results from Bø et al. (2015) [54] or the 12-year follow-up of conservative management of postnatal urinary and fecal incontinence and POP outcomes by Glazener et al. (2014) [57]. The training dosage and level of supervision might have been too low in the Glazener study (2001) [58] but was quite high in the study by Bø et al. (2015) [54]. However, the primary outcome of Bø et al. [54] and Glazener et al.’s [58] RCTs was UI, and both studies included women with and without POP; thus, the sample size may have been too small to detect significant differences for POP. In addition, in the Bø et al. RCT [54], a substantial number of the participants had major levator ani tears, which may have made it more difficult to achieve positive results. Higher IAP with lifting of a newborn infant and baby equipment may further explain difficulties in achieving positive effect of PFMT in the postpartum period. Further RCTs are warranted to investigate the effect of early prevention and treatment using PFMT on women with symptomatic POP in the peripartum period.
General population
The effect of PFMT in the general female population with POP showed overall positive short-term results on POP symptoms, and in most of the studies measuring anatomical POP, the prolapse improved one stage [40, 42,43,44, 46, 48]. The studies with no effect on POP-Q stage had a lower training dosage compared with studies finding statistically significant improvement in anatomical POP [45, 49, 51]. Interventional quality of exercise training studies is dependent on training dosage [22, 76]. We did not find any RCT comparing different training dosages. Ahadi et al. (2017) [51] claimed to compare PFMT with or without biofeedback but added 4 weeks of PFMT with biofeedback to home exercise. Hence, this is not an equivalent comparison. For UI, no additional effect of adding biofeedback was found in an RCT with equal dosage and supervision of PFMT [82]. Kashyap et al. (2013) [46] compared six visits over a 6-month training period using a self-instruction manual only to one-on-one PFMT plus instruction manual, and the results showed the same overall beneficial effect on symptoms and POP-Q stage in the one-on-one PFMT group as Brækken et al. [25, 43]. As for all exercise training programs, this review found that there is a dose-response relationship with more intensive and supervised programs showing better overall results, both for symptoms and POP-Q stage of POP.
This review found only three RCTs comparing PFMT with a pessary, highlighting the need for further high-quality RCTs for this comparison. The level of evidence for pessaries as an effective intervention for POP was level three evidence in the 2017 ICI systematic review [26] and this corresponds with the latest Cochrane review [83]. As wearing a pessary over time may unmask occult stress urinary incontinence, this should not be considered a complication of pessary use [84].
Sexual, bladder and anorectal comorbidities
Many of the RCTs on PFMT in women with POP also evaluated the effect on comorbidities such as sexual dysfunction, bladder and anorectal symptoms and found positive results. However, none of the studies had these comorbidities as primary outcomes and the studies included women with and without these symptoms. The power of the studies not finding an effect may be too low for these secondary analyses. Most studies used general validated instruments for the overall conditions, and more detailed information on the effect of UI and AI was not always available.
Sexual dysfunction in women is frequently associated with pelvic organ prolapse (POP) [85]. In a systematic review [86], the authors found only Level 2 evidence that PFMT can improve women's sexual function, and the literature is scarce about the effect of PFMT on sexual function in women with POP. As for other comorbidities, the training duration in some of the studies was short because it was done as an adjunct to surgery [64, 71], had a limited number of supervised sessions which may have limited adherence to the training protocol [49, 72] and included women both with and without sexual dysfunction. There is some evidence that women without sexual dysfunction have increased PFM strength compared to women with sexual dysfunction [87]. However, sexual function is influenced by several interpersonal, contextual, personal, psychological and biological factors including POP. Partner factors may adversely affect sexual function and diminish the benefit of PFMT [86]. We found that only two RCTs which showed some positive effects of PFMT on sexual function of women with POP [71, 74]. There is need for new RCTs specially designed to investigate the effect of PFMT in specific types of sexual dysfunction in women with POP.
Some of the studies assessing bladder and anorectal symptoms had a relatively short duration of the PFMT protocol as they were investigating perioperative PFMT [64, 71, 75] or a limited number of supervised sessions that could have limited the adherence to training protocol [37, 42, 47, 49, 69, 72]. The two RCTs offering supervised PFMT for a longer time showed improvement in bladder and anorectal symptoms in women with POP [25, 39, 74]. Future high quality RCTs are therefore still needed to investigate the impact of intensive supervised PFMT protocols on bladder and anorectal symptoms in women with POP.
Effect of PFMT pre- and post-POP surgery
It is somewhat counterintuitive that PFMT does not seem to be effective pre- and post-POP surgery. This is despite evidence that it is effective in the treatment of POP [26]. However, women included in surgical studies may be a selected group with more severe POP resulting from major PFM tears, perineal tears or higher hiatal area ballooning. In addition, it may be difficult to show additional effect of PFMT if surgery alone is effective, and a possible effect of PFMT may only be expected to be seen after many years of continuous PFMT. The longest follow-up period was 5 years after surgery, but there were no incentives for continuous PFMT during the follow-up period after the last training session 12 weeks post-surgery, and there was no report on adherence to maintenance training [67]. Furthermore, there was no effect of the original training program in this study [62], and a long-term effect may therefore not be expected. The lack of effect of PFMT in connection to POP surgery warrants that such studies should be analyzed separately from treatment trials in the general population and not be merged in meta-analyses.
Furthermore, the recurrence rate following traditional surgery for POP is approximately 30% [88, 89], and surgery for prolapse can be associated with various adverse events and potentially poorer quality of life than the original condition [90, 91]. Mesh is one option for surgical treatment of stress urinary incontinence (SUI) and POP. However, some women experience serious complications [88, 89], and mesh is now the subject of intense global scrutiny after reports of serious negative long-term effects [92]. The National Institute for Health and Care Excellence (NICE) Guidelines (2019) [27] state that there is some evidence of benefit for all surgical procedures for POP recommended in their guideline, including mesh procedures, but limited evidence on long-term effectiveness and adverse effects. They conclude that “the true prevalence of long-term complications is unknown.” Although the rate of severe complications may be low [90], due to high surgery rates, a substantial number of women will suffer after POP surgery worldwide [92]. Non-invasive treatments, such as lifestyle interventions and PFMT, should therefore be considered before surgical interventions [26, 27].
Long-term studies
There are general challenges to long-term studies of any intervention due to loss-to follow-up, co-interventions, treatment switching and competing events [93, 94]. For exercise training there are additional challenges such as non-adherence to maintenance training [93, 94]. In a systematic review of long-term effect of PFMT for SUI/MUI 19 studies with follow-up ranging from 1–15 years were found [93]. Only two studies provided follow-up incentives for continuous PFMT during follow-up and long-term adherence to PFMT varied between 10% and 70%. For the POP studies found in the present review, there were no incentives for continuous PFMT after cessation of the original intervention, and only Barber et al. (2014) [62] reported long-term adherence to PFMT. They found that 93.4% reported to adhere to PFMT 6 months after the intervention and 81.4% at 2 years. However, there was no effect of PFMT in this study on either PFM strength or POP. In the 5-year follow-up of the Barber et al. study (2014) [62], Jelovsek et al. (2018) [67] reported that the estimated surgical failure rate was 61.5% and 70.3% in the two surgical groups, respectively. They concluded that rates of surgical failure increased during the follow-up period, although prolapse symptom scores remained improved.
There are challenges in adherence to long-term PFMT when there is no structured follow-up regimen or encouragement for further training after the initial supervised PFMT. This could explain the diminishing effect. Furthermore, if there was no short-term effect of a PFMT program [49, 50, 62, 67, 71, 75], then long-term effects are unlikely. Long-term success of any exercise training program relies on maintenance training. When women are left alone to do PFMT with no further incentives this is a challenge to some. The promotion of PFMT from a women’s health perspective should include strategies to support building PFMT into their general exercise/physical activity programs and/or daily routines. However, today < 30% of the adult population follows the WHO’s recommendations for participation in physical activity and exercise training, and it is likely that only those who are already physically fit and motivated for general training will attend structured exercise classes which could include specific PFMT [95,96,97]. New ways of reaching women with information on why and how to perform PFMT in addition to more general physical activity are needed. Due to injuries and weaknesses of the PFM and inability to contract correctly, PFMT may be even more difficult to adhere to than other exercise. More work is required to improve women’s long-term adherence to pelvic floor rehabilitation programs.
At present, one can question whether today’s health services for non-surgical interventions for POP are optimal. In a focus group study of 22 women receiving prolapse care through urogynecology services in the UK [98], the authors found that women often delayed seeking help for their symptoms because of lack of awareness, embarrassment and stigma. When they did present to their family doctors, their symptoms were often dismissed and unaddressed until they became more severe, and the women reported receiving little or no choice in treatment decisions. Choices were often influenced by health professionals' preferences and inconsistent with women's preferences and needs. Physical therapy-based interventions were reported as helping women regain control over their symptoms and life.
The results of the present narrative review support the conclusion of the ICI 2017 with 1A evidence/recommendation for PFMT in treatment of POP in the general female population [26]. In addition, the NICE guidelines (2019) [27] recommend considering a program of supervised PFMT for at least 16 weeks as a first option for women with symptomatic POP-Q stage I or stage II. If the program is beneficial, they recommend advising women to continue PFMT. There is no strong evidence for strength training maintenance programs, but intensity of the contraction seems to be the main factor. We therefore recommend 1–2 sessions a week with 8–12 close to maximum contractions. The overall best results found in our review were in an RCT with 18 supervised training sessions over a 6-month training period [25, 43]. We were only able to find one study on predictors of success of PFMT in women with POP [99]. They found that young age and having ≥ 1 indicators of obstetric trauma were predicting factors but discussed that many factors such as PFM function were not included in the analysis. We agree with the authors that there is a need for further studies on this important clinical question.
Clinical recommendations for effective PFMT for POP
*Provide proper information about the pelvic floor, exercise physiology and evidence for how PFMT can improve pelvic floor morphology and POP
*Teach proper PFM contraction technique and assess whether the woman can do a correct contraction (vaginal palpation, manometry, dynamometry, ultrasound) and give immediate feedback of performance
*Use validated outcome measures to assess POP symptoms, stage of POP (POP-Q) and comorbidities before and after treatment
*Offer individual weekly visits or group training with a physical therapist for at least 6 months with additional home training
*Teach women at risk for POP strategies to reduce IAP during activities of daily living
*Use motivational strategies to favor adherence
*Strength training regimens should follow general principles for strength training (3 sets of 8-12 close to maximum contractions at least 3-4 times/week and continue for at least 4 months)
*Register adherence to both supervised PFMT and home training
*Assess PFM variables (resting value, PFM strength and endurance) before and after treatment
*Recommend a suitable PFMT maintenance program with intensity of the contraction being the most important factor (8-12 contractions 1-2 times/week)
Recommendations for further studies
*Primary and secondary prevention studies in the general female population and studies in women with POP within 12 months after childbirth
*Monitoring long-term adherence and study predictors of success of PFMT for POP including pelvic floor biological/anatomical factors
References
Brown HW, Hegde A, Huebner M, Neels H, Barnes HC, Marquini GV, et al. International urogynecology consultation chapter 1 committee 2: Epidemiology of pelvic organ prolapse: prevalence, incidence, natural history, and service needs. Int Urogynecol J. 2022;33(2):173–87. https://doi.org/10.1007/s00192-021-05018-z.
Lowenstein L, Gamble T, Sanses TV, van Raalte H, Carberry C, Jakus S, et al. Sexual function is related to body image perception in women with pelvic organ prolapse. J Sex Med. 2009;6(8):2286–91. https://doi.org/10.1111/j.1743-6109.2009.01329.x.
Deprest JA, Cartwright R, Dietz HP, Brito LGO, Koch M, Allen-Brady K, et al. International Urogynecological Consultation (IUC): pathophysiology of pelvic organ prolapse (POP). Int Urogynecol J. 2022;33(7):1699–710. https://doi.org/10.1007/s00192-022-05081-0.
DeLancey JO. What's new in the functional anatomy of pelvic organ prolapse? Curr Opin Obstet Gynecol. 2016;28(5):420–9. https://doi.org/10.1097/GCO.0000000000000312.
DeLancey JO, Hurd WW. Size of the urogenital hiatus in the levator ani muscles in normal women and women with pelvic organ prolapse. Obstet Gynecol. 1998;91(3):364–8. https://doi.org/10.1016/s0029-7844(97)00682-0.
Dietz HP, Franco AV, Shek KL, Kirby A. Avulsion injury and levator hiatal ballooning: two independent risk factors for prolapse? An observational study. Acta Obstet Gynecol Scand. 2012;91(2):211–4. https://doi.org/10.1111/j.1600-0412.2011.01315.x.
Ghetti C, Gregory WT, Edwards SR, Otto LN, Clark AL. Severity of pelvic organ prolapse associated with measurements of pelvic floor function. Int Urogynecol J Pelvic Floor Dysfunct. 2005;16(6):432–6. https://doi.org/10.1007/s00192-004-1274-1.
Hoyte L, Jakab M, Warfield SK, Shott S, Flesh G, Fielding JR. Levator ani thickness variations in symptomatic and asymptomatic women using magnetic resonance-based 3-dimensional color mapping. Am J Obstet Gynecol. 2004;191(3):856–61. https://doi.org/10.1016/j.ajog.2004.06.067.
Hsu Y, Summers A, Hussain HK, Guire KE, Delancey JO. Levator plate angle in women with pelvic organ prolapse compared to women with normal support using dynamic MR imaging. Am J Obstet Gynecol. 2006;194(5):1427–33. https://doi.org/10.1016/j.ajog.2006.01.055.
Siahkal SF, Iravani M, Mohaghegh Z, Sharifipour F, Zahedian M, Nasab MB. Investigating the association of the dimensions of genital hiatus and levator hiatus with pelvic organ prolapse: a systematic review. Int Urogynecol J. 2021;32(8):2095–109. https://doi.org/10.1007/s00192-020-04639-0.
Singh K, Jakab M, Reid WM, Berger LA, Hoyte L. Three-dimensional magnetic resonance imaging assessment of levator ani morphologic features in different grades of prolapse. Am J Obstet Gynecol. 2003;188(4):910–5. https://doi.org/10.1067/mob.2003.254.
Volløyhaug I, Morkved S, Salvesen KA. Association between pelvic floor muscle trauma and pelvic organ prolapse 20 years after delivery. Int Urogynecol J. 2016;27(1):39–45. https://doi.org/10.1007/s00192-015-2784-8.
Xuan Y, Friedman T, Dietz HP. Does levator ani hiatal area configuration affect pelvic organ prolapse? Ultrasound Obstet Gynecol. 2019;54(1):124–7. https://doi.org/10.1002/uog.20210.
DeLancey JO, Morgan DM, Fenner DE, Kearney R, Guire K, Miller JM, et al. Comparison of levator ani muscle defects and function in women with and without pelvic organ prolapse. Obstet Gynecol. 2007;109(2 Pt 1):295–302. https://doi.org/10.1097/01.AOG.0000250901.57095.ba.
Handa VL, Roem J, Blomquist JL, Dietz HP, Munoz A. Pelvic organ prolapse as a function of levator ani avulsion, hiatus size, and strength. Am J Obstet Gynecol. 2019;221(1):41 e1–7. https://doi.org/10.1016/j.ajog.2019.03.004.
Huebner M, Margulies RU, DeLancey JO. Pelvic architectural distortion is associated with pelvic organ prolapse. Int Urogynecol J Pelvic Floor Dysfunct. 2008;19(6):863–7. https://doi.org/10.1007/s00192-007-0546-y.
Braekken IH, Majida M, Engh ME, Bo K. Are pelvic floor muscle thickness and size of levator hiatus associated with pelvic floor muscle strength, endurance and vaginal resting pressure in women with pelvic organ prolapse stages I-III? A cross sectional 3D ultrasound study. Neurourol Urodyn. 2014;33(1):115–20. https://doi.org/10.1002/nau.22384.
Hilde G, Staer-Jensen J, Siafarikas F, Gjestland K, Ellstrom Engh M, Bo K. How well can pelvic floor muscles with major defects contract? A cross-sectional comparative study 6 weeks after delivery using transperineal 3D/4D ultrasound and manometer. BJOG. 2013;120(11):1423–9. https://doi.org/10.1111/1471-0528.12321.
Braekken IH, Majida M, Ellstrom Engh M, Holme IM, Bo K. Pelvic floor function is independently associated with pelvic organ prolapse. BJOG. 2009;116(13):1706–14. https://doi.org/10.1111/j.1471-0528.2009.02379.x.
Kegel AH. Stress incontinence and genital relaxation; a nonsurgical method of increasing the tone of sphincters and their supporting structures. Ciba Clin Symp. 1952;4(2):35–51.
Bø K. Pelvic floor muscle training is effective in treatment of female stress urinary incontinence, but how does it work? Int Urogynecol J Pelvic Floor Dysfunct. 2004;15(2):76–84. https://doi.org/10.1007/s00192-004-1125-0.
Bø K. Physiotherapy management of urinary incontinence in females. J Physiother. 2020;66(3):147–54. https://doi.org/10.1016/j.jphys.2020.06.011.
Miller JM, Perucchini D, Carchidi LT, DeLancey JO, Ashton-Miller J. Pelvic floor muscle contraction during a cough and decreased vesical neck mobility. Obstet Gynecol. 2001;97(2):255–60. https://doi.org/10.1016/s0029-7844(00)01132-7.
Peschers UM, Fanger G, Schaer GN, Vodusek DB, DeLancey JO, Schuessler B. Bladder neck mobility in continent nulliparous women. BJOG. 2001;108(3):320–4. https://doi.org/10.1111/j.1471-0528.2001.00066.x.
Braekken IH, Majida M, Engh ME, Bo K. Morphological changes after pelvic floor muscle training measured by 3-dimensional ultrasonography: a randomized controlled trial. Obstet Gynecol. 2010;115(2 Pt 1):317–24. https://doi.org/10.1097/AOG.0b013e3181cbd35f.
Dumoulin C, Adewuyi T, Booth J, Bradley C, Burgio K, Hagen S, et al. Adult Conservative Management. In: Abrams P, Cardozo L, Wagg A, Wein A, editors. 6th International Consultation on Incontinence. ICI-ICS. Bristol: International Continence Society; 2017. p. 1443–628.
Excellence NIfHaC. NICE guideline. Urinary incontinence and pelvic organ prolapse in women: management [NG123]
Bø K, Frawley H. Pelvic floor muscle training in prevention and treatment of pelvic organ prolapse. In: Bø K, Berghmans B, Mørkved S, Van Kampen M, editors. Evidence based physical therapy for the pelvic floor Bridging science and clinical practice. 2nd ed. Edinburgh: Elsevier; 2015. p. 234–42.
Kamper SJ, Moseley AM, Herbert RD, Maher CG, Elkins MR, Sherrington C. 15 years of tracking physiotherapy evidence on PEDro, where are we now? Br J Sports Med. 2015;49(14):907–9. https://doi.org/10.1136/bjsports-2014-094468.
Sherrington C, Herbert RD, Maher CG, Moseley AM, PEDro. A database of randomized trials and systematic reviews in physiotherapy. Man Ther. 2000;5(4):223–6. https://doi.org/10.1054/math.2000.0372.
Cashin AG, McAuley JH. Clinimetrics: Physiotherapy Evidence Database (PEDro) Scale. J Physiother. 2020;66(1):59. https://doi.org/10.1016/j.jphys.2019.08.005.
Macedo LG, Elkins MR, Maher CG, Moseley AM, Herbert RD, Sherrington C. There was evidence of convergent and construct validity of Physiotherapy Evidence Database quality scale for physiotherapy trials. J Clin Epidemiol. 2010;63(8):920–5. https://doi.org/10.1016/j.jclinepi.2009.10.005.
Maher CG, Sherrington C, Herbert RD, Moseley AM, Elkins M. Reliability of the PEDro scale for rating quality of randomized controlled trials. Phys Ther. 2003;83(8):713–21.
Bø K, Frawley HC, Haylen BT, Abramov Y, Almeida FG, Berghmans B, et al. An International Urogynecological Association (IUGA)/International Continence Society (ICS) joint report on the terminology for the conservative and nonpharmacological management of female pelvic floor dysfunction. Int Urogynecol J. 2017;28(2):191–213. https://doi.org/10.1007/s00192-016-3123-4.
Frawley H, Shelly B, Morin M, Bernard S, Bø K, Digesu GA, et al. An International Continence Society (ICS) report on the terminology for pelvic floor muscle assessment. Neurourol Urodyn. 2021;40(5):1217–60. https://doi.org/10.1002/nau.24658.
Haylen BT, de Ridder D, Freeman RM, Swift SE, Berghmans B, Lee J, et al. An International Urogynecological Association (IUGA)/International Continence Society (ICS) joint report on the terminology for female pelvic floor dysfunction. Int Urogynecol J. 2010;21(1):5–26. https://doi.org/10.1007/s00192-009-0976-9.
Hagen S, Glazener C, McClurg D, Macarthur C, Elders A, Herbison P, et al. Pelvic floor muscle training for secondary prevention of pelvic organ prolapse (PREVPROL): a multicentre randomised controlled trial. Lancet. 2017;389(10067):393–402. https://doi.org/10.1016/s0140-6736(16)32109-2.
Wiegersma M, Panman CM, Kollen BJ, Berger MY, Lisman-Van Leeuwen Y, Dekker JH. Effect of pelvic floor muscle training compared with watchful waiting in older women with symptomatic mild pelvic organ prolapse: randomised controlled trial in primary care. BMJ. 2014;349:g7378. https://doi.org/10.1136/bmj.g7378.
Panman C, Wiegersma M, Kollen BJ, Berger MY, Lisman-Van Leeuwen Y, Vermeulen KM, et al. Two-year effects and cost-effectiveness of pelvic floor muscle training in mild pelvic organ prolapse: a randomised controlled trial in primary care. BJOG. 2017;124(3):511–20. https://doi.org/10.1111/1471-0528.13992.
Piya-Anant M, Therasakvichya S, Leelaphatanadit C, Techatrisak K. Integrated health research program for the Thai elderly: prevalence of genital prolapse and effectiveness of pelvic floor exercise to prevent worsening of genital prolapse in elderly women. J Med Assoc Thai. 2003;86(6):509–15.
Ghroubi S, Kharrat O, Chaari M, Ben Ayed B, Guermazi M, Elleuch MH. Effect of conservative treatment in the management of low-degree urogenital prolapse. Ann Readapt Med Phys. 2008;51(2):96–102. https://doi.org/10.1016/j.annrmp.2007.11.002.
Hagen S, Stark D, Glazener C, Sinclair L, Ramsay I. A randomized controlled trial of pelvic floor muscle training for stages I and II pelvic organ prolapse. Int Urogynecol J Pelvic Floor Dysfunct. 2009;20(1):45–51. https://doi.org/10.1007/s00192-008-0726-4.
Braekken IH, Majida M, Engh ME, Bo K. Can pelvic floor muscle training reverse pelvic organ prolapse and reduce prolapse symptoms? An assessor-blinded, randomized, controlled trial. Am J Obstet Gynecol. 2010;203(2):170 e1–7. https://doi.org/10.1016/j.ajog.2010.02.037.
Stupp L, Resende AP, Oliveira E, Castro RA, Girao MJ, Sartori MG. Pelvic floor muscle training for treatment of pelvic organ prolapse: an assessor-blinded randomized controlled trial. Int Urogynecol J. 2011;22(10):1233–9. https://doi.org/10.1007/s00192-011-1428-x.
Frawley HC, Hagen S, Sherburn M, Neumann P, Herbison P, Hay-Smith J, et al. Changes in prolapse following pelvic floor muscle training: a randomised controlled trial. Neurourol Urodyn. 2012;31(6):938–9. https://doi.org/10.1002/nau.22287.
Kashyap R, Jain V, Singh A. Comparative effect of 2 packages of pelvic floor muscle training on the clinical course of stage I-III pelvic organ prolapse. Int J Gynaecol Obstet. 2013;121(1):69–73. https://doi.org/10.1016/j.ijgo.2012.11.012.
Hagen S, Stark D, Glazener C, Dickson S, Barry S, Elders A, et al. Individualised pelvic floor muscle training in women with pelvic organ prolapse (POPPY): a multicentre randomised controlled trial. Lancet. 2014;383(9919):796–806. https://doi.org/10.1016/s0140-6736(13)61977-7.
Alves FK, Riccetto C, Adami DB, Marques J, Pereira LC, Palma P, et al. A pelvic floor muscle training program in postmenopausal women: A randomized controlled trial. Maturitas. 2015;81(2):300–5. https://doi.org/10.1016/j.maturitas.2015.03.006.
Due U, Brostrom S, Lose G. Lifestyle advice with or without pelvic floor muscle training for pelvic organ prolapse: a randomized controlled trial. Int Urogynecol J. 2016;27(4):555–63. https://doi.org/10.1007/s00192-015-2852-0.
Due U, Brostrom S, Lose G. The 12-month effects of structured lifestyle advice and pelvic floor muscle training for pelvic organ prolapse. Acta Obstet Gynecol Scand. 2016;95(7):811–9. https://doi.org/10.1111/aogs.12884.
Ahadi T, Taghvadoost N, Aminimoghaddam S, Forogh B, Bazazbehbahani R, Raissi GR. Efficacy of biofeedback on quality of life in stages I and II pelvic organ prolapse: A Pilot study. Eur J Obstet Gynecol Reprod Biol. 2017;215:241–6. https://doi.org/10.1016/j.ejogrb.2017.06.023.
McClurg D, Hagen S, Berry K, Elders A, Best C, Wane S, et al. A 10 year data-linkage follow-up study of a trial of pelvic floor muscle training for prolapse. Neurourol Urodyn. 2019;38:S368–S9. https://doi.org/10.1002/nau.24118.
Wu YM, McInnes N, Leong Y. Pelvic Floor Muscle Training Versus Watchful Waiting and Pelvic Floor Disorders in Postpartum Women: A Systematic Review and Meta-analysis. Female Pelvic Med Reconstr Surg. 2018;24(2):142–9. https://doi.org/10.1097/SPV.0000000000000513.
Bø K, Hilde G, Staer-Jensen J, Siafarikas F, Tennfjord MK, Engh ME. Postpartum pelvic floor muscle training and pelvic organ prolapse-a randomized trial of primiparous women. Am J Obstet Gynecol. 2015;212(1):38 e1–7. https://doi.org/10.1016/j.ajog.2014.06.049.
Li Y, Lei X, Jin YL, Wang J, Zhang LP. Effect of postpartum pelvic floor muscle training on pelvic organ prolapse in primiparous women. Chinese Journal of Woman and Child Health Research. 2016;27(11):1384–7.
Yang X, Liu Y. Analysis of the effect of pelvic floor muscle training in postpartum pelvic floor dysfunction. Journal of International Obstetrics and Gynecology. 2013;40(2):164–6.
Glazener CM, MacArthur C, Hagen S, Elders A, Lancashire R, Herbison GP, et al. Twelve-year follow-up of conservative management of postnatal urinary and faecal incontinence and prolapse outcomes: randomised controlled trial. BJOG. 2014;121(1):112–20. https://doi.org/10.1111/1471-0528.12473.
Glazener CM, Herbison GP, Wilson PD, MacArthur C, Lang GD, Gee H, et al. Conservative management of persistent postnatal urinary and faecal incontinence: randomised controlled trial. BMJ. 2001;323(7313):593–6. https://doi.org/10.1136/bmj.323.7313.593.
Manonai J, Harnsomboon T, Sarit-apirak S, Wattanayingcharoenchai R, Chittacharoen A, Suthutvoravut S. Effect of Colpexin Sphere on pelvic floor muscle strength and quality of life in women with pelvic organ prolapse stage I/II: a randomized controlled trial. Int Urogynecol J. 2012;23(3):307–12. https://doi.org/10.1007/s00192-011-1569-y.
Cheung RY, Lee JH, Lee LL, Chung TK, Chan SS. Vaginal Pessary in Women With Symptomatic Pelvic Organ Prolapse: A Randomized Controlled Trial. Obstet Gynecol. 2016;128(1):73–80. https://doi.org/10.1097/AOG.0000000000001489.
Panman CM, Wiegersma M, Kollen BJ, Berger MY, Lisman-van Leeuwen Y, Vermeulen KM, et al. Effectiveness and cost-effectiveness of pessary treatment compared with pelvic floor muscle training in older women with pelvic organ prolapse: 2-year follow-up of a randomized controlled trial in primary care. Menopause. 2016;23(12):1307–18. https://doi.org/10.1097/GME.0000000000000706.
Barber MD, Brubaker L, Burgio KL, Richter HE, Nygaard I, Weidner AC, et al. Comparison of 2 transvaginal surgical approaches and perioperative behavioral therapy for apical vaginal prolapse: the OPTIMAL randomized trial. JAMA. 2014;311(10):1023–34. https://doi.org/10.1001/jama.2014.1719.
Brandt C, Janse van Vuuren EC. Postoperative Physiotherapy in Women Undergoing Pelvic Floor Reconstructive Surgery: A Randomized Controlled Clinical Trial. Physiotherapy Canada. 2021;0(0):e20200053. https://doi.org/10.3138/ptc-2020-0053.
Duarte TB, Bø K, Brito LGO, Bueno SM, Barcelos TM, Bonacin MA, et al. Perioperative pelvic floor muscle training did not improve outcomes in women undergoing pelvic organ prolapse surgery: a randomised trial. J Physiother. 2020;66(1):27–32. https://doi.org/10.1016/j.jphys.2019.11.013.
Frawley HC, Phillips BA, Bø K, Galea MP. Physiotherapy as an adjunct to prolapse surgery: an assessor-blinded randomized controlled trial. Neurourol Urodyn. 2010;29(5):719–25. https://doi.org/10.1002/nau.20828.
Jarvis SK, Hallam TK, Lujic S, Abbott JA, Vancaillie TG. Peri-operative physiotherapy improves outcomes for women undergoing incontinence and or prolapse surgery: results of a randomised controlled trial. Aust N Z J Obstet Gynaecol. 2005;45(4):300–3. https://doi.org/10.1111/j.1479-828X.2005.00415.x.
Jelovsek JE, Barber MD, Brubaker L, Norton P, Gantz M, Richter HE, et al. Effect of Uterosacral Ligament Suspension vs Sacrospinous Ligament Fixation With or Without Perioperative Behavioral Therapy for Pelvic Organ Vaginal Prolapse on Surgical Outcomes and Prolapse Symptoms at 5 Years in the OPTIMAL Randomized Clinical Trial. JAMA. 2018;319(15):1554–65. https://doi.org/10.1001/jama.2018.2827.
Mathew S, Nyhus MO, Salvesen O, Salvesen KA, Stafne SN, Volloyhaug I. The effect of preoperative pelvic floor muscle training on urinary and colorectal-anal distress in women undergoing pelvic organ prolapse surgery-a randomized controlled trial. Int Urogynecol J. 2021;32(10):2787–94. https://doi.org/10.1007/s00192-021-04684-3.
McClurg D, Hilton P, Dolan L, Monga A, Hagen S, Frawley H, et al. Pelvic floor muscle training as an adjunct to prolapse surgery: a randomised feasibility study. Int Urogynecol J. 2014;25(7):883–91. https://doi.org/10.1007/s00192-013-2301-x.
Nyhus MO, Mathew S, Salvesen O, Salvesen KA, Stafne S, Volloyhaug I. Effect of preoperative pelvic floor muscle training on pelvic floor muscle contraction and symptomatic and anatomical pelvic organ prolapse after surgery: randomized controlled trial. Ultrasound Obstet Gynecol. 2020;56(1):28–36. https://doi.org/10.1002/uog.22007.
Pauls RN, Crisp CC, Novicki K, Fellner AN, Kleeman SD. Pelvic floor physical therapy: impact on quality of life 6 months after vaginal reconstructive surgery. Female Pelvic Med Reconstr Surg. 2014;20(6):334–41. https://doi.org/10.1097/SPV.0000000000000090.
Weidner AC, Barber MD, Markland A, Rahn DD, Hsu Y, Mueller ER, et al. Perioperative Behavioral Therapy and Pelvic Muscle Strengthening Do Not Enhance Quality of Life After Pelvic Surgery: Secondary Report of a Randomized Controlled Trial. Phys Ther. 2017;97(11):1075–83. https://doi.org/10.1093/ptj/pzx077.
Mouritsen L, Larsen JP. Symptoms, bother and POPQ in women referred with pelvic organ prolapse. Int Urogynecol J Pelvic Floor Dysfunct. 2003;14(2):122–7. https://doi.org/10.1007/s00192-002-1024-1.
Braekken IH, Majida M, Ellstrom Engh M, Bo K. Can pelvic floor muscle training improve sexual function in women with pelvic organ prolapse? A randomized controlled trial. J Sex Med. 2015;12(2):470–80. https://doi.org/10.1111/jsm.12746.
Pauls RN, Crisp CC, Novicki K, Fellner AN, Kleeman SD. Impact of physical therapy on quality of life and function after vaginal reconstructive surgery. Female Pelvic Med Reconstr Surg. 2013;19(5):271–7. https://doi.org/10.1097/SPV.0b013e31829c64ea.
Hoogeboom TJ, Kousemaker MC, van Meeteren NL, Howe T, Bo K, Tugwell P, et al. i-CONTENT tool for assessing therapeutic quality of exercise programs employed in randomised clinical trials. Br J Sports Med. 2021;55(20):1153–60. https://doi.org/10.1136/bjsports-2019-101630.
Dietz HP, Chavez-Coloma L, Friedman T, Turel F. Pelvic organ prolapse in nulliparae. Aust N Z J Obstet Gynaecol. 2022. https://doi.org/10.1111/ajo.13481.
Woodley SJ, Lawrenson P, Boyle R, Cody JD, Morkved S, Kernohan A, et al. Pelvic floor muscle training for preventing and treating urinary and faecal incontinence in antenatal and postnatal women. Cochrane Database Syst Rev. 2020;5:CD007471. https://doi.org/10.1002/14651858.CD007471.pub4.
Chu X, Huang O, Zhou J. The effect of biofeedback and electrical stimulation combined with pelvic floor muscle exercises for postpartum pelvic floor rehabilitation. Progress in Obstetrics and Gynecology. 2012;21(9):679–83.
Zhang R, Wang Q, Zhao G. Effect on pelvic floor muscle function and quality of life by pelvic floor muscle exercise combined with lifestyle intervention in postpartum women. Chinese Journal of Health Care and Medicine. 2015;17(6):469–72.
Yang S, Sang W, Feng J, Zhao H, Li X, Li P, et al. The effect of rehabilitation exercises combined with direct vagina low voltage low frequency electric stimulation on pelvic nerve electrophysiology and tissue function in primiparous women: A randomised controlled trial. J Clin Nurs. 2017;26(23-24):4537–47. https://doi.org/10.1111/jocn.13790.
Hagen S, Elders A, Henderson L, Kilonzo M, McClurg D, Hay-Smith J, et al. Effectiveness and cost-effectiveness of biofeedback-assisted pelvic floor muscle training for female urinary incontinence: a multicentre randomised controlled trial. Neurourol Urodyn. 2019;38:S365–S6.
Bugge C, Adams EJ, Gopinath D, Stewart F, Dembinsky M, Sobiesuo P, et al. Pessaries (mechanical devices) for managing pelvic organ prolapse in women. Cochrane Database Syst Rev. 2020;11:CD004010. https://doi.org/10.1002/14651858.CD004010.pub4.
Chughtai B, Spettel S, Kurman J, De E. Ambulatory pessary trial unmasks occult stress urinary incontinence. Obstet Gynecol Int. 2012;2012:392027. https://doi.org/10.1155/2012/392027.
Antosh DD, Kim-Fine S, Meriwether KV, Kanter G, Dieter AA, Mamik MM, et al. Changes in Sexual Activity and Function After Pelvic Organ Prolapse Surgery: A Systematic Review. Obstet Gynecol. 2020;136(5):922–31. https://doi.org/10.1097/AOG.0000000000004125.
Ferreira CH, Dwyer PL, Davidson M, De Souza A, Ugarte JA, Frawley HC. Does pelvic floor muscle training improve female sexual function? A systematic review. Int Urogynecol J. 2015;26(12):1735–50. https://doi.org/10.1007/s00192-015-2749-y.
de Menezes FM, Driusso P, Bo K, Carvalho de Abreu DC, da Silva Lara LA, de Sa Rosa ESACJ, et al. Relationship between pelvic floor muscle strength and sexual dysfunction in postmenopausal women: a cross-sectional study. Int Urogynecol J. 2017;28(6):931–6. https://doi.org/10.1007/s00192-016-3211-5.
Glazener C, Breeman S, Elders A, Hemming C, Cooper K, Freeman R, et al. Clinical effectiveness and cost-effectiveness of surgical options for the management of anterior and/or posterior vaginal wall prolapse: two randomised controlled trials within a comprehensive cohort study - results from the PROSPECT Study. Health Technol Assess. 2016;20(95):1–452. https://doi.org/10.3310/hta20950.
Glazener CM, Breeman S, Elders A, Hemming C, Cooper KG, Freeman RM, et al. Mesh, graft, or standard repair for women having primary transvaginal anterior or posterior compartment prolapse surgery: two parallel-group, multicentre, randomised, controlled trials (PROSPECT). Lancet. 2017;389(10067):381–92. https://doi.org/10.1016/s0140-6736(16)31596-3.
Reid FM, Elders A, Breeman S, Freeman RM, group Ps. How common are complications following polypropylene mesh, biological xenograft and native tissue surgery for pelvic organ prolapse? A secondary analysis from the PROSPECT trial. BJOG. 2021;128(13):2180–9. https://doi.org/10.1111/1471-0528.16897.
Vergeldt TF, Weemhoff M, IntHout J, Kluivers KB. Risk factors for pelvic organ prolapse and its recurrence: a systematic review. Int Urogynecol J. 2015;26(11):1559–73. https://doi.org/10.1007/s00192-015-2695-8.
Haskell H. Cumberlege review exposes stubborn and dangerous flaws in healthcare. BMJ. 2020;370:m3099. https://doi.org/10.1136/bmj.m3099.
Bø K, Hilde G. Does it work in the long term?--A systematic review on pelvic floor muscle training for female stress urinary incontinence. Neurourol Urodyn. 2013;32(3):215–23. https://doi.org/10.1002/nau.22292.
Herbert RD, Kasza J, Bø K. Analysis of randomised trials with long-term follow-up. BMC Med Res Methodol. 2018;18(1):48. https://doi.org/10.1186/s12874-018-0499-5.
Hansen BH, Kolle E, Steene-Johannessen J, Dalene KE, Ekelund U, Anderssen SA. Monitoring population levels of physical activity and sedentary time in Norway across the lifespan. Scand J Med Sci Sports. 2019;29(1):105–12. https://doi.org/10.1111/sms.13314.
Loyen A, Clarke-Cornwell AM, Anderssen SA, Hagstromer M, Sardinha LB, Sundquist K, et al. Sedentary Time and Physical Activity Surveillance Through Accelerometer Pooling in Four European Countries. Sports Med. 2017;47(7):1421–35. https://doi.org/10.1007/s40279-016-0658-y.
Bull FC, Al-Ansari SS, Biddle S, Borodulin K, Buman MP, Cardon G, et al. World Health Organization 2020 guidelines on physical activity and sedentary behaviour. Br J Sports Med. 2020;54(24):1451–62. https://doi.org/10.1136/bjsports-2020-102955.
Abhyankar P, Uny I, Semple K, Wane S, Hagen S, Wilkinson J, et al. Women's experiences of receiving care for pelvic organ prolapse: a qualitative study. BMC Womens Health. 2019;19(1):45. https://doi.org/10.1186/s12905-019-0741-2.
Wiegersma M, Panman C, Hesselink LC, Malmberg AGA, Berger MY, Kollen BJ, et al. Predictors of Success for Pelvic Floor Muscle Training in Pelvic Organ Prolapse. Phys Ther. 2019;99(1):109–17. https://doi.org/10.1093/ptj/pzy114.
Acknowledgement
We thank the librarians Helen Curtis, Calderdale and Huddersfield NHS Foundation Trust, UK and Anne Grete Gabrielsen, Norwegian School of Sport Sciences for assistance with search strategies and search for literature and Giovana Vesentini for extracting data for the tables controlling and setting up the reference list. Professor Suzanne Hagen, Nursing, Midwifery & Allied Health Professions Research Unit Buchanan House Glasgow Caledonian University, Glasgow, UK kindly provided insight in the references to RCTs from the Cochrane review update which is in preparation.
Funding
Open access funding provided by Norwegian School Of Sport Sciences - The Library.
Author information
Authors and Affiliations
Contributions
All authors: project development, data collection, manuscript writing and editing
Corresponding author
Ethics declarations
Conflicts of interest
None.
Additional information
Publisher’s note
Springer Nature remains neutral with regard to jurisdictional claims in published maps and institutional affiliations.
Rights and permissions
Open Access This article is licensed under a Creative Commons Attribution 4.0 International License, which permits use, sharing, adaptation, distribution and reproduction in any medium or format, as long as you give appropriate credit to the original author(s) and the source, provide a link to the Creative Commons licence, and indicate if changes were made. The images or other third party material in this article are included in the article's Creative Commons licence, unless indicated otherwise in a credit line to the material. If material is not included in the article's Creative Commons licence and your intended use is not permitted by statutory regulation or exceeds the permitted use, you will need to obtain permission directly from the copyright holder. To view a copy of this licence, visit http://creativecommons.org/licenses/by/4.0/.
About this article
Cite this article
Bø, K., Anglès-Acedo, S., Batra, A. et al. International urogynecology consultation chapter 3 committee 2; conservative treatment of patient with pelvic organ prolapse: Pelvic floor muscle training. Int Urogynecol J 33, 2633–2667 (2022). https://doi.org/10.1007/s00192-022-05324-0
Accepted:
Published:
Issue Date:
DOI: https://doi.org/10.1007/s00192-022-05324-0