Abstract
Purpose
To systematically review the literature on the association between knee joint line obliquity (KJLO) and clinical outcome after high tibial osteotomy (HTO) for medial knee osteoarthritis and summarize the KJLO cut-off value used when studying this association.
Methods
A systematic search was conducted in three databases (PubMed, Embase, and Web of Science) on September 2022, updated on February 2023. Eligible studies describing postoperative KJLO in relation to clinical outcome after HTO for medial knee osteoarthritis were included. Nonpatient studies and conference abstracts without full-text were excluded. Two independent reviewers assessed title, abstract and full-text based on the inclusion and exclusion criteria. The modified Downs and Black checklist was used to assess the methodological quality of each included study.
Results
Of the seventeen studies included, three had good methodological quality, thirteen fair quality, and one had poor quality. Conflicting findings were shown on the associations between postoperative KJLO and patient-reported outcome, medial knee cartilage regeneration, and 10-year surgical survival in sixteen studies. Three good-quality studies found no significant differences in lateral knee cartilage degeneration between postoperative medial proximal tibial angle > 95° and < 95°. Joint line orientation angles by the tibial plateau of 4° and 6°, joint line orientation angle by the middle knee joint space of 5°, medial proximal tibial angles of 95° and 98°, and Mikulicz joint line angle of 94° were KJLO cut-off values used in the included studies.
Conclusion
Based on current evidence, the actual association between postoperative KJLO and clinical consequences after HTO for medial knee osteoarthritis cannot be ascertained. The clinical relevance of KJLO after HTO remains controversial.
Level of evidence
IV.
Similar content being viewed by others
Avoid common mistakes on your manuscript.
Introduction
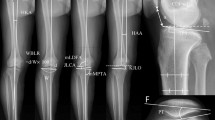
As a bony correction technique performed at the proximal tibia, HTO can result in knee joint line obliquity (KJLO) increase, particularly when there is a large correction [1, 4, 35]. Different KJLO measurement methods of joint line orientation angle by the femoral condyles (JLOAF), joint line orientation angle by the middle knee joint space (JLOAM), joint line orientation angle by the tibial plateau (JLOAT), medial proximal tibial angle (MPTA), and Mikulicz joint line angle (MJLA) are described in literature (Fig. 1) [1, 4, 35, 53].
KJLO measurement methods illustrated on anteroposterior long-standing radiograph. A Joint line orientation angle by the tibial plateau (JLOAT) [48]: angle between the proximal tibial line and the horizontal line; B Joint line orientation angle by the middle knee joint space (JLOAM) [35]: angle between the middle knee joint space line and the horizontal line; C Joint line orientation angle by the femoral condyles (JLOAF) [1]: angle between the distal femoral line and the horizontal line; D Medial proximal tibial angle (MPTA) [53]: medial angle between the proximal tibial line and the tibial mechanical axis; E Mikulicz joint line angle (MJLA) [53]: medial angle between the middle knee joint space line and the weight-bearing line
To the best of our knowledge, there is no published consensus on whether to take a suspected excessive postoperative KJLO into consideration during osteotomy planning. Some studies suggest a double-level osteotomy when there is a predicted excessive postoperative KJLO during HTO planning, which involves a postoperative MPTA > 95° [2, 29, 43] or a postoperative JLOAT > 6° [59]. Another study suggests that HTO is still justifiable despite a predicted slightly excessive postoperative KJLO [14]. A review of current evidence is therefore necessary, with a focus on associations between postoperative KJLO and patient-reported outcome, status of knee ligament and cartilage, radiological outcomes, surgical survival, and outcome of gait analysis or physical function after HTO.
The aim of this paper is to systematically review the literature on the association between KJLO and clinical outcome after HTO for medial knee osteoarthritis and summarize the KJLO cut-off value used when studying this association. We hypothesize that an increase of KJLO after HTO has adverse influences on clinical outcome.
Methods
This systematic review followed the Preferred Reporting Items for Systematic Reviews and Meta-analyses (PRISMA) guideline [49]. The protocol of this review was preregistered in the PROSPERO registry with no. CRD42022359034.
Search strategy
A “PEO” method was used to develop the search strategy for this systematic review [42]. The population (P) was defined as patients who underwent HTO for medial knee osteoarthritis. Exposure (E) was defined as postoperative knee joint line obliquity. Outcome (O) was defined as the association between postoperative KJLO and certain clinical outcomes that include the score on a patient-reported outcome measure, assessment of knee cartilage and ligament status, radiological outcome, outcome of gait analysis or physical function, and surgical survival (revision to knee arthroplasty).
Search strategies used in three databases, PubMed, Embase, and Web of Science, are presented in Table 1. Articles were searched from the databases’ inception to 14 September 2022, with an updated search on 9 February 2023 for additional articles. No language restriction was used during the search.
Eligibility criteria
Eligible clinical study designs were randomized controlled trials and observational studies including cohort studies, comparative studies, case–control studies and case series (≥ 10 cases). Clinical studies were included in this review when KJLO was measured and the clinical outcome in relation to this KJLO was reported. Nonpatient studies and conference abstracts without full-text were excluded.
Identification of eligible studies
Endnote software (version 20, Clarivate) was used to exclude duplicates. Based on the predefined eligible criteria, two reviewers (TX and HV) independently screened the studies through three ordered rounds: first titles, then abstracts, and last full-texts. Disagreement between two reviewers was resolved by discussion. If no consensus was achieved, a third reviewer was consulted (IA).
Data extraction
One reviewer (TX) extracted the following data from included studies: publication year, study location, study design, included knees, mean patient age, mean follow-up time, HTO technique used, KJLO change after HTO, KJLO cut-off value used, and KJLO-related clinical outcome.
Methodological quality
The modified Downs and Black checklist was used to assess the methodological quality of each included study, with an assessment of study reporting, external and internal validity, and statistical power of patient sample size [9, 61]. Methodological quality was graded by the overall score obtained: excellent (26–28), good (20–25), fair (15–19), and poor (≤ 14) [17, 31]. Two independent reviewers evaluated the methodological quality (TX and HV). Disagreements between the two reviewers were solved by discussion, and a third reviewer was consulted when necessary (IA).
Results
The article selection procedure based on the PRISMA guideline is presented in Fig. 2. A total of seventeen clinical observational studies were included: thirteen cohort studies, three case series, and one case–control study. Fifteen studies performed medial opening wedge HTO, and two studies performed lateral closing wedge HTO. Article publication years and study locations are specified in Fig. 3. The extracted information is depicted in Table 2.
Quality assessment of the included studies
The methodological quality of each included study is presented in Table 3 [1, 4, 14, 15, 24, 26,27,28,29, 32, 35, 37, 48, 53, 55, 58, 59]. Three studies were rated as good quality, thirteen as fair quality, and one study as poor quality.
Assessment tools
Patient-reported outcome was assessed by nine different tools in fourteen studies [1, 14, 15, 24, 27, 29, 32, 35, 37, 48, 53, 55, 58, 59] (Table 4). Knee cartilage was assessed arthroscopically in four studies [1, 14, 26, 27] and by medial joint space width (mJSW) in one study [59].
Patient-reported outcome
Of the eight included studies assessing the association between postoperative MPTA and postoperative patient-reported outcome, one good-quality study showed inferior Knee injury and Osteoarthritis Outcome Score (KOOS) (sports and recreation) [1], and two fair-quality studies showed inferior Knee Society Score (KSS) (function), Short-Form 36, and International Knee Document Committee (IKDC) scores [29, 55] when postoperative MPTA was > 95°. Two good-quality studies and two fair-quality studies presented no significant differences in KOOS, KSS, Western Ontario and McMaster Universities Osteoarthritis Index score, Japanese Orthopaedic Association Score, Oxford Knee Score, and Hospital for Special Surgery Knee Score between postoperative MPTA > 95° and < 95° [14, 27, 53, 58], and one fair-quality study presented no significant difference in KSS between postoperative MPTA ≥ 98° and ≤ 95° [15].
Out of five fair-quality included studies assessing the association between postoperative JLOAT and postoperative patient-reported outcome, one study showed that postoperative JLOAT ≥ 4° and ≥ 6° were both significant predictors for inferior KSS [59]; another study presented no significant difference in KSS between postoperative JLOAT > 4° and < 4° [48]. A third study stated that postoperative JLOAT was weakly negatively correlated with KOOS and negligibly correlated with KSS [32]; a fourth study showed negligible correlation between postoperative JLOAT and IKDC score [37]. The last of these studies showed weak negative correlation between JLOAT increase post-HTO and postoperative KOOS (pain) [24].
Knee cartilage
Three good-quality studies showed no significant difference arthroscopically in medial knee cartilage regeneration and lateral knee cartilage degeneration post-HTO between postoperative MPTA > 95° and < 95° [1, 14, 27]. One fair-quality study showed arthroscopically that postoperative JLOAM > 5° was one of the risk factors leading to inferior medial knee cartilage regeneration [26]. Another fair-quality study showed that postoperative JLOAT ≥ 6° was a significant predictor of mJSW narrowing, as assessed by a Rosenberg view X-ray [59].
Surgical survival
One fair-quality study showed no significant difference in 10-year surgical survival rate between postoperative MPTA > 95° and ≤ 95° [55]. One poor-quality study showed that a postoperative JLOAT < 4° was one of the criteria for achieving 10-year surgical survival after HTO [4].
Discussion
The most important finding of this review is that there is conflicting evidence on the associations between postoperative KJLO and patient-reported outcome, knee cartilage regeneration, and 10-year surgical survival. Six different KJLO cut-off values are used when studying these associations. Only three of the seventeen included studies meet the criteria of good methodological quality.
The evidence about the association between postoperative KJLO and patient-reported outcome after HTO is conflicting, due to the presence of both supportive and opposite findings on whether a suspected excessive postoperative KJLO is significantly related to an inferior patient-reported outcome. Regarding the supportive findings [1, 29, 55, 59], the patient-reported outcome difference between suspected excessive postoperative KJLO and normal postoperative KJLO also exceeds the published minimal clinically important difference of the assessment tool used [11, 21, 38, 45, 51]. A possible explanation for the current conflicting findings could be that most included studies do not properly match the covariates that can affect postoperative patient-reported outcomes when comparing between suspected excessive postoperative KJLO and normal postoperative KJLO patient groups. This can involve covariates such as patient age, gender, body mass index, preoperative patient-reported outcome, degree of preoperative varus alignment, amount of correction, and postoperative follow-up time [13, 25, 30, 63]. In one study the between-group covariate matching is incorporated into the study design using the propensity score-matching method [27], yet some important covariates such as preoperative patient-reported outcome and amount of correction are not used for propensity score-matching. Some supportive findings should be re-interpreted: Kubota et al. [32] concluded there was a significant correlation between postoperative KJLO and postoperative KOOS (pain, activity daily living, sports and recreation), as the p value was < 0.05; however, the correlation coefficient magnitude between postoperative KJLO and the postoperative subscales can be classified as weak, which should be the main outcome rather than whether the correlation is significant or not. Future research should have a better consideration of the covariates that can affect postoperative patient-reported outcome.
The association between postoperative KJLO and medial knee cartilage regeneration after HTO is conflicting, and postoperative KJLO seems not to affect lateral knee cartilage deterioration. A finite element analysis study reported that excessive KJLO (MPTA > 95°) could result in a rapid increase of shear stress in the knee joint [43]. In vitro research shows that abnormal shear stress could induce inflammation and apoptosis of chondrocytes [6, 16, 65], decreasing chondrocyte viability [62]; this may negatively influence cartilage status. However, the above finite element analysis and in vitro findings can only be partially confirmed in clinical research. When comparing between patients with postoperative MPTA > 95° and < 95°, there is no significant difference arthroscopically in medial knee cartilage regeneration and lateral knee cartilage degeneration at mean follow-ups at 1/1.5 years [1, 14, 27]. However, JLOAM > 5° is one of the arthroscopic risk factors for inferior medial knee cartilage regeneration at mean follow-up of 1.9 years, along with the other risk factors which include preoperative severe knee osteoarthritis and a medial knee cartilage bipolar lesion [26]. This conflicting finding may be due to the difference in KJLO measurement method and cut-off value used, as well as the time interval between HTO and follow-up arthroscopy, where a longer time interval benefits medial cartilage regeneration [1, 23]. Also, the difference of lateral knee cartilage degeneration between excessive and normal postoperative KJLO may be evident in a long-term follow-up [1, 14, 27]. Furthermore, a previous study used mJSW on X-ray to assess medial knee cartilage and concluded that JLOAT ≥ 6° was a significant predictor of mJSW narrowing after HTO [59]. However, what the mJSW truly represents remains controversial in recent studies: One study reported that mJSW correlated moderately with knee cartilage thickness on magnetic resonance imaging (MRI) [57], whereas another study reported that mJSW change after HTO reflected the weight-bearing line ratio change on X-ray instead of cartilage regeneration arthroscopically [41]. It is therefore better to use MRI or arthroscopy than mJSW to assess knee cartilage status.
The evidence for the association between suspected excessive postoperative KJLO and long-term surgical survival (revision to knee arthroplasty) after HTO is conflicting. To achieve 10-year surgical survival after HTO, one study stated that patients should have postoperative JLOAT < 4°, postoperative 0–6° valgus alignment, and adequate medial knee loading [4]. Another study found no significant difference in 10-year surgical survival rate between postoperative MPTA > 95° and ≤ 95° patient groups [55]; however, whether between-group covariates were taken into account is not specified. Covariates of patient age, knee cartilage condition, preoperative knee osteoarthritis severity, and postoperative alignment could all affect long-term surgical survival after HTO [10, 22], which may further influence such between-group surgical survival comparisons and the conclusions. Furthermore, although longer operation time has already been described for total knee arthroplasty following HTO than primary arthroplasty [60], an excessive KJLO after HTO might further increase technical challenges when there is a need of conversion to total knee arthroplasty, such as difficulties in restoring soft tissue and ligament balance, joint line height, and mechanics and kinematics of tibiofemoral and patellofemoral joints. In some cases, a stemmed augmented tibial component may be required. Computer assisted three-dimensional planning and simulation may help overcome these difficulties.
There is limited clinical evidence that a KJLO increase after HTO negatively influences the anterior cruciate ligament (ACL), as shown by MRI and arthroscopy in one fair-quality study [28]. Possibly explaining this finding, a previous cadaver study reported that KJLO increase is significantly related to femorotibial subluxation [64]; Ogawa et al. [46, 47] discussed that an abnormal femorotibial subluxation might escalate ligament tension, which might result in ACL deterioration. Not only KJLO increases but also the post-HTO posterior tibial slope increase is found to be related to ACL deterioration [28]. The tibial slope may play a more prominent role than KJLO on ACL status by influencing the ligament strain and laxity in the sagittal plane [12]. Future research could focus on how much KJLO increase is acceptable after HTO.
There is limited clinical evidence that postoperative KJLO is only weakly/negligibly correlated with postoperative physical performance (single-leg standing/timed up-and-go) and isometric muscle strength (quadriceps/hamstrings) after HTO. As discussed by Kubota et al. [32], the two physical performance tests used are too easy for patients to accomplish after HTO, which might be a reason for the weak/negligible correlation determined. A high-demand physical performance test focusing on medial knee loading might result in a better correlation. A previous study reported that postoperative KJLO can affect knee adduction moment after total knee arthroplasty [44], where the knee adduction moment during gait indicates the medial knee contact pressure [33]. Moreover, each HTO-operated patient can present a difference in preoperative KJLO, correction magnitude for targeted alignment, and preoperative physical performance and muscle strength. The influence of KJLO increase after HTO on physical performance test outcomes that determine knee loading should be investigated in future research.
As mentioned in the Introduction concerning the excessive KJLO problem after HTO, double-level osteotomy is suggested when there is a predicted postoperative MPTA > 95° or JLOAT > 6° [2, 29, 43, 59]. Yet again, whether a postoperative MPTA > 95° is associated with inferior clinical outcome after HTO remains uncertain. Also, the proposed 6° JLOAT might not be accurately measured, as the JLOAT measurement can be affected by single-leg and double-leg standing as well as by the bipedal distance used at filming [36, 50]; the patient’s standing position is not well described in the study that proposes a JLOAT of 6° as acceptable KJLO upper limit [59]. According to the present review’s findings, no postoperative KJLO cut-off value is sufficiently supported for clinical usage.
A limitation is that, due to the large variabilities in KJLO measurement methods, KJLO cut-off values, and clinical outcome assessment tools used in the included studies, a meta-analysis could not be performed. Also, there is a lack of the literature regarding the clinical effects of KJLO after double-level osteotomy and varus-producing HTO.
The strength of this systematic review lies in its investigation of the association between postoperative KJLO and clinical outcome, providing a summary of current knowledge for orthopaedic surgeons who perform HTO procedures and are concerned about postoperative KJLO. This review revealed the need of unified KJLO measurement methods and adequate covariate control for future research when assessing the association between postoperative KJLO measurements and clinical outcome.
Conclusion
Due to the conflicting and limited evidence, the actual association between postoperative KJLO and clinical consequences after HTO for medial knee osteoarthritis cannot be ascertained. The clinical relevance of KJLO after HTO remains controversial.
Data availability
The datasets generated during the current study are available from the corresponding author upon reasonable request.
Abbreviations
- ACL:
-
Anterior cruciate ligament
- HSSKS:
-
Hospital for Special Surgery Knee Score
- HTO:
-
High tibial osteotomy
- IKDC:
-
International Knee Document Committee
- JLOAF:
-
Joint line orientation angle by the femoral condyles
- JLOAM:
-
Joint line orientation angle by the middle knee joint space
- JLOAT:
-
Joint line orientation angle by the tibial plateau
- JOAS:
-
Japanese Orthopaedic Association Score
- KJLO:
-
Knee joint line obliquity
- KOOS:
-
Knee injury and Osteoarthritis Outcome Score
- KSS:
-
Knee Society Score
- MJLA:
-
Mikulicz joint line angle
- mJSW:
-
Medial joint space width
- MPTA:
-
Medial proximal tibial angle
- MRI:
-
Magnetic resonance imaging
- OKS:
-
Oxford Knee Score
- SF-36:
-
Short-Form 36
- WOMAC:
-
Western Ontario and McMaster Universities Osteoarthritis Index
References
Akamatsu Y, Kumagai K, Kobayashi H, Tsuji M, Saito T (2018) Effect of increased coronal inclination of the tibial plateau after opening-wedge high tibial osteotomy. Arthroscopy 34:2158-2169.e2152
Akamatsu Y, Nejima S, Tsuji M, Kobayashi H, Muramatsu S (2022) Joint line obliquity was maintained after double-level osteotomy, but was increased after open-wedge high tibial osteotomy. Knee Surg Sports Traumatol Arthrosc 30:688–697
Aoki Y, Yasuda K, Mikami S, Ohmoto H, Majima T, Minami A (2006) Inverted V-shaped high tibial osteotomy compared with closing-wedge high tibial osteotomy for osteoarthritis of the knee. Ten-year follow-up result. J Bone Joint Surg Br 88:1336–1340
Babis GC, An KN, Chao EY, Larson DR, Rand JA, Sim FH (2008) Upper tibia osteotomy: long term results—realignment analysis using OASIS computer software. J Orthop Sci 13:328–334
Bellamy N, Buchanan WW, Goldsmith CH, Campbell J, Stitt LW (1988) Validation study of WOMAC: a health status instrument for measuring clinically important patient relevant outcomes to antirheumatic drug therapy in patients with osteoarthritis of the hip or knee. J Rheumatol 15:1833–1840
Cheng HJ, Hsu WT, Chen CN, Li C (2020) Activation of NOTCH1 by shear force elicits immediate cytokine expression in human chondrocytes. Int J Mol Sci 21:4958
Dawson J, Fitzpatrick R, Murray D, Carr A (1998) Questionnaire on the perceptions of patients about total knee replacement. J Bone Joint Surg Br 80:63–69
Dekkers OM, Egger M, Altman DG, Vandenbroucke JP (2012) Distinguishing case series from cohort studies. Ann Intern Med 156:37–40
Downs SH, Black N (1998) The feasibility of creating a checklist for the assessment of the methodological quality both of randomised and non-randomised studies of health care interventions. J Epidemiol Community Health 52:377–384
Efe T, Ahmed G, Heyse TJ, Boudriot U, Timmesfeld N, Fuchs-Winkelmann S et al (2011) Closing-wedge high tibial osteotomy: survival and risk factor analysis at long-term follow up. BMC Musculoskelet Disord 12:46
Escobar A, Quintana JM, Bilbao A, Aróstegui I, Lafuente I, Vidaurreta I (2007) Responsiveness and clinically important differences for the WOMAC and SF-36 after total knee replacement. Osteoarthritis Cartilage 15:273–280
Feucht MJ, Mauro CS, Brucker PU, Imhoff AB, Hinterwimmer S (2013) The role of the tibial slope in sustaining and treating anterior cruciate ligament injuries. Knee Surg Sports Traumatol Arthrosc 21:134–145
Floerkemeier S, Staubli AE, Schroeter S, Goldhahn S, Lobenhoffer P (2014) Does obesity and nicotine abuse influence the outcome and complication rate after open-wedge high tibial osteotomy? A retrospective evaluation of five hundred and thirty three patients. Int Orthop 38:55–60
Goshima K, Sawaguchi T, Shigemoto K, Iwai S, Fujita K, Yamamuro Y (2019) Comparison of clinical and radiologic outcomes between normal and overcorrected medial proximal tibial angle groups after open-wedge high tibial osteotomy. Arthroscopy 35:2898-2908.e2891
Goto N, Akasaki Y, Okazaki K, Kuwashima U, Iwasaki K, Kawamura H et al (2020) The influence of post-operative knee coronal alignment parameters on long-term patient-reported outcomes after closed-wedge high tibial osteotomy. J Orthop 20:177–180
Healy ZR, Lee NH, Gao X, Goldring MB, Talalay P, Kensler TW et al (2005) Divergent responses of chondrocytes and endothelial cells to shear stress: cross-talk among COX-2, the phase 2 response, and apoptosis. Proc Natl Acad Sci U S A 102:14010–14015
Hooper P, Jutai JW, Strong G, Russell-Minda E (2008) Age-related macular degeneration and low-vision rehabilitation: a systematic review. Can J Ophthalmol 43:180–187
Insall JN, Dorr LD, Scott RD, Scott WN (1989) Rationale of the knee society clinical rating system. Clin Orthop Relat Res 248:13–14
Insall JN, Ranawat CS, Aglietti P, Shine J (1976) A comparison of four models of total knee-replacement prostheses. J Bone Joint Surg Am 58:754–765
Irrgang JJ, Anderson AF, Boland AL, Harner CD, Kurosaka M, Neyret P et al (2001) Development and validation of the international knee documentation committee subjective knee form. Am J Sports Med 29:600–613
Jacquet C, Pioger C, Khakha R, Steltzlen C, Kley K, Pujol N et al (2021) Evaluation of the “Minimal Clinically Important Difference” (MCID) of the KOOS, KSS and SF-12 scores after open-wedge high tibial osteotomy. Knee Surg Sports Traumatol Arthrosc 29:820–826
Jin C, Song EK, Santoso A, Ingale PS, Choi IS, Seon JK (2020) Survival and risk factor analysis of medial open wedge high tibial osteotomy for unicompartment knee osteoarthritis. Arthroscopy 36:535–543
Jung WH, Takeuchi R, Chun CW, Lee JS, Ha JH, Kim JH et al (2014) Second-look arthroscopic assessment of cartilage regeneration after medial opening-wedge high tibial osteotomy. Arthroscopy 30:72–79
Kawashima F, Takagi H (2022) Evaluation of postoperative orientation of the knee and ankle joint after open wedge high tibial osteotomy. Asia Pac J Sports Med Arthrosc Rehabil Technol 29:9–14
Keenan OJF, Clement ND, Nutton R, Keating JF (2019) Older age and female gender are independent predictors of early conversion to total knee arthroplasty after high tibial osteotomy. Knee 26:207–212
Kim CW, Seo SS, Lee CR, Gwak HC, Kim JH, Jung SG (2017) Factors affecting articular cartilage repair after open-wedge high tibial osteotomy. Knee 24:1099–1107
Kim GW, Kang JK, Song EK, Seon JK (2021) Increased joint obliquity after open-wedge high tibial osteotomy induces pain in the lateral compartment: a comparative analysis of the minimum 4-year follow-up outcomes using propensity score matching. Knee Surg Sports Traumatol Arthrosc 29:3495–3502
Kim JE, Won S, Jaffar MSA, Lee JI, Kim TW, Lee YS (2020) How does geometric change after open-wedge high tibial osteotomy affect anterior cruciate ligament status? Knee 27:940–948
Kim JS, Lim JK, Choi HG, Jeong HW, Park SB, Shim SJ et al (2022) Excessively increased joint-line obliquity after medial opening-wedge high tibial osteotomy is associated with inferior radiologic and clinical outcomes: what is permissible joint-line obliquity. Arthroscopy 38:1904–1915
Kim MS, Koh IJ, Choi YJ, Lee JY, In Y (2017) Differences in patient-reported outcomes between unicompartmental and total knee arthroplasties: a propensity score-matched analysis. J Arthroplasty 32:1453–1459
Korakakis V, Whiteley R, Tzavara A, Malliaropoulos N (2018) The effectiveness of extracorporeal shockwave therapy in common lower limb conditions: a systematic review including quantification of patient-rated pain reduction. Br J Sports Med 52:387–407
Kubota M, Kim Y, Sato T, Yamaguchi J, Ohno R, Kaneko K et al (2020) The actual knee function was not influenced by joint line obliquity after open-wedge high tibial osteotomy. Sicot J 6:4
Kutzner I, Trepczynski A, Heller MO, Bergmann G (2013) Knee adduction moment and medial contact force–facts about their correlation during gait. PLoS ONE 8:e81036
Laucis NC, Hays RD, Bhattacharyya T (2015) Scoring the SF-36 in orthopaedics: a brief guide. J Bone Joint Surg Am 97:1628–1634
Lee KM, Chang CB, Park MS, Kang SB, Kim TK, Chung CY (2015) Changes of knee joint and ankle joint orientations after high tibial osteotomy. Osteoarthritis Cartilage 23:232–238
Lee NK, Kim TW, Lee S, Choi YS, Kang SB, Chang CB (2022) Effect of distance between the feet on knee joint line orientation after total knee arthroplasty in standing full-limb radiographs. Knee Surg Sports Traumatol Arthrosc 30:3032–3040
Lee SJ, Kim JH, Choi W (2021) Factors related to the early outcome of medial open wedge high tibial osteotomy: coronal limb alignment affects more than cartilage degeneration state. Arch Orthop Trauma Surg 141:1339–1348
Lee WC, Kwan YH, Chong HC, Yeo SJ (2017) The minimal clinically important difference for Knee Society Clinical Rating System after total knee arthroplasty for primary osteoarthritis. Knee Surg Sports Traumatol Arthrosc 25:3354–3359
Lysholm J, Gillquist J (1982) Evaluation of knee ligament surgery results with special emphasis on use of a scoring scale. Am J Sports Med 10:150–154
Mathes T, Pieper D (2017) Clarifying the distinction between case series and cohort studies in systematic reviews of comparative studies: potential impact on body of evidence and workload. BMC Med Res Methodol 17:107
Moon HS, Choi CH, Yoo JH, Jung M, Lee TH, Byun JW et al (2021) An increase in medial joint space width after medial open-wedge high tibial osteotomy is associated with an increase in the postoperative weight-bearing line ratio rather than with cartilage regeneration: comparative analysis of patients who underwent second-look arthroscopic assessment. Arthroscopy 37:657-668.e654
Morgan RL, Whaley P, Thayer KA, Schünemann HJ (2018) Identifying the PECO: a framework for formulating good questions to explore the association of environmental and other exposures with health outcomes. Environ Int 121:1027–1031
Nakayama H, Schröter S, Yamamoto C, Iseki T, Kanto R, Kurosaka K et al (2018) Large correction in opening wedge high tibial osteotomy with resultant joint-line obliquity induces excessive shear stress on the articular cartilage. Knee Surg Sports Traumatol Arthrosc 26:1873–1878
Niki Y, Nagura T, Nagai K, Kobayashi S, Harato K (2018) Kinematically aligned total knee arthroplasty reduces knee adduction moment more than mechanically aligned total knee arthroplasty. Knee Surg Sports Traumatol Arthrosc 26:1629–1635
Nishitani K, Yamamoto Y, Furu M, Kuriyama S, Nakamura S, Ito H et al (2019) The minimum clinically important difference for the Japanese version of the new Knee Society Score (2011KSS) after total knee arthroplasty. J Orthop Sci 24:1053–1057
Ogawa H, Matsumoto K, Akiyama H (2019) ACL degeneration after an excessive increase in the medial proximal tibial angle with medial open wedge high tibial osteotomy. Knee Surg Sports Traumatol Arthrosc 27:3374–3380
Ogawa H, Matsumoto K, Akiyama H (2018) Coronal tibiofemoral subluxation is correlated to correction angle in medial opening wedge high tibial osteotomy. Knee Surg Sports Traumatol Arthrosc 26:3482–3490
Oh KJ, Ko YB, Bae JH, Yoon ST, Kim JG (2016) Analysis of knee joint line obliquity after high tibial osteotomy. J Knee Surg 29:649–657
Page MJ, McKenzie JE, Bossuyt PM, Boutron I, Hoffmann TC, Mulrow CD et al (2021) The PRISMA 2020 statement: an updated guideline for reporting systematic reviews. Int J Surg 88:105906
Paley D (2002) Principles of deformity correction. Springer Berlin, Heidelberg. https://doi.org/10.1007/978-3-642-59373-4
Patel S, Haunschild E, Gilat R, Knapik D, Evuarherhe A, Parvaresh KC et al (2021) Defining clinically significant outcomes following high tibial osteotomy with or without concomitant procedures. J Cartilage Joint Preservation 1:100014
Roos EM, Lohmander LS (2003) The knee injury and osteoarthritis outcome score (KOOS): from joint injury to osteoarthritis. Health Qual Life Outcomes 1:64
Rosso F, Rossi R, Cantivalli A, Pilone C, Bonasia DE (2022) Joint line obliquity does not affect the outcomes of opening wedge high tibial osteotomy at an average 10-year follow-up. Am J Sports Med 50:461–470
Schober P, Boer C, Schwarte LA (2018) Correlation coefficients: appropriate use and interpretation. Anesth Analg 126:1763–1768
Schuster P, Geßlein M, Schlumberger M, Mayer P, Mayr R, Oremek D et al (2018) Ten-year results of medial open-wedge high tibial osteotomy and chondral resurfacing in severe medial osteoarthritis and varus malalignment. Am J Sports Med 46:1362–1370
Scuderi GR, Bourne RB, Noble PC, Benjamin JB, Lonner JH, Scott WN (2012) The new knee society knee scoring system. Clin Orthop Relat Res 470:3–19
Sekiya I, Sasaki S, Miura Y, Aoki H, Katano H, Okanouchi N et al (2022) Medial tibial osteophyte width strongly reflects medial meniscus extrusion distance and medial joint space width moderately reflects cartilage thickness in knee radiographs. J Magn Reson Imaging 56:824–834
Sohn S, Koh IJ, Kim MS, In Y (2022) Risk factors and preventive strategy for excessive coronal inclination of tibial plateau following medial opening-wedge high tibial osteotomy. Arch Orthop Trauma Surg 142:561–569
Song JH, Bin SI, Kim JM, Lee BS (2020) What is an acceptable limit of joint-line obliquity after medial open wedge high tibial osteotomy? Analysis based on midterm results. Am J Sports Med 48:3028–3035
Sun X, Wang J, Su Z (2020) A meta-analysis of total knee arthroplasty following high tibial osteotomy versus primary total knee arthroplasty. Arch Orthop Trauma Surg 140:527–535
Trac MH, McArthur E, Jandoc R, Dixon SN, Nash DM, Hackam DG et al (2016) Macrolide antibiotics and the risk of ventricular arrhythmia in older adults. CMAJ 188:E120-e129
Trevino RL, Pacione CA, Malfait AM, Chubinskaya S, Wimmer MA (2017) Development of a cartilage shear-damage model to investigate the impact of surface injury on chondrocytes and extracellular matrix wear. Cartilage 8:444–455
van Wulfften Palthe AFY, Clement ND, Temmerman OPP, Burger BJ (2018) Survival and functional outcome of high tibial osteotomy for medial knee osteoarthritis: a 10–20-year cohort study. Eur J Orthop Surg Traumatol 28:1381–1389
Wang D, Willinger L, Athwal KK, Williams A, Amis AA (2021) Knee joint line obliquity causes tibiofemoral subluxation that alters contact areas and meniscal loading. Am J Sports Med 49:2351–2360
Wang P, Zhu F, Tong Z, Konstantopoulos K (2011) Response of chondrocytes to shear stress: antagonistic effects of the binding partners Toll-like receptor 4 and caveolin-1. FASEB J 25:3401–3415
Funding
There is no funding.
Author information
Authors and Affiliations
Contributions
HV, RB, IA and TX contributed to the concept of this systematic review. TX developed the search strategy, conducted the database search, assessed the methodological quality and drafted the manuscript. HV conducted the database search, assessed the methodological quality and revised the manuscript. IA and RB revised the manuscript. All authors approved the final manuscript.
Corresponding author
Ethics declarations
Conflict of interest
The authors declare that they have no conflict of interest.
Ethical approval
This article does not contain any studies with human participants or animals conducted by any of the authors.
Informed consent
Informed consent is not applicable for this systematic review.
Additional information
Publisher's Note
Springer Nature remains neutral with regard to jurisdictional claims in published maps and institutional affiliations.
Rights and permissions
Open Access This article is licensed under a Creative Commons Attribution 4.0 International License, which permits use, sharing, adaptation, distribution and reproduction in any medium or format, as long as you give appropriate credit to the original author(s) and the source, provide a link to the Creative Commons licence, and indicate if changes were made. The images or other third party material in this article are included in the article's Creative Commons licence, unless indicated otherwise in a credit line to the material. If material is not included in the article's Creative Commons licence and your intended use is not permitted by statutory regulation or exceeds the permitted use, you will need to obtain permission directly from the copyright holder. To view a copy of this licence, visit http://creativecommons.org/licenses/by/4.0/.
About this article
Cite this article
Xie, T., Brouwer, R.W., van den Akker-Scheek, I. et al. Clinical relevance of joint line obliquity after high tibial osteotomy for medial knee osteoarthritis remains controversial: a systematic review. Knee Surg Sports Traumatol Arthrosc 31, 4355–4367 (2023). https://doi.org/10.1007/s00167-023-07486-w
Received:
Accepted:
Published:
Issue Date:
DOI: https://doi.org/10.1007/s00167-023-07486-w