Abstract
Purpose
The goal of this study was to analyze the effect of positive end-expiratory pressure (PEEP), with and without a lung recruitment maneuver, on dead space.
Methods
16 anesthetized patients were sequentially studied in three steps: 1) without PEEP (ZEEP), 2) with 5 cm H2O of PEEP and 3) with 5 cm H2O of PEEP after an alveolar recruitment strategy (ARS). Ventilation was maintained constant. The single breath test of CO2 (SBT-CO2), arterial oxygenation, end-expiratory lung volume (EELV) and respiratory compliance were recorded every 30 min.
Results
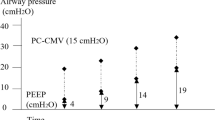
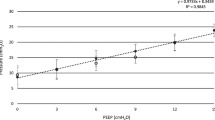
Physiological dead space to tidal volume decreased after ARS (0.45 ±0.01) compared with ZEEP (0.50 ± 0.07, P < 0.05) and PEEP (0.51 ± 0.06, P < 0.05). The elimination of CO2 per breath increased during PEEP (25 ± 3.3 mL · min−1) and ARS (27 ± 3.2 mL · min−1) compared to ZEEP (23 ± 2.6 mL · min−1, P < 0.05), although ARS showed larger values than PEEP(P < 0.05). Pa-etCO2 difference was lower after recruitment (0.9 ± 0.5 kPa, P < 0.05) compared to ZEEP (1.1 ± 0.5 kPa) and PEEP (1.2 ± 0.5 kPa). Slope II increased after ARS (63 ± 11%/L, P < 0.05) compared with ZEEP (46 ± 7.7%/L) and PEEP (56 ± 10%/L). Slope III decreased significantly after recruitment (0.13 ± 0.07 1/L) compared with ZEEP (0.21 ±0.1 1/L) and PEEP (0.18 ± 0.10 1/L). The angle between slope II and III decreased only after ARS. After lung recruitment, PaO2, EELV, and compliance increased significantly compared with ZEEP and PEEP
Conclusion
Lung recruitment improved the efficiency of ventilation in anesthetized patients.
Résumé
Objectif
Analyser l’effet de la pression télé-expiratoire positive (PEEP) sur l’espace mort, avec et sans recrutement pulmonaire.
Méthode
Nous avons réalisé une étude séquentielle en trois étapes auprès de 16 patients anesthésiés: 1) sans PEEP (ZEEP), 2) avec 5 cm H2O de PEEP et 3) avec 5 cm H2O de PEEP à la suite d’une stratégie de recrutement alvéolaire (SRA). La ventilation a été maintenue constante. L’épreuve de l’apnée inspiratoire du CO2, l’oxygénation artérielle, le volume pulmonaire télé-expiratoire (VPTE) et la compliance respiratoire ont été enregistrées toutes les 30 min.
Résultats
Le rapport espace mort/volume courant a été réduit après la SRA (0,45 ±0,01) comparée à la ZEEP (0,50 ± 0,07, P < 0,05) et à la PEEP (0,51 ± 0,06, P < 0,05). Lélimination du CO2 pour chaque respiration a augmenté pendant la PEEP (25 ± 3,3 mL · min−1) et la SRA (21 ± 3,2 mL · min−1) comparées à la ZEEP (23 ± 2,6 mL · min−1, P < 0,05), même si la SRA a présenté des valeurs plus élevées que la PEEP (P < 0,05). La différence Pa-etCO2 a été plus faible après le recrutement (0,9 ± 0,5 kPa, P < 0,05) comparé à la ZEEP (1,1 ± 0,5 kPa) et à la PEEP (1,2 ± 0,5 kPa). La pente II s’est accentuée après la SRA (63 ± 11 %/L, P < 0,05) comparée à la ZEEP (46 ±7,7 %/L) et à la PEEP (56 ± 10 %/L). La pente III s’est abaissée significativement après le recrutement (0,13 ± 0,01 1/L) comparé à la ZEEP (0,21 ±0,11 1/L) et à la PEEP (0,18 ± 0,10 1/L). Langle entre les pentes II et III a diminué seulement après la SRA. Après le recrutement alvéolaire, comparé à la ZEEP et à la PEEP, la PaO2, le VPTE et la compliance ont augmenté significativement.
Conclusion
Le recrutement alvéolaire améliore l’efficacité de la ventilation chez les patients anesthésiés.
Article PDF
Similar content being viewed by others
References
Bendixen HH, Hedley-White J, Chir B, Laver MB. Impaired oxygenation in surgical patients during general anesthesia with controlled ventilation. N Engl J Med 1963; 269: 991–6.
Brismar B, Hedenstierna G, Lundquist H, Strandberg A, Svensson L, Tokios L. Pulmonary densities during anesthesia with muscular relaxation — a proposal of atelectasis. Anesthesiology 1985; 62: 422–8.
Hedenstierna G, Strandberg A, Brismar B, Lundquist H, Svensson L, Tokics L. Functional residual capacity, thoracoabdominal dimensions, and central blood volume during general anesthesia with muscle paralysis and mechanical ventilation. Anesthesiology 1985, 62: 247–54.
Rothen HU, Sporre B, Engberg G, Wegenius G, Hedenstierna G. Re-expansion of atelectasis during general anaesthesia: a computed tomography study. Br J Anaesth 1993; 71: 788–95.
Tusman G, Böhm SH, Vazquez de Anda GF, do Campo JL, Lachmann B. ‘Alveolar recruitment strategy’ improves arterial oxygenation during general anaesthesia. Br J Anaesth 1999; 82: 8–13.
Amato MB, Barbas CS, Medeiros DM, et al. Effect of a protective-ventilation strategy on mortality in the acute respiratory distress syndrome. N Engl J Med 1998; 338: 347–54.
Böhm SH, Vazquez de Anda GF, Lachmann B. The open lung concept.In: Vincent JL (Ed.). Yearbook of Intensive Care and Emergency Medicine, 2nd ed. Berlin, Heidelberg, New York: Springer-Verlag; 1999: 430–40.
Fletcher R, Jonson B, Cumming G, Brew J. The concept of deadspace with special reference to the single breath test for carbon dioxide. Br J Anaesth 1981; 53: 77–88.
Hofbrand BL. The expiratory capnogram: a measure of ventilation-perfusion inequalities. Thorax 1966; 21: 518–24.
Fletcher R, Jonson B. Deadspace and the single breath test for carbon dioxide during anaesthesia and artificial ventilation. Effects of tidal volume and frequency of respiration. Br J Anaesth 1984; 56: 109–19.
Tusman G, Böhm SH, Tempra A, et al. Effects of recruitment maneuver on atelectasis in anesthetized children. Anesthesiology 2003; 98: 14–22.
Naureckas ET, Dawson CA, Gerber BS, et al. Airway reopening pressure in isolated rat lungs. J Appl Physiol 1994; 76: 1372–7.
Bergman NA, Tien YK. Contribution of the closure of pulmonary units to impaired oxygenation during anesthesia. Anesthesiology 1983; 59: 395–401.
Verbeken EK, Cauberghs M, Mertens I, Clement J, Lauweryns JM, Van de Woestijne KP. The senile lung. Comparison with normal and emphysematous lungs. 1. Structural aspects. Chest 1992; 101: 793–9.
You B, Peslin R, Duvivier C, Vu VD, Grilliat JP. Expiratory capnography in asthma: evaluation of various shape indices. Eur Respir J 1994; 7: 318–23.
Schwardt JD, Neufeld GR, Baumgardner JE, Scherer PW. Noninvasive recovery of acinar anatomic information from CO2 expirograms. Ann Biomed Eng 1994; 22: 293–306.
Ream RS, Schreiner MS, Neff JD, et al. Volumetric capnography in children. Influence of growth on the alveolar plateau slope. Anesthesiology 1995; 82: 64–73.
Schwardt JD, Gobran SR, Neufeld GR, Aukburg SJ, Scherer PW. Sensitivity of CO2 washout to changes in acinar structure in a single-path model of lung airways. Ann Biomed Eng 1991; 19: 679–97.
Author information
Authors and Affiliations
Corresponding author
Rights and permissions
About this article
Cite this article
Tusman, G., Böhm, S.H., Suarez-Sipmann, F. et al. Alveolar recruitment improves ventilatory efficiency of the lungs during anesthesia. Can J Anesth 51, 723–727 (2004). https://doi.org/10.1007/BF03018433
Accepted:
Issue Date:
DOI: https://doi.org/10.1007/BF03018433