Abstract
Dynamic brain activity requires timely communications between the brain parenchyma and circulating blood. Brain–blood communication is facilitated by intricate networks of brain vasculature, which display striking heterogeneity in structure and function. This vascular cell heterogeneity in the brain is fundamental to mediating diverse brain functions and has long been recognized. However, the molecular basis of this biological phenomenon has only recently begun to be elucidated. Over the past century, various animal species and in vitro systems have contributed to the accumulation of our fundamental and phylogenetic knowledge about brain vasculature, collectively advancing this research field. Historically, dye tracer and microscopic observations have provided valuable insights into the anatomical and functional properties of vasculature across the brain, and these techniques remain an important approach. Additionally, recent advances in molecular genetics and omics technologies have revealed significant molecular heterogeneity within brain endothelial and perivascular cell types. The combination of these conventional and modern approaches has enabled us to identify phenotypic differences between healthy and abnormal conditions at the single-cell level. Accordingly, our understanding of brain vascular cell states during physiological, pathological, and aging processes has rapidly expanded. In this review, we summarize major historical advances and current knowledge on blood endothelial cell heterogeneity in the brain, and discuss important unsolved questions in the field.
Similar content being viewed by others
Avoid common mistakes on your manuscript.
Introduction
Throughout the body, blood vessels deliver oxygen and nutrients while removing metabolic wastes. In the brain, continuous and coordinated blood supply and waste clearance ensure the constant engagement of brain cells in processing enormous amounts of environmental stimuli and executing commands. To meet the high energy demands of the brain, an elaborate network of blood vessels is formed during development and maintained afterwards. Brain vasculature is organized in a specialized manner to support the diverse functions of the brain while protecting it from harmful blood-borne factors [1, 2]. Similar to peripheral blood vessels, vascular endothelial cells (vECs), the innermost layer of blood vessels, are covered by perivascular cells, such as smooth muscle cells and pericytes, to build functional brain vasculature. A notable difference in the brain as compared to other tissues is that vascular cells form close associations with neurons and glial cells to develop the neurovascular unit (NVU)—a brain–vascular interface where the blood–brain barrier (BBB) forms to limit cellular and molecular transport into the brain parenchyma [3, 4]. Most blood vessels in the brain establish this semi-permeable barrier, while others lack BBB properties and instead develop more permeable (fenestrated) phenotypes [5, 6]. Regardless of this heterogeneity in barrier properties, blood vECs in the brain are broadly classified into three types based on structural, molecular, and functional features: arterial, venous, and capillary endothelium [7,8,9]. Arterial and venous ECs share multiple conserved markers between the brain and other organs, while more prominent transcriptional heterogeneity is noted for capillary ECs [10]. A greater extent of organotypic features at the level of capillaries along the arterial–capillary–venous axis raises the question of how endothelial phenotypes are uniquely specified along this axis to meet organ-specific needs. However, the mechanisms by which brain vECs are specified into distinct subtypes within an interconnected brain vascular network have been understudied, and therefore remain unclear.
Across species, brain barriers are critical interfaces between the brain parenchyma and circulating blood [11,12,13,14,15]. Thus, disruptions in barrier properties of brain vasculature can be detrimental to brain health. For instance, current evidence has illuminated age-related changes in brain vascular structure and function. Declines in capillary density, reduced angiogenic potentials, decreased blood flow, impaired barrier properties, and vascular hypoperfusion are all hallmarks of aging brains [16,17,18]. These age-induced vascular declines, along with increased BBB permeability, can trigger neuroinflammation, which may lead to neurodegeneration and subsequent neurological deficits [19, 20]. A recent study suggests that counteracting the insufficiency of vascular endothelial growth factor (VEGF) signaling that occurs as animals age may prevent these vascular declines, thereby promoting healthy aging and extended life spans [21]. Other studies have proposed that age-induced shifts in endothelial transcellular transport machinery [22] and increased senescence in brain vECs [23] are potential underlying mechanisms of the endothelial dysfunction that causes BBB breakdown [22, 23]. However, it remains unknown whether aging has a specific or global impact on distinct subtypes of brain vECs, and which structural and functional changes individual vEC subtypes experience with aging.
BBB breakdown is not only observed during brain aging, but it has also been documented during the progression of numerous neurological diseases, including Alzheimer’s disease (AD) and multiple sclerosis (MS) [24, 25]. Hence, therapeutic interventions which could mitigate BBB dysfunction have been pursued as promising treatment options to prevent the progression of these disorders [26,27,28]. For example, a recent study demonstrates that genetically engineered Wnt7 ligands, which are crucial for BBB integrity, can prevent BBB breakdown and disease progression in several neurological disease models, illuminating their pharmaceutical potential to protect BBB function in both aged and neurological disease states [26]. However, in light of studies showing that forced activation of canonical Wnt/β-catenin signaling in fenestrated brain vECs can partially convert them into a BBB state [29, 30], it remains unclear how BBB restoration therapies may affect physiological function of fenestrated brain vECs. A deeper understanding of brain vEC subtype dysfunction and restoration will help develop vEC type-specific vascular therapies for neurological disorders.
The purpose of this review is to provide an overview of the major advances in the field of brain vascular biology, thereby clarifying our current knowledge and setting the ground for future research. This review focuses on covering topics related to the heterogeneous nature of brain blood vECs and does not describe in great detail topics that have been thoroughly reviewed elsewhere, including BBB cell biology, physiology, and pathology [6, 25, 31,32,33,34,35].
Heterogeneous permeability, anatomy, and transcriptional profiling of brain endothelial cells: from historical observations to current perspectives
The first evidence of brain barrier properties came from dye injection studies in embryos [36,37,38,39]. Vital dyes such as trypan red, Evans blue, methylene blue, and trypan blue were injected into embryos of different species, including rodents, rabbits, dogs, cats, guinea pigs, and chicks [36, 37, 39, 40]. These dyes stained almost all tissues throughout the body, but they were excluded from the cerebrospinal fluid and most parts of the central nervous system (CNS). Later studies discovered that the lack of staining in the brain was due to the barrier properties of brain vECs, marking the identification of the endothelial BBB [41,42,43]. Conversely, there are small regions of the brain localized in close proximity to the midline brain ventricular systems that were stained after vital dye injections [38, 39, 44,45,46]. These stained brain regions were the choroid plexuses (CPs) and circumventricular organs (CVOs), named by Helmut Hofer in 1958 [47].
The CVOs include the subcommissural organ (SCO), organum vasculosum of the lamina terminalis (OVLT), subfornical organ (SFO), median eminence (ME), area postrema (AP), pineal gland (PG), and neurohypophysis (NH) [5, 48]. All CVOs contain neural tissues responsible for neuroendocrine function. In contrast, the CPs do not contain a neural tissue, thus they are not typically classified as CVOs. In both the CPs and CVOs, capillary networks lack the BBB and tight junctions that create a paracellular barrier in vECs, permitting high vascular permeability. These structural and functional features are in stark contrast to the limited permeability of those that form the BBB in the rest of the brain. The exception to this high vascular permeability is the SCO which does not form fenestrated capillaries [49]. Previous studies noted vascular permeability differences between the sensory and secretory CVOs in the adult mouse brain [50, 51]. In these studies, the authors used tracers of various molecular masses and observed different degrees of extravascular leakage and diffusion of these tracers across and within the CVOs, indicating that vasculature in each CVO displays unique barrier properties [50, 51]. Tight junction protein ZO-1 immunolabeling displays discrete protein localization patterns associated with vECs across the CVOs, providing additional evidence of heterogeneous vEC barrier properties in the CVOs [52].
Ultrastructural analyses using electron microscopy have been the gold standard to date for characterization of vEC anatomical structures. Electron microscopic studies in the 1960s revealed the presence of specialized tight junctions in vECs of the cerebral cortex that form the BBB [41, 42, 53]. In the late 1900s, studies identified the presence of endothelial fenestrae in the NH [54, 55], the AP [56, 57], the PG [58, 59], the SFO [60, 61], the OVLT [62, 63], the ME [54, 64, 65], and the CPs [66, 67]. Additionally, electron microscopic studies in some of these CVOs suggest that the number of endothelial fenestrae increases during development following vessel formation [54, 55, 65, 67], indicating that the induction of endothelial fenestrations takes place progressively after vessel formation.
The evolution of DNA sequencing and genome editing technologies since the late 1900s has facilitated molecular genetic studies in a variety of model organisms. Besides mammals, zebrafish are an excellent example of an emerging model organism that exhibits barrier and non-barrier properties across the brain, similar to mammals [13, 68, 69]. Moreover, the well-conserved anatomical features of resident cell types and endothelial fenestrations in the CVOs and CPs have been documented between mammals and zebrafish [48, 70,71,72,73]. The fruit fly, Drosophila melanogaster, has also recently emerged as a genetic model to study BBB biology [12, 74], although it is unclear whether or not this organism possesses fenestrated brain vECs. The use of a range of model organisms has compensated for the limitations of each individual organism, and allows insights into evolutionarily conserved mechanisms of brain barrier operations. Comparative anatomy and function of BBB and fenestrated vECs between the human, mouse, and zebrafish brain are illustrated in Fig. 1.
Comparative anatomy and function of BBB and fenestrated vECs between human, mouse, and zebrafish. A Schematic diagrams of the midline sagittal views of the brain in human, mouse, and zebrafish, indicating the locations of the CPs (blue) and CVOs (green). B Representative anatomical and functional features of BBB and fenestrated endothelium. C Schematic diagrams of the unique anatomical and functional features of BBB (left two panels) and fenestrated (right two panels) endothelium listed in B. AJs adherens junctions, AP area postrema, BBB blood–brain barrier, CB cerebellum, CC cerebral cortex, CP choroid plexus, CVOs circumventricular organs, ME median eminence, NH neurohypophysis, OB olfactory bulb, OT optic tectum, OVLT organum vasculosum of the lamina terminalis, PG pineal gland, SCO subcommissural organ, SFO subfornical organ, TC telencephalon, vECs vascular endothelial cells
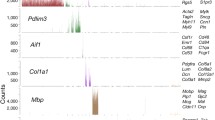
Most recently, cutting-edge next-generation sequencing platforms have offered genome-wide gene expression profiling at a wide range of sample scales and cellular resolutions. For instance, bulk transcriptomic analyses of vECs isolated from different organs using microarray and RNA-seq technologies have identified organ-specific, endothelial transcriptional signatures, including those unique to the brain [75,76,77,78,79]. Furthermore, single-cell RNA sequencing (scRNA-seq) of adult mouse and human brain vECs revealed gradual transcriptional changes along the artery–capillary–vein axis, a phenomenon known as zonation (Fig. 2) [9, 10, 80,81,82]. Even greater transcriptional differences were noted between BBB and fenestrated vECs [10]. Unsupervised clustering of the scRNA-seq data obtained from male and female adult mouse brain vECs revealed sex differences in brain endothelial cell transcriptomes [83, 84], indicating that sex is a crucial factor influencing transcriptional heterogeneity in brain vECs. These technologies have begun to be applied to the generation of brain vEC transcriptomes in many different contexts, which are discussed in later sections.
Embryonic origins of brain endothelial cells
The initial steps of vascular development take place during gastrulation as mesodermal progenitors commit to an endothelial fate [85, 86]. vECs have been shown to derive from both the lateral plate mesoderm and the paraxial mesoderm (also known as the presomitic mesoderm) in zebrafish [87,88,89], chicks [90,91,92], and mice [93,94,95]. It was long believed that after the de novo formation of a primitive vascular network, new blood vessels arise exclusively by sprouting from pre-existing endothelial cells via angiogenesis [96, 97]. However, a recent study identified yolk sac-derived erythro-myeloid progenitors (EMPs) as another source of brain vECs in mice [98], challenging the current dogma that embryonic vessels expand solely by the proliferation of pre-existing endothelial cells. These findings have become controversial after a separate study found no evidence for the contribution of EMPs to brain vasculature using similar murine genetic tools [99]. It is presently unclear whether ECs derived from different embryonic origins are functionally distinct, or preferentially contribute to different brain vascular beds.
Previous studies in zebrafish indicated that vECs in the head derive from the anterior lateral plate mesoderm (ALPM) while those in the trunk and tail originate from the posterior lateral plate mesoderm [100,101,102]. A recent study employing retrospective cell-lineage tracing via light-sheet fluorescence microscopy implied that the dorsal–anterior side of the gastrula, early embryonic cell populations present even before the ALPM forms, is the major origin of vECs in the zebrafish head [102].
Despite these advances, how distinct brain vEC subtypes are specified and how they develop lineages from embryonic origins remain unanswered. Single-cell resolution fate mapping of whole brain vECs using a combination of lineage tracing, clonal analysis, time-lapse cell tracking, and omics approaches will help reveal vEC lineage trajectories from embryonic origins, filling this knowledge gap.
Molecular and structural signatures of brain endothelial cell types
The BBB represents an evolutionarily conserved, highly selective separation at the interface between the circulatory system and brain parenchyma. To limit paracellular and transcellular molecular transport, BBB vECs establish a unique physical barrier characterized by the presence of tight junctions, an extensive transport machinery, and restricted transcytosis [25, 33, 34]. Additionally, the expression of leukocyte adhesion molecules in BBB vECs is maintained at low levels to limit the entry of immune cells into the brain parenchyma [25, 34]. Various isoforms of tight junction proteins belonging to the claudin family are expressed in brain vECs [103]; however, Claudin-5 is the most abundant claudin [103, 104], and its localization at BBB endothelial membranes and cell junctions is conserved across vertebrates [103, 105,106,107]. Conversely, Claudin-5 expression is undetectable in fenestrated brain vECs [29, 30, 73, 106, 108]. Thus, Claudin-5 has been used as a specific marker for BBB vECs. Other well-established specific markers for BBB vECs include the glucose transporter GLUT1, the docosahexaenoic acid transporter MFSD2A, the transcription factor LEF1, the tight junction proteins Occludin and ZO1, and the multi-drug resistance pump MDR1 [29]. The BBB vEC-specific expression of these genes relative to fenestrated brain vECs is also supported by recent transcriptomic data [29].
Plasmalemma vesicle-associated protein (PLVAP) is an endothelial cell-specific protein, and the only known molecular component of fenestral diaphragms and stomatal diaphragms of caveolae and trans-endothelial channels [109,110,111]. Fenestrae and trans-endothelial channels are transcellular pores that allow rapid exchange of molecules [111], while caveolae are spherical invaginations of the plasma membrane that play a role in transcytosis, the vesicular transcellular transport of macromolecules [112, 113]. Once vasculature becomes mature, PLVAP expression is restricted to fenestrated vECs in the brain, making it a unique molecular signature for these cells [10, 29, 72, 73]. PLVAP has also been implicated in controlling angiogenesis and immune cell trafficking in addition to its functions as a regulator of trans-endothelial molecular transport and vascular permeability via the formation of fenestral and stomatal diaphragms [72, 110, 111]. Inactivation and forced activation of endothelial-specific β-catenin in mice suggest a model whereby active β-catenin signaling suppresses PLVAP expression in brain vECs to limit their permeability, thereby establishing the BBB [29, 30, 114].
Over the past decades, studies have revealed that eliminating the unique molecular component(s) underlying BBB or fenestrated vEC properties leads to impaired vascular development and/or integrity. For example, Claudin-5 deficiency in mice resulted in vascular leakage of small molecular tracers in the brain, while endothelial tight junctions at the BBB were largely preserved [115]. Additionally, recent studies showed that haploinsufficiency or endothelial-specific deletion of GLUT1 in mice leads to impaired angiogenesis and diminished vascular complexity in the thalamus [116] and the cerebral cortex [117], in addition to reduced pericyte coverage resulting in increased BBB leakage [118, 119]. Lastly, in mice and zebrafish deficient for PLVAP or its zebrafish ortholog, impaired formation of fenestral and stomatal diaphragms led to excessive or accelerated transcellular transport of blood-borne proteins through fenestrated vasculature [72, 120, 121].
Cellular and molecular control of brain endothelial acquisition of unique properties
Over the last two decades, substantial progress has been made with regards to our understanding of the molecular mechanisms governing brain vascularization and endothelial cells’ acquisition of BBB and fenestrated properties. Brain vascularization is initiated by angiogenic sprouting from the peri-neural vascular plexus (PNVP), a primitive vascular network that covers the entire surface of the neural tube, into the brain parenchyma [122,123,124]. Paracrine VEGF-A signaling derived from the developing CNS is critical for PNVP formation and subsequent blood vessel invasion, branching, and density in neural tubes across multiple vertebrate species [125,126,127,128,129,130]. Genetic loss of heparin-binding VEGF-A isoforms (VEGF120/120 mice that are genetically engineered to produce solely the soluble isoform VEGF-A120) led to a significant reduction in vessel branch points and complexity in the brain [131], demonstrating VEGF isoform-specific control of brain vascularization.
Classical chick-quail transplantation experiments suggested that BBB barrier properties are not intrinsic to brain vECs, but rather, they are induced and maintained by neural environmental signals [132, 133]. These studies showed that neural tissues transplanted into the coelomic cavities are sufficient to induce BBB characteristics in mesenteric vessels, whereas brain vessels do not display BBB properties when invading into somite tissues transplanted into the brain ventricles [132, 133]. Isolated brain vECs in culture exhibit a rapid loss of BBB-specific transcripts and chromatin features [134], supporting the notion that neural environmental signals are necessary for vECs to maintain BBB properties.
Development and maintenance of endothelial BBB properties
Wnt/β-catenin signaling Canonical Wnt/β-catenin signaling has been well established as a central regulator of brain angiogenesis, as well as of the induction and maintenance of endothelial BBB properties. Transgenic Wnt/β-catenin reporter mice demonstrated the specific activation of Wnt/β-catenin signaling in CNS vECs [114, 135, 136], but not in those of other organs [135]. Recent work revealed that β-catenin activities in fenestrated vECs of the CPs and CVOs are maintained at much lower levels than in those forming the BBB in both mouse and zebrafish models [29, 30]. Mechanistically, endothelial cell-specific deletion of β-catenin in developing mice results in a drastic reduction of BBB-specific proteins, including Claudin-5 and GLUT1, while leading to increased expression of the fenestrated vEC marker PLVAP [114, 135, 136]. Conversely, endothelial cell-specific β-catenin stabilization leads to the opposite outcomes in these gene/protein expressions [114]. Moreover, β-catenin stabilization in fenestrated vECs of the CPs and CVOs is sufficient to partially convert them into BBB-like states in vivo [29, 30], although it is unable to restore the loss of the BBB transcriptional and chromatin landscapes in primary brain vECs after short-term in vitro culture [134]. The critical role of β-catenin in BBB maintenance was further demonstrated via its deletion in endothelial cells of postnatal or adult mice [137, 138]. Endothelial β-catenin signaling was also shown to regulate vascular pericyte coverage in the mouse brain via modulation of Pdgfb expression [139]. Altogether, these findings support a model in which endothelial β-catenin signaling is central to the induction and maintenance of BBB properties in vECs and inhibits the expression of the fenestration marker PLVAP to limit vascular permeability.
Two classes of β-catenin activators (Wnt7a/Wnt7b and Norrin) have been well characterized in mice, which redundantly direct brain angiogenesis and BBB formation/maintenance in a brain region-specific manner. Wnt7a and Wnt7b are expressed largely in overlapping domains, and the combined, but not individual, loss of these two genes results in severe brain angiogenesis defects in mice [135, 136]. Wnt7a overexpression in the neural tube in vivo, or in primary cultures of mouse brain endothelial cells in vitro, is sufficient to enhance GLUT-1 expression in brain endothelial cells [135, 136]. Functional redundancy between Wnt7a and Norrin in BBB maintenance was identified in the cerebellum where these double mutant mice displayed increased BBB permeability and elevated PLVAP expression in vECs [140]. The key components of Wnt7s/β-catenin signaling are the receptor complexes consisting of Frizzled, Lrps, Gpr124, and Reck [138, 141,142,143,144], while Norrin/β-catenin signaling requires Frizzled-4 [145, 146] and another co-receptor component called Tspan12 [140, 147]. A recent study has reported that the guidance cue Netrin-1 signaling through its Unc5B receptor is critical for activating endothelial β-catenin pathways to maintain BBB integrity in mice [148].
Similarly, the crucial roles of Wnt7/β-catenin signaling through Gpr124/Reck receptors in regulating brain angiogenesis and BBB formation have been well documented in zebrafish [26, 149,150,151]. Additionally, a study in zebrafish showed that brain angiogenesis and transcriptional induction of endothelial BBB differentiation occur simultaneously during development [152]. Whether brain vECs establish BBB or fenestrated functional properties in a simultaneous or progressive manner in relation to vessel formation remains an important question.
Retinoic acid (RA) signaling RA signaling is indicated to be another important inducer of BBB properties in brain vECs, although its role in vivo is not entirely clear. High concentrations of RA treatments in vitro can induce BBB properties in cultured murine brain endothelial cells [153]. Pharmacological inhibition of RA receptor signaling in pregnant mice at the stage of brain angiogenesis and BBB formation (E10.5–16.5) leads to increased vascular leakage of tracers in the brain, in addition to resulting in significantly reduced expression of several BBB marker genes [154]. Endothelial RA signaling acts upstream of the Wnt/β-catenin pathway and suppress β-catenin expression in vECs via transcriptional suppression and phosphorylation-dependent protein degradation [139]. In mice globally lacking the RA-biosynthetic enzyme Rdh10, reduced levels of RA production occur. Subsequently, Wnt signaling activation and Wnt-responsive gene expression were significantly diminished, while gene expression of endogenous Wnt inhibitors (Dkk1 and Sfrps) was upregulated [155]. In zebrafish, pharmacological inhibition of the RA degrading enzymes, cytochrome P450 family 26 (Cyp26), led to increased expression of Claudin-5 in fenestrated hypophyseal vessels [71], indicating that increased levels of RA can induce BBB properties in these fenestrated vessels and that Cyp26-mediated RA degradation represses the induction of the BBB properties. Further investigations into the signaling crosstalk between RA and Wnt/β-catenin pathways in vivo will clarify the epistatic and redundant relationships between these two pathways in BBB function.
Suppressed transcytosis Brain vECs with BBB properties display low rates of transcytosis, the transcellular vesicular transport of macromolecules from one side of vECs to the other [156, 157]. Recent studies have revealed molecular components that actively suppress transcytosis specifically in brain vECs. Selective expression of the lipid transporter Mfsd2a was identified in BBB vECs [158, 159], and its genetic deletion results in impaired BBB function in mice [158] and zebrafish [160]. This BBB endothelial-specific expression of Mfsd2a is important to establish a unique lipid environment that inhibits caveolae-mediated transcytosis in these ECs, thereby maintaining BBB integrity [161]. Endothelial cell-specific deletion of β-catenin in mice results in significant reduction of Mfsd2a expression in the brain [162], while EC-specific β-catenin stabilization leads to the upregulation of Mfsd2a in fenestrated vECs of the brain [29]. A recent study has identified the extracellular-matrix protein Vitronectin secreted from brain pericytes as a crucial ligand that restricts endothelial transcytosis in a cell non-autonomous manner [163], illuminating a cellular mechanism by which transcytosis in BBB vECs is suppressed.
Pericytes Pericytes are an important cell type that induces and maintains endothelial BBB properties [164,165,166]. A recent scRNA-seq study investigated endothelial cell transcriptional changes in response to pericyte deficiency (70–80% brain pericyte loss) in adult brains of Pdgfbret/ret mice [167]. This study showed that pericyte deficiency led to a significant reduction of BBB endothelial gene expression, notably transporters such as Mfsd2a, while inducing the upregulation of Plvap and leukocyte adhesion molecule expression, resulting in BBB disruptions. Expression of many BBB markers (e.g., Claudin-5 and Glut1) remained unchanged in this pericyte deficiency model, indicating a specific role for pericytes in regulating BBB function. These gene expression changes in the adult brains are consistent with the earlier study that identified the critical role of pericytes in BBB induction during embryogenesis and described similar gene expression changes in embryonic brains of Pdgfrb mutant mice deficient for pericytes [164]. In this pericyte-deficient mouse model, 2 distinct modes of BBB disruptions were observed: widespread increase in vesicular transcytosis across brain vECs [166, 167] and focal disruption of tight junctions causing hotspot leakage [167]. Reduced endothelial expression of Angiopoietin 2 triggers the latter mode of BBB disruptions in the absence of brain pericytes [167].
Studies among several taxa revealed multiple embryonic origins of brain pericytes [168], including avians [169, 170], mice [171,172,173], and zebrafish [174]. A recent study suggests the existence of differences in morphology and distribution pattern of pericytes along capillary vessels across brain regions [175], indicating that pericytes from different developmental origins exhibit morphological and functional differences in regulating specific types and/or function of brain vasculature. The well-conserved role of PDGF-B signaling through its cognate PDGFR-β receptor in brain pericyte development was documented between mice [176,177,178,179] and zebrafish [174, 180]. CD146 is indicated to function as a co-receptor of PDGFR-β to mediate pericyte recruitment to cerebrovascular ECs and promote BBB maturation [181]. Notch3 expression in pericytes was shown to have a conserved role in maintaining BBB integrity and mural cell coverage of brain vasculature between mice [182] and zebrafish [183]. A recent study identified lactate, a metabolite produced through glucose metabolism in brain vECs, as a crucial energy source for pericytes in maintaining BBB function [119]. Emerging scRNA-seq data have identified potential new specific markers for brain pericytes in humans [81, 184, 185], mice [80, 186], and zebrafish [187], accelerating the study on brain pericyte heterogeneity in structure and function.
Astrocytes Astrocytes are another important cellular constitute of the BBB in mammals. Generation of astrocytes in the mammalian brain occurs postnatally after the functional BBB is established [158, 164], eliminating the possibility of an astrocyte role in endothelial acquisition of BBB properties during embryonic development. However, after passing through postnatal developmental stages, astrocytes can be critical for BBB maintenance and repair. A recent study indicated that mature astrocyte ablation from the mouse brain using the inducible astrocyte glutamate transporter Glast-CreERT line led to increased leakage of fluorescently labeled small molecule Cadaverine (< 1 kDa) into the brain parenchyma, suggesting BBB dysfunction following brain astrocyte ablation [188]. However, several studies using similar astrocyte-targeted genetic ablation systems with larger molecular tracers in the spinal cord did not report significantly increased BBB permeability [189, 190].
In the developing mouse brain, Reelin-induced activation of endothelial Dab1 plays an instructive role in directing astrocyte end-feet attachment to cerebral blood vessels for functional BBB development, as genetic inactivation of this signaling axis led to insufficient astrocyte end-feet coverage of these vessels, resulting in defective barrier properties [191]. This Reelin-endothelial Dab signaling is not critical for pericyte coverage and maintenance of the BBB [191], suggesting its developmental role in the assembly of the NVU. In adulthood, astrocyte-specific deletion of Netrin-1 or Neogenin in mice resulted in increased BBB leakage and reduced pericyte vascular coverage [192], indicating a crucial role for astrocyte-derived Netrin-1 signaling in maintaining BBB and NVU integrity. Similarly, genetic inhibition of Wnt secretions from astrocytes led to impaired astrocyte end-feet morphology, reduced pericyte coverage, and increased levels of BBB permeability and endothelial transcytosis [193]. Thus, astrocyte-derived Wnts maintain BBB and NVU integrity after developmental stages by sustaining adequate levels of Wnt/β-catenin activity in brain vECs and astrocytes. Future studies will be needed to identify the specific Wnt ligand(s) secreted from astrocytes and their underlying cellular mechanisms responsible for maintaining the NVU integrity.
Development and maintenance of endothelial fenestrations and permeable properties
VEGF signaling has been demonstrated as a key regulator of endothelial fenestrations in both in vitro [194] and in vivo [195]. VEGF-A signaling downregulates the expression of the tight junction proteins Claudin-5 and Occludin at the mRNA and protein levels [196], while it upregulates the mRNA and protein expression of PLVAP [197]. Across the CVOs, higher levels of Vegf-A mRNA expression were observed than in adjacent brain regions in adult mice [198]. Distinct cell types have been shown to regulate endothelial fenestrations across the CPs and CVOs.
In the ME, specialized ependymal cells, tanycytes, display increased Vegf-A expression in response to fasting, which results in increased levels of endothelial PLVAP expression, density, and fenestrations [199]. Recent work indicated that Melanin-concentrating hormone-expressing neurons, which extend axonal projections to the ME in close proximity to fenestrated capillaries, directly controls endothelial density and fenestrations via activity-dependent Vegf-A release from their axon terminals [200]. These results are consistent with a previous study that reported Vegf signaling-dependent continuous endothelial proliferation and angiogenesis in the ME of adult mice [201].
In the NH, Vegf-A signaling derived from pituicytes, glial cells of the posterior pituitary, controls continuous endothelial proliferation and angiogenesis in adult mice [202]. In the developing zebrafish NH, pituicyte-derived Vegf and TGF-β signaling induces plvap expression and high vascular permeability in its fenestrated capillaries [71]. In the same system, defective fenestrated vasculature forms in the pituitary in the absence of both the hypothalamic–hypophyseal axon tract and signaling evoked by the neuropeptide oxytocin secreted from its axon terminals [203].
In the CPs, several studies suggest a role for Vegf-A and TGF-β signaling derived from the ependymal epithelium in maintaining the integrity and fenestrations of capillaries in adult mice [195, 204]. Our recent study identified a unique combination of Vegf ligands required for driving fenestrated vascular development in the zebrafish hindbrain CP, while these ligands have little impact on the formation of neighboring BBB brain vasculature [73].
In the AP, OVLT, and SFO, Vegf-A expression in neurons and/or astrocytes is indicated to sustain continuous endothelial proliferation and vascular permeability of fenestrated capillaries in adult mice [198]. Additionally, in the AP, Wnt Inhibitory Factor-1 knockout mice displayed an elevated level of the GLUT1 BBB marker [29], suggesting that locally expressed endogenous inhibitors of Wnt/β-catenin signaling suppress vEC’s β-catenin activities to prevent BBB formation in the fenestrated vascular beds of the brain. Melatonin, a hormone secreted by the PG, has been implied in the regulation of angiogenesis [205], especially inhibition of multiple tumor angiogenesis; however, its role in fenestrated capillary development or maintenance in the PG remains unclear.
Perivascular cell diversity and their emerging roles in controlling endothelial properties
Recent scRNA-seq data have revealed transcriptionally diverse subtypes of brain perivascular cells, including pericytes [80, 81, 184], fibroblasts [80, 82, 206, 207], smooth muscle cells [80, 186, 208], as well as macrophages and microglia [209,210,211,212]. An increasing number of scRNA-seq datasets that contain brain perivascular cell populations have been reported under physiological and pathological conditions across species, developmental stages, and brain regions. However, except pericytes, the functional roles of each perivascular cell type in regulating brain vEC properties remain largely unknown.
A recent study showed that perivascular fibroblasts lie adjacent to smooth muscle cells in arterioles and large-diameter venules, but are absent in capillaries, in the adult mouse brain [213]. scRNA-seq results of embryonic mouse brain meninges identified transcriptionally distinct fibroblast subtypes derived from different embryonic origins in brain meningeal compartments [206]. Our recent work identified mesoderm-derived meningeal fibroblasts as important sources of Vegf ligands critical for directing fenestrated vessel formation in the zebrafish CP [73]. Future studies will be needed to uncover how fibroblast subtypes, including perivascular fibroblasts, contribute to the establishment of brain vascularization and the endothelial acquisition of unique properties across the brain.
Similarly, recent scRNA-seq data have indicated the unique transcriptional signatures of perivascular macrophages, which are distinguishable from those of microglia, in the mouse cortex [212]. This and other emerging scRNA-seq results have provided valuable information to identify and establish reliable cell type-specific markers for perivascular cells. Given the unique distributions of perivascular cell types along vEC types and across brain regions [175, 213, 214], future studies on dissecting the functional roles of each cell population and subtype in regulating vEC properties across the brain will expand our understanding of dynamic and heterogeneous brain vEC properties.
Current and emerging models for the fate determination of brain endothelial cells
In light of classical studies that conducted chick-quail transplantation experiments, neural environmental signals or extrinsic factors are thought to be the key determinants of brain vEC barrier properties [132, 133]. In support of this finding, additional studies have established that canonical Wnt/β-catenin signaling is necessary [114, 135] and sufficient [29, 30] to induce and maintain BBB properties in brain vECs (Fig. 3A). However, it remains unknown whether neural environmental signals are necessary and sufficient to induce a fenestrated endothelial cell fate and if so, what the molecular determinants of this cell fate are. This incomplete knowledge has limited our current understanding of brain vEC fate specification across the brain, leaving open the question of whether BBB and fenestrated vEC properties in the brain are determined entirely by extrinsic signals.
Current and emerging models for the fate determination of brain endothelial cells. A In a prevailing model, brain-specific signaling induced by extrinsic factors, such as Wnt7s and Norrin, induces the differentiation of primitive endothelial cells into a BBB EC type as they migrate to target brain regions. B In an emerging model, primitive endothelial cells first undergo pre-differentiation, which allows them to migrate to target brain regions in response to specific sets of angiogenic cues via EC type-specific angiogenesis. In the CPs and CVOs where fenestrated ECs are generated and maintained, BBB inducing extrinsic signals, such as Wnt7s, Norrin, and RA, are suppressed by Wnt inhibitory factors and/or RA degrading enzymes, Cyp26. BBB blood–brain barrier, CPs choroid plexuses, CVOs circumventricular organs, Cyp26 cytochrome P450 family 26 enzymes, ECs endothelial cells, RA retinoic acid, TGF-β transforming growth factor beta, VEGFs vascular endothelial growth factors, WIFs Wnt inhibitory factors
There still remains the possibility that the distinct fates of brain vECs derive from different embryonic origins. Our recent results indicate that during brain vascularization in zebrafish, adjacent vECs exhibit individually distinct responses to local Vegf ligands, resulting in different fates [73]. These findings suggest that brain vECs undergo fate pre-determination prior to angiogenesis and that these intrinsic properties facilitate migration of vECs to their destinations in response to environmental angiogenic factors via “EC type-specific angiogenesis” (Fig. 3B). Thus, it is possible that a combination of intrinsically programed pre-determination and dynamic spatiotemporal presentation of local morphogenetic cues direct fate decisions and heterogeneous network formation of brain vECs. This model is in line with a recent study that demonstrated lineage history as a critical determinant of EC specialization [95]. The authors reported that the lymphatic lineage derived from the paraxial mesoderm contributes to lymphatic endothelium in multiple organs, but in an organ-restricted manner [95], indicating that EC fate is imprinted before the established endothelial genetic specification process is initiated. Identifying the key developmental determinants of fenestrated brain vEC identities will accelerate our understanding of the mechanisms underlying the generation of brain vEC heterogeneity.
Plasticity of brain endothelial fates and states under physiological and experimental conditions
Endothelial fates and states are plastic during development and in adulthood [215,216,217], resulting in heterogeneous permeability of this cell type. Neuronal activity has been proposed as a crucial modulator of influx [218] and efflux [219] transport activities in BBB vECs, thereby controlling BBB permeability dynamics [220]. In addition, efflux transporter function in BBB vECs undergoes circadian regulation [219, 221, 222], inducing circadian changes in BBB permeability throughout the day. Since the production of certain molecules and metal ions such as hormones, neuropeptides, cytokines, and magnesium has been reported to undergo circadian oscillations [223], the rhythmic expression of these molecules and ions may mediate circadian changes in BBB permeability. Sleep loss also causes BBB permeability changes through down-regulation of tight-junction protein expression [224] and levels of endocytosis [225] in brain vECs. Other physiological factors that modulate BBB tightness include pregnancy, nutrition, body temperature, physical activity, gut microbiota, and psychological stress [226].
In contrast to our increasing knowledge of BBB permeability dynamics and their modulators, much less is known about physiological states that modulate fenestrated vEC permeability in the brain. One study showed that fasting, or glucose deprivation, increases PLVAP expression and endothelial fenestrations in fenestrated capillaries of the murine ME [199]. The activity of hypothalamic neurons involved in food intake, locomotor activity, and sleep also controls fenestrated endothelial density and permeability in the ME [200], suggesting that these physiological factors modulate vEC permeability states in this brain region. Seasonal changes in the length of daylight (i.e., photoperiod) lead to the oscillatory pattern of melatonin secretion from the PG, which is indicated to affect fenestrated vascular density in the sheep ME [227].
Recent studies in mice demonstrated that fenestrated brain vECs respond differentially to forced activation of β-catenin across the CVOs and CPs in terms of their phenotypic conversions into a BBB state [29, 30], suggesting that heterogeneity in the phenotypic plasticity of vECs exists across fenestrated vascular beds of the brain. Changes in fenestrated brain vEC permeability can influence fluid balance, waste clearance, immune surveillance, and the efficiency of hormonal secretion and reception, through this vessel type. However, fenestrated vascular permeability dynamics have been understudied. Future studies on structural and functional changes in fenestrated brain vasculature in response to physiological and pathological stimuli will advance our knowledge of the plasticity of this vEC type.
Pathological and age-induced changes in brain endothelial properties and heterogeneity
Significant structural and functional changes of brain capillaries have been reported with aging and in disease states [2, 228,229,230]. For example, the brain of elderly humans [231] and of aged mice [22] displays capillary wall thinning and declines in capillary density, blood flow, vascular perfusion, angiogenic potentials, and barrier properties [16,17,18]. Decreased pericyte coverage of brain vasculature and diminished Mfsd2a expression were also observed with aging [22]. Moreover, pericyte degeneration is associated with BBB disruptions in patients with neurological diseases such as AD and amyotrophic lateral sclerosis (ALS) [232,233,234,235]. Since brain pericytes regulate blood flow via capillary constriction [236, 237], reduced cerebral blood flow as a consequence of pericyte degeneration is another hallmark associated with aging and age-related neurodegenerative diseases [238]. In support of these observations, forced pericyte ablation with diphtheria toxin using an inducible pericyte-specific Cre line in mice led to rapid BBB breakdown and neurodegeneration [239].
While brain pericyte deficiency clearly promotes BBB disruptions, viable pericytes can also produce numerous proinflammatory mediators that are detrimental to BBB function [240]. In aging human and rodent brains, increased production of the pleiotropic cytokine TGF-β was reported [241], which can upregulate a number of inflammatory genes in pericytes in vitro [242]. Conditional loss of the transcription factor RBPJ in pericytes of mouse brains triggers excessive production of TGF-β3 that leads to overexpression of inflammation-related genes, suggesting a potential role for RBPJ in regulating a proinflammatory genetic program in pericytes [243]. Notably, pharmacological inhibition of TGF-β signaling restored cognitive impairments in aged mice [241] and ameliorated autoimmune encephalomyelitis in a mouse model [244], indicating that TGF-β signaling inhibition counteracts detrimental consequences of neuroinflammation.
There is a growing body of transcriptomic datasets that offer enriched information on gene expression changes of brain vECs over the course of development, and also in response to disease conditions. A recently established transcriptome database of isolated mouse brain vECs under healthy and various neurological disease states identified a common, core pathway leading to BBB dysfunction regardless of BBB disruption triggers [79]. This common BBB dysfunction module among diseases includes upregulation of genes that are enriched in vECs of peripheral organs under normal physiological conditions, indicating a shift of the BBB vEC identity toward peripheral non-BBB cell states [79]. Moreover, single-cell atlases of human brain vasculature from individuals with AD [245], Huntington’s disease [185], or arteriovenous malformations [81] have provided valuable resources to understand vascular cell-type-specific perturbations of gene expression under these disease states compared to healthy individuals.
In contrast to BBB dysfunction linked to aging and neurological disorders, very little is known about structural and functional alterations of fenestrated brain capillaries under these conditions. Given that defective brain–blood communications via fenestrated vasculature can lead to impaired metabolic sensing and hormonal release into the bloodstream, it is likely that structural and functional changes in this vEC type abrogate neuroendocrine control and action. Indeed, alterations of neuroendocrine function with aging have been documented [246, 247], which include imbalanced hormone production [248] and reduced signaling reception and sensitivity for secreted hormones [249]. Considering age-related VEGF signaling declines [21] and the crucial role of this signaling in maintaining endothelial fenestrations in the CPs and CVOs [71, 195, 204], it is likely that endothelial fenestration numbers, sizes, and permeability in these brain regions decline with aging and that these age-related changes affect neuroendocrine function. Future investigations into age-related changes in the number, size, and/or permeability of endothelial fenestrations across the CPs and CVOs will help understand the malfunction and disease associated with these brain regions.
Development of potential therapeutics targeting unique brain endothelial properties
Pharmacological inhibition of the PDGF-C/PDGFR-α signaling axis has been pursued as a powerful approach to restore BBB dysfunction in neurological disorders [27]. Previous studies showed that the intracerebroventricular injection of either PDGF-C or tissue plasminogen activator was sufficient to increase BBB permeability and induce BBB dysfunction [250, 251]. Conversely, inhibition of the PDGF-CC signaling by neutralizing antibodies or inhibition of PDGFR-α with imatinib reduced BBB dysfunction in mouse models of ischemic stroke [250, 252], MS [253, 254], seizure [255], and traumatic brain injury [256]. Thus, preserving BBB integrity by targeting this signaling axis is a promising therapeutic approach for a wide range of neurodegenerative and neuroinflammatory diseases associated with BBB breakdown.
Strong neuroprotective effects of activated protein C (APC) on both acute brain injury and chronic neurodegenerative conditions make it another potential therapeutic target [28]. Intravenous injections of APC were shown to exert beneficial therapeutic effects in mouse models of ischemic stroke [257], MS [258], ALS [259], and AD [260]. It has been proposed that APC functions by eliciting anti-inflammatory effects and neuroprotective actions within the NVU to prevent BBB breakdown [28].
Another therapeutic strategy is the repurposing of a key developmental BBB induction signal as a BBB protective agent for neurological pathology [26]. This successful translation of developmental biology knowledge into potential therapies opens a new avenue for developing therapeutics for a variety of neurological and cerebrovascular diseases, as well as for age-related vascular declines in the brain. By conducting a screen of the numerous Wnt7a variants generated via single-residue substitutions, the authors identified genetically engineered Wnt7a ligands that can preferentially activate the Gpr124/Reck co-receptor complex while dramatically reducing activation of its other cognate Frizzled receptors [26, 144]. This study further demonstrated that these Gpr124/Reck-specific activators acted as BBB repair agents and mitigated the progression of neurological disease in mouse models, including glioblastoma and stroke. This finding is consistent with a separate study where endothelial-specific β-catenin stabilization improves BBB function in conditional Gpr124-deficient mice under pathological neurological conditions [261].
Emerging therapeutic targets include the Netrin1-Unc5B signaling axis that is indicated to act upstream of canonical β-catenin pathways in the brain [148]. Current evidence shows that Netrin-1 global knockouts [262] or endothelial-specific deletion of the Unc5B receptor in mice [148] led to the down-regulation of BBB markers in vECs, while upregulating their PLVAP expression [148]. In contrast, Netrin-1 treatments can enhance BBB marker expression both in vitro and in vivo [148, 192, 262] and reduce BBB leakage in mouse models of MS [262] and BBB breakdown [192], suggesting BBB protective effects of Netrin-1-Unc5B signaling.
The four strategies discussed above all help mitigate BBB dysfunction, thereby preventing the progression and worsening of neuroinflammation and BBB breakdown that are the hallmarks of a broad range of neurological diseases (Fig. 4). Future studies may seek to test whether treatment approaches targeting different signaling pathways could have additive or synergistic therapeutic effects on these diseases. Furthermore, our increasing knowledge of brain vEC’s transcriptomic changes under a variety of disease conditions and their shared BBB dysfunction module [79, 245] can help identify potential new therapeutic options for BBB repairs that may stand alone or boost the effects of the existing approaches.
Expected therapeutic effects of a BBB repair agent(s) on brain disease/injury associated with BBB dysfunction. (A) In a healthy brain, no neuroinflammation and pathological BBB breakdown are detected. (B) In a diseased/injured brain without any treatment, severe neuroinflammation and BBB breakdown cause serious brain damage. Brain disease/injury elicits a series of neuroimmune responses via activation of microglia, astrocytes, and pericytes into proinflammatory states [240] that lead to their release of inflammatory mediators involved in BBB disruptions. This permits blood-circulating immune cell infiltration into the damaged brain region. These neuroinflammatory events induce neurological damage. (C) In a diseased/injured brain subjected to treatment with a BBB repair agent, mitigated neuroinflammation and BBB breakdown cause only limited brain damage. As compared to the scenario described in (B), timely administration of a BBB repair agent, such as PDGF-C signaling inhibitor or engineered Wnt7a ligand, can ameliorate the damaging effects of neuroinflammation by limiting BBB disruptions. BBB blood–brain barrier, PDGF-C platelet-derived growth factor C
In many pathological and developmental conditions where endothelial BBB integrity and identities are disrupted, upregulation of PLVAP expression in vECs has been reported. For example, PLVAP upregulation is detected in microvasculature associated with brain tumors and ischemia [263,264,265] where neuroinflammation and BBB breakdown occur, or in vasculature where reduced levels of endothelial β-catenin signaling are observed [114, 138, 140, 148]. These observations are consistent with the current model that active β-catenin signaling suppresses PLVAP expression in brain vECs to establish the BBB [29, 30, 114]. Since anti-PLVAP therapy has been explored as a potential anti-angiogenesis and anti-edema therapeutic option for cerebral edema caused by ischemic stroke and brain tumors [110, 111], this option may be pursued to limit vascular leakage and BBB breakdown in conjunction with the other BBB repair strategies. However, further investigations will be needed to define the cellular and molecular mechanisms underlying PLVAP upregulation and its contributions to vascular leakage and BBB breakdown during aging and neuroinflammation.
Beyond BBB-targeted therapies, efficient drug delivery across the BBB has remained a significant challenge in treating or preventing the progression of neurological deficits. Efforts have been made to exploit endogenous receptor-mediated transcytosis pathways to enhance uptake of large molecules and therapeutics in the brain [266, 267]. Transferrin/transferrin receptor (TFRC) pathway is one of the major transport pathways specific to the brain and BBB [268,269,270]. Since TFRC is highly expressed in BBB vECs [268, 269] and brain tumors such as glioblastomas [271,272,273], nanoparticles targeted with TFRC-binding peptides have been explored as diagnostic probes for imaging brain tumors [274, 275] and for boosting brain uptake of therapeutic antibodies [276,277,278]. Another strategy for promoting drug delivery across the BBB includes the use of the monoclonal antibodies that can block specific Netrin-1-Unc5B interactions or induce Unc5B internalization [148]. These Unc5B blocking agents were suggested to enhance size-selective BBB permeability within a limited time window [148], indicating their potential application to transient BBB opening for therapeutic uptakes in the brain.
In contrast to the promising BBB repair approaches, current molecular targets for repairing fenestrated brain vECs are substantially limited. PLVAP is a well-established marker for fenestrated brain vECs and currently known to be the only structural components of fenestral and stomatal diaphragms [109,110,111]. In conditions where high vascular permeability in fenestrated brain vECs declines due to reduced numbers of endothelial fenestrations with aging and/or disease, restorations of fenestrations can be possibly achieved by targeting PLVAP itself, or VEGF and/or TGF-β signaling, which are indicated to be required for induction of PLVAP expression during development [71] and maintenance of endothelial fenestrations in adults [195, 204]. However, systemic upregulation of PLVAP expression can be problematic because this may result in a significant increase in overall brain vascular permeability or unwanted angiogenesis due to the potential role of PLVAP in developmental and pathological angiogenesis [72, 263].
Recent bulk and single-cell transcriptomes have indicated many other genes that are highly expressed in fenestrated brain vECs [10, 29, 279], including Plpp1, Plpp3, Igfbp3, Cd24a, and Ldb2. Future studies on these and other candidate genes in the development and/or maintenance of fenestrated brain vEC will shed new light on potential new targets for repairing this cell type.
Future perspectives
Brain barriers act as the important boundaries that separate the brain parenchyma from the periphery across species. Multiple blood vEC types present in the brain play a central role in establishing and maintaining some of these barriers, thereby ensuring an optimal brain microenvironment. In addition to the widely recognized BBB properties that a majority of brain vECs exhibit, fenestrated vECs possess unique barrier properties across the CVOs and CPs. Numerous factors can affect the states of brain vECs globally or locally, thereby generating the heterogeneity and highly dynamic changes in their vascular permeability. The evolution of technology has enabled us to explore more diverse scientific approaches and research directions than in the past. Here, we discuss some emerging approaches untouched in earlier sections that will help address unsolved questions in the field.
Recently, there have been significant advances in in vitro model systems. These include the vascularization models of human brain organoids-on-a-chip [280, 281], self-assembling multicellular BBB spheroids [282, 283], and improved endothelial BBB differentiation protocols using human pluripotent, or induced pluripotent, stem cells [284, 285]. Human organoid and cell reprogramming technologies have been rapidly expanding to mimic human brain development and disease modeling with the construction of a functional vasculature. These in vitro models will become powerful tools for studying human-specific vascular traits absent in animal models, drug delivery across the BBB, and as a drug-screening platform for ameliorating BBB dysfunction in neurological diseases.
Emerging large-scale biological resources from multi-omics data have increased the demand for an efficient in vivo platform to screen numerous candidate genes emerging from big data analytics. Given the high conservation of the molecular mechanisms underlying brain vascularization across vertebrates, one effective approach includes the use of the zebrafish system, which provides technical advantages such as rapid ex utero development and facile 3D visualization of brain vasculature. Recently, our group, along with others, reported highly efficient and scalable CRISPR/Cas9-based mutagenesis protocols to generate F0 zebrafish knockouts [73, 286, 287]. These technical advantages will make the zebrafish a valuable model to perform phenotype-based F0 screens of many candidate genes individually, or in combinations, in vivo.
The identification of brain regional differences in BBB or fenestrated vEC barrier properties has indicated brain area-specific regulations of brain vEC characteristics mediated by their surrounding cellular compositions (e.g., perivascular, glial, and/or neuronal types). Cutting-edge technologies, such as spatial transcriptomics [288], combined with an in situ sequencing method [289] will enable the visualization and analysis of many transcripts with single-cell resolution [290,291,292]. These approaches will compensate for the lack of positional information on emerging single-cell and bulk transcriptome data of brain vECs and perivascular cell types in health and disease, allowing for spatial mapping of gene expression profiles in situ.
The discovery of novel regulators of BBB permeability in recent years has illuminated potential new targets for delivering therapeutics across the BBB. Endothelial transcytosis pathways have been a major target of non-invasive brain delivery approaches [293]. Several recently identified molecules (Mfsd2a, Vitronectin, and Integrin α5) critical for suppression of transcytosis in BBB vECs [158,159,160,161, 163] have become attractive targets for non-invasive drug transport into the brain parenchyma. For example, drugs that inhibit MFSD2A activity may release the suppression of transcytosis in BBB vECs, thereby increasing endothelial molecular transport via transcytosis into the brain parenchyma. Recent advances in structural biology and protein design methods [294,295,296,297,298] will facilitate in silico structure-based molecular designs that can enhance the efficiency of drug delivery across the BBB.
The approaches listed here represent only a few examples of emerging directions in the field that have evolved with technological advances. Cutting-edge multi-omics platforms have offered the opportunity to simultaneously profile RNA and DNA/protein at the single-cell level and with spatial resolution, becoming increasingly powerful tools to study the heterogeneous identities and states of brain vascular cell types in health and disease. Future investigations into the complex physiology and pathology of brain–blood interfaces using multifaceted approaches will reveal new therapeutic horizons for treatments of cerebrovascular and neurological diseases.
Availability of data and materials
Not applicable.
Abbreviations
- AD:
-
Alzheimer’s disease
- ALPM:
-
Anterior lateral plate mesoderm
- ALS:
-
Amyotrophic lateral sclerosis
- AP:
-
Area postrema
- APC:
-
Activated protein C
- BBB:
-
Blood–brain barrier
- CNS:
-
Central nervous system
- CPs:
-
Choroid plexuses
- CVOs:
-
Circumventricular organs
- Cyp26:
-
Cytochrome P450 family 26 enzymes
- EMPs:
-
Erythro-myeloid progenitors
- ME:
-
Median eminence
- MS:
-
Multiple sclerosis
- NH:
-
Neurohypophysis
- NVU:
-
Neurovascular unit
- OVLT:
-
Organum vasculosum of the lamina terminalis
- PDGF-B:
-
Platelet-derived growth factor B
- PDGF-C:
-
Platelet-derived growth factor C
- PG:
-
Pineal gland
- PLVAP:
-
Plasmalemma vesicle-associated protein
- RA:
-
Retinoic acid
- SCO:
-
Subcommissural organ
- SFO:
-
Subfornical organ
- TGF-β:
-
Transforming growth factor beta
- TFRC:
-
Transferrin receptor
- vECs:
-
Vascular endothelial cells
- VEGFs:
-
Vascular endothelial growth factors
References
Daneman R, Prat A (2015) The blood–brain barrier. Cold Spring Harb Perspect Biol 7(1):a020412
Sweeney MD, Zhao Z, Montagne A, Nelson AR, Zlokovic BV (2019) Blood–brain barrier: from physiology to disease and back. Physiol Rev 99(1):21–78
Schaeffer S, Iadecola C (2021) Revisiting the neurovascular unit. Nat Neurosci 24(9):1198–1209
Hawkins BT, Davis TP (2005) The blood-brain barrier/neurovascular unit in health and disease. Pharmacol Rev 57(2):173–185
Miyata S (2015) New aspects in fenestrated capillary and tissue dynamics in the sensory circumventricular organs of adult brains. Front Neurosci 9:390
Ben-Zvi A, Liebner S (2021) Developmental regulation of barrier- and non-barrier blood vessels in the CNS. J Intern Med 292(1):31–46
Augustin HG, Koh GY (2017) Organotypic vasculature: from descriptive heterogeneity to functional pathophysiology. Science 357(6353):eaal2379
Potente M, Makinen T (2017) Vascular heterogeneity and specialization in development and disease. Nat Rev Mol Cell Biol 18(8):477–494
Ross JM, Kim C, Allen D, Crouch EE, Narsinh K, Cooke DL et al (2020) The expanding cell diversity of the brain vasculature. Front Physiol 11:600767
Kalucka J, de Rooij L, Goveia J, Rohlenova K, Dumas SJ, Meta E et al (2020) Single-cell transcriptome atlas of murine endothelial cells. Cell 180(4):764–79 e20
Saunders NR, Daneman R, Dziegielewska KM, Liddelow SA (2013) Transporters of the blood-brain and blood-CSF interfaces in development and in the adult. Mol Asp Med 34(2–3):742–752
Limmer S, Weiler A, Volkenhoff A, Babatz F, Klambt C (2014) The Drosophila blood-brain barrier: development and function of a glial endothelium. Front Neurosci 8:365
O’Brown NM, Pfau SJ, Gu C (2018) Bridging barriers: a comparative look at the blood-brain barrier across organisms. Genes Dev 32(7–8):466–478
Abbott NJ (2005) Dynamics of CNS barriers: evolution, differentiation, and modulation. Cell Mol Neurobiol 25(1):5–23
Bundgaard M, Abbott NJ (2008) All vertebrates started out with a glial blood-brain barrier 4–500 million years ago. Glia 56(7):699–708
Watanabe C, Imaizumi T, Kawai H, Suda K, Honma Y, Ichihashi M et al (2020) Aging of the vascular system and neural diseases. Front Aging Neurosci 12:557384
Brown WR, Thore CR (2011) Review: cerebral microvascular pathology in ageing and neurodegeneration. Neuropathol Appl Neurobiol 37(1):56–74
Montagne A, Barnes SR, Sweeney MD, Halliday MR, Sagare AP, Zhao Z et al (2015) Blood-brain barrier breakdown in the aging human hippocampus. Neuron 85(2):296–302
Graves SI, Baker DJ (2020) Implicating endothelial cell senescence to dysfunction in the ageing and diseased brain. Basic Clin Pharmacol Toxicol 127(2):102–110
Zlokovic BV (2011) Neurovascular pathways to neurodegeneration in Alzheimer’s disease and other disorders. Nat Rev Neurosci 12(12):723–738
Grunewald M, Kumar S, Sharife H, Volinsky E, Gileles-Hillel A, Licht T et al (2021) Counteracting age-related VEGF signaling insufficiency promotes healthy aging and extends life span. Science 373(6554):eabc8479
Yang AC, Stevens MY, Chen MB, Lee DP, Stahli D, Gate D et al (2020) Physiological blood-brain transport is impaired with age by a shift in transcytosis. Nature 583(7816):425–430
Yamazaki Y, Baker DJ, Tachibana M, Liu CC, van Deursen JM, Brott TG et al (2016) Vascular cell senescence contributes to blood-brain barrier breakdown. Stroke 47(4):1068–1077
Obermeier B, Daneman R, Ransohoff RM (2013) Development, maintenance and disruption of the blood-brain barrier. Nat Med 19(12):1584–1596
Profaci CP, Munji RN, Pulido RS, Daneman R (2020) The blood-brain barrier in health and disease: important unanswered questions. J Exp Med 217(4):e20190062
Martin M, Vermeiren S, Bostaille N, Eubelen M, Spitzer D, Vermeersch M et al (2022) Engineered Wnt ligands enable blood-brain barrier repair in neurological disorders. Science 375(6582):eabm4459
Lewandowski SA, Fredriksson L, Lawrence DA, Eriksson U (2016) Pharmacological targeting of the PDGF-CC signaling pathway for blood-brain barrier restoration in neurological disorders. Pharmacol Ther 167:108–119
Griffin JH, Zlokovic BV, Mosnier LO (2018) Activated protein C, protease activated receptor 1, and neuroprotection. Blood 132(2):159–169
Wang Y, Sabbagh MF, Gu X, Rattner A, Williams J, Nathans J (2019) Beta-catenin signaling regulates barrier-specific gene expression in circumventricular organ and ocular vasculatures. Elife 8:e43257
Benz F, Wichitnaowarat V, Lehmann M, Germano RF, Mihova D, Macas J, et al. Low wnt/beta-catenin signaling determines leaky vessels in the subfornical organ and affects water homeostasis in mice. Elife. 2019;8.
Haddad-Tovolli R, Dragano NRV, Ramalho AFS, Velloso LA (2017) Development and function of the blood-brain barrier in the context of metabolic control. Front Neurosci 11:224
Zlokovic BV (2008) The blood-brain barrier in health and chronic neurodegenerative disorders. Neuron 57(2):178–201
Saunders NR, Dziegielewska KM, Mollgard K, Habgood MD (2018) Physiology and molecular biology of barrier mechanisms in the fetal and neonatal brain. J Physiol 596(23):5723–5756
Langen UH, Ayloo S, Gu C (2019) Development and cell biology of the blood-brain barrier. Annu Rev Cell Dev Biol 35:591–613
Abbott NJ, Patabendige AA, Dolman DE, Yusof SR, Begley DJ (2010) Structure and function of the blood-brain barrier. Neurobiol Dis 37(1):13–25
Ehrlich P (1885) Das Sauerstoffbedürfnis des Organismus. Eine Farbenanalytische Studie Berlin, Hirschwald
Zur LM, von der Cerebrospinalflüssgkeit L (1900) Z Clin Med 40:480–494
Goldmann EE (1909) Die äussere und innere Sekretion des gesunden und kranken Organismus im Lichte der ‘vitalen Färbung. Beiträg Klinische Chirurgie 64:192–265
Bouffard G (1906) Injection des couleurs de benzidine aux animaux normaux. Ann d l’lnst Pasteur Paris 20:539–548
Stern L, Gautier R (1918) Le passage dans le liquide céphalo-rachidien de substances introduites dans la circulation et leur action sur le système nerveux central chez les différentes espèces animales. RCR d Ia Soc de Phys et d’hist natur de Genève 35:91–94
Brightman MW, Reese TS (1969) Junctions between intimately apposed cell membranes in the vertebrate brain. J Cell Biol 40(3):648–677
Reese TS, Karnovsky MJ (1967) Fine structural localization of a blood-brain barrier to exogenous peroxidase. J Cell Biol 34(1):207–217
Stern L, Gautier R (1921) Recherches sur le liquide céphalo-rachidien. 1. Les rapports entre le liquide céphalo-rachidien et la circulation sanguine. Arch Int Physiol 17:138–192
Wislocki GB, Leduc EH (1952) Vital staining of the hematoencephalic barrier by silver nitrate and trypan blue, and cytological comparisons of the neurohypophysis, pineal body, area postrema, intercolumnar tubercle and supraoptic crest. J Comp Neurol 96(3):371–413
Wislocki GB, King LS (1936) The permeability of the hypophysis and hypothalamus to vital dyes, with a study of the hypophyseal vascular supply. Am J Anat 58:421–472
Goldmann EE (1913) Vitalfärbung am Zentralnervensyatem. Beitrag zur Physio-Pathologie des plexus chorioideus und der Hirnhäute. Abh preuss, Akad Wiss Phys-Math Kl 1:1–60
Hofer H (1958) Zur morphologie der circumventriculären Organe des Zwischenhirnes der Säugetiere. Verh Dtsch Zool Ges 202–51
Duvernoy HM, Risold PY (2007) The circumventricular organs: an atlas of comparative anatomy and vascularization. Brain Res Rev 56(1):119–147
Weindl A, Joynt RJ (1973) Barrier properties of the subcommissural organ. Arch Neurol 29(1):16–22
Morita S, Miyata S (2012) Different vascular permeability between the sensory and secretory circumventricular organs of adult mouse brain. Cell Tissue Res 349(2):589–603
Morita S, Miyata S (2013) Accessibility of low-molecular-mass molecules to the median eminence and arcuate hypothalamic nucleus of adult mouse. Cell Biochem Funct 31(8):668–677
Petrov T, Howarth AG, Krukoff TL, Stevenson BR (1994) Distribution of the tight junction-associated protein ZO-1 in circumventricular organs of the CNS. Brain Res Mol Brain Res 21(3–4):235–246
Donahue S, Pappas GD (1961) The fine structure of capillaries in the cerebral cortex of the rat at various stages of development. Am J Anat 108:331–347
Fink G, Smith GC (1971) Ultrastructural features of the developing hypothalamo-hypophysial axis in the rat. A correlative study. Z Zellforsch Mikrosk Anat 119(2):208–226
Eurenius L (1977) An electron microscope study of the differentiating capillaries of the mouse neurohypophysis. Anat Embryol (Berl) 152(1):89–108
Rivera-Pomar JM (1966) The ultrastructure of the capillaries in the area postrema of the cat. Z Zellforsch Mikrosk Anat 75(3):542–554
Dermietzel R, Leibstein AG (1978) The microvascular pattern and perivascular linings of the area postrema. A combined freeze-etching and ultrathin section study. Cell Tissue Res 186(1):97–110
Matsushima S, Reiter RJ (1975) Ultrastructural observations at pineal gland capillaries in four rodent species. Am J Anat 143(3):265–281
Wolfe DE (1965) The epiphyseal cell: an electron-microscopic study of its intercellular relationships and intracellular morphology in the pineal body of the albino rat. Prog Brain Res 10:332–386
Rohr VU (1966) On the fine structure of the subfornical organ of the cat. I. The blood vessel apparatus. Z Zellforsch Mikrosk Anat 73(2):246–271
Sposito NM, Gross PM (1987) Topography and morphometry of capillaries in the rat subfornical organ. J Comp Neurol 260(1):36–46
McKinley MJ, Denton DA, Leventer M, Penschow J, Weisinger RS, Wright RD (1983) Morphology of the organum vasculosum of the lamina terminalis (OVLT) of the sheep. Brain Res Bull 11(6):649–657
Yamaguchi K, Morimoto A, Murakami N (1993) Organum vasculosum laminae terminalis (OVLT) in rabbit and rat: topographic studies. J Comp Neurol 330(3):352–362
Eurenius L, Jarskar R (1971) Electron microscope studies on the development of the external zone of the mouse median eminence. Z Zellforsch Mikrosk Anat 122(4):488–502
Monroe BG, Holmes EM (1983) The freeze-fractured median eminence. II. Developmental changes in the neurohemal contact zone of the median eminence of the rat. Cell Tissue Res 233(1):81–97
Maxwell DS, Pease DC (1956) The electron microscopy of the choroid plexus. J Biophys Biochem Cytol 2(4):467–474
Keep RF, Jones HC (1990) A morphometric study on the development of the lateral ventricle choroid plexus, choroid plexus capillaries and ventricular ependyma in the rat. Brain Res Dev Brain Res 56(1):47–53
Jeong JY, Kwon HB, Ahn JC, Kang D, Kwon SH, Park JA et al (2008) Functional and developmental analysis of the blood-brain barrier in zebrafish. Brain Res Bull 75(5):619–628
Quinonez-Silvero C, Hubner K, Herzog W (2020) Development of the brain vasculature and the blood-brain barrier in zebrafish. Dev Biol 457(2):181–190
Tessmar-Raible K, Raible F, Christodoulou F, Guy K, Rembold M, Hausen H et al (2007) Conserved sensory-neurosecretory cell types in annelid and fish forebrain: insights into hypothalamus evolution. Cell 129(7):1389–1400
Anbalagan S, Gordon L, Blechman J, Matsuoka RL, Rajamannar P, Wircer E et al (2018) Pituicyte cues regulate the development of permeable neuro-vascular interfaces. Dev Cell 47(6):711–26 e5
Gordon L, Blechman J, Shimoni E, Gur D, Anand-Apte B, Levkowitz G (2019) The fenestrae-associated protein Plvap regulates the rate of blood-borne protein passage into the hypophysis. Development 146(23):dev177790
Parab S, Quick RE, Matsuoka RL (2021) Endothelial cell type-specific molecular requirements for angiogenesis drive fenestrated vessel development in the brain. Elife 10:e64295
Stork T, Engelen D, Krudewig A, Silies M, Bainton RJ, Klambt C (2008) Organization and function of the blood-brain barrier in Drosophila. J Neurosci 28(3):587–597
Jambusaria A, Hong Z, Zhang L, Srivastava S, Jana A, Toth PT et al (2020) Endothelial heterogeneity across distinct vascular beds during homeostasis and inflammation. Elife 9:e51413
Sabbagh MF, Heng JS, Luo C, Castanon RG, Nery JR, Rattner A et al (2018) Transcriptional and epigenomic landscapes of CNS and non-CNS vascular endothelial cells. Elife 7:e36187
Hupe M, Li MX, Kneitz S, Davydova D, Yokota C, Kele J et al (2017) Gene expression profiles of brain endothelial cells during embryonic development at bulk and single-cell levels. Sci Signal 10(487):eaag2476
Nolan DJ, Ginsberg M, Israely E, Palikuqi B, Poulos MG, James D et al (2013) Molecular signatures of tissue-specific microvascular endothelial cell heterogeneity in organ maintenance and regeneration. Dev Cell 26(2):204–219
Munji RN, Soung AL, Weiner GA, Sohet F, Semple BD, Trivedi A et al (2019) Profiling the mouse brain endothelial transcriptome in health and disease models reveals a core blood-brain barrier dysfunction module. Nat Neurosci 22(11):1892–1902
Vanlandewijck M, He L, Mae MA, Andrae J, Ando K, Del Gaudio F et al (2018) A molecular atlas of cell types and zonation in the brain vasculature. Nature 554(7693):475–480
Winkler EA, Kim CN, Ross JM, Garcia JH, Gil E, Oh I et al (2022) A single-cell atlas of the normal and malformed human brain vasculature. Science eabi7377
Saunders A, Macosko EZ, Wysoker A, Goldman M, Krienen FM, de Rivera H et al (2018) Molecular diversity and specializations among the cells of the adult mouse brain. Cell 174(4):1015–30 e16
Paik DT, Tian L, Williams IM, Rhee S, Zhang H, Liu C et al (2020) Single-cell RNA sequencing unveils unique transcriptomic signatures of organ-specific endothelial cells. Circulation 142(19):1848–1862
Tabula Muris C, Overall C, Logistical C, Organ C, Processing, Library P et al (2018) Single-cell transcriptomics of 20 mouse organs creates a Tabula Muris. Nature 562(7727):367–372
Matsuoka RL, Stainier DYR (2018) Recent insights into vascular development from studies in zebrafish. Curr Opin Hematol 25(3):204–211
Stone OA, Zhou B, Red-Horse K, Stainier DYR (2021) Endothelial ontogeny and the establishment of vascular heterogeneity. BioEssays 43(7):e2100036
Nguyen PD, Hollway GE, Sonntag C, Miles LB, Hall TE, Berger S et al (2014) Haematopoietic stem cell induction by somite-derived endothelial cells controlled by meox1. Nature 512(7514):314–318
Reischauer S, Stone OA, Villasenor A, Chi N, Jin SW, Martin M et al (2016) Cloche is a bHLH-PAS transcription factor that drives haemato-vascular specification. Nature 535(7611):294–298
Mosimann C, Panakova D, Werdich AA, Musso G, Burger A, Lawson KL et al (2015) Chamber identity programs drive early functional partitioning of the heart. Nat Commun 6:8146
Pardanaud L, Luton D, Prigent M, Bourcheix LM, Catala M, Dieterlen-Lievre F (1996) Two distinct endothelial lineages in ontogeny, one of them related to hemopoiesis. Development 122(5):1363–1371
Couly G, Coltey P, Eichmann A, Le Douarin NM (1995) The angiogenic potentials of the cephalic mesoderm and the origin of brain and head blood vessels. Mech Dev 53(1):97–112
Wilting J, Brand-Saberi B, Huang R, Zhi Q, Kontges G, Ordahl CP et al (1995) Angiogenic potential of the avian somite. Dev Dyn 202(2):165–171
Wasteson P, Johansson BR, Jukkola T, Breuer S, Akyurek LM, Partanen J et al (2008) Developmental origin of smooth muscle cells in the descending aorta in mice. Development 135(10):1823–1832
Hutcheson DA, Zhao J, Merrell A, Haldar M, Kardon G (2009) Embryonic and fetal limb myogenic cells are derived from developmentally distinct progenitors and have different requirements for beta-catenin. Genes Dev 23(8):997–1013
Stone OA, Stainier DYR (2019) Paraxial mesoderm is the major source of lymphatic endothelium. Dev Cell 50(2):247-255 e3
Gore AV, Monzo K, Cha YR, Pan W, Weinstein BM (2012) Vascular development in the zebrafish. Cold Spring Harb Perspect Med 2(5):a006684
Carmeliet P (2000) Mechanisms of angiogenesis and arteriogenesis. Nat Med 6(4):389–395
Plein A, Fantin A, Denti L, Pollard JW, Ruhrberg C (2018) Erythro-myeloid progenitors contribute endothelial cells to blood vessels. Nature 562(7726):223–228
Feng T, Gao Z, Kou S, Huang X, Jiang Z, Lu Z et al (2020) No evidence for erythro-myeloid progenitor-derived vascular endothelial cells in multiple organs. Circ Res 127(10):1221–1232
Proulx K, Lu A, Sumanas S (2010) Cranial vasculature in zebrafish forms by angioblast cluster-derived angiogenesis. Dev Biol 348(1):34–46
Vogeli KM, Jin SW, Martin GR, Stainier DY (2006) A common progenitor for haematopoietic and endothelial lineages in the zebrafish gastrula. Nature 443(7109):337–339
Pang M, Bai L, Zong W, Wang X, Bu Y, Xiong C et al (2020) Light-sheet fluorescence imaging charts the gastrula origin of vascular endothelial cells in early zebrafish embryos. Cell Discov 6:74
Berndt P, Winkler L, Cording J, Breitkreuz-Korff O, Rex A, Dithmer S et al (2019) Tight junction proteins at the blood-brain barrier: far more than claudin-5. Cell Mol Life Sci 76(10):1987–2002
Ohtsuki S, Yamaguchi H, Katsukura Y, Asashima T, Terasaki T (2008) mRNA expression levels of tight junction protein genes in mouse brain capillary endothelial cells highly purified by magnetic cell sorting. J Neurochem 104(1):147–154
Morita K, Sasaki H, Furuse M, Tsukita S (1999) Endothelial claudin: claudin-5/TMVCF constitutes tight junction strands in endothelial cells. J Cell Biol 147(1):185–194
van Leeuwen LM, Evans RJ, Jim KK, Verboom T, Fang X, Bojarczuk A et al (2018) A transgenic zebrafish model for the in vivo study of the blood and choroid plexus brain barriers using claudin 5. Biol Open 7(2):bio030494
Collins MM, Baumholtz AI, Ryan AK (2012) Claudin-5 expression in the vasculature of the developing chick embryo. Gene Expr Patterns 12(3–4):123–129
Willis CL, Garwood CJ, Ray DE (2007) A size selective vascular barrier in the rat area postrema formed by perivascular macrophages and the extracellular matrix. Neuroscience 150(2):498–509
Stan RV, Tkachenko E, Niesman IR (2004) PV1 is a key structural component for the formation of the stomatal and fenestral diaphragms. Mol Biol Cell 15(8):3615–3630
Guo L, Zhang H, Hou Y, Wei T, Liu J (2016) Plasmalemma vesicle-associated protein: a crucial component of vascular homeostasis. Exp Ther Med 12(3):1639–1644
Bosma EK, van Noorden CJF, Schlingemann RO, Klaassen I (2018) The role of plasmalemma vesicle-associated protein in pathological breakdown of blood-brain and blood-retinal barriers: potential novel therapeutic target for cerebral edema and diabetic macular edema. Fluids Barriers CNS 15(1):24
Stan RV (2005) Structure of caveolae. Biochim Biophys Acta 1746(3):334–348
Palade GE (1953) Fine structure of blood capillaries. J Appl Phys 24:1424
Liebner S, Corada M, Bangsow T, Babbage J, Taddei A, Czupalla CJ et al (2008) Wnt/beta-catenin signaling controls development of the blood-brain barrier. J Cell Biol 183(3):409–417
Nitta T, Hata M, Gotoh S, Seo Y, Sasaki H, Hashimoto N et al (2003) Size-selective loosening of the blood-brain barrier in claudin-5-deficient mice. J Cell Biol 161(3):653–660
Tang M, Gao G, Rueda CB, Yu H, Thibodeaux DN, Awano T et al (2017) Brain microvasculature defects and Glut1 deficiency syndrome averted by early repletion of the glucose transporter-1 protein. Nat Commun 8:14152
Veys K, Fan Z, Ghobrial M, Bouche A, Garcia-Caballero M, Vriens K et al (2020) Role of the GLUT1 glucose transporter in postnatal CNS angiogenesis and blood-brain barrier integrity. Circ Res 127(4):466–482
Winkler EA, Nishida Y, Sagare AP, Rege SV, Bell RD, Perlmutter D et al (2015) GLUT1 reductions exacerbate Alzheimer’s disease vasculo-neuronal dysfunction and degeneration. Nat Neurosci 18(4):521–530
Lee HW, Xu Y, Zhu X, Jang C, Choi W, Bae H et al (2022) Endothelium-derived lactate is required for pericyte function and blood-brain barrier maintenance. EMBO J 41(9):e109890
Herrnberger L, Seitz R, Kuespert S, Bosl MR, Fuchshofer R, Tamm ER (2012) Lack of endothelial diaphragms in fenestrae and caveolae of mutant Plvap-deficient mice. Histochem Cell Biol 138(5):709–724
Stan RV, Tse D, Deharvengt SJ, Smits NC, Xu Y, Luciano MR et al (2012) The diaphragms of fenestrated endothelia: gatekeepers of vascular permeability and blood composition. Dev Cell 23(6):1203–1218
Walchli T, Wacker A, Frei K, Regli L, Schwab ME, Hoerstrup SP et al (2015) Wiring the vascular network with neural cues: a CNS perspective. Neuron 87(2):271–296
Ruhrberg C, Bautch VL (2013) Neurovascular development and links to disease. Cell Mol Life Sci 70(10):1675–1684
Strong LH (1964) The early embryonic pattern of internal vascularization of the mammalian cerebral cortex. J Comp Neurol 123:121–138
Haigh JJ, Morelli PI, Gerhardt H, Haigh K, Tsien J, Damert A et al (2003) Cortical and retinal defects caused by dosage-dependent reductions in VEGF-A paracrine signaling. Dev Biol 262(2):225–241
Raab S, Beck H, Gaumann A, Yuce A, Gerber HP, Plate K et al (2004) Impaired brain angiogenesis and neuronal apoptosis induced by conditional homozygous inactivation of vascular endothelial growth factor. Thromb Haemost 91(3):595–605
Matsuoka RL, Marass M, Avdesh A, Helker CS, Maischein HM, Grosse AS et al (2016) Radial glia regulate vascular patterning around the developing spinal cord. Elife 5:e20253
Matsuoka RL, Rossi A, Stone OA, Stainier DYR (2017) CNS-resident progenitors direct the vascularization of neighboring tissues. Proc Natl Acad Sci USA 114(38):10137–10142
Takahashi T, Takase Y, Yoshino T, Saito D, Tadokoro R, Takahashi Y (2015) Angiogenesis in the developing spinal cord: blood vessel exclusion from neural progenitor region is mediated by VEGF and its antagonists. PLoS ONE 10(1):e0116119
Hogan KA, Ambler CA, Chapman DL, Bautch VL (2004) The neural tube patterns vessels developmentally using the VEGF signaling pathway. Development 131(7):1503–1513
Ruhrberg C, Gerhardt H, Golding M, Watson R, Ioannidou S, Fujisawa H et al (2002) Spatially restricted patterning cues provided by heparin-binding VEGF-A control blood vessel branching morphogenesis. Genes Dev 16(20):2684–2698
Stewart PA, Wiley MJ (1981) Developing nervous tissue induces formation of blood-brain barrier characteristics in invading endothelial cells: a study using quail–chick transplantation chimeras. Dev Biol 84(1):183–192
Ikeda E, Flamme I, Risau W (1996) Developing brain cells produce factors capable of inducing the HT7 antigen, a blood-brain barrier-specific molecule, in chick endothelial cells. Neurosci Lett 209(3):149–152
Sabbagh MF, Nathans J (2020) A genome-wide view of the de-differentiation of central nervous system endothelial cells in culture. Elife 9:e51276
Daneman R, Agalliu D, Zhou L, Kuhnert F, Kuo CJ, Barres BA (2009) Wnt/beta-catenin signaling is required for CNS, but not non-CNS, angiogenesis. Proc Natl Acad Sci USA 106(2):641–646
Stenman JM, Rajagopal J, Carroll TJ, Ishibashi M, McMahon J, McMahon AP (2008) Canonical Wnt signaling regulates organ-specific assembly and differentiation of CNS vasculature. Science 322(5905):1247–1250
Tran KA, Zhang X, Predescu D, Huang X, Machado RF, Gothert JR et al (2016) Endothelial beta-catenin signaling is required for maintaining adult blood-brain barrier integrity and central nervous system homeostasis. Circulation 133(2):177–186
Zhou Y, Wang Y, Tischfield M, Williams J, Smallwood PM, Rattner A et al (2014) Canonical WNT signaling components in vascular development and barrier formation. J Clin Investig 124(9):3825–3846
Bonney S, Dennison BJC, Wendlandt M, Siegenthaler JA (2018) Retinoic acid regulates endothelial beta-catenin expression and pericyte numbers in the developing brain vasculature. Front Cell Neurosci 12:476
Wang Y, Cho C, Williams J, Smallwood PM, Zhang C, Junge HJ et al (2018) Interplay of the Norrin and Wnt7a/Wnt7b signaling systems in blood-brain barrier and blood-retina barrier development and maintenance. Proc Natl Acad Sci USA 115(50):E11827–E11836
Zhou Y, Nathans J (2014) Gpr124 controls CNS angiogenesis and blood-brain barrier integrity by promoting ligand-specific canonical wnt signaling. Dev Cell 31(2):248–256
Cho C, Smallwood PM, Nathans J (2017) Reck and Gpr124 are essential receptor cofactors for Wnt7a/Wnt7b-specific signaling in mammalian CNS angiogenesis and blood-brain barrier regulation. Neuron 95(5):1056–73 e5
Kuhnert F, Mancuso MR, Shamloo A, Wang HT, Choksi V, Florek M et al (2010) Essential regulation of CNS angiogenesis by the orphan G protein-coupled receptor GPR124. Science 330(6006):985–989
Eubelen M, Bostaille N, Cabochette P, Gauquier A, Tebabi P, Dumitru AC et al (2018) A molecular mechanism for Wnt ligand-specific signaling. Science 361(6403):eaat1178
Xu Q, Wang Y, Dabdoub A, Smallwood PM, Williams J, Woods C et al (2004) Vascular development in the retina and inner ear: control by Norrin and Frizzled-4, a high-affinity ligand-receptor pair. Cell 116(6):883–895
Ye X, Wang Y, Cahill H, Yu M, Badea TC, Smallwood PM et al (2009) Norrin, frizzled-4, and Lrp5 signaling in endothelial cells controls a genetic program for retinal vascularization. Cell 139(2):285–298
Junge HJ, Yang S, Burton JB, Paes K, Shu X, French DM et al (2009) TSPAN12 regulates retinal vascular development by promoting Norrin- but not Wnt-induced FZD4/beta-catenin signaling. Cell 139(2):299–311
Boye K, Geraldo LH, Furtado J, Pibouin-Fragner L, Poulet M, Kim D et al (2022) Endothelial Unc5B controls blood-brain barrier integrity. Nat Commun 13(1):1169
Hubner K, Cabochette P, Dieguez-Hurtado R, Wiesner C, Wakayama Y, Grassme KS et al (2018) Wnt/beta-catenin signaling regulates VE-cadherin-mediated anastomosis of brain capillaries by counteracting S1pr1 signaling. Nat Commun 9(1):4860
Vanhollebeke B, Stone OA, Bostaille N, Cho C, Zhou Y, Maquet E et al (2015) Tip cell-specific requirement for an atypical Gpr124- and Reck-dependent Wnt/beta-catenin pathway during brain angiogenesis. Elife 4:e06489
Ulrich F, Carretero-Ortega J, Menendez J, Narvaez C, Sun B, Lancaster E et al (2016) Reck enables cerebrovascular development by promoting canonical Wnt signaling. Development 143(1):147–159
Umans RA, Henson HE, Mu F, Parupalli C, Ju B, Peters JL et al (2017) CNS angiogenesis and barriergenesis occur simultaneously. Dev Biol 425(2):101–108
Bonney S, Siegenthaler JA (2017) Differential effects of retinoic acid concentrations in regulating blood-brain barrier properties. eNeuro 4(3):ENEURO.0378–16.2017
Mizee MR, Wooldrik D, Lakeman KA, van het Hof B, Drexhage JA, Geerts D et al (2013) Retinoic acid induces blood-brain barrier development. J Neurosci 33(4):1660–1671
Bonney S, Harrison-Uy S, Mishra S, MacPherson AM, Choe Y, Li D et al (2016) Diverse functions of retinoic acid in brain vascular development. J Neurosci 36(29):7786–7801
Ayloo S, Gu C (2019) Transcytosis at the blood-brain barrier. Curr Opin Neurobiol 57:32–38
Tuma P, Hubbard AL (2003) Transcytosis: crossing cellular barriers. Physiol Rev 83(3):871–932
Ben-Zvi A, Lacoste B, Kur E, Andreone BJ, Mayshar Y, Yan H et al (2014) Mfsd2a is critical for the formation and function of the blood-brain barrier. Nature 509(7501):507–511
Nguyen LN, Ma D, Shui G, Wong P, Cazenave-Gassiot A, Zhang X et al (2014) Mfsd2a is a transporter for the essential omega-3 fatty acid docosahexaenoic acid. Nature 509(7501):503–506
O'Brown NM, Megason SG, Gu C (2019) Suppression of transcytosis regulates zebrafish blood-brain barrier function. Elife 8:e47326
Andreone BJ, Chow BW, Tata A, Lacoste B, Ben-Zvi A, Bullock K et al (2017) Blood-brain barrier permeability is regulated by lipid transport-dependent suppression of caveolae-mediated transcytosis. Neuron 94(3):581–94 e5
Martowicz A, Trusohamn M, Jensen N, Wisniewska-Kruk J, Corada M, Ning FC et al (2019) Endothelial beta-catenin signaling supports postnatal brain and retinal angiogenesis by promoting sprouting, tip cell formation, and VEGFR (Vascular Endothelial Growth Factor Receptor) 2 Expression. Arterioscler Thromb Vasc Biol 39(11):2273–2288
Ayloo S, Lazo CG, Sun S, Zhang W, Cui B, Gu C (2022) Pericyte-to-endothelial cell signaling via vitronectin-integrin regulates blood-CNS barrier. Neuron 110(10):1641–1655.e6
Daneman R, Zhou L, Kebede AA, Barres BA (2010) Pericytes are required for blood-brain barrier integrity during embryogenesis. Nature 468(7323):562–566
Bell RD, Winkler EA, Sagare AP, Singh I, LaRue B, Deane R et al (2010) Pericytes control key neurovascular functions and neuronal phenotype in the adult brain and during brain aging. Neuron 68(3):409–427
Armulik A, Genove G, Mae M, Nisancioglu MH, Wallgard E, Niaudet C et al (2010) Pericytes regulate the blood-brain barrier. Nature 468(7323):557–561
Mae MA, He L, Nordling S, Vazquez-Liebanas E, Nahar K, Jung B et al (2021) Single-cell analysis of blood-brain barrier response to pericyte loss. Circ Res 128(4):e46–e62
Girolamo F, de Trizio I, Errede M, Longo G, d’Amati A, Virgintino D (2021) Neural crest cell-derived pericytes act as pro-angiogenic cells in human neocortex development and gliomas. Fluids Barriers CNS 18(1):14
Korn J, Christ B, Kurz H (2002) Neuroectodermal origin of brain pericytes and vascular smooth muscle cells. J Comp Neurol 442(1):78–88
Etchevers HC, Vincent C, Le Douarin NM, Couly GF (2001) The cephalic neural crest provides pericytes and smooth muscle cells to all blood vessels of the face and forebrain. Development 128(7):1059–1068
Yamamoto S, Muramatsu M, Azuma E, Ikutani M, Nagai Y, Sagara H et al (2017) A subset of cerebrovascular pericytes originates from mature macrophages in the very early phase of vascular development in CNS. Sci Rep 7(1):3855
Simon C, Lickert H, Gotz M, Dimou L (2012) Sox10-iCreERT2: a mouse line to inducibly trace the neural crest and oligodendrocyte lineage. Genesis 50(6):506–515
Yamazaki T, Nalbandian A, Uchida Y, Li W, Arnold TD, Kubota Y et al (2017) Tissue myeloid progenitors differentiate into pericytes through TGF-beta signaling in developing skin vasculature. Cell Rep 18(12):2991–3004
Ando K, Fukuhara S, Izumi N, Nakajima H, Fukui H, Kelsh RN et al (2016) Clarification of mural cell coverage of vascular endothelial cells by live imaging of zebrafish. Development 143(8):1328–1339
Grant RI, Hartmann DA, Underly RG, Berthiaume AA, Bhat NR, Shih AY (2019) Organizational hierarchy and structural diversity of microvascular pericytes in adult mouse cortex. J Cereb Blood Flow Metab 39(3):411–425
Lindahl P, Johansson BR, Leveen P, Betsholtz C (1997) Pericyte loss and microaneurysm formation in PDGF-B-deficient mice. Science 277(5323):242–245
Tallquist MD, French WJ, Soriano P (2003) Additive effects of PDGF receptor beta signaling pathways in vascular smooth muscle cell development. PLoS Biol 1(2):E52
Lindblom P, Gerhardt H, Liebner S, Abramsson A, Enge M, Hellstrom M et al (2003) Endothelial PDGF-B retention is required for proper investment of pericytes in the microvessel wall. Genes Dev 17(15):1835–1840
Hellstrom M, Kalen M, Lindahl P, Abramsson A, Betsholtz C (1999) Role of PDGF-B and PDGFR-beta in recruitment of vascular smooth muscle cells and pericytes during embryonic blood vessel formation in the mouse. Development 126(14):3047–3055
Ando K, Shih YH, Ebarasi L, Grosse A, Portman D, Chiba A et al (2021) Conserved and context-dependent roles for pdgfrb signaling during zebrafish vascular mural cell development. Dev Biol 479:11–22
Chen J, Luo Y, Hui H, Cai T, Huang H, Yang F et al (2017) CD146 coordinates brain endothelial cell-pericyte communication for blood-brain barrier development. Proc Natl Acad Sci USA 114(36):E7622–E7631
Henshall TL, Keller A, He L, Johansson BR, Wallgard E, Raschperger E et al (2015) Notch3 is necessary for blood vessel integrity in the central nervous system. Arterioscler Thromb Vasc Biol 35(2):409–420
Wang Y, Pan L, Moens CB, Appel B (2014) Notch3 establishes brain vascular integrity by regulating pericyte number. Development 141(2):307–317
Parker KR, Migliorini D, Perkey E, Yost KE, Bhaduri A, Bagga P et al (2020) Single-cell analyses identify brain mural cells expressing CD19 as potential off-tumor targets for CAR-T immunotherapies. Cell 183(1):126–42 e17
Garcia FJ, Sun N, Lee H, Godlewski B, Mathys H, Galani K et al (2022) Single-cell dissection of the human brain vasculature. Nature 603(7903):893–899
He L, Vanlandewijck M, Mae MA, Andrae J, Ando K, Del Gaudio F et al (2018) Single-cell RNA sequencing of mouse brain and lung vascular and vessel-associated cell types. Sci Data 5:180160
Shih YH, Portman D, Idrizi F, Grosse A, Lawson ND (2021) Integrated molecular analysis identifies a conserved pericyte gene signature in zebrafish. Development 148(23):dev200189
Heithoff BP, George KK, Phares AN, Zuidhoek IA, Munoz-Ballester C, Robel S (2021) Astrocytes are necessary for blood-brain barrier maintenance in the adult mouse brain. Glia 69(2):436–472
Tsai HH, Li H, Fuentealba LC, Molofsky AV, Taveira-Marques R, Zhuang H et al (2012) Regional astrocyte allocation regulates CNS synaptogenesis and repair. Science 337(6092):358–362
Schreiner B, Romanelli E, Liberski P, Ingold-Heppner B, Sobottka-Brillout B, Hartwig T et al (2015) Astrocyte depletion impairs redox homeostasis and triggers neuronal loss in the adult CNS. Cell Rep 12(9):1377–1384
Segarra M, Aburto MR, Cop F, Llao-Cid C, Hartl R, Damm M et al (2018) Endothelial Dab1 signaling orchestrates neuro-glia-vessel communication in the central nervous system. Science 361(6404):eaao2861
Yao LL, Hu JX, Li Q, Lee D, Ren X, Zhang JS et al (2020) Astrocytic neogenin/netrin-1 pathway promotes blood vessel homeostasis and function in mouse cortex. J Clin Investig 130(12):6490–6509
Guerit S, Fidan E, Macas J, Czupalla CJ, Figueiredo R, Vijikumar A et al (2021) Astrocyte-derived Wnt growth factors are required for endothelial blood-brain barrier maintenance. Prog Neurobiol 199:101937
Esser S, Wolburg K, Wolburg H, Breier G, Kurzchalia T, Risau W (1998) Vascular endothelial growth factor induces endothelial fenestrations in vitro. J Cell Biol 140(4):947–959
Kamba T, Tam BY, Hashizume H, Haskell A, Sennino B, Mancuso MR et al (2006) VEGF-dependent plasticity of fenestrated capillaries in the normal adult microvasculature. Am J Physiol Heart Circ Physiol 290(2):H560–H576
Argaw AT, Gurfein BT, Zhang Y, Zameer A, John GR (2009) VEGF-mediated disruption of endothelial CLN-5 promotes blood-brain barrier breakdown. Proc Natl Acad Sci USA 106(6):1977–1982
Strickland LA, Jubb AM, Hongo JA, Zhong F, Burwick J, Fu L et al (2005) Plasmalemmal vesicle-associated protein (PLVAP) is expressed by tumour endothelium and is upregulated by vascular endothelial growth factor-A (VEGF). J Pathol 206(4):466–475
Morita S, Furube E, Mannari T, Okuda H, Tatsumi K, Wanaka A et al (2015) Vascular endothelial growth factor-dependent angiogenesis and dynamic vascular plasticity in the sensory circumventricular organs of adult mouse brain. Cell Tissue Res 359(3):865–884
Langlet F, Levin BE, Luquet S, Mazzone M, Messina A, Dunn-Meynell AA et al (2013) Tanycytic VEGF-A boosts blood-hypothalamus barrier plasticity and access of metabolic signals to the arcuate nucleus in response to fasting. Cell Metab 17(4):607–617
Jiang H, Gallet S, Klemm P, Scholl P, Folz-Donahue K, Altmuller J et al (2020) MCH neurons regulate permeability of the median eminence barrier. Neuron 107(2):306–19 e9
Morita S, Ukai S, Miyata S (2013) VEGF-dependent continuous angiogenesis in the median eminence of adult mice. Eur J Neurosci 37(4):508–518
Furube E, Mannari T, Morita S, Nishikawa K, Yoshida A, Itoh M et al (2014) VEGF-dependent and PDGF-dependent dynamic neurovascular reconstruction in the neurohypophysis of adult mice. J Endocrinol 222(1):161–179
Gutnick A, Blechman J, Kaslin J, Herwig L, Belting HG, Affolter M et al (2011) The hypothalamic neuropeptide oxytocin is required for formation of the neurovascular interface of the pituitary. Dev Cell 21(4):642–654
Maharaj AS, Walshe TE, Saint-Geniez M, Venkatesha S, Maldonado AE, Himes NC et al (2008) VEGF and TGF-beta are required for the maintenance of the choroid plexus and ependyma. J Exp Med 205(2):491–501
Rahbarghazi A, Siahkouhian M, Rahbarghazi R, Ahmadi M, Bolboli L, Keyhanmanesh R et al (2021) Role of melatonin in the angiogenesis potential; highlights on the cardiovascular disease. J Inflamm (Lond) 18(1):4
DeSisto J, O’Rourke R, Jones HE, Pawlikowski B, Malek AD, Bonney S et al (2020) Single-cell transcriptomic analyses of the developing meninges reveal meningeal fibroblast diversity and function. Dev Cell 54(1):43-59 e4
Zeisel A, Hochgerner H, Lonnerberg P, Johnsson A, Memic F, van der Zwan J et al (2018) Molecular architecture of the mouse nervous system. Cell 174(4):999-1014 e22
Chasseigneaux S, Moraca Y, Cochois-Guegan V, Boulay AC, Gilbert A, Le Crom S et al (2018) Isolation and differential transcriptome of vascular smooth muscle cells and mid-capillary pericytes from the rat brain. Sci Rep 8(1):12272
Li Q, Cheng Z, Zhou L, Darmanis S, Neff NF, Okamoto J et al (2019) Developmental heterogeneity of microglia and brain myeloid cells revealed by deep single-cell RNA sequencing. Neuron 101(2):207–23 e10
Jordao MJC, Sankowski R, Brendecke SM, Sagar Locatelli G, Tai YH et al (2019) Single-cell profiling identifies myeloid cell subsets with distinct fates during neuroinflammation. Science 363(6425):eaat7554
Van Hove H, Martens L, Scheyltjens I, De Vlaminck K, Pombo Antunes AR, De Prijck S et al (2019) A single-cell atlas of mouse brain macrophages reveals unique transcriptional identities shaped by ontogeny and tissue environment. Nat Neurosci 22(6):1021–1035
Goldmann T, Wieghofer P, Jordao MJ, Prutek F, Hagemeyer N, Frenzel K et al (2016) Origin, fate and dynamics of macrophages at central nervous system interfaces. Nat Immunol 17(7):797–805
Bonney SK, Sullivan LT, Cherry TJ, Daneman R, Shih AY (2021) Distinct features of brain perivascular fibroblasts and mural cells revealed by in vivo two-photon imaging. J Cereb Blood Flow Metab 271678X211068528
Dorrier CE, Jones HE, Pintaric L, Siegenthaler JA, Daneman R (2022) Emerging roles for CNS fibroblasts in health, injury and disease. Nat Rev Neurosci 23(1):23–34
Dejana E, Hirschi KK, Simons M (2017) The molecular basis of endothelial cell plasticity. Nat Commun 8:14361
Pasut A, Becker LM, Cuypers A, Carmeliet P (2021) Endothelial cell plasticity at the single-cell level. Angiogenesis 24(2):311–326
Greenspan LJ, Weinstein BM (2021) To be or not to be: endothelial cell plasticity in development, repair, and disease. Angiogenesis 24(2):251–269
Nishijima T, Piriz J, Duflot S, Fernandez AM, Gaitan G, Gomez-Pinedo U et al (2010) Neuronal activity drives localized blood-brain-barrier transport of serum insulin-like growth factor-I into the CNS. Neuron 67(5):834–846
Pulido RS, Munji RN, Chan TC, Quirk CR, Weiner GA, Weger BD et al (2020) Neuronal activity regulates blood-brain barrier efflux transport through endothelial circadian genes. Neuron 108(5):937–52 e7
Kaplan L, Chow BW, Gu C (2020) Neuronal regulation of the blood-brain barrier and neurovascular coupling. Nat Rev Neurosci 21(8):416–432
Zhang SL, Lahens NF, Yue Z, Arnold DM, Pakstis PP, Schwarz JE et al (2021) A circadian clock regulates efflux by the blood-brain barrier in mice and human cells. Nat Commun 12(1):617
Zhang SL, Yue Z, Arnold DM, Artiushin G, Sehgal A (2018) A circadian clock in the blood-brain barrier regulates xenobiotic efflux. Cell 173(1):130–9 e10
Cuddapah VA, Zhang SL, Sehgal A (2019) Regulation of the blood-brain barrier by circadian rhythms and sleep. Trends Neurosci 42(7):500–510
He J, Hsuchou H, He Y, Kastin AJ, Wang Y, Pan W (2014) Sleep restriction impairs blood-brain barrier function. J Neurosci 34(44):14697–14706
Artiushin G, Zhang SL, Tricoire H, Sehgal A (2018) Endocytosis at the Drosophila blood-brain barrier as a function for sleep. Elife 7:e43326
Segarra M, Aburto MR, Acker-Palmer A (2021) Blood-brain barrier dynamics to maintain brain homeostasis. Trends Neurosci 44(5):393–405
Castle-Miller J, Bates DO, Tortonese DJ (2017) Mechanisms regulating angiogenesis underlie seasonal control of pituitary function. Proc Natl Acad Sci U S A 114(12):E2514–E2523
Banks WA, Reed MJ, Logsdon AF, Rhea EM, Erickson MA (2021) Healthy aging and the blood-brain barrier. Nat Aging 1(3):243–254
Erdo F, Denes L, de Lange E (2017) Age-associated physiological and pathological changes at the blood-brain barrier: a review. J Cereb Blood Flow Metab 37(1):4–24
Finger CE, Moreno-Gonzalez I, Gutierrez A, Moruno-Manchon JF, McCullough LD (2021) Age-related immune alterations and cerebrovascular inflammation. Mol Psychiatry 27(2):803–818
Stewart PA, Magliocco M, Hayakawa K, Farrell CL, Del Maestro RF, Girvin J et al (1987) A quantitative analysis of blood-brain barrier ultrastructure in the aging human. Microvasc Res 33(2):270–282
Sengillo JD, Winkler EA, Walker CT, Sullivan JS, Johnson M, Zlokovic BV (2013) Deficiency in mural vascular cells coincides with blood-brain barrier disruption in Alzheimer’s disease. Brain Pathol 23(3):303–310
Cheng J, Korte N, Nortley R, Sethi H, Tang Y, Attwell D (2018) Targeting pericytes for therapeutic approaches to neurological disorders. Acta Neuropathol 136(4):507–523
Lendahl U, Nilsson P, Betsholtz C (2019) Emerging links between cerebrovascular and neurodegenerative diseases—a special role for pericytes. EMBO Rep 20(11):e48070
Garbuzova-Davis S, Hernandez-Ontiveros DG, Rodrigues MC, Haller E, Frisina-Deyo A, Mirtyl S et al (2012) Impaired blood-brain/spinal cord barrier in ALS patients. Brain Res 1469:114–128
Hall CN, Reynell C, Gesslein B, Hamilton NB, Mishra A, Sutherland BA et al (2014) Capillary pericytes regulate cerebral blood flow in health and disease. Nature 508(7494):55–60
Peppiatt CM, Howarth C, Mobbs P, Attwell D (2006) Bidirectional control of CNS capillary diameter by pericytes. Nature 443(7112):700–704
Brown LS, Foster CG, Courtney JM, King NE, Howells DW, Sutherland BA (2019) Pericytes and neurovascular function in the healthy and diseased brain. Front Cell Neurosci 13:282
Nikolakopoulou AM, Montagne A, Kisler K, Dai Z, Wang Y, Huuskonen MT et al (2019) Pericyte loss leads to circulatory failure and pleiotrophin depletion causing neuron loss. Nat Neurosci 22(7):1089–1098
Rustenhoven J, Jansson D, Smyth LC, Dragunow M (2017) Brain pericytes as mediators of neuroinflammation. Trends Pharmacol Sci 38(3):291–304
Senatorov VV Jr, Friedman AR, Milikovsky DZ, Ofer J, Saar-Ashkenazy R, Charbash A et al (2019) Blood-brain barrier dysfunction in aging induces hyperactivation of TGFbeta signaling and chronic yet reversible neural dysfunction. Sci Transl Med 11(521):eaaw8283
Rustenhoven J, Aalderink M, Scotter EL, Oldfield RL, Bergin PS, Mee EW et al (2016) TGF-beta1 regulates human brain pericyte inflammatory processes involved in neurovasculature function. J Neuroinflammation 13:37
Dieguez-Hurtado R, Kato K, Giaimo BD, Nieminen-Kelha M, Arf H, Ferrante F et al (2019) Loss of the transcription factor RBPJ induces disease-promoting properties in brain pericytes. Nat Commun 10(1):2817
Luo J, Ho PP, Buckwalter MS, Hsu T, Lee LY, Zhang H et al (2007) Glia-dependent TGF-beta signaling, acting independently of the TH17 pathway, is critical for initiation of murine autoimmune encephalomyelitis. J Clin Investig 117(11):3306–3315
Yang AC, Vest RT, Kern F, Lee DP, Agam M, Maat CA et al (2022) A human brain vascular atlas reveals diverse mediators of Alzheimer's risk. Nature
Rehman HU, Masson EA (2001) Neuroendocrinology of ageing. Age Ageing 30(4):279–287
van den Beld AW, Kaufman JM, Zillikens MC, Lamberts SWJ, Egan JM, van der Lely AJ (2018) The physiology of endocrine systems with ageing. Lancet Diabetes Endocrinol 6(8):647–658
Nessi AC, De Hoz G, Tanoira C, Guaraglia E, Consens G (1995) Pituitary physiological and ultrastructural changes during aging. Endocrine 3(10):711–716
Lai Z, Roos P, Zhai O, Olsson Y, Fholenhag K, Larsson C et al (1993) Age-related reduction of human growth hormone-binding sites in the human brain. Brain Res 621(2):260–266
Su EJ, Fredriksson L, Geyer M, Folestad E, Cale J, Andrae J et al (2008) Activation of PDGF-CC by tissue plasminogen activator impairs blood-brain barrier integrity during ischemic stroke. Nat Med 14(7):731–737
Yepes M, Sandkvist M, Moore EG, Bugge TH, Strickland DK, Lawrence DA (2003) Tissue-type plasminogen activator induces opening of the blood-brain barrier via the LDL receptor-related protein. J Clin Investig 112(10):1533–1540
Ma Q, Huang B, Khatibi N, Rolland W 2nd, Suzuki H, Zhang JH et al (2011) PDGFR-alpha inhibition preserves blood-brain barrier after intracerebral hemorrhage. Ann Neurol 70(6):920–931
Adzemovic MV, Zeitelhofer M, Eriksson U, Olsson T, Nilsson I (2013) Imatinib ameliorates neuroinflammation in a rat model of multiple sclerosis by enhancing blood-brain barrier integrity and by modulating the peripheral immune response. PLoS ONE 8(2):e56586
Zeitelhofer M, Adzemovic MZ, Moessinger C, Stefanitsch C, Strell C, Muhl L et al (2020) Blocking PDGF-CC signaling ameliorates multiple sclerosis-like neuroinflammation by inhibiting disruption of the blood-brain barrier. Sci Rep 10(1):22383
Fredriksson L, Stevenson TK, Su EJ, Ragsdale M, Moore S, Craciun S et al (2015) Identification of a neurovascular signaling pathway regulating seizures in mice. Ann Clin Transl Neurol 2(7):722–738
Su EJ, Fredriksson L, Kanzawa M, Moore S, Folestad E, Stevenson TK et al (2015) Imatinib treatment reduces brain injury in a murine model of traumatic brain injury. Front Cell Neurosci 9:385
Huuskonen MT, Wang Y, Nikolakopoulou AM, Montagne A, Dai Z, Lazic D et al (2022) Protection of ischemic white matter and oligodendrocytes in mice by 3K3A-activated protein C. J Exp Med 219(1):e20211372
Han MH, Hwang SI, Roy DB, Lundgren DH, Price JV, Ousman SS et al (2008) Proteomic analysis of active multiple sclerosis lesions reveals therapeutic targets. Nature 451(7182):1076–1081
Winkler EA, Sengillo JD, Sagare AP, Zhao Z, Ma Q, Zuniga E et al (2014) Blood-spinal cord barrier disruption contributes to early motor-neuron degeneration in ALS-model mice. Proc Natl Acad Sci USA 111(11):E1035–E1042
Lazic D, Sagare AP, Nikolakopoulou AM, Griffin JH, Vassar R, Zlokovic BV (2019) 3K3A-activated protein C blocks amyloidogenic BACE1 pathway and improves functional outcome in mice. J Exp Med 216(2):279–293
Chang J, Mancuso MR, Maier C, Liang X, Yuki K, Yang L et al (2017) Gpr124 is essential for blood-brain barrier integrity in central nervous system disease. Nat Med 23(4):450–460
Podjaski C, Alvarez JI, Bourbonniere L, Larouche S, Terouz S, Bin JM et al (2015) Netrin 1 regulates blood-brain barrier function and neuroinflammation. Brain 138(Pt 6):1598–1612
Carson-Walter EB, Hampton J, Shue E, Geynisman DM, Pillai PK, Sathanoori R et al (2005) Plasmalemmal vesicle associated protein-1 is a novel marker implicated in brain tumor angiogenesis. Clin Cancer Res 11(21):7643–7650
Madden SL, Cook BP, Nacht M, Weber WD, Callahan MR, Jiang Y et al (2004) Vascular gene expression in nonneoplastic and malignant brain. Am J Pathol 165(2):601–608
Shue EH, Carson-Walter EB, Liu Y, Winans BN, Ali ZS, Chen J et al (2008) Plasmalemmal vesicle associated protein-1 (PV-1) is a marker of blood-brain barrier disruption in rodent models. BMC Neurosci 9:29
Pardridge WM (2012) Drug transport across the blood-brain barrier. J Cereb Blood Flow Metab 32(11):1959–1972
Banks WA (2016) From blood-brain barrier to blood-brain interface: new opportunities for CNS drug delivery. Nat Rev Drug Discov 15(4):275–292
Jefferies WA, Brandon MR, Hunt SV, Williams AF, Gatter KC, Mason DY (1984) Transferrin receptor on endothelium of brain capillaries. Nature 312(5990):162–163
Kissel K, Hamm S, Schulz M, Vecchi A, Garlanda C, Engelhardt B (1998) Immunohistochemical localization of the murine transferrin receptor (TfR) on blood-tissue barriers using a novel anti-TfR monoclonal antibody. Histochem Cell Biol 110(1):63–72
Johnsen KB, Burkhart A, Thomsen LB, Andresen TL, Moos T (2019) Targeting the transferrin receptor for brain drug delivery. Prog Neurobiol 181:101665
Calzolari A, Larocca LM, Deaglio S, Finisguerra V, Boe A, Raggi C et al (2010) Transferrin receptor 2 is frequently and highly expressed in glioblastomas. Transl Oncol 3(2):123–134
Prior R, Reifenberger G, Wechsler W (1990) Transferrin receptor expression in tumours of the human nervous system: relation to tumour type, grading and tumour growth fraction. Virch Arch A Pathol Anat Histopathol 416(6):491–496
Recht L, Torres CO, Smith TW, Raso V, Griffin TW (1990) Transferrin receptor in normal and neoplastic brain tissue: implications for brain-tumor immunotherapy. J Neurosurg 72(6):941–945
Ni XR, Zhao YY, Cai HP, Yu ZH, Wang J, Chen FR et al (2020) Transferrin receptor 1 targeted optical imaging for identifying glioma margin in mouse models. J Neurooncol 148(2):245–258
Dixit S, Miller K, Zhu Y, McKinnon E, Novak T, Kenney ME et al (2015) Dual receptor-targeted theranostic nanoparticles for localized delivery and activation of photodynamic therapy drug in glioblastomas. Mol Pharm 12(9):3250–3260
Couch JA, Yu YJ, Zhang Y, Tarrant JM, Fuji RN, Meilandt WJ et al (2013) Addressing safety liabilities of TfR bispecific antibodies that cross the blood-brain barrier. Sci Transl Med 5(183):18357 (1–12)
Yu YJ, Zhang Y, Kenrick M, Hoyte K, Luk W, Lu Y et al (2011) Boosting brain uptake of a therapeutic antibody by reducing its affinity for a transcytosis target. Sci Transl Med 3(84):84ra44
Niewoehner J, Bohrmann B, Collin L, Urich E, Sade H, Maier P et al (2014) Increased brain penetration and potency of a therapeutic antibody using a monovalent molecular shuttle. Neuron 81(1):49–60
Chen Q, Leshkowitz D, Blechman J, Levkowitz G (2020) Single-cell molecular and cellular architecture of the mouse neurohypophysis. eNeuro 7(1):ENEURO.0345-19.2019
Matsui TK, Tsuru Y, Hasegawa K, Kuwako KI (2021) Vascularization of human brain organoids. Stem Cells 39(8):1017–1024
Zhang S, Wan Z, Kamm RD (2021) Vascularized organoids on a chip: strategies for engineering organoids with functional vasculature. Lab Chip 21(3):473–488
Cho CF, Wolfe JM, Fadzen CM, Calligaris D, Hornburg K, Chiocca EA et al (2017) Blood-brain-barrier spheroids as an in vitro screening platform for brain-penetrating agents. Nat Commun 8:15623
Bergmann S, Lawler SE, Qu Y, Fadzen CM, Wolfe JM, Regan MS et al (2018) Blood-brain-barrier organoids for investigating the permeability of CNS therapeutics. Nat Protoc 13(12):2827–2843
Gastfriend BD, Nishihara H, Canfield SG, Foreman KL, Engelhardt B, Palecek SP et al (2021) Wnt signaling mediates acquisition of blood-brain barrier properties in naive endothelium derived from human pluripotent stem cells. Elife 10:e70992
Workman MJ, Svendsen CN (2020) Recent advances in human iPSC-derived models of the blood-brain barrier. Fluids Barriers CNS 17(1):30
Quick RE, Buck LD, Parab S, Tolbert ZR, Matsuoka RL (2021) Highly efficient synthetic CRISPR RNA/Cas9-based mutagenesis for rapid cardiovascular phenotypic screening in F0 zebrafish. Front Cell Dev Biol 9:735598
Kroll F, Powell GT, Ghosh M, Gestri G, Antinucci P, Hearn TJ et al (2021) A simple and effective F0 knockout method for rapid screening of behaviour and other complex phenotypes. Elife 10:e59683
Stahl PL, Salmen F, Vickovic S, Lundmark A, Navarro JF, Magnusson J et al (2016) Visualization and analysis of gene expression in tissue sections by spatial transcriptomics. Science 353(6294):78–82
Qian X, Harris KD, Hauling T, Nicoloutsopoulos D, Munoz-Manchado AB, Skene N et al (2020) Probabilistic cell typing enables fine mapping of closely related cell types in situ. Nat Methods 17(1):101–106
Chen WT, Lu A, Craessaerts K, Pavie B, Sala Frigerio C, Corthout N et al (2020) Spatial transcriptomics and in situ sequencing to study alzheimer’s disease. Cell 182(4):976–91 e19
Rodriques SG, Stickels RR, Goeva A, Martin CA, Murray E, Vanderburg CR et al (2019) Slide-seq: a scalable technology for measuring genome-wide expression at high spatial resolution. Science 363(6434):1463–1467
Vickovic S, Eraslan G, Salmen F, Klughammer J, Stenbeck L, Schapiro D et al (2019) High-definition spatial transcriptomics for in situ tissue profiling. Nat Methods 16(10):987–990
Terstappen GC, Meyer AH, Bell RD, Zhang W (2021) Strategies for delivering therapeutics across the blood-brain barrier. Nat Rev Drug Discov 20(5):362–383
Huang PS, Boyken SE, Baker D (2016) The coming of age of de novo protein design. Nature 537(7620):320–327
Jumper J, Evans R, Pritzel A, Green T, Figurnov M, Ronneberger O et al (2021) Highly accurate protein structure prediction with AlphaFold. Nature 596(7873):583–589
Subramaniam S, Kleywegt GJ (2022) A paradigm shift in structural biology. Nat Methods 19(1):20–23
Pan X, Kortemme T (2021) Recent advances in de novo protein design: Principles, methods, and applications. J Biol Chem 296:100558
Renaud JP, Chari A, Ciferri C, Liu WT, Remigy HW, Stark H et al (2018) Cryo-EM in drug discovery: achievements, limitations and prospects. Nat Rev Drug Discov 17(7):471–492
Acknowledgements
We apologize to colleagues whose work could not be cited in this review due to space limitations. We thank Dr. Olga Cherepanova for helpful comments on this manuscript. All Figures were created with BioRender.com.
Funding
This work was supported by funding from the National Institutes of Health (R01 NS117510) and start-up funds from the Cleveland Clinic Foundation to R.L.M.
Author information
Authors and Affiliations
Contributions
RLM wrote the manuscript; LDB, KPV, REQ, and OAC collected literature information and edited the manuscript. All authors reviewed and commented on the manuscript.
Corresponding author
Ethics declarations
Conflict of interest
The authors declare that they have no conflict of interest.
Ethics approval and consent to participate
Not applicable.
Consent for publication
All authors have approved the manuscript for publication at Cellular and Molecular Life Sciences.
Additional information
Publisher's Note
Springer Nature remains neutral with regard to jurisdictional claims in published maps and institutional affiliations.
Rights and permissions
Open Access This article is licensed under a Creative Commons Attribution 4.0 International License, which permits use, sharing, adaptation, distribution and reproduction in any medium or format, as long as you give appropriate credit to the original author(s) and the source, provide a link to the Creative Commons licence, and indicate if changes were made. The images or other third party material in this article are included in the article's Creative Commons licence, unless indicated otherwise in a credit line to the material. If material is not included in the article's Creative Commons licence and your intended use is not permitted by statutory regulation or exceeds the permitted use, you will need to obtain permission directly from the copyright holder. To view a copy of this licence, visit http://creativecommons.org/licenses/by/4.0/.
About this article
Cite this article
Matsuoka, R.L., Buck, L.D., Vajrala, K.P. et al. Historical and current perspectives on blood endothelial cell heterogeneity in the brain. Cell. Mol. Life Sci. 79, 372 (2022). https://doi.org/10.1007/s00018-022-04403-1
Received:
Revised:
Accepted:
Published:
DOI: https://doi.org/10.1007/s00018-022-04403-1