Abstract
Background
Up to 40% of patients with epilepsy experience seizures despite treatment with antiepileptic drugs; however, branched-chain amino acid (BCAA) supplementation has shown promise in treating refractory epilepsy.
Objectives
The purpose of this systematic review was to evaluate all published studies that investigated the effects of BCAAs on seizures, emphasizing therapeutic efficacy and possible underlying mechanisms.
Methods
On 31 January, 2017, the following databases were searched for relevant studies: MEDLINE (OvidSP), EMBASE (OvidSP), Scopus (Elsevier), the Cochrane Library, and the unindexed material in PubMed (National Library of Medicine/National Institutes of Health). The searches were repeated in all databases on 18 February, 2019. We only included full-length preclinical and clinical studies that were published in the English language that examined the effects of BCAA administration on seizures.
Results
Eleven of 2045 studies met our inclusion criteria: ten studies were conducted in animal models and one study in human subjects. Seven seizure models were investigated: the strychnine (one study), pentylenetetrazole (two studies), flurothyl (one study), picrotoxin (two studies), genetic absence epilepsy in rats (one study), kainic acid (two studies), and methionine sulfoximine (one study) paradigms. Three studies investigated the effect of a BCAA mixture whereas the other studies explored the effects of individual BCAAs on seizures. In most animal models and in humans, BCAAs had potent anti-seizure effects. However, in the methionine sulfoximine model, long-term BCAA supplementation worsened seizure propagation and caused neuron loss, and in the genetic absence epilepsy in rats model, BCAAs exhibited pro-seizure effects.
Conclusions
The contradictory effects of BCAAs on seizure activity likely reflect differences in the complex mechanisms that underlie seizure disorders. Some of these mechanisms are likely mediated by BCAA’s effects on glucose, glutamate, glutamine, and ammonia metabolism, activation of the mechanistic target of rapamycin signaling pathway, and their effects on aromatic amino acid transport and neurotransmitter synthesis. We propose that a better understanding of mechanisms by which BCAAs affect seizures and neuronal viability is needed to advance the field of BCAA supplementation in epilepsy.




Similar content being viewed by others
References
Chang BS, Lowenstein DH. Epilepsy. N Engl J Med. 2003;349(13):1257–66.
ILAE Commission Report. The epidemiology of the epilepsies: future directions. International League Against Epilepsy. Epilepsia. 1997;38(5):614–8.
Begley CE, Famulari M, Annegers JF, Lairson DR, Reynolds TF, Coan S, et al. The cost of epilepsy in the United States: an estimate from population-based clinical and survey data. Epilepsia. 2000;41(3):342–51.
de Lanerolle NC, Lee TS, Spencer DD. Histopathology of human epilepsy. In: Noebels JL, Avoli M, Rogawski MA, Olsen RW, Delgado-Escueta AV, editors. Jasper’s basic mechanisms of the epilepsies. 4th ed. Bethesda: National Center for Biotechnology Information; 2012.
Annegers J. The treatment of epilepsy: principles and practice. 2nd ed. Baltimore: Williams and Wilkins; 1996.
Eid T, Gruenbaum SE, Dhaher R, Lee TW, Zhou Y, Danbolt NC. The glutamate-glutamine cycle in epilepsy. Adv Neurobiol. 2016;13:351–400.
McCormick DA, Contreras D. On the cellular and network bases of epileptic seizures. Annu Rev Physiol. 2001;63:815–46.
Zimmerman G, Njunting M, Ivens S, Tolner EA, Behrens CJ, Gross M, et al. Acetylcholine-induced seizure-like activity and modified cholinergic gene expression in chronically epileptic rats. Eur J Neuurosci. 2008;27(4):965–75.
Eid T, Thomas MJ, Spencer DD, Runden-Pran E, Lai JC, Malthankar GV, et al. Loss of glutamine synthetase in the human epileptogenic hippocampus: possible mechanism for raised extracellular glutamate in mesial temporal lobe epilepsy. Lancet. 2004;363(9402):28–37.
Yudkoff M. Brain metabolism of branched-chain amino acids. Glia. 1997;21(1):92–8.
Fernstrom JD. Branched-chain amino acids and brain function. J Nutr. 2005;135(6):1539S–46S.
Matsuo H, Tsukada S, Nakata T, Chairoungdua A, Kim DK, Cha SH, et al. Expression of a system L neutral amino acid transporter at the blood–brain barrier. Neuroreport. 2000;11(16):3507–11.
Takanaga H, Mackenzie B, Peng JB, Hediger MA. Characterization of a branched-chain amino-acid transporter SBAT1 (SLC6A15) that is expressed in human brain. Biochem Biophys Res Commun. 2005;337(3):892–900.
Giorgi FS, Pizzanelli C, Biagioni F, Murri L, Fornai F. The role of norepinephrine in epilepsy: from the bench to the bedside. Neurosci Biobehav Rev. 2004;28(5):507–24.
Kumar U, Medel-Matus JS, Redwine HM, Shin D, Hensler JG, Sankar R, et al. Effects of selective serotonin and norepinephrine reuptake inhibitors on depressive- and impulsive-like behaviors and on monoamine transmission in experimental temporal lobe epilepsy. Epilepsia. 2016;57(3):506–15.
Svob Strac D, Pivac N, Smolders IJ, Fogel WA, De Deurwaerdere P, Di Giovanni G. Monoaminergic mechanisms in epilepsy may offer innovative therapeutic opportunity for monoaminergic multi-target drugs. Front Neurosci. 2016;10(10):492.
Fernstrom JD. Aromatic amino acids and monoamine synthesis in the central nervous system: influence of the diet. J Nutr Biochem. 1990;1(10):508–17.
Smith QR, Momma S, Aoyagi M, Rapoport SI. Kinetics of neutral amino acid transport across the blood–brain barrier. J Neurochem. 1987;49(5):1651–8.
Pardridge WM, Choi TB. Neutral amino acid transport at the human blood–brain barrier. Fed Proc. 1986;45(7):2073–8.
Fernstrom MH, Volk EA, Fernstrom JD. In vivo inhibition of tyrosine uptake into rat retina by large neutral but not acidic amino acids. Am J Physiol. 1986;251(4 Pt 1):E393–9.
Blomstrand E, Eliasson J, Karlsson HK, Kohnke R. Branched-chain amino acids activate key enzymes in protein synthesis after physical exercise. J Nutr. 2006;136(1 Suppl.):269S–73S.
Rothman DL, De Feyter HM, Maciejewski PK, Behar KL. Is there in vivo evidence for amino acid shuttles carrying ammonia from neurons to astrocytes? Neurochem Res. 2012;37(11):2597–612.
Lynch CJ, Adams SH. Branched-chain amino acids in metabolic signalling and insulin resistance. Nat Rev Endocrinol. 2014;10(12):723–36.
De Simone R, Vissicchio F, Mingarelli C, De Nuccio C, Visentin S, Ajmone-Cat MA, et al. Branched-chain amino acids influence the immune properties of microglial cells and their responsiveness to pro-inflammatory signals. Biochim Biophys Acta. 2013;1832(5):650–9.
Scarna A, McTavish SF, Cowen PJ, Goodwin GM, Rogers RD. The effects of a branched chain amino acid mixture supplemented with tryptophan on biochemical indices of neurotransmitter function and decision-making. Psychopharmacology (Berl). 2005;179(4):761–8.
Contrusciere V, Paradisi S, Matteucci A, Malchiodi-Albedi F. Branched-chain amino acids induce neurotoxicity in rat cortical cultures. Neurotox Res. 2010;17(4):392–8.
Testa D, Caraceni T, Fetoni V. Branched-chain amino acids in the treatment of amyotrophic lateral sclerosis. J Neurol. 1989;236(8):445–7.
Mayers JR, Vander Heiden MG. BCAT1 defines gliomas by IDH status. Nat Med. 2013;19(7):816–7.
Bastone A, Micheli A, Beghi E, Salmona M. The imbalance of brain large-chain aminoacid availability in amyotrophic lateral sclerosis patients treated with high doses of branched-chain aminoacids. Neurochem Int. 1995;27(6):467–72.
Aquilani R, Iadarola P, Contardi A, Boselli M, Verri M, Pastoris O, et al. Branched-chain amino acids enhance the cognitive recovery of patients with severe traumatic brain injury. Arch Phys Med Rehabil. 2005;86(9):1729–35.
Korein J, Sansaricq C, Kalmijn M, Honig J, Lange B. Maple syrup urine disease: clinical, eeg, and plasma amino acid correlations with a theoretical mechanism of acute neurotoxicity. Int J Neurosci. 1994;79(1–2):21–45.
Carlson H, Ronne-Engstrom E, Ungerstedt U, Hillered L. Seizure related elevations of extracellular amino acids in human focal epilepsy. Neurosci Lett. 1992;140(1):30–2.
Gietzen DW, Dixon KD, Truong BG, Jones AC, Barrett JA, Washburn DS. Indispensable amino acid deficiency and increased seizure susceptibility in rats. Am J Physiol. 1996;271(1 Pt 2):R18–24.
Eid T, Ghosh A, Wang Y, Beckstrom H, Zaveri HP, Lee TS, et al. Recurrent seizures and brain pathology after inhibition of glutamine synthetase in the hippocampus in rats. Brain. 2008;131(Pt 8):2061–70.
Gruenbaum SE, Dhaher R, Rapuano A, Zaveri HP, Tang A, de Lanerolle N, et al. Effects of branched-chain amino acid supplementation on spontaneous seizures and neuronal viability in a model of mesial temporal lobe epilepsy. J Neurosurg Anesthesiol. 2019;31(2):247–56.
Rho JM, Donevan SD, Rogawski MA. Direct activation of GABAA receptors by barbiturates in cultured rat hippocampal neurons. J Physiol. 1996;497(Pt 2):509–22.
Qian H, Pan Y, Zhu Y, Khalili P. Picrotoxin accelerates relaxation of GABAC receptors. Mol Pharmacol. 2005;67(2):470–9.
Skeie B, Petersen AJ, Manner T, Askanazi J, Jellum E, Steen PA. Branched-chain amino acids increase the seizure threshold to picrotoxin in rats. Pharmacol Biochem Behav. 1992;43(3):669–71.
Skeie B, Petersen AJ, Manner T, Askanazi J, Steen PA. Effects of valine, leucine, isoleucine, and a balanced amino acid solution on the seizure threshold to picrotoxin in rats. Pharmacol Biochem Behav. 1994;48(1):101–3.
Kandratavicius L, Balista PA, Lopes-Aguiar C, Ruggiero RN, Umeoka EH, Garcia-Cairasco N, et al. Animal models of epilepsy: use and limitations. Neuropsychiatr Dis Treat. 2014;10:1693–705.
Bogdanov NN, Poletaeva II, Popova NV. Pentylenetetrazol and strychnine convulsions in brain weight selected mice. Seizure. 1997;6(2):135–8.
Curtis DR, Duggan AW, Johnston GAR. The specificity of strychnine as a glycine antagonist in the mammalian spinal cord. Exp Brain Res. 1971;12(5):547–65.
Loscher W. Animal models of intractable epilepsy. Prog Neurobiol. 1997;53(2):239–58.
Jeske J, Misterek K, Dorociak A. Some pharmacological effects of amino acid 4 aminoantipyrine derivatives. Bull Pol Med Sci Hist. 1974;15:II.
Dhir A. Pentylenetetrazol (PTZ) kindling model of epilepsy. Curr Protoc Neurosci. 2012;Chapter 9:Unit 9.37.
Dufour F, Nalecz KA, Nalecz MJ, Nehlig A. Modulation of pentylenetetrazol-induced seizure activity by branched-chain amino acids and alpha-ketoisocaproate. Brain Res. 1999;815(2):400–4.
Pinto JMB, Maher TJ. Administration of aspartame potentiates pentylenetetrazole- and fluorothyl-induced seizures in mice. Neuropharmacology. 1988;27(1):51–5.
Kadiyala SB, Yannix JQ, Nalwalk JW, Papandrea D, Beyer BS, Herron BJ, et al. Eight flurothyl-induced generalized seizures lead to the rapid evolution of spontaneous seizures in mice: a model of epileptogenesis with seizure remission. J Neurosci. 2016;36(28):7485–96.
Sperber EF, Veliskova J, Germano IM, Friedman LK, Moshe SL. Age-dependent vulnerability to seizures. Adv Neurol. 1999;79:161–9.
Hashimoto Y, Araki H, Suemaru K, Gomita Y. Effects of drugs acting on the GABA-benzodiazepine receptor complex on flurothyl-induced seizures in Mongolian gerbils. Eur J Pharmacol. 2006;536(3):241–7.
Marescaux C, Vergnes M, Depaulis A. Genetic absence epilepsy in rats from Strasbourg—a review. J Neural Transm Suppl. 1992;35:37–69.
Snead OC 3rd. Basic mechanisms of generalized absence seizures. Ann Neurol. 1995;37(2):146–57.
Dufour F, Nalecz KA, Nalecz MJ, Nehlig A. Metabolic approach of absence seizures in a genetic model of absence epilepsy, the GAERS: Study of the leucine-glutamate cycle. J Neurosci Res. 2001;66(5):923–30.
Dufour F, Nalecz KA, Nalecz MJ, Nehlig A. Modulation of absence seizures by branched-chain amino acids: correlation with brain amino acid concentrations. Neurosci Res. 2001;40(3):255–63.
Zhang XM, Zhu J. Kainic Acid-induced neurotoxicity: targeting glial responses and glia-derived cytokines. Curr Neuropharmacol. 2011;9(2):388–98.
Levesque M, Avoli M. The kainic acid model of temporal lobe epilepsy. Neurosci Biobehav Rev. 2013;37(10 Pt 2):2887–99.
Hartman AL, Santos P, O’Riordan KJ, Stafstrom CE, Hardwick JM. Potent anti-seizure effects of d-leucine. Neurobiol Dis. 2015;82:46–53.
Holden K, Hartman AL. d-Leucine: evaluation in an epilepsy model. Epilepsy Behav. 2018;78:202–9.
Yudkoff M, Daikhin Y, Nissim I, Lazarow A, Nissim I. Ketogenic diet, brain glutamate metabolism and seizure control. Prostaglandins Leukot Essent Fatty Acids. 2004;70(3):277–85.
Evangeliou A, Spilioti M, Doulioglou V, Kalaidopoulou P, Ilias A, Skarpalezou A, et al. Branched chain amino acids as adjunctive therapy to ketogenic diet in epilepsy: pilot study and hypothesis. J Child Neurol. 2009;24(10):1268–72.
During MJ, Spencer DD. Extracellular hippocampal glutamate and spontaneous seizure in the conscious human brain. Lancet. 1993;341(8861):1607–10.
Hutson SM, Lieth E, LaNoue KF. Function of leucine in excitatory neurotransmitter metabolism in the central nervous system. J Nutr. 2001;131(3):846S–50S.
Hutson SM, Berkich D, Drown P, Xu B, Aschner M, LaNoue KF. Role of branched-chain aminotransferase isoenzymes and gabapentin in neurotransmitter metabolism. J Neurochem. 1998;71(2):863–74.
Norenberg MD, Martinez-Hernandez A. Fine structural localization of glutamine synthetase in astrocytes of rat brain. Brain Res. 1979;161(2):303–10.
Su TZ, Campbell GW, Oxender DL. Glutamine transport in cerebellar granule cells in culture. Brain Res. 1997;757(1):69–78.
Hogstad S, Svenneby G, Torgner IA, Kvamme E, Hertz L, Schousboe A. Glutaminase in neurons and astrocytes cultured from mouse brain: kinetic properties and effects of phosphate, glutamate, and ammonia. Neurochem Res. 1988;13(4):383–8.
Broer S, Brookes N. Transfer of glutamine between astrocytes and neurons. J Neurochem. 2001;77(3):705–19.
Plaitakis A. Abnormal glutamatergic mechanisms and branched-chain aminoacids in amyotrophic lateral sclerosis. Lancet. 1989;1(8630):157.
Plaitakis A, Smith J, Mandeli J, Yahr MD. Pilot trial of branched-chain aminoacids in amyotrophic lateral sclerosis. Lancet. 1988;1(8593):1015–8.
Dhaher R, Damisah EC, Wang H, Gruenbaum SE, Ong C, Zaveri HP, et al. 5-aminovaleric acid suppresses the development of severe seizures in the methionine sulfoximine model of mesial temporal lobe epilepsy. Neurobiol Dis. 2014;67:18–23.
Fritsche E, Humm A, Huber R. The ligand-induced structural changes of human l-arginine:glycine amidinotransferase: a mutational and crystallographic study. J Biol Chem. 1999;274(5):3026–32.
Nanavati SM, Silverman RB. Design of potential anticonvulsant agents: mechanistic classification of GABA aminotransferase inactivators. J Med Chem. 1989;32(11):2413–21.
Tasaka J, Sakai S, Tosaka T, Yoshihama I. Glial uptake system of GABA distinct from that of taurine in the bullfrog sympathetic ganglia. Neurochem Res. 1989;14(3):271–7.
Levy RG, Cooper PN, Giri P. Ketogenic diet and other dietary treatments for epilepsy. Cochrane Database Syst Rev. 2012;3:CD001903.
Kinsman SL, Vining EP, Quaskey SA, Mellits D, Freeman JM. Efficacy of the ketogenic diet for intractable seizure disorders: review of 58 cases. Epilepsia. 1992;33(6):1132–6.
Bixel MG, Hamprecht B. Generation of ketone bodies from leucine by cultured astroglial cells. J Neurochem. 1995;65(6):2450–61.
Yudkoff M, Daikhin Y, Nissim I, Lazarow A, Nissim I. Brain amino acid metabolism and ketosis. J Neurosci Res. 2001;66(2):272–81.
Yudkoff M, Daikhin Y, Nissim I, Lazarow A, Nissim I. Ketogenic diet, amino acid metabolism, and seizure control. J Neurosci Res. 2001;66(5):931–40.
Jirapinyo P, Kankirawatana P, Densupsoontorn N, Thamonsiri N, Wongarn R. High plasma branched-chain amino acids: aromatic amino acids ratio in children on the ketogenic diet: a mechanism in controlling epilepsy. J Med Assoc Thail. 2004;87(4):432–7.
Cota D, Proulx K, Smith KA, Kozma SC, Thomas G, Woods SC, et al. Hypothalamic mTOR signaling regulates food intake. Science. 2006;312(5775):927–30.
Arrieta-Cruz I, Su Y, Gutiérrez-Juárez R. Suppression of endogenous glucose production by isoleucine and valine and impact of diet composition. Nutrients. 2016;8(2):79.
Arieff AI, Doerner T, Zelig H, Massry SG. Mechanisms of seizures and coma in hypoglycemia evidence for a direct effect of insulin on electrolyte transport in brain. J Clin Investig. 1974;54(3):654–63.
Stafstrom CE. Hyperglycemia lowers seizure threshold. Epilepsy Curr. 2003;3(4):148–9.
Koltai M, Minker E. Changes of electro-shock seizure threshold in alloxan diabetic rats. Experientia. 1975;31(11):1369.
Schwechter EM, Veliskova J, Velisek L. Correlation between extracellular glucose and seizure susceptibility in adult rats. Ann Neurol. 2003;53(1):91–101.
Berkovic SF, Johns JA, Bladin PF. Focal seizures and systemic metabolic disorders. Aust N Z J Med. 1982;12(6):620–3.
Huang CW, Huang CC, Cheng JT, Tsai JJ, Wu SN. Glucose and hippocampal neuronal excitability: role of ATP-sensitive potassium channels. J Neurosci Res. 2007;85(7):1468–77.
Weber JD, Gutmann DH. Deconvoluting mTOR biology. Cell Cycle. 2012;11(2):236–48.
Cho CH. Frontier of epilepsy research: mTOR signaling pathway. Exp Mol Med. 2011;43(5):231–74.
Yang Z, Ming XF. mTOR signalling: the molecular interface connecting metabolic stress, aging and cardiovascular diseases. Obes Rev. 2012;13(Suppl. 2):58–68.
Meng X-F, Yu J-T, Song J-H, Chi S, Tan L. Role of the mTOR signaling pathway in epilepsy. J Neurol Sci. 2013;332(1):4–15.
Amara S, Fontana A. Excitatory amino acid transporters: keeping up with glutamate. Neurochem Int. 2002;41(5):313–8.
Almilaji A, Pakladok T, Guo A, Munoz C, Föller M, Lang F. Regulation of the glutamate transporter EAAT3 by mammalian target of rapamycin mTOR. Biochem Biophys Res Commun. 2012;421(2):159–63.
Erecińska M, Nelson D. Activation of glutamate dehydrogenase by leucine and its nonmetabolizable analogue in rat brain synaptosomes. J Neurochem. 1990;54(4):1335–43.
Sugimoto H, Koehler RC, Wilson DA, Brusilow SW, Traystman RJ. Methionine sulfoximine, a glutamine synthetase inhibitor, attenuates increased extracellular potassium activity during acute hyperammonemia. J Cereb Blood Flow Metab. 1997;17(1):44–9.
Cavus I, Kasoff WS, Cassaday MP, Jacob R, Gueorguieva R, Sherwin RS, et al. Extracellular metabolites in the cortex and hippocampus of epileptic patients. Ann Neurol. 2005;57(2):226–35.
Laake JH, Slyngstad TA, Haug FM, Ottersen OP. Glutamine from glial cells is essential for the maintenance of the nerve terminal pool of glutamate: immunogold evidence from hippocampal slice cultures. J Neurochem. 1995;65(2):871–81.
Erecinska M, Nelson D. Activation of glutamate dehydrogenase by leucine and its nonmetabolizable analogue in rat brain synaptosomes. J Neurochem. 1990;54(4):1335–43.
Burrage LC, Nagamani SC, Campeau PM, Lee BH. Branched-chain amino acid metabolism: from rare Mendelian diseases to more common disorders. Hum Mol Genet. 2014;23(R1):R1–8.
Coulter DA, Eid T. Astrocytic regulation of glutamate homeostasis in epilepsy. Glia. 2012;60(8):1215–26.
Tripathi PP, Bozzi Y. The role of dopaminergic and serotonergic systems in neurodevelopmental disorders: a focus on epilepsy and seizure susceptibility. Bioimpacts. 2015;5(2):97–102.
Yan QS, Mishra PK, Burger RL, Bettendorf AF, Jobe PC, Dailey JW. Evidence that carbamazepine and antiepilepsirine may produce a component of their anticonvulsant effects by activating serotonergic neurons in genetically epilepsy-prone rats. J Pharmacol Exp Ther. 1992;261(2):652–9.
Ahmad S, Fowler LJ, Whitton PS. Lamotrigine, carbamazepine and phenytoin differentially alter extracellular levels of 5-hydroxytryptamine, dopamine and amino acids. Epilepsy Res. 2005;63(2–3):141–9.
Kanner AM. Association between selective serotonin-reuptake inhibitor antidepressants and increased risk of poststroke epilepsy. Mayo Clin Proc. 2017;92(2):179–81.
Favale E, Rubino V, Mainardi P, Lunardi G, Albano C. Anticonvulsant effect of fluoxetine in humans. Neurology. 1995;45(10):1926–7.
Krahl SE, Clark KB, Smith DC, Browning RA. Locus coeruleus lesions suppress the seizure-attenuating effects of vagus nerve stimulation. Epilepsia. 1998;39(7):709–14.
Suryawan A, Hawes JW, Harris RA, Shimomura Y, Jenkins AE, Hutson SM. A molecular model of human branched-chain amino acid metabolism. Am J Clin Nutr. 1998;68(1):72–81.
Daikhin Y, Yudkoff M. Compartmentation of brain glutamate metabolism in neurons and glia. J Nutr. 2000;130(4S Suppl.):1026s–31s.
Pardridge WM. Brain metabolism: a perspective from the blood–brain barrier. Physiol Rev. 1983;63(4):1481–535.
Young SN, Ervin FR, Pihl RO, Finn P. Biochemical aspects of tryptophan depletion in primates. Psychopharmacology (Berl). 1989;98(4):508–11.
Williams WA, Shoaf SE, Hommer D, Rawlings R, Linnoila M. Effects of acute tryptophan depletion on plasma and cerebrospinal fluid tryptophan and 5-hydroxyindoleacetic acid in normal volunteers. J Neurochem. 1999;72(4):1641–7.
Fernstrom MH, Fernstrom JD. Acute tyrosine depletion reduces tyrosine hydroxylation rate in rat central nervous system. Life Sci. 1995;57(9):97–102.
Smith GS, Barrett FS, Joo JH, Nassery N, Savonenko A, Sodums DJ, et al. Molecular imaging of serotonin degeneration in mild cognitive impairment. Neurobiol Dis. 2017;105:33–41.
von Coelln R, Thomas B, Savitt JM, Lim KL, Sasaki M, Hess EJ, et al. Loss of locus coeruleus neurons and reduced startle in parkin null mice. Proc Natl Acad Sci. 2004;101(29):10744–9.
Vilela TC, Scaini G, Furlanetto CB, Pasquali MA, Santos JP, Gelain DP, et al. Apoptotic signaling pathways induced by acute administration of branched-chain amino acids in an animal model of maple syrup urine disease. Metab Brain Dis. 2017;32(1):115–22.
Tonjes M, Barbus S, Park YJ, Wang W, Schlotter M, Lindroth AM, et al. BCAT1 promotes cell proliferation through amino acid catabolism in gliomas carrying wild-type IDH1. Nat Med. 2013;19(7):901–8.
Yudkoff M, Daikhin Y, Nissim I, Horyn O, Lazarow A, Nissim I. Metabolism of brain amino acids following pentylenetetrazole treatment. Epilepsy Res. 2003;53(1–2):151–62.
Treacy E, Clow CL, Reade TR, Chitayat D, Mamer OA, Scriver CR. Maple syrup urine disease: Interrelations between branched-chain amino-, oxo- and hydroxyacids; implications for treatment; associations with CNS dysmyelination. J Inherit Metab Dis. 1992;15(1):1–35.
Jouvet P, Rustin P, Taylor DL, Pocock JM, Felderhoff-Mueser U, Mazarakis ND, et al. Branched chain amino acids induce apoptosis in neural cells without mitochondrial membrane depolarization or cytochrome c release: implications for neurological impairment associated with maple syrup urine disease. Mol Biol Cell. 2000;11(5):1919–32.
Bridi R, Araldi JN, Sgarbi MB, Testa CG, Durigon K, Wajner M, et al. Induction of oxidative stress in rat brain by the metabolites accumulating in maple syrup urine disease. Int J Dev Neurosci. 2003;21(6):327–32.
Bible E. Neuro-oncology: BCAT1 promotes cell proliferation in aggressive gliomas. Nat Rev Neurol. 2013;9(8):420.
Schauwecker PE. The effects of glycemic control on seizures and seizure-induced excitotoxic cell death. BMC Neurosci. 2012;13:94.
Wang X. Nonketotic hyperglycemia-related epileptic seizures. Chin Neurosurg J. 2017;3(1):16.
Hennis A, Corbin D, Fraser H. Focal seizures and non-ketotic hyperglycaemia. J Neurol Neurosurg Psychiatry. 1992;55(3):195–7.
Yoon M-S. The emerging role of branched-chain amino acids in insulin resistance and metabolism. Nutrients. 2016;8(7):E405.
Vary TC, Lynch CJ. Nutrient signaling components controlling protein synthesis in striated muscle. J Nutr. 2007;137(8):1835–43.
Acknowledgements
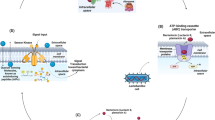
The authors gratefully acknowledge Garrett Sendlewski (Yale Media Laboratory Associate) for his outstanding illustrative work for Fig. 4, and Alexandria Brackett, MA, MLIS (Clinical Librarian) for her assistance in performing the literature review.
Author information
Authors and Affiliations
Corresponding author
Ethics declarations
Funding
Tore Eid and Roni Dhaher are supported by grants from the National Institute of Health (NIH): NINDS K08 NS058674 and R01 NS070824. Tore Eid is supported by an Innovator Award from Citizens United for Research in Epilepsy (CURE). Shaun E. Gruen is supported by grants from the NIH: T32 GM086287 and the Foundation of Anesthesia Education and Research (FAER). This work was also made possible by a grant from the National Center for Advancing Translational Science (NCATS; UL1 TR000142), a component of the NIH and the NIH roadmap for Medical Research. Its contents are solely the responsibility of the authors and do not necessarily represent the official view of the NIH.
Conflict of interest
Shaun E. Gruenbaum, Eric C. Chen, Mani Ratnesh S. Sandhu, Ketaki Deshpande, Roni Dhaher, Denise Hersey, and Tore Eid have no conflicts of interest that are directly relevant to the content of this article.
Electronic supplementary material
Below is the link to the electronic supplementary material.
Rights and permissions
About this article
Cite this article
Gruenbaum, S.E., Chen, E.C., Sandhu, M.R.S. et al. Branched-Chain Amino Acids and Seizures: A Systematic Review of the Literature. CNS Drugs 33, 755–770 (2019). https://doi.org/10.1007/s40263-019-00650-2
Published:
Issue Date:
DOI: https://doi.org/10.1007/s40263-019-00650-2